International Cartilage Repair Society
|
|
|
- Nickolas Melton
- 5 years ago
- Views:
Transcription
1 Osteoarthritis and Cartilage (2008) 16, 1433e1441 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi: /j.joca Review The osteoarthritis initiative: report on the design rationale for the magnetic resonance imaging protocol for the knee C. G. Peterfy M.D., Ph.D.y*, E. Schneider Ph.D.zx and M. Nevitt Ph.D.k y Synarc Inc., San Francisco, CA, USA z SciTrials LLC, Rocky River, OH, USA x Imaging Institute, The Cleveland Clinic, Cleveland, OH, USA k Prevention Sciences Group, Department of Epidemiology, University of California, San Francisco, CA, USA Summary Objectives: To report on the process and criteria for selecting acquisition protocols to include in the osteoarthritis initiative (OAI) magnetic resonance imaging (MRI) study protocol for the knee. Methods: Candidate knee MR acquisition protocols identified from the literature were first optimized at 3 Tesla (T). Twelve knees from 10 subjects were scanned one time with each of 16 acquisitions considered most likely to achieve the study goals and having the best optimization results. The resultant images and multi-planar reformats were evaluated for artifacts and structural discrimination of articular cartilage at the cartilageefluid, cartilageefat, cartilageecapsule, cartilageemeniscus and cartilageecartilage interfaces. Results: The five acquisitions comprising the final OAI MRI protocol were assembled based on the study goals for the imaging protocol, the image evaluation results and the need to image both knees within a 75 min time slot, including positioning. For quantitative cartilage morphometry, fat-suppressed, 3D dual-echo in steady state (DESS) acquisitions appear to provide the best universal cartilage discrimination. Conclusions: The OAI knee MRI protocol provides imaging data on multiple articular structures and features relevant to knee OA that will support a broad range of existing and anticipated measurement methods while balancing requirements for high image quality and consistency against the practical considerations of a large multi-center cohort study. Strengths of the final knee MRI protocol include cartilage quantification capabilities in three planes due to multi-planar reconstruction of a thin slice, high spatial resolution 3D DESS acquisition and the multiple, non-fat-suppressed image contrasts measured during the T2 relaxation time mapping acquisition. ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. Key words: Osteoarthritis, Knee, MRI, Protocol. International Cartilage Repair Society Abbreviations: COR coronal, CNR contrast-to-noise ratio, DESS dual-echo steady state, ETL echo-train length, FDA food and drug administration, FLASH fast low-angle shot, FOV field of view, FS fat suppression, GRE gradient-echo, IW intermediate-weighted, MEMS multi-echo, multi-slice, NEX number of excitations, MPR multiplanar reformation, PD proton density, SAG sagittal, SE spin-echo, SNR signal-to-noise ratio, SPGR spoiled gradient-recalled echo, T1W T1-weighted, T2W T2-weighted, TE echo time, TR repetition time, TSE turbo spin-echo, WE water excitation. Backround Osteoarthritis (OA) of the knee is a significant contributor to disability and loss of independence among middle age and elderly persons and presents a clear and growing public health need ( Because of the chronic nature of OA and its variable clinical outcomes, the use of clinical endpoints in studies of risk and prognostic factors and in clinical trials that test interventions to prevent or slow the progression of this disease requires studying large numbers of patients for long periods of time, often at great expense. Developing effective medical treatments to prevent or to reduce progression of OA is hampered by the lack of robust biomarkers of disease onset and progression. *Address correspondence and reprint requests to: Charles Peterfy, M.D., Ph.D., Synarc Inc., 575 Market Street, 17th Floor, San Francisco, CA 94105, USA. Tel: ; Fax: ; charles.peterfy@synarc.com Received 1 August 2007; revision accepted 26 June The osteoarthritis initiative (OAI) is a publiceprivate partnership jointly sponsored by the National Institutes of Health (NIH), including the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), National Institute on Aging (NIA), National Institute of Dental and Craniofacial Research (NIDCR), National Center for Complementary and Alternative Medicine (NCCAM), Office of Research on Women s Health (ORWH), National Institute of Biomedical Imaging and Bioengineering (NIBIB), and National Center on Minority Health and Health Disparities (NCMHD), and the pharmaceutical industry. The OAI is focused on identifying the most promising biomarkers of development and progression of symptomatic knee OA. A total of 4796 men and women, aged 45e79 years, who either have or are at increased risk of developing knee OA have been enrolled in the study. Annual radiography and magnetic resonance imaging (MRI) of the knee and clinical assessments of disease activity are being performed in all participants over a period of 4 years. Genetic and biochemical specimens are also being collected annually from all participants. 1433
2 1434 C. G. Peterfy et al.: Knee MRI protocol for the osteoarthritis initiative Table I Final OAI knee MRI protocol acquisition time (min) Scan Right knee Left knee Total 1 Localizer (3-plane) COR IW 2D TSE SAG 3D DESS WE COR MPR SAG 3D DESS WE AXIAL MPR SAG 3D DESS WE COR T1W 3D FLASH WE* 8.6 e SAG IW 2D TSE FS SAG 2D MESE* 10.6 e 10.6 Total *Acquired on only right knee, unless right knee contains metal in which case, acquired on only left knee. A primary objective of the OAI is to create a public resource for identifying, characterizing and validating a broad range of imaging biomarkers for OA of the knee that could be used to investigate basic research hypotheses as well as to serve as outcomes in clinical trials of new therapies. Accordingly, the goals for the OAI MRI study protocol are to (1) provide imaging data on as many articular structures and features believed to be relevant to knee OA as possible; (2) provide images that are able to support as broad a range of existing and anticipated measurement methods for each of these structures and features as possible; and (3) balance scientific requirements for image quality and consistency against the need to maintain high throughput of the participants and the ability of the participants to tolerate the annual MRI examinations. The report outlines the rationale used by the OAI Imaging Working Group, which included scientists and clinicians from academia and industry with expertise in MRI of OA and cartilage (see Acknowledgements), to address these design considerations and ultimately to arrive at the knee MRI protocol used in the OAI. This report is not intended to serve as a review of the literature on existing or emerging imaging biomarkers of knee OA using MRI technology. Several excellent reviews have recently been published, and readers are referred to these for broad overviews of the field 1e5. A key consideration in protocol development for the OAI was to identify which knee OA features to target. Since OA affects several articular structures, and is believed to progress through multiple pathogenic pathways, the imaging protocol had to support multi-feature, structural assessment of the knee. The OAI Imaging Working Group prioritized the following knee structures: articular cartilage, osteophytes, bone marrow abnormality (BMA), bone attrition and cysts, the osteochondral junction (bone surface area), meniscal integrity, synovial tissue, joint effusion, anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), medial collateral ligament (MCL) and lateral collateral ligament (LCL). Quantitative assessment of articular cartilage