european urology 51 (2007)
|
|
|
- Horatio James
- 6 years ago
- Views:
Transcription
1 european urology 51 (2007) available at journal homepage: Kidney Cancer Surgical Management of Renal Cell Carcinoma with Tumor Thrombus in the Renal and Inferior Vena Cava: The University of Miami Experience in Using Liver Transplantation Techniques Gaetano Ciancio a,c, *, Alan S. Livingstone b, Mark Soloway c a Department of Surgery, Division of Transplantation, University of Miami Miller School of Medicine, Miami, Florida, United States b Department of Surgery, Division of Surgical Oncology, University of Miami Miller School of Medicine, Miami, Florida, United States c Department of Urology, University of Miami Miller School of Medicine, Miami, Florida, United States Article info Article history: Accepted November 29, 2006 Published online ahead of print on December 8, 2006 Keywords: Renal cell carcinoma Surgical technique Caval thrombus Tumor thrombus Radical nephrectomy Abstract Objectives: Renal cell carcinoma (RCC) with tumor thrombus in the inferior vena cava (IVC) poses a challenge to the surgeon due to the potential for massive hemorrhage and tumor thromboemboli. We developed a technique for safe resection of these tumors through a transabdominal approach, without recourse to cardiopulmonary bypass (CPB). Materials and methods: From August 1997 to February 2005, 66 patients underwent resection of a RCC with tumor thrombus in the IVC. The extent of the tumor thrombus was renal in 13, infrahepatic in 7; retrohepatic in 38; and intra-atrial in 8 patients. Results: Mean operative time was hours. The estimated blood loss ranged from 200 cc to 16,000 cc, with a mean of transfusions being U. CBP was required in only 3 patients. Three patients (4.5%) died in the immediate postoperative period. Median follow-up among the 56 survivors was 7.1 months. Six patients died due to metastasis and 1 died of a cause unrelated to the cancer. The estimated actuarial survival at 36 months was 66%. Conclusions: An aggressive surgical approach is the only hope for curing patients having RCC with a tumor thrombus in the IVC. The extent of dissection is predicated on the extent and level of tumor thrombus. Our surgical approach uses liver transplant techniques to mobilize the liver off the IVC and to separate the IVC from the posterior abdominal wall. This maneuver provides excellent exposure and enables safe vascular control of the IVC. # 2006 European Association of Urology. Published by Elsevier B.V. All rights reserved. * Corresponding author. University of Miami Miller School of Medicine, Department of Surgery, Division of Transplantation, P.O. Box , Miami, FL 33101, United States. Tel ; Fax: address: gciancio@med.miami.edu (G. Ciancio) /$ see back matter # 2006 European Association of Urology. Published by Elsevier B.V. All rights reserved. doi: /j.eururo
2 european urology 51 (2007) Introduction Renal cell carcinoma infrequently extends into the inferior vena cava [1]. When it occurs, surgery offers the only potential cure [2]. The approach varies among surgeons yet all agree that the surgery is complex and requires an excellent understanding of the anatomy and, generally, a team approach [3 8]. Some surgeons prefer a thoracoabdominal incision or median sternotomy to provide adequate exposure and vascular control. Both approaches facilitate the use of cardiopulmonary bypass. While CPB provides a measure of safety, postoperative coagulopathy and neurological sequelae from CPB and deep hypothermic circulatory arrest (DHCA) warrant consideration of alternatives. We describe our experience managing 66 patients with RCC and IVC tumor thrombus utilizing a transabdominal approach, usually without recourse to intraoperative bypass maneuvers. Our approach merges surgical principles from the fields of urologic oncology and transplantation and, thus, these patients should be referred to facilities with expertise in dealing with RCC with IVC tumor thrombus. 2. Materials and methods From August 1997 to February 2005, 66 patients, 34 men and 32 women, underwent resection of a RCC with extension of tumor thrombus into the IVC (Stage T3b/c). Their ages ranged from 25 to 84 (mean 62 years). Initial diagnosis was made by computed tomography (CT). Cardiac, renal, and respiratory status were evaluated pre-operatively. The level of the thrombus confirmed in 48 patients with magnetic resonance imaging (MRI). The cranial extent of the tumor was initially defined per Neves and Zincke [3]; however, for a level III thrombus we used our modified definition [8]. Clinical and pathological staging was performed using the TNM classification. Tumor grade was classified according to the Furhman grading system. Thirteen patients had a level I thrombus (renal vein only), 7 had a level II thrombus (infrahepatic IVC), 38 had a level III thrombus (retrohepatic IVC) [8], and 8 had a level IV thrombus (intra-atrial). Sixty three were managed by a transabdominal approach without bypass maneuvers; 3 patients (4.5%) with a level IV tumor thrombus that was adherent to the atrial wall had CPB. The tumor was on the right side in 48 and on the left in 18 patients. Transesophageal echocardiography (TEE) was occasionally used to monitor the tumor thrombi that were above the infrahepatic vena cava. TEE is helpful in delineating the cranial extent of the thrombus. For a level I or level II tumor thrombus, TEE was not used; however, TEE is useful for level III and IV Statistical methods Actuarial patient survival and