Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
|
|
|
- Angelina Tyler
- 6 years ago
- Views:
Transcription
1 Case Report pissn X eissn Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun Kim, Hyung Mook Lim, Min Joon Oh, Jae Doo Yoo Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea To remind physicians of the importance of thorough preoperative planning, we reviewed 3 cases of recurrent lateral patellar dislocation despite proximal realignment. The purpose of this study was to evaluate the reasons for the recalcitrant dislocations and to report the outcomes of the revision surgery. This study describes retrospectively a series of 9 cases consisting of patients who underwent revision surgery for recurrent patellar dislocations in spite of a previous treatment of proximal realignment. The following 5 pairs of revision-initial surgery were performed among our 9 patients to treat the recurrent patellar dislocations: (1) trochleoplasty after medial patellofemoral ligament repair in 1 patient; (2) tibial tuberosity transfer after medial patellofemoral ligament reconstruction in 2; (3) tibial tuberosity transfer and medial patellofemoral ligament reconstruction after medial patellofemoral ligament repair in 3; (4) medial patellofemoral ligament reconstruction after lateral release and medial imbrications in 2; and (5) tibial tuberosity transfer, medial patellofemoral ligament reconstruction, and distal femoral varization osteotomy after arthroscopic lateral retinacular release and medial imbrications in 1. Making detailed preoperative evaluations is very important when planning surgeries of recurrent patella dislocations. In light of our experience, the most common cause of recurrent patellar dislocations was inadequate preoperative planning, which leads especially to underestimation of the tibial tuberosity-trochlear groove distance. Keywords: Recurrent lateral patellar dislocation; Proximal realignment surgery INTRODUCTION A recurrent lateral patellar dislocation is one of the most common knee disorders in children and in adolescents [1,2]. It predominantly affects young adults, particularly women in their second or third decade of life [3]. Patellar instability is the resulting phenomenon of recurrent lateral patellar dislocation and several etiologies of the instability have been suggested, such as trochlear dysplasia, medial patellofemoral ligament insufficiency, increased Q-angle, patella alta, increased tibial tuberosity-trochlear groove (TT-TG) distance, vastus medialis obliquus muscle weakness, and valgus malalignment [4]. The management of recurrent patellar instability is difficult for many reasons, for example, on account of the heterogeneity of the demographic characteristics of patients, a multifactorial etiology of the condition, a lack of a gold standard surgical technique, and a lack of long-term clinical outcome studies related this condition [5]. The recent trend has seen a decrease in the use of long-term conservative management and an increase in early surgical management for patellar instability, especially for patients whose initial conservative management had failed. Although, many surgical procedures have been described to treat it, the optimal procedure remains to be determined and, currently, the general preference varies from one country to another. Further, various criteria have also been proposed to guide the choice of surgical procedure; elements of the criteria include patellar height, trochlear dysplasia, lateralization of the tibial tuberosity, patellar mobility, and patellar tracking [6]. Because the etiology of recurrent lateral patellar insta- Arthroscopy and Orthopedic Sports Medicine AOSM Received November 30, 2016; Revised December 20, 2016; Accepted December 21, 2016 Correspondence to: Jae Doo Yoo, Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, 1071 Anyangcheon-ro, Yangcheon-gu, Seoul 07985, Korea. Tel: , Fax: , koreanknee@gmail.com Copyright 2017 Korean Arthroscopy Society and Korean Orthopedic Society for Sports Medicine. All rights reserved. CC This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( by-nc/4.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 28 Arthrosc Orthop Sports Med 2017;4(1):28-33
