Ganglion cysts of the wrist: pathophysiology, clinical picture, and management
|
|
|
- Alannah Sanders
- 6 years ago
- Views:
Transcription
1 Curr Rev Musculoskelet Med (2008) 1: DOI /s Ganglion cysts of the wrist: pathophysiology, clinical picture, and management Warren Gude Æ Vincent Morelli Published online: 26 August 2008 Ó Humana Press 2008 Abstract This article reviews what is known about ganglion cyst formation, natural history (50% of cysts will spontaneously resolve), diagnosis, and management of this common malady. Although the exact mechanism of cyst formation is unknown, most current theories hold that extraarticular mucin droplets coalesce to form the main body of the tumor. Only subsequently are the cyst wall and pedicle (connecting the cyst to a nearby synovial joint) formed. Treatment options include watchful waiting, nonoperative aspiration/injection, and surgical removal. Although treatment is often unnecessary, many patients seeking consultation desire some form of definitive treatment. Cyst aspiration/injection is fraught with a high incidence of recurrence. Surgery generally results in lower rates of recurrence, but a higher incidence of complications. All current treatment options are suboptimal. Keywords Cyst Ganglion Wrist ganglion Ganglion cyst Pathophysiology Ganglia are benign soft tissue tumors most commonly encountered in the wrist, but which may occur in any joint. W. Gude Sports and Emergency Medicine, 600 N Robbins Rd, Boise, ID 83702, USA wwgude@yahoo.com V. Morelli (&) Family and Sports Medicine, Meharry/Vanderbilt Family Medicine, 1005 DB Todd BLvd, Nashville, TN 37208, USA morellivincent@yahoo.com Sixty to seventy percent of ganglion cysts are found in the dorsal aspect of the wrist and communicate with the joint via a pedicle. This pedicle usually originates not only at the scapholunate ligament [1], but also may arise from a number of other sites over the dorsal aspect of the wrist capsule [2]. Thirteen to twenty percent of ganglia are found on the volar aspect of the wrist, arising via a pedicle from the radio scaphoid/scapholunate interval, scaphotrapezial joint, or the metacarpotrapezial joint, in that order of frequency [3]. Ganglia arising from a flexor tendon sheath in the hand account for approximately 10% of ganglia. Occurrence in other joints as well as intraosseus and intratendinous ganglia are much less common [4]. Microscopically, the pedicle contains a tortuous lumen, connecting the cyst to the underlying joint [5]. The presence of this connection is supported by the intraoperative and arthrographic findings of Angelides and by Andren and Eiken who demonstrated movement of intra-articular contrast from the radiocarpal joint into the ganglia in 44% of patients with a dorsal wrist ganglion and 85% of patients with a volar wrist ganglion. As contrast does not appear to travel from the cyst into the joint, a one-way valve mechanism has been postulated [6, 7]. Such a one-way valve is thought to be formed by the number of small micro-cysts present in the tissue surrounding the pedicle. These micro-cysts communicate with the primary ganglion and are felt to be part of the tortuous pedicle lumen, connecting cyst to joint, and, in the process, creating the one-way valve mechanism [8]. Evaluation via electron microscopy demonstrates the wall of the ganglion to be composed of randomly oriented sheets of collagen arranged in loose layers, one on top of another. Rare cells are present in the collagen sheets and appear to be fully functional fibroblasts or mesynchymal cells. It should be emphasized that since no synovial lining
2 206 Curr Rev Musculoskelet Med (2008) 1: exists in these structures, they cannot be classified as true cysts. Though there are focal areas of mucinous degeneration in the cyst wall, neither significant global degenerative changes, necrosis nor inflammatory changes within the pseudocyst or surrounding tissues have been demonstrated [9, 10]. Analysis of cystic fluid reveals that it is a gelatinous material containing mainly hyaluronic acid and lesser amounts of glucosamine, globulins, and albumen. This fluid is different biochemically and is much thicker than intra-articular synovial fluid. The origin of the fluid has not been fully elucidated, but it has been postulated to arise from one of three mechanisms. First, it may originate from within the joint, pumped into the cyst by motion of the wrist, second, from an extra-articular degenerative process resulting in cyst formation and subsequent communication to the joint, or finally it may originate from mesenchymal cells within the cell wall. It is possible that a combination of these mechanisms contribute. Unfortunately, the origin of the ganglion itself remains as enigmatic as the origin of its fluid. Theories on cyst genesis have been difficult to prove and most are unable to account for all of the known features of the ganglion cyst. The concept that the cyst is a simple herniation of the joint capsule is difficult to support in light of the lack of synovial lining within the cyst itself. The theory that ganglion have an inflammatory etiology has been debunked by pathologic studies showing no pericystic inflammatory changes [9, 11]. Three other theories though, still warrant consideration. In the first, joint stress (acute or chronic) may lead to a rent in the joint capsule and allow leakage of synovial fluid into the peri-articular tissue. Subsequent reaction between this fluid and local tissue results in the creation of the gelatinous cystic fluid and the formation of the cyst wall. In support of this capsular rent theory, some authors have postulated that pre-existing joint pathology (periscaphiod ligamentous injury, etc.) is the underlying cause of rent/cyst formation. Joint abnormalities are thought to lead to altered biomechanics, eventual weakening of the capsule, and finally leakage of fluid, and cyst formation. However, despite arthroscopic findings confirming the presence of intra-articular joint pathology in 50% of ganglion patients, no correlation between this pathology and postoperative cyst recurrence can be demonstrated. This leads some to conclude that intra-articular pathology is not the inciting event in the rent theory of ganglion formation. Alternatively, joint stress may lead to mucioid degeneration of adjacent extra-articular connective tissue with subsequent fluid accumulation and eventual cyst formation. This theory holds that the cyst and pedicle form a direct connection to the joint only after the creation of the cystic. Lastly, some believe that joint stress may stimulate mucin secretion by the mesenchymal cells detected by electron microscopy in the surrounding tissues. The final common pathway of all of these theories is the coalescence of small pools of mucin to form the main cyst. Production of the surrounding pseudocapsule is induced by an unknown mechanism, though possibly from compression of surrounding tissues [4, 12 14]. Clinical picture On examination, wrist ganglion are usually 1 2 cm cystic structures, feeling much like a firm rubber ball that is well tethered in place by its attachment to the underlying joint capsule or tendon sheath. There is no associated warmth or erythema and the cyst readily transilluminates. The clinical presentation is usually adequate for diagnosis, and X-ray evaluation is rarely indicated (except in the case of occult wrist ganglion where MRI is needed to make a diagnosis). Symptoms include aching in the wrist that may also radiate up the patient s arm, pain with activity or palpation of the mass, decreased range of motion and decrease grip strength. Volar ganglia may also cause paresthesias from compression of the ulnar or median nerves or their branches [4, 15]. The cause of pain is unknown but, in the case of dorsal ganglia, has been postulated to be from compression of the terminal branches of the posterior interroseus nerve [16]. There is some difference of opinion as to the frequency of pain. Thornburg reports that a painless mass is the most common presenting complaint, and Gang and Makhlouf support this noting that less than one third of patients involved in their study reported pain and that it was invariably mild. Zubowicz and other authors report that most of their patients did not have pain [17, 18]. On the other hand, various other studies report pain in % of patients [3, 8, 19, 20]. In one study, 89% of patients reported pain but only 19% felt that it interfered with normal daily activities [2]. The most likely conclusion is that pain, even when present, is more likely to be annoying than debilitating. Management The management of ganglion cysts has weighed on the conscious of medicine for some time. According to Heister (1743), The inspissated matter of a ganglion may often be happily dispersed by rubbing the tumor well each morning with fasting saliva and binding a plate of lead upon it for several weeks successively Others prefer a bullet that has killed some wild creature, especially a stag.
