The American Journal of Sports Medicine
|
|
|
- Lenard Hutchinson
- 6 years ago
- Views:
Transcription
1 The American Journal of Sports Medicine Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men Petri J Sillanpää, Erno Peltola, Ville M. Mattila, Martti Kiuru, Tuomo Visuri and Harri Pihlajamäki Am J Sports Med : 1513 originally published online April 17, 2009 DOI: / The online version of this article can be found at: Published by: On behalf of: American Orthopaedic Society for Sports Medicine Additional services and information for The American Journal of Sports Medicine can be found at: Alerts: Subscriptions: Reprints: Permissions:
2 Femoral Avulsion of the Medial Patellofemoral Ligament After Primary Traumatic Patellar Dislocation Predicts Subsequent Instability in Men A Mean 7-Year Nonoperative Follow-Up Study Petri J Sillanpää,* MD, PhD, Erno Peltola, MD, Ville M. Mattila, MD, PhD, Martti Kiuru, MD, PhD, Tuomo Visuri, MD, PhD, and Harri Pihlajamäki, MD, PhD From the Centre for Military Medicine, Lahti, Finland, the Department of Orthopaedic Surgery, Tampere University Hospital, Tampere, Finland, the Department of Radiology, Helsinki University Hospital, Helsinki, Finland, the Centre for Military Medicine, Department of Radiology, Helsinki, Finland, and the Department of Orthopedic Surgery, Central Military Hospital, Helsinki, Finland Background: The clinical relevance of medial patellofemoral ligament (MPFL) injury location in primary patellar dislocation has not been studied. Hypothesis: Prognosis after primary traumatic patellar dislocation may vary by MPFL injury location. Study Design: Cohort study; Level of evidence, 3. Methods: The initial magnetic resonance imaging (MRI) findings in 53 patients with identical nonoperative management were retrospectively analyzed for medial restraint injuries. The MPFL injury sites were classified as follows: femoral, midsubstance, and patellar. Magnetic resonance imaging was used to assess initial and control articular cartilage lesions in the patellofemoral joint. After a mean follow-up of 7 years, 42 patients were evaluated for redislocations, subjective symptoms, and functional limitations. Results: Based on the initial MRIs, MPFL rupture was classified as femoral in 35 patients, midsubstance in 11, and patellar in 7. At follow-up, 15 patients reported an unstable patella (13 femoral, 1 patellar, 1 midsubstance; P =.01) and 9 reported patellar redislocations (8 femoral, 1 midsubstance; P =.05). The proportion of patients who regained their preinjury activity level was significantly smaller among those with femoral MPFL injury than among those with midsubstance or patellar MPFL injury (P =.05). The median Kujala score was as follows: 90 for femoral, 91 for patellar, and 96 for midsubstance (P =.76). Control MRI showed full-thickness patellofemoral cartilage lesions in 50% of the patients, unrelated to MPFL injury location. Conclusion: An MPFL avulsion at the femoral attachment in primary traumatic patellar dislocations predicts subsequent patellar instability. The authors suggest that MPFL injury location be taken into account when planning treatment of primary traumatic patellar dislocation. Keywords: patella; dislocation; medial patellofemoral ligament; knee; injury In the patellofemoral joint, the medial structures preventing lateral displacement of the patella include the superficial medial retinaculum and the medial patellofemoral ligament *Address correspondence to Petri J Sillanpää, MD, PhD, Kerkkäkatu 5, FIN Tampere, Finland ( petri.sillanpaa@uta.fi). No potential conflict of interest declared. The American Journal of Sports Medicine, Vol. 37, No. 8 DOI: / The Author(s) (MPFL), the patellotibial ligament, and the patellomeniscal ligament. 13 According to biomechanical cadaveric studies, 7,9,16 the MPFL acts as the major ligamentous restraint against lateral patellar dislocation. In 1979, Warren and Marshall 36 delineated the MPFL as an extracapsular structure of layer 2 of the medial aspect of the knee, outside the synovium. Based on the dissection of 154 fresh-frozen cadavers, their description revealed only minor anatomical variations in the medial structures of the knee. In the literature, the MPFL is thus considered a thickening of the medial retinaculum, 1513
3 1514 Sillanpää et al The American Journal of Sports Medicine always present but with considerable variation with respect to the size and thickness. 7,9,16,28 The MPFL extends from the superior medial border of the patella (at approximately the 2- to 4-o clock position on a right knee), and it attaches firmly to bone between to the adductor tubercle and the medial epicondyle. 19,36 Injuries to both the MPFL and the medial retinaculum are commonly discovered in patients with acute lateral patellar dislocation (the medial retinaculum is closely related to ligamentous MPFL midsubstance structure, as described later). 1,5,12,25,31 Although some studies have concluded that between 75% and 100% of MPFL disruptions are located in the femoral attachment, 1,5 others have reported figures up to 50% at the midsubstance 12,25 or patellar region, 12 depending on the classification. The MPFL is estimated to contribute an average of 50% to 80% of the restraining force against lateral patellar displacement. 7,9,16 This finding was supported by Hautamaa et al, 16 who found an increase of 50% in lateral patellar displacement after the MPFL function was eliminated. Repair of the MPFL restored lateral displacement to within-normal values, and further repair of other retinacular structures provided no additional stability in their study. 16 The clinical relevance of MPFL injury after primary patellar dislocation has not been studied. Nomura 25 categorized MPFL injuries into 2 groups: avulsion tear and substantial tear. Medial patellofemoral ligament injuries have been further classified into 3 regions: the MPFL at the level of its patellar insertion, the MPFL (and medial retinaculum) at its midsubstance, and the MPFL at its femoral origin, as assessed from transverse MRIs. 12,33 Although the potential benefits of initial surgical repair of these MPFL injuries in stabilizing the patella have not been established, several MPFL reconstruction techniques have been described. 1,11,20,32 As based on biomechanical studies, the evidence suggests that the MPFL provides the critical soft tissue restraint against lateral patellar translation; as such, we designed a retrospective study of primary traumatic patellar dislocations in young adults. Our hypothesis was that the MPFL injury location may predict different prognosis and that the healing capacity for stabilizing the patella after identical nonoperative treatment may vary according to the MPFL injury location. In addition, we evaluated the possible chondral lesions occurring at the primary event, their relation to the MPFL injury, and the overall outcome after nonoperative treatment. MATERIALS AND METHODS Patients This study focused on cases that can be defined as acute traumatic physical injury resulting in a first-time (primary) patellar dislocation. The main inclusion criterion was acute primary traumatic patellar dislocation confirmed by physical examination by an orthopaedic surgeon and by MRI (within 21 days from injury). We excluded all patients with a history of previous patellar dislocation or subluxation. In addition, the purpose of this study was to investigate longterm nonoperative healing of the injured MPFL; thus, we excluded patients who had had patellofemoral surgery of any kind (ie, any realignment procedure open or arthroscopic, proximal or distal) during the first 6 months after injury. Patients with multiligamentous knee injuries and other previous traumas or major complaints of the knee joint were excluded as well. Also, nontraumatic situations, such as dislocation during normal gait or squatting or dislocation without forceful knee stress, were excluded because patients with spontaneous subluxation or patellar dislocation without immediate knee pain usually have pathologic laxity of the patellofemoral joint and a history of knee complaints since