Systemic markers of inflammation in stable bronchiectasis
|
|
|
- Gervase Ward
- 5 years ago
- Views:
Transcription
1 Eur Respir J 1998; 12: DOI: / Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN Systemic markers of inflammation in stable bronchiectasis C.B. Wilson*, P.W. Jones +, C.J. O'Leary +, D.M. Hansell, R.B. Dowling*, P.J. Cole*, R. Wilson* aa Systemic markers of inflammation in stable bronchiectasis. C.B. Wilson, P.W. Jones, C.J. O'Leary, D.M. Hansell, R.B. Dowling, P.J. Cole, R. Wilson. ERS Journals Ltd ABSTRACT: Patients with bronchiectasis have an active local and systemic inflammatory response during infective exacerbations. Systemic markers of inflammation were investigated during a stable phase of their illness, because continued inflammation could affect their general health and be involved in disease progression. The relationship between levels of various systemic markers of inflammation and extent of disease on computed tomographic scan, lung function, sputum bacteriology and health related quality of life (HRQoL) was investigated in 87 noncystic fibrosis bronchiectasis patients. Several markers were elevated and correlated with the extent of disease and poor lung function. The total white cell count, neutrophil count and erythrocyte sedimentation rate correlated with both disease measures. Sputum bacteriology did not correlate with inflammation markers and patients with positive and negative cultures were similar. C-reactive protein and total white cell count correlated with some components of a disease-specific HRQoL questionnaire. In conclusion, patients with bronchiectasis in a stable phase have raised systemic markers of inflammation. Some markers, particularly the neutrophil count, correlate with disease severity. This result is in keeping with the hypothesis that the level of inflammation determines disease progression and health status. Eur Respir J 1998; 12: *Host Defence Unit, Imperial College of Science Technology and Medicine, National Heart and Lung Institute, London, UK. + Dept of Physiological Medicine, St George's Hospital Medical School, London, UK. Dept of Radiology, Royal Brompton Hospital, London, UK. Correspondence: R. Wilson Host Defence Unit National Heart and Lung Institute Emmanuel Kaye Building Manresa Road London SW3 6LR Fax: Keywords: Bronchiectasis inflammation quality of life Received: October Accepted after revision July Bronchiectasis is a chronic lung condition in which damage to the bronchial wall causes abnormal dilation leading to poor clearance and pooling of mucus in the affected areas [1]. Patients are predisposed to lower respiratory tract infections which stimulate a chronic host inflammatory response. Chronic inflammation causes lung damage which, in turn, facilitates persistent infection. This has been termed a vicious circle and culminates in the progression of bronchiectasis and deterioration in lung function [1 3]. The patient's condition can be monitored by lung function tests and high-resolution computed tomography (HRCT), although the latter requires exposure to radiation. Several studies have investigated markers of inflammation in the blood as indicators of the intensity of the host inflammatory response to pulmonary infections and used them to evaluate the efficacy of antibiotic treatment in bronchiectasis, cystic fibrosis (CF) and community-acquired pneumonia [4 7]. These studies report a rise in the level of inflammation markers during an acute exacerbation and a subsequent fall with antibiotic treatment. However, possibly because of chronic infection, patients with bronchiectasis and CF continue to have an active local and systemic inflammatory response even if they have mild disease, are in a stable phase of their illness, or have just completed antibiotic treatment [4, 5, 8, 9]. The purpose of the present study was to examine the levels of systemic markers of inflammation in a stable, non-cf bronchiectasis population. The study aimed to investigate the relationship between levels of various systemic markers of inflammation and extent of disease as measured by HRCT, lung function, sputum bacteriology and health-related quality of life (HRQoL). Finally, patients who were on long-term antibiotic treatment were compared with those who were not. Study population Methods One hundred and twenty patients with bronchiectasis diagnosed clinically and by HRCT scan were approached over a four month period to participate in this prospective study in the Host Defence Unit outpatient clinics at the Royal Brompton Hospital, a tertiary referral centre. Of these, nine patients refused to participate and 24 were excluded because of a recent exacerbation within the preceding 6 weeks. The remaining 87 patients (49 females, 38 males) were recruited into the study. Their mean age was 53.6 (SD 12.8) yrs (range yrs). The population covered a wide spectrum of aetiologies, including idiopathic 63%, allergic bronchopulmonary aspergillosis 9%, hypogammaglobulinaemia 7%, postinfective (defined as chronic cough and sputum production directly following pneumonia in childhood, e.g. whooping cough or measles, or following adult tuberculosis or pneumonia where bronchiectasis was predominantly localized
2 MARKERS OF INFLAMMATION IN BRONCHIECTASIS 821 to the area affected by the illness) 10%, primary ciliary dyskinesia or Young's syndrome 8% and association with inflammatory bowel disease 2%. All patients had a normal sweat test. Ten patients had previously undergone surgery to remove bronchiectatic lung but had residual bronchiectasis, five patients had coexisting emphysema and one patient had mild pulmonary fibrosis by HRCT criteria, but in all cases bronchiectasis was the predominant pathology. Study protocol Patients were excluded from the study if they had suffered a severe exacerbation of their symptoms during the preceding 6 weeks, although some patients were chronically unwell. On the day of testing, blood samples were taken from each patient for measurement of C-reactive protein (CRP), total white blood cell count (WBC), neutrophil count, erythrocyte sedimentation rate (ESR) and immunoglobulins (Ig)A, IgG and IgM. Each patient also had a recent HRCT scan assessed and scored, performed comprehensive lung function tests, which included examination of arterial blood gases by earlobe sampling, and provided a fresh sputum sample during physiotherapy. The sputum was taken directly to the microbiology laboratory and after mechanical homogenization with an equal volume of Ringer's solution, inoculated onto blood (aerobic and anaerobic) and MacConkey (aerobic) agar plates (Oxoid, Basingstoke, UK) which were incubated at 37 C for 24 h, and a chocolate agar plate, which was incubated in 10% CO 2 for 48 h. Finally, each of the 87 patients completed three HRQL measures: the St George's Respiratory Questionnaire (SGRQ) [10], the SF-36 Health Survey Questionnaire, United Kingdom version (SF-36) [11], and a 14-item Fatigue Scale [12]. The questionnaires were presented to the patients in a randomized order. High-resolution computed tomographic examination A recent HRCT scan of 80 of the patients was assessed and scored by the same consultant pulmonary radiologist, who was blinded to all other details concerning the patient. Six scans were unavailable for scoring and these patients were excluded from all analyses involving HRCT scores. Each lobe of both lungs was graded for bronchiectatic changes on a 0 3 scale (the lingula was scored as a separate lobe), giving a maximum of 18 points: 0: no bronchiectasis; 1: one or no bronchopulmonary segment involved; 2: more than one bronchopulmonary segment involved; and 3: gross cystic bronchiectasis. This