2 bility is heterogeneous, it is all the more important to understand their exact cause when preoperatively planning. The rate of recurrent dislocation after nonoperative treatment for patellar instability has been shown to be up to 80% and after surgical treatment, up to 40%. Despite such unpromising treatment outcomes, the number of studies that have investigated the cause of the failed treatment or the outcomes of revision surgeries of these recalcitrant knees is meager. To this end, this study describes three cases of revision surgery for recurrent lateral patellar dislocation despite proximal realignment, investigates putative reasons for the recurrent dislocations, and evaluates the outcomes of the revision surgery. CASE REPORTS This study was performed in two stages. The first part of the study involved an analysis of the sample of patients who had undergone only proximal realignment before presenting with a recurrent patellar dislocation. We identified a total of 51 knees (50 patients; gender ratio, 36 women to 14 men) with recurrent patellar instability after proximal realignment that had been performed by a single surgeon (J.D.Y.) between March 2002 and March 2014 at Ewha Womans University Mokdong Hospital (Seoul, Korea). Arthroscopic lateral retinacular release and medial imbrication had been performed on 20 knees, and medial patellofemoral ligament reconstruction had been performed on 31 knees, of which 22 had undergone simultaneous lateral retinacular release. The second part of the study involved an assessment of patients who after proximal realignment had recurrent patellar dislocation and received revision surgery for it. A total of 9 patients were evaluated, amongst them, two were returning patients whilst the others were new to our hospital. Again, the revision surgeries had been performed by a single surgeon (J.D.Y.). The study was performed in accordance to the Declaration of Helsinki. Informed consent was obtained from each participant before the investigation began, and no monetary compensation was provided. We identified a total of nine patients who underwent revision surgery. Amongst the 51 knees that had received surgery for the initial patellar dislocation, we found that only 2 knees, of the 20 that received a treatment of lateral retinacular release and medial imbrication, had required a revision surgery, which was medial patellofemoral ligament reconstruction. At the last follow-up (average, 16 months), we found that symptoms of instability were no longer seen. In contrast, none of the 31 knees that received a treatment of medial patellofemoral ligament reconstruction showed recurrence of instability at least until the last follow-up (average, 18.5 months). Amongst those that had received only proximal realignment for patellar dislocation, the following 5 pairs of revision-initial surgery were found: trochleoplasty after medial patellofemoral ligament reconstruction in 1 patient; tibial tuberosity transfer after medial patellofemoral ligament reconstruction in 2; tibial tuberosity transfer and medial patellofemoral ligament reconstruction after medial patellofemoral ligament repair in 3; and tibial tuberosity transfer, medial patellofemoral ligament reconstruction, and distal femoral varization osteotomy after arthroscopic lateral retinacular release in 1. A detailed summary of the patient demographic data is presented in Table 1. At the 1-year follow-up, we found that none of the patients needed a reoperation or developed complications. Table 1. Detailed demographic data of patients Gender Age (yr) TT-TG I/S ratio Trochlea dysplasia First operative Second operative F B MPFL repair + LR Trochleoplasty + LR F B LR + medial imbrication DFO + MPFLR + TTT M B MPFL repair MPFLR + TTT M No MPFL repair MPFLR + TTT F No MPFL repair MPFLR + TTT F No MPFL reconstruction TTT M No MPFL reconstruction TTT M No LR + medial imbrication MPFLR F No LR + medial imbrication MPFLR F, female; M, male; TT-TG, tibial tuberosity-trochlear groove; I/S, Insall-Salvati ratio; MPFL, medial patellofemoral ligament; LR, lateral retinacular release; DFO, distal femur osteotomy; MPFLR, medial patellofemoral ligament reconstruction; TTT, tibial tubercle transfer. 29
