Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
|
|
|
- Anissa Casey
- 5 years ago
- Views:
Transcription
1 DOI: / JTN Received: / Accepted: Published Online: Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior Longitudinal Ligament of the Cervical Spine in Patients without Myelopathy: Results of a 1-year Pilot Study Byung-Wan CHOI Inje University, Haeundae Paik Hospital, Department of Orthopedic Surgery, Busan, Korea ABSTRACT AIm: We analyzed the demographics, clinical and radiological characteristics of non-myelopathic cervical ossification of the posterior longitudinal ligament (OPLL) patients. MaterIal and Methods: This study included 115 patients with cervical OPLL but without myelopathy. Demographic features of age, sex, and the nature of the patient s symptoms were evaluated. Clinically, visual analog scale (VAS) scores for the neck and arm, and Japanese Orthopaedic Association (JOA) scores were evaluated. Radiologically, the number of involved segments, type of OPLL, and the maximal compression ratio were analyzed using a computed tomography (CT) scan. The relationship between clinical scores and radiological parameters was analyzed. Results: At the time of diagnosis, there was absence of symptoms in 23, axial neck pain in 44, radiculopathy in 40, and tingling sensation of fingers in 8. VAS score for the neck was 4.42 and that for the arm was The mean JOA score was Radiologically, the mean number of involved segments was The type of OPLL mass was continuous, mixed, segmental, and local in 10, 43, 42, and 20 cases, respectively. The maximal compression ratio was There was a significant relationship between the maximal compression ratio and the number of involved segments (p<0.001). No relationship was found between clinical symptoms, clinical scores, and radiological findings. ConclusIon: Some non-myelopathic cervical OPLL patients showed no symptoms, some presented axial neck pain and radiculopathy. Radiologically, a significant relationship between the maximal compression ratio and the number of involved segments was found. However, there was no relationship between clinical symptoms and radiological findings in neurologically intact patients. Keywords: Cervical spine, OPLL, Asymptomatic, Non-myelopathic INTRODUCTION Ossification of the posterior longitudinal ligament (OPLL) involves the abnormal calcification of the posterior longitudinal ligament that mostly occurs at the cervical spine. OPLL-induced spinal compression may lead to neurologic symptoms and surgery is required in cases with severe neurologic deficit. Although the literature is rich regarding various surgical treatments and outcomes, there are few studies reporting data regarding conservative management of these patients (3,9,13). While early diagnosis and careful observation of OPLL patients is important, the nature of the symptoms and that of asymptomatic OPLL have been unclear. Also, patients with OPLL may be asymptomatic or may have simple neck pain, radiculopathy, or myelopathy, regardless of radiological findings. Previous reports that examined the natural course of OPLL included a simple analysis of the development of new neurological symptoms during follow-up. Furthermore, most of the studies evaluated Corresponding author: Byung Wan CHOI alla1013@naver.com 414 Turk Neurosurg 27(3): , 2017
2 only operated cases. To our knowledge, no study has reported on the analysis of OPLL patients without myelopathy. The purpose of this study was to analyze the demographic, clinical, and radiological characteristics of cervical OPLL in patients without myelopathy and to serve as a basic reference for evaluating the treatment strategy. Moreover, the effect of OPLL on their symptoms was examined especially in patients without myelopathy. MATERIAL and METHODS Between March 2010 and December 2012, a total of 115 consecutive patients who were diagnosed with cervical OPLL and had no neurological deterioration at the initial period were examined retrospectively. Institutional Review Board approval was obtained for this study. Neurological deterioration was defined as decreased motor power or sensory tone related to the cervical compression level. Among patients who suspicious of myelopathy, those with a grip and release test result of greater than 20/10 seconds, negative results in the Hoffman test, and those with no objective gait deterioration were considered neurologically unaffected and were included in this study. Patients, who initially showed neurological symptoms were followed up for less than 1 year, and/or lacked radiological evaluation with computed tomography (CT) were excluded from this study. Conservative