Practical guide to joint and soft tissue injection techniques James Galloway MRCP and Marwan Bukhari PhD, FRCP
|
|
|
- Claud Gaines
- 5 years ago
- Views:
Transcription
1 Practical guide to joint and soft tissue injection techniques James Galloway MRCP and Marwan Bukhari PhD, FRCP Figure 1. The authors encourage a medial approach to injection of the knee joint; a combination of 40mg triamcinolone acetonide and 4ml lidocaine is recommended Musculoskeletal conditions account for a vast number of attendances in primary care. Treatment of these problems involves a number of therapeutic options, including intra-articular aspiration and injection. Joint injections were first attempted in the 1920s, using substances such as lactic acid or petroleum jelly. It was not until the early 1950s that intra-articular injections of steroids was introduced and shown to be helpful. 1,2 They are now the most frequently performed procedure in rheumatological practice. 3 Indications Joint injection The primary indication for joint injection is inflammatory arthritis 4 (eg rheumatoid arthritis, spondylarthropathies). Many patients will experience prolonged improvement up to six months from a single joint injection. The longerterm benefits of intra-articular steroids have been less well defined. There is limited evidence that supports their role in reducing synovial inflammation and destruction, and no evidence suggesting that they cause adverse effects on the joint when given in appropriate doses at not more than three or four times per year. 1,2 Osteoarthritis (OA) is a weaker indication for steroid injection a single trial has shown no benefit of intra-articular steroids over saline, although other studies have been more optimistic. 5 However, in practice, many rheumatologists use intra-articular steroids for OA with apparent success. Soft tissue injection There are many soft tissue injections that are regularly performed Steroid injections are a key tool in the management of musculoskeletal conditions and are now the most frequently performed procedure in rheumatological practice. Here, the authors illustrate the correct technique for administering these injections and highlight some of the points to consider. for the treatment of localised inflammation. These include trochanteric bursitis, flexor tenosynovitis, medial or lateral epicondylitis, and carpal tunnel syndrome. Joint aspiration The usual indication for joint aspiration is to evaluate an acutely swollen and inflamed ( hot ) joint. Synovial fluid analysis allows differentiation between crystal arthropathy and sepsis. There is also some evidence to support the routine aspiration of joints prior to steroid injection to improve efficacy. 6 Type of agent to use (see Table 1) Should lidocaine be mixed with the steroid? Many rheumatologists will mix some local anaesthetic with their steroid preparation for injection. Prescriber 19 October
2 Available Depo-Medrone Kenalog 40mg/ml 25mg/ml (1ml doses 40mg/ml Adcortyl 10mg/ml vials) (1, 2 or 3ml vials) (both available in available premixed 1ml vials) with lidocaine Advantages possibly causes possibly causes less associated soft less postinjection less postinjection tissue atrophy Disadvantages crystal precipitates shown to be less can form if mixed efficacious in with lidocaine joint injection Typical site/ dose knee 80mg 40mg shoulder 80mg 40mg subacromial 40mg 20mg bursa ankle 40mg 20mg soft tissue Table 1. Commonly used preparations for joint injections There have been several studies over the years that have not conclusively shown benefit of this practice. However, there are some theoretical reasons why it may be of benefit: Absolute sepsis within the joint or soft tissue prosthetic joints injection into a tendon Relative in the joint postinjection when performed previously active psoriatic lesions (or other skin disease) at the site of injection oral anticoagulation (although experienced injectors may proceed with caution) Table 2. Contraindications to joint injection Methylpred- Triamcinolone Hydrocortisone nisolone acetonide 25mg there may be a volume effect of the local anaesthetic on expanding the joint capsule in shoulder capsulitis and other large joints 7 anaesthetics may reduce postinjection anaesthetics may also prolong the duration of time the steroid remains within the joint by promoting vasoconstriction and thereby delaying clearance. What size needle should be used? Generally, the smallest needle possible should be used, which is normally a 25-gauge (blue) for most sites. A 22-gauge (green) is preferable for knee joints, or for when aspiration is expected to reveal viscous fluid. Hyaluronic acid Intra-articular hyaluronans are becoming an increasingly used treatment for OA. Hyaluronic acid is a large glycosaminoglycan that occurs naturally within the synovial fluid. Their use in veterinary practice to improve performance in arthritic joints dates back many years. In the USA they were first licensed for human use in 1997, using a regimen of three to five injections at weekly intervals. Following the publication of several randomised trials in the USA there was considerable hope for the use of these products. However, a