for Development of Airway Hyperresponsiveness after Aerosolized Allergen Exposure in the Absence of Adjuvant
|
|
|
- Dayna Gilmore
- 6 years ago
- Views:
Transcription
1 This information is current as of May 14, References Subscription Permissions Alerts Mast Cells, FcεRI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized Allergen Exposure in the Absence of Adjuvant Christian Taube, Xudong Wei, Christina H. Swasey, Anthony Joetham, Simona Zarini, Tricia Lively, Katsuyuki Takeda, Joan Loader, Nobuaki Miyahara, Taku Kodama, Lenny D. Shultz, Debra D. Donaldson, Eckard H. Hamelmann, Azzeddine Dakhama and Erwin W. Gelfand J Immunol 2004; 172: ; ; doi: /jimmunol This article cites 62 articles, 28 of which you can access for free at: Why The JI? Submit online. Rapid Reviews! 30 days* from submission to initial decision No Triage! Every submission reviewed by practicing scientists Fast Publication! 4 weeks from acceptance to publication *average Information about subscribing to The Journal of Immunology is online at: Submit copyright permission requests at: Receive free -alerts when new articles cite this article. Sign up at: Downloaded from by guest on May 14, 2018 The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD Copyright 2004 by The American Association of Immunologists All rights reserved. Print ISSN: Online ISSN:
2 The Journal of Immunology Mast Cells, Fc RI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized Allergen Exposure in the Absence of Adjuvant 1 Christian Taube,* Xudong Wei,* Christina H. Swasey,* Anthony Joetham,* Simona Zarini,* Tricia Lively,* Katsuyuki Takeda,* Joan Loader,* Nobuaki Miyahara,* Taku Kodama,* Lenny D. Shultz, Debra D. Donaldson, Eckard H. Hamelmann,* Azzeddine Dakhama,* and Erwin W. Gelfand 2 * In certain models of allergic airway disease, mast cells facilitate the development of inflammation and airway hyper-responsiveness (AHR). To define the role of the high affinity IgE receptor (Fc RI) in the development of AHR, mice with a disruption of the subunit of the high affinity IgE receptor (Fc RI / ) were exposed on 10 consecutive days to nebulized OVA. Forty-eight hours after the last nebulization, airway responsiveness was monitored by the contractile response of tracheal smooth muscle to electrical field stimulation (EFS). After the 10-day OVA challenge protocol, wild-type mice demonstrated increased responsiveness to EFS, whereas similarly challenged Fc RI / mice showed a low response to EFS, similar to nonexposed animals. Further, allergenchallenged Fc RI / mice showed less airway inflammation, goblet cell hyperplasia, and lower levels of IL-13 in lung homogenates compared with the controls. IL-13-deficient mice failed to develop an increased response to EFS or goblet cell hyperplasia after the 10-day OVA challenge. We transferred bone marrow-derived mast cells from wild-type mice to Fc RI / mice 1 day before initiating the challenge protocol. After the 10-day OVA challenge, recipient Fc RI / mice demonstrated EFS-induced responses similar to those of challenged wild-type mice. Transferred mast cells could be detected in tracheal preparations. These results show that Fc RI is important for the development of AHR after an aerosolized allergen sensitization protocol and that this effect is mediated through Fc RI on mast cells and production of IL-13 in the lung. The Journal of Immunology, 2004, 172: A feature of allergic disease is the increased production of IgE in response to common environmental allergens, and numerous studies have shown a significant relationship between sensitization to various allergens and allergic asthma (1, 2). In patients with asthma, exposure to allergen increases airway inflammation and airway hyperresponsiveness (AHR) 3 (3, 4) even with small amounts of allergen, indicating a local amplification mechanism contributing significantly to inflammation and development of AHR in this setting. One of the cell populations responding to low doses of allergen and amplifying the response are tissue mast cells, which release a number of potent mediators of inflammation in an Ab-dependent mechanism (5). In asthmatics, mast cells have been described in increased numbers in the airway *Division of Cell Biology, Department of Pediatrics, National Jewish Medical and Research Center, Denver, CO 80206; The Jackson Laboratory, Bar Harbor, ME 04609; and Wyeth Institute, Cambridge, MA Received for publication August 20, Accepted for publication March 15, The costs of publication of this article were defrayed in part by the payment of page charges. This article must therefore be hereby marked advertisement in accordance with 18 U.S.C. Section 1734 solely to indicate this fact. 1 This work was supported by National Institutes of Health Grants AI42246, HL36577, and HL61005 (to E.W.G.) and AI30389 (to L.D.S.); Environmental Protection Agency Grant R (to E.W.G.); and Deutsche Forschungsgemeinschaft Grant Ta 275/2-1 (to C.T.). 2 Address correspondence and reprint requests to Dr. Erwin W. Gelfand, National Jewish Medical and Research Center, 1400 Jackson Street, Denver, CO address: gelfande@njc.org 3 Abbreviations used in this paper: AHR, airway hyperresponsiveness; BMMC, bone marrow-derived mast cell; EFS, electrical field stimulation; ES 50, frequency resulting in 50% of the maximal contraction; EU, ELISA unit; GFP, green fluorescent protein; MBP, major basic protein; MCh, methacholine; PAS, periodic acid-schiff; sil-13, soluble IL-13; UBI, human ubiquitin C promoter. wall, and recent reports have found these cells infiltrating airway smooth muscle (6). Mast cells may recognize allergen through the high affinity IgE receptor (Fc RI), and IgE is thought to build a complex with allergen binding to this receptor. Allergen-cross-linking of receptors leads to the activation of mast cells, with the release of numerous mediators and cytokines (7 9). However, the role of mast cells in the development of AHR is somewhat controversial. When studying mechanisms of allergic airway disease in animals models, mast cell-deficient mice have variable decreases in eosinophil numbers (10, 11) after allergen challenge, but systemically sensitized and challenged mast cell-deficient mice are capable of developing a Th2 response, airway inflammation, and AHR similar to wild-type control mice (12 15). In most of these studies allergen sensitization was achieved by systemically injecting the allergen in combination with an adjuvant, whereas other studies, using less potent sensitization protocols, demonstrated a more obvious role for mast cells in the development of AHR (16, 17). To characterize the role of mast cells and Fc RI in the development of AHR, we used an allergen challenge protocol in which wild-type, mast cell-deficient, and Fc RI-deficient mice were challenged repeatedly with allergen via the airways without the use of an adjuvant (18). In this model allergen exposure leads to dysfunction of muscarinic receptor 2, which results in an increase in acetylcholine release after electrical field stimulation (EFS) (19). After exclusive aerosolized allergen exposure, allergen-specific IgE and IgG1 are elevated in the serum of exposed mice (20), and the presence of B cells is essential for the development of AHR in this model (21). In the present study we show that after repeated Copyright 2004 by The American Association of Immunologists, Inc /04/$02.00
