doi: /jor.20426
|
|
|
- Scot Clark
- 5 years ago
- Views:
Transcription
1 doi: /jor.20426
2 Title Repair of large osteochondral defects with allogeneic cartilaginous aggregates formed from bone marrow-derived cells using RWV bioreactor Tomokazu Yoshioka 1,MD, Hajime Mishima 1,MD,PhD Yoshimi Ohyabu 2,3, Shinsuke Sakai 1,MD Hiroshi Akaogi 1,MD,PhD Tomoo Ishii 1,MD,PhD Naoyuki Ochiai 1,MD,PhD Hiroko Kojima 2,PhD Junzo Tanaka 3,PhD Toshimasa Uemura 2,3,PhD 1. Department of Orthopaedic Surgery, Control of Musculoskeltal System, Advanced Biomedical Applications, Graduate School of Comprehensive Human Sciences, University of Tsukuba,1-1-1 Tennodai, Tsukuba, Ibaraki, , Japan. 2. Nanotechnology Research Institute, AIST (National Institute of Advanced Industrial Science and Technology), Higashi, Tsukuba, Ibaraki, , Japan 1
3 3. Biomaterials Center, National Institute for Materials Science (NIMS), 1-1 Namiki, Tsukuba Ibaraki, , Japan Corresponding author: Hajime Mishima, MD, PhD Tel: Fax: address: 2
4 Abstract Objective: To examine the technique of regenerating cartilage tissue from bone marrow-derived cells by three-dimensional (3-D) culture using the rotating wall vessel (RWV) bioreactor. Methods: 3-D and cylindrical aggregates of allogeneic cartilage with dimensions of 10mm x 5mm (height x diameter) formed by the RWV bioreactor were transplanted into osteochondral defects of Japanese white rabbits (Group-T, n=15). For the control, some osteochondral defects were left empty (Group-C, n=18). At 4, 8, and 12 weeks post-implantation, the reparative tissues were evaluated macroscopically, histologically, and biochemically. Results: In Group-T at as early as 4 weeks, histological observation, especially via safranin-o staining, suggested that the reparative tissues resembled hyaline cartilage. And we observed no fibrous tissues between reparative tissue and adjacent normal tissues. In the deeper portion of the bony compartment, the osseous tissues were well remodeled. At 4 and 8 weeks post-implantation, the mean histological score of Group-T was significantly better than that of Group-C (P<0.05). The glycosaminoglycans (GAG) / DNA ratio in both groups increased gradually from 4 to 8 weeks and then decreased from 8 to 12 weeks. 3
5 Conclusions: We here in report the first successful regeneration of cartilage in osteochondral defects in vivo using allogeneic cartilaginous aggregates derived from bone marrow-derived cells by 3-D culture using the RWV bioreactor. Key Words: Cartilage, RWV bioreactor, Mesenchymal stem cells, 3-D culture, Tissue engineering 4
6 Introduction Artificial cartilage fabricated in vitro using techniques of tissue engineering has been employed to repair and regenerate damaged cartilage 1,2,3. There have been numerous reports in this field on experiments with animals or clinical cases 4,5,6. However, no treatment has been reported to regenerate either a complete or a long-lasting hyaline cartilage. Our research group has recently examined the application of a rotating wall vessel (RWV) bioreactor that simulates a micro-gravity environment with a low shear stress for regenerating cartilage tissue and successfully established a three-dimensional (3-D) cell culture technique for the formation of large and homogenous cartilaginous aggregates from bone marrow-derived cells without using a scaffold 7. This bioreactor generates stress through the horizontal rotation of a cylindrical vessel equipped with a gas exchange membrane. The bioreactor compensates for the effect of gravity, resulting in homogenous cell growth and differentiation without sinking, and the cells aggregate and form 3-D tissue 8. Figure.1, A shows a cartilaginous aggregate formed in the RWV bioreactor according to the method described in our previous paper 7. Fig.1B shows the result of safranin-o staining of a section of the formed cartilaginous aggregate, which shows that the aggregate is large and homogenous and simulates hyaline cartilage with abundant extracellular matrix. The purpose of this study is to evaluate the usefulness of transplanting cartilaginous aggregates formed from rabbit bone marrow-derived cells using RWV bioreactor. 1
7 Materials and Methods Cell culture and formation of cartilage aggregates: All experiments were performed in accordance with the guidelines of the Japanese Government for the care and use of laboratory animals. Bone marrow-derived cells were collected from the femurs and tibias of six female 12-day-old Japanese white rabbits. The femurs and tibias were removed aseptically, cleaned of soft tissues, and washed three times in PBS with antibiotics. Then both ends were removed from the epiphyses, and the marrow was flushed out from the modularly cavity using 20ml of standard medium. Next, the cell suspension was distributed through thirty T-75 culture flasks (BD) with 15 ml of a standard medium and then cultured in a humidified atmosphere containing 95% air and 5% CO 2. The standard medium consisted of Dulbecco s Modified Eagle s Medium (DMEM; Sigma) containing 10% fetal bovine serum (FBS; Sigma) and antibiotics (antibiotic-antimicotic: Gibco BRL). Approximately 3 weeks after the seeding, when the adherent cells grew become over-confluent, at which time they were subcultured by trypsinization, and then resuspended in a rotating medium. The rotating medium consisted of DMEM containing 10%FBS, 50μg/ml of ascorbic acid (WAKO), 40μ g/ml of L-proline, ITS culture supplement (BD), 10-7 M dexamethasone (Sigma), 10ng/ml of TGF-β 3 (Sigma), and antibiotics (antibiotic-antimicotic:gibco BRL). Then, 10ml of the cell suspension ( x 10 7 cells) was seeded into the RWV bioreactor (RCCS TM -4D system 2
