Psychosis prediction: 12-month follow up of a high-risk ( prodromal ) group
|
|
|
- Theodora Sharp
- 5 years ago
- Views:
Transcription
1 Schizophrenia Research 60 (2003) Psychosis prediction: 12-month follow up of a high-risk ( prodromal ) group Alison R. Yung a,b, Lisa J. Phillips a,b, Hok Pan Yuen a, Shona M. Francey a,b, Colleen A. McFarlane b,1, Mats Hallgren b,2, Patrick D. McGorry a,c, * a Department of Psychiatry, University of Melbourne, Parkville, Victoria, Australia b PACE Clinic, Parkville, Victoria, Australia c Youth Program, Mental Health Services for Kids and Youth (MHSKY), Locked Bag 10, Parkville, Victoria 3052, Australia Received 20 May 2001; accepted 9 January 2002 Abstract Intervention in the prodromal phase of schizophrenia and related psychoses may result in attenuation, delay or even prevention of the onset of psychosis in some individuals. However, a prodrome is difficult to recognise prospectively because of its nonspecific symptoms. This study set out to recruit and follow up subjects at high risk of transition to psychosis with the aim of examining the predictive power for psychosis onset of certain mental state and illness variables. Symptomatic individuals with either a family history of psychotic disorder, schizotypal personality disorder, subthreshold psychotic symptoms or brief transient psychotic symptoms were assessed and followed up monthly for 12 months or until psychosis onset. Twenty of 49 subjects (40.8%) developed a psychotic disorder within 12 months. Some highly significant predictors of psychosis were found: long duration of prodromal symptoms, poor functioning at intake, low-grade psychotic symptoms, depression and disorganization. Combining some predictive variables yielded a strategy for psychosis prediction with good sensitivity (86%), specificity (91%) positive predictive value (80%) and negative predictive value (94%) within 6 months. This study illustrates that it is possible to recruit and follow up individuals at ultra high risk of developing psychosis within a relatively brief follow-up period. Despite low numbers some highly significant predictors of psychosis were found. The findings support the development of more specific preventive strategies targeting the prodromal phase for some individuals at ultra high risk of schizophrenia. D 2002 Elsevier Science B.V. All rights reserved. Keywords: Psychosis; Schizophrenia; Prevention; Prediction; High risk; Prodrome * Corresponding author. Youth Program, Mental Health Services for Kids and Youth (MHSKY), Locked Bag 10, Parkville, Victoria 3052, Australia. Tel.: ; fax: address: mcgorry@ariel.unimelb.edu.au (P.D. McGorry). 1 From 1994 to 1995: Department of Psychiatry, University of Melbourne, Parkville, Victoria, Australia. 2 From 1997 to 1999: Department of Psychiatry, University of Melbourne, Parkville, Victoria, Australia. 1. Introduction Schizophrenia and other psychotic disorders are usually characterized by a prepsychotic or prodromal phase of illness in which a change from premorbid functioning occurs. This period is characterized by various mental state features, including nonspecific symptoms such as depressed mood and anxiety as well as subthreshold or attenuated psychotic symptoms /02/$ - see front matter D 2002 Elsevier Science B.V. All rights reserved. PII: S (02)
2 22 A.R. Yung et al. / Schizophrenia Research 60 (2003) (Yung et al., 1996). Subtle subjectively experienced cognitive, vegetative and perceptual disturbances, called basic symptoms, have also been described (Gross, 1989, 1997). The prodrome extends from a stable or premorbid phase until the time of onset of frank psychotic features (Keith and Matthews, 1991; Loebel et al., 1992; Beiser et al., 1993). It may be lengthy, lasting on average between 1 and 5 years (Loebel et al., 1992; Beiser et al., 1993; Häfner et al., 1993), and is often associated with substantial levels of psychosocial impairment and disability (Jones et al., 1993; Yung et al., 1996). The mechanism by which this prodromal state evolves into psychosis is not really understood (Hodges et al., 1999). One important aspect of the prodrome is that it is a period in which early intervention could occur if it could be recognized prospectively. The possibility of preventing, delaying or ameliorating the onset of diagnosable psychotic disorder then arises (McGorry, 1998). Such intervention in a subthreshold syndrome, aiming to prevent the full-blown disorder from developing, is known as indicated prevention (Mrazek and Haggarty, 1994). So far, however, the diverse range of symptoms and signs manifest in a psychotic prodrome has only limited predictive power in relation to subsequent psychosis, (McGorry, 1998). This cluster of symptoms may well be followed by psychosis (a true positive), or may not (a false positive). The retrospective term prodrome therefore cannot appropriately be applied to prospective investigations. The term at risk mental state (ARMS) has been suggested instead, implying that a subthreshold syndrome can be regarded as a risk factor for subsequent psychosis, but that psychosis is not inevitable (McGorry and Singh, 1995). Indicated prevention will need to be based upon the delineation of ARMS features with increased sensitivity and specificity for subsequent psychosis. Researchers in Germany have made some inroads into this search. They assessed a cohort of patients presenting with personality and neurotic disorders for presence of basic symptoms and then followed them up several years later. After an average follow-up period of 8 years, over 50% of the cohort had developed schizophrenia. Presence of certain basic symptoms (subjective disturbances of attention, thinking, perception, speech and motor action) was found to be highly predictive of psychosis (Klosterkötter et al., 1997, 2001). This paper describes an alternative method of investigating the predictive power of some prodromal features. It builds on previous interim reports from the same sample (Yung et al., 1998a,b) Aim The aim of the project was to recruit and follow up putatively prodromal or ultra-high-risk (UHR) subjects, to determine the number of subjects who became psychotic within a year of study entry and to assess the predictive power of certain variables, including markers of psychopathology and disability Hypothesis It was hypothesized that the rate of transition to psychosis over 12 months would be 20 30% of cases. This estimate was based on our experience during a pilot study in a similar high-risk group in which the 12-month transition rate was 21.2% (7 of 33 cases: Yung et al., 1996). The pilot study inclusion criteria were modified for the current project in an attempt to increase the proportion of cases developing a psychosis, for example by including only first-degree relatives of psychotic patients (the pilot study also allowed the recruitment of second degree relatives). Such criteria already define a sample with massively increased risk of incidence when compared with the general population (greater than 10,000 times the risk: Jablensky, 2000). It was also hypothesized that subjects who became psychotic would display higher levels of certain dimensions of psychopathology and other clinical features than those who did not develop psychosis. These features could then be utilised in enhancing the predictive power within the already enriched sample. 2. Method 2.1. Setting: the PACE Clinic The Personal Assessment and Crisis Evaluation (PACE) Clinic was the deliberately generic name given to the outpatient clinical service specifically developed to assess, manage and follow up putatively high-risk subjects. PACE is located at a community
3 A.R. Yung et al. / Schizophrenia Research 60 (2003) adolescent service for general medical as well as psychological problems. Its location was intended to promote access and avoid stigma. The rationale, development and the clinical infrastructure of this service have been described previously (Yung et al., 1995, 1996). Subjects received supportive counselling and case management in addition to treatment of target symptoms such as depression. Participants in this project may have received antidepressant or anxiolytic medication but no neuroleptic medication was used Sample The lack of specificity of many ARMS symptoms means that additional risk factors need to be identified in order to enhance the predictive power. Such an approach is called a close in strategy (Bell et al., 1982), and for example could involve adding presence of a family history of psychosis (a known risk factor: Gottesman and Shields, 1982) to presence of an ARMS to improve predictive capacity. Alternatively, symptoms that seem to have some specificity for subsequent psychosis could be added to the nonspecific symptoms. These include subthreshold or attenuated forms of frank psychotic features (Cameron, 1938; Chapman, 1966; Strauss, 1969; Chapman and Chapman, 1980; Allen et al., 1987; van Os et al., 2000) and brief, transient episodes of psychotic symptoms, which spontaneously resolve (Faegerman, 1963; Allen et al., 1987; Jauch and Carpenter, 1988). We used these strategies to operationally define three groups thought to be at very high risk of developing a psychotic disorder in the near future ( prodromal ) or ultra high risk (UHR). Group 1: Attenuated Psychotic Symptoms defines a group of people who have symptoms that deviate from normal phenomena but which are not yet frankly psychotic. For example, overvalued ideas that people are laughing at or are hostile towards the subject, but the subject realises that it is not really true and that he or she is just being a bit paranoid. A strange feeling that something has changed in the world or with one s self in the absence of any crystallised delusion is another example. Also included in this group were people who had perceptual disturbances of below psychotic intensity such as visual or auditory distortions. Thus, the difference between these phenomena and frank psychotic symptoms is in the degree or intensity of the symptom. These types of phenomena, which can be seen as subthreshold psychotic symptoms, have been described in retrospective studies of emerging first episode psychosis or psychotic relapse (Yung and McGorry, 1996a,b; Yung et al., 1996; Møller and Husby, 2000). Group 2: Brief Limited Intermittent Psychotic Symptoms (BLIPS) defines a group who have symptoms of psychotic intensity but which are very infrequent, or which have a total duration of less than 7 days before resolving spontaneously. For example, a person with auditory hallucinations that occur twice a month for 6 months (psychotic phenomena infrequent but have been occurring for a long time), or auditory hallucinations that have been occurring every second day for 6 days before resolving spontaneously (psychotic phenomena frequent but present for only a short duration) would meet this intake criterion. Group 3: Trait and State Risk Factors defines a group who have nonspecific symptoms such as lowered mood or anxiety symptoms plus some trait-risk factors for psychotic disorder, either a schizotypal personality disorder or a family history of a psychotic disorder in a first-degree relative. The nonspecific symptoms must have a duration of at least 1 month and be associated with marked disability or decrease in functioning. This severity criterion is necessary to exclude otherwise normal relatives of patients with psychotic illnesses who have a brief period of mild symptoms. The operationalised criteria for each of these groups are described in Table 1. Additionally, all subjects were required to be aged between 14 and 30 (the period of maximum risk of becoming psychotic; Häfner et al., 1993). Exclusion criteria were: intellectual disability, lack of fluency in English, presence of known organic brain disorder and history of previous psychotic disorder for longer than 1 week (treated or untreated) Instruments At intake, the Psychotic Disorders section of the Structured Clinical Interview for DSM IV (SCID: First et al., 1996) was administered to all cases to establish that none was psychotic at study entry. The Family Interview for Genetic Studies (FIGS: Max-