3 The Journal of Immunology 6399 airway challenge, mast cell- and Fc RI-deficient mice fail to develop increased reactivity to EFS, a response that could be reconstituted by transfer of Fc RI-sufficient mast cells before the airway challenge. Materials and Methods Animals Female BALB/cByJ mice, C57BL/6 mice, mast cell-deficient mice ([WB/ Rej-kit W / C57BL6J-kit W-v / ]F 1 [W/W v ] mice) and congenic WBB6F 1 normal mice from 8 to 12 wk of age were obtained from The Jackson Laboratory (Bar Harbor, ME). Mice with a disruption of the subunit of the high affinity IgE receptor (Fc RI / ; BALB/c background; provided by Drs. D. Dombrowicz and J. P. Kinet, Harvard Medical School, Boston, MA) (22, 23), IL-13-deficient mice (IL-13 / ; BALB/c background; provided by Dr. D. Umetsu, Stanford University, Stanford, CA) (24), and CD57BL/6 mice that express a transgene for green fluorescent protein (GFP) under control of a human ubiquitin C promoter (UBI-GFP) (25) (provided by Dr. P. Marrack, National Jewish Medical and Research Center, Denver, CO) were maintained and bred in the animal facility. All mice were maintained on OVA-free diets. All experimental animals used in this study were under a protocol approved by the institutional animal care and use committee of National Jewish Medical and Research Center. Experimental protocols Experimental groups consisted of three or four mice per group, and each experiment was performed at least twice. Mice were exposed to OVA (Sigma-Aldrich, St. Louis, MO) as described previously (18). Briefly, a solution of 1% OVA in 0.9% saline or endotoxin-depleted 1% OVA solution was delivered by ultrasonic nebulization for 20 min daily over 10 consecutive days in a closed chamber. Control mice were exposed to 0.9% saline alone following the same protocol. AHR was assessed 48 h after the last nebulization. Administration of the soluble IL-13R 2-IgGFc fusion protein (sil-13r 2-Fc) Murine IL-13R 2-hIgG fusion protein was prepared as previously described (26). In the 10-day OVA challenge protocol, IL-13R 2-hIgG fusion protein was administered by i.p. injection (300 g/mouse) 1 h before OVA challenge on days 1, 4, 7, and 10. As a control, the same amount of human IgG was injected at the identical time points. Detection of endotoxin and removal of endotoxin from OVA solution Endotoxin concentrations in OVA solution were assessed by Limulus amebocyte lysate (Charles Rivers Breeding Laboratories, Charleston, SC). Endotoxin depletion of OVA solutions was performed following previously described protocols (27, 28). Briefly, OVA solution (30 mg/ml in endotoxin-free saline) was mixed with 1% Triton X-114 (Sigma-Aldrich) by vigorously vortexing and was placed in an ice bath. After vortexing the chilled samples, the tubes were warmed at 37 C for 5 min to allow two phases to form. Samples were then centrifuged (10 min, 7000 rpm). After centrifugation, the detergent layer was found as an oily droplet at the bottom of the tube. The upper aqueous layer was removed carefully. Residual detergent in the aqueous phase was removed by treatment with endotoxinfree Bio-Beads SM-4 (Bio-Rad, Hercules, CA) as described previously (28). The resultant solution contained little endotoxin (1.8 ELISA unit (EU)/mg protein) Transfer of bone marrow-derived mast cells (BMMC) Mast cells were derived from bone marrow as previously described (29). Bone marrow was obtained from wild-type mice, Fc RI / mice, IL-13 / mice, and UBI-GFP mice and was cultured in IMDM (Life Technologies, Grand Island, NY) supplemented with 5% FBS (Summit Biotechnology, Fort Collins, CO), 50 M 2-ME (Life Technologies), 2 mm glutamine, 100 g/ml streptomycin, 100 U/ml penicillin, 0.5 g/ml amphotericin B, IL-3 obtained from medium conditioned by X63-AG8-653 myeloma cells transfected with a vector expressing IL-3 (30), and Kit ligand from medium conditioned by CHO cells (provided by S. Webb, National Jewish Medical and Research Center, Denver, CO). After 4 wk of culture, 98% of nonadherent cells contained granules that stained positively with toluidine blue, and 98% expressed c-kit on their surface as determined by FACS analysis using anti-c-kit mab. Wild-type or Fc RI / mice were injected with BMMC i.v. either 1 day or 20 wk before staring the airway challenges and received either 10-day treatment with OVA or saline nebulization. C57BL/6 mice received BMMC from UBI-GFP mice i.v. 1 day before initiating the airway challenges with either saline or OVA. Assessment of airway smooth muscle responsiveness Forty-eight hours after the last airway challenge, AHR was monitored as airway smooth muscle responsiveness to EFS, measured as described previously (18). Tracheas were removed, and 0.5-cm preparations were placed in Krebs-Henseleit solution suspended by triangular supports transducing the force of contractions. EFS with an increasing frequency from 0.5 to 30 Hz was applied, and the contractions were measured. The duration of the stimulation was 1 ms. Frequencies resulting in 50% of the maximal contraction (ES 50 ) were calculated from linear plots from each individual animal and were compared between the groups. In addition, to assess postsynaptic cholinergic sensitivity of the tissues, cumulative dose-response curves to methacholine (MCh) were performed in half-log increments using concentrations ranging from 10 8 to 10 4 M. Results in the control and experimental groups at each time point were expressed in terms of the maximal contractile response as well as the EC 50 for MCh. Histology Lungs were fixed by inflation (1 ml) and immersion in 10% formalin. Cells containing eosinophilic major basic protein (MBP) were identified by immunohistochemical staining as previously described using rabbit antimouse MBP (provided by Dr. J. J. Lee, Mayo Clinic, Scottsdale, AZ). The slides were examined in a blinded fashion with a Nikon microscope (Melville, NY) equipped with a fluorescein filter system. The numbers of peribronchial eosinophils in the tissues were evaluated using IPLab2 software (Signal Analytics, Vienna, VA) for the Macintosh, counting six to eight different fields per animal. For detection of mucus-containing cells in formalin-fixed airway tissue, sections were stained with periodic acid- Schiff (PAS) and H&E and were quantitated as previously described (31). Tracheal sections were stained with 1% toluidine blue (Sigma-Aldrich) to detect metachromatic mast cell cytoplasmic granules. To maximize the ability to detect mast cells stained with toluidine blue, lung tissue was fixed in formalin for 24 h. Nonetheless, this may result in some underestimation of mast cell numbers. Tracheal sections from C57BL/6 mice receiving BMMCs derived from UBI-GFP mice were deparaffinized and mounted using mounting medium with 4,6-diamido-2-phenylindole hydrochloride (Vector Laboratories, Burlingame, CA). Assessment of IL-13 levels in lung homogenates Lungs were weighed and completely homogenized in dilution buffer (PBS, 0.1% Triton X (Sigma-Aldrich), and proteinase inhibitor (BD PharMingen, San Diego, CA)) using a tissue homogenizer (Tissue Tearor; BioSpec, Bartlesville, OK) and then centrifuged at 14,000 rpm for 30 min. Supernatants were collected and frozen at 80 C until further analysis. Total protein content was measured by colorimetric assay (DC Protein Assay; Bio-Rad), and levels of IL-13 were assessed by ELISA (R&D Systems, Minneapolis, MN) according to the manufacturer s directions. Measurement of total and OVA-specific Ab Serum levels of total IgE and OVA-specific IgE and IgG1 were measured by ELISA as previously described (31). Briefly, 96-well plates (Immunlon 2; Dynatech, Chantilly, VA) were coated with either OVA (5 g/ml) or purified anti-ige (02111D; BD PharMingen). After addition of serum samples, a biotinylated anti-ige Ab (02122D; BD PharMingen) was used as the detecting Ab, and the reaction was amplified with avidin-hrp (Sigma- Aldrich). IgG1 was detected using alkaline phosphatase-labeled anti-igg1 (02003E; BD PharMingen). The OVA-specific Ab titers of the samples were related to pooled standards that were generated in the laboratory and expressed as ELISA units per milliliter. Total IgE levels were calculated by comparison with known mouse IgE standards (BD PharMingen). The limit of detection was 100 pg/ml for total IgE. Statistical analysis ANOVA was used to determine the levels of difference between all groups. Comparisons for all pairs were performed using Tukey-Kramer honestly significant difference test, and p values for significance were set at Values for all measurements were expressed as the mean SEM. Results Aerosolized exposure to OVA increases total IgE and OVA-specific IgE and IgG1 in Fc RI / mice Mice exposed to 10-day OVA challenge (in the absence of adjuvant) demonstrate increased serum levels of OVA-specific IgE and
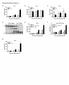