8 with 10 ml disposable vessels, Synthecon Incorporated, TX) in a CO 2 incubator, and the rotatory culture was performed for 1 week. The speed of rotation was adjusted manually in order to balance the aggregation of cells in the vessel without allowing the aggregate to sink. Animal model: Thirty-six female 10-week-old Japanese white rabbits (Tokyo Experimental Animals, Tokyo, Japan), weighing 2.3 to 2.5kg, were used in this study. The experiments were approved by the University Committee for Animal Experimentation. All operations were performed on the left knee joint of the rabbits under a general anesthesia induced by intravenous injections of pentobarbital sodium (0.6ml/kg bodyweight i.v.) and under sterile conditions. The left knee was opened via a medial parapatellar approach and the patella was dislocated laterally to expose the patellar groove of the femur. A hand drill, with depth-controlled bits, was used to create cylindrical defects 5 5 mm in area and 4 mm in depth which did not spontaneously regenerate 9 along the midline of the patella groove. For control, the defects were left empty (Group-C: control group, n=18), whereas 3-D cartilage aggregates with dimensions of 10 mm x 5 mm (height diameter) were cut into two pieces into the defects without any flap covering (Group-T: transplanted group, n=18). The patella was relocated and the wound was closed in layers using 4-0 nylon sutures. The animals were then caged and allowed to move freely without any splinting after recovery, 3
9 before finally being sacrificed at 4 (n=6), 8 (n=6) and 12 (n=6) weeks after the operation. However, two rabbits that died during the anesthetic interval and one infected in the operated knee joint were excluded from this study. Thus, the total number of rabbits used for this study was 33. Macroscopic assessment: The animals were sacrificed by injecting them with a lethal dose of pentobarbital sodium. At necropsy, the defects were examined macroscopically, and photographed. The surface of the grafts was inspected in terms of color, integrity, contour, and smoothness. The quality of repair and the presence of any gross damage to the articular surface were then recorded. Histology and Immunohistochemistry: At sacrifice, the upper half of the reparative tissue was cut along the coronal plane from the distal femur and fixed by microwave in 4% paraformaldehyde and 1 % glutaraldehyde in PBS for four days. After decalcification in 0.5M EDTA and 0.1M Tris and NaOH for four weeks, the samples were embedded in paraffin, and sectioned (5μm) with a microtome. Using the sections obtained at 4, 8, and 12 weeks in each group, we assessed the central one-third of the reparative tissue. The histological sections, stained with safranin-o and fast green to demonstrate the presence of glycosaminoglycans (GAG) and fibrous tissue, respectively, were observed under an optical microscope (Olympus IX-70) equipped with a CCD camera (CoolSnap cf), and graded using 4
10 the O Driscoll scoring system 10, by two blinded observers. Regarding immunohistochemical staining, the sections were deparaffinized with xylene and then rehydrated with decreasing concentrations of ethanol in solution. They were incubated with 3% H 2 O 2 for 10 minutes and proteinase K (Dako, Glostrup, Denmark) for 10 minutes to block any endogenous peroxidase activity. They were then incubated with monoclonal mouse antibodies for type- Ⅰcollagen (clone; M35 Developmental Studies Hybridoma Bank)and type-Ⅱ collagen (clone; 4C11 ONCOGENE) at an optimal dilution in 0.05M tris buffered saline (TBS) for one hour. The sections were rinsed with 0.05M TBS three times for five minutes each and incubated with Envision + (Dako) for thirty minutes. They were rinsed three times with TBS and then incubated with DAB solution (Dako) for a few minutes. Biochemical analysis: To examine PG content, levels of GAG in the reparative tissue were measured. The lower half of the reparative tissue was dissected off the central portions of the subdivided femora using a scalpel, and then frozen. The frozen samples were carefully crushed and digested with 1 ml of proteinase K solution overnight at 60. The amount of sulfated GAG was measured with the Blyscan Sulfated Glycosaminoglycan Assay Kit (Biocolor, Ltd) according to the manufacturer s recommendations. DNA quantification was carried out with a fluorometric assay using the Hoechst dye H33258 (Sigma B-2883) Statistical analysis: For the data on histological scores and the GAG/DNA ratio of the 5