more recent meta-analysis suggested only a small benefit over placebo perhaps more comparable to the use of NSAIDs. It also raised concerns over the likelihood of publication bias. In summary, because of its increased cost along with the inconvenience of requiring a series of three to five injections, it should be reserved for people in whom other treatment options have failed. Side-effects Side-effects of injecting steroids include skin atrophy at the site of injection, depigmentation and discoloration at the site. Postinjection is a wellreported phenomenon, which is due to steroid crystals forming within the joint. Infection is not common 8 and is estimated at between 1:2000 and 1: procedures. It can sometimes be difficult to differentiate infection and postinjection. Typically, postinjection starts and resolves within 48 hours, whereas infection develops after 48 hours and is associated with systemic features, eg fever, malaise. There is no real evidence to suggest joint injections predispose to Charcot s joints, although there are some anecdotal reports associated with more frequent injections. Systemic glucocorticoid effects have been seen only in patients 52 Prescriber 19 October
3 Injection technique Joint and soft tissue injections should be used in conditions that are clearly demarcated and well diagnosed and in which the injector is comfortable with the procedure. Some general guidance follows: exact location of the needle is not always necessary as even the more experienced injectors can obtain good response rates with periarticular injections 13 it is a clean, not sterile procedure; evidence suggests that, despite wide variation in precaution against sepsis, this is rare 8 anatomical landmarks are important and using them reduces the discomfort of scraping bone a drawing-up needle should be used that is separate from the injecting needle (no touch technique) hours rest is beneficial, especially in weight-bearing joints 15 they should be administered at a maximum of 3 a year as they tend to lose their efficacy over time in noninflammatory conditions receiving injections on a regular basis, ie every month. 9,10 Hypersensitivity to injected steroids can occur and is probably due to the diluent rather than the steroid itself. Common injection areas anatomical approach to specific injection sites Knee joint Painful knee effusions in patients with rheumatic disease are both common and disabling. Aspiration can relieve significant pressure and increase range of movement, while steroid instillation will often produce many months of symptom relief. We recommend using 40mg triamcinolone acetonide Figure 2. The glenohumeral joint is one of the most common sites for injection (Kenalog) combined with 4ml lidocaine. There are multiple approaches that are described for knee joint injection. We recommend a medial approach. Locating the insertion of the tendon of quadriceps femoris into the proximal patella, follow onethird of the way around the medial border of the patella and insert the needle 2cm below this parallel to the horizontal axis (see Figure 1). Shoulder Glenohumeral joint This is one of the commonest places for injection. Pathology in the glenohumeral joint tends to present as a global restriction in internal and external rotation. The classical example is adhesive capsulitis (frozen shoulder). The other main indication is rheumatoid or other inflammatory arthritides. Injecting the glenohumeral joint is easiest using the posterior approach. Tracing the spine of the scapula laterally to the acromial angle, the needle should be inserted approximately 2cm below this mark, pointing towards the coracoid process (see Figure 2). Use 4ml of 2 per cent lidocaine and 40mg triamcinolone acetonide. 54 Prescriber 19 October
4 Subacromial bursa (rotator cuff) Pain is often described over the lateral aspect of the upper arm (over the deltoid). Examination reveals a painful arc, with pain on resisted abduction. This can be due to the impingement syndrome, with inflammation in the subacromial bursa causing restriction of the supraspinatus tendon. It is important to remember that space is limited in the subacromial bursa, and not more than a total of 3ml can be injected. We recommend 1ml of lidocaine and 1ml of triamcinolone. The safest technique uses a lateral approach. The patient should relax their neck and shoulder muscles, sitting up with hands resting in their lap. The injection is placed approximately 2cm below the midpoint of the lateral edge of the acromion the gap between the inferior border of the acromion and the humeral head is usually palpable and is angled towards the opposite humeral head. Wrist We recommend the use of 2ml of lidocaine combined with 40mg of triamcinolone. Position the hand prone and locate the base of the second metacarpal bone. The joint space is palpable between the extensor of the index finger and the thumb abductor. Elbow (epicondylitis) Many patients presenting with elbow pain have inflammation not of the joint but of the periarticular structures. The most common site is the lateral epicondyle (known as tennis elbow ). The aetiology is repetitive wrist movements, resulting in rubbing of the extensor carpi radialis tendons over the lateral epicondyle. Classically (and anecdotally), it occurs in novice tennis players who use a tight grip Figure 3. Injection technique for lateral epicondylitis (tennis elbow) on the racket and have poor technique at backhand. Medial epicondylitis is often referred to as golfer s elbow, again due to presentation in people learning to play golf. There have been some case reports of this condition occurring with the use of fluoroquinolones, possibly through the same mechanism through which Achilles tendonitis occurs. Treatment should initially be with rest and analgesics but, if these fail to control symptoms, a corticosteroid injection is an efficacious option. 