Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure
|
|
|
- Kristian Anthony
- 6 years ago
- Views:
Transcription
1 Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure Shigeki Matsubara 1, Christina H. Swasey 1, Joan E. Loader 1, Azzeddine Dakhama 1, Anthony Joetham 1, Hiroshi Ohnishi 1, Annette Balhorn 1, Nobuaki Miyahara 1, Katsuyuki Takeda 1, and Erwin W. Gelfand 1 1 Division of Cell Biology, Department of Pediatrics, National Jewish Medical and Research Center, Denver, Colorado The female hormone estrogen is an important factor in the regulation of airway function and inflammation, and sex differences in the prevalence of asthma are well described. Using an animal model, we determined how sex differences may underlie the development of altered airway function in response to allergen exposure. We compared sex differences in the development of airway hyperresponsiveness (AHR) after allergen exposure exclusively via the airways. Ovalbumin (OVA) was administered by nebulization on 10 consecutive days in BALB/c mice. After methacholine challenge, significant AHR developed in male mice but not in female mice. Ovariectomized female mice showed significant AHR after 10-day OVA inhalation. ICI182,780, an estrogen antagonist, similarly enhanced airway responsiveness even when administered 1 hour before assay. In contrast, 17b-estradiol dose-dependently suppressed AHR in male mice. In all cases, airway responsiveness was inhibited by the administration of a neurokinin 1 receptor antagonist. These results demonstrate that sex differences in 10-day OVAinduced AHR are due to endogenous estrogen, which negatively regulates airway responsiveness in female mice. Cumulatively, the results suggest that endogenous estrogen may regulate the neurokinin 1 dependent prejunctional activation of airway smooth muscle in allergen-exposed mice. Keywords: estrogen; sex; airway hyperresponsiveness; EFS; neuronal activation (Received in original form August 3, 2007 and in final form November 21, 2007) This work was supported by National Institutes of Health grants HL and HL and by Environmental Protection Agency grant R The content is solely the responsibility of the authors and does not necessarily represent the official views of the NHLBI or the NIH. Correspondence and requests for reprints should be addressed to Erwin W. Gelfand, M.D., National Jewish Medical and Research Center, 1400 Jackson Street, Denver, CO gelfande@njc.org Am J Respir Cell Mol Biol Vol 38. pp , 2008 Originally Published in Press as DOI: /rcmb OC on December 6, 2007 Internet address: CLINICAL RELEVANCE Sex differences impact asthma. For the first time, a mechanism demonstrating the ability of estrogen to regulate an NK-1 dependent pathway has been identified. Interventions targeting this pathway may affect asthma outcomes. Sex differences have been described to play a role in various diseases, including atherosclerosis (1), osteoporosis (2), and certain neurologic disorders (3). Accumulating evidence suggests that hormonal factors are important in the expression of such sex differences at the phenotypic and genotypic levels. A number of epidemiologic and experimental reports suggest that the female hormone estrogen is an important factor in the regulation of airway function and inflammation. Estrogen can prevent cholinergic constriction of asthmatic tracheal rings in vitro (4), and estrogen treatment decreases airway responsiveness to acetylcholine in ovariectomized rats (5). On the other hand, female mice may be more susceptible than male mice to allergen-induced airway inflammation (6 8). The role of estrogen on sex differences in asthma has been the subject of much discussion (9, 10). There are many animal protocols for investigating allergeninduced airway hyperresponsiveness (AHR) and inflammation, with the majority using initial sensitization to allergen together with an adjuvant such as alum. Using this sensitization approach, some mouse studies have suggested a female superiority in the development of allergic airway inflammation (6 8). We examined the development of AHR after allergen exposure exclusively via the airways for 10 consecutive days in the absence of any adjuvant. Although AHR to inhaled methacholine (MCh) was not detected in female mice after 10-day ovalbumin (OVA) inhalation in vivo, electrical field stimulation (EFS) in vitro detected altered airway responsiveness. In large part, this EFS response has been attributed to muscarinic receptor dysfunction, activation of neurokinin 1 (NK-1) dependent pathways, and increased acetylcholine (ACh) release (11, 12). In the present study, we identified major differences in the development of MCh-induced alterations in airway resistance (R L ) and dynamic compliance (C dyn ) after 10-day OVA inhalation between male and female mice. The aim of the present study was to compare the mechanism(s) underlying this sex difference and demonstrate that one of the sex hormones, estrogen, regulates the development of AHR after allergen exposure in female mice. The data suggest that estrogen may inhibit the activation of NK-1 related prejunctional pathways, which are enhanced by allergen exposure. MATERIALS AND METHODS Animals Female and male BALB/c mice, 8 to 10 weeks of age (Jackson Laboratories, Bar Harbor, ME) were maintained on an OVA-free diet. All experimental animals used in this study were under a protocol approved by the Institutional Animal Care and Use Committee of the National Jewish Medical and Research Center. Ovariectomy Female mice at 5 to 6 weeks of age were anesthetized by intraperitoneal injection of 50 mg/kg of pentobarbital sodium and underwent ovariectomy (OVX) using a dorsolateral approach. Sham operation and OVX were performed at least 2 weeks before initiation of the experiments. OVA Exposure Without Adjuvant Experimental groups consisted of four mice per group, and each experiment was performed at least twice. Mice were exposed to OVA (albumin from chicken egg white, Grade V; Sigma, St. Louis, MO) as described previously (13). Briefly, a solution of 0.9% saline or endotoxindepleted 1% OVA solution was delivered by ultrasonic nebulization (Omron, Kyoto, Japan) for 20 minutes daily over 10 consecutive days in a closed chamber. Twenty-four hr after the last airway challenge, airway responsiveness was assessed in vivo and in vitro, and bronchoalveolar lavage fluid (BALF), blood, and lung tissue were collected.