childhood or adolescence. Because of the high occurrence of osteochondral injuries associated with primary traumatic patellar dislocations, we decided to not exclude patients who had undergone diagnostic arthroscopy or initial arthroscopic removal of an osteochondral fragment without any patellofemoral surgery or other restraint interventions. Arthroscopy performed either for diagnosis or for removal of a loose osteochondral fragment was thus not an exclusion criterion. All other surgical procedures were excluded, including open or arthroscopic procedures of an osteochondral fragment requiring fixation. Most of the traumatic dislocations occurred during sports activity or exercise, and the patients were almost immediately admitted to a hospital afterward because of acute knee pain. The management of primary traumatic patellar dislocations in the study hospital was not restricted to operative or nonoperative treatment; those who were surgically treated usually had an osteochondral fracture. In addition to stipulating the above criteria, we expected all participants to complete the initial nonoperative treatment. The rehabilitation protocol of the hospital included a knee joint motion restriction period of 6 weeks with patellar orthosis; that is, the affected knee joint was allowed to progress to 30 of flexion in the first 3 weeks after which, the movement was allowed to reach 60 of flexion. Immediate full weightbearing was allowed, and the study hospital provided a rehabilitation program with musclestrengthening exercises under a physiotherapist s supervision, usually 2 to 4 months after the incident. The patient was expected to have completed a recovery period between 4 and 6 weeks (median, 4.5; range, 4-6), during which a patellar orthosis was worn. To identify candidates for our study, we used our hospital discharge register database and, in doing so, identified 163 patients hospitalized between January 1, 1997, and December 31, 2002, with a dislocated patella and the appropriate diagnosis code, per the 10th revision of the International Classification of Diseases (ie, S83.0 of the ICD-10). We reviewed their medical records from the day of their admission to the hospital until their completion of the first 6 months of control visits at the same hospital. The Institutional Review Board accepting the protocol of this study was the Medical Ethics Committee of the study hospital, and a written consent was obtained from all patients. At the time of injury, our hospital policy stipulated that initial management of traumatic patellar dislocation not be restricted to a specific form of treatment (surgical or nonsurgical), mainly because of the lack of supportive
4 Vol. 37, No. 8, 2009 Femoral Avulsion of the Medial Patellofemoral Ligament 1515 evidence. Those who were treated surgically usually had an osteochondral fracture; otherwise, the decision to operate was based on the discretion of the surgeon. After careful reconsideration of the medical records by 2 of the authors (P.S. and V.M.), 92 acute patellar dislocations were found with initial surgery, and 71 acute patellar dislocations were found without any patellofemoral surgery performed during the first 6 months after the incident. Of the 71 latter patients, 53 met all the inclusion criteria that is, they sustained a first-time patellar dislocation (as confirmed by medical records and MRI) and they completed supervised aftercare (as confirmed by documentation) and were thus enrolled into the follow-up study. All enrolled patients were male recruits with a mean age of 20 years (range, 19-23) at time of injury. For the purpose of this study, we invited all 53 patients who met the inclusion criteria to a follow-up examination, or to fill out a postal questionnaire if a visit was not possible. The clinical assessment at the follow-up was made by the first author. Forty-two of the 53 patients participated in the follow-up: 32 attended the physical examination and control MRI, performed at a minimum of 4 years (mean, 7; range, 4-10) postoperatively, and 10 participated by returning the questionnaire. The number of subsequent redislocations, subjective instability (painful subluxation), and other problems were elicited and recorded. For subjective assessment of symptoms and functional outcomes, we used the patellofemoral scoring scale by Kujala et al, 18 with a maximum possible score of 100 points (ie, no symptoms). A score of 95 points or more was considered excellent; 94 to 85, good; 84 to 65, fair; and 64 or less, poor. A 100-mm visual analog scale (0, no pain; 100, most severe pain) was used to determine the patient s subjective pain in the affected knee. Physical activity levels were assessed on the Tegner scale, 35 with 0 denoting severe disability and 10 indicating a national- or international-level competing athlete. Patients were also asked whether they had regained their preinjury level of activity by follow-up. Magnetic Resonance Imaging During the study period ( ), MRI was routinely performed at our hospital soon after any kind of knee injury, including all cases of traumatic patellar dislocation, with the purpose of ensuring correct diagnosis, excluding other intra-articular traumas, and defining possible injuries to the medial restraints. All patients enrolled into the study had undergone MRI within 21 days after the injury. As shown by our hospital register, 140 of the 163 patients admitted with acute patellar dislocation underwent an initial MRI during the study period, thereby indicating that no significant patient selection bias in MRI occurred. The MPFL injury location was assessed on both coronal and sagittal images and divided into 3 regions, as described by Elias et al 12 : the MPFL at the level of its patellar insertion, the MPFL (and medial retinaculum) at its midsubstance, and the MPFL at its femoral origin. As Elias et al described, the MPFL was visualized as low-signal-intensity fibers arising between the region near to the adductor tubercle and the medial epicondyle of the femur (Figure 1), Figure 1. A transverse T2-weighted fast spin-echo MRI of the knee, obtained immediately inferior to the adductor tubercle. Arrowhead indicates normal medial patellofemoral ligament femoral insertion. running just inferior to the inferior border of the vastus medialis obliquus muscle, and passing forward and inferiorly toward the medial patella. Complete disruption was defined as fibers in the expected region of the MPFL being completely discontinuous (Figures 2-4) or appearing absent with extensive surrounding edema. The MPFL was considered partially disrupted when some fibers were identified but with partial discontinuity, marked irregularity of fiber contour, and/or intraligamentous or extensive periligamentous edema. Regarding the primary disruption location, usually only a single MPFL location with total disruption was seen in each knee; sometimes, additional partial discontinuity was detected. To reassess the initial MPFL injuries, all MRI images were independently reviewed by 2 musculoskeletal radiologists (M.K., E.P.), with 10 and 3 years of experience, respectively, who had not been involved with the treatment and were blinded to the original interpretation of the images and the follow-up results. The radiologists were also blinded to each other s interpretations, and in case of discrepancy, the images were reviewed again to reach a consensus. The radiologists were asked to determine the location of the main ligamentous disruption of the MPFL and to record any other visible partial disruptions. The MRIs were obtained using a 1.0-T MRI scanner (Signa Horizon, GE Medical Systems, Milwaukee, Wisconsin) and a dedicated knee coil. Slice thickness was 3 mm, with a 0.5- or 1.0-mm intersection gap. The routine sequences were as follows: sagittal T2-weighted fat saturated and proton density, coronal T1-weighted and proton density fast, and axial T2-weighted fat saturated and proton density fat saturated. In every patient, a primary MPFL disruption location was identified. None of the cases showed 2 independent locations with total discontinuity of the MPFL fibers.
