Ion Composition of Airway Surface Liquid of Patients with Cystic Fibrosis as Compared with Normal and Disease-control Subjects
|
|
|
- Millicent Byrd
- 6 years ago
- Views:
Transcription
1 Ion Composition of Airway Surface Liquid of Patients with Cystic Fibrosis as Compared with Normal and Disease-control Subjects Michael R. Knowles,* Joseph M. Robinson,* Robert E. Wood, Charles A. Pue,* William M. Mentz, Gilbert C. Wager, John T. Gatzy, and Richard C. Boucher* *Cystic Fibrosis/Pulmonary Research and Treatment Center, School of Medicine, Division of Pulmonary Diseases, Department of Pediatrics, and Department of Pharmacology, The University of North Carolina at Chapel Hill, Chapel Hill, North Carolina 27599; Pulmonary Medicine, St. Vincent s Medical Center, Jacksonville, Florida 32204; Dover, New Hampshire Abstract To test whether a major contribution of airways epithelial ion transport to lung defense reflects the regulation of airway surface liquid (ASL) ionic composition, we measured ASL composition using the filter paper technique. On nasal surfaces, the Cl concentration ( 125 meq/liter) was similar to plasma, but the Na concentration ( 110 meq/liter) was below plasma, and K concentration ( 30 meq/liter) above plasma. The resting ASL osmolarity [2(Na K ); 277 meq/liter] approximated isotonicity. There were no detectable differences between cystic fibrosis (CF) and normal subjects. In the lower airways, the Na concentrations were meq/liter, K levels 15 meq/liter, and Cl concentrations meq/liter. Measurements of Na activity with Na -selective electrodes and osmolality with freezing point depression yielded values consistent with the monovalent cation measurements. Like the nasal surfaces, no differences in cations were detected between CF, normal, or chronic bronchitis subjects. The tracheobronchial ASL hypotonicity was hypothesized to reflect collection-induced gland secretion, a speculation consistent with observations in which induction of nasal gland secretion produced hypotonic secretions. We conclude that there are no significant differences in ASL ion concentrations between CF, normal, and chronic bronchitis subjects and, because ASL ion concentrations exceed values consistent with defensin activity, the failure of CF lung defense may reflect predominantly factors other than salt-dependent defensins. (J. Clin. Invest : ) Key words: airway surface liquid defensins airway epithelia filter paper gland secretions CF ion composition Introduction The surface of the conducting airways is covered by a liquid that contains mucin macromolecules, electrolytes, and water. Address correspondence to Michael R. Knowles, Cystic Fibrosis/Pulmonary Research and Treatment Center, The University of North Carolina at Chapel Hill, CB 7248, 7019 Thurston-Bowles Bldg., Chapel Hill, NC Received for publication 28 May 1997 and accepted in revised form 11 September J. Clin. Invest. The American Society for Clinical Investigation, Inc /97/11/2588/08 $2.00 Volume 100, Number 10, November 1997, This airway surface liquid (ASL) 1 is thought to be organized into two components: a mucus layer and a periciliary liquid layer (1). The interaction of cilia with ASL promotes continuous clearance of inhaled foreign materials from the lung, which is believed to be a key lung defense mechanism (2). It is not yet clear how the ion transport properties of the cells lining the airway surface contribute to lung defense. Because ion and water transport are difficult to measure in vivo, regulation of epithelial ion and water transport across the conducting airways has largely been inferred from studies of freshly excised airway epithelia in vitro or cultured epithelial cells (1, 3). One view suggests that airway epithelial ion transport promotes effective mucociliary clearance by regulating both the volume and ionic composition of ASL (4, 5). This view proposes that the failure of cystic fibrosis (CF) lung defense reflects, in part, accelerated volume absorption of an isotonic fluid from airway surfaces (6), impairing lung defense by slowing mucociliary clearance. In contrast, a view emphasizing the role for the ionic strength of ASL in lung defense has been proposed (7, 8). This view suggests that airway epithelia regulate the ionic composition but not the volume of ASL (7, 8). A recent study reported a raised concentration of Cl in nasal surface liquid of CF as compared with normal subjects, and proposed that the failed lung defense in CF reflected the inhibitory effect of raised Cl concentrations on antibacterial factors in CF airways (9). A key point discriminating between these two views of the relationship of ASL to airways defense is the ionic composition of ASL of both normal and CF subjects. In this study, we used carefully calibrated techniques to measure under basal conditions the ionic concentration of the ASL lining the nasal mucosa of normal individuals and subjects with CF. Because a major role for cystic fibrosis transmembrane conductance regulator (CFTR) in gland function has been inferred from in situ hybridization studies localizing CFTR in the lung to gland acini (10), we also tried to define the contribution of glandular secretion to ASL composition. Finally, we extended these measurements to the basal ASL ion concentrations in bronchi of normal subjects, noninfected CF patients, and disease control (chronic bronchitis) subjects. Methods Subjects Normal. For nasal protocols, we studied a cohort of eight normal subjects (three female, five male; age yr) with no history of 1. Abbreviations used in this paper: ALI, air liquid interface; ASL, airway surface liquid; CB, chronic bronchitis; CF, cystic fibrosis; CFTR, cystic fibrosis transmembrane conductance regulator; DDH 2 O, double-distilled, deionized H 2 O Knowles et al.
2 chronic rhinitis and no acute nasal symptoms for at least 2 wk. None took any chronic medication. For each protocol, subjects were studied on separate days. For bronchial surface liquid studies with filter papers and the Na electrode, we studied 15 normal subjects (seven female, eight male; mean age yr). These subjects exhibited no chronic respiratory symptoms and no acute respiratory illness for at least 2 wk; none took any chronic medication. CF. Nasal protocols included nine CF patients (four female, five male; mean age yr) with no acute nasal symptoms for at least 2 wk. None took chronic nasal medication. For each protocol, subjects were studied on separate days. For bronchial surface liquid, we analyzed filter paper samples from bronchoscopies in nine newly diagnosed CF patients (six female, three male; mean age yr) who had no evidence of lower airway infection by quantitative bacteriology ( 10,000 cfu of pathogenic bacteria) in bronchial lavage. All CF patients had diagnostic sweat Cl concentrations. Chronic bronchitis. For the bronchial ASL measurements, we studied nine patients (six female, three male; mean age yr) with a history of cigarette-induced chronic bronchitis, but no acute change in pulmonary symptoms for at least 1 mo. None were taking inhaled or systemic steroids or oral bronchodilators. Inhaled bronchodilators were held for at least 12 h before bronchoscopy. Filter paper studies Filter papers. Filter paper pledgets were cut from Whatman 541 hardened ashless paper (Clifton, NJ). Individual papers for the nasal studies were 4 cm in length and 5 mm in width. The papers were washed trebly in double-distilled, deionized water (DDH 2 O) and dried in an oven overnight and then stored. Papers were folded in half width-wise, and weighed on the day used (just before sampling). For sampling, the end of the paper was grasped in a hemostat and positioned as a V laterally under the inferior turbinate for 20 s. For the adult bronchial studies, the filter papers were prepared in the same manner, but five papers ( 2 3 cm 2 3 mm) were loaded into biopsy forceps as previously described (11, 12). For the pediatric CF bronchial samples, three filter papers ( 2 cm 1 mm) were used. Weighing filter paper samples. The first measurement of the weight of samples collected on filter papers was made 15 s after removal from the subject, and serial measurements were made over the next 90 s (model No. 27; Cahn Electronic Balance, Cerritos, CA). A regression line was fit from these points and extrapolated to time zero to determine an initial weight as previously described (11, 12). To estimate the accuracy of weighing filter paper samples, and control for evaporative water loss during transfer of the sample from the patient to the electronic balance, we added a known amount ( 10 l) of saline (150 meq/liter NaCl) to the filter paper, and then transferred the sample to the balance as the nasal samples were handled. The loss of weight during transfer of the filter paper to the balance and the first weight measurement ( 15 s) was % (n 6). Back extrapolation from serial weighing projected an initial weight that was % of the volume added to the filter paper at time zero. We also measured the change in weight of filter paper exposed to the high humidity of the lower airways before the dry filter paper was touched to the airway surface. We noted a small weight gain over 30 s in the tracheal lumen ( mg; n 4; 1% of the mean sample weight), and a similar increase ( mg; n 6) in the mouth over 30 s during slow exhalation through tightly pursed lips. Extraction. After weighing, filter papers and aluminum-weighing pans were placed in acid-washed plastic vials. For ion analyses, 1 ml of DDH 2 O was added to each specimen, and the vials were shaken on a gyrotory shaker (model G2, at 4 C; Vendor, Edison, NJ) for at least 24 h. For analyses for albumin and osmolarity, filter papers were eluted overnight in 200 l of DDH 2 O. For ion analyses, the solution in the vials was transferred to acid-washed volumetric tubes (2 ml) and 0.5 ml of 0.2 N HNO 3 was added to the vial. The paper was stirred and then wrung out with forceps to remove the liquid. This liquid was added to the volumetric tube. The maneuver was repeated and the extract was brought up to 2 ml with 0.2 N HNO 3. We tested the efficiency of extraction from filter papers of ion solutions of known composition. Solutions (10 and 25 l) with known composition (Na mm, Cl 134.8, K 3.1 mm) were applied to filter papers and the papers were carried through the extraction and ion analysis protocol. The extraction efficiency from five experiments with each volume (10 and 25 l) was similar, and mean recovery of each ion exceeded 99% as compared with the concentration of ions pipetted directly into aluminum pans. Ionic analysis. Chloride was measured with