4 24 A.R. Yung et al. / Schizophrenia Research 60 (2003) Table 1 Inclusion and acute psychosis criteria Group 1: Attenuated Psychotic Symptoms Presence of at least one of the following symptoms ideas of reference, odd beliefs or magical thinking, perceptual disturbance, paranoid ideation, odd thinking and speech, odd behaviour and appearance (2 3 on Unusual Thought Content scale; 1 2 on Hallucinations scale; 2 3 on Suspiciousness scale or 1 3 on Conceptual Disorganisation scale of BPRS: McGorry et al., 1988). Held with a reasonable degree of conviction, as defined by a score of 2 on the Comprehensive Assessment of Symptoms and History (CASH) rating scale for delusions (Andreasen et al., 1992). Frequency of symptoms at least several times per week. Change in mental state present for at least 1 week and not longer than 5 years. Group 2: Brief Limited Intermittent Psychotic Symptoms ( BLIPS ) Transient psychotic symptoms Presence of at least one of the following: ideas of reference, magical thinking, perceptual disturbance, paranoid ideation, odd thinking and speech [4+ on Unusual Thought Content scale; 3+ on Hallucinations scale; 4+ on Suspiciousness scale (or it is held strong conviction, as defined by a score of 3 or more on the CASH rating scale for delusions) or 4+ on Conceptual Disorganisation scale of BPRS]. Duration of episode of less than 1 week. Symptoms resolve spontaneously. The BLIP must have occurred within the past year. Group 3: Trait and State Risk Factors First degree relative with a DSM-IV psychotic disorder or schizotypal personality disorder (as defined by DSM-IV). Significant decrease in mental state or functioning maintained for at least a month and not longer than 5 years (reduction in GAF Scale of 30 points from premorbid level). The decrease in functioning occurred within the past year. Acute psychosis threshold Presence of at least one of the following: ideas of reference, magical thinking, perceptual disturbance, paranoid ideation, odd thinking and speech [4+ on Unusual Thought Content scale; 3+ on Hallucinations scale; 4+ on Suspiciousness scale (or it is held strong conviction, as defined by a score of 3 or more on the CASH rating scale for delusions) or 4+ on Conceptual Disorganisation scale of BPRS]. Frequency of symptoms is at least several times a week. Duration of mental state change is longer than 1 week. well, unpublished) was used to document family history of psychotic disorders. An interview was performed to assess the duration of symptoms and decline in functioning. The Quality of Life Scale (QLS: Heinrichs et al., 1984) and Global Assessment of Functioning (GAF: APA, 1994) were used for each subject at intake and at 12 months to assess functioning and disability. Subjects were assessed at intake and at monthly intervals on measures of psychopathology in order to monitor the development of psychotic features and other symptoms that could be precursor features of psychotic disorders, such as mood and anxiety symptoms. A modified 24-item version of the Brief Psychiatric Rating Scale (BPRS) was used (Mc- Gorry et al., 1988) rating items 0 6. Other scales were: the Scale for the Assessment of Negative Symptoms (SANS: Andreasen, 1982), Hamilton Rating Scale for Depression (HRSD: Hamilton, 1960), Hamilton Rating Scale for Anxiety (HRSA: Hamilton, 1959), and a mania rating scale (MRS: Young et al., 1978). A full SCID was done on subjects after the development of psychosis to determine the DSM IV diagnosis. Subjects who did not become psychotic within 12 months had a SCID completed at 12- month follow up to detect any other psychiatric disorders Data analysis SPSS for Windows (SPSS, 1998) and S-PLUS for Windows (MathSoft, 1997) were used to perform the analysis. For categorical variables, such as gender, the chi-square or Fisher s exact test were used to assess if different categories of a variable differ in terms of the proportion of subjects becoming psychotic within 1 year. For numerical variables, such as GAF, the t-test was used to compare mean scores of those who became psychotic within 1 year and those who did not. The Cox proportional hazards regression model was also applied to each variable to test for the association between a particular variable and the risk of psychosis. The Cox model is widely used for survival data. It takes into account the time to psychosis and can accommodate time-dependent variables such as BPRS for which repeated measures were collected over time. The calculation of measures such as sensitivity and specificity are an attempt to provide a practically oriented interpretation of the results.
5 A.R. Yung et al. / Schizophrenia Research 60 (2003) Results 3.1. Referrals Between March 1995 to October 1996, 162 referrals were made to PACE. Telephone screening assessment of these referrals excluded 23 (14.2%), the remaining 139 (85.8%) were offered a screening interview at the PACE Clinic. Forty-four of these never attended the appointment. The reasons for this are unknown. The other 95 (58.6% of the 162 referred) were seen in the clinic by either the PACE consultant psychiatrist (ARY,3 ) or a research psychologist (CAM, LJP, and MH,4 ) or both. Of these, 60 met the intake criteria and 35 did not and forty-five of those meeting intake criteria consented to involvement in the research project. Reasons for not being recruited included refusal to participate (n=13), and being subsequently treated with neuroleptic medication by another clinician (despite not being psychotic: n=2). Additionally, four subjects who had been seen at PACE in the months prior to March 1995 were recruited into the study. They had been included in the pilot project but still met PACE inclusion criteria at the commencement of this project. Thus, the total number in the research sample was 49. All subjects included in the study were assessed by at least two experienced clinicians prior to study entry. In all cases, a psychiatrist was either directly involved in the assessment or the case was discussed in detail with a psychiatrist prior to being formally accepted into the clinic. Subjects were frequently reviewed at a consensus meeting by all clinicians. On one occasion, a person originally included in the study revealed more symptoms to his clinician some time after being first involved in the research. This led the team to suspect that he had actually been psychotic at the time of entry into the study. He was subsequently completely withdrawn from the study and appropriate treatment was commenced. We are confident that no other subject was psychotic at the time of entry into the study. However, eight individuals defined by our criteria as having BLIPS met 3 Alison Yung. 4 Colleen McFarlene, Lisa Phillips, Mats Hallgren. Fig. 1. Intake criteria, number and number with transition to psychosis in brackets. DSM IV criteria for a past Brief Psychotic Disorder (four subjects) or Substance Induced Psychosis (four subjects). These diagnoses can be made with a duration of psychotic symptoms as brief as 1 day. In all cases, duration of frank psychosis was less than 1 week, and resolution of symptoms was spontaneous. As indicated below, the threshold for onset of a psychotic episode was aligned with the consensus between PACE psychiatrists of when neuroleptic treatment would usually be commenced. A separate study (n=21) was conducted to assess the inter-rater reliability of clinicians and research staff in relation to assessing whether potential subjects met intake or exit criteria for the study. Written case summaries including detailed description of symptomatology, frequency, duration and recency of symptoms were presented to five staff members who then rated whether potential subjects met intake or exit criteria. The pairwise kappa values for entry criteria ( ) and exit criteria ( ) were excellent, indicating that all raters were consistent when evaluating intake and exit criteria Intake criteria Most subjects met the attenuated intake criterion (n=35: 71.4%). Twelve cases (24.5%) met the BLIP criterion and 18 cases (36.7%) met the trait marker criterion. There was a considerable degree of overlap between the groups. Six cases (12.2%) fulfilled both the trait criterion and the attenuated criterion, four (8.1%) subjects met both attenuated and BLIP criteria and two (4.1%) met both trait and BLIP
6 26 A.R. Yung et al. / Schizophrenia Research 60 (2003) criteria. Two subjects (4.1%) fulfilled all three criteria. Fig. 1 illustrates this Intake characteristics Mean age at first assessment was 19.1 years (median 19, SD=3.8, range 14 28). Twenty-five of the subjects were male (51.0%) and 24 were female (49.0%). The 15 who met criteria but did not consent to involvement in the study did not differ significantly from the research sample in terms of age (mean 18.5 years, median 18, SD=2.6, range 14 24: p=0.48) or gender [seven (46.7%) male, eight (53.3%) female: p=1.00]. The time between symptom onset and first contact with psychiatric services in the pathway to the PACE Clinic varied widely between subjects, with a range of 0 to 4015 days (11 years), median 183 days. Time to being seen at the PACE Clinic was similarly variable (range 3 to 7286 days, median 495 days) (see Table 2). Measures of functioning and symptomatology at intake are shown in Table 2. A mean GAF score of 58.1 indicates moderate difficulty in social and role functioning or moderate psychiatric symptoms. The mean QLS score of 77.1 is also consistent with moderate disability. The intake BPRS and SANS scores indicate moderate to high levels of symptomatology Transition to psychosis The main outcome measure in this study was the development of psychosis. This onset point needed to Table 2 Intake data Mean SD Median Range Age (years) GAF QLS BPRS SANS Duration of sys (days) Duration to PACE (days) GAF=Global Assessment of Functioning; QLS=Quality of Life Scale; BPRS=Brief Psychiatric Rating Scale; SANS=Schedule for Assessment of Negative Symptoms; Duration of sys=time between onset of symptoms and first contact with psychiatric services in the pathway to the PACE Clinic; Duration to PACE=time between onset of symptoms and first contact with the PACE Clinic. Fig. 2. Survival curve for the whole sample. be arbitrarily defined using the BPRS to determine a cut-off point at which psychosis is said to have begun (see Table 1). As is the case with any operational definition, there is inherent error in this approach. However, as we have discussed previously, there are difficulties in defining onset of a frank psychosis prospectively (Yung and McGorry, 1996a,b). This threshold, which excludes cases of brief psychosis (according to the DSM-IV), is essentially the threshold at which neuroleptic medication would be commenced in common clinical practice and was developed via local consensus of PACE and Early Psychosis Prevention and Intervention Centre (EPPIC, Melbourne, Australia: McGorry et al., 1996) psychiatrists. Over the 12-month follow-up period, 20 subjects became psychotic according to the above definition. Therefore, the 12-month transition rate was 40.8% (20 of 49). Additionally, we have become aware of two further cases who developed psychosis after 12 months, at 15 and 25 months. However, the whole sample has not yet been followed up over a longer period and there may be further cases still with psychosis onset after the 12-month point. Fig. 2 shows a survival curve indicating the timing of onset of psychosis. The steepness of the curve in Fig. 2 indicates that the period of highest risk of developing psychosis was within about 4.5 months of study entry. Of the 20 cases who became psychotic within 1 year, 14 (70%) made the transition within this period. However, subjects continued to be at risk over the whole 12-month study period (and beyond). For those who became