morphology (e.g., volume, thickness, cartilaginous/denuded surface area, etc.) was considered to be particularly important. Many assessments of the selected knee structures have been previously validated using MRI at 1.5 T, and are used widely clinically and in research 6e14. The above priorities determined that anatomical coverage had to include at least the entire patellar, femoral and tibial cartilages but ideally the entire synovial cavity. Other decisions with respect to acquisition planes, spatial resolution, image contrast, and acquisition time are discussed below, but the general principles underlying the tradeoffs are outlined in a report from the Workshop on Imaging Osteoarthritis of the Knee 15, held on December 5e6, 2002 in Bethesda, MD by Outcome Measures in Rheumatology Clinical Trials (OMERACT) and Osteoarthritis Research Society International (OARSI). Early in the planning stages of the OAI, the decision was made to purchase dedicated, state-of-the-art MRI systems for each of the four study sites (The Ohio State University, Columbus, OH; University of Maryland, School of Medicine, Scan Localizer COR IW 2D TSE Table II Final OAI knee MRI protocol acquisition parameters SAG 3D DESS WE COR T1W 3D FLASH WE SAG 2D MESE SAG IW 2D TSE FS Plane 3-plane Coronal Sagittal Coronal Sagittal Sagittal FS No No WE WE No FS Matrix (phase) Matrix (frequency) No. of slices FOV (mm) Slice thickness/gap (mm/mm) 5/1 3/0 0.7/0 1.5/0 3/0.5 3/0 Flip angle (() n/a 180 TE/TR (ms/ms) 5/10 29/ / /20 10, 20, 30, 40, 30/ , 60, 70/2700 Bandwidth (Hz/pixel) Chemical shift (pixels) No. excitations averaged ETL Phase encode axis A/P, R/L R/L A/P R/L A/P A/P Distance factor (%) Phase oversampling Slice oversampling Phase resolution Phase partial Fourier (8/8 ¼ 1) Readout partial Fourier (8/8 ¼ 1) Slice partial Fourier (8/8 ¼ 1) X-resolution (mm) Y-resolution (mm)
3 Osteoarthritis and Cartilage Vol. 16, No. 12 Baltimore, MD; University of Pittsburgh, Pittsburgh, PA; and Memorial Hospital of Rhode Island, Pawtucket, RI) to minimize acquisition variability and accommodate the large number of subjects to be examined over the course of the study. In 2003, when the OAI study was being designed and implemented, 3 Tesla (T) MRI systems had recently been introduced to the commercial market but were not yet routinely available in clinical settings. MRI at 3 T offered potential advantages over 1.5 T in terms of signal level that could be traded for increased signal-to-noise (SNR), spatial resolution or imaging speed. This advantage was felt to be particularly useful for T2 relaxation time measurement of cartilage 2,10,16,17 and was believed to outweigh potential disadvantages of high field strength, such as increased susceptibility to metallic artifacts, increased fat-water chemical shift, and different tissue relaxation times than those observed at 1.5 T 18,19. Inspite of the relative lack of clinical and research experience at 3 T, it was understood that 1.5 T knee MRI protocols would not translate directly to 3 T without adjusting for the differences detailed above. Other important considerations for the OAI included: use of commercially available, food and drug administration (FDA)-approved, pulse sequences and radiofrequency 1435 (RF) coils; minimizing redundancy among acquisitions in the measurements that could be derived from them; the need to position and image both knees within 75 min to prevent subject discomfort and minimize the risk of dropout; and minimizing individual sequence acquisition times to reduce the possibility of motion artifacts and associated image degradation, especially for 3D acquisitions and 2D multi-echo spin-echo (MESE) acquisitions. The process of meeting these diverse goals with a single, uniform protocol entailed selecting the image contrasts most likely to satisfy the anticipated needs and making careful tradeoffs in image spatial resolution and tissue contrasts. To facilitate this process, a pilot study was undertaken in which selected candidate acquisition sequences, based on contrast parameters at 1.5 T, were optimized for use at 3 T. A small sample of knees was then scanned with the most promising acquisitions and the resulting images visually evaluated by musculoskeletal imaging experts affiliated with the OAI (see Acknowledgements) for suitability in cartilage segmentation and semi-quantitative assessments of relevant tissues. Details of this pilot study and its results can found on the OAI website ( Fig. 1. Orientation of coronal acquisitions. Coronal 2D and 3D acquisitions are prescribed coronal to the joint, with the slice axis parallel to the long axis of the femoral diaphysis on the sagittal localizer (A) and to a line tangent to the posterior cortices of the femoral condyles on the axial localizer (B). Depiction of both posterior femoral cortices (arrows) within two slices (3 mm) of each other confirms proper alignment on this example of COR 3D FLASH WE (C).
4 1436 C. G. Peterfy et al.: Knee MRI protocol for the osteoarthritis initiative Fig. 2. Example of COR IW 2D TSE. Note delineation of the MCL, LCL, body segments of the menisci, central tibial and femoral bone margins and the central tibiofemoral articular cartilage. Note that chemical-shift artifact is relatively mild. The OAI MRI protocol The final OAI knee MRI protocol is shown in Tables I and II. Subject positioning and scan set up can be found in detail in the OAI MRI Operator s Manual available on the website ( The knee MRI acquisition begins with a three-plane localizer, followed by a coronal intermediate-weighted (IW) 2D turbo spin-echo (TSE) (COR IW 2D TSE) 7 for evaluating the MCL and LCL, marginal femoral and tibial osteophytes, the medial and lateral meniscal body segments, and the presence/extent of subchondral bone cysts and bone attrition. All 2D and 3D coronal acquisitions are oriented coronal to the joint based on anatomic landmarks using a double oblique prescription (Figs. 1 and 2) 9 in order to improve the reproducibility of crosssectional anatomy depicted on serially acquired MRI exams. The coronal plane 1,9,15 is excellent for evaluating articular cartilage along the central weight-bearing surfaces of the Fig. 4. SAG 3D DESS WE. Note the clear delineation of the cartilage-cartilage (small arrows) and cartilage-capsule (large arrow) interfaces as well as the interfaces between cartilage and adipose (F), bone (B) and meniscus (M). femur and tibia, where the cartilage curves up the tibial spines and the corresponding curves of the adjacent femoral condyles near the notch. This plane is also excellent for delineating the osteochondral junctions at the medial and lateral margins of the femur and tibia. Intermediate weighting 7 is used in COR IW 2D TSE to balance the need for an echo time (TE) short enough to detect non-displaced meniscal tears but still long enough to discriminate articular cartilage. Because of the high density and linear orientation of collagen fibers in the MCL and LCL, these structures show very rapid T2 relaxation and therefore good delineation with intermediate-te sequences. Although the 3D dual-echo in steady state (DESS) image contrast 21 has not been as extensively evaluated for quantitative cartilage measurements as have fat-suppressed 3D fast low-angle shot (FLASH) or 3D spoiled gradient-recalled Fig. 3. Orientation of the sagittal acquisitions. Anatomical coverage on sagittal 2D and 3D acquisitions should include the tibial tubercle, the entire patella and as much of the suprapatellar bursa as possible (A) Sagittal acquisitions are prescribed orthogonal to the coronal acquisitions and sagittal to the joint, with the slice axis parallel to the long axis of the femoral diaphysis on the coronal localizer (B) and perpendicular to a line tangent to the posterior cortices of the femoral condyles on the axial localizer (C).
