BLEEDING DISORDER IN CHILDREN
|
|
|
- Lorraine Logan
- 5 years ago
- Views:
Transcription
1 BLEEDING DISORDER IN CHILDREN
2
3 Platelets Coagulation factors Blood vessels integrity
4 Blood is kept in a liquid form because the endothelium produce inhibitory factors to deactivate the platelets and coagulation factors. Healthy endothelium is crucial for hemostasis Injury to endothelial cells can be by: bacteria, viruses, drugs( intrinsic) OR external trauma, thermal injury (extrinsic)
5 Enzymes, made in the liver some are Vitamin K dependent(gamma carboxylation) 10,9,7,2 require Ionized calcium Intrinsic pathway contact with non endothelial cell eg: Tube activate XII Extrinsic pathway tissue lipoprotin factor, tissue thrombin Activate factor VII Goal: fibrinogen fibrin
6 From BM megakaryocytes Size 2-3micron Count No nucleus Granules receptors Life span 7-10 days decrease number or function bleeding
7 Vasoconstriction neurogenic reflex endothelien by injured cells Von Wilibrands factors by injured cells Attach to platelets by Gp1b. platelet adhesion Platelet activation ( TXA2) vaso.const. inc. aggregation Platelet aggregation Primary hemostatic plug AKA primary plat. Plug Primary hemostatic + fibrin secondary plug
8
9
10 Blood vessels Coagulation factors Decrease platelets Hemorrhagic telangiectasia Hemophilias ( A, B, C)) Number Function Scurvy, PEM Liver dises BM depression Hereditary: Von Willibrand s congenital Acquired Henoch-Scholein purpura SLE DIC BM infiltration Meningococcemia Infective endocarditis Afibrinogenemia Vit K deficiency Increase destruction immune no immune Acquire: Drugs Aspirin CRF Leukemia
11 Petichea < 3mm Purpura <3mm>1cm Ecchymoses > 1cm -ve glass test ( non blanching)
12 Bleeding disorder Platelet(decrease #) or fuctions Vascular (hereditary / acquired) Coagulation Congenital Acquried
13 Test for vascular and platelets disorder: 1- bleeding time 2- blood count 3-tourniquet test 4-bone marrow examination 5- platelets morphology and functions.
14 Tests for coagulation factors :- 1- clotting time 2- thrombin time N sec 3- prothrombin time N sec 4- partial thromboplastin time N 25-45sec 5- specific assessment for clotting factors
15 Bleeding defects Coagulation defects Purpura + - ecchymosis + ++ Hemarthrosis - + Precipitating factots Spontaneous Minor trauma Bleeding time Prolonged Normal Coagulation time Normal Prolonged
16 A male child 4 years old admitted since one week, c/o fever, abdominal pain and anorexia since one week.. Pallor for 3days, red spots, bluish patches in the skin and epistaxis for one day.
17 Commonest platelet disorder
18 Platelets Count : /mm^3 Life span: 8 to 9 days Normally account for 1 out of 10,000
19 Thrombocytopenia less than /mm^3 Presence of antiplatelet in plasma Short life span No primary disease Normal / increased # of megakaryocyte
20 Megakaryocytes stem cells in BM hematopoietic - Its lobulated nucleus responsible for the production of blood thrombocytes (platelets), which are necessary for normal blood clotting.
21 Autoimmune thrombocytopenic purpura is common disorder that usually preceded by a viral infections usually late winter and spring. Usually EBV, RUBELLA 1-4 wks after exposure. Commonly affect children between 1-4 years. 1/20,000 children.
22
23 Platelets destruction Antiplatelets antibodies IgG, IgM IgG against Megakaryocyte FC receptor recognition Splenic macrophage
24 1- common 1-4 years old 2- sudden onset of Generalized Petechiae and Purpura 3- bleeding from the gums and mucous membrane Platelets <10, History of a preceding viral infection 1 to 4 wks before onset of the thrombocytopenia.
25 Use to asses severity of bleeding basis of symptoms and signs, but not platelet count : NO SYMPTOMS MILD SYMPTOMS MODERATE SEVER
26 Class 1 NO SYMPTOMS CLASS 2 Mild Symptoms Bruises and petechiae, Minor epistaxis Interference with daily life.
27 Class 3 CLASS 4 Moderate More severe skin and mucosal lesions More sever epistaxis Sever bleeding episodes epistaxis melena requiring transfusion or hospitalization symptoms more interfering with the quality of life
28 History and examination A- Laboratory investigation: 1- CBC - In acute cases usually ( HB, WBC, and differential count are normal). - Severe thrombocytopenia (platelet count < /L) - Platelet size is normal or increased
29 2- bone marrow - Normal or increased numbers of megakaryocytes
30 Abnormal WBC count or differential Unexplained anemia Signs suggestive bone marrow disease on history and physical examination.