5 1516 Sillanpää et al The American Journal of Sports Medicine Figure 2. A transverse T2-weighted fast spin-echo MRI of the knee, obtained at the level of the superior pole of the patella demonstrates a complete disruption of the medial patellofemoral ligament patellar insertion (arrow) in a 22-yearold male patient 2 days after a primary traumatic lateral dislocation of the patella. Note the osteochondral fracture (arrowhead) on the medial patella; also note the excess fluid due to hemarthrosis. Figure 4. A transverse T2-weighted fast spin-echo MRI of the knee obtained at the level of the medial patellofemoral ligament femoral insertion in a 21-year-old male patient 2 days after a primary traumatic lateral dislocation of the patella. Arrow indicates complete disruption of the medial patellofemoral ligament at its midsubstance. The arrowhead marks a large bone contusion of the lateral femoral condyle. Figure 3. A transverse T2-weighted fast spin-echo MRI of the knee, obtained at the level of the medial patellofemoral ligament femoral insertion in a 20-year-old male patient 2 days after a primary traumatic lateral dislocation of the patella. Arrows indicate complete avulsion of the medial patellofemoral ligament off its femoral insertion in the knee. In addition, plain radiographs of the patellofemoral joint were obtained in every patient, including posteroanterior, lateral, and patellofemoral axial radiographs. The parameter measured on the axial views included the sulcus angle, as described by Brattstroem, 3 with a measurement greater than 150 representing trochlear dysplasia. Patellar height was measured on the lateral views so that a Blackburne- Peel 2 ratio greater than 1.06 was considered as patella alta. To measure the clinical Q angle, superimposed MRIs at the level of the tibial tubercle and the femoral trochlear groove 37 were obtained to assess tibial tubercle trochlear groove distance, as described by Dejour et al 8 ; values exceeding 20 mm were considered an abnormal Q angle. At final follow-up, 32 of the 42 patients underwent a control MRI for assessment of chondral lesions. The same 2 musculoskeletal radiologists reviewed the images. The chondral lesions were classified according to their depth using the numeric grading system developed by the International Cartilage Repair Society and described by Brittberg and Winalski. 4 Grade 1 lesions were excluded because of the difficulties in differentiating these lesions from normal (grade 0) cartilage on MRI. 4 Because previous studies have shown MRI to be unreliable in detecting superficial lesions (softening), 10,15,17 only grade 2 to grade 4 lesions were documented, to avoid false-positive MRI findings. Grade 2 describes articular cartilage defects extending down to less than 50% of cartilage depth; grade 3, extending deeper than 50% of cartilage depth; and grade 4, defects with full-thickness articular cartilage loss. Statistical Methods The Kruskal-Wallis test was used to test differences in the nonparametric ordinal data; the independent samples t test was used to determine differences in the continuous,
6 Vol. 37, No. 8, 2009 Femoral Avulsion of the Medial Patellofemoral Ligament 1517 TABLE 1 Patient Characteristics and Radiological Findings According to Location of Medial Patellofemoral Ligament Injury in Traumatic Primary Patellar Dislocation a Injury Location Femur Patella Midsubstance Total Number of patients Age at time of injury, years 20.0 (19-22) 20.2 (19-23) 20.3 (20-21) 20.0 (19-23) Age at follow-up, years 26.9 (23-31) 27.1 (25-33) 27.0 (25-31) 27.0 (23-33) Follow-up time, years 6.9 (4-10) 6.9 (6-10) 6.7 (5-10) 6.9 (4-10) Hemarthrosis, % 60 (15-110) 55 (20-90) 60 (15-110) 50 (15-110) Interval to MRI from trauma, days 3 (0-21) 4 (0-21) 5 (1-21) 3 (0-21) Additional medial patellofemoral ligament injury b locations: Partial femoral tear Not possible 1/7 6/11 Partial patellar tear 13/35 Not possible 6/11 Sulcus angle, degrees 142 ( ) 142 ( ) 143 ( ) 142 ( ) Abnormal values given above the measurements /53 (9%) Blackburne-Peel ratio 1.00 ( ) 0.93 ( ) 0.97 ( ) 0.99 ( ) Abnormal values given above the measurements /53 (21%) Tibial tubercle trochlear groove distance, mm 12.7 (5-22) 13.3 (7-19) 16.9 (11-23) 13 (5-23) Abnormal values given above the measurements /53 (8%) a Major injury location divided into 3 regions and assessed by 2 radiologists in consensus. Values presented in means (and ranges), unless stated otherwise. b Location of partial disruptions recorded (besides main medial patellofemoral ligament disruption). normally distributed data specifically, in the tests between the injury locations. Differences in the 2-way tables were determined with the Pearson chi-square test or with the Fisher exact test, when appropriate. Because the chi-square test is not reliable if the expected values are small (as was the case in injury locations other than femoral MPFL), further testing to localize a significant finding was performed using either a subset of the original 6-cell table (femoral, midsubstance, and patellar locations) or the 2 2 table statistics (femoral location compared with any other location) with the Fisher exact test. Significance was set at P.05, and SPSS 14.1 for Windows (SPSS Inc, Chicago, Illinois) was used for the statistical analysis. RESULTS Of the 53 patients, 35 had femoral MPFL avulsions, 11 had midsubstance MPFL disruptions, and 7 had patellar MPFL disruptions (Table 1). Of the 42 patients who participated at follow-up, 25 had MPFL disruptions in the femoral region, 11 in the midsubstance region, and 6 in the patellar region (Table 2; see also, Figures 2-4). Overall patellar instability (including redislocation and painful subluxation) was significantly associated with femoral MPFL avulsion. In the femoral MPFL avulsion group, 13 of the 25 patients reported unstable patellae, compared with 1 of 11 in the midsubstance group and 1 of 6 in the patellar group (P =.01). There were 8 subsequent patellar redislocations in the femoral group (as documented by an emergency visit to a physician), compared with 1 redislocation in the midsubstance group and 0 in the patellar group (P =.05). Given the final follow-up results, the patellae of 6 patients who reported subsequent patellofemoral stabilizing operations owing to patellar redislocation (5 in the femoral group and 1 in midsubstance group) were considered unstable after initial nonoperative management (Table 2). Preinjury activity level was best regained in the midsubstance region group (9 of 11), followed by the patellar region group (4 of 6) and the femoral region group (13 of 25). When the femoral region group was compared with the other groups, a significant