Giant invasive spinal schwannomas: definition and surgical management
|
|
|
- Elisabeth Freeman
- 5 years ago
- Views:
Transcription
1 J Neurosurg (Spine 2) 94: , 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D., D.N.B. (NEUROSURG), AND B. RAMAMURTHI, M.S., F.R.C.S. ED. Dr. A. Lakshmipathi Neurosurgical Centre, V.H.S. Medical Centre, Madras, India Object. Confusion exists regarding the term giant spinal schwannoma. There are a variety of nerve sheath tumors that, because of their size and extent, justify the label giant schwannoma. The authors propose a classification system for spinal schwannomas as a means to define these giant lesions. The classification is confined to tumors that are essentially intraspinal, with or without extraspinal components. Lesions that erode the vertebral bodies (VBs) and extend posteriorly and laterally into the myofascial planes are classified as giant invasive spinal schwannomas. Methods. The records of patients with giant invasive spinal schwannoma were analyzed. The radiological features, operative approaches, and intraoperative findings were noted. Ten patients with giant invasive tumors were surgically treated over the last 8 years. Six patients were male. Erosion of the posterior surface of the VBs was the diagnostic finding demonstrated on plain x-ray films. Magnetic resonance imaging delineated the extent of the tumors and helped in preoperative planning. Radical excision of the tumors in multiple stages was possible in eight of the 10 patients. Dural reconstruction was required in four patients. All patients required fusion, and an additional stabilization procedure was undertaken in three patients. Conclusions. The authors conclude that giant invasive schwannomas are uncommon lesions and propose a new classification system. Because of their locally invasive nature and extension in all directions, careful preoperative planning of the surgical approach is very important. Although radical excision is possible and promises good results, recurrences may occur and multiple surgical procedures may be required. KEY WORDS giant schwannoma spine surgical approach reconstructive surgery classification system S PINAL schwannomas comprise approximately 25% of all spinal tumors. 2,5 They are most commonly seen in the thoracic region and are then most commonly found, with almost equal frequency, in the cervical and the lumbar regions. Until this report, no attempt had been made to classify these lesions on the basis of their location and extent. This has resulted in confusion in the use of the term giant spinal schwannoma. By convention, the term refers only to lumbosacral and sacral tumors eroding the VBs and extending into the paraspinal tissues. There are, however, other categories of tumors, that, due to their size and extent, justify the designator giant schwannoma. The authors propose a classification system of spinal schwannomas, in which a giant tumor is defined and discuss the surgical management of patients with giant invasive spinal schwannomas. Clinical Material and Methods The case records of patients with spinal schwannomas surgically treated at our center between 1990 and 1999 Abbreviations used in this paper: MR = magnetic resonance; VB = vertebral body. 210 were analyzed retrospectively. The lesions were diagnosed by radiography, myelography, and/or MR imaging. Classification of Spinal Schwannomas Based on the radiological findings, the authors have devised a classification system of spinal schwannomas (Table 1 and Fig. 1). Giant spinal schwannomas are defined as those that extend over more than two vertebral levels (Type II), those that have an extraspinal extension of more than 2.5 cm (giant dumbbell Type IVb), and those lesions that erode the VBs and extend posteriorly and laterally into the myofascial planes (giant invasive tumors, Type V). In the present study we focus on patients with the giant invasive, or Type V, spinal schwannomas. Results Ten patients underwent resection of their giant invasive schwannomas in the last 8 years (Table 2). They formed 10.9% of the cases of spinal neuromas surgically treated at our center during the same period. Six of the 10 patients were male. The youngest patient was 13 years of age and the oldest was 60 years of age (mean age 33.8 years). Only one of the patients had neurofibromatosis.