3 Curr Rev Musculoskelet Med (2008) 1: Sometimes, indeed, a recent ganglion will speedily vanish by adding a repeated pressure with the thumb or a wooden mallet. If none of these means prove effectual they may be safely removed by incision provided you are careful to avoid the adjacent tendons and ligaments. But as for rubbing them with the hand of a dead man and the like I presume, my reader will excuse me from insisting on them [2]. Although the methods of Heister have since been abandoned by the medical community, other scientifically unfounded treatment methods have taken their place. As could be expected, results have proven inconsistent and unreliable. For example, closed rupture with digital pressure or a book, hence the name Bible cyst, demonstrates recurrence rates of 22 64% [21], and offends the sensibilities of the fastidious patient or physician [16]. Our current (suboptimal) treatment of choice is aspiration the mainstay of nonsurgical treatment. Studies have shown remarkably variable rates of success. Zubowicz reported 85% success with up to three aspirations. He does, note that failure was much more common with each subsequent aspiration, a fact confirmed by other studies, of which some report no benefit with repeat aspiration [22, 23]. The impressive results of Zubowicz have been elusive in subsequent investigations, and, most studies, even with repeat aspirations, demonstrate a success rate of only 30 50%. It should be noted that aspiration appears to be significantly more successful in ganglia of the flexor tendon sheath of the hand with success up to 60% or 70% of the time [24 26]. Additionally, some authors note the poorest success rates with aspirations of volar ganglia of the wrist and recommend against this procedure due to the risk of adjacent structures, including the radial artery and the palmar cutaneous branch of the median nerve [4, 12, 23]. However, Wright et al. report that conservative treatment (of volar ganglia) with aspiration is often recommended and aspiration of volar ganglia has been included in a number of studies [23, 24, 27]. Aspiration should probably be based on physician experience and patient symptomatology. This may be a use for ultrasoundguided aspiration as has been advocated by some [11, 15]. To improve upon the success rate of simple aspiration, numerous adjunctive measures have been developed. Based on the mistaken theory that ganglia are inflammatory in origin, Becker, in 1953, introduced steroid injection after aspiration. Derbyshire, in 1966, reported a remarkable 86% success rate, but in a study of only 22 patients, some of whom were followed for only 2 months, and such lofty results have not been reproduced. In fact, success is really no better than aspiration alone [22] as would be expected since there is no evidence supporting inflammation as the cause of ganglia. As noted by Thornburg, Injection of corticosteroids at the time of aspiration has not proved beneficial. To obtain more complete drainage of the cyst s mucinous contents, instillation of hyaluranidase prior to aspiration has been advocated. It has also been purported that hyaluronidase makes the ganglion wall more permeable to steroids instilled after aspiration, but there was no elaboration on the mechanism by which hyaluronidase would affect the collagenous cyst wall [Paul and Sochart]. Otu reported a success rate of 95% in the initial study of this technique. Subsequent trials have demonstrated much less optimistic results [14, 17, 21]. In fact, results appear no better than simple aspiration alone, probably based on the fact that neither technique addresses the actual cause of the cyst. Several authors have attempted splinting the wrist after aspiration (and surgery) to prevent wrist motion from pumping synovial fluid through the one-way valve mechanism and refilling the cyst. This also has proven no more effective than simple aspiration and in postoperative patients leads to prolonged joint stiffness and decreased range of motion [20, 24, 25]. Ironically, since the use of steroids remains fairly common, a number of techniques have been developed that are actually designed to increase inflammation within the ganglia to enhance scarring and thus close the potential space of the empty cyst and prevent recurrence. These include aspiration with multiple punctures of the wall, aspiration with injection of a sclerosant, and a thread technique in which two loops of silk suture are passed through the cyst and the ends left protruding for 3 weeks. This is to provide a path for drainage of re-accumulated ganglion fluid to drain and to enhance scar formation via the presence of a foreign body. Multiple punctures and simple aspiration yield similar results [24, 25, 28]. Injection of sclerosant has been used in numerous patients in the past, and McEvedy reported an 82% success rate. This procedure, however, fell out of favor after studies demonstrated a connection between the ganglion and the joint [5, 6]. Mackie et al. reassessed this technique in 1985, but had a 93% recurrence rate. Additionally, they demonstrated significant inflammatory injury when the sclerosant was injected into the tendons of chickens and joints of rats. Lack of success and potential side effects have led to a general abandonment of this approach [5, 29]. The thread technique, though successful in a single study, has not been widely adopted based on concerns of infection [4, 30]. It seems logical that efforts at enhancing inflammation and subsequent scarring within the ganglia would meet with limited success because the wall of the cyst is essentially acellular, and, thus, possesses limited potential to produce any mediators of inflammation. A review of the history of the studies listed in Table 1 indicates a pattern of remarkable early success that is unable to be reproduced in subsequent investigations.