2 502 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Drugs ICI182,780, an estrogen receptor antagonist (Tocris Bioscience, Ellisville, MO) and 17b-estradiol (E2; Sigma) were suspended in 0.1% Tween 80 containing phosphate-buffered saline at concentrations of 10 ml/kg and 50 to 100 mg/kg body weight. The highly selective NK-1 receptor antagonist Sendide was obtained from Bachem California (Torrance, CA). The estrogen receptor antagonist ICI182,780 was administered intraperitoneally immediately before each OVA inhalation or 1 hour before determination of AHR to inhaled MCh (Sigma). Sendide was administered intraperitoneally 2 hours before determination of AHR. Determination of Airway Responsiveness R L and C dyn were determined as changes in airway function after aerosolized MCh challenge in vivo. Mice were anesthetized with sodium pentobarbital (90 mg/kg, intraperitoneally), tracheostomized, and mechanically ventilated at a rate of 160 breaths/minute with a constant tidal volume of air (0.2 ml). Lung function was assessed as previously described (14). Aerosolized MCh was administered for eight breaths at a rate of 60 breaths/min, tidal volume of 500 ml by a second ventilator (Model 683; Harvard Apparatus, South Natick, MA) in increasing concentrations (1.6, 3.1, 6.3, and 12.5 mg/ml). After each MCh challenge, the data were continuously collected for 1 to 5 minutes, and maximum values of R L and minimum values for C dyn were obtained. For determination of airway responsiveness in vitro, airway responsiveness was assessed by measuring airway smooth muscle (tracheal rings) responsiveness to carbachol (CCh) (Sigma) and EFS 24 hours after the last airway challenge. CCh challenge was performed with increasing doses of the drug from to M. EFS was administered with an increasing frequency from 0.5 to 30 Hz. We have established earlier (15) that the EFS at the frequency range and mode used stimulates cholinergic fibers causing release of endogenous acetylcholine which mediates airway smooth muscle contraction; the EFS response is abolished in the presence of atropine. The effective concentrations of CCh resulting in 50% of the maximal contraction (EC 50 ) and the electrical frequency resulting in 50% of the maximal contraction (ES 50 ) were calculated from linear plots for each individual animal and were compared between the groups. Measurement of Total and OVA-Specific Immunoglobulin E Serum levels of total immunoglobulin (Ig)E and OVA-specific IgE were measured by enzyme-linked immunosorbent assay (ELISA) as described (13). The OVA-specific IgE titers of the samples were related to pooled standards that were generated in the laboratory and expressed as ELISA units per milliliter. Total IgE levels were calculated by comparison with known mouse IgE standards (BD Pharmingen, San Diego, CA). The limit of detection was 100 pg/ml for total IgE. Determination of Cell Numbers and Cytokine Levels in BALF Immediately after the assessment of AHR, lungs were lavaged via the tracheal cannula with Hanks balanced salt solution (1 ml/mouse). Total leukocyte numbers were measured with a Coulter Counter (Coulter Corporation, Hialeah, FL). Differential cell counts were made from cytocentrifuged preparations using a Cytospin 2 (Shandon Ltd., Runcorn, Cheshire, UK) and stained with Leukostat (Fisher Diagnostics, Pittsburgh, PA). At least 200 cells were counted under 4003 magnification. Bronchoalveolar lavage (BAL) supernatants were collected and kept frozen at 2808C until assayed. The levels of cytokine in the supernatants of BALF samples were determined by ELISA. IL-4, IL-5, IL-12 (p70), IFN-g (all from BD Pharmingen) and IL-13 (R&D Systems, Minneapolis, MN) were measured following the manufacturers directions. The limits of detection were 4 pg/ml for IL-4 and IL- 5, 1.5 pg/ml for IL-13, and 15 pg/ml for IL-12 and IFN-g. Histopathologic Examination Lungs were fixed by inflation (1 ml/whole lung) and immersion in 10% formalin. Cells containing eosinophilic major basic protein were identified by immunohistochemical staining as previously described using rabbit anti-mouse major basic protein (provided by Dr. J. J. Lee, Mayo Clinic, Scottsdale, AZ). The slides were examined in a blinded fashion with a Nikon microscope (Melville, NY) equipped with a fluorescein filter system. For detection of mucus-containing cells in formalin-fixed airway tissue, sections were stained with periodic acid-schiff and H&E and quantitated as previously described (16). Data Analysis All parametric data were compared using Student s t test between two groups and Tukey-Kramer to compare multiple groups. Because measured values may not be normally distributed and due to the small sample sizes, nonparametric analysis using the Mann-Whitney U test was also used to confirm that the statistical differences remained significant. A P value of,0.05 was considered statistically significant. Values for all measurements were expressed as the mean 6 SEM. RESULTS Sex Differences after OVA Inhalation The extent of 10-day OVA-induced AHR to inhaled MCh in female and male BALB/c mice were compared. There were no significant differences in the baseline values between female and male mice. Responses in the 10-day saline-treated groups showed low level MCh dose-responsiveness for R L and C dyn in male and female mice (Figure 1A). After 10-day OVA inhalation, significant AHR to inhaled MCh was elicited in male mice, but not in female mice (Figure 1A). This 10-day exposure protocol was previously shown to elicit little in the way of BAL inflammatory cell accumulation and there were no differences between female and male mice (Figure 1B). Ten-day OVA inhalation elicited significant increases in numbers of goblet cells and eosinophils in the lung tissue but there were no differences in the numbers of these cells (comparing male and female mice) (Figure 1C). Neither OVA inhalation nor sex differences influenced the levels of IL-4, IL-5, IL-12, IL-13, or IFN-g in the BALF (data not shown). Serum levels of total IgE were significantly increased in both sexes after 10-day OVA inhalation; the baseline values for total IgE were higher in female than in male mice (Table 1). Serum levels of OVAspecific IgE were increased in both sexes after 10-day OVA inhalation, and no differences between the sexes were detected (Table 1). Airway Smooth Muscle Contractility To compare airway (tracheal) smooth muscle contractility, which may contribute to the development of AHR, CCh- and EFS-induced responses were evaluated in vitro and compared. The effective concentration required for EC 50 for CCh in salineand OVA-treated groups were and M in female mice, and and M in male mice, respectively (Figure 2), indicating no upregulation of cholinergic airway responsiveness after 10-day OVA inhalation in male or female mice. In contrast, the electrical frequency required for ES 50 in the saline- and OVAtreated groups were and Hz in females, and and Hz in males, respectively (Figure 2) demonstrating comparable and significant decreases in ES 50 values in both after 10-day OVA inhalation. Maximal contractile responses (Tmax) were also determined in both CCh- and EFS-induced response. However, no significant differences were observed in Tmax (data not shown) as previously reported (17). Development of AHR to Inhaled MCh in Ovariectomized Female Mice after 10-Day OVA Inhalation In Vivo Based on the MCh-induced AHR data distinguishing male and female mice, it appeared that there may be factors related to sex differences which regulate airway responsiveness in vivo, but not in vitro. We therefore evaluated the influence of OVX as