2 Giant invasive spinal schwannomas TABLE 1 Classification of benign nerve sheath tumors Classification Type I intraspinal tumor, 2 vertebral segments in length; a: intradural; b: extradural. Type II intraspinal tumor 2 vertebral segments in length (giant tumor) Type III intraspinal tumor w/ extension into nerve root foramen Type IV intraspinal tumor w/ extraspinal extension (dumbbell tumors); a: extraspinal component 2.5 cm; b: extraspinal component 2.5 cm (giant tumor) Type V tumor w/ erosion into the VBs (giant invasive tumor), lat & posterior extentions into myofascial planes Findings on plain radiographs included a widened interpedicular distance, erosion of the pedicle, enlargement of the intervertebral foramen, and erosion of the posterior surface of the VBs to a variable extent. The latter finding was diagnostic of a giant invasive schwannoma. In two patients a total block of the contrast column demonstrated on myelography was the definitive indicator of giant schwannoma. On MR imaging the lesions appeared isointense or of varying intensity on T 1 -weighted images, and the entire extent of the lesion, including the extraspinal extensions and erosion of the VBs, was delineated. Five of the lesions were located in the lumbar region, two each in the thoracic and lumbosacral regions, and one in the cervical region. Three or more operations were performed in three patients, two in four patients, and one in three patients. Radical microscopic excision of the tumor was achieved in eight patients, and dural reconstruction was necessary in four patients. Fusion in which we used autologous bone was performed in all patients. Three patients required an additional stabilization procedure, as it was believed that the spine was unstable. Bed rest for 3 months was ordered for one patient after which mobilization was allowed after application of an external brace. One patient developed a postoperative cerebrospinal fluid leak through the wound, which subsided following repeated lumbar punctures. Follow-up periods ranged from 6 months to 4 years (mean 20 months). One patient with a lumbar tumor developed an asymptomatic recurrence after 3 years and has been advised to undergo repeated surgery. Illustrative Cases Two patients who presented with problems requiring different approaches and management are described in detail. Case 5 This 25-year-old woman presented with a 5-month history of progressive quadriparesis. History. She had undergone two previous surgeries one at age 16 years and one at age 19 years for similar complaints. A myelogram obtained prior to the first operation had demonstrated a total block at the lower border of the C-6 VB. A C3 7 laminectomy had been performed, and radical excision of the intraspinal portion of an intra/ FIG. 1. Diagrammatic representation of the proposed classification of spinal schwannomas Types I to V. Type II (not shown) is an intraspinal schwannoma extending for more than two vertebral segments. See Table 1 for definitions. extradural schwannoma was accomplished. She regained normal power and sensation within 8 months of surgery. At the age of 19 years she was admitted with a progressively increasing swelling in the neck. The lesion was approached anterolaterally, and a near-total excision of the extraspinal schwannoma was achieved. A remnant of the tumor was left at the region of the nerve root foramen. Examination. Plain radiography performed at the present admission demonstrated the C3 7 laminectomy, as well as a swan-neck deformity of the cervical spine with localized porosis of the C-6 VB (Fig. 2 upper left). Magnetic resonance imaging of the cervical spine revealed a lobulated lesion isointense in relation to the spinal cord on T 1 -weighted images and of a mixed intensity on T 2 -weighted images, extending from the lower border of the C-4 VB to the middle of the C-7 VB. The lesion had eroded the C-6 VB and was extending through the left intervertebral foramen into the neck with a large extraspinal component. The swanneck deformity was causing pressure on the cord contralateral to the upper border of C-4, at a level where there was no tumor (Fig. 2 upper right and lower left). 211
3 K. Sridhar, et al. TABLE 2 Characteristics of patients with a giant spinal neurofibroma/schwannoma Case Age (yrs), No. of Stabilization No. Sex Region Ops Required 1 55, M lumbar 3 yes 2 25, M lumbosacral 5 no 3 55, M thoracic 2 no 4 60, M lumbar 2 yes 5 25, F cervical 4 yes 6 15, F lumbar 2 no 7 30, F thoracic 1 no 8 19, M lumbar 1 no 9* 40, F lumbosacral 2 no 10 13, M lumbar 1 no * This patient had neurofibromatosis. Operation. A posterior approach to the tumor was undertaken as the first step. The previous laminectomy wound was reopened only on the left side where the tumor was exiting from the spinal canal. The bone removal was extended laterally to include the facet joints at C-5 and C-6 to facilitate removal of the extraspinal part of the tumor. Radical excision of the intra- and extraspinal portions of the tumor was performed, leaving only tags of lesion in the eroded C-6 VB. A rib graft was used for fusion across the operated levels. The