4 208 Curr Rev Musculoskelet Med (2008) 1: Table 1 Review of studies Method Recurrence rate (%) Follow-up Aspiration 1. Nield and Evans 59 1 year 2. Varley 67 (no improvement with multiple aspirations) 4 months 3. Zubowicz 15 (multiple aspirations) 1 year 4. Stephen et al Dias and Buch 47 2 and 5 years 6. Westbrook 49 6 weeks Average 51 Aspiration and steroid 1. Derbyshire 14 2 months 5 years 2. Paul and Sochart Wright et al. 83 (even with repeat aspirations) 4. Breidahl and Adler 60 Average 52 Aspiration with hyaluronidase 1. Otu 5 6 months 2. Paul and Sochart 51 2 years 3. Nelson years 4. Jagert 77 1 year Average 44 Aspiration and sclerosant 1. McEvedy years 2. Mackie 93 3 months Average 55 Aspiration with splinting 1. Korman et al. 48 (same as nonimmobilized) 1 year 2. Richman et al. 60 (better than nonimmobilized control) 22 months Average 54 Aspiration with multiple puncture 1. Stephen et al Richman et al months 3. Korman et al months Average 64 Potential causes of this variability include the fact that many studies are small and may introduce statistical error. Follow-up is often incomplete, at times, no better than 70 80%, and of variable length [22, 25, 27, 28, 31, 32]. This is significant since the natural history of the ganglion is one of spontaneous regression in up to half of patients (Table 2). Studies with an extended period of follow-up may incorrectly include cysts that naturally resolved as an indication of a successful intervention. On the other hand, follow-up that is too brief may not provide adequate time for recurrence. In short, results from nonsurgical treatment appear no better than expectant management and carries up to a 5% complication rate [27] (It should be noted that these same difficulties with study design are common in investigations of surgical ganglion management) [1, 2, 23]. For example, follow-up was only 28% in one study, and, clearly, overall results might be quite different with inclusion of such a large number of unaccounted for patients [3]. Surgical excision remains the gold standard for treatment of ganglion cysts. Prior to the work of Angelides, postoperative recurrence rates were as high as 40%, results that were rivaled by expectant management. Since the adoption of surgical techniques that include excision of the entire ganglion complex, including cyst, pedicle, and a cuff of the adjacent joint capsule, recurrence rates have improved significantly. Some authors claim recurrence rates for dorsal wrist ganglia as low as 1 5% [1] and as low as 7% for volar wrist ganglia [4]. Generally, higherreported rates of recurrence are attributed to inadequate dissection in which the tortuous duct system located at the joint capsule is not fully excised.
5 Curr Rev Musculoskelet Med (2008) 1: Table 2 Expectant management Study Spontaneous resolution Follow-up 1. Westbrook et al. (2002) 5/11 (45%) 4 months 2. McEvedy [7] 10/21 (47.6%) 12 years 3. Carp and Stout (1928) 7/12 (58%) 3 years 4. Rossen and Walker (1989) 22/29 (76%) 5 years (Involved only children) 20/29 (70%) 2 years 5. Dias and Buch [27] 20/38 (53%) 2 and 5 years 6. Zachariae and 40/101 (40%) 6 years Vibe-Hansen (1973) Average 49% Despite the remarkably low postoperative recurrence rates often reported, a review of the literature actually appears to demonstrate higher rates of recurrence. A significant number of patients included in studies of dorsal wrist ganglia are actually undergoing a second surgery after cyst recurrence. This may triple the number of patients reported to have had a recurrence at the conclusion of the investigation. Even if only a small percentage of patients experienced a recurrence during the study period, it does not mean that the patients undergoing a repeat operation did not have a recurrence. Although the authors of the article may have exceptional skill and an exceedingly low recurrence rate, it would appear that in the context of day-to-day patient care, it may not be possible for all surgeons to obtain the results published by highly experienced surgeons or from high volume specialty hand clinics. Greendyke notes in his discussion that both recurrences in his study occurred early in the authors experience with these lesions. It is likely that patients will seek care from surgeons with similar levels of experience, thus making recurrence more common than what is reported in many studies. As noted above, adding in the patients who are undergoing a second surgery with those who experience a recurrence while the study is ongoing, the average rate of recurrence jumps from 5.6% to 16%. (This calculation is the same if you exclude Satko and Ganesh, as they only studied children, and Angelides, who might be excluded for several reasons. First, prior to this study, complete excision of the ganglion complex was not as commonly practiced and could negatively skew the calculations. Second, no other study has even approached this degree of success, with a phenomenal recurrence rate of only 0.6%.) The question is not whether recurrence of 5% or 7% can be achieved, but rather, what recurrence rate actually occurs in the general surgical community. Although Angelides achieved remarkable success, it has not been demonstrated that these results will be consistently replicated. The complication rate and recurrence rate of volar wrist ganglia are not the same as that of dorsal wrist ganglia. As the origin of volar ganglia is more variable and access is more difficult due to adjacent neurovascular structures, recurrence of volar ganglia may be as high as 42% and may average 30%. Complications are also more common, reaching rates [20% in some studies [20, 27]. Jacobs and Govaers identified surgeon inexperience as a risk factor for higher recurrence rates and concluded one cannot be confident that surgical excision of volar ganglia will be successful. Surgery improves the rate of ganglion resolution and generally provides good to excellent results, but is not a panacea, and thus, the development and continued use of numerous nonsurgical techniques. It has been estimated that initial nonsurgical management of patients would save 100,000 dollars per 100 patients, though this study probably reports an unrealistically high success rate with aspiration (85%) and assumes that all patients with a recurrence will opt for surgery [32]. Additionally, there is the cost of postoperative time lost from work, which is documented to be as long as 24 days and may average as long as 2 weeks. This may represent a significant indirect cost [8, 16, 20, 27, 33]. Despite excellent results by a number of authors with low complication and recurrence rates, surgery is not without risk. Complications include infection, neuroma, unsightly scar, and keloid. Additionally, postoperative stiffness, grip weakness, and decreased range of motion may occur. Rizzo reported stiffness in 25% of patients and required up to 8 weeks and occupational therapy to regain maximal function. Wright reported that 14% of patients complained of limitation of activities due to loss of wrist motion. Postoperative pain is not uncommon [8, 19, 32, 33]. Several authors have documented a relationship to open ganglionectomy and scapholunate instability. It has, though, been postulated that instability is not the result of surgery, but rather the pre-existing cause of the ganglion [13, 17, 34, 35]. Damage to the palmar cutaneous branch of the median nerve and radial artery are at risk during surgery for volar ganglia [4, 20, 27]. Dias and Buch report a recurrence rate of 42% and a complication rate of 20% in their study of volar ganglia. Additionally, 8% of their patients report being worse postoperatively. Clay and Clement noted that 21% of their patients undergoing surgery of dorsal wrist ganglia were no better or worse after surgery. And this number does not include the fact that 11% of patients involved in the study were undergoing a repeat excision for a recurrent cyst. Equally informative is the fact that many patients who have a postoperative or even postaspiration cyst recurrence elect to not undergo a second operation (Table 3). Wright et al. operated on only 29% of recurrences and Jacobs and Govaers insightfully noted, Only five of twenty [patients]