3 Matsubara, Swasey, Loader, et al.: Estrogen Regulates Allergic AHR 503 Figure 1. Comparison of airway responsiveness and inflammation in female and male mice after 10-day ovalbumin (OVA) inhalation. Female and male mice were exposed to either a 0.9% saline solution or a 1% OVA solution for 10 days (20 min/d). (A) Airway hyperresponsiveness (AHR) to inhaled methacholine (MCh) after 10- day OVA inhalation. AHR (airway resistance [R L ] and lung dynamic compliance [C dyn ]) to inhaled MCh was assayed 24 hours after the last OVA challenge. Circles, female mice; squares, male mice; open symbols, 10-day saline; solid symbols, 10-day OVA. (B) Bronchoalveolar lavage (BAL) cell composition after 10-day OVA inhalation. BAL fluid was recovered immediately after the AHR assay was completed. (C) Numbers of periodic acid-schiff positive and major basic protein positive cells. Results represent the mean 6 SEM (n 5 8). *P, 0.05 and **P, 0.01 versus 10-day saline exposure in each sex. ND 5 not detected. The baseline values of R L and C dyn were as follows: cm H 2 O/ml/second (n 5 16) and ml/cm H 2 O(n5 16) in female saline-treated mice, respectively; cm H 2 O/ml/s (n 5 12) and ml/cm H 2 O(n 5 12) in female OVA-treated mice, respectively; cm H 2 O/ml/second (n 5 16) and ml/cm H 2 O(n 5 16) in male saline-treated mice, respectively; cm H 2 O/ml/second (n 5 21) and ml/cm H 2 O(n 5 21) in male OVA-treated mice, respectively. BM 5 basement membrane. a means of reducing endogenous female hormone production (Figure 3). Sham-surgery female mice did not develop AHR after 10-day OVA inhalation and no differences were detected in OVX female mice after 10-day saline inhalation. However, airway responsiveness to inhaled MCh was significantly enhanced after 10-day OVA inhalation in the OVX mice, and this was reversed after E2 administration. These results suggested that hormonal factors derived from the ovary are directly (or indirectly) critical to regulating airway function in vivo after allergen challenge exclusively via the airways. These increases in AHR were not accompanied by any changes in BAL cell composition or cytokine levels (data not shown). Effect of an Estrogen Antagonist on 10-Day OVA-Induced AHR in Female Mice In Vivo TABLE 1. COMPARISON OF ENDOGENOUS IgE ANTIBODIES BETWEEN FEMALE AND MALE MICE AFTER 10-d OVALBUMIN INHALATION Treatment Total IgE (ng/ml) OVA-Specific IgE (EU/ml) Female saline Female OVA * * Male saline Male OVA * Definition of abbreviation: EU, ELISA units; IgG, immunoglobulin G; OVA, ovalbumin. * P, 0.01, statistically significant compared with saline group in each sex. P, 0.05, statistically significant compared with saline group in each sex. Estrogen is a leading candidate as the female hormonal factor produced and released from the ovaries. To define the differences between male and female mice, effects of an estrogen antagonist were evaluated on 10-day OVA-induced AHR to inhaled MCh in vivo. Ten-day vehicle and 10-day OVA treatment did not elicit significant AHR to MCh in female mice (Figure 4A). After daily administration of the estrogen receptor antagonist ICI182,780 (10 mg/kg/d, intraperitoneally) increases in R L were significantly enhanced in female mice but only in OVA-exposed and not saline-exposed mice (Figure 4A). In saline-exposed mice, administration of the estrogen receptor antagonist had no effect. In male mice, daily administration of this compound did not influence AHR (Figure 4B). Despite the increases in AHR in the estrogen receptor antagonist-treated female mice, no changes in BAL inflammatory cell composition or cytokine levels were detected (data not shown). Effect of Exogenous Estrogen on 10-Day OVA-Induced AHR in Male Mice In Vivo As significant AHR in vivo developed in male mice after 10-day OVA inhalation, we evaluated the effects of exogenous estrogen administration on this response. In male mice, administration of E2 suppressed the development of AHR after 10-day OVA inhalation in a dose-dependent manner, with complete attenuation of AHR at a dose of 100 mg/kg/d of E2 (Figure 5). Suppression of AHR was not accompanied by any changes in BAL cell accumulation or cytokine levels (data not shown). This suppression was reversed with daily coadministration of the estrogen receptor antagonist (10 mg/kg/d of ICI182,780 for 10 days), establishing the specificity of the exogenous estrogen effect (Figure 5). Together, these results demonstrate the negative regulatory effects of endogenous and exogenous estrogen on AHR in female and male mice, respectively.
4 504 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Figure 2. Tracheal smooth muscle responsiveness to carbachol (CCh) and electrical field stimulation (EFS) after 10-day OVA inhalation. (A) Representative CCh and EFS responses. Top panels: Solid circles, female saline; open squares, female OVA. Bottom panels: Solid circles, male saline; open squares, male OVA. (B) Summary of results of CCh- and EFS-induced contractility. Results represent the mean 6 SEM (n 5 8). **P, 0.01 statistically significant. NS 5 not significant. 95% confidence intervals overlapped among the groups. Acute Effects of an Estrogen Antagonist and Exogenous Estrogen on AHR to MCh after 10-Day OVA Inhalation In Vivo The results reported above were obtained in a protocol which saw the compounds administered on 10 consecutive days. To focus on the response targeted by estrogen, airway constriction, the estrogen antagonist or exogenous estrogen were administered 1 h before the AHR assay, and 24 hours after the last OVA inhalation. AHR to inhaled MCh did not appear in female mice after 10-day OVA inhalation with vehicle treatment (Figure 6A). ICI182,780 at a dose of 10 mg/kg administered 1 hour before assay, significantly enhanced airway responsiveness in female mice after 10-day OVA exposure (but not saline) (Figure 6A). In parallel, the increases in the response to inhaled MCh which developed in male mice after 10-day OVA inhalation, were totally suppressed when estrogen was given 1 hour before assay (Figure 6B). Based on these results and the absence of changes in BAL cell composition or cytokine levels, it appeared that endogenous or exogenous estrogen given after allergen exposure was completed, regulated airway contractility directly. In no case did the estrogen receptor antagonist or estrogen itself impact AHR in the absence of allergen exposure. Figure 3. Development of AHR to inhaled MCh after 10-day OVA inhalation in ovariectomized (OVX) female mice. Sham-operated or OVX female mice were exposed to 0.9% saline or 1% OVA solution for 10 days. AHR was assayed 24 hours after the last OVA challenge. Sham operation or OVX was performed at least 2 weeks before initiation of allergen exposure. 