11 tissue, means and standard deviations were calculated for each group. The two-tailed unpaired Student s t-test with Welch s correction was performed to analyze any significant difference between Group-T and Group-C regarding the histological score and the GAG/DNA ratio. P values of less than 0.05 were considered to be statistically significant. Results Characterization of cartilage aggregates: Figure.1, A shows an image of a 3-D aggregate formed in the RWV bioreactor after 1 week of culture. The aggregates were not round but slender, though they could be handled with surgical forceps. In size they averaged approximately 10mm 5mm (height diameter). They resembled well-differentiated hyaline cartilage in cellular morphology and were stained strongly by safranin-o as shown in Figure.1, B. This kind of aggregate was formed repeatedly in the same experiment 7. Macroscopic findings: All the rabbits could run normally and had a normal range of motion in the operated knee at all experimental times. After the animals were sacrificed, the defects of the patella groove were examined macroscopically. In Group-T and Group-C, no signs of immunological rejection or synovial proliferation were observed in the knees at any time after the operation (at 4, 8 or 12 weeks), although osteophytes were present near the medial side of the femoral condyle at the junction of the patellar and tibial articular area, with 5 cases in Group-C and 3 cases in Group-G. In Group-C, at 4 weeks after the operation, an 6
12 ulceration of cartilage was observed in only one case at the medial upper side of the patellar groove. At 4 and 8 weeks, the regenerated area in Group-C contained red, irregular tissue with a depression and the margins of the defects were clearly distinguishable from the surrounding normal cartilage (Fig.2, A B). At 12 weeks, the defects were filled with a white tissue, but the regenerated area still had an irregular appearance with a depression and the margins of the defects were also clearly recognizable (Fig.2, C). By contrast, in Group-T, the regenerated area showed a normal contour as early as 4 weeks after the operation. The defects were covered with a white, glossy, smooth membrane, which resembled articular cartilage at 4 weeks after the operation and was maintained up until weeks 8 and 12 (Fig.2, D E F). Results of safranin-o fast green staining: In Group-T at as early as 4 weeks, the defects were filled with reparative tissue that resembled hyaline cartilage (Fig.3, A). The cells were round and arranged vertically as columns consisting of a few cells (Fig.3, D). At 8 and 12 weeks, the cells remained their morphology, and the extracellular matrices were strongly stained by safranin-o, suggesting the active production of GAG (Fig.3, B C). The reparative tissue had a smooth surface and there were no fibrous tissues between the reparative tissue and adjacent normal cartilage (Fig.3, E). At 8 weeks, in addition to the presence of the hyaline-like cartilage, enchondral bone was observed in the deeper portion of the reparative 7
13 tissue. At 12 weeks, although the surface of the reparative tissue seemed to be slightly irregular, most cells were round. Safranin-O staining was evident throughout the reparative tissue, but in some cases its intensity was slightly reduced in comparison to that of the adjacent normal cartilage. However, the reparative tissue retained its thickness (Fig.3, C). In the deeper portion of the bony compartment, the osseous tissue was well remodeled (Fig.3, F). In contrast, in Group-C at 4 weeks after the operation, the defects were filled with fibrous tissue with an irregular surface, and some fissures were noted in it but were partially stained by safranin-o (Fig.3, G). The junction between the tissue and the adjacent normal cartilage was loose and recognizable. At 8 weeks, the defects were filled with reparative tissue similar to that seen at 4 weeks after the operation, (Fig.3, H). At 12 weeks, the reparative tissue showed a loss in intensity of safranin-o staining and a reduction in thickness (Fig.3, I). In general, the untreated defects filled with disorganized fibrocartilage did not recover to develop an articular surface continuous with the surrounding hyaline cartilage. Immunohistochemical staining for type-Ⅰand -Ⅱcollagen: The regenerated cartilage in Group-T had greater staining of type-Ⅱcollagen on the matrix as well as in the surrounding normal cartilage at all time points after the operation (Fig.3, J). The staining of type-Ⅰ collagen was less intense in the regenerated cartilage zone, but it was more intense in the calcified zone (Fig.3, K). 8
14 Histological scoring of the reparative tissue: For a quantitative histological analysis of the reparative tissue, the sections were examined independently by two observers, and scored according to the grading scale established by O Driscoll et al. 10 from 0 (worst) to 24 (best; normal). The mean scores of the histological assessments are shown in Figure.4. The mean score of both groups increased gradually from 4 to 8 weeks and then slightly decreased from 8 to 12 weeks. At 4 and 8 weeks after the operation, the mean score of Group-T was significantly better than that of Group-C (P<0.05). At 12 weeks, the mean score of Group-T was not significantly different from that of Group-C. Biochemical findings: The time course of the change in the GAG / DNA ratio of the reparative tissues is shown in Figure.5. In both groups, the ratio was increased gradually from 4 to 8 weeks and then decreased slightly from 8 to 12 weeks. However, there was no significant change with time or difference between the two groups. Discussion In the present study, large osteochondral defects in the knee joints of rabbits were successfully repaired with hyaline-like cartilage after the transplantation of allogeneic cartilaginous aggregates formed from bone marrow-derived cells using the RWV bioreactor. As early as 4 weeks after the operation, the defects were filled with reparative tissue that resembled hyaline cartilage. The reparative tissue had a smooth surface and there were no fibrous tissues between the reparative tissue and adjacent normal cartilage. At 8 weeks, 9