6 210 Curr Rev Musculoskelet Med (2008) 1: Table 3 (a) Patients undergoing procedures (aspiration, injection, etc.) who experience recurrence and request further intervention and (b) patients undergoing surgery who experience cyst recurrence and request further intervention (a) Procedure 1. Stephen et al. 21/119 (18%) 2. Wright et al. 12/24 (50%) 3. Varley et al. 22/57 (38%) 4. Westbrook et al. 2/50 (4%) (b) Surgery 1. Wright et al. 4/14 (29%) 2. Jacobs and Govaers 5/20 (25%) Further intervention (surgery) with recurrence had enough symptoms from it to warrant a second operation. This is not to imply that surgery is not the most effective available treatment option or that complications are so onerous as to make surgery too risky. Rather it appears to represent the patient s perception of the ganglion as a disease. In the only study to address why patients actually seek medical attention for ganglia, Westbrook found that 38% expressed cosmetic concerns, 28% were concerned about malignancy, and only 26% presented because of pain. This supports the conclusions of other authors that pain, no matter how commonly it is present, is rarely significant or impairs activity and is not usually the impetus for seeking medical care [2, 7, 17, 18, 20, 23, 30, 32]. As cosmesis is a common concern, surgery may simply be exchanging an unsightly lump with a 50% chance of spontaneous resolution for an unsightly and permanent scar [16, 20]. The literature supports the fact that a significant number of ganglia will undergo spontaneous resolution with some authors stating that, in the majority this will occur with in a couple of years (Table 2). An explanation of the benign nature of the cyst, combined with a discussion of its natural history of regression will often alleviate patient fears and desire for surgery. This may be especially true with aspiration of the cyst to provide temporary relief of any symptoms and to demonstrate the innocuous nature of its contents [4, 18]. Westbrook noted that in 52% of patients treated via aspiration or with expectant management, the ganglion was still present at 6 weeks, yet none requested further intervention. Out of a total of 50 patients, only two consented to surgery. In numerous operative and nonoperative studies, patient satisfaction far exceeds the actual rate of ganglion resolution, implying that concerns over what the ganglion represents are more important to the patient than its actual presence [17, 18, 22, 27]. It would appear that the ganglion cyst is more commonly a nuisance than a significant medical problem, even in the mind of the patient. The cyst will often be tolerated in lieu of an invasive procedure [22, 28]. In the absence of function limiting symptoms, McEvedy may have been correct when he commented that ganglia are a benign condition taking up the time of competent surgeons who might be more usefully engaged. Conclusion The interest in ganglia and the wide variety of treatments that have been developed are probably a result of its frequent presentation to physicians and lack of a fully satisfactory mode of treatment. Aspiration is a beneficial and simple option for acute management, but appears to have little long-term impact on resolution. Current adjunctive measures, on the other hand, provide no benefit over aspiration alone. Surgery offers improved resolution of ganglia, but is often more invasive than is warranted by patient symptoms [31]. Individual patient concerns regarding the ganglion cyst must first be ascertained. Using a thorough knowledge of the natural history of ganglia and the available treatment options and outcomes, the physician can provide guidance as the patient selects the most appropriate course of action for their circumstances. References 1. Angelides AC, Wallace PF. The dorsal ganglion of the wrist: its pathogenesis, gross and microscopic anatomy, and surgical treatment. J Hand Surg. 1976;1(3): Clay NR, Clement DA. The treatment of dorsal wrist ganglia by radical excision. J Hand Surg. 1988;13(2): Greendyke SD, Wilson M, Shepler TR. Anterior wrist ganglia from the scaphotrapezial joint. J Hand Surg. 1992;17(3): Thornburg LE. Ganglions of the hand and wrist. J Am Acad Orthop Surg. 1999;7(4): Tophoj K, Henriques U. Ganglion of the wrist a structure developed from the joint. Acta Orthop Scand. 1971;42(3): Andren L, Eiken O. Arthrographic studies of wrist ganglions. J Bone Joint Surg Am. 1971;53(2): McEvedy BV. The simple ganglion. A review of modes of treatment and an explanation of the frequent failures of surgery. Lancet. 1954;266(6803): Osterman AL, Raphael J. Arthroscopic treatment of dorsal ganglion of the wrist. Hand Clin. 1995;11: Psalia JV, Mansel RE. The surface ultrastructure of ganglia. J Bone Joint Surg Br. 1978;60-B(2): Loder RT, Robinson JH, Jackson WT, Allen DJ. A surface ultrastructure study of ganglia and digital mucous cysts. J Hand Surg. 1988;13(5): Breidahl WH, Adler RS. Ultrasound-guided injection of ganglia with corticosteroids. Skeletal Radiol. 1996;25(7): Nahra ME, Bucchieri JS. Ganglion cysts and other tumor related conditions of the hand and wrist. Hand Clin. 2004;20(3): Duncan KH, Lewis RC. Scapholunate instability following ganglion cyst excision: a case report. Clin Orthop Relat Res. 1988;228:250 3.
7 Curr Rev Musculoskelet Med (2008) 1: Jagers M, Akkerhuis P, Van Der Heijden M, Brink PRG. Hyaluronidase versus surgical excision of ganglia: a prospective, randomized clinical trial. J Hand Surg. 2002;27(3): Nishikawa S, Toh S, Miura K, Arai K, Irie T. Arthroscopic diagnosis and treatment of dorsal wrist ganglion. J Hand Surg. 2001;26(6): Derbyshire RC. Observations on the treatment of ganglia with a report on hydrocortisone. Am J Surg. 1966;112(5): Paul AS, Sochart DH. Improving the results of ganglion aspiration by the use of hyaluronidase. J Hand Surg. 1997;22(2): Westbrook AP, Stephen AB, Oni J, Davis TR. Ganglia: the patient s perception. J Hand Surg. 2000;25(6): Rizzo M, Berger R, Steinmann S, Bishop A. Arthroscopic resection in the management of dorsal wrist ganglions: results with a minimum two-year follow-up period. J Hand Surg. 2004;29(1): Jacobs LGH, Govaers KHM. The volar wrist ganglion: just a simple cyst? J Hand Surg. 1990;15(3): Nelson CL, Sawmiller S. Phalen GS: ganglions of the wrist and hand. J Bone Joint Surg Am. 1972;54(7): Varley GW, Neidoff M, Davis TRC, Clay NR. Conservative management of wrist ganglia: aspiration versus steroid infiltration. J Hand Surg. 1997;22(5): Wright TW, Cooney WP, Ilstrup M. Anterior wrist ganglion. J Hand Surg. 1994;19(6): Richman JA, Gelberman RH, Engber WD, Salamon PB, Bean DJ. Ganglions of the wrist and digits and results of treatment by aspiration and cyst wall puncture. J Hand Surg. 1987;12(6): Korman J, Pearl R, Hentz VR. Efficacy of immobilization following aspiration of carpal and digital ganglions. J Hand Surg. 1992;17(6): Bruner JM. Treatment of sesamoid synovial ganglia of the hand by needle rupture. J Bone Joint Surg Am. 1963;45: Dias J, Buch K. Palmar wrist ganglion: does intervention improve outcome? J Hand Surg. 2003;28(2): Stephen AB, Lyons AR, Davis TRC. A prospective study of two conservative treatments for ganglia of the wrist. J Hand Surg. 1999;24(1): Mackie IG, Howard CB, Wilkens P. The dangers of sclerotherapy in the treatment of ganglia. J Hand Surg. 1984;9(2): Gang RK, Makhlouf S. Treatment of ganglia by a thread technique. J Hand Surg. 1988;13(2): Oni JA. Letter to the editor. J Hand Surg. 1993;18B: Zubowicz VN, Ischii CH. Management of ganglion cysts of the hand by simple aspiration. J Hand Surg. 1987;12(4): Luchetti R, Badia A, Alfarano M, Orbay J, Indriago I, Mustapha B. Arthroscopic resection of dorsal wrist ganglia and treatment of recurrences. J Hand Surg. 2000;25(1): Crawford GP, Taleisnik J. Rotary subluxation of the scaphoid after excision of dorsal carpal ganglion and wrist manipulation: a case report. J Hand Surg. 1983;8(6): Watson HK, Rogers WD, Ashmead DIV. Re-evaluation of the cause of the wrist ganglion. J Hand Surg. 1989;14(5):812 7.