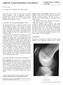
3 TT-TG :20.1 mm A B C D Fig. 1. (A) Preoperative scanogram of the whole lower extremity of Case 1 shows valgus alignment.(b) A preoperative tibial tuberosity-trochlear groove (TT-TG) distance of 20.1 mm was observed in Case 1. (C) Postoperative scanogram of the whole lower extremity (left) and intraoperative images of the medial patellofemoral ligament reconstruction (right) in Case 1. (D) Intraoperative images of the tibial tuberosity transfer in Case 1 are shown. 30
4 Case 1 A 16-year-old female patient was admitted to our clinic with symptoms of persistent instability. She had undergone lateral retinacular release and medial imbrication at another hospital 4 years ago, but despite treatment, she suffered from subluxation and recurrent instability after 1 year of surgery. Bone surgery was delayed on account of the open growth plate. As preoperative planning, we carried out simple radiography, which included taking a standing whole lower extremity scanogram and radiographs of the knee (true anteroposterior view; lateral view in 30 flexion; and the merchant view), and computed tomography. We found that the patient had a varus hipknee-ankle angle of 6 (Fig. 1A), a TT-TG distance of 20.1 mm (Fig. 1B), and a patella tilt of 52. As revision surgery, we performed distal femoral varization osteotomy, medial patellofemoral ligament reconstruction (Fig. 1C), tibial tuberosity medialization osteotomy, and lateral retinacular release (Fig. 1D). At the 1-year follow-up, we found that the hip-knee-ankle angle improved to a varus 2 and that the patella tilt improved to 15. Also, all instability-related symptoms were absent. Case 2 A 28-year-old male patient was admitted to our clinic for anterior knee pain during flexion, instability of the knee during gait, and difficulty in walking up the stairs. He had undergone arthroscopic lateral retinacular release and medial patellofemoral ligament advancement 10 years ago at a different hospital. However, the symptoms did not resolve. The same protocol for preoperative planning was used for Case 2 as in Case 1. We found that the patient had Type B trochlear dysplasia with patellofemoral arthritis (Fig. 2A), a varus hip-knee-ankle angle of 2, a TT- TG distance of 20.0 mm (Fig. 2B), and a patella tilt of 17. As revision surgery, we performed tibial tuberosity medialization osteotomy and lateral retinacular release (Fig. 2C) after which, although the J sign persisted, the symptoms of instability improved moderately. To address the residual symptoms, we performed a secondary medial patellofemoral ligament reconstruction 18 months after the initial surgery. The symptoms of instability and the J sign resolved after the secondary surgery and remained so until the 1-year follow-up. Case 3 An 18-year-old female patient was admitted to our clinic with recurrent patellar subluxation. She had undergone arthroscopic lateral retinacular release and medial patellofemoral ligament repair 7 years ago at another hospital. But subluxation and instability persisted even after surgery. The uniform protocol for preoperative planning was used as in Cases 1 and 2. We found that the patient had Type B trochlear dysplasia (Fig. 3A) with concomitant patella alta. Further, a valgus hip-knee-ankle angle of 3.5, a TT-TG distance of 22.1 mm (Fig. 3B), and a patella tilt of 25 were observed. The symptoms of instability resolved after we performed revision trochleoplasty and lateral retinacular release (Fig. 3C). At the 1-year follow-up, we found that the patella was well-positioned at the trochlea on the Merchant view (Fig. 3D). TT-TG :20.0 mm A B C Fig. 2. (A) Case 2 presented with Type B trochlear dysplasia with patellofemoral arthritis. (B) A preoperative tibial tuberosity-trochlear groove (TT-TG) distance of 20.0 mm was observed in Case 2. (C) An anteroposterior radiograph of the knee was taken after tibial tuberosity medicalization osteotomy and lateral release in Case