management was provided to patients with axial neck pain or radiculopathy, but who did not have neurological impairment. Surgery was performed in patients with myelopathy, radiculopathy with neurological deterioration, or sustained radicular pain despite aggressive medical treatment for more than 6 weeks. Three hundred sixty-five patients were diagnosed with OPLL, and 151 underwent operative treatment (Figure 1). Among the 214 patients who received conservative management, 53 were excluded because they lacked radiological evaluation or had been followed up for less than 1 year. Another 46 patients were excluded because of neurological deterioration at initial visit. In all patients, medical records, questionnaires, and CT scans were evaluated. The demographic analysis included the nature of the patient s symptoms, concomitant medical disease, familial history of OPLL, and the progression or development of symptoms. The nature of patients symptoms was categorized as 1) absence of any symptom, 2) axial neck pain, 3) pain radiating to the upper extremity, 4) tingling sensation of the fingers, 5) difficulty in gait or clumsiness of the hand, and 6) others. Clinically, the visual analog scale (VAS) scores of the neck and arm, and Japanese Orthopaedic Association (JOA) scores were evaluated. Radiological analysis, including the number of involved segments, type of OPLL, and maximal compression ratio using a CT scan, was performed. The maximal compression ratio (the ratio of the length occupied by the OPLL to the normal spinal canal length) was determined by measuring the space available for the spinal cord (SAC) and the length of the unaffected spinal canal on sagittal view on the CT scan in the maximal compression area (Figure 2). The relationship between the clinical scores and radiological parameters was analyzed. CT data for all participants was analyzed by 2 orthopedic spine surgeons based on the number of involved segments, types of ossification, and maximal compression ratio in the sagittal view (10). The CT images (Discovery CT 750 HD, GE, USA) were 1-mm thick in the disk spaces and 2-mm thick in the vertebral body and sagittal planes. The patients who showed spondylotic or cord compression lesion in other parts outside OPLL were excluded from this analysis. The OPLL types were categorized as local, segmental, continuous, and mixed, based on the classification determined by the Figure 1: Flow diagram showing patient allocation. Figure 2: Maximal compression ratio. a) Sagittal SAC, b) Sagittal canal length, (b-a)/b: maximal compression ratio. Turk Neurosurg 27(3): ,
3 Investigation Committee on OPLL of the Japanese Ministry of Public Health and Welfare (12). The local type of OPLL is observed at the posterior rim of the intervertebral disc; the segmental type is observed at the posterior rim of each vertebral body; the continuous type is observed continuously over many segments; and the mixed type is a combination of the above types. All CT measurements were performed by the picture archiving and communication system (PACS) (m-view TM, MaroTech, Seoul, Korea) system. Two blinded observers independently interpreted each of the radiological findings, and the average measurements were used in the analysis. When there was a difference in the interpretation, the 2 observers drew a mutual conclusion, which was used for analysis. To verify the reliability of measured values, intra- and inter-observer consistencies were checked using the kappa coefficient test. SPSS 18.0 (SPSS Inc., Chicago, IL, USA) was used for statistical analysis and to determine the relationship between radiological parameters. The relationship between the patient s symptoms, clinical scores, and radiological findings was also analyzed using correlation analysis or chi-square analysis. The results were deemed statistically significant at p < RESULTS Clinical Features The mean age of the 115 recruited patients was 57.3 ± 9.16 (range, 32 86) years, and 56 men and 59 women were included. The mean follow-up period was 15.2 ± 7.9 (range, 13 37) months. At the time of diagnosis, there were no symptoms in 23 patients, axial neck pain in 44, radiculopathy in 40, and tingling sensation of the fingers in eight. Six patients complained of difficulty in gait or clumsiness of the hand without objective neurological abnormality. Two patient underwent operative treatment during the follow up. One was due to aggravation of radicular pain and the other due to the development of objective gait disturbance. Fifty-nine patients had no concomitant medical disease, and 29, 14, and six patients had hypertension, diabetes mellitus, and thyroid