Effect of Influenza Virus Infection in a Murine Model of Asthma
|
|
|
- Nickolas Walters
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Iran J Allergy Asthma Immunol August 2015; 14(4): Effect of Influenza Virus Infection in a Murine Model of Asthma Hwan Soo Kim, Huisu Lee, Hyun Sook Kim, Sulmui Won, Eu Kyoung Lee, Kyongwon Bang, Yoon Hong Chun, Jong-seo Yoon, Hyun Hee Kim, and Jin Tack Kim Department of Pediatrics, College of Medicine, The Catholic University of Korea, Seoul, Republic of Korea Received: 20 October 2014; Received in revised form: 9 December 2014; Accepted: 17 December 2014 ABSTRACT Respiratory virus infection is a major cause of asthma exacerbation. However, the underlying mechanisms of this exacerbation are unknown. Therefore, to determine the mechanisms, we examined the effect of influenza infection in a murine model of asthma. Mice were divided into four groups: the phosphate-buffered saline (PBS), house dust mite (HDM), influenza, and HDM/influenza groups. The influenza group and the HDM/influenza group were infected with influenza A virus. We measured airway resistance (Penh value), examined the lung tissue for pathology, and analyzed the cells and cytokines in bronchoalveolar lavage fluid (BALF) by ELISA. At 50 mg/ml methacholine, the HDM/influenza group showed a significantly higher Penh value than the PBS, HDM, and influenza groups. The number of neutrophils in BALF was higher in the HDM/influenza group than in the HDM group. A significantly greater number of lymphocytes and macrophages were detected in the HDM/influenza group than in the HDM group. IFN-γ and IL-1β levels were higher in the HDM/influenza group than in the HDM group. IL-5 levels did not vary between the HDM and HDM/influenza groups, IL-10 was significantly lower in the HDM/influenza than in the HDM group. Chemokine (C-X-C motif) ligand 1 (CXCL1) and regulated upon activation, normal T cell expressed and secreted (RANTES) were higher in the HDM/influenza group than in the HDM group. In a murine model of asthma, influenza-induced airway inflammation appeared to be caused by simultaneous activation of neutrophilic and eosinophilic inflammation. Keywords: Asthma; Cytokine; Eosinophil; Histology; Influenza; Mouse; Neutrophil INTRODUCTION Asthma exacerbations are associated with shortness of breath, coughing, wheezing, and chest tightness, and are accompanied by decreased expiratory airflow manifested by a reduction in peak expiratory flow. Corresponding Author: Jong-seo Yoon, MD, PhD, Department of Pediatrics, Seoul St. Mary s Hospital, College of Medicine, The Catholic University of Korea, 222 Banpo-daero, Asthma exacerbations are related to several factors, including allergen exposure, air pollution, and stress; however, the major cause of exacerbation is respiratory virus infection. 1 Much of our knowledge regarding the mechanisms of virus-induced asthma exacerbations is derived from Seocho-gu, Seoul , Republic of Korea. Tel: (+82 2) ; Fax: (+82 2) , pedjsyoon@catholic.ac.kr Copyright Summer 2015, Iran J Allergy Asthma Immunol. All rights reserved. 392
2 Influenza Virus in a Murine Model of Asthma of experimental respiratory virus infection in asthmatic volunteers as a model of exacerbation. 2 Despite the abundant epidemiologic evidence linking respiratory virus infection to asthma exacerbation, the cellular and molecular mechanisms by which these viruses cause exacerbations are not yet known. In a previous experimental study using animal models of asthma, cytokine release by airway epithelial cells after viral infection led to an influx of inflammatory cells. These inflammatory cells release products, such as neutrophil elastase and reactive oxygen species that can cause tissue damage, stimulate mucus production, and further stimulate cytokine production. 3 Most of these experimental studies used rhinovirus (RV). However, the pathophysiological changes that occur following infection differ according to virus type. For example, influenza typically causes extensive epithelial necrosis, whereas RV causes only patchy damage of epithelial cells. 4 In this study, we aimed to determine the effect of influenza infection in a murine model of asthma, and we assessed airway resistance, lung tissue pathology, and the changes in bronchoalveolar lavage fluid (BALF) cells and cytokines (IFN-γ, IL-1β, IL-5, IL-10, CXCL1, and RANTES) to investigate the mechanism of acute asthma exacerbation induced by influenza virus infection. We compared our results to those in previous studies of influenza and other respiratory viruses. MATERIALS AND METHODS Test Animal Groups For comparison, the test animals were divided into four groups, the phosphate buffered saline (PBS) group, house dust mite (HDM)-exposed group, influenza group, and a group of HDM-exposed mice infected with influenza virus (HDM/influenza). A total of six experiments with 5 8 mice per group were performed. Sensitization and Allergen Challenge BALB/c mice aged 6 8 weeks (Orient Bio INC, Gyeonggi-do, Korea) were sensitized and challenged with Dermatophagoides farinae crude extract (D. farinae; Arthropods of Medical Importance Resource Bank, Seoul, Korea) or PBS. For sensitization, mice in the HDM and HDM/influenza groups were injected intraperitoneally with 200 μl of a 2-mg/mL solution of aluminum potassium sulfate and 250 μg of a crude extract of D. farinae or PBS on day 0 and day 14. For the challenge, mice were administered 50 μg of a crude extract of D. farinae (0.25 mg/ml) intranasally in 50 μl of PBS on days 14, 15, and 