Ce rv i c a l spondylosis is a progressive disease that is
|
|
|
- Christopher Haynes
- 6 years ago
- Views:
Transcription
1 J Neurosurg Spine 11: , 2009 Effect of spinal cord signal intensity changes on clinical outcome after surgery for cervical spondylotic myelopathy Clinical article An o o j Ch a t l e y, M.S., M.Ch., Ra j Ku m a r, M.S., M.Ch., Vi j e n d r a K. Ja i n, M.Ch., Sanjay Behari, M.Ch., and Rabi Narayan Sahu, M.Ch. Department of Neurosurgery, Sanjay Gandhi Institute of Postgraduate Medical Sciences, Lucknow, India Object. The presence of intramedullary T2 high signal intensity changes in patients with cervical spondylotic myelopathy (CSM) indicates the existence of a chronic spinal cord compressive lesion. However, the prognostic significance of signal intensity changes remains controversial. The purpose of this study was to evaluate the effect of spinal cord T2 signal intensity changes on the outcome after surgery for CSM. Method. In a prospective study, 64 patients with CSM who underwent surgical treatment between October 2006 and April 2008 using an anterior approach were included. Based on the clinical symptoms and signs present, the severity of neurological deficits of all patients was scored according to a modified Japanese Orthopaedic Association scale score for CSM just before the surgery and at 6 months follow-up. Recovery rates were calculated at 6 months. Results. There were 22 patients who did not have spinal cord intensity changes on MR imaging and 44 who demonstrated high-intensity signal changes on T2-weighted images (focal or segmental). No statistically significant differences were found in recovery rates between cases with T2 signal intensity changes and those with no signal intensity changes. However, the postoperative modified Japanese Orthopaedic Association scale scores and the recovery rates were much lower in patients with multisegmental signal intensity changes compared with those without these changes or those with focal signal intensity change, and ANOVA demonstrated this difference to be statistically significant (p < 0.05). Conclusion. Multisegmental spinal cord signal intensity changes on T2-weighted MR imaging are predictors of a poor outcome in terms of functional recovery rate in patients undergoing operations for CSM. (DOI: / SPINE091) Ke y Wo r d s cervical spine cervical spondylotic myelopathy spinal cord signal intensity Abbreviations used in this paper: CSM = cervical spondylotic myelopathy; mjoa = modified Japanese Orthopaedic Association. Ce rv i c a l spondylosis is a progressive disease that is a frequent cause of cervical myelopathy, especially in patients > 50 years of age. The natural history of CSM is frequently one of slow, progressive neurological deterioration. The sequences of degenerative changes that constitute cervical spondylosis include intervertebral disc degeneration, disc space collapse, osteophyte formation, and hypertrophy of the ligamentum flavum, lamina, and facets. These changes, when occurring in conjunction with a narrow canal, predispose the aging patient to CSM. 25 Spinal cord injury may occur due to mechanical compression and vascular compromise, with resultant lesions in the dorsal and lateral columns and degeneration of the ascending and descending tracts. 18 In the past, the radiological diagnosis of CSM was dependent on myelography, CT, and CT myelography. At present, MR imaging is the preferred radiological diagnostic tool that can not only depict spinal cord compression, but also reflect the pathological changes in the spinal cord. 15,31 The neurological outcome of decompressive surgery for CSM is influenced by several factors. Although each factor may have an independent effect, it is more likely that the outcome is influenced by more than 1 factor. Many authors 15,28,29,31 have reported intramedullary high signal intensity changes on T2-weighted MR imaging in patients with compressive spondylotic lesions of the cervical spinal cord. Such intramedullary high signal intensity abnormality is presumed to be myelomalacia or cord gliosis secondary to a long standing compressive effect on the spinal cord. 29 Therefore, the presence of intramedullary high signal intensity in patients with CSM indicates the existence of a chronic spinal cord compressive lesion. However, the prognostic significance of signal intensity changes remains controversial. The purpose of this study was to evaluate the effect of spinal cord signal intensity 562 J Neurosurg: Spine / Volume 11 / November 2009