correlation was found in not regaining preinjury activity level (P =.05). The median follow-up Tegner activity scores were as follows: 5 for the femoral group (range, 3-8), 6 for the patellar (range, 4-7), and 5 for the midsubstance (range, 2-7; P =.32). The overall subjective outcomes were not related to MPFL injury location. The median Kujala scores for subjective symptoms and functional outcome were as follows: 90 for the femoral region (range, ), 91 for the patellar (range, ), and 96 points for the midsubstance (range, ; P =.76). When we excluded the 5 patients with femoral MPFL injury who later underwent stabilizing surgery, the median Kujala score for the 20 remaining patients in the femoral group was 85 (range, ), compared with 94 (range, ) for the patients with MPFL injury in the midsubstance and patellar regions (P =.59). Based on MRI, an additional MPFL injury location was identified in 45% of the patients (24 of 53) namely, a primary MPFL disruption location and partial MPFL tear in a different location. There were no cases of 2 separate total MPFL disruptions in the same knee. The presence of an additional MPFL injury location was not associated with increased patellar instability (P =.12). Initial osteochondral fractures were seen in 28% of cases (15 of 53), but they
7 1518 Sillanpää et al The American Journal of Sports Medicine TABLE 2 Results of the Functional Follow-up Examinations According to Location of Medial Patellofemoral Ligament Injury a Injury Location Femur Patella Midsubstance P Patients With follow-up Redislocation Overall instability c Kujala score (max 100 points), median (range) Excellent ( points) Good (85-94 points) Fair (65-84 points) Poor (64 or less points) Tegner activity level (1-10) Regain preinjury activity level Visual analog scale (0-100 mm) Subsequent surgery 35 25/35 (71%) 8/25 (32%) 13/25 (52%) 90 (76-100), 85 (76-100) d 8/25 (32%) 10/25 (40%) 6/25 (24%) 1/25 (4%) 5 (3-8) 13/25 (52%) 10 (0-70) 5/25 (20%) 7 6/7 (86%) None 1/6 (17%) 91 (59-100) 2/6 (33%) 4/6 (66%) None None 6 (4-7) 4/6 (67%) 10 (0-50) None 11 11/11 (100%) 1/11 (9%) 1/11 (9%) 96 (68-100) 6/11 (55%) 3/11 (27%) 2/11 (18%) None 5 (2-7) 9/11 (82%) 10 (0-20) 1/11 (9%).05 b.01 b b a Major injury location divided into 3 regions and assessed by 2 radiologists in consensus. Values presented in sample size, n (and either range or proportion, as indicated). b Considered significant (P.05) when femoral medial patellofemoral ligament injury was compared to patella and midsubstance injuries. c Overall instability including subjective symptoms of patellar instability (multiple subluxations). d A subset of patients who did not undergo later stabilizing surgery, the median Kujala score for the remaining patients in the femoral group. did not predict subsequent instability (P =.74). Large fractures requiring fixative surgery were excluded. The occurrence of osteochondral fractures was not related to any MPFL injury location (P =.97). Distributions of the initial chondral lesions showed no statistically significant differences between the MPFL injury locations (Table 3). In radiographic measurements at the time of dislocation, 5 of 53 patients had abnormal trochlear groove, 11 patients had patella alta, and 4 patients had increased tibial tubercle trochlear groove distance. However, as the summarized findings in Table 1 indicate, the majority of values in each MPFL injury group were normal. Between patients with or without recurrent patellar instability, no significant differences in radiographic measurements were found (Table 4). At follow-up, full-thickness articular cartilage lesions, as signs of patellofemoral osteoarthritis development, were frequently found specifically, in 45% of cases at the medial or lateral patellar facets and in 31% of cases at the articular surface of the femoral trochlear groove. This finding was unrelated to the MPFL injury location. Similarly, the presence of osteoarthritis characteristics was not associated with poor results in Kujala scores, and patellar instability was not significantly more frequent in patients with initial osteochondral fracture when compared with patients without osteochondral fracture (Table 3). DISCUSSION The principal finding of the present study was that MPFL avulsion at the femoral attachment in primary traumatic patellar dislocation predicted subsequent patellar instability. A significantly lower proportion of patients with femoral avulsion type MPFL injury regained their previous activity level, as compared with patients with MPFL disruption in the midsubstance or patellar region. However, no differences were found in subjective scores between the injury locations. Although many studies have reported MPFL injury to be closely related to primary patellar dislocation, this study is the first to our knowledge to explore the clinical relevance of the anatomical location of MPFL injury after primary traumatic patellar dislocation. Thirteen of the 15 patients who had subsequent patellar instability after the primary incident suffered MPFL rupture at its femoral attachment, thereby indicating a significant relationship between patellofemoral instability and a femoral avulsion type MPFL injury. As such, we suggest that the anatomical location of MPFL injury be taken into account when planning treatment for primary traumatic patellar dislocation. Previous biomechanical studies suggest that the procedures that are intended to restore the normal passive limits against lateral patellar motion should include the repair or the reestablishment of the integrity and function of the MPFL. 13,16 Given the present study, we conclude that femoral avulsion of the MPFL is strongly associated with subsequent patellar instability, if stabilizing procedures are not performed. Ruptures at the MPFL midsubstance or patellar insertion regions were not related to subsequent instability, nor was the presence of primary disruption and additional partial MPFL tear. We therefore suggest that a rupture of the MPFL at its midsubstance or at its patellar attachment can be successfully treated nonoperatively, with infrequent subsequent symptoms of patellar instability. Furthermore, a nonoperatively treated femoral avulsion of the MPFL may result in some potential lengthening