a digital chloridometer (model ; Labconco, Kansas City, MO) as previously described (13). To prepare for titration, 1 ml of the 2-ml extract was added to a solution of 1 ml DDH 2 O, 2 ml of Labconco acid reagent, 0.2 ml of glacial acetic acid, and two drops of indicator. Standards of known Cl concentration (0, 20, 40, 60, 80, 100, 200, 300, 500, 1,000, and 2,000 eq/liter) were prepared with the same reagent indicator solution. Values for blanks (1 ml of 0.2 N HNO 3 ; 4% of the value for any specimen) were subtracted to yield final sample value. The standard curve for Cl concentration was linear from 100 to 2,000 eq/liter, and hyperbolic from 0 to 100 eq/liter. Na and K in the remaining 1 ml of extract were measured with a flame photometer (model 51 ca; Perkin-Elmer Corp., Norwalk, CT) as previously described (13). Standard curves for K were linear over a wide range of concentration (20 to 2,000 eq/liter), whereas the relationships for Na were curvilinear (0 to 2,000 eq/liter). We estimate a limit of detection for Cl and K of 500 and 20 neq, respectively. These limits correspond to 2.5 l of a 100 mm NaCl solution and 1 l of a solution with 25 meq/liter K. Accordingly, specimens 3 l (i.e., 3 mg) were not analyzed. Because our analyses routinely underestimated the nominal Na and Cl concentrations of physiologic salt solutions (e.g., media, Ringer s solution) by an average of 6%, we applied this correction to all specimens. The correction did not change the pattern of ion composition of airway liquid from any subject population, or comparisons among populations, but tended to bring estimated osmolarities for basal nasal specimens close to isosmolarity. Protein and osmolarity analysis. Albumin was determined by radioimmunoassay (13), and osmolality was measured by freezing point depression (Osmette, model 2007; Precision Systems, Sudbury, MA), as previously described (13). Analysis of [Na ] in airway surface liquid with Na -selective electrodes Na -selective glass electrodes ( MI-420; selectivity Na over K 1000:1; Microelectrodes, Inc., Londonderry, NH) were used, coupled to a reference electrode (5.0 silk thread), and saturated with 100 mm KCl. The output (mv) of the Na electrode was determined in four NaCl solutions (25.6, 77, 154, and 256 mm). A standard curve was generated before each study, and repeated immediately after each study. A semilog plot yielded a mean slope of mv per decade change in Na activity at 34 C. Surface liquid [Na ] on airways was assayed in anesthetized dogs. After anesthesia with parenteral pentobarbital (25 mg/kg) and intubation with a shortened endotracheal tube, the Na and reference electrodes (housed in a protective catheter) were passed transbronchoscopically into the lower airways and touched lightly to the distal tracheal surface until a stable measurement was obtained for s at two to four different sites. Canine epithelial cell cultures To estimate the potential damage induced by placement of filter papers on epithelial surfaces, and potential artifacts generated by this effect and/or sampling of cellular ionic contents due to adherence of epithelial cells to the filter paper, a series of studies was performed in air liquid interface (ALI) cultures. Dog tracheal cells were cultured to confluence on 24-mm Transwell Col supports, and exposed to an ALI to allow development of a well-differentiated phenotype (3 4 wk after seeding) (14, 15). The ALI epithelial preparations were equilibrated with lumenal media (500 l) containing (in meq/liter) Na 132, Cl 120, and K 5.8, and measurements of transepithelial resistance (R t ) made (EVO-M; World Precision Instruments, Ion Composition of Airway Surface Liquid 2589
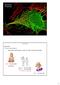
3 Sarasota, FL), after which excess fluid was gently removed. 4 h later, ASL was sampled. Surface liquid was aspirated directly from some cultures using a micropipette for measurements of ion concentration. Surface liquid was sampled from other cultures with filter paper applied to the surface for 20 s. Measurements of transepithelial resistance (R t ) were repeated after sampling by aspiration or filter paper. Human protocols Studies of solution recovery. For studies of the accuracy of the sampling and measurement techniques, Atrovent (168 g in 150 mm NaCl) was applied topically (spray) to the nasal mucosa in each nostril to inhibit secretion (16, 17). After min, Atrovent-pretreated nasal surfaces were sprayed under direct vision (six sprays; 0.25 ml per spray) with saline (150 mm NaCl) in each nostril, and the mucosal surface liquid was sampled immediately with filter papers ( s later). Baseline nasal ASL collections. Each nostril was completely occluded with a polyethylene plug to minimize evaporative water loss from nasal surfaces before sampling after defined times (5, 10, 20 min) to determine the time required to reach steady-state equilibration of electrolytes. Because 10 min of occlusion was found to be required for equilibration of ASL (see Results), this time (10 min) was used for most protocols. To obtain samples of basal surface liquid, the plug was removed and filter paper was gently placed under direct vision on the nasal surface in a region that allowed contact with liquid on the inferior surface of the inferior turbinate and the floor. The filter paper was left in place for 20 s and then removed and weighed as described above. Gland contribution to nasal ASL composition. The gland secretion was stimulated without adding a drug/vehicle directly to the nasal surfaces by occluding the nasal passages with plugs for 10 min and then having subjects chew hot chili peppers, a maneuver that has been shown to induce a glandular reflex secretion in the nasal mucosa, for 5 min (18). Surface liquid was sampled from nostrils after the chili pepper gustation. Lower airway protocols. (a) Normal subjects and patients with chronic bronchitis: after topical anesthesia of the nose (viscous lidocaine, 2%), the throat was anesthetized with topical lidocaine (1%) with the patient in the Trendelenburg position. Normal subjects undergoing filter paper sampling received atropine (0.6 mg I.M.; n 6) or no atropine (n 5); there was no difference in volume (wt) or electrolyte composition of ASL samples obtained with or without atropine, and data were grouped for presentation. After parenteral sedation (meperidine, mg; midazolam, 2 10 mg), a fiberoptic bronchoscope was introduced into the lower airways, and pretared filter paper strips held by standard biopsy forceps housed in a protective catheter were placed transbronchoscopically onto the mucosal surface for 20 s as previously described (11, 12). The filter papers with sampled ASL were withdrawn into the catheter, removed from the broncoscope, and immediately weighed to determine volume of sample. Two to five filter paper samples were obtained from the mainstem and lobar bronchus, and one to two samples from distal trachea, of each subject, and samples were processed as described above. For studies with the Na -selective electrode in normal subjects, topical anesthesia and sedation without atropine were performed as for filter paper studies. The Na and reference electrodes were housed in a protective catheter and passed transbronchoscopically into the lower airways (as above), and held lightly against the airway surface of the mainstem or lobar bronchus until a stable measurement was obtained for s at two to five different sites. (b) Cystic fibrosis: these patients were bronchoscoped shortly after the diagnosis of CF to define the infection status of the lower airways. The filter paper samples were obtained under a research protocol coupled to the clinically indicated bronchoscopy. After topical anesthesia of the nose (viscous lidocaine), the throat was anesthetized with topical lidocaine (2%; 1 ml) with the patient in the Trendelenberg position. After parenteral sedation (meperidine, 1 2 mg/kg; midazolam, mg/kg), pretared filter papers held by biopsy forceps housed in a protective catheter were placed onto the mucosal surface of the mainstem bronchus for 20 s. The filter papers with ASL were withdrawn into the catheter, removed, and sample weighed and processed as described. After this maneuver, a 20-ml bronchoalveolar lavage was performed for quantitative bacterial colony counts (19). Statistical analysis Nasal surface liquid electrolyte concentrations from each nostril of an individual, and multiple bronchial values for an individual, were averaged to give a value per subject for each electrolyte; study cohort mean values were derived from data per study subject. The difference between study cohorts was tested by nonpaired t test. The response to gustatory submucosal gland stimulation within each study population was not normally distributed, and the change from baseline was tested by Wilcoxon sign rank (paired test). A P value 0.05 was considered significant. The relationship between estimated osmolarity of bronchial surface liquid and size of sample was assessed by linear regression plot (Figure P ; Biosoft, Cambridge, United Kingdom). All human protocols were approved by the UNC Human Rights Committee (IRB), and informed consent obtained. All animal protocols were approved by the International Animal Care and Use Committee. Results Controls for sampling, weighing, elution, and ion concentration measurements Recovery of a defined electrolyte solution added to the nasal mucosa in vivo. Because the ion concentrations in nasal surface liquid are quite different from those of plasma (see below), we evaluated the accuracy of our technique by measuring the concentration of ions in a defined solution deposited on the nasal surface. After Atrovent pretreatment to inhibit gland secretion, nasal surfaces were sprayed with a 150-mM NaCl solution (1.5 ml), using an atomizer spray. Ionic concentrations of surface liquid sampled immediately ( s after nasal spray) approximated those of the saline spray (Fig. 1) for both normal and CF subjects. These data strongly suggest that the sampling and elution protocols accurately measure the composition of the solution on the nasal surface. ASL sampled by aspiration or filter paper from the surface of cultured canine epithelia. The ALI epithelial cultures (n 6) were equilibrated with lumenal media (500 l) containing Figure 1. Ionic composition and estimated osmolarity of liquid on nasal surfaces of normal subjects (n 6; open bars) and CF patients (n 5; solid bars) after nasal spray with isosmotic NaCl (150 meq/ liter). The estimated osmolarity [sum of cation concentrations, i.e., 2(Na K )] is expressed in meq/liter Knowles et al.