Arthroscopic resection of dorsal wrist ganglion
 International Journal of Research in Orthopaedics Patel MR et al. Int J Res Orthop. 2016 Sep;2(3):127-131 http://www.ijoro.org Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20162871
International Journal of Research in Orthopaedics Patel MR et al. Int J Res Orthop. 2016 Sep;2(3):127-131 http://www.ijoro.org Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20162871
A Patient's Guide to Ganglions of the Wrist
 Introduction A ganglion is a small, harmless cyst, or sac of fluid, that sometimes develops in the wrist. Doctors don't know exactly what causes ganglions, but a ganglion that isn't painful and doesn't
Introduction A ganglion is a small, harmless cyst, or sac of fluid, that sometimes develops in the wrist. Doctors don't know exactly what causes ganglions, but a ganglion that isn't painful and doesn't
Volar Wrist Ganglion: A Report of an Unusual Case. Eyad Alqasim, MD* Rashid Kameshki, MBBS** Maged Mostafa, MD***
 Bahrain Medical Bulletin, Vol. 34, No. 3, September 2012 Volar Wrist Ganglion: A Report of an Unusual Case Eyad Alqasim, MD* Rashid Kameshki, MBBS** Maged Mostafa, MD*** A patient presented with wrist
Bahrain Medical Bulletin, Vol. 34, No. 3, September 2012 Volar Wrist Ganglion: A Report of an Unusual Case Eyad Alqasim, MD* Rashid Kameshki, MBBS** Maged Mostafa, MD*** A patient presented with wrist
A new method in the management of wrist ganglion (Silk thread passed through the ganglion); in comparison with other traditional methods
 A new method in the management of wrist ganglion (Silk thread passed through the ganglion); in comparison with other traditional methods Abdulqadir M. Zangana (1) Kawa F. Dizaye (2) (1) Professor of Surgery,
A new method in the management of wrist ganglion (Silk thread passed through the ganglion); in comparison with other traditional methods Abdulqadir M. Zangana (1) Kawa F. Dizaye (2) (1) Professor of Surgery,
A Patient s Guide to Ganglions of the Wrist
 A Patient s Guide to Ganglions of the Wrist 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Ganglions of the Wrist 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
ISSN X (Print) Original Research Article. College, Hospital & Research Institute, Budhera, Gurgaon , Haryana, India
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(4D):1366-1370 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(4D):1366-1370 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Excision of painful dorsal wrist ganglion by open or arthroscopic approach : a compariso n study
 Acta Orthop. Belg., 2015, 83, 315-321 ORIGINAL STUDY Excision of painful dorsal wrist ganglion by open or arthroscopic approach : a compariso n study Hyun l.l. Lee, Keun Ho Lee, Kyoung Hwan Koh, Hee Jae
Acta Orthop. Belg., 2015, 83, 315-321 ORIGINAL STUDY Excision of painful dorsal wrist ganglion by open or arthroscopic approach : a compariso n study Hyun l.l. Lee, Keun Ho Lee, Kyoung Hwan Koh, Hee Jae
Interesting Case Series. Ganglion Cyst of the Peroneus Longus
 Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
2013/10/18 GANGLION CYSTS ENDOSCOPIC GANGLIONECTOMY ARTHROSCOPIC GANGLIONECTOMY OPEN GANGLIONECTOMY COMPARED TO FOOT AND ANKLE
 GANGLION CYSTS gelatinous fluid filled, encapsulated soft tissue masses adjacent to a joint or tendon ENDOSCOPIC GANGLIONECTOMY OF THE FOOT AND ANKLE Dr TH Lui North District Hospital HKSAR Pain, mass
GANGLION CYSTS gelatinous fluid filled, encapsulated soft tissue masses adjacent to a joint or tendon ENDOSCOPIC GANGLIONECTOMY OF THE FOOT AND ANKLE Dr TH Lui North District Hospital HKSAR Pain, mass
PATIENTS, METHODS AND RESULTS
 WRIST GANGLION Pages with reference to book, From 123 To 124 Ijaz Ahmad ( Department of Surgery, King Edward Medical College, Lahore. ) Ganglia account for about two third of all hand tumours 1. They occur
WRIST GANGLION Pages with reference to book, From 123 To 124 Ijaz Ahmad ( Department of Surgery, King Edward Medical College, Lahore. ) Ganglia account for about two third of all hand tumours 1. They occur
Endoscopic surgery has gained much popularity
 Sonography-Assisted Arthroscopic Resection of Volar Wrist Ganglia: A New Technique Michiro Yamamoto, M.D., Ph.D., Shigeru Kurimoto, M.D., Nobuyuki Okui, M.D., Ph.D., Masahiro Tatebe, M.D., Ph.D., Takaaki
Sonography-Assisted Arthroscopic Resection of Volar Wrist Ganglia: A New Technique Michiro Yamamoto, M.D., Ph.D., Shigeru Kurimoto, M.D., Nobuyuki Okui, M.D., Ph.D., Masahiro Tatebe, M.D., Ph.D., Takaaki
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS. Renita Sirisena Mark Puhaindran
 TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
CARPAL TUNNEL SYNDROME
 CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley.
 TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
A Patient s Guide to Mucous Cysts of the Fingers
 A Patient s Guide to Mucous Cysts of the Fingers Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can better
A Patient s Guide to Mucous Cysts of the Fingers Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can better
ADHESIVE CAPSULITIS (FROZEN SHOULDER)
 ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
University of Groningen. Fracture of the distal radius Oskam, Jacob
 University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Triangular Fibrocartilage Complex Repair. The triangular fibrocartilage complex (TFCC) is one of the main stabilizers of the
 Michelle Brandt and Megan Passarelle Surgical Assignment Due: 11/9/14 Triangular Fibrocartilage Complex Repair Abstract The triangular fibrocartilage complex (TFCC) is one of the main stabilizers of the
Michelle Brandt and Megan Passarelle Surgical Assignment Due: 11/9/14 Triangular Fibrocartilage Complex Repair Abstract The triangular fibrocartilage complex (TFCC) is one of the main stabilizers of the
Health Technology Assessment of Scheduled Procedures
 Health Technology Assessment of Scheduled Procedures Ganglion Cyst Surgery December 2013 Safer Better Care 1 2 About the The (HIQA) is the independent Authority established to drive continuous improvement
Health Technology Assessment of Scheduled Procedures Ganglion Cyst Surgery December 2013 Safer Better Care 1 2 About the The (HIQA) is the independent Authority established to drive continuous improvement
Workplace Hand Injuries & Disorders: Evaluation and Treatments. Hervey L. Kimball MD, MS Hand Surgical Associates Occupational Medicine Center
 Workplace Hand Injuries & Disorders: Evaluation and Treatments Hervey L. Kimball MD, MS Hand Surgical Associates Occupational Medicine Center Outline Hand Anatomy and Function Workplace injuries & Case
Workplace Hand Injuries & Disorders: Evaluation and Treatments Hervey L. Kimball MD, MS Hand Surgical Associates Occupational Medicine Center Outline Hand Anatomy and Function Workplace injuries & Case
The Painful Elbow, Wrist, and Hand. Jennifer R Marks, MD
 The Painful Elbow, Wrist, and Hand Jennifer R Marks, MD The Painful Elbow A 44 yo M presents to clinic complaining of a sore elbow What further questions do you have for this patient? What is on your differential
The Painful Elbow, Wrist, and Hand Jennifer R Marks, MD The Painful Elbow A 44 yo M presents to clinic complaining of a sore elbow What further questions do you have for this patient? What is on your differential
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
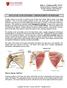 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Duputytren's Contracture
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
When is Enough, Enough. The Second Opinion: When is it time to ask for help? Introduction. Disclaimer 10/3/2017
 When is Enough, Enough Over Treatment of Upper Extremity Disorders The Second Opinion: When is it time to ask for help? Roger A. Daley M.D., Ph.D. Professor and Director Division Hand Upper Extremity and
When is Enough, Enough Over Treatment of Upper Extremity Disorders The Second Opinion: When is it time to ask for help? Roger A. Daley M.D., Ph.D. Professor and Director Division Hand Upper Extremity and
Common Tendon Disorders of the Upper Extremity. Mark Tait MD
 Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Chapter 24. Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty. Introduction. Operative Technique. Patient Preparation and Positioning
 Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Safety and Efficacy of Arthroscopic Volar Carpal Ganglion Excision: An Anatomic and Clinical Study
 DOJ Safety and Efficacy of Arthroscopic Volar Carpal Ganglion Excision: 10.5005/jp-journals-10017-1046 An Anatomic and Clinical Study Retrospective review Safety and Efficacy of Arthroscopic Volar Carpal
DOJ Safety and Efficacy of Arthroscopic Volar Carpal Ganglion Excision: 10.5005/jp-journals-10017-1046 An Anatomic and Clinical Study Retrospective review Safety and Efficacy of Arthroscopic Volar Carpal
Common Hand Problems and Case Examples. September 22, 2017 Carolyn Berg, MD Advanced Orthopedics of Oklahoma
 Common Hand Problems and Case Examples September 22, 2017 Carolyn Berg, MD Advanced Orthopedics of Oklahoma Sometimes the problem is obvious Sometimes the problem is everywhere Anatomy Skin Tendon Extrinsic
Common Hand Problems and Case Examples September 22, 2017 Carolyn Berg, MD Advanced Orthopedics of Oklahoma Sometimes the problem is obvious Sometimes the problem is everywhere Anatomy Skin Tendon Extrinsic
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome Concord Orthopaedics 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this
A Patient s Guide to Carpal Tunnel Syndrome Concord Orthopaedics 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Carpal Tunnel Syndrome 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
Arhtroscopy of the wrist joint: Setup, instrumentation, anatomy & indications
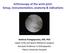 Arhtroscopy of the wrist joint: Setup, instrumentation, anatomy & indications Andreas Panagopoulos, MD, PhD Upper Limb and Sports Medicine Surgeon Assistant Professor in Orthopaedics Patras University
Arhtroscopy of the wrist joint: Setup, instrumentation, anatomy & indications Andreas Panagopoulos, MD, PhD Upper Limb and Sports Medicine Surgeon Assistant Professor in Orthopaedics Patras University
Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet Page 1 Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a common problem which affects the hand and wrist. Symptoms are caused
Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet Page 1 Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a common problem which affects the hand and wrist. Symptoms are caused
Volar Plate Avulsion Fractures
 Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) William T. Grant, MD
 A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
Common Hand Conditions SHAMIM UMARJI MA (Oxon) FRCS (Tr & Orth) CONSULTANT TRAUMA & ORTHOPAEDIC SURGEON
 Common Hand Conditions SHAMIM UMARJI MA (Oxon) FRCS (Tr & Orth) CONSULTANT TRAUMA & ORTHOPAEDIC SURGEON Common Hand Conditions Carpal tunnel syndrome Dupuytren s Disease Ganglia Trigger Digits De Quervain
Common Hand Conditions SHAMIM UMARJI MA (Oxon) FRCS (Tr & Orth) CONSULTANT TRAUMA & ORTHOPAEDIC SURGEON Common Hand Conditions Carpal tunnel syndrome Dupuytren s Disease Ganglia Trigger Digits De Quervain
Interesting Case Series. Dupuytren s Contracture
 Interesting Case Series Dupuytren s Contracture Aditya Sood, MD, Angie Paik, BA, and Edward Lee, MD Division of Plastic Surgery, University of Medicine and Dentistry of New Jersey, Newark, NJ Correspondence:
Interesting Case Series Dupuytren s Contracture Aditya Sood, MD, Angie Paik, BA, and Edward Lee, MD Division of Plastic Surgery, University of Medicine and Dentistry of New Jersey, Newark, NJ Correspondence:
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Proximal row carpectomy : a motion-preserving procedure in the treatment of advanced Kienbock s disease
 Acta Orthop. Belg., 2006, 72, 530-534 ORIGINAL STUDY Proximal row carpectomy : a motion-preserving procedure in the treatment of advanced Kienbock s disease Hani EL-MOWAFI, Mahmoud EL-HADIDI, Esam EL-KAREF
Acta Orthop. Belg., 2006, 72, 530-534 ORIGINAL STUDY Proximal row carpectomy : a motion-preserving procedure in the treatment of advanced Kienbock s disease Hani EL-MOWAFI, Mahmoud EL-HADIDI, Esam EL-KAREF
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Introduction. The wrist contains eight small carpal bones, which as a group act as a flexible spacer between the forearm and hand.