4 6400 AHR DEVELOPMENT REQUIRES MAST CELLS, Fc RI, AND IL-13 Table I. Levels of serum Igs a BALB/c 10 days saline BALB/c 10 days OVA BALB/c 10 days OVA higg BALB/c 10 days OVA sil-13rc 2 Fc RI / 10 days saline Fc RI / 10 days OVA IL-13 / 10 days saline IL-13 / 10 days OVA Total IgE (ng/ml) OVA-specific IgE (EU/ml) OVA-specific IgG1 (EU/ml) a Mice were challenged as described in Materials and Methods. Serum levels of Igs were assessed 48 h after the last challenge. Mean values SEM are given; Fc RI /, mice deficient of the high affinity IgE receptor; IL-13 /, mice deficient of IL-13; higg, mice treated with control Ab; sil-13rc 2, mice treated with soluble IL-13R 2 fusion protein; EU, ELISA units. IgG1 (32). To assess the effect of 10-day OVA nebulization exposure on Ig production in Fc RI / mice, we measured serum levels of total IgE and OVA-specific IgE and IgG1. OVA-challenged Fc RI / mice showed increased serum levels of total IgE and OVA-specific IgE and IgG1, which were similar to those in OVA-challenged wild-type mice and significantly higher ( p 0.05) than those in saline-challenged Fc RI / and wild-type mice (Table I). Fc RI / mice fail to develop AHR after 10-day OVA challenge To assess whether mast cells play a role in the development of AHR in this model, we challenged mast cell-deficient mice on 10 consecutive days with OVA. Indeed, OVA-challenged, mast celldeficient mice demonstrated no significant difference in ES 50 compared with the saline-challenged, mast cell-deficient mice (Fig. 1A), whereas the respective 10-day OVA-challenged, wild-type mice showed significantly ( p 0.05) lower ES 50 values than the saline-exposed wild-type mice (Fig. 1A). Similar results were found for Fc RI / mice. After 10-day OVA nebulization, wild-type mice showed a significantly lower ES 50 than saline-challenged animals, whereas OVA-challenged Fc RI / mice showed a response to EFS similar to that of salineexposed wild-type or Fc RI / mice (Fig. 1B). Overall responses to carbachol and maximal generated force were not statistically different between any of the groups (data not shown). Lung inflammation and goblet cell hyperplasia after 10-day OVA nebulization Following this protocol, few inflammatory cells were detectable in the bronchoalveolar lavage fluid. Lung tissue inflammation and, in particular, eosinophil accumulation were assessed using immunohistochemistry with anti-mbp. After the 10-day OVA challenge, wild-type mice demonstrated a modest increase in peribronchial eosinophil numbers compared with the saline-challenged control mice (Fig. 2). In OVA-challenged Fc RI / mice, no such increase in tissue inflammation was found (Fig. 2). To assess goblet cell hyperplasia, slides were stained with PAS. After 10-day OVA nebulization, wild-type mice demonstrated PAS-positive cells (mean SEM; PAS-positive cells/mm of basement membrane; p compared with other groups), whereas saline-challenged wild-type and saline- and OVA-challenged Fc RI / mice showed no PAS-positive cells (Fig. 3). Endotoxin has been shown to directly induce the expression of IL-13 in mast cells (33, 34) and therefore might induce increased airway responsiveness and goblet cell hyperplasia. To address potential contamination of the nebulized OVA with endotoxin on the development of increased airway reactivity and goblet cell hyperplasia, mice were exposed for 10 days to 1% OVA (endotoxin concentration, EU/mg OVA) or endotoxin-depleted 1% OVA (endotoxin concentration, 1.8 EU/mg OVA). After 10-day OVA exposure, mice receiving the endotoxin-depleted OVA developed similar increases in airway reactivity (Fig. 4A) and similar exposure of goblet cells (Fig. 4B) compared with mice receiving the untreated OVA. IL-13 levels in lung homogenates are not increased after allergen challenge in Fc RI-deficient mice IL-13 has been shown to be an important mediator in the development of AHR and goblet cell hyperplasia (35 38). To assess whether IL-13 is up-regulated in the 10-day challenge model, we FIGURE 1. Airway responsiveness in mast cell-deficient mice (A) and Fc RI-deficient mice (B). Mast cell-deficient mice were exposed to either 10-day saline (W/W v saline; n 8) or 10-day OVA (W/W v 10 day OVA; n 10) as were the wild-type control mice ( / saline, n 8; / 10 day OVA, n 8, respectively; data from two independent experiments). Similarly Fc RI-deficient mice received either 10-day saline (Fc RI / saline; n 12) or 10-day OVA (Fc RI / 10 day OVA; n 16) as did the wild-type controls (Fc RI / saline; n 12; Fc RI / 10 day OVA, n 18, respectively; data from four independent experiments). The mean SEM are given., p 0.01 compared with / saline, W/W v saline, and W/W v 10 day OVA; #, p 0.01 compared with Fc RI / saline, Fc RI / saline, and Fc RI / 10 day OVA.
5 The Journal of Immunology 6401 FIGURE 2. Role of Fc RI in eosinophil inflammation in the lung after allergen exposure. Peribronchial eosinophil inflammation was quantified in lung tissue stained with an Ab to MBP, and results are expressed as the number of MBP-positive cells per millimeter of basement membrane (BM). Peribronchial inflammation was assessed in saline-challenged (saline Fc RI / ; n 8) and OVA-challenged (OVA Fc RI / ; n 8) Fc RI / mice and in saline-challenged (saline Fc RI / ; n 6) and OVA-challenged (OVA Fc RI / ; n 8) Fc RI / mice. Data were obtained from two independent experiments; the mean SEM are given., p 0.05 compared with all other groups. measured levels of IL-13 in lung homogenates. Indeed, OVA-challenged wild-type mice exhibited increased levels of IL-13 in lung homogenates 48 h after the last challenge compared with levels in saline-challenged control mice (Fig. 4). However, OVA-challenged Fc RI / mice showed no elevation in the levels of IL-13 in their lung homogenates (Fig. 5). Similarly, lung homogenates of OVA-challenged mast cell-deficient mice exhibited significantly ( p 0.05) lower IL-13 levels compared with those of OVA-challenged mast cell-sufficient mice (Fig. 5). IL-13 mediates the development of AHR after 10-day OVA challenge To elucidate the role of IL-13 in the development of AHR after 10-day OVA challenge, we monitored tracheal smooth muscle responses to EFS in IL-13 / and IL-13 / mice challenged with OVA as well as after treatment with an inhibitor of IL-13 (sil- 13R 2). OVA-challenged IL-13 / mice showed no differences in EFS compared with saline-challenged IL-13 / and IL-13 / mice, and they were significantly different than the responses in OVA-challenged IL-13 / mice (Fig. 6). In parallel, OVA-challenged IL-13 / mice treated with sil-13r 2 during the challenge period normalized their EFS responses to levels seen in saline-challenged IL-13 / mice or IL-13 / animals (Fig. 6). The OVA-challenged IL-13 / and IL-13 / mice treated with sil- 13R 2 also showed no PAS-positive cells. Importantly, in these experiments, serum Ab levels were not statistically different in OVA-challenged IL-13 / vs IL-13 / mice or in sil-13r 2- vs human IgG-treated mice (Table I). Transfer of BMMC from wild-type to Fc RI-deficient mice restores their ability to develop AHR In rodents, Fc RI is expressed only on mast cells and basophils (39). We therefore investigated whether the inability of high affinity IgE receptor-deficient (Fc RI / IL-13 / ) and IL-13-deficient mice (Fc RI / IL-13 / ) to develop AHR could be overcome by adoptive transfer of BMMC from wild-type (Fc RI / IL-13 / ) animals. Bone marrow cells from Fc RI / IL-13 /, Fc RI / IL-13 /, and Fc RI / IL-13 / mice were cultured FIGURE 3. Role of Fc RI in goblet cell hyperplasia after allergen exposure. Goblet cell hyperplasia was detected using PAS staining 48 h after the last airway challenge in either 10-day saline-exposed (saline) or OVAexposed (10 day OVA) wild-type (Fc RI / ) or Fc RI-deficient (Fc RI / ) mice. Bar 50 m. under conditions described in Materials and Methods. After 4 wk, 98% of the cells in culture were considered to be mast cells, because they expressed c-kit (CD117) and Fc RI (in the case of Fc RI / donors) on their surfaces (data not shown). Mast cells were injected i.v. into wild-type, Fc RI /, and IL- 13 / recipients 1 day before starting the 10-day OVA challenge protocol. None of the recipients exposed to saline challenge alone showed any response to EFS (Fig. 7). The positive response to EFS was restored in Fc RI / IL-13 / mice that received BMMC from Fc RI / IL-13 / or Fc RI / IL-13 / mice before 10- day OVA challenge. Administration of sil-13r 2 to the Fc RI / IL-13 / recipients prevented the reconstitution of EFS responsiveness after transfer of BMMC from Fc RI / IL-13 / (mean SEM; ES 50, Hz; n 8 from two independent experiments) and Fc RI / IL-13 / donors ( Hz; n 7 from two independent experiments) and OVA exposure. In contrast, Fc RI / IL-13 / mice receiving autologous BMMC from Fc RI / IL-13 / mice and 10-day OVA challenge showed FIGURE 4. Endotoxin contamination does not affect airway responsiveness and goblet cell hyperplasia after allergen exposure. To assess the effect of endotoxin contamination on the development of increased airway responsiveness, BALB/c mice were exposed to 10-day saline (10 day saline; n 8 from two independent experiments), 10-day OVA (10 day OVA; n 8; from two independent experiments), or 10-day OVA that had been depleted of endotoxin (10 day OVA endotoxin-depleted). Forty-eight hours after the last challenge, airway responsiveness was assessed by EFS (A), and lung tissue was obtained and stained with PAS for quantification of goblet cells (B). N.D., not detected. The mean SEM are given., p 0.01 compared with 10-day saline.