4 (in meq/liter) Na 132, Cl 120, and K 5.8, and measurements of V t and R t made, following which excess fluid was gently aspirated. 4 h later, ASL was sampled. Liquid sampled by direct sampling techniques revealed concentrations (in meq/liter) of Na equal to 124 3, Cl concentrations of 125 7, and K concentrations of Surface liquid recovered from the cultured epithelial cells with filter paper revealed concentrations (in meq/liter) of Na of , Cl 104 6, K The electrical resistance of cultures before and after direct and filter paper sampling were (in.cm 2 ) pre , post ; pre , post , respectively. Nasal ASL electrolyte concentrations Basal conditions. Preliminary experiments demonstrated that the variability of the electrolyte concentrations and the volume of liquid sampled from nasal surfaces increased until the occlusion time approached 10 min; values at 20 min were no different in magnitude or variability than at 10 min. At 10 min, the weights collected by filter paper from normal ( mg) and CF subjects ( mg) were not different. The composition of ASL from normal subjects was characterized by a mean Na concentration 25% below those of plasma, whereas the K concentration was more than fivefold greater than plasma (Fig. 2). The concentration of Cl was slightly higher than that of plasma and the calculated anion gap, i.e., (Na K -Cl ), an estimate of the putative HCO 3 concentration, was less ( 8 12 meq/liter) than the concentration of HCO 3 in plasma. We multiplied the sum of cation concentrations (Na K ) by two to estimate osmolarity, and nasal surface liquid was close to isotonic (estimated 277 mosm/ liter) with plasma ( 285 mosm/liter). Importantly, the mean ionic composition of samples from CF and normal subjects were not different for any ion. Stimulation of nasal gland secretion. The ionic composition and sample weight of surface liquid for normal and CF subjects after stimulation of gland secretion with chili peppers were compared with paired basal values (Fig. 3). For normal subjects, the weight (volume) of secretions collected (20 s) increased approximately threefold after stimulation. Compared to the basal composition, there were small decreases in the Figure 2. Ionic composition ( Na, Cl, K ) and estimated osmolarity of nasal surface liquid (at baseline) in normal subjects (n 8; open bars) and CF patients (n 8; solid bars) after 10 min of nasal occlusion. The estimated osmolarity [sum of cation concentrations, i.e., 2(Na K )] is expressed in meq/liter. Figure 3. The volume (wt), ionic composition (Na, Cl, K ) and estimated osmolarity [2 (Na K )] of nasal surface liquid samples at baseline (open bars) and after gustatory stimulation of submucosal glands (solid bars) with chili peppers. (A) Normal subjects (n 8) and (B) CF patients (n 8). *P 0.05, different from baseline. concentration of Na, Cl, and K, and a 40 meq/liter decrease in estimated [2(Na K )] osmolarity, suggesting that a hypotonic solution was secreted from glands. The ionic composition of nasal surface liquid from CF subjects followed the same pattern as identified in normals (Fig. 3 B). Wet weights rose more than twofold after chili pepper stimulation. Like nasal surface liquid from normals, there was a decrease in the concentration of Na, Cl, and K, and a 30 meq/liter decrease in estimated osmolarity after stimulation. Lower airway surface liquid compositions Basal ASL values. The ionic composition of bronchial ASL from 11 normal subjects (compare Fig. 4 A with Fig. 2) differs substantially from the nasal cavity. The concentration of Na in bronchial surface liquids was 15% lower than in nasal surface liquid and 35% lower than plasma, and the concentration of Cl in bronchial surface liquids was substantially lower than the concentration in either nasal surface liquids or plasma. Like nasal liquid, bronchial K concentrations were greater than plasma (approximately three- to fourfold). The ion compositions of ASL from distal trachea (Na , Cl , and K meq/liter) of five normal subjects were similar to those of bronchial ASL. Differences among the ion compositions of bronchial and nasal surface liquids and plasma led us to check the estimates of bronchial surface liquid composition by alternative tech- Ion Composition of Airway Surface Liquid 2591
5 Finally, we measured albumin concentrations in normal human ASL to estimate the contribution of interstitial fluid that might enter surface liquid through leaks induced by filter paper sampling. The concentration of albumin in bronchial and tracheal surface liquid of six normal subjects ( and mg/dl, respectively) was 60 times less than that of plasma, suggesting that contamination of ASL by interstitial liquid that entered through albumin-permeant leaks was minimal. We then compared the ionic composition of ASL collected from the lower airways of uninfected cystic fibrosis and uninfected chronic bronchitis patients with that collected from the normal volunteers (Fig. 4 A). Like the ASL of normal subjects, liquids collected from these patients were characterized by low Na, low Cl, and raised K concentrations compared to plasma. Importantly, we found ASL from each subject population was characterized by similar ion compositions, except for the 20% increase in Cl in the noninfected chronic bronchitis subjects. Relationship between volume of bronchial samples and osmolarity. To gain some insight into the contribution of collection-induced gland secretions to the hyposmotic ASL measured in the three study groups, we examined the relationship between the estimated osmolarity [2(Na K )] and volume (wt) of samples collected for each group (Fig. 5). Bronchial surface liquid approaches isosmolarity in smaller samples (low wt) and becomes increasingly hyposmotic with increasing volume (wt) of samples. Discussion Figure 4. Ionic composition of surface liquid in lower airways. (A) Ion composition (Na, Cl, K ) and estimated osmolarity [2(Na K )] of bronchial surface liquid in normal subjects (n 11; open bars), CF patients (n 9; hatched bars), and patients with chronic bronchitis (n 9; solid bars). *P 0.05, different from normal and CF; P 0.05, different from CF. (B) Na concentration and osmolarity in airway surface liquid in normal human bronchi and canine trachea, and osmolarity in human bronchi, as determined by techniques of filter paper sampling (open bars), Na electrode (hatched bars), and freezing point depression (solid bar). Canine tracheal filter paper data shown for comparison; previously published (13). niques. The osmolality of surface liquid sampled by filter paper from five normal subjects, measured by freezing point depression, was found to be hyposmotic compared to plasma, and to be similar in magnitude to the estimate of 2(Na K ), suggesting that no molecules other than monovalent ions contribute to ASL osmolarity (Fig. 4 B). Bronchial Na concentrations were measured with Na -selective electrodes immersed in ASL in vivo. We assessed the accuracy and sensitivity of the Na electrode system in vivo by first making measurements in dog airways. The concentration of Na measured with Na -selective electrodes in canine tracheal surface liquid were comparable ( meq/liter, n 3) to previously reported values (Fig. 4 B) (13). Human bronchial ASL Na concentrations measured with Na -selective electrodes in vivo approximate closely those estimated from samples on filter paper (Fig. 4 A). The congruence of Na concentrations measured by two independent techniques indicates that the filter paper protocol does not induce unique artifacts. Despite intense interest in the characterization of ion transport by human airway epithelia over the last 15 yr, it is still not clear whether airway epithelia regulate volume and ionic composition of airway surface liquids or ionic composition alone (1, 3, 6 9, 20, 21). Recent studies focusing on the relationship between ion composition of airway surface liquid and infectious pathogenesis of CF lung disease (9, 22) led us to measure and compare ion compositions of upper and lower ASL in normal subjects and subjects with airways disease. Because the surface liquid layer is shallow, sampling and measurement of its composition are difficult, leading to a wide spectrum of reported values for human ASL (1). We therefore tested the accuracy of our sampling technique and compared our analytic protocols with independent techniques. Sampling with filter paper raises several questions. First, does the volume collected in the paper reflect the surface liquid volume/ unit area relationship in vivo? One approach to this question is to compare the volume on the airway surface in the region probed by the paper with the volume collected. Unfortunately, the depth of ASL on human airways is not known precisely and published values in mammalian proximal airways range from m (23 25). However, assuming a 25- thick liquid layer, the volume of ASL in the vicinity of the filter paper (defined by its physical dimensions: 2 3 mm mm) should approximate 5 10 l. In the nose and in the lower airways, the volume collected in the basal state is approximately twofold higher than predicted ( l). Possible explanations include epithelial damage and serum leak, wicking of surface liquid from outside of the estimated area sampled by the filter papers, and/or induction of reflex gland secretion. The very low albumin concentrations in airway surface liquids 2592 Knowles et al.
