Surfactant Protein D Regulates Airway Function and Allergic Inflammation through Modulation of Macrophage Function
|
|
|
- Amos Rafe Booker
- 5 years ago
- Views:
Transcription
1 Surfactant Protein D Regulates Airway Function and Allergic Inflammation through Modulation of Macrophage Function Katsuyuki Takeda, Nobuaki Miyahara, Yeong-Ho Rha, Christian Taube, Eun-Seok Yang, Anthony Joetham, Taku Kodama, Annette M. Balhorn, Azzeddine Dakhama, Catherine Duez, Amanda J. Evans, Dennis R. Voelker, and Erwin W. Gelfand Program in Cell Biology, Department of Pediatrics; and Department of Medicine, National Jewish Medical and Research Center, Denver, Colorado The lung collectin surfactant protein D (SP-D) is an important component of the innate immune response but is also believed to play a role in other regulatory aspects of immune and inflammatory responses within the lung. The role of SP-D in the development of allergeninduced airway inflammation and hyperresponsiveness (AHR) is not well defined. SP-D levels progressively increased up to 48 hours after allergen challenge of sensitized mice and then subsequently decreased. The levels of SP-D paralleled the development of airway eosinophilia and AHR. To determine if this association was functionally relevant, mice were administered rat SP-D (rsp-d) intratracheally. When given to sensitized mice before challenge, AHR and eosinophilia were reduced by rsp-d in a dose-dependent manner but not by mutant rsp-d. rsp-d administration resulted in increased levels of interleukin (IL)-10, IL-12, and IFN- in bronchoalveolar lavage fluid and reduced goblet cell hyperplasia. Culture of alveolar macrophages together with SP-D and allergen resulted in increased production of IL-10, IL-12, and IFN-. These results indicate that SP-D can (negatively) regulate the development of AHR and airway inflammation after airway challenge of sensitized mice, at least in part, by modulating the function of alveolar macrophages. Keywords: surfactant protein D; airway hyperresponsiveness; eosinophils; macrophages The incidence of allergic asthma worldwide has generated increasing alarm in terms of the economic burden imposed and the rising morbidity and mortality despite significant advances in therapeutics (1). The currently accepted theory is that the disease is the result of chronic airway inflammation, largely dependent on eosinophils that lead to airway hyperresponsiveness (AHR) and reversible airway obstruction (2, 3). With the rising incidence and therapeutic insufficiencies, it is now more apparent that asthma is first and foremost a very heterogeneous syndrome, with numerous cell types and mediators contributing to the disease phenotype. Central to the pathogenesis of the airway disease are antigen-specific, memory T cell responses and perhaps to a lesser degree, antigen-specific IgE responses (4, 5). Although antigen-specific (adaptive immune) responses are a major focus in the disease, the role of innate immunity in the regulation of airway function and inflammation may also be important (6). As an example, / T cells have been shown to exhibit both contributory and inhibitory activities in the development and expression of allergic airway disease. In a similar manner, the complement system has also attracted recent attention (Received in original form April 18, 2003; accepted in final form July 16, 2003) Correspondence and requests for reprints should be addressed to Erwin W. Gelfand, M.D., 1400 Jackson Street, Denver, CO gelfande@njc.org Am J Respir Crit Care Med Vol 168. pp , 2003 Originally Published in Press as DOI: /rccm OC on July 25, 2003 Internet address: (7). The hydrophilic surfactant proteins (SPs) SP-A and SP-D are also important components of the innate immune response (8, 9). Increasing evidence indicates that SP-A and SP-D regulate immune cell function as well as surfactant homeostasis (10). These SPs may affect allergen uptake by antigen-presenting cells or inhibit allergen-specific IgE binding to allergen, thereby inhibiting the triggering of allergic responses (11). Alveolar macrophages, which are major resident cells in the airways may be playing a role in the SP-D regulatory effects in allergic inflammation (12 14). SP-A and SP-D have been shown to play protective roles in an allergic bronchopulmonary aspergillosis model in mice (15). It has been reported that mite allergen induced airway inflammation leads to decreased levels of SP-A and SP-D in the bronchoalveolar lavage fluid (BALF) from sensitized mice (16). In contrast, elevated levels of SP-A and SP-D have also been found in BALF from sensitized and challenged mice (17) and in the BALF of patients with asthma (18). The purpose of the present study was to determine if SP-D levels are linked to allergic inflammation and AHR, whether administration of SP-D could attenuate airway inflammation, and normalize airway responsiveness, and to define potential mechanisms for such effects. METHODS Animals Female BALB/c mice from 6 to 8 weeks of age were obtained from Jackson Laboratories (Bar Harbor, ME). The animals were maintained on an ovalbumin (OVA)-free diet. Experiments were conducted under a protocol approved by the Institutional Animal Care and Use Committee of the National Jewish Medical and Research Center. Sensitization and Airway Challenge Mice were sensitized by intraperitoneal injection of 20 g of ovalbumin (OVA, Grade V; Sigma Chemical Co., St. Louis, MO) emulsified in 2.25 mg alum (AlumImuject; Pierce, Rockford, IL) in a total volume of 100 l on Days 1 and 14. Mice were challenged via the airways with OVA (1% in saline) for 20 minutes on Days 28, 29, and 30 using an ultrasonic nebulizer (model NE-07; Omron Healthcare, Vernon Hills, IL). The control groups of mice were challenged alone, that is, received three challenges but no sensitization. In all groups, assays were performed 48 hours after the last challenge. Determination of Airway Responsiveness Airway responsiveness was assessed as a change in airway function after challenge with aerosolized methacholine (Sigma). Mice were anesthetized, tracheostomized, mechanically ventilated, and lung function was assessed as described previously (19). Briefly, the mice were anesthetized with an intraperitoneal injection of pentobarbital sodium (100 mg/kg). When an appropriate level of anesthesia was achieved, a stainless steel 18G tube was inserted as a tracheostomy cannula and tied into place. The tracheostomy tube was passed through a hole in the whole body plethysmograph. A four-way connector was attached to