5 Osteoarthritis and Cartilage Vol. 16, No Fig. 5. Coronal MPR of SAG 3D DESS WE. Orientation is identical to that described in Fig. 1. Note the excellent delineation of the cartilageefluid interface (arrow), and the high contrast between cartilage and bone (B) and cartilage and meniscus (M). echo (SPGR) image contrast, 3D DESS with selective water excitation (WE) appeared to show better cartilage discrimination in pilot scans using volunteer subjects, and therefore was included in the OAI MRI protocol. Sagittal Fig. 6. Axial MPR of SAG 3D DESS WE. Axial coverage includes any superior or inferior patellar osteophytes and extends to the tibial epiphysis. Note the good cartilageefluid contrast revealing thinning of articular cartilage over the lateral facet of the patella (large arrow). Note also, that a small aliasing artifact (small arrow) is present at the top of the image but does not obscure any anatomy of interest. Fig. 7. Sensitivity to subarticular BMA and cysts. SAG IW 2D TSE FS (A) shows both bone cysts (small arrow) and surrounding BMA (large arrow) in the femoral trochlea of this knee. However, both GRE scans, SAG 3D DESS WE (B) and COR 3D FLASH WE (C), of the same knee show only the cysts in this location.
6 1438 C. G. Peterfy et al.: Knee MRI protocol for the osteoarthritis initiative Fig. 8. SAG 2D MESE. Multiple contrast acquisitions having progressively longer TEs can be combined to generate T2 maps of the articular cartilage and adjacent tissues. These seven images illustrate how changing the TE affects the relative signal and relative contrast among the different tissues in the knee. (SAG) 3D DESS WE was found not only to provide excellent cartilage delineation for morphological measurements, such as total joint cartilage thickness and volume, it also delineates osteophytes along the anterior and posterior margins of the femur and tibia and the superior and inferior margins of the patella with high resolution, shows tears of the anterior and posterior horns of the menisci, depicts subarticular bone cysts and bone attrition, and assesses
7 Osteoarthritis and Cartilage Vol. 16, No Fig. 8. (continued) integrity of the ACL and PCL and the patellar and quadriceps tendons 1,15. In addition, the SAG 3D DESS acquisition is faster than an equivalent 3D FLASH (or SPGR) acquisition; the resultant time savings can be potentially traded for increased SNR or spatial resolution. All 2D and 3D sagittal acquisitions are oriented sagittal to the joint based on anatomic landmarks and are orthogonal to the coronal acquisitions (Figs. 3 and 4). The 3D DESS WE acquisition selected uses 0.7 mm thick slices. Thinner slices could have been obtained, however, the cost in increased scan time and subsequent loss of SNR was considered to be excessive. The 3D FLASH WE acquisition, in contrast, uses 1.5 mm slices, as was the coronal slice thickness that was previously validated at 1.5 T 3,11,12,22,23. Because the SAG 3D DESS WE acquisition has thin slices, the resultant images can also be reformatted (MPR) into the coronal and axial planes (Figs. 5 and 6) to display optimally the tibial and central weight-bearing surface of the femoral cartilage, as well as the trochlear and patellar cartilage, respectively 1,3,6,11,13. The multiplanar reformation (MPR) images can be of variable slice thickness; 1.5 mm was chosen for the OAI to enable comparison with the previously validated coronal 3D FLASH images. Other MPR orientations and slice thicknesses can be retrospectively calculated from the sagittal images. However, the in-plane spatial resolution of the MPR images is governed by the size and orientation of the voxels in the original acquisition. The SAG 3D DESS WE series utilizes near anisotropic voxels (0.7 mm slice thickness 0.37 mm 0.46 mm) to maximize in-plane sagittal spatial resolution in a reasonable acquisition time (10.5 min). The resultant in-plane coronal MPR spatial resolution is thus 0.7 mm 0.37 mm. The COR T1-weighted (T1W) 3D FLASH WE acquisition also provides high-resolution delineation of articular cartilage 9, and as noted above has been extensively validated at 1.5 T and shown to support accurate quantification of the volume and thickness of cartilage over the tibial plateaus and the central surface of the femur 3,11,12. Since the OAI MRI protocol was designed and implemented, 3D FLASH WE at 3 T has been cross-validated with 3D FLASH WE at 1.5 T for quantitative analysis of cartilage morphology 23,24. The OAI protocol also includes SAG IW 2D TSE fat suppression (FS), which provides excellent assessment of the ACL and PCL, the anterior and posterior horns of the menisci, anterior and posterior osteophytes, synovial effusion and peri-articular cysts and bursae. This technique also delineates articular cartilage; although, not as well as the 3D acquisitions do. To obtain relatively high spatial resolution in a relatively short acquisition time, the field of view (FOV) was made smaller (16 cm) than desired (24 cm) for complete coverage of the synovial cavity. The unique contribution of the SAG IW 2D TSE FS acquisition to the protocol is its sensitivity to BMA and subchondral cysts 1,25e27 (Fig. 7A). Gradient-echo (GRE) techniques, such as 3D DESS (Fig. 7B) and 3D FLASH (Fig. 7C), even with robust FS, are relatively insensitive to BMA (large arrow in Fig. 7A). They are, however, sensitive for subchondral cysts (thin arrow). Finally, SAG 2D MESE is included in the protocol to allow quantification of cartilage T2 relaxation times as well as to provide a range of non-fat-suppressed image contrasts (proton density [PD], IW, T2-weighted [T2W]) (Fig. 8) to improve assessment of many joint components, including ligaments and tendons, and the cartilageebone interface. T2 relaxation times are believed to relate to the integrity of cartilage matrix, particularly collagen, and therefore to be potentially useful for evaluating early degeneration 2,10,16. Based on the acquisition time constraints, the OAI Imaging Working Group decided that it was not feasible to obtain all acquisitions in the final protocol on both knees. Accordingly, two acquisitions were excluded from the left knee examination (Table I) unless subjects had surgical hardware in the right knee, in which case, the two sequences would be performed on the knee without surgical hardware. Subjects with unilateral knee arthroplasty would have no MRI examinations of the operated knee. COR T1W 3D FLASH WE was elected to be acquired on only one knee because SAG 3D DESS WE was considered to provide better contrast for delineating the interface between articular cartilage and a range of degenerated and normal tissues, as well as better contrast for evaluating menisci, ligaments and synovial effusion. In pilot scans of volunteer knees, the cartilageecapsule and cartilageecartilage interfaces (Fig. 4) were often difficult to discriminate with 3D FLASH WE, but were well discriminated with 3D DESS WE. Both 3D FLASH WE and 3D DESS WE were felt to provide excellent delineation of osteophytes, however, the most important contribution of SAG 3D DESS WE in this protocol is high-resolution delineation of articular cartilage. 3D FLASH WE and 3D DESS WE have subsequently been cross-validated at 3 T for cartilage volume quantification 28e35. The absolute value performance and testeretest precision of the direct SAG 3D DESS and the coronal MPR DESS image series were found to be comparable to that provided by coronal 3D FLASH in a cross-sectional analysis. These results, and the history of use in knee OA studies, support the decision to include COR T1W 3D FLASH WE in the OAI MRI protocol. However, insufficient acquisition time was available to perform this technique in both knees. Similarly, SAG 2D MESE was performed on only one of the two knees to meet imaging time constraints. Finally, the Imaging Working Group felt that axial MPR of the high-resolution SAG 3D DESS WE would provide sufficient visualization of the patellofemoral joint in a plane orthogonal to the cartilage plate, and therefore excluded direct axial imaging of either knee. Total imaging time for the final OAI knee MRI protocol is 58 min (Table I), leaving 17 min for subject positioning, coil placement and for scan prescription to stay within the total examination time limit of 75 min for both knees.