17b-estradiol (E2) at a dose of 100 mg/kg was administered intraperitoneally to OVX mice 1 hour before assay of AHR. Results represent the mean 6 SEM (n 5 8). **P, 0.01 versus sham/ OVA (open triangles) or OVX/saline (solid circles). # P, 0.05 and ## P, 0.01 versus sham/saline (open circles) or OVX/OVA/E2 (squares). Solid triangles, OVX/OVA. Effect of Exogenous Estrogen on CCh- and EFS-Induced Airway Constriction after 10-Day OVA Inhalation To directly investigate whether estrogen influences airway constriction directly, we examined the effects of estrogen on CCh- and EFS-induced airway constriction in 10-day saline- or OVA-exposed mice in vitro. Estrogen at a dose of 100 nm did not affect CCh- or EFS-induced constriction of trachea smooth muscle from mice exposed to 10-day saline inhalation, and no differences were observed between males and females (Figure 7A). However, ES 50 values were decreased in male and female mice after 10-day OVA exposure, and E2 dose-dependently
5 Matsubara, Swasey, Loader, et al.: Estrogen Regulates Allergic AHR 505 Figure 4. Estrogen receptor antagonist alters AHR in female mice. (A) Effect of daily administration of an estrogen antagonist on AHR in female mice. Open circles, 10 days saline/ 10 days vehicle; solid circles, 10 days OVA/10 days vehicle; open triangles, 10 days saline/ 10 days ICI (10 mg/kg/d); solid triangles, 10 days OVA/10 days ICI (10 mg/kg/d). (B) Effect of daily administration of the antagonist in male mice after 10-day OVA inhalation in vivo. Open squares, 10 days saline/ 10 days vehicle; solid squares, 10 days OVA/10 days vehicle; diamonds, 10 days OVA/10 days ICI (10 mg/kg/d). AHR was assayed 24 hours after the last OVA challenge. ICI182,780 at a dose of 10 mg/kg/d was administered intraperitoneally immediately before each OVA challenge. Results represent the mean 6 SEM (n 5 8). **P, 0.01 and ## P, 0.01 comparing 10-day saline/ 10-day vehicle and 10-day OVA/10-day vehicle. normalized ES 50 values (Figure 7B). These results imply that estrogen does not affect cholinergic airway constriction directly but may inhibit prejunctional activation by factors generated during the 10 days of allergen exposure. In Vivo Effects of an NK-1 Receptor Antagonist Neuropeptides, such as substance P, are critical regulators of airway responsiveness. Activation of NK-1 receptors enhances ACh release by EFS (11). We evaluated the effects of Sendide, an NK-1 receptor antagonist, on 10-day OVA-induced AHR in male mice and on the enhancement of AHR by ICI182,780 in female mice. Sendide at a dose of 40 nmol/kg, given 2 hours before assay, significantly suppressed AHR (R L and C dyn ) in 10- day OVA-exposed male mice but not in 10-day saline-exposed mice (Figure 8A). ICI182,780, given 1 hour before assay, significantly enhanced airway responsiveness in female mice after 10-day OVA exposure (Figure 8B). Sendide, at a dose of 40 nmol/kg, fully suppressed this enhancement of RL and decrease in Cdyn (Figure 8B). These data suggest that NK-1 is critical to the development of AHR after 10-day OVA inhalation in vivo, and that endogenous estrogen regulates the Figure 5. Effect of daily administration of E2 on 10-day OVA-induced AHR in male mice in vivo. AHR was assayed 24 hours after the last OVA challenge. E2 at doses of 50 and 100 mg/kg was administered intraperitoneally immediately before each OVA challenge. Results represent the mean 6 SEM (n 5 8). # P, 0.05 and ## P, 0.01 comparing 10-day OVA/10-day vehicle (squares); *P, 0.05 and **P, 0.01 comparing 10-day OVA/ 10-day E2 100 mg/kg/day (circles). Diamonds, 10-day OVA/10-day E2 (50 mg/kg/d); triangles, 10-day OVA/10-day E2 (mg/kg/d) 1 10-day ICI. development of AHR in female mice exposed to OVA exclusively via the airways via an NK-1 dependent pathway. In Vitro Effects of an NK-1 Receptor Antagonist Together, the data suggested that endogenous estrogen may regulate an NK-1 dependent pathway leading to AHR in mice exposed to 10-day OVA. Furthermore, exogenous estrogen suppressed the 10-day OVA-induced AHR detected by EFS in vitro (see Figure 7B). We next confirmed the contribution of the NK-1 pathway to 10-d OVA-induced AHR detected by EFS in vitro. Pretreatment of tracheal smooth muscle preparations with Sendide (100 nm) significantly suppressed the decrease in ES 50 in female and male mice exposed to OVA for 10 days, and there were no sex differences in the degree of suppression (Figure 9). Thus, NK-1 seems to be critical to development of AHR after 10-day OVA inhalation. DISCUSSION Figure 6. Rapid effect of (A) an estrogen antagonist and (B) exogenous E2 on airway responsiveness to MCh in vivo. AHR was assayed 24 hours after the last OVA challenge. ICI182,780 (ICI) at a dose of 10 mg/kg to female mice (A) or E2 at a dose of 100 mg/kg to male mice (B) was administered intraperitoneally 1 hour before the AHR assay. Results represent the mean 6 SEM (n 5 8). # P, 0.05 and ## P, 0.01 comparing 10-day OVA/vehicle. *P, 0.05 and **P, 0.01 comparing 10-day saline/vehicle. Open circles, 10-day saline/vehicle; solid circles, 10-day OVA/ vehicle; open triangles,10-day saline/ici; solid triangles, 10-day OVA ICI. Squares, 10-day OVA/E2. There is substantial evidence that female sex hormones play a regulatory role in asthma pathophysiology, and in particular, development of AHR. Asthma prevalence rates are higher in women than men with a switch occurring at the time of puberty (18 20). There are impressive menstrual cycle associated variations in pulmonary function with asthma worsening during low hormone levels premenstrually (21, 22). Although these clinical findings suggest that sex hormones may influence the prevalence and severity of asthma, the role of specific hormones in dictating these changes is unclear. A number of studies in this area have been reported without consensus, likely reflecting the complexity of the pathways involved and undefined regulatory factors at various times in established disease. In particular, the effects of estrogen in asthma have been discordant, with both beneficial and negative effects described (7, 8, 23). In the former, supplemental estrogens were used as a steroid-sparing agent in females with asthma; in the latter, post-menopausal estrogen therapy increased the subsequent risk of asthma. A number of papers describe a worsening of asthma during the premenstrual and intramenstrual periods in a subgroup of women with asthma (21, 24 27), although the mechanism