disease free survival were estimated (along with standard errors of those estimates) using Kaplan-Meier curves. Subgroup differences for a particular hazard rate were tested by the log-rank test. Although the total cohort size and observed number of failures were relatively small, multivariable analysis of both outcome variables was performed using a Cox model stepwise regression approach. Baseline characteristics that were considered for their prognostic value included: patient age at surgery, presentation with distant metastasis, local lymph node involvement, tumor grade, tumor size, and tumor level Operative technique A triradiate incision is made commencing approximately 2 fingerbreadths below the right costal margin, extending out laterally to the mid axillary line. This is extended below the left costal margin as far as necessary, and vertically in the midline to the xiphoid process. A Rochard self-retaining retractor is placed elevating the costal margins and splaying them laterally toward the axillae. We pursue early intraoperative ligation of the involved renal artery. The kidney is mobilized medially until the renal artery is identified and ligated [9]. Arterial ligation results in decompression of collateral circulation and decreasing blood loss. Exposure of the left kidney begins by mobilization of the descending colon. The spleen is dissected off the diaphragm and mobilized en bloc with the pancreas toward the midline. This exposes the entire upper retroperitoneal space from the diaphragm to the inferior border of the kidney Surgical approach based upon degree of thrombus extension Liver mobilization begins with dissection of the ligamentum teres which is divided. The falciform ligament is divided with cautery and this incision is carried around both to the right superior coronary ligament and by passing to the left side, dividing the left triangular ligament. The visceral peritoneum on the right of the hepatic hilum and the infrahepatic vena cava is incised in conjunction with the right inferior coronary and hepato-renal ligaments. The liver is gradually rolled to the left using these techniques as described for liver transplantation [8 13]. Once the liver is mobilized, RCC with a level I tumor thrombus can be resected with minimal vena cava dissection. After vascular control is achieved, a cavotomy is performed and the tumor extracted. The tumor can be milked back into the renal vein and a vascular clamp applied. Level II tumors invade the IVC with the superior extent below the level of the intrahepatic IVC. Complete inferior vena cava obstruction is often present. For better proximal control, the liver may need to be dissected off the IVC in its inferior aspect (see level III). Once vascular control is achieved, the IVC can be clamped partially or totally. The cava is opened along its anterolateral aspect and the tumor thrombus is removed. If the IVC has been completely clamped, the vascular clamps can be repositioned to allow blood return from the legs and the opposite renal vein. For level III and IV an opening in the lesser omentum allows the porta hepatis to be controlled with a Rummel tourniquet; a Pringle maneuver can then be carried out (temporarily occluding the portal venous and arterial inflow
3 990 european urology 51 (2007) Fig. 1 A. The whole abdominal inferior vena cava with tumor thrombus is exposed by mobilizing the liver off of retrohepatic inferior vena cava. B. Inferior vena cava dissected off the posterior abdominal wall. Mobility allows tumor milking below the major hepatic veins by the surgeon s fingers. IVC = inferior vena cava; KT = kidney tumor; L = liver. to the liver) as required. Then we proceed with the piggyback liver transplantation technique [20]. Piggyback liver transplantation is so called because the recipient s vena cava is left in situ and the liver mobilized off the vessel [13]. Small hepatic veins passing from the right and caudate lobe are ligated and divided. The liver is dissected off the inferior vena cava until it lies in a piggyback fashion, attached to the inferior vena cava only by the major hepatic veins (Fig. 1A). In this fashion, the infrahepatic, intrahepatic, and suprahepatic portions of the IVC are completely exposed (Fig. 1A). In addition to mobilizing the liver off the cava, a plane between the IVC and the posterior abdominal wall is important because it permits circumferential vascular control of the cava [15 18] (Fig. 1B). Small tributaries can become engorged to look like lumbar vessels, and they need to be identified and ligated. A useful technique, which we have applied for a thrombus located above the hepatic veins, is to milk the thrombus below the major hepatic veins and then apply a vascular clamp just below the major hepatic veins (Fig. 2). This technique is often feasible since ligation of the renal artery reduces the blood Fig. 2 Abdominal removal of renal cell carcinoma with level III supradiaphragmatic, suprahepatic, infra-atrial tumor thrombus. A. The entire abdominal inferior vena cava is exposed by mobilization of the liver off the retrohepatic inferior vena cava. Diaphragm is dissected off of the suprahepatic inferior vena cava. A plane is created between the inferior vena cava and the posterior abdominal wall () )))). B. Mobility of the inferior vena cava allows milking the tumor below the hepatic veins. Clamp is placed below the hepatic veins and continual hepatic venous drainage is permitted during the closure or reconstruction of the inferior vena cava.
