White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term
|
|
|
- Barnaby O’Connor’
- 5 years ago
- Views:
Transcription
1 AJNR Am J Neuroradiol 24: , May 2003 White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term Terrie E. Inder, Nigel J. Anderson, Carole Spencer, Scott Wells, and Joseph J. Volpe BACKGROUND AND PURPOSE: The accuracy of cranial sonography (US) in characterizing white matter (WM) injury in the premature infant is unclear. This study was aimed to assess the sensitivity and specificity of serial cranial US during the first 6 weeks of life in comparison to MR imaging at term (week of expected delivery) in characterizing the presence of WM injury in a cohort of 96 very low birth weight (VLBW) infants. METHOD: A blinded investigator reviewed serial cranial sonograms for the presence of WM echolucency and echodensity, including its duration and extent. These abnormalities were compared with a second independent investigator s evaluation to determine the sensitivity and specificity of cranial WM abnormalities at US. RESULTS: The presence of prolonged echodensity (>7 days) in the WM on neonatal cranial sonograms demonstrated low sensitivity (26%) and a low positive predictive value (36%) for the presence of noncystic WM injury, as detected on MR images at term. Extensive cystic lesions detected on MR images were all identified during earlier cranial US. CONCLUSION: Neonatal cranial US of the VLBW infant demonstrates high reliability in the detection of cystic WM injury but has significant limitations in the demonstration of noncystic WM injury. This deficiency of neonatal cranial US is important, because noncystic WM injury is considerably more common than cystic WM injury. Cranial sonography (US) is the most widely used neuroimaging procedure in the study of the premature infant. The technique is readily applied at the bedside, does not involve ionizing radiation, is costeffective, and can be used sequentially. In recent years, the particular importance of cerebral white matter (WM) injury in the genesis of neurologic sequelae in the premature infant has been increasingly recognized (1). WM injury in the premature infant is characterized by focal necroses deep in the WM, with Received August 20, 2002; accepted after revision December 16. From the Murdoch Children s Research Institute (T.E.I.), and the Howard Florey Institute (T.E.I.), Melbourne, Australia; the Department of Radiology and NICU, Christchurch Hospital, New Zealand (N.J.A., C.S., S.W.); and the Department of Neurology, Children s Hospital, Harvard Medical School, Boston (T.E.I., J.J.V.). Supported by grants from the Neurological Foundation of New Zealand, Health Research Council of New Zealand and Lottery Health of New Zealand. Presented at the Society for Pediatric Research, Baltimore, MD, May Address reprint requests to Terrie Inder, MD, 2nd Floor, Royal Children s Hospital, Flemington Road, Parkville VIC 3052, Australia. American Society of Neuroradiology subsequent cyst formation, and the more common, diffuse and noncystic WM injury characterized by loss of early differentiating oligodendrocytes, astrogliosis, and subsequent impairment of myelination (1). Although cranial US has been shown to be reliable in the detection of focal areas of cystic WM injury (2 5), the value of this imaging technique in detecting the more common diffuse, noncystic WM injury is unclear. MR imaging has previously been compared with cranial US for the detection of cerebral injury in the premature infant (6 9). The investigators concluded that MR imaging was superior in the definition of the extent of WM injury and associated abnormalities, such as abnormal signal intensity in the posterior limb of the internal capsule. All of these studies, however, were retrospective and related the MR imaging and cranial US findings in relatively small, select clinical cohorts of premature infants with vastly mixed cerebral lesions. Thus, our prospective study included an unselected cohort of very low birth weight infants (VLBW). Our aim was to define the sensitivity and specificity of cranial WM abnormalities found during serial US studies in the first 6 weeks of life for the detection of both cystic and noncystic WM injury observable at term (week of expected due date) on MR images. 805
2 806 INDER AJNR: 24, May 2003 TABLE 1: Characteristics of the total cohort of VLBW No. of Infants Characteristic (n 96) Birth weight Gestational age, weeks Male/Female 48/48 Singletons 64 Intrauterine growth restriction 25 Prolonged Ruptured Membranes 22 Oxygen therapy, days Mean arterial pressure 30 mmhg 18* Inotropic use for low blood pressure 34 Patent ductus arteriosus 45 Intraventricular hemorrhage grade III or IV 4 Pneumothorax 6 * Of 66 infants with intra-arterial catheter monitoring. Confirmed at echocardiography. Methods Subjects From November 1998 to December 2000, 100 consecutively born, premature infants with VLBW, or a birth weight less than 1500 g, were recruited into a study of advanced imaging techniques for an assessment of brain injury in the premature infant. These infants represented 98% of eligible infants admitted to a regional level III neonatal intensive care unit. The mean gestational age of the infants was 27.9 weeks 2.4, with mean birth weight of 1063 g 292. The characteristics of these infants are summarized in Table 1. Permission for this study was granted by the Canterbury Regional Health Research Ethics Committee, and written parental consent was obtained for each infant. Cranial US Sequential cranial US scans were obtained by using a standardized protocol, with images acquired at a minimum of the first 48 hours, at 5 7 days, and at 4 and 6 weeks of age. If any abnormality was detected, weekly US assessments were undertaken. Sonograms were acquired with 7.5- or 8.5-MHz probes by using various sonography machines (XP-10, Aspen, and Sequoia; Acuson, Mountain View, CA). A standardized series of images was obtained at every sonographic examination. Six coronal views (at the level of the orbits, middle cerebral arteries, third ventricle, fourth ventricle, bodies of lateral ventricles, and centrum semiovale), and five sagittal-parasagittal views (midline, ventricles, and paraventricular WM) were obtained via the anterior fontanelle. Three coronal images (occipital horns, splenium, and centrum semiovale) and three sagittalparasagittal images (midline, trigone, and occipital horns) were obtained via the posterior fontanelle. WM echogenicity in frontal regions was assessed on the anterior fontanelle sonograms. In parieto-occipital regions, the echogenicity was assessed from the anterior fontanelle approach and corroborated with the posterior fontanelle view. Analysis of Cranial Sonograms An experienced radiologist (N.J.A.) who was blinded to the infant s clinical course and to the MR imaging results analyzed all cranial US scans. Blinded repeat readings were undertaken