scoring system has been used in previous studies and is associated with low interobserver variation [13, 14]. In order to adjust the scores of those patients who had lobectomies, the bronchiectasis score was calculated as the sum of all points divided by the maximum points available for the individual 100. Thus, if an individual had one lobe resected, their maximum score was 15. Health-related quality-of-life measures Three questionnaires were used to measure different aspects of HRQoL. The SGRQ is a disease-specific measure containing 76 weighted responses divided into three domains: Symptoms, Activity and Impacts. This measure was designed to be used in patients with asthma and chronic obstructive pulmonary disease (COPD) [10]. However, it has recently been shown that the scores of bronchiectasis patients fall in the same range as these two populations, their degree of airflow obstruction is similar and the SGRQ has high levels of validity, reliability and responsiveness when used in a bronchiectasis population [15, 16]. Component scores ranging are calculated for each domain, as well as a total score summarizing the responses to all items. The SF-36 [11] is a general measure with 36 items covering functional status, well-being and overall evaluation of health. The responses can be summarized into two component scores, the physical component summary (PCS) and the mental component summary (MCS). The Fatigue Scale [12] consists of eight items covering physical aspects of fatigue and six items covering mental aspects of fatigue. All three measures are self-administered and a higher score on both the SGRQ and the Fatigue Scale and a lower score on the SF-36 indicates worse HRQoL. Statistical analysis Summary results are presented as mean±sd or as median with interquartile range (IQR). All correlations were performed using the Spearman rank correlation. The Kruskal Wallis analysis of variance (ANOVA) and Mann- Whitney U-test were used to compare the characteristics of each of the groups. Measurements from six patients with hypogammaglobulinaemia were removed before any statistical analysis of data correlating immunoglobulin levels was performed. Statistical significance was accepted at p<0.05. Results The characteristics of the population are summarized in table 1. The population covered a wide range of disease Table 1. Clinical characteristics of the 87 bronchiectasis patients enrolled in the study All patients* Range Sex M/F Age yrs Pulmonary function measures: FEV1 FVC PEFR Pa,O 2 kpa HRCT bronchiectasis score % Infective exacerbations in previous year* n Hospital admissions in previous year* n 39/48 54±13 63±27 86±22 84±31 10±6 42±20 5.0± ± Values are mean±sd. *: patients were asked to self-report this number; : visits to hospital for i.v. immunoglobulin replacement not included in data. M: male; F: female; FEV1: forced expiratory volume in one second; FVC: forced vital capacity; PEFR: peak expiratory flow rate; Pa,O 2 : arterial oxygen tension; HRCT: high-resolution computed tomography.
3 822 C.B. WILSON ET AL. severity, as measured by HRCT bronchiectasis scores, pulmonary function measures and number of infective exacerbations and hospital admissions experienced in the previous year. The number of infective exacerbations, defined as an increase in symptoms thought to be due to infection on the basis of sputum characteristics, was selfreported by the patients. Systemic markers of inflammation Normal ranges for each of the systemic markers of inflammation along with median measurement values with IQR of the study population are summarized in table 2. The percentage of patients with measurements above the normal range for each of the systemic markers of inflammation was: CRP 30%, WBC 15%, neutrophil count 14%, ESR 33%, IgA 49%, IgG, 12% and IgM 1%. High-resolution computed tomographic scores Correlations between HRCT bronchiectasis scores and systemic markers of inflammation are shown in table 3. Significant associations were found between the HRCT bronchiectasis scores and ESR, CRP, WBC and neutrophil count, but not with any of the three immunoglobulin measurements. Lung function Correlations between the lung function measures and the measurements of the systemic markers of inflammation are summarized in table 4. WBC, neutrophil count and IgG were shown to correlate significantly with most of the lung function measures performed. ESR correlated significantly with forced vital capacity (FVC), peak expiratory flow rate (PEFR), alveolar volume and the transfer factor of the lung for carbon monoxide, while IgA correlated significantly with forced expiratory volume in one second, FVC, PEFR and residual volume. The only lung function measure with which CRP significantly correlated was arterial oxygen tension, and IgM did not correlate significantly with any of the lung function measures. Table 2. Systemic markers of inflammation in 87 bronchiectasis patients Patients Reference ranges Total white blood cell count 109 L-1 Erythrocyte sedimentation rate mm h -1 Immunoglobulin A g L -1 Immunoglobulin G g L -1 Immunoglobulin M g L (8.0) 7.7 (3.0) 4.9 (2.5) 11.5 (15.0) 3.3 (1.9)* 12.5 (3.6)* 1.1 (0.8)* Values are median (interquartile range). *: six hypogammaglobulinaemia patients excluded from data. Table 3. Spearman rank correlations between highresolution computed tomographic (HRCT) bronchiectasis scores and systemic markers of inflammation in 87 bronchiectasis patients HRCT score p-value Total white blood cell count 109 L-1 Erythrocyte sedimentation rate mm h -1 Immunoglobulin A g L -1 Immunoglobulin G g L -1 Immunoglobulin M g L -1 : nonsignificant. Bacteriology In order to assess the effect of bacteriology on systemic markers of inflammation, patients were grouped according to the results of their sputum cultures. Thirty-three patients had no bacterial growth (NG group) at the time of testing, 22 patients cultured Pseudomonas aeruginosa (Pa group) and 17 patients cultured Haemophilus influenzae (Hi group); 15 patients who grew other species (0 group) were grouped together because of low individual numbers. The 0 group consisted of Staphylococcus aureus (n=4), Moraxella catarrhalis (n=3), Streptococcus pneumoniae (n=5), and coliforms (n=3). The median value with IQR of each of the systemic markers of inflammation for each of the bacteriology groups is summarized in table 5. Analyses showed that there were no significant differences between the four groups for any of the systemic markers of inflammation. Health-related quality of life Correlations were performed between each of the systemic markers of inflammation and each of the component and total scores of the three HRQoL measures. ESR, CRP and WBC were all significantly associated with the SGRQ activity score (r s =0.265, and 0.215, respectively, p< 0.05). CRP and WBC were also significantly associated with the SGRQ total score (r s =0.215 and 0.218, respectively, p<0.05). No significant correlations were found between any of the systemic markers of inflammation and the SGRQ symptoms and impacts scores, the PCS and MCS scores of the SF-36, or the component and total scores of the 14-item Fatigue Scale. Antibiotics < < In order to assess whether patients on long-term antibiotic therapy had significantly different measurements of systemic markers of inflammation to patients not on antibiotics, the patients were divided into three groups: those not on any antibiotics at the time of testing (n=65), those on long-term oral antibiotics (n=15) and those on longterm nebulized antibiotics (n=7). No significant differences were found between any of the three groups, nor between those not on any antibiotics and the other two groups combined.