4 european urology 51 (2007) Fig. 3 A. Central tendon of the diaphragm and the posterior wall of the IVC are dissected. Right atrium, IVC, porta hepatis, left renal vein, and distal IVC are clamped. B. The tumor thrombus is milked down or dissected off the atrium wall and suprahepatic IVC, then the vascular clamp is repositioned below the major hepatic veins and the porta hepatis clamp is released. supply to the tumor thrombus. It serves a dual function. First, it allows the liver to drain into the IVC avoiding hypotension from decreased venous return. Second, by not clamping the major hepatic veins or porta hepatis, liver congestion and postoperative hepatic dysfunction are avoided. The surgeon must be careful when touching the thrombus so as to avoid dislodging it. For level IV and some level III thrombi [8], the central tendon of the diaphragm is dissected until the supradiaphragmatic, intrapericardial IVC is identified (Fig. 3A). This dissection is carried out circumferentially so that the intrapericardial IVC can be encircled at its confluence with the right atrium. The right atrium is gently pulled beneath the diaphragm (Fig. 3). The Pringle maneuver is then performed to temporarily occlude the vascular inflow to the liver. The infrarenal cava and left or right renal vein are controlled, and a Satinsky clamp is placed across the right atrium. For a level III tumor thrombus a vascular clamp is placed across the intrapericardial or suprahepatic IVC [8]. The IVC is incised from the diaphragm to the renal vein, and the tumor is sharply dissected off the atrial wall and/or IVC. The three major hepatic veins can be directly visualized, their orifices inspected, and tumor removed if it is invading them. Following removal of the tumor thrombus and closure of the upper cava, the clamp is repositioned below the hepatic veins, the Pringle is released, and normal liver blood flow is reestablished (Fig. 3). The remaining IVC below the hepatic veins is sutured closed [14,15] Budd-Chiari Syndrome (BCS) associated with RCC with tumor thrombus In 5 patients, the tumor invaded the major hepatic veins causing a BCS. In 4 of them, the tumor also extended into the right atrium (level IV), and in 1 the tumor extended above the diaphragm but below the atrium. One patient with severe BCS had to go on cardiopulmonary bypass. This, in conjunction with cirrhosis, discovered only at surgery, resulted in a coagulopathy requiring 47 units of blood, 98 units of platelets, and component therapy. Hemostasis was achieved, but she developed liver failure and died 2 weeks postoperatively due to multiorgan dysfunction. Another patient with BCS also had large transfusion requirements of 20 units of blood during tumor removal. His convalescence was uneventful, but he died 6 months after surgery from metastatic renal cancer [10] Resection of the IVC during tumor thrombus removal Four patients underwent radical nephrectomy with resection of the abdominal IVC. The first patient had a left RCC with a tumor thrombus, as well as a thrombosed infrarenal cava containing an IVC filter that had been placed at another hospital. The infrarenal and juxtarenal cava were resected along with the tumor thrombus, left renal vein, and left kidney. The IVC was oversewn distally above the confluence of the iliac veins, and the suprarenal cava was repaired restoring antegrade flow through the right renal vein. Two patients had a right nephrectomy and removal of most of the abdominal IVC. The left renal vein, the distal IVC, and the cava just below the hepatic veins were oversewn (Fig. 4). The left renal vein was not reimplanted as there were extensive collaterals draining the kidney. The fourth patient had a similar resection but in his case a large segment of the left renal vein had to be removed. The remaining left renal vein was anastomosed endto-end to the proximal IVC to avoid renal dysfunction [11]. 3. Results Sixty six patients underwent radical nephrectomy with resection of tumor thrombus from the IVC. Serum creatinine values ranged from 0.6 mg/dl to 4.6 mg/dl (mean 1.28 mg/dl, normal mg/dl). Two patients were on hemodialysis preoperatively. Clinical staging revealed T3b with level I thrombus in 13 (19.7%), level II thrombus in 7 (10.6%), level III thrombus in 38 (57.6%), and T3c with level IV thrombus in 8 (12.1%) (Table 1). The level of thrombus
5 992 european urology 51 (2007) Fig. 4 The surgical specimen includes en-block resection of the inferior vena cava (A), tumor thrombus (B) and kidney tumor (C). on CT/MRI correlated well with the intraoperative findings. All patients had complete extraction of tumor from the IVC. Mean operative time was h (range h). Estimated blood loss ranged from 200 cc to 16,000 cc (mean 1, cc). The number of transfusions ranged from 0 to 47 (mean U). Four patients received cell saver blood only, 34 received allogeneic blood, and 28 did not require a transfusion (Table 1). Three patients required CPB. Veno-venous bypass was not used. Ten patients had known metastatic RCC. Sixty three of the patients had an uneventful postoperative course. One patient with a level III thrombus died on the first postoperative day from a cardiac arrhythmia. Another patient had severe BCS and needed to go on CPB. She developed a coagulopathy and liver failure, and died 2 weeks postoperatively of multiorgan dysfunction. The third patient died of sepsis 2 weeks after surgery. Pathological examination revealed RCC of the clear cell variety in 53 patients, sarcomatoid in 2, granular in 3, clear/granular in 3, and papillary in 5. There were lymph node metastases in 12 patients (18%) 1 with a level I, 9 with level III and 1 with a level IV tumor thrombus. The median Furhman grade was 3 and the mean tumor size was 10 cm (range cm). The median follow-up among the 56 survivors was 7.1 months (range months). Ten deaths have been observed so far, with 3 occurring in the immediate postoperative period, 6 due to metastasis and 1 due to complication of a pelvic fracture. Actuarial survival for the whole cohort at 36 months was 66% 13%. A multivariable analysis of survival identified 2 factors that were unfavorable: distant metastasis at the time of surgery (P = 0.003) and a level IV thrombus (P = 0.004). Ten patients had distant metastasis at the time of surgery, and 8 patients had a level IV tumor (1 patient had both of these characteristics). Among the 49 patients having a more favorable prognosis, i.e., presentation without metastasis and a level I-III tumor, only 3 deaths were observed (actuarial survival at 3 years post-surgery was 82% 10%). Conversely, among the 17 patients at high risk of death, i.e. presentation with distant metastasis or a level IV tumor, 7 have died (actuarial survival estimate at 3 years postsurgery was 0%) (P = by the log-rank test). Among the 56 patients who were free of distant metastasis at the time of surgery, 14 patients developed a distant metastasis. The actuarial probability of developing metastasis by 2 years post-surgery was 47% 11%. One factor was found to be associated with a significantly higher rate of developing metastasis: patients having a level IV tumor (P = 0.005). The observed proportion of patients who developed a distant metastasis post-surgery was 10/49 among those having a level I-III tumor in comparison with 4/7 among those with a level IV tumor. 4. Discussion Patients with a thrombus from RCC which extends into the IVC, without lymph node metastasis, have a reasonable prognosis [16]. Five-year survival rates of 32% 64% with surgery have been reported [3,5,17 19]. Table 1 Patients with renal cell carcinoma and level tumor thrombus Level N Operative time (hours) * Transfusion (n) * Blood loss (ml) * I II III , IV , Total , * Standard error; N, number of patients; (n), number of units of blood.
