Rossini et al. Acta Neuropathologica Communications 2014, 2:45
|
|
|
- Mitchell Wright
- 6 years ago
- Views:
Transcription
1 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 RESEARCH Open Access Layer-specific gene expression in epileptogenic type II focal cortical dysplasia: normal-looking neurons reveal the presence of a hidden laminar organization Laura Rossini 1, Valentina Medici 1, Laura Tassi 2, Francesco Cardinale 2, Giovanni Tringali 3, Manuela Bramerio 4, Flavio Villani 1, Roberto Spreafico 1 and Rita Garbelli 1* Abstract Background: Type II focal cortical dysplasias (FCDs) are malformations of cortical development characterised by the disorganisation of the normal neocortical structure and the presence of dysmorphic neurons (DNs) and balloon cells (BCs). The pathogenesis of FCDs has not yet been clearly established, although a number of histopathological patterns and molecular findings suggest that they may be due to abnormal neuronal and glial proliferation and migration processes. In order to gain further insights into cortical layering disruption and investigate the origin of DNs and BCs, we used in situ RNA hybridisation of human surgical specimens with a neuropathologically definite diagnosis of Type IIa/b FCD and a panel of layer-specific genes (LSGs) whose expression covers all cortical layers. We also used anti-phospho-s6 ribosomal protein antibody to investigate mtor pathway hyperactivation. Results: LSGs were expressed in both normal and abnormal cells (BCs and DNs) but their distribution was different. Normal-looking neurons, which were visibly reduced in the core of the lesion, were apparently located in the appropriate cortical laminae thus indicating a partial laminar organisation. On the contrary, DNs and BCs, labelled with anti-phospho-s6 ribosomal protein antibody, were spread throughout the cortex without any apparent rule and showed a highly variable LSG expression pattern. Moreover, LSGs did not reveal any differences between Type IIa and IIb FCD. Conclusion: These findings suggest the existence of hidden cortical lamination involving normal-looking neurons, which retain their ability to migrate correctly in the cortex, unlike DNs which, in addition to their morphological abnormalities and mtor hyperactivation, show an altered migratory pattern. Taken together these data suggest that an external or environmental hit affecting selected precursor cells during the very early stages of cortical development may disrupt normal cortical development. Keywords: Layer-specific genes, Focal cortical dysplasia, Epilepsy, Neuronal migration, Dysmorphic neurons * Correspondence: garbelli.r@istituto-besta.it 1 Clinical Epileptology and Experimental Neurophysiology Unit, Istituto Neurologico C. Besta, Via Amadeo 42, Milano, Italy Full list of author information is available at the end of the article 2014 Rossini et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 2 of 15 Introduction Focal cortical dysplasias (FCDs) are malformations of cortical development that are frequently associated with intractable epilepsy and are characterised by cortical dyslamination and abnormal cell morphology [1]. The most recent classification [2] recognises three types of FCD, with Type II being divided into two subtypes on the basis of the presence of dysmorphic neurons (DNs) alone (type IIa) or DNs together with balloon cells (BCs; Type IIb). In both cases, cortical architecture is profoundly altered particularly within the core of the lesion, where DNs and normal-sized pyramidal cells co-exist with an overall reduction in neuronal density [3,4]. In addition to morphological changes (cytomegaly, abnormal dendritic arbors, and the loss of radial orientation), DNs are characterised by the aberrant expression of neuronal and glial markers with a prevalently neuronal-mature identity. BCs are also characterised by morphological anomalies such as voluminous cytoplasms, displaced nuclei and the co-expression of different mature/immature neuronal/glial markers with a prevalently glial-immature phenotype [5-7]. The lack of a clear cell-type specification may reflect alterations in normal neuronal and glial proliferation [2,8] and subsequent migration. The cytological similarities between Type II FCD and tuberous sclerosis complex (TSC), a genetic disorder due to mutations in the TSC1 or TSC2 gene, and evidence of abnormal activation of the mammalian target of rapamycin (mtor) signalling cascade, have led to the hypothesis that this pathway is involved in the pathogenesis of DNs and BCs [7,9,10], the origin of which is still