DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS
|
|
|
- Tamsin Young
- 5 years ago
- Views:
Transcription
1 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS INTRDUCTION In the last lecture we discussed the difference between restrictive and obstructive lung diseases. As we said obstructive diseases are four: emphysema, chronic bronchitis, asthma and bronchiectasis. Emphysema is already discussed, so we will talk about chronic bronchitis and bronchiectasis in this handout and we will cover bronchial asthma in the next lecture. Reference: Robbins,10 th : pages CHRONIC BRONCHITIS: Chronic bronchitis is defined as: the presence of a persistent productive cough for at least 3 consecutive months in at least 2 consecutive years, in the absence of other identifiable causes. Productive cough means: cough associated with sputum.( if there is no sputum with cough we call it dry cough) So: diagnosis of chronic bronchitis is based on clinical criteria ( remember that emphysema diagnosis is based on morphological features) OVERVIEW: Chronic bronchitis is an itis! Which means it is inflammation. With chronic cycles of inflammation, fibrosis occurs, and this causes thickness of the wall and narrowing of the lumen. Also: remember that there is productive cough, so there is increased mucous production in these patients. The increased mucous is caused by increased goblet cells in the respiratory epithelium and, more importantly, by increased submucosal mucous secreting glands. The disease is called chronic bronchitis, so large bronchi are affected at first, but with time smaller airways (bronchioles) will be affected. 1
2 PATHOGENESIS: Chronic bronchitis, like emphysema is caused mainly by smoking. That s why these two diseases co-exist in the same patient, although their pathogenesis is different (but they share the same etiology). Heavy air pollution can also cause chronic bronchitis. In chronic bronchitis there are two main changes, both are caused by smoking: 1. Mucus hypersecretion. The earliest feature of chronic bronchitis is hypersecretion of mucus in the large airways, associated with hypertrophy of the submucosal glands in the trachea and bronchi. The basis for mucus hypersecretion is incompletely understood, but it appears to involve inflammatory mediators such as histamine and IL-13. With time, there is also a marked increase in goblet cells in small airways small bronchi and bronchioles leading to excessive mucus production that contributes to airway obstruction. It is thought that both the submucosal gland hypertrophy and the increase in goblet cells are protective reactions against tobacco smoke or other pollutants (e.g., sulfur dioxide and nitrogen dioxide). Note that smoking also interferes with the ciliary action of the respiratory epithelium, preventing the clearance of mucus and increasing the risk of infection. 2. Inflammation. Inhalants that induce chronic bronchitis cause cellular damage, eliciting both acute and chronic inflammatory responses involving neutrophils, lymphocytes, and macrophages. Long-standing inflammation and accompanying fibrosis involving small airways (small bronchi and bronchioles, less than 2 to 3 mm in diameter) can also lead to chronic airway obstruction. In the early stages of the disease, the productive cough causes mucoid sputum, but airflow is not obstructed (because large airways are affected and even narrowed, they are large enough for the inhalation and exhalation. 2
3 VERY IMPORTANT: Obstructive features in chronic bronchitis occur later in the disease and are not caused by inflammation and destruction of large airways, rather it is the result of: 1. Small airway disease chronic bronchiolitis) which needs time to develop and is induced by: a. Goblet cell metaplasia with mucous plugging of the bronchiolar lumen, b. Inflammation, c. Bronchiolar wall fibrosis, 2. Coexistent emphysema MORPHOLOGY Grossly, there is hyperemia, swelling, and edema of the mucous membranes accompanied by excessive mucinous or mucopurulent secretions The characteristic microscopic features are 1. Mild chronic inflammation of the airways (predominantly lymphocytes) 2. Enlargement ( hypertrophy and hyperplasia) of the mucus-secreting glands of the trachea and bronchi. 3. Increased numbers of goblet cells, 3