16. The mice were treated with a mixture of aluminum hydroxide (alum) and D. farinae crude extract to enhance the immunogenicity of the allergen. We used PBS as a control in all procedures. Successful induction of the mouse asthma model was assessed by determining the total number of cells and eosinophils in BALF and examining lung histopathology. All experimental animal protocols were reviewed by the Committee for Ethics on Animal Experiments of the Catholic University. Viruses and Infection of Mice The mouse-adapted influenza A (H1N1) virus was provided by the Korea Bank for Pathogenic viruses (Seoul, Korea) and propagated in monolayer cultures of HeLa cells. On day 17, the influenza A (IA) virus was administered intranasally at a concentration of fifty percent tissue culture infectivity doses (TCID 50 )/μl; the TCID 50 was determined by the Spearman-Karber method. The mice were euthanized, and samples were collected on day 18 (post-infection day 1) (Figure 1). Measurement of Airway Hyper-responsiveness We measured airway responsiveness to methacholine in all four groups of mice. For the HDM/influenza group, we measured airway responsiveness 24 hours after IA virus infection. Airway responsiveness was measured using four different concentrations of methacholine (0 mg/ml, 12.5 mg/ml, 25 mg/ml, and 50 mg/ml) using an OCP3000 instrument (Allmedicus, Anyang, Korea). Methacholine was administered over a period of 3 minutes using an Ultra-Neb ultrasonic nebulizer (3650p; Pulmo-Aide LT Lompressor, Somerset, PA, USA). The enhanced pause (Penh value) variable was measured over a period of 3 minutes. Bronchoalveolar Lavage (BAL) Procedure BALF was collected 24 hours after IA virus infection. The BAL was performed by inserting a 22- gauge needle into the trachea. Then, the trachea was ligated and the entire lung was lavaged by instilling 1 ml of PBS. The BALF was harvested once Vol. 14, No. 4, August 2015 Iran J Allergy Asthma Immunol, Summer 2015/393
3 H.S. Kim, et al. Figure 1. Study design: Dermatophagoides farinae (Df)- sensitized mice were immunized with Df and aluminum adjuvant by intraperitoneal injection (IP) once on days 0 and 14. Two weeks later, these mice were inoculated intranasally (IN) once daily with Df for 3 consecutive days (days 14 to 16). Df- sensitized mice were infected with influenza A virus (IA virus) 24 hours after the final Df inoculation. Penh values and cytokine levels in bronchoalveolar lavage (BAL) fluid were measured 24 hours after IA virus infection. IT, intratracheally. IP, intraperitoneal; IT, intratracheal; IN, intranasal. and centrifuged at 387 g (2000 rpm) for 10 minutes at 4 C. Supernatants were stored at -70 C. Assessment of Cells in the BALF Cell precipitates were suspended in 0.4 ml of PBS, and a 10-μL aliquot was mixed with 10 μl of trypan blue solution (Gibco, Grand Island, NY, USA). The total number of cells in each sample was counted using a hemocytometer. Slides were prepared using a cytocentrifuge (Cytospin 2; Shandon, Runcorn, UK) and stained with Diff-Quick (Sysmex Corporation, Kobe, Japan). Macrophages, eosinophils, lymphocytes, and neutrophils (500 minimum) were counted at 400 magnification. Measurement of Cytokines and Chemokines in the BALF and Lung Homogenate Interferon (IFN)-γ, interleukin (IL)-1β, IL-5, IL-10, chemokine (C-X-C motif) ligand 1 (CXCL1), and regulated upon activation normal T cell expressed and secreted (RANTES) concentrations in the supernatant of the BALF were determined using an enzyme linked immunosorbent assay (ELISA) kit (R&D systems, Inc., Minneapolis, MN, USA), according to the manufacturer s protocol. Histopathology We conducted a histopathological analysis of the lung sections of mice in the four groups 24 hours after the final D. farinae challenge. Once the washing was complete, the lungs were immediately removed. The removed lung tissues were fixed in 4% paraformaldehyde (Wako pure chemical industries, Ltd., Osaka, Japan) for 24 hours and then embedded in paraffin. The fixed tissues were cut into 5-μm-thick sections and were stained with hematoxylin and eosin (H&E). The sections were observed by light microscopy to evaluate the degree of airway inflammation. Pathological changes were described using a previously described system with some modification. 5,6 The degree of peribronchial and perivascular inflammation was evaluated on a subjective scale of 0 to 3. A value of 0 was assigned when no inflammation was detected, a value of 1 was assigned for occasional cuffing with inflammatory cells, a value of 2 was assigned for most bronchi or vessels surrounded by a thin layer (1 5 cells) of inflammatory cells, and a value of 3 was assigned when most bronchi or vessels were surrounded by a thick layer (>5 cells) of inflammatory cells. Statistical Analysis All results are shown as mean ± standard error of the mean (SEM). The data were analyzed with the Kruskal-Wallis test for comparing continuous nonparametric variables in 3 groups or more and the Mann- Whitney test for comparing continuous non-parametric variables in 2 groups. Statistical significance was assessed by using SPSS v (SPSS Inc., Chicago, IL, USA). P values less than 0.05 were considered statistically significant. RESULTS Increased Airway Resistance We measured the Penh value using four different concentrations of methacholine. At 50 mg/ml methacholine, the HDM group showed a higher Penh value than the PBS group (p= 0.045). At 50 mg/ml methacholine, the HDM/influenza group showed a significantly higher Penh value than the other three groups (PBS, HDM, and influenza, p < 0.05; Figure 2). 394/ Iran J Allergy Asthma Immunol, Summer 2015 Vol. 14, No. 4, August 2015