disease, respectively. There were only two patients with a family history of OPLL (Table I). The mean neck and arm VAS scores were 4.42 (range, 0 10) and 3.64 (range, 0 10), respectively. The mean JOA score was A significant relationship was found between the neck and arm VAS scores (p < 0.01); the arm VAS scores also showed a significant relationship with JOA scores (p = 0.002) (Table II). Radiological Features Inter-(K1) and intra-(k2) observer consistencies of radiologically measured values indicated high levels of reliability (K1 = 0.81, K2 = 0.84). The mean number of involved segments of OPLL was The type of OPLL mass was continuous, mixed, segmental, and local in 10, 43, 42, and 20 cases, respectively (Figure 3A- D). The mean maximal compression ratio was There was a significant relationship between the maximal compression ratio and the number of involved segments (r = 0.471, p < 0.001). The continuous and mixed type showed many more involved segments (p < 0.001), and the maximal compression ratio was high (p < 0.001) (Table III). Relationship Between Clinical and Radiological Features There was no significant relationship between clinical symptoms and the number of involved segments (p = 0.83), type of OPLL (p = 0.88), and the maximal compression ratio (p = 0.167). Neck VAS, arm VAS, and JOA scores were not related to radiological parameters. DISCUSSION The investigation Committee on Ossification of the Spinal Ligaments of the Japanese Ministry of Public Health, Labour, and Welfare performed the first national survey of OPLL in Table I: Summary of Demographic Data of the Patients Factor Number of Cases (%) Sex Male 56 (48.69) Female 59 (51.3) Symptoms at time of diagnosis No symptoms 23 (20.1) Axial neck pain 44 (38.26) Radiculopathy 40 (34.78) Tingling sensation of fingers 8 (6.95) Concomitant medical disease No 59 (51.30) Hypertension 29 (25.21) Diabetes Mellitus 14 (12.17) Thyroid disease 6 (5.21) Table II: Relationship between Clinical Scores Neck VAS Correlation ratio p value Arm VAS Correlation ratio p value Neck VAS* Arm VAS JOA** <0.01 JOA 1 *: visual analog scale. **: Japanese Orthopaedic Association score Turk Neurosurg 27(3): , 2017
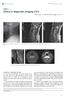
4 1975, and 2142 OPLL patients were registered. Ninety-five percent of the patients had clinical symptoms, but 5% of these patients were asymptomatic. As many as 16.8% of the patients needed assistance in their activities of daily living; Table III: Relationship Between Type of OPLL and Radiological Features No. of involved segment Maximal compression ratio Continuous type Mixed type Segmental type Local type p value <0.001 < % of patients showed a rapid aggravation of symptoms, and 11.4% of patients showed chronic aggravation. These data were meaningful. However, most of the patients had clinical symptoms at the time of diagnosis, and there were some limitations in the evaluation of the natural course of OPLL. In our study, 168 of the 365 cervical OPLL patients (46%) were neurologically intact. Even though there is some possibility of selection bias, we can evaluate a large number of asymptomatic OPLL cases. OPLL is formed mainly through enchondral ossification, and part of it develops through membranous ossification. McAfee et al. reported that the pathology of most OPLL cases is composed of a lamellar bone with mature Haversian canals, in addition to fibrous cartilages and woven bones wrapped with calcified cartilage (6). Ossification begins at the connection area of lateral limbus of vertebral body and posterior longitudinal ligament, and progresses up and down. OPLL progresses slowly, and shows a wide variety of neuronal A C B D Figure 3: A 42-year-old man complained of neck pain with no myelopathic symptoms. Magnetic resonance imaging and computed tomography scan showing ossification of the posterior longitudinal ligament mixed type in C2 6, resulting in spinal canal stenosis. The Japanese Orthopaedic Association (JOA) score, neck visual analog scale (VAS) score, and arm VAS score were 17, 5, and 3, respectively. A, B) Sagittal and axial view in MRI. C, D) Sagittal and axial view in CT. Turk Neurosurg 27(3): ,