8 1440 C. G. Peterfy et al.: Knee MRI protocol for the osteoarthritis initiative Conclusion In summary, the OAI MRI protocol offers a balance between the scientific and practical considerations in assessing the key articular structures and features believed to be involved in the development and progression of OA in the knee. While implementation of such a long and rigorous MRI protocol may not be feasible in the clinic or in all clinical trials, it is hoped that OAI will help guide the development of more streamlined protocols applicable for use at either 3 T or 1.5 T. Several limitations of the protocol development process should be noted. We were limited to the acquisition and analysis methods which had been validated as of Although other MRI biomarkers that relate to cartilage matrix damage 2,5,20,36,37 and subchondral trabecular architecture and bone volume 14 have been described, the current OAI MRI protocol does not have sufficient imaging time to support those measurements and still satisfies its primary scientific objectives. Given time constraints for planning and startup of the OAI, the knee MRI protocol was finalized and implemented without formally assessing the performance characteristics of any biomarker measurements, such as cartilage volume, semi-quantitative assessments of articular lesions, etc. Since the OAI protocol was implemented, several studies of quantitative cartilage morphology using images acquired with the OAI protocol and addressing measurement precision, 3D FLASH vs 3D DESS comparisons and sensitivity to change have been published 28e35,38,39. These performance parameters will continue to be important topics for investigation. No external validation (compared to cadaver or arthroscopy) of cartilage measurements or assessments has been done using the OAI MRI protocol or any other acquisition protocol at 3 T. Key parameters (e.g., spatial resolution) of the 3D FLASH acquisitions included in the OAI protocol were identical to those previously validated at 1.5 T for quantitative cartilage measurements compared to cadaver knees 12. Moreover, 3D FLASH acquisitions acquired with the same resolution at 1.5 T and 3 T gave identical precision for quantitative cartilage measurements 23. We have no reason to believe that external validation results would differ between 3 T and 1.5 T acquisitions, but studies are needed to confirm this. The OAI clinical data set as well as the radiographic and MRI images are available through the study s public website ( It is hoped that the OAI MRI images will support not only the majority of analysis methods and imaging biomarker measurements that are currently available but many of those yet to be developed. We urge users of the OAI public data to employ a systematic framework, such as the OMERACT filter 40, to the development and validation of imaging biomarkers of OA. The availability of these images to the general community of investigators should serve to accelerate research in OA and thus our understanding of this enigmatic disease and how to combat it. Conflict of interest None of the authors have any financial or other interests related to the manuscript submitted to Osteoarthritis and Cartilage that might constitute a potential conflict of interest. Acknowledgements This manuscript has been reviewed by the OAI Publications committee for scientific content and data interpretation. The research reported in this article was supported in part by contracts N01-AR , N01-AR and N01-AR from NIAMS. We are grateful to the Ohio State University team for acquiring the MRI images used for the study. The team that reviewed the pilot images was composed of (alphabetical order): BJ Dardzinski PhD, F Eckstein MD, D Goodwin MD, A Guermazi MD, R Jackson MD, M Nevitt PhD, S Totterman, MD PhD, L Martin BS RT (R) (MR), A Padua Jr RT, CG Peterfy MD PhD, J Pitts RT (R) (MR), E Schneider PhD, D White PhD, CS Winalski MD, J Yu MD. We are also grateful to Wendy Bommer RN (Cincinnati Children s Hospital), Kim Toussant (Ohio State University), David Purdy PhD (Siemens Medical Solutions), Joseph Murphy- Bosch PhD (USA Instruments), Katherine Hall (Synarc Inc), Mary Hochman MD (Beth Israel Medical Center), Perry Renshaw MD, PhD (McLean Hospital, Brain Imaging Center), H. Cecil Charles PhD (Duke University Medical School). The OAI Imaging Working Group was composed of the following individuals: Charles Peterfy MD PhD (chair), and in alphabetical order, Mostafa Analoui PhD, Fernando Boada PhD, Denise Davis RTR(MR), Bernard J. Dardzinski PhD, Felix Eckstein PhD, Jeff Evelhoch PhD, Faiza Fawaz- Estrup PhD MD FACP FACR, David Felson MD MPH, Garry E. Gold MD PhD, Doug Goodwin MD, Rao Gullapalli PhD, Marie-Pierre Hellio Le Graverand MD, Ali Guermazi MD, Manish Kothari PhD, Philipp K. Lang MD PhD MBA, Gayle Lester PhD, Larry Martin BS RT(R) (MR), Michael Nevitt PhD, Theodore Pellas VMD PhD, David Purdy PhD, Charles Resnick MD, Douglas Robertson MD, Erika Schneider PhD, Leena Sharma MD, Saara Totterman MD PhD, Glenn Tung MD, Joseph Yu MD, David White PhD, Katherine Wildy MD, Carl Winalski MD, and Thasia Woodworth MD. The OAI is a publiceprivate partnership which comprised five contracts (N01-AR ; N01-AR ; N01-AR ; N01-AR ; N01-AR ) funded by the National Institutes of Health, a branch of the Department of Health and Human Services, and conducted by the OAI Study Investigators. Private funding partners include Merck Research Laboratories; Novartis Pharmaceuticals Corporation, GlaxoSmithKline; and Pfizer, Inc. Private sector funding for the OAI is managed by the Foundation for the National Institutes of Health. This manuscript has received the approval of the OAI Publications Committee based on a review of its scientific content and data interpretation. References 1. Peterfy CG, Gold G, Eckstein F, Cicuttini F, Dardzinski B, Stevens R. MRI protocols for whole-organ assessment of the knee in osteoarthritis. Osteoarthritis Cartilage 2006;14(Suppl A):A95eA Gold GE, Burstein D, Dardzinski B, Lang P, Boada F, Mosher T. MRI of articular cartilage in OA: novel pulse sequences and compositional/- functional markers. Osteoarthritis Cartilage 2006;14(Suppl A): A76e Eckstein F, Cicuttini F, Raynauld JP, Waterton JC, Peterfy C. Magnetic resonance imaging (MRI) of articular cartilage in knee osteoarthritis (OA): morphological assessment. Osteoarthritis Cartilage 2006; 14(Suppl A):A46e Eckstein F, Mosher T, Hunter D. Imaging of knee osteoarthritis: data beyond the beauty. Curr Opin Rheumatol 2007;19(5):435e Burstein D, Gray ML. Is MRI fulfilling its promise for molecular imaging of cartilage in arthritis? Osteoarthritis Cartilage 2006;14(11):1087e90.