11 We recommend using 1ml of local anaesthetic and 25mg hydrocortisone (Hydrocortistab). Lateral epicondyle The patient should sit with the elbow flexed to 90 and, with the forearm supinated (palm upwards), the needle should then be inserted into the area over the epicondyle where there is maximal tenderness (see Figure 3). Medial epicondyle Laying the patient supine, the shoulder should be rotated externally to around 90 and the elbow flexed to 90. The injection is made slightly distal to the centre of the epicondyle. Trochanteric bursa Bursitis is one of the commonest causes of hip pain. Friction occurs between the bursae around the greater trochanter and both the tendon of gluteus medius (which inserts distally into the greater trochanter) and also the tensor fascia lata (running from the anterior superior iliac crest into the iliotibial tract, which in turn attaches to the lateral tibial condyle). The patient will often complain of difficulty walking and of being unable to sleep on the affected side. Examination is usually diagnostic and it is important to exclude underlying hip joint pathology. Initial therapy with analgesics and passive stretching exercises should be tried in the first instance. If these fail, then lidocaine and steroid injection are an effective option. 12 Placing the patient in the lateral decubitus position, with the hip flexed to 90 to allow identification of the superior aspect of the greater trochanter, the point of maximal tenderness should be identified and marked as the site for injection (see Figure 4). There is more than one bursa over the greater trochanter so the exact location of the pain may vary. Figure 4. Injection technique for trochanteric bursa; analgesics and stretching exercises should be tried in the first instance in cases of bursitis Prescriber 19 October
5 Other injections In patients in whom recurrent joint injections into typically large joints are needed more than three times a year, a yttrium 90 isotope injection can be used in specialist centres; alternatively osmium could be used. This is usually reserved for patients with mono- or oligoarthritis. Conclusion In the past many doctors have been reluctant to administer joint injections. This has been due to fears regarding adverse events based on old studies using much larger doses of steroids. More recent data now support the use of joint injections for many conditions, and the techniques involved are both safe and simple. This article aims to increase the knowledge and skills available to the general practitioner, therefore allowing more comprehensive management of rheumatic disease in primary care. Further reading Doherty M. Rheumatology examination and injection techniques. 2nd ed. London: WB Saunders, References 1. Hollander JL, Brown EM Jr, Jessar RA, et al. Hydrocortisone and cortisone injected into arthritic joints: comparative effect of and use of hydrocortisone as a local antiarthritic agent. J Am Med Assoc 1951;147: Ziff M, Scull E, Ford D, et al. Effects in rheumatoid arthritis of hydrocortisone and cortisone injected intra-articularly. AMA Arch Intern Med 1952;90: Bamji AN, Dieppe PA, Haslock DI, et al. What do rheumatologists do? A pilot audit study. Br J Rheumatol 1990;29: Gumpel JM. Intra-articular therapy. In: Scott JT, ed. Copeman s textbook of the rheumatic diseases. 6th ed. Churchill Livingstone, Jones A, Doherty M. Intra-articular corticosteroids are effective in osteoarthritis but there are no clinical predictors of response. Ann Rheum Dis 1996;55: Weitoft T, Uddenfeldt P. Importance of synovial fluid aspiration when injecting intra-articular corticosteroids. Ann Rheum Dis 2000;59: Mulcahy KA, Baxter AD, Oni OO, et al. The value of shoulder distension arthrography with intraarticular injection of steroid and local anaesthetic: a follow-up study. Br J Radiol 1994;67: Pal B, Morris J. Perceived risks of joint infection following intra-articular corticosteroid injections: a survey of rheumatologists. Clin Rheumatol 1999;18: Mader R, Lavi I, Luboshitzky R. Evaluation of the pituitary-adrenal axis function following single intraarticular injection of methylprednisolone. Arthritis Rheum 2005;52: Emkey RD, Lindsay R, Lyssy J, et al. The systemic effect of intraarticular administration of corticosteroid on markers of bone formation and bone resorption in patients with rheumatoid arthritis. Arthritis Rheum 1996;39: Smidt N, van der Windt DA, Assendelft WJ, et al. Corticosteroid injections, physiotherapy, or