4 Influenza Virus in a Murine Model of Asthma Analysis of the Inflammatory Cells in BALF The HDM/influenza group had a significantly higher number of eosinophils than the PBS and influenza groups (p< and p< 0.001). The HDM/influenza group had more neutrophils than the PBS group (p= 0.003). The HDM/influenza group had a significantly higher number of lymphocytes than the PBS, HDM, and influenza groups (p< 0.001, p= 0.003, and p= 0.001, respectively). The HDM/influenza group had more macrophages than the control and HDM groups (p< and p= 0.003, respectively; Figure 3). Cytokine and Chemokine Secretion upon Airway Inflammation We measured the levels of cytokines and chemokines in the four groups of mice using ELISA. Levels of the cytokines IFN-γ, and IL-1β were significantly higher in the HDM, influenza, and HDM/influenza groups than in the PBS group (p< 0.05). The Th2 inflammation cytokine, IL-5, was higher in the HDM/influenza group than in the PBS group (p= 0.005) and was also higher in the HDM/influenza group than in the influenza group (p= 0.042). The regulatory T- cell-related cytokine, IL-10, was lower in the HDM/influenza group than in the HDM group (p= 0.007). The neutrophil-related chemokine CXCL1 was higher in the HDM/influenza group than in the HDM group (p< 0.001), and the eosinophil-related chemokine RANTES was higher in the HDM/influenza group than in the PBS group (p= 0.012, Figure 4). Histological Analysis of Lungs Compared to the PBS group, there were histological changes in the bronchial wall, lung parenchyma, interstitium, and the pulmonary vasculature in the HDM, influenza, and HDM/influenza groups (Figure 5). There were no pathologic changes in the H&Estained lung sections from the PBS group. Compared to the PBS group, the HDM/influenza group showed greater inflammatory cell infiltration, interstitial inflammation, and thickening of the alveolar wall. Figure 2. Airway responsiveness determined by measurement of Penh (n=6 mice per group). First bar in each group is at 0 mg/ml concentration of methacholine, second bar in each group is 12.5 mg/ml concentration of methacholine, third bar in each group is 25 mg/ml concentration of methacholine, and fourth bar in each group is 50 mg/ml concentration of methacholine. Vol. 14, No. 4, August 2015 Iran J Allergy Asthma Immunol, Summer 2015/395
5 H.S. Kim, et al. Figure 3. Differential cell counts of neutrophils and eosinophilslymophocyte, and macrophage in bronchialveolar lavage fluid (n=6 mice per group). Compared to the influenza group, the HDM/influenza group showed denudation, dense infiltration of inflammatory cells in the bronchial lining epithelium, and a higher grade of vascular congestion and interstitial widening. Compared to the HDM group, in the HDM/influenza group, a higher grade of multifocal infiltration of various cells, such as lymphocytes, macrophages, plasma cells, and eosinophils was observed in the interstitium. Thus, the HDM/influenza group showed the most severe grade of inflammation. The HDM/influenza group also had higher eosinophil and neutrophil counts and more prominent neutrophil infiltration than the HDM and influenza groups. The peribronchial inflammatory scores of the HDM, influenza, and HDM/influenza groups were higher than that of the PBS group. When each group was scored according to the level of eosinophil and neutrophil infiltration, the HDM/influenza group showed proportionally higher neutrophil infiltration than eosinophil infiltration (Table 1). Table 1. Histological scoring of peribronchial inflammation at day 18 (n = 6 mice per group). Variables PBS HDM Influenza HDM/influenza P value Cellular ± ± ± Infiltration Eosinophil ± ± Infiltration Neutrophil Infiltration ± ± Data are expressed as mean ± standard error of the mean. 396/ Iran J Allergy Asthma Immunol, Summer 2015 Vol. 14, No. 4, August 2015
6 Influenza Virus in a Murine Model of Asthma Figure 4. Concentrations of cytokines and chemokines in BALF (n=6 mice per group), IFN: interferon, IL: interleukin, ELISA: enzyme linked immunosorbant assay, CXCL: chemokine ligand, RANTES: regulated upon activation, normal T cell expressed and secreted, BALF: bronchoalveolar lavage fluid. The perivascular inflammatory scores of the HDM, influenza, and HDM/influenza groups were higher than that of the control (PBS) group. When each group was scored according to the level of eosinophil and neutrophil infiltration, in the HDM/influenza group, neutrophil infiltration was higher than eosinophil infiltration (Table 2). Table 2. Histological scoring of perivascular inflammation at day 18 (n = 6 mice per group). Variables PBS HDM Influenza HDM/influenza P value Cellular infiltration Eosinophil infiltration Neutrophil infiltration Data are expressed as mean ± standard error of the mean ± ± ± ± ± ± ± Vol. 14, No. 4, August 2015 Iran J Allergy Asthma Immunol, Summer 2015/397
