PULMONARY FUNCTION IN SARCOIDOSIS
|
|
|
- Suzan Clark
- 6 years ago
- Views:
Transcription
1 Thorax (1958), 13, 48. PULMONARY FUNCTION IN SARCOIDOSIS BY R. MARSHALL,* HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, AND D. V. BATESt From the Medical Unit, St. Bartholomew's Hospital, London, and King's College Hospital, London The effects of sarcoidosis upon lung function have already been studied by a number of investigators. Usually, however, sarcoidosis has been included only as one of a group of diseases producing pulmonary fibrosis, and sarcoidosis itself has not been specifically investigated. The purpose of this investigation was to study pulmon.ary function in sarcoidosis at all stages and to determine the nature of any disturbance and changes associated with progression of the disease. The abnormalities of function associated with particular radiographic appearances were also investigated, and we tried to assess the value of the various tests of function in gauging disability, progress, and prognosis. METHODS In order to study the disea4e at different stages the patients were chosen for investigation from a series of 2 according to the duration and radiographic form of their disease. They were allocated accordingly to one of five groups. These groups were: GROUP I.-Patients with long-standing pulmonary fibrosis as shown radiographically by hilar distortion, often with elevation, and linear shadows. GROUP II.-Patients with infiltrative shadows present for more than two years. GROUP III.-Patients with infiltrative shadows known to have been present for less than two years since diagnosis. GROUP IV.-Patients known to have been in Groups II or III but in whom radiologically the lung fields had cleared completely. GROUP V.-Patients with hilar lymph node enlargement only and normal lungs radiographically. Twenty-six patients (11 men and 15 women) were investigated: of these, six were in Group I, three in Group II, six in Group III, six in Group *Present address: Nuffield Department of Surgery. Radcliffe Infirmary, Oxford. tpresent address: Royal Victoria Hospital, Montreal, Canada. (RECEIVED FOR PUBLICATION JANUARY 13, 1958) IV, and five in Group V. The diagnosis of sarcoidosis was supported by biopsy of either liver, lymph node, skin, or conjunctiva in 2 of the 26 patients. In four others liver biopsy was negative and in two was not attempted. Most patients had previously been treated with streptomycin and P.A.S. and nine had received cortisone (Table I). We excluded patients with cardiac disease or pulmonary disease other than sarcoidosis and the one patient with dyspnoea more severe than grade 3 (see classification below) who was unsuitable for exercise tests. The clinical category of the patients and the clinician's assessment of dyspnoea were not known to the observers carrying out the pulmonary function tests until after these had been assessed. A clinical assessment of dyspnoea was made from the history of exercise tolerance according to the following grades: Grade.-Normal performance without dyspnoea for a person of comparable age. Grade 1.-Dyspnoea on moderate effort, i.e., running for a bus or inability to climb stairs pr hills quickly. Grade 2.-Can walk on the level without dyspnoea but additional tasks not possible. Can climb one flight of stairs without undue distress. Grade 3.-Can walk up to 5 yards on level without stopping. Capable of sedentary work and light household duties. PULMONARY FUNCTION TESTS The measurements of pulmonary function made on these patients were (a) the subdivisions of lung volume, (b) the mixing efficiency of the lungs, (c) the maximum breathing capacity (M.B.C.), (d) the fast expiratory flow rate (E.F.R.4), (e) the diffusing capacity for carbon monoxide (D.A), (D) the lung compliance, and (g) the non-elastic resistance of the lungs. The subdivisions of lung volume have been named according to the standard terminology (Pappenheimer, Comroe, Cournand, Ferguson,
2 PULMONARY FUNCTION IN SARCOIDOSIS TABLE I CLINICAL DATA ON 26 PATIENTS WITH PULMONARY SARCOIDOSIS Biopsy Known Patient Sex Age Height Weight B.S.A. Liver, Duration Previous Date of Radiological Appearances No. ex (yr.) (cm.) (kg.) (m2) Skin, or of Disease Treatment Treatment Lymph Node (yr.) Group I 1 F * S, P, C 1953 Bilateral reticulo-nodular shadows with fibrotic streaks in upper zones 2 F _ 7 Nil Bilateral upper zone reticulation with fibrotic streaks 3 F S, P. C 1953 Bilateral confluent mottling with fibrotic streaks in upper zones 4 F S, P, C 1949,1951 Gross upper lobe fibrosis and fine mottling 5 F * C 1956 Bilateral coarse nodular shadows with large conglomeration right upper lobe 6 F i S, P, C 1952 Bilateral stippling. Minimal linear streaks both bases and right upper Ill J zone Group II-11_ 7 F * S, P, C 1953 Diffuse bilateral fine stippling (1-2 mm. spots) 8 M * S, P 1956 Diffuse reticulo-nodular shadows both lungs (1-3 mm. spots). Hilar nodes + 9 F * S, P, C 1952,1953 Diffuse bilateral reticulo-nodular shadows (2-4 mm. spots) Group III 1 F S, I 1956 Diffuse bilateral reticulo-nodular shadows 11 M S, P Bilateral coarse reticular shadows in upper lobes 12 M Nil Sparse pulmonary reticular shadows Hilar nodesi+ 13 M I P,, I 1956 Bilateral perihilar stippling (1-2 mm. spots). Hilar nodes , Nil Diffuse faint ground-glass shadowing 15 M I S, P, C Slight bilateral mottling (1-5 mm. spots). Hilar nodes + Group IV 16 F S, P Normal 17 M S, P F Nil 19 F I S, P M Nil 21 M Group V 22 F j, Hilar nodes + + Lung fields clear 23 F Calciferol,,,, I I 24 M * Nil i,,,, 25 M S, I ,,,, + 26 F i P, I, C 1956,,,, + + Filley, Fowler, Gray, Helmholtz, Otis, Rahn, and Riley, 195; Comroe, Forster, DuBois, Briscoe, and Carlsen, 1955). The mixing efficiency of the lungs is predominantly a measure of the uniformity of alveolar ventilation. The fast expiratory flow rate is the maximum rate of air flow which is attained when a subject makes a forced expiration from the full inspiratory position. This was measured in addition to the M.B.C., because, although the latter is more familiar to clinicians, the former gives more consistent results, is easier to perform, and is not so fatiguing to the patient. The diffusing capacity of the lungs is a measure of the quantity of a gas, such as oxygen, which can pass per minute from the alveoli into the blood with a pressure gradient of S=Streptomycin. P=P.A.S. C=Cortisone. I=Isoniazid. 1 mm. Hg. The diffusing capacity for carbon monoxide has been measured, since carbon monoxide behaves similarly to oxygen and the method is technically easier. The lung compliance is a measure of the elastic properties of the lung and is expressed as the increase in lung volume (in litres) per centimetre water increase in the pressure distending the lung. The non-elastic resistance which has been measured is the total frictional resistance to lung movement; this includes both the resistance to flow of air through the airways and the frictional resistances of the lung tissues themselves. In this study it was not possible to measure the two factors separately, but previous work (Marshall and DuBois, 1956) has shown that in sarcoidosis the tissue resistance 49
3 5 R. MARSHALL, HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, and D. V. BATES factor may be the major component of the nonelastic resistance, The pulmonary function tests were summarized for each patient by separate assessment of ventilatory defect, diffusion defect, and compliance defect, these assessments being made on the results of the expiratory flow rate, diffusing capacity for carbon monoxide, and compliance measurements respectively. Each function was assessed on the basis of four grades and points were allotted according to the following scale: normal, ; slightly reduced, 1; moderately reduced, 2; and severely reduced, 3. The patient's F.R.C. was taken into consideration in the assessment of both the diffusing capacity (Bates, Boucot, and Dormer, 1955) and compliance (Marshall, 1957). The normality of the D. was assessed on ihe exercise figure. The compliance was assessed from the resting figures only, since in these patients there was usually no appreciable change on exercise. A major difficulty arises in deciding whether particular values of the diffusing capacity and the compliance are normal, namely, should these values be compared to normal values predicted from the surface area of the subject, or to values predicted for a normal subject of similar lung volume? In analysing the results the latter method has been followed, as this seems a more practical way of assessing the changes in this particular condition. TECHNIQUES.-All the pulmonary function tests on each patient were carried out on the same day. The subdivisions of the vital capacity were measured using a closed circuit spirometer and with the patient seated. The functional residual capacity (F.R.C.) and mixing efficiency (M.E. %) were measured by the closed circuit helium method described by Bates and Christie (195) and the index used here is independent of tidal volume and lung volume. The values obtained for lung volumes were corrected to body temperature and pressure saturated. The predicted values for lung volumes shown in Table II were calculated from the formulae derived by Needham, Rogan, and McDonald (1954). All the predicted lung volumes except for the F.R.C. in adults were calculated from the simplified regression equations. The predicted F.R.C. in adults was calculated from the " best regression equation " (Table X of Needham and others). The comparisons between these predicted values and the lung volumes found is believed to be valid, since identical methods of measurement have been used, and the range and means of values found in normal subjects by Needham and others and by ourselves have been comparable. The maximum breathing capacity (M.B.C.) was measured by breathing through a low-resistance valve from a bag containing 5% CO2 in oxygen. The volume removed from the bag during 15 seconds of maximum ventilation was measured, and this volume, multiplied by 4, is given as the M.B.C. The expiratory flow rate (E.F.R.4) was measured as described by Kennedy (1953) but using a spirometer with a light-weight bell. The diffusing capacity for carbon monoxide was measured by the method described by Bates and others (1955) and calculated by their second method (D.11) which assumes that the end tidal sample represents the mean alveolar tension. The lung compliance and non-elastic resistance were measured by simultaneous measurement of