6 6402 AHR DEVELOPMENT REQUIRES MAST CELLS, Fc RI, AND IL-13 FIGURE 5. Levels of IL-13 in lung homogenates. Levels of IL-13 and total protein content were assessed in lung homogenates 48 h after the last challenge from either saline-challenged (Fc RI / 10 day saline; n 8) or OVA-challenged (Fc RI / 10 day OVA; n 8) wild-type mice, OVA-challenged Fc RI / mice (Fc RI / 10 day OVA; n 7), and OVA-challenged mast cell-deficient mice (W/W v 10 day OVA; n 8) as well as their respective OVA-challenged wild-type controls ( / 10 day OVA; n 8). The mean SEM from two independent experiments are given., p 0.01; #, p no response to EFS. This confirms the requirement for Fc RIsufficient mast cells in the development of a positive response to EFS. The results were similar when BMMC transfer was performed 20 wk before staring the 10-day OVA exposure. Again, Fc RI / IL-13 / mice receiving BMMC from Fc RI / IL-13 / mice before 10-day OVA exposure showed a significantly ( p 0.012) lower ES 50 (mean SEM; Hz; n 9 from two independent experiments) compared with Fc RI / IL-13 / mice receiving autologous BMMC from Fc RI / IL-13 / mice before 10-day OVA exposure ( Hz; n 6 from two independent experiments). Transfer of BMMC from wild-type to IL-13-deficient mice does not restore their ability to develop AHR In addition to the need for Fc RI-sufficient mast cells in the development of smooth muscle hyper-responsiveness to EFS after 10-day OVA challenge, a role for IL-13 was also identified. Mast cells are a potential source of IL-13 (40). However, in the adoptive transfer experiments described in Fig. 7, Fc RI / IL-13 / recipients of Fc RI / IL-13 / BMMC failed to develop EFS responses after 10-day OVA challenge. This occurred despite the fact that these cells, in the same numbers, were capable of reconstituting the EFS response in Fc RI / IL-13 / mice (Fig. 7). Mast cells are can be detected in tracheal tissue of Fc RI / mice To assess whether mast cells can be detected in tracheal tissue from Fc RI / mice, tracheal sections from 10-day OVA-challenged Fc RI / mice and 10-day OVA-challenged Fc RI / after transfer of BMMCs were stained with toluidine blue. In both groups mast cells were detected in the subepithelial region as well as in close proximity to smooth muscle (Fig. 8). To further assess whether transferred BMMCs migrate to tracheal tissue, green-fluorescent BMMCs from UBI-GFP mice were transferred to C57BL/6 recipients 1 day before initiating the airway challenges. After 10-day exposure to either saline or OVA, transferred greenfluorescent cells could be detected in the tracheal tissue 48 h after the last challenge (Fig. 8). In saline-exposed mice we detected 1 1 GFP mast cells per section, whereas in OVA-exposed mice, we detected GFP mast cells (n 4 in each group). Discussion Among the many features of allergic asthma is an increase in levels of serum IgE, and in epidemiologic studies a relationship between IgE serum levels and severity of AHR has been established (41). In the present study we examined the role of the high affinity IgE receptor (Fc RI) and by implication IgE in the development of allergic airway disease, using mice deficient in Fc RI due to disruption of the Fc RI gene. These mice are essentially normal in all aspects of their development and maturation, have functional mast cells (22, 23), which can be found in tracheal tissue. Additionally, Fc RI / mice are able to mount an immune response to allergen exposure, as shown by elevated levels of total IgE and allergen-specific IgE and IgG1. In these respects Fc RI-deficient mice are similar to wild-type mice. In contrast, in other aspects of allergic airway disease, allergen-exposed Fc RI / mice failed to develop increased airway reactivity, goblet cell hyperplasia, and airway inflammation. This phenotype in Fc RI / mice is unmasked only when they are exposed to allergen, in this case via the airways, in the absence of adjuvant. This contrasts with their response to systemic sensitization (together with adjuvant), followed by airway challenge, where Fc RI / mice develop AHR and airway inflammation similar to those exhibited by their sensitized and challenged wild-type littermates (42). Furthermore, in the 10-day OVA challenge model the heightened airway reactivity they develop is detected as a change in the response of tracheal smooth muscle to EFS, a consequence of altered muscarinic receptor 2 function and increased acetylcholine release (18) The allergen exposure protocols have been associated with differences in the approaches to detect altered airway function. After the 10-day aerosolized allergen exposure, these mice do not develop MChinduced AHR as seen in systemically sensitized mice (42). FIGURE 6. IL-13 mediates the development of increased airway responsiveness after 10-day OVA exposure. Wild-type mice treated with control Ab (IL-13 /, 10 day OVA; n 6) or with sil-13r 2 (IL-13 /, 10 day OVA; n 10) as well as IL-13-deficient mice (IL-13 / 10 day OVA; n 8) were exposed to 10-day OVA challenge. As a control, IL- 13-deficient mice were exposed to 10-day saline (IL-13 / saline OVA; n 6). The mean SEM from two independent experiments are given., p 0.01 compared with all other groups.
7 The Journal of Immunology 6403 FIGURE 7. Transfer of wild-type BM- MCs to Fc RI / mice reconstitutes their ability to develop AHR. BMMCs derived from wild-type mice (Fc RI / IL-13 / ), Fc RI-deficient mice (Fc RI / IL-13 / ), or IL-13-deficient mice (Fc RI / IL- 13 / ) were transferred to wild-type (wildtype), Fc RI-deficient (Fc RI / ), or IL-13- deficient (IL-13 / ) recipients, which were then challenged with OVA (10 day OVA). Each condition contained eight mice, and the mean SEM from two independent experiments are given., p 0.01 compared with saline-challenged (10 day OVA-) wild-type recipients; #, p 0.01 compared with salinechallenged (OVA-) and Fc RI / IL-13 / transferred Fc RI / recipients. In rodents, Fc RI has been found to be expressed only on mast cells and basophils (39). Indeed, in support of the findings in Fc RI / mice, mast cell-deficient mice also failed to develop increased airway reactivity after 10-day OVA exposure. This finding is somewhat in contrast to previous studies using mast celldeficient mice, which suggested that the induction of airway inflammation and AHR does not require the presence of mast cells FIGURE 8. Transferred BMMCs can be found in tracheal tissue. Sections of tracheal tissue from 10-day OVA-challenged Fc RI / (A and B) and from 10-day OVA-challenged Fc RI / after transfer of BMMCs (C and D) were stained with toluidine blue. Mast cells (arrows) were detected in the subepithelial region as well as in close proximity to smooth muscle (bar 50 m). After transfer, BMMCs derived from UBI-GFP mice were detected in tracheal tissue of 10-day saline-challenged recipient C57BL/6 mice (E) as well as 10-day OVA-challenged recipient C57BL/6 mice (F) 48 h after the last challenge. In saline- as well as OVA-challenged mice, fluorescent signals from GFP positive cells (green) were detected in tracheal tissue. Blue staining are nuclei stained with DAPI. Note the weak background fluorescence in epithelial cells. Magnification, 100. (13, 15). Similarly, it has been shown that the presence of IgE is not mandatory for the development of allergic airway disease (43, 44). In most of these studies animals were sensitized systemically by injection of the allergen in combination with an adjuvant and then challenged via the airways, which leads to marked inflammatory changes in the lung, high serum levels of allergen-specific Abs, increased airway reactivity including sensitivity to inhaled MCh, and prominent goblet cell hyperplasia. In the present study mice were exposed to a less potent exposure protocol using aerosolized allergen alone. This resulted in little airway inflammation and less goblet cell hyperplasia than seen after systemic sensitization. Under these conditions without adjuvant, mast cells appear to play an essential role in the development of allergic airway disease, as mast cell-deficient mice fail to develop increased airway reactivity after aerosolized allergen exposure. Similarly, mice lacking the Fc RI fail to develop AHR after this exposure protocol. These findings share some features with recent reports using different systemic allergen exposure protocols (16, 45). In those reports, where mast cells and Fc RI were found to be critical for the development of AHR and airway inflammation, the exposure protocol deviated from those using repeated systemic sensitization and adjuvant, conditions under which mast cells and IgE were shown not to be important (15, 43). Williams et al. (16) found that mast cell-deficient mice exhibited weaker airway responsiveness and lung tissue eosinophil inflammation after a systemic sensitization protocol, but without adjuvant. In a different study, Mayr et al. (45) described the inability of Fc RI-deficient mice to develop allergic airway inflammation and AHR to MCh after systemic sensitization consisting of a single OVA injection (with adjuvant) and consecutive intranasal challenges. IgE can bind either to Fc RI or to the low affinity IgE receptor (Fc RII, CD23). Whereas cross-linking of Fc RI with IgE and allergen has been associated with mast cell activation, ligation of Fc RII can be either activating (carrying an immunoreceptor tyrosine-based activation motif) or inhibitory (carrying an immunoreceptor tyrosine-based inhibitory motif). In allergic airway disease, Fc RII has been shown to exhibit negative regulatory effects (46). In the present study cross-linking of Fc RI seemed to be activating in the development of increased airway reactivity and goblet cell hyperplasia, as Fc RI / mice failed to develop increased smooth muscle responsiveness after allergen exposure. Interestingly, transfer of Fc RI / BMMC to Fc RI / animals 14 days before the assessment of airway function fully reconstituted