6 Figure 5. Relationship between the estimated osmolarity [2(Na K ); meq/l] and volume (wt) of bronchial surface liquid sampled from normal subjects (11 subjects; 13 samples, r 0.31), patients with cystic fibrosis (nine subjects; 21 samples, r 0.65), and patients with chronic bronchitis (nine subjects; 28 samples, r 0.41). and absence of detectable changes in epithelial resistance with filter paper sampling in vitro argue against the first explanation. The composition of gland secretions and their contribution to surface liquid volume in nose or lower airways of humans has not been previously described, so we cannot distinguish between or eliminate the other possibilities. However, our subsequent studies designed to measure ionic compositions under conditions that maximize the relative contribution of the glands to nasal surface liquid suggest that reflex gland secretion is probably induced in lower airways (see below). Second, do the collection and elution protocols lead to an accurate measure of electrolytes? Because sampling from the surface of epithelial cell cultures did not raise the ASL concentration of K, we conclude that raised concentration of K in liquid sampled in vivo did not reflect cellular damage or adherent cells, consistent with previous analyses (13). We confirmed our previous experience with elution efficiency and analytic errors, showing that 99% of known electrolyte added to filter paper is recovered (13). We have extended this experimental modeling further in the current study to define the limit of accuracy associated with sampling small volumes. The sensitivity of our analysis (3- l limit) was adequate to avoid excluding any samples due to insufficient sampled volume. Finally, the congruence of the concentrations of Na and Cl of the solutions sprayed onto the nasal surface with those measured within 1 min of deposition by filter paper sampling and analysis (Fig. 1) indicates that the entire procedure of sampling, weighing, and analyses is accurate and reliable. We focused our studies on nasal surfaces so that our data could be compared with recent reports of Cl concentrations in airway surface liquid from CF and normal subjects (9). After nasal occlusion, we found that there were time-dependent increases in volume collected and reductions in ionic concentrations. Approximately 10 min were required for equilibration after evaporative water loss was minimized with the nasal plugs. For both normal and CF subjects, Na concentrations ( 109 mm) were lower than those of plasma, Cl concentrations ( 125 mm) were similar to plasma, and K concentrations ( 30 mm) were higher than plasma. We found no significant difference between the ionic composition of liquid from CF and normal subjects. Subsequent to the original report of higher concentration of Cl in CF surface liquid, Smith et al. have retracted the observations because the difference between CF and normal liquid could not be reproduced (26). Our study not only found no difference in Na and Cl concentrations between CF and normal nasal surface liquid, but our measured concentrations far exceed the values of Na or Cl (and tonicity) that are optimal for activity of salt-dependent defensins in the respiratory tract (9, 22). We extended our studies to the lower airways, evaluating samples from the mainstem and second generation bronchi in normal healthy volunteers (mean age 26 yr). The ion composition of samples collected with filter paper differed from those taken from the nose in that Na, Cl, and K concentrations were lower (Fig. 4 A). Importantly, the sum of the cations suggested that the solution on bronchial surfaces is hyposmotic. A hyposmotic lower airway surface liquid is difficult to reconcile with water permeabilities reported for surface airway epithelia (27, 28). Consequently, we determined the osmolarity of filter paper samples and measured the concentration of Na, the dominant cation, on the airway surface with Na -selective electrodes. The concentration of Na determined by these electrodes agreed with flame photometry of liquid sampled by filter paper, and the osmolarity measured by freezing point depression was comparable to the value estimated from Na and K concentrations (Fig. 4 B). Thus, we conclude that the filter paper technique accurately measured the ionic composition of secretions on airway surfaces at the time of sampling. We compared the normal data with those of bronchial surface liquid from nine infants with cystic fibrosis who were noninfected based on low bacterial counts in bronchoalveolar lavage (Fig. 4 A). Concentrations of Na, Cl, and K in CF ASL were not different from normal adult controls (Fig. 4 A). Finally, we characterized electrolyte concentrations in surface liquid of adults with cigarette-induced chronic bronchitis without infection, a disease control. Again, electrolyte concentra- Ion Composition of Airway Surface Liquid 2593
7 tions in these subjects did not differ from those of CF or normal subjects, except for a modest (20%) increase in Cl. Our values for the ionic composition of CF bronchial ASL disagree with two published reports. Gilljam et al. (29) reported K concentrations equal to plasma and Cl concentrations higher than plasma in mucopurulent bronchial secretions (mean sample weights mg) aspirated by a dry catheter (29). Our data also describe CF surface liquid that is more hyposmotic than that recovered by Joris and colleagues (20). We do not know the reason for these discrepancies. However, Gilljam et al., like Smith et al. (9), reported Cl concentrations that predict a hyperosmotic surface liquid, a composition that is not compatible with any known physiologic process in airway epithelia. The most likely explanation for a high Cl concentration is evaporative water loss during sample collection and processing, or inadequate time for surface liquid humidification in vivo. The higher Na and Cl concentrations of bronchial samples from three CF patients (two intubated) reported by Joris et al. (20) may also reflect evaporative water loss, but we have no way to estimate the magnitude of these putative losses. Our data on CF ionic composition are similar to those reported by Wills et al. (5), the patient cohort in our study is relatively large, and this is the first uninfected CF cohort reported. The volume of secretions recovered by the filter paper technique and apparent incompatibility of hypotonic bronchial surface liquid and the relatively high water permeability reported for superficial bronchial epithelia raised the possibility that the filter paper sampling technique induces reflex glandular secretion and that glands, as a function of their ductal ion transport activities, are the source of hypotonic solutions on airway surfaces. We attempted to separate the contribution of glands from superficial epithelium to the composition of liquid on airway surfaces by studying the effects of stimulated gland secretion. We sampled liquid from nasal surfaces because this surface is accessible to manipulation and all liquid on the superficial epithelia in this region is derived from the glands (i.e., there is no axial flow from more distal airways [1]). Reflex stimulation of nasal glands resulted in an increase in volume collected by filter papers from both CF and normal subjects (Fig. 3). Interestingly, the increase in volume was similar in normal and CF subjects, suggesting that non-cftr Cl transport pathways may be important in gland secretion in upper airways. Stimulation of gland secretion diluted the concentration of measured ions ( Na, Cl, K ), and there was a decrease (30 40 meq/liter) in the estimated osmolarity [2(Na K )] of CF and normal nasal surface liquid after stimulation of submucosal glandular secretion (Fig. 3). Usually, hyposmotic gland secretion results from (hyperosmotic) NaCl absorption by ductal epithelium (20, 30). Although absorption by human submucosal gland ducts has not been measured directly, Na channels are expressed in the ducts of human normal and CF nasal glands (31). Our conclusion that nasal gland secretions are hyposmotic led us to re-examine the estimated osmolarity of bronchial ASL. Fig. 5 displays the relationships between estimated osmolarity (2[Na K ]) and volume of surface liquid samples from normal, CF, and CB subjects. For each group, the smaller volume samples approach isotonicity, and as volume increased, osmolarity fell. We speculate that these relationships are the consequence of gland secretion induced by the collection technique. When this effect is minimized (e.g., volumes become smaller), ASL approximates isotonicity for all groups. Consequently, the low osmolarity in the bronchial surface liquid could reflect glandular secretion in this region. In summary, we found no difference in ionic composition between surface liquid collected from nasal surfaces of CF and normal subjects under basal conditions. Nasal surface liquid is close to isosmotic. Stimulation of glands suggests that both CF and normal glands secrete a solution that is more hyposmotic than resting (basal) surface liquid. We suggest that submucosal gland ductal salt absorption lowers the osmolarity of solution secreted from gland acini. Our studies also did not reveal any difference among the ionic composition of airway surface liquids from bronchial regions of normal subjects, CF patients, or disease control patients. Human bronchial ASL tended to be hyposmotic relative to plasma, suggesting that the sampling technique in the lower airways disproportionately reflects glandular secretions rather than ambient airway surface liquids, or, less likely, that the high water permeability reported for excised airway epithelia is not relevant in vivo. Regardless of the explanation, the degree of hyposmolarity measured in either the nasal or bronchial surface is unlikely to activate saltsensitive defensin-like antimicrobial activities (9, 22). Finally, our studies point to the need for better collection techniques and reliable measurements of ionic composition in the bronchioles, the site at which CF disease is initiated. Although the conductive properties of bronchioles make it unlikely (32), it is possible that bronchiolar ASL is hypotonic in normal, but not CF, and distal CF airways might be more susceptible to infection, if the hypothesis about salt-sensitive antimicrobial activity is valid. In addition, other important components of airway surface liquid (e.g., the water content, ph) may be the key to the mystery of the early pathogenesis of CF airways infection. Note added in proof: Since submission of this manuscript, we have become aware of a similar study, Elemental content of airway surface liquid from infants with cystic fibrosis, Hull, J. et al. Am. J. Respir. Crit. Care Med. In press. Acknowledgments Thanks to Nina Church, Carla Foy, and Jon Winders for technical assistance, Peter Gilligan, Ph.D., for quantitative microbiology, and Lisa Brown for editorial assistance. Support was provided by National Institutes of Health grants P and RR000046, and CFF RDP 026. References 1. Boucher, R.C Human airway ion transport (part 1). Am. J. Respir. Crit. Care Med. 150: Wanner, A., M. Salathe, and T.G. O Riordan Mucociliary clearance in the airways [State of the art]. Am. J. Respir. Crit. Care Med. 154: Boucher, R.C Human airway ion transport (part 2). Am. J. Respir. Crit. Care Med. 150: App, E.M., J.G. Zayas, and M. King Rheology of mucus and transepithelial potential difference: small airways versus trachea. Eur. Respir. J. 6: Wills, P.J., R.L. Hall, W. Chan, and P.J. Cole Sodium chloride increases the ciliary transportability of cystic fibrosis and bronchiectasis sputum on the mucus-depleted bovine trachea. J. Clin. Invest. 99: Jiang, C., W.E. Finkbeiner, J.H. Widdicombe, P.B. McCray, Jr., and S.S. Miller Altered fluid transport across airway epithelium in cystic fibrosis. Science. 262: Smith, J.J., P.H. Karp, and M.J. Welsh Defective fluid transport by cystic fibrosis airway epithelia. J. Clin. Invest. 93: Quinton, P.M Viscosity versus composition in airway pathology [editorial]. Am. J. Respir. Crit. Care Med. 149: Knowles et al.