for both cranial US and MR imaging to determine the validity and reliability of the measures. Although the cranial US scans were analyzed extensively, for the purposes of this study, WM echodensities and echolucencies were emphasized. Abnormal periventricular echodensity was defined as abnormal signal intensity in the periventricular WM with signal intensity characteristics greater than those in the choroid plexus (10). Peritrigonal flush was excluded. Echodensity in the periventricular WM was classified as absent, transient ( 7 days in duration), prolonged ( 7 days n duration), or were described as echodensities evolving to echolucencies (cysts) (Fig 1). The extent of the WM echodensity or echolucency was recorded by the regions involved: frontal, parietal, or occipital. The number and size of the cystic lesions were classified as single or multiple and as small, moderate, or large (11). MR Imaging MR imaging was performed with a 1.5-T system (Signa; GE Medical Systems, Milwaukee, WI). For the acquisition of the primary MR imaging data, two imaging modes were applied: a three-dimensional (3D) Fourier-transform spoiled gradientrecalled (SPGR) sequence (1.5-mm coronal sections; flip angle, 45 ; TR/TE, 35/5; field of view, 18 cm; matrix, ) and a double-echo (proton density [PD] and T2-weighted) spinecho sequence (3-mm axial sections; 3,000/36 and 162; field of view, 18 cm; matrix, , interleaved acquisition). An experienced neuroradiologist (S.W.) evaluated the MR images in a blinded manner for WM abnormality. Although the MR images were analyzed extensively, for the purposes of this study, we focused our definition of WM injury on the presence and severity of WM signal intensity abnormalities. The MR imaging diagnosis of WM signal intensity abnormality required T1 hyperintensity in the absence of marked T2 hypointensity in the periventricular WM; this was interpreted as astrogliosis (12). Areas of notable T1 hyperintensity and substantial T2 hypointensity were interpreted as signal intensity abnormalities suggestive of foci of hemorrhage. WM signal intensity was classified as normal, a focal signal intensity abnormality (eg, involving one lobar region only), an extensive signal intensity abnormality (eg, involving more than one lobar region), or a cystic change. We took the license of using a pathologic term cystic change for the MR imaging abnormality that is indicative of areas of tissue dissolution (characteristic of cystic periventricular leukomalacia [PVL]) Representative sagittal MR images in the infants with these grades of WM injury are shown in Figure 2. Statistical Analysis The value of cranial US as a predictor of WM abnormality, as shown on MR images at term, was assessed by calculating the sensitivity, specificity, positive predictive value, and negative predictive value of cranial US findings. Results Ninety-six infants completed the protocol of all cranial US scans during their admission. Four infants were excluded, because they were transferred to other units during their admission. MR Imaging Findings At term, 38 infants (40%) had MR imaging findings indicative of WM injury (Fig 1B D, Table 2). A total of 18 infants (19%) had extensive WM signal intensity abnormalities or cystic WM injury on MR images (Table 2). Fourteen of these infants had extensive signal intensity abnormality (Fig 2C), usually with loss of WM volume and ventriculomegaly. The remaining four infants had cystic WM injury: two with bilateral cystic PVL, one with periventricular hemorrhagic infarction and a unilateral WM cyst, and one
3 AJNR: 24, May 2003 NEONATAL WHITE MATTER INJURY 807 Representative cranial sonograms. A, Normal image, coronal view. B, Flaring in the periventricular WM, coronal image. C, Cystic PVL with a cystic abnormality in a region of a signal intensity abnormality, axial view. FIG 1. FIG 2. Representative sagittal T1- weighted MR images (3-mm sagittal T 1 ; 550/12; FOV, 18 cm) in premature infants obtained at term. A, Normal image. B, Focal signal intensity abnormality (arrow). C, Extensive signal intensity abnormality (arrow). D, Cystic change (arrow). with severe posthemorrhagic ventriculomegaly and a single small periventricular cyst. The presence of cystic change in the WM is illustrated in Figure 2D. Cranial US Findings Forty infants (42%) had persistently normal cranial US findings (Table 3). In 22 infants (23%), prolonged echodensities ( 7 days) (n 19) or echodensities evolved into echolucencies (cysts) in the periventricular WM (n 3) (Table 3). The distribution of echodensities or echolucencies in the periventricular WM were found to be frontal-parietal-occipital (n 4), frontoparietal (n 1), parietal-occipital (n 8), frontal (n 2), parietal (n 4), or isolated occipital (n 3). The infants with echolucencies had a single encephalomalacic frontal cyst (secondary to apparent parenchymal hemorrhagic infarction, n 1), multiple small and large parietal-occipital cysts (n 2), or a single parietal cystic (n 1). Sensitivity, Specificity, and Predictive Values of Cranial US for WM Injury Of the 74 infants with normal neonatal cranial US findings or only transient echodensity ( 7 days) on
4 808 INDER AJNR: 24, May 2003 TABLE 2: Results of neonatal cranial US and MRI at term Cranial US Finding Normal (n 58) No. of Infants with MRI WM Finding Focal Signal Abnormality (n 20) Extensive Signal Abnormality (n 14) Normal (n 40) Transient echodensity (n 34) Prolonged echodensity (n 19) Echolucencies (n 3) Cystic Change (n 4) TABLE 3: Statistical comparison of neonatal cranial US and MRI findings at term Neonatal Cranial US Finding MRI Finding at Term Sensitivity Specificity Positive Predictive Value Negative Predictive Value No echodensity or transient echodensity Normal WM or focal signal intensity 82% 44% 86% 36% 7 days abnormality Prolonged echodensity 7 days Extensive signal abnormality or cystic 26% 85% 36% 82% change Echolucency Cystic change 75% 100% 100% 98% serial cranial sonograms, at-term MR images in 10 (14%) showed evidence of notable WM injury, with an extensive signal intensity abnormality or cystic injury (Table 2). Of the 22 infants with more overt WM abnormalities on cranial sonograms, that is, prolonged echodensity ( 7days) or echolucency in the periventricular WM, 14 infants (64%) had normal or only focal signal intensity changes in the WM on MR images at term. The remaining eight infants with these WM abnormalities on cranial US scans had extensive or cystic WM injury on MR images at term (Table 2). Of the 18 infants with extensive or cystic WM injury during MR imaging at term, only eight infants had prominent abnormalities (prolonged echodensity or echolucencies), detected with cranial US during their neonatal course, while 10 infants had either normal US findings or transient echodensity ( 7 days) (Table 2). Neonatal cranial US results were abnormal in the four infants, with the most severe WM injury; findings