 Wrist Introduction The wrist contains eight small carpal bones, which as a group act as a flexible spacer between the forearm and hand. Distal forearm Distal forearm 4 Distal end of the radius A. anterior
Wrist Introduction The wrist contains eight small carpal bones, which as a group act as a flexible spacer between the forearm and hand. Distal forearm Distal forearm 4 Distal end of the radius A. anterior
Interesting Case Series. Perilunate Dislocation
 Interesting Case Series Perilunate Dislocation Tom Reisler, BSc (Hons), MB ChB, MRCS (Ed), Paul J. Therattil, MD, and Edward S. Lee, MD Division of Plastic and Reconstructive Surgery, Department of Surgery,
Interesting Case Series Perilunate Dislocation Tom Reisler, BSc (Hons), MB ChB, MRCS (Ed), Paul J. Therattil, MD, and Edward S. Lee, MD Division of Plastic and Reconstructive Surgery, Department of Surgery,
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Frozen Shoulders FAQs. Dr Kelvin TAM
 Frozen Shoulders FAQs Dr Kelvin TAM Summary Shoulder pain is a common problem. Shoulder pain is commonly labeled frozen shoulder. But what is frozen shoulder? Is shoulder pain always frozen shoulder or
Frozen Shoulders FAQs Dr Kelvin TAM Summary Shoulder pain is a common problem. Shoulder pain is commonly labeled frozen shoulder. But what is frozen shoulder? Is shoulder pain always frozen shoulder or
journal ORIGINAL RESEARCH
 texas orthopaedic journal ORIGINAL RESEARCH Assessment of Volar Tilt Measurements with Variations in X-Ray Beam Centralization Along the Longitudinal Axis of the Radius Russell A. Wagner, MD; Will Junius,
texas orthopaedic journal ORIGINAL RESEARCH Assessment of Volar Tilt Measurements with Variations in X-Ray Beam Centralization Along the Longitudinal Axis of the Radius Russell A. Wagner, MD; Will Junius,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Shoulder Instability Latarjet Procedure
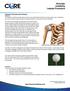 Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
Watson Classification. Proximal Row Carpectomy SLAC Wrist. Disclosure 11/13/2017. No Shiney Metal Objects Utilized NONE
 Proximal Row Carpectomy SLAC Wrist H. Brent Bamberger, D.O Program Director of Orthopaedic Residency and Hand Fellowship Nick Hollis, D. O. Hand Fellow Grandview Hospital Department of Orthopaedic Surgery
Proximal Row Carpectomy SLAC Wrist H. Brent Bamberger, D.O Program Director of Orthopaedic Residency and Hand Fellowship Nick Hollis, D. O. Hand Fellow Grandview Hospital Department of Orthopaedic Surgery
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
A Patient s Guide to Dupuytren s Contracture
 A Patient s Guide to Dupuytren s Contracture Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this booklet
A Patient s Guide to Dupuytren s Contracture Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this booklet
The Kienböck disease and scaphoid fractures. Mariusz Bonczar
 The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
Ganglion of the peroneal nerve. CULLY A. COBB, III, M.D., AND RICHARD H. MoIr4 M.D.
 Ganglion of the peroneal nerve Report of two cases CULLY A. COBB, III, M.D., AND RICHARD H. MoIr4 M.D. Division of Neurological Surgery, Baylor College of Medicine, Houston, Texas ~" Peroneal nerve ganglion
Ganglion of the peroneal nerve Report of two cases CULLY A. COBB, III, M.D., AND RICHARD H. MoIr4 M.D. Division of Neurological Surgery, Baylor College of Medicine, Houston, Texas ~" Peroneal nerve ganglion
SPORTS INJURIES IN HAND
 Grundkurs SGSM-SSMS Sion 2015 SPORTS INJURIES IN HAND Dr S. KŠmpfen EPIDEMIOLOGY Incidence of hand, finger and wrist injuries in sports : 3% Ð 9 % RADIAL-SIDED WRIST PAIN 1)! Distal Radius Fractures 2)!
Grundkurs SGSM-SSMS Sion 2015 SPORTS INJURIES IN HAND Dr S. KŠmpfen EPIDEMIOLOGY Incidence of hand, finger and wrist injuries in sports : 3% Ð 9 % RADIAL-SIDED WRIST PAIN 1)! Distal Radius Fractures 2)!
A Patient s Guide to Posterior Tibial Tendon Problems
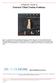 A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
A Patient s Guide to Carpal Tunnel Syndrome. William T. Grant, MD
 A Patient s Guide to Carpal Tunnel Syndrome Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Carpal Tunnel Syndrome Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
Kokko Wrist 3/11/17. Updates in General Internal Medicine for Primary Care Wrist Pain
 Updates in General Internal Medicine for Primary Care 2017 Wrist Pain Kyle P. Kokko, MD, PhD Assistant Professor Hand, Wrist, and Microvascular Surgeon MUSC Department of Orthopaedics Disclosures I pulled
Updates in General Internal Medicine for Primary Care 2017 Wrist Pain Kyle P. Kokko, MD, PhD Assistant Professor Hand, Wrist, and Microvascular Surgeon MUSC Department of Orthopaedics Disclosures I pulled
MR IMAGING OF THE WRIST
 MR IMAGING OF THE WRIST Wrist Instability Dissociative Pattern apparent on routine radiographs Non-dissociative Stress / positional radiographs Dynamic fluoroscopy during stress Arthrography MRI / MR arthrography
MR IMAGING OF THE WRIST Wrist Instability Dissociative Pattern apparent on routine radiographs Non-dissociative Stress / positional radiographs Dynamic fluoroscopy during stress Arthrography MRI / MR arthrography
Index. Note: Page numbers of article titles are in boldface type. Hand Clin 21 (2005)
 Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Hand Clin 21 (2005) 501 505 Index Note: Page numbers of article titles are in boldface type. A Antibiotics, following distal radius fracture treatment, 295, 296 Arthritis, following malunion of distal
Solitary Bone Cyst of the Lunate: A Case Report
 Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Your Arthroscopic Shoulder Procedure
 Your Arthroscopic Shoulder Procedure Education from Contents Regain Your Active Lifestyle 3 What is Arthroscopic Shoulder Surgery? 4 Who is a Candidate for Arthroscopic Shoulder Surgery? 6 Anatomy and
Your Arthroscopic Shoulder Procedure Education from Contents Regain Your Active Lifestyle 3 What is Arthroscopic Shoulder Surgery? 4 Who is a Candidate for Arthroscopic Shoulder Surgery? 6 Anatomy and
Wrist movements, apart from the distal radioulnar joint, take place in two planes:
 The wrist consists of eight bones in two rows: the proximal and distal. The proximal row includes (starting from the radial bone): the scaphoid bone, the lunate bone, the triangular bone and the postulnar
The wrist consists of eight bones in two rows: the proximal and distal. The proximal row includes (starting from the radial bone): the scaphoid bone, the lunate bone, the triangular bone and the postulnar
Work Related Musculoskeletal Disorders
 Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
Management of Chronic Elbow Pain
 Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Ultrasound-guided reduction of distal radius fractures
 American Journal of Emergency Medicine (2010) 28, 1002 1008 www.elsevier.com/locate/ajem Original Contribution Ultrasound-guided reduction of distal radius fractures Shiang-Hu Ang, Shu-Woan Lee, Kai-Yet
American Journal of Emergency Medicine (2010) 28, 1002 1008 www.elsevier.com/locate/ajem Original Contribution Ultrasound-guided reduction of distal radius fractures Shiang-Hu Ang, Shu-Woan Lee, Kai-Yet
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity
 Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
Case 1. Your diagnosis
 Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
A Patient s Guide to Popliteal Cysts
 A Patient s Guide to Popliteal Cysts 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Popliteal Cysts 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled
Scaphoid Fracture of the Wrist
 A Patient s Guide to Scaphoid Fracture of the Wrist 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Scaphoid Fracture of the Wrist 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled
Interesting Case Series. Ulnolunate Impaction Syndrome
 Interesting Case Series Ulnolunate Impaction Syndrome Saptarshi Biswas, MD, FRCS Westchester University Medical Center, Valhalla, NY Keywords: ulnar impaction, ulnar impaction syndrome, ulnar wrist pain,
Interesting Case Series Ulnolunate Impaction Syndrome Saptarshi Biswas, MD, FRCS Westchester University Medical Center, Valhalla, NY Keywords: ulnar impaction, ulnar impaction syndrome, ulnar wrist pain,
Wrist & Hand Assessment and General View
 Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
University of Groningen. Fracture of the distal radius Oskam, Jacob
 University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
Link to related CJSM article: ts Frequency_and.5.