debated. It has been suggested that they may arise from radial glial progenitor cells in the Ventricular Zone (VZ) [11], but it is still unclear whether they derived from a single or multiple progenitor cell, or whether they arise at a particular moment or at different times during the proliferation phase [12]. One means of gaining further insights into the structural abnormalities of dysplastic cortex and clarifying the cellular origin of DNs and BCs is to evaluate the expression patterns of an appropriate panel of layerspecific genes (LSGs). Despite their specific functions such as transcription factors, calcium-binding proteins, receptors, etc.), these genes have the distinctive characteristic of being expressed in (mainly glutamatergic) cortical neurons with very high laminar specificity, and can thus be used as markers to identify different cortical layers. This not only allows specific neuronal subpopulations to be identified on the basis of their expression profiles, but also provides information concerning their birth dates and migration [13,14]. Over the last few years, a number of studies have used LSGs to investigate cortical development under normal and pathological conditions in animal models [15-18] and humans [19-25]. The aim of this study was to investigate the expression of a panel of LSGs covering all cortical layers (Cux2, Rorβ, Er81, Nurr1 and CTGF) in surgical specimens from a cohort of 20 patients with a neuropathological diagnosis of Type IIa/b FCD in order to learn more about cortical layering disruption and the origin of DNs and BCs. Methods Patient and specimen selection We collected specimens from 20 patients who underwent surgery to treat intractable epilepsy at the C. Munari Epilepsy Surgery Centre of Niguarda Hospital and the Department of Neurosurgery of Besta Neurological Institute (both in Milan, Italy). The protocols of the pre-surgical investigation procedures were the same at both centres, and included high-resolution magnetic resonance imaging (MRI) and video-electroencephalography (VEEG) monitoring in order to define the epileptogenic zone and surgical strategy. The following individual MRI aspects were considered: focal thickening of the cortex, blurring of the grey/white matter junction, abnormal signal intensity in the cortex and subcortical white matter, tapering of white matter signal changes towards the ventricle (trasmantle sign). The C. Munari Centre also used invasive presurgical procedures (i.e. stereo-eeg) after appropriate discussions when the imaging and non-invasive electroclinical data were discordant. All of the resections were performed for strictly therapeutic reasons after informed consent had been obtained. The pre-surgical procedures for selecting candidates for epilepsy surgery have been described in detail elsewhere [26]. All of the patients had a neuropathological diagnosis of Type II FCD. The cortical specimens were divided into two groups: Type IIa (8 cases) and Type IIb (12 cases). Table 1 summarises the patients main clinical features. Immunohistochemical procedures After surgical resection, the specimens were fixed in 4% paraformaldehyde for hours, and alternate 5 mm thick slabs were embedded in paraffin for routine neuropathology or cut into 50 μm thick serial sections by means of a vibratome (VT1000S, Leica, Heidelberg, Germany) and addressed for the present study. For the routine neuropathological investigations, 7 μm thick sections were stained with hematoxylin and eosin, thionin, Kluver-Barrera and Bielschowsky stains, and additional series were processed for immunohistochemistry (IHC). The vibratome sections were also stained with thionin and processed for IHC. The following primary antibodies were used: monoclonal antibodies against
3 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 3 of 15 Table 1 Clinical and neuropathological findings ID Age at seizure onset (years) Age at surgery (years) Monthly seizure frequency Side/site of surgery Neuro-pathological diagnosis Outcome (Engel class) L/TO FCD IIa Ia L/T FCD IIa IV L/O FCD IIa Ia L/O FCD IIa Ia R/F FCD IIa Ia R/FCP FCD IIa Ia L/T FCD IIa Ia L/TO FCD IIa Ic R/TPO FCD IIb Ia R/T FCD IIb Ia L/P FCD IIb Ia R/F FCD IIb Id L/F FCD IIb IIb L/T FCD IIb Ia R/F FCD IIb III R/F FCD IIb II L/T FCD IIb Ia R/F FCD IIb Ia R/T FCD IIb Ia L/P FCD IIb Ib Abbreviations: FCD focal cortical dysplasia, F frontal, ID patient identification number, L left, O occipital, P parietal, R right, T temporal. neuronal nuclear protein (NeuN, 1:3000, Chemicon, Temecula, CA, USA), pan-neuronal specific for nonphosphorylated