9 Osteoarthritis and Cartilage Vol. 16, No Waldschmidt JG, Rilling RJ, Kajdacsy-Balla AA, Boynton MD, Erickson SJ. In vitro and in vivo MR imaging of hyaline cartilage: zonal anatomy, imaging pitfalls, and pathologic conditions. Radiographics 1997;17(6):1387e Potter HG, Linklater JM, Allen AA, Hannafin JA, Haas SB. Magnetic resonance imaging of articular cartilage in the knee. An evaluation with use of fast-spin-echo imaging. J Bone Joint Surg Am 1998; 80(9):1276e Woertler K, Strothmann M, Tombach B, Reimer P. Detection of articular cartilage lesions: experimental evaluation of low- and high-fieldstrength MR imaging at 0.18 and 1.0 T. J Magn Reson Imaging 2000;11(6):678e Glaser C, Burgkart R, Kutschera A, Englmeier KH, Reiser M, Eckstein F. Femoro-tibial cartilage metrics from coronal MR image data: technique, testeretest reproducibility, and findings in osteoarthritis. Magn Reson Med 2003;50(6):1229e Mosher TJ, Dardzinski BJ. Cartilage MRI T2 relaxation time mapping: overview and applications. Semin Musculoskelet Radiol 2004;8(4): 355e Eckstein F, Glaser C. Measuring cartilage morphology with quantitative magnetic resonance imaging. Semin Musculoskelet Radiol 2004;8(4): 329e Graichen H, von Eisenhart-Rothe R, Vogl T, Englmeier KH, Eckstein F. Quantitative assessment of cartilage status in osteoarthritis by quantitative magnetic resonance imaging: technical validation for use in analysis of cartilage volume and further morphologic parameters. Arthritis Rheum 2004;50(3):811e Cicuttini FM, Wluka AE, Wang Y, Stuckey SL. Longitudinal study of changes in tibial and femoral cartilage in knee osteoarthritis. Arthritis Rheum 2004;50(1):94e Eckstein F, Burstein D, Link TM. Quantitative MRI of cartilage and bone: degenerative changes in osteoarthritis. NMR Biomed 2006;19(7): 822e Peterfy C, Woodworth T, Altman R. Workshop for consensus on osteoarthritis imaging: MRI of the knee. Osteoarthritis Cartilage 2006;(14): A44e Dardzinski BJ, Mosher TJ, Li S, Van Slyke MA, Smith MB. Spatial variation of T2 in human articular cartilage. Radiology 1997;205(2): 546e Goodwin DW, Dunn JF. MR imaging and T2 mapping of femoral cartilage. AJR Am J Roentgenol 2002;178(6):1568e9 [author reply 1569e1570]. 18. Bottomley PA, Foster TH, Argersinger RE, Pfeifer LM. A review of normal tissue hydrogen NMR relaxation times and relaxation mechanisms from 1e100 MHz: dependence on tissue type, NMR frequency, temperature, species, excision, and age. Med Phys 1984;11(4): 425e Gold GE, Han E, Stainsby J, Wright G, Brittain J, Beaulieu C. Musculoskeletal MRI at 3.0 T: relaxation times and image contrast. AJR Am J Roentgenol 2004;183(2):343e Gray ML, Burstein D, Kim YJ, Maroudas A. Magnetic resonance imaging of cartilage glycosaminoglycan: basic principles, imaging technique, and clinical applications. J Orthop Res Hardy PA, Recht MP, Piraino D, Thomasson D. Optimization of a dual echo in the steady state (DESS) free-precession sequence for imaging cartilage. J Magn Reson Imaging 1996;6(2):329e Eckstein F, Sittek H, Milz S, Putz R, Reiser M. The morphology of articular cartilage assessed by magnetic resonance imaging (MRI). Reproducibility and anatomical correlation. Surg Radiol Anat 1994;16(4): 429e Eckstein F, Charles HC, Buck RJ, Kraus VB, Remmers AE, Hudelmaier M, et al. Accuracy and precision of quantitative assessment of cartilage morphology by magnetic resonance imaging at 3.0 T. Arthritis Rheum 2005;52(10):3132e Tamez-Pena J, Barbu-McInnes M, Buck R, Totterman S. Cross validation of fused SPGR-GRE T2* MRI at 1.5 T and 3.0 T for morphological cartilage analysis. Osteoarthritis and Cartilage 2005;12(Suppl 2):S1e Peterfy C. Medial knee pain in the aging patient. In: Rheumatology. Philadelphia: Mosby; 1998:8.12.8e Felson DT, Chaisson CE, Hill CL, Totterman SM, Gale ME, Skinner KM, et al. The association of bone marrow lesions with pain in knee osteoarthritis. Ann Intern Med 2001;134(7):541e Felson DT, McLaughlin S, Goggins J, LaValley MP, Gale ME, Totterman S, et al. Bone marrow edema and its relation to progression of knee osteoarthritis. Ann Intern Med 2003;139(5 Pt 1):330e Peterfy C, Schneider E, White D, Guermazi A, Zhao J, Kothari M, et al. Cartilage volume quantification with 3 tesla MRI: comparison of 3D- DESS with 3D-FLASH imaging sequences. Osteoarthritis Cartilage 2004;12(SB): Tamez-Pena J, Barbu-McInnes M, Jackson R, Yu J, Eaton CB, Totterman S. Boneecartilage contrast ratio (BCCR) from MRI DESS sequences: signal-based quantitative biomarker in OA studies. ACR 2005; Barbu-McInnes M, Tamez-Pena J, Jackson R, Yu J, Eaton CB, Totterman S. Subject specific bone atlas: segmentation applications and validation on OA subjects. MICCAI 2005;P1-6, S-T1, p Tamez-Pena J, Barbu-McInnes M, Jackson R, Yu J, Eaton CB, Totterman S. Cartilage quantification: comparison between 3 T DESS and 3 T FLASH sequences. Osteoarthritis and Cartilage 2005;12(Suppl 2: S1e2): Eckstein F, Hudelmaier M, Wirth W, Kiefer B, Jackson R, Yu J, et al. Double echo steady state