6 european urology 51 (2007) The critical factor is successful surgery, mainly management of the IVC [17], and the important goals are to minimize bleeding and prevent embolism from the thrombus during surgery. Either event often leads to fatal consequences. While the oncological prognostic value of this series was obviously limited by the small numbers and presence of many subgroups in terms of level, presence or not of nodes and metastasis, our overall results were quite expected: (i) a very small percentage (3/66) of our patients died of a post-operative complication, (ii) presence of metastasis at the time of surgery was significantly associated with a poorer survival, and (iii) level IV tumors were associated with a significantly higher risk of the development of metastatic spread. Over the years, several approaches have been developed to aid in the safe removal of these tumors. The improvement in surgical technique has often been due to the application of surgical principles from different disciplines. Cardiopulmonary bypass, with or without deep hypothermic circulatory arrest, is an example of using cardiac surgery tools in an oncologic operation [20,21]. We propose blending lessons learned in the fields of liver transplantation surgery and urologic oncology to deal with a tumor thrombus of the IVC. The concept of resorting to an entirely intra-abdominal approach without cardiopulmonary or veno-venous bypass is the byproduct of this approach [12]. Cardiopulmonary bypass, with or without deep hypothermic circulatory arrest [6,21,22], can produce platelet dysfunction and coagulopathy, resulting in bleeding from the extensive raw retroperitoneal surfaces [5]. Cardiopulmonary bypass in patients with a bulky, intra-atrial thrombus may be required. However those with a minimal, non-adherent atrial thrombus, or level III tumor extension, may not require cardiopulmonary bypass. Advocates of preoperative renal artery embolization claim it makes the operation easier because (a) it reduces blood loss by collapsing the many collaterals on the surface of the kidney and the hilum, (b) it allows ligation of the renal vein without first ligating the artery and (c) if 24 to 48 hours are allowed to elapse after infarction, considerable edema develops around the tumor facilitating dissection from contiguous structures. We have never preoperatively embolized any of our patients, but an important principle of our surgical approach includes mobilization of the kidney with resection early ligation of the renal artery. With the posterior approach, fewer varices are encountered as opposed to dissection anterior to the kidney. Once the kidney is mobilized medially, the renal artery is identified, ligated and divided. The collateral circulation quickly collapses making the rest of the dissection easier, and has the same effect as preoperative embolization without the morbidity [9]. Budd-Chiari syndrome (BCS) is a rare disorder resulting from the occlusion of the major hepatic veins or the suprahepatic inferior vena cava. It classically presents with the triad of hepatomegaly, right-sided abdominal pain, and ascites [23]. A variety of underlying conditions predispose to the development of BCS, but hepatocellular, adrenal, and renal cell carcinomas are the most common malignant causes [24,25]. The presence of hepatic vein obstruction causing a BCS is an adverse feature. Portosystemic varices add to the problem of enlarged caval collaterals and meticulous attention to homeostasis is essential. Liver congestion makes mobilization more difficult and poor liver function and increased third space losses due to the portal hypertension further complicate the post-operative management and can be associated with imminently life-threatening sequelae like hepatic failure seen in one of our patient. Our five patients with hepatic vein occlusion and secondary BCS had collateral circulation and varices of sufficient magnitude that partially compensated for the greatly reduced outflow from the hepatic veins. These extensive collaterals, caused by both the cava and hepatic vein occlusion, make the surgery especially challenging. Our technique allows complete removal of all gross tumor extending into the hepatic veins, and can be used in conjunction with cardiopulmonary bypass when necessary. Fortunately in the present series it was not associated with mortality. Our experience affirms the possibility of resection of the IVC en-bloc with RCC and tumor thrombi without the need for IVC reconstruction. Complete piggyback liver mobilization [8 12] facilitates thrombectomy because cavotomy may be extended cranially to remove any adherent tumor thrombus, and makes removal of the IVC easier when necessary. Although prosthetic grafts can be placed in this setting, we have successfully avoided them. 5. Conclusions A strict abdominal approach to RCC with tumor thrombus in the IVC can provide the surgeon with exposure similar to the thoracoabdominal incision without the pain and chest tube associated with a thoracotomy. The use of liver and IVC mobilization techniques helps in achieving additional exposure and enables the surgeon to have excellent control of the IVC for safe resection of these tumors.