included bilateral cystic WM injury in the two infants with severe PVL, cystic change with apparent periventricular hemorrhagic infarction in one infant, and severe posthemorrhagic ventriculomegaly in one infant. Cranial US did not depict the single minor cyst in the infant with severe posthemorrhagic ventriculomegaly, but it accurately depicted all other cystic lesions. The sensitivity of the prominent neonatal cranial US abnormality of prolonged echodensity ( 7 days) for overt WM injury on MR images at term, as manifested by extensive signal intensity abnormality or cystic change, was only 26% (Table 3). Moreover, the positive predictive value of this US finding was only 36%. For cystic changes on MR images at term, cranial US was more useful; that is, echolucency on US scans had a sensitivity of 75% and a specificity of 100% with high positive and negative predictive values (Table 3). No substantial alteration in these results occurred with an analysis of the extent of the cranial US abnormality. The sensitivity of normal cranial US findings or the finding of only transient echodensities for the finding of normal WM or only focal signal intensity abnormality on MR images at term was 82% (Table 3). However, the specificity was only 44%, and the negative predictive value was only 36%. Discussion To our knowledge, this study of 96 premature infants is the largest published prospective study of the accuracy of serial neonatal cranial US in the detection of cerebral WM injury, as identified with MR imaging at term. This study revealed several findings of clinical relevance. First, the findings show that cranial US has poor sensitivity for the detection of WM injury. In approximately 55% of infants with extensive signal intensity abnormalities or cystic changes in the cerebral WM, as shown with MR imaging at term, neonatal cranial US findings were either entirely normal or consisted of only transient echodensity. Thus, cranial US is not an adequate screening method for WM injury in the VLBW infant. Second, our findings showed that the cranial US abnormality of prolonged echodensity ( 7 days) demonstrated a high false-positive rate with a low positive predictive value. Thus, only approximately 26% (five of 19) of infants with prolonged echodensity had an extensive signal intensity abnormality or cystic WM injury on MR images at term. In contrast to the poor sensitivity of the finding of prolonged echodensity in the prediction of WM injury, the cranial US finding of echolucency was sensitive for cystic WM injury. Nevertheless, based on MR imaging results at term, cystic WM injury occurred in only four of the 96 infants in this study, whereas extensive noncystic WM injury occurred in 14. This study documents the low sensitivity of serial cranial US for the detection of WM injury in the
5 AJNR: 24, May 2003 NEONATAL WHITE MATTER INJURY 809 premature infant during the first 6 weeks of life. These findings are entirely consistent with those of previous correlative neuropathologic studies demonstrating that as few as 30% of WM injuries, especially small areas of necrosis, diffuse gliosis, and myelin loss, are consistently detected in vivo with US (2 5). Our data are also consistent with those of previously published studies comparing cranial US and MR imaging in the premature infant. In a recent study of 32 VLBW infants, a sensitivity of 0.5 was found for a moderate or severe degree of echodensity with single cranial US (at days 1 95 of life) in the detection of simultaneous WM signal intensity abnormalities on MR images (6). In that study, a WM signal intensity abnormality was defined as diffuse, excessive, hyperintense area on T2-weighted MR images, a finding observed in nearly 80% of the infants at term equivalent. The frequency of this MR signal intensity abnormality at term equivalent was greater than at the earlier time points (25% in the first four postnatal days, 53% at postnatal days 7 95 but 37 weeks postconceptional age). Our study differs notably from this other investigation in that our hypothesis was defined a priori to examine the relationship of standard serial cranial US assessments in the first 6 weeks of life with MR imaging defined WM injury at term, as manifested by more definable focal or extensive signal intensity abnormalities or cystic change (Fig 1). By term equivalent, the extent of WM injury is more clearly established with better delineation of cystic lesions and signal intensity abnormalities on both T1- and T2-weighted images, as well as the loss of WM volume with secondary ventriculomegaly. Moreover, in our study, we wished to address the accuracy of the finding of prolonged echodensity ( 7 days) on serial cranial sonograms in the first 6 weeks of life, rather than the degree of echodensity on a single scan at a random time interval in the neonatal course, in predicting the presence and severity of WM injury. The cranial US finding of prolonged echodensities demonstrated a low positive predictive value for the presence of extensive signal intensity abnormality in the cerebral WM at term. The detection of prolonged echodensities in the periventricular WM on cranial sonograms in the premature infant has been considered an important abnormal finding (10). However, echodensities in the posterior parietal region without any neuropathologic correlate (13) are common in the preterm infant. Our demonstration of the low positive predictive value of cranial US is also consistent with the findings of a recent study of 34 premature infants with a birth weight less than 1750 g (8). In this earlier report, WM findings from serial cranial US scans were compared with those of a single MR image obtained during the neonatal period (mean age at MR imaging, 18.7 days; mean gestational age, 33.2 weeks). In the 10 infants with prolonged WM echodensities ( 7 days), only two had definite WM injury on neonatal MR images. Conclusion Our study of a large unselected cohort of VLBW infants shows that the finding of cranial US WM echodensities lacks sensitivity and positive predictive value for the presence of prominent WM injury, as defined by means of MR imaging at term. Our findings are consistent with related observations from neuropathologic studies and previous smaller published imaging series and emphasize the appreciable limitations of this bedside technology in the diagnosis of WM injury. Such limitations restrict the clinician s ability to used cranial US to accurately diagnose this common cerebral disease in high-risk populations of premature infants. Acknowledgments We are grateful to the Neurologic Foundation of New Zealand, Health Research Council, and Lottery Health for their funding support; to the Canterbury District Health Board and the Christchurch Womens Health Service for their support; and to the Canterbury Radiology Group, Christchurch, New Zealand for their assistance with the acquisition of the MR images. References 1. Volpe JJ. Neurology of the Newborn. 