Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility
|
|
|
- Cecily Young
- 6 years ago
- Views:
Transcription
1 N. R. Howells, J. D. Eldridge From Bristol Royal Infirmary, Bristol, United Kingdom KNEE Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility A CASE CONTROL STUDY Hypermobility is an acknowledged risk factor for patellar instability. In this case control study the influence of hypermobility on clinical outcome following medial patellofemoral ligament (MPFL) reconstruction for patellar instability was studied. A total of 25 patients with hypermobility as determined by the Beighton criteria were assessed and compared with a control group of 50 patients who were matched for age, gender, indication for surgery and degree of trochlear dysplasia. The patients with hypermobility had a Beighton Score of 6; the control patients had a score of < 4. All patients underwent MPFL reconstruction performed using semitendinosus autograft and a standardised arthroscopically controlled technique. The mean age of the patients was 25 years (17 to 49) and the mean follow-up was 15 months (6 to 30). Patients with hypermobility had a significant improvement in function following surgery, with reasonable rates of satisfaction, perceived improvement, willingness to repeat and likelihood of recommendation. Functional improvements were significantly less than in control patients (p < 0.01). Joint hypermobility is not a contraindication to MPFL reconstruction although caution is recommended in managing the expectations of patients with hypermobility before consideration of surgery. N. R. Howells, MRCS, MSc, Specialist Registrar in Trauma and Orthopaedics J. D. Eldridge, FRCS(Orth), Consultant Orthopaedic Surgeon Bristol Royal Infirmary, Upper Maudlin Street, Bristol BS2 8HW, UK. Correspondence should be sent to Mr N. R. Howells; nickrhowells@yahoo.co.uk 2012 British Editorial Society of Bone and Joint Surgery doi: / x.94b $2.00 J Bone Joint Surg Br 2012;94-B: Received 13 March 2012; Accepted after revision 14 August 2012 The incidence of primary patellar dislocation has been quoted as 5.8 per in the general population, and is 29 per in adolescents. 1,2 Rates of recurrence in the literature range from 15% to 44%. 1,2 Following a single recurrent episode there is a 50% chance of further dislocation and many patients continue to have pain and mechanical symptoms. 3 Patients with generalised hypermobility have both an increased incidence of isolated dislocation of the patella and an increased risk of subsequent instability. 4-7 Patellar instability is increasingly being managed surgically with reconstruction of the medial patellofemoral ligament (MPFL). There is limited but growing evidence that these techniques can lead to excellent functional outcome Generalised hypermobility is assessed according to the criteria described by Beighton, Solomon and Soskolne. 12 Its prevalence is between 10% to 20%. 13 Hypermobility can be associated with joint symptoms, 14 and it is thought that surgical outcomes in hypermobile patients may be inferior to those in patients without hypermobility. 13 We are unaware of any published data assessing the outcome of MPFL reconstruction specifically in patients with hypermobility. This study is a prospective analysis of the influence of hypermobility on clinical outcome following MPFL reconstruction for patellar instability. Patients and Methods We performed a 2:1 frequency case-matched control study to investigate the influence of hypermobility on outcome from MPFL reconstruction for patellar instability. Data was collected prospectively on consecutive patients undergoing this procedure between October 2005 and October They were identified from a larger series of patients whose outcome has been previously reported. 11 All procedures were performed by or under the supervision of the senior author (JDE) using the standardised technique described previously. All patients were evaluated clinically and radiologically pre- and post-operatively by two authors (NRH and JDE). A total of 25 consecutive patients who met the Beighton criteria for hypermobility with a score 4 at pre-operative assessment were included in the study. The Beighton criteria for hypermobility are scored out of a maximum of nine points. Points are awarded for thumb hyperextension, wrist hyper-dorsiflexion, VOL. 94-B, No. 12, DECEMBER