7 994 european urology 51 (2007) Conflicts of interest The authors have no disclosure to make. We have no commercial relationship such as: consultancies, stock ownership or other equity interests, patents received and/or pending, or any commercial relationship which might be in any way considered related to a submitted article. Acknowledgments The authors thank the illustration expertise of Claudia Gutierrez. References [1] Williams RD. Renal, perirenal and ureteral neoplasms. In: Adult and Pediatric Urology. Gillenwater JY, Grayhack JT, Howards SS, Duckett JW, editors. 1st ed. Chicago, Vol 1, Chapt 16; p [2] Tribble CG, Gerkin TM, Flanagan TL, et al. Vena caval involvement with renal tumors: surgical considerations. Ann Thorac Surg 1988;46:36 9. [3] Neves RJ, Zincke H. Surgical treatment of renal cancer with vena cava extension. Br J Urol 1987;59: [4] Marshall FF, Dietrick DD, Baumgartner WA, et al. Surgical management of renal cell carcinoma with intracaval neoplastic extension above the hepatic veins. J Urol 1988; 139: [5] Skinner DG, Pritchett TR, Lieskovsky G, et al. Vena caval involvement by renal cell carcinoma. Surgical resection provides meaningful long-term survival. Ann Surg 1989;210: [6] Novick AC, Kaye MC, Cosgrove DM, et al. Experience with cardiopulmonary bypass and deep hypothermic circulatory arrest in the management of retro-peritoneal tumors with large vena caval thrombi. Ann Surg 1990;212: [7] Nesbit JC, Soltero ER, Dinney CP, et al. Surgical management of renal cell carcinoma with inferior vena cava tumor thrombus. Ann Thorac Surg 1997;63: [8] Ciancio G, Vaidya A, Savoie M, et al. Management of renal cell carcinoma with level III thrombus in the inferior vena cava. J Urol 2002;168: [9] Ciancio G, Vaidya A, Soloway M. Early ligation of the renal artery using the posterior approach: a basic surgical concept reinforced during resection of large hypervascular renal cell carcinoma with or without inferior vena cava thrombus. BJU Int 2003;92: [10] Ciancio G, Soloway M. Renal cell carcinoma invading the hepatic veins. Cancer 2001;92: [11] Ciancio G, Soloway M. Resection of the abdominal inferior vena cava for complicated renal cell carcinoma with tumor thrombus. Br J Urol Int 2005;96: [12] Ciancio G, Hawke C, Soloway M. The use of liver transplant techniques to aid in the surgical management of urological tumors. J Urol 2000;164: [13] Tzakis A, Todo S, Starzl TE. Orthotopic liver transplantation with preservation of the inferior vena cava. Ann Surg 1989;210: [14] Ciancio G, Soloway M. Renal cell carcinoma with tumor thrombus extending above the diaphragm: avoiding cardiopulmonary bypass. Urology 2005;66: [15] Cerwicka WH, Ciancio G, Salerno TA, Soloway M. Renal cell cancer with invasive atrial tumor thrombus excised off-pump. Urol 2005;66:1319.e e11. [16] Patard JJ. Renal cell carcinoma with inferior vena cava invasion: An orphan disease? Eur Urol 2006;50: [17] Swierzewski DJ, Swierzewski MJ, Libertino JA. Radical nephrectomy in patients with renal cell carcinoma with venous, vena caval and atrial extension. Am J Surg 1994;168: [18] Glazer AA, Novick AC. Long-term followup after surgical treatment for renal cell carcinoma extending into the right atrium. J Urol 1996;155: [19] Montie JE, el Ammar R, Pontes JE, et al. Renal carcinoma with inferior vena cava thrombi. Surg Gynecol Obstet 1991;173: [20] Vaislic C, Puel P, Grondin P, et al. Surgical resection of neoplastic thrombus in the inferior vena cava by neoplasms of renal-adrenal tract. Vasc Surg 1983;17: [21] Marshall FF, Reitz BA, Diamond DA. A new technique for management of renal cell carcinoma involving the right atrium. Hypothermia and cardiac arrest. J Urol 1984;131: [22] Vaislic C, Puel P, Grondin P, et al. Cancer of the kidney invading the vena cava and heart. Results after 11 years of treatment. J Thorac Cardiovasc Surg 1986;91: [23] Mahmoud AEA, Elias E. New approaches to the Budd- Chiari syndrome. J Gastroenterol Hepatol 1996;11: [24] Kume H, Kameyama S, Kasuya Y, Tajima A, Kawabe K. Surgical treatment of renal cell carcinoma associated with Budd-Chiari syndrome: report of four cases and review of the literature. Eur J Sur Oncol 1999;25:71 5. [25] Mitchell MC, Boitnott JK, Kaufman S, Cameron JL, Maddrey WC. Budd-Chiari syndrome: etiology, diagnosis and management. Medicine 1982;61: Editorial Comment Peter F.A. Mulders, Radboud University Nijmegen Medical Center, Nijmegen, The Netherlands P.Mulders@uro.umcn.nl This article deals with a technique that can make the removal of tumour thrombus in the caval vena more accessible. Real prognostication for these patients and standardised procedures for indication and surgical approaches are lacking because of the limited numbers of patients and the variety of staging systems. Several issues are addressed in the article and can be discussed.