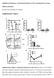
2 784 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL Figure 1. (A) Changes in airway resistance (RL) after sensitization and challenge at various time points. RL values were obtained in response to increasing concentrations of inhaled methacholine (MCh). Values are expressed as mean ( SEM) (n 8). Open squares, challenge alone; open triangles, 0 hours after the last antigen challenge; closed squares, 24 hours after; closed diamonds, 48 hours after; closed triangles, 1 week after; open diamonds, 2 weeks after. *Significant differences (p 0.05) occurred between the groups of challenge alone, 0 hours, and 2 weeks versus 24 hours, 48 hours, and 1 week after challenge. (B) Numbers of eosinophils in bronchoalveolar lavage fluid (BALF) at different time points after the last antigen challenge. *After antigen challenge, mice developed significantly higher number of eosinophils (p 0.05) when compared with the challenged-alone group. (C) surfactant protein D (SP-D) levels in BALF at different time points after antigen challenge. Significant differences (*p 0.05) occurred between 24 hours, 48 hours, or 1 week after and challenge alone. n 8 in each group. the tracheostomy tube, with two ports connected to the inspiratory and expiratory sides of a ventilator (SN-480-7; Shinano, Tokyo, Japan). Ventilation was achieved at 160 breaths per minute and a Vt of 0.16 ml with a positive end-expiratory pressure of 2 to 4 cm H 2 O. Changes in lung volume were measured by detecting pressure changes in the plethysmographic chamber through a port in the connecting tube with a differential pressure transducer and then referenced to a second copper gauze filled 1.0-L glass bottle. Flow was measured by digital differentiation of the volume signal. Lung resistance was continuously computed (Labview; National Instruments, Austin, TX) by fitting flow, volume, and pressure to an equation of motion, using a recessive least squares algorithm. The aerosolized methacholine was administered through bypass tubing via an ultrasonic nebulizer (model 5500D; DeVilbiss, Somerset, PA) placed between the expiratory port of the ventilator and the fourway connector. Aerosolized methacholine was administered for 8 seconds with a Vt of 0.45 ml and frequency of 60 breaths per minute by another ventilator (model 683; Harvard Apparatus, South Natwick, MA). The data of lung resistance was continuously collected for up to 3 minutes. Maximum values of lung resistance were taken to express changes in airway function. BAL Immediately after assessment of AHR, lungs were lavaged via the tracheal tube with Hank s balanced solution (1 1mlat37 C). The volume of collected BALF was measured in each sample and the number of leukocytes was counted (Coulter Counter; Coulter Corporation, Hialeah, FL). Differential cell counts were performed by counting at least 300 cells on cytocentrifuged preparations (Cytospin 3; Shandon Ltd., Runcorn, Cheshire, UK). Slides were stained with modified Wright-Giemsa (Hema 3; Protocol, Swedesboro, NJ) and differentiated by standard hematologic procedures. Administration of Rat SP-D and Mutant Rat SP-D To determine the direct effects of SP-D on the airway, we administered rat SP-D (rsp-d), which shares a high degree of homology with mouse SP-D (identities 91% and positives 94%). A mutated form of rsp-d with altered carbohydrate binding was used as a negative control [E321Q, N323D]. rsp-d and the [E321Q-N323D] mutant were isolated from culture medium of CHO-K1 cells expressing the recombinant protein by the method described previously (20). Briefly, the harvested medium containing rsp-d was centrifuged at 3,000 g at 4 C for 15 minutes to obtain cell debris free solution, and the resultant supernatant was applied to a mannose-sepharose affinity matrix in the presence of 5 mm calcium. For purification of mutant SP-D, multilamellar liposomes containing phosphatidylinositol, phosphatidylserine, and cholesterol (3:4:3) were mixed with the protein and subsequently separated by centrifugation. The proteins were subsequently eluted from affinity columns or liposomes with either 2 or 15 mm ethylenediaminetetraacetic acid, respectively. The ethylenediaminetetraacetic acid was subsequently removed by gel filtration. The purified SP-D contained both dodecamers and larger molecular aggregates of the proteins. The proteins were dialyzed against Tris-buffered saline (5 mm tris(hydroxymethyl)aminomethane hydrochloride, 150 mm sodium chloride, ph 7.4) at 4 C and stored at 20 C until use. Endotoxin levels in the purified SP preparations were determined using a kit (QCL-1000; Biowhittaker, Inc., Wakersville, MD) and the levels were under 0.25 pg for each sample. At these levels, there are no effects on airway inflammation (neutrophils) or AHR (data not shown). Before administration of wild-type or mutant rsp-d, the mice were anesthetized with avertin (400 mg/kg) and 2 g of the recombinant proteins in 50 l or the same volume of vehicle per mouse was administered as an aerosol using the intratracheal aerosolizer (Microsprayer; PennCentury, Philadelphia, PA). Agents were given 1 day before and 5 hours before the first allergen challenge. To examine the dose-dependent effects of rsp-d, various doses of the protein (0.02, 0.2, 2, and 10 g in50 l) were instilled into the trachea. Measurements of SP-D Levels in BALF Mouse SP-D levels in lavage were quantified by ELISA (21). Recombinant mouse SP-D used as a standard was purified from culture supernatants of CHO-K1 cells expressing the protein using methods similar to rsp-d as described previously. Horseradish peroxidase conjugated rabbit anti-mouse SP-D IgG was used for antigen detection. 2,2 -azi-