2 Spinal cord intensity changes in cervical spondylotic myelopathy changes on outcome following surgery for CSM, and to identify other factors associated with these cord intensity changes that may affect the outcome. Methods J Neurosurg: Spine / Volume 11 / November 2009 TABLE 1: Clinical features of the 64 patients included in the study Clinical Features No. of Cases (%) symptoms weakness 50 (78.1) all 4 limbs 31 (48.4) both upper limbs 10 (15.6) both lower limbs 2 (3.1) right-sided limbs 1 (1.6) 1 upper limb 6 (9.4) stiffness 51 (79.7) numbness radicular myelopathic radiculo-myelopathic paraesthesia radicular myelopathic radiculo-myelopathic pain neck pain radicular funicular sphincteric dysfunction bladder bowel 12 (18.8) 33 (51.6) 1 (1.6) 15 (23.4) 19 (29.7) 6 (9.4) 25 (39.1) 17 (26.6) 3 (4.7) 27 (42.2) 21 (32.9) walking difficulty 55 (86.0) clumsiness of hands 47 (73.4) Lhermitte phenomenon 1 (1.6) respiratory difficulty 1 (1.6) signs increased tone 59 (92.2) wasting 9 (14.1) weakness 54 (84.4) Hoffman sign 33 (51.6) sensory loss 46 (71.9) loss of proprioception 20 (31.3) spinal tenderness 13 (20.3) Patient Population In a prospective study, 64 of 137 consecutive patients who underwent operations for symptomatic CSM/radiculomyelopathy using the anterior approach between October 2006 and April 2008 at Sanjay Gandhi Postgraduate Institute of Medical Sciences in Lucknow, India, were included for the purpose of the study. The inclusion criteria for the study were those patients with CSM/radiculomyelopathy who underwent an operation using an anterior approach with follow-up > 6 months. The study exclusion criteria were: 1) the presence of an ossified posterior longitudinal ligament; 2) history of trauma; 3) cervical radiculopathy with no features of myelopathy; 4) undergoing an operation using the posterior approach; 5) previous surgery for CSM; 6) associated disorders such as atlantoaxial dislocation, basilar invagination, rheumatoid arthritis, and ankylosing spondylitis; and 7) follow-up < 6 months. Cervical laminectomy for treatment of CSM may lead to late instability with progressive kyphotic deformity or swan neck deformity. This procedure does not directly address the ventral compression or correct the dynamic component. To address these shortcomings, fusion following laminectomy or laminoplasty may be performed. However, we prefer using the anterior approach for all patients with ventral compression, except for older patients with significant comorbid conditions, a lordotic spine, and compression at > 3 levels. Therefore, these cases were not included in the study because they were very few in number and included other significant factors such as very old age and significant comorbid conditions that adversely affect prognosis. Of the 137 patients, 73 were excluded because they did not fulfill the inclusion criteria. There were 19 patients with ossified posterior longitudinal ligaments, 12 with a history of trauma, 11 who underwent surgery using a posterior approach, 15 with previous surgery for CSM, 8 with associated disorders (as noted in the exclusion criteria), and another 8 patients with follow-up < 6 months. All of these patients were excluded from the study. Among the 64 patients, 57 were men and 7 were women. The mean age of the patients was 47.1 years (range years). Duration of symptoms ranged from 1 to 84 months (mean months). The diagnosis of CSM was made on the basis of clinical and radiological findings. Clinical symptoms and signs of the patient population are summarized in Table 1. All patients showed neurological findings compatible with CSM/radiculomyelopathy. Based on the clinical symptoms and signs, the severity of neurological deficits of all patients was scored according to an mjoa scale score 2,7 for CSM (Table 2) just before surgery and at 6 months follow-up. The range of this score is 0 17, in which 0 represents maximal neurological deficits and 17 represents no neurological deficits. All patients were followed up for a minimum of 6 months. The mean follow-up period was months (range 6 20 months). The recovery rate after treatment was calculated using the Hirabayashi 6 method as follows: (postoperative mjoa scale score preoperative mjoa scale score / 17 preoperative mjoa scale score) 100 Imaging Studies Radiological investigations included plain radiographs of the cervical spine in the anteroposterior and lateral flexion-extension views, and MR imaging of the cervical spine. The curvature of the spine, reduced disc space height, and presence of osteophytes, spondylolisthesis, and vertebral fusion were examined using plain radiographs of the cervical spine. The MR imaging protocol 563
3 A. Chatley et al. TABLE 2: Neurological outcome for anterior spondylectomy and laminoplasty* Parameter Anterior Spondylectomy Laminoplasty p Value preop JOA score 11.6 ± ± postop (4 6 weeks) JOA score 14.7 ± ± follow-up JOA score 14.5 ± ± neurological improvement rate at follow-up (%) 67.5 ± ± * Data expressed as the mean ± SD. Mann-Whitney U-test. included sagittal and axial T1- and T2-weighted images, using a slice thickness of 5 mm to detect the level and type of disc protrusion. Attention was mainly directed to the sagittal T2-weighted images, to examine increased signal intensity resulting from spinal cord compression. Intensity changes in the spinal cord on T1-weighted images were not taken into consideration. The T2 hyperintensity changes were further quantified and divided into 2 groups: focal (< 2 segments) and multisegmental ( 2 segments). Radiological findings are summarized in Table 3. The disc level at which MR imaging showed either an intrinsic signal intensity change of the spinal cord or a maximal compression of the spinal cord was considered the intervertebral disc level responsible for cervical compressive myelopathy. Surgical Procedures All patients underwent surgery using an anterior approach. The surgical procedures performed are summarized in Table 4. The decision to perform surgery was made on the basis of clinical-radiological correlation. Mild disc herniations, without any compression