7 A.R. Yung et al. / Schizophrenia Research 60 (2003) psychotic within 1 year, the mean number of days to psychosis was 123 days (SD=107), with median of 103 days, range days. Table 3 shows the 12-month SCID diagnoses (current diagnosis only). Thirteen subjects had an onset of schizophrenia, three cases had affective psychoses (one bipolar disorder, two major depression with psychotic features). One case developed schizoaffective disorder (depressed type) and one had a brief psychosis with duration greater than 1 week. There were two cases of psychotic disorder not otherwise specified (NOS). Of the remaining 29 nonpsychotic subjects, 12 had no current diagnosis at 12 months and 15 had other nonpsychotic diagnoses (mainly mood and anxiety disorders). Final diagnosis was missing for two subjects Prediction of psychosis Baseline measures Comparison was made between the subjects who became psychotic and those who did not become psychotic over the 12-month follow-up period in order to assess predictive utility of some of the independent variables. Age and gender were not significantly related to the onset of psychosis. The time between the onset of symptoms and first contact with psychiatric services was significantly longer in the group that became psychotic (mean=915 days, SD=1134) compared with the group that did not (mean=324, SD=347: t-test, p=0.035). The association was even more significant using Cox regression ( p=0.0061). Table 3 Diagnoses at 12-month follow up Diagnosis N Percentage Psychotic Schizophrenia Schizoaffective Bipolar disorder with psychotic features Major depression with psychotic features Brief psychotic disorder Psychotic disorder NOS Nonpsychotic No diagnosis Other nonpsychotic diagnosis Missing Level of functioning as assessed by the GAF was significantly lower at baseline in the group that became psychotic (mean=52.7, SD=14.2) compared with the group that did not (mean=61.8, SD=13.5: t-test, p=0.029). Using Cox regression p= Repeated measures As the pattern of symptoms experienced by putatively prodromal individuals are likely to vary over time, ratings of psychopathology were completed at monthly periods over a course of a year. These repeated measures were analysed using survival analysis and Cox regression to identify factors that make the development of psychosis more likely. If a subject were nonpsychotic at 2 months, the measures of psychopathology at 1 month were treated as those for someone who was not psychotic. If the same person then became psychotic at 10.5 months, then the psychopathological measures immediately preceding the transition (i.e. 10 months) were treated as for someone with psychosis (the measures at 1 month would still be analysed as if for someone without psychosis). We needed to determine how long the psychopathological measures were assumed to be valid, given that they are likely to change over time (we called this time period the duration of validity). Ideally, this would have been 30 days in line with the monthly follow-up design. A number of subjects were missing one or more monthly assessments, or assessment occurred late, however, so a valid limit of only 30 days would have resulted in the loss of important information. If the subject described above had missed assessments at both 9 and 10 months, then the length of time between last assessment and psychosis onset is about 75 days. Hence, if a duration of validity of 60 days were used, then we would not be able to include this subject in the analysis (as the length of time between last assessment and psychosis onset is over 60 days). However, this subject would be included using a duration of validity of 130 days. In order to assess the effects of different values for the duration of validity, Cox regression was applied with duration of validity ranging from 60 to 390 days. The p-values associated with total BPRS score, BPRS psychotic subscales (unusual thought content, suspiciousness, hallucinations, conceptual disorganization), total SANS score, SANS subscales, HRSD, HRSA and MRS scores using Cox regression are shown in
8 28 A.R. Yung et al. / Schizophrenia Research 60 (2003) Table 4. For the sake of simplicity, only the p-values and hazard ratios for duration of validity of 60 and 130 days are shown. Scores on BPRS total, BPRS psychotic subscales, SANS attention and HRSD were consistently highly significant predictors, even with different durations of validity Measures of predictive ability Using only the consistently highly significant predictors ( p<0.01 based on Cox regression across all durations of validity tested): time between the onset of symptoms and first contact with psychiatric services ( duration ), GAF score, BPRS total, BPRS psychotic subscale score, SANS attention and HRSD scores, we then examined how well these variables together predict onset of psychosis. For each variable, a cutoff point was used to define a positive result. This was achieved by establishing which point gave the lowest p-value using Cox regression. Using this method, the following cut off points were found: duration of symptoms greater than 900 days, GAF score less than 51, BPRS total greater than 15, BPRS psychotic subscale greater than 2, SANS attention score greater than 1 and HRSD greater than 18. These features were then considered as potential predictors of psychosis. Next, an examination was made of how many of these features were needed to most accurately distinguish between those likely to develop psychosis and those likely to remain nonpsychotic. The risk of developing psychosis associated with having 2 or more, 3 or more, 4 or more and 5 or more Table 4 Results of Cox regression ( p-values) for duration of validity of 60 and 130 days 60 days 130 days p-value Hazard ratio p-value Hazard ratio BPRS total BPRS Psych subscales SANS total SANS affective flattening SANS alogia SANS avolition apathy SANS anhedonia asociality SANS attention HRSD HRSA Mania Scale total > Table 5 Number of subjects becoming psychotic within limited time periods using a score of 4 or more potential predictors of psychosis as a positive test Outcome At 90 days At 180 days At 270 days At 360 days NP P NP P NP P NP P Number of V predictors 4or more NP=not psychotic; P=psychotic. potential predictors of psychosis was examined using Cox regression. The smallest p-value ( ) corresponded to having 4 or more potential predictors (and a duration of validity of 130 days for the repeated measures). In order to gain an idea of the predictive ability of this 4 or more prediction rule, each subject was classified as positive or negative according to whether or not his/her baseline measurements of the potential predictors satisfied this rule. This classification was then compared with the actual outcome within 90, 180, 270 and 360 days from entry. Results are shown in Tables 5 and 6. Note that conceptually, the prediction rule could also be applied to measurements at the follow-up time points. However, this was not done because of the reduction in sample size at these time points due to subjects missing assessments or becoming psychotic. As can be seen from the tables, the PPV suggests that the majority (13 of 15 subjects or 80%) of those with 4 or more potential predictors of psychosis at baseline will become psychotic within 6 months. The hazard ratio of having 4 or more of these features is estimated to be 30 [95% CI (8110), using Cox regression]. Although the estimate lacks precision, both the Table 6 Sensitivity, specificity, PPV and NPV of having 4 or more potential predictors of psychosis at baseline Sensitivity Specificity PPV NPV 90 days days days days PPV=positive predictive value; NPV=negative predictive value.
9 A.R. Yung et al. / Schizophrenia Research 60 (2003) value 30 itself and the confidence interval are way above 1, suggesting that those with 4 or more potential predictors of psychosis are at higher risk of becoming psychotic than those with fewer than four predictors. Subjects with 4 or more potential predictors of psychosis can be considered to have been truly in the prodromal phase of illness when recruited. The above analysis assumed that all factors contribute equally to the risk of psychosis, which may not be the case. To address this problem, the risks associated with different combinations of the potential predictors were estimated using Cox regression. These estimated risks were then utilised in the prediction of psychosis. The results were not changed significantly. 4. Discussion The search for predictors of psychosis is an important area of investigation with implications for early intervention in a subsample of the population at ultra high risk (UHR) of psychosis. This design of this study is unique in that it prospectively investigates symptomatic high-risk individuals in the peak age range of psychosis onset. This was a two-stage process. Subjects who met specific intake criteria were selected (the UHR cohort). Enhanced prediction of psychosis within this enriched sample was then investigated. Monthly assessment allowed close monitoring of change in psychopathology and functioning and accurate determination of timing and pattern of onset of psychosis. The high rate of transition to psychosis in our study group suggests that we are identifying many young people who are in the prodromal phase preceding a first episode of psychosis. The 12-month risk of 40.8% (a vastly increased risk for 12-month incidence in contrast to young people in the general population) may in fact have been higher if the subjects had not attended PACE where they received some treatment. Hence, there may be some false false positives where the genuine risk was averted or postponed at least (Yung and McGorry, 1996a,b), as well as cases who were never at risk of psychosis ( true false positives ). Moderate levels of disability and psychopathology were found in the sample at intake. This is to be expected, as the subjects tended to be help-seekers who were referred to the PACE service by other professionals. Nonetheless, as is the case with first episode psychosis (Johnstone et al., 1986; Vaglum, 1996), there were still long delays in some subjects seeking and/or receiving help (Phillips et al., 1999). This may be because of diagnostic confusion, uncertainty about what help is needed and where to seek it and/or a lack of appropriate services. Unfortunately, for many individuals, this delay in receiving help may result in social decline and increasing levels of disability, and indeed the PACE attendees invariably were distressed and experiencing a significant decline in functioning. Some highly significant predictors of psychosis were found. Long duration of prodromal symptoms before help seeking was one predictor. It may be that subjects with shorter duration of symptoms were earlier in the process of development of psychosis or psychotic disorder than those with longer durations, or perhaps the interventions provided were more effective at an earlier stage of disorder development. Alternatively, the high-risk period soon after study entry could indicate the presence of a referral bias with patients being referred to the PACE Clinic when there is a noticeable worsening of symptoms. Poor functioning at intake was another significant predictor of psychosis transition within 12 months. It can be difficult to distinguish premorbid abnormalities, including developmental deviance, from the onset of prodrome, particularly in an adolescent population though conceptually it is very important to attempt this. Attempts were made to date the onset of prodrome by asking about change from normal self. However, since adolescence is a period of major psychological and social change as well as a time of brain maturation (Davies et al., 1998), the distinction between premorbid personality and prodromal symptoms may not be clear cut. Our sample with very long duration of prodrome may include some subjects with long-standing poor premorbid adjustment, a known risk factor for schizophrenia (Jones et al., 1993), and other psychotic disorders (Done et al., 1994). The finding that poor functioning at intake predicted onset of psychosis may also reflect this. It may also be that, since our criteria are weighted towards recruiting subjects with positive symptoms (attenuated psychotic symptoms and BLIPS), low functioning in combination with these positive symptoms increases risk of psychosis transition.