31 In case of adolescents with new-onset ITP, ANA test should evaluate for SLE. A coombs should be done in unexplained anemia to rule out EVAN SYNDROME (autoimmune hemolytic anemia & thrombocytopenia)
32 1- In case of minimal, mild, and moderate no treatment is required Counselling and educations of the family. 2- For sever and moderate thrombocytopenia (Platelets count <10.000/mm^3) therefore Intravenous immunoglobulin (IVIG) g/kg/day for 1 2 days lead to rapid rise in platelet within 48h.
33 3- Intravenous anti-d therapy: - For Rh positive patients - IV anti-d at a dose of 50 75μg/kg causes a rise in platelet count to > /L in 80 90% of patients within 48 72h
34 4- Prednisone: Corticosteroid therapy 1 4 mg/kg/24 h. Continued for 2-3 wks or until rise in platelets count > /L than rapid taper.
35 5- Splenectomy reserved for 1 of 2 circumstances : 1- >4 years child with sever ITP lasting >1y. 2- symptoms not controlled by medical therapy. 3-platelets count can not be corrected rapidly by (BT,IVIG, & Corticosteroid)
36 1- Leukaemia 2- Aplastic anemia 3- allergic purpura <henoch shonlein 4- collagen vascular disease < SLE
37
38 In a class of diseases known as autoimmune disorders, the body's immune system attacks its own tissues. Some of these diseases are similar to each other such as arthritis and inflammation of arteries in the tissues. People who developed these disorders were previously said to have "connective tissue" or "collagen vascular" disease. We now have names for many of many specific conditions such as: Ankylosing spondylitis Dermatomyositis Polyarteritis nodosa Psoriatic arthritis Rheumatoid arthritis Scleroderma Systemic lupus erythematosus When a specific disease cannot be diagnosed, more general terms may be used. These include as undifferentiated systemic rheumatic (connective tissue) diseases or overlap syndromes
39 Systemic lupus erythematosus (SLE) is an autoimmune disease. In this disease, the body's immune system mistakenly attacks healthy tissue. It can affect the skin, joints, kidneys, brain, and other organs.
40 Signs and symptoms Joint manifestations Skin and mucous membrane manifestations Cardiopulmonary manifestations Lymphoid tissue Neurologic manifestations Renal manifestations Obstetric manifestations Hematologic manifestations GI manifestations
41 Causes : The cause of autoimmune diseases is not fully known. SLE is more common in women than men. It may occur at any age most often in people between the ages of 15 and 44. The disease affects African Americans and Asians more often than people from other races. Certain drugs may also cause SLE. The most common medicines known to cause druginduced lupus erythematosus are: Isoniazid Hydralazine
42 Diagnosis Clinical criteria Cytopenias Autoantibodie Laboratory testing differentiates SLE from other connective tissue disorders. Routine testing should include the following: Antinuclear antibodies (ANA) and anti doublestranded (ds) DNA CBC Urinalysis Chemistry profile including renal and liver enzymes6 Fluorescent ANA Screening for renal involvement
43 Treatment NSAIDs and often antimalarials for mild disease Corticosteroids and often immunosuppressants for severe disease Mild or remittent disease Severe disease
44 Increased Platelet Destruction The hallmark of increased platelet destruction is increased marrow megakaryocytes or, when available, high reticulated platelet count. Platelet destruction results from various Disorders of Platelet Function immune conditions, including the following: Immune thrombocytopenic purpura (ITP) Thrombotic microangiopathies Post-transfusion purpura (PTP) Heparin-induced thrombocytopenia (HIT) Disseminated intravascular coagulation (DIC)
45 Types of platelet function disorders:- 1-hereditary 2-acquired
46 Disorders of platelet adhesion bernard-soulier syndrome
47 Hereditary disorders:- 1-disorder of platelet adhesion(bernard-soilier syndrome) 2-disorders of platelet aggregation(glanzmann thrombasthenia) 3-disorder of platelet secretion 4-disorders of platelet procoagulant activity
48 is a rare autosomal recessive coagulopathy (bleeding disorder) that causes a deficiency of glycoprotein Ib (GpIb), the receptor for von Willebrand factor
49 disorders of platelet aggregation(glanzmann thrombasthenia) is an abnormality of the platelets. It is an extremely rare coagulopathy (bleeding disorder due to a blood abnormality), in which the platelets contain defective or low levels of glycoprotein IIb/IIIa (GpIIb/IIIa), which is a receptor for fibrinogen. As a result, no fibrinogen bridging of platelets to other platelets can occur, and the bleeding time is significantly prolonged.
50 Disorders of platelet adhesion bernard-soulier syndrome
51 Acquired Abnormalities of Platelet Function MYELOPROLIFERATIVE DISEASE DYSPROTEINEMIA CARDIOPULMONARY BYPASS UREMIA LIVER DISEASE DRUG INHIBITION infections
52 MYELOPROLIFERATIVE DISEASE Patients with myeloproliferative disorders (ie, polycythemia vera, myeloid metaplasia, idiopathic myelofibrosis, essential thrombocythemia, and chronic myelogenous leukemia) frequently exhibit abnormal platelet function. Some of these patients have very high platelet counts and demonstrate either abnormal bleeding, or a tendency for arterial or venous thrombosis, or even both. Although the height of the platelet count alone does not correlate with the bleeding or thrombotic tendency, thrombocytosis in excess of 1 million/µl is considered to be a risk factor.