15 enchondral bone had formed in the deeper portion of the reparative tissue. At 12 weeks, in some cases the intensity of staining with safranin-o was slightly reduced in comparison to that in the adjacent normal cartilage, but the reparative tissue retained its thickness. This is the first report of the rapid regeneration of critical osteochondral defects with allogeneic cartilaginous aggregates formed from bone marrow-derived cells without any scaffold using the RWV bioreactor. There are two important points in this study. First, the cells are derived from bone marrow and mesenchymal stem cells (MSCs). Therefore it is possible for the cells to proliferate in a monolayer culture and then to differentiate into cartilage and bone 11,12. An additional advantage to using bone marrow-derived cells in a clinical context is that they can be collected through aspiration of both sides of the iliac crest under partial anesthesia, a procedure that is very easy to perform and minimally invasive. Previous study 20 found that synovium was a better cell source than bone marrow-derived cells with regard to the regeneration of cartilage by comparing chondrogenic potential using a pellet culture system in vitro. However, the cartilaginous aggregates formed by the RWV bioreactor are approximately five-fold in diameter larger than those formed in a pellet culture, which is an advantage for clinical application. Moreover, collecting synovium from joints is invasive, and the amount from each joint differs depending on the disease such as osteoarthritis, rheumatoid arthritis, or trauma. Consequently, bone marrow-derived cells are a more 10
16 suitable source than the synovium for obtaining MSCs and the RWV bioreactor is a more suitable cell culture system than a pellet culture with regard to the regeneration of cartilage in a clinical context. Second, we used the RWV bioreactor as the 3-D culture system which stimulates chondrogenesis in a simulated micro-gravity environment 7. In previous reports 2,13, engineered cartilage from MSCs required a scaffold for the cells to remain in the defect and to act as a support for inducing the formation of hyaline cartilage. However, using our technique, it is possible to form large and homogenous cartilaginous aggregates without any scaffold which can thus be transplanted into large osteochondral defects, which do not spontaneously regenerate in the rabbit 9. These aggregates have already produced an abundance of extracellular matrix and type-Ⅱ collagen which was used to identify the chondrogenic phenotype in vitro 7. It suggests that the aggregates formed in the RWV bioreactor have the character of hyaline cartilage. Rich extracellular matrix embedded chondrocytes to maintain their phenotype protecting them from dedifferentiation. In addition, we had a specific reason to choose aggregates at as early as 1 week after culture in the RWV bioreactor for transplantation. According to our in vitro study 7, the cells of cartilaginous aggregates after 1 week of culture are not mature, but consist of undifferentiated or chondrogenic precursor cells, which might exhibit plasticity to differentiate into another phenotype such as osteoblasts etc. The aggregates of such kinds of cells were influenced 11
17 by various biological factors from the host bone marrow side 14,15 and interacted with adjacent cartilage 16,17. A suitable distribution of mechanical stress and synovial factors 18,19 also influence the lineage of these cells. These characteristics may thus make it possible to rapidly and suitably regenerate cartilage-bone structure in vivo. The limitations of this preliminary study are that we used 10-week-old rabbit model and only observed short-term results. And it remains unclear, at this preliminary stage, what precisely occurred at the site of repair. Therefore, more systematic experiments to assess this repair mechanism are currently in progress. In conclusion, we successfully induced the repair of large osteochondral defects with 3-D cartilaginous aggregates formed by bone marrow-derived cells in the RWV bioreactor. This novel technique may have the advantage of achieving a rapid regeneration of cartilage in large osteochondral defects and is a promising technology for the tissue engineering of articular cartilage. Experiments aimed at combining this technique with the use of scaffolds are currently underway. Cartilage tissue of various shapes and sizes could potentially be formed in the RWV bioreactor using scaffolds. Clinical applications for the treatment of focal defects of articular cartilage due to disease or trauma are anticipated in the near future. 12