 Link to related CJSM article: https://journals.lww.com/cjsportsmed/abstract/2002/11000/wrist_pain_in_young_gymnas ts Frequency_and.5.aspx Link to related case: https://www.amssm.org/when_a_quot%3bsimple_fractur-csa-437.html?startpos=0&part=
Link to related CJSM article: https://journals.lww.com/cjsportsmed/abstract/2002/11000/wrist_pain_in_young_gymnas ts Frequency_and.5.aspx Link to related case: https://www.amssm.org/when_a_quot%3bsimple_fractur-csa-437.html?startpos=0&part=
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 The Stiff Hand: Manual Therapy Sylvia Dávila, PT, CHT San Antonio, Texas Orthopedic Manual Therapy Common Applications Passive stretch Tensile force to tissue to increase extensibility of length & ROM
The Stiff Hand: Manual Therapy Sylvia Dávila, PT, CHT San Antonio, Texas Orthopedic Manual Therapy Common Applications Passive stretch Tensile force to tissue to increase extensibility of length & ROM
A Patient s Guide to Biceps Tendon Tears at the Elbow
 A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Early Arthroscopic Management of Heterotopic Ossification of the Elbow
 25 Early Arthroscopic Management of Heterotopic Ossification of the Elbow Felix H. Savoie III, MD; Michael J. O Brien, MD; and Matthew Wert Introduction The formation of heterotopic ossification (HO) about
25 Early Arthroscopic Management of Heterotopic Ossification of the Elbow Felix H. Savoie III, MD; Michael J. O Brien, MD; and Matthew Wert Introduction The formation of heterotopic ossification (HO) about
Initial experience with endoscopic carpal tunnel release surgery
 Initial experience with endoscopic carpal tunnel release surgery Craig H. Rabb, M.D., and Todd Kuether, M.D. Division of Neurosurgery, Oregon Health Sciences University, Portland, Oregon; and Portland
Initial experience with endoscopic carpal tunnel release surgery Craig H. Rabb, M.D., and Todd Kuether, M.D. Division of Neurosurgery, Oregon Health Sciences University, Portland, Oregon; and Portland
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb
 Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report
 CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
Difference Between Angle You Can Bend Your Left Wrist Back vs Your Right Wrist Jenna Priest Science Department Altoona High School January 25, 2017
 Difference Between Angle You Can Bend Your Left Wrist Back vs Your Right Wrist Jenna Priest Science Department Altoona High School January 25, 2017 Background 1- The wrist joint (also known as the radiocarpal
Difference Between Angle You Can Bend Your Left Wrist Back vs Your Right Wrist Jenna Priest Science Department Altoona High School January 25, 2017 Background 1- The wrist joint (also known as the radiocarpal
A Patient s Guide to Popliteal Cysts
 A Patient s Guide to Popliteal Cysts Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Popliteal Cysts Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Union rate: Union: Stable 94% All fracture 90% Union after surgery for nonunion with surgery 80% OA in healed scaphoid: 9%
 Complications Incidence of Non-union 1 cm displacement of fracture caused 55% Non-union It takes 5-20 yrs to develop SNAC. SNAC appears to be more common with waist fracture than a proximal pole. However
Complications Incidence of Non-union 1 cm displacement of fracture caused 55% Non-union It takes 5-20 yrs to develop SNAC. SNAC appears to be more common with waist fracture than a proximal pole. However
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb
 Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body Reaction
 Department of Orthopedics and Rehabilitation Publications 9-2-2016 New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body
Department of Orthopedics and Rehabilitation Publications 9-2-2016 New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Mark VanDer Kaag 1, Ajmal Ikram 2. Hand Unit, Tygerberg Hospital University of Stellenbosch
 A Prospective, Randomized Controlled Study To Determine The Radiological And Functional Outcomes Of IMN Fixation Of Distal Radius Fractures Using A Novel Device The Sonoma Wrx Distal Radius Nail Compared
A Prospective, Randomized Controlled Study To Determine The Radiological And Functional Outcomes Of IMN Fixation Of Distal Radius Fractures Using A Novel Device The Sonoma Wrx Distal Radius Nail Compared
The role of orthopedic surgery in the Ehlers-Danlos syndromes
 The Ehlers-Danlos Society P.O. Box 87463 Montgomery Village, MD 20886 USA Phone: +1 410-670-7577 The Ehlers-Danlos Society - Europe Office 7 35-37 Ludgate Hill London EC4M 7JN UK Phone: +44 203 887 6132
The Ehlers-Danlos Society P.O. Box 87463 Montgomery Village, MD 20886 USA Phone: +1 410-670-7577 The Ehlers-Danlos Society - Europe Office 7 35-37 Ludgate Hill London EC4M 7JN UK Phone: +44 203 887 6132
INFORMED CONSENT EXTREMITY TUMOR REMOVAL SURGERY
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
Physical therapy of the wrist and hand
 Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