4th ed. Philadelphia: WB Saunders, Hope PL, Gould SJ, Howard S, Hamilton PA, Costello AM, Reynolds EO. Precision of ultrasound diagnosis of pathologically verified lesions in the brains of very preterm infants. Dev Med Child Neurol 1988;30: Paneth N, Rudelli R, Monte W, et al. White matter necrosis in very low birth weight infants: neuropathologic and ultrasonographic findings in infants surviving six days or longer. J Pediatr 1990;116: Carson SC, Hertzberg BS, Bowie JD, Burger PC. Value of sonography in the diagnosis of intracranial hemorrhage and periventricular leukomalacia: A postmortem study of 35 cases. Am J Neuroradiol 1990;155: Adcock LM, Moore PJ, Schlesinger AE, Armstrong DL. Correlation of ultrasound with postmortem neuropathologic studies in neonates. Pediatr Neurol 1998;19: Maalouf EF, Duggan PJ, Counsell S, et al. Comparison of findings on cranial ultrasound and magnetic resonance imaging in preterm infants. Pediatrics 2001;107: Roelants-Van Rijn AM, Groenendaal F, Beek FJA, Eken P, van Haastert IC, de Vries LS. Parenchymal brain injury in the preterm infant: comparison of cranial ultrasound, MRI and neurodevelopmental outcome. Neuropediatrics 2001;32: van Wezel-Meijler G, van der Knaap MS, Oosting J, et al. Predictive value of neonatal MRI as compared to ultrasound in premature infants with mild periventricular white matter changes. Neuropediatrics 1999;30: Childs AM, Cornette L, Ramenghi LA, et al. Magnetic resonance and cranial ultrasound characteristics of periventricular white matter abnormalities in newborn infants. Clin Radiol 2001;56: Goveart P, De Vries LS. Section V, An Atlas of Neonatal Brain. London: MacKeith Press, Holling EE, Leviton A. Characteristics of cranial ultrasound white matter echolucencies that predict disability: a review. Dev Med Child Neurol 1998;41: Schouman-Claeys E, Henry-Feugeas MC, Roset F, et al. Periventricular leukomalacia: correlation between MR imaging and autopsy findings during the 1st 2 months of life. Radiology 1993;189: Di Pietro MA. The periventricular echogenic blush on cranial ultrasonography. AJR Am J Roentgenol 1983;141:851
P eriventricular leucomalacia (PVL), which is characterised
 F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
I mprovements in perinatal and neonatal care have contributed
 ORIGINAL ARTICLE Posthaemorrhagic ventricular in the premature infant: natural history and predictors of outcome B P Murphy, T E Inder, V Rooks, G A Taylor, N J Anderson, N Mogridge, L J Horwood, J J Volpe...
ORIGINAL ARTICLE Posthaemorrhagic ventricular in the premature infant: natural history and predictors of outcome B P Murphy, T E Inder, V Rooks, G A Taylor, N J Anderson, N Mogridge, L J Horwood, J J Volpe...
Extremely preterm infants are at high risk of brain injury
 ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
During the past several decades, neonatal medicine has advanced
 Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
Ultrasound diagnosis and neurodevelopmental outcome of localised and extensive cystic periventricular leucomalacia
 Arch Dis Child Fetal Neonatal Ed 2001;84:F151 F156 F151 ORIGINAL ARTICLES Department of Neonatology, Jeanne de Flandre s Hospital, Lille, France V Pierrat C Duquennoy N Guilley Department of Neonatology,
Arch Dis Child Fetal Neonatal Ed 2001;84:F151 F156 F151 ORIGINAL ARTICLES Department of Neonatology, Jeanne de Flandre s Hospital, Lille, France V Pierrat C Duquennoy N Guilley Department of Neonatology,
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography
 Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
 Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Ultrasound examination of the neonatal brain
 Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review
 Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review Poster No.: C-2615 Congress: ECR 2013 Type: Educational Exhibit Authors: S. E. Vazquez, R. E. Ochoa Albíztegui
Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review Poster No.: C-2615 Congress: ECR 2013 Type: Educational Exhibit Authors: S. E. Vazquez, R. E. Ochoa Albíztegui
Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants?
 Neuroradiology (2010) 52:397 406 DOI 10.1007/s00234-010-0668-7 PAEDIATRIC NEURORADIOLOGY Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants? Lara M.
Neuroradiology (2010) 52:397 406 DOI 10.1007/s00234-010-0668-7 PAEDIATRIC NEURORADIOLOGY Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants? Lara M.
Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants
 The new england journal of medicine original article Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants Lianne J. Woodward, Ph.D., Peter J. Anderson, Ph.D., Nicola C. Austin, M.D.,
The new england journal of medicine original article Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants Lianne J. Woodward, Ph.D., Peter J. Anderson, Ph.D., Nicola C. Austin, M.D.,
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY
 Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
ECMUS The Safety Committee of EFSUMB : Tutorial
 Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review
 Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Posterior Fontanelle Sonography: An Acoustic Window into the Neonatal Brain
 AJNR Am J Neuroradiol 25:1274 1282, August 2004 Posterior Fontanelle Sonography: An Acoustic Window into the Neonatal Brain Flavia Correa, Goya Enríquez, José Rosselló, Javier Lucaya, Joaquim Piqueras,
AJNR Am J Neuroradiol 25:1274 1282, August 2004 Posterior Fontanelle Sonography: An Acoustic Window into the Neonatal Brain Flavia Correa, Goya Enríquez, José Rosselló, Javier Lucaya, Joaquim Piqueras,
Neonatal Periventricular Leukomalacia: Real-Time
 383 Neonatal Periventricular Leukomalacia: Real-Time Sonographic Diagnosis with CT Correlation Peter P. Chow 1. 2 J. Gerard Horgan 1, 3 Kenneth J. W. Taylor 1 The utility of real-time sonography in the
383 Neonatal Periventricular Leukomalacia: Real-Time Sonographic Diagnosis with CT Correlation Peter P. Chow 1. 2 J. Gerard Horgan 1, 3 Kenneth J. W. Taylor 1 The utility of real-time sonography in the
Prevalence of "Compressed" and Asymmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic
 Prevalence of "Compressed" and symmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic Study 149 Patricia Winchester 1 Paula W. rill1 Rebecca Cooper2 lfred N. Krauss 2 Hart dec Peterson
Prevalence of "Compressed" and symmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic Study 149 Patricia Winchester 1 Paula W. rill1 Rebecca Cooper2 lfred N. Krauss 2 Hart dec Peterson
Chapter 5. Lara M. Leijser Francisca T. de Bruïne Sylke J. Steggerda Jeroen van der Grond Frans J. Walther Gerda van Wezel-Meijler
 Chapter 5 Brain imaging findings in very preterm infants throughout the neonatal period: Part I. Incidences and evolution of lesions, comparison between ultrasound and MRI Lara M. Leijser Francisca T.