18 Acknowledgments This work is supported by Research Promotion Bureau, Ministry of Education, Culture, Sports, Science and Technology (MEXT), Japan, under the contract No and is carried out as a part of Ground Research Announcement for Space Utilization promoted by Japan Space Forum. References 1. Li WJ, Tuli R, Okafor C, et al A three-dimensional nanofibrous scaffold for cartilage tissue engineering using human mesenchymal stem cells. Biomaterials 26: Wakitani S, Goto T, Pineda SJ, et al Mesenchymal cell-based repair of large, full-thickness defects of articular cartilage. J Bone Joint Surg Am 76: Gao J, Caplan AI Mesenchymal stem cells and tissue engineering for orthopaedic surgery. Chir Organi Mov 88: Hunziker EB Articular cartilage repair: basic science and clinical progress. A review of the current status and prospects. Osteoarthritis Cartilage 10: Barry FP, Murphy JM Mesenchymal stem cells: clinical applications and biological characterization. Int J Biochem Cell Biol 36: Guo X, Wang C, Zhang Y, et al Repair of large articular cartilage defects with implants of autologous mesenchymal stem cells seeded into beta-tricalcium phosphate in a 13
19 sheep model. Tissue Eng 10: Ohyabu Y, Kida N, Kojima H, et al Cartilaginous tissue formation from bone marrow cells using rotating wall vessel (RWV) bioreactor. Biotechnol Bioeng 95: Unsworth BR, Lelkes PI Growing tissues in microgravity. Nat Med 4: Shapiro F, Koide S, Glimcher MJ Cell origin and differentiation in the repair of full-thickness defects of articular cartilage. J Bone Joint Surg Am 75: O'Driscoll SW, Keeley FW, Salter RB Durability of regenerated articular cartilage produced by free autogenous periosteal grafts in major full-thickness defects in joint surfaces under the influence of continuous passive motion. A follow-up report at one year. J Bone Joint Surg Am 70: Pittenger MF, Mackay AM, Beck SC, et al Multilineage potential of adult human mesenchymal stem cells. Science 284: Caplan AI Mesenchymal stem cells. J Orthop Res 9: Im GI, Kim DY, Shin JH, et al Repair of cartilage defect in the rabbit with cultured mesenchymal stem cells from bone marrow J Bone Joint Surg Br 83: Engstrand T Molecular biologic aspects of cartilage and bone: potential clinical applications. Ups J Med Sci 108: Wozney JM, Rosen V, Byrne M, et al Growth factors influencing bone 14
20 development. J Cell Sci Suppl 13: Tognana E, Chen F, Padera RF, et al Adjacent tissues (cartilage, bone) affect the functional integration of engineered calf cartilage in vitro. Osteoarthritis Cartilage 13: Zhang Z, McCaffery JM, Spencer RG, et al Growth and integration of neocartilage with native cartilage in vitro. J Orthop Res 23: Serink MT, Nachemson A, Hansson G The effect of impact loading on rabbit knee joints. Acta Orthop Scand 48: Yanai T, Ishii T, Chang F, et al Repair of large full-thickness articular cartilage defects in the rabbit: the effects of joint distraction and autologous bone-marrow-derived mesenchymal cell transplantation. J Bone Joint Surg Br 87: Sakaguchi Y, Sekiya I, Yagishita K, et al Comparison of human stem cells derived from various mesenchymal tissues: superiority of synovium as a cell source. Arthritis Rheum 52:
21 Figure legend Figure 1. (A) A photograph of an aggregate of cartilage formed in a RWV bioreactor. (B) A histological section of the aggregate. (Safranin-O staining) bar=500μm Figure 2. Macroscopic appearance of the reparative tissue in Group-C (A,B,C) and Group-T (D,E,F). (A,D): At 4 weeks (B,E): At 8 weeks (C,F): At 12 weeks after the operation. bar=5mm Figure 3. Histological photomicrographs of reparative tissue in Group-T (A-F) and Group-C (G, H, I). (Safranin-O staining) (A, D, E): At 4 weeks (B): At 8 weeks (C, F): At 12 weeks after the operation. Photomicrographs showing the results of immunohistochemical staining of type Ⅱ(J) and Ⅰ(K) collagen in Group-T. (A~C, G~I): bar=1000μm (D~F, J, K): bar=100μm Figure 4. The histological score of the reparative tissue using the O Driscoll grading scale. (*P<0.05) Figure 5. The time course of the change in the GAG / DNA ratio of the reparative tissue. 16
22
23
24
25
26
27
o~ r;'c' - OSTEOARTHRITIS
 Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental Studies in Rabbits
 Biocybernetics and Biomedical Engineering 2008, Volume 28, Number 2, pp. 87 93 Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental
Biocybernetics and Biomedical Engineering 2008, Volume 28, Number 2, pp. 87 93 Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Abstract. 1. Introduction CLINICAL CASE STUDY
 JOURNAL OF TISSUE ENGINEERING AND REGENERATIVE MEDICINE J Tissue Eng Regen Med 2007; 1: 74 79. Published online in Wiley InterScience (www.interscience.wiley.com).8 CLINICAL CASE STUDY Repair of articular
JOURNAL OF TISSUE ENGINEERING AND REGENERATIVE MEDICINE J Tissue Eng Regen Med 2007; 1: 74 79. Published online in Wiley InterScience (www.interscience.wiley.com).8 CLINICAL CASE STUDY Repair of articular
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Cartilage. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
BIOMATERIALS-TISSUE TISSUE INTERACTIONS: INTRODUCTION
 Massachusetts Institute of Technology Harvard Medical School Brigham and Women s Hospital VA Boston Healthcare System 2.79J/3.96J/BE.441/HST522J BIOMATERIALS-TISSUE TISSUE INTERACTIONS: INTRODUCTION M.
Massachusetts Institute of Technology Harvard Medical School Brigham and Women s Hospital VA Boston Healthcare System 2.79J/3.96J/BE.441/HST522J BIOMATERIALS-TISSUE TISSUE INTERACTIONS: INTRODUCTION M.