a wait-andsee policy for lateral epicondylitis: a randomised controlled trial. Lancet 2002;359: Shbeeb MI, O Duffy JD, Michet CJ Jr, et al. Evaluation of glucocorticosteroid injection for the treatment of trochanteric bursitis. J Rheumatol 1996;23: Jones A, Regan M, Ledingham J, et al. Importance of placement of intraarticular steroid injections. BMJ 1993;307: Charalambous CP, Tryfonidis M, Sadiq S, et al. Septic arthritis following intra-articular steroid injection of the knee a survey of current practice regarding antiseptic technique used during intra-articular steroid injection of the knee. Clin Rheumatol 2003;22: Chakravarty K, Pharaoh PD, Scott DG. A randomised controlled study of post injection rest following intra-articular steroid therapy for knee synovitis. Br J Rheumatol 1994;33: Dr Galloway is specialist registrar in rheumatology and Dr Bukhari is consultant rheumatologist in the Department of Rheumatology, University Hospitals of Morecambe Bay, Royal Lancaster Infirmary 56 Prescriber 19 October
Benefits of Aspiration and Injection JOINT INJECTIONS. Injection Indications. Mechanism of Action 1/11/2016
 Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
GP practical procedures Joint and soft tissue injections. Dr Monica Gupta Dr Hilary Wilson Dr John Hunter
 GP practical procedures Joint and soft tissue injections Dr Monica Gupta Dr Hilary Wilson Dr John Hunter Outline of talk Acute mono arthritis Pros & Cons of injections Regional problems Shoulder Knee Soft
GP practical procedures Joint and soft tissue injections Dr Monica Gupta Dr Hilary Wilson Dr John Hunter Outline of talk Acute mono arthritis Pros & Cons of injections Regional problems Shoulder Knee Soft
Introduction to Ultrasound Guided Shoulder Injections. Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital
 Introduction to Ultrasound Guided Shoulder Injections Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital Safe Robust Aim: to provide a service that is Cost effective To enable patients
Introduction to Ultrasound Guided Shoulder Injections Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital Safe Robust Aim: to provide a service that is Cost effective To enable patients
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES
 ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
Subacromial Bursa Injection
 Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Aspiration, Intra-articular and Soft Tissue Injections. MR KEWAL SINGH, MS(orth), FRCS(Eng)
 Aspiration, Intra-articular and Soft Tissue Injections MR KEWAL SINGH, MS(orth), FRCS(Eng) Indications for Aspiration Haemarthrosis Septic arthritis Symptomatic relief of a large effusion Crystal-induced
Aspiration, Intra-articular and Soft Tissue Injections MR KEWAL SINGH, MS(orth), FRCS(Eng) Indications for Aspiration Haemarthrosis Septic arthritis Symptomatic relief of a large effusion Crystal-induced
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop. W. Scott Black, MD Physician Assistant Studies Program University of Kentucky
 KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
Hands on - Steroid Injections. Jan Schulz, MD Associate professor of medicine McGill University
 Hands on - Steroid Injections Jan Schulz, MD Associate professor of medicine McGill University Disclosures Abbott Pharmaceuticals Amgen Roche Bristol-Myers Squibb Janssen Ortho Novartis Adult Rheumatology
Hands on - Steroid Injections Jan Schulz, MD Associate professor of medicine McGill University Disclosures Abbott Pharmaceuticals Amgen Roche Bristol-Myers Squibb Janssen Ortho Novartis Adult Rheumatology
Professor Lisa Stamp
 Professor Lisa Stamp Rheumatologist University of Otago, Christchurch 8:30-9:25 WS #65: Joint Injection Techniques 9:35-10:30 WS #75: Joint Injection Techniques (Repeated) Joint/soft tissue corticosteroid
Professor Lisa Stamp Rheumatologist University of Otago, Christchurch 8:30-9:25 WS #65: Joint Injection Techniques 9:35-10:30 WS #75: Joint Injection Techniques (Repeated) Joint/soft tissue corticosteroid
Workshop Hands on - Steroid Injections. Michael Stein MDCM, FRCP(C) Date: Nov
 Workshop Hands on - Steroid Injections Michael Stein MDCM, FRCP(C) Date: Nov 26 2018 Disclosure of Commercial Support This program has received no financial support Faculty/Presenter Disclosures I am a
Workshop Hands on - Steroid Injections Michael Stein MDCM, FRCP(C) Date: Nov 26 2018 Disclosure of Commercial Support This program has received no financial support Faculty/Presenter Disclosures I am a
Injections of the Joints & Soft Tissues. Matthew Kanaan DO, MS
 Injections of the Joints & Soft Tissues Matthew Kanaan DO, MS Outline / Goals! Injection basics (risks, contraindications, supplies )! Upper extremity Injections! HANDS ON - Simulated needle w/ marking
Injections of the Joints & Soft Tissues Matthew Kanaan DO, MS Outline / Goals! Injection basics (risks, contraindications, supplies )! Upper extremity Injections! HANDS ON - Simulated needle w/ marking
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review
 Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Live On Screen: Knee Injections ABCs of Musculoskeletal Care. Knee aspiration. Objectives. I have no disclosures.