53 Signs and symptoms Perioperative (and postoperative bleeding) Bleeding gums BruisingEpistaxis (nosebleeds) Abnormal bleeding (from small injuries) Unusual menstrual periods
54 CLINICAL FEATURES Bleeding gums Easy Bruising
55 CLINICAL FEATURES There are no specific symptoms or signs that indicate a platelet functional defect. Inherited defects are rare and are generally characterized by a relatively mild bleeding tendency. von Willebrand disease (vwd) is an exception to this rule, since certain vwd subtypes are associated with severe and even fatal bleeding. Patients with platelet functional defects generally present with: Easy bruisability Mucocutaneous bleeding of a purpuric nature Bleeding from the gastrointestinal and genitourinary tracts (often with severe menorrhagia) rather than the petechial bleeding that characterizes thrombocytopenia. It is not unusual for the bleeding tendency to escape detection until aggravated by another abnormality. For example, the defect may first be suspected because of excessive bleeding following minor surgery or a dental extraction or unusual mucocutaneous bleeding following the administration of anticoagulants or a platelet inhibitor such as aspirin. Therefore, a history of unusual bleeding, a family history suggestive of a congenital abnormality, and the clinical picture can provide important clues.
56 Laboratory Studies 1. BLEEDING TIME AND TESTS FOR FACTOR DEFICIENCIES The bleeding time (BT) has traditionally been used as a screening test for the presence of a platelet functional defect. If performed carefully in a well-standardized manner, the BT correlates with both platelet number and function. With platelet counts greater than 100,000/µL, the BT should be less than 8 minutes. As the count falls below this level, the BT lengthens, reaching times of 20 to 25 minutes when the count falls to 10,000/µL. Patients with functional defects, such as severe vwd, can show BTs in excess of 20 minutes with a normal platelet count. Patients with an acquired functional defect secondary to aspirin therapy or uremia show more modest prolongations of the BT (8 20 minutes).
57 2. COMPLETE BLOOD COUNT AND BLOOD FILM A complete blood count (CBC) with examination of the blood film can also be helpful. The CBC can provide evidence of hematopoietic disease, especially a myeloproliferative disorder where high numbers of circulating platelets are associated with abnormal function. Platelet morphology can help in diagnosing disorders such as Bernard-Soulier syndrome and αgranule deficiency (gray platelet syndrome).
58 3. MEASUREMENTS OF PLATELET ACTIVATION/AGGREGATION Direct measurements of platelet activation/aggregation are possible using an aggregometer or flow cytometer. The aggregometer provides a graphic display of the wave of platelet aggregation seen in response to agonists such as ADP, epinephrine, or collagen, and the agglutination response to ristocetin. Specific functional defects respond differently to these agonists. For example, patients with vwd specifically show decreased or absent agglutination with ristocetin [ristocetin-induced platelet agglutination assay (RIPA)], whereas other disorders such as storage pool disease demonstrate poor responses to ADP, epinephrine, and collagen.
59 ASSAYS FOR VON WILLEBRAND FACTOR Full evaluation of the patient with vwd requires an array of tests, including assays for factor VIII activity, vwf antigen, vwf activity, and vwf multimer pattern by agarose gel electrophoresis. Together with the patient's bleeding history, family history, and BT, these assays will diagnose and classify vwd into one of several clinically important subtypes.
60 How can bleeding difficulties in patients with platelet function disorders be treated?
61 TREATMENT for abnormalities of platelet function Abnormalities in platelet function are often first appreciated as a complication of an acute illness or surgery and multiple aggravating factors may play a role in determining the severity of the bleeding tendency. An accurate diagnosis is not usually easily made Hence, treatment should address as many potential contributing factors as possible. This list includes discontinuing drugs that inhibit platelet function, empirically replacing vwf or treating with DDAVP (Desmopressin) and, according to the severity of the patient's bleeding, transfusing normal platelets. Although this approach lacks precision, it is effective. Both acquired and congenital disorders of platelet function can be acutely reversed in order to control severe clinical bleeding.
62 Treatment cont d Long-term management of a platelet functional defect should be based on an accurate diagnosis. Patients with congenital defects should be counseled to avoid drugs that can aggravate the functional abnormality and cause bleeding. Obviously, aspirin and nonsteroidal analgesics are prime offenders. vwd and thrombasthenia patients demonstrate significant prolongations of the bleeding time with aspirin ingestion and are at greater risk for clinical bleeding. These patients should also be educated regarding the nature of their abnormality and should carry identification or wear a medical alert bracelet. This information can be invaluable as a guide to appropriate transfusion therapy in an emergency situation.