patient was placed in traction postoperatively for 4 days, after which the anterior approach was used, and a three-level corpectomy (C4 6) was performed to correct the swan-neck deformity and to remove the tumor remnants in the C-6 VB. An anterior C3 7 plate was placed to stabilize the spine (Fig. 2 lower right). Follow-Up Course. The patient made excellent progress in the postoperative period and was mobilized wearing a cervical collar on the 3rd postoperative day. At the last follow-up visit, 30 months after surgery, the patient was asymptomatic and neurologically normal. An x-ray film demonstrated good fusion and implant position. Case 6 History. This 15-year-old girl had undergone surgery at another center 1 year prior to presentation to us for back pain, symptoms and signs of a conus medullaris cauda equina lesion, and urinary retention. The lesion was a giant schwannoma of the lumbar spine. An L2 5 laminectomy had been performed, but the surgery was abandoned following decompression of the tumor because the surgeon had believed that the lesion engulfed the nerve roots. Presentation. The patient presented to us with an increasing lower-limb weakness and had received an indwelling catheter. Examination. Plain radiography of the lumbosacral spine demonstrated the L2 5 laminectomy, posterior scalloping of the L-3 and L-4 VBs of greater than 60% of the body, and a scoliotic curve of the lumbar spine. Magnetic resonance imaging demonstrated the multilobulated lesion extending from the upper border of the L-2 VB to the lower border of L-5 (Fig. 3 left). The tumor was shown on MR imaging to be eroding the L-3 and L-4 VBs and extending to the extraspinal tissues on the left side only (Fig. 3 center). The lesion extended through the laminectomy up to the subcutaneous plane. A pseudomeningocoele was observed posterior to the lesion. Operation. The tumor was exposed via a posterolateral approach on the left side where it was exiting from the spinal canal. In addition, the facet joint at that level was also removed. The dura was deficient over most of the lesion, and the tumor was in direct contact with the muscles. Normal dura was exposed at the superior and inferior ends of the lesion as well as the superior and inferior poles of the tumor. Using the operating microscope, the tumor was debulked and space was created to dissect the lesion radically. It was found that the cauda equina was pushed posteriorly and to the right by the lesion. There was no difficulty in dissecting the tumor from the nerve roots, and the tumor was excised radically (Fig. 3 right). The tumor had eroded the VBs up to the anterior vertebral margin, leaving behind a thin shell of bone and intact intervertebral discs. Autologous bone chips were packed into the defect in the VBs. The edges of the normal dura were identified, and using a fascia lata graft, reconstruction of the dural tube was performed. Follow-Up Course. The patient s neurological condition improved in the postoperative period, and by the end of 2 weeks normal power and lower-limb sensation and normal bladder function had returned. The patient was mobilized after 3 months, and she wore a lumbar brace. As of the 18-month follow up, she was mobile and experiencing a minimal residual neurological deficit. Discussion Spinal nerve sheath tumors are most often single, small, benign lesions that are relatively simple to remove and are associated with a good postoperative result. Giant schwannomas are uncommon. The majority of giant spinal schwannomas are dumbbell shaped, which poses difficulty mainly in the radical removal of the extraspinal part of the lesion. Various approaches have been conducted to help remove these tumors totally. 3,4,6 Giant invasive (Type V) schwannomas differ from the other giant schwannomas in that they erode the posterior surface of the VBs, infiltrate through the posterior dura, and invade the myofascial planes while still remaining histologically benign. They are reported most often as case reports, and in many large series of spinal schwannomas the authors make no mention of these lesions. Rao 8 and Levy, et al., 5 while reporting on 80 and 66 spinal schwannomas, respectively, do not refer to these giant tumors. Giant invasive tumors have been described almost exclusively in the lumbosacral spine and as intrasacral lesions. 1,2,7 There have been no reports in the literature of a giant invasive nerve sheath tumor in the thoracic or cervical spine. Giant invasive (Type V) schwannomas make surgery difficult because of their growth in all directions. They extend 1) commonly over more than three vertebral levels; 2) anterolaterally into the extraspinal space via the foramen, which they erode and widen; 3) posteriorly, thinning and attenuating the dura and the posterior elements and, occasionally, extending into the posterior myofascial planes; and 4) anteriorly, eroding the VBs to varying extents. These extensions cause problems for the surgeon in terms of approach, resectability, and stability of the spine. 212