of the thecal sac, were not targeted. In all cases, postoperative radiographs of the cervical spine were performed on the 1st postoperative day. Operative complications in these patients included graft extrusion in 3 cases, CSF leak in 2, hoarseness of voice in 2, and donor site infection in 2 cases. Statistical Analysis Statistical analysis was conducted using SPSS statistical software version 15 for Windows (SPSS, Inc.). The primary variable analyzed as an indicator of surgical outcome was the recovery rate; other factors taken into account were duration of symptoms, age at surgery, and the pre- and postoperative mjoa scale scores. Initially the entire population was divided into 2 groups: one in which high-intensity signal changes were present on T2-weighted images, and one in which they were absent. The group in which these signal changes were present was then divided into 2 subgroups according to the extension of the lesion: focal (lesion spanning < 2 segments) and multisegmental (lesion spanning 2 segments). To compare the recovery rate between groups, we used the independent sample t-test when data were continuous and normally distributed. The Mann-Whitney U-test was used when these conditions were not fulfilled. A linear regression model was performed to verify whether signal intensity changes could be used to predict outcome. Probability values < 0.05 were considered statistically significant. Results For the entire population the mean preoperative and postoperative (at 6 months) mjoa scale scores were ± 2.86 and ± 2.71, respectively. The mean followup duration was months (range 6 20 months). The mean recovery rate was ± 36.92%. There were 22 patients who did not have cord signal intensity changes on MR imaging and 44 who demonstrated high-intensity signal changes on T2-weighted images. Differences in mean values between patients with and without high-intensity signal changes on T2-weighted images are shown in Table 5 for the following variables: age at surgery, duration of symptoms, pre- and postoperative mjoa scale scores, and postoperative recovery rates. The Student t- test revealed no statistically significant differences in recovery rates between cases of T2 signal intensity change and those with no signal change, and none of the other variables was shown to exhibit any significant intergroup differences. A summary of the data obtained in the subgroups of patients (focal and segmental intensity changes) in whom the T2-weighted imaging revealed high-intensity signals is provided in Table 6. The postoperative mjoa scale scores and the recovery rates were much lower in patients with multisegmental signal intensity change as compared with those without this change or those with focal signal intensity change; ANOVA demonstrated this difference to be statistically significant (p < 0.05). All other variables (age at surgery, duration of symptoms, preoperative mjoa scale scores) did not exhibit any significant differences between the 2 groups. However, there were no statistically significant differences in recovery rates between cases of focal T2 signal intensity change and those with no signal change. All other variables (age at surgery, duration of symptoms, pre- and postoperative mjoa scale scores) also did not exhibit any significant differences. Discussion The role of MR imaging signal intensity changes in patients with cervical spine disorders has been widely studied. Abnormal T2-weighted signal intensity has been described in numerous disorders of the cervical spine. Different authors have speculated on both the histolopatho- 564 J Neurosurg: Spine / Volume 11 / November 2009
4 Spinal cord intensity changes in cervical spondylotic myelopathy TABLE 3: Radiological findings Cervical Spine Characteristic No. of Cases (%) plain radiograph prominent osteophytes 41 (64.1) configuration lordotic straightening kyphotic reduced height of disc space single level multiple level 45 (70.3) 17 (26.6) 2 (3.1) 35 (54.7) 15 (23.4) vertebral fusion 5 (7.8) subluxation 4 (6.3) MR imaging level of disc bulge C2 3 1 (1.6) C3 4 7 (10.9) C4 5 5 (7.8) C (26.6) C6 7 7 (10.9) C2 3, C3 4 1 (1.6) C3 4, C4 5 3 (4.7) C3 4, C5 6 2 (3.1) C3 4, C5 6, C6 7 1 (1.6) C4 5, C5 6 7 (10.9) C4 5, C6 7 2 (3.1) C4 5, C5 6, C6 7 1 (1.6) C5 6, C (15.6) spinal cord intensity changes absent focal multisegmental 22 (34.4) 31 (48.4) 11 (17.2) logical 1,12,16,17,21,28 and prognostic significance 12,17,19,22,29,35 of these signal intensity changes. In 1987, Takahashi et al. 28 originally proposed that the T2 high-intensity signal changes represented myelomalacia from gliosis, edema, demyelination, and microcavity formation. However, controversy persisted with respect to the specific pathological mechanism involved. Ramanauskas et al. 24 divided myelomalacia into 3 stages. They proposed that in the early stage, a change in the signal intensity of the spinal cord observed on MR imaging reflected cord edema, and that in the intermediate stage, a change reflected cystic necrosis of the central gray matter after prolonged cord edema. These authors also reported that in the early and intermediate stages, the spinal cord demonstrated high signal intensity on T2-weighted sequences, and that in the late stage, low signal intensity on T1-weighted images and high signal intensity