neurofilaments (SMI311R, 1:1000, Covance, San Diego, CA, USA) and microtubule associated protein- 2a and b (MAP2, 1:200, Neomarkers, Freemont, CA, USA) as neuronal markers; monoclonal antibody against glial fibrillary acidic protein (GFAP, 1:15000, Chemicon) as a glial marker; monoclonal antibody against intermediate filament protein vimentin (VIM, 1:3000, Dako, Carpinteria, CA, USA) as a marker of BCs; and rabbit monoclonal antibody against phospho-s6 ribosomal protein (ps6 Ser235/ 236, 1:500, Cell Signaling Technology, Beverly, MA, USA) as a marker indicative of mtor pathway hyperactivation. The IHC procedures have been described in detail elsewhere [27]. In situ hybridisation In all cases, vibratome sections adjacent to the IHC sections were processed for in situ hybridisation (ISH) experiments designed to detect Cux2, Rorβ, Er81, Nurr1 and CTGF mrna expression. Free-floating sections were incubated with digoxigenin(dig)-labelled riboprobes that specifically hybridise with each of the five mrna of interest, and then with an alkaline phosphatase-conjugated anti-dig antibody (1:1000, Roche Diagnostics Mannheim, Germany). The procedure and riboprobe characteristics have been described in detail elsewhere [16,20,22,28]. There were no apparent signals in control sections with the sense probes. Quantitative analysis of ISH signals To estimate the reduction of normal-looking neurons, we counted the number of positive cells for the different LSG in a single section for each sample using Image Pro Plus 7.0 software (Media Cybernetics, Bethesta, MD, USA). For each LSG, we outlined at 10 objective two equal regions of interest (lesional area and, when present, adjacent perilesional area) including the specific layer. Using a 20 objective, all the immunopositive normallooking neurons within this area were manually counted. The considered areas were: 1.44 mm 2 for Cux2, 1.35mm 2 for Rorβ, 1.5mm 2 for Er81 and 1.1 mm 2 for Nurr1. Differences between lesional and perilesional areas were assessed by means of a t test, with p-values of <0.05 being considered significant. Double fluorescence ISH/IHC It was not always possible to make a clear morphological distinction between LSG-positive DNs and BCs when BCs and giant round-shaped neurons coexisted in the same areas. In these cases, we used double fluorescence ISH/ICC combining Rorβ, Er81 and Nurr1 riboprobes
4 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 4 of 15 with anti-smi, anti-map2 (to identify DNs) and antivimentin antibodies (to identify BCs); the Cux2 riboprobe was not used because of its low fluorescent hybridisation signal. After the ISH procedures, the sections were incubated overnight with a mixture of rabbit anti-dig antibody (1:100000, Sigma, St. Louis, MO, USA) and mouse anti-smi (1:300) or anti-map2 (1:300) or anti-vim antibodies (1:300), and then incubated with biotinylated goat anti-rabbit antibody (1:200, Vector, Burlingame, CA, USA) and indocarbocyanine (Cy) 3-conjugated goat anti-mouse antibody (1:500, Jackson Immunoresearch Laboratories, West Grove, PA, USA) at room temperature for 60 minutes. Finally, the sections were incubated with streptavidine-hrp (1:1000, PerkinElmer, Boston, MA, USA) at room temperature for 30 minutes, and then with biotinil tyramide fluorescinated in amplification reagent (1:50, PerkinElmer) at room temperature for three minutes. The fluorescent sections were examined using a Nikon D-Eclipse C1 confocal laser scanning microscope (Nikon, Tokyo, Japan) equipped with an argonion laser system and mounted on a light inverted microscope Eclipse TE2000 (Nikon). Er81 and Nurr1 cortical layer thickness in perilesional cortex Sections of five samples of temporal cortex taken from different patients and processed using the Er81 and Nurr1 riboprobes were analysed in order to evaluate possible changes in cortical distribution in the perilesional zone. The thickness of the layers was calculated on the basis of the extent of the neurons labelled by each riboprobe, and was expressed as a percentage of the total depth of the cortical ribbon. Cortical thickness was measured only in the linear portion of the cortex, far from gyri and sulci. One section per case was considered, and three measures of each marker were made using scanned images at 20 magnification (Scanscope; Aperio Technologies, Vista,CA,USA).Thedatawerecomparedwiththose obtained in a previous study in witch six normal temporal cortices were evaluated [22], and the differences were assessed by means of a t test, with p-values of <0.05 being considered significant. Results Clinical aspects