6 506 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Figure 7. Effect of exogenous E2 on in vitro airway responsiveness to CCh or EFS after (A) 10-day saline or (B) 10-day OVA exposure. Tracheas from female (open bars) and male (solid bars) mice were isolated from 10-day saline- or OVA-treated mice. The tracheas were preincubated with vehicle or E2 (1 100 nm) for 30 minutes. After incubation, airway contractility to CCh or EFS was determined. Results represent the mean 6 SEM (n 5 8). **P, 0.01 comparing 10-day saline/vehicle group in either sex. # P, 0.05 and ## P, 0.01 comparing 10-day OVA/vehicle group in either sex. In the CCh and EFS groups, the 95% confidence intervals overlapped. underlying this susceptibility remains unclear. Ensom and colleagues demonstrated the beneficial effects of estradiol in a severely asthmatic woman with premenstrual worsening of asthma (24). The present study examined sex differences in a model of allergen exposure that was exclusively delivered via the airways and in the absence of systemic sensitization and adjuvant. This approach has been shown to be dependent on IgE, FceRI expression, and mast cells, and differs from the requirements when systemic sensitization with adjuvant are employed (13). In some studies which use systemic sensitization to allergen with adjuvant followed by allergen challenge via the airways, female mice developed greater AHR, with estrogen enhancing airway inflammation (6 8). In contrast, in naive mice or following less robust sensitization and challenge, as performed here, the inhibitory effects of estrogen on development of AHR may be more obvious (4, 5, 23). Carey et al also showed that deficiency of the estrogen receptor resulted in higher AHR. In our study, OVA exposure exclusively via the airways resulted in little inflammatory cell accumulation in the BALF but did elicit a modest eosinophilic inflammatory response in lung tissue as well as goblet cell metaplasia (23). In female mice, 10 days of OVA exposure failed to alter lung function in vivo when assessed after MCh inhalation. Increased airway responsiveness was detected only by the altered response to electrical field stimulation, a decrease in ES 50. Such decreases have been linked to muscarinic receptor dysfunction, endogenous substance P, and increased acetylcholine release (13, 15), perhaps the result of eosinophilic inflammation (28). In contrast to female mice, male mice subjected to 10 days of OVA exposure developed a similar decrease in ES 50 but also exhibited a robust MCh dose-dependent increase in R L and a decrease in C dyn in vivo. These differences in MCh-induced AHR between male and female mice did not seem to be related to differences in airway inflammation, BAL cytokine levels, or numbers of goblet cells. Together, these data pointed to sex differences in the response of airway smooth muscle to inhaled MCh after allergen exposure as opposed to differences in the immune/ inflammatory response often associated with increased MCh reactivity (29, 30). Figure 8. Effect of a neurokinin-1 receptor antagonist (Sendide) on (A) 10-day OVA-induced AHR in male mice and (B) enhancement of AHR by an estrogen antagonist in 10-day OVA-exposed female mice. AHR was assayed 24 hours after the last OVA challenge. Sendide at a dose of 40 nmol/kg and/or ICI182,780 at a dose of 10 mg/kg was administered intraperitoneally 2 hours and/or 1 hour, respectively, before the AHR assay. Results represent the mean 6 SEM (n 5 8). # P, 0.05 and ## P, 0.01 comparing 10-day OVA/vehicle or 10-day saline/sendide. *P, 0.05 and **P, 0.01 comparing 10-day saline/vehicle or 10-day saline/sendide. P, 0.05 and P, 0.01 comparing 10-day OVA/ICI/PBS. PBS was a vehicle for Sendide. ICI 5 ICI182,780. A: open circles, 10-day saline/vehicle; solid circles, 10-day OVA/vehicle; open diamonds, 10-day saline/sendide; solid diamonds, 10-day OVA/Sendide. B: open circles, 10-day saline/vehicle/pbs; solid circles, 10-day OVA/vehicle/PBS; triangles, 10-day OVA/ICI/PBS; diamonds, 10-day OVA/ICI/Sendide.
7 Matsubara, Swasey, Loader, et al.: Estrogen Regulates Allergic AHR 507 Figure 9. Involvement of neurokinin-1 in 10-day OVA-induced AHR detected by EFS in vitro. Tracheas from female (open bars) and male (solid bars) mice were isolated from 10-day saline- or OVA-exposed mice. The tracheas were preincubated with vehicle or Sendide (100 nm) for 30 minutes. After the preincubation, airway contractility to EFS was assayed. Results represent the mean 6 SEM (n 5 8). P, 0.01 comparing 10-day saline/vehicle. ## P, 0.01 comparing 10-day OVA/ vehicle. ES % of maximal contraction. In different models, estrogen has been shown to recapitulate sex differences. As examples, estrogen pretreatment of male mice prevented endotoxin-induced hepatic injury and reduced poly-adp-ribosylation in vivo (31). Down-modulation of E- selectin and IL-6 gene expression by estrogen may have contributed to a reduction in the cellular infiltration seen in a model of acute anterior uveitis (32). Several reports of risk factors associated with AHR have noted a higher level of responsiveness in female compared with male subjects (6, 23, 33 35), implicating that sex hormones play a role in altered airway responsiveness. However, the specific mechanisms responsible for the development of AHR were unclear. In female mice, ovariectomy enabled development of MChinduced changes in R L (increased) and C dyn (decreased). Confirmation of the role of estrogen as an important regulator of airway function was demonstrated by the administration of an estrogen receptor antagonist, which similarly enhanced MChinduced changes in airway function in female mice. Because administration of the estrogen receptor antagonist 1 hour before assay of airway function showed similar enhancement of AHR, this suggested direct effects on airway smooth muscle, but only in the allergen-exposed group. In male mice, administration of estrogen reduced the 10-day OVA-induced changes in MCh-dependent reactivity, and this could be prevented by coadministration of an estrogen receptor antagonist. Together, these data identified estrogen as a critical regulator of the development of AHR after exposure to allergen exclusively via the airways. Furthermore, because manipulation of airway reactivity to MCh with estrogen, the estrogen receptor antagonist, or ovariectomy was accomplished without concomitant changes in airway inflammation, BAL cytokine levels, or numbers of goblet cells, this was consistent with estrogen regulating airway function at the level of airway smooth muscle. This notion was also supported by the in vivo findings that these manipulations (other than OVX) could be performed after full completion of allergen exposure, just 1 hour before measuring AHR to inhaled MCh, with very similar results. These in vivo results were paralleled by examining the effects of estrogen in vitro on CCh- or EFS-induced contractility of tracheal smooth muscle. Estrogen has been reported to inhibit CCh-induced airway constriction after passive sensitization with serum from patients with asthma (4). In the present study, no enhancement of CCh-induced contractility was detected in vitro after 10-day OVA inhalation. Exogenous estrogen did not influence CCh-induced tracheal smooth muscle responses in male or female mice after OVA exposure. In contrast, exogenous estrogen added to the muscle preparation suppressed EFS-induced contractility in tracheal smooth muscle from male and female mice after OVA exposure but not after saline exposure. These data demonstrate that the effects of estrogen on airway smooth muscle