intraoesophageal pressure and air flow or tidal volume. The technique used for measurement of compliance was that described by Marshall and DuBois (1956) and the non-elastic resistance was measured by the subtraction method of Mead and Whittenberger (1953). Measurements of diffusing capacity and lung mechanics were made with the patient seated at rest and were then repeated with the patient exercising on a motor-driven treadmill. No attempt was made to exercise the patients to their limits of tolerance, and the treadmill speed was one that the patient could maintain for about 1 minutes without undue discomfort. The " experimental" assessment of dyspnoea was made by two observers (R. M. and D. V. B.) on the patients' performance on the treadmill, and on whether the patient was actually dyspnoeic at the end of the exercise period. At the time this assessment was made, none of the results of the function tests had been calculated. RESULTS The results obtained from measurement of lung volumes are shown in Table II. All the lung volumes are, in general, slightly reduced and this reduction is greater in Groups I, II, and III, where there is more radiographic change in the lungs than in Groups IV and V. In each group, however, there is a large variation, and, in particular in patient 23 in Group V, lung volumes are grossly reduced. The mixing efficiency is normal in most of the subjects. The diffusing capacity on exercise assessed in relation to the patients' F.R.C. is shown in Fig. 1. Impairment of diffusing capacity is more marked in patients in Groups I and II (Table III) although tw, patients in Group I have a normal diffusing capacity. Five patients in Group III have a normal D. in spite of radiographic changes in the lung. On the other hand, five out of six patients in Group IV have a diffusion defect although the lung fields are now normal radiographically. The patients in Group V who have never had any evidence of lung involvement have, with one exception, normal diffusing capacities. The pulmonary compliance, when assessed in relation to the patient's F.R.C., is surprisingly normal in most patients and only lies below the lower limit of normal in four patients, two in
4 TABLE II LUNG VOLUMES, M.B.C., AND E.F.R.4 IN 26 PATIENTS WITH PULMONARY SARCOIDOSIS Patient V.C. (.) I.C. (I.) E.R.V. (.) F.R.C. (.) R.V.(I. R.V. M E M.B.C. No. Observedl % Pred. Observedi /Y Pred. Observed % Pred. Observed % Pred.iObservedj % Pred. T.LC. min.) Group II Gr-oup II _; Group III E.F.R/.) (I./min.) * * G p 2: Group V * V.C. =Vital capacity. I.C. =Inspiratory capacity. E.R.V.=Expiratory reserve volume. F.R.C.=Functional residual capacity. R.V. Residual volume. T.L.C.=Total lung capacity. Obs.-Observed value. % Pred.=Observed values as a percentage of predicted value. M.E.%=Mixing efficiency percentage of normal. M.B.C.= Maximum breathing capacity. E.F.R.4 =Expiratory flow rate (Kennedy, 1953). E 14Ii I IG ROUP I - I DL ZM I HI Il I GROUP HUE I ER _ 6 _ 8 ' EXERCISE co (ML CQ/MIN /MM. HG) F. R. C. (LITRES) GROUP I Iv kjroupj FIG. 1.-Histogram of Dco,'F.R.C. in the patients with sarcoidosis compared with the values obtained in 18 normal subjects. Il I--I- 2.- L- D Lu - w z l i l t I 3 4 S 6 7 COMPLIANCE (LITRES PER CM H2J F R C (L ITRES FIG. 2.-Histogram of compliance/f.r.c. in the patients with sarcoidosis compared with the values obtained in 5 normal subjects. G
5 52 R. MARSHALL, HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, anid D. V. BATES TABLE III DIFFUSING CAPACITY FOR CARBON MONOXIDE AND LUNG MECHANICS IN 26 PATIENTS WITH SARCOIDOSIS AT REST AND ON EXERCISE Rest Exercise Patient Minute Res- D Co-Non-elastic Tread- Res- 2 D Corn Non-elastic No. Volume pirations plianci Resistance mm Mnute pirations Uptake CO (1./min.) 2 pliance Reisn per (mi./mmn. (1. cm (cm.h2/ Sped Volume pe (MI./ M.V (ml. min. (1./cm. (cm.h2' G Group I at(1.mi.) (m.p.h.) Minute mm.hg) H2) 51./sec.) (mph.m.) Minute min.) mm.hg) H2) :5'.sec.) mi)mmh)/)sec. at * *9-13 2* * i Group II , Group III i , , * , , Group IV ' , , Group V , i , Group I, one in Group II, and one in Group V. Fig. 2 shows the distribution of the ratio compliance c-f.r.ce in each of the groups of patients in comparison with a group of 5 normal subjects (Marshall, 1957). In Group I there is a tendency to low compliance figures, but the compliance in the other groups is distributed throughout the normal range. The non-elastic resistance in a series of 5 normal subjects has been found to lie between 1.2 and 3.4 cm. water per litre per second measured at a flow rate of.5 litres per second in those 37 subjects in whom the F.R.C. was 2.5 litres or more. In the 13 in whom the F.R.C. was below 2.5 litres there was a considerable increase in airway resistance with decreasing F.R.C. The number of normal subjects tested with F.R.C.s below 2.5 litres was too small to define accurate limits of normality, but if an " envelope " is drawn to enclose all the normal values (Fig. 3) the values in only three patients with sarcoidosis lie outside this envelope. In this figure conductance (reciprocal of resistance) has been plotted against F.R.C. Two patients with abnormal values are in Group I and both of these patients have normal compliance; the third patient is in Group V, also with normal compliance. There is fair agreement between the E.F.R.-t" and the M.B.C., but where these two values differ widely (patients 5, 16, 18, and 26) the M.B.C. is the lower one, presumably due to an insufficient effort on the patient's part. The results obtained -7, CONDUCTANCE., NORMAL LITRES /IMITS PER/ 4 /\ SECOND / 3 / - PER / *. M22 /.. _ S FUNCTIONAL RESIDUAL CAPACITY- LITRES FIG. 3.-The relationship between lung conductance (reciprocal'of non-elastic resistance) and F.R.C. The interrupted lines show the limits of normal values (Marshall, 1957).
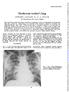
6 PULMONARY FUNCTION IN in these patients suggest that the E.F.R.4 test gives the more reliable estimate of expiratory obstruction. The assessment of ventilatory defect (based on the results of the E.F.R.4 test) shows impaired ventilation in some of the patients in all groups. Points of note, however, are the relative normality of patients in Group III -(infiltration for less than two years) and the reduction in expiratory flow rates of patients in Group V (enlarged hilar nodes). The assessment of ventilatory defect, based on the E.F.R.4, agrees fairly well with the values obtained for non-elastic resistance, but, since it does not take into account the F.R.C., the agreement is poor in some patients who have a low F.R.C. and in whom the non-elastic resistance is considered normal. DISCUSSION The principal disturbance of pulmonary function that has been found in these patients is a defect of diffusion. Other abnormalities such as a ventilatory defect and reduced compliance were encountered, but are of minor importance. The fact that pulmonary sarcoidosis may not be a disabling condition in spite of marked radiographic changes is supported by the findings in TABLE IV ASSESSMENT OF PULMONARY FUNCTION IN 26 PATIENTS WITH PULMONARY SARCOIDOSIS Dyspnoea Assessment Ventila- Dfuin Cm Patient Experi- tor pifusoncon-e No. Clinical mental Defect Defect Defe Group I Group II Group III Group IV J1 Group V =Normal. I -Slight impairment. 2=Moderate impairment. 3 = Severe impairment. SARCOIDOSIS these patients. A few patients with very severe dyspnoea were excluded from this study, but of the 26 investigated only five had moderate or severe dyspnoea as assessed from their history and only four as assessed on the basis of treadmill exercise (Table IV). Of the five patients with dyspnoea of grade 2 or 3 as assessed clinically, two appeared to have no appreciable dyspnoea during treadmill exercise, and in these two (patients 1 and 2) the function tests showed no abnormality. A diffusion defect was found in nine of 12 patients who gave a history of dyspnoea and in six of seven in whom dyspnoea was observed on treadmill exercise. From the overall assessment of function shown in Table IV it is clear that patients in Groups I and II have the most severely impaired function, the mean of the points allotted on assessment of Groups I and II being 2.7 and 4 per patient respectively, whilst in Groups III, IV, and V it is only.5, 1.3, and 1.6 respectively. In order to relate disturbance of pulmonary function to the radiographic appearances in the lungs the latter may be divided in our 26 patients into four categories, namely, advanced fibrosis. (Fig. 4), diffuse fine stippling (shadows measuring approximately 1 mm. or less in diameter) (Fig. 5), diffuse reticulo-nodular shadows, measuring several millimetres in diameter (Fig. 6), and clear, including those with enlarged hilar nodes. The most severe defects of function occur in those FiG. 4.-Chest radiograph of a woman aged 45 years (patient No. 4), showing advanced and fibrotic pulmonary sarcoidosis of 1 years' duration. The patient also had splenomegaly and a chronic uveitis. The diagnosis was supported histologically by liver and conjunctival biopsy. 53
7 54 R. MARSHALL, HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, and D. V. BATES patients with advanced fibrosis, though patients 1 and 2 are exceptions. The pattern of fibrosis in those two patients is quite typical (Fig. 7) but of lesser extent than the others. Severe diffusion defect most commonly occurs in patients with diffuse fine stippling (patients 6, 7, and 14). We found that function is as impaired in patients whose lung fields have cleared as in those with diffuse reticulo-nodular shadows. This emphasizes that there is no close relationship between the radiographic appearances and pul- FIG. 5.-Radiograph of part of the right lung field of a woman aged 39 years (patient No. 7), showing diffuse fine stippling in pulmonary sarcoidosis. The patient also had splenomegaly and enlarged peripheral lymph nodes. The diagnosis was supported histologically by liver biopsy. FIG. 6.-Radiograph of part of the right lung field of a man aged 35 years (patient No. 8), showing diffuse reticulo-nodular shadows in pulmonary sarcoidosis. The patient also had sarcoidosis of the skin. FIG. 7.-Chest radiograph of a woman aged 45 years (patient No. 2), with sarcoidosis of eight years' duration, showing pulmonary fibrosis to a lesser extent than that shown in Fig. 4 and associated with normal pulmonary function. FIo. 6 Thorax: first published as /thx on 1 March Downloaded from Fla. 5 FIG. 7 on 2 June 218 by guest. Protected by copyright.