magnetic resonance imaging of knee articular cartilage at 3 Tesla: a pilot study for the osteoarthritis initiative. Ann Rheum Dis 2006;65(4):433e Duryea J, Neumann G, Brem MH, Koh W, Noorbakhsh F, Jackson RD, et al. Novel fast semi-automated software to segment cartilage for knee MR acquisitions. Osteoarthritis Cartilage 2007;15(5):487e Eckstein F, Kunz M, Hudelmaier M, Jackson R, Yu J, Eaton CB, et al. Impact of coil design on the contrast-to-noise ratio, precision, and consistency of quantitative cartilage morphometry at 3 Tesla: a pilot study for the osteoarthritis initiative. Magn Reson Med 2007;57(2):448e Eckstein F, Kunz M, Schutzer M, Hudelmaier M, Jackson RD, Yu J, et al. Two year longitudinal change and testeretest-precision of knee cartilage morphology in a pilot study for the osteoarthritis initiative. Osteoarthritis Cartilage 2007;15(11):1326e Gray ML, Eckstein F, Peterfy C, Dahlberg L, Kim YJ, Sorensen AG. Toward imaging biomarkers for osteoarthritis. Clin Orthop Relat Res 2004;(Suppl 427):S175e Borthakur A, Mellon E, Niyogi S, Witschey W, Kneeland JB, Reddy R. Sodium and T1rho MRI for molecular and diagnostic imaging of articular cartilage. NMR Biomed 2006;19(7):781e Hunter D, Niu J, Zhang Y, Totterman S, Tamez J, Dabrowski C, et al. Change in cartilage morphometry: a sample of the progression cohort of the osteoarthritis initiative. Arthritis Rheum 2007;56(9S):S Eckstein F, Maschek S, Wirth W, Wyman B, Hudelmaier M, Nevitt M, et al. Change in femorotibial cartilage volume and subregional cartilage thickness over 1 year e data from the osteoarthritis initiative progression subcohort. Arthritis Rheum 2007;56(9S):S Lassere MN. A users guide to measurement in medicine. Osteoarthritis Cartilage 2006;14(Suppl A):A10e3.
Accuracy and Precision of Quantitative Assessment of Cartilage Morphology by Magnetic Resonance Imaging at 3.0T
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3132 3136 DOI 10.1002/art.21348 2005, American College of Rheumatology Accuracy and Precision of Quantitative Assessment of Cartilage Morphology
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3132 3136 DOI 10.1002/art.21348 2005, American College of Rheumatology Accuracy and Precision of Quantitative Assessment of Cartilage Morphology
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2007) 15, 487e492 ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.11.002 Novel fast semi-automated
OsteoArthritis and Cartilage (2007) 15, 487e492 ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.11.002 Novel fast semi-automated
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis
 In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis Jose G. Raya 1, Annie Horng 2, Olaf Dietrich 2, Svetlana Krasnokutsky 3, Luis S. Beltran 1, Maximilian F.
In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis Jose G. Raya 1, Annie Horng 2, Olaf Dietrich 2, Svetlana Krasnokutsky 3, Luis S. Beltran 1, Maximilian F.
MRI Assessments of Cartilage
 SNR IMPACTS THE ACCURACY AND PRECISION OF KNEE ARTICULAR CARTILAGE T2 RELAXATION TIME MEASUREMENTS B.J. Dardzinski 1, E. Schneider 2 1 Merck Sharp & Dohme Corp., West Point, PA USA 2 Imaging Institute,
SNR IMPACTS THE ACCURACY AND PRECISION OF KNEE ARTICULAR CARTILAGE T2 RELAXATION TIME MEASUREMENTS B.J. Dardzinski 1, E. Schneider 2 1 Merck Sharp & Dohme Corp., West Point, PA USA 2 Imaging Institute,
kmri_qcart_eckstein_descrip 8/7/2017 1
 Central Assessments of MRI Images for Quantitative Measurements of Cartilage Morphology from knee MRI Scans (Felix Eckstein: Chondrometrics and Paracelsus) 1. Overview... 2 1.1 SAS dataset... 2 1.2 Contents
Central Assessments of MRI Images for Quantitative Measurements of Cartilage Morphology from knee MRI Scans (Felix Eckstein: Chondrometrics and Paracelsus) 1. Overview... 2 1.1 SAS dataset... 2 1.2 Contents
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping
 TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
E. ÇAĞLAR, G. ŞAH N 1, T. OĞUR, E. AKTAŞ. Introduction. Abstract. OBJECTIVE: To identify changes in
 European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Orthopedic Hardware Imaging Part II: MRI v. Metal
 Orthopedic Hardware Imaging Trent Roth, MD And Lauren Ladd, MD Indiana University School of Medicine IU Health Physicians-Radiology Recap: Imaging Techniques Radiography Standard for initial and surveillance
Orthopedic Hardware Imaging Trent Roth, MD And Lauren Ladd, MD Indiana University School of Medicine IU Health Physicians-Radiology Recap: Imaging Techniques Radiography Standard for initial and surveillance
Osteoarthritis and Cartilage 18 (2010)
 Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
Imaging of Articular Cartilage
 Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
Comparative study of imaging at 3.0 T versus 1.5 T of the knee
 Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Osteoarthritis and Cartilage 18 (2010) 1402e1407
 Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
How Much Tesla Is Too Much?