5 degeneration by compressing the spinal cord and nerve roots. Jeon et al. assume that segmental OPLL progresses to mixed OPLL or continuous OPLL and that mixed OPLL progresses to continuous OPLL (2). When they evaluated the age of each type of OPLL, localized and segmental OPLL types were more often identified in younger patients, whereas mixed and continuous types of OPLL were more often identified in older patients. Our result also showed a significant relationship between the maximal compression ratio and the number of involved segments. The continuous and mixed types showed much more involved segments, and the maximal compression ratio was high. In the cases of mixed or continuous type, OPLL has progressed and can involve multiple levels simultaneously due to the growth of the OPLL mass. Matsunaga et al. reported that only 17% of the patients without myelopathy at the first visit developed myelopathy during the follow-up (5). Pham et al. (9) also showed that patients without myelopathy had a 16.7% chance of progressive myelopathy over an aggregate mean follow-up of 14.6 years. However, there was no report about the clinical pattern or radiological features of asymptomatic OPLL patients. Our study showed that 197 patients of the 365 patients who were diagnosed with cervical OPLL required surgery because of neurological deterioration, and 46% of the OPLL patients did not need surgical intervention. Neurologically unaffected patients did not have any symptom (20%), or had neck pain (38%), or radicular pain (34%). Sasaki et al. reported that 86.7% of the OPLL patients had symptoms, while 77% of the non-opll patients had symptoms (11). Their result showed many OPLL patients did not have severe symptoms compared with that in the non-opll group. We can draw two important conclusions from these results. While most of the subjects with OPLL had pain between the neck and arm, a number of patients with OPLL did not receive treatment (11). Another point is that OPLL patients do not show severe symptoms but rather radiological findings, and surgical intervention should be considered according to the patients symptoms, especially myelopathy. Our result showed no significant relationship between clinical symptoms and radiological findings in neurologically intact cervical OPLL patients. The mean JOA score was Conservative treatment is required for patients with a JOA score of at least 14 points (7). Morio et al. reported a mean JOA score of 12.9 and 16.1 in patients with and without myelopathy, respectively (8). Based on the review of four studies by Pham et al., the mean aggregate JOA score of 111 OPLL patients was 15.3 on presentation; these patients were subsequently managed with conservative treatment (9). In order to establish radiological predictors for the development of myelopathy in patients with OPLL, Matsunaga et al. performed a multicenter cohort study analyzing 156 patients with a mean follow-up of 10.3 years (4). They found that 60% or greater spinal canal stenosis; large ROM of the cervical spine and laterally deviated-type OPLL were risk factors for developing myelopathy. The maximal compression was less than 40% in asymptomatic OPLL cases in our study. Chang et al. evaluated the factors related to the manifestation of my- elopathic symptoms in patients with OPLL (1). In patients with OPLL of the cervical spine, the manifestation of myelopathic symptoms was not related to the range of motion of the cervical spine or the number of involved segments. However, age at the time of diagnosis and the maximum compression of the spinal canal were related factors. However, there is controversy surrounding the management of asymptomatic patients. In a survey of 774 spine surgeons, the majority deemed the presence of clinically symptomatic radiculopathy to predict progression to myelopathy in nonmyelopathic patients with cervical stenosis (14). This was a pilot study to evaluate the clinical and radiological features of asymptomatic OPLL patients. Our study is limited in that it included a short-term follow-up period, and the data obtained were not sufficient to determine the clinical application for predicting the clinical course of asymptomatic OPLL patients. Our center has renown for OPLL and many patients were consulted from other institutions. That is the reason we can collect many asymptomatic OPLL patients. This can be another limitation as selection bias. However, we evaluated a relatively large number of asymptomatic OPLL patients. With serial follow up and further evaluation, these data can be beneficial to understand the natural history of OPLL. CONCLUSION The demographic characteristics, clinical presentation, and radiography findings of OPLL in neurologically intact cervical OPLL patients were analyzed, which could serve as a basis for further study on and treatment of OPLL. Some neurologically intact cervical OPLL patients showed no symptoms; however, some presented with axial neck pain and radiculopathy. Most patients had no family history of OPLL. Radiologically, a significant relationship between the maximal compression ratio and the number of involved segments was found. However, there