10 30 A.R. Yung et al. / Schizophrenia Research 60 (2003) Level of psychopathology and particularly low level psychotic-like symptoms (attenuated positive symptoms) as measured by the psychotic subscales of the BPRS, depression, and disorganization (as assessed by the SANS attention variable) were all risk factors for development of psychosis within 60 and 130 days. Avolition/apathy and anxiety were also significantly associated with psychosis within 60 days. Thus, the hypothesis that impending psychosis can be detected prospectively and prediction further enhanced within the UHR group was supported. Further data analysis yielded a strategy for psychosis prediction using a combination of risk factors. Having four or more of the following: duration greater than 900 days, GAF score less than 51, BPRS total greater than 15, BPRS psychotic subscale greater than 2, SANS attention score greater than 1 and HRSD greater than 18, predicted psychosis onset within 6 months with good sensitivity (86%), specificity (91%) PPV (80%) and PPV (94%). This compares favourably to the sensitivity and specificity data reported by Klosterkötter et al. (2001). They reported that the presence of basic symptoms at intake predicted schizophrenia at follow up with a probability of 70% specificity 0.59, false-positive predictions 20%. It should be noted, however, that the length of follow up from recruitment differs between this study and that of Klosterkötter with the current study being much shorter (12 months compared to 8 years). It must be acknowledged that numbers are small and the findings cannot be generalised to the whole population of people in the prodromal phase of a first psychotic episode. Furthermore, these predictors only apply to young people at ultra high risk for psychosis as defined by our intake criteria. Values for sensitivity, specificity, PPV and NPV are affected by prevalence; hence, if our same test were applied to the general population, PPV would be lower and NPV higher due to the low prevalence of psychosis in the general community. However, services similar to the PACE Clinic are in development, and these findings have clinical implications for these and other like services. First, the period of highest risk of transition to psychosis was in the first 4.5 months after study entry. UHR patients should therefore be monitored most closely during this time. Second, young people who meet PACE UHR criteria and four or more of the above markers should be monitored particularly closely for psychosis onset. Meeting the intake criteria alone is associated with a 40% risk of developing a psychotic episode. Refining the UHR sample further considerably increases the risk of psychosis. In the sample of 15 who not only met intake criteria but also four or more of the additional risk factors, 13 (87%) developed psychosis. These subjects were truly experiencing the prodromal phase of a first psychotic episode when initially recruited. Such a high rate of transition to psychosis in this subsample could justify assertive treatment in patients meeting these criteria. The result of this research therefore lays the groundwork for the development of targeted intervention or indicated prevention models (Mrazek and Haggarty, 1994), which aim to minimise the impact of, delay, or even prevent onset of psychotic disorder. Acknowledgements This research was supported by a grant from the Victor Hurley Medical Research Fund and by a Research Program Grant from the Victorian Health Promotion Foundation. Our thanks also to Dr. Lorelle Drew and John Gleeson. References Allen, J.J., Chapman, L.J., Chapman, J.P., Vuchetich, J.P., Frost, L.A., Prediction of psychoticlike symptoms in hypothetically psychosis prone college students. J. Abnorm. Psychol. 96, American Psychiatric Association, Diagnostic and Statistical Manual of Mental Disorders American Psychiatric Association, Washington. Andreasen, N., Negative symptoms in schizophrenia: definition and reality. Arch. Gen. Psychiatry 39, Andreasen, N.C., Flaum, M., Arndt, S., The comprehensive assessment of symptoms and history (CASH): an instrument for assessing diagnosis and psychopathology. Arch. Gen. Psychiatry 49, Beiser, M., Erikson, D., Fleming, J.A.E., Iacono, W.G., Establishing the onset of psychotic illness. Am. J. Psychiatry 150, Bell, R.A., LeRoy, J.B., Stevenson, J.J., Evaluating the mediating effects of social supports upon life events and depressive symptoms. J. Commun. Psychol. 10, Cameron, D.E., Early schizophrenia. Am. J. Psychiatry 95, Chapman, J., The early symptoms of schizophrenia. Br. J. Psychiatry 112,
11 A.R. Yung et al. / Schizophrenia Research 60 (2003) Chapman, L.J., Chapman, J.P., Scales for rating psychotic and psychoticlike experiences as continua. Schizophr. Bull. 6, Davies, N., Russell, A., Jones, P., Murray, R.M., Which characteristics of schizophrenia predate psychosis? J. Psychiatr. Res. 32, Done, D.J., Sacker, A., Crow, T.J., Childhood antecedents of schizophrenia and affective illness: intellectual performance at ages 7 and 11. Schizophr. Res. 11, 96. Faegerman, P., Psychogenic Psychoses Butterworth, London. First, M.B., Spitzer, R.L., Gibbon, M., Williams, J.B.W., Structured clinical interview for DSM-IV Axis I Disorders-Patient Edition (SCID-I/P, Version 2.0). NY State Psychiatric Institute, New York. Gottesman, I.I., Shields, J., Schizophrenia: The Epigenetic Puzzle Cambridge Univ. Press, Cambridge. Gross, G., The basic symptoms of schizophrenia. Br. J. Psychiatry 155 (Suppl. 7), Gross, G., The onset of schizophrenia. Schizophr. Res. 28, Häfner, H., Maurer, K., Loffler, W., Riecher-Rossler, A., The influence of age and sex on the onset and early course of schizophrenia. Br. J. Psychiatry 162, Hamilton, M., The assessment of anxiety states by rating. Br. J. Psychiatry 32, Hamilton, M., A rating scale for depression. J. Neurol., Neurosurg. Psychiatry 23, Heinrichs, D., Hanlon, T., Carpenter, W., The quality of life scale: an instrument for rating the schizophrenia deficit syndrome. Schizophr. Bull. 10, Hodges, A., Byrne, M., Grant, E., Johnstone, E., People at risk of schizophrenia: sample characteristics of the first 100 cases in the Edinburgh high-risk study. Br. J. Psychiatry 174, Jablensky, A., Prevalence and incidence of schizophrenia spectrum disorders: implications for prevention. Aust. N. Z. J. Psychiatry 34, S26 S34 (Supplement). Jauch, D.A., Carpenter, W.T., Reactive psychosis I: does the DSM III concept define a third psychosis? J. Nerv. Ment. Dis. 176, Johnstone, E.C., Crow, T.J., Johnson, A.L., MacMillan, J.F., The Northwick study of first episodes of schizophrenia: I. Presentation of the illness and problems related to admission. Br. J. Psychiatry 148, Jones, P.B., Bebbington, P., Foerster, A., Lewis, S.W., Murray, R.M.,Russell,A.,Sham,P.C.,Toone,B.K.,Wilkins,S., Premorbid social underachievement in schizophrenia: results from the Camberwell Collaborative Psychosis Study. Br. J. Psychiatry 162, Keith, S.J., Matthews, S.M., The diagnosis of schizophrenia: a review of onset and duration issues. Schizophr. Bull. 17, Klosterkötter, J., Schultze-Lutter, F., Gross, G., Huber, G., Steinmeyer, E.M., Early self-experienced neuropsychological deficits and subsequent schizophrenic diseases: an 8-year average follow-up prospective study. Acta Psychiatr. Scand. 95, Klosterkötter, J., Hellmich, M., Steinmeyer, E.M., Schultze-Lutter, F., Diagnosing schizophrenia in the initial prodromal phase. Arch. Gen. Psychiatry 58, Loebel, A.D., Lieberman, J.A., Alvir, J.M., Mayerhoff, D.I., Geisler, S.H., Szymanski, S.R., Duration of psychosis and outcome in first episode schizophrenia. Am. J. Psychiatry 149, MathSoft, S-PLUS for Windows 4.0. Seattle, WA. Maxwell, M.E., unpublished. Manual for the FIGS, Clinical Neurogenetics Branch, Intramural Research Branch, National Institute of Mental Health, USA. McGorry, P.D., A stitch in time... the scope for preventive strategies in early psychosis. Eur. Arch. Psychiatry Clin. Neurosci. 248, McGorry, P.D., Singh, B.S., Schizophrenia: risk and possibility. In: Raphael, B., Burrows, G.D. (Eds.), Handbook of Studies on Preventive Psychiatry, Elsevier, Amsterdam, pp McGorry, P.D., Goodwin, R.J., Stuart, G.W., The development, use and reliability of the Brief Psychiatric Rating Scale (nursing modification) an assessment procedure for the nursing team in clinical and research settings. Comp. Psychiatry 29, McGorry, P.D., Edwards, J., Mihalopolous, C., Harrigan, S.M., Jackson, H.J., EPPIC: an evolving system of early detection and optimal management. Schizophr. Bull. 22, Møller, P., Husby, R., The initial prodrome in schizophrenia: searching for naturalistic core dimensions of experience and behavior. Schizophr. Bull. 26, Mrazek, P.J., Haggarty, R.J., Reducing risks for mental disorders: frontiers for preventive intervention research National Academy Press, Washington, DC. Phillips, L.J., Yung, A.R., Hearn, N., McFarlane, C.A., Hallgren, M., McGorry, P.D., Preventive mental health care: accessing the target population. Aust. N. Z. J. Psychiatry 33, SPSS, SPSS for Windows 8.0. Chicago, IL. Strauss, J.S., Hallucinations and delusions as points on continua function. Arch. Gen. Psychiatry 21, Vaglum, P., Earlier detection and intervention in schizophrenia: unsolved questions. Schizophr. Bull. 22, van Os, J., Hanssen, M., Bijl, R.V., Ravelli, A., Strauss (1969) revisited: a psychosis continuum in the general population? Schizophr. Res. 45, Young, R.C., Biggs, J.T., Ziegler, V.E., Meyer, D.A., A rating scale for mania: reliability, validity and sensitivity. Br. J. Psychiatry 133, Yung, A.R., McGorry, P.D., 1996a. The initial prodrome in psychosis: descriptive and qualitative aspects. Aust. N. Z. J. Psychiatry 30, Yung, A.R., McGorry, P.D., 1996b. The prodromal phase of firstepisode psychosis: past and current conceptualizations. Schizophr. Bull. 22, Yung, A.R., McGorry, P.D., McFarlane, C.A., Patton, G.C., The PACE Clinic: development of a clinical service for young people at high risk of psychosis. Aust. Psychiatry 3, Yung, A.R., McGorry, P.D., McFarlane, C.A., Jackson, H.J., Patton,
12 32 A.R. Yung et al. / Schizophrenia Research 60 (2003) G.C., Rakkar, A., Monitoring and care of young people at incipient risk of psychosis. Schizophr. Bull. 22, Yung, A.R., Phillips, L.J., McGorry, P.D., Hallgren, M.A., McFarlane, C.A., Jackson, H.J., Francey, S., Patton, G.C., 1998a. Can we predict onset of first episode psychosis in a high risk group? Int. Clin. Psychopharmacol. 13, S23 S30. Yung, A.R., Phillips, L.J., McGorry, P.D., McFarlane, C.A., Francey, S., Patton, G.C., Jackson, H.J., 1998b. The prediction of psychosis: a step towards indicated prevention. Br. J. Psychiatry 172 (Suppl. 33),
Initial Prodrome Description in Recent Onset Schizophrenia
 Amr El-Shribiny et al. Initial Prodrome Description in Recent Onset Schizophrenia Amr M M El-Shribiny, Salwa M. Rabie, Hanaa S. Soliman, Refaat Mahfouz Department of Neurology and Psychiatry, El-Minia
Amr El-Shribiny et al. Initial Prodrome Description in Recent Onset Schizophrenia Amr M M El-Shribiny, Salwa M. Rabie, Hanaa S. Soliman, Refaat Mahfouz Department of Neurology and Psychiatry, El-Minia
BREWER, WOOD, MCGORRY, ET AL. (N=81) (56.7% male) were consecutively admitted to a personal assessment and crisis evaluation clinic. Detailed criteria
 Article Impairment of Olfactory Identification Ability in Individuals at Ultra-High Risk for Psychosis Who Later Develop Schizophrenia Warrick J. Brewer, Ph.D. Stephen J. Wood, Ph.D. Patrick D. McGorry,
Article Impairment of Olfactory Identification Ability in Individuals at Ultra-High Risk for Psychosis Who Later Develop Schizophrenia Warrick J. Brewer, Ph.D. Stephen J. Wood, Ph.D. Patrick D. McGorry,
Distress in relation to attenuated psychotic symptoms in the ultra-high-risk population is not associated with increased risk of psychotic disorder.