63 Treatment Cont d As a general principle, the nature of the functional abnormality will guide the choice of therapy. For example, the vwd patient who lacks normal amounts of vwf will respond to agents that increase plasma vwf levels. In this situation, the platelets will function normally once the vwf abnormality is corrected. In contrast, patients with congenital defects of platelet receptor expression, granule content, or platelet metabolism will require platelet transfusion. As for the acquired abnormalities of platelet function, the best approach to therapy lies somewhere in between. There is clinical evidence that patients with acquired defects secondary to drug ingestion, uremia, and liver disease will respond to DDAVP, vwf replacement, or both. These data suggest that an increase in plasma vwf levels may partially compensate for a platelet-based defect.
64 infections May be bactrial characterized by bloody and puruloid mucus stool, and is often accompanied by fever, tenesmus, and severe abdominal pain. Pathogenic bacteria causing the inflammatory diarrhea syndrome include Salmonella, Vibrio, Shigella, enteroinvasive and enterohemorrhagic Escherichia coli, Campylobacter, Yersinia, Chlamydia, and Clostridium difficile
65 May be Hemorrhagic fevers which can be caused by many different types of virus. The viruses most often associated with hemorrhagic fever arefiloviruses, such as Ebola and Marburg viruses (Ebola Virus and Marburg Virus Infections), which occur mainly in parts of Central AfricaArenaviruses, such as Lassa fever virus in West Africa and Junin virus in South America (Lassa Fever and South American Hemorrhagic
66 Fevers)Bleeding occurs because the viruses make the blood vessels leak. These infections are often fatal.many other viruses, including the dengue virus (Dengue), hantavirus (Hantavirus Infection), and yellow fever virus (Yellow Fever), can cause hemorrhagic symptoms.some of these viruses naturally reside in animals. Some are spread by the bite of a tick or mosquito.
67 Henoch-shoulei purpura: characterized by sudden development of pupric rash arthritis, abdominal pain, renal involvement. The rash : - Consist of petechae and often palpable purpura - Involve lower extermities and buttoks - In kidney causes focal glomerulonephritis.
68 Ethiler- Danlos syndrome: - Disorder of collagen structure that causes easy bruising and poor wound healing. - Skin is hyperelastic : joint lax - The most serious form have been associated with sudden rupture of visceral organ.
69 Acquired disorder: - Survey, chronic corticosteroids therapy, and sever malnutrition associated with weaking of collagen matrix that support blood vessles.
70
71
72 VWD is a congenital bleeding disorder characterized by a lifelong tendency toward easy bruises,frequent epistaxis and menorrhagia. It s a family of bleeding disorders caused by an abnormality of VWF. VWD is the most common hereditary bleeding disorder.
73 pathophysiology VWF is a large glycoprotein required for normal platelet adhesion and also functions as the carrier protein for factor VIII. As such VWF functions in both primary and secondary homeostasis. VWD is due to abnormality either qualitative or quantitative of the VWF.
74 :Types TYPE (1) VWD : Account for 70-80% of cases Characterized by partial quantitative decrease in VWF and FVIII Pt generally has mild symptoms Inherited as autosomal dominant
75 Type (2) VWD: Accounts for 15-20% of cases Qualitative defect of VWF Can be either autosomal dominant or recessive Type(3) VWD: Is the rarest and most sever form Inherited as autosomal recessive trait Characterized by marked deficiencies of both VWF and FVIII
76 presentation May be asymptomatic Easy bruising Recurrent epistaxis Menorrhagia Post-operative bleeding
77 D/Dx: Hemophilia A,B or C Platelet disorders
78 Laboratory studies: CBC BT,PT,aptt VWF levels FVIII activity VWF antigen Gene studies
79 Treatment: Vasopressin analogues(desmopressin) Plasma products Aminocarporic acid (Amicar) Pt-Education
80
81 Definition: It is most common and serious congenital coagulation factor deficiencies. it is an inherited bleeding disorder,it is sex linked recessive. Famales are carriers. Occurs in males.
82 Types: Hemophalia A(classic type), (factor 8 deficiency): Occurs in 1 in 5000 males a represents 85% of all hemophalia. while hemophalia B (factor 9 deficiency) occurs in approximately 1 in The lack of factor 8 or 9 delays the generation of thrombin,which is important for forming a normal functional fibrin clot and solidifying the platelet plug that has formed in areas of vascular injury.
83 Factors 8 and 9 cross placenta,so the presentation starting early ( neonatal bleeding). Patients with less than 1% ( severe hemophalia) Factor 8 or 9 may have spontaneous bleeding into muscle,git,joint and soft tissues OR bleeding with minor trauma. Patients with (1-5%) (moderate hemophalia) Factor 8 or 9 usually require moderate trauma to induce bleeding episodes. In mild hemophalia (less than 5% factor 8 or 9 ) Significant trauma is necessary to induce bleeding.
84 Clinical picture: At birth: unusual bleeding from umbilicus OR circumcision site. Later: 1/ external bleeding: epistaxis,dental bleeding,hematuria and gastrointestinal. 2/ internal bleeding: intracranial hemorrhage, muscles hematoma. 3/ skin: echymosis and hematoma. 4/ hemarthrosis: mainly in big joints of lower limb: Joint become swollen,red,hot,tender with limited mobility, later on: fibrosis and ankylosis.