Chapter 5 Brain imaging findings in very preterm infants throughout the neonatal period: Part I. Incidences and evolution of lesions, comparison between ultrasound and MRI Lara M. Leijser Francisca T.
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection
 Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
Chapter 3. Neonatal cranial ultrasonography: how to optimize its performance
 Chapter 3 Neonatal cranial ultrasonography: how to optimize its performance Sylke J. Steggerda Lara M. Leijser Frans J. Walther Gerda van Wezel-Meijler Early Human Development 2009; 85(2): 93-99 Chapter
Chapter 3 Neonatal cranial ultrasonography: how to optimize its performance Sylke J. Steggerda Lara M. Leijser Frans J. Walther Gerda van Wezel-Meijler Early Human Development 2009; 85(2): 93-99 Chapter
leucomalacia: ultrasound and autopsy correlation
 Archives of Disease in Childhood, 1986, 61, 1203-1207 Intraventricular haemorrhage and periventricular leucomalacia: ultrasound and autopsy correlation J Q TROUNCE, D FAGAN, AND M I LEVENE Department of
Archives of Disease in Childhood, 1986, 61, 1203-1207 Intraventricular haemorrhage and periventricular leucomalacia: ultrasound and autopsy correlation J Q TROUNCE, D FAGAN, AND M I LEVENE Department of
The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1
 9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
Cranial ultrasound abnormalities in full term infants in a postnatal ward: outcome at 12 and 18 months
 F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
The rationale for routine cerebral ultrasound in premature infants
 Pediatr Radiol (2015) 45:646 650 DOI 10.1007/s00247-014-2985-1 RESEARCH FORUM The rationale for routine cerebral ultrasound in premature infants Maria I. Argyropoulou & Corinne Veyrac Received: 4 October
Pediatr Radiol (2015) 45:646 650 DOI 10.1007/s00247-014-2985-1 RESEARCH FORUM The rationale for routine cerebral ultrasound in premature infants Maria I. Argyropoulou & Corinne Veyrac Received: 4 October
Periventricular white matter injury, that is, periventricular
 ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation
 Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
P rominent Extraaxial CSF Space on Cranial Ultra s o u n d in Infants: C o r relation with Neuro d evelopmental Outc o m e 1
 P rominent Extraaxial CSF Space on Cranial Ultra s o u n d in Infants: C o r relation with Neuro d evelopmental Outc o m e 1 Bokyung Kim Han, M.D., Mu n hyang Lee, M.D. 2, Hye - Kyung Yoon, M.D., Kyung-Jae
P rominent Extraaxial CSF Space on Cranial Ultra s o u n d in Infants: C o r relation with Neuro d evelopmental Outc o m e 1 Bokyung Kim Han, M.D., Mu n hyang Lee, M.D. 2, Hye - Kyung Yoon, M.D., Kyung-Jae
Cranial Ultrasonography in Maple Syrup Urine Disease
 Cranial Ultrasonography in Maple Syrup Urine Disease Giuseppe Fariello, Carlo Dionisi-Vici, Cinzia Orazi, Saverio Malena, Andrea Bartuli, Paolo Schingo, Enza Carnevale, Isora Saponara, and Gaetano Sabetta
Cranial Ultrasonography in Maple Syrup Urine Disease Giuseppe Fariello, Carlo Dionisi-Vici, Cinzia Orazi, Saverio Malena, Andrea Bartuli, Paolo Schingo, Enza Carnevale, Isora Saponara, and Gaetano Sabetta
Quick practical guide to Cranial Ultrasound in the newborn
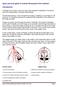 Quick practical guide to Cranial Ultrasound in the newborn Introduction A standard set of views is taken to assist with consistent visualisation of structures and in the interpretation of possible abnormalities.
Quick practical guide to Cranial Ultrasound in the newborn Introduction A standard set of views is taken to assist with consistent visualisation of structures and in the interpretation of possible abnormalities.
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
The clinical presentation of preterm cerebellar haemorrhage
 Eur J Pediatr (2010) 169:1249 1253 DOI 10.1007/s00431-010-1217-4 ORIGINAL PAPER The clinical presentation of preterm cerebellar haemorrhage Ginette M. Ecury-Goossen & Jeroen Dudink & Maarten Lequin & Monique
Eur J Pediatr (2010) 169:1249 1253 DOI 10.1007/s00431-010-1217-4 ORIGINAL PAPER The clinical presentation of preterm cerebellar haemorrhage Ginette M. Ecury-Goossen & Jeroen Dudink & Maarten Lequin & Monique
Cranial ultrasound findings in preterm infants predict the development of cerebral palsy
 Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
neurodevelopmental outcome in
 Archives of Disease in Childhood, 1987, 62, 3-36 Periventricular leucomalacia and neurodevelopmental outcome in C L FAWER, P DIEBOLD, AND A CALAME preterm infants Centre Hospitalier Universitaire Vaudois,
Archives of Disease in Childhood, 1987, 62, 3-36 Periventricular leucomalacia and neurodevelopmental outcome in C L FAWER, P DIEBOLD, AND A CALAME preterm infants Centre Hospitalier Universitaire Vaudois,
Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool.
 Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool. Poster No.: C-1115 Congress: ECR 2012 Type: Educational Exhibit Authors:
Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool. Poster No.: C-1115 Congress: ECR 2012 Type: Educational Exhibit Authors:
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound
 Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18
 IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18 Dhanashree Rajderkar,MD Assistant Professor Department of Radiology University of Florida
IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18 Dhanashree Rajderkar,MD Assistant Professor Department of Radiology University of Florida
Safety of routine early MRI in preterm infants
 Pediatr Radiol (2012) 42:1205 1211 DOI 10.1007/s00247-012-2426-y ORIGINAL ARTICLE Safety of routine early MRI in preterm infants Annemarie Plaisier & Marlou M. A. Raets & Cynthia van der Starre & Monique
Pediatr Radiol (2012) 42:1205 1211 DOI 10.1007/s00247-012-2426-y ORIGINAL ARTICLE Safety of routine early MRI in preterm infants Annemarie Plaisier & Marlou M. A. Raets & Cynthia van der Starre & Monique
Neuropathology Specialty Conference
 Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
The Encephalopathic Neonate: Choosing the Proper Imaging Technique
 The Encephalopathic Neonate: Choosing the Proper Imaging Technique A. James Barkovich, University of California, San Francisco The central nervous system (CNS) of the neonate may be injured by a number
The Encephalopathic Neonate: Choosing the Proper Imaging Technique A. James Barkovich, University of California, San Francisco The central nervous system (CNS) of the neonate may be injured by a number
Developmental sequence of periventricular leukomalacia
 Archives of Disease in Childhood, 1985, 60, 349-355 Developmental sequence of periventricular leukomalacia Correlation of ultrasound, clinical, and nuclear magnetic resonance functions L M S DUBOWITZ,
Archives of Disease in Childhood, 1985, 60, 349-355 Developmental sequence of periventricular leukomalacia Correlation of ultrasound, clinical, and nuclear magnetic resonance functions L M S DUBOWITZ,
/06/ PEDIATRIC RESEARCH Vol. 60, No. 1, 2006 Copyright 2006 International Pediatric Research Foundation, Inc.
 0031-3998/06/6001-0097 PEDIATRIC RESEARCH Vol. 60, No. 1, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. Reduction in Cerebellar Volumes in Preterm Infants: Relationship
0031-3998/06/6001-0097 PEDIATRIC RESEARCH Vol. 60, No. 1, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. Reduction in Cerebellar Volumes in Preterm Infants: Relationship
The "Keyhole": A Sign of
 473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
Cerebral Maturation in Premature Infants: Quantitative Assessment Using MR Imaging
 AJNR Am J Neuroradiol 22:1577 1582, September 2001 Cerebral Maturation in Premature Infants: Quantitative Assessment Using MR Imaging Anne-Marie Childs, Luca A. Ramenghi, Luc Cornette, Steven F. Tanner,
AJNR Am J Neuroradiol 22:1577 1582, September 2001 Cerebral Maturation in Premature Infants: Quantitative Assessment Using MR Imaging Anne-Marie Childs, Luca A. Ramenghi, Luc Cornette, Steven F. Tanner,
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI
 Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
Intraventricular Hemorrhage in the Neonate
 Intraventricular Hemorrhage in the Neonate Angela Forbes, RN, MN, ARNP Seattle Children s Hospital Division of Pediatric Neurosurgery Seattle, Washington, U.S.A. Intraventricular Hemorrhage Who Premature
Intraventricular Hemorrhage in the Neonate Angela Forbes, RN, MN, ARNP Seattle Children s Hospital Division of Pediatric Neurosurgery Seattle, Washington, U.S.A. Intraventricular Hemorrhage Who Premature
Periventricular Cavitations in the First Week of Life
 291 Periventricular Cavitations in the First Week of Life Marc S. Keller 1 Michael A. DiPietro 2 Rita L. T eele 3 Susan J. White 2 Harbhajan S. Chawla 4 Marjorie Curtis-Cohen4 Caroline E. Blane 2 Eleven
291 Periventricular Cavitations in the First Week of Life Marc S. Keller 1 Michael A. DiPietro 2 Rita L. T eele 3 Susan J. White 2 Harbhajan S. Chawla 4 Marjorie Curtis-Cohen4 Caroline E. Blane 2 Eleven
Neurosonography of the Pre-Term Neonate
 Neurosonography of the Pre-Term Neonate Neurosonography of the Pre-Term Neonate Edited by Edward G. Grant With Contributions by James D. Richardson, Dieter Schellinger, Yolande F. Smith, K.N. Siva Subramanian,
Neurosonography of the Pre-Term Neonate Neurosonography of the Pre-Term Neonate Edited by Edward G. Grant With Contributions by James D. Richardson, Dieter Schellinger, Yolande F. Smith, K.N. Siva Subramanian,
BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE
 From the Institution of Clinical Science, Intervention, and Technology Division of Paediatics Karolinska Institutet, Stockholm, Sweden BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE VALUE AND
From the Institution of Clinical Science, Intervention, and Technology Division of Paediatics Karolinska Institutet, Stockholm, Sweden BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE VALUE AND
Advanced magnetic resonance imaging for monitoring brain development and injury
 Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
T he developing brain is vulnerable to injury
 REVIEW Magnetic resonance imaging of preterm brain injury S J Counsell, M A Rutherford, F M Cowan, A D Edwards... Magnetic resonance imaging (MRI) has proved to be a valuable tool for monitoring development
REVIEW Magnetic resonance imaging of preterm brain injury S J Counsell, M A Rutherford, F M Cowan, A D Edwards... Magnetic resonance imaging (MRI) has proved to be a valuable tool for monitoring development
PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES
 PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES Term Equivalent Brain MRIs For Very Preterm Infants Clinical Practice Guideline: Term Equivalent Brain MRIs For Very Preterm Infants Points of emphasis/primary
PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES Term Equivalent Brain MRIs For Very Preterm Infants Clinical Practice Guideline: Term Equivalent Brain MRIs For Very Preterm Infants Points of emphasis/primary
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants
 Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
MR Signal Intensity of the Optic Radiation
 MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
intracranial anomalies
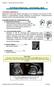 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Periventricular leucomalacia and intraventricular haemorrhage in the preterm neonate
 Archives of Disease in Childhood, 1986, 61, 1196-1202 Periventricular leucomalacia and intraventricular haemorrhage in the preterm neonate J Q TROUNCE, N RUTTER, AND M LEVENE Department of Child Health,
Archives of Disease in Childhood, 1986, 61, 1196-1202 Periventricular leucomalacia and intraventricular haemorrhage in the preterm neonate J Q TROUNCE, N RUTTER, AND M LEVENE Department of Child Health,
ultrasonography in preterm infants: association with outcome
 Archives ofdisease in Childhood 1990; 65: 1033-1037 nstitut de la Sante et de la Recherche Medicale (NSERM), Unite 316, Tours, France Philippe Bertrand Francis Gold Sophie Marchand Department of Paediatric
Archives ofdisease in Childhood 1990; 65: 1033-1037 nstitut de la Sante et de la Recherche Medicale (NSERM), Unite 316, Tours, France Philippe Bertrand Francis Gold Sophie Marchand Department of Paediatric
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
The view from the mastoid fontanel of the neonatal brain
 The view from the mastoid fontanel of the neonatal brain Poster No.: C-0974 Congress: ECR 2016 Type: Educational Exhibit Authors: Y. Pekcevik, F. C. Sarioglu, H. Sahin ; Karabaglar/Izmir/TR, 1 2 2 1 2
The view from the mastoid fontanel of the neonatal brain Poster No.: C-0974 Congress: ECR 2016 Type: Educational Exhibit Authors: Y. Pekcevik, F. C. Sarioglu, H. Sahin ; Karabaglar/Izmir/TR, 1 2 2 1 2
MR Imaging of Periventricular Leukomalacia in Childhood
 111 MR Imaging of Periventricular Leukomalacia in Childhood Olof Flodmark 1 Brian Lupton 2 David Li 1 Gary K. Stimac 3 Elke H. Roland 2 Alan HiII2 Michael F. Whitfield 2 Margaret G. Norman 4 Eight children
111 MR Imaging of Periventricular Leukomalacia in Childhood Olof Flodmark 1 Brian Lupton 2 David Li 1 Gary K. Stimac 3 Elke H. Roland 2 Alan HiII2 Michael F. Whitfield 2 Margaret G. Norman 4 Eight children
Neurosonography: State of the art
 Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Department of Neurosurgery, Emory University; and 2 Pediatric Neurosurgery Associates at Children s Healthcare of Atlanta, Georgia
 J Neurosurg Pediatrics 14:184 189, 2014 AANS, 2014 Poor correlation between head circumference and cranial ultrasound findings in premature infants with intraventricular hemorrhage Clinical article Martha-Conley
J Neurosurg Pediatrics 14:184 189, 2014 AANS, 2014 Poor correlation between head circumference and cranial ultrasound findings in premature infants with intraventricular hemorrhage Clinical article Martha-Conley
Superficial Echogenic Lesions Detected on Neonatal Cranial Sonography
 ORIGINAL RESEARCH Superficial Echogenic Lesions Detected on Neonatal Cranial Sonography Possible Indicators of Severe Birth Injury Byoung Hee Han, MD, Mi Jin Song, MD, Kyung Sang Lee, MD, Young-Hwa Kim,
ORIGINAL RESEARCH Superficial Echogenic Lesions Detected on Neonatal Cranial Sonography Possible Indicators of Severe Birth Injury Byoung Hee Han, MD, Mi Jin Song, MD, Kyung Sang Lee, MD, Young-Hwa Kim,
Intraventricular Hemorrhage and Periventricular Leukomalacia
 Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
IMPAIRED CEREBRAL CORTICAL GRAY MATTER GROWTH FOLLOWING TREATMENT WITH DEXAMETHASONE FOR NEONATAL CHRONIC LUNG DISEASE
 IMPAIRED CEREBRAL CORTICAL GRAY MATTER GROWTH FOLLOWING TREATMENT WITH DEXAMETHASONE FOR NEONATAL CHRONIC LUNG DISEASE Brendan P. Murphy, MB BCh 1, Terrie E. Inder, MD 2,5, Petra S. Huppi, MD 3,5, Simon
IMPAIRED CEREBRAL CORTICAL GRAY MATTER GROWTH FOLLOWING TREATMENT WITH DEXAMETHASONE FOR NEONATAL CHRONIC LUNG DISEASE Brendan P. Murphy, MB BCh 1, Terrie E. Inder, MD 2,5, Petra S. Huppi, MD 3,5, Simon
Cribside Neurosonography:
 501 Cribside Neurosonography: Real-Time Sonography for Intracranial Investigation of the Neonate Mary K. Edwards 1 David L. Brown 1 Jans Muller Charles B. Grossman 1 Gonzalo T. Chua 1 prospective study
501 Cribside Neurosonography: Real-Time Sonography for Intracranial Investigation of the Neonate Mary K. Edwards 1 David L. Brown 1 Jans Muller Charles B. Grossman 1 Gonzalo T. Chua 1 prospective study
MR Assessment of Myelination in Infants and Children: Usefulness of Marker Sites
 731 MR ssessment of Myelination in Infants and Children: Usefulness of Marker Sites C. Roger ird 1 Mary Hedberg urton P. Drayer Paul J. Keller Richard. Flom John. Hodak retrospective study was made of
731 MR ssessment of Myelination in Infants and Children: Usefulness of Marker Sites C. Roger ird 1 Mary Hedberg urton P. Drayer Paul J. Keller Richard. Flom John. Hodak retrospective study was made of
Intracranial Abnormalities in Infants Treated with Extracorporeal Membrane Oxygenation: Update on Sonographic and CT Findings
 Intracranial Abnormalities in Infants Treated with Extracorporeal Membrane Oxygenation: Update on Sonographic and CT Findings Dorothy I. Bulas, George A. Taylor, Regina M. O Donnell, Billie Lou Short,
Intracranial Abnormalities in Infants Treated with Extracorporeal Membrane Oxygenation: Update on Sonographic and CT Findings Dorothy I. Bulas, George A. Taylor, Regina M. O Donnell, Billie Lou Short,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Transcranial Perinatal Neurosonogram for Intracranial Pathology: Study of 165 Cases