 How Much Tesla Is Too Much? Johnny U. V. Monu, MB, BS; MSc Professor of Radiology and Orthopedics University of Rochester School of Medicine Rochester, New York Historical Timeline Clinical Imaging 1970
How Much Tesla Is Too Much? Johnny U. V. Monu, MB, BS; MSc Professor of Radiology and Orthopedics University of Rochester School of Medicine Rochester, New York Historical Timeline Clinical Imaging 1970
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
International Cartilage Repair Society
 OsteoArthritis and (2007) 15, 110e115 ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.08.006 Brief report Accuracy and testeretest
OsteoArthritis and (2007) 15, 110e115 ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.08.006 Brief report Accuracy and testeretest
ARTICLE IN PRESS. International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Osteoarthritis and Cartilage 18 (2010) 1393e1401
 Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Personalized Solutions. MRI Protocol for PSI and Signature Guides
 Personalized Solutions MRI Protocol for PSI and Signature Guides 2 Personalized Solutions MRI Protocol for PSI and Signature Guides Purpose and Summary This protocol is applicable for the Zimmer Biomet
Personalized Solutions MRI Protocol for PSI and Signature Guides 2 Personalized Solutions MRI Protocol for PSI and Signature Guides Purpose and Summary This protocol is applicable for the Zimmer Biomet
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol
 KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
Quantitative magnetic resonance imaging of osteoarthritis
 For reprint orders, please contact: reprints@futuremedicine.com PERSPECTIVE Quantitative magnetic resonance imaging of osteoarthritis Felix Eckstein Institute of Anatomy & Musculoskeletal Research, Paracelsus
For reprint orders, please contact: reprints@futuremedicine.com PERSPECTIVE Quantitative magnetic resonance imaging of osteoarthritis Felix Eckstein Institute of Anatomy & Musculoskeletal Research, Paracelsus
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging
 Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging cases. Hitachi Medical Systems America, Inc. 1959 Summit
Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging cases. Hitachi Medical Systems America, Inc. 1959 Summit
Meniscal tears on 3T MR: Patterns, pearls and pitfalls
 Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
Intraosseous Bio Filler. Surgical Technique
 Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
A Method to Monitor Local Changes in MR Signal Intensity in Articular Cartilage: A Potential Marker for Cartilage Degeneration in Osteoarthritis
 A Method to Monitor Local Changes in MR Signal Intensity in Articular Cartilage: A Potential Marker for Cartilage Degeneration in Osteoarthritis Josephine H. Naish 1, Graham Vincent 2, Mike Bowes 2, Manish
A Method to Monitor Local Changes in MR Signal Intensity in Articular Cartilage: A Potential Marker for Cartilage Degeneration in Osteoarthritis Josephine H. Naish 1, Graham Vincent 2, Mike Bowes 2, Manish
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
OAI Data Users ACR Study Group
 OAI Data Users ACR Study Group ACR Annual Meeting Oct 27, 2008 Outline of session Objectives: introduce prospective and new users to the OAI, describe how to access the public data, images and biospecimens,
OAI Data Users ACR Study Group ACR Annual Meeting Oct 27, 2008 Outline of session Objectives: introduce prospective and new users to the OAI, describe how to access the public data, images and biospecimens,
Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR Imaging
 Provläsningsexemplar / Preview TECHNICAL REPORT ISO/TR 16379 First edition 2014-03-01 Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR
Provläsningsexemplar / Preview TECHNICAL REPORT ISO/TR 16379 First edition 2014-03-01 Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR
Review Article Quantitative Cartilage Imaging in Knee Osteoarthritis
 Arthritis Volume 2011, Article ID 475684, 19 pages doi:10.1155/2011/475684 Review Article Quantitative Cartilage Imaging in Knee Osteoarthritis Felix Eckstein 1, 2 and Wolfgang Wirth 1, 2 1 Institute of
Arthritis Volume 2011, Article ID 475684, 19 pages doi:10.1155/2011/475684 Review Article Quantitative Cartilage Imaging in Knee Osteoarthritis Felix Eckstein 1, 2 and Wolfgang Wirth 1, 2 1 Institute of
Osteoarthritis and Cartilage 18 (2010) 1275e1283
 Osteoarthritis and Cartilage 18 (2010) 1275e1283 Reference values and s for subregional femorotibial cartilage thickness e results from a large population-based sample (Framingham) and comparison with
Osteoarthritis and Cartilage 18 (2010) 1275e1283 Reference values and s for subregional femorotibial cartilage thickness e results from a large population-based sample (Framingham) and comparison with
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and Radiographic Progression in Men and Women With Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
MRI of the Knee: Part 2 - menisci. Mark Anderson, M.D. University of Virginia Health System
 MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
Personal use only. MRI Metal Artifact Reduction: Shoulder Implants and Arthroplasty. Reto Sutter, MD
 MRI Metal Artifact Reduction: Shoulder Implants and Arthroplasty Reto Sutter, MD University Hospital Balgrist Zurich University of Zurich Cor PD fat sat 56-year old male patient with positive lift-off
MRI Metal Artifact Reduction: Shoulder Implants and Arthroplasty Reto Sutter, MD University Hospital Balgrist Zurich University of Zurich Cor PD fat sat 56-year old male patient with positive lift-off
ACR MRI Accreditation: Medical Physicist Role in the Application Process
 ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
Knee Joint Anatomy 101
 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
High Field MR of the Spine
 Department of Radiology University of California San Diego 3T for MR Applications Advantages High Field MR of the Spine Increased signal-to-noise Better fat suppression Increased enhancement with gadolinium
Department of Radiology University of California San Diego 3T for MR Applications Advantages High Field MR of the Spine Increased signal-to-noise Better fat suppression Increased enhancement with gadolinium
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
ACR MRI Accreditation Program. ACR MRI Accreditation Program Update. Educational Objectives. ACR accreditation. History. New Modular Program
 ACR MRI Accreditation Program Update Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives Present requirements of the new
ACR MRI Accreditation Program Update Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives Present requirements of the new
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
3D high-resolution MR imaging can provide reliable information
 Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies
 Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Biomechanics of the Knee. Valerie Nuñez SpR Frimley Park Hospital
 Biomechanics of the Knee Valerie Nuñez SpR Frimley Park Hospital Knee Biomechanics Kinematics Range of Motion Joint Motion Kinetics Knee Stabilisers Joint Forces Axes The Mechanical Stresses to which
Biomechanics of the Knee Valerie Nuñez SpR Frimley Park Hospital Knee Biomechanics Kinematics Range of Motion Joint Motion Kinetics Knee Stabilisers Joint Forces Axes The Mechanical Stresses to which
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Post-injury painful and locked knee