3 Takeda, Miyahara, Rha, et al.: Surfactant Protein D and Airway Hyperresponsiveness 785 Figure 2. A) Airway responsiveness to methacholine (MCh) and (B) eosinophil numbers in bronchoalveolar lavage fluid (BALF) after administration of different doses of rat surfactant protein D (rsp-d). Airway responsiveness is expressed as the MCh concentration required to induce 200% change over saline-treated mice (PC200). Significant differences (p 0.05) * compared with vehicle treatment; # compared with SP-D 0.02 g treatment (n 8). nobis(3-ethylbenzthiazoline-6-sulfonic acid) (ABTS, Sigma) was used as the substrate for the peroxidase reaction. Antibody binding to the proteins was measured by absorbance at 410 nm, and protein levels in BALF were expressed as nanograms per ml (ng/ml). Effects of SP-D on Cytokine Production from Alveolar Macrophages To elucidate the direct effects of SP-D on cytokine production from alveolar macrophages, the cells were purified from BAL and cultured with SP-D and/or OVA. Briefly, mice were anesthetized with avertin as described previously, lungs of sensitized but nonchallenged mice were lavaged via the tracheal tube with Hank s balanced solution (5 1ml37 C). Cells were washed with Hank s balanced solution and cells were cultured in 200 l of RPMI 1640 medium with l-glutamine (Mediatech, Herndon, VA) supplemented with 10% fetal bovine serum and 10 g/ml polymyxin B sulfate (Sigma). The cells were confirmed to be more than 99% macrophages on stained cytocentrifuged slides. To obtain sufficient macrophages for these experiments, BALF was pooled from 2 to 3 mice. Cells were incubated with OVA, and various concentrations of rsp-d and the supernatants were harvested after 24 hours. The optimal OVA concentration was determined to be 10 g/ ml in preliminary experiments. Measurement of Cytokines Cytokine levels in the BALF or supernates of cultured airway macrophages were measured by ELISA as described previously (22). Briefly, measurements of interleukin (IL)-10, IL-12, IFN-, IL-4, and IL-5 were performed using OptEIA sets (BD PharMingen, San Diego, CA) with 96-well plates (Immulon 2; Dynatech, Chantilly, VA) according to the manufacturer s protocol. The limits of detection were 4 pg/ml for IL-4 and IL-5, and 10 pg/ml for IL-12, IL-10, and IFN-. For measuring IFN- levels from cultured macrophages, OptEIA set for small amounts (AN-18; BD PharMingen) was also used and the limit of detection was 1.5 pg/ml. Histologic and Immunohistochemistry Studies Lungs were inflated through the trachea with 1 ml of 10% formalin and fixed in 10% formalin by immersion. Blocks of lung tissue were cut around the main bronchus and embedded in paraffin. For detection of mucus-containing cells in formalin-fixed airway tissue, sections (6 m) were cut and stained with periodic acid Schiff and counterstained with hematoxylin. Goblet cell numbers were counted in sections by measuring the length of epithelium and the luminal area using an National Institutes of Health image analysis system (23, 24). Statistical Analysis All results were expressed as the mean and SEM. Analysis of variance was used to determine the levels of difference between all groups. Pairs of groups were compared by unpaired two-tailed Student s t test. The p values for significance were set at Figure 3. (A) Airway response to inhaled methacholine (MCh) after rat surfactant protein D (rsp-d), mutant SP-D, or vehicle treatment before ovalbumin (OVA) challenge after sensitization. Values are expressed as mean ( SEM) (n 8). Open squares, vehicle treatment; open triangles, mutant SP-D treatment; closed squares, rsp-d treatment. (B) Numbers of eosinophils in bronchoalveolar lavage fluid (BALF) from same groups of mice. Significant differences (p 0.05) between *, rsp-d versus vehicle treatment, # rsp-d versus mutant SP-D.
4 786 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL Figure 4. Cytokine levels in bronchoalveolar lavage fluid (BALF) after rat surfactant protein D (rsp-d) or vehicle treatment. Animals were treated with 2 g SP-D, 1 day and 5 hours before antigen challenge. Lung lavage was performed 2 days after antigen challenge. *Significant differences (p 0.05) occurred between rsp-d and vehicle. n 8 in each group. RESULTS Kinetics of AHR, Eosinophil, and SP-D Responses Sensitization followed by challenge to allergen-induced significant AHR to inhaled methacholine and resulted in increased numbers of eosinophils in the BALF. Naive mice, that were sensitized but not challenged, and mice challenged alone, showed lower levels of SP-D when compared with sensitized and challenged mice (data not shown). To assess any association between SP-D, AHR, and eosinophilic infiltration into the airways, these parameters were examined at different time points after antigen challenge of sensitized and challenged mice. AHR was detected 24 hours after the third allergen challenge and was sustained for 1 week. By 2 weeks after challenge, airway function returned to near baseline levels (Figure 1A). Investigation of the number of eosinophils in the BALF revealed a similar time course: eosinophils began to increase earlier than airway responsiveness; after 2 weeks, eosinophil numbers were still significantly elevated when compared with nonsensitized animals (Figure 1B). The kinetics of the elevations in SP-D in the BALF revealed a similar pattern to airway responsiveness or eosinophil numbers in BALF (Figure 1C). Increased levels of SP-D were detected 24 hours after OVA challenge and returned to baseline levels 2 weeks after the last challenge. All three parameters, AHR, eosinophil numbers, and BAL SP-D levels peaked 48 hours after the last of the three OVA challenges. Effects of SP-D Administration Despite the association of elevated SP-D levels, AHR and eosinophilic infiltration in the lungs, the role played by SP-D in these Figure 5. Goblet cell hyperplasia was quantified in periodic acid-schiff (PAS) stained sections and expressed per millimeter of basement