8 european urology 51 (2007) Extension of tumour thrombus in the vena cava is divided into different levels. The study has a substantial number of patients who have only limited vena caval extension. The question is whether the procedure with liver mobilisation and retrograde ligation of the artery should always be used. The procedure can be especially beneficial in tumour thrombi with extension below the atrium but above the hepatic vein to avoid cardiac arrest and reduce morbidity. Therefore, it is important to use adequate diagnostic tools to determine the exact extension. The use of magnetic resonance imaging, multislice computer tomography scanning, and colour flow ultrasound can be used with reasonable accuracy, with ultrasound giving information on blood flow and attachment of the thrombus to the caval wall [1,2]. It can individualise the necessary extent of preparation for the procedure, especially for the indication of cardiac arrest. The low prevalence of patients with extensive vena caval involvement of thrombus and the higher morbidity and even mortality risks also indicate the need for experience with performing the procedure. Guidelines advise that these patients be referred to experienced centres with all equipment available. The manoeuvre with mobilising the liver and the possibility for cardiac arrest explain the need for a multidisciplinary surgical team to obtain optimal oncology outcome with acceptable morbidity. Indications for surgery should be discussed with oncology teams because of the prognostic differences based on the extent of the thrombus [3]. References [1] Lawrentschuk N, Gani J, Riordan R, Esler S, Bolton DM. Multidetector computed tomography vs magnetic resonance imaging for defining the upper limit of tumour thrombus in renal cell carcinoma: a study and review. BJU Int 2005;96: [2] Gupta NP, Ansari MS, Khaitan A, et al. Impact of imaging and thrombus level in management of renal cell carcinoma extending to veins. Urol Int 2004;72: [3] Kim HL, Zisman A, Han KR, Figlin RA, Belldegrun AS. Prognostic significance of venous thrombus in renal cell carcinoma. Are renal vein and inferior vena cava involvement different? J Urol 2004;171(2 pt 1):
IVC THROMBECTOMY: OPEN
 IVC THROMBECTOMY: OPEN Gennady Bratslavsky, M.D. Professor and Chairman Department of Urology SUNY Upstate Medical University Syracuse, NY Disclosures None I am not an ideal candidate to argue for open
IVC THROMBECTOMY: OPEN Gennady Bratslavsky, M.D. Professor and Chairman Department of Urology SUNY Upstate Medical University Syracuse, NY Disclosures None I am not an ideal candidate to argue for open
Renal Carcinoma With Supradiaphragmatic Tumor Thrombus: Avoiding Sternotomy and Cardiopulmonary Bypass
 Renal Carcinoma With Supradiaphragmatic Tumor Thrombus: Avoiding Sternotomy and Cardiopulmonary Bypass Gaetano Ciancio, MD, Samir P. Shirodkar, MD, Mark S. Soloway, MD, Alan S. Livingstone, MD, Michael
Renal Carcinoma With Supradiaphragmatic Tumor Thrombus: Avoiding Sternotomy and Cardiopulmonary Bypass Gaetano Ciancio, MD, Samir P. Shirodkar, MD, Mark S. Soloway, MD, Alan S. Livingstone, MD, Michael
Long-term Survival in Patients Undergoing Radical Nephrectomy and Inferior Vena Cava Thrombectomy: Single-Center Experience
 EUROPEAN UROLOGY 57 (2010) 667 672 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Long-term Survival in Patients Undergoing Radical Nephrectomy and Inferior
EUROPEAN UROLOGY 57 (2010) 667 672 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Long-term Survival in Patients Undergoing Radical Nephrectomy and Inferior
Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
 Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Financial and Other Disclosures
 Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Renal and adrenal tumors might involve the inferior vena cava
 Surgery for Acquired Cardiovascular Disease Cavoatrial tumor thrombus: Single-stage surgical approach with profound hypothermia and circulatory arrest, including a review of the literature Bruno Chiappini,
Surgery for Acquired Cardiovascular Disease Cavoatrial tumor thrombus: Single-stage surgical approach with profound hypothermia and circulatory arrest, including a review of the literature Bruno Chiappini,
Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor Thrombectomy
 EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
The Mayo Clinic experience with surgical management, complications and outcome for patients with renal cell carcinoma and venous tumour thrombus
 Original Article SURGERY, COMPLICATIONS AND OUTCOME OF RCC WITH THROMBUS BLUTE et al. The Mayo clinic experience with renal carcinoma and venous tumour thrombus is presented in this section. The authors
Original Article SURGERY, COMPLICATIONS AND OUTCOME OF RCC WITH THROMBUS BLUTE et al. The Mayo clinic experience with renal carcinoma and venous tumour thrombus is presented in this section. The authors
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Correspondence to: Jagdeesh Kulkarni,
 Original Article Surgical management of renal cell carcinoma with inferior vena caval thrombus: A teaching hospital experience Kulkarni Jagdeesh N, Acharya Purushothama U, Rizvi S Jamal, Somaya Anand C*
Original Article Surgical management of renal cell carcinoma with inferior vena caval thrombus: A teaching hospital experience Kulkarni Jagdeesh N, Acharya Purushothama U, Rizvi S Jamal, Somaya Anand C*
Patient Selection for Surgery in RCC with Thrombus. E. Jason Abel, M.D.
 Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
Renal cell carcinoma with extension of tumor thrombus into the vena cava: Surgical strategy and prognosis
 Renal cell carcinoma with extension of tumor thrombus into the vena cava: Surgical strategy and prognosis Yoshihiko Tsuji, MD, a Akinobu Goto, MD, b Isao Hara, MD, b Keiji Ataka, MD, a Chojiro Yamashita,
Renal cell carcinoma with extension of tumor thrombus into the vena cava: Surgical strategy and prognosis Yoshihiko Tsuji, MD, a Akinobu Goto, MD, b Isao Hara, MD, b Keiji Ataka, MD, a Chojiro Yamashita,
Surgery for retrohepatic caval thrombus in patients with advanced renal cell carcinoma: a case series
 Polańska-Płachta et al. World Journal of Surgical Oncology (2016) 14:11 DOI 10.1186/s12957-015-0765-5 RESEARCH Open Access Surgery for retrohepatic caval thrombus in patients with advanced renal cell carcinoma:
Polańska-Płachta et al. World Journal of Surgical Oncology (2016) 14:11 DOI 10.1186/s12957-015-0765-5 RESEARCH Open Access Surgery for retrohepatic caval thrombus in patients with advanced renal cell carcinoma:
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
2 Adrenal Disease. Open Surgery. Andrew C. Novick SURGICAL ANATOMY
 Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Leiomyosarcoma involving the inferior vena cava in an. elderly patient with reference to its operative modalities: a case report
 Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Surgical Management of Renal Cell Carcinoma (RCC) with Vena Cava Tumour Thrombus
 european urology supplements 5 (2006) 610 618 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgical Management of Renal Cell Carcinoma (RCC) with Vena Cava Tumour Thrombus
european urology supplements 5 (2006) 610 618 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgical Management of Renal Cell Carcinoma (RCC) with Vena Cava Tumour Thrombus
University of Colorado Health Sciences Center, Denver Colorado ******************** ******************
 University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
european urology 50 (2006)
 european urology 50 (2006) 302 310 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Surgical Care, Morbidity, Mortality and Follow-up after Nephrectomy for Renal
european urology 50 (2006) 302 310 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Surgical Care, Morbidity, Mortality and Follow-up after Nephrectomy for Renal
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Case Report Reresection of Colorectal Liver Metastasis with Vena Cava Resection
 Case Reports in Surgery Volume 2016, Article ID 8173048, 4 pages http://dx.doi.org/10.1155/2016/8173048 Case Report Reresection of Colorectal Liver Metastasis with Vena Cava Resection Ali Tardu, Cuneyt
Case Reports in Surgery Volume 2016, Article ID 8173048, 4 pages http://dx.doi.org/10.1155/2016/8173048 Case Report Reresection of Colorectal Liver Metastasis with Vena Cava Resection Ali Tardu, Cuneyt
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
T3 NSCLC: Chest Wall, Diaphragm, Mediastinum
 for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
Surgical Management Of TAPVR. Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital
 Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
GUIDELINES ON RENAL CELL CARCINOMA
 GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting Renal Cell Carcinoma
 Case Study TheScientificWorldJOURNAL (2009) 9, 5 9 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.6 Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting
Case Study TheScientificWorldJOURNAL (2009) 9, 5 9 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.6 Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
RPLND: Tips and Tricks
 RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma
 ONCOLOGY LETTERS 9: 125-130, 2015 Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma KEIICHI ITO 1, KENJI SEGUCHI 1, HIDEYUKI SHIMAZAKI 2, EIJI TAKAHASHI
ONCOLOGY LETTERS 9: 125-130, 2015 Tumor necrosis is a strong predictor for recurrence in patients with pathological T1a renal cell carcinoma KEIICHI ITO 1, KENJI SEGUCHI 1, HIDEYUKI SHIMAZAKI 2, EIJI TAKAHASHI
Pulmonary thromboendarterectomy (PTE) is indicated for
 Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
SURGICAL ANATOMY OF RETROPERITONEUM AND LYMPHADENECTOMY
 SURGICAL ANATOMY OF RETROPERITONEUM AND LYMPHADENECTOMY P. De Iaco S.Orsola-Malpighi Hospital - Bologna Unit Oncological Gynecology PELVIC AND AORTIC LYMPH NODE METASTASIS IN EPITHELIEL OVARIAN CANCER
SURGICAL ANATOMY OF RETROPERITONEUM AND LYMPHADENECTOMY P. De Iaco S.Orsola-Malpighi Hospital - Bologna Unit Oncological Gynecology PELVIC AND AORTIC LYMPH NODE METASTASIS IN EPITHELIEL OVARIAN CANCER
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava
 Original Article Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava P.K. Bundi, BSc. (Anat). 4 th year Medical Student, University of Nairobi, J.A. Ogeng o, BSc.
Original Article Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava P.K. Bundi, BSc. (Anat). 4 th year Medical Student, University of Nairobi, J.A. Ogeng o, BSc.
Development of a surgical safety checklist for the performance of radical nephrectomy and tumor thrombectomy
 Joshi et al. Patient Safety in Surgery 2012, 6:27 REVIEW Open Access Development of a surgical safety checklist for the performance of radical nephrectomy and tumor thrombectomy Shivam Joshi 1, Michael
Joshi et al. Patient Safety in Surgery 2012, 6:27 REVIEW Open Access Development of a surgical safety checklist for the performance of radical nephrectomy and tumor thrombectomy Shivam Joshi 1, Michael
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22
 Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Renal and Adrenal Tumors with Cardiac Invasion: Immediate Surgical Results in 14 Patients
 Renal and Adrenal Tumors with Cardiac Invasion: Immediate Surgical Results in 14 Patients Rafael Fagionato Locali, Priscila Katsumi Matsuoka, Tiago Cherbo, Edmo Atique Gabriel, Enio Buffolo Universidade
Renal and Adrenal Tumors with Cardiac Invasion: Immediate Surgical Results in 14 Patients Rafael Fagionato Locali, Priscila Katsumi Matsuoka, Tiago Cherbo, Edmo Atique Gabriel, Enio Buffolo Universidade
The management of chronic thromboembolic pulmonary
 Technique of Pulmonary Thromboendarterectomy Isabelle Opitz, MD, and Marc de Perrot, MD, MSc, FRCSC Toronto Pulmonary Endarterectomy Program, Toronto General Hospital, Ontario, Canada. Address reprint
Technique of Pulmonary Thromboendarterectomy Isabelle Opitz, MD, and Marc de Perrot, MD, MSc, FRCSC Toronto Pulmonary Endarterectomy Program, Toronto General Hospital, Ontario, Canada. Address reprint