4 MARKERS OF INFLAMMATION IN BRONCHIECTASIS 823 Table 4. Spearman-rank correlations between lung function measures and systemic markers of inflammation in 87 bronchiectasis patients FEV ** -0.33** * FVC ** -0.33** PEFR * RV ** * VA ** -0.39** ** TL,CO ** Total white blood cell count 109 L ** Erythrocyte sedimentation rate mm h Immunoglobulin A g L Immunoglobulin G g L ** Immunoglobulin M g L : six hypogammaglobulinaemia patients excluded from analyses. FEV1: forced expiratory volume in one second; FVC: forced vital capacity; PEFR: peak expiratory flow rate; RV: residual volume; VA: alveolar volume; TL,CO: carbon monoxide gas transfer factor; Pa,O 2 : arterial oxygen tension. *: p<0.05; **: p<0.01. Pa,O 2 kpa Discussion Bacterial infections are a major cause of morbidity and mortality in patients with bronchiectasis. Acute inflammation is an important host defence against bronchial infection, but if it fails to clear the infection and becomes chronic it can cause lung damage and lead to disease progression [1 3]. Both local and systemic markers of inflammation have been used in bronchiectasis patients to measure disease activity during acute and stable phases of illness. Several studies have shown that sputum from bronchiectasis patients in a stable clinical state contains neutrophil chemotactic activity and elastolytic activity [1, 4, 17] and there is a significant increase in both of these levels during clinical exacerbations [4, 5]. HILL et al. [5] demonstrated similar results with serum α 1 -antichymotrypsin. Bronchiectasis patients in a stable phase of their illness have elevated levels of systemic markers of inflammation. At least one-third of the present patients had elevated levels of CRP and ESR and almost half the study population had an elevated serum IgA level. Similar findings have also been reported in CF patients, even with mild disease [8]. However, despite being the most commonly elevated marker, IgA was not significantly correlated with the HRCT bronchiectasis score (table 3). This was also true of the other immunoglobulin measures, IgG and IgM. However, WBC, neutrophil count, CRP and, to a lesser extent, ESR were all positively correlated with the HRCT bronchiectasis score. This may simply reflect more widespread infection, but is also in keeping with the vicious circle hypothesis [1 3]. WBC, neutrophil count, ESR and, to a lesser extent, IgA and IgG were all correlated with several measures of poor lung function (table 4). IP et al. [18] also showed that higher serum globulin levels were associated with worse lung function in a bronchiectasis population [18]. Interestingly, while CRP correlated significantly with the HRCT bronchiectasis score it was very poorly correlated with lung function measures. The opposite was found with IgA and IgG. Therefore, some markers of inflammation correlate more closely with the anatomical extent of disease, while others correlate more closely with poor lung function. WBC, neutrophil count and ESR correlated with both disease measures. The bacteriology results in this study were similar to other published work [1], with P. aeruginosa and H. influenzae being the major pathogens. However, there were no significant differences between the three infected groups, so the type of bacterial infection did not affect the systemic markers of inflammation. Sputum bacteriology may not accurately reflect infection in the lower airways in chronic bronchitis [19], but bronchiectasis patients produce sputum more easily and the sputum sample was obtained during physiotherapy. Therefore, a negative culture is more significant and the lack of a difference in systemic markers of inflammation between infected and noninfected patients suggests that inflammation can be present with-out current infection. Only a few of the markers of inflammation were found to be associated with HRQoL. CRP and WBC correlated significantly with the activity and total scores of the SGRQ, while ESR correlated significantly with only the SGRQ activity score. None of the measures correlated significantly with the symptoms and impacts scores of the SGRQ, the SF-36 or the Fatigue Scale. It is very interesting that the significant correlations were with the SGRQ activity component, which is concerned with physical Table 5. Comparative analysis of systemic markers of inflammation between 87 bronchiectasis patients grouped according to bacteriology Total white blood cell count 109 L-1 Erythrocyte sedimentation rate mm h -1 Immunoglobulin A g L -1 Immunoglobulin G g L -1 Immunoglobulin M g L -1 Pa group n= (7.0) 8.4 (5.1) 5.2 (4.0) 9.0 (22.3) 3.7 (1.6) 12.9 (3.1) 1.3 (0.7) Hi group n= (11.8) 8.7 (2.9) 5.7 (2.6) 13.0 (16.5) 3.5 (1.6) 12.2 (3.4) 1.0 (0.5) 0 group n= (9.3) 7.3 (3.2) 4.1 (2.4) 10.0 (8.0) 2.7 (2.9) 13.7 (2.8) 1.0 (0.9) NG group n= (9.5) 7.2 (2.5) 4.5 (2.2) 12.0 (11.8) 2.5 (2.1) 11.5 (4.3) 1.1 (0.8) Values are median (interquartile range). Pa: Pseudomonas aeruginosa; Hi: Haemophilus influenzae; 0: other; NG: no growth. : six hypogammaglobulinaemia patients excluded from analyses.