membrane. Values are expressed as mean ( SEM). *Significant differences (p 0.05) occurred between groups (n 8) receiving rat surfactant protein D (rsp-d) treatment or vehicle. responses remained to be defined. To directly address this issue, we administered exogenous rsp-d intratracheally and determined whether this treatment improved or exacerbated AHR and eosinophilic airway inflammation. rsp-d was administered at different doses as shown in Figure 2; AHR and eosinophil numbers in BAL were reduced in a dose-dependent manner. After preliminary experiments to determine the most effective dose, 2 g of rsp-d was administered through the trachea before antigen challenge. As a control, the [E321Q, N323D] mutant rsp-d was administered in the same manner as rsp-d. As shown in Figure 3, only rsp-d treatment significantly decreased AHR and eosinophil numbers in BALF, whereas the mutant protein was without effect, implying a requirement for wild-type carbohydrate recognition specificity for the response (it should be noted that the instillation of any substance, even saline, results in lower eosinophil numbers [Figures 2 and 3] than seen without any manipulation [Figure 1]). Levels of cytokines in BALF and goblet cell hyperplasia were also assessed after administration of rsp-d. Intratracheal instillation of rsp-d before challenge was associated with increased levels of IL-10, IL-12, and IFN-, as shown in Figure 4. The levels of IL-4 or IL-5 were not significantly altered in response to rsp-d treatment (data not shown). There was also a small decrease in goblet cell numbers after rsp-d treatment (Figure 5). Effects of SP-D on Cytokine Production by Alveolar Macrophages On the basis of these results, we investigated the effect of SP-D on in vitro cytokine production by alveolar macrophages obtained from mice after sensitization to OVA. As shown in Figure 6, culture of the macrophages with either allergen alone or rsp-d alone resulted in small increases in cytokine production. In contrast, in vitro production of IFN-, IL-12, and IL-10 was significantly upregulated when cells were cultured together with allergen and rsp-d, which is consistent with the increase in levels of cytokines after in vivo rsp-d treatment. IL-4 and IL-5 were not detected under these conditions (data not shown). DISCUSSION SP-D belongs to the collectin protein family that also includes SP-A. Both of these bronchoalveolar proteins are considered to be important regulatory molecules of the pulmonary innate immune system, involved in the first-line defense of the lung against microbial or allergen challenge (15, 25 27). In addition to
5 Takeda, Miyahara, Rha, et al.: Surfactant Protein D and Airway Hyperresponsiveness 787 Figure 6. Cytokine production from airway macrophages cultured together with allergen and/or surfactant protein D (SP-D). The cells were cultured in the presence of ovalbumin (OVA) or SP-D as indicated for 24 hours. The cell-free medium was analyzed for cytokines by ELISA. The levels of (A) IL-10, (B) IFN-, (C) IL-12 are expressed as mean ( SEM) (n 8). Significant differences (p 0.05) are indicated by * when treatments are compared with medium. Significant differences (p 0.05) are also indicated by # when treatments are compared with OVA or rsp-d alone. promoting clearance of infectious pathogens, SP-D can modulate cellular immune responses in response to allergen challenge. Here, we examined the interrelationship between SP-D and allergen-induced AHR and airway inflammation by first determining if there was an association between these processes after allergen challenge of sensitized mice. Allergen challenge of sensitized mice resulted in significant increases in the levels of SP-D in the BALF. The kinetics of the SP-D response (increases) appeared to closely follow those of airway eosinophilia and AHR to inhaled methacholine. Moreover, administration of wild-type rsp-d, but not a variant with altered carbohydrate recognition before allergen challenge, reversed the consequences of allergen exposure by reducing airway eosinophilia, inducing IL-10 and Th1 cytokines (IL-12, IFN- ), and normalizing airway function. The ability of allergen challenge in sensitized, but not in nonsensitized, mice to trigger an increase in the levels of SP-D, implicates this protein in the response to allergen. SP-D is a multivalent homooligomeric protein that binds carbohydrate, lipids, and protein ligands with high affinity (9). SP-D binds to oligosaccharides on the surface of a variety of pathogenic microorganisms as well as directly to cells such as alveolar macrophages (28). SP-D also enhances chemotaxis of phagocytic cells (29) and exhibits immunomodulatory function, inhibiting T cell proliferation and IL-2 production (30). SP-D is also capable of inhibiting specific IgE binding to allergen and preventing allergen-induced histamine release from human basophils (31). The mechanism underlying the increase in SP-D levels in BALF in this model is not known. The response appears specific as it was only seen in mice challenged with the original sensitizing allergen. The levels of BALF SP-D appeared to parallel the inflammatory response in the lung, especially BAL eosinophil numbers. Similar results have been demonstrated in human asthma and other animal models of allergic inflammation (17, 18, 32, 33). Serum levels of SP-D also have served as a biomarker of inflammation in interstitial lung disease (34). Although SP-D may serve as a marker of acute airway inflammation, such as in acute asthma exacerbation, increased levels of SP-D in the airway may also be a consequence of epithelial cell damage. SP-D could play a role in limiting the allergic inflammatory response, limiting proliferation of various inflammatory cells by binding to the allergen and interfering with its recognition by antigen-presenting cells (29, 30) or by modifying the production and secretion of various inflammatory cytokines (35 37). Thus, endogenous SP-D production after allergen challenge of sensitized mice may play a role in limiting the extent and persistence of the inflammatory