4 The increase in mucous secreting glands can be assessed by the ratio of the thickness of the mucous gland layer to the thickness of the wall between the epithelium and the cartilage (Reid index). The Reid index (normally 0.4) is increased in chronic bronchitis, usually in proportion to the severity and duration of the disease. In the pic below Reids index is calculated as bc/ ad: The bronchial epithelium may exhibit squamous metaplasia and dysplasia. The bronchial walls are fibrotic and this fibrosis along with the inflammation, is the main cause of the narrowing, see below: 4
5 CLINICAL FEATURES - In patients with chronic bronchitis, a prominent cough and the production of sputum may persist indefinitely without ventilatory dysfunction - Some patients develop significant COPD with outflow obstruction. This results in hypercapnia, hypoxemia, and (in severe cases) cyanosis (hence the term "blue bloaters" that describes patients with pure chronic bronchitis). Hypercapnea: due to expiratory obstruction causing CO2 retention Hypoxemia: due to ventilation/perfusion mismatch that happens due to increased cardiac output. So why patients with chronic bronchitis are cyanotic and those with emphysema are not?? In emphysema, the expiratory effort ( the puff! In pink puffers) can overcome the functional obstruction keeping oxygen and carbon dioxide level normal or near normal, whereas in chronic bronchitis the obstruction is structural and cannot be corrected, so it causes cyanosis. Please note that these two diseases coexist and that s why we lump them in one entity ( COPD) so it is rare to see a classic case of pink puffer or blue bloater. Patients present with a spectrum of changes related to these two diseases. Complications of chronic bronchitis: -Pneumonia and recurrent respiratory infections -Respiratory failure -Right sided cardiac failure: cor pulmonale = cardiac failure secondary to lung disease ( discussed below) -Bronchiectasis. 5
6 Cor Pulmonale Definition: right ventricular hypertrophy and dilation caused by pulmonary hypertension due to primary lung disorders. This can result in right sided heart failure. Note: right sided heart failure can be caused by left ventricular failure or congenital heart disease. These are more common causes of right heart failure than cor pulmonale. Pulmonary hypertension: is high blood pressure in the pulmonary vessels. The pathogenesis involves narrowing of blood vessels within the lungs. This makes it harder for the heart to pump blood through the lungs. Over time, the affected blood vessels become fibrotic which makes them stiffer and thicker. This further increases the blood pressure within the lungs and impairs their blood flow. These changes cause increased workload for the right side of the heart. The right heart operates normally under low pressure so it cannot cope with higher pressures, and although right ventricular adaptations (hypertrophy and increased contractility of the heart muscle) initially help to preserve stroke volume, ultimately these mechanisms fail. Any lung disease that causes hypoxia will cause pulmonary hypertension. This is because hypoxia causes constriction of the pulmonary arteries. This is called hypoxic pulmonary vasoconstriction and it is a protective mechanism that aims to stop too much blood flowing to areas of the lung that are damaged and do not contain oxygen. When the alveolar hypoxia is severe and prolonged, this vasoconstriction occurs across a large portion of the pulmonary vascular bed and leads to an increase in pulmonary arterial pressure, with thickening of the pulmonary vessel walls contributing to the development of sustained pulmonary hypertension. Causes of cor pulmonale: 1. Acute respiratory distress syndrome 2. Pulmonary embolism 3. COPD 4. Primary pulmonary hypertension 5. Interstitial lung diseases 6. Cystic fibrosis 7. Sarcoidosis 8. Pulmonary arteritis 9. Bronchiectasis Please do not memorize these as a list!!! It is obvious that any lung disease which results in hypoxia will cause cor pulmonale. Please note that ARDS and pulmonary emboli are acute events, so they cause an acute form of right sided failure whereas the rest of the causes are chronic and will result in chronic cardiac failure. 6