5 824 C.B. WILSON ET AL. activities that cause or are limited by breathlessness, but not the symptoms component, which includes questions about cough and sputum production. Previous studies have shown that HRQoL of bronchiectasis patients is poorly correlated with other clinical features such as extent of disease as measured by HRCT bronchiectasis scores and lung function measures [15, 20]. A weak association between HRQoL, and clinical markers of disease activity has also been shown to exist in COPD and asthma, where lung function measures are very poor predictors of HRQoL [16, 21]. No evidence was found that long-term antibiotic treatment reduced systemic markers of inflammation in the stable phase. The results of this study showed no significant difference in levels of inflammation between those patients on long-term antibiotics and those not on antibiotics. In fact, patients on long-term antibiotics consistently had the higher measurements. However, since no comparison was made of levels of systemic markers of inflammation of these patients before and after commencing long-term antibiotic treatment, one cannot justly comment on the efficacy of this treatment strategy. It is possible that the patients on long-term antibiotics in this study had significantly elevated markers of inflammation before commencing long-term antibiotics, which have subsequently been lowered to a similar level to those not on antibiotics. Several other studies have examined the effect of antibiotics on markers of inflammation and have shown that antibiotics effectively reduce the amount of inflammation during an exacerbation towards a basal level, but that they are inadequate in dealing with persistent airway inflammation [4, 5]. In conclusion, patients with bronchiectasis in a stable phase have raised systemic markers of inflammation and this is not dependent on the presence of infected sputum. Some of the markers, particularly while blood cell and neutrophil counts, correlate with disease severity. Overall, there was weak correlation between markers of inflammation and health-related quality of life, although some, particularly white blood cells and C-reactive protein correlated with some of the components of the St George's Respiratory Questionnaire. This suggests that the level of inflammation, as measured by systemic markers, affects patients' overall health status, but that the relationship is indirect and, as such, poorly correlated. Future studies should investigate whether markers of inflammation in the lung correlate more closely with measures of disease severity and health-related quality of life. These studies could use either lung secretions [4, 5, 19] or an imaging technique [22]. In addition, a high-resolution computed tomographic scoring system that incorporated bronchial wall thickness may correlate more closely with the level of inflammation than the simple extent of bronchiectasis. Acknowledgements: The authors would like to thank J. Crisell for her help in the preparation of the manuscript. References 1. Cole PJ. Bronchiectasis. In: Brewis RAL, Corrin B, Geddes DM, Gibson GJ, eds. Respiratory Medicine, 2nd Edn. Vol. 2. London, W.B. Saunders Co., 1995; pp Cole PJ. Inflammation: a two-edged sword - the model of bronchiectasis. Eur J Respir Dis 1986; 69: Suppl. 147, Cole PJ, Wilson R. Host-microbial interrelationships in respiratory infection. Chest 1989; 95: Ip M, Shum D, Lauder I, Lam WK, So SY. Effect of antibiotics on sputum inflammatory contents in acute exacerbations of bronchiectasis. Respir Med 1993; 87: Hill SL, Burnett D, Hewetson KA, Stockley RA. The response of patients with purulent bronchiectasis to antibiotics for four months. Q J Med 1988; 66: Valletta EA, Rigo A, Bonazzi L, Zanolla L, Mastella G. Modification of some markers of inflammation during treatment for acute respiratory exacerbation in cystic fibrosis. Acta Paediatr 1992; 81: Smith RP, Lipworth BJ, Cree IA, Spiers EM, Winter JH. C-reactive protein. A clinical marker in communityacquired pneumonia. Chest 1995; 108: Konstan MW, Hilliard KA, Norvell TM, Berger M. Bronchoalveolar lavage findings in cystic fibrosis patients with stable, clinically mild lung disease suggest ongoing infection and inflammation. Am J Respir Crit Care Med 1994; 150: Elborn JS, Cordon SM, Parker D, Delamere FM, Shale DJ. The host inflammatory response prior to death in pati-ents with cystic fibrosis and chronic Pseudomonas aeruginosa infection. Respir Med 1987; 87: Jones PW, Quirk FH, Baveystock CM, Littlejohns P. A self-complete measure of health status for chronic airflow limitation. The St. George's Respiratory Questionnaire. Am Rev Respir Dis 1992; 145: Bousquet J, Knani H, Dhivert A, et al. Quality of life in asthma: I. Internal consistency and validity of the SF-36 questionnaire. Am J Respir Crit Care Med 1994; 149: Chandler T, Berelowitz G, Pawlikowska T, et al. Development of a fatigue scale. J Psychosom Res 1993; 37: Miszkiel KA, Wells AU, Rubens MB, Cole PJ, Hansell DM. The effects of airway colonization by Pseudomonas aeruginosa: a CT study. Thorax 1997; 52: Reiff DB, Wells AU, Carr DH, Cole PJ, Hansell DM. CT findings in bronchiectasis: limited value in distinguishing between idiopathic and specific types. Am J Roentgenol 1995; 2: Wilson CB, Jones P, O'Leary C, Cole PJ, Wilson R. Validation of the St. George's Respiratory Questionnaire in bronchiectasis. Am J Respir Crit Care Med 1997; 156: Jones PW. Issues concerning health-related quality of life in COPD. Chest 1995; 107: Suppl., Stockley RA, Shaw J, Hill SL, Burnett D. Neutrophil chemotaxis in bronchiectasis: a study of peripheral cells and lung secretions. Clin Sci 1988; 74: Ip M, Lauder IJ, Wong WY, So SY. Multivariate analysis of factors affecting pulmonary function in bronchiectasis. Respiration 1993; 60: Fagon JY, Chastre J, Trouillet JL, et al. Characterisation of distal bronchial microflora during acute exacerbations of chronic bronchitis. Use of the protected specimen brush technique in 54 mechanically ventilated patients. Am Rev Respir Dis 1990; 142: Haynes C, Jones P, O'Leary C, et al. Comparison of quality of life measures, physiological measures, and extent of disease measured by CT scan in bronchiectasis. Thorax 1995; 50: A Guyatt GH, Thompson PJ, Berman LB, et al. How should we measure function in patients with chronic heart and lung diseases? J Chronic Dis 1985; 38: Currie DC, Peters AM, Garbett ND, et al. Indium-111- labelled granulocyte scanning to detect inflammation in the lungs of patients with chronic sputum expectoration. Thorax 1990; 45:
Effect of sputum bacteriology on the quality of life of patients with bronchiectasis
 Eur Respir J 1997; 10: 1754 1760 DOI: 10.1183/09031936.97.10081754 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Effect of sputum bacteriology
Eur Respir J 1997; 10: 1754 1760 DOI: 10.1183/09031936.97.10081754 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Effect of sputum bacteriology
Bronchiectasis Domiciliary treatment. Prof. Adam Hill Royal Infirmary and University of Edinburgh
 Bronchiectasis Domiciliary treatment Prof. Adam Hill Royal Infirmary and University of Edinburgh Plan of talk Background of bronchiectasis Who requires IV antibiotics Domiciliary treatment Results to date.