8 6404 AHR DEVELOPMENT REQUIRES MAST CELLS, Fc RI, AND IL-13 their ability to develop increased airway reactivity, suggesting that in this model the expression of Fc RI on the mast cells is important and that mast cells alone can reconstitute this response. Previously, transfer experiments with BMMCs have been performed mainly to reconstitute mast cells in mast cell-deficient mice (16, 47 49). In that approach the analysis was conducted 10 wk or more after mast cell transfer. In the present study we assessed the response to 10- day OVA challenge at 2 and 20 wk after transfer of Fc RI / BMMC into Fc RI / mice. In both cases the responses were similar. After transfer of green fluorescent BMMCs derived from GFP-overexpressing mice, we were able to detect transferred cells in the tracheal tissue 14 days post-transfer, suggesting that this time period is sufficient for migration of transferred cells to the trachea. Transfer of Fc RI / cells reconstituted the ability of Fc RI / mice to develop increased airway reactivity independent of the time point after the transfer was made. In other disease models, mast cell reconstitution in mast cell-deficient mice normalized the ability to mount a mast cell-dependent response 2 days (50) and 9 days (51) after the transfer. In the present study we used BMMCs cultured in a mixture of IL-3 and Kit ligand for 4 wk. Under these conditions, 98% of the cells expressed Fc RI as well as c-kit on their surface and previous studies have suggested that the overwhelming majority of cells grown under these culture conditions are mast cells (52, 53) as well as out own electron microscopy studies. A very small percentage have features of basophils (52, 53), so it cannot be completely excluded that basophils, which may also express Fc RI and c-kit on their surface, may contribute to the reconstitution of the response. The finding that Fc RI / mast cells alone can restore responsiveness in Fc RI / mice does not differentiate between the activated mast cells having a direct role in the EFS response and their having an indirect effect through the release of mediators that trigger other cells necessary for the EFS response. Activation of lung mast cells through Fc RI leads to the release of a variety of mediators via degranulation. Activation also triggers cytokine transcription and protein synthesis. A significant finding was that lung homogenates from allergen-exposed Fc RI / mice had significantly lower levels of IL-13 than those from allergenexposed wild-type controls. Altered airway function and goblet cell hyperplasia have been closely linked to IL-13 expression in the lung (35 38, 54), and IL-13 may directly act on epithelial cells to induce goblet cell hyperplasia and airway hyper-reactivity (55). As a pleiotropic cytokine, IL-13 is secreted by activated Th2 cells and exhibits immunoregulatory activities that partially overlap with those of IL-4 (56). IL-13 also facilitates the preferential recruitment of eosinophils (and T cells) to the airway tissues (57) and airway mucus secretion, which can exacerbate airway responsiveness (54, 58). Although not necessary for, or even capable of, inducing Th2 development, IL-13 plays a regulatory role in Th2 cell activation (24). Administration of IL-13 or overexpression of IL-13 in the airways induced airway eosinophilia, mucus production, and AHR to varying degrees (35, 36, 54). In further attempts to link mast cells, Fc RI, and IL-13 in the present model, we chose two approaches: using IL-13 gene-targeted mice (24, 37) and the other treatment of mice during the challenge period with the decoy receptor sil-13r 2 (35, 36, 38). Both IL-13 / mice and sil-13r 2-treated mice had levels of serum Abs similar to those of the wild-type mice, confirming that in mice, IL-13 does not regulate serum Ab production (37, 38). Furthermore, IL-13 / mice have fully functional mast cells that signal through Fc RI, degranulate, express similar amounts of cytokines (other than IL-13) and release of lipid mediators and after activation with allergen-specific IgE and allergen (data not shown). Both approaches revealed that the presence of IL-13 was necessary for development of the heightened response to EFS and goblet cell hyperplasia after the 10-day OVA challenge. In addition to T cells, mast cells produce and secrete IL-13 (40). In rodents it has been shown that, depending on their phenotype, mast cells express IL-13 mrna either constitutively or only after Fc RI-mediated activation (59). All of our results in the 10-day OVA challenge model are consistent with the idea that mast cells are an important source of IL-13. Mast cells may produce IL-13 after stimulation with endotoxin (33, 34). However, in the present model endotoxin contamination of OVA seemed to be irrelevant to the development of increased airway reactivity and goblet cell hyperplasia, as OVA depleted of endotoxin, induced similar degrees of airway reactivity and goblet cell hyperplasia. Interestingly, IL- 13 / mice failed to develop AHR even after adoptive transfer of IL-13 / mast cells, suggesting that the reconstitution solely of mast cells capable of producing IL-13 is not enough to change airway reactivity. This observation, together with the demonstration that transfer of BMMC from Fc RI / IL-13 / mice to Fc RI / IL-13 / recipients restores their ability to develop AHR, indicates that activation of mast cells through Fc RI is directing IL-13 production in the lung, a critical element in the development of altered airway function. However, under these conditions, mast cells may not be the predominant source of the IL-13 needed for this response. This does not diminish the need for IL- 13, as reconstitution of airway responsiveness after mast cell transfer (even from IL-13 / mice) was still critically dependent on IL-13; treatment with IL-13R 2 after the mast cell transfer completely inhibited the reconstitution of increased airway responsiveness. We may speculate either that the IL-13 derived from the numbers of transferred mast cells (IL-13 / into IL-13 / ) was insufficient to restore AHR or that other cell types are a major source of IL-13 when stimulated by factors released from activated mast cells. There are a number of other cell types that may serve as a source of IL-13 after activation by a factor(s) released from IgE-Fc RI-activated mast cells, including T cells, smooth muscle cells (60), basophils, and NKT cells (61, 62). Studies assessing these potential sources are underway. In summary, we have demonstrated essential roles for Fc RI, mast cells, and IL-13 in the development of allergic airway disease after allergen exposure exclusively via the lungs in the absence of adjuvant. Fc RI on mast cells mediates these effects by regulating the production of IL-13. As aeroallergen exposure via the lungs in the absence of adjuvant is a major factor in the etiology of asthma, this IgE-mast cell-il-13 pathway may play a significant contributory role in the development, maintenance, and exacerbation of the disease. Acknowledgments We thank Dr. J. J. Lee (Mayo Clinic, Scottsdale, AZ) for providing the anti-mbp Ab, and L. N. Cunningham, D. Nabighian, and L. Sharp (National Jewish Medical and Research Center, Denver, CO) for their assistance. References 1. Sporik, R., S. T. Holgate, T. A. Platts-Mills, and J. J. Cogswell Exposure to house-dust mite allergen (Der p I) and the development of asthma in childhood: a prospective study. N. Engl. J. Med. 323: Peat, J. K., E. Tovey, B. G. Toelle, M. M. Haby, E. J. Gray, A. Mahmic, and A. J. Woolcock House dust mite allergens: a major risk factor for childhood asthma in Australia. Am. J. Respir. Crit. Care Med. 153: Cartier, A., N. C. Thomson, P. A. Frith, R. Roberts, and F. E. Hargreave Allergen-induced increase in bronchial responsiveness to histamine: relationship to the late asthmatic response and change in airway caliber. J. Allergy Clin. Immunol. 70: Boulet, L. P., A. Cartier, N. C. Thomson, R. S. Roberts, J. Dolovich, and F. E. Hargreave Asthma and increases in nonallergic bronchial responsiveness from seasonal pollen exposure. J. Allergy Clin. Immunol. 71:399.