5 TT-TG :22.1 mm A B C D Fig. 3. (A) Case 3 presented with Type B trochlear dysplasia. (B) A preoperative tibial tuberosity-trochlear groove (TT- TG) distance of 22.1 mm was observed in Case 3. (C) Intraoperative images of trochleoplasty in Case 3 are shown. (D) Merchant view of Case 3 was taken at the 1-year postoperative follow-up. DISCUSSION A recurrent patellar dislocation is a common injury sustained by young, active patients, with nearly 70% of dislocations occurring during sports activities [7]. The risk of postoperative redislocation has been reported to be between 0% and 71% in young athletes. Until recently, the main surgical option for recurrent patellar dislocation was either lateral retinacular release and medial imbrication or medial patellofemoral ligament repair. But the poor clinical outcomes associated with these options have meant that new options must be sought. In our study, amongst the 20 knees that underwent lateral retinacular release and medial imbrication, 2 presented with recurrent instability upon trauma. No recurrent of instability was seen after medial patellofemoral ligament reconstruction. Of the 9 patients who received revision surgery, 6 patients had a TT-TG distance of 20 mm or greater. Indications for proximal realignment surgery alone for patellar dislocations are a normal Q angle, a normal patella height, and non-severe trochlear dysplasia. On the other hand, contraindications for proximal realignment-only are gross patellar instability, increased TT-TG distance of greater than 20 mm, severe trochlear dysplasia, lateral patella arthritis, and patella alta [2]. Lateral retinacular release is often performed concomitantly to proximal realignment. However, these procedures may sometimes increase the risk of postoperative instability, particularly medial patellar subluxation [8], and a postoperative complication of medial subluxation of the patella after lateral release may paradoxically worsen symptoms [9]. Thus, an inappropriate surgical indication especially that of lateral release may cause poorer outcomes [10]. When we evaluated the patients who had recurrent lateral patellar dislocation in spite of a previous proximal realignment, we found that 9 patients required revision surgery. The main reason for revision was patellar instability. All patients, except for 2, could not be indicated for proximal realignment surgery alone. On the basis of our experience, we deduced that the cause of failed proximal realignment was inadequate preoperative planning. The mean TT-TG distance of the 7 patients was 20.9 mm, and trochlear dysplasia was observed preoperatively in 3. Specifically, because Case 3 patient had a TT-TG distance of 22.1 mm and severe Type B trochlear dysplasia, we 32
6 performed sulcus deepening trocheoplasty without tibial tuberosity osteotomy on account of the reducing effect of trochleoplasty on TT-TG distance. In conclusion, it is very important to make a detailed preoperative evaluation when planning surgeries to address recurrent patellar dislocations. In light of our experience, the common causes of recurrent patellar dislocations usually pertains to inadequate preoperative planning, which often leads to an underestimated TT-TG distance. CONFLICT OF INTEREST No potential conflicts of interest relevant to this article are reported. REFERENCES 1. Mitchell J, Magnussen RA, Collins CL, et al. Epidemiology of patellofemoral instability injuries among high school athletes in the United States. Am J Sports Med 2015;43: Schneider DK, Grawe B, Magnussen RA, et al. Outcomes after isolated medial patellofemoral ligament reconstruction for the treatment of recurrent lateral patellar dislocations: a systematic review and meta-analysis. Am J Sports Med 2016;44: Csintalan RP, Latt LD, Fornalski S, Raiszadeh K, Inacio MC, Fithian DC. Medial patellofemoral ligament (MPFL) reconstruction for the treatment of patellofemoral instability. J Knee Surg 2014;27: Testa EA, Camathias C, Amsler F, Henle P, Friederich NF, Hirschmann MT. Surgical treatment of patellofemoral instability using trochleoplasty or MPFL reconstruction: a systematic review. Knee Surg Sports Traumatol Arthrosc 2015 Jul 18 [Epub] Weber AE, Nathani A, Dines JS, et al. An algorithmic approach to the management of recurrent lateral patellar dislocation. J Bone Joint Surg Am 2016;98: Arendt EA, Dejour D. Patella instability: building bridges across the ocean a historic review. Knee Surg