7 H.S. Kim, et al. Figure 5. Histopathological changes in lungs of 4 groups. (H&E staining of lung sections; original magnification 400 ) HDM/influenza group showed the most severe grade of inflammation compared to the HDM group and the influenza group. The HDM/influenza group also had higher eosinophil and neutrophil counts, together with prominent neutrophil infiltration compared to the HDM group and the influenza group. DISCUSSION In this study, we aimed to investigate the effect of influenza infection in a murine model of asthma, and we analyzed airway resistance, lung tissue pathology, and the changes in the cells and cytokines in BALF to determine the mechanism underlying these effects. We found that the mechanism underlying the pathogenic effect of influenza infection in a murine model of asthma includes simultaneous activation of neutrophilic and eosinophilic inflammation. Several animal models of asthma have been developed to understand the pathogenesis of asthma. The two most commonly used mouse models of asthma are the OVA model of asthma and the HDM model of asthma. 7 In the mouse model of OVA-induced asthma, active sensitization is achieved either by concurrent administration of Al(OH)3 as an adjuvant or via repetitive exposure to low doses of ovalbumin. 7 The use of adjuvant has been reported to induce a mast cellindependent form of airway inflammation in the mouse model of asthma, led mostly by a strong lymphocytedriven induced Th2 inflammation and eosinophilia. 7 Models not using an adjuvant, such as Al(OH)3, are reportedly dependent on the presence of mast cells for the development of airway inflammation. 7 However, the shortfall of the OVA mouse model of asthma is the use of a nonantigenic protein, and the development of an artificial immune response to this protein via the use of adjuvant. Therefore, we used the HDM model of asthma, which uses a natural antigenic protein. Latest studies report that administration of HDM extract once a day for 10 days causes an asthmatic response characterized by increased IgE, airway and parenchymal eosinophilia, a Th2 cytokine response, as well as the development of an increased response to methacholine as a measure of airway hyperresponsiveness. 8 These characteristics indicate that mast cells are likely to play a major role in the development of the asthma-like response in this disease. 7 Ever since viruses have been implicated as a cause of asthma exacerbation, many studies have attempted to investigate the mechanism of asthma exacerbation caused by viral infection, with conflicting results. Regarding airway resistance, we found that at 50 mg/ml methacholine, the HDM/influenza group showed a significantly higher Penh value than the PBS, HDM, and influenza groups. This finding shows that influenza infection aggravates airway inflammation in a murine model of asthma. This result was similar to that of a previous study in which mice infected with influenza A and exposed to HDM during infancy exhibited marked functional impairment as measured by significant increases in airway resistance. 9,10 However, in a recent study, effect of influenza infection on airway resistance differed on age. 10 RV infection has also been shown to increase maximal airway responses to methacholine in normal human subjects. 11,12 In our study, we found that the number of inflammatory cells retrieved from BALF was significantly higher in the HDM/influenza group than in the HDM group. Neutrophils were increased in the HDM/influenza group compared with the number in the HDM group. Lymphocytes and macrophages were significantly higher in the HDM/influenza group than in the HDM group. These findings were similar to those of a previous study, which reported a significant increase in the total number of cells retrieved in the 398/ Iran J Allergy Asthma Immunol, Summer 2015 Vol. 14, No. 4, August 2015
8 Influenza Virus in a Murine Model of Asthma BALF of influenza-treated mice, and early innate immune responses marked by significant increases in neutrophils, macrophages, and other monocytic cells. 10 The adaptive immune response was characterized by marked increases in lymphocytes and eosinophils. 13 Regarding cytokine and chemokine secretion, we measured IFN-γ, IL-1β, IL-5, IL-10, CXCL1, and RANTES. The innate immunity cytokines, IFN-γ and IL-1β, are known to have antiviral activity, IL-5 acts as a proinflammatory cytokine, reflecting Th2 inflammation. IL-10 is a regulatory cytokine with anti-allergic effects, CXCL1 shows neutrophil activation, and RANTES has eosinophil activation activity. We found that IFN-γ and IL-1β levels were higher in HDM/influenza group than in the HDM group as a result of influenza infection. IL-5 and IL-10, which are related to Th2 inflammation, showed mixed results. Even though IL-5 showed no significant difference between the HDM group and the HDM/influenza group, IL-10 was significantly lower in the HDM/influenza group than in the HDM group. We postulated that influenza infection can stimulate Th2 inflammation. This also supports findings from a previous study in which IL-4, a Th2 cytokine, was increased in the lung but was not increased in the spleens after influenza infection in a mouse model of asthma. 14 Likewise, CXCL1 and RANTES levels were higher in the HDM/influenza group than in the HDM group. Therefore, we concluded that influenza infection stimulates both neutrophil and eosinophil activation. A previous study of experimental RV infection 15 reported increased levels of IL-8 and IL-1β in nasal lavage samples from asthmatic patients compared to the levels in samples from control subjects. However, another study 12 reported no differences in IL-6, IL-8, IL-11, and granulocytemonocyte-colony stimulating factor (GM-CSF) levels in nasal lavage and sputum samples from asthma patients and control subjects. In another study of RV infection, increased production of various proinflammatory substances, including IL-1α, IL-1β, IL-6, IL-8, IL-11, TNF-α, RANTES, and GM-CSF, was detected in primary cultures of epithelial cells or established cell lines Based on clinical studies, influenza infection induced the NF-κB-mediated release of cytokines, including IL-1β, IL-6, and IL-8, from human tracheal epithelial cells. 