 Royal College of Surgeons in Ireland e-publications@rcsi Psychiatry Articles Department of Psychiatry 15-3-2015 Distress in relation to attenuated psychotic symptoms in the ultra-high-risk population is
Royal College of Surgeons in Ireland e-publications@rcsi Psychiatry Articles Department of Psychiatry 15-3-2015 Distress in relation to attenuated psychotic symptoms in the ultra-high-risk population is
4. General overview Definition
 4. General overview 4.1. Definition Schizophrenia is a severe psychotic mental disorder characterized by significant disturbances of mental functioning. It has also been called early dementia, intrapsychic
4. General overview 4.1. Definition Schizophrenia is a severe psychotic mental disorder characterized by significant disturbances of mental functioning. It has also been called early dementia, intrapsychic
Monitoring and Care of Young People at Incipient Risk of Psychosis
 VOL 22, NO. 2, 1996 Monitoring and Care of Young People at Incipient Risk of Psychosis 2 by Alison ft Yung, Patrick D. McGorry, Colleen A. McFarlane, Henry J. Jackson, George C. Patton, and Arun Rakkar
VOL 22, NO. 2, 1996 Monitoring and Care of Young People at Incipient Risk of Psychosis 2 by Alison ft Yung, Patrick D. McGorry, Colleen A. McFarlane, Henry J. Jackson, George C. Patton, and Arun Rakkar
Preventing psychosis and targeting people at risk: From bright idea to NICE Guidelines. Paul French
 Preventing psychosis and targeting people at risk: From bright idea to NICE Guidelines Paul French Psychosis: The Early Course Adapted from Larsen et al., 2001 Early Intervention in the atrisk phase ARMS
Preventing psychosis and targeting people at risk: From bright idea to NICE Guidelines Paul French Psychosis: The Early Course Adapted from Larsen et al., 2001 Early Intervention in the atrisk phase ARMS
Early detection and intervention of psychosis
 Early detection and intervention of psychosis New Data Benno G. Schimmelmann University Hospital of Child and Adolescent Psychiatry Bern, Bern, Switzerland Early detection of psychosis Early Detection
Early detection and intervention of psychosis New Data Benno G. Schimmelmann University Hospital of Child and Adolescent Psychiatry Bern, Bern, Switzerland Early detection of psychosis Early Detection
The prodromal stage of psychotic illness: Observation, detection or intervention?
 Commentary Commentaire The prodromal stage of psychotic illness: Observation, detection or intervention? Jean Addington, PhD Department of Psychiatry, University of Toronto, Toronto, Ont. Accurate identification
Commentary Commentaire The prodromal stage of psychotic illness: Observation, detection or intervention? Jean Addington, PhD Department of Psychiatry, University of Toronto, Toronto, Ont. Accurate identification
c01 WU083-French January 22, :40 Char Count= 0 PART I BACKGROUND 1
 PART I BACKGROUND 1 THE IMPORTANCE OF EARLY RECOGNITION RATIONALE The length of time between the onset of psychotic symptoms and the subsequent detection, diagnosis and commencement of treatment has been
PART I BACKGROUND 1 THE IMPORTANCE OF EARLY RECOGNITION RATIONALE The length of time between the onset of psychotic symptoms and the subsequent detection, diagnosis and commencement of treatment has been
EVIDENCE AND PERSPECTIVES IN EARLY RECOGNITION AND INTERVENTION FOR PSYCHOSIS and BEYOND. Patrick McGorry
 EVIDENCE AND PERSPECTIVES IN EARLY RECOGNITION AND INTERVENTION FOR PSYCHOSIS and BEYOND Patrick McGorry TOTAL IEPA MEMBERS PER YEAR 3000 2900 2500 2000 1500 1000 1127 1328 1540 1828 1856 2090 2133 2489
EVIDENCE AND PERSPECTIVES IN EARLY RECOGNITION AND INTERVENTION FOR PSYCHOSIS and BEYOND Patrick McGorry TOTAL IEPA MEMBERS PER YEAR 3000 2900 2500 2000 1500 1000 1127 1328 1540 1828 1856 2090 2133 2489
Symptomatology of the Initial Prodromal Phase in Schizophrenia
 Symptomatology of the Initial Prodromal Phase in Schizophrenia by Philippos Qourzis, Aggeliki Jatrivanou, and Stavroula Beratis Abstract The initial prodromal symptoms in schizophrenia were studied in
Symptomatology of the Initial Prodromal Phase in Schizophrenia by Philippos Qourzis, Aggeliki Jatrivanou, and Stavroula Beratis Abstract The initial prodromal symptoms in schizophrenia were studied in
Early Intervention Teams services for early psychosis
 Early Intervention Teams services for early psychosis Early intervention services work with people who are usually between 14 and 35, and are either at risk of or are currently experiencing a first episode
Early Intervention Teams services for early psychosis Early intervention services work with people who are usually between 14 and 35, and are either at risk of or are currently experiencing a first episode
Psychosis. Paula Gibbs, MD Department of Psychiatry University of Utah
 Psychosis Paula Gibbs, MD Department of Psychiatry University of Utah Psychotic Symptoms Psychosis in a broad sense, signifies impaired reality testing ability Symptoms include: hallucinations, delusions,
Psychosis Paula Gibbs, MD Department of Psychiatry University of Utah Psychotic Symptoms Psychosis in a broad sense, signifies impaired reality testing ability Symptoms include: hallucinations, delusions,
Schizophrenia: New Concepts for Therapeutic Discovery
 Schizophrenia: New Concepts for Therapeutic Discovery William T. Carpenter, M.D. Professor of Psychiatry and Pharmacology University of Maryland School of Medicine Department of Psychiatry Maryland Psychiatric
Schizophrenia: New Concepts for Therapeutic Discovery William T. Carpenter, M.D. Professor of Psychiatry and Pharmacology University of Maryland School of Medicine Department of Psychiatry Maryland Psychiatric
Goal: To recognize and differentiate different forms of psychopathology that involve disordered thinking and reasoning and distorted perception
 Goal: To recognize and differentiate different forms of psychopathology that involve disordered thinking and reasoning and distorted perception Psychotic disorders, or psychoses, are among the most serious
Goal: To recognize and differentiate different forms of psychopathology that involve disordered thinking and reasoning and distorted perception Psychotic disorders, or psychoses, are among the most serious
Stigma, well-being, attitudes to service use and transition to schizophrenia: Longitudinal findings among young people at risk of psychosis
 Stigma, well-being, attitudes to service use and transition to schizophrenia: Longitudinal findings among young people at risk of psychosis Nicolas Rüsch, Mario Müller, Karsten Heekeren, Ana Theodoridou,
Stigma, well-being, attitudes to service use and transition to schizophrenia: Longitudinal findings among young people at risk of psychosis Nicolas Rüsch, Mario Müller, Karsten Heekeren, Ana Theodoridou,
Early prodromal symptoms and diagnoses before first psychotic episode in 219 inpatients with schizophrenia
 Psychiatry and Clinical Neurosciences (2007), 61, 348 354 doi:10.1111/j.1440-1819.2007.01685.x Regular Article Early prodromal symptoms and diagnoses before first psychotic episode in 219 inpatients with
Psychiatry and Clinical Neurosciences (2007), 61, 348 354 doi:10.1111/j.1440-1819.2007.01685.x Regular Article Early prodromal symptoms and diagnoses before first psychotic episode in 219 inpatients with
BADDS Appendix A: The Bipolar Affective Disorder Dimensional Scale, version 3.0 (BADDS 3.0)
 BADDS Appendix A: The Bipolar Affective Disorder Dimensional Scale, version 3.0 (BADDS 3.0) General information The Bipolar Affective Disorder Dimension Scale (BADDS) has been developed in order to address
BADDS Appendix A: The Bipolar Affective Disorder Dimensional Scale, version 3.0 (BADDS 3.0) General information The Bipolar Affective Disorder Dimension Scale (BADDS) has been developed in order to address
Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna
 University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
Accurate Diagnosis of Primary Psychotic Disorders
 Accurate Diagnosis of Primary Psychotic Disorders The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart
Accurate Diagnosis of Primary Psychotic Disorders The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart
November 2014 MRC2.CORP.X.00004
 This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid consultant of Otsuka America Pharmaceutical, Inc. advice or professional diagnosis. Users seeking
This program is paid for by Otsuka America Pharmaceutical, Inc. and Lundbeck, LLC. The speaker is a paid consultant of Otsuka America Pharmaceutical, Inc. advice or professional diagnosis. Users seeking
What is psychosis? The Challenge 4/11/2011. Psychotic Spectrum Symptoms in Youth
 What is psychosis? Psychotic Spectrum Symptoms in Youth Nick Weiss, MD PART Program Director, Child and Adolescent Psychiatry Clinics University of California, San Francisco Often thought of as catastrophically
What is psychosis? Psychotic Spectrum Symptoms in Youth Nick Weiss, MD PART Program Director, Child and Adolescent Psychiatry Clinics University of California, San Francisco Often thought of as catastrophically
Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale
 Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale By: Thomas R Kwapil, Monica C. Mann and Michael L. Raulin Kwapil, T.R., Mann, M.C., & Raulin, M.L. (2002). Psychometric
Psychometric Properties and Concurrent Validity of the Schizotypal Ambivalence Scale By: Thomas R Kwapil, Monica C. Mann and Michael L. Raulin Kwapil, T.R., Mann, M.C., & Raulin, M.L. (2002). Psychometric
Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention
 Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention Margaret Migliorati, MA, LPCC The University of New Mexico mmigliorati@salud.unm.edu Mental Health As a Public Health
Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention Margaret Migliorati, MA, LPCC The University of New Mexico mmigliorati@salud.unm.edu Mental Health As a Public Health
By Jason H. King DECONSTRUCTING THE DSM-5 ASSESSMENT AND DIAGNOSIS OF SCHIZOPHRENIA SPECTRUM DISORDERS THE NEW LANDSCAPE
 DECONSTRUCTING THE DSM-5 By Jason H. King ASSESSMENT AND DIAGNOSIS OF SCHIZOPHRENIA SPECTRUM DISORDERS Happy New Year as you engage in your counseling, research, supervision or educational endeavors. I
DECONSTRUCTING THE DSM-5 By Jason H. King ASSESSMENT AND DIAGNOSIS OF SCHIZOPHRENIA SPECTRUM DISORDERS Happy New Year as you engage in your counseling, research, supervision or educational endeavors. I
Schizophrenia: Early Intervention
 Focus on CME at The University of Western Ontario Schizophrenia: Early Intervention Rahul Manchanda, MD, MRCPsych, FRCP(C); and Ross M.G. Norman, PhD, CPsych Presented at A Psychiatric Update 2003, Regional
Focus on CME at The University of Western Ontario Schizophrenia: Early Intervention Rahul Manchanda, MD, MRCPsych, FRCP(C); and Ross M.G. Norman, PhD, CPsych Presented at A Psychiatric Update 2003, Regional
Psychotic disorders Dr. Sarah DeLeon, MD PGYIV, Psychiatry ConceptsInPsychiatry.com
 Psychotic disorders Dr. Sarah DeLeon, MD PGYIV, Psychiatry ConceptsInPsychiatry.com Introduction Psychotic spectrum disorders include schizotypal personality disorder, delusional disorder, brief psychotic
Psychotic disorders Dr. Sarah DeLeon, MD PGYIV, Psychiatry ConceptsInPsychiatry.com Introduction Psychotic spectrum disorders include schizotypal personality disorder, delusional disorder, brief psychotic
Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence
 Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
ENTITLEMENT ELIGIBILITY GUIDELINE SCHIZOPHRENIA
 Entitlement Eligibility Guideline SCHIZOPHRENIA Page 1 of 8 ENTITLEMENT ELIGIBILITY GUIDELINE SCHIZOPHRENIA MPC 00607 ICD-9 295 ICD-10 F20 DEFINITION SCHIZOPHRENIA Characteristic symptoms of Schizophrenia
Entitlement Eligibility Guideline SCHIZOPHRENIA Page 1 of 8 ENTITLEMENT ELIGIBILITY GUIDELINE SCHIZOPHRENIA MPC 00607 ICD-9 295 ICD-10 F20 DEFINITION SCHIZOPHRENIA Characteristic symptoms of Schizophrenia
NeuRA Schizophrenia diagnosis May 2017
 Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
NIH Public Access Author Manuscript Schizophr Res. Author manuscript; available in PMC 2012 June 1.