7 BRONCHECTASIS Bronchiectasis is not a primary disease; it is complication of several diseases. It is defined as permanent dilation of bronchi and bronchioles caused by destruction of the muscle and the elastic tissue, resulting from or associated with chronic necrotizing infections. Note from the definition that the dilatation is in the bronchi and bronchioles, whereas in emphysema the dilation is in the alveoli. Bronchiectasis is secondary to persisting infection and obstruction caused by a variety of conditions that include 1. Bronchial obstruction, common causes of this obstruction are : a- Tumors, foreign bodies, and impaction of mucus. - With these conditions, the bronchiectasis is localized to the obstructed lung segment. b- mucous plugging like in atopic asthma and chronic bronchitis 2. Necrotizing, or suppurative, pneumonia, particularly with Staphylococcus aureus or Klebsiella spp., may predispose affected patients to development of bronchiectasis. Note: Post-tuberculosis bronchiectasis continues to be a significant cause of morbidity in endemic areas. PREDISPOSING FACTORS Several diseases increase the risk of developing bronchiectasis including: 1. Cystic fibrosis, the patients have thick mucous which is difficult to get rid of. This causes obstruction. 2. intralobar sequestration of the lung, this is a congenital anomaly where there are abnormal lung segments. Their presence increases risk of infections. 3. immunodeficiency states, 4. primary ciliary dyskinesia and Kartagener syndromes. Here there is abnormal motility of cilia which increases risk of infection PATHOGENESIS Two processes are crucial in pathogenesis: obstruction and chronic infection and either of these may come first. If the patient has obstruction (due to bronchitis or asthma, or tumor..) the obstruction will affect the normal clearance mechanisms,so secondary infection soon follows and the combination of obstruction and infection will cause destruction of the bronchial walls. With 7
8 time this destruction causes dilation due to the weakness of the bronchial walls by the repeated infection and The alternative scenario occurs when the patient s story starts with chronic infection. Here, the infection, over time causes damage to; bronchial walls, leading to weakening and dilation. MORPHOLOGY Bronchiectasis usually affects the lower lobes bilaterally, - When caused by tumors or foreign bodies the involvement may be localized to a single segment and the most severe involvement is in the more distal bronchi and bronchiole - The airways may be dilated to as much as four times their usual diameter and on gross examination of the lung the bronchican be followed almost to the pleural surfaces. By contrast, in normal lungs, the bronchioles cannot be followed by ordinary gross examination beyond a point 2 to 3 cm from the pleural surfaces Clinical Features Bronchiectasis causes severe, persistent cough; expectoration of foul smelling, sometimes bloody sputum; dyspnea and hemoptysis, which may be massive. Symptoms are often episodic and are precipitated by upper respiratory tract infections or the introduction of new pathogenic agents. 8
9 Paroxysms of cough are particularly frequent when the patient rises in the morning, as the change in position causes collections of pus and secretions to drain into the bronchi. Obstructive respiratory insufficiency can lead to marked dyspnea and cyanosis. Due to current treatment with better antibiotics and physical therapy, outcome has improved considerably and life expectancy has almost doubled. Complications like cor pulmonale, brain abscesses, and amyloidosis are less frequent complications than in the past. I hope you know why bronchiectasis causes amyloidosis! If you remember, chronic inflammation increases SAA (serum amyloid associated) protein which can accumulate and cause secondary amyloidosis. Clubbing of the fingers may develop in bronchiectasis. And it occurs in several neoplastic and non neoplastic lung disease. Finger clubbing: Clubbing is diagnosed clinically when you observe Loss of the normal <165 angle (Lovibond angle) between the nailbed and the fold (cuticula). Clubbing is a deformity of the finger or toe nails associated with several diseases within the respiratory system and other systems. Most important lung diseases causing clubbing : 1. Lung cancer, mainly non-small-cell cell carcinoma 2. Interstitial lung disease 3. Complicated tuberculosis 4. Suppurative lung disease: lung abscess, empyema, bronchiectasis, cystic fibrosis 5. Mesothelioma of the pleura 6. Arteriovenous fistula or malformation 9