 Transcranial Perinatal Neurosonogram for Intracranial Pathology: Study of 165 Cases K Humsene 1, N Krishnaveni 2, B Sarada 3 ORIGINAL ARTICLE ABSTRACT Background: The presence of open fontanelle in infants
Transcranial Perinatal Neurosonogram for Intracranial Pathology: Study of 165 Cases K Humsene 1, N Krishnaveni 2, B Sarada 3 ORIGINAL ARTICLE ABSTRACT Background: The presence of open fontanelle in infants
Neonatal Hypoxic ischemic Encephalopathy: A Radiological Review
 Review Article Neonatal Hypoxic ischemic Encephalopathy: A Radiological Review Shahina Bano, Vikas Chaudhary 1, Umesh Chandra Garga Department of Radiodiagnosis, PGIMER, Dr. RML Hospital, 1 Department
Review Article Neonatal Hypoxic ischemic Encephalopathy: A Radiological Review Shahina Bano, Vikas Chaudhary 1, Umesh Chandra Garga Department of Radiodiagnosis, PGIMER, Dr. RML Hospital, 1 Department
Punctate white matter lesions in infants: new insights using susceptibility-weighted imaging
 Neuroradiology (2011) 53:669 679 DOI 10.1007/s00234-011-0872-0 PAEDIATRIC NEURORADIOLOGY Punctate white matter lesions in infants: new insights using susceptibility-weighted imaging Tetsu Niwa & Linda
Neuroradiology (2011) 53:669 679 DOI 10.1007/s00234-011-0872-0 PAEDIATRIC NEURORADIOLOGY Punctate white matter lesions in infants: new insights using susceptibility-weighted imaging Tetsu Niwa & Linda
Cerebrovascular Accidents in Neonates Treated with Extracorporeal Membrane Oxygenation: Sonographic-Pathologic Correlation
 355 Cerebrovascular Accidents in Neonates Treated with Extracorporeal Membrane Oxygenation: Sonographic-Pathologic Correlation George A. Taylor1 "3 Charles R. Fitz 1-2 Sudesh Kapur2 ' 4 Billie L. Short2-5
355 Cerebrovascular Accidents in Neonates Treated with Extracorporeal Membrane Oxygenation: Sonographic-Pathologic Correlation George A. Taylor1 "3 Charles R. Fitz 1-2 Sudesh Kapur2 ' 4 Billie L. Short2-5
The Asymmetric Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR
 The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
multiple sclerosis by magnetic resonance imaging
 Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
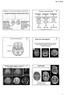 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
Periventricular/Intraventricular Hemorrhage in the Newborn
 Khalid N. Haque, FRCP(Ed), FRCP(I), FAAP, FICP, DCH, DTM&H; Omar B. A. Basit, MRCP(UK), DCH; Meeralebbae M. Shaheed, MD, MRCP(UK), DCH From the Division of Neonatology, Department of Pediatrics, College
Khalid N. Haque, FRCP(Ed), FRCP(I), FAAP, FICP, DCH, DTM&H; Omar B. A. Basit, MRCP(UK), DCH; Meeralebbae M. Shaheed, MD, MRCP(UK), DCH From the Division of Neonatology, Department of Pediatrics, College
Cystic Periventricular Leukomalacia: Sonographic
 439 Cystic Periventricular Leukomalacia: Sonographic and CT Findings Dieter Schellinger 1 Edward G. Grant James D. Richardson Periventricular leukoencephalopathy (PVL) is a pathologic process that has
439 Cystic Periventricular Leukomalacia: Sonographic and CT Findings Dieter Schellinger 1 Edward G. Grant James D. Richardson Periventricular leukoencephalopathy (PVL) is a pathologic process that has
Perinatal cerebral white matter injuries influence early communication and language development
 Perinatal cerebral white matter injuries influence early communication and language development Blazenka Brozovic University of Zagreb Department of Speech and Language Pathology Developmental Neurolinguistic
Perinatal cerebral white matter injuries influence early communication and language development Blazenka Brozovic University of Zagreb Department of Speech and Language Pathology Developmental Neurolinguistic
Cerebellar Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy
 AJNR Am J Neuroradiol 25:1008 1015, June/July 2004 Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy Michael A. Sargent, Kenneth J. Poskitt, Elke H. Roland, Alan Hill, and Glenda Hendson BACKGROUND
AJNR Am J Neuroradiol 25:1008 1015, June/July 2004 Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy Michael A. Sargent, Kenneth J. Poskitt, Elke H. Roland, Alan Hill, and Glenda Hendson BACKGROUND
Sonography of Brain Tumors in Infants
 253 Sonography of Brain Tumors in Infants Bokyung K. Han 1 Diane S. Babcock Alan E. Oestreich Cranial sonograms of six children with brain tumors (one newborn, four infants, and one 4-year-old child) are
253 Sonography of Brain Tumors in Infants Bokyung K. Han 1 Diane S. Babcock Alan E. Oestreich Cranial sonograms of six children with brain tumors (one newborn, four infants, and one 4-year-old child) are
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
SOP: Cerebral Ultrasound
 SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea
 Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Insults to the Term Brain
 Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Complete Summary GUIDELINE TITLE
 Complete Summary GUIDELINE TITLE Practice parameter: neuroimaging of the neonate: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child
Complete Summary GUIDELINE TITLE Practice parameter: neuroimaging of the neonate: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child
Surgical Options in Post Haemorrhagic Ventricular Dilation
 Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
Predicting outcome using neonatal MRI in preterm infants. Manon Benders, neonatologist. Summer Conference on Neonatology in Provence
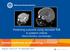 Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
With advances in obstetric and neonatal care of the preterm
 ORIGINAL RESEARCH PEDIATRICS New MR Imaging Assessment Tool to Define Brain Abnormalities in Very Preterm Infants at Term H. Kidokoro, J.J. Neil, and T.E. Inder ABSTRACT BACKGROUND AND PURPOSE: WM injury
ORIGINAL RESEARCH PEDIATRICS New MR Imaging Assessment Tool to Define Brain Abnormalities in Very Preterm Infants at Term H. Kidokoro, J.J. Neil, and T.E. Inder ABSTRACT BACKGROUND AND PURPOSE: WM injury