8 9. Smith, J.J., S.M. Travis, E.P. Greenberg, and M.J. Welsh Cystic fibrosis airway epithelia fail to kill bacteria because of abnormal airway surface fluid. Cell. 85: Engelhardt, J.F., J.R. Yankaskas, S.A. Ernst, Y. Yang, C.R. Marino, R.C. Boucher, J.A. Cohn, and J.M. Wilson Submucosal glands are the predominant site of CFTR expression in human bronchus. Nat. Genet. 2: Knowles, M.R., N.L. Church, W.E. Waltner, J.T. Gatzy, and R.C. Boucher Amiloride in cystic fibrosis: safety, pharmacokinetics, and efficacy in the treatment of pulmonary disease. In Amiloride and its Analogs: Unique Cation Transport Inhibitors. E.J. Cragoe, Jr., T.R. Kleyman, and L. Simchowitz, editors. VCH Publishers, Inc. New York Noone, P.G., J.A. Regnis, X. Liu, K.L.R. Brouwer, M. Robinson, L.J. Edwards, and M.R. Knowles Airway deposition and clearance, and systemic pharmacokinetics of amiloride following aerosolization with an ultrasonic nebulizer to normal airways. Chest. 112: Boucher, R.C., M.J. Stutts, P.A. Bromberg, and J.T. Gatzy Regional differences in airway surface liquid composition. J. Appl. Physiol. 50: Gray, T.E., K. Guzman, C.W. Davis, L.H. Abdullah, and P. Nettesheim Mucociliary differentiation of serially passaged normal human tracheobronchial epithelial cells. Am. J. Respir. Cell Mol. Biol. 14: Matsui, H., L.G. Johnson, S.H. Randell, and R.C. Boucher Loss of binding and entry of liposome-dna complexes decreases transfection efficiency in differentiated airway epithelial cells. J. Biol. Chem. 272: Wagenmann, M., F.M. Baroody, R. Jankowski, J.C. Nadal, M. Roecker- Cooper, C.C. Wood, and R.M. Naclerio Onset and duration of inhibition of ipratropium bromide nasal spray on methacholine-induced nasal secretions. Clin. Exp. Allergy. 24: Baroody, F.M., A.M. Majchel, M.M. Roecker, P.J. Roszko, E.C. Zegarelli, C.C. Wood, and R.M. Naclerio Ipratropium bromide (Atrovent nasal spray) reduces the nasal response to methacholine. J. Allergy Clin. Immunol. 89: Raphael, G.O., M.H. Raphael, and M.A. Kaliner Gustatory rhinitis: a syndrome of food-induced rhinorrhea. J. Allergy Clin. Immunol. 83: Gilligan, P.H Microbiology of airway disease in patients with cystic fibrosis. Clin. Microbiol. Rev. 4: Joris, L., I. Dab, and P.M. Quinton Elemental composition of human airway surface liquid in healthy and diseased airways. Am. Rev. Respir. Dis. 148: Smith, J.J., and M.J. Welsh Fluid and electrolyte transport by cultured human airway epithelia. J. Clin. Invest. 91: Goldman, M.J., G.M. Anderson, E.D. Stolzenberg, U.P. Kari, M. Zasloff, and J.M. Wilson Human beta-defensin-1 is a salt-sensitive antibiotic that is inactivated in cystic fibrosis. Cell. 88: Yager, D., T. Cloutier, H. Feldman, J. Bastacky, J.M. Drazen, and R.D. Kamm Airway surface liquid thickness as a function of lung volume in small airways of the guinea pig. J. Appl. Physiol. 77: Rahmoune, H., and K.L. Shephard State of airway surface liquid on guinea pig trachea. J. Appl. Physiol. 78: Widdicombe, J Airway and alveolar permeability and surface liquid thickness: theory. J. Appl. Physiol. 82: Smith, J.J., S.M. Travis, E.P. Greenberg, and M.J. Welsh Erratum. Cell Folkesson, H.G., M.A. Matthay, A. Frigeri, and A.S. Verkman Transepithelial water permeability in microperfused distal airways. Evidence for channel-mediated water transport. J. Clin. Invest. 97: Willumsen, N.J., C.W. Davis, and R.C. Boucher Selective response of human airway epithelia to luminal but not serosal solution hypertonicity: possible role for proximal airway epithelia as an osmolality transducer. J. Clin. Invest. 94: Gilljam, H., A. Ellin, and B. Strandvik Increased bronchial chloride concentration in cystic fibrosis. Scand. J. Clin. Lab. Invest. 49: Quinton, P.M., and M.M. Reddy The sweat gland. In Cystic Fibrosis. P.B. Davis, editor. Marcel Dekker, Inc. New York Burch, L., C. Talbot, M.R. Knowles, C. Canessa, B. Rossier, and R.C. Boucher Relative expression of the human epithelial Na channel (ENaC) sub-units in normal and cystic fibrosis airways. Am. J. Physiol. 269: C511 C Ballard, S.T., S.M. Schepens, J.C. Falcone, G.A. Meininger, and A.E. Taylor Regional bioelectric properties of porcine airway epithelium. J. Appl. Physiol. 73: Ion Composition of Airway Surface Liquid 2595
Journal of Physiology (1999), 516.3, pp Topical Review. Molecular insights into the physiology of the thin film of airway surface liquid
 Keywords: 9127 Journal of Physiology (1999), 516.3, pp. 631 638 631 Topical Review Molecular insights into the physiology of the thin film of airway surface liquid R. C. Boucher Cystic FibrosisÏPulmonary
Keywords: 9127 Journal of Physiology (1999), 516.3, pp. 631 638 631 Topical Review Molecular insights into the physiology of the thin film of airway surface liquid R. C. Boucher Cystic FibrosisÏPulmonary
Hypertonic saline alters ion transport across the human airway epithelium
 Eur Respir J 21; 17: 19 199 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Hypertonic saline alters ion transport across the human airway epithelium
Eur Respir J 21; 17: 19 199 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Hypertonic saline alters ion transport across the human airway epithelium
Relative Ion Permeability of Normal and Cystic Fibrosis Nasal Epithelium
 Relative Ion Permeability of Normal and Cystic Fibrosis Nasal Epithelium MICHAEL KNOWLES, JOHN GATZY, and RICHARD BOUCHER, Departments of Medicine and Pharmacology, School of Medicine, University of North
Relative Ion Permeability of Normal and Cystic Fibrosis Nasal Epithelium MICHAEL KNOWLES, JOHN GATZY, and RICHARD BOUCHER, Departments of Medicine and Pharmacology, School of Medicine, University of North
150 mm HCO How Does the Pancreas Do It? Clues from Computer Modelling of the Duct Cell
 JOP. J. Pancreas (Online) 2001; 2(4 Suppl):198202. 150 mm How Does the Pancreas Do It? Clues from Computer Modelling of the Duct Cell Yoshiro Sohma 1, Michael A Gray 2, Yusuke Imai 1, Barry E Argent 2
JOP. J. Pancreas (Online) 2001; 2(4 Suppl):198202. 150 mm How Does the Pancreas Do It? Clues from Computer Modelling of the Duct Cell Yoshiro Sohma 1, Michael A Gray 2, Yusuke Imai 1, Barry E Argent 2
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Increasing Concentration of Inhaled Saline with or without Amiloride Effect on Mucociliary Clearance in Normal Subjects
 Increasing Concentration of Inhaled Saline with or without Amiloride Effect on Mucociliary Clearance in Normal Subjects Namita Sood, William D. Bennett, Kirby Zeman, James Brown, Carla Foy, Richard C.
Increasing Concentration of Inhaled Saline with or without Amiloride Effect on Mucociliary Clearance in Normal Subjects Namita Sood, William D. Bennett, Kirby Zeman, James Brown, Carla Foy, Richard C.