on T2-weighted sequences were noted. It was proposed by Al Mefty et al. 1 that the high-intensity signal on T2-weighted images is secondary to myelomalacia, with cystic cord necrosis and syrinx formation evidenced by low T1/high T2 signal characteristics. Haupts and Haan 5 observed that there can be extension of T2 signal changes above and below the regions of stenosis and proposed a shearing mechanism as the underlying pathological process. Mehalic et al. 15 proposed that T2 high-intensity signal changes were nonspecific and may represent a variety of pathological processes including edema, inflammation, vascular ischemia, gliosis, or myelomalacia. In acute spinal cord trauma, hyperintense T2-weighted changes have been assumed to be secondary to cord edema or small, petechial intramedullary hemorrhage. Larger hemorrhage, with proportionally greater deoxyhemoglobin, appears as hypointense lesions on T2-weighted images. 4,8,10 Eventual cyst formation may present with hypointensity on T1-weighted images and hyperintensity on T2-weighted sections. 23,33,34 Matsuda et al. 12 proposed that reversible signal changes may be secondary to vascular pathology and irreversible lesions could represent chronic cord damage, with ensuing gliosis, demyelination, and microcavity formation. Similarly, Taneichi et al. 30 proposed that reversible T2-weighted hyperintensity correlates with simple edema, whereas gliosis presents with irreversible signal changes, based on serial MR imaging results and correlation with patient clinical status. Based on the results reported in the literature, high-intensity signal changes on T2-weighted images indicate edema and gliosis (which may be reversible), whereas low-intensity signal changes on T1-weighted images can represent myelomalacia and necrosis (which are considered irreversible). 21 Correlation between MR imaging findings and clinical presentation/recovery after therapy remain unclear. TABLE 4: Summary of the surgical procedures performed Surgical Procedure No. of Cases (%) discoidectomy without bone grafting 9 (14.1) Smith-Robinson procedure 25 (39.1) Cloward procedure 2 (3.1) corpectomy with grafting 22 (34.4) corpectomy with grafting and plating 4 (6.3) Smith-Robinson at upper level and corpectomy with grafting at lower level 1 (1.6) 2 consecutive-level corpectomy with grafting and plating 1 (1.6) J Neurosurg: Spine / Volume 11 / November
5 A. Chatley et al. TABLE 5: Comparison between patients with no signal intensity change and those with signal intensity change on T2-weighted images* Variable Signal Intensity Change Absent (22 Patients) Present (44 Patients) age (yrs) ± ± duration of symptoms (mos) 6.16 ± ± preop mjoa scale score ± ± 2.65 postop mjoa scale score ± ± 2.86 recovery rate (%) ± ± * All values given as mean ± SD; p > 0.05 for all comparisons. TABLE 6: Comparison between patients with focal signal intensity change and those with multisegmental signal intensity change on T2-weighted images* Variable Signal Intensity Change Focal (31 Patients) Multisegmental (11 Patients) p Value age (yrs) ± ± >0.05 duration of symptoms (mos) ± ± >0.05 preop mjoa scale score ± ± 2.58 >0.05 postop mjoa scale score ± ± 3.64 <0.05 recovery rate (%) ± ± <0.05 * All values given as mean ± SD. Several studies have confirmed that patients with lowintensity signal changes on T1-weighted images have a poor prognosis. 14,17,27 However, the prognostic value of high-intensity signal changes on T2-weighted images remains controversial. Therefore, we limited our study to the changes on T2-weighted images. Some authors attest to increased severity of neurological deficit concomitant with an increased T2 signal, 9,12,20,29,34 whereas others note no correlation between the two factors. 21,31 Matsumoto et al. 13 and other authors 11,19,35 have observed that altered signal intensity on T2-weighted images was not related to poor outcome in patients with CSM. Singh et al. 26 reported that patients with worse signal changes on MR imaging subsequently experienced greater benefits from surgery as measured by improvement in walking parameters and other rating scales (myelopathy disability index, Nurick scale, and Ranawat classification). In some other studies, 3,32 although it appeared that there was a tendency toward a poorer outcome in patients with T2 high-intensity signal changes, statistical significance was reached only after quantifying these images. In our study, patients were initially divided into 2 groups: those without T2 high-intensity signal change and those with T2 high-intensity signal change. The recovery rate, although higher in patients without these signal changes (58.53 ± 32.45% vs ± 38.38%, respectively), did not differ significantly between the 2 groups. The other parameters (age at surgery, duration of symptoms, preand postoperative mjoa scale scores) also did not exhibit statistically significant intergroup differences. On further quantification of the T2 spinal cord signal-intensity changes (focal/multisegmental), it was observed that the recovery rate of the 11 patients in whom T2-weighted images revealed signal intensity changes spanning multiple levels was significantly worse (17.33 ± 38.74%) than that in patients with focal (52.35 ± 34.36%) or no signal changes (58.53 ± 32.45%) on T2-weighted images. The postoperative