2 1656 N. R. HOWELLS, J. D. ELDRIDGE Table I. Case-matching criteria Hypermobile (n = 25) Not hypermobile (n = 50) p-value Mean age (SE; range) (yrs) (1.35; 17 to 49) (1.19; 16 to 49) * Mean follow-up (SE; range) (mths) (1.33; 6 to 30) (1.21; 6 to 42) * Gender (n, %) Male 2 (8) 5 (10) Female 23 (92) 45 (90) Indication for surgery (n, %) Atraumatic dislocation 18 (72) 35 (70) Traumatic dislocation 4 (16) 7 (14) Pain and instability 3 (12) 8 (16) Grade of trochlear dysplasia (n, %) Normal 3 (12) 6 (12) Mild 14 (56) 24 (48) Moderate 8 (32) 20 (40) * t-test chi-squared test Table II. Comparison of subjective question responses between hypermobile and control patients Subjective question response of YES (n, %) Hypermobile (n = 25) Not hypermobile (n = 50) p-value (t-test) Are you satisfied with the outcome of the operation? 19 (76) 47 (94) Did the operation improve or abolish your symptoms? 19 (76) 47 (94) Would you have the same procedure again? 22 (88) 48 (96) Would you recommend this procedure to others? 21 (84) 48 (96) Have you had a recurrence of your symptoms? 8 (32) 4 (8) Have you resumed sport/activity? 9 (36) 41 (82) < Do you have any residual symptoms? 18 (72) 16 (32) elbow hyperextension and knee hyperextension on each side and achievement of hands flat on the floor with legs straight. 12 Of these 25 patients, all had a Beighton Score of 6. Eight of the 25 had a diagnosis of joint hypermobility syndrome with associated multifocal arthralgia. 13,14 These patients were matched with 50 patients who had a score of < 4 pre-operatively. Patients were matched for age, gender, indication for surgery and degree of trochlear dysplasia as described below on MRI scan (Table I). No patient was lost to follow-up. The mean age was 25.4 years (17 to 49) and 26.1 years (16 to 49) in the hypermobile and control groups, respectively. In the hypermobile group 23 patients (92%) were women and in the control group 45 (90%) were women. The mean follow-up was 16 months (6 to 42). Indications for surgery were recurrent patellar dislocation following an atraumatic or a traumatic initial dislocation, or patellar instability with pain. The most frequent indication was atraumatic recurrent dislocation, comprising 18 (72%) of the hypermobile patients and 35 (70%) of the control patients (Table I). Trochlear dysplasia was graded from MRI scans by an author (NRH) as: 1) normal; 2) mild (a shallow trochlear groove); 3) moderate (a flat surface); or 4) severe (a domed trochlea). We have previously described use of this straightforward classification. 11 It is the authors opinion that in clinical practice this is a more useful and reproducible system than the classification system of Dejour et al. 15 Severe trochlear dysplasia was an exclusion criteria for this study as the senior author (JDE) considers trochleoplasty to be more appropriate in these patients. 16 The most frequent grade of dysplasia was mild, comprising 14 (56%) of the hypermobile patients and 24 (48%) of the controls (Table I). Our surgical technique, as previously described, uses a semitendinosus autograft passed extra-synovially and attached through tunnels at the isometric points of the patella and femur with an Endobutton and interference screw respectively. 11 Patellar tracking is assessed arthroscopically through a superolateral portal before fixation of the graft to ensure correct tension and avoid medial overload. The presence of any associated chondral defects was recorded. Patients were allowed to bear full weight as tolerated postoperatively and underwent a standardised rehabilitation programme. They were reviewed post-operatively at two weeks, six weeks, three months, one year and annually thereafter. Outcome was assessed at a minimum of six months postoperatively using the International Knee Documentation Committee (IKDC) score, 17 Kujala score, 18 Oxford knee score (OKS), 19 Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), 20 the Fulkerson modification 21 of the Lysholm and Tegner activity scores 22 THE JOURNAL OF BONE AND JOINT SURGERY
3 MEDIAL PATELLOFEMORAL LIGAMENT RECONSTRUCTION FOR PATELLAR INSTABILITY IN PATIENTS WITH HYPERMOBILITY 1657 Table III. Comparison of outcome scores between patients with and without hypermobility Outcome score * Hypermobile (n = 25) Not hypermobile (n = 50) p-value Mean IKDC score (range) Pre-operative (26 to 62) (26 to 64) Post-operative (20 to 93) (18 to 100) < p-value Mean Kujala score (range) Pre-operative (37 to 61) (29 to 85) Post-operative (31 to 94) (34 to 100) < p-value < Mean OKS (range) Pre-operative (15 to 30) (17 to 35) Post-operative (11 to 47) (18 to 48) < p-value Mean WOMAC (range) Pre-operative (48 to 96) (48 to 92) Post-operative (6 to 100) (25 to 100) < p-value Mean Fulkerson Pre-operative (29 to 63) (27 to 82) Post-operative (17 to 95) (22 to 100) < p-value Mean Tegner level (range) Pre-operative 3.80 (3 to 5) 4.60 (1 to 9) Post-operative 4.13 (0 to 8) 5.44 (1 to 10) p-value Mean SF-12PCS (range) Pre-operative (23 to 45) (32 to 53) Post-operative (17 to 62) (21 to 66) p-value Mean SF-12MCS (range) Pre-operative (24 to 65) (29 to 63) Post-operative (52 to 65) (23 to 63) p-value * IKDC, International Knee Documentation Committee; OKS, Oxford