changes, for example, by curtailing the eosinophilic inflammatory response. To directly assess the influence of SP-D on allergic inflammation, we administered rsp-d after sensitization but before allergen challenge. A microsprayer capable of delivering small particles was used to deliver the protein to ensure a diffuse distribution to the airways. When administered in this way, we observed a marked reduction in the eosinophilic inflammatory response; eosinophil numbers in the BAL were reduced to roughly 50% by rsp-d but not by a mutant form of the protein or vehicle. The effects of rsp-d were dose-dependent. These results suggest that SP-D is playing a role through its carbohydrate recognition domain, similar to that shown previously in an RSV infection model (38). When BAL cytokine levels were examined, increased levels of the three critical disease-modifying cytokines (IL-10, IFN-, IL-12) were demonstrated, suggesting that the effects of SP-D were not likely due to interference with allergen recognition or antigen-presenting cell function. After sensitization and challenge, the levels of these three cytokines typically decrease in BALF. IL-10 has been shown to play a complex role in allergic inflammation. Tournoy and coworkers
6 788 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL showed that endogenous IL-10 can suppress airway allergic inflammation, including numbers of BAL eosinophils as well as airway responsiveness (39), whereas van Scott and coworkers showed that IL-10 can increase AHR (40). Both IL-12 and IFN- have also exhibited similar negative influences on eosinophilic airway inflammation and AHR (41, 42). Of interest, levels of IL-4 and IL-5 were unaffected by administration of SP-D under these conditions. Overexpression of IL-4 in Clara cells was associated with marked increases in SP-D levels in the lung (26). In a model of allergic bronchopulmomary aspergillosis, administration of SP-D did decrease IL-4 and IL-5 while increasing IFN- levels, when spleen cells from the treated mice were cultured in vitro (15). Because of its widespread effects, there are a number of different ways that SP-D may have functioned to reduce airway inflammation and normalize airway function. Because rsp-d but not mutant SP-D is capable of binding mannose glucose (20), a mannosylated glycoprotein such as OVA may be captured and cleared from the airway more efficiently after administration of rsp-d. This could contribute to some of the effects of rsp-d, but would not explain the increases in IL-10, IFN-, or IL-12 levels. Alternatively, rsp-d coupled with OVA may be a more effective activator of macrophages, accounting for the increases in these cytokine levels both in vivo and in vitro. IL-10, IFN-, and IL-12 may be produced by non-t cells, epithelial cells, dendritic cells, and macrophages. SP-D has previously been shown to induce IL-10 and IL-12 production in macrophages (36). We investigated the effects of culturing airway macrophages together with rsp-d and/or allergen to determine whether SP-D could modify cytokine production from these cells in vitro. Together with allergen, rsp-d increased macrophage production of IFN-, IL-10, and IL-12 in a dose-dependent fashion. Because airway macrophages are the dominant cells in the airways of sensitized but not challenged mice, these data suggest that one of the mechanisms underlying the antiinflammatory effects of SP-D on airway allergic inflammation is by upregulating Th1 type cytokine production from airway macrophages and potentially other cell types. SP-D may do so by enhancing antigen presentation by antigen-presenting cells (43). Furthermore, SP-D is reported to decrease metalloproteinase activity and oxidant production in the lung (44), effects that may also result in normalization of airway function. SP-D may regulate tissue metalloproteinase activity by increasing tissue inhibitor of metalloproteinase activity production from alveolar macrophages via increasing levels of IL-10 (45). Finally, SP-D may play a significant role in the pulmonary clearance of apoptotic cells by alveolar macrophages, contributing to the resolution or inhibition of inflammation (27, 46). In summary, SP-D exhibits a number of potentially important activities in the lung during the inflammatory response elicited by allergen challenge of sensitized mice. These effects of SP-D may be expressed on cells of both the innate and adaptive immune systems and appear dependent on the integrity of the carbohydrate recognition domain. For these reasons, SP-D may be of benefit in the reduction or resolution of allergen-induced AHR and airway inflammation. Conflict of Interest Statement : K.T. has no declared conflict of interest; N.M. has no declared conflict of interest; Y-H.R. has no declared conflict of interest; C.T. has no declared conflict of interest; E-S.Y. has no declared conflict of interest; A.J. has no declared conflict of interest; T.K. has no declared conflict of interest; A.B. has no declared conflict of interest; A.D. has no declared conflict of interest; C.D. has no declared conflict of interest; A.E. has no declared conflict of interest; D.R.V. has no declared conflict of interest; E.W.G. has no declared conflict of interest. References 1. Sly RM. Decreases in asthma mortality in the United States. Ann Allergy Asthma Immunol 2000;85: Lacy P, Moqbel R. Immune effector functions of eosinophils in allergic airway inflammation. Curr Opin Allergy Clin Immunol 2001;1: Tattersfield AE, Knox AJ, Britton JR, Hall IP. Asthma. Lancet 2000;360: Oshiba A, Hamelmann E, Haczku A, Takeda K, Conrad DH, Kikutani H, Gelfand EW. Modulation of antigen-induced B and T cell responses by antigen-specific IgE antibodies. J Immunol 1997;159: De Sanctis GT, Itoh A, Green FH, Qin S, Kimura T, Grobholz JK, Martin TR, Maki T, Drazen JM. T-lymphocytes regulate genetically determined airway hyperresponsiveness in mice. Nat Med 1997;3: Lahn M, Kanehiro A, Takeda K, Joetham A, Schwarze J, Kohler G, O Brien R, Gelfand EW, Born W. Negative regulation of airway responsiveness that is dependent on