Aerosol Therapy. Aerosol Therapy. RSPT 1410 Humidity & Aerosol Therapy Part 4
 1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
We describe a novel student course in membrane physiology in which
 MEASUREMENT OF HUMAN NASAL POTENTIAL DIFFERENCE TO TEACH THE THEORY OF TRANSEPITHELIAL FLUID TRANSPORT Ulrich Kersting, 1 Albrecht Schwab, 2 and Alexandra Hebestreit 3 1 Institute of Clinical Biochemistry
MEASUREMENT OF HUMAN NASAL POTENTIAL DIFFERENCE TO TEACH THE THEORY OF TRANSEPITHELIAL FLUID TRANSPORT Ulrich Kersting, 1 Albrecht Schwab, 2 and Alexandra Hebestreit 3 1 Institute of Clinical Biochemistry
Respiratory Pharmacology: Treatment of Cystic Fibrosis
 Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
The Relative Roles of Passive Surface Forces and Active Ion Transport in the Modulation of Airway Surface Liquid Volume and Composition
 The Relative Roles of Passive Surface Forces and Active Ion Transport in the Modulation of Airway Surface Liquid Volume and Composition Robert Tarran, Barbara R. Grubb, John T. Gatzy, C. William Davis,
The Relative Roles of Passive Surface Forces and Active Ion Transport in the Modulation of Airway Surface Liquid Volume and Composition Robert Tarran, Barbara R. Grubb, John T. Gatzy, C. William Davis,
Effects of Topically Delivered Benzamil and Amiloride on Nasal Potential Difference in Cystic Fibrosis
 Effects of Topically Delivered Benzamil and Amiloride on Nasal Potential Difference in Cystic Fibrosis T. HOFMANN, M. J. STUTTS, A. ZIERSCH, C. RÜCKES, W. M. WEBER, M. R. KNOWLES, H. LINDEMANN, and R.
Effects of Topically Delivered Benzamil and Amiloride on Nasal Potential Difference in Cystic Fibrosis T. HOFMANN, M. J. STUTTS, A. ZIERSCH, C. RÜCKES, W. M. WEBER, M. R. KNOWLES, H. LINDEMANN, and R.
Applications of Freezing Point Osmometry
 Applications of Freezing Point Osmometry Table of Contents Chapter 1 Introduction and Basic Principles 1 Chapter 2 Biological Applications 3 2.1 Range of, and reason for, abnormal serum values 5 2.2 Osmolality
Applications of Freezing Point Osmometry Table of Contents Chapter 1 Introduction and Basic Principles 1 Chapter 2 Biological Applications 3 2.1 Range of, and reason for, abnormal serum values 5 2.2 Osmolality
Cystic Fibrosis the future
 Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
Evaluation of Patients with Diffuse Bronchiectasis
 Evaluation of Patients with Diffuse Bronchiectasis Dr. Patricia Eshaghian, MD Assistant Clinical Professor of Medicine Director, UCLA Adult Cystic Fibrosis Affiliate Program UCLA Division of Pulmonary
Evaluation of Patients with Diffuse Bronchiectasis Dr. Patricia Eshaghian, MD Assistant Clinical Professor of Medicine Director, UCLA Adult Cystic Fibrosis Affiliate Program UCLA Division of Pulmonary
1. Introduction. Obstructive lung disease remains the leading cause of morbidity and mortality in cystic fibrosis
 1. Introduction Obstructive lung disease remains the leading cause of morbidity and mortality in cystic fibrosis (CF) [1]. With time it has become increasingly clear that CF lung disease is present very
1. Introduction Obstructive lung disease remains the leading cause of morbidity and mortality in cystic fibrosis (CF) [1]. With time it has become increasingly clear that CF lung disease is present very
Hypertonic Saline (7%) Administration Guideline (adults)
 Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions
 CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
Respiratory System. Organization of the Respiratory System
 Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis
 ORIGINAL ARTICLE INFECTIOUS DISEASES Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis Z. Luo, Z. Fu, E. Liu, X. Xu, X. Fu, D. Peng, Y. Liu, S.
ORIGINAL ARTICLE INFECTIOUS DISEASES Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis Z. Luo, Z. Fu, E. Liu, X. Xu, X. Fu, D. Peng, Y. Liu, S.
P.G. Middleton, D.M. Geddes, E.W.F.W Alton
 Eur Respir J, 1994, 7, 2 26 DO: 1.1183/931936.94.7112 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal SSN 93-1936 RAPD COMMUNCAON Protocols for in vivo
Eur Respir J, 1994, 7, 2 26 DO: 1.1183/931936.94.7112 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal SSN 93-1936 RAPD COMMUNCAON Protocols for in vivo
Early Studies. Then, the Meta-analysis. Recent Studies Al-Ansari. Recent Studies Luo University of Texas Health Science Center at San Antonio
 Pediatrics Grand Rounds Objectives Review the available literature on the use of nebulized hypertonic saline in the treatment of acute viral bronchiolitis Review proposed mechanism(s) of action and safety
Pediatrics Grand Rounds Objectives Review the available literature on the use of nebulized hypertonic saline in the treatment of acute viral bronchiolitis Review proposed mechanism(s) of action and safety
FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC
 FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC N. Somu D. Vijayasekaran T.P. Ashok A. Balachandran L. Subramanyam ABSTRACT The value of route, sedation and
FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC N. Somu D. Vijayasekaran T.P. Ashok A. Balachandran L. Subramanyam ABSTRACT The value of route, sedation and
TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Chapter 4 Cell Membrane Transport
 Chapter 4 Cell Membrane Transport Plasma Membrane Review o Functions Separate ICF / ECF Allow exchange of materials between ICF / ECF such as obtaining O2 and nutrients and getting rid of waste products
Chapter 4 Cell Membrane Transport Plasma Membrane Review o Functions Separate ICF / ECF Allow exchange of materials between ICF / ECF such as obtaining O2 and nutrients and getting rid of waste products
HANS H. USSING, THOMAS U. L. BIBER, and NEAL S. BRICKER
 Exposure of the Isolated Frog Skin to High Potassium Concentrations at the Internal Surface II. Changes in epithelial cell volume, resistance, and response to antidiuretic hormone HANS H. USSING, THOMAS
Exposure of the Isolated Frog Skin to High Potassium Concentrations at the Internal Surface II. Changes in epithelial cell volume, resistance, and response to antidiuretic hormone HANS H. USSING, THOMAS
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Characterization of Ion and Fluid Transport in Human Bronchioles
 Characterization of Ion and Fluid Transport in Human Bronchioles Sabine Blouquit, Hugues Morel, Jocelyne Hinnrasky, Emmanuel Naline, Edith Puchelle, and Thierry Chinet Laboratoire de Biologie et Pharmacologie
Characterization of Ion and Fluid Transport in Human Bronchioles Sabine Blouquit, Hugues Morel, Jocelyne Hinnrasky, Emmanuel Naline, Edith Puchelle, and Thierry Chinet Laboratoire de Biologie et Pharmacologie
Loss of CFTR Chloride Channels Alters Salt Absorption by Cystic Fibrosis Airway Epithelia In Vitro
 Molecular Cell, Vol. 2, 397 403, September, 1998, Copyright 1998 by Cell Press Loss of CFTR Chloride Channels Alters Salt Absorption by Cystic Fibrosis Airway Epithelia In Vitro Joseph Zabner, 1,7 Jeffrey
Molecular Cell, Vol. 2, 397 403, September, 1998, Copyright 1998 by Cell Press Loss of CFTR Chloride Channels Alters Salt Absorption by Cystic Fibrosis Airway Epithelia In Vitro Joseph Zabner, 1,7 Jeffrey
Bronchoscopy: approaches to evaluation and sampling
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Bronchoscopy: approaches to evaluation and sampling Author : Simon Tappin Categories : Companion animal, Vets Date : December
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Bronchoscopy: approaches to evaluation and sampling Author : Simon Tappin Categories : Companion animal, Vets Date : December
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
What is Cystic Fibrosis? CYSTIC FIBROSIS. Genetics of CF
 What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
EFFECT OF CARBENOXOLONE ON THE GASTRIC MUCOSAL BARRIER IN MAN AFTER ADMINISTRATION OF TAUROCHOLIC ACID
 GASTROENTEROLOGY 64: 1101-1105, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64 No.6 Printed in U.S.A. EFFECT OF CARBENOXOLONE ON THE GASTRIC MUCOSAL BARRIER IN MAN AFTER ADMINISTRATION OF TAUROCHOLIC
GASTROENTEROLOGY 64: 1101-1105, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64 No.6 Printed in U.S.A. EFFECT OF CARBENOXOLONE ON THE GASTRIC MUCOSAL BARRIER IN MAN AFTER ADMINISTRATION OF TAUROCHOLIC
Abnormal Apical Cell Membrane in Cystic Fibrosis Respiratory Epithelium An In Vitro Electrophysiologic Analysis
 Abnormal Apical Cell Membrane in Cystic Fibrosis Respiratory Epithelium An In Vitro Electrophysiologic Analysis C. U. Cotton, M. J. Stutts, M. R. Knowles, J. T. Gatzy, and R. C. Boucher Division ofpulmonary