8 PULMONARY FUNCTION IN SARCOIDOSIS 'f*4 FIG. 8.-ection of a lung biopsy taken from a woman aged 45 years (p,atient No. 16), showing areas of fibrosis (haematoxylin and eosin, X 5). The patient presented with erythemau nodosum and hilar node enlargemnent with bilateral coarse miliary shadows in the chest radiograph. The biopsy was taken one year later at a time when the chest radiograph had returned to normal. monary function in sarcoidosis, a discrepancy which may be caused by the presence of subradiographic granulomata or fibrosis (Fig. 8). In estimating the effects of such changes we have related the duration of the disease in the clinical groups II, III, and IV (patients who have all had at some time diffuse mottling in the lung fields) to the degree of diffusion defect. The mean duration of disease in patients in these groups with diffusion defect is 44 months, while the mean for those with normal diffusion is 21 months, and there is a significant correlation between duration of disease and degree of diffusion defect as graded in Table IV (r= +.695; S.E. = +.27). It also seems from this that the advent of radiographic clearing, as occurred in Group IV, is of little value in assessing the prognosis in regard to function, especially pulmonary gas diffusion. Some previous investigators have emphasized the tendency of patients with sarcoidosis to develop chronic obstructive emphysema. The largest reported series studied by means of function tests has been that of Stone, Schwartz, Feltman, and Lovelock (1953). They divided their patients into three groups based on the duration of the disease. They found that in the group (seven patients) with pulmonary involvement lasting for more than three years the type of functional abnormality could be either of the "emphysema " pattern with respiratory obstruction (three patients) or of the fibrosis pattern with predominant restriction of lung movement (three patients). One patient in this group had essentially normal pulmonary function tests. McClement, Renzetti, Himmelstein, and Cournand (1953) studied 1 patients and on the basis of pulmonary function tests divided them into three groups. The first group had evidence of reduced lung volume only, the second group reduced lung volumes and evidence of alveolar-capillary block 55
9 56 R. MARSHALL, HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, and D. V. BATES (diffusion defect), and the third group (one patient only) pulmonary function tests suggestive of chronic obstructive emphysema. Coates and Comroe (1951) also reported findings suggestive of emphysematous changes in the five patients with pulmonary sarcoidosis whom they studied, as also was the case in the patient reported by Lukas (1951). On the other hand, Baldwin, Cournand, and Richards (1949) in their study of pulmonary fibrosis included five patients with sarcoidosis and specifically excluded any patients with ventilatory obstruction or raised residual air percentage. The diagnosis of emphysema in sarcoidosis has been based on increased residual volume, increased residual volume/total lung capacity ratio, impaired mixing efficiency, and spirographic evidence of respiratory obstruction. These criteria are often considered diagnostic of chronic obstructive emphysema such as occurs as the end-result of long-standing chronic bronchitis, but they could well be indicative of bronchial constriction alone without the development of loss of tissue and the tendency to bronchial collapse usually present in emphysema. The ratio of residual volume to total lung capacity so often used as an indication of emphysema is particularly misleading in a disease like sarcoidosis in which the reduction in total lung capacity alone can increase this ratio above the level at which it is often considered U INSP. LL 1. _- -Jj cci._ EXP 1 CIH2 PRESSURE EXERTED AGAINST NON-ELASTIC RESISTANCE FIG. 9.-Tracings of flow and non-elastic pressure obtained by the method Whittenberger (1953). The subjects were panting to produce high rat (a) patient with sarcoidosis, (b) patient with emphysema. nostic of emphysema. Only two of the nts studied here had a residual volume greater one coefficient of variation more than the pred, but nine patients had a residual volume/ lung capacity ratio greater than 35,, (the e often taken to indicate emphysema). Of wo patients with an increased residual volume, ier had a non-elastic resistance greater than im. water per litre per second or a mixing trncy less than 5%. Moreover, the tracing 9) of air flow and non-elastic pressure ined on the oscilloscope screen by the method lead and Whittenberger was not looped in the ratory phase, as is found in patients with hysema (Mead, Lindgren, and Gaensler, ). Although the pulmonary function tests in patients studied here show no evidence of nic obstructive emphysema, this does not exthe presence of localized areas of bullous iysema which are often demonstrated histoally in sarcoidosis (Mallory, 1948; Longcope Freiman, 1952). any previous investigators have demonstrated *eduction in vital capacity and lung volumes rcoidosis (Leitner, 1946; Galdston, Weisen- Benjamin, and Rosenbluth, 1951; Bruce and den, 194; Small, 1951 ; Riley, Riley, and Hill, Austrian, McClement, Renzetti, Donald, and Cournand, 1951; Williams, 1953), and some have reported a close association between changes in vital capacity and other lung function tests and the radiographic changes or clinical findings (Bruce and Wassen, 194; Small, 1951; Lukas, 1951; Riley and others, 1952). If diminution of vital capacity or inspiratory capacity were due to changes in the lung one might expect that the diminuj tion would be accompanied by abnormal stiffness of the lungs. In our patients there is a significant correlation between compliance and inspiratory capacity (r= +.738; S.E.= +.2), but of the seven patients with a significantly low vital capacity (less than 8% of predicted) six have a compliance within d of Mead and normal limits taking into account the patient's F.R.C.
10 PULMONARY FUNCTION IN This suggests that the reduction of vital capacity in sarcoidosis is due more to the replacement of gas-containing lung by solid tissue than it is to increased stiffness of the lung tissue that is expanding. On the other hand, the reduction in diffusing capacity does not appear to be related to the reduction in lung volumes and the diffusing capacity is found to be impaired in many patients even when assessed in relation to the reduced F.R.C. Thus the effect of sarcoidosis is not only that of producing a " lobectomy "; the defect of function is not solely due to the reduction in the volume of functioning lung. Several investigators have attempted to account for different patterns of impaired pulmonary function in sarcoidosis on the basis of different patterns of pulmonary fibrosis. The peribronchial pattern of fibrosis is thought to give rise to emphysema (Coates and Comroe, 1951; Stone and others, 1953; Spain, 195), the interstitial type to alveolar capillary block (Austrian and others, 1951), and perivascular fibrosis to impaired diffusion and increased venous admixture (Riley and others, 1952). Our results show that ventilation, diffusion, and compliance are often affected simultaneously, but there is an isolated instance of increased non-elastic resistance without any other defect (patient 23), and in five patients an impaired diffusing capacity was found with no other, or out of proportion to any other, defect (patients 6, 9, 14, 16, and 17). In fact, of the three assessments-ventilation, diffusion, and compliance the diffusion defect is the one most often seen in these patients, and change in compliance is least often seen. The relatively normal values for compliance are interesting in view of the degree of lung involvement seen radiographically. Patients in Group I with radiographic evidence of fibrosis most commonly show decreased compliance, but even in them the compliance may still be normal. On the other hand, the compliance may be significantly reduced in patients with apparently normal lung fields (patient 24). The normal values for compliance in relation to the F.R.C. suggest that, although the sarcoid lesion has reduced the volume of expanding lung, the elastic properties of the remaining alveoli have not altered and expansion therefore occurs in the relatively normal tissue between the granulomata. In