 NIH Public Access Author Manuscript Published in final edited form as: Schizophr Res. 2011 June ; 129(1): 42 46. doi:10.1016/j.schres.2011.03.029. Psychosis Risk Screening with the Prodromal Questionnaire
NIH Public Access Author Manuscript Published in final edited form as: Schizophr Res. 2011 June ; 129(1): 42 46. doi:10.1016/j.schres.2011.03.029. Psychosis Risk Screening with the Prodromal Questionnaire
DSM5: How to Understand It and How to Help
 DSM5: How to Understand It and How to Help Introduction: The DSM5 is a foreign language! Three Questions: I. The first was, What the key assumptions made to determine the organization of the DSM5? A. Mental
DSM5: How to Understand It and How to Help Introduction: The DSM5 is a foreign language! Three Questions: I. The first was, What the key assumptions made to determine the organization of the DSM5? A. Mental
4/7/2016. Auditory Hallucinations in Youth: The Good, the Bad, and the Reassuring. Objectives. Disclosures
 Auditory Hallucinations in Youth: The Good, the Bad, and the Reassuring Nick Weiss, MD April 30, 2016 Objectives Participants will learn about the prevalence and patterns of auditory hallucinations in
Auditory Hallucinations in Youth: The Good, the Bad, and the Reassuring Nick Weiss, MD April 30, 2016 Objectives Participants will learn about the prevalence and patterns of auditory hallucinations in
Schizophrenia. This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available.
 This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a severe mental health condition. However,
This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a severe mental health condition. However,
THE STABILITY OF SYMPTOMS AND SYNDROMES IN CHRONIC SCHIZOPHRENIC PATIENTS MILIND BORDE 1, ELIZABETH J.B. DAVIS 1 AND L.N. SHARMA 2
 Indian J. Psychiat. 1992, 34(2), 133-139 THE STABILITY OF SYMPTOMS AND SYNDROMES IN CHRONIC SCHIZOPHRENIC PATIENTS MILIND BORDE 1, ELIZABETH J.B. DAVIS 1 AND L.N. SHARMA 2 36 chronic schizophrenic patients
Indian J. Psychiat. 1992, 34(2), 133-139 THE STABILITY OF SYMPTOMS AND SYNDROMES IN CHRONIC SCHIZOPHRENIC PATIENTS MILIND BORDE 1, ELIZABETH J.B. DAVIS 1 AND L.N. SHARMA 2 36 chronic schizophrenic patients
Help-seeking pathways in early psychosis
 Soc Psychiatry Psychiatr Epidemiol (2006) 41:967 974 DOI 10.1007/s00127-006-0117-4 ORIGINAL PAPER Christoph Platz Æ Daniel S. Umbricht Æ Katja Cattapan-Ludewig Æ Diane Dvorsky Æ Dima Arbach Hans-Dieter
Soc Psychiatry Psychiatr Epidemiol (2006) 41:967 974 DOI 10.1007/s00127-006-0117-4 ORIGINAL PAPER Christoph Platz Æ Daniel S. Umbricht Æ Katja Cattapan-Ludewig Æ Diane Dvorsky Æ Dima Arbach Hans-Dieter
Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment
 Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment Stuart Fine, MB, FRCP (C), Marlene Moretti, MA, Glenn Haley, MA, Simon Fraser University.
Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment Stuart Fine, MB, FRCP (C), Marlene Moretti, MA, Glenn Haley, MA, Simon Fraser University.
Psychosis, Mood, and Personality: A Clinical Perspective
 Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
Toward a world consensus on prevention of schizophrenia Jim Van Os, MD, PhD; Philippe Delespaul, MA, PhD
 Toward a world consensus on prevention of schizophrenia Jim Van Os, MD, PhD; Philippe Delespaul, MA, PhD The detection of psychotic disorder in the prodromal phases, coupled with specialized early interventions
Toward a world consensus on prevention of schizophrenia Jim Van Os, MD, PhD; Philippe Delespaul, MA, PhD The detection of psychotic disorder in the prodromal phases, coupled with specialized early interventions
Schizophrenia and Other Psychotic Disorders
 Schizophrenia and Other Psychotic Disorders Chapter 14 This multimedia product and its contents are protected under copyright law. The following are prohibited by law: any public performance or display,
Schizophrenia and Other Psychotic Disorders Chapter 14 This multimedia product and its contents are protected under copyright law. The following are prohibited by law: any public performance or display,
Overseas Corporate Scholarship Program for Clinical Leaders 2014/15
 Overseas Corporate Scholarship Program for Clinical Leaders 2014/15 Early Psychosis Nursing Speaker: Li Yiu Bun, Advanced Practice Nurse (Psy.) of Pamela Youde Nethersole Eastern Hospital Expected learning
Overseas Corporate Scholarship Program for Clinical Leaders 2014/15 Early Psychosis Nursing Speaker: Li Yiu Bun, Advanced Practice Nurse (Psy.) of Pamela Youde Nethersole Eastern Hospital Expected learning
Citation for published version (APA): Boonstra, T. C. (2011). Early detection of psychosis; why should we care? Groningen: s.n.
 University of Groningen Early detection of psychosis; why should we care? Boonstra, Trijntje Cornelia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Early detection of psychosis; why should we care? Boonstra, Trijntje Cornelia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Effectiveness of early intervention in psychosis Eóin Killackey a,b and Alison R. Yung a,c
 Effectiveness of early intervention in psychosis Eóin Killackey a,b and Alison R. Yung a,c Purpose of review Over 15 years, early intervention in psychosis has grown to become a mainstream funded approach
Effectiveness of early intervention in psychosis Eóin Killackey a,b and Alison R. Yung a,c Purpose of review Over 15 years, early intervention in psychosis has grown to become a mainstream funded approach
Early Stages of Psychosis. Learning Objectives
 Early Stages of Psychosis Stephan Heckers, MD MSc Department of Psychiatry and Behavioral Sciences Vanderbilt University Learning Objectives Summarize the five domains of psychosis Describe how psychotic
Early Stages of Psychosis Stephan Heckers, MD MSc Department of Psychiatry and Behavioral Sciences Vanderbilt University Learning Objectives Summarize the five domains of psychosis Describe how psychotic
Schizoaffective Disorder
 Roseanna Parkhurst-Gatewood MSN FNP-BC, PMHNP-BC DSM-5 diagnostic criteria for schizoaffective disorder 3 A. An uninterrupted period of illness during which there is a major mood episode (major depressive
Roseanna Parkhurst-Gatewood MSN FNP-BC, PMHNP-BC DSM-5 diagnostic criteria for schizoaffective disorder 3 A. An uninterrupted period of illness during which there is a major mood episode (major depressive
UC San Francisco UC San Francisco Previously Published Works
 UC San Francisco UC San Francisco Previously Published Works Title Prodromal psychosis screening in adolescent psychiatry clinics. Permalink https://escholarship.org/uc/item/3g7145j0 Journal Early intervention
UC San Francisco UC San Francisco Previously Published Works Title Prodromal psychosis screening in adolescent psychiatry clinics. Permalink https://escholarship.org/uc/item/3g7145j0 Journal Early intervention
Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing
 Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing Mental Health Exchange Group December 3, 2014 W Joy Maddigan, PhD RN Background One component [the quantitative
Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing Mental Health Exchange Group December 3, 2014 W Joy Maddigan, PhD RN Background One component [the quantitative
4/29/2016. Psychosis A final common pathway. Early Intervention in Psychotic Disorders: Necessary, Effective, and Overdue
 Early Intervention in Psychotic Disorders: Necessary, Effective, and Overdue Disclosures Financial relationships with commercial interests Douglas R. Robbins, M.D. Maine Medical Center Tufts University
Early Intervention in Psychotic Disorders: Necessary, Effective, and Overdue Disclosures Financial relationships with commercial interests Douglas R. Robbins, M.D. Maine Medical Center Tufts University
Clinical Staging and the At-Risk Phase of Psychotic Disorder
 Clinical Staging and the At-Risk Phase of Psychotic Disorder Sabina Abidi MD FRCPC IWK Youth Psychosis Program Capital Health Nova ScoCa Early Psychosis Program Key Findings in Early Psychosis Knowledge
Clinical Staging and the At-Risk Phase of Psychotic Disorder Sabina Abidi MD FRCPC IWK Youth Psychosis Program Capital Health Nova ScoCa Early Psychosis Program Key Findings in Early Psychosis Knowledge
EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 7 (56) No. 1-2014 EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 7 (56) No. 1-2014 EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
Youth Mental Health and 22q11
 Youth Mental Health and 22q11 Cameron S. Carter M.D. Director Center for Neuroscience U.C. Davis Early Diagnosis & Preventative Treatment Clinic (EDAPT) UC Davis Department of Psychiatry of Mental Health
Youth Mental Health and 22q11 Cameron S. Carter M.D. Director Center for Neuroscience U.C. Davis Early Diagnosis & Preventative Treatment Clinic (EDAPT) UC Davis Department of Psychiatry of Mental Health