Abnormal Apical Cell Membrane in Cystic Fibrosis Respiratory Epithelium An In Vitro Electrophysiologic Analysis C. U. Cotton, M. J. Stutts, M. R. Knowles, J. T. Gatzy, and R. C. Boucher Division ofpulmonary
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
The Amiloride-inhibitable Na
 The Amiloride-inhibitable Na Conductance Is Reduced by the Cystic Fibrosis Transmembrane Conductance Regulator in Normal But Not in Cystic Fibrosis Airways M. Mall, M. Bleich, R. Greger, R. Schreiber,
The Amiloride-inhibitable Na Conductance Is Reduced by the Cystic Fibrosis Transmembrane Conductance Regulator in Normal But Not in Cystic Fibrosis Airways M. Mall, M. Bleich, R. Greger, R. Schreiber,
New Models of the Tracheal Airway Define the Glandular Contribution to Airway Surface Fluid and Electrolyte Composition
 New Models of the Tracheal Airway Define the Glandular Contribution to Airway Surface Fluid and Electrolyte Composition Xiaorong Wang, Yulong Zhang, Anson Amberson, and John F. Engelhardt Departments of
New Models of the Tracheal Airway Define the Glandular Contribution to Airway Surface Fluid and Electrolyte Composition Xiaorong Wang, Yulong Zhang, Anson Amberson, and John F. Engelhardt Departments of
Selective Activation of Cystic Fibrosis Transmembrane Conductance Regulator Cl - and HCO 3 - Conductances
 JOP. J. Pancreas (Online) 2001; 2(4 Suppl):212218. Selective Activation of Cystic Fibrosis Transmembrane Conductance Regulator Cl and HCO 3 Conductances MallaReddy M Reddy 1, Paul M Quinton 1,2 1 Department
JOP. J. Pancreas (Online) 2001; 2(4 Suppl):212218. Selective Activation of Cystic Fibrosis Transmembrane Conductance Regulator Cl and HCO 3 Conductances MallaReddy M Reddy 1, Paul M Quinton 1,2 1 Department
Cl - channel regulated by camp-dependent phosphorylation
 Defective Fluid Transport by Cystic Fibrosis Airway pithelia Rapid Publication Jeffrey J. Smith, Philip H. Karp,* and Michael J. Welsh* Department ofpediatrics and *Howard Hughes Medical Institute, Departments
Defective Fluid Transport by Cystic Fibrosis Airway pithelia Rapid Publication Jeffrey J. Smith, Philip H. Karp,* and Michael J. Welsh* Department ofpediatrics and *Howard Hughes Medical Institute, Departments
Cellular Physiology. Body Fluids: 1) Water: (universal solvent) Body water varies based on of age, sex, mass, and body composition
 Membrane Physiology Body Fluids: 1) Water: (universal solvent) Body water varies based on of age, sex, mass, and body composition H 2 O ~ 73% body weight Low body fat; Low bone mass H 2 O ( ) ~ 60% body
Membrane Physiology Body Fluids: 1) Water: (universal solvent) Body water varies based on of age, sex, mass, and body composition H 2 O ~ 73% body weight Low body fat; Low bone mass H 2 O ( ) ~ 60% body
There is a substantial need for new biomarkers. Absorptive clearance of DTPA as an aerosol-based biomarker in the cystic fibrosis airway
 Eur Respir J 2010; 35: 781 786 DOI: 10.1183/09031936.00059009 CopyrightßERS Journals Ltd 2010 Absorptive clearance of DTPA as an aerosol-based biomarker in the cystic fibrosis airway T.E. Corcoran*, K.M.
Eur Respir J 2010; 35: 781 786 DOI: 10.1183/09031936.00059009 CopyrightßERS Journals Ltd 2010 Absorptive clearance of DTPA as an aerosol-based biomarker in the cystic fibrosis airway T.E. Corcoran*, K.M.
The Human Respiration System
 The Human Respiration System Nasal Passage Overall function is to filter, warm and moisten air as it enters the body. The nasal passages are the primary site of air movement we tend to be nose breathers.
The Human Respiration System Nasal Passage Overall function is to filter, warm and moisten air as it enters the body. The nasal passages are the primary site of air movement we tend to be nose breathers.
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Correspondence: Dr Sushil K. Kabra, Professor, Department of Pediatrics, AIIMS, New Delhi , India.
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
High blood pressure is common in black people living in
 Transepithelial Sodium Absorption Is Increased in People of African Origin Emma H. Baker, Nicola J. Ireson, Christine Carney, Nirmala D. Markandu, Graham A. MacGregor Abstract Salt-sensitive hypertension
Transepithelial Sodium Absorption Is Increased in People of African Origin Emma H. Baker, Nicola J. Ireson, Christine Carney, Nirmala D. Markandu, Graham A. MacGregor Abstract Salt-sensitive hypertension
Mouse C-Peptide ELISA Kit
 Mouse C-Peptide ELISA Kit Cat.No: DEIA4507 Lot. No. (See product label) Size 96T Intended Use The Mouse C-Peptide ELISA kit is for the quantitative determination of c-peptide in mouse serum, plasma, and
Mouse C-Peptide ELISA Kit Cat.No: DEIA4507 Lot. No. (See product label) Size 96T Intended Use The Mouse C-Peptide ELISA kit is for the quantitative determination of c-peptide in mouse serum, plasma, and
CF: Understanding the Biology Curing the Disease
 CF: Understanding the Biology Curing the Disease Scott H. Donaldson, MD Associate Professor of Medicine Director, Adult CF Care Center University of North Carolina at Chapel Hill Defining the path Drilling
CF: Understanding the Biology Curing the Disease Scott H. Donaldson, MD Associate Professor of Medicine Director, Adult CF Care Center University of North Carolina at Chapel Hill Defining the path Drilling
Mucus clearance as a primary innate defense mechanism for mammalian airways
 PERSPECTIVE SERIES Innate defenses in the lung Jeffrey A. Whitsett, Series Editor Mucus clearance as a primary innate defense mechanism for mammalian airways Michael R. Knowles and Richard C. Boucher Cystic
PERSPECTIVE SERIES Innate defenses in the lung Jeffrey A. Whitsett, Series Editor Mucus clearance as a primary innate defense mechanism for mammalian airways Michael R. Knowles and Richard C. Boucher Cystic
Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis
 Acta Biomed 2014; Vol. 85, Supplement 4: 10-18 Mattioli 1885 Original article Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis Azienda Ospedaliero Universitaria Policlinico, DAI Scienze
Acta Biomed 2014; Vol. 85, Supplement 4: 10-18 Mattioli 1885 Original article Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis Azienda Ospedaliero Universitaria Policlinico, DAI Scienze
Day-to-day management of Tracheostomies & Laryngectomies
 Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
squamous-cell carcinoma1
 Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
Purity Tests for Modified Starches
 Residue Monograph prepared by the meeting of the Joint FAO/WHO Expert Committee on Food Additives (JECFA), 82 nd meeting 2016 Purity Tests for Modified Starches This monograph was also published in: Compendium
Residue Monograph prepared by the meeting of the Joint FAO/WHO Expert Committee on Food Additives (JECFA), 82 nd meeting 2016 Purity Tests for Modified Starches This monograph was also published in: Compendium
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS
 Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
中国科技论文在线. * CFTR cl - [5]
![中国科技论文在线. * CFTR cl - [5] 中国科技论文在线. * CFTR cl - [5]](/thumbs/91/105488871.jpg) CFTR 1 * 410078 *E-mailxiaoqun1988@xysm.net CFTR PCR western blot CFTR CFTR cl - CFTR Real-time PCR 4h CFTR mrna CFTR Western blot 4h CFTR CFTR cl - 5 µm forskolin CFTR cl - forskolin 4h BECs CFTR cl -
CFTR 1 * 410078 *E-mailxiaoqun1988@xysm.net CFTR PCR western blot CFTR CFTR cl - CFTR Real-time PCR 4h CFTR mrna CFTR Western blot 4h CFTR CFTR cl - 5 µm forskolin CFTR cl - forskolin 4h BECs CFTR cl -
A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis
 A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis Edwin A. Bronsky, MD, Howard Druce, MD, Steven R. Findlay, MD, Frank C. Hampel, MD, Harold Kaiser, MD,
A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis Edwin A. Bronsky, MD, Howard Druce, MD, Steven R. Findlay, MD, Frank C. Hampel, MD, Harold Kaiser, MD,
Preventive but Not Late Amiloride Therapy Reduces Morbidity and Mortality of Lung Disease in benac-overexpressing Mice
 Preventive but Not Late Amiloride Therapy Reduces Morbidity and Mortality of Lung Disease in benac-overexpressing Mice Zhe Zhou 1 *, Diana Treis 1 *, Susanne C. Schubert 1, Maria Harm 1, Jolanthe Schatterny
Preventive but Not Late Amiloride Therapy Reduces Morbidity and Mortality of Lung Disease in benac-overexpressing Mice Zhe Zhou 1 *, Diana Treis 1 *, Susanne C. Schubert 1, Maria Harm 1, Jolanthe Schatterny
Cell Membranes, Epithelial Barriers and Drug Absorption p. 1 Introduction p. 2 The Plasma Membrane p. 2 The phospholipid bilayer p.