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model
 Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
The cellfree matrix for autoregeneration of articular cartilage defects
 The cellfree matrix for autoregeneration of articular cartilage defects What is Amedrix GmbH? Amedrix GmbH, located in Esslingen near Stuttgart, is a medical biotech company which develops highly innovative
The cellfree matrix for autoregeneration of articular cartilage defects What is Amedrix GmbH? Amedrix GmbH, located in Esslingen near Stuttgart, is a medical biotech company which develops highly innovative
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway
 Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
The potential of intra-articular injection of chondrogenicinduced bone marrow stem cells to retard the progression of osteoarthritis in a sheep model
 Health and Biomedicine http://dx.doi.org/ 10.5339/qfarf.2012.BMP30 The potential of intra-articular injection of chondrogenicinduced bone marrow stem cells to retard the progression of osteoarthritis in
Health and Biomedicine http://dx.doi.org/ 10.5339/qfarf.2012.BMP30 The potential of intra-articular injection of chondrogenicinduced bone marrow stem cells to retard the progression of osteoarthritis in
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model
 Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
Introduction. Key words: mesenchymal stem cells, cytokines in vitro culture. (Centr Eur J Immunol 2005; 30 (1-2): 26-31)
 Preservation of chondrogenic potential of mesenchymal stem cells isolated from osteoarthritic patients during proliferation in response to platelet-derived growth factor (PDGF) EWA WARNAWIN 1, TOMASZ BURAKOWSKI
Preservation of chondrogenic potential of mesenchymal stem cells isolated from osteoarthritic patients during proliferation in response to platelet-derived growth factor (PDGF) EWA WARNAWIN 1, TOMASZ BURAKOWSKI
Knee Articular Cartilage Restoration: From cells to the patient. Professor Lars Engebretsen, University of Oslo, Norway
 Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
Articular Cartilage Repair with Mesenchymal Stem Cells After Chondrogenic Priming: A Pilot Study
 Supplementary Materials and Methods Articular Cartilage Repair with Mesenchymal Stem Cells After Chondrogenic Priming: A Pilot Study Troy D. Bornes, MD, PhD, Adetola B. Adesida, PhD, and Nadr M. Jomha,
Supplementary Materials and Methods Articular Cartilage Repair with Mesenchymal Stem Cells After Chondrogenic Priming: A Pilot Study Troy D. Bornes, MD, PhD, Adetola B. Adesida, PhD, and Nadr M. Jomha,
PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION
 A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
Evaluation of the Viability And Chondrogenic Capability of Cadaveric Chondrocytes For Clinical Application In Cartilage Repair.
 Evaluation of the Viability And Chondrogenic Capability of Cadaveric Chondrocytes For Clinical Application In Cartilage Repair. ANELL OLIVOS-MEZA, MD, CARMINA ORTEGA, Biol, VALENTIN MARTINEZ, Biol, ENRIQUE
Evaluation of the Viability And Chondrogenic Capability of Cadaveric Chondrocytes For Clinical Application In Cartilage Repair. ANELL OLIVOS-MEZA, MD, CARMINA ORTEGA, Biol, VALENTIN MARTINEZ, Biol, ENRIQUE
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice
 Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation for the Repair of Chondral Defects of the Knee
 International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
CONSULTATION DURING SURGERY / NOT A FINAL DIAGNOSIS. FROZEN SECTION DIAGNOSIS: - A. High grade sarcoma. Wait for paraffin sections results.
 Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
PARTIAL KNEE REPLACEMENT
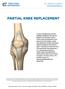 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Articular cartilage repair using collagen type I hydrogels Clincal results
 Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular. State Key Laboratory of Bioreactor Engineering, East China University of
 Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular Chondrocytes by Paracrine Secretion Lei Xu, Yuxi Wu, Zhimiao Xiong, Yan Zhou, Zhaoyang Ye *, Wen-Song Tan * State Key Laboratory of
Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular Chondrocytes by Paracrine Secretion Lei Xu, Yuxi Wu, Zhimiao Xiong, Yan Zhou, Zhaoyang Ye *, Wen-Song Tan * State Key Laboratory of
Original Policy Date
 MP 8.01.30 Orthopedic Applications of Stem Cell Therapy Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
MP 8.01.30 Orthopedic Applications of Stem Cell Therapy Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
An Owner's Guide to Natural Healing. Autologous Conditioned Plasma (ACP)
 An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Partial Knee Replacement
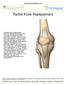 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
contains an antiangiogenesis factor
 CARTILAGE & BONE Cartilage and Bone objectives Student must learn :. What is the meaning of cartilage, and their function, location in human body.. To distinguish the 3 types of cartilage. And their cells,
CARTILAGE & BONE Cartilage and Bone objectives Student must learn :. What is the meaning of cartilage, and their function, location in human body.. To distinguish the 3 types of cartilage. And their cells,