4 Giant invasive spinal schwannomas FIG. 2. Case 5. Imaging studies. Upper Left: Lateral x-ray film of the cervical spine demonstrating evidence of a previous laminectomy, a kyphotic deformity of the spine, and a localized porosis of the C-6 VB. Upper Right: Sagittal T 1 - weighted MR image revealing an intraspinal tumor opposite the C-5 and C-6 VBs and extending anteriorly into the C-6 VB. The kyphotic deformity is causing spinal cord compression opposite the C-4 VB. Lower Left: Axial T 2 -weighted MR image demonstrating the hyperintense tumor extending into and eroding the C-6 VB and extending extraspinally through the left intervertebral foramen. Lower Right: Postoperative lateral x-ray film obtained following radical excision of the tumor via both the posterior and anterior approaches. Correction of the kyphotic deformity was achieved as well as total excision of the tumor with a median corpectomy from C-3 to C-6. An anterior plate was placed from C-2 to C-7. Approach and Resectability Magnetic resonance imaging has made the preoperative planning of giant tumors easier than when myelography was the most commonly used neurodiagnostic tool. The entire extent of the lesion is seen in all three planes, and the relationship of the tumor to the neural elements, vascular structures, and other organs is clearly delineated. Plain radiographs and/or computerized tomography scans reveal clearly the bone destruction and are required to evaluate the stability of the spine. Radical excision is difficult because these tumors lack a capsule that would help in dissecting them from the surrounding structures. It has been the observation of some authors, however, that these tumors often engulf the nerve roots of the cauda equina. 2 We have found that the relationship between the tumor and the neural structures is constant. Depending on the 213
5 K. Sridhar, et al. FIG. 3. Case 6. Magnetic resonance imaging studies. Left: Sagittal T 1 -weighted image demonstrating a mixed-intensity lesion occupying the entire spinal canal from L-2 to L-5 and eroding and extending into the L-3 and L-4 VBs. Center: Axial T 2 -weighted image demonstrating the tumor extending from the spinal canal into the VB, as well as lateral extraspinal extension though the left intervertebral foramen, and posteriorly into the myofascial planes. The tumor is capped posteriorly by a small pseudomeningocele related to previous surgery. Right: Axial T 2 -weighted image revealing total excision of the lesion. There is a meningocele extending laterally through the foramen. The reconstructed dura is seen as a thin line. side of origin of the tumor, the cord/nerve roots are pushed and/or splayed to the opposite direction. On MR imaging it is seen that the tumors extend laterally most often only on one side and that the cord and/or cauda equina is pushed to the opposite side. This relationship is more clearly observed on the axial cuts obtained at either pole of the lesion. It is, therefore, possible to perform a radical excision of the tumor without causing neurological damage. By approaching the lesion in the midline, the surgeon may encounter the splayed nerve roots first and it may appear as though the nerves are engulfed by the lesion. Using a posterolateral approach on the side of the tumor, initial debulking can be performed to reduce the size, create more space, and then allow the tumor to be separated from the neural elements. We have been able to separate the tumor from the cord and/or nerve roots without any difficulty when using this approach. Dissecting the tumors from the surrounding soft tissue may be difficult when the tumors do not have a firm capsule and are vascular. The anatomy of the region is confusing when an essentially intradural tumor is seen at the muscle plane without the dural layer to delineate it. In such cases it is always preferable to take the exposure to the normal dura above and below both poles of the tumor and to start the dissection there so that the anatomy of the lesion is understood before the excision is begun. The tumor may erode into the VBs and may even present as a presacral or retroperitoneal mass. 1,2,7,9 11 The tumor should be followed into the bone and removed. Extraspinal extensions of these tumors are usually multilobulated. Although there is no firm capsule, the surrounding tissues often form a pseudocapsule around the lesion. The bone removal should be extended well lateral into the facet joint and lateral cuts made in the dura to follow the lesion laterally. Occasionally, the paraspinal muscles may have to be divided to reach the far end of the extraspinal lesion. It is possible to excise even large extraspinal extensions when using a high-magnification operating microscope and constantly tipping the operating table. However, even with all these maneuvers, because of the large size, extensive nature, and invasiveness of these tumors, it may not be possible to be certain at surgery that the tumor has been totally removed. The surgeon, therefore, must be aware of the prospect of having to reoperate a number of times. Reconstruction and Stabilization It is important to plan for reconstruction once tumor removal has been achieved. Deficient dura has to be repaired using fascia lata if necessary. Erosion of the VB coupled with removal of the posterior elements with the facet joint at more than one level is likely to leave the spine unstable. Because the VB will slowly reconstitute itself, some surgeons have preferred not to fuse or stabilize the spine. 