10 The exact cause for clubbing is unknown, it is thought that vasodilation, secretion of growth factors (e.g., platelet-derived growth factor and hepatocyte growth factor) from the lungs have a role in the pathogenesis of clubbing. It is also suggested that overproduction of PGE2 by other tissues may be the causative factor for clubbing NOTE: CLUBBNG IS AN IMPORTANT TOPIC IN YOUR CLINICAL YEARS, MAKE SURE YOU ARE FAMILIA WITH IT!!! THANK YOY 10
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Diseases of the respiratory system/ summary for mid material Dr Heyam Awad FRCPath
 Diseases of the respiratory system/ summary for mid material 2017 Dr Heyam Awad FRCPath notes I have 15 theory questions in the final. 4-5 of which will be from the mid material.. Study the mid material
Diseases of the respiratory system/ summary for mid material 2017 Dr Heyam Awad FRCPath notes I have 15 theory questions in the final. 4-5 of which will be from the mid material.. Study the mid material
Obstructive Lung Diseases. By: Shefaa Qa qa
 Obstructive Lung Diseases By: Shefaa Qa qa Obstructive lung diseases (or airway diseases) are characterized by an increase in resistance to airflow due to partial or complete obstruction at any level from
Obstructive Lung Diseases By: Shefaa Qa qa Obstructive lung diseases (or airway diseases) are characterized by an increase in resistance to airflow due to partial or complete obstruction at any level from
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
How does COPD really work?
 How does COPD really work? by Alex Goodell View online Where does COPD fit in the mix of respiratory diseases? I ve made a map of the major pathologies outlined in Robbins and First Aid (obviously these
How does COPD really work? by Alex Goodell View online Where does COPD fit in the mix of respiratory diseases? I ve made a map of the major pathologies outlined in Robbins and First Aid (obviously these
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
The Respiratory System
 The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA
 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Respiratory diseases in Ostrołęka County
 Respiratory diseases in Ostrołęka County 4400 persons underwent examination 950 persons were given referrals to more detailed investigation 600 persons were examined so far The results of more detailed
Respiratory diseases in Ostrołęka County 4400 persons underwent examination 950 persons were given referrals to more detailed investigation 600 persons were examined so far The results of more detailed
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
PATHOPHYSIOLOGY OF RESPIRATION 2
 PATHOPHYSIOLOGY OF RESPIRATION 2 Obstructive disorders R. Benacka Department of Pathophysiology, Medical faculty, P.J. Safarik University Košice Respiratory diseases Obstructive diseases (OPD) - restricted
PATHOPHYSIOLOGY OF RESPIRATION 2 Obstructive disorders R. Benacka Department of Pathophysiology, Medical faculty, P.J. Safarik University Košice Respiratory diseases Obstructive diseases (OPD) - restricted
Respiratory Pathophysiology
 Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
Respiratory Medicine
 Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Exam 2 Respiratory Disorders
 Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
COPD: Change in Definition. COPD Pathology with 3D Interactive. COPD: Definitions of 21st Century 1. COPD Includes Chronic Bronchitis 2
 COPD: Change in Definition COPD Pathology with 3D Interactive by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org COPD used to include 5 disease processes 1 1 Chronic Bronchitis 2 Emphysema
COPD: Change in Definition COPD Pathology with 3D Interactive by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org COPD used to include 5 disease processes 1 1 Chronic Bronchitis 2 Emphysema
Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)*
 Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)* ORHAN MUREN, M.D. Associate Professor of Medicine and Anesthesiology, Medical College of Virginia, Health Sciences Division
Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)* ORHAN MUREN, M.D. Associate Professor of Medicine and Anesthesiology, Medical College of Virginia, Health Sciences Division
Slide 120, Lobar Pneumonia. Slide 120, Lobar Pneumonia. Slide 172, Interstitial Pneumonia. Slide 172, Interstitial Pneumonia. 53 Year-Old Smoker
 Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Anatomy. The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs.
 Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Restrictive lung diseases
 Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
SCPA502-Respiratory Pathology
 Problem Mr. B is 57 years old, high 157 cm and weight 76 kg. He has worked as the dump truck driver in the coal mine since 1980, and also smoked cigarette 1 pack/day more than 30 years. What are the risk
Problem Mr. B is 57 years old, high 157 cm and weight 76 kg. He has worked as the dump truck driver in the coal mine since 1980, and also smoked cigarette 1 pack/day more than 30 years. What are the risk
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease COPD Gábor Smuk M.D. COPD FEV1 Chronic bronchitis inflammatory thickening of the wall and intermittent luminal plugging or chronic obstructive bronchiolitis inflammatory
Chronic obstructive pulmonary disease COPD Gábor Smuk M.D. COPD FEV1 Chronic bronchitis inflammatory thickening of the wall and intermittent luminal plugging or chronic obstructive bronchiolitis inflammatory
Bronchiectasis: An Imaging Approach
 Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Pulmonary Diseases. We Move A Lot of Air. Basic Categories. Alveolar Level. Developmental
 Pulmonary Diseases We Move A Lot of Air Alveolar Level Functions Oxygenation CO 2 & ph Basic defenses Nose hairs Cilia Mucus Cough reflex Immune system Basic Categories Congenital Infectious Neoplastic
Pulmonary Diseases We Move A Lot of Air Alveolar Level Functions Oxygenation CO 2 & ph Basic defenses Nose hairs Cilia Mucus Cough reflex Immune system Basic Categories Congenital Infectious Neoplastic
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Vascular Lung Diseases
 Vascular Lung Diseases SESSION SPECIFIC OBJECTIVES List the major types of vascular lung disease Recognize and describe the pathology of vascular lung disease: Pulmonary embolism, thrombosis, hypertension,
Vascular Lung Diseases SESSION SPECIFIC OBJECTIVES List the major types of vascular lung disease Recognize and describe the pathology of vascular lung disease: Pulmonary embolism, thrombosis, hypertension,
Pulmo-Park Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D
 Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
PATHOLOGY OF RESPIRATORY SYSTEM
 PATHOLOGY OF RESPIRATORY SYSTEM Upper respiratory tract Lower respiratory tract Nose Lung Pharynx (Throat) - Bronchi Larynx - Bronchiole Trachea - Alveoli PEERAYUT SITTHICHAIYAKUL, M.D. CONTENT Upper respiratory
PATHOLOGY OF RESPIRATORY SYSTEM Upper respiratory tract Lower respiratory tract Nose Lung Pharynx (Throat) - Bronchi Larynx - Bronchiole Trachea - Alveoli PEERAYUT SITTHICHAIYAKUL, M.D. CONTENT Upper respiratory
RESPIRATORY EMERGENCIES. Michael Waters MD April 2004
 RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
PULMONARY ARTERIES IN CHRONIC LUNG DISEASE
 Brit. Heart J., 1963, 25, 583. RIGHT VENTRICULAR HYPERTROPHY AND THE SMALL PULMONARY ARTERIES IN CHRONIC LUNG DISEASE BY W. R. L. JAMES AND A. J. THOMAS From Llandough Hospital (United Cardiff Hospitals)
Brit. Heart J., 1963, 25, 583. RIGHT VENTRICULAR HYPERTROPHY AND THE SMALL PULMONARY ARTERIES IN CHRONIC LUNG DISEASE BY W. R. L. JAMES AND A. J. THOMAS From Llandough Hospital (United Cardiff Hospitals)
Respiratory System. Organization of the Respiratory System
 Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
PATHOLOGY OF RESPIRATORY SYSTEM
 PATHOLOGY OF RESPIRATORY SYSTEM PEERAYUT SITTHICHAIYAKUL, M.D. Upper respiratory tract Nose Pharynx (Throat) Larynx Trachea Lower respiratory tract Lung - Bronchi - Bronchiole - Alveoli 1 CONTENT Upper