8 Vol. 37, No. 8, 2009 Femoral Avulsion of the Medial Patellofemoral Ligament 1519 TABLE 3 Distribution of MRI-Detected Articular Cartilage Lesions in the Medial Patellofemoral Ligament Injury Locations a Injury Location Femoral Patella Midsubstance Total Initial chondral lesions / patella b Grades /35 (37%) 3/7 (43%) 7/11 (64%) 23/53 (43%) Grade 4 None None None Initial chondral lesions / femur b Grades 2-3 8/35 (23%) 1/7 (14%) 1/11 (9%) 10/53 (19%) Grade 4 None None None Initial osteochondral fracture c 10/35 (29%) 3/7 (43%) 2/11 (18%) 15/53 (28%) Follow-up chondral lesions / patella b Grades 2-3 4/19 (21%) 2/5 (40%) 3/8 (38%) 9/32 (28%) Grade 4 7/19 (37%) 2/5 (40%) 4/8 (50%) 13/32 (41%) Follow-up chondral lesions / femur b Grades 2-3 2/19 (11%) 1/5 (20%) 1/8 (13%) 4/32 (13%) Grade 4 7/19 (37%) 1/5 (20%) 2/8 (25%) 10/32 (31%) a Major injury location divided into 3 regions and assessed by 2 radiologists in consensus. b MRI-detected chondral lesions in the patellofemoral joint (at medial or lateral facets of the patellar articular surface or the femoral trochlear groove articular surface) including grades 2 to 4 (grade 1, superficial fibrillation only, excluded because of insensitivity of MRI detection). Classification according to depth using the numeric grading system developed by the International Cartilage Repair Society. 4 c Initial osteochondral fracture detected by MRI. TABLE 4 Radiographic Findings in Patients With Stable or Unstable Patellae, Final Follow-Up Stable Patella Unstable Patella Measure Median (Range) Median (Range) P Blackburne-Peel ratio 0.99 ( ) 1.00 ( ).94 TT-TG distance, a mm 13 (8-23) 15 (5-22).12 Sulcus angle, degrees 143 ( ) 142 ( ).34 a Tibial tubercle trochlear groove distance. or loosening of the MPFL ligament (as in collateral ligament injuries of the knee) and in subsequent patellar instability. Therefore, if initial surgery is considered, it should be targeted at repairing the femoral MPFL avulsion, and reconstructive surgery should be aimed at restoring the integrity of the anatomical femoral attachment of the MPFL to ensure better stability. The increased Q angle and other major dysplastic features of the patellofemoral joint should be observed. A recent prospective randomized study by Palmu et al 27 on acute patellar dislocations in children and adolescents failed to prove the superiority of initial medial repair over nonoperative treatment for later patellar instability. However, contrary to our study, nearly all of Palmu s patients exhibited dysplastic features of the patellofemoral joint. In a prospective randomized study, Nikku et al 24 found no difference in outcome scores or instability rates between operative and nonoperative management of the primary dislocations. A recent prospective study comparing initial arthroscopic stabilization and nonoperative treatment for primary traumatic patellar dislocation also revealed unimproved patellar stability; yet, a better regain of preinjury activity level was noted. 33 Another recent pro spective randomized study this one of delayed femoral reinsertion of the MPFL, compared with nonoperative management described no surgery-related benefits. 6 However, the investigators did not assess the MPFL injury location, and they used the same femoral reinsertion method for all their surgical cases. This study has several limitations, the first being its retrospective nature. However, by reviewing the clinical and radiological examinations, we attempted to verify that the traumatic dislocation was primary and that the initial management had been identical in all patients. Second, owing to the lack of female patients, conclusions should be drawn with caution concerning the clinical prognosis of primary traumatic patellar dislocation in women. Also, because osteochondral fractures requiring fixation sometimes occurred near the patellar MPFL attachment and so acted as bony MPFL avulsions, we may have lost some MPFL injuries in the patellar region. These cases were not included in this study because the fixation procedure itself or the possible failure of the procedure might have affected the final results and because the misplaced fragment can produce patellofemoral pain. Exclusion of the large fragments suggests that the occurrence of osteochondral fractures (28%) might be somewhat lower than that among previous studies regarding traumatic primary patellar dislocations. 31,34 The strengths of the study include the homogeneity of the patients that is, all were young healthy male adults, which resulted in good comparability between the individuals. Also, our enrollment was limited to patients with acute primary dislocations who had identical aftercare provided by the same hospital and under the same physiotherapist s guidance. In addition, in our
9 1520 Sillanpää et al The American Journal of Sports Medicine opinion, the findings are quite generalizable to members of the standard young adult male population who sustain primary traumatic patellar dislocations during various physical activities, as compared with reports on athletic study populations selected from single-sport databases. 14,31 Injuries to the MPFL and the medial retinaculum (a definition widely used in the literature before recognition of the MPFL injury) have been frequently reported in association with an acute lateral patellar dislocation. 1,29,31,34 Various authors have studied the anatomical locations of MPFL injuries. Avikainen et al 1 reported that in all 14 patients who underwent surgical exploration for acute patellar dislocation, the MPFL was avulsed from its femoral attachment. Sallay et al 29 reported an avulsion of the MPFL from the adductor tubercle in 94% of the knees in 23 patients with acute primary patellar dislocation. Burks et al 5 reported a simulation of patellar dislocation by comparing MRI findings and gross anatomical findings in 10 cadaveric knees; the MPFL was found injured in 8 knees, most commonly at its femoral origin. Elias et al 12 reported MRI findings of medial retinacular and MPFL injuries in 81 patients with acute lateral patellar dislocation. Although a medial retinacular structure was visualized in all patients, an MPFL injury was visualized in only 87% of the cases (76% at patellar insertion, 30% at midsubstance, 49% at femoral origin, and 55% in more than 1 site). This low incidence might be due to the long interval between dislocation and MRI (8 weeks). The same categorization of MPFL injuries was used in a recent prospective study in which the MPFL injury sites were 57% femoral, 23% midsubstance, and 20% patellar. 33 Nomura 25 reported the surgical findings of 67 knees (18 acute and 49 chronic patellar dislocations): Among the 18 acute dislocations, avulsion or detachment of the ligament from the epicondyle was evident in 7 knees; a midsubstance-type tear was present in 10 knees, with a tear of the MPFL found typically near its femoral attachment; and in 1 patient, the ligament was loose yet without a discrete injury. Sanders et al, 30 comparing surgical results with MRI, reported an MPFL injury in all 14 patients and concluded that MRI is an accurate method for depicting MPFL injuries. The nonoperative treatment method used on our patients aimed to prevent further loss of integrity of the injured MPFL. It is not known whether knee flexion restriction prevents the MPFL lengthening. 