knee score; WOMAC, Western Ontario and McMaster Universities osteoarthritis index; SF-12PCS/MCS, Short-Form 12 Physical/Mental Component Score comparison between the post-operative scores of each group (t-test) comparison between the pre- and post-operative score (t-test) and the Short-Form (SF) In addition patients were asked subjective evaluation questions requiring yes or no responses (Table II). Statistical analysis. This was performed using SPSS v16.0 (SPSS Inc., Chicago, Illinois). Kolmogorov-Smirnoff tests were performed to confirm the normality of data. Independent sample t-tests and one-way analysis of variance (ANOVA) were used where appropriate for data analysis. A p-value < 0.05 was considered statistically significant. Results There were no significant differences in the pre-operative scores between hypermobile patients and controls but a trend towards worse function in the hypermobile group (Table III). The hypermobile patients had significantly worse post-operative scores for all scoring systems (all p < 0.010) with the exception of the Mental Component Score of the SF-12, in which the hypermobile patients had a significantly better mean score than the control patients (58.88 (52 to 65) versus (23 to 63); p = 0.011) (Table III). For the hypermobile group, significant improvements were seen post-operatively for the Kujala score (p = 0.018), the OKS (p = 0.009), Fulkerson (p = 0.033) and SF-12MCS scores (p = 0.005), with improvements in the other scores that did not reach statistical significance (all p > 0.107). Significant improvements were seen between all of the pre-and post-operative outcome scores in the control group, except the Tegner activity level (p = 0.598) (Table III). There was no significant difference between the two groups for the subjective questions, with the exception of an VOL. 94-B, No. 12, DECEMBER 2012
4 1658 N. R. HOWELLS, J. D. ELDRIDGE increased rate of residual and recurrent symptoms (p = and p = 0.027, respectively) and lower rates of resuming sport in the hypermobile group (p < 0.001) (Table II). Despite not reaching statistical significance, the rates of satisfaction with outcome and effective improvement of symptoms were noticeably lower in the hypermobile group than the controls (both 76% versus 94%, both p = 0.066) There have been no recurrent patellar dislocations or subluxations. None of the hypermobile patients have required further surgery to date. One patient in the hypermobile group suffered a patellar fracture in a fall; this was treated conservatively and united without incident. In the hypermobile group there was a trend to worse outcomes in the eight patients diagnosed with joint hypermobility syndrome in comparison with the other hypermobile patients. This reached significance for the SF12-MCS (p = 0.045). The prevalence of lesions affecting the articular cartilage of the patellofemoral joint identified intra-operatively was comparable between hypermobile patients and controls (p = 0.516, t-test). In all 21 hypermobile patients (84%) and 40 control patients (80%) had no identifiable cartilage damage; three hypermobile and six control patients had associated osteochondral defects, and one hypermobile patient and three controls had grade II/III osteo-arthritic changes and one control patient had grade IV osteo-arthritic changes as assessed by the Outerbridge classification. 24 Discussion The MPFL is the primary static stabilising structure for the patella towards full extension. 25 It is inevitably damaged at the time of patellar dislocation and often heals poorly. 26,27 In vitro studies have confirmed the ability of MPFL reconstruction to prevent lateralisation of the patella. 28 Many reconstructive techniques have been described There is, however, no consensus on the most appropriate technique. Hypermobility has been implicated in a wide variety of musculoskeletal conditions including anterior cruciate ligament (ACL) injury, ankle ligament injury and instability of the shoulder as well as patellar instability. 29 Patients with hypermobility often have chronic generalised musculoskeletal symptoms due to joint laxity and multifocal arthralgia. 29 Hypermobile patients have been shown to have poor knee proprioception in comparison with matched controls. 30 They have also been shown to require longer to recover following injury. 31 This study adds to the existing literature on MPFL reconstruction by exploring the effect of hypermobility on outcome following surgery. Case matching provided appropriate controls for comparison. The distribution of age and gender between the groups was comparable. There was a marked difference in proportion of males and females identified with hypermobility and the control group was matched to reflect that. This is in keeping with previous studies assessing the epidemiology of hypermobility. 