mjoa scale scores were also significantly lower in these patients (11.27 ± 3.64) as compared with the patients with focal (13.90 ± 2.21) or no signal changes (14.45 ± 2.24). Although patients with multisegmental changes were older and were symptomatic for a longer duration as compared with patients in the other 2 groups, these differences were not statistically significant (Tables 5 and 6). Similarly, there were no significant differences in the 3 groups regarding preoperative mjoa scale scores. The regression model confirmed the value of multisegmental T2 spinal cord signal intensity changes as predictors of a poor outcome in terms of recovery rate. Conclusions Based on our study, we conclude that patients with CSM and high-intensity signal changes on T2-weighted images do not necessarily have a poorer prognosis when compared with patients with no signal intensity changes. Multisegmental T2 cord intensity changes, however, are predictors of a poor outcome in terms of functional recovery rate in patients who undergo operations for CSM. Finally, focal high-intensity changes on T2-weighted images do not indicate a poor functional recovery rate. Disclaimer The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Acknowledgment The authors gratefully acknowledge the kind help provided by Professor Uttam Singh of the Department of Biostatistics, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow, India, in the statistical analysis conducted in this paper. References 1. Al-Mefty O, Harkey LH, Middleton TH, Smith RR, Fox JL: Myelopathic cervical spondylotic lesions demonstrated by magnetic resonance imaging. J Neurosurg 68: , Benzel EC, Lancon J, Kesterson L, Hadden T: Cervical laminectomy and dentate ligament section for cervical spondylotic myelopathy. J Spinal Disord 4: , Fernández de Rota JJ, Meschian S, Fernández de Rota A, Urbano V, Baron M: Cervical spondylotic myelopathy due to chronic compression: the role of signal intensity changes in magnetic resonance images. J Neurosurg Spine 6:17 22, Flanders AE, Schaefer DM, Doan HT, Mishkin MM, Gonzalez CF, Northrup BE: Acute cervical spine trauma: correlation of MR imaging findings with degree of neurologic deficit. Radiology 177:25 33, J Neurosurg: Spine / Volume 11 / November 2009
6 Spinal cord intensity changes in cervical spondylotic myelopathy 5. Haupts M, Haan J: Further aspects of MR-signal enhancements in stenosis of the cervical spinal canal. MRI investigations in correlation to clinical and CSF findings. Neuroradiology 30: , Hirabayashi K, Miyakawa J, Satomi K, Maruyama T, Wakano K: Operative results and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine 6: , Hukuda S, Mochizuki T, Ogata M, Shichikawa K, Shimomura Y: Operations for cervical spondylotic myelopathy: A comparison of the results of anterior and posterior procedures. J Bone Joint Surg Br 67: , Kadoya S, Nakamura T, Kobayashi S, Yamamoto I: Magnetic resonance imaging of acute spinal cord injury. Report of three cases. Neuroradiology 29: , Kohno K, Kumon Y, Oka Y, Matsui S, Ohue S, Sakaki S: Evaluation of prognostic factors following expansive laminoplasty for cervical spinal stenotic myelopathy. Surg Neurol 48: , Kulkarni MV, McArdle CB, Kopanicky D, Miner M, Cotler HB, Lee KF, et al: Acute spinal cord injury: MR imaging at 1.5 T. Radiology 164: , Lee TT, Manzano GR, Green BA: Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement. J Neurosurg 86:64 68, Matsuda Y, Miyazaki K, Tada K, Yasuda A, Nakayama T, Murakami H, et al: Increased MR signal intensity due to cervical myelopathy. Analysis of 29 surgical cases. J Neurosurg 74: , Matsumoto M, Toyama Y, Ishikawa M, Chiba K, Suzuki N, Fujimura Y: Increased signal intensity of the spinal cord on magnetic resonance images in cervical compressive myelopathy. Does it predict the outcome of conservative treatment? Spine 25: , Matsuyama Y, Kawakami N, Yanase M, Yoshihara H, Ishiguro N, Kameyama T, et al: Cervical myelopathy due to OPLL: clinical evaluation by MRI and intraoperative spinal sonography. J Spinal Disord Tech 17: , Mehalic TF, Pezzuti RT, Applebaum BI: Magnetic resonance imaging and cervical spondylotic myelopathy. Neurosurgery 26: , Morio Y, Teshima R, Nagashima H, Nawata K, Yamasaki D, Nanjo Y: Correlation between operative outcomes of cervical compression myelopathy and mri of the spinal cord. Spine 26: , Morio Y, Yamamoto K, Kuranobu K, Murata M, Tuda K: Does increased signal intensity of the spinal cord on MR images due to cervical myelopathy predict prognosis? Arch Orthop Trauma Surg 113: , Morishita Y, Hida S, Naito M, Matsushima U: Evaluation of cervical spondylotic myelopathy using somatosensory-evoked potentials. Int Orthop 29: , Naderi S, Ozgen S, Pamir MN, Ozek MM, Erzen C: Cervical spondylotic myelopathy: surgical results and factors affecting prognosis. Neurosurgery 43:43 50, Nakamura M, Fujimura Y: Magnetic resonance imaging of the spinal cord in cervical ossification of the posterior longitudinal ligament. Can it predict surgical outcome? Spine 23: 38 40, Ohshio I, Hatayama A, Kaneda K, Takahara M, Nagashima K: Correlation between histopathologic features and magnetic resonance images of spinal cord lesions. Spine 18: , Okais N, Moussa R, Hage P: Value of increased MRI signal intensity in cervical arthrosis in myelopathies. Neurochirurgie 