20,21 Increases in cytokines and monokines, including IL-6, IL-8, and RANTES, were also observed in the sera of patients infected with influenza virus. 22 Wang et al. demonstrated that influenza virus infection increased the vascular endothelial permeability of mouse lungs by increasing the levels of IL-1β, IL-6, TNF-α, and trypsin. 23 Our results were quite similar to those in previous studies of both RV and influenza infection. The peribronchial inflammatory scores of the HDM, influenza, and HDM/influenza groups were higher than that of the PBS group. When each group was scored according to the level of eosinophil and neutrophil infiltration, the HDM/influenza group showed proportionally higher neutrophil infiltration than eosinophil infiltration (Table 1). The perivascular inflammatory scores of the HDM, influenza, and HDM/influenza groups were higher than those of the control group. When each group was scored according to the level of eosinophil and neutrophil infiltration, in the HDM/influenza group, neutrophil infiltration was higher than eosinophil infiltration. To the best of our knowledge, our study is the first to apply a scoring system to assess the effect of viral infection in a murine model of asthma. We found that influenza virus infection-induced endothelial cell damage may be involved in the mucosal edema associated with airway inflammation due to neutrophil and eosinophil infiltration. This finding is similar to those of previous studies, which have shown that the production of proinflammatory cytokines and mediators and the production of inflammatory substances, such as ECP, in cells other than epithelial cells may also be related to airway hyper-responsiveness in asthma patients infected with respiratory viruses. 24 In conclusion, influenza infection may influence asthma via several mechanisms, including airway inflammation, mucus hypersecretion, and bronchial hyper-responsiveness. The pathogenic mechanism of influenza-induced airway inflammation in this murine model of asthma may be a result of simultaneous activation of neutrophilic and eosinophilic inflammation. In addition to the development of vaccines and anti-viral drugs for the treatment of influenza virus infection, the most effective methods for the treatment and prevention of influenza-induced asthma exacerbation should inhibit all of the abovementioned contributing factors. Vol. 14, No. 4, August 2015 Iran J Allergy Asthma Immunol, Summer 2015/399
9 H.S. Kim, et al. ACKNOWLEDGEMENTS The authors wish to acknowledge the financial support of the Catholic Medical Center Research Foundation during the 2013 program year. REFERENCES 1. Mallia P, Johnston SL. How viral infections cause exacerbation of airway diseases. Chest 2006; 130(4): Corne JM, Marshall C, Smith S, Schreiber J, Sanderson G, Holgate ST, et al. Frequency, severity, and duration of rhinovirus infections in asthmatic and nonasthmatic individuals: a longitudinal cohort study. Lancet 2002; 359(9309): Wark PA, Johnston SL, Bucchieri F, Powell R, Puddicombe S, Laza-Stanca V, et al. Asthmatic bronchial epithelial cells have a deficient innate immune response to infection with rhinovirus. J Exp Med 2005; 201(6): Arruda E, Boyle TR, Winther B, Pevear DC, Gwaltney JM Jr, Hayden FG. Localization of human rhinovirus replication in the upper respiratory tract by in situ hybridization. J Infect Dis 1995; 171(5): Curtis JL, Byrd PK, Warnock ML, Kaltreider HB. Requirement of CD4-positive T cells for cellular recruitment to the lungs of mice in response to a particulate intratracheal antigen. J Clin Invest 1991; 88(4): Li J, Liu Z, Wu Y, Wu H, Ran P. Chitosan microparticles loaded with mite group 2 allergen Der f 2 alleviate asthma in mice. J Investig Allergol Clin Immunol 2008; 18(6): Gold M, Marsolais D, Blanchet MR. Mouse models of allergic asthma. In: Hughes MR, McNagny KM. Mast cells: methods and protocols. USA: Springer Science & Business Media, 2015: Cates EC, Fattouh R, Wattie J, Inman MD, Goncharova S, Coyle AJ, et al. Intranasal exposure of mice to house dust mite elicits allergic airway infl ammation via a GM- CSF-mediated mechanism. J Immunol 2004; 173(10): Al-Garawi A, Fattouh R, Botelho F, Walker TD, Goncharova S, Moore CL, et al. Influenza A facilitates sensitization to house dust mite in infant mice leading to an asthma phenotype in adulthood. Mucosal Immunol 2011; 4(6): Birmingham JM, Gillespie VL, Srivastava K, Li XM, Busse PJ. Influenza A infection enhances antigen-induced airway inflammation and hyperresponsiveness in young but not aged mice. Clin Exp Allergy 2014; 44(9): de Kluijver J, Grunberg K, Sont JK, Hoogeveen M, van Schadewijk WA, de Klerk EP, et al. Rhinovirus infection in nonasthmatic subjects: effects on intrapulmonary airways. Eur Respir J 2002; 20(2): Fleming H, Little F, Schnurr D, Avila P, Wong H, Liu J, et al. Rhinovirus-16 colds in healthy and in asthmatic subjects: similar changes in upper and lower airways. Am J Respir Crit Care Med 1999; 160(1): Buchweitz JP, Harkema JR, Kaminski NE. Timedependent airway epithelial and inflammatory cell responses induced by influenza virus A/PR/8/34 in C57BL/6 mice. Toxicol Pathol 2007; 35(3): Chirkova T, Petukhova G, Korenkov D, Naikhin A, Rudenko L. Immunization with live influenza viruses in an experimental model of allergic bronchial asthma: infection and vaccination. Influenza Other Respir Viruses 2008; 