7,9,16 In the case of femoral avulsion of the MPFL, however, the ligament may fail to heal altogether because of the loss of integrity of the ligamentous structure. Whether the knee should be immobilized in nearly full extension to prevent further loosening of the MPFL femoral attachment is unknown 21,23 ; at the very least, it demands considerable compliance by the patient to accept immobilization for 3 to 6 weeks (splint or cast). However, in this study, some MPFL ruptures in the femoral region healed to produce reasonable patellar stability, but there was no evidence of any MRI-specific finding that predicted this phenomenon. Although we found that initial patellofemoral articular cartilage injuries were common, they were unrelated to a MPFL injury site. In the present study, initial osteochondral fractures were not associated with recurrent patellar instability, although authors of previous studies have suggested operative management of primary dislocations with osteochondral fracture. 34 Our findings suggest that dislocation with an osteochondral fracture requiring surgical intervention may benefit from MRI assessment, to enable localization of a possible MPFL disruption and to decide on concurrent stabilizing repair or reconstruction surgery. Furthermore, given that previous studies have described good comparability between MRI findings and surgical findings in MPFL injuries, 26,30 no surgical exploration of MPFL injury location might be necessary if initial repair or reconstruction is chosen. In the present study, MRI revealed frequent osteoarthritis characteristics at follow-up, but these were unrelated to the MPFL injury site. The number of patients with patellofemoral osteoarthritis was consistent with earlier research. 22 In conclusion, this study provides strong evidence that MPFL avulsion at the femoral attachment in primary traumatic patellar dislocations predicts patellar instability. The MPFL has been defined as the critical soft tissue restraint against lateral patellar translation. Hence, residual laxity in the femoral region of the MPFL might be responsible for the frequent subsequent patellar instability reported after primary patellar dislocation. Our findings indicate that the outcomes after MPFL rupture vary according to the rupture location; in patients with a disruption at the midsubstance or at the patella, recurrent instability seems significantly less common than in patients with an avulsion of the MPFL in the femoral region. Even when MPFL avulsion at its femoral attachment is accompanied by a partial MPFL tear in the midsubstance or patellar region, no additional risk for instability is predicted. Consequently, the findings may be helpful in planning treatment modalities; that is, initial stabilizing surgery might be considered when femoral MPFL avulsion has occurred in a high-demand patient who requires good patellar stability, whereas initial surgery cannot be recommended for midsubstance or patellar MPFL ruptures. However, because the subjective scores were the same between the study groups, our results deserve further prospective investigations to ascertain the clinical significance of the MPFL injury location, particularly in terms of whether surgical stabilizing interventions are superior to nonoperative healing and reestablishment of the critical restraint function of the MPFL in certain injury patterns. ACKNOWLEDGMENT We thank Marja Vajaranta for language editing. The study did not receive funding. REFERENCES 1. Avikainen VJ, Nikku RK, Seppanen-Lehmonen TK. Adductor magnus tenodesis for patellar dislocation: technique and preliminary results. Clin Orthop Relat Res. 1993;297: Blackburne JS, Peel TE. A new method of measuring patellar height. J Bone Joint Surg Br. 1977;59:
10 Vol. 37, No. 8, 2009 Femoral Avulsion of the Medial Patellofemoral Ligament Brattstroem H. Shape of the intercondylar groove normally and in recurrent dislocation of patella: a clinical and x-ray-anatomical investigation. Acta Orthop Scand. 1964;68(suppl 68): Brittberg M, Winalski CS. Evaluation of cartilage injuries and repair. J Bone Joint Surg Am. 2003;85(suppl 2): Burks RT, Desio SM, Bachus KN, Tyson L, Springer K. Biomechanical evaluation of lateral patellar dislocations. Am J Knee Surg. 1998;11: Christiansen SE, Jakobsen BW, Lund B, Lind M. Isolated repair of the medial patellofemoral ligament in primary dislocation of the patella: a prospective randomized study. Arthroscopy. 2008;24: Conlan T, Garth WP Jr, Lemons JE. Evaluation of the medial soft-tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg Am. 1993;75: Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc. 1994;2: Desio SM, Burks RT, Bachus KN. Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med. 1998;26: Disler DG, McCauley TR, Kelman CG, et al. Fat-suppressed threedimensional spoiled gradient-echo MR imaging of hyaline cartilage defects in the knee: comparison with standard MR imaging and arthroscopy. AJR Am J Roentgenol. 1996;167: Dopirak RM, Steensen RN, Maurus PB. The medial patellofemoral ligament. Orthopedics. 2008;31: Elias DA, White LM, Fithian DC. Acute lateral patellar dislocation at MR imaging: injury patterns of medial patellar soft-tissue restraints and osteochondral injuries of the inferomedial patella. Radiology. 2002;225: Feller JA, Amis AA, Andrish JT, Arendt EA, Erasmus PJ, Powers CM. Surgical biomechanics of the patellofemoral joint. Arthroscopy. 2007;23: Fithian DC, Paxton EW, Stone ML, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med. 2004;32: Gagliardi JA, Chung EM, Chandnani VP, et al. Detection and staging of chondromalacia patellae: relative efficacies of conventional MR imaging, MR arthrography, and CT arthrography. AJR Am J Roentgenol. 1994;163: Hautamaa PV, Fithian DC, Kaufman KR, Daniel DM, Pohlmeyer AM. Medial soft tissue restraints in lateral patellar instability and repair. Clin Orthop Relat Res. 1998;349: Kawahara Y, Uetani M, Nakahara N, et al. Fast spin-echo MR of the articular cartilage in the osteoarthrotic knee: correlation of MR and arthroscopic findings. Acta Radiol. 1998;39: Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O. Scoring of patellofemoral disorders. Arthroscopy. 1993;9: LaPrade RF, Engebretsen AH, Ly TV, Johansen S, Wentorf FA, Engebretsen L. The anatomy of the medial part of the knee. J Bone Joint Surg Am. 2007;89: Lind M, Jakobsen BW, Lund B, Christiansen SE. Reconstruction of the medial patellofemoral ligament for treatment of patellar instability. Acta Orthop. 