32 The indications for surgery between cases and controls were also comparable, with a slightly increased number of patients treated for pain and instability in the control group. We have previously shown that patients with this indication have a tendency towards slightly worse outcomes in comparison with other indications 11 and therefore this will not have increased the differences found. The degree of dysplasia was also comparable between the groups, again with the controls having a slightly increased proportion of patients with moderate dysplasia in whom it can be harder to achieve an excellent outcome. Patients with hypermobility who undergo MPFL reconstruction achieved significantly worse functional outcomes than controls. However, function was improved in hypermobile patients, albeit to a lesser extent than in controls. In addition their rates of satisfaction and levels of perceived improvement were not as poor as might have been expected given the difference in outcome scores and were not significantly different from those in controls, although there was a trend to reduced satisfaction. These findings appear to be independent of the degree of hypermobility and of associated chondral damage. The pre-operative level of function in the hypermobile patients in comparison with the controls is an important consideration as there was a trend to poorer function in hypermobile patients although this did not reach statistical significance. This suggests that the differences seen in function post-operatively between hypermobile patients and controls were in fact not all present pre-operatively and that proportionately the hypermobile patients improved, but by less than the controls. It is an interesting finding of this study that the rates of satisfaction and perceived improvement following surgery were still good in the hypermobile patients although not to the same extent as in controls. A large proportion of hypermobile patients remained satisfied with the outcome despite poorer functional scores. Expectations appear to play an important role, with hypermobile patients with marked patellar instability in some cases simply hoping for, and satisfied with, a stable patella rather than a highly functioning symptom free joint. Joint hypermobility is not a contraindication to MPFL reconstruction although caution is recommended in managing the expectations of patients with hypermobility before consideration of surgery. No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article. References 1. Fithian DC, Paxton EW, Stone ML, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 2004;32: Hawkins RJ, Bell RH, Anisette G. Acute patellar dislocations: the natural history. Am J Sports Med 1986;14: Cofield RH, Bryan RS. Acute dislocation of the patella: results of conservative treatment. J Trauma 1977;17: Rünow A. The dislocating patella: etiology and prognosis in relation to generalized joint laxity and anatomy of the patellar articulation. Acta Orthop Scand Suppl 1983;201: Nomura E, Inoue M, Kobayashi S. Generalized joint laxity and contralateral patellar hypermobility in unilateral recurrent patellar dislocators. Arthroscopy 2006;22: THE JOURNAL OF BONE AND JOINT SURGERY
5 MEDIAL PATELLOFEMORAL LIGAMENT RECONSTRUCTION FOR PATELLAR INSTABILITY IN PATIENTS WITH HYPERMOBILITY Carter C, Sweetnam R. Familial joint laxity and recurrent dislocation of the patella. J Bone Joint Surg [Br] 1958;40-B: Pacey V, Nicholson LL, Adams RD, Munn J, Munns CF. Generalized joint hypermobility and risk of lower limb joint injury during sport: a systematic review with meta-analysis. Am J Sports Med 2010;38: Buckens CF, Saris DB. Reconstruction of the medial patellofemoral ligament for treatment of patellofemoral instability: a systematic review. Am J Sports Med 2010;38: Fisher B, Nyland J, Brand E, Curtin B. Medial patellofemoral ligament reconstruction for recurrent patellar dislocation: a systematic review including rehabilitation and return-to-sports efficacy. Arthroscopy 2010;26: Smith TO, Walker J, Russell N. Outcomes of medial patellofemoral ligament reconstruction for patellar instability: a systematic review. Knee Surg Sports Traumatol Arthrosc 2007;15: Howells NR, Barnett A, Ahearn N, Ansari A, Eldridge JD. Medial patellofemoral ligament reconstruction: prospective outcome assessment of a large single centre series. J Bone Joint Surg [Br] 2012;94-B: Beighton P, Solomon L, Soskolne CL. Articular mobility in an African population. Ann Rheum Dis 1973;32: Ross J, Grahame R. Joint hypermobility syndrome. BMJ 2011;342: Grahame R, Bird HA, Child A. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS). J Rheumatol 2000;27: Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 1994;2: Utting MR, Mulford JS, Eldridge JD. A prospective evaluation of trochleoplasty for the treatment of patellofemoral dislocation and instability. J Bone Joint Surg [Br] 2008;90-B: Irrgang JJ, Anderson AF, Boland AL, et al. Development and validation of the International Knee Documentation Committee subjective knee form. Am J Sports Med 2001;29: Kujala UM, Jaakkola LH, Koskinen SK, et al. Scoring of patellofemoral disorders. Arthroscopy 1993;9: Dawson J, Fitzpatrick R, Murray D, Carr A. Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg [Br] 1998;80-B: Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW. Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 1988;15: Fulkerson JP, Shea KP. Disorders of patellofemoral alignment. J Bone Joint Surg [Am] 1990;72-A: Tegner Y, Lysholm J. Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 1985;198: Ware JE, Kosinski M, Keller SD. A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care 1996;34: Outerbridge RE. The aetiology of chondromalacia patellae. J Bone Joint Surg [Br] 1961;43-B: Amis AA, Fir P, Mountney J, Senavongse W, Thomas NP. Anatomy and biomechanics of the medial patellofemoral ligament. Knee 2003;10: Sallay PI, Poggi J, Speer KP, Garrett WE. Acute dislocation of the patella: a correlative pathoanatomic study. Am J Sports Med 1996;24: Nomura E. Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop 1999;23: Ostermeier S, Stukenborg-Colsman C, Hurschler C, Wirth CJ. In vitro investigation of the effect of medial patellofemoral ligament reconstruction and medial tibial tuberosity transfer on lateral patellar stability. Arthroscopy 2006;22: Moriatis Wolf J, Cameron KL, Owens BD. Impact of joint laxity and hypermobility on the musculoskeletal system. J Am Acad Orthop Surg 2011;19: Hall MG, Ferrell WR, Sturrock RD, Hamblen DL, Baxendale RH. The effect of hypermobility syndrome on knee joint proprioception. Br J Rheumatol 1995;34: Hardin JA, Voight ML, Blackburn TA, Canner GC, Soffer SR. The effects of decelerated rehabilitation following anterior cruciate ligament reconstruction on a hyperelastic female adolescent: a case study. J Orthop Sports Phys Ther 1997;28: Decoster LC, Vailas JC, Lindsay RH, Williams GR. Prevalence and features of joint hypermobility among adolescent athletes. Arch Pediatr Adolesc Med 1997;151: VOL. 94-B, No. 12, DECEMBER 2012
Medial patellofemoral ligament reconstruction
 KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes
 All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction
 ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Disclaimers. Concerns after ACL Tear 3/13/2018. Outcomes after ACLR. Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018
 Outcomes after ACLR Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018 Christopher Kaeding M.D. Judson Wilson Professor of Orthopaedics Executive Director, OSU Sports Medicine Medical Director,
Outcomes after ACLR Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018 Christopher Kaeding M.D. Judson Wilson Professor of Orthopaedics Executive Director, OSU Sports Medicine Medical Director,
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
The influence of preserving Infrapatellar fatpad in ACL reconstruction
 The influence of preserving Infrapatellar fatpad in ACL reconstruction Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1) Department of Orthopaedic Surgery,
The influence of preserving Infrapatellar fatpad in ACL reconstruction Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1) Department of Orthopaedic Surgery,
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
PROSPECTIVE AND COMPAR TMENT (MEDIAL PETELLOFEMOR
 ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft
 384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai
 Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai Case History 9 year old boy presented with a 3 week history of: Swelling of major lower limb joints Progression was additive (right ankle followed
Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai Case History 9 year old boy presented with a 3 week history of: Swelling of major lower limb joints Progression was additive (right ankle followed
The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Pre-operative clinical and radiological
 Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Why anteromedial portal is the best
 Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Adult Reconstruction Hip Education Tracks
 Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Introduction. Helmut Wegmann 1 Christoph Würnschimmel 2 Tanja Kraus 2 Georg Singer 1 Robert Eberl 1 Holger Till 1 Matthias Sperl 2
 DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
The patella connects the quadriceps tendon in the thigh to the patellar tendon below the knee attaching to the tibial tuberosity of the shin bone.
 ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
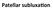 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique
 *smith&nephew Knee Technique Guide MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique Prof. Elvire Servien, MD, PhD Prof. Philippe Neyret, MD Knee Hip Shoulder Extremities
*smith&nephew Knee Technique Guide MPFL reconstruction with autologous gracilis tendon using the two bone tunnel technique Prof. Elvire Servien, MD, PhD Prof. Philippe Neyret, MD Knee Hip Shoulder Extremities
Surgical treatments of patellar instability have been
 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
About the Measure. Pain, Pain (Type and Intensity), Impairment, Arthritis/Osteoarthritis, Exercise Capacity/Six-Minute Walk Test
 About the Measure Domain: Geriatrics Measure: Knee Injury and Osteoarthritis Definition: Purpose: Essential PhenX Measures: Related PhenX Measures: A self-administered questionnaire to assess the patient
About the Measure Domain: Geriatrics Measure: Knee Injury and Osteoarthritis Definition: Purpose: Essential PhenX Measures: Related PhenX Measures: A self-administered questionnaire to assess the patient
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
1st Department of Orthopaedic Surgery, P. & A. Kyriakou Children s Hospital, Athens, Greece 2
 Advances in Orthopedics Volume 2012, Article ID 249687, 4 pages doi:10.1155/2012/249687 Clinical Study Bioabsorbable Pins for Treatment of Osteochondral Fractures of the Knee after Acute Patella Dislocation
Advances in Orthopedics Volume 2012, Article ID 249687, 4 pages doi:10.1155/2012/249687 Clinical Study Bioabsorbable Pins for Treatment of Osteochondral Fractures of the Knee after Acute Patella Dislocation
Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m
 Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m Operation for Chronic Lateral Ankle Instability NO CONFLICT
Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m Operation for Chronic Lateral Ankle Instability NO CONFLICT
Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation
 Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation Andy Phillipson MB ChB FRCS (Orth) Consultant Orthopaedic Surgeon Introduction The ACL is one of the most important ligaments in the knee.
Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation Andy Phillipson MB ChB FRCS (Orth) Consultant Orthopaedic Surgeon Introduction The ACL is one of the most important ligaments in the knee.
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Arthroscopy in sports medicine
 Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
The American Journal of Sports Medicine http://ajs.sagepub.com/ Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men
40 th Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
40 th Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio Knee Injuries In The Pediatric Athlete Disclosure Dr. Travis Murray
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Kohei Kawaguchi, Shuji Taketomi, Hiroshi Inui, Ryota Yamagami, Kenichi Kono, Keiu Nakazato, Kentaro Takagi, Manabu Kawata, Sakae Tanaka
 Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
Remnant Preservation in ACL Reconstruction: Is it Worth Doing?