85 Diagnosis:- 1/ diagnostic: Diagnosis is based on activated partial thromboplastin time (PTT). When an abnormal PTT is obtained,specific factor assay (factor 8 and 9 level) are needed to make a precise diagnosis to determine the appropriate facor replacement therapy. Early appropriate replacement therapy is the hallmark of excellent hemophalia care.
86 Cont.. 2/ carrier detection: *direct gene mutation analysis *F VIII/ Vwf ratio ( less than 1%) 3/ prenatal diagnosis: *DNA analysis * fatal blood sample at( 18-20) weeks.
87 Treatment.1/ prophylactic treatment: Early institution of factor replacement and continuous prophylaxis starting in early childhood should prevent the chronic joint disease associated with hemophalia. Regular F VIII replacement(20 unite/kg three times a week.) Hepatitis B vaccine. Avoid trauma, IM injection and aspirin.
88 Cont... 2/ during bleeding attacks: A- factor VIII replacement: 1/ recombinant factor VIII dose( unite/kg) according to severity. 2/ others: *fresh frozen plasma * factor VIII concentrate.
89 Cont... B- adjuvant drugs: 1/ desmopressin ( DDAVP): increase plasma F VIII by 4 folds. 2/ antifibrinolytics: inhibit fibrinolysis, so stabilize the clot (e.g: Tranexamic acid) Indication: mucosal bleeding, menorrhagia. 3/ prednisone: (short coarse) in hemarthrosis and hematuria.
90 Cont... C/ special cases: 1/ intracranial hemorrhage: high dose of F VIII ( unite/kg) for 2 weeks. 2/ hemarthrosis: Local: cold compresses. F VIII replacement + prednisone(short coarse). Rest for 48 hr then physiotherapy to avoid ankylosis.
91 complication Of bleeding: 1/ severe blood loss : hypovolemic shock. 2/ severe intracranial hemorrhage. 3/ hemophilic arthropathy: joint stiffness. 4/ muscle atrophy.
92 Cont... Of treatment: Treatment may be complicated with: 1/ F8 antibodies development,which is treated using high levels of the factor VIII( unite/kg) or using procine F8. 2/ allergic reaction. 3/ risk of acquiring blood-borne disease especially hepatitis C. Note ; hemophalia occurs in famale with turner`s syndrome.
93 Hemophalia B:( chrismas disease) Factor IX deficiency. Sex linked recessive disorder. As hemophalia A but milder. Treated by recombinant F IX OR F IX concentrate given / 24 hr.
94 Hemophalia C: Factor XI deficiency. Autosomal recessive disorder, so can affect both sexes. Very mild disease. Treated by fresh frozen plasma given / 48 hr.
95 - DIC is a condition that results from widespread activation of coagulation in the circulation. This result in: Consumption of some coagulation factors and platelets Fibrin deposition and secondary fibrinolysis.
96 Etiology: Severe infection such as septicemia. Extensive tissue damage in burn and magor surgery. Shock Heat stroke Acute liver failure Neoplastic disorders as promyelocytic leukemia,adenocarcinoma.
97 CLINICAL FEATURES 1. Acute hemorrhagic manifestation: Hematemesis Bleeding from injection site Intracranial hemorrhage Melena Ischemia and necrosis: Skin gangrene Kedneys acute cortical necrosis leading to renal falilure. Heamolytic anemia due to destruction of RBCs lead to pallor and red urine.
98 Laboratory finding Thrombocytopenia Prolonged prothrombin time Deficincy of factors I,II,V,VIII Increased concentration of fibrin degradation products specially D dimers TREATMENT Correction of the cause [shock,infection,hypoxia] Infusion of fresh frozen plasma Heprin small dose 100 units\6 hours In newborn exchange transfusion with fresh blood.
99
100 Is now the preferred term for haemorrhagic disease of the newborn( HDN). Vitamin K is required for the production of clotting factors ll, Vll,lX,X. Is present in some plant and it's also synthesised by some E. Coli in the gut. All newborn infants have low level of vitamin K are at risk of developing VKDB.
101 Classification 1) early VKDB : present within 24 hrs of birth. 2) classic VKDB: present between day 1 and day 7 of life. 3) late VKDB:present between week2 and week 12 of life.
102 Risk factors 1)children who are entirely breast-fed have a20 times greater risk of developing VKDB than those who receive formula milk. 2)several drugs such as isoniazid, rifampicin, anticonvulsion and anticoagulant agent which have taken by the mother. 3) warm enviromental temperature. 4)unsuspected liver disease especially alpha-1 antitrypsin deficincy. 5) malabsorption of fat soluble vitamin due to diarrhoea, coeliac disease or cystic fibrosis.
103 Presentation *Early : Present with bleeding at sites related to trauma of birth 1_bleeding from scalp monitor site. 2_cephalhaematoma espcially after ventous delivery. 3_intracranial bleeding after traumatic delivery. 4_intrathoracic bleeding 5_intraabdominal bleeding.