 Cell Membranes, Epithelial Barriers and Drug Absorption p. 1 Introduction p. 2 The Plasma Membrane p. 2 The phospholipid bilayer p. 3 Dynamic behaviour of membranes p. 4 Modulation of membrane fluidity
Cell Membranes, Epithelial Barriers and Drug Absorption p. 1 Introduction p. 2 The Plasma Membrane p. 2 The phospholipid bilayer p. 3 Dynamic behaviour of membranes p. 4 Modulation of membrane fluidity
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
National Horizon Scanning Centre. Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis. April 2008
 Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Aerosolized Antibiotics in Mechanically Ventilated Patients
 Aerosolized Antibiotics in Mechanically Ventilated Patients Gerald C Smaldone MD PhD Introduction Topical Delivery of Antibiotics to the Lung Tracheobronchitis Aerosolized Antibiotic Delivery in the Medical
Aerosolized Antibiotics in Mechanically Ventilated Patients Gerald C Smaldone MD PhD Introduction Topical Delivery of Antibiotics to the Lung Tracheobronchitis Aerosolized Antibiotic Delivery in the Medical
Product Size Catalog Number
 Epithelial Cells Instruction Manual Product Size Catalog Number Human Nasal Epithelial Cells (HNEpC) Human Tracheal Epithelial Cells (HTEpC) Human Bronchial Epithelial Cells (HBEpC) Human Small Airway
Epithelial Cells Instruction Manual Product Size Catalog Number Human Nasal Epithelial Cells (HNEpC) Human Tracheal Epithelial Cells (HTEpC) Human Bronchial Epithelial Cells (HBEpC) Human Small Airway
7/12/2012. Respiratory system. Respiratory Response to Toxic Injury (Lung) Ninth Industrial Toxicology and Pathology Short Course.
 Ninth Industrial Toxicology and Pathology Short Course 23 27 July, 2012 Contemporary Concepts in Target Organ Toxicologic Pathology Respiratory system Respiratory Response to Toxic Injury (Lung) Eric Wheeldon
Ninth Industrial Toxicology and Pathology Short Course 23 27 July, 2012 Contemporary Concepts in Target Organ Toxicologic Pathology Respiratory system Respiratory Response to Toxic Injury (Lung) Eric Wheeldon
Thawing. 10,000-15,000 cells per cm² 10,000-15,000 cells per cm² C ,000-15,000 cells per cm². Product Size Catalog Number
 5 Instruction Manual Epithelial Cells Specifications Product Recommended Culture Media* Plating Density Passage after Thawing Marker Population Doublings Human Nasal Epithelial Cells (HNEpC) Human Tracheal
5 Instruction Manual Epithelial Cells Specifications Product Recommended Culture Media* Plating Density Passage after Thawing Marker Population Doublings Human Nasal Epithelial Cells (HNEpC) Human Tracheal
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Effect of Luminal Sodium Concentration
 Effect of Luminal Sodium Concentration on Bicarbonate Absorption in Rat Jejunum KENNETH A. HUBEL From the Department of Medicine, University of Iowa, Iowa City, Iowa 52242 A B S T R A C T An exchange of
Effect of Luminal Sodium Concentration on Bicarbonate Absorption in Rat Jejunum KENNETH A. HUBEL From the Department of Medicine, University of Iowa, Iowa City, Iowa 52242 A B S T R A C T An exchange of
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Physiology of the body fluids, Homeostasis
 Physiology of the body fluids, Homeostasis Tamas Banyasz The Body as an open system 1. Open system: The body exchanges material and energy with its environment 2. Homeostasis: The process through which
Physiology of the body fluids, Homeostasis Tamas Banyasz The Body as an open system 1. Open system: The body exchanges material and energy with its environment 2. Homeostasis: The process through which
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage)
 NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always
 1 3 4 5 6 7 8 9 10 Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always take appropriate Standard measures
1 3 4 5 6 7 8 9 10 Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always take appropriate Standard measures
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Mucus Clearance and Lung Function in Cystic Fibrosis with Hypertonic Saline
 The new england journal of medicine original article Mucus Clearance and Lung Function in Cystic Fibrosis with Hypertonic Saline Scott H. Donaldson, M.D., William D. Bennett, Ph.D., Kirby L. Zeman, Ph.D.,
The new england journal of medicine original article Mucus Clearance and Lung Function in Cystic Fibrosis with Hypertonic Saline Scott H. Donaldson, M.D., William D. Bennett, Ph.D., Kirby L. Zeman, Ph.D.,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
GSI Canine IL-5 ELISA Kit-2 Plates DataSheet
 Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Function: to supply blood with, and to rid the body of
 1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
Pharmacokinetic Phase
 RSPT 2317 Principles of Drug Action Part 2: The Pharmacokinetic Phase Pharmacokinetic Phase This phase describes the time course and disposition of a drug in the body, based on its absorption, distribution,
RSPT 2317 Principles of Drug Action Part 2: The Pharmacokinetic Phase Pharmacokinetic Phase This phase describes the time course and disposition of a drug in the body, based on its absorption, distribution,
Lab 4: Osmosis and Diffusion
 Page 4.1 Lab 4: Osmosis and Diffusion Cells need to obtain water and other particles from the fluids that surround them. Water and other particles also move out of cells. Osmosis (for water) and diffusion
Page 4.1 Lab 4: Osmosis and Diffusion Cells need to obtain water and other particles from the fluids that surround them. Water and other particles also move out of cells. Osmosis (for water) and diffusion
CYSTIC FIBROSIS OBJECTIVES NO CONFLICT OF INTEREST TO DISCLOSE
 CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
The average potassium content during the last 5. solids. This average decrease of 2.2 meq. per 100. initial potassium content of the arteries.
 THE EFFECT OF NOR-EPINEPHRINE ON THE ELECTROLYTE COMPOSITION OF ARTERIAL SMOOTH MUSCLE' By LOUIS TOBIAN 2 AND ADACIE FOX (From the Departments of Pharmacology and Internal Medicine, Southwesters Medical
THE EFFECT OF NOR-EPINEPHRINE ON THE ELECTROLYTE COMPOSITION OF ARTERIAL SMOOTH MUSCLE' By LOUIS TOBIAN 2 AND ADACIE FOX (From the Departments of Pharmacology and Internal Medicine, Southwesters Medical
ACETYLSALICYLIC ACID AND IONIC FLUXES ACROSS THE GASTRIC MUCOSA OF MAN
 GASTROENTEROLOGY Copyright 1968 by The Williams & Wilkins Co. Vol. 54, No.4, Part 1 of 2 Parts Printed in U.S.A. ACETYLSALICYLIC ACID AND IONIC FLUXES ACROSS THE GASTRIC MUCOSA OF MAN BERGEIN F. OVERHOLT,
GASTROENTEROLOGY Copyright 1968 by The Williams & Wilkins Co. Vol. 54, No.4, Part 1 of 2 Parts Printed in U.S.A. ACETYLSALICYLIC ACID AND IONIC FLUXES ACROSS THE GASTRIC MUCOSA OF MAN BERGEIN F. OVERHOLT,
Transport of Solutes and Water
 Transport of Solutes and Water Across cell membranes 1. Simple and Facilitated diffusion. 2. Active transport. 3. Osmosis. Simple diffusion Simple diffusion - the red particles are moving from an area
Transport of Solutes and Water Across cell membranes 1. Simple and Facilitated diffusion. 2. Active transport. 3. Osmosis. Simple diffusion Simple diffusion - the red particles are moving from an area
Worth Its SALT? Hypertonic Saline Revisited
 Worth Its SALT? Hypertonic Saline Revisited 1 NYC Long Island Michael McPeck, RRT FAARC Aerosol Research Scientist Aerosol Laboratory Division of Pulmonary, Critical Care & Sleep Medicine State University
Worth Its SALT? Hypertonic Saline Revisited 1 NYC Long Island Michael McPeck, RRT FAARC Aerosol Research Scientist Aerosol Laboratory Division of Pulmonary, Critical Care & Sleep Medicine State University
NURSE-UP RESPIRATORY SYSTEM
 NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Ch 3 Membrane Transports
 Ch 3 Membrane Transports what's so dynamic about cell membranes? living things get nutrients and energy from the envrionment this is true of the entire organism and each cell this requires transport in/out
Ch 3 Membrane Transports what's so dynamic about cell membranes? living things get nutrients and energy from the envrionment this is true of the entire organism and each cell this requires transport in/out
ORIGINAL ARTICLE. Potential Role of Abnormal Ion Transport in the Pathogenesis of Chronic Sinusitis
 ORIGINAL ARTICLE Potential Role of Abnormal Ion Transport in the Pathogenesis of Chronic Sinusitis Kenji Dejima, MD; Scott H. Randell, PhD; M. Jackson Stutts, PhD; Brent A. Senior, MD; Richard C. Boucher,
ORIGINAL ARTICLE Potential Role of Abnormal Ion Transport in the Pathogenesis of Chronic Sinusitis Kenji Dejima, MD; Scott H. Randell, PhD; M. Jackson Stutts, PhD; Brent A. Senior, MD; Richard C. Boucher,
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
4.6 Small airways disease
 4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
(Received 22 July 1957) It is now generally accepted that the unequal distribution of ions between cells
 190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
The absorption of water from the whole stomach. or one of its parts has not been demonstrated. Many years ago Pavlov showed that water was a
 GASTRIC SECRETION. III. THE ABSORPTION OF HEAVY WATER FROM POUCHES OF THE BODY AND ANTRUM OF THE STOMACH OF THE DOG By OLIVER COPE, HESTER BLATT, AND MARGARET R. BALL (From the Surgical Research Laboratories
GASTRIC SECRETION. III. THE ABSORPTION OF HEAVY WATER FROM POUCHES OF THE BODY AND ANTRUM OF THE STOMACH OF THE DOG By OLIVER COPE, HESTER BLATT, AND MARGARET R. BALL (From the Surgical Research Laboratories