was no relationship between clinical symptoms and radiological findings in neurologically intact patients. ACKNOWLEDGMENT This study was conducted in accordance with the declaration of Helsinki. This study was conducted with approval from the ethics committee of Inje University Haeundae Paik Hospital ( ). REFERENCES 1. Chang H, Song KJ, Kim HY, Choi BW: Factors related to the development of myelopathy in patients with cervical ossification of the posterior longitudinal ligament. J Bone Joint Surg Br 94: , Jeon TS, Chang H, Choi BW: Analysis of demographics, clinical, and radiographical findings of ossification of posterior longitudinal ligament of the cervical spine in 146 Korean patients. Spine (Phila Pa 1976) 37(24):E , Turk Neurosurg 27(3): , 2017
6 3. Matsumoto M, Chiba K, Toyama Y, Takeshita K, Seichi A, Nakamura K, Arimizu J, Fujibayashi S, Hirabayashi S, Hirano T, Iwasaki M, Kaneoka K, Kawaguchi Y, Ijiri K, Maeda T, Matsuyama Y, Mikami Y, Murakami H, Nagashima H, Nagata K, Nakahara S, Nohara Y, Oka S, Sakamoto K, Saruhashi Y, Sasao Y, Shimizu K, Taguchi T, Takahashi M, Tanaka Y, Tani T, Tokuhashi Y, Uchida K, Yamamoto K, Yamazaki M, Yokoyama T, Yoshida M, Nishiwaki Y: Surgical results and related factors for ossification of posterior longitudinal ligament of the thoracic spine: A multi-institutional retrospective study. Spine 33(9): , Matsunaga S, Nakamura K, Seichi A, Yokoyama T, Toh S, Ichimura S, Satomi K, Endo K, Yamamoto K, Kato Y, Ito T, Tokuhashi Y, Uchida K, Baba H, Kawahara N, Tomita K, Matsuyama Y, Ishiguro N, Iwasaki M, Yoshikawa H, Yonenobu K, Kawakami M, Yoshida M, Inoue S, Tani T, Kaneko K, Taguchi T, Imakiire T, Komiya S: Radiographic predictors for the development of myelopathy in patients with ossification of the posterior longitudinal ligament: A multicenter cohort study. Spine (Phila Pa 1976) 33(24): , Matsunaga S, Sakou T, Taketomi E, Komiya S: Clinical course of patients with ossification of the posterior longitudinal ligament: A minimum 10-year cohort study. J Neurosurg 100(3 Suppl Spine): , McAfee PC, Regan JJ, Bohlman HH: Cervical cord compression from ossification of the posterior longitudinal ligament in non-orientals. J Bone Joint Surg Br 69(4): , Mochizuki M, Aiba A, Hashimoto M, Fujiyoshi T, Yamazaki M: Cervical myelopathy in patients with ossification of the posterior longitudinal ligament. J Neurosurg Spine 10(2): , Morio Y, Nagashima H, Teshima R, Nawata K: Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossification of the posterior longitudinal ligament. Spinal Cord 37(12): , Pham MH, Attenello FJ, Lucas J, He S, Stapleton CJ, Hsieh PC: Conservative management of ossification of the posterior longitudinal ligament. Neurosurg Focus 30(3): E2, Sakai K, Okawa A, Takahashi M, Arai Y, Kawabata S, Enomoto M, Kato T, Hirai T, Shinomiya K: Five year followup evaluation of surgical treatment for cervical myelopathy caused by ossification of the posterior longitudinal ligament: A prospective comparative study of anterior decompression and fusion with floating method versus laminoplasty. Spine 37(5): , Sasaki E, Ono A, Yokoyama T, Wada K, Tanaka T, Kumagai G, Iwasaki H, Takahashi I, Umeda T, Nakaji S, Ishibashi Y: Prevalence and symptom of ossification of posterior longitudinal ligaments in the Japanese general population. J Orthop Sci 19(3): , Tsuyama N: Ossification of the posterior longitudinal ligament of the spine. Clin Orthop Relat Res 184:71-84, Wang MY, Shah S, Green BA: Clinical outcomes following cervical laminoplasty for 204 patients with cervical spondylotic myelopathy. Surg Neurol 62: , Wilson JR, Barry S, Fischer DJ, Skelly AC, Arnold PM, Riew KD, Shaffrey CI, Traynelis VC, Fehlings MG: Frequency, timing, and predictors of neurological dysfunction in the nonmyelopathic patient with cervical spinal cord compression, canal stenosis, and/or ossification of the posterior longitudinal ligament. Spine 38:S37-54, 2013 Turk Neurosurg 27(3): ,
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Narrative Review Cervical Ossified Posterior Longitudinal Ligament
 Narrative Review Cervical Ossified Posterior Longitudinal Ligament Introduction Cervical ossified posterior longitudinal ligament is a common cause of myelopathy. It is frequently encountered in busy spine
Narrative Review Cervical Ossified Posterior Longitudinal Ligament Introduction Cervical ossified posterior longitudinal ligament is a common cause of myelopathy. It is frequently encountered in busy spine
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Ossification of the posterior longitudinal ligament. Conservative management of ossification of the posterior longitudinal ligament.