104 *classic : Bleeding most often affect non vital organs 1_gastrointestinal bleeding. 2_bleeding from skin and mucouse membrane. 3_prolong bleeding following circumcision. 4_bleeding from umbilical stump.
105 *late : It typically present with intracranial haemorrhage and is often caused by undiagnosed cholestasis with resultant malabsorption of vitamin K. Produce the greatest morbidity and mortality amongst the infant due to sudden bleeding into CNS.
106 If VKDB is suspected it is important to go over certain aspect at history: 1_drugs taken in pregnancy 2_gestation at delivery. 3_type and length of delivery. 4_feeding history.
107 Investigation 1_FBC. 2_clotting screen. 3_CXR or ultrasound scan 4_MRI or CT.
108 Management When VKDB is suspected vitamin K should be given as soon as possible. This will result in reduction in bleeding time within a few hrs. The injection should be subcutaneos. Infant of mother taking drugs that inhibit vitamin K are at risk of early VKDB should receive 1mg IM as soon as possible after delivery Babies with severe bleeding or intracranial haemorrhage may require fresh frozen plasma to be give in addition to vitamin K.
109
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN
 Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College
 Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Bleeding disorders. Hemostatic failure: Inappropriate and excessive bleeding either spontaneous or in response to injury.
 1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
Bleeding Disorders. Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph
 Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Platelet Disorders. By : Saja Al-Oran
 Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Hemostatic System - general information
 PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
Approach to bleeding disorders &treatment. by RAJESH.N General medicine post graduate
 Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Haemostasis & Coagulation disorders Objectives:
 Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
BLEEDING (PLATELET) DISORDER. IAP UG Teaching slides
 BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
BLEEDING DISORDERS Simple complement:
 BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
Bleeding Disorders HOPE Maram Al-anbar
 Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Bleeding Disorders: (Hemorrhagic Diatheses) Tests used to evaluate different aspects of hemostasis are the following:
 Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
Easy Bleeding General Presentation
 Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
Bleeding and Thrombotic Disorders. Kristine Krafts, M.D.
 Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Pathology note 8 BLEEDING DISORDER
 Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
EDUCATIONAL COMMENTARY PLATELET DISORDERS
 EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
BLEEDING DISORDERS. JC Opperman 2012
 BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
There are two main causes of a low platelet count
 Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Approach To A Bleeding Patient
 ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
INHERITED COAGULOPATHY
 Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Congenital bleeding disorders
 Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
Haemorrhagic Disorders. Dr. Bashar Department of Pathology Mosul Medical College
 Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
COAGULATIONS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin)
 COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
The LaboratoryMatters
 Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
PCCN Review Hematology
 PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012
 Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
LAMA SHATAT TTP, ITP, DIC
 TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89
 Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood
 Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
Miss. kamlah ahmed 1
 Miss. kamlah ahmed 1 Anatomy & Physiology Blood has two compartments: 1- a fluid portion called plasma. 2- a cellular portion known as the formed elements of the blood. Which are RBC (erythrocytes), WBC
Miss. kamlah ahmed 1 Anatomy & Physiology Blood has two compartments: 1- a fluid portion called plasma. 2- a cellular portion known as the formed elements of the blood. Which are RBC (erythrocytes), WBC
Easy bruising vs Coagulopathy
 Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Bleeding Disorders.2 MS Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD
 Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE
 TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE Dr Susan Russell Director HTC Sydney Children s Hospital, Randwick HFA Meeting 2015 What is von Willebrand Factor? VWF is a large multimeric protein Two
TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE Dr Susan Russell Director HTC Sydney Children s Hospital, Randwick HFA Meeting 2015 What is von Willebrand Factor? VWF is a large multimeric protein Two
Guidelines for Shared Care Centres and Community Staff
 Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
ACQUIRED COAGULATION ABNORMALITIES
 ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
Sysmex Educational Enhancement and Development No
 SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
Bleeding and Haemostasis. Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon
 Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Coagulation an Overview Dr.Abdolreza Abdolr Afrasiabi Thal assem a & Heamophili hilia G ene i tic R esearc C en er Shiraz Medical Medic University
 In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
Disseminated Intravascular Coagulation. M.Bahmanpour MD Assistant professor IUMS
 به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
Instructor s Manual Chapter 26 Hematological Alterations. 1. A man and woman both test positive for the sickle cell trait. The couple asks the
 1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion
 This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche
 L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
HENOCH SCHÖNLEIN PURPURA (VASCULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests (SC)
 HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
Approach to bleeding
 Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Blood Transfusion Guidelines in Clinical Practice
 Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13
 Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Chapter 19. Hemostasis
 Chapter 19 Hemostasis Hemostasis Hemostasis is the cessation of bleeding stopping potentially fatal leaks important in small blood vessels not effective in hemorrhage excessive bleeding from large blood
Chapter 19 Hemostasis Hemostasis Hemostasis is the cessation of bleeding stopping potentially fatal leaks important in small blood vessels not effective in hemorrhage excessive bleeding from large blood
Some renal vascular disorders
 Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal tumors, in children, 530 531 Alkalinization, in tumor lysis syndrome, 516 Allopurinol, in tumor lysis syndrome, 515 Anaphylaxis, drug
Note: Page numbers of article titles are in boldface type. A Abdominal tumors, in children, 530 531 Alkalinization, in tumor lysis syndrome, 516 Allopurinol, in tumor lysis syndrome, 515 Anaphylaxis, drug
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Index. Note: Page numbers of article numbers are in boldface type.