43: , Quencer RM, Bunge RP, Egnor M, Green BA, Puckett W, Naidich TP, et al: Acute traumatic central cord syndrome: MRI-pathological correlations. Neuroradiology 34:85 94, Ramanauskas WL, Wilner HI, Metes JJ, Lazo A, Kelly JK: MR imaging of compressive myelomalacia. J Comput Assist Tomogr 13: , Sadasivan KK, Reddy RP, Albright JA: The Natural History of Cervical Spondylotic Myelopathy. Yale J Biol Med 66: , Singh A, Crockard HA, Platts A, Stevens J: Clinical and radiological correlates of severity and surgery-related outcome in cervical spondylosis. J Neurosurg 94 (2 Suppl): , Suri A, Chabbra RP, Mehta VS, Gaikwad S, Pandey RM: Effect of intramedullary signal changes on the surgical outcome of patients with cervical spondylotic myelopathy. Spine J 3:33 45, Takahashi M, Sakamoto Y, Miyawaki M, Bussaka H: Increased MR signal intensity secondary to chronic cervical cord compression. Neuroradiology 29: , Takahashi M, Yamashita Y, Sakamoto Y, Kojima R: Chronic cervical cord compression: clinical significance of increased signal intensity on MR images. Radiology 173: , Taneichi H, Abumi K, Kaneda K, Terae S: Monitoring the evolution of intramedullary lesions in cervical spine cord injury. Qualitative and quantitative analysis with sequential MR imaging. Paraplegia 32:9 18, Wada E, Ohmura M, Yonenobu K: Intramedullary changes of the spinal cord in cervical spondylotic myelopathy. Spine 20: , Wada E, Yonenobu K, Suzuki S, Kanazawa A, Ochi T: Can intramedullary signal change on magnetic resonance imaging predict surgical outcome in cervical spondylotic myelopathy? Spine 24: , Yamashita Y, Takahashi M, Matsuno Y, Kojima R, Sakamoto Y, Oguni T, et al: Acute spinal cord injury: magnetic resonance imaging correlated with myelopathy. Br J Radiol 64: , Yamashita Y, Takahashi M, Matsuno Y, Sakamoto Y, Oguni T, Sakae T, et al: Chronic injuries of the spinal cord: assessment with MR imaging. Radiology 175: , Yone K, Sakou T, Yanase M, Ijiri K: Preoperative and postoperative magnetic resonance image evaluations of the spinal cord in cervical myelopathy. Spine 17 (10 Suppl):S388 S392, 1992 Manuscript submitted January 1, Accepted June 23, Address correspondence to: Raj Kumar, M.S., M.Ch., Department of Neurosurgery, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow, UP, India rajkumar@sgpgi. ac.in. J Neurosurg: Spine / Volume 11 / November
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 13:319 323, 2010 Using the T2-weighted magnetic resonance imaging signal intensity ratio and clinical manifestations to assess the prognosis of patients with cervical ossification of
J Neurosurg Spine 13:319 323, 2010 Using the T2-weighted magnetic resonance imaging signal intensity ratio and clinical manifestations to assess the prognosis of patients with cervical ossification of
Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
Spinal Cord (2005) 43, & 2005 International Spinal Cord Society All rights reserved /05 $
 (2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
(2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
CSM is the most common cause of spinal cord dysfunction
 Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
CERVICAL SPONDYLOTIC myelopathy is one of the
 ORIGINAL ARTICLE Gait Analysis for Evaluating the Relationship Between Increased Signal Intensity on T2-Weighted Magnetic Resonance Imaging and Gait Function in Cervical Spondylotic Myelopathy Chung Reen
ORIGINAL ARTICLE Gait Analysis for Evaluating the Relationship Between Increased Signal Intensity on T2-Weighted Magnetic Resonance Imaging and Gait Function in Cervical Spondylotic Myelopathy Chung Reen
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Disclosures. Introduction. Purpose. Pulmonary Function and Complications in Patients with Cervical Myelopathy and Myelomalacia
 Pulmonary Function and Complications in Patients with Cervical Myelopathy and Myelomalacia Jeremy D. Shaw, MD, MS; Juli Martha, MPH; Ling Li, MSPH; David J. Hunter, MD, PhD; Brian Kwon, MD; Tal Rencus,
Pulmonary Function and Complications in Patients with Cervical Myelopathy and Myelomalacia Jeremy D. Shaw, MD, MS; Juli Martha, MPH; Ling Li, MSPH; David J. Hunter, MD, PhD; Brian Kwon, MD; Tal Rencus,
Impact of Preoperative Spinal Cord Signal Intensity and Symptom Duration on Surgical Outcome of the Patients with Cervical Spondylotic Myelopathy
 American Journal of Clinical Neurology and Neurosurgery Vol. 1, No. 2, 2015, pp. 102-106 http://www.aiscience.org/journal/ajcnn Impact of Preoperative Spinal Cord Signal Intensity and Symptom Duration
American Journal of Clinical Neurology and Neurosurgery Vol. 1, No. 2, 2015, pp. 102-106 http://www.aiscience.org/journal/ajcnn Impact of Preoperative Spinal Cord Signal Intensity and Symptom Duration
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Spinal cord edema: unusual magnetic resonance imaging findings in cervical spondylosis
 J Neurosurg (Spine 1) 99:8 13, 2003 Spinal cord edema: unusual magnetic resonance imaging findings in cervical spondylosis JANGBO LEE, M.D., IZUMI KOYANAGI, M.D., KAZUTOSHI HIDA, M.D., TOSHITAKA SEKI,
J Neurosurg (Spine 1) 99:8 13, 2003 Spinal cord edema: unusual magnetic resonance imaging findings in cervical spondylosis JANGBO LEE, M.D., IZUMI KOYANAGI, M.D., KAZUTOSHI HIDA, M.D., TOSHITAKA SEKI,