 Remnant Preservation in ACL Reconstruction: Is it Worth Doing? 1. Presentation (4 x approx. 5min.) i. Mitsuo Ochi ii. Freddie Fu, iii. Takeshi Muneta iv. Rainer Siebold, 2. Debate (approx. 10 min.) 1 ACL
Remnant Preservation in ACL Reconstruction: Is it Worth Doing? 1. Presentation (4 x approx. 5min.) i. Mitsuo Ochi ii. Freddie Fu, iii. Takeshi Muneta iv. Rainer Siebold, 2. Debate (approx. 10 min.) 1 ACL
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN. Guy BELLIER PARIS France
 BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Comparison of effects of Mckenzie exercises and conventional therapy in ACL reconstruction on knee range of motion and functional ability
 2018; 4(4): 415-420 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(4): 415-420 www.allresearchjournal.com Received: 25-02-2018 Accepted: 26-03-2018 Riya Sadana BPTh Student,
2018; 4(4): 415-420 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(4): 415-420 www.allresearchjournal.com Received: 25-02-2018 Accepted: 26-03-2018 Riya Sadana BPTh Student,
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Torn ACL - Anatomic Footprint ACL Reconstruction
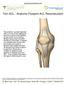 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Five year results of the first ten ACL patients treated with dynamic intraligamentary stabilisation
 Eggli et al. BMC Musculoskeletal Disorders (2016) 17:105 DOI 10.1186/s12891-016-0961-7 RESEARCH ARTICLE Open Access Five year results of the first ten ACL patients treated with dynamic intraligamentary
Eggli et al. BMC Musculoskeletal Disorders (2016) 17:105 DOI 10.1186/s12891-016-0961-7 RESEARCH ARTICLE Open Access Five year results of the first ten ACL patients treated with dynamic intraligamentary
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions
 Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Incidence of graft rupture 15 years after bilateral anterior cruciate ligament reconstructions
 M. Goddard, L. Salmon, A. Waller, E. Papapetros, L. A. Pinczewski From North Sydney Orthopaedic and Sports Medicine Centre, Sydney, Australia M. Goddard, FRCS(Tr & Orth), Orthopaedic Surgeon L. Salmon,
M. Goddard, L. Salmon, A. Waller, E. Papapetros, L. A. Pinczewski From North Sydney Orthopaedic and Sports Medicine Centre, Sydney, Australia M. Goddard, FRCS(Tr & Orth), Orthopaedic Surgeon L. Salmon,
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
PATELLA REALIGNMENT SURGERY
 PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO PATELLA REALIGNMENT SURGERY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office Paillard 2011 YOU HAVE A PATELLA DYSFUNCTION YOU
PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO PATELLA REALIGNMENT SURGERY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office Paillard 2011 YOU HAVE A PATELLA DYSFUNCTION YOU
42 nd Annual Symposium on Sports Medicine. Knee Injuries In The Pediatric Athlete. Disclosure
 42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
42 nd Annual Symposium on Sports Medicine Travis Murray, MD Assistant Professor University of Texas Health Science Center San Antonio January 23, 2015 Knee Injuries In The Pediatric Athlete Disclosure
Save the meniscus Mais pourquoi?
 Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Options in the Young ACL Deficient Knee
 BOSTON SHOULDER AND SPORTS SYMPOSIUM 2013 Thomas M. DeBerardino, MD Disclosure Information Disclosure Information: The following relationships exist: Research Support from: 1. Musculoskeletal Transplant
BOSTON SHOULDER AND SPORTS SYMPOSIUM 2013 Thomas M. DeBerardino, MD Disclosure Information Disclosure Information: The following relationships exist: Research Support from: 1. Musculoskeletal Transplant
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Key words: arthroscopy, orthopaedic examination, magnetic resonance imaging, knee injury.
 Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
ACL INJURIES WHEN TO OPERATE
 ACL INJURIES WHEN TO OPERATE Ziali Sivardeen BMedSci, (MRCS), AFRCS, FRCS (Tr & Orth) Consultant Trauma and Orthopaedic Surgeon (Shoulder, Knee and Sports Injuries) ziali@theolympiaclinic.com www.theolympiaclinic.com
ACL INJURIES WHEN TO OPERATE Ziali Sivardeen BMedSci, (MRCS), AFRCS, FRCS (Tr & Orth) Consultant Trauma and Orthopaedic Surgeon (Shoulder, Knee and Sports Injuries) ziali@theolympiaclinic.com www.theolympiaclinic.com
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction
 Abstract # 18074 Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction Prakash Ayyadurai, Suresh Perumal, Parthiban Jeganathan, Karthik Parachur, Arumugam Sivaraman Sri
Abstract # 18074 Primary Tunnel Dilatation in Tibia, An Unrecognised Complication of ACL Reconstruction Prakash Ayyadurai, Suresh Perumal, Parthiban Jeganathan, Karthik Parachur, Arumugam Sivaraman Sri
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
many patients seen on secondary referral as normal results in the presence of what had been considered
 Archives of Disease in Childhood, 1983, 58, 988-992 Articular hypermobility simulating chronic rheumatic disease R M LEWKONIA AND B M ANSELL Division of Rheumatology, Medical Research Council Clinical
Archives of Disease in Childhood, 1983, 58, 988-992 Articular hypermobility simulating chronic rheumatic disease R M LEWKONIA AND B M ANSELL Division of Rheumatology, Medical Research Council Clinical
TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear Search Terms
 Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