some of the patients the diffusing capacity in relation to the F.R.C. is moderately or severely impaired in spite of a normal compliance. If the functioning alveoli were thickened one would expect a decrease in compliance to accompany the impaireld diffusing capacity, as happens, for SARCOIDOSIS instance, in the alveolar fibrosis of the Hamman- Rich syndrome. Histological examination of the lungs in sarcoidosis (Schaumann, 1936; Mallory, 1948) shows that the granulomata may have a perivascular distribution and may also invade and obliterate blood vessels; this focal obstruction to perfusion of the lung could cause the reduced diffusing capacity. Five out of the six patients in Group IV in whom the lung lesions cleared radiographically were left with impaired diffusion. In order to provide more definite evidence of the relationship of diffusing capacity to progress of the disease it is necessary to carry out repeated tests of diffusing capacity during the different stages of the disease. Riley and others (1952) found no significant increase of the diffusing capacity for oxygen in three patients after A.C.T.H. treatment although the lesions partially cleared in two. McClement and others (1953) reported an increase of the oxygen-diffusing capacity in two out of five patients treated with cortisone. It is possible that vessels involved in the early stages of granulomata may have their function restored when the granulomata regress, but vessels which are more seriously involved are obliterated completely by fibrous tissue. The oxygen utilization (2/V, the oxygen uptake in ml. per litre of ventilation) in only four subjects falls below the range of values ( ) found by Donald, Bishop, Cumming, and Wade (1955) for normal subjects exercising to approximately the same degree. In their subjects there 141 Ui o 12- we LI- -j ~ U) tlx LId I 8. 6, L.ti w w /v o (EXERCISE) FIG. 1.-The relationship between Doo per litre F.R.C. and the OJV ratio on exercise. The numerals, 1, 2, and 3 indicate the asesssment of the diffusion defect
11 58 R. MARSHALL, HUGH SMELLIE, J. H. BAYLIS, CLIFFORD HOYLE, and D. V. BATES was no variation in the oxygen utilization on exercise with oxygen uptakes between about 3 and 1, ml. per minute. The oxygen uptake in the patients investigated here varied from 39 to 1,6 ml. per minute (mean 92 ml. per minute). Of the four patients with low oxygen utilization three were in Group I and one in Group II. If the ventilation in these patients is determined by the need to maintain an adequate oxygen uptake, then the oxygen utilization might be expected to correlate with the diffusing capacity of the lungs. In Fig. 1 the exercise D per unit volume of F.R.C. is plotted against the O2/V, both measurements being made on exercise. This shows a general relationship between the two observations, the correlation coefficient being significant at the 2% level (r= +.476). The work of Ogilvie, Forster, Blakemore, and Morton (1957) has shown that the diffusing capacity, as measured by a single breath technique, is proportional to body surface area. In this study, the correlation coefficient between D, per unit body surface area and oxygen utilization is (S.E. +.2). These observations certainly suggest a relationship between the diffusing capacity and the level of ventilation required for a given oxygen uptake. We conclude from this investigation that the main lesion of pulmonary function in sarcoidosis is a reduction in diffusing capacity of the lungs. In addition, reduction of the lung volume by the disease may contribute to the disability by impairing the mechanical functions of the lung. Long-standing disease is accompanied by greater impairment of diffusion and possibly by decreased compliance when fibrosis occurs. Radiographic clearing of the lesions may not be accompanied by a return of normal function. No close relationship exists between the radiographic appearances of the lungs and the defects in pulmonary function, but patients with diffuse fine stippling or reticulation were more often found to have a lowered diffusing capacity, and radiographic evidence of fibrosis was sometimes accompanied by decreased compliance. As far as can be determined from this study, in which patients at different stages of the disease were examined on one occasion only, detailed pulmonary function tests are capable of indicating the effect of the present and past le^-ions on the performance of the lungs. Measurements of lung volumes and ventilatory defect alone give little useful information. SUMMARY The lung volumes, mixing efficiency, mechanical properties of the lungs, and diffusing capacity were measured in 26 patients with pulmonary sarcoidosis. The patients were selected to represent all stages of the disorder and each was allocated to one of five groups according to the duration of the disease and the radiographic appearances of the lungs. The results of the pulmonary function tests are discussed in relation to these groups. No evidence of obstructive emphysema was found and the compliance of the lungs was usually normal. The commonest lesion of pulmonary function was a diffusion defect which occurred more frequently with long-standing disease. Five out of six patients in whom pulmonary sarcoidosis had cleared radiographically at the time of the tests showed impaired diffusion. We are indebted to all the patients in this series for their willing co-operation and to many colleagues who referred them to the care of one of us (C. H.); to Professor H. A. Magnus for his generous help with the histology of biopsy specimens; and to Mr. L. S. Bartlett and Miss J. A. West for technical assistance. Some of our expenses were defrayed by a grant from King's College Hospital Research Fund. REFERENCES Austrian, R., McClement, J. H., Renzetti, A. D., Donald, K. W., Riley, R. L., and Cournand, A. (1951). Amer. J. Med., 11, 667. Baldwin, E. def., Cournand, A., and Richards, D. W. (jr.) (1949). Medicine (Baltimore), 28, 1. Bates, D. V., Boucot, N. G., and Dormer, A. E. (1955). J. Physiol. (Lond.), 129, and Christie, R. V. (195). Clin. Sci., 9, 17. Bruce, T., and Wassen, E. (194). Acta med. scand., 14, 63. Coates, E. O., and Comroe, J. H. (jr.) (1951). J. clin. Invest., 3, 848. Comroe, J. H. (jr.), Forster, R. E., DuBois, A. B., Briscoe, W. A., and Carlsen, E. (1955). The Lung. Year Book Publishers, Chicago. Donald, K. W., Bishop, J. M., Cumming, G., and Wade, O. L. (1955). Clin.Sci., 14, 37. Dornhorst, A. C., and Kelly, H. B. (1954). Lancet, 1, 29. Galdston, M., Weisenfeld, S., Benjamin, B., and Rosenbluth, M. B. (1951). Amer. J. Med., 1, 166. Kennedy, M. C. S. (1953). Thorax, 8, 73. Leitner, S. J. (1946). Cardiologia (Basel), 1, 379. Longcope, W. T., and Freiman, D. G. (1952). Medicine (Baltimore), 31, 1. Lukas, D. S. (1951). Amer. Rev. Tuberc., 64, 279. McClement, J. H., Renzetti, A. D., Himmelstein, A., and Cournand, A. (1953). Amer. Rev. Tuberc., 67, 154. Mallory, T. B. (1948). Radiology, 51, 468. Marshall, R. (1957). Clin. Sci., 16, 57. -and DuBois, A. B. (1956). Ibid., 15, 473. Mead, J., Lindgren, I., and Gaensler, E. A. (1955). J. clin. Invest., 34, and Whittenberger, J. L. (1953). J. appl. Physiol., 5, 779. Needham, C. D., Rogan, M. C., and McDonald, I. (1954). Thorax, 9, 313. Ogilvie, C. M., Forster, R. E., Blakemore, W. S., and Morton, J. W. (1957). J. clin. Invest., 36, 1. Pappenheimer, J. R., Comroe, J. H., Cournand, A., Ferguson J. K. W., Filley, G. F., Fowler, W. S., Gray, J. S., Helmholtz, H. T., Otis, A. B., Rahn, H., and Riley, R. L. (195). Fed. Proc., 9, 62. Riley, R. L., Riley, M. C., and Hill, H. M. (1952). Bull. Johns Hopk. Hosp., 91, 345. Schaumann, J. (1936). Brit. J. Derm., 48, 399. Small, M. J. (1951). J. Amer. med. Ass., 147, 932. Spain, D. M. (195). Ann. intern. Med., 33, 115. Stone, D. J., Schwartz, A., Feltman, J. A., and Lovelock, F. J. (1953). Amer. J. Med., 15, 468. Williams, M. H. (jr.) (1953). J. clin. Invest., 32, 99.
PULMONARY FUNCTION IN BOECK'S SARCOID
 PULMONARY FUNCTION IN BOECK'S SARCOID By M. HENRY WILLIAMS, JR. (From the Department of Cardiorespiratory Diseases, Army Medical Service Graduate School, Walter Reed Army Medical Center, Washington, D.
PULMONARY FUNCTION IN BOECK'S SARCOID By M. HENRY WILLIAMS, JR. (From the Department of Cardiorespiratory Diseases, Army Medical Service Graduate School, Walter Reed Army Medical Center, Washington, D.