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Orthopaedics and Rehabilitation Medicine Fuculty of Medical Sciences University of Fukui
 Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical spondylotic myelopathy (CSM) is a
 WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Risk factors for development of cervical spondylotic myelopathy: results of a systematic review
 Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
Cervical spondylotic myelopathy: Make the difficult diagnosis, then refer for surgery
 REVIEW CME CREDIT WILLIAM E. MCCORMICK, MD Department of Neurosurgery, The Cleveland Clinic MICHAEL P. STEINMETZ, MD Department of Neurosurgery, The Cleveland Clinic EDWARD C. BENZEL, MD Department of
REVIEW CME CREDIT WILLIAM E. MCCORMICK, MD Department of Neurosurgery, The Cleveland Clinic MICHAEL P. STEINMETZ, MD Department of Neurosurgery, The Cleveland Clinic EDWARD C. BENZEL, MD Department of
Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
 283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
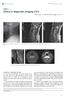 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Clinical significance of MRI/ 18 F-FDG PET fusion imaging of the spinal cord in patients with cervical compressive myelopathy
 Eur J Nucl Med Mol Imaging (2012) 39:1528 1537 DOI 10.1007/s00259-012-2192-y ORIGINAL ARTICLE Clinical significance of MRI/ 18 F-FDG PET fusion imaging of the spinal cord in patients with cervical compressive
Eur J Nucl Med Mol Imaging (2012) 39:1528 1537 DOI 10.1007/s00259-012-2192-y ORIGINAL ARTICLE Clinical significance of MRI/ 18 F-FDG PET fusion imaging of the spinal cord in patients with cervical compressive
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical Treatment of Cervical Compressive Myelopathy
 International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis
 Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
C ervical spondylosis is an important and frequent cause
 256 PAPER The use of evoked potentials for clinical correlation and surgical outcome in cervical spondylotic myelopathy with intramedullary high signal intensity on MRI R K Lyu, L M Tang, C J Chen, C M
256 PAPER The use of evoked potentials for clinical correlation and surgical outcome in cervical spondylotic myelopathy with intramedullary high signal intensity on MRI R K Lyu, L M Tang, C J Chen, C M
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement
 Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy
 Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy Rui Gao., Lili Yang., Huajiang Chen, Yang Liu, Lei Liang, Wen Yuan* Department of Spine Surgery, Changzheng Orthopedic
Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy Rui Gao., Lili Yang., Huajiang Chen, Yang Liu, Lei Liang, Wen Yuan* Department of Spine Surgery, Changzheng Orthopedic
It is recommended that preoperative SEPs be considered. Clinical prognostic indicators of surgical outcome in cervical spondylotic myelopathy
 J Neurosurg Spine 11:000 000, 11:112 118, 2009 Clinical prognostic indicators of surgical outcome in cervical spondylotic myelopathy La n g s t o n T. Ho l ly, M.D., 1 Pa u l G. Ma t z, M.D., 2 Pa u l
J Neurosurg Spine 11:000 000, 11:112 118, 2009 Clinical prognostic indicators of surgical outcome in cervical spondylotic myelopathy La n g s t o n T. Ho l ly, M.D., 1 Pa u l G. Ma t z, M.D., 2 Pa u l
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
흉추척수증을유발한황색인대골화증의골절 - 증례보고 -
 대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
Title. Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): Issue Date Doc URL
 Title Secondary medulla oblongata involvement following mi instability in a patient with ossification of the po Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): 126-129 Issue
Title Secondary medulla oblongata involvement following mi instability in a patient with ossification of the po Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): 126-129 Issue
Surgical outcomes for lumbar spinal canal stenosis with coexisting cervical stenosis (tandem spinal stenosis): a retrospective analysis of 565 cases
 Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Junming Cao, Yongsheng Lin, Xiangbei Qi, Zhihong Wang, Yipeng Yang, Hehuan Xia, Bin Xu
 Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Key words: Professional Med J 2018;25(8): CERVICAL LAMINOPLASTY
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Effect of Age on the Benefits of Early Decompression for Cervical Spondylotic Myelopathy
 The Effect of Age on the Benefits of Early Decompression for Cervical Spondylotic Myelopathy Publish date: September 20, 2018 Authors: David J. Kusin, MD Uri M. Ahn, MD Nicholas U. Ahn, MD Author Affiliation
The Effect of Age on the Benefits of Early Decompression for Cervical Spondylotic Myelopathy Publish date: September 20, 2018 Authors: David J. Kusin, MD Uri M. Ahn, MD Nicholas U. Ahn, MD Author Affiliation
Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy
 852 Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy LING-DE KONG *, LING-CHEN MENG *, LIN-FENG WANG, YONG SHEN, PAN WANG and ZI-KUN
852 Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy LING-DE KONG *, LING-CHEN MENG *, LIN-FENG WANG, YONG SHEN, PAN WANG and ZI-KUN
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Cervical myelopathy is caused by spinal canal narrowing