 Neurosurg Focus 30 (3):E2, 2011 Conservative management of ossification of the posterior longitudinal ligament A review Martin H. Pham, M.D., 1 Frank J. Attenello, M.D., 1 Joshua Lucas, B.S., 1 Shuhan
Neurosurg Focus 30 (3):E2, 2011 Conservative management of ossification of the posterior longitudinal ligament A review Martin H. Pham, M.D., 1 Frank J. Attenello, M.D., 1 Joshua Lucas, B.S., 1 Shuhan
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Cervical spondylotic myelopathy (CSM) is a
 WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
흉추척수증을유발한황색인대골화증의골절 - 증례보고 -
 대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability
 J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma?
 Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years)
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament
 Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Surgical outcomes for lumbar spinal canal stenosis with coexisting cervical stenosis (tandem spinal stenosis): a retrospective analysis of 565 cases
 Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
ASJ. Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy. Asian Spine Journal.
 Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Kazunari Takeuchi Æ Toru Yokoyama Æ Atsushi Ono Æ Takuya Numasawa Æ Kanichiro Wada Æ Taito Itabashi Æ Satoshi Toh
 Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Risk factors for development of cervical spondylotic myelopathy: results of a systematic review
 Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty
 Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Spinal Cord (2005) 43, & 2005 International Spinal Cord Society All rights reserved /05 $
 (2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
(2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
We have reviewed the cervical spine radiographs
 THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for severity scores
 J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 13:319 323, 2010 Using the T2-weighted magnetic resonance imaging signal intensity ratio and clinical manifestations to assess the prognosis of patients with cervical ossification of
J Neurosurg Spine 13:319 323, 2010 Using the T2-weighted magnetic resonance imaging signal intensity ratio and clinical manifestations to assess the prognosis of patients with cervical ossification of
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
Orthopaedics and Rehabilitation Medicine Fuculty of Medical Sciences University of Fukui
 Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
The Incidence Of An Epidural Hematoma Following Cervical Spine Surgery
 The Incidence Of An Epidural Hematoma Following Cervical Spine Surgery Gregory D. Schroeder, MD, Alan S. Hilibrand MD, Paul Arnold, MD, David Fish, MD, Jeffrey C. Wang, MD, Jeffrey L. Gum, MD, Zachary
The Incidence Of An Epidural Hematoma Following Cervical Spine Surgery Gregory D. Schroeder, MD, Alan S. Hilibrand MD, Paul Arnold, MD, David Fish, MD, Jeffrey C. Wang, MD, Jeffrey L. Gum, MD, Zachary
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures
 Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
INTRODUCTION.