THE FORCED EXPIRATORY VOLUME AFTER EXERCISE,
 Thorax (1959), 14, 161. THE FORCED EXPIRATORY VOLUME AFTER EXERCISE, FORCED INSPIRATION, AND THE VALSALVA AND MULLER MAN(EUVRES BY L. H. CAPEL AND J. SMART From the London Chest Hospital (RECEIVED FOR
Thorax (1959), 14, 161. THE FORCED EXPIRATORY VOLUME AFTER EXERCISE, FORCED INSPIRATION, AND THE VALSALVA AND MULLER MAN(EUVRES BY L. H. CAPEL AND J. SMART From the London Chest Hospital (RECEIVED FOR
normal and asthmatic males
 Lung volume and its subdivisions in normal and asthmatic males MARGARET I. BLACKHALL and R. S. JONES1 Thorax (1973), 28, 89. Institute of Child Health, University of Liverpool, Alder Hey Children's Hospital,
Lung volume and its subdivisions in normal and asthmatic males MARGARET I. BLACKHALL and R. S. JONES1 Thorax (1973), 28, 89. Institute of Child Health, University of Liverpool, Alder Hey Children's Hospital,
Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases. Part III. On Pulmonary Fibrosis
 Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases Part III. On Pulmonary Fibrosis Kazuaki SERA, M.D. Pulmonary function studies have been undertaken on the pulmonary fibrosis as diagnosed
Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases Part III. On Pulmonary Fibrosis Kazuaki SERA, M.D. Pulmonary function studies have been undertaken on the pulmonary fibrosis as diagnosed
Prolonged treatment of pulmonary sarcoidosis
 Thorax (1967), 22, 519. Prolonged treatment of pulmonary sarcoidosis with corticosteroids CLIFFORD HOYLE, HUGH SMYLLIE1, AND DAVID LEAK From King's College Hospital, London The results are described of
Thorax (1967), 22, 519. Prolonged treatment of pulmonary sarcoidosis with corticosteroids CLIFFORD HOYLE, HUGH SMYLLIE1, AND DAVID LEAK From King's College Hospital, London The results are described of
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PATIENTS WITH CHRONIC OBSTRUCTIVE
 Thorax (1959), 14, 113. PATTERNS OF DISTURBED LUNG FUNCTION IN PATIENTS WITH CHRONIC OBSTRUCTIVE VESICULAR EMPHYSEMA BY From the London Hospital (RECEIVED FOR PUBLICATION AUGUST 15, 1958) Emphysema has
Thorax (1959), 14, 113. PATTERNS OF DISTURBED LUNG FUNCTION IN PATIENTS WITH CHRONIC OBSTRUCTIVE VESICULAR EMPHYSEMA BY From the London Hospital (RECEIVED FOR PUBLICATION AUGUST 15, 1958) Emphysema has
VENTILATION AND DIFFUSION IN ASTHMA
 Thorax (1959), 14, 146. THE EFFECTS OF BRONCHODILATORS ON PULMONARY VENTILATION AND DIFFUSION IN ASTHMA AND EMPHYSEMA BY From Brompton Hospital and the Institute of Diseases of the Chest, London (RECEIVED
Thorax (1959), 14, 146. THE EFFECTS OF BRONCHODILATORS ON PULMONARY VENTILATION AND DIFFUSION IN ASTHMA AND EMPHYSEMA BY From Brompton Hospital and the Institute of Diseases of the Chest, London (RECEIVED
PATTERNS OF DISTURBED LUNG FUNCTION IN PATIENTS
 Thorax (1959), 14, 216 PATTERNS OF DISTURBED LUNG FUNCTION IN PATIENTS WITH EMPHYSEMATOUS BULLAE BY COLIN OGILVIE AND MARY CATTERALL From the London Hospital In a previous publication (Ogilvie, 1959) an
Thorax (1959), 14, 216 PATTERNS OF DISTURBED LUNG FUNCTION IN PATIENTS WITH EMPHYSEMATOUS BULLAE BY COLIN OGILVIE AND MARY CATTERALL From the London Hospital In a previous publication (Ogilvie, 1959) an
Pulmonary function studies in bird breeder's lung
 Thorax (1969X, 24, 374. Pulmonary function studies in bird breeder's lung P. DINDA, S. S. CHATTERJEE, AND W. D. RIDING From Baguley Hospital, Manchester Pulmonary function studies were performed at the
Thorax (1969X, 24, 374. Pulmonary function studies in bird breeder's lung P. DINDA, S. S. CHATTERJEE, AND W. D. RIDING From Baguley Hospital, Manchester Pulmonary function studies were performed at the
A COMPARISON OF EXPIRATORY AND INSPIRATORY FLOW RATES IN HEALTH AND IN CHRONIC PULMONARY DISEASE
 Thorax (1959), 14, 225. A COMPARSON OF EXPRATORY AND NSPRATORY FLOW RATES N HEALTH AND N CHRONC PULMONARY DSEASE BY R. S. McNELL, G. D. MALCOLM, AND W. RHND BROWN From the Department of Pharmacology and
Thorax (1959), 14, 225. A COMPARSON OF EXPRATORY AND NSPRATORY FLOW RATES N HEALTH AND N CHRONC PULMONARY DSEASE BY R. S. McNELL, G. D. MALCOLM, AND W. RHND BROWN From the Department of Pharmacology and
EFFECTS OF INACTIVITY, WEIGHT GAIN AND ANTITUBERCULAR CHEMOTHERAPY UPON LUNG FUNCTION IN WORKING COAL-MINERS
 Ann. Occup. Hyg: Vol. 10, pp. 327-335. Pergamon Press Ltd., 1967. Printed in Great Britain EFFECTS OF INACTIVITY, WEIGHT GAIN AND ANTITUBERCULAR CHEMOTHERAPY UPON LUNG FUNCTION IN WORKING COAL-MINERS J.
Ann. Occup. Hyg: Vol. 10, pp. 327-335. Pergamon Press Ltd., 1967. Printed in Great Britain EFFECTS OF INACTIVITY, WEIGHT GAIN AND ANTITUBERCULAR CHEMOTHERAPY UPON LUNG FUNCTION IN WORKING COAL-MINERS J.
Serial pulmonary function tests in progressive systemic sclerosis
 Thorax, 1979, 34, 224-228 Serial pulmonary function tests in progressive systemic sclerosis L R BAGG AND D T D HUGHES From the Pulmonary Research Unit, Departnment of Chest Medicine, London Hospital, London,
Thorax, 1979, 34, 224-228 Serial pulmonary function tests in progressive systemic sclerosis L R BAGG AND D T D HUGHES From the Pulmonary Research Unit, Departnment of Chest Medicine, London Hospital, London,
CIRCULATION IN CONGENITAL HEART DISEASE*
 THE EFFECT OF CARBON DIOXIDE ON THE PULMONARY CIRCULATION IN CONGENITAL HEART DISEASE* BY R. J. SHEPHARD From The Cardiac Department, Guy's Hospital Received July 26, 1954 The response of the pulmonary
THE EFFECT OF CARBON DIOXIDE ON THE PULMONARY CIRCULATION IN CONGENITAL HEART DISEASE* BY R. J. SHEPHARD From The Cardiac Department, Guy's Hospital Received July 26, 1954 The response of the pulmonary
Spirometric studies on normal Turkish subjects aged 8 to 20 years
 Thorax (1969), 24, 714. Spirometric studies on normal Turkish subjects aged 8 to 20 years NECATI AKGUN AND HAMIT OZGONUL From the Departmenit of Physiology, Ege University Medical Faculty, Izmir, Turkey
Thorax (1969), 24, 714. Spirometric studies on normal Turkish subjects aged 8 to 20 years NECATI AKGUN AND HAMIT OZGONUL From the Departmenit of Physiology, Ege University Medical Faculty, Izmir, Turkey
Regional Lung Mechanics in Pulmonary Disease *
 Journal of Clinical Investigation Vol. 44, No. 6, 1965 Regional Lung Mechanics in Pulmonary Disease * C. J. MARTIN,t A. C. YOUNG, AND KOH ISHIKAWA (From the Firland Sanatorium and the Department of Physiology
Journal of Clinical Investigation Vol. 44, No. 6, 1965 Regional Lung Mechanics in Pulmonary Disease * C. J. MARTIN,t A. C. YOUNG, AND KOH ISHIKAWA (From the Firland Sanatorium and the Department of Physiology
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
PULMONARY ARTERIES IN CHRONIC LUNG DISEASE
 Brit. Heart J., 1963, 25, 583. RIGHT VENTRICULAR HYPERTROPHY AND THE SMALL PULMONARY ARTERIES IN CHRONIC LUNG DISEASE BY W. R. L. JAMES AND A. J. THOMAS From Llandough Hospital (United Cardiff Hospitals)
Brit. Heart J., 1963, 25, 583. RIGHT VENTRICULAR HYPERTROPHY AND THE SMALL PULMONARY ARTERIES IN CHRONIC LUNG DISEASE BY W. R. L. JAMES AND A. J. THOMAS From Llandough Hospital (United Cardiff Hospitals)
3. Which statement is false about anatomical dead space?
 Respiratory MCQs 1. Which of these statements is correct? a. Regular bronchioles are the most distal part of the respiratory tract to contain glands. b. Larynx do contain significant amounts of smooth
Respiratory MCQs 1. Which of these statements is correct? a. Regular bronchioles are the most distal part of the respiratory tract to contain glands. b. Larynx do contain significant amounts of smooth
Pulmonary function during pregnancy in normal women and in patients with cardiopulmonary disease
 Thorax (1970), 25, 445. Pulmonary function during pregnancy in normal women and in patients with cardiopulmonary disease KUDDUSI GAZIOGLU, NOLAN L. KALTREIDER, MORTIMER ROSEN, and PAUL N. YU Cardiology
Thorax (1970), 25, 445. Pulmonary function during pregnancy in normal women and in patients with cardiopulmonary disease KUDDUSI GAZIOGLU, NOLAN L. KALTREIDER, MORTIMER ROSEN, and PAUL N. YU Cardiology
Regional lung function in ankylosing
 Regional lung function in ankylosing RUSSELL M. STEWART', JOHN B. RIDYARD, and JOHN D. PEARSON Regional Cardio-Thoracic Centre, Broadgreen Hospital, Liverpool L14 3LB Thorax (1976), 31, 433. Stewart, R.
Regional lung function in ankylosing RUSSELL M. STEWART', JOHN B. RIDYARD, and JOHN D. PEARSON Regional Cardio-Thoracic Centre, Broadgreen Hospital, Liverpool L14 3LB Thorax (1976), 31, 433. Stewart, R.
PFT Interpretation and Reference Values
 PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
Respiratory Pathophysiology Cases Linda Costanzo Ph.D.
 Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
Factors determining maximum inspiratory flow and
 Thorax (1968), 23, 33. Factors determining maximum inspiratory flow and maximum expiratory flow of the lung J. JORDANOGLOU AND N. B. PRIDE From the M.R.C. Clinical Pulmonary Physiology Research Unit, King's
Thorax (1968), 23, 33. Factors determining maximum inspiratory flow and maximum expiratory flow of the lung J. JORDANOGLOU AND N. B. PRIDE From the M.R.C. Clinical Pulmonary Physiology Research Unit, King's
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Schlueter et al., 1969). The object of this study. was to investigate by measurements of lung. mechanics the nature of airflow obstruction in
 Mechanical properties of the lung in extrinsic allergic alveolitis1 C. P. W. WARREN, K. S. TSE, AND R. M. CHERNIACK Thorax, 1978, 33, 315-321 From the Departments of Medicine and Immunology, University
Mechanical properties of the lung in extrinsic allergic alveolitis1 C. P. W. WARREN, K. S. TSE, AND R. M. CHERNIACK Thorax, 1978, 33, 315-321 From the Departments of Medicine and Immunology, University
ACETYLCHOLINE AND THE PULMONARY CIRCULATION
 ACETYLCHOLINE AND THE PULMONARY CIRCULATION IN MITRAL VALVULAR DISEASE BY BROR SODERHOLM AND LARS WERKO* From the Department of Clinical Physiology and the First Medical Service, Sahlgrenska Sjukhuset,
ACETYLCHOLINE AND THE PULMONARY CIRCULATION IN MITRAL VALVULAR DISEASE BY BROR SODERHOLM AND LARS WERKO* From the Department of Clinical Physiology and the First Medical Service, Sahlgrenska Sjukhuset,
Finally, these data have been compared
 THE MECHANICAL BEHAVIOR OF THE LUNGS IN HEALTHY ELDERLY PERSONS 1, 2 By N. R. FRANK, J. MEAD, AND B. G. FERRIS, JR. (From the Department of Physiology, Harvard School of Publc Health, Boston, Mass.) (Submitted
THE MECHANICAL BEHAVIOR OF THE LUNGS IN HEALTHY ELDERLY PERSONS 1, 2 By N. R. FRANK, J. MEAD, AND B. G. FERRIS, JR. (From the Department of Physiology, Harvard School of Publc Health, Boston, Mass.) (Submitted
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
Inspiratory crackles-early and late
 Inspiratory crackles-early and late A. R. NATH and L. H. CAPEL The London Chest Hospital, Bonner Road, London E2 Thorax (1974), 29, 223. Nath, A. R. and Capel, L. H. (1974). Thorax, 29, 223-227. Inspiratory
Inspiratory crackles-early and late A. R. NATH and L. H. CAPEL The London Chest Hospital, Bonner Road, London E2 Thorax (1974), 29, 223. Nath, A. R. and Capel, L. H. (1974). Thorax, 29, 223-227. Inspiratory
during Dyspnea in Chronic Obstructive Pulmonary Disease
 Alterations in the Mechanical Properties of the Lung during Dyspnea in Chronic Obstructive Pulmonary Disease JEsus T. Sulmo and CouN R. WooLF From the Respiratory Research Laboratory, Toronto General Hospital
Alterations in the Mechanical Properties of the Lung during Dyspnea in Chronic Obstructive Pulmonary Disease JEsus T. Sulmo and CouN R. WooLF From the Respiratory Research Laboratory, Toronto General Hospital
Respiration Lesson 3. Respiration Lesson 3
 Respiration Lesson 3 and Airway Resistance (key factors affecting air flow) 1) What is the arterial blood pressure in a healthy 18 year old male? 2) What would his venous blood pressure be? 3) What is
Respiration Lesson 3 and Airway Resistance (key factors affecting air flow) 1) What is the arterial blood pressure in a healthy 18 year old male? 2) What would his venous blood pressure be? 3) What is
1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation.
 Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Lab 4: Respiratory Physiology and Pathophysiology
 Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
ventilation-perfusion inequalities
 Thorax (1966), 21, 518. The expiratory capnogram: ventilation-perfusion inequalities Current methods of estimating ventilationperfusion imbalance using radioactive gases (Dollery and Hugh-Jones, 1963),
Thorax (1966), 21, 518. The expiratory capnogram: ventilation-perfusion inequalities Current methods of estimating ventilationperfusion imbalance using radioactive gases (Dollery and Hugh-Jones, 1963),
RESPIRATORY FUNCTION AFTER PNEUMONECTOMY
 Thorax (1956), 11, 33. RESPIRATORY FUNCTION AFTER PNEUMONECTOMY BY M. B. McILROY AND D. V. BATES From the Dunn Laboratory, St. Bartholomew's Hospital, London, E.C.J After a pneumonectomy which is not combined
Thorax (1956), 11, 33. RESPIRATORY FUNCTION AFTER PNEUMONECTOMY BY M. B. McILROY AND D. V. BATES From the Dunn Laboratory, St. Bartholomew's Hospital, London, E.C.J After a pneumonectomy which is not combined
Lung mechanics in subjects showing increased residual volume without bronchial obstruction
 Lung mechanics in subjects showing increased residual volume without bronchial obstruction S VULTERINI, M R BIANCO, L PELLICCIOTTI, AND A M SIDOTI From the Divisione di Medicina Generale, Ospedale Fatebenefratelli,
Lung mechanics in subjects showing increased residual volume without bronchial obstruction S VULTERINI, M R BIANCO, L PELLICCIOTTI, AND A M SIDOTI From the Divisione di Medicina Generale, Ospedale Fatebenefratelli,
the maximum of several estimations was taken and corrected to body temperature. The maximum responses to carbon dioxide were measured
 THE EFFECT OF OBSTRUCTION TO BREATHING ON THE VENTILATORY RESPONSE TO Co21 By R. M. CHERNIACK2 AND D. P. SNIDAL (From The Department of Physiology and Medical Research, the University of Manitoba, and
THE EFFECT OF OBSTRUCTION TO BREATHING ON THE VENTILATORY RESPONSE TO Co21 By R. M. CHERNIACK2 AND D. P. SNIDAL (From The Department of Physiology and Medical Research, the University of Manitoba, and
TESTS IN CLINICAL MEDICINE
 274 THE PLACE OF RESPIRATORY FUNCTION TESTS IN CLINICAL MEDICINE D. V. BATES, M.D., M.R.C.P. First Assistant, Mledical Unit, St. Bartholomew's Hospital, London, E.C.i Introduction It is difficult to settle
274 THE PLACE OF RESPIRATORY FUNCTION TESTS IN CLINICAL MEDICINE D. V. BATES, M.D., M.R.C.P. First Assistant, Mledical Unit, St. Bartholomew's Hospital, London, E.C.i Introduction It is difficult to settle
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Multiple bronchiolar stenoses in a patient with
 Thorax (1965), 20, 309. Multiple bronchiolar stenoses in a patient with generalized airways obstruction JOHN R. ESTERLY AND BRIAN E. HEARD From the Postgraduate Medical School of London In a previous article
Thorax (1965), 20, 309. Multiple bronchiolar stenoses in a patient with generalized airways obstruction JOHN R. ESTERLY AND BRIAN E. HEARD From the Postgraduate Medical School of London In a previous article
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ]
![The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ] The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ]](/thumbs/77/74805557.jpg) The role of Pulmonary function Testing In Interstitial lung disease in infants [ ipft in child ] Introduction Managing infants with diffuse lung disease (DLD) suspected to have interstitial lung disease
The role of Pulmonary function Testing In Interstitial lung disease in infants [ ipft in child ] Introduction Managing infants with diffuse lung disease (DLD) suspected to have interstitial lung disease
Surgical treatment of bullous lung disease
 Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Variation in airways resistance when defined over different ranges of airflows
 Thorax, 1978, 33, 401-405 Variation in airways resistance when defined over different ranges of airflows P. W. LORD AND J. M. EDWARDS From the MRC Toxicology Unit, Clinical Section, St. Bartholomew's Hlospital
Thorax, 1978, 33, 401-405 Variation in airways resistance when defined over different ranges of airflows P. W. LORD AND J. M. EDWARDS From the MRC Toxicology Unit, Clinical Section, St. Bartholomew's Hlospital
Respiratory gas exchange in patients with
 Respiratory gas exchange in patients with spontaneous pneumothorax R. M. NORRIS', J. G. JONES, AND J. M. BISHOP Thorax (1968), 23, 427. From the Department of Medicine, University of Birmingham, Queen
Respiratory gas exchange in patients with spontaneous pneumothorax R. M. NORRIS', J. G. JONES, AND J. M. BISHOP Thorax (1968), 23, 427. From the Department of Medicine, University of Birmingham, Queen
Prognosis of cryptogenic fibrosing alveolitis
 P TUKIAINEN, E TASKINEN, P HOLSTI, 0 KORHOLA, AND M VALLE Thorax 1983;38:349-355 From the Departments of Pulmonary Diseases, Oncology, and Diagnostic Radiology, University Central Hospital ofhelsinki,
P TUKIAINEN, E TASKINEN, P HOLSTI, 0 KORHOLA, AND M VALLE Thorax 1983;38:349-355 From the Departments of Pulmonary Diseases, Oncology, and Diagnostic Radiology, University Central Hospital ofhelsinki,
FEVI before (5% predicted) 62 (49-77) 59 (44-77) FEV, after (% predicted) 92 (84-108) 89 (69-107) to the entire group received aerosol isoprenaline.
 Tl.orax, 1980, 35, 298-302 Lung elastic recoil and reduced airflow in clinically stable asthma D S McCARTHY AND M SIGURDSON From the Department of Medicine, University ofmanitoba, Respiratory Division,
Tl.orax, 1980, 35, 298-302 Lung elastic recoil and reduced airflow in clinically stable asthma D S McCARTHY AND M SIGURDSON From the Department of Medicine, University ofmanitoba, Respiratory Division,
Spirometry. Obstruction. By Helen Grim M.S. RRT. loop will have concave appearance. Flows decreased consistent with degree of obstruction.