PATHOLOGY OF RESPIRATORY SYSTEM PEERAYUT SITTHICHAIYAKUL, M.D. Upper respiratory tract Nose Pharynx (Throat) Larynx Trachea Lower respiratory tract Lung - Bronchi - Bronchiole - Alveoli 1 CONTENT Upper
Respiratory Toxicology
 Respiratory Toxicology Loch-Caruso ENVIRON 310 2017 1 Breathing Oxygen Carbon Dioxide http://www.webmd.com/lung/picture-of-the-lungs Loch-Caruso ENVIRON 310 2017 2 Breathing Enlarged view of the airways,
Respiratory Toxicology Loch-Caruso ENVIRON 310 2017 1 Breathing Oxygen Carbon Dioxide http://www.webmd.com/lung/picture-of-the-lungs Loch-Caruso ENVIRON 310 2017 2 Breathing Enlarged view of the airways,
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Chronic Obstructive Pulmonary Disease
 136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
Diseases of the Lung and Respiratory Tract, Part I. William Bligh-Glover M.D. Department of Anatomy, CWRU
 Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
PomPom SHOOTER. Activity Background: Common Obstructive Lung Disorders:
 CAUTION: Students with asthma or other respiratory problems should NOT perform the breathing exercises in this activity because they involve repeated maximal inhalations and exhalations and use of a breathing
CAUTION: Students with asthma or other respiratory problems should NOT perform the breathing exercises in this activity because they involve repeated maximal inhalations and exhalations and use of a breathing
HASPI Medical Anatomy & Physiology 14b Lab Activity
 HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Tuesday, December 13, 16. Respiratory System
 Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Notes to complete gas exchange in mammals
 Notes to complete gas exchange in mammals Mass flow of air to respiratory surface this is achieved through the mechanics of ventilation (breathing). This ensures a regular supply of air into and out of
Notes to complete gas exchange in mammals Mass flow of air to respiratory surface this is achieved through the mechanics of ventilation (breathing). This ensures a regular supply of air into and out of
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Pathology of Pneumonia
 Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Respiratory System. December 20, 2011
 Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Key Difference - Pleural Effusion vs Pneumonia
 Difference Between Pleural Effusion and Pneumonia www.differencebetween.com Key Difference - Pleural Effusion vs Pneumonia Pleural effusion and pneumonia are two conditions that affect our respiratory
Difference Between Pleural Effusion and Pneumonia www.differencebetween.com Key Difference - Pleural Effusion vs Pneumonia Pleural effusion and pneumonia are two conditions that affect our respiratory
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Chapter 13 Respiration & Excretion
 Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
The development of chronic obstructive pulmonary
 THE PATHOGENESIS AND PATHOLOGY OF COPD: IDENTIFYING RISK FACTORS AND IMPROVING MORBIDITY AND MORTALITY * Paul D. Scanlon, MD ABSTRACT Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory
THE PATHOGENESIS AND PATHOLOGY OF COPD: IDENTIFYING RISK FACTORS AND IMPROVING MORBIDITY AND MORTALITY * Paul D. Scanlon, MD ABSTRACT Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
COPD COPD. C - Chronic O - Obstructive P - Pulmonary D - Disease OBJECTIVES
 COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
7/12/2012. Respiratory system. Respiratory Response to Toxic Injury (Lung) Ninth Industrial Toxicology and Pathology Short Course.