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.5.442 J Korean Neurosurg Soc 58 (5) : 442-447, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.5.442 J Korean Neurosurg Soc 58 (5) : 442-447, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Range of motion of thoracic spine in sagittal plane
 DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing multilevel versus single-level surgery
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy. Spine January 1, 2009; Volume 34; Issue 1; pp 82-86
 Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment
 Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates for Cervical Myelopathy
 Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study
 CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
Morphological changes of the cervical spinal canal and cord due to aging on MR imaging
 Morphological changes of the cervical spinal canal and cord due to aging on MR imaging Shigeru Kobayashi, MD,PhD 1, Katsuhiko Hayakawa, MD, PhD 2, Takashi Nakane, MD, PhD 2, Riya Kosaka MD,PhD 3. 1 Department
Morphological changes of the cervical spinal canal and cord due to aging on MR imaging Shigeru Kobayashi, MD,PhD 1, Katsuhiko Hayakawa, MD, PhD 2, Takashi Nakane, MD, PhD 2, Riya Kosaka MD,PhD 3. 1 Department
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Clinical Article. Key Words : Ossification Posterior longitudinal ligament Volume 3D analysis MIMICS.
 Clinical Article J Korean Neurosurg Soc 60 (4) : 441-447, 2017 https://doi.org/10.3340/jkns.2015.0708.014 pissn 2005-3711 eissn 1598-7876 Inter- and Intra-Observer Variability of the Volume of Cervical
Clinical Article J Korean Neurosurg Soc 60 (4) : 441-447, 2017 https://doi.org/10.3340/jkns.2015.0708.014 pissn 2005-3711 eissn 1598-7876 Inter- and Intra-Observer Variability of the Volume of Cervical
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis
 Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Diagnosis of Neck & Upper Extremity Pain
 Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Abstract Study Design Prospective clinical study.
 812 Technical Report GLOBAL SPINE JOURNAL THIEME Resection of Beak-Type Thoracic Ossification of the Posterior Longitudinal Ligament from a Posterior Approach under Intraoperative Neurophysiological Monitoring
812 Technical Report GLOBAL SPINE JOURNAL THIEME Resection of Beak-Type Thoracic Ossification of the Posterior Longitudinal Ligament from a Posterior Approach under Intraoperative Neurophysiological Monitoring
Analysis of C5 palsy in cervical myelopathy with massive anterior compression following laminoplasty
 Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): Part 2. Endorsement of the alternative item
 J Orthop Sci (2007) 12:241 248 DOI 10.1007/s00776-007-1119-0 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): Part 2. Endorsement of the alternative
J Orthop Sci (2007) 12:241 248 DOI 10.1007/s00776-007-1119-0 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): Part 2. Endorsement of the alternative
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
Neurological manifestations of thoracic myelopathy in 203 patients
 Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
The Prevalence of Cervical Foraminal Stenosis on Computed Tomography of a Selected Community-Based Korean Population
 Original Article Clinics in Orthopedic Surgery 2018;10:433-438 https://doi.org/10.4055/cios.2018.10.4.433 The Prevalence of Cervical Foraminal Stenosis on Computed Tomography of a Selected Community-Based
Original Article Clinics in Orthopedic Surgery 2018;10:433-438 https://doi.org/10.4055/cios.2018.10.4.433 The Prevalence of Cervical Foraminal Stenosis on Computed Tomography of a Selected Community-Based
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty
 Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels
 National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
National Imaging Associates, Inc. CERVICAL SPINE SURGERY: Original Date: July 2008 Cervical ACDF - Anterior Decompression with Fusion Single or Multiple Levels Page 1 of 13 Cervical Posterior Decompression
Appendix: Diagnostic Criteria for OPLL and Diagnosis and Treatment Algorithm
 Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
CSM is the most common cause of spinal cord dysfunction
 Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
CERVICAL SPONDYLOTIC myelopathy is one of the
 ORIGINAL ARTICLE Gait Analysis for Evaluating the Relationship Between Increased Signal Intensity on T2-Weighted Magnetic Resonance Imaging and Gait Function in Cervical Spondylotic Myelopathy Chung Reen
ORIGINAL ARTICLE Gait Analysis for Evaluating the Relationship Between Increased Signal Intensity on T2-Weighted Magnetic Resonance Imaging and Gait Function in Cervical Spondylotic Myelopathy Chung Reen
Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients
 Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Comparative Effectiveness of Different Types of Cervical Laminoplasty
 Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Adjacent segment disease after anterior cervical discectomy and fusion
 Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