 1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
THE RELATION BETWEEN LEFT ATRIAL HYPERTENSION
 Thorax (1960), 15, 54. THE RELATION BETWEEN LEFT ATRIAL HYPERTENSION AND LYMPHATIC DISTENSION IN LUNG BIOPSIES BY DONALD HEATH AND PETER HICKEN From the Department of Pathology, University of Birmingham
Thorax (1960), 15, 54. THE RELATION BETWEEN LEFT ATRIAL HYPERTENSION AND LYMPHATIC DISTENSION IN LUNG BIOPSIES BY DONALD HEATH AND PETER HICKEN From the Department of Pathology, University of Birmingham
RESPIRATORY FUNCTION IN EMPHYSEMA IN RELATION TO PROGNOSIS 1
 137 616.4-007.63-037 RESPIRATORY FUNCTION IN EMPHYSEMA IN RELATION TO PROGNOSIS 1 BY D. V. BATES, J. M. S. KNOTT, AND R. V. CHRISTIE (From the Professorial Medical Unit, St. Bartholomew's Hospital, London)
137 616.4-007.63-037 RESPIRATORY FUNCTION IN EMPHYSEMA IN RELATION TO PROGNOSIS 1 BY D. V. BATES, J. M. S. KNOTT, AND R. V. CHRISTIE (From the Professorial Medical Unit, St. Bartholomew's Hospital, London)
health and disease, and between one subject and another, have frequently been
 76 J. Physiol. (949) IIO, 76-82 6I2.24 VARIABILITY OF THE VITAL CAPACITY OF THE NORMAL HUMAN SUBJECT BY J. N. MILLS Fellow of Jesus College, Cambridge From the Department of Physiology, University of Cambridge
76 J. Physiol. (949) IIO, 76-82 6I2.24 VARIABILITY OF THE VITAL CAPACITY OF THE NORMAL HUMAN SUBJECT BY J. N. MILLS Fellow of Jesus College, Cambridge From the Department of Physiology, University of Cambridge
Evaluation of two techniques for measurement of respiratory resistance by forced oscillation A study in young subjects with obstructive lung disease
 Thorax (1973), 28, 136. Evaluation of two techniques for measurement of respiratory resistance by forced oscillation study in young subjects with obstructive lung disease L. I. LNDU and P. D. PHELN Clinical
Thorax (1973), 28, 136. Evaluation of two techniques for measurement of respiratory resistance by forced oscillation study in young subjects with obstructive lung disease L. I. LNDU and P. D. PHELN Clinical
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
(RECEIVED FOR PUBLICATION FEBRUARY 6, 1960) 29 subjects followed for three and a half years. nine no evidence of pneumoconiosis; 16 showed the
 Thorax (1960), 15, 244. RESPIRATORY FUNCTION AND PORTABLE OXYGEN THERAPY IN CHRONIC NON-SPECIFIC LUNG DISEASE IN RELATION TO PROGNOSIS BY J. E. COTES From the Pneumoconiosis Research Unit of the Medical
Thorax (1960), 15, 244. RESPIRATORY FUNCTION AND PORTABLE OXYGEN THERAPY IN CHRONIC NON-SPECIFIC LUNG DISEASE IN RELATION TO PROGNOSIS BY J. E. COTES From the Pneumoconiosis Research Unit of the Medical
Interpreting pulmonary function tests: Recognize the pattern, and the diagnosis will follow
 REVIEW FEYROUZ AL-ASHKAR, MD Department of General Internal Medicine, The Cleveland Clinic REENA MEHRA, MD Department of Pulmonary and Critical Care Medicine, University Hospitals, Cleveland PETER J. MAZZONE,
REVIEW FEYROUZ AL-ASHKAR, MD Department of General Internal Medicine, The Cleveland Clinic REENA MEHRA, MD Department of Pulmonary and Critical Care Medicine, University Hospitals, Cleveland PETER J. MAZZONE,
Pulmonary involvement in ankylosing spondylitis
 Annals of the Rheumatic Diseases 1986, 45, 736-74 Pulmonary involvement in ankylosing spondylitis NILS FELTELIUS,1 HANS HEDENSTROM,2 GUNNAR HILLERDAL,3 AND ROGER HALLGREN' From the Departments of 'Internal
Annals of the Rheumatic Diseases 1986, 45, 736-74 Pulmonary involvement in ankylosing spondylitis NILS FELTELIUS,1 HANS HEDENSTROM,2 GUNNAR HILLERDAL,3 AND ROGER HALLGREN' From the Departments of 'Internal
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Diaphragm Activity in
 Diaphragm Activity in Obesity Ruy V. LOURENQO From the Department of Medicine, University of Illinois College of Medicine and The Hektoen Institute for Medical Research, Chicago, Illinois 668 A B S T R
Diaphragm Activity in Obesity Ruy V. LOURENQO From the Department of Medicine, University of Illinois College of Medicine and The Hektoen Institute for Medical Research, Chicago, Illinois 668 A B S T R
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
Adverse effect of additional weight on exercise against gravity in patients with chronic obstructive airways disease
 Thorax 1989;44:716-720 Adverse effect of additional weight on exercise against gravity in patients with chronic obstructive airways disease C R SWINBURN, B G COOPER, H MOULD, P A CORRIS, G J GIBSON From
Thorax 1989;44:716-720 Adverse effect of additional weight on exercise against gravity in patients with chronic obstructive airways disease C R SWINBURN, B G COOPER, H MOULD, P A CORRIS, G J GIBSON From
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
ARTERIAL BLOOD GAS MEASUREMENTS IN THE MANAGE- MENT OF PATIENTS WITH CHRONIC BRONCHITIS AND EMPHYSEMA
 Thorax (1957), 12, 236. ARTERIAL BLOOD GAS MEASUREMENTS IN THE MANAGE- MENT OF PATIENTS WITH CHRONIC BRONCHITIS AND EMPHYSEMA BY MARGARET M. PLATTS* AND MAVIS S. GREAVES From the University Department
Thorax (1957), 12, 236. ARTERIAL BLOOD GAS MEASUREMENTS IN THE MANAGE- MENT OF PATIENTS WITH CHRONIC BRONCHITIS AND EMPHYSEMA BY MARGARET M. PLATTS* AND MAVIS S. GREAVES From the University Department
Omar Sami. Mustafa Khader. Yanal Shafaqouj
 8 Omar Sami Mustafa Khader Yanal Shafaqouj Let us retrieve our discussion about the ventilation-perfusion ratio (V/Q). - When (V/Q) is Zero this means that no ventilation is taking place, V is Zero; bronchial
8 Omar Sami Mustafa Khader Yanal Shafaqouj Let us retrieve our discussion about the ventilation-perfusion ratio (V/Q). - When (V/Q) is Zero this means that no ventilation is taking place, V is Zero; bronchial
-SQA-SCOTTISH QUALIFICATIONS AUTHORITY. Hanover House 24 Douglas Street GLASGOW G2 7NQ NATIONAL CERTIFICATE MODULE DESCRIPTOR
 -SQA-SCOTTISH QUALIFICATIONS AUTHORITY Hanover House 24 Douglas Street GLASGOW G2 7NQ NATIONAL CERTIFICATE MODULE DESCRIPTOR -Module Number- 0099111 -Session-1989-90 -Superclass- PB -Title- PRINCIPLES
-SQA-SCOTTISH QUALIFICATIONS AUTHORITY Hanover House 24 Douglas Street GLASGOW G2 7NQ NATIONAL CERTIFICATE MODULE DESCRIPTOR -Module Number- 0099111 -Session-1989-90 -Superclass- PB -Title- PRINCIPLES
FINDINGS IN CHRONIC BRONCHITIS AND EMPHYSEMA,
 Thorax (1961), 16, 56. A COMPARISON OF PHYSIOLOGICAL AND PATHOLOGICAL FINDINGS IN CHRONIC BRONCHITIS AND EMPHYSEMA, WITH SPECIAL REFERENCE TO RESPONSE TO EXERCISE BY G. R. McNAB, W. S. GROVE, AND S. NARIMAN*
Thorax (1961), 16, 56. A COMPARISON OF PHYSIOLOGICAL AND PATHOLOGICAL FINDINGS IN CHRONIC BRONCHITIS AND EMPHYSEMA, WITH SPECIAL REFERENCE TO RESPONSE TO EXERCISE BY G. R. McNAB, W. S. GROVE, AND S. NARIMAN*
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
INTRATHORACIC SARCOIDOSIS
 268 -- INTRATHORACIC SARCOIDOSIS Sarcoidosis is a systemic disease in which the lungs and intrathoracic lymph nodes are frequently involved. Although the clinical features of patients with sarcoidosis
268 -- INTRATHORACIC SARCOIDOSIS Sarcoidosis is a systemic disease in which the lungs and intrathoracic lymph nodes are frequently involved. Although the clinical features of patients with sarcoidosis
Relation between severity of mitral valve disease and results of routine lung function tests in non-smokers
 Thorax 1982;37:751-755 Relation between severity of mitral valve disease and results of routine lung function tests in non-smokers KM RHODES, K EVEMY, S NARIMAN, GJ GIBSON From the Cardiothoracic Centre,
Thorax 1982;37:751-755 Relation between severity of mitral valve disease and results of routine lung function tests in non-smokers KM RHODES, K EVEMY, S NARIMAN, GJ GIBSON From the Cardiothoracic Centre,
COMPREHENSIVE RESPIROMETRY
 INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
Chronic Obstructive Pulmonary Disease
 136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
Variation in lung with normal, quiet breathing. Minimal lung volume (residual volume) at maximum deflation. Total lung capacity at maximum inflation
 r Total lung capacity at maximum inflation Variation in lung with normal, quiet breathing Volume of lungs at end of normal inspiration (average 2,200 ml) Minimal lung volume (residual volume) at maximum
r Total lung capacity at maximum inflation Variation in lung with normal, quiet breathing Volume of lungs at end of normal inspiration (average 2,200 ml) Minimal lung volume (residual volume) at maximum
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Mushroom worker's lung
 Mushroom worker's lung EDWARD JACKSON, K. M. A. WELCH The Royal Hospital, West Street, Sheffield Thorax (1970), 25, 25. Two cases of an acute chest illness occurring in mushroom workers are described.