Sports Traumatol Arthrosc 2013;21: Fithian DC, Paxton EW, Stone ML, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 2004;32: Christoforakis J, Bull AM, Strachan RK, Shymkiw R, Senavongse W, Amis AA. Effects of lateral retinacular release on the lateral stability of the patella. Knee Surg Sports Traumatol Arthrosc 2006;14: Shannon BD, Keene JS. Results of arthroscopic medial retinacular release for treatment of medial subluxation of the patella. Am J Sports Med 2007;35: Song GY, Hong L, Zhang H, Zhang J, Li Y, Feng H. Iatrogenic medial patellar instability following lateral retinacular release of the knee joint. Knee Surg Sports Traumatol Arthrosc 2016;24:
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
The value of weight-bearing functional CT scans
 The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
The value of weight-bearing functional scans In musculoskeletal medicine, advanced imaging like computed axial tomography () scanning, has become invaluable to the evaluation and management of patients
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Surgical treatments of patellar instability have been
 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
The Role of Medial Patellofemoral Ligament Repair and Imbrication
 A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Back out of Locking Pin with Hinge Fracture after High Tibial Osteotomy
 Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
A Systematic Review of 21 Tibial Tubercle Osteotomy Studies and More Than 1000 Knees: Indications, Clinical Outcomes, Complications, and Reoperations
 A Systematic Review of 21 Tibial Tubercle Osteotomy Studies and More Than 1000 Knees: Indications, Clinical Outcomes, Complications, and Reoperations Am J Orthop. 2017 November;46(6):E396-E407 Authors:
A Systematic Review of 21 Tibial Tubercle Osteotomy Studies and More Than 1000 Knees: Indications, Clinical Outcomes, Complications, and Reoperations Am J Orthop. 2017 November;46(6):E396-E407 Authors:
Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique
 Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique Jin Hwan Ahn, MD, PhD; Jun Hee Kang, MD; Niraj Sharad Kasat, MD; Jae Gyoon
Patellar Instability With and Without Trochlear Dysplasia: New Arthroscopic Medial Soft Tissue Plication With Pullout Technique Jin Hwan Ahn, MD, PhD; Jun Hee Kang, MD; Niraj Sharad Kasat, MD; Jae Gyoon
Please answer the following questions by responding with a score of 0 to 10. Please answer for how your dog is doing NOW.
 Online Supplementary Material to: Distal femoral lateral closing wedge osteotomy as a component of comprehensive treatment of medial patellar luxation and distal femoral varus in dogs Barry E. Brower;
Online Supplementary Material to: Distal femoral lateral closing wedge osteotomy as a component of comprehensive treatment of medial patellar luxation and distal femoral varus in dogs Barry E. Brower;
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Patellar malalignment: a new method on knee MRI
 DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
Grand Rounds from HSS
 winter 2014 Volume 4 Issue 3 Grand Rounds from HSS Management of complex cases Authors Beth E. Shubin Stein, MD Associate Attending Orthopaedic Surgeon Associate Professor of Orthopaedic Surgery Sabrina
winter 2014 Volume 4 Issue 3 Grand Rounds from HSS Management of complex cases Authors Beth E. Shubin Stein, MD Associate Attending Orthopaedic Surgeon Associate Professor of Orthopaedic Surgery Sabrina
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
The Diagnosis and Initial Treatment of Patellofemoral Disorders
 The Diagnosis and Initial Treatment of Patellofemoral Disorders Am J Orthop. 2017 March;46(2):68-75 Authors: Alan C. Merchant, MD, MS John P. Fulkerson, MD Wayne Leadbetter, MD Author Affiliation Disclosures
The Diagnosis and Initial Treatment of Patellofemoral Disorders Am J Orthop. 2017 March;46(2):68-75 Authors: Alan C. Merchant, MD, MS John P. Fulkerson, MD Wayne Leadbetter, MD Author Affiliation Disclosures
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
The patella connects the quadriceps tendon in the thigh to the patellar tendon below the knee attaching to the tibial tuberosity of the shin bone.
 ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Biomedical Research 2017; 28 (22):
 Biomedical Research 2017; 28 (22): 9966-9970 ISSN 0970-938X www.biomedres.info Clinical curative effect and logistic regression analysis of bone anchor assisted knee extensor mechanism reconstruction for
Biomedical Research 2017; 28 (22): 9966-9970 ISSN 0970-938X www.biomedres.info Clinical curative effect and logistic regression analysis of bone anchor assisted knee extensor mechanism reconstruction for
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
CHRONIC PATELLOFEMORAL INSTABILITY
 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
The Operative Management of Patella Malalignment
 The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M11) 327-339 327 The Operative Management of Patella Malalignment Alexios Dimitrios Iliadis *,1, Parag Kumar Jaiswal 1, Wasim Khan 2 and David Johnstone
The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M11) 327-339 327 The Operative Management of Patella Malalignment Alexios Dimitrios Iliadis *,1, Parag Kumar Jaiswal 1, Wasim Khan 2 and David Johnstone
Patella position in the trochlea groove: comparison between supine and standing radiographs
 Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Patellofemoral pain and patellofemoral instability
 A Review Paper A Systematic Review of Tibial Tubercle Osteotomy Studies and More Than 000 Knees: Indications, Clinical Outcomes, Complications, and Reoperations Bryan M. Saltzman, MD, Allison Rao, MD,
A Review Paper A Systematic Review of Tibial Tubercle Osteotomy Studies and More Than 000 Knees: Indications, Clinical Outcomes, Complications, and Reoperations Bryan M. Saltzman, MD, Allison Rao, MD,
Jin Wan Kim, Youn Soo Hwang, Kyu Pill Moon, Kyung Taek Kim, Joon Yeon Song
 Case Report http://dx.doi.org/10.14517/aosm15022 pissn 2289-005X eissn 2289-0068 rthroscopic fixation with a cannulated screw for avulsion fractures of the tibial spine in children: a report of two cases
Case Report http://dx.doi.org/10.14517/aosm15022 pissn 2289-005X eissn 2289-0068 rthroscopic fixation with a cannulated screw for avulsion fractures of the tibial spine in children: a report of two cases
Orthopaedic Surgeon, University Hospital of Heraklion, and Creta Interclinic Hospital, 47 Filipoupoleos str., Heraklion, 71305, Crete, Greece.
 Authors Postprint of: Christoforakis J, Bull AMJ, Strachan R, Shymkiw R, Senavongse W, Amis AA. Effects of lateral retinacular release on the lateral stability of the patella. Knee Surg. Sports Traumatol.
Authors Postprint of: Christoforakis J, Bull AMJ, Strachan R, Shymkiw R, Senavongse W, Amis AA. Effects of lateral retinacular release on the lateral stability of the patella. Knee Surg. Sports Traumatol.
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
THANK YOU 7/29/2016 DISCLOSURES PATELLOFEMORAL INSTABILITY INTO THE MYSTIC. Skeletally Immature Patients. Anthropology. Epidemiology.
 DETROIT REGIONAL SPORTS MEDICINE SYMPOSIUM THANK YOU Richard Hinton, MD, MPH, MEd, PT Medical and Fellowship Director MedStar Sports Medicine Baltimore / Washington richard.hinton@medstar.net, (410) 554
DETROIT REGIONAL SPORTS MEDICINE SYMPOSIUM THANK YOU Richard Hinton, MD, MPH, MEd, PT Medical and Fellowship Director MedStar Sports Medicine Baltimore / Washington richard.hinton@medstar.net, (410) 554
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Anterior Knee Pain in Patients with Cerebral Palsy
 Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality
 International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy
 Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
Patellar Ligament Disease.
 Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Imaging in patellofemoral instability is essential to the accurate
 REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
Patellar instability - An update
 Acta Orthop. Belg., 2017, 83, 367-386 ORIGINAL STUDY Patellar instability - An update Lars Blønd From the Zealand University Hospital, Køge, Department of Orthopedics, Arthroscopic Section, Koege, Denmark
Acta Orthop. Belg., 2017, 83, 367-386 ORIGINAL STUDY Patellar instability - An update Lars Blønd From the Zealand University Hospital, Køge, Department of Orthopedics, Arthroscopic Section, Koege, Denmark
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Anteromedializing Tibial Tubercle Osteotomy for Patellofemoral Instability: Occupational and Functional Outcomes in U.S. Military Service Members
 Original Article Anteromedializing Tibial Tubercle Osteotomy for Patellofemoral Instability: Occupational and Functional Outcomes in U.S. Military Service Members Philip J. Belmont Jr., MD 1 Tuesday F.