2(5): de Kluijver J, Grunberg K, Pons D, de Klerke EP, Dick CR, Sterke PJ, et al. Interleukin-1 beta and interleukin-1ra levels in nasal lavages during experimental rhinovirus infection in asthmatic and non-asthmatic subjects. Clin Exp Allergy 2003; 33(10): Subauste MC, Jacoby DB, Richards SM, Proud D. Infection of a human respiratory epithelial cell line with rhinovirus. Induction of cytokine release and modulation of susceptibility to infection by cytokine exposure. J Clin Invest 1995; 96(1): Zhu Z, Tang W, Ray A, Wu Y, Einarsson O, Landry ML, et al. Rhinovirus stimulation of interleukin-6 in vivo and in vitro: evidence for nuclear factor κb-dependent transcriptional activation. J Clin Invest 1996; 97(2): Terajima M, Yamaya M, Sekizawa K, Okinaga S, Suzuki T, Yamada N, et al. Rhinovirus infection of primary cultures of human tracheal epithelium: role of ICAM-1 and IL-1β. Am J Physiol 1997; 273(4 Pt 1):L Yamaya M, Sekizawa K, Suzuki T, Yamada N, Furukawa M, Ishizuka S, et al. Infection of human respiratory submucosal glands with rhinovirus: effects on cytokine and ICAM-1 production. Am J Physiol 1999; 277(4):L Yamaya M, Shinya K, Hatachi Y, Kubo H, Asada M, Yasuda H, et al. Clarithromycin inhibits type A seasonal influenza virus infection in human airway epithelial cells. J Pharmacol Exp Ther 2010; 333(1): / Iran J Allergy Asthma Immunol, Summer 2015 Vol. 14, No. 4, August 2015
10 Influenza Virus in a Murine Model of Asthma 21. Yamaya M, Nishimura H, Shinya K, Hatachi Y, Sasaki T, Yasuda H, et al. Inhibitory effects of carbocisteine on type A seasonal influenza virus infection in human airway epithelial cells. Am J Physiol Lung Cell Mol Physiol 2010; 299(2):L Deng R, Lu M, Korteweg C, Gao Z, McNutt MA, Ye J, et al. Distinctly different expression of cytokines and chemokines in the lungs of two H5N1 avian influenza patients. J Pathol 2008; 216(3): Wang S, Le TQ, Kurihara N, Chida J, Cisse Y, Yano M, et al. Influenza virus cytokine-protease cycle in the pathogenesis of vascular hyperpermeability in severe influenza. J Infect Dis 2010; 202(7): Yamaya M. Virus Infection-Induced Bronchial Asthma Exacerbation. Pulm Med 2012; 2012:1-14. Vol. 14, No. 4, August 2015 Iran J Allergy Asthma Immunol, Summer 2015/401
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Review Article Virus Infection-Induced Bronchial Asthma Exacerbation
 Pulmonary Medicine Volume 212, Article ID 834826, 14 pages doi:1.1155/212/834826 Review Article Virus Infection-Induced Bronchial Asthma Exacerbation Mutsuo Yamaya Department of Advanced Preventive, Medicine
Pulmonary Medicine Volume 212, Article ID 834826, 14 pages doi:1.1155/212/834826 Review Article Virus Infection-Induced Bronchial Asthma Exacerbation Mutsuo Yamaya Department of Advanced Preventive, Medicine
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Alveolar macrophages modulate allergic inflammation in a murine model of asthma
 EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
The effect of an experimental rhinovirus 16 infection on bronchial lavage neutrophils
 The effect of an experimental rhinovirus 16 infection on bronchial lavage neutrophils Nizar N. Jarjour, MD, James E. Gern, MD, Elizabeth A. B. Kelly, PhD, Cheri A. Swenson, BS, Claire R. Dick, BS, and
The effect of an experimental rhinovirus 16 infection on bronchial lavage neutrophils Nizar N. Jarjour, MD, James E. Gern, MD, Elizabeth A. B. Kelly, PhD, Cheri A. Swenson, BS, Claire R. Dick, BS, and
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation in an organ- and cytokine-specific manner
 e-issn 1643-375 Med Sci Monit, 214; 2: 297-32 DOI: 1.12659/MSM.889865 Received: 213.1.6 Accepted: 213.12.2 Published: 214.2.22 Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation
e-issn 1643-375 Med Sci Monit, 214; 2: 297-32 DOI: 1.12659/MSM.889865 Received: 213.1.6 Accepted: 213.12.2 Published: 214.2.22 Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation
The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu
 The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu Research Center for Human Natural Defense system College of Medicine Yonsei University Mucosal epithelium in innate immunity Mucosal
The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu Research Center for Human Natural Defense system College of Medicine Yonsei University Mucosal epithelium in innate immunity Mucosal
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Nishino, Tomoya; Fukushima, Chizu; Asthma and Immunology, 113, 2, (201
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
Peak expiratory flow changes during experimental rhinovirus infection
 Eur Respir J 2000; 16: 980±985 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Peak expiratory flow changes during experimental rhinovirus
Eur Respir J 2000; 16: 980±985 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Peak expiratory flow changes during experimental rhinovirus
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Triggers Allergens Allografts Helminths Viruses Tissue Injury
 Rothenberg et al. Adv Immunol; 2001 Triggers Allergens Allografts Helminths Viruses Tissue Injury Rothenberg et al. Adv Immunol; 2001 Triggers Allergens Allografts Helminths Viruses Tissue Injury Cytotoxic
Rothenberg et al. Adv Immunol; 2001 Triggers Allergens Allografts Helminths Viruses Tissue Injury Rothenberg et al. Adv Immunol; 2001 Triggers Allergens Allografts Helminths Viruses Tissue Injury Cytotoxic
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Coronaviruses cause acute, mild upper respiratory infection (common cold).