 I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
Soft Tissue Rheumatism. Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group
 Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care. Jackson Orthopaedic Foundation
 ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care Jackson Orthopaedic Foundation Joint Injections in Primary Care Kathleen A. Geier, DNP, NP, ONC A.J. Benham, DNP, NP, ONC kgeier@jacksonortho.org
ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care Jackson Orthopaedic Foundation Joint Injections in Primary Care Kathleen A. Geier, DNP, NP, ONC A.J. Benham, DNP, NP, ONC kgeier@jacksonortho.org
In which arm muscle are intramuscular injections most often given? (not in text)
 AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
Rheumatology & Immunology. Regional pain syndromes to be covered today. Some definitions. Tendinitis. Bursitis. History. History. Exam.
 Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Connects arm to thorax 3 joints. Glenohumeral joint Acromioclavicular joint Sternoclavicular joint
 Connects arm to thorax 3 joints Glenohumeral joint Acromioclavicular joint Sternoclavicular joint Scapula Elevation Depression Protraction (abduction) Retraction (adduction) Downward Rotation Upward Rotation
Connects arm to thorax 3 joints Glenohumeral joint Acromioclavicular joint Sternoclavicular joint Scapula Elevation Depression Protraction (abduction) Retraction (adduction) Downward Rotation Upward Rotation
ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW
 PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
Anatomy and Physiology 2016
 Anatomy and Physiology 2016 O = Temporal line I = coronoid process (Mandible) A = elevates mandible (chewing) O = galea aponeurotica (layer of dense fibrous tissue which covers the upper part of the cranium)
Anatomy and Physiology 2016 O = Temporal line I = coronoid process (Mandible) A = elevates mandible (chewing) O = galea aponeurotica (layer of dense fibrous tissue which covers the upper part of the cranium)
9/25/2014. Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC. Disclosure: No Disclosures. Strategic Nurse Practitioner Solutions, LLC
 Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC 1 Dr. Ricki S. Loar, Ph.D., FNP-BC, GNP-BC Clinical Director, Be Well Partners in Health Nurse Practitioner, South Naperville Family Practice Faculty, Advanced Practice
Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC 1 Dr. Ricki S. Loar, Ph.D., FNP-BC, GNP-BC Clinical Director, Be Well Partners in Health Nurse Practitioner, South Naperville Family Practice Faculty, Advanced Practice
ORTHOPEDIC OFFICE INTERVENTIONS. Objectives of this discussion. Why me? By Steve Benz M.D.
 ORTHOPEDIC OFFICE INTERVENTIONS By Steve Benz M.D. Objectives of this discussion Learn about injections and castings that you can perform in your clinic setting. Learn about the agents that you can inject.
ORTHOPEDIC OFFICE INTERVENTIONS By Steve Benz M.D. Objectives of this discussion Learn about injections and castings that you can perform in your clinic setting. Learn about the agents that you can inject.
How to Do a Subacromial Shoulder Injection
 How to Do a Subacromial Shoulder Injection UCSF Primary Care Sports Medicine Conference 2018 Carlin Senter, MD Associate Professor Co-Director UCSF Sports Concussion Program Primary Care Sports Medicine
How to Do a Subacromial Shoulder Injection UCSF Primary Care Sports Medicine Conference 2018 Carlin Senter, MD Associate Professor Co-Director UCSF Sports Concussion Program Primary Care Sports Medicine
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
A guide to joint and soft ti s su e corti co s teroid injecti on. Pa rt 1: gen eral principles and the k n ee
 Me d i c i n etoday Pe e r R e v i e w e d Practical procedures A guide to joint and soft ti s su e corti co s teroid injecti on. Pa rt 1: gen eral principles and the k n ee ARVIN KUMAR DAMODARAN BSc,
Me d i c i n etoday Pe e r R e v i e w e d Practical procedures A guide to joint and soft ti s su e corti co s teroid injecti on. Pa rt 1: gen eral principles and the k n ee ARVIN KUMAR DAMODARAN BSc,
Musculoskeletal Ultrasound. Technical Guidelines SHOULDER
 Musculoskeletal Ultrasound Technical Guidelines SHOULDER 1 Although patient s positioning for shoulder US varies widely across different Countries and Institutions reflecting multifaceted opinions and
Musculoskeletal Ultrasound Technical Guidelines SHOULDER 1 Although patient s positioning for shoulder US varies widely across different Countries and Institutions reflecting multifaceted opinions and
MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow.
 MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow. Pectoralis Minor Supine, arm at side, elbows extended, supinated Head of Table
MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow. Pectoralis Minor Supine, arm at side, elbows extended, supinated Head of Table
Regional Pain. Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru
 Regional Pain Dr. B. G. Dharmanand M.D., D.M. (Rheumatology) Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru Dharmanand B.G. Regional Pain In Wagh S. (Ed). Rheumatology
Regional Pain Dr. B. G. Dharmanand M.D., D.M. (Rheumatology) Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru Dharmanand B.G. Regional Pain In Wagh S. (Ed). Rheumatology
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Electrode Placement. Skin Preparation. Frontalis (FRL) (Specific) Temporalis Anterior (TA) (Specific) Sternocleidomastoid (SCM) (Specific)
 Electrode Placement Skin Preparation 1) Removing the hair: Shave if necessary 2) Clean the skin: Use a towel or abrasive pad with conductive cleaning paste or alcohol to remove dead skin cells (high impedance)
Electrode Placement Skin Preparation 1) Removing the hair: Shave if necessary 2) Clean the skin: Use a towel or abrasive pad with conductive cleaning paste or alcohol to remove dead skin cells (high impedance)
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Joint Range of Motion Assessment Techniques. Presentation Created by Ken Baldwin, M.Ed Copyright
 Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Musculoskeletal corticosteroid use:
 Musculoskeletal corticosteroid use: Types, Indications, Contraindications, Equivalent doses, Frequency of use and Adverse effects. Dr Jide Olubaniyi MBBS, FRCR Dr Sean Crowther MB BCh, MRCS, FRCR Dr Sukhvinder
Musculoskeletal corticosteroid use: Types, Indications, Contraindications, Equivalent doses, Frequency of use and Adverse effects. Dr Jide Olubaniyi MBBS, FRCR Dr Sean Crowther MB BCh, MRCS, FRCR Dr Sukhvinder
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
1. The coordinated action of a scapular upward rotation and humeral abduction is known as the:
 1 1. The coordinated action of a scapular upward rotation and humeral abduction is known as the: a. Carrying angle of the arm b. Scapulohumeral rhythm c. Glenohumeral capsular pattern d. Abduction resistance
1 1. The coordinated action of a scapular upward rotation and humeral abduction is known as the: a. Carrying angle of the arm b. Scapulohumeral rhythm c. Glenohumeral capsular pattern d. Abduction resistance
Larry Rosenberger, CNP
 Larry Rosenberger, APRN CNP Julie Melendez, APRN CNP Larry Rosenberger, CNP Northwest Ohio Orthopedics and Sports Medicine Findlay, Ohio lrosenberger@nwoortho.com 419 233 2215 Julie Melendez, CNP Northwest
Larry Rosenberger, APRN CNP Julie Melendez, APRN CNP Larry Rosenberger, CNP Northwest Ohio Orthopedics and Sports Medicine Findlay, Ohio lrosenberger@nwoortho.com 419 233 2215 Julie Melendez, CNP Northwest
MSK INJECTION THERAPY
 MSK INJECTION THERAPY MATS 2017 AIMS and Objectives Brief overview of Injection therapy, assessment tips and advice Small group work in 3 rotating groups. Use models and GLOVES (please take a pair round
MSK INJECTION THERAPY MATS 2017 AIMS and Objectives Brief overview of Injection therapy, assessment tips and advice Small group work in 3 rotating groups. Use models and GLOVES (please take a pair round
Impingement syndrome. Clinical features. Management. Rotator cuff tear diagnosed. Go to rotator cuff tear
 Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Lab Activity 11: Group II
 Lab Activity 11: Group II Muscles Martini Chapter 11 Portland Community College BI 231 Origin and Insertion Origin: The place where the fixed end attaches to a bone, cartilage, or connective tissue. Insertion:
Lab Activity 11: Group II Muscles Martini Chapter 11 Portland Community College BI 231 Origin and Insertion Origin: The place where the fixed end attaches to a bone, cartilage, or connective tissue. Insertion:
Radiographic Positioning Summary (Basic Projections RAD 222)
 Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Anatomy and Physiology II. Review Shoulder Girdle New Material Upper Extremities - Bones
 Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Kinesiology Tape. Table of contents:
 1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
Management of Chronic Elbow Pain
 Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy
 The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy Learning Objectives When to use an acute rheumatology service Appropriate use of steroids by condition Injection or Oral or Intramuscular
The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy Learning Objectives When to use an acute rheumatology service Appropriate use of steroids by condition Injection or Oral or Intramuscular
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Upper limb injuries II. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
The Articular System OBJECTIVES ACTIVITIES. A. Completion
 C H A P T E R 8 The Articular System OBJECTIVES After studying this chapter, you should be able to: 1. Name and describe the three types of joints. 2. Name the two types of synarthroses joints. 3. Name
C H A P T E R 8 The Articular System OBJECTIVES After studying this chapter, you should be able to: 1. Name and describe the three types of joints. 2. Name the two types of synarthroses joints. 3. Name
Outline. Knee Anatomy. Physical Exam Skills and Office Procedures in Orthopaedics. The quadriceps muscles extend the knee 7/23/2013
 Physical Exam Skills and Office Procedures in Orthopaedics Outline Knee exam Knee aspiration and injection Shoulder exam Subacromial bursa injection UCSF Essentials of Primary Care August 14, 2012 Carlin