2008;79: Maenpaa H, Lehto MU. Patellar dislocation: the long-term results of nonoperative management in 100 patients. Am J Sports Med. 1997;25: Maenpaa H, Lehto MU. Patellofemoral osteoarthritis after patellar dislocation. Clin Orthop Relat Res. 1997;339: Mehta VM, Inoue M, Nomura E, Fithian DC. An algorithm guiding the evaluation and treatment of acute primary patellar dislocations. Sports Med Arthrosc. 2007;15: Nikku R, Nietosvaara Y, Aalto K, Kallio PE. Operative treatment of primary patellar dislocation does not improve medium-term outcome: a 7-year follow-up report and risk analysis of 127 randomized patients. Acta Orthop. 2005;76: Nomura E. Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop. 1999;23(5): Nomura E, Horiuchi Y, Inoue M. Correlation of MR imaging findings and open exploration of medial patellofemoral ligament injuries in acute patellar dislocations. Knee. 2002;9: Palmu S, Kallio PE, Donell ST, Helenius I, Nietosvaara Y. Acute patellar dislocation in children and adolescents: a randomized clinical trial. J Bone Joint Surg Am. 2008;90: Reider B, Marshall JL, Koslin B, Ring B, Girgis FG. The anterior aspect of the knee joint. J Bone Joint Surg Am. 1981;63: Sallay PI, Poggi J, Speer KP, Garrett WE. Acute dislocation of the patella: a correlative pathoanatomic study. Am J Sports Med. 1996;24: Sanders TG, Morrison WB, Singleton BA, Miller MD, Cornum KG. Medial patellofemoral ligament injury following acute transient dislocation of the patella: MR findings with surgical correlation in 14 patients. J Comput Assist Tomogr. 2001;25: Sillanpaa P, Mattila VM, Iivonen T, Visuri T, Pihlajamaki H. Incidence and risk factors of acute traumatic primary patellar dislocation. Med Sci Sports Exerc. 2008;40: Sillanpaa P, Mattila VM, Visuri T, Maenpaa H, Pihlajamaki H. Ligament reconstruction versus distal realignment for patellar dislocation. Clin Orthop Relat Res. 2008;466: Sillanpaa PJ, Maenpaa H, Mattila VM, Visuri T, Pihlajamaki H. Arthroscopic surgery for primary traumatic patellar dislocation: a prospective, nonrandomized study comparing patients treated with and without acute arthroscopic stabilization with a median 7-year follow-up. Am J Sports Med. 2008;36: Stefancin JJ, Parker RD. First-time traumatic patellar dislocation: a systematic review. Clin Orthop Relat Res. 2007;455: Tegner Y, Lysholm J. Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res. 1985;198: Warren LF, Marshall JL. The supporting structures and layers on the medial side of the knee: an anatomical analysis. J Bone Joint Surg Am. 1979;61: Wittstein JR, Bartlett EC, Easterbrook J, Byrd JC. Magnetic resonance imaging evaluation of patellofemoral malalignment. Arthroscopy. 2006;22: For reprints and permission queries, please visit SAGE s Web site at
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration
 Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
MRI of Osteochondral Defects of the Lateral Femoral Condyle: Incidence and Pattern of Injury After Transient Lateral Dislocation of the Patella
 Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
Primary traumatic patellar dislocation
 Tsai et al. Journal of Orthopaedic Surgery and Research 2012, 7:21 REVIEW Primary traumatic patellar dislocation Chun-Hao Tsai 1, Chin-Jung Hsu 1, Chih-Hung Hung 1 and Horng-Chaung Hsu 1,2* Open Access
Tsai et al. Journal of Orthopaedic Surgery and Research 2012, 7:21 REVIEW Primary traumatic patellar dislocation Chun-Hao Tsai 1, Chin-Jung Hsu 1, Chih-Hung Hung 1 and Horng-Chaung Hsu 1,2* Open Access
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
The Role of Medial Patellofemoral Ligament Repair and Imbrication
 A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
A Review Paper The Role of Medial Patellofemoral Ligament Repair and Imbrication Kyle R. Duchman, MD, and Matthew J. Bollier, MD Abstract Repair, reefing, and advancement of the medial patellofemoral ligament
PROSPECTIVE AND COMPAR TMENT (MEDIAL PETELLOFEMOR
 ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Department of Orthopaedic Surgery, Tampere University Hospital, Tampere, Finland 3
 Scandinavian Journal of Surgery 101: 56 61, 2012 Sensitivity of MRI for articular cartilage lesions of the patellae V. M. Mattila 1, 2, M. Weckström 1, V. Leppänen 1, M. Kiuru 1, H. Pihlajamäki 1, 3 1
Scandinavian Journal of Surgery 101: 56 61, 2012 Sensitivity of MRI for articular cartilage lesions of the patellae V. M. Mattila 1, 2, M. Weckström 1, V. Leppänen 1, M. Kiuru 1, H. Pihlajamäki 1, 3 1
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Medial collateral ligament (MCL) injury, is one
 )3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
)3( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY EDITORIAL Medial Collateral Ligament Injury; A New Classification Based on MRI and Clinical Findings. A Guide for Patient Selection and Early
Surgical treatments of patellar instability have been
 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
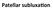 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Medial Patellofemoral Ligament Reconstruction
 53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
53 Medial Patellofemoral Ligament Reconstruction Hany Elrashidy, Joseph Carney, Najeeb Khan, and Donald C. Fithian CHAPTER DEFINITION Stability of the patellofemoral joint (PFJ) is multifactorial as it
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
1st Department of Orthopaedic Surgery, P. & A. Kyriakou Children s Hospital, Athens, Greece 2
 Advances in Orthopedics Volume 2012, Article ID 249687, 4 pages doi:10.1155/2012/249687 Clinical Study Bioabsorbable Pins for Treatment of Osteochondral Fractures of the Knee after Acute Patella Dislocation
Advances in Orthopedics Volume 2012, Article ID 249687, 4 pages doi:10.1155/2012/249687 Clinical Study Bioabsorbable Pins for Treatment of Osteochondral Fractures of the Knee after Acute Patella Dislocation
The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears
 Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears Anterior cruciate ligament (ACL) tears are difficult to diagnose and treat (DeFranco). The preoperative
Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears Anterior cruciate ligament (ACL) tears are difficult to diagnose and treat (DeFranco). The preoperative
SLARD Symposium: MCL s Injuries
 SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
Patellofemoral instability is a common cause of knee
 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon
 J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Acute dislocation of the patella: should these patients be operated on more often?