Bronchiectasis Domiciliary treatment Prof. Adam Hill Royal Infirmary and University of Edinburgh Plan of talk Background of bronchiectasis Who requires IV antibiotics Domiciliary treatment Results to date.
Assessing response to treatment of exacerbations of bronchiectasis in adults
 Eur Respir J 2009; 33: 312 317 DOI: 10.1183/09031936.00122508 CopyrightßERS Journals Ltd 2009 Assessing response to treatment of exacerbations of bronchiectasis in adults M.P. Murray, K. Turnbull, S. MacQuarrie
Eur Respir J 2009; 33: 312 317 DOI: 10.1183/09031936.00122508 CopyrightßERS Journals Ltd 2009 Assessing response to treatment of exacerbations of bronchiectasis in adults M.P. Murray, K. Turnbull, S. MacQuarrie
NON-CF BRONCHIECTASIS IN ADULTS
 Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Bronchiectasis in Adults - Suspected
 Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Dr Conroy Wong. Professor Richard Beasley. Dr Sarah Mooney. Professor Innes Asher
 Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
The effect of Pseudomonas aeruginosa on pulmonary function in patients with bronchiectasis
 ERJ Express. Published on August 9, 2006 as doi: 10.1183/09031936.06.00074605 The effect of Pseudomonas aeruginosa on pulmonary function in patients with bronchiectasis Davies G +, Wells AU*, Doffman S
ERJ Express. Published on August 9, 2006 as doi: 10.1183/09031936.06.00074605 The effect of Pseudomonas aeruginosa on pulmonary function in patients with bronchiectasis Davies G +, Wells AU*, Doffman S
Online Data Supplement. Impulse Oscillometry in Adults with Bronchiectasis
 Online Data Supplement Impulse Oscillometry in Adults with Bronchiectasis Wei-jie Guan *1, Ph. D.; Yong-hua Gao *2, Ph. D.; Gang Xu *3, Ph. D.; Zhi-ya Lin 1, Ph. D.; Yan Tang 1, M. D.; Hui-min Li 1, M.
Online Data Supplement Impulse Oscillometry in Adults with Bronchiectasis Wei-jie Guan *1, Ph. D.; Yong-hua Gao *2, Ph. D.; Gang Xu *3, Ph. D.; Zhi-ya Lin 1, Ph. D.; Yan Tang 1, M. D.; Hui-min Li 1, M.
Bronchiectasis. Introduction. Key points
 15 Bronchiectasis Introduction i Key points Patients with bronchiectasis typically have chronic airway infection, punctuated by acute exacerbations and accompanied by progressive airflow obstruction. Bronchiectasis
15 Bronchiectasis Introduction i Key points Patients with bronchiectasis typically have chronic airway infection, punctuated by acute exacerbations and accompanied by progressive airflow obstruction. Bronchiectasis
How To Assess Severity and Prognosis
 How To Assess Severity and Prognosis Gregory Tino, M.D. Chief, Department of Medicine Penn Presbyterian Medical Center Associate Professor of Medicine Perelman School of Medicine at the University of Pennsylvania
How To Assess Severity and Prognosis Gregory Tino, M.D. Chief, Department of Medicine Penn Presbyterian Medical Center Associate Professor of Medicine Perelman School of Medicine at the University of Pennsylvania
COPD Bronchiectasis Overlap Syndrome.
 COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
A comparison of global questions versus health status questionnaires as measures of the severity and impact of asthma
 Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Non-cystic fibrosis bronchiectasis in childhood: longitudinal growth and lung function
 1 Portex Anaesthesia, Intensive Therapy and Respiratory Unit, UCL, Institute of Child Health, London, UK; 2 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London,
1 Portex Anaesthesia, Intensive Therapy and Respiratory Unit, UCL, Institute of Child Health, London, UK; 2 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London,
Pulmonary function abnormalities in adult patients with acute exacerbation of bronchiectasis: A retrospective risk factor analysis
 Original Article Pulmonary function abnormalities in adult patients with acute exacerbation of bronchiectasis: A retrospective risk factor analysis Chronic Respiratory Disease 2015, Vol. 12(3) 222 229
Original Article Pulmonary function abnormalities in adult patients with acute exacerbation of bronchiectasis: A retrospective risk factor analysis Chronic Respiratory Disease 2015, Vol. 12(3) 222 229
Do processing time and storage of sputum influence quantitative bacteriology in bronchiectasis?