7 However, if the lesion is in the cervical or upper-lumbar spine, early mobilization may be hazardous if the spinal column has not been stabilized. Erosion of more than 25% of the VB, in our opinion, requires some form of reconstructive procedure. The use of implants, however, is not free of problems, the most important of them being the difficulty of imaging studies during the follow-up period. The surgeon, therefore, has to decide on the use of hardware depending on whether the tumor removal has been radical or not. Results of radical excision of these large tumors have been encouraging, and most patients do well. Recurrences can be managed with repeat surgeries, and at each attempt an aggressive effort should be made to excise the lesion radically. 214
6 Giant invasive spinal schwannomas Conclusions Giant invasive spinal schwannomas are uncommon lesions distinct from other giant spinal schwannomas. Because of their locally invasive nature and extensions in all directions, careful preoperative planning of the surgical approach is very important. Although radical excision of these extensive lesions is possible with good results, they have a tendency to recur, necessitating repeated surgeries. Acknowledgment The authors thank Mr. Srinivasan for his help in preparing the figures and illustrations. References 1. Abernathey CD, Onofrio BM, Scheithauer B, et al: Surgical management of giant sacral schwannomas. J Neurosurgery 65: , Bhatia S, Khosla A, Dhir R, et al: Giant lumbosacral nerve sheath tumors. Surg Neurol 37: , Hakuba A, Komiyama M, Tsujimoto T, et al: Transuncodiscal approach to dumbbell tumors of the cervical spinal canal. J Neurosurg 61: , McCormick PC: Surgical management of dumbbell tumors of the cervical spine. Neurosurgery 38: , Levy WJ, Latchaw J, Hahn JF, et al: Spinal neurofibromas: a report of 66 cases and a comparison with meningiomas. Neurosurgery 18: , Lot G, George B: Cervical neuromas with extradural components: surgical management in a series of 57 patients. Neurosurgery 41: , Piera JB, Durand J, Pannier S, et al: [10 cases of giant lumbosacral neurinoma.] Ann Med Interne (Paris) 126: ,1975 (Fr) 8. Rao SB: Spinal neurinoma. A study of 80 operated cases. Neurol India 23:1 12, Rengachary S, O Boynick P, Batnitzky S, et al: Giant intrasacral Schwannoma: case report. Neurosurgery 9: , Turk PS, Peters N, Libbey NP, et al: Diagnosis and management of giant intrasacral schwannoma. Cancer 70: , Wu WQ: Management of two giant neurilemomas of the cauda equina. South Med J 73: , 1980 Manuscript received May 8, Accepted in final form October 31, Address reprint requests to: K. Sridhar, D.N.B. (Neurosurg.), Dr. A. Lakshmipathi Neurosurgical Centre, V.H.S. Medical Centre, Madras , India. ksree@md2.vsnl.net.in. 215
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Clinico-pathological study of intradural extramedullary spinal tumors
 International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Transparaspinal exposure of dumbbell tumors of the spine
 J Neurosurg 88:106 110, 1998 Transparaspinal exposure of dumbbell tumors of the spine Report of two cases STEPHEN T. ONESTI, M.D., ELY ASHKENAZI, M.D., AND W. JOST MICHELSEN, M.D. Department of Neurological
J Neurosurg 88:106 110, 1998 Transparaspinal exposure of dumbbell tumors of the spine Report of two cases STEPHEN T. ONESTI, M.D., ELY ASHKENAZI, M.D., AND W. JOST MICHELSEN, M.D. Department of Neurological
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT
 IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Wound healing in trophic ulcers in spina bifida patients
 J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass
 , Article ID 953579, 4 pages http://dx.doi.org/10.1155/2014/953579 Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass Jason Hoover 1,2 and Stephen Pirris 3 1 The Texas Brain and Spine Institute,
, Article ID 953579, 4 pages http://dx.doi.org/10.1155/2014/953579 Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass Jason Hoover 1,2 and Stephen Pirris 3 1 The Texas Brain and Spine Institute,
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective Case Analysis Based on Tumor Location and Extension
 ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of 15 Cases
 Asian Spine Journal Vol. 6, No. 1, pp 43~49, 2012 http://dx.doi.org/10.4184/asj.2012.6.1.43 Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of
Asian Spine Journal Vol. 6, No. 1, pp 43~49, 2012 http://dx.doi.org/10.4184/asj.2012.6.1.43 Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of
ASJ. Myxopapillary Ependymoma of the Cauda Equina in a 5-Year-Old Boy. Asian Spine Journal. Introduction
 Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
Codes for Back and Spinal Procedures