 Index Note: Page numbers of article numbers are in boldface type. A Abdomen, acute, as cancer emergency, 381 399 in cancer patients, etiologies unique to, 390 392 in perforation, 388 surgery of, portal
Index Note: Page numbers of article numbers are in boldface type. A Abdomen, acute, as cancer emergency, 381 399 in cancer patients, etiologies unique to, 390 392 in perforation, 388 surgery of, portal
Disseminated Intravascular Coagulation (DIC) Seminar. Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.
 Disseminated Intravascular Coagulation (DIC) Seminar Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.2012 1 Our plan: Understand the pathophysiology Identify risk factors
Disseminated Intravascular Coagulation (DIC) Seminar Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.2012 1 Our plan: Understand the pathophysiology Identify risk factors
von Willebrand Disease
 von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP
 Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP OVERVIEW Von Willebrand Disease (VWD) is the most common hereditary bleeding disorder in humans, with an estimated prevalence ranging upward
Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP OVERVIEW Von Willebrand Disease (VWD) is the most common hereditary bleeding disorder in humans, with an estimated prevalence ranging upward
UNIT VI. Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav. Copyright 2011 by Saunders, an imprint of Elsevier Inc.
 UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
Moath Darweesh. Omar Sami. Saleem Khreisha. 1 P a g e
 7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
Evaluation Of Bleeding Disorders /AAP Baton Rouge. Raj Warrier
 Evaluation Of Bleeding Disorders /AAP Baton Rouge Raj Warrier Evaluation and approach to management of a bleeding child Raj Warrier Ochsner /Tulane/LSU Manipal University University Of Queenland Objectives
Evaluation Of Bleeding Disorders /AAP Baton Rouge Raj Warrier Evaluation and approach to management of a bleeding child Raj Warrier Ochsner /Tulane/LSU Manipal University University Of Queenland Objectives
Heme (Bleeding and Coagulopathies) in the ICU
 Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Document Title: Hemostasis: Platelet and Coagulation Disorders. Author(s): Joseph H. Hartmann (University of Michigan), DO 2012
 Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Chapter 19 Blood Lecture Outline
 Chapter 19 Blood Lecture Outline Cardiovascular system Circulatory system Blood 1. distribution 2. regulation 3. protection Characteristics: ph 7.4 38 C 4-6 L Composition: Plasma Formed elements Erythrocytes
Chapter 19 Blood Lecture Outline Cardiovascular system Circulatory system Blood 1. distribution 2. regulation 3. protection Characteristics: ph 7.4 38 C 4-6 L Composition: Plasma Formed elements Erythrocytes
Recommendations for Celiac Disease Testing. IgA & ttg IgA
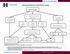 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Platelet vs. Coagulation Bleeding. Qualitative and Quantitative Platelet Disorders. Laboratory Tests. Platelet Signaling. Jeffrey S. Jhang, M.D.
 Qualitative and Quantitative Platelet isorders Platelet vs. Coagulation Bleeding Findings Petechiae Hematomas and Hemarthroses elayed Bleeding Coagulation Rare Common Common Platelet Common Rare Rare Bleeding
Qualitative and Quantitative Platelet isorders Platelet vs. Coagulation Bleeding Findings Petechiae Hematomas and Hemarthroses elayed Bleeding Coagulation Rare Common Common Platelet Common Rare Rare Bleeding
GOOD MORNING! Thursday, July Heidi Murphy, MD Leslie Carter-King, MD
 GOOD MORNING! Thursday, July 10 2014 Heidi Murphy, MD Leslie Carter-King, MD PREP QUESTION Almost all infants experience a transient increase in bilirubin concentrations known as physiologic jaundice during
GOOD MORNING! Thursday, July 10 2014 Heidi Murphy, MD Leslie Carter-King, MD PREP QUESTION Almost all infants experience a transient increase in bilirubin concentrations known as physiologic jaundice during
Do Now pg What part of the blood causes a blood clot? 2. Could you survive without this? Why?
 Do Now pg 95 1. What part of the blood causes a blood clot? 2. Could you survive without this? Why? What is Hemostasis? The stopping of bleeding, which is vitally important when blood vessels are damaged.
Do Now pg 95 1. What part of the blood causes a blood clot? 2. Could you survive without this? Why? What is Hemostasis? The stopping of bleeding, which is vitally important when blood vessels are damaged.