 Journal of Medical Microbiology (), 59, 89 833 DOI.99/jmm..6683- Do processing time and storage of sputum influence quantitative bacteriology in bronchiectasis? Maeve P. Murray, Catherine J. Doherty, John
Journal of Medical Microbiology (), 59, 89 833 DOI.99/jmm..6683- Do processing time and storage of sputum influence quantitative bacteriology in bronchiectasis? Maeve P. Murray, Catherine J. Doherty, John
A Place For Airway Clearance Therapy In Today s Healthcare Environment
 A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
Pulmonary Hypertension in Patients With Bronchiectasis: Prognostic Significance of CT Signs
 Cardiopulmonary Imaging Original Research Devaraj et al. CT of Pulmonary Hypertension Cardiopulmonary Imaging Original Research Anand Devaraj 1,2 Athol U. Wells 3 Mark G. Meister 1 Michael R. Loebinger
Cardiopulmonary Imaging Original Research Devaraj et al. CT of Pulmonary Hypertension Cardiopulmonary Imaging Original Research Anand Devaraj 1,2 Athol U. Wells 3 Mark G. Meister 1 Michael R. Loebinger
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Validity and Reliability of CAT and Dyspnea-12 in Bronchiectasis and Tuberculous Destroyed Lung
 http://dx.doi.org/10.4046/trd.2012.72.6.467 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:467-474 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2012.72.6.467 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:467-474 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
A.A. Okubadejo*, E.A. Paul*, P.W. Jones**, J.A. Wedzicha
 Eur Respir J, 1996, 9, 2335 2339 DOI: 10.1183/09031936.96.09112335 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Does long-term oxygen
Eur Respir J, 1996, 9, 2335 2339 DOI: 10.1183/09031936.96.09112335 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Does long-term oxygen
The Bacteriology of Bronchiectasis in Australian Indigenous children
 The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
Bronchiectasis. What is bronchiectasis? What causes bronchiectasis?
 This factsheet explains what bronchiectasis is, what causes it, and how it is diagnosed and managed. More detailed information is available on the Bronchiectasis Patient Priorities website: www.europeanlunginfo.org/bronchiectasis
This factsheet explains what bronchiectasis is, what causes it, and how it is diagnosed and managed. More detailed information is available on the Bronchiectasis Patient Priorities website: www.europeanlunginfo.org/bronchiectasis
the potentially harmful nature of these secretions3 s even when given in the apparently stable clinical state.
 Thorax 1986;41:559-65 Short term response of patients with bronchiectasis to treatment with amoxycillin given in standard or high doses orally or by inhalation SL HILL, HM MORRISON, D BURNETT, RA STOCKLEY
Thorax 1986;41:559-65 Short term response of patients with bronchiectasis to treatment with amoxycillin given in standard or high doses orally or by inhalation SL HILL, HM MORRISON, D BURNETT, RA STOCKLEY
The Importance of Appropriate Treatment of Chronic Bronchitis
 ...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
C hronic obstructive pulmonary disease (COPD) is one of
 589 RESPIRATORY INFECTIONS Time course of recovery of health status following an infective exacerbation of chronic bronchitis S Spencer, P W Jones for the GLOBE Study Group... Thorax 2003;58:589 593 See
589 RESPIRATORY INFECTIONS Time course of recovery of health status following an infective exacerbation of chronic bronchitis S Spencer, P W Jones for the GLOBE Study Group... Thorax 2003;58:589 593 See
Understanding the heterogeneity of the disease
 Symposium: Bronchiectasis in Europe: an update from the European Bronchiectasis Network (EMBARC) Understanding the heterogeneity of the disease Stefano Aliberti Health Science Department University of
Symposium: Bronchiectasis in Europe: an update from the European Bronchiectasis Network (EMBARC) Understanding the heterogeneity of the disease Stefano Aliberti Health Science Department University of
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Chronic suppurative lung disease in adults
 Case Report Chronic suppurative lung disease in adults Mark L. Metersky 1, Antranik Mangardich 2 1 Division of Pulmonary and Critical Care Medicine, University of Connecticut School of Medicine, Farmington,
Case Report Chronic suppurative lung disease in adults Mark L. Metersky 1, Antranik Mangardich 2 1 Division of Pulmonary and Critical Care Medicine, University of Connecticut School of Medicine, Farmington,
CCLI. Bronchiectasis Treatment Antibiotics. Charles Haworth. Physician / Patient Conference, Georgetown University, May 2017
 Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD?
 AUTHOR COPY ORIGINAL RESEARCH Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD? Kian-Chung Ong 1 Suat-Jin Lu 1 Cindy Seok-Chin Soh 2 1 Department
AUTHOR COPY ORIGINAL RESEARCH Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD? Kian-Chung Ong 1 Suat-Jin Lu 1 Cindy Seok-Chin Soh 2 1 Department
Bronchiectasis exacerbations; differences and management. Michael Loebinger Royal Brompton Imperial College
 Bronchiectasis exacerbations; differences and management Michael Loebinger Royal Brompton Imperial College Plan Bronchiectasis background and burden Exacerbation and Management Longer term Management Cases
Bronchiectasis exacerbations; differences and management Michael Loebinger Royal Brompton Imperial College Plan Bronchiectasis background and burden Exacerbation and Management Longer term Management Cases
Chronic sputum production: correlations between clinical features and findings on high resolution computed tomographic scanning of the chest
 914 Department of Radiology, Addenbrooke's Hospital, Cambridge, UK E Jurriaans S Diedrich C D R Flower Department of Respiratory Medicine, Papworth Hospital, Cambridge CB3 8RE, UK I E Smith N Ali JM Shneerson
914 Department of Radiology, Addenbrooke's Hospital, Cambridge, UK E Jurriaans S Diedrich C D R Flower Department of Respiratory Medicine, Papworth Hospital, Cambridge CB3 8RE, UK I E Smith N Ali JM Shneerson
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Surgery versus non-surgical treatment for bronchiectasis (Review)
 Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
Bronchiectasis: An Imaging Approach
 Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012
 Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Short- and Long-Term Antibiotic Treatment Reduces Airway and Systemic Inflammation in Non Cystic Fibrosis Bronchiectasis