 Coronaviruses David A. J. Tyrrell Steven H. Myint GENERAL CONCEPTS Clinical Presentation Coronaviruses cause acute, mild upper respiratory infection (common cold). Structure Spherical or pleomorphic enveloped
Coronaviruses David A. J. Tyrrell Steven H. Myint GENERAL CONCEPTS Clinical Presentation Coronaviruses cause acute, mild upper respiratory infection (common cold). Structure Spherical or pleomorphic enveloped
Association of Rhinovirus Infections with Asthma
 CLINICAL MICROBIOLOGY REVIEWS, Jan. 1999, p. 9 18 Vol. 12, No. 1 0893-8512/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Association of Rhinovirus Infections with
CLINICAL MICROBIOLOGY REVIEWS, Jan. 1999, p. 9 18 Vol. 12, No. 1 0893-8512/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Association of Rhinovirus Infections with
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Respiratory Pharmacology PCTH 400 Asthma and β-agonists
 Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression
 Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
1/30/2016 RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM
 RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM 1 2 year old male HISTORY -Daycare since 9 months of age -Recurrent symptoms since 10 months of age:
RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM 1 2 year old male HISTORY -Daycare since 9 months of age -Recurrent symptoms since 10 months of age:
IL-33 Dependent Type 2 Inflammation during Rhinovirus-induced Asthma Exacerbations In Vivo
 IL-33 Dependent Type 2 Inflammation during Rhinovirus-induced Asthma Exacerbations In Vivo David J. Jackson, Heidi Makrinioti1, Batika M. J. Rana, Betty W. H. Shamji, Maria-Belen Trujillo-Torralbo, Joseph
IL-33 Dependent Type 2 Inflammation during Rhinovirus-induced Asthma Exacerbations In Vivo David J. Jackson, Heidi Makrinioti1, Batika M. J. Rana, Betty W. H. Shamji, Maria-Belen Trujillo-Torralbo, Joseph
Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY. Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p.
 Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
Effect of early vitamin D supplementation on asthma and the possible mechanisms
 Effect of early vitamin D supplementation on asthma and the possible mechanisms X. Chen 1, S.Q. Rao 2, B.H. Gao 3 and Z.Q. Jiang 1 1 Department of Nutrition, College of Public Health, Sun Yat-Sen University,
Effect of early vitamin D supplementation on asthma and the possible mechanisms X. Chen 1, S.Q. Rao 2, B.H. Gao 3 and Z.Q. Jiang 1 1 Department of Nutrition, College of Public Health, Sun Yat-Sen University,
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
The Link Between Viruses and Asthma
 The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
Biomerker onderzoek voor isocyanaatgeïnduceerd
 CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
The role of dendritic cells in asthma
 Mechanisms of allergic diseases Series editors: Joshua A. Boyce, MD, Fred Finkelman, MD, William T. Shearer, MD, and Donata Vercelli, MD The role of dendritic cells in asthma Michelle Ann Gill, MD, PhD
Mechanisms of allergic diseases Series editors: Joshua A. Boyce, MD, Fred Finkelman, MD, William T. Shearer, MD, and Donata Vercelli, MD The role of dendritic cells in asthma Michelle Ann Gill, MD, PhD
A sthma is characterised by episodic symptoms
 909 REVIEW SERIES Asthma exacerbations? 3: Pathogenesis P A B Wark, P G Gibson... Asthma exacerbations are an exaggerated lower airway response to an environmental exposure. Respiratory virus infection
909 REVIEW SERIES Asthma exacerbations? 3: Pathogenesis P A B Wark, P G Gibson... Asthma exacerbations are an exaggerated lower airway response to an environmental exposure. Respiratory virus infection
Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice
 Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
The immunology of virus infection in asthma
 Eur Respir J 2001; 18: 1013 1025 Copyright #ERS Journals Ltd 2001 DOI: 10.1183/09031936.01.00228701 European Respiratory Journal Printed in UK all rights reserved ISSN 0903-1936 SERIES 0LUNG INFECTIONS
Eur Respir J 2001; 18: 1013 1025 Copyright #ERS Journals Ltd 2001 DOI: 10.1183/09031936.01.00228701 European Respiratory Journal Printed in UK all rights reserved ISSN 0903-1936 SERIES 0LUNG INFECTIONS
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
(JPC ) Caprine lungs
 2011-7-2 (JPC 3133973) Caprine lungs Bat Otgontugs Bovine Pathology Contributor: Natoinal Institute Animal Health, Tsukuba, Japan Signalment: 5-year 3-month old female Japanese native breed goat, (Capra
2011-7-2 (JPC 3133973) Caprine lungs Bat Otgontugs Bovine Pathology Contributor: Natoinal Institute Animal Health, Tsukuba, Japan Signalment: 5-year 3-month old female Japanese native breed goat, (Capra
Clinical Implications of Asthma Phenotypes. Michael Schatz, MD, MS Department of Allergy
 Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Novel biomarkers of chemical-induced asthma: a murine model. Jeroen Vanoirbeek
 Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Supplementary Figures
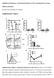 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergen and Environment in Severe Asthma