9 The Journal of Immunology Turner, H., and J. P. Kinet Signalling through the high-affinity IgE receptor Fc epsilonri. Nature 402:B Brightling, C. E., P. Bradding, F. A. Symon, S. T. Holgate, A. J. Wardlaw, and I. D. Pavord Mast-cell infiltration of airway smooth muscle in asthma. N. Engl. J. Med. 346: Metcalfe, D. D., D. Baram, and Y. A. Mekori Mast cells. Physiol. Rev. 77: Garrington, T. P., T. Ishizuka, P. J. Papst, K. Chayama, S. Webb, T. Yujiri, W. Sun, S. Sather, D. M. Russell, S. B. Gibson, et al MEKK2 gene disruption causes loss of cytokine production in response to IgE and c-kit ligand stimulation of ES cell-derived mast cells. EMBO J. 19: Chayama, K., P. J. Papst, T. P. Garrington, J. C. Pratt, T. Ishizuka, S. Webb, S. Ganiatsas, L. I. Zon, W. Sun, G. L. Johnson, et al Role of MEKK2- MEK5 in the regulation of TNF- gene expression and MEKK2-MKK7 in the activation of c-jun N-terminal kinase in mast cells. Proc. Natl. Acad. Sci. USA 98: Kung, T. T., D. Stelts, J. A. Zurcher, H. Jones, S. P. Umland, W. Kreutner, R. W. Egan, and R. W. Chapman Mast cells modulate allergic pulmonary eosinophilia in mice. Am. J. Respir. Cell Mol. Biol. 12: Ogawa, K., O. Kaminuma, H. Kikkawa, R. Kameda, K. Ikezawa, M. Suko, H. Okudaira, K. Akiyama, and A. Mori Primary role of CD4 T cells and supplemental role of mast cells in allergic pulmonary eosinophilia. Int. Arch. Allergy Immunol. 120(Suppl. 1): Nogami, M., M. Suko, H. Okudaira, T. Miyamoto, J. Shiga, M. Ito, and S. Kasuya Experimental pulmonary eosinophilia in mice by Ascaris suum extract. Am. Rev. Respir. Dis. 141: Brusselle, G. G., J. C. Kips, J. H. Tavernier, J. G. van der Heyden, C. A. Cuvelier, R. A. Pauwels, and H. Bluethmann Attenuation of allergic airway inflammation in IL-4 deficient mice. Clin. Exp. Allergy. 24: Nagai, H., S. Yamaguchi, Y. Maeda, and H. Tanaka Role of mast cells, eosinophils and IL-5 in the development of airway hyperresponsiveness in sensitized mice. Clin. Exp. Allergy 26: Takeda, K., E. Hamelmann, A. Joetham, L. D. Shultz, G. L. Larsen, C. G. Irvin, and E. W. Gelfand Development of eosinophilic airway inflammation and airway hyperresponsiveness in mast cell-deficient mice. J. Exp. Med. 186: Williams, C. M., and S. J. Galli Mast cells can amplify airway reactivity and features of chronic inflammation in an asthma model in mice. J. Exp. Med. 192: Kobayashi, T., T. Miura, T. Haba, M. Sato, I. Serizawa, H. Nagai, and K. Ishizaka An essential role of mast cells in the development of airway hyperresponsiveness in a murine asthma model. J. Immunol. 164: Larsen, G. L., H. Renz, J. E. Loader, K. L. Bradley, and E. W. Gelfand Airway response to electrical field stimulation in sensitized inbred mice: passive transfer of increased responsiveness with peribronchial lymph nodes. J. Clin. Invest. 89: Larsen, G. L., T. M. Fame, H. Renz, J. E. Loader, J. Graves, M. Hill, and E. W. Gelfand Increased acetylcholine release in tracheas from allergenexposed IgE-immune mice. Am. J. Physiol. 266:L Renz, H., G. Lack, J. Saloga, R. Schwinzer, K. Bradley, J. Loader, A. Kupfer, G. L. Larsen, and E. W. Gelfand Inhibition of IgE production and normalization of airways responsiveness by sensitized CD8 T cells in a mouse model of allergen-induced sensitization. J. Immunol. 152: Hamelmann, E., A. T. Vella, A. Oshiba, J. W. Kappler, P. Marrack, and E. W. Gelfand Allergic airway sensitization induces T cell activation but not airway hyperresponsiveness in B cell-deficient mice. Proc. Natl. Acad. Sci. USA 94: Dombrowicz, D., V. Flamand, K. K. Brigman, B. H. Koller, and J. P. Kinet Abolition of anaphylaxis by targeted disruption of the high affinity immunoglobulin E receptor chain gene. Cell 75: Dombrowicz, D., V. Flamand, I. Miyajima, J. V. Ravetch, S. J. Galli, and J. P. Kinet Absence of Fc RI chain results in upregulation of Fc RIIIdependent mast cell degranulation and anaphylaxis: evidence of competition between Fc RI and Fc RIII for limiting amounts of FcR and chains. J. Clin. Invest. 99: McKenzie, G. J., C. L. Emson, S. E. Bell, S. Anderson, P. Fallon, G. Zurawski, R. Murray, R. Grencis, and A. N. McKenzie Impaired development of Th2 cells in IL-13-deficient mice. Immunity 9: Schaefer, B. C., M. L. Schaefer, J. W. Kappler, P. Marrack, and R. M. Kedl Observation of antigen-dependent CD8 T-cell/dendritic cell interactions in vivo. Cell. Immunol. 214: Donaldson, D. D., M. J. Whitters, L. J. Fitz, T. Y. Neben, H. Finnerty, S. L. Henderson, R. M. O Hara, Jr., D. R. Beier, K. J. Turner, C. R. Wood, et al The murine IL-13 receptor 2: molecular cloning, characterization, and comparison with murine IL-13 receptor 1. J. Immunol. 161: Bordier, C Phase separation of integral membrane proteins in Triton X-114 solution. J. Biol. Chem. 256: Aida, Y., and M. J. Pabst Removal of endotoxin from protein solutions by phase separation using Triton X-114. J. Immunol. Methods 132: Ishizuka, T., K. Chayama, K. Takeda, E. Hamelmann, N. Terada, G. M. Keller, G. L. Johnson, and E. W. Gelfand Mitogen-activated protein kinase activation through Fc receptor I and stem cell factor receptor is differentially regulated by phosphatidylinositol 3-kinase and calcineurin in mouse bone marrowderived mast cells. J. Immunol. 162: Karasuyama, H., and F. Melchers Establishment of mouse cell lines which constitutively secrete large quantities of interleukin 2, 3, 4 or 5, using modified cdna expression vectors. Eur. J. Immunol. 18: Tomkinson, A., C. Duez, G. Cieslewicz, J. C. Pratt, A. Joetham, M. C. Shanafelt, R. Gundel, and E. W. Gelfand A murine IL-4 receptor antagonist that inhibits IL-4- and IL-13-induced responses prevents antigen-induced airway eosinophilia and airway hyperresponsiveness. J. Immunol. 166: Renz, H., H. R. Smith, J. E. Henson, B. S. Ray, C. G. Irvin, and E. W. Gelfand Aerosolized antigen exposure without adjuvant causes increased IgE production and increased airway responsiveness in the mouse. J. Allergy Clin. Immunol. 89: Stassen, M., C. Muller, M. Arnold, L. Hultner, S. Klein-Hessling, C. Neudorfl, T. Reineke, E. Serfling, and E. Schmitt IL-9 and IL-13 production by activated mast cells is strongly enhanced in the presence of lipopolysaccharide: NF- B is decisively involved in the expression of IL-9. J. Immunol. 166: Masuda, A., Y. Yoshikai, K. Aiba, and T. Matsuguchi Th2 cytokine production from mast cells is directly induced by lipopolysaccharide and distinctly regulated by c-jun N-terminal kinase and p38 pathways. J. Immunol. 169: Grunig, G., M. Warnock, A. E. Wakil, R. Venkayya, F. Brombacher, D. M. Rennick, D. Sheppard, M. Mohrs, D. D. Donaldson, R. M. Locksley, et al Requirement for IL-13 independently of IL-4 in experimental asthma. Science 282: Wills-Karp, M., J. Luyimbazi, X. Xu, B. Schofield, T. Y. Neben, C. L. Karp, and D. D. Donaldson Interleukin-13: central mediator of allergic asthma. Science 282: Walter, D. M., J. J. McIntire, G. Berry, A. N. McKenzie, D. D. Donaldson, R. H. DeKruyff, and D. T. Umetsu Critical role for IL-13 in the development of allergen-induced airway hyperreactivity. J. Immunol. 167: Taube, C., C. Duez, Z. H. Cui, K. Takeda, Y. H. Rha, J. W. Park, A. Balhorn, D. D. Donaldson, A. Dakhama, and E. W. Gelfand The role of IL-13 in established allergic airway disease. J. Immunol. 169: Kinet, J. P The high-affinity IgE receptor (Fc RI): from physiology to pathology. Annu. Rev. Immunol. 17: Burd, P. R., W. C. Thompson, E. E. Max, and F. C. Mills Activated mast cells produce interleukin 13. J. Exp. Med. 181: Burrows, B., F. D. Martinez, M. Halonen, R. A. Barbee, and M. G. Cline Association of asthma with serum IgE levels and skin-test reactivity to allergens. N. Engl. J. Med. 320: Hamelmann, E., K. Tadeda, A. Oshiba, and E. W. Gelfand Role of IgE in the development of allergic airway inflammation and airway hyperresponsiveness: a murine model. Allergy 54: Mehlhop, P. D., M. van de Rijn, A. B. Goldberg, J. P. Brewer, V. P. Kurup, T. R. Martin, and H. C. Oettgen Allergen-induced bronchial hyperreactivity and eosinophilic inflammation occur in the absence of IgE in a mouse model of asthma. Proc. Natl. Acad. Sci. USA 94: Hamelmann, E., G. Cieslewicz, J. Schwarze, T. Ishizuka, A. Joetham, C. Heusser, and E. W. Gelfand Anti-interleukin 5 but not anti-ige prevents airway inflammation and airway hyperresponsiveness. Am. J. Respir. Crit. Care Med. 160: Mayr, S. I., R. I. Zuberi, M. Zhang, J. de Sousa-Hitzler, K. Ngo, Y. Kuwabara, L. Yu, W. P. Fung-Leung, and F. T. Liu IgE-dependent mast cell activation potentiates airway responses in murine asthma models. J. Immunol. 