D. Exclusion of schizoaffective disorder and mood disorder with psychotic features.
 65 CHAPTER 8: APPENDIX. ADDENDUM A DSM-IV diagnostic criteria for schizophrenia A. Characteristic symptoms: Two or more of the following, each present for a significant portion of time during a one-month
65 CHAPTER 8: APPENDIX. ADDENDUM A DSM-IV diagnostic criteria for schizophrenia A. Characteristic symptoms: Two or more of the following, each present for a significant portion of time during a one-month
Tilburg University. Published in: Schizophrenia Research. Publication date: Link to publication
 Tilburg University Does the schizotypal personality questionnaire reflect the biological-genetic vulnerability to schizophrenia? Vollema, M.G.; Sitskoorn, Margriet; Appels, M.C.M.; Kahn, R.S. Published
Tilburg University Does the schizotypal personality questionnaire reflect the biological-genetic vulnerability to schizophrenia? Vollema, M.G.; Sitskoorn, Margriet; Appels, M.C.M.; Kahn, R.S. Published
** * *Correspondence ***
 Journal of Clinical Psychology Vol. 2, No. 2 (6), Summer 2010 Pages:11-26 1389 (6 ) 2 11-26 : - The Effectiveness of Anxiety-Reduction Cognitive-Behavioral Techniques in Treating Paranoid Ideation and
Journal of Clinical Psychology Vol. 2, No. 2 (6), Summer 2010 Pages:11-26 1389 (6 ) 2 11-26 : - The Effectiveness of Anxiety-Reduction Cognitive-Behavioral Techniques in Treating Paranoid Ideation and
Update on First Psychotic Episodes in Childhood and Adolescence. Cheryl Corcoran, MD Assistant Professor of Psychiatry Columbia University
 Update on First Psychotic Episodes in Childhood and Adolescence Cheryl Corcoran, MD Assistant Professor of Psychiatry Columbia University Childhood-Onset Psychosis 8% of psychiatrically referred youth
Update on First Psychotic Episodes in Childhood and Adolescence Cheryl Corcoran, MD Assistant Professor of Psychiatry Columbia University Childhood-Onset Psychosis 8% of psychiatrically referred youth
Rating Mental Impairment with AMA Guides 6 th edition:
 Rating Mental Impairment with AMA Guides 6 th edition: Practical Considerations and Strategies CSME/CAPDA C-CAT Course, March 24, 2018 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant
Rating Mental Impairment with AMA Guides 6 th edition: Practical Considerations and Strategies CSME/CAPDA C-CAT Course, March 24, 2018 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant
Week #1 Classification & Diagnosis
 Week #1 Classification & Diagnosis 3 Categories in the Conceptualisation of Abnormality Psychological Dysfunction: Refers to a breakdown in cognitive, emotional or behavioural functioning. Knowing where
Week #1 Classification & Diagnosis 3 Categories in the Conceptualisation of Abnormality Psychological Dysfunction: Refers to a breakdown in cognitive, emotional or behavioural functioning. Knowing where
Chapter 12. Schizophrenia and Other Psychotic Disorders. PSY 440: Abnormal Psychology. Rick Grieve Western Kentucky University
 Chapter 12 Schizophrenia and Other Psychotic Disorders PSY 440: Abnormal Psychology Rick Grieve Western Kentucky University psychotic disorders disorders so severe that the person has essentially lost
Chapter 12 Schizophrenia and Other Psychotic Disorders PSY 440: Abnormal Psychology Rick Grieve Western Kentucky University psychotic disorders disorders so severe that the person has essentially lost
Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health
 Schizophrenia: What Do We Know? Where Do We Go From Here? Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health Objectives Participants will be able to: Understand the clinical
Schizophrenia: What Do We Know? Where Do We Go From Here? Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health Objectives Participants will be able to: Understand the clinical
The "Close-in" or Ultra High-Risk Model: A Safe and Effective Strategy for Research and Clinical Intervention in Prepsychotic Mental Disorder
 The "Close-in" or Ultra High-Risk Model: A Safe and Effective Strategy for Research and Clinical Intervention in Prepsychotic Mental Disorder by Patrick D. hicqorry, Alison R. Yung, and Lisa J. PhiUips
The "Close-in" or Ultra High-Risk Model: A Safe and Effective Strategy for Research and Clinical Intervention in Prepsychotic Mental Disorder by Patrick D. hicqorry, Alison R. Yung, and Lisa J. PhiUips
The use of CBT to prevent transition to psychosis in patients at ultra-high risk. a Journal Club presentation brought to you by Lisa Valentine
 The use of CBT to prevent transition to psychosis in patients at ultra-high risk a Journal Club presentation brought to you by Lisa Valentine The Background Recent interest in early detection and intervention
The use of CBT to prevent transition to psychosis in patients at ultra-high risk a Journal Club presentation brought to you by Lisa Valentine The Background Recent interest in early detection and intervention
Results. NeuRA Essential fatty acids August 2016
 Introduction Alternative treatments are investigated as a possible replacement for antipsychotic medication, which can be associated with severe side effects. Alternative therapies may have less debilitating
Introduction Alternative treatments are investigated as a possible replacement for antipsychotic medication, which can be associated with severe side effects. Alternative therapies may have less debilitating
The psychological disorders
 The psychological disorders Defining abnormal Statistical infrequency Normal distribution; the normal curve Violation of norms Culture bound syndromes Personal distress Some disorders do not involve distress
The psychological disorders Defining abnormal Statistical infrequency Normal distribution; the normal curve Violation of norms Culture bound syndromes Personal distress Some disorders do not involve distress
NeuRA Schizophrenia diagnosis June 2017
 Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
Psychotic prodrome: Are antipsychotics effective? Ethical?
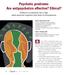 Psychotic prodrome: Are antipsychotics effective? Ethical? Evidence is mixed but risk is high when abnormal cognition falls short of schizophrenia Meera Narasimhan, MD Director, psychopharmacology division
Psychotic prodrome: Are antipsychotics effective? Ethical? Evidence is mixed but risk is high when abnormal cognition falls short of schizophrenia Meera Narasimhan, MD Director, psychopharmacology division
Hope FIRST: An Innovative Treatment for First Episode Psychosis PRESENTATION BY REBECCA FLATTERY, LCSW AND BRIAN ROHLOFF, LPC
 Hope FIRST: An Innovative Treatment for First Episode Psychosis PRESENTATION BY REBECCA FLATTERY, LCSW AND BRIAN ROHLOFF, LPC What is a first episode of psychosis? The word psychosis is used to describe
Hope FIRST: An Innovative Treatment for First Episode Psychosis PRESENTATION BY REBECCA FLATTERY, LCSW AND BRIAN ROHLOFF, LPC What is a first episode of psychosis? The word psychosis is used to describe
Identifying Youth at Clinical High Risk for Psychosis
 Identifying Youth at Clinical High Risk for Psychosis Jean Addington PhD University of Calgary Department of Psychiatry 1 Identifying Youth at Clinical High Risk for Psychosis Part 1: What do we know about
Identifying Youth at Clinical High Risk for Psychosis Jean Addington PhD University of Calgary Department of Psychiatry 1 Identifying Youth at Clinical High Risk for Psychosis Part 1: What do we know about
Early Psychosis Services: Philadelphia PEACE Program
 Early Psychosis Services: Philadelphia PEACE Program Irene Hurford, M.D. Clinical Director, PEACE Program, Horizon House Assistant Professor, Department of Psychiatry, University of Pennsylvania 1 John
Early Psychosis Services: Philadelphia PEACE Program Irene Hurford, M.D. Clinical Director, PEACE Program, Horizon House Assistant Professor, Department of Psychiatry, University of Pennsylvania 1 John
RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges. CSME/CAPDA Conference, April 1, 2017
 RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges CSME/CAPDA Conference, April 1, 2017 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant Psychiatrist
RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges CSME/CAPDA Conference, April 1, 2017 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant Psychiatrist
Supplementary Online Content
 Supplementary Online Content Subotnik KL, Casaus LR, Ventura J, et al. Long-acting injectable risperidone for relapse prevention and control of breakthrough symptoms after a recent first episode of schizophrenia:
Supplementary Online Content Subotnik KL, Casaus LR, Ventura J, et al. Long-acting injectable risperidone for relapse prevention and control of breakthrough symptoms after a recent first episode of schizophrenia:
EARLY ONSET SCHIZOPHRENIA
 Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences EARLY ONSET SCHIZOPHRENIA JON MCCLELLAN CHILD STUDY AND TREATMENT CENTER GENERAL DISCLOSURES The University of Washington
Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences EARLY ONSET SCHIZOPHRENIA JON MCCLELLAN CHILD STUDY AND TREATMENT CENTER GENERAL DISCLOSURES The University of Washington
Adult Mental Health Services applicable to Members in the State of Connecticut subject to state law SB1160
 Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
MEMORY AND PSYCHOSIS studies) and the long follow-up period of years, with high attrition rates and low rates of transition to psychosis (6% 15%
 Article Memory Impairments Identified in People at Ultra-High Risk for Psychosis Who Later Develop First-Episode Psychosis Warrick J. Brewer, Ph.D. Shona M. Francey, Ph.D. Stephen J. Wood, Ph.D. Henry
Article Memory Impairments Identified in People at Ultra-High Risk for Psychosis Who Later Develop First-Episode Psychosis Warrick J. Brewer, Ph.D. Shona M. Francey, Ph.D. Stephen J. Wood, Ph.D. Henry
Program Outline. DSM-5 Schizophrenia Spectrum and Psychotic Disorders: Knowing it Better and Improving Clinical Practice.
 DSM-5 Spectrum and Disorders: Knowing it Better and Improving Clinical Practice Rajiv Tandon, MD Professor of Psychiatry University of Florida College of Medicine Gainesville, Florida Program Outline Changes
DSM-5 Spectrum and Disorders: Knowing it Better and Improving Clinical Practice Rajiv Tandon, MD Professor of Psychiatry University of Florida College of Medicine Gainesville, Florida Program Outline Changes
Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies
 Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies Henry A. Nasrallah, MD Sydney W. Souers Professor and Chair, Department of Psychiatry, Saint Louis University,
Suboptimal Response in Psychotic & Mood Disorders: Causes, Consequences, and Management Strategies Henry A. Nasrallah, MD Sydney W. Souers Professor and Chair, Department of Psychiatry, Saint Louis University,
Relationship Between Duration of Untreated Psychosis and Outcome in First-Episode Schizophrenia: A Critical Review and Meta-Analysis
 Reviews and Overviews Relationship Between Duration of Untreated Psychosis and Outcome in First-Episode Schizophrenia: A Critical Review and Meta-Analysis Diana O. Perkins, M.D., M.P.H. Hongbin Gu, Ph.D.