 Review Article Page 1 of 7 Acute dislocation of the patella: should these patients be operated on more often? Vicente Sanchis-Alfonso 1, Erik Montesinos-Berry 2 1 Department of Orthopaedic Surgery, Hospital
Review Article Page 1 of 7 Acute dislocation of the patella: should these patients be operated on more often? Vicente Sanchis-Alfonso 1, Erik Montesinos-Berry 2 1 Department of Orthopaedic Surgery, Hospital
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Patella Alta: Lack of Correlation Between Patellotrochlear Cartilage Congruence and Commonly Used Patellar Height Ratios
 Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
The patellofemoral joint is the articulation between. Patellofemoral Instability. Brian J. White, M.D., and Orrin H. Sherman, M.D.
 22 Bulletin of the NYU Hospital for Joint Diseases 2009;67(1):22-9 Patellofemoral Instability Brian J. White, M.D., and Orrin H. Sherman, M.D. Abstract This review describes the normal patellofemoral joint
22 Bulletin of the NYU Hospital for Joint Diseases 2009;67(1):22-9 Patellofemoral Instability Brian J. White, M.D., and Orrin H. Sherman, M.D. Abstract This review describes the normal patellofemoral joint
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. MPFL RECONSTRUCTION
 ! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Abstract. Introduction. Michele Vasso 1 Katia Corona 2 Giuseppe Toro 1 Marco Rossini 1 Alfredo Schiavone Panni 1
 256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study
 Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study G. Placella, M. M. Tei, E. Sebastiani, G. Criscenti, A. Speziali, C. Mazzola, A. Georgoulis
Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study G. Placella, M. M. Tei, E. Sebastiani, G. Criscenti, A. Speziali, C. Mazzola, A. Georgoulis
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Key words: arthroscopy, orthopaedic examination, magnetic resonance imaging, knee injury.
 Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
 Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Surgical treatment of patellar instability can be
 Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Introduction. Helmut Wegmann 1 Christoph Würnschimmel 2 Tanja Kraus 2 Georg Singer 1 Robert Eberl 1 Holger Till 1 Matthias Sperl 2
 DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
DOI 10.1007/s00167-017-4425-x KNEE Medial patellofemoral ligament (MPFL) reconstruction in combination with a modified grammont technique leads to favorable mid-term results in adolescents with recurrent
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
The Knee 20 S1 (2013) S3 S15. Contents lists available at SciVerse ScienceDirect. The Knee
 The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
The Knee 20 S1 (2013) S3 S15 Contents lists available at SciVerse ScienceDirect The Knee Review The contemporary management of anterior knee pain and patellofemoral instability Toby O. Smith, Iain McNamara,
Medial patellofemoral ligament reconstruction
 KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
KNEE Medial patellofemoral ligament reconstruction A PROSPECTIVE OUTCOME ASSESSMENT OF A LARGE SINGLE CENTRE SERIES N. R. Howells, A. J. Barnett, N. Ahearn, A. Ansari, J. D. Eldridge From Bristol Royal
Patellofemoral Instability in Children: Correlation Between Risk Factors, Injury Patterns, and Severity of Cartilage Damage
 Pediatric Imaging Original Research Kim et al. Patellofemoral Instability in Children Pediatric Imaging Original Research Hee Kyung Kim 1 Sahar Shiraj 1 Chang Ho Kang 2 Christopher Anton 1 Dong Hoon Kim
Pediatric Imaging Original Research Kim et al. Patellofemoral Instability in Children Pediatric Imaging Original Research Hee Kyung Kim 1 Sahar Shiraj 1 Chang Ho Kang 2 Christopher Anton 1 Dong Hoon Kim
Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility
 N. R. Howells, J. D. Eldridge From Bristol Royal Infirmary, Bristol, United Kingdom KNEE Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility A CASE CONTROL
N. R. Howells, J. D. Eldridge From Bristol Royal Infirmary, Bristol, United Kingdom KNEE Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility A CASE CONTROL
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Patellar malalignment: a new method on knee MRI
 DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
Post-injury painful and locked knee
 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
Imaging in patellofemoral instability is essential to the accurate
 REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving primary dislocations
 High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving 24.154 primary dislocations Kasper Skriver Gravesen, Thomas Kallemose, Lars Blønd,
High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving 24.154 primary dislocations Kasper Skriver Gravesen, Thomas Kallemose, Lars Blønd,
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
Downloaded from by on 12/22/17 from IP address Copyright ARRS. For personal use only; all rights reserved
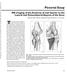 Downloaded from www.ajronline.org by 46.3.205.8 on 12/22/17 from IP address 46.3.205.8. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
Downloaded from www.ajronline.org by 46.3.205.8 on 12/22/17 from IP address 46.3.205.8. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
International Journal of Orthopaedics Sciences 2017; 3(3): Dr. Anas M and Dr. Ansari N. DOI:
 2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
Magnetic resonance imaging evaluation of lateral ankle ligaments and peroneal tendons in a group of asymptomatic patients
 Magnetic resonance imaging evaluation of lateral ankle ligaments and peroneal tendons in a group of asymptomatic patients Abstract: Background: The role of magnetic resonance (MR) imaging in patients with
Magnetic resonance imaging evaluation of lateral ankle ligaments and peroneal tendons in a group of asymptomatic patients Abstract: Background: The role of magnetic resonance (MR) imaging in patients with
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Bone Contusion Patterns of the Knee at MR Imaging: Footprint of the Mechanism of Injury
 SCIENTIFIC EXHIBIT Bone Contusion Patterns of the Knee at MR Imaging: Footprint of the Mechanism of Injury 1 S135 CME FEATURE See accompanying test at http:// www.rsna.org /education /rg_cme.html LEARNING
SCIENTIFIC EXHIBIT Bone Contusion Patterns of the Knee at MR Imaging: Footprint of the Mechanism of Injury 1 S135 CME FEATURE See accompanying test at http:// www.rsna.org /education /rg_cme.html LEARNING