Physical Exam Skills and Office Procedures in Orthopaedics Outline Knee exam Knee aspiration and injection Shoulder exam Subacromial bursa injection UCSF Essentials of Primary Care August 14, 2012 Carlin
Goniometry. Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm)
 Goniometry Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm) Wrist Extension: Pt seated with forearm resting on table (Goniometer
Goniometry Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm) Wrist Extension: Pt seated with forearm resting on table (Goniometer
In-Depth Foundations: Anatomy Terms to Know
 Be familiar with / able to identify and define all the following parts. The Spine Cranium Vertebrae Cervical, Thoracic, Lumbar Sacrum Coccyx Bones of Upper Body Cranium Mastoid process; Occipital condyle,
Be familiar with / able to identify and define all the following parts. The Spine Cranium Vertebrae Cervical, Thoracic, Lumbar Sacrum Coccyx Bones of Upper Body Cranium Mastoid process; Occipital condyle,
8 1 Basic Principles. Palpating Muscle Bellies. Palpating Bony Prominences
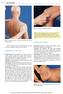 8 1 Basic Principles Fig. 1.4 Locating the medial epicondyle. Tip: The shape of bony prominences can be visualized by looking at their morphology. However, variations are expected to be encountered quite
8 1 Basic Principles Fig. 1.4 Locating the medial epicondyle. Tip: The shape of bony prominences can be visualized by looking at their morphology. However, variations are expected to be encountered quite
Practical 2 Worksheet
 Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
The Upper Limb II. Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa
 The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
Hands PA; Obl. Lat.; Norgaard s Thumb AP; Lat. PA. PA; Lat.: Obls.; Elongated PA with ulnar deviation
 Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
Bio 113 Anatomy and Physiology The Muscles. Muscles of the Head and Neck. Masseter. Orbicularis occuli. Orbicularis oris. Sternocleidomastoid
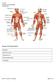 Bio 113 Anatomy and Physiology The Muscles Muscles of the Head and Neck Masseter Orbicularis occuli Orbicularis oris Sternocleidomastoid Temporalis BIO 113 Fall 2011 Muscles Page 1 of 5 Muscles of the
Bio 113 Anatomy and Physiology The Muscles Muscles of the Head and Neck Masseter Orbicularis occuli Orbicularis oris Sternocleidomastoid Temporalis BIO 113 Fall 2011 Muscles Page 1 of 5 Muscles of the
Musculoskeletal Examination
 Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity
 Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity Sheldon C. Yao, D.O. Acting Department Chair March 1, 2013 Clinical significance Upper extremity
Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity Sheldon C. Yao, D.O. Acting Department Chair March 1, 2013 Clinical significance Upper extremity
JOINT INJECTIONS AJ DURFEE PA-C CHRIS MAYBERRY PA-C
 JOINT INJECTIONS AJ DURFEE PA-C Worked with sports group in San Diego for 7 ½ years Worked for Kaiser Orthopedics since 2011 I grew up in San Diego CHRIS MAYBERRY PA-C 1 XAVIER VALDEZ Grew up in Texas
JOINT INJECTIONS AJ DURFEE PA-C Worked with sports group in San Diego for 7 ½ years Worked for Kaiser Orthopedics since 2011 I grew up in San Diego CHRIS MAYBERRY PA-C 1 XAVIER VALDEZ Grew up in Texas
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
Musculoskeletal Referral Guidelines
 Musculoskeletal Referral Guidelines Introduction These guidelines have been developed to provide an integrated musculoskeletal service. They are based on reasonable clinical practice and will initially
Musculoskeletal Referral Guidelines Introduction These guidelines have been developed to provide an integrated musculoskeletal service. They are based on reasonable clinical practice and will initially
Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate medication into the exact site of th
 The Art of the Injection By Jon C. Brillhart PA-C Daivd Lannik MD Portsmouth Orthopedics, Inc Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate
The Art of the Injection By Jon C. Brillhart PA-C Daivd Lannik MD Portsmouth Orthopedics, Inc Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate
Joint Injection Workshop ACP Scientific Meeting February 28, Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD
 Joint Injection Workshop ACP Scientific Meeting February 28, 2015 Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD Workshop Schedule 1:00 1:15 A Practical Approach to the Shoulder Exam 1:15 1:40
Joint Injection Workshop ACP Scientific Meeting February 28, 2015 Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD Workshop Schedule 1:00 1:15 A Practical Approach to the Shoulder Exam 1:15 1:40
Arthritis and Rheumatology Clinics of Kansas Patient Education
 Arthritis and Rheumatology Clinics of Kansas Patient Education Regional Pain Syndromes Introduction: At some time in the course of life, virtually everyone will experience pain in a tendon, muscle, or
Arthritis and Rheumatology Clinics of Kansas Patient Education Regional Pain Syndromes Introduction: At some time in the course of life, virtually everyone will experience pain in a tendon, muscle, or
Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists
 Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Key Points for Success:
 SELF WRIST & HAND 1 2 All of the stretches described in this chapter are detailed to stretch the right side. Key Points for Success: Sit comfortably in a position where you can straighten or fully extend
SELF WRIST & HAND 1 2 All of the stretches described in this chapter are detailed to stretch the right side. Key Points for Success: Sit comfortably in a position where you can straighten or fully extend
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D.
 Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Structure and Function of the Bones and Joints of the Shoulder Girdle
 Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Spondyloarthritis Physical Exam Measures. Axial SpA Measures. Ear Anatomy (Wikipedia) 5/4/2018. Tragus to Wall and Occiput to Wall Measurement
 AxSpA Measures in Clinical Trials Spondyloarthritis Physical Exam Measures Philip Mease MD, MACR Director, Rheumatology Research, Swedish-Providence-St. Joseph Health Systems Clinical Professor, University
AxSpA Measures in Clinical Trials Spondyloarthritis Physical Exam Measures Philip Mease MD, MACR Director, Rheumatology Research, Swedish-Providence-St. Joseph Health Systems Clinical Professor, University
Office Knee Injections
 CME Workshop Office Knee Injections Step By Step Prem Sequeira, MD, CCFP Presented at Family Medicine Potpourri, Memorial University of Newfoundland Corticosteroid injections can give dramatic and long-lasting
CME Workshop Office Knee Injections Step By Step Prem Sequeira, MD, CCFP Presented at Family Medicine Potpourri, Memorial University of Newfoundland Corticosteroid injections can give dramatic and long-lasting
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain. Plamen Todorov
 Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Dupuytrens contracture
 OA Wrist Ganglion/Cysts Dupuytrens contracture Carpal Tunnel Syndrome Carpal Tunnel pathway For advice on management of CTS please follow link to Map of Medicine Trigger Finger Trigger finger pathway For
OA Wrist Ganglion/Cysts Dupuytrens contracture Carpal Tunnel Syndrome Carpal Tunnel pathway For advice on management of CTS please follow link to Map of Medicine Trigger Finger Trigger finger pathway For
Joints Dr. Ali Ebneshahidi
 Joints Dr. Ali Ebneshahidi Function of Joints 1. Serve as functional junctions between bones. 2. Bind bones, strokes, and other related tissues together. 3. Allow bone growth to occur. 4. Permit certain
Joints Dr. Ali Ebneshahidi Function of Joints 1. Serve as functional junctions between bones. 2. Bind bones, strokes, and other related tissues together. 3. Allow bone growth to occur. 4. Permit certain
Muscular Nomenclature and Kinesiology - One
 Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
The examination of the painful knee. Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University
 The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
Trauma & Orthopaedic Undergraduate Syllabus
 Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
11/15/2018. Temporalis Elevates & retracts mandible. Masseter = Prime mover of jaw closure. Levator scapulae Supraspinatus Clavicle.
 Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
EPICONDYLITIS, LATERAL (Tennis Elbow)
 EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
Ultrasound in Rheumatology
 Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
The Elbow and the cubital fossa. Prof Oluwadiya Kehinde
 The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
The Appendicular Skeleton
 8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
Gross Anatomy Questions That Should be Answerable After October 27, 2017
 Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center
 Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
Philip Bayliss St Albans Osteopathy
 Philip Bayliss St Albans Osteopathy 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Subacromial (Shoulder) Bursitis 1 Experts estimate that 65% of people
Philip Bayliss St Albans Osteopathy 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Subacromial (Shoulder) Bursitis 1 Experts estimate that 65% of people
Due in Lab weeks because of Thanksgiving Prelab #10. Homework #8. Both sides! Both sides!
 Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Main Menu. Joint and Pelvic Girdle click here. The Power is in Your Hands
 1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be difficult Bony abnormalities less common than li
 SPORTS MEDICINE CASES A quick tour of some local joints Featuring gco common o and unusual problems SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be
SPORTS MEDICINE CASES A quick tour of some local joints Featuring gco common o and unusual problems SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