contractility are restricted to those triggered by EFS and not CCh. To extend these findings, we showed using a specific NK-1 receptor antagonist that OVA exposure activated an NK-1 dependent pathway resulting in altered airway function in vitro and in vivo. Moreover, the NK-1 receptor antagonist attenuated the effects of the estrogen receptor antagonist in enhancing AHR in female mice in vivo. NK1 receptor stimulation has been shown to augment cholinergic neurotransmission in mouse trachea when in vitro airway responsiveness was detected by EFS (36). Thus, these data support the notion that the rapid onset of estrogen regulation of smooth muscle contractility is NK-1 dependent and involves prejunctional activation but does not interfere with cholinergic airway smooth muscle constriction. The 10-day OVA inhalation leads to a cascade of immunologic/inflammatory responses (13). The assumption is that these events trigger and up-regulate an NK-1 dependent pathway, leading to increases in ACh release. The role of NK receptors and their agonistic tachykinins in allergic airway inflammation is somewhat controversial (37). In a recent study, Boot and colleagues demonstrated that a NK1/ NK2 dual antagonist failed to modulate AHR and airway inflammation after allergen challenge in patients with asthma (38). However, the role of NK receptors cannot be discounted because it is difficult to confirm blocking of all available NK receptors in the airways within such a clinical design. In this study, male female differences in the response to allergen exposure were revealed when MCh-induced changes in airway function were monitored. Investigation of these differences identified estrogen as an important regulator of airway function at the prejunctional level in vitro and in vivo. Manipulation of estrogen production or estrogen receptor antagonism converted female mice from nonresponders to responders and male mice from responders to nonresponders in an NK-1 dependent manner. These findings identify potential approaches to modify altered airway function in patients with asthma, especially at critical stages of their disease. Conflict of Interest Statement: None of the authors has a financial relationship with a commercial entity that has an interest in the subject of this manuscript. Acknowledgment: The authors thank Dr. J. J. Lee (Mayo Clinic, Scottsdale, AZ) for providing the anti major basic protein antibodies and L. N. Cunningham and D. Nabighian (National Jewish Medical and Research Center, Denver, CO) for their assistance. References 1. Meyer MR, Haas E, Barton M. Sex differences of cardiovascular disease: new perspectives for estrogen receptor signaling. Hypertension 2006;47: Most W, van der Wee-Pals L, Ederveen A, Papapoulos S, Lowik C. Ovariectomy and orchidectomy induce a transient increase in the osteoclastogenic potential of bone marrow cells in the mouse. Bone 1997;20: Gillies GE, Murray HE, Dexter D, McArthur S. Sex dimorphisms in the neuroprotective effects of estrogen in an animal model of Parkinson s disease. Pharmacol Biochem Behav 2004;78: Dimitropoulou C, White RE, Ownby DR, Catravas JD. Estrogen reduces carbachol-induced constriction of asthmatic airways by stimulating large-conductance voltage and calcium-dependent potassium channels. Am J Respir Cell Mol Biol 2005;32:
8 508 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Degano B, Prevost MC, Berger P, Molimard M, Pontier S, Rami J, Escamilla R. Estradiol decreases the acetylcholine-elicited airway reactivity in ovariectomized rats through an increase in epithelial acetylcholinesterase activity. Am J Respir Crit Care Med 2001;164: Melgert BN, Postma DS, Kuipers I, Geerlings M, Luinge MA, van der Strate BW, Kerstjens HA, Timens W, Hylkema MN. Female mice are more susceptible to the development of allergic airway inflammation than male mice. Clin Exp Allergy 2005;35: Corteling R, Trifilieff A. Sex comparison in a murine model of allergendriven airway inflammation and the response to budesonide treatment. BMC Pharmacol 2004;4:4. 8. Riffo-Vasquez Y, Ligeiro de Oliveira AP, Page CP, Spina D, Tavaresde-Lima W. Role of sex hormones in allergic inflammation in mice. Clin Exp Allergy 2007;37: Dijkstra A, Howard TD, Vonk JM, Ampleford EJ, Lange LA, Bleecker ER, Meyers DA, Postma DS. Estrogen receptor 1 polymorphisms are associated with airway hyperresponsiveness and lung function decline, particularly in female subjects with asthma. J Allergy Clin Immunol 2006;117: Schatz M, Clark S, Camargo CA Jr. Sex differences in the presentation and course of asthma hospitalizations. Chest 2006;129: Colasurdo GN, Loader JE, Graves JP, Larsen GL. Modulation of acetylcholine release in rabbit airways in vitro. Am J Physiol 1995; 268:L432 L Larsen GL, Loader JE, Nguyen DD, Fratelli C, Dakhama A, Colasurdo GN. Mechanisms determining cholinergic neural responses in airways of young and mature rabbits. Pediatr Pulmonol 2004;38: Taube C, Wei X, Swasey CH, Joetham A, Zarini S, Lively T, Takeda K, Loader J, Miyahara N, Kodama T, et al. Mast cells, Fc epsilon RI, and IL-13 are required for development of airway hyperresponsiveness after aerosolized allergen exposure in the absence of adjuvant. J Immunol 2004;172: Takeda K, Hamelmann E, Joetham A, Shultz LD, Larsen GL, Irvin CG, Gelfand EW. Development of eosinophilic airway inflammation and airway hyperresponsiveness in mast cell-deficient mice. J Exp Med 1997;186: Larsen GL, Fame TM, Renz H, Loader JE, Graves J, Hill M, Gelfand EW. Increased acetylcholine release in tracheas from allergenexposed IgE-immune mice. Am J Physiol 1994;266:L263 L Tomkinson A, Duez C, Cieslewicz G, Pratt JC, Joetham A, Shanafelt MC, Gundel R, Gelfand EW. A murine IL-4 receptor antagonist that inhibits IL-4- and IL-13-induced responses prevents antigen-induced airway eosinophilia and airway hyperresponsiveness. J Immunol 2001; 166: Larsen GL, Renz H, Loader JE, Bradley KL, Gelfand EW. Airway response to electrical field stimulation in sensitized inbred mice: passive transfer of increased responsiveness with peribronchial lymph nodes. J Clin Invest 1992;89: Skobeloff EM, Spivey WH, St Clair SS, Schoffstall JM. The influence of age and sex on asthma admissions. JAMA 1992;268: Hyndman SJ, Williams DR, Merrill SL, Lipscombe JM, Palmer CR. Rates of admission to hospital for asthma. BMJ 1994;308: Bloomberg GR, Trinkaus KM, Fisher EB Jr, Musick JR, Strunk RC. Hospital readmissions for childhood asthma: a 10-year metropolitan study. Am J Respir Crit Care Med 2003;167: Gibbs CJ, Coutts II, Lock R, Finnegan OC, White RJ. Premenstrual exacerbation of asthma. Thorax 1984;39: Pauli BD, Reid RL, Munt PW, Wigle RD, Forkert L. Influence of the menstrual cycle on airway function in asthmatic and normal subjects. Am Rev Respir Dis 1989;140: Carey MA, Bradbury JA, Card JW, Noorman MP, Haykal-Coates N, Gavett SH, Graves JP, Walker VR, Zhu D, Jacobs ER, et al. Spontaneous airway hyperresponsiveness in estrogen receptor-alpha deficient mice. Am J Respir Crit Care Med 2007;175: Ensom MH, Chong G, Beaudin B, Bai TR. Estradiol in severe asthma with premenstrual worsening. Ann Pharmacother 