169: Haczku, A., K. Takeda, E. Hamelmann, J. Loader, A. Joetham, I. Redai, C. G. Irvin, J. J. Lee, H. Kikutani, D. Conrad, et al CD23 exhibits negative regulatory effects on allergic sensitization and airway hyperresponsiveness. Am. J. Respir. Crit. Care Med. 161: Nakano, T., T. Sonoda, C. Hayashi, A. Yamatodani, Y. Kanayama, T. Yamamura, H. Asai, T. Yonezawa, Y. Kitamura, and S. J. Galli Fate of bone marrow-derived cultured mast cells after intracutaneous, intraperitoneal, and intravenous transfer into genetically mast cell-deficient W/Wv mice: evidence that cultured mast cells can give rise to both connective tissue type and mucosal mast cells. J. Exp. Med. 162: Otsu, K., T. Nakano, Y. Kanakura, H. Asai, H. R. Katz, K. F. Austen, R. L. Stevens, S. J. Galli, and Y. Kitamura Phenotypic changes of bone marrow-derived mast cells after intraperitoneal transfer into W/Wv mice that are genetically deficient in mast cells. J. Exp. Med. 165: Kraneveld, A. D., H. P. van der Kleij, M. Kool, A. H. van Houwelingen, A. C. Weitenberg, F. A. Redegeld, and F. P. Nijkamp Key role for mast cells in nonatopic asthma. J. Immunol. 169: Wershil, B. K., Y. A. Mekori, T. Murakami, and S. J. Galli I-fibrin deposition in IgE-dependent immediate hypersensitivity reactions in mouse skin: demonstration of the role of mast cells using genetically mast cell-deficient mice locally reconstituted with cultured mast cells. J. Immunol. 139: Qureshi, R., and B. A. Jakschik The role of mast cells in thioglycollateinduced inflammation. J. Immunol. 141: Rottem, M., J. P. Goff, J. P. Albert, and D. D. Metcalfe The effects of stem cell factor on the ultrastructure of Fc RI cells developing in IL-3-dependent murine bone marrow-derived cell cultures. J. Immunol. 151:4950.
Role of immunoglobulin E and mast cells in murine models of asthma
 Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Mast Cell-Derived Tumor Necrosis Factor is Essential. for Allergic Airway Disease
 ERJ Express. Published on December 19, 2007 as doi: 10.1183/09031936.00058907 Mast Cell-Derived Tumor Necrosis Factor is Essential for Allergic Airway Disease Sebastian Reuter 1, Anke Heinz 1, Michael
ERJ Express. Published on December 19, 2007 as doi: 10.1183/09031936.00058907 Mast Cell-Derived Tumor Necrosis Factor is Essential for Allergic Airway Disease Sebastian Reuter 1, Anke Heinz 1, Michael
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice
 Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
IL-13 is essential to the late-phase response in allergic rhinitis
 Original articles IL-13 is essential to the late-phase response in allergic rhinitis Satoko Miyahara, MD, PhD, Nobuaki Miyahara, MD, PhD, Shigeki Matsubara, PhD, Katsuyuki Takeda, MD, PhD, Toshiyuki Koya,
Original articles IL-13 is essential to the late-phase response in allergic rhinitis Satoko Miyahara, MD, PhD, Nobuaki Miyahara, MD, PhD, Shigeki Matsubara, PhD, Katsuyuki Takeda, MD, PhD, Toshiyuki Koya,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Figure S1. Generation of inducible PTEN deficient mice and the BMMCs (A) B6.129 Pten loxp/loxp mice were mated with B6.
 Figure S1. Generation of inducible PTEN deficient mice and the BMMCs (A) B6.129 Pten loxp/loxp mice were mated with B6.129-Gt(ROSA)26Sor tm1(cre/ert2)tyj /J mice. To induce deletion of the Pten locus,
Figure S1. Generation of inducible PTEN deficient mice and the BMMCs (A) B6.129 Pten loxp/loxp mice were mated with B6.129-Gt(ROSA)26Sor tm1(cre/ert2)tyj /J mice. To induce deletion of the Pten locus,
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c)
 1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure
 Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure Shigeki Matsubara 1, Christina H. Swasey 1, Joan E. Loader 1, Azzeddine Dakhama 1, Anthony Joetham 1, Hiroshi Ohnishi
Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure Shigeki Matsubara 1, Christina H. Swasey 1, Joan E. Loader 1, Azzeddine Dakhama 1, Anthony Joetham 1, Hiroshi Ohnishi
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Mast cells can promote the development of multiple features of chronic asthma in mice
 Research article Mast cells can promote the development of multiple features of chronic asthma in mice Mang Yu, 1 Mindy Tsai, 1 See-Ying Tam, 1 Carol Jones, 1 James Zehnder, 1 and Stephen J. Galli 1,2
Research article Mast cells can promote the development of multiple features of chronic asthma in mice Mang Yu, 1 Mindy Tsai, 1 See-Ying Tam, 1 Carol Jones, 1 James Zehnder, 1 and Stephen J. Galli 1,2
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice
 Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Allergic diseases and treatment. Feng Qian ( 钱峰 )
 Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
colorimetric sandwich ELISA kit datasheet
 colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma
 Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Allergen and Environment in Severe Asthma
 Allergen and Environment in Severe Asthma Hye-Ryun Kang MD., PhD. Department of Internal Medicine, Seoul National University Hospital Role of Allergen in Asthma Pathogenesis Early response of allergen
Allergen and Environment in Severe Asthma Hye-Ryun Kang MD., PhD. Department of Internal Medicine, Seoul National University Hospital Role of Allergen in Asthma Pathogenesis Early response of allergen
Supplemental Figures: Supplemental Figure 1
 Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin
 CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs
 Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538
 Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538 Background: TIGIT is a co-inhibitory receptor that is highly expressed in Natural Killer (NK) cells, activated CD4+, CD8+ and regulatory
Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538 Background: TIGIT is a co-inhibitory receptor that is highly expressed in Natural Killer (NK) cells, activated CD4+, CD8+ and regulatory
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
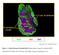 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
GSI Canine IL-5 ELISA Kit-2 Plates DataSheet
 Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
(a) Significant biological processes (upper panel) and disease biomarkers (lower panel)
 Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Comparative Roles of IL-4, IL-13, and IL-4R α in Dendritic Cell Maturation and CD4 + Th2 Cell Function
 This information is current as of July 3, 2018. Comparative Roles of IL-4, IL-13, and IL-4R α in Dendritic Cell Maturation and CD4 + Th2 Cell Function Dianne C. Webb, Yeping Cai, Klaus I. Matthaei and
This information is current as of July 3, 2018. Comparative Roles of IL-4, IL-13, and IL-4R α in Dendritic Cell Maturation and CD4 + Th2 Cell Function Dianne C. Webb, Yeping Cai, Klaus I. Matthaei and
New millennium: The conquest of allergy (Supported by a grant from Novartis Pharmaceutical Corp., East Hanover, NJ)
 New millennium: The conquest of allergy (Supported by a grant from Novartis Pharmaceutical Corp., East Hanover, NJ) Series editors: Donald Y. M. Leung, MD, PhD, Stanley J. Szefler, MD, and Harold S. Nelson,
New millennium: The conquest of allergy (Supported by a grant from Novartis Pharmaceutical Corp., East Hanover, NJ) Series editors: Donald Y. M. Leung, MD, PhD, Stanley J. Szefler, MD, and Harold S. Nelson,
Assessment of a rapid liquid based cytology method for measuring sputum cell counts
 Assessment of a rapid liquid based cytology method for measuring sputum cell counts Martin MJ, Lee H, Meakin G, Green A, Simms RL, Reynolds C, Winters S*, Shaw DE, Soomro I*, Harrison TW The Asthma Centre