Reviews and Overviews Relationship Between Duration of Untreated Psychosis and Outcome in First-Episode Schizophrenia: A Critical Review and Meta-Analysis Diana O. Perkins, M.D., M.P.H. Hongbin Gu, Ph.D.
The Diagnostic Stability of DSM-IV Diagnoses: An Examination of Major Depressive Disorder, Bipolar I Disorder, and Schizophrenia in Korean Patients
 Original Article pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2011;9(3):117-121 Copyrightc 2011, Korean College of Neuropsychopharmacology The Diagnostic Stability of
Original Article pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2011;9(3):117-121 Copyrightc 2011, Korean College of Neuropsychopharmacology The Diagnostic Stability of
Early psychosis intervention
 Review Article Singapore Med J 2010, 51(9) 689 Early psychosis intervention Yap H L ABSTRACT Early psychosis intervention programmes have been around for 20 years. The duration of psychosis has been hypothesised
Review Article Singapore Med J 2010, 51(9) 689 Early psychosis intervention Yap H L ABSTRACT Early psychosis intervention programmes have been around for 20 years. The duration of psychosis has been hypothesised
Effect of age and gender on schizotypal personality traits in the normal populationpcn_
 Psychiatry and Clinical Neurosciences 2009; 63: 663 669 doi:10.1111/j.1440-1819.2009.02011.x Regular Article Effect of age and gender on schizotypal personality traits in the normal populationpcn_2011
Psychiatry and Clinical Neurosciences 2009; 63: 663 669 doi:10.1111/j.1440-1819.2009.02011.x Regular Article Effect of age and gender on schizotypal personality traits in the normal populationpcn_2011
Routine clinical measures in a newly commissioned Psychiatric Intensive Care Unit (PICU): Predictors of favourable outcomes.
 Routine clinical measures in a newly commissioned Psychiatric Intensive Care Unit (PICU): Predictors of favourable outcomes. Rebecca Carleton, 1 Matthew Cordiner, 1 Patrick Hughes, 1 Susan Cochrane, 1
Routine clinical measures in a newly commissioned Psychiatric Intensive Care Unit (PICU): Predictors of favourable outcomes. Rebecca Carleton, 1 Matthew Cordiner, 1 Patrick Hughes, 1 Susan Cochrane, 1
Bizarre delusions and DSM-IV schizophrenia
 Psychiatry and Clinical Neurosciences (2002), 56, 391 395 Regular Article Bizarre delusions and DSM-IV schizophrenia MAKOTO NAKAYA, md, phd, 1 KATSUNORI KUSUMOTO, md, phd, 2 TAKAYUKI OKADA, md, phd 3 AND
Psychiatry and Clinical Neurosciences (2002), 56, 391 395 Regular Article Bizarre delusions and DSM-IV schizophrenia MAKOTO NAKAYA, md, phd, 1 KATSUNORI KUSUMOTO, md, phd, 2 TAKAYUKI OKADA, md, phd 3 AND
Early intervention for people with psychosis
 Policy Research Programme Early intervention for people with psychosis This paper summarises findings of a review of research evidence about early intervention for severe mental illness (Marshall and Lockwood,
Policy Research Programme Early intervention for people with psychosis This paper summarises findings of a review of research evidence about early intervention for severe mental illness (Marshall and Lockwood,
Supplementary Online Content
 Supplementary Online Content Vorstman JAS, Breetvelt EJ, Duijff SN, et al; International Consortium on Brain and Behavior in 22q11.2 Deletion Syndrome. Cognitive decline preceding the onset of psychosis
Supplementary Online Content Vorstman JAS, Breetvelt EJ, Duijff SN, et al; International Consortium on Brain and Behavior in 22q11.2 Deletion Syndrome. Cognitive decline preceding the onset of psychosis
Parkinsonian Disorders with Dementia
 Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Severe Mental Disorders. Etheldreda Nakimuli-Mpungu, MMed (Psych), MBChB Johns Hopkins University
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL. Ng CG
 ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
Expanding Behavioral Health Data Collection:
 Expanding Behavioral Health Data Collection: ADULT MENTAL ILLNESS DIAGNOSES WITH FUNCTIONAL IMPAIRMENT Center for Behavioral Health Statistics and Quality Substance Abuse and Mental Health Services Administration
Expanding Behavioral Health Data Collection: ADULT MENTAL ILLNESS DIAGNOSES WITH FUNCTIONAL IMPAIRMENT Center for Behavioral Health Statistics and Quality Substance Abuse and Mental Health Services Administration
SCHIZOPHRENIA AN OVERVIEW
 SCHIZOPHRENIA AN OVERVIEW Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com IMPORTANT The health information contained herein is not meant as a substitute for advice from your physician,
SCHIZOPHRENIA AN OVERVIEW Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com IMPORTANT The health information contained herein is not meant as a substitute for advice from your physician,
NeuRA Schizophrenia diagnosis October 2017
 Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
Introduction Diagnostic scales are widely used within clinical practice and research settings to ensure consistency of illness ratings. These scales have been extensively validated and provide a set of
DOWNLOAD OR READ : TREATMENT OF SCHIZOPHRENIA FAMILY ASSESSMENT AND INTERVENTION PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT OF SCHIZOPHRENIA FAMILY ASSESSMENT AND INTERVENTION PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of schizophrenia family assessment and intervention treatment of schizophrenia
DOWNLOAD OR READ : TREATMENT OF SCHIZOPHRENIA FAMILY ASSESSMENT AND INTERVENTION PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of schizophrenia family assessment and intervention treatment of schizophrenia
Hospital comorbidity bias and the concept of schizophrenia
 Soc Psychiatry Psychiatr Epidemiol (2005) 40: 817 821 ORIGINAL PAPER DOI 10.1007/s00127-005-0971-0 Maarten Bak. Marjan Drukker. Jim van Os. Philippe Delespaul Hospital comorbidity bias and the concept
Soc Psychiatry Psychiatr Epidemiol (2005) 40: 817 821 ORIGINAL PAPER DOI 10.1007/s00127-005-0971-0 Maarten Bak. Marjan Drukker. Jim van Os. Philippe Delespaul Hospital comorbidity bias and the concept
schizophrenia :The latest news By Dr. Gamal Suliman Elgorashi MB BS,DPM, MRCpsych Consultant psychiatrist Kent & Medway NHS Trust UK
 schizophrenia :The latest news By Dr. Gamal Suliman Elgorashi MB BS,DPM, MRCpsych Consultant psychiatrist Kent & Medway NHS Trust UK The argument Schizophrenia has for too long been known as a single
schizophrenia :The latest news By Dr. Gamal Suliman Elgorashi MB BS,DPM, MRCpsych Consultant psychiatrist Kent & Medway NHS Trust UK The argument Schizophrenia has for too long been known as a single
The British Approach to Understanding and Treating Psychosis
 The British Approach to Understanding and Treating Psychosis Robin M Murray Professor of Psychiatric Research Department of Psychosis Studies Institute of Psychiatry robin.murray@kcl.ac.uk Which boy will
The British Approach to Understanding and Treating Psychosis Robin M Murray Professor of Psychiatric Research Department of Psychosis Studies Institute of Psychiatry robin.murray@kcl.ac.uk Which boy will
Affective Disorders most often should be viewed in conjunction with other physical and mental impairments.
 THESE ARE THE FORMS I USE THIS IS NOT LEGAL ADVICE AND INTENDED TO SUPPLEMENT YOUR PARTICULAR FACTUAL SITUATION ONLY It is crucial you educate yourself on the Social Security Regulations that define and
THESE ARE THE FORMS I USE THIS IS NOT LEGAL ADVICE AND INTENDED TO SUPPLEMENT YOUR PARTICULAR FACTUAL SITUATION ONLY It is crucial you educate yourself on the Social Security Regulations that define and
Date of Onset is defined as the first day the claimant meets the definition of disability as defined in the Act and regulations.
 THESE ARE THE FORMS I USE THIS IS NOT LEGAL ADVICE AND INTENDED TO SUPPLEMENT YOUR PARTICULAR FACTUAL SITUATION ONLY It is crucial you educate yourself on the Social Security Regulations that define and
THESE ARE THE FORMS I USE THIS IS NOT LEGAL ADVICE AND INTENDED TO SUPPLEMENT YOUR PARTICULAR FACTUAL SITUATION ONLY It is crucial you educate yourself on the Social Security Regulations that define and
Positive and Negative Symptoms of Psychosis The Care Transitions Network
 Positive and Negative Symptoms of Psychosis The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart
Positive and Negative Symptoms of Psychosis The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health Netsmart
ALCOHOLIC HALLUCINOSIS AND PARANOID SCHIZOPHRENIA A PARATIVE (CLINICAL AND FOLLOW UP) STUDY
 Mun J. Pnckiiu. {1), 2(4), S W2 ALCOHOLIC HALLUCINOSIS AND PARANOID SCHIZOPHRENIA A PARATIVE (CLINICAL AND FOLLOW UP) STUDY COM-* G. SAMPATH* MD Y. VIKRAM KUMAR" DM* S. M. CHANNABASAVANNA* MD M.S. KESHAVAN*
Mun J. Pnckiiu. {1), 2(4), S W2 ALCOHOLIC HALLUCINOSIS AND PARANOID SCHIZOPHRENIA A PARATIVE (CLINICAL AND FOLLOW UP) STUDY COM-* G. SAMPATH* MD Y. VIKRAM KUMAR" DM* S. M. CHANNABASAVANNA* MD M.S. KESHAVAN*
What is Schizophrenia?
 What is Schizophrenia? What is schizophrenia? Schizophrenia is a mental illness which affects one person in every hundred. Schizophrenia interferes with the mental functioning of a person and, in the long
What is Schizophrenia? What is schizophrenia? Schizophrenia is a mental illness which affects one person in every hundred. Schizophrenia interferes with the mental functioning of a person and, in the long
Proceedings of the International Conference on RISK MANAGEMENT, ASSESSMENT and MITIGATION
 COGNITIVE-BEHAVIOURAL THERAPY EFFICACY IN MAJOR DEPRESSION WITH ASSOCIATED AXIS II RISK FACTOR FOR NEGATIVE PROGNOSIS DANIEL VASILE*, OCTAVIAN VASILIU** *UMF Carol Davila Bucharest, ** Universitary Military
COGNITIVE-BEHAVIOURAL THERAPY EFFICACY IN MAJOR DEPRESSION WITH ASSOCIATED AXIS II RISK FACTOR FOR NEGATIVE PROGNOSIS DANIEL VASILE*, OCTAVIAN VASILIU** *UMF Carol Davila Bucharest, ** Universitary Military