 Short- and Long-Term Antibiotic Treatment Reduces Airway and Systemic Inflammation in Non Cystic Fibrosis Bronchiectasis James D. Chalmers 1, Maeve P. Smith 2, Brian J. McHugh 1, Cathy Doherty 3, John
Short- and Long-Term Antibiotic Treatment Reduces Airway and Systemic Inflammation in Non Cystic Fibrosis Bronchiectasis James D. Chalmers 1, Maeve P. Smith 2, Brian J. McHugh 1, Cathy Doherty 3, John
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
The team. Medical staff Dr Adam Hill Vacant post- Dr Lithgow Dr Ruzanna Frangulyan Specialist Trainee
 Bronchiectasis The team Medical staff Dr Adam Hill Vacant post- Dr Lithgow Dr Ruzanna Frangulyan Specialist Trainee Specialist staff Kim Turnbull Denise Gillian Jenny Scott Jo Pentland Research nurses
Bronchiectasis The team Medical staff Dr Adam Hill Vacant post- Dr Lithgow Dr Ruzanna Frangulyan Specialist Trainee Specialist staff Kim Turnbull Denise Gillian Jenny Scott Jo Pentland Research nurses
Surgical treatment of bullous lung disease
 Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
4.6 Small airways disease
 4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
C.S. HAWORTH 1, A. WANNER 2, J. FROEHLICH 3, T. O'NEAL 3, A. DAVIS 4, I. GONDA 3, A. O'DONNELL 5
 Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
A. Service Specifications
 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No: 170050S Service Primary Ciliary Dyskinesia Management Service (adults) Commissioner Lead Provider Lead 1. Scope 1.1 Prescribed
SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No: 170050S Service Primary Ciliary Dyskinesia Management Service (adults) Commissioner Lead Provider Lead 1. Scope 1.1 Prescribed
Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation
 Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation Yung-Yang Liu, MD Taipei Veterans General Hospital Aug 29, 2015 G O lobal Initiative for Chronic bstructive L D ung isease
Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation Yung-Yang Liu, MD Taipei Veterans General Hospital Aug 29, 2015 G O lobal Initiative for Chronic bstructive L D ung isease
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Referring for specialist respiratory input. Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL
 Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
BTS Guideline for non-cf Bronchiectasis
 ISSN 2040-2023 July 2010 BTS Guideline for non-cf Bronchiectasis A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk BTS GUIDELINE FOR NON-CF BRONCHIECTASIS A QUICK REFERENCE GUIDE
ISSN 2040-2023 July 2010 BTS Guideline for non-cf Bronchiectasis A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk BTS GUIDELINE FOR NON-CF BRONCHIECTASIS A QUICK REFERENCE GUIDE
Human neutrophil lipocalin, a highly specific marker for acute exacerbation in cystic fibrosis
 Eur Respir J 1999; 14: 1145±1149 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 Human neutrophil lipocalin, a highly specific marker for
Eur Respir J 1999; 14: 1145±1149 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 Human neutrophil lipocalin, a highly specific marker for
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
BRONCHIECTASIS AND CYSTIC FIBROSIS
 BRONCHIECTASIS AND CYSTIC FIBROSIS Page 1 1 Bronchiectasis 1.1 Description Bronchiectasis is a chronic disease characterised by irreversible dilatation of the bronchi due to bronchial wall damage from
BRONCHIECTASIS AND CYSTIC FIBROSIS Page 1 1 Bronchiectasis 1.1 Description Bronchiectasis is a chronic disease characterised by irreversible dilatation of the bronchi due to bronchial wall damage from
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Upper airway involvement in bronchiectasis is marked by early onset and allergic features
 ORIGINAL ARTICLE BRONCHIECTASIS Upper airway involvement in bronchiectasis is marked by early onset and allergic features Michal Shteinberg 1,2,3, Najwan Nassrallah 4, Jenny Jrbashyan 5, Nechama Uri 5,
ORIGINAL ARTICLE BRONCHIECTASIS Upper airway involvement in bronchiectasis is marked by early onset and allergic features Michal Shteinberg 1,2,3, Najwan Nassrallah 4, Jenny Jrbashyan 5, Nechama Uri 5,
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Goyal V, Grimwood K, Byrnes CA, et al. Amoxicillin
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Goyal V, Grimwood K, Byrnes CA, et al. Amoxicillin
Non Cystic Fibrosis Bronchiectasis: How to Proceed?
 Non Cystic Fibrosis Bronchiectasis: How to Proceed? Dr Ankit Parakh MD, DNB, MNAMS, RCPCH Fellow (UK), European Diplomate of Pediatric Respiratory Medicine ERS Fellowship Pediatric Medicine & NIV (GOSH,
Non Cystic Fibrosis Bronchiectasis: How to Proceed? Dr Ankit Parakh MD, DNB, MNAMS, RCPCH Fellow (UK), European Diplomate of Pediatric Respiratory Medicine ERS Fellowship Pediatric Medicine & NIV (GOSH,
REFERRAL GUIDELINES RESPIRATORY
 REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
Serological evidence of Legionella species infection in acute exacerbation of COPD
 Eur Respir J 2002; 19: 392 397 DOI: 10.1183/09031936.02.00256702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Serological evidence of Legionella
Eur Respir J 2002; 19: 392 397 DOI: 10.1183/09031936.02.00256702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Serological evidence of Legionella
Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles
 Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles This document provides guidance for elective outpatient referrals to the Starship Tertiary
Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles This document provides guidance for elective outpatient referrals to the Starship Tertiary
bronchitis: effect of acute respiratory infection
 Thorax, 198, 35, 22-26 Local IgA production in patients with chronic bronchitis: effect of acute respiratory infection R A STOCKLEY AND D BURNETT From the Department of Medicine and Immunodiagnostic Research
Thorax, 198, 35, 22-26 Local IgA production in patients with chronic bronchitis: effect of acute respiratory infection R A STOCKLEY AND D BURNETT From the Department of Medicine and Immunodiagnostic Research
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease
 Thorax 1999;54:581 586 581 Academic Department of Respiratory Medicine, St Bartholomew s and Royal London School of Medicine and Dentistry, London Chest Hospital, London, UK EAPaul R Garrod R Garnham J
Thorax 1999;54:581 586 581 Academic Department of Respiratory Medicine, St Bartholomew s and Royal London School of Medicine and Dentistry, London Chest Hospital, London, UK EAPaul R Garrod R Garnham J