 20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Coding Companion for Neurosurgery/Neurology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Neurosurgery/Neurology A comprehensive illustrated guide to coding and reimbursement 2011 Contents Getting Started with Coding Companion...i Skin...1 Repair...5 General Musculoskeletal...27
Coding Companion for Neurosurgery/Neurology A comprehensive illustrated guide to coding and reimbursement 2011 Contents Getting Started with Coding Companion...i Skin...1 Repair...5 General Musculoskeletal...27
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Penetrating Thoracic Spinal Injury with Impacted Glass Fragment
 case report Penetrating Thoracic Spinal 10.5005/jp-journals-10039-1040 Injury with Impacted Glass Fragment Penetrating Thoracic Spinal Injury with Impacted Glass Fragment 1 Vinu V Gopal, 2 K Mahadevan
case report Penetrating Thoracic Spinal 10.5005/jp-journals-10039-1040 Injury with Impacted Glass Fragment Penetrating Thoracic Spinal Injury with Impacted Glass Fragment 1 Vinu V Gopal, 2 K Mahadevan
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
RETROLISTHESIS. Retrolisthesis. is found mainly in the cervical spine and lumbar region but can also be often seen in the thoracic spine
 RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
Cervical dumbbell meningioma and thoracic dumbbell schwannoma in a patient with neurofibromatosis
 Clinical Neurology and Neurosurgery 107 (2005) 253 257 Case report Cervical dumbbell meningioma and thoracic dumbbell schwannoma in a patient with neurofibromatosis Jin-Cherng Chen a, Sheng-Hong Tseng
Clinical Neurology and Neurosurgery 107 (2005) 253 257 Case report Cervical dumbbell meningioma and thoracic dumbbell schwannoma in a patient with neurofibromatosis Jin-Cherng Chen a, Sheng-Hong Tseng
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Thoracoscopic surgical resection of thoracic neurogenic tumors
 Neurosurg Focus 7 (5):Article 1, 1999 Thoracoscopic surgical resection of thoracic neurogenic tumors Patrick P. Han, M.D., and Curtis A. Dickman, M.D. Division of Neurological Surgery, Barrow Neurological
Neurosurg Focus 7 (5):Article 1, 1999 Thoracoscopic surgical resection of thoracic neurogenic tumors Patrick P. Han, M.D., and Curtis A. Dickman, M.D. Division of Neurological Surgery, Barrow Neurological
Stab wound of the neck: potential pitfalls in management
 Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Bony framework of the vertebral column Structure of the vertebral column
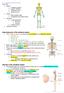 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Spinal schwannoma: Size has no correlation with presentation and outcome
 Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Giant invasive spinal schwannoma in children: a case report and review of the literature
 Vadivelu et al. Journal of Medical Case Reports 2013, 7:289 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant invasive spinal schwannoma in children: a case report and review of the literature
Vadivelu et al. Journal of Medical Case Reports 2013, 7:289 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant invasive spinal schwannoma in children: a case report and review of the literature
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
nerve sheath tumors: Analysis of 32 cases
 C 1 : Analysis of 32 cases Original Article Parmatma Maurya, Kulwant Singh, Vivek Sharma Department of Neurosurgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi - 221 005, India Abstract
C 1 : Analysis of 32 cases Original Article Parmatma Maurya, Kulwant Singh, Vivek Sharma Department of Neurosurgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi - 221 005, India Abstract
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Schwannoma of T12 vertebra: case report and review of literature
 Sarcoma (2000) 4, 185± 190 CASE REPORT Schwannoma of T12 vertebra: case report and review of literature P. RAMASAMY, I. SHACKLEFORD & M. AL JAFARI Warrington General Hospital,WarringtonWA5 1QG, UK Abstract
Sarcoma (2000) 4, 185± 190 CASE REPORT Schwannoma of T12 vertebra: case report and review of literature P. RAMASAMY, I. SHACKLEFORD & M. AL JAFARI Warrington General Hospital,WarringtonWA5 1QG, UK Abstract
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Anatomy of the Nervous System. Brain Components
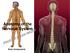 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION
 CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
Spinal meningioma imaging
 Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Case Report One-Step Posterior and Anterior Combined Approach for L5 Retroperitoneal Schwannoma Eroding a Lumbar Vertebra
 Case Reports in Surgery Volume 2016, Article ID 1876765, 7 pages http://dx.doi.org/10.1155/2016/1876765 Case Report One-Step Posterior and Anterior Combined Approach for L5 Retroperitoneal Schwannoma Eroding
Case Reports in Surgery Volume 2016, Article ID 1876765, 7 pages http://dx.doi.org/10.1155/2016/1876765 Case Report One-Step Posterior and Anterior Combined Approach for L5 Retroperitoneal Schwannoma Eroding
Neuroimaging. spine / spinal cord
 Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
MR imaging the post operative spine - What to expect!
 MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set
 Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set Benzel, E ISBN-13: 9781437705874 Table of Contents SECTION 1 - HISTORY 1 - History 2 - History of Spine Instrumentation -
Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set Benzel, E ISBN-13: 9781437705874 Table of Contents SECTION 1 - HISTORY 1 - History 2 - History of Spine Instrumentation -
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Long segment composite split cord malformation with double bony spur
 Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
MEDICAL IMAGING OF THE VERTEBRAE
 MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
Symptomatic Vertebral Artery Loop: A case report and review of literature
 Symptomatic Vertebral Artery Loop: A case report and review of literature Ahmed Doweidar 1*, Saeed Al-Sayed 2, Salwa Al-Kandery 1 1. Department of Clinical Radiology, Al-Razi hospital, Kuwait, Kuwait 2.
Symptomatic Vertebral Artery Loop: A case report and review of literature Ahmed Doweidar 1*, Saeed Al-Sayed 2, Salwa Al-Kandery 1 1. Department of Clinical Radiology, Al-Razi hospital, Kuwait, Kuwait 2.
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island. Long Island
 Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Regions of the Spine
 Anatomy The spine is a very complex mechanical structure that is highly flexible yet very strong and stable. In the normal spine, regardless of your position or activity, including sleeping, there is always
Anatomy The spine is a very complex mechanical structure that is highly flexible yet very strong and stable. In the normal spine, regardless of your position or activity, including sleeping, there is always
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
A Patient s Guide to Spinal Tumors
 A Patient s Guide to Spinal Tumors 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Spinal Tumors 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass
 32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
ESCOME Pre-Course Outline (v1.09)
 ESCOME Pre-Course Outline (v1.09) 1. Basics of Spinal Disorders Introduction to Spinal Surgery Spinal Anatomy Introduction to Vertebral Anatomical Concepts Anatomy and Function of Joints and Ligaments
ESCOME Pre-Course Outline (v1.09) 1. Basics of Spinal Disorders Introduction to Spinal Surgery Spinal Anatomy Introduction to Vertebral Anatomical Concepts Anatomy and Function of Joints and Ligaments
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
ASJ. A Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia. Asian Spine Journal. Introduction
 sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Tumors of the posterior mediastinum, located in the paravertebral
 Technique of Thoracoscopic Resection of Posterior Mediastinal Tumors Michael F. Reed, MD Tumors of the posterior mediastinum, located in the paravertebral sulcus, account for about 25% of all mediastinal
Technique of Thoracoscopic Resection of Posterior Mediastinal Tumors Michael F. Reed, MD Tumors of the posterior mediastinum, located in the paravertebral sulcus, account for about 25% of all mediastinal
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness
 3 7 A B Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness (case 1). MR sagittal image shows a posterior epidural mass (solid black arrows) showing iso intensity on T1-weighted image
3 7 A B Fig. 1. A 58-year-old woman with severe lower extremity pain and weakness (case 1). MR sagittal image shows a posterior epidural mass (solid black arrows) showing iso intensity on T1-weighted image
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Open surgery for posterior mediastinal neurogenic tumors
 Review Article Page 1 of 5 Open surgery for posterior mediastinal neurogenic tumors Erkan Kaba 1, Mazen Rasmi Alomari 2, Alper Toker 2 1 Department of Thoracic Surgery, Istanbul Bilim University Medical
Review Article Page 1 of 5 Open surgery for posterior mediastinal neurogenic tumors Erkan Kaba 1, Mazen Rasmi Alomari 2, Alper Toker 2 1 Department of Thoracic Surgery, Istanbul Bilim University Medical
C-THRU Anterior Spinal System
 C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
Sir William Asher ANATOMY
 SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Advantages of MISS. Disclosures. Thoracolumbar Trauma: Minimally Invasive Techniques. Minimal Invasive Spine Surgery 11/8/2013.
 3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report
 Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