Assessment of a rapid liquid based cytology method for measuring sputum cell counts Martin MJ, Lee H, Meakin G, Green A, Simms RL, Reynolds C, Winters S*, Shaw DE, Soomro I*, Harrison TW The Asthma Centre
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells
 1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
MyBioSource.com. Instructions for use. Histamine Release
 Instructions for use Histamine Release Supplementary kit for the determination of the release of histamine from heparinized whole blood (this kit has to be used in combination with the Histamine ELISA,
Instructions for use Histamine Release Supplementary kit for the determination of the release of histamine from heparinized whole blood (this kit has to be used in combination with the Histamine ELISA,
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Grass pollen immunotherapy induces Foxp3 expressing CD4 + CD25 + cells. in the nasal mucosa. Suzana Radulovic MD, Mikila R Jacobson PhD,
 Radulovic 1 1 2 3 Grass pollen immunotherapy induces Foxp3 expressing CD4 + CD25 + cells in the nasal mucosa 4 5 6 7 Suzana Radulovic MD, Mikila R Jacobson PhD, Stephen R Durham MD, Kayhan T Nouri-Aria
Radulovic 1 1 2 3 Grass pollen immunotherapy induces Foxp3 expressing CD4 + CD25 + cells in the nasal mucosa 4 5 6 7 Suzana Radulovic MD, Mikila R Jacobson PhD, Stephen R Durham MD, Kayhan T Nouri-Aria
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
How close are we to predicting allergenicity of new proteins? 13 April 2012, Praha Corinne Herouet-Guicheney, PhD
 How close are we to predicting allergenicity of new proteins? 13 April 2012, Praha Corinne Herouet-Guicheney, PhD Agenda/ Content Potential risk and basic principles Current status in developing a model
How close are we to predicting allergenicity of new proteins? 13 April 2012, Praha Corinne Herouet-Guicheney, PhD Agenda/ Content Potential risk and basic principles Current status in developing a model
Mouse Serum Anti-HDM IgE Antibody Assay Kit
 Mouse Serum Anti-HDM IgE Antibody Assay Kit Catalog # 3037 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people
Mouse Serum Anti-HDM IgE Antibody Assay Kit Catalog # 3037 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge
 Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Regulation of Type 2 Immunity by Basophils Prof. Dr. David Voehringer
 Regulation of Type 2 Immunity by Basophils Department of Infection Biology Institute of Clinical Microbiology, Immunology and Hygiene Outline of the presentation The concept of type 2 immunity Basophil
Regulation of Type 2 Immunity by Basophils Department of Infection Biology Institute of Clinical Microbiology, Immunology and Hygiene Outline of the presentation The concept of type 2 immunity Basophil
EXOTESTTM. ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids
 DATA SHEET EXOTESTTM ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids INTRODUCTION Exosomes are small endosome-derived lipid nanoparticles
DATA SHEET EXOTESTTM ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids INTRODUCTION Exosomes are small endosome-derived lipid nanoparticles
Electron micrograph of phosphotungstanic acid-stained exosomes derived from murine
 1 SUPPLEMENTARY INFORMATION SUPPLEMENTARY FIGURES Supplementary Figure 1. Physical properties of murine DC-derived exosomes. a, Electron micrograph of phosphotungstanic acid-stained exosomes derived from
1 SUPPLEMENTARY INFORMATION SUPPLEMENTARY FIGURES Supplementary Figure 1. Physical properties of murine DC-derived exosomes. a, Electron micrograph of phosphotungstanic acid-stained exosomes derived from
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Canberra, Australia). CD11c-DTR-OVA-GFP (B6.CD11c-OVA), B6.luc + and. Cancer Research Center, Germany). B6 or BALB/c.FoxP3-DTR-GFP mice were
 Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin
 Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin Ming Yang, Simon P. Hogan, Peter J. Henry, Klaus I. Matthaei, Andrew N.
Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin Ming Yang, Simon P. Hogan, Peter J. Henry, Klaus I. Matthaei, Andrew N.
9607 Dr. Perry Road Suite 103. Ijamsville, MD Tel: (301) Fax: (301) Ultrasensitive Samoa Human IL-33 Immunoassay
 AssayGate, Inc. 9607 Dr. Perry Road Suite 103. Ijamsville, MD 21754. Tel: (301)874-0988. Fax: (301)560-8288. Ultrasensitive Samoa Human IL-33 Immunoassay INTRODUCTION Interleukin-33 (IL-33), a cytokine
AssayGate, Inc. 9607 Dr. Perry Road Suite 103. Ijamsville, MD 21754. Tel: (301)874-0988. Fax: (301)560-8288. Ultrasensitive Samoa Human IL-33 Immunoassay INTRODUCTION Interleukin-33 (IL-33), a cytokine
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma
 Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the
 Supplementary Figure 1. LAG3 + Treg-mediated regulation of germinal center B cells and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the experimental protocol for the
Supplementary Figure 1. LAG3 + Treg-mediated regulation of germinal center B cells and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the experimental protocol for the
Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood
 Antibody-mediated depletion of CD19-CAR T cells Supplemental 1 Supplemental Materials Supplemental Figure 1. Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood cells were
Antibody-mediated depletion of CD19-CAR T cells Supplemental 1 Supplemental Materials Supplemental Figure 1. Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood cells were
Instructions for use. Histamine Release
 Instructions for use Histamine Release Supplementary kit for the determination of the release of histamine from heparinized whole blood (this kit has to be used in combination with the Histamine ELISA,
Instructions for use Histamine Release Supplementary kit for the determination of the release of histamine from heparinized whole blood (this kit has to be used in combination with the Histamine ELISA,
Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive
 Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
The TLR5 ligand flagellin promotes asthma by. priming allergic responses to indoor allergens
 The TLR ligand flagellin promotes asthma by priming allergic responses to indoor allergens Rhonda H. Wilson 1,3, Shuichiro Maruoka 1,3, Gregory S. Whitehead 1, Julie F. Foley 1, Gordon P. Flake 1, Michelle
The TLR ligand flagellin promotes asthma by priming allergic responses to indoor allergens Rhonda H. Wilson 1,3, Shuichiro Maruoka 1,3, Gregory S. Whitehead 1, Julie F. Foley 1, Gordon P. Flake 1, Michelle
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4
 Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4 Christina A. Herrick, 1,2 Heather MacLeod, 2 Earl Glusac, 1,3 Robert E. Tigelaar, 1,2 and Kim
Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4 Christina A. Herrick, 1,2 Heather MacLeod, 2 Earl Glusac, 1,3 Robert E. Tigelaar, 1,2 and Kim
Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice
 Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Nair S, Branagan AR, Liu J, Boddupalli CS, Mistry PK, Dhodapkar
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Nair S, Branagan AR, Liu J, Boddupalli CS, Mistry PK, Dhodapkar
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice
 Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice Jimmy A. Rotolo 1, Branka Stancevic 1, Jianjun Zhang 1, Guoqiang Hua 1, John Fuller 1, Xianglei Yin 1, Adriana Haimovitz-Friedman 2, Kisu
Anti-ceramide Antibody Prevents the Radiation GI Syndrome in Mice Jimmy A. Rotolo 1, Branka Stancevic 1, Jianjun Zhang 1, Guoqiang Hua 1, John Fuller 1, Xianglei Yin 1, Adriana Haimovitz-Friedman 2, Kisu
Utilizing AlphaLISA Technology to Screen for Inhibitors of the CTLA-4 Immune Checkpoint
 APPLICATION NOTE AlphaLISA Technology Authors: Matthew Marunde Stephen Hurt PerkinElmer, Inc. Hopkinton, MA Utilizing AlphaLISA Technology to Screen for Inhibitors of the CTLA-4 Immune Checkpoint Introduction
APPLICATION NOTE AlphaLISA Technology Authors: Matthew Marunde Stephen Hurt PerkinElmer, Inc. Hopkinton, MA Utilizing AlphaLISA Technology to Screen for Inhibitors of the CTLA-4 Immune Checkpoint Introduction