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Discovery of a Small Molecule Inhibitor of the Wnt Pathway (SM04690) as a Potential Disease Modifying Treatment for Knee Osteoarthritis
 Discovery of a Small Molecule Inhibitor of the Wnt Pathway (SM469) as a Potential Disease Modifying Treatment for Knee Osteoarthritis Vishal Deshmukh, Ph.D., Charlene Barroga, Ph.D., Yong Hu, Ph.D., John
Discovery of a Small Molecule Inhibitor of the Wnt Pathway (SM469) as a Potential Disease Modifying Treatment for Knee Osteoarthritis Vishal Deshmukh, Ph.D., Charlene Barroga, Ph.D., Yong Hu, Ph.D., John
Total Knee Replacement
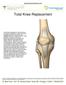 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Department of Plastic Surgery, Royal Melbourne Hospital, Australia
 ARTICULAR CARTILAGE LOSS IN LONG-STANDING IMMOBILISATION OF INTERPHALANGEAL JOINTS By P. L. FIELD, F.R.C.S., and J. T. HUESTON,/Vi.S., F.R.C.S., F.R.A.C.S. Department of Plastic Surgery, Royal Melbourne
ARTICULAR CARTILAGE LOSS IN LONG-STANDING IMMOBILISATION OF INTERPHALANGEAL JOINTS By P. L. FIELD, F.R.C.S., and J. T. HUESTON,/Vi.S., F.R.C.S., F.R.A.C.S. Department of Plastic Surgery, Royal Melbourne
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
Bone. Development. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
 AJSM PreView, published on February 9, 9 as doi:1.1177/3635465838415 The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
AJSM PreView, published on February 9, 9 as doi:1.1177/3635465838415 The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury
 Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe
 Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Prof. Steven S. Saliterman. Department of Biomedical Engineering, University of Minnesota
 Department of Biomedical Engineering, University of Minnesota http://saliterman.umn.edu/ The meniscus is a fibrocartilaginous tissue primarily of type 1 collagen fibers. (In contrast to hyaline cartilage
Department of Biomedical Engineering, University of Minnesota http://saliterman.umn.edu/ The meniscus is a fibrocartilaginous tissue primarily of type 1 collagen fibers. (In contrast to hyaline cartilage
Title. CitationJournal of Bioscience and Bioengineering, 100(1): 12. Issue Date Doc URL. Type. File Information
 Title Effect of chondroitin sulfate and hyaluronic acid on Author(s)Nishimoto, Shohei; Takagi, Mutsumi; Wakitani, Shigey CitationJournal of Bioscience and Bioengineering, 100(1): 12 Issue Date 2005-07
Title Effect of chondroitin sulfate and hyaluronic acid on Author(s)Nishimoto, Shohei; Takagi, Mutsumi; Wakitani, Shigey CitationJournal of Bioscience and Bioengineering, 100(1): 12 Issue Date 2005-07
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
CHONDROTOXICITY OF LOCAL ANESTHETIC
 CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
ORTHOBIOLOGIC TREATMENTS IN BASEBALL. Casey G. Batten MD PBATS - January 19th, 2018
 ORTHOBIOLOGIC TREATMENTS IN BASEBALL Casey G. Batten MD PBATS - January 19th, 2018 The Problem Musculoskeletal injuries are common in sport Pressure to minimize down time, swift return Many injuries involve
ORTHOBIOLOGIC TREATMENTS IN BASEBALL Casey G. Batten MD PBATS - January 19th, 2018 The Problem Musculoskeletal injuries are common in sport Pressure to minimize down time, swift return Many injuries involve
Growth and repair: Cartilage is a vascular tissues that receives nutrients by diffusion through its matrix, cartilage grow by 2 mechanisms:
 Skeletal connective tissues: (cartilage and bone): Cartilage and bone are specialized connective tissues both adapted to serve as skeletal framework in most vertebrates the presence of solid inter cellular
Skeletal connective tissues: (cartilage and bone): Cartilage and bone are specialized connective tissues both adapted to serve as skeletal framework in most vertebrates the presence of solid inter cellular
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
ACI < > < > +/- MSC MSC MASS
 Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Quiz 6. Cartilage and Bone
 Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Transient Trimethylamine N-oxide Supplementation Confers Chondroprotection to Engineered Cartilage Post-Culture Under Stress Conditions
 Transient Trimethylamine N-oxide Supplementation Confers Chondroprotection to Engineered Cartilage Post-Culture Under Stress Conditions Eben G. Estell, BS, Sonal Ravin Sampat, M.S., J. Chloe Bulinski,
Transient Trimethylamine N-oxide Supplementation Confers Chondroprotection to Engineered Cartilage Post-Culture Under Stress Conditions Eben G. Estell, BS, Sonal Ravin Sampat, M.S., J. Chloe Bulinski,
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Chapter 7 Skeletal System. Skeletal System: Bone Functions: Describe the role the skeletal system plays in each of the following functions.
 Chapter 7 Skeletal System Skeletal System: Bone Functions: Describe the role the skeletal system plays in each of the following functions. support protection muscle attachment - movement blood production
Chapter 7 Skeletal System Skeletal System: Bone Functions: Describe the role the skeletal system plays in each of the following functions. support protection muscle attachment - movement blood production
Articulations. Articulation. Joint between bones. Does not mean movement! Some joints are immovable; sutures.