Mushroom worker's lung EDWARD JACKSON, K. M. A. WELCH The Royal Hospital, West Street, Sheffield Thorax (1970), 25, 25. Two cases of an acute chest illness occurring in mushroom workers are described.
Physiology lab (RS) First : Spirometry. ** Objectives :-
 Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
VENTILATORY FUNCTION IN BRONCHIAL ASTHMA
 Thorax (1952), 7, 66. VENTILATORY FUNCTION IN BRONCHIAL ASTHMA BY W. A. BRISCOE AND G. A. McLEMORE, Jr. From the Postgraduate Medical School of London (RECEIVED FOR PUBLICATION SEPTEMBER 3, 1951) Ventilation
Thorax (1952), 7, 66. VENTILATORY FUNCTION IN BRONCHIAL ASTHMA BY W. A. BRISCOE AND G. A. McLEMORE, Jr. From the Postgraduate Medical School of London (RECEIVED FOR PUBLICATION SEPTEMBER 3, 1951) Ventilation
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Pulmonary sarcoidosis with an alveolar radiographic
 Thorax 1982;37:448-452 Pulmonary sarcoidosis with an alveolar radiographic pattern JP BATTESTI, G SAUMON, D VALEYRE, J AMOUROUX, B PECHNICK, D SANDRON, R GEORGES From the Service de Pneumologie, H6pital
Thorax 1982;37:448-452 Pulmonary sarcoidosis with an alveolar radiographic pattern JP BATTESTI, G SAUMON, D VALEYRE, J AMOUROUX, B PECHNICK, D SANDRON, R GEORGES From the Service de Pneumologie, H6pital
A Primer on Reading Pulmonary Function Tests. Joshua Benditt, M.D.
 A Primer on Reading Pulmonary Function Tests Joshua Benditt, M.D. What Are Pulmonary Function Tests Used For? Pulmonary function testing provides a method for objectively assessing the function of the
A Primer on Reading Pulmonary Function Tests Joshua Benditt, M.D. What Are Pulmonary Function Tests Used For? Pulmonary function testing provides a method for objectively assessing the function of the
PULMONARY FUNCTION TEST(PFT)
 PULMONARY FUNCTION TEST(PFT) Objectives: By the end of the present lab, students should be able to: 1. Record lung volumes and capacities and compare them with those of a typical person of the same gender,
PULMONARY FUNCTION TEST(PFT) Objectives: By the end of the present lab, students should be able to: 1. Record lung volumes and capacities and compare them with those of a typical person of the same gender,
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Describe regional differences in pulmonary blood flow in an upright person. Describe the major functions of the bronchial circulation
 OBJECTIVES Describe regional differences in pulmonary blood flow in an upright person Define zones I, II, and III in the lung, with respect to pulmonary vascular pressure and alveolar pressure Describe
OBJECTIVES Describe regional differences in pulmonary blood flow in an upright person Define zones I, II, and III in the lung, with respect to pulmonary vascular pressure and alveolar pressure Describe
emphysema may result in serious respiratory acidosis, coma, and even death (4, 5). The
 Journal of Clinical Investigation Vol. 41, No. 2, 1962 STUDIES ON THE MECHANISM OF OXYGEN-INDUCED HYPOVENTILATION. AN EXPERIMENTAL APPROACH.* By THOMAS B. BARNETT AND RICHARD M. PETERS (From the Departnments
Journal of Clinical Investigation Vol. 41, No. 2, 1962 STUDIES ON THE MECHANISM OF OXYGEN-INDUCED HYPOVENTILATION. AN EXPERIMENTAL APPROACH.* By THOMAS B. BARNETT AND RICHARD M. PETERS (From the Departnments
Chapter. Diffusion capacity and BMPR2 mutations in pulmonary arterial hypertension
 Chapter 7 Diffusion capacity and BMPR2 mutations in pulmonary arterial hypertension P. Trip B. Girerd H.J. Bogaard F.S. de Man A. Boonstra G. Garcia M. Humbert D. Montani A. Vonk Noordegraaf Eur Respir
Chapter 7 Diffusion capacity and BMPR2 mutations in pulmonary arterial hypertension P. Trip B. Girerd H.J. Bogaard F.S. de Man A. Boonstra G. Garcia M. Humbert D. Montani A. Vonk Noordegraaf Eur Respir
PULMONARY FUNCTION IN DIAPHRAGMATIC PARALYSIS
 Thorax (1962), 17, 213. PULMONARY FUNCTION IN DIAPHRAGMATIC PARALYSIS BY MICHAEL McCREDIE,* FRANK W. LOVEJOY Jr., AND NOLAN L. KALTREIDER From the Cardioplulmonary Laboratory of the Department of Medicine,
Thorax (1962), 17, 213. PULMONARY FUNCTION IN DIAPHRAGMATIC PARALYSIS BY MICHAEL McCREDIE,* FRANK W. LOVEJOY Jr., AND NOLAN L. KALTREIDER From the Cardioplulmonary Laboratory of the Department of Medicine,
Pulmonary Function Testing The Basics of Interpretation
 Pulmonary Function Testing The Basics of Interpretation Jennifer Hale, M.D. Valley Baptist Family Practice Residency Objectives Identify the components of PFTs Describe the indications Develop a stepwise
Pulmonary Function Testing The Basics of Interpretation Jennifer Hale, M.D. Valley Baptist Family Practice Residency Objectives Identify the components of PFTs Describe the indications Develop a stepwise
The Influence of Altered Pulmonarv
 The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
Static and dynamic lung volumes and ventilationperfusion
 Thorax (1971), 26, 591. Static and dynamic lung volumes and ventilationperfusion abnormality in adult asthma J. D. MAYFIELD, P. N. PAEZ, and D. P. NICHOLSON Department of Medicine, Woodlawn Chest Dirision,
Thorax (1971), 26, 591. Static and dynamic lung volumes and ventilationperfusion abnormality in adult asthma J. D. MAYFIELD, P. N. PAEZ, and D. P. NICHOLSON Department of Medicine, Woodlawn Chest Dirision,
PNEUMOTACHOGRAPHIC MEASUREMENT OF
 Thorax (1955), 1, 258. PNEUMOTACHOGRAPHIC MEASUREMENT OF BREATHING CAPACITY BY From the R.A.F. Institute of A viation Medicine, Farnborough (RECEIVED FOR PUBLICATION APRIL 11, 1955) The measurement of
Thorax (1955), 1, 258. PNEUMOTACHOGRAPHIC MEASUREMENT OF BREATHING CAPACITY BY From the R.A.F. Institute of A viation Medicine, Farnborough (RECEIVED FOR PUBLICATION APRIL 11, 1955) The measurement of
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Maximal expiratory flow rates (MEFR) measured. Maximal Inspiratory Flow Rates in Patients With COPD*
 Maximal Inspiratory Flow Rates in Patients With COPD* Dan Stănescu, MD, PhD; Claude Veriter, MA; and Karel P. Van de Woestijne, MD, PhD Objectives: To assess the relevance of maximal inspiratory flow rates
Maximal Inspiratory Flow Rates in Patients With COPD* Dan Stănescu, MD, PhD; Claude Veriter, MA; and Karel P. Van de Woestijne, MD, PhD Objectives: To assess the relevance of maximal inspiratory flow rates
Pulmonary Function Testing
 In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
Chest Deformity, Residual Airways Obstruction and Hyperinflation, and Growth in Children with Asthma
 rchives of Disease in Childhood, 197, 45, 789. Chest Deformity, Residual irways Obstruction and Hyperinflation, and Growth in Children with sthma II: Significance of Chronic Chest Deformity G. L. GILLM*,
rchives of Disease in Childhood, 197, 45, 789. Chest Deformity, Residual irways Obstruction and Hyperinflation, and Growth in Children with sthma II: Significance of Chronic Chest Deformity G. L. GILLM*,
The late stages of pulmonary sarcoidosis
 Postgraduate Medical Journal (August 1970) 46, 530-536. The late stages of pulmonary sarcoidosis J. G. SCADDING The Brompton Hospital, London, S. W.3 Summary Pulmonary sarcoidosis is frequently preceded
Postgraduate Medical Journal (August 1970) 46, 530-536. The late stages of pulmonary sarcoidosis J. G. SCADDING The Brompton Hospital, London, S. W.3 Summary Pulmonary sarcoidosis is frequently preceded
Distribution of ventilation and frequency-dependence
 Thorax (1971), 26, 721. Distribution of ventilation and frequencydependence of dynamic lung compliance S. T. CHIANG Pulmonary Laboratory, Department of Medicine, National Defence Medical Centre, Taipei,
Thorax (1971), 26, 721. Distribution of ventilation and frequencydependence of dynamic lung compliance S. T. CHIANG Pulmonary Laboratory, Department of Medicine, National Defence Medical Centre, Taipei,
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