gammadelta T cells and independent of alphabeta T cells. Nat Med 1999;5: Karp CL, Grupe A, Schadt E, Ewart SL, Keane-Moore M, Cuomo PJ, Kohl J, Wahl L, Kuperman D, Germer S, et al. Identification of complement factor 5 as a susceptibility locus for experimental allergic asthma. Nat Immunol 2000;1: Wright JR. Pulmonary surfactant: a front line of lung host defense. J Clin Invest 2003;111: Crouch E, Wright JR. Surfactant proteins a and d and pulmonary host defense. Annu Rev Physiol 2001;63: Ikegami M, Hull WM, Yoshida M, Wert SE, Whitsett JA. SP-D and GM-CSF regulate surfactant homeostasis via distinct mechanisms. Am J Physiol Lung Cell Mol Physiol 2001;281:L697 L Wang JY, Kishore U, Lim BL, Strong P, Reid KB. Interaction of human lung surfactant proteins A and D with mite (Dermatophagoides pteronyssinus) allergens. Clin Exp Immunol 1996;106: Wert SE, Yoshida M, LeVine AM, Ikegami M, Jones T, Ross GF, Fisher JH, Korfhagen TR, Whitsett JA. Increased metalloproteinase activity, oxidant production, and emphysema in surfactant protein D geneinactivated mice. Proc Natl Acad Sci USA 2000;97: Sano H, Chiba H, Iwaki D, Sohma H, Voelker DR, Kuroki Y. Surfactant proteins A and D bind CD14 by different mechanisms. J Biol Chem 2000;275: Tang C, Inman MD, van Rooijen N, Yang P, Shen H, Matsumoto K, O Byrne PM. Th type 1-stimulating activity of lung macrophages inhibits Th2-mediated allergic airway inflammation by an IFN-gammadependent mechanism. J Immunol 2001;166: Madan T, Kishore U, Singh M, Strong P, Clark H, Hussain EM, Reid KB, Sarma PU. Surfactant proteins A and D protect mice against pulmonary hypersensitivity induced by Aspergillus fumigatus antigens and allergens. J Clin Invest 2001;107: Wang JY, Shieh CC, Yu CK, Lei HY. Allergen-induced bronchial inflammation is associated with decreased levels of surfactant proteins A and D in a murine model of asthma. Clin Exp Allergy 2001;31: Haczku A, Atochina EN, Tomer Y, Chen H, Scanlon ST, Russo S, Xu J, Panettieri RA Jr, Beers MF. Aspergillus fumigatus-induced allergic airway inflammation alters surfactant homeostasis and lung function in BALB/c mice. Am J Respir Cell Mol Biol 2001;25: Cheng G, Ueda T, Numao T, Kuroki Y, Nakajima H, Fukushima Y, Motojima S, Fukuda T. Increased levels of surfactant protein A and D in bronchoalveolar lavage fluids in patients with bronchial asthma. Eur Respir J 2000;16: Takeda K, Haczku A, Lee JJ, Irvin CG, Gelfand EW. Strain dependence of airway hyperresponsiveness reflects differences in eosinophil localization in the lung. Am J Physiol Lung Cell Mol Physiol 2001;281: L394 L Ogasawara Y, Voelker DR. Altered carbohydrate recognition specificity engineered into surfactant protein D reveals different binding mechanisms for phosphatidylinositol and glucosylceramide. J Biol Chem 1995; 270: Sano H, Kuroki Y, Honma T, Ogasawara Y, Sohma H, Voelker DR, Akino T. Analysis of chimeric proteins identifies the regions in the carbohydrate recognition domains of rat lung collectins that are essential for interactions with phospholipids, glycolipids, and alveolar type II cells. J Biol Chem 1998;273: Rha YH, Taube C, Haczku A, Joetham A, Takeda K, Duez C, Siegel M, Aydintug MK, Born WK, Dakhama A, et al. Effect of microbial heat shock proteins on airway inflammation and hyperresponsiveness. J Immunol 2002;169: Tomkinson A, Cieslewicz G, Duez C, Larson KA, Lee JJ, Gelfand EW. Temporal association between airway hyperresponsiveness and airway eosinophilia in ovalbumin-sensitized mice. Am J Respir Crit Care Med 2001;163:
7 Takeda, Miyahara, Rha, et al.: Surfactant Protein D and Airway Hyperresponsiveness Tomkinson A, Duez C, Cieslewicz G, Pratt JC, Joetham A, Shanafelt MC, Gundel R, Gelfand EW. A murine IL-4 receptor antagonist that inhibits IL-4- and IL-13-induced responses prevents antigen-induced airway eosinophilia and airway hyperresponsiveness. J Immunol 2001; 166: Mishra A, Weaver TE, Beck DC, Rothenberg ME. Interleukin-5- mediated allergic airway inflammation inhibits the human surfactant protein C promoter in transgenic mice. J Biol Chem 2001;276: Ikegami M, Whitsett JA, Zissis CC, Ross GF, Reed JA, Bachurski CJ, Jobe AH. IL-4 increases surfactant and regulates metabolism in vivo. Am J Physiol Lung Cell Mol Physiol 2000;278:L75 L Clark H, Palaniyar N, Strong P, Edmonson J, Hawgood S, Reid KBM. Surfactant protein D reduces alveolar macrophage apoptosis in vivo. J Immunol 2002;169: Kuan SF, Persson A, Parghi D, Crouch E. Lectin-mediated interactions of surfactant protein D with alveolar macrophages. Am J Respir Cell Mol Biol 1994;10: Madan T, Eggleton P, Kishore U, Strong P, Aggrawal SS, Sarma PU, Reid KB. Binding of pulmonary surfactant proteins A and D to Aspergillus fumigatus conidia enhances phagocytosis and killing by human neutrophils and alveolar macrophages. Infect Immun 1997;65: Borron PJ, Crouch EC, Lewis JF, Wright JR, Possmayer F, Fraher LJ. Recombinant rat surfactant-associated protein D inhibits human T lymphocyte proliferation and IL-2 production. J Immunol 1998;161: Wang JY, Shieh CC, You PF, Lei HY, Reid KB. Inhibitory effect of pulmonary surfactant proteins A and D on allergen-induced lymphocyte proliferation and histamine release in children with asthma. Am J Respir Crit Care Med 1998;158: Haley KJ, Ciota A, Contreras JP, Boothby MR, Perkins DL, Finn PW. Alterations in lung collectins in an adaptive allergic immune response. Am J Physiol Lung Cell Mol Physiol 2002;282:L573 L Kasper M, Sim G, Kosowski R, Kass H, Thuemmler M, Fehrenbach H, Auten RL. Increased surfactant protein D in rat airway goblet and Clara cells during ovalbumin-induced allergic airway inflammation. Clin Exp Allergy 2002;32: Takahashi H, Kuroki Y, Tanaka H, Saito T, Kurokawa K, Chiba H, Sagawa A, Nagae H, Abe S. Serum levels of surfactant proteins A and D are useful biomarkers for interstitial lung disease in patients with progressive systemic sclerosis. Am J Respir Crit Care Med 2000; 162: Strong P, Reid KB, Clark H. Intranasal delivery of a truncated recombinant human SP-D is effective at down-regulating allergic hypersensitivity in mice sensitized to