 Articulations Joint between bones Articulation Does not mean movement Some joints are immovable; sutures. Classification of joints Two questions about joints: 1- How does it move? - functional 2- How is
Articulations Joint between bones Articulation Does not mean movement Some joints are immovable; sutures. Classification of joints Two questions about joints: 1- How does it move? - functional 2- How is
Tissue engineering of cartilage
 Tissue engineering of cartilage Cartilage responds to mechanical forces and is able to remodel in response to the prevailing stress Cartilage, like bone, may respond to mechanical stimulation by increasing
Tissue engineering of cartilage Cartilage responds to mechanical forces and is able to remodel in response to the prevailing stress Cartilage, like bone, may respond to mechanical stimulation by increasing
Supplementary Data. Supplementary Methods:
 Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
Biology of platelet-rich plasma and its clinical application in cartilage repair
 Xie et al. Arthritis Research & Therapy REVIEW Biology of platelet-rich plasma and its clinical application in cartilage repair Xuetao Xie 1,2, Changqing Zhang 1 and Rocky S Tuan 2* Abstract Platelet-rich
Xie et al. Arthritis Research & Therapy REVIEW Biology of platelet-rich plasma and its clinical application in cartilage repair Xuetao Xie 1,2, Changqing Zhang 1 and Rocky S Tuan 2* Abstract Platelet-rich
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim The cartilage General characteristics: 1. Cartilage is a specialized type of connective tissue (supporting connective tissue). 2. Consists, like other connective tissues, of
Biology Dr. Khalida Ibrahim The cartilage General characteristics: 1. Cartilage is a specialized type of connective tissue (supporting connective tissue). 2. Consists, like other connective tissues, of
Disclosures: C.B. Raub: None. B.C. Hansen: None. T. Yamaguchi: None. M.M. Temple-Wong: None. K. Masuda: None. R.L. Sah: None.
 En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
Anatomy & Physiology Skeletal System
 I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
I. Functions of the Skeletal System A. the body Anatomy & Physiology Skeletal System B. of vital organs C. Provide for movement D. storage (calcium & phosphate) E. cell formation II. Bone Structure A.
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Patella Planing System
 REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
Chp. 6: Bones and Skeletal Tissue Student Worksheet. 1. The skeletal system is composed of bones,,, and.
 Chp. 6: Bones and Skeletal Tissue Student Worksheet 1. The skeletal system is composed of bones,,, and. 2. What are 5 functions of the skeletal system? 3. Besides osseous tissue (connective tissue with
Chp. 6: Bones and Skeletal Tissue Student Worksheet 1. The skeletal system is composed of bones,,, and. 2. What are 5 functions of the skeletal system? 3. Besides osseous tissue (connective tissue with
Chapter 5 The Skeletal System
 Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Stem Cells and Sport Medicine
 Stem Cells and Sport Medicine Rehal Abbas Bhojani, MD CAQSM Memorial Hermann Medical Group 2014 Sports Medicine Symposium of the Americas Stem cell biology Overview Potential applications of stem cells
Stem Cells and Sport Medicine Rehal Abbas Bhojani, MD CAQSM Memorial Hermann Medical Group 2014 Sports Medicine Symposium of the Americas Stem cell biology Overview Potential applications of stem cells
Figure ) The area that causes the lengthwise growth of a long bone is indicated by letter. Diff: 2 Page Ref:
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 5 The Skeletal System Short Answer Figure 5.1 Using Figure 5.1, identify the following: 1) Spongy bone is indicated by letter. Diff: 1 Page Ref:
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 5 The Skeletal System Short Answer Figure 5.1 Using Figure 5.1, identify the following: 1) Spongy bone is indicated by letter. Diff: 1 Page Ref:
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
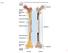 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit)
 Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit) Cat. No. 280560-N INTRODUCTION Glycosaminoglycans (GAGs) are a major component of the extracellular matrix (ECM)
Assay Kit for Measurement of Proteoglycan. (Sulfated Glycosaminoglycan Quantification Kit) Cat. No. 280560-N INTRODUCTION Glycosaminoglycans (GAGs) are a major component of the extracellular matrix (ECM)
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
2 PROCESSES OF BONE OSSIFICATION
 2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
ORS 2015 Annual Meeting (Orthopedic Research Society)
 ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis
 Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis Charlene Barroga, Ph.D., Yong Hu, Ph.D., Vishal Deshmukh, Ph.D., and John Hood,
Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis Charlene Barroga, Ph.D., Yong Hu, Ph.D., Vishal Deshmukh, Ph.D., and John Hood,
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Joint homeostasis. From the University Medical Center, Utrecht, The Netherlands 15,19, Eventually, the new matrix shows loss of normal
 Joint homeostasis TE DISCREPANCY BETWEEN OLD AND FRES DEFECTS IN CARTILAGE REPAIR D. B. F. Saris, W. J. A. Dhert, A. J. Verbout From the University Medical Center, Utrecht, The Netherlands T he discrepancy
Joint homeostasis TE DISCREPANCY BETWEEN OLD AND FRES DEFECTS IN CARTILAGE REPAIR D. B. F. Saris, W. J. A. Dhert, A. J. Verbout From the University Medical Center, Utrecht, The Netherlands T he discrepancy
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Repair of osteochondral defects with a new porous synthetic polymer scaffold
 Repair of osteochondral defects with a new porous synthetic polymer scaffold I. Nagura, H. Fujioka, T. Kokubu, T. Makino, Y. Sumi, M. Kurosaka From Kobe University Graduate School of Medicine, Kobe, Japan
Repair of osteochondral defects with a new porous synthetic polymer scaffold I. Nagura, H. Fujioka, T. Kokubu, T. Makino, Y. Sumi, M. Kurosaka From Kobe University Graduate School of Medicine, Kobe, Japan
Human Anatomy and Physiology I Laboratory
 Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
Meniscus Problems - Torn Meniscus Repair
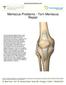 Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