 Ninth Industrial Toxicology and Pathology Short Course 23 27 July, 2012 Contemporary Concepts in Target Organ Toxicologic Pathology Respiratory system Respiratory Response to Toxic Injury (Lung) Eric Wheeldon
Ninth Industrial Toxicology and Pathology Short Course 23 27 July, 2012 Contemporary Concepts in Target Organ Toxicologic Pathology Respiratory system Respiratory Response to Toxic Injury (Lung) Eric Wheeldon
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
The Respiratory System
 The Respiratory System Cells continually use O2 & release CO2 Respiratory system designed for gas exchange Cardiovascular system transports gases in blood Failure of either system rapid cell death from
The Respiratory System Cells continually use O2 & release CO2 Respiratory system designed for gas exchange Cardiovascular system transports gases in blood Failure of either system rapid cell death from
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Biochemistry of Lungs. Lecture # 35 Lecturer: Alexander Koval
 Biochemistry of Lungs Lecture # 35 Lecturer: Alexander Koval Introduction Biochemistry of lungs Overview of substances produced (surfactant, mucus, collagen), inactivated (ROS, kinins, serotonin, catecholamines)
Biochemistry of Lungs Lecture # 35 Lecturer: Alexander Koval Introduction Biochemistry of lungs Overview of substances produced (surfactant, mucus, collagen), inactivated (ROS, kinins, serotonin, catecholamines)
Histopathology: pulmonary pathology
 Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
Group B: Directed self-study Group C: Anatomy lab. Lecture: Structure and function of larynx. Lecture: Dead space & compliance of lungs
 Timetable Week 1 (1 st January 2018) Theme: Structure and functions of the lungs Group A: Anatomy lab Group C: Histology lab Upper Group B: Anatomy lab Group C: Anatomy lab Group A: Histology lab Upper
Timetable Week 1 (1 st January 2018) Theme: Structure and functions of the lungs Group A: Anatomy lab Group C: Histology lab Upper Group B: Anatomy lab Group C: Anatomy lab Group A: Histology lab Upper
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
The Circulatory System
 The Circulatory System Single-celled organisms do not need a circulatory system. They are in direct contact with their environment, so transport of materials occurs by diffusion and osmosis. Larger organisms
The Circulatory System Single-celled organisms do not need a circulatory system. They are in direct contact with their environment, so transport of materials occurs by diffusion and osmosis. Larger organisms
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
Organs of the Respiratory System Laboratory Exercise 52
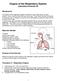 Organs of the Respiratory System Laboratory Exercise 52 Background The organs of the respiratory system include the nose, nasal cavity, sinuses, pharynx, larynx, trachea, bronchial tree, and lungs. They
Organs of the Respiratory System Laboratory Exercise 52 Background The organs of the respiratory system include the nose, nasal cavity, sinuses, pharynx, larynx, trachea, bronchial tree, and lungs. They
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
COPD Management in LTC: Presented By: Jessica Denney RRT
 COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
Lec #2 histology. Bronchioles:
 Lec #2 histology. Last lecture we talked about the upper respiratory tract histology, this one is about the lower part histology. We will discuss the histology of: -bronchioles -respiratory bronchioles
Lec #2 histology. Last lecture we talked about the upper respiratory tract histology, this one is about the lower part histology. We will discuss the histology of: -bronchioles -respiratory bronchioles
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
CASE REPORTS. Inflammatory Polyp of the Bronchus. V. K. Saini, M.S., and P. L. Wahi, M.D.
 CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
Chapter Effects of Smoke on the Respiratory System Part 2 pages
 Chapter 18.1 Effects of Smoke on the Respiratory System Part 2 pages 417-419 Hemoglobin has 4 separate protein chains. Each protein chain has a single iron atom (Fe 3+ ). Each iron atom can bind to a single
Chapter 18.1 Effects of Smoke on the Respiratory System Part 2 pages 417-419 Hemoglobin has 4 separate protein chains. Each protein chain has a single iron atom (Fe 3+ ). Each iron atom can bind to a single
The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body.
 Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Session Guidelines. This is a 15 minute webinar session for CNC physicians and staff
 Respiratory Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars monthly to address topics related to risk adjustment documentation and coding
Respiratory Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars monthly to address topics related to risk adjustment documentation and coding
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