2003;37: Ensom MH, Chong E, Carter D. Premenstrual symptoms in women with premenstrual asthma. Pharmacotherapy 1999;19: Oguzulgen IK, Turktas H, Erbas D. Airway inflammation in premenstrual asthma. J Asthma 2002;39: Tan KS. Premenstrual asthma: epidemiology, pathogenesis and treatment. Drugs 2001;61: Fryer AD, Stein LH, Nie Z, Curtis DE, Evans CM, Hodgson ST, Jose PJ, Belmonte KE, Fitch E, Jacoby DB. Neuronal eotaxin and the effects of CCR3 antagonist on airway hyperreactivity and M2 receptor dysfunction. J Clin Invest 2006;116: Tomkinson A, Duez C, Cieslewicz G, Gelfand EW. Eotaxin-1-deficient mice develop airway eosinophilia and airway hyperresponsiveness. Int Arch Allergy Immunol 2001;126: Wolyniec WW, De Sanctis GT, Nabozny G, Torcellini C, Haynes N, Joetham A, Gelfand EW, Drazen JM, Noonan TC. Reduction of antigen-induced airway hyperreactivity and eosinophilia in ICAM-1- deficient mice. Am J Respir Cell Mol Biol 1998;18: Mabley JG, Horvath EM, Murthy KG, Zsengeller Z, Vaslin A, Benko R, Kollai M, Szabo C. Sex differences in the endotoxin-induced inflammatory and vascular responses: potential role of poly(adp-ribose) polymerase activation. J Pharmacol Exp Ther 2005;315: Miyamoto N, Mandai M, Suzuma I, Suzuma K, Kobayashi K, Honda Y. Estrogen protects against cellular infiltration by reducing the expressions of E-selectin and IL-6 in endotoxin-induced uveitis. J Immunol 1999;163: Whitacre CC, Reingold SC, O Looney PA. A sex gap in autoimmunity. Science 1999;283: Da Silva JA, Pinto A, Cutolo M, Porto A. Sex differences in adrenal and gonadal responses to inflammatory aggression. Ann N Y Acad Sci 1999;876: Amadori A, Zamarchi R, De Silvestro G, Forza G, Cavatton G, Danieli GA, Clementi M, Chieco-Bianchi L. Genetic control of the CD4/CD8 T-cell ratio in humans. Nat Med 1995;1: Tournoy KG, De Swert KO, Leclere PG, Lefebvre RA, Pauwels RA, Joos GF. Modulatory role of tachykinin NK1 receptor in cholinergic contraction of mouse trachea. Eur Respir J 2003;21: Joos GF, De Swert KO, Schelfhout V, Pauwels RA. The role of neural inflammation in asthma and chronic obstructive pulmonary disease. Ann N Y Acad Sci 2003;992: Boot JD, de Haas S, Tarasevych S, Roy C, Wang L, Amin D, Cohen J, Sterk PJ, Miller B, Paccaly A, et al. Effect of an NK1/NK2 receptor antagonist on airway responses and inflammation to allergen in asthma. Am J Respir Crit Care Med 2007;175:
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Dual-Controller Asthma Therapy: Rationale and Clinical Benefits
 B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
for Development of Airway Hyperresponsiveness after Aerosolized Allergen Exposure in the Absence of Adjuvant
 This information is current as of May 14, 2018. References Subscription Permissions Email Alerts Mast Cells, FcεRI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized
This information is current as of May 14, 2018. References Subscription Permissions Email Alerts Mast Cells, FcεRI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice
 Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge
 Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge
 Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
Surfactant Protein D Regulates Airway Function and Allergic Inflammation through Modulation of Macrophage Function
 Surfactant Protein D Regulates Airway Function and Allergic Inflammation through Modulation of Macrophage Function Katsuyuki Takeda, Nobuaki Miyahara, Yeong-Ho Rha, Christian Taube, Eun-Seok Yang, Anthony
Surfactant Protein D Regulates Airway Function and Allergic Inflammation through Modulation of Macrophage Function Katsuyuki Takeda, Nobuaki Miyahara, Yeong-Ho Rha, Christian Taube, Eun-Seok Yang, Anthony
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
special communication
 Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
The case for extra fine particle ICS:! to cover the entire lung!
 The case for extra fine particle ICS: to cover the entire lung Richard J. Martin, M.D. Chairman Department of Medicine National Jewish Health The Edelstein Chair in Pulmonary Medicine Professor of Medicine
The case for extra fine particle ICS: to cover the entire lung Richard J. Martin, M.D. Chairman Department of Medicine National Jewish Health The Edelstein Chair in Pulmonary Medicine Professor of Medicine
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients
 Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Specific CD8 T cells in IgE-mediated allergy correlate with allergen dose and allergic phenotype
 Specific CD8 T cells in IgE-mediated allergy correlate with allergen dose and allergic phenotype Juan A. Aguilar-Pimentel, Francesca Alessandrini, Katharina M. Huster, Thilo Jakob, Holger Schulz, Heidrun
Specific CD8 T cells in IgE-mediated allergy correlate with allergen dose and allergic phenotype Juan A. Aguilar-Pimentel, Francesca Alessandrini, Katharina M. Huster, Thilo Jakob, Holger Schulz, Heidrun
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
SERIES 'OCCUPATIONAL ASTHMA' Edited by C. Mapp
 Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Current Asthma Management: Opportunities for a Nutrition-Based Intervention
 Current Asthma Management: Opportunities for a Nutrition-Based Intervention Stanley J. Szefler, MD Approximately 22 million Americans, including 6 million children, have asthma. It is one of the most prevalent
Current Asthma Management: Opportunities for a Nutrition-Based Intervention Stanley J. Szefler, MD Approximately 22 million Americans, including 6 million children, have asthma. It is one of the most prevalent
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
IL-13 is essential to the late-phase response in allergic rhinitis
 Original articles IL-13 is essential to the late-phase response in allergic rhinitis Satoko Miyahara, MD, PhD, Nobuaki Miyahara, MD, PhD, Shigeki Matsubara, PhD, Katsuyuki Takeda, MD, PhD, Toshiyuki Koya,
Original articles IL-13 is essential to the late-phase response in allergic rhinitis Satoko Miyahara, MD, PhD, Nobuaki Miyahara, MD, PhD, Shigeki Matsubara, PhD, Katsuyuki Takeda, MD, PhD, Toshiyuki Koya,
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Supporting Information Table of Contents
 Supporting Information Table of Contents Supporting Information Figure 1 Page 2 Supporting Information Figure 2 Page 4 Supporting Information Figure 3 Page 5 Supporting Information Figure 4 Page 6 Supporting
Supporting Information Table of Contents Supporting Information Figure 1 Page 2 Supporting Information Figure 2 Page 4 Supporting Information Figure 3 Page 5 Supporting Information Figure 4 Page 6 Supporting
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma
 Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Full Paper. Hiroyasu Hirose, Jian Jiang, and Masaru Nishikibe*
 J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice
 Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Supplementary Medications during asthma attack. Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus
 Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life
 Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice.