 Allergen and Environment in Severe Asthma Hye-Ryun Kang MD., PhD. Department of Internal Medicine, Seoul National University Hospital Role of Allergen in Asthma Pathogenesis Early response of allergen
Allergen and Environment in Severe Asthma Hye-Ryun Kang MD., PhD. Department of Internal Medicine, Seoul National University Hospital Role of Allergen in Asthma Pathogenesis Early response of allergen
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Infantile respiratory syncytial virus and human rhinovirus infections: respective role in inception and persistence of wheezing
 REVIEW RSV AND HRV INFECTION Infantile respiratory syncytial virus and human rhinovirus infections: respective role in inception and persistence of wheezing Giovanni A. Rossi 1 and Andrew A. Colin 2 Affiliations:
REVIEW RSV AND HRV INFECTION Infantile respiratory syncytial virus and human rhinovirus infections: respective role in inception and persistence of wheezing Giovanni A. Rossi 1 and Andrew A. Colin 2 Affiliations:
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
Role of cyclooxygenase-2 in H5N1 viral pathogenesis and the potential use of its inhibitors
 Title Role of cyclooxygenase-2 in HN viral pathogenesis and the potential use of its inhibitors Author(s) Lee, MY; Cheung, CY; Peiris, JSM Citation Hong Kong Medical Journal, 2, v. 9 n. Suppl. 4, p. 29-
Title Role of cyclooxygenase-2 in HN viral pathogenesis and the potential use of its inhibitors Author(s) Lee, MY; Cheung, CY; Peiris, JSM Citation Hong Kong Medical Journal, 2, v. 9 n. Suppl. 4, p. 29-
a b c Esophageal eosinophilia
 TSLP-elicited basophil responses can mediate the pathogenesis of eosinophilic esophagitis. Mario Noti, Elia D. Tait Wojno, Brian S. Kim, Mark C. Siracusa, Paul R. Giacomin, Meera G. Nair, Alain J. Benitez,
TSLP-elicited basophil responses can mediate the pathogenesis of eosinophilic esophagitis. Mario Noti, Elia D. Tait Wojno, Brian S. Kim, Mark C. Siracusa, Paul R. Giacomin, Meera G. Nair, Alain J. Benitez,
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Understanding How Allergic Responses End: The Allergy Resolvome. Lipid mediators
 Understanding How Allergic Responses End: The Allergy Resolvome Lipid mediators Koichiro Asano Tokai University School of Medicine, Kanagawa, JAPAN ko-asano@tokai-u.jp Resolution of granulocytic inflammation
Understanding How Allergic Responses End: The Allergy Resolvome Lipid mediators Koichiro Asano Tokai University School of Medicine, Kanagawa, JAPAN ko-asano@tokai-u.jp Resolution of granulocytic inflammation
Significance. Asthma Definition. Focus on Asthma
 Focus on Asthma (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Asthma Definition Chronic inflammatory disorder of airways Causes airway hyperresponsiveness
Focus on Asthma (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Asthma Definition Chronic inflammatory disorder of airways Causes airway hyperresponsiveness
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach
 Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
2010 Health Press Ltd.
 Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD)
 WAC2011, Dec 7, 2011 Cancun, Mexico Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD) Hae- Sim Park, MD, Ph D Department of Allergy & Clinical Immunology Ajou University School of
WAC2011, Dec 7, 2011 Cancun, Mexico Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD) Hae- Sim Park, MD, Ph D Department of Allergy & Clinical Immunology Ajou University School of
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life
 Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Basis of Immunology and
 Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
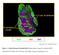 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Supporting Information
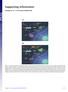 Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Supplementary Figure 1. NAFL enhanced immunity of other vaccines (a) An over-the-counter, hand-held non-ablative fractional laser (NAFL).
 Supplementary Figure 1. NAFL enhanced immunity of other vaccines (a) An over-the-counter, hand-held non-ablative fractional laser (NAFL). (b) Depiction of a MTZ array generated by NAFL. (c-e) IgG production
Supplementary Figure 1. NAFL enhanced immunity of other vaccines (a) An over-the-counter, hand-held non-ablative fractional laser (NAFL). (b) Depiction of a MTZ array generated by NAFL. (c-e) IgG production
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
COPD lungs show an attached stratified mucus layer that separate. bacteria from the epithelial cells resembling the protective colonic
 COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
Heat-killed Lactobacillus casei
 Heat-killed Lactobacillus casei confers broad protection against influenza A virus primary infection and develops heterosubtypic immunity against future secondary infection Yu-Jin Jung, Young-Tae Lee,
Heat-killed Lactobacillus casei confers broad protection against influenza A virus primary infection and develops heterosubtypic immunity against future secondary infection Yu-Jin Jung, Young-Tae Lee,