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
A 31-year-old female with a rare cause of recurrent lower lobar collapses
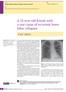 Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
What is Cystic Fibrosis? CYSTIC FIBROSIS. Genetics of CF
 What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Inhaled steroids improve quality of life in patients with steady-state bronchiectasis
 Respiratory Medicine (2006) 100, 1623 1632 Inhaled steroids improve quality of life in patients with steady-state bronchiectasis Miguel A. Martínez-García a,, Miguel Perpiñá-Tordera b, Pilar Román-Sánchez
Respiratory Medicine (2006) 100, 1623 1632 Inhaled steroids improve quality of life in patients with steady-state bronchiectasis Miguel A. Martínez-García a,, Miguel Perpiñá-Tordera b, Pilar Román-Sánchez
JMSCR Vol 04 Issue 12 Page December 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i12.124 COPD: Microbial Pattern in Acute Exacerbation
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i12.124 COPD: Microbial Pattern in Acute Exacerbation
M.N. Pond, M. Newport, D. Joanes, S.P. Conway
 Eur Respir J, 1994, 7, 1640 1644 DOI: 10.1183/09031936.94.07091640 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 Home versus hospital intravenous
Eur Respir J, 1994, 7, 1640 1644 DOI: 10.1183/09031936.94.07091640 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 Home versus hospital intravenous
ERS 2016 Congress Highlights Interstitial Lung Disease (ILD)
 ERS 216 Congress Highlights Interstitial Lung Disease (ILD) London, UK September 3 rd 7 th 216 The 26 th European Respiratory Society International Congress, (ERS) the largest respiratory meeting in the
ERS 216 Congress Highlights Interstitial Lung Disease (ILD) London, UK September 3 rd 7 th 216 The 26 th European Respiratory Society International Congress, (ERS) the largest respiratory meeting in the
Diagnosis of Ventilator- Associated Pneumonia: Where are we now?
 Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
The precise role of bacterial infection in COPD has. Bacterial Infection and the Pathogenesis of COPD* Childhood Infection and Adult Lung Function
 Bacterial Infection and the Pathogenesis of COPD* Sanjay Sethi, MD Bacterial infection of the lower respiratory tract can impact on the etiology, pathogenesis, and the clinical course of COPD in several
Bacterial Infection and the Pathogenesis of COPD* Sanjay Sethi, MD Bacterial infection of the lower respiratory tract can impact on the etiology, pathogenesis, and the clinical course of COPD in several
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions
 CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr.
 The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD
 Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD Thys van der Molen, University of Groningen, Department of General Practice, The Netherlands Mr Valette Smoking
Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD Thys van der Molen, University of Groningen, Department of General Practice, The Netherlands Mr Valette Smoking
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
Clinical phenotypes in adult patients with bronchiectasis
 ORIGINAL ARTICLE BRONCHIECTASIS Clinical phenotypes in adult patients with bronchiectasis Stefano Aliberti 1, Sara Lonni 1, Simone Dore 2, Melissa J. McDonnell 3, Pieter C. Goeminne 4,5, Katerina Dimakou
ORIGINAL ARTICLE BRONCHIECTASIS Clinical phenotypes in adult patients with bronchiectasis Stefano Aliberti 1, Sara Lonni 1, Simone Dore 2, Melissa J. McDonnell 3, Pieter C. Goeminne 4,5, Katerina Dimakou
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c)
 Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c) Bronchiolitis obliterans d) Complicated acute pneumonia e)
Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c) Bronchiolitis obliterans d) Complicated acute pneumonia e)
Pneumonia. Dr. Rami M Adil Al-Hayali Assistant professor in medicine
 Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Asthma COPD Overlap (ACO)
 Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma
 Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Palliative and Supportive Care in Cystic Fibrosis
 Palliative and Supportive Care in Cystic Fibrosis Dr William Flight Consultant in Respiratory Medicine Oxford Adult Cystic Fibrosis Centre 27 th January 2017 Overview 1. Cystic Fibrosis Clinical Aspects
Palliative and Supportive Care in Cystic Fibrosis Dr William Flight Consultant in Respiratory Medicine Oxford Adult Cystic Fibrosis Centre 27 th January 2017 Overview 1. Cystic Fibrosis Clinical Aspects
PSYCHOMETRIC ASSESSMENT OF THE CHINESE LANGUAGE VERSION OF THE ST. GEORGE S RESPIRATORY QUESTIONNAIRE IN TAIWANESE PATIENTS WITH BRONCHIAL ASTHMA
 St. George's Respiratory Questionnaire PSYCHOMETRIC ASSESSMENT OF THE CHINESE LANGUAGE VERSION OF THE ST. GEORGE S RESPIRATORY QUESTIONNAIRE IN TAIWANESE PATIENTS WITH BRONCHIAL ASTHMA Kwua-Yun Wang, Chi-Hue
St. George's Respiratory Questionnaire PSYCHOMETRIC ASSESSMENT OF THE CHINESE LANGUAGE VERSION OF THE ST. GEORGE S RESPIRATORY QUESTIONNAIRE IN TAIWANESE PATIENTS WITH BRONCHIAL ASTHMA Kwua-Yun Wang, Chi-Hue
High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
 European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
Roflumilast (Daxas) for chronic obstructive pulmonary disease
 Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
production Comparison of thin section computed tomography with bronchography for identifying bronchiectatic segments in patients with chronic sputum
 Thorax 1990;45:135-139 Host Defence Unit, Department of Thoracic Medicine, National Heart and Lung Institute, London N C Munro D C Currie P J Cole Department of Radiology, Brompton Hospital, London J C
Thorax 1990;45:135-139 Host Defence Unit, Department of Thoracic Medicine, National Heart and Lung Institute, London N C Munro D C Currie P J Cole Department of Radiology, Brompton Hospital, London J C
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease
 Skin reactivity to autologous bacteria 149 Original Article Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease J. Halasa 1, M. Halasa
Skin reactivity to autologous bacteria 149 Original Article Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease J. Halasa 1, M. Halasa
APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS
 Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Bronchiectasis. Examples include: Viral infections (measles, adenovirus, influenza)
 Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