 An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for severity scores
 J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy
 Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Spine. Neuroradiology. Spine. Spine Pathology. Distribution of fractures. Radiological algorithm. Role of radiology 18/11/2015
 Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Spinal Imaging. ssregypt.com. Mamdouh Mahfouz MD
 Spinal Imaging Degenerative diseases ssregypt.com Mamdouh Mahfouz MD mamdouh.m5@gmail.com MRI Open MRI Closed Extremity MRI Dynamic MRI Dynamic MRI The bed rotates from Upright to Recumbent, stopping at
Spinal Imaging Degenerative diseases ssregypt.com Mamdouh Mahfouz MD mamdouh.m5@gmail.com MRI Open MRI Closed Extremity MRI Dynamic MRI Dynamic MRI The bed rotates from Upright to Recumbent, stopping at
Cervical spondylotic myelopathy (CSM) is a progressive
 literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
Study of current pattern of Cervical Spondylotic Myelopathy and to evaluate the modalities of treatment
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 01-14 www.iosrjournals.org Study of current pattern of Cervical Spondylotic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 01-14 www.iosrjournals.org Study of current pattern of Cervical Spondylotic
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Results of a Survey of the Cervical Spine Research Society
 Ventral Versus Dorsal Decompression for Cervical Spondylotic Myelopathy: Surgeons Assessment of Eligibility for Randomization in a Proposed Randomized Controlled Trial Results of a Survey of the Cervical
Ventral Versus Dorsal Decompression for Cervical Spondylotic Myelopathy: Surgeons Assessment of Eligibility for Randomization in a Proposed Randomized Controlled Trial Results of a Survey of the Cervical
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels
 National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
This man needs to see a Doctor! So wrote an exasperated neurologist after reviewing a patient
 i34* SURGICAL DISORDERS OF THE CERVICAL SPINE: PRESENTATION AND MANAGEMENT OF COMMON DISORDERS c SPINAL Correspondence to: Mr George Malcolm, Department of Neurosurgery, Frenchay Hospital, Frenchay Park
i34* SURGICAL DISORDERS OF THE CERVICAL SPINE: PRESENTATION AND MANAGEMENT OF COMMON DISORDERS c SPINAL Correspondence to: Mr George Malcolm, Department of Neurosurgery, Frenchay Hospital, Frenchay Park
ASJ. Analysis of the Prevalence and Distribution of Cervical and Thoracic Compressive Lesions of the Spinal Cord in Lumbar Degenerative Disease
 Asian Spine Journal Asian Spine Clinical Journal Study Cervical and thoracic Asian compressive Spine J 2014;8(1):19-26 lesions in http://dx.doi.org/10.4184/asj.2014.8.1.19 lumbar degenerative disease 19
Asian Spine Journal Asian Spine Clinical Journal Study Cervical and thoracic Asian compressive Spine J 2014;8(1):19-26 lesions in http://dx.doi.org/10.4184/asj.2014.8.1.19 lumbar degenerative disease 19
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Laminoplasty versus laminectomy for multi-level cervical spondylotic myelopathy: a systematic review of the literature
 Lao et al. Journal of Orthopaedic Surgery and Research 2013, 8:45 RESEARCH ARTICLE Open Access Laminoplasty versus laminectomy for multi-level cervical spondylotic : a systematic review of the literature
Lao et al. Journal of Orthopaedic Surgery and Research 2013, 8:45 RESEARCH ARTICLE Open Access Laminoplasty versus laminectomy for multi-level cervical spondylotic : a systematic review of the literature
Review Article The Natural History and Clinical Presentation of Cervical Spondylotic Myelopathy
 Advances in Orthopedics Volume 2012, Article ID 480643, 4 pages doi:10.1155/2012/480643 Review Article The Natural History and Clinical Presentation of Cervical Spondylotic Myelopathy ChesterK.Yarbrough,RoryK.J.Murphy,WilsonZ.Ray,andToddJ.Stewart
Advances in Orthopedics Volume 2012, Article ID 480643, 4 pages doi:10.1155/2012/480643 Review Article The Natural History and Clinical Presentation of Cervical Spondylotic Myelopathy ChesterK.Yarbrough,RoryK.J.Murphy,WilsonZ.Ray,andToddJ.Stewart
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
The Comparison of Hemilaminectomy and Laminoplasty Procedures in the Surgical Treatment of Cervical Spondylotic Myelopathy
 DOI: 10.5137/1019-5149.JTN.14736-15.1 Received: 28.03.2015 / Accepted: 05.06.2015 Published Online: 27.07.2016 Original Investigation The Comparison of Hemilaminectomy and Laminoplasty Procedures in the
DOI: 10.5137/1019-5149.JTN.14736-15.1 Received: 28.03.2015 / Accepted: 05.06.2015 Published Online: 27.07.2016 Original Investigation The Comparison of Hemilaminectomy and Laminoplasty Procedures in the
Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty
 Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Morphological Patterns of the Anterior Median Fissure in the Cervical Spinal Cord Evaluated by Computed Tomography After Myelography
 Neurospine 2018;15(4):388-393. https://doi.org/10.14245/ns.1836112.056 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yuki Oichi https://orcid.org/0000-0002-0225-8158
Neurospine 2018;15(4):388-393. https://doi.org/10.14245/ns.1836112.056 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yuki Oichi https://orcid.org/0000-0002-0225-8158