Hemostasis. Learning objectives Dr. Mária Dux. Components: blood vessel wall thrombocytes (platelets) plasma proteins
 Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
Chapter 13 The Blood
 Chapter 13 The Blood Copyright 2015 Wolters Kluwer Health Lippincott Williams & Wilkins Overview Key Terms agglutination erythrocyte lymphocyte albumin fibrin megakaryocyte anemia hematocrit monocyte antigen
Chapter 13 The Blood Copyright 2015 Wolters Kluwer Health Lippincott Williams & Wilkins Overview Key Terms agglutination erythrocyte lymphocyte albumin fibrin megakaryocyte anemia hematocrit monocyte antigen
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 ١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
Bleeding from the Nose (Epistaxis) Basics
 Bleeding from the Nose (Epistaxis) Basics OVERVIEW Bleeding from the nose SIGNALMENT/DESCRIPTION OF PET Species Dogs Cats Breed Predilections Mean Age and Range Predominant Sex SIGNS/OBSERVED CHANGES IN
Bleeding from the Nose (Epistaxis) Basics OVERVIEW Bleeding from the nose SIGNALMENT/DESCRIPTION OF PET Species Dogs Cats Breed Predilections Mean Age and Range Predominant Sex SIGNS/OBSERVED CHANGES IN
Hemostasis and. Blood Coagulation
 Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Effective Date: Approved by: Laboratory Director, Jerry Barker (electronic signature)
 1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
Chapter 06 Lecture Outline. See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes.
 Chapter 06 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. 2012 Pearson Permission Education,
Chapter 06 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. 2012 Pearson Permission Education,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
WISKOTT-ALDRICH SYNDROME. An X-linked Primary Immunodeficiency
 WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
Routine preoperative coagulation tests: are they necessary?
 Routine preoperative coagulation tests: are they necessary? Dr Azzah Alzahrani MD Pediatrics Hematology /Oncology PSMMS Outline Introduction. Brief review of hemostatic mechanisms. A clinical aspect of
Routine preoperative coagulation tests: are they necessary? Dr Azzah Alzahrani MD Pediatrics Hematology /Oncology PSMMS Outline Introduction. Brief review of hemostatic mechanisms. A clinical aspect of
Topics of today lectures: Hemostasis
 Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Chapter 19 Cardiovascular System Blood: Functions. Plasma
 Chapter 19 Cardiovascular System Blood: Functions 19-1 Plasma Liquid part of blood. Colloid: liquid containing suspended substances that don t settle out of solution 91% water. Remainder proteins, ions,
Chapter 19 Cardiovascular System Blood: Functions 19-1 Plasma Liquid part of blood. Colloid: liquid containing suspended substances that don t settle out of solution 91% water. Remainder proteins, ions,
DIC. Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated.
 Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric
 Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric Hematology/Oncology Sanford Children s Specialty Clinic Sioux
Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric Hematology/Oncology Sanford Children s Specialty Clinic Sioux
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN. All children in whom there is concern regarding bruising / bleeding
 GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
It s a bird, It s a plane, No It s a. Presented by Julie Kirkegaard & Miche Swofford
 It s a bird, It s a plane, No It s a Presented by Julie Kirkegaard & Miche Swofford 55 year old woman admitted 11/23/2015 for colon cancer that metastasized to her liver History of 3 pregnancies Surgery
It s a bird, It s a plane, No It s a Presented by Julie Kirkegaard & Miche Swofford 55 year old woman admitted 11/23/2015 for colon cancer that metastasized to her liver History of 3 pregnancies Surgery
M B Garvey. University of Toronto
 Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
Most Common Hemostasis Consults: Thrombocytopenia
 Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
GUIDELINES FOR THE TRANSFUSION OF BLOOD COMPONENTS
 CHILDREN S HOSPITALS AND CLINICS OF MINNESOTA Introduction: GUIDELINES FOR THE TRANSFUSION OF BLOOD COMPONENTS These guidelines have been developed in conjunction with the hospital Transfusion Committee.
CHILDREN S HOSPITALS AND CLINICS OF MINNESOTA Introduction: GUIDELINES FOR THE TRANSFUSION OF BLOOD COMPONENTS These guidelines have been developed in conjunction with the hospital Transfusion Committee.
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
Rare Bleeding Disorders
 Rare Bleeding Disorders Item type Authors Publisher Other Irish Haemophilia Society (IHS) Irish Haemophilia Society (IHS) Downloaded 20-Jun-2018 06:21:18 Link to item http://hdl.handle.net/10147/575445
Rare Bleeding Disorders Item type Authors Publisher Other Irish Haemophilia Society (IHS) Irish Haemophilia Society (IHS) Downloaded 20-Jun-2018 06:21:18 Link to item http://hdl.handle.net/10147/575445
Blood Lecture Test Questions Set 2 Summer 2012
 Blood Lecture Test Questions Set 2 Summer 2012 1. Leukocytes are attracted to a site of injury or disease by: a. diapedesis b. chemotaxis c. leukocytosis d. heparin e. leukomotosis 2. Leukocytes leave
Blood Lecture Test Questions Set 2 Summer 2012 1. Leukocytes are attracted to a site of injury or disease by: a. diapedesis b. chemotaxis c. leukocytosis d. heparin e. leukomotosis 2. Leukocytes leave