 Author's response to reviews Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice. Authors: Mike Burrows (mburrows@tampabayresearch.org)
Author's response to reviews Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice. Authors: Mike Burrows (mburrows@tampabayresearch.org)
Learning Outcomes. Systems Pharmacology PHAR3320. Nerves of the Respiratory Tract. Dr Fernandes
 Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Assessment of a rapid liquid based cytology method for measuring sputum cell counts
 Assessment of a rapid liquid based cytology method for measuring sputum cell counts Martin MJ, Lee H, Meakin G, Green A, Simms RL, Reynolds C, Winters S*, Shaw DE, Soomro I*, Harrison TW The Asthma Centre
Assessment of a rapid liquid based cytology method for measuring sputum cell counts Martin MJ, Lee H, Meakin G, Green A, Simms RL, Reynolds C, Winters S*, Shaw DE, Soomro I*, Harrison TW The Asthma Centre
Neuronal eotaxin and the effects of ccr3 antagonist on airway hyperreactivity and M2 receptor dysfunction
 Research article Neuronal eotaxin and the effects of ccr3 antagonist on airway hyperreactivity and M2 receptor dysfunction Allison D. Fryer, 1,2,3 Louis H. Stein, 3 Zhenying Nie, 2 Damian E. Curtis, 2
Research article Neuronal eotaxin and the effects of ccr3 antagonist on airway hyperreactivity and M2 receptor dysfunction Allison D. Fryer, 1,2,3 Louis H. Stein, 3 Zhenying Nie, 2 Damian E. Curtis, 2
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin
 CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Estrogen effects on human airway smooth muscle involve camp and protein kinase A
 Am J Physiol Lung Cell Mol Physiol 303: L923 L928, 2012. First published September 21, 2012; doi:10.1152/ajplung.00023.2012. Estrogen effects on human airway smooth muscle involve camp and protein kinase
Am J Physiol Lung Cell Mol Physiol 303: L923 L928, 2012. First published September 21, 2012; doi:10.1152/ajplung.00023.2012. Estrogen effects on human airway smooth muscle involve camp and protein kinase
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: ,
 INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: 631-635, 2007 631 Effective microorganism fermentation extract (EM-X) attenuates airway hyperreactivity and inflammation through selective inhibition of
INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: 631-635, 2007 631 Effective microorganism fermentation extract (EM-X) attenuates airway hyperreactivity and inflammation through selective inhibition of
The FDA Critical Path Initiative
 The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
COPD and Asthma: Similarities and differences Prof. Peter Barnes
 and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
The Link Between Viruses and Asthma
 The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
PIERIS PHARMACEUTICALS, INC. (Exact Name of Registrant as Specified in its Charter)
 UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
Asthma Update A/Prof. John Abisheganaden. Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital
 Asthma Update - 2013 A/Prof. John Abisheganaden Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital Asthma A complex syndrome Multifaceted disease Heterogeneous Genetic and
Asthma Update - 2013 A/Prof. John Abisheganaden Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital Asthma A complex syndrome Multifaceted disease Heterogeneous Genetic and
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
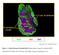 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma
 Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts
 Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Original Article. ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma
 J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
AND COPD ADVANCES IN COMBINATION THERAPY FOR ASTHMA. Jan Lotvall. Editor. Krefting Research Centre, University of Gothenburg,
 ADVANCES IN COMBINATION THERAPY FOR ASTHMA AND COPD Editor Jan Lotvall Krefting Research Centre, University of Gothenburg, Sweden A Wiley Sons, Ltd., Publication Contents Contributors xi Preface 1 Similarities
ADVANCES IN COMBINATION THERAPY FOR ASTHMA AND COPD Editor Jan Lotvall Krefting Research Centre, University of Gothenburg, Sweden A Wiley Sons, Ltd., Publication Contents Contributors xi Preface 1 Similarities
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Asthma Pathophysiology and Treatment. John R. Holcomb, M.D.
 Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Determinants of Severe and Fatal Anaphylaxis
 Determinants of Severe and Fatal Anaphylaxis Peter Vadas MD PhD Chief, Division of Allergy and Clinical Immunology St. Michael s Hospital University of Toronto The Problem Peanut the most common cause
Determinants of Severe and Fatal Anaphylaxis Peter Vadas MD PhD Chief, Division of Allergy and Clinical Immunology St. Michael s Hospital University of Toronto The Problem Peanut the most common cause
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Role of immunoglobulin E and mast cells in murine models of asthma
 Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c)
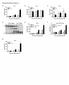 1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
Histamine Develops Homologous Desensitization under Ca 2+ -free Conditions with Increase in Basal Tone in Smooth Muscle of Guinea Pig Taenia Caeci
 YAKUGAKU ZASSHI 130(3) 451 455 (2010) 2010 The Pharmaceutical Society of Japan 451 Notes Histamine Develops Homologous Desensitization under Ca 2+ -free Conditions with Increase in Basal Tone in Smooth
YAKUGAKU ZASSHI 130(3) 451 455 (2010) 2010 The Pharmaceutical Society of Japan 451 Notes Histamine Develops Homologous Desensitization under Ca 2+ -free Conditions with Increase in Basal Tone in Smooth
Online Data Supplement
 Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Four of 10 patients with asthma suffer moderate REVIEW DUAL-CONTROLLER REGIMENS II: OBSERVATIONAL DATA. Michael S. Blaiss, MD ABSTRACT
 DUAL-CONTROLLER REGIMENS II: OBSERVATIONAL DATA Michael S. Blaiss, MD ABSTRACT The differences between clinical trials and clinical practice often create difficulty for generalizing results of controlled
DUAL-CONTROLLER REGIMENS II: OBSERVATIONAL DATA Michael S. Blaiss, MD ABSTRACT The differences between clinical trials and clinical practice often create difficulty for generalizing results of controlled
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Recent advances in diagnosis and management of ABPA. Arindam SR(Pulmonary Medicine)
 Recent advances in diagnosis and management of ABPA Arindam SR(Pulmonary Medicine) Conventional diagnostic criteria for ABPA Primary Episodic bronchial obstruction (asthma) Peripheral blood eosinophilia
Recent advances in diagnosis and management of ABPA Arindam SR(Pulmonary Medicine) Conventional diagnostic criteria for ABPA Primary Episodic bronchial obstruction (asthma) Peripheral blood eosinophilia
Biologic Agents in the treatment of Severe Asthma
 Biologic Agents in the treatment of Severe Asthma Daniel L Maxwell, D.O., FACOI, FAASM Clinical Assistant Professor of Medicine Michigan State University College of Osteopathic Medicine College of Human
Biologic Agents in the treatment of Severe Asthma Daniel L Maxwell, D.O., FACOI, FAASM Clinical Assistant Professor of Medicine Michigan State University College of Osteopathic Medicine College of Human
Felix R. Shardonofsky, MD Reference List
 Book Chapter Shardonofsky FR. Heart Failure in Pediatric Patients. In: Heart Failure in Children and Young Adults: From Molecular Mechanisms To Medical Management. Editors: AC Chang and J Towbin. Elsevier,
Book Chapter Shardonofsky FR. Heart Failure in Pediatric Patients. In: Heart Failure in Children and Young Adults: From Molecular Mechanisms To Medical Management. Editors: AC Chang and J Towbin. Elsevier,
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