Original Article Anteromedializing Tibial Tubercle Osteotomy for Patellofemoral Instability: Occupational and Functional Outcomes in U.S. Military Service Members Philip J. Belmont Jr., MD 1 Tuesday F.
Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty
 Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty Takuya Konno, MD 1, Tomohiro Onodera, MD, PhD 1, Yasuhiko Kasahara, MD, PhD 1, Daisuke Takahashi 1, Norimasa
Correlation between Knee Kinematics and Patello-femoral Contact Pressure in Total Knee Arthroplasty Takuya Konno, MD 1, Tomohiro Onodera, MD, PhD 1, Yasuhiko Kasahara, MD, PhD 1, Daisuke Takahashi 1, Norimasa
The Knee 20 S1 (2013) S3 S15. Contents lists available at SciVerse ScienceDirect. The Knee
 The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
Introduction. Helmut Wegmann 1 Christoph Würnschimmel 2 Tanja Kraus 2 Georg Singer 1 Robert Eberl 1 Holger Till 1 Matthias Sperl 2
 DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Malalignment can affect any of the three
 ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
Knee Surg Relat Res 2011;23(3): pissn eissn Knee Surgery & Related Research
 Original Article Knee Surg Relat Res 2011;23(3):142-148 http://dx.doi.org/10.5792/ksrr.2011.23.3.142 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research A Comparison of Patella Retention versus
Original Article Knee Surg Relat Res 2011;23(3):142-148 http://dx.doi.org/10.5792/ksrr.2011.23.3.142 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research A Comparison of Patella Retention versus
Medial patellofemoral ligament reconstruction
 KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
Patellofemoral instability is a common cause of knee
 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
To diagnose any disease or disorder implies. The Diagnosis and Initial Treatment of Patellofemoral Disorders. A Review Paper
 A Review Paper The Diagnosis and Initial Treatment of Patellofemoral Disorders Alan C. Merchant, MD, MS, John P. Fulkerson, MD, and Wayne Leadbetter, MD Abstract Our purpose is to provide simple guidelines
A Review Paper The Diagnosis and Initial Treatment of Patellofemoral Disorders Alan C. Merchant, MD, MS, John P. Fulkerson, MD, and Wayne Leadbetter, MD Abstract Our purpose is to provide simple guidelines
Axial Scan Orientation and the Tibial Tubercle Trochlear Groove Distance: Error Analysis and Correction
 Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Medial Patellofemoral Ligament Reconstruction
 53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Tibial Tuberosity Osteotomy
 AJSM PreView, published on November 6, 2013 as doi:10.1177/0363546513507423 Tibial Tuberosity Osteotomy Indications, Techniques, and Outcomes Clinical Sports Medicine Update Seth L. Sherman,* MD, Brandon
AJSM PreView, published on November 6, 2013 as doi:10.1177/0363546513507423 Tibial Tuberosity Osteotomy Indications, Techniques, and Outcomes Clinical Sports Medicine Update Seth L. Sherman,* MD, Brandon
Does the patellofemoral joint need articular cartilage? clinical relevance
 Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
Concepts in managing canine medial patellar luxation cases
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Concepts in managing canine medial patellar luxation cases Author : Toby Gemmill, Bill Oxley Categories : Companion animal,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Concepts in managing canine medial patellar luxation cases Author : Toby Gemmill, Bill Oxley Categories : Companion animal,
Simultaneous Bilateral Patellar Tendon Ruptures Associated with Osteogenesis Imperfecta
 432 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2016; 51: 432-436 https://doi.org/10.4055/jkoa.2016.51.5.432 www.jkoa.org Simultaneous Bilateral Patellar Tendon Ruptures Associated
432 pissn : 1226-2102, eissn : 2005-8918 Case Report J Korean Orthop Assoc 2016; 51: 432-436 https://doi.org/10.4055/jkoa.2016.51.5.432 www.jkoa.org Simultaneous Bilateral Patellar Tendon Ruptures Associated