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
Wilms Tumor and Neuroblastoma
 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Guidelines on Renal Cell
 Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
Dmytro Shchukin, 1 Vladimir Lesovoy, 1 Igor Garagatiy, 1 Gennadiy Khareba, 1 and Redouane Hsaine Introduction
 Advances in Urology, Article ID 924269, 9 pages http://dx.doi.org/10.1155/2014/924269 Research Article Surgical Approaches to Supradiaphragmatic Segment of and Right Atrium through Abdominal Cavity during
Advances in Urology, Article ID 924269, 9 pages http://dx.doi.org/10.1155/2014/924269 Research Article Surgical Approaches to Supradiaphragmatic Segment of and Right Atrium through Abdominal Cavity during
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
Lecture 02 Anatomy of the LIVER
 Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Deliberate Renal Ischemia
 Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
CT abdomen and pelvis
 CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
Obliterative hepatocavopathy ultrasound and cavography findings
 doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
Combined resection of a tumor and the inferior vena cava: report of two cases
 Surg Today (2014) 44:166 170 DOI 10.1007/s00595-012-0337-z CASE REPORT Combined resection of a tumor and the inferior vena cava: report of two cases Masatoshi Jibiki Yoshinori Inoue Toshifumi Kudo Takahiro
Surg Today (2014) 44:166 170 DOI 10.1007/s00595-012-0337-z CASE REPORT Combined resection of a tumor and the inferior vena cava: report of two cases Masatoshi Jibiki Yoshinori Inoue Toshifumi Kudo Takahiro
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Obstructed total anomalous pulmonary venous connection
 Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
LIVER RESECTION WITH INFLOW OCCLUSION. 1/2 years, then the other 11 patients died between 4 and 30 months (average survival
 HPB INTERNATIONAL 297 tumour was more aggressive or more advanced at the time of diagnosis; the figures only demonstrate that, without resection, some patients can live for prolonged periods of time (60%
HPB INTERNATIONAL 297 tumour was more aggressive or more advanced at the time of diagnosis; the figures only demonstrate that, without resection, some patients can live for prolonged periods of time (60%
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Prosthetic replacement of the inferior vena cava for malignancy
 Prosthetic replacement of the inferior vena cava for malignancy Rajabrata Sarkar, MD, PhD, Frederick R. Eilber, MD, Hugh A. Gelabert, MD, and William J. Quinones-Baldrich, MD, Los Angeles, Calif. Purpose:
Prosthetic replacement of the inferior vena cava for malignancy Rajabrata Sarkar, MD, PhD, Frederick R. Eilber, MD, Hugh A. Gelabert, MD, and William J. Quinones-Baldrich, MD, Los Angeles, Calif. Purpose:
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings
 Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Acute type A aortic dissection (Type I, proximal, ascending)
 Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Absence of infra-renal segment of inferior vena cava with anomalous right renal vein
 Absence of infra-renal segment of inferior vena cava with anomalous right renal vein Authors: VS Ajay-Chandrasekar, V Kaliyaperumal & D Alfred Location: Aintree University Hospitals NHS trust, Liverpool,
Absence of infra-renal segment of inferior vena cava with anomalous right renal vein Authors: VS Ajay-Chandrasekar, V Kaliyaperumal & D Alfred Location: Aintree University Hospitals NHS trust, Liverpool,
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Lung Cancer Resection on Cardiopulmonary Bypass. Daniel J. Boffa, MD Yale University
 Lung Cancer Resection on Cardiopulmonary Bypass Daniel J. Boffa, MD Yale University None related to talk Disclosures Disclaimers I love operating on CPB Disclaimers I love operating on CPB I avoid it for
Lung Cancer Resection on Cardiopulmonary Bypass Daniel J. Boffa, MD Yale University None related to talk Disclosures Disclaimers I love operating on CPB Disclaimers I love operating on CPB I avoid it for
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine
 Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
LiverGroup.org. Case Report Form (CRF) for STAGED procedures
 Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Impact of lymphadenectomy in management of renal cell carcinoma
 Journal of the Egyptian National Cancer Institute (2012) 24, 57 61 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com ORIGINAL ARTICLE Impact of
Journal of the Egyptian National Cancer Institute (2012) 24, 57 61 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com ORIGINAL ARTICLE Impact of
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
[7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved
![[7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved [7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved](/thumbs/82/86447000.jpg) 136 HPB INTERNATIONAL mosis. In our experience, roughly 10% of patients will have low volume amylase-rich fluid draining via the drains. Over 85% of these low volume pancreatic fistulas will heal with
136 HPB INTERNATIONAL mosis. In our experience, roughly 10% of patients will have low volume amylase-rich fluid draining via the drains. Over 85% of these low volume pancreatic fistulas will heal with
In the name ofgod. Abdomen 3. Dr. Zahiri
 In the name ofgod Abdomen 3 Dr. Zahiri Peritoneum Peritoneum It is the serous membrane(a type of loose connective tissue and is covered by mesothelium) that lines the abdominal cavity. Extensions of the
In the name ofgod Abdomen 3 Dr. Zahiri Peritoneum Peritoneum It is the serous membrane(a type of loose connective tissue and is covered by mesothelium) that lines the abdominal cavity. Extensions of the
THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR
 Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
Day 5 Respiratory & Cardiovascular: Respiratory System
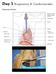 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Liver lacerations in abdominal trauma management based on anatomical knowledge: A Case report
 American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Liver lacerations in abdominal trauma management based on anatomical Ashfaq ul Hassan 1*, Rohul 1, Shifan 2,
American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Liver lacerations in abdominal trauma management based on anatomical Ashfaq ul Hassan 1*, Rohul 1, Shifan 2,