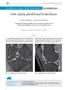 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Imaging the Knee 17/10/2017. Friction syndrome Common in runners or cyclists Fluid between ITB and Lateral femoral condyle
 17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2006) 14, A46eA75 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.02.026 Magnetic resonance imaging
OsteoArthritis and Cartilage (2006) 14, A46eA75 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.02.026 Magnetic resonance imaging
Role of Magnetic Resonance Imaging in Patients with Knee Trauma
 Original Research Article Role of Magnetic Resonance Imaging in Patients with Knee Trauma Bhautik Kapadia 1, Bhumika Suthar 2* 1 Associate Professor, 2 Assistant Professor, Department of Radiodiagnosis,
Original Research Article Role of Magnetic Resonance Imaging in Patients with Knee Trauma Bhautik Kapadia 1, Bhumika Suthar 2* 1 Associate Professor, 2 Assistant Professor, Department of Radiodiagnosis,
Distribution of MR-detected cartilage defects of the patellofemoral joint in chronic knee pain
 OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
Disclosures. Background. Background
 Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Osteoarthritis and Cartilage 19 (2011) 689e699
 Osteoarthritis and Cartilage 19 (2011) 689e699 MRI-based extended ordered values more efficiently differentiate cartilage loss in knees with and without joint space narrowing than region-specific approaches
Osteoarthritis and Cartilage 19 (2011) 689e699 MRI-based extended ordered values more efficiently differentiate cartilage loss in knees with and without joint space narrowing than region-specific approaches
Planning knee OA prevention studies in obese populations Lessons from the Multicenter Osteoarthritis Study (MOST) and Osteoathritis Initiative (OAI)
 Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
MRI of Bucket-Handle Te a rs of the Meniscus of the Knee 1
 MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA
 Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
MRI EVALUATION OF KNEE CARTILAGE
 UPDATING ARTICLE MRI EVALUATION OF KNEE CARTILAGE Marcelo Bordalo Rodrigues 1, Gilberto Luís Camanho 2 ABSTRACT Through the ability of magnetic resonance imaging (MRI) to characterize soft tissue noninvasively,
UPDATING ARTICLE MRI EVALUATION OF KNEE CARTILAGE Marcelo Bordalo Rodrigues 1, Gilberto Luís Camanho 2 ABSTRACT Through the ability of magnetic resonance imaging (MRI) to characterize soft tissue noninvasively,
Accurate Automated Volumetry of Cartilage of the Knee using Convolutional Neural Networks: Data from the Osteoarthritis Initiative 1
 Zuse Institute Berlin Takustr. 7 14195 Berlin Germany ALEXANDER TACK, STEFAN ZACHOW Accurate Automated Volumetry of Cartilage of the Knee using Convolutional Neural Networks: Data from the Osteoarthritis
Zuse Institute Berlin Takustr. 7 14195 Berlin Germany ALEXANDER TACK, STEFAN ZACHOW Accurate Automated Volumetry of Cartilage of the Knee using Convolutional Neural Networks: Data from the Osteoarthritis
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
High-Resolution 3D Cartilage Imaging with IDEAL SPGR at 3 T
 Siepmann et al. Knee MRI with IDEL SPGR Musculoskeletal Imaging Technical Innovation David. Siepmann 1 Jeff McGovern 2 Jean H. rittain 3 Scott. Reeder 1,4 Siepmann D, McGovern J, rittain JH, Reeder S Keywords:
Siepmann et al. Knee MRI with IDEL SPGR Musculoskeletal Imaging Technical Innovation David. Siepmann 1 Jeff McGovern 2 Jean H. rittain 3 Scott. Reeder 1,4 Siepmann D, McGovern J, rittain JH, Reeder S Keywords:
Thanks. As something to help remember. Thanks 07/02/14. Arthroscopy TKR V Uni. Arthroscopy TKR V Uni. Role of arthroscopy to choose operation
 07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION
 LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
Objectives. The BIG Joint. Case 1. Boney Architecture. Presenter Disclosure Information. Common Knee Problems
 3:30 4:15 pm Common Knee Problems SPEAKER Christopher J. Visco, MD Presenter Disclosure Information The following relationships exist related to this presentation: Christopher J. Visco, MD: Speaker s Bureau
3:30 4:15 pm Common Knee Problems SPEAKER Christopher J. Visco, MD Presenter Disclosure Information The following relationships exist related to this presentation: Christopher J. Visco, MD: Speaker s Bureau
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Case study #11 Rt. knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/442 Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy T Sundara
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/442 Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy T Sundara
Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations.
 Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations. Poster No.: C-0998 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Soscia, G. Palma, C. Sirignano, D. Iodice,
Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations. Poster No.: C-0998 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Soscia, G. Palma, C. Sirignano, D. Iodice,
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Viviane Khoury, MD. Assistant Professor Department of Radiology University of Pennsylvania
 U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence and Progression
 ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
Available online at
 Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Definition of osteoarthritis on MRI: results of a Delphi exercise
 Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Magnetic Resonance Imaging of Superficial Cartilage Lesions: Role of Contrast in Lesion Detection
 JOURNAL OF MAGNETIC RESONANCE IMAGING 10:178 182 (1999) Original Research Magnetic Resonance Imaging of Superficial Cartilage Lesions: Role of Contrast in Lesion Detection Timothy J. Mosher, MD* and Steven
JOURNAL OF MAGNETIC RESONANCE IMAGING 10:178 182 (1999) Original Research Magnetic Resonance Imaging of Superficial Cartilage Lesions: Role of Contrast in Lesion Detection Timothy J. Mosher, MD* and Steven
Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain
 Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain Mahesh R. Patel, Roman A. Klufas, Ronald A. Alberico, and Robert R. Edelman PURPOSE:
Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain Mahesh R. Patel, Roman A. Klufas, Ronald A. Alberico, and Robert R. Edelman PURPOSE:
Correspondence should be addressed to Thomas Kurien;
 Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Assessment of Adipose Tissue from Whole Body 3T MRI Scans
 Assessment of Adipose Tissue from Whole Body 3T MRI Scans Ting Song 1, Jing An 2, Qun Chen 2, Vivian Lee 2, Andrew Laine 1 1 Department of Biomedical Engineering, Columbia University, New York, NY, USA
Assessment of Adipose Tissue from Whole Body 3T MRI Scans Ting Song 1, Jing An 2, Qun Chen 2, Vivian Lee 2, Andrew Laine 1 1 Department of Biomedical Engineering, Columbia University, New York, NY, USA
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Case study #12 Left knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration
 Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Knee Cartilage Extraction and Bone-Cartilage Interface Analysis from 3D MRI Data Sets
 Knee Cartilage Extraction and Bone-Cartilage Interface Analysis from 3D MRI Data Sets José G. Tamez-Peña, Monica Barbu-McInnis and Saara Totterman VirtualScopics, 350 Linden Oaks, Rochester NY, 14625,
Knee Cartilage Extraction and Bone-Cartilage Interface Analysis from 3D MRI Data Sets José G. Tamez-Peña, Monica Barbu-McInnis and Saara Totterman VirtualScopics, 350 Linden Oaks, Rochester NY, 14625,
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