allergens of Aspergillus fumigatus. Clin Exp Immunol 2002;130: Keisari Y, Wang H, Mesika A, Matatov R, Nissimov L, Crouch E, Ofek I. Surfactant protein D-coated Klebsiella pneumoniae stimulates cytokine production in mononuclear phagocytes. J Leukoc Biol 2001;70: Fisher JH, Larson J, Cool C, Dow SW. Lymphocyte activation in the lungs of SP-D null mice. Am J Respir Cell Mol Biol 2002;27: Hickling TP, Bright H, Wing K, Gower D, Martin SL, Sim RB, Malhotra R. A recombinant trimeric surfactant protein D carbohydrate recognition domain inhibits respiratory syncytial virus infection in vitro and in vivo. Eur J Immunol 1999;29: Tournoy KG, Kips JC, Pauwels RA. Endogenous interleukin-10 suppresses allergen-induced airway inflammation and nonspecific airway responsiveness. Clin Exp Allergy 2000;30: van Scott MR, Justice JP, Bradfield JF, Enright E, Sigounas A, Sur S. IL-10 reduces Th2 cytokine production and eosinophilia but augments airway reactivity in allergic mice. Am J Physiol Lung Cell Mol Physiol 2000;278:L667 L Schwarze J, Hamelmann E, Cieslewicz G, Tomkinson A, Joetham A, Bradley K, Gelfand EW. Local treatment with IL-12 is an effective inhibitor of airway hyperresponsiveness and lung eosinophilia after airway challenge in sensitized mice. J Allergy Clin Immunol 1998;102: Lack G, Bradley KL, Hamelmann E, Renz H, Loader J, Leung DY, Larsen G, Gelfand EW. Nebulized IFN-gamma inhibits the development of secondary allergic responses in mice. J Immunol 1996;157: Brinker KG, Martin E, Borron P, Mostaghel E, Doyle C, Harding CV, Wright JR. Surfactant protein D enhances bacterial antigen presentation by bone marrow-derived dendritic cells. Am J Physiol Lung Cell Mol Physiol 2001;281:L1453 L Wert SE, Yoshida M, LeVine AM, Ikegami M, Jones T, Ross GF, Fisher JH, Korfhagen TR, Whitsett JA. Increased metalloproteinase activity, oxidant production, and emphysema in surfactant protein D geneinactivated mice. Proc Natl Acad Sci USA 2000;97: Lim S, Roche N, Oliver BG, Mattos W, Barnes PJ, Fan Chung K. Balance of matrix metalloprotease-9 and tissue inhibitor of metalloprotease-1 from alveolar macrophages in cigarette smokers: regulation by interleukin-10. Am J Respir Crit Care Med 2000;162: Vandivier RW, Ogden CA, Fadok VA, Hoffman PR, Brown KK, Botto M, Walport MJ, Fisher JH, Henson PM, Greene KE. Role of surfactant proteins A, D, and C1q in the clearance of apoptotic cells in vivo and in vitro: calreticulin and CD91 as a common collectin receptor complex. J Immunol 2002;169:
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge
 Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Mechanisms of allergy Fas deficiency delays the resolution of airway hyperresponsiveness after allergen sensitization and challenge Catherine Duez, PhD, a Adrian Tomkinson, PhD, a Leonard D. Shultz, PhD,
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Nishino, Tomoya; Fukushima, Chizu; Asthma and Immunology, 113, 2, (201
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Innate Immunity. Bởi: OpenStaxCollege
 Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice
 Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Phagocytosis of apoptotic cells Prof. Peter Henson
 National Jewish Medical and Research Center Denver, CO. U.S.A. Aimee decathelineau 1 1. Apoptosis and other forms of programmed cell death (PCD) are mechanisms for cell deletion in vivo Examples: Inflammation
National Jewish Medical and Research Center Denver, CO. U.S.A. Aimee decathelineau 1 1. Apoptosis and other forms of programmed cell death (PCD) are mechanisms for cell deletion in vivo Examples: Inflammation
Structure and Function of Antigen Recognition Molecules
 MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge
 Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Supplementary Figures
 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure
 Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure Shigeki Matsubara 1, Christina H. Swasey 1, Joan E. Loader 1, Azzeddine Dakhama 1, Anthony Joetham 1, Hiroshi Ohnishi
Estrogen Determines Sex Differences in Airway Responsiveness after Allergen Exposure Shigeki Matsubara 1, Christina H. Swasey 1, Joan E. Loader 1, Azzeddine Dakhama 1, Anthony Joetham 1, Hiroshi Ohnishi
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
OpenStax-CNX module: m Innate Immunity. OpenStax College. Abstract
 OpenStax-CNX module: m45542 1 Innate Immunity OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
OpenStax-CNX module: m45542 1 Innate Immunity OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin
 CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
CD23 Deficient Mice Develop Allergic Airway Hyperresponsiveness Following Sensitization with Ovalbumin ANGELA HACZKU, KATSUYUKI TAKEDA, ECKARD HAMELMANN, AKIHIRO OSHIBA, JOAN LOADER, ANTHONY JOETHAM, CHARLES
Depletion of Alveolar Macrophages by Treatment with 2-Chloroadenosine Aerosol
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
1. Specificity: specific activity for each type of pathogens. Immunity is directed against a particular pathogen or foreign substance.
 L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
There are 2 major lines of defense: Non-specific (Innate Immunity) and. Specific. (Adaptive Immunity) Photo of macrophage cell
 There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life
 Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System Multiple-Choice Questions
 Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
Chapter 23 Immunity Exam Study Questions
 Chapter 23 Immunity Exam Study Questions 1. Define 1) Immunity 2) Neutrophils 3) Macrophage 4) Epitopes 5) Interferon 6) Complement system 7) Histamine 8) Mast cells 9) Antigen 10) Antigens receptors 11)
Chapter 23 Immunity Exam Study Questions 1. Define 1) Immunity 2) Neutrophils 3) Macrophage 4) Epitopes 5) Interferon 6) Complement system 7) Histamine 8) Mast cells 9) Antigen 10) Antigens receptors 11)
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Chapter 1. Chapter 1 Concepts. MCMP422 Immunology and Biologics Immunology is important personally and professionally!
 MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
3/28/2012. Immune System. Activation of Innate Immunity. Innate (non-specific) Immunity
 Chapter 5 Outline Defense Mechansims Functions of B Lymphocytes Functions of T Lymphocytes Active and Passive Immunity Tumor Immunology Diseases Caused By Immune System Immune System Anatomy - Lymphoid
Chapter 5 Outline Defense Mechansims Functions of B Lymphocytes Functions of T Lymphocytes Active and Passive Immunity Tumor Immunology Diseases Caused By Immune System Immune System Anatomy - Lymphoid
special communication
 Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
Allergic diseases and treatment. Feng Qian ( 钱峰 )
 Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
Innate immunity. Abul K. Abbas University of California San Francisco. FOCiS
 1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved
 Bio 100 Guide 21 Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved inorganic ions, proteins, nutrients,
Bio 100 Guide 21 Blood consists of red and white blood cells suspended in plasma Blood is about 55% plasma and 45% cellular elements Plasma 90% water 10% dissolved inorganic ions, proteins, nutrients,
colorimetric sandwich ELISA kit datasheet
 colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
Introduction to Immune System
 Introduction to Immune System Learning outcome You will be able to understand, at a fundamental level, the STRUCTURES and FUNCTIONS of cell surface and soluble molecules involved in recognition of foreign
Introduction to Immune System Learning outcome You will be able to understand, at a fundamental level, the STRUCTURES and FUNCTIONS of cell surface and soluble molecules involved in recognition of foreign
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma
 Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Supplementary Information. Paired immunoglobulin-like receptor A is an intrinsic, self-limiting
 Supplementary Information Paired immunoglobulin-like receptor A is an intrinsic, self-limiting suppressor of IL-5-induced eosinophil development Netali Ben Baruch-Morgenstern 1,4, Dana Shik 1,4, Itay Moshkovits
Supplementary Information Paired immunoglobulin-like receptor A is an intrinsic, self-limiting suppressor of IL-5-induced eosinophil development Netali Ben Baruch-Morgenstern 1,4, Dana Shik 1,4, Itay Moshkovits
Innate Immunity: Nonspecific Defenses of the Host
 PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
Mouse Anti-HDM IgG Antibody Assay Kit
 Mouse Anti-HDM IgG Antibody Assay Kit Catalog # 3030 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people of
Mouse Anti-HDM IgG Antibody Assay Kit Catalog # 3030 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people of
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms. Table 2: Innate Immunity: First Lines of Defense
 I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms Table 2: Innate Immunity: First Lines of Defense Innate Immunity involves nonspecific physical & chemical barriers that are adapted for
I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms Table 2: Innate Immunity: First Lines of Defense Innate Immunity involves nonspecific physical & chemical barriers that are adapted for
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
HISTO-PHYSIOLOGY HISTO-PHYSIOLOGY HISTO-PHYSIOLOGY. 09-Mar-15. Dr. Muhammad Tariq Javed. RESPIRATORY SYSTEM Lec-1
 RESPIRATORY SYSTEM Lec-1 Dr. Muhammad Tariq Javed Professor Department of Pathology, University of Agriculture, Faisalabad. Email: mtjaved@uaf.edu.pk Web: http://www.geocities.ws/mtjaved 1 2 Conducting
RESPIRATORY SYSTEM Lec-1 Dr. Muhammad Tariq Javed Professor Department of Pathology, University of Agriculture, Faisalabad. Email: mtjaved@uaf.edu.pk Web: http://www.geocities.ws/mtjaved 1 2 Conducting
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research
 Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Mouse Serum Anti-HDM IgE Antibody Assay Kit
 Mouse Serum Anti-HDM IgE Antibody Assay Kit Catalog # 3037 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people
Mouse Serum Anti-HDM IgE Antibody Assay Kit Catalog # 3037 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD.
 Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
16 Innate Immunity: M I C R O B I O L O G Y. Nonspecific Defenses of the Host. a n i n t r o d u c t i o n
 ninth edition TORTORA FUNKE CASE M I C R O B I O L O G Y a n i n t r o d u c t i o n 16 Innate Immunity: Nonspecific Defenses of the Host PowerPoint Lecture Slide Presentation prepared by Christine L.
ninth edition TORTORA FUNKE CASE M I C R O B I O L O G Y a n i n t r o d u c t i o n 16 Innate Immunity: Nonspecific Defenses of the Host PowerPoint Lecture Slide Presentation prepared by Christine L.
Exploring the PD-L1 Pathway
 Active Within the tumor microenvironment Steps 1-3: Initiating and propagating anticancer immunity 1 may inhibit T-cell activity in the tumor microenvironment Dendritic cells capture cancer and then prime
Active Within the tumor microenvironment Steps 1-3: Initiating and propagating anticancer immunity 1 may inhibit T-cell activity in the tumor microenvironment Dendritic cells capture cancer and then prime
Overview of the immune system
 Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
Anastasios E. Germenis
 Anastasios E. Germenis Professor and Chairman Department of Immunology & Histocompatibility School of Medicine University of Thessaly University Hospital of Larissa Greece agermen@med.uth.gr The Complement
Anastasios E. Germenis Professor and Chairman Department of Immunology & Histocompatibility School of Medicine University of Thessaly University Hospital of Larissa Greece agermen@med.uth.gr The Complement
Diseases-causing agents, pathogens, can produce infections within the body.
 BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Immune System AP SBI4UP
 Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
ANATOMY OF THE IMMUNE SYSTEM
 Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
2. Innate immunity 2013
 1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A.
 UvA-DARE (Digital Academic Repository) Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A. Link to publication Citation for published
The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma
 Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces
 Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
for Development of Airway Hyperresponsiveness after Aerosolized Allergen Exposure in the Absence of Adjuvant
 This information is current as of May 14, 2018. References Subscription Permissions Email Alerts Mast Cells, FcεRI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized
This information is current as of May 14, 2018. References Subscription Permissions Email Alerts Mast Cells, FcεRI, and IL-13 Are Required for Development of Airway Hyperresponsiveness after Aerosolized