Table 1 shows the patients clinical data. Their mean age at epilepsy onset was three years (range 0 10; SD 3) and mean seizure frequency at the time surgery was 95 per month (range 1 600; SD 145). Mean age at the time of surgery was 20 years (range 1 47; SD 15), when the mean duration of epilepsy was 16 years (range 1 43, SD 14). On the basis of the MRI diagnostic criteria recently described by Colombo et al. [29], the imaging investigation allowed a diagnosis of Type II FCD in 19 patients (95%), whereas only temporo-polar blurring was observed in one patient. Trasmantle sign was present in 12 patients. The mean follow-up was five years (range 1 13; SD 3). The surgical outcome was fairly good, with 16 patients in Engel class I (80%; seven with Type IIa FCD and nine with Type IIb); in particular, 13 patients are in Engel class Ia. The remaining four patients are in class II, III, and IV because of the incomplete resection of the lesion. Although the study population was small, the data concerning seizure outcome are in line with previous reports [29,30], thus suggesting that the good results were independent of the subtype and the site and side of the excised lesion. Neuropathological characteristics of FCD The resections of the 20 patients (eight with Type IIa FCD and 12 with Type IIb) involved different cortical areas (see Table 1). The analysed specimen from 16 patients (seven with Type IIa and nine with Type IIb) was characterised by severe disruption of the laminar cortical structure. DNs were distributed throughout the cortical laminae except for layer I, sometime aggregated in neuronal clusters and, in six cases, were also present in the underlying white matter (Figure 1a,d,e). In four patients (one with Type IIa and three with Type IIb), the laminar structure was less severely affected, with fewer DNs mainly clustered in particular cortical layers (Figure 1b,f,g). However, it should be noted that other slabs from these cases used for histopathology rather than LSG detection showed profound disruption of the cortical architecture, suggesting the periphery of the lesion. Both the severely and less severely affected contained normal-looking neurons intermingled with DNs (Figure 1j,k,m,n). BCs (the hallmark of Type IIb FCD identified by means of vimentin immunopositivity) were always present in the white matter (Figure 1l), and dispersed throughout the cortex (in five cases) or clustered in layer I (three cases). Fifteen of the 20 specimens showed a normal perilesional cortex in which only rare and scattered DNs were detected (Figure 1c,h,i). Layer-specific gene expression in FCD The lamina-specific expression patterns of the considered genes have been previously demonstrated in normal temporal and frontal cortex tissue: briefly, Cux2 mrna expression is observed in many cells in layers II and III; Rorβ mrna is intensely expressed in layer IV and a few scattered cells in neighbouring layers; Er81 and Nurr1 mrnas are respectively detected in neuronal subpopulations in layers V and VI; and CTGF mrna is observed in a few cells in layer VI and the white matter [20,22]. An additional figure shows these features in detail (see Additional file 1).
5 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 5 of 15 Figure 1 Histopathological features of surgical samples taken from patients with Type IIb FCD. a, d, e: Examples of a severe lesion (parietal lobe): a, d (SMI immunoreactivity, ir) and e (NeuN ir) highlight typical features of Type II FCD, which is characterised by the total disruption of cortical lamination and the presence of numerous DNs throughout the cortex intermingled with fewer normal-looking neurons. j, k: Details of the regions marked with asterisks in d and e, respectively, show DNs that are clearly distinguishable by their very large size and abnormal shape (arrows). In the same case, vimentin-positive BCs (l) are diffusely distributed in the subcortical white matter. b, f, g: Examples of a less severe lesion (frontal lobe). b, f (SMI ir) and g (NeuN ir) showing cortical areas in which lamination is relatively preserved and DNs (arrows) are scattered in restricted cortical layers (deep layers) intermingled with numerous normal-looking neurons. m, n: Details of the regions marked with asterisks in f and g, respectively, show DNs (arrow) and normal-looking neurons. c, h, i: Examples of perilesional cortex (temporal lobe). c, h (SMI ir) and i (NeuN ir) showing normal cortex adjacent to the principal lesion. Scale bars: 3.8 mm (a); 2.5mm(b); 3.6mm(c); 540μm (d, e); 450 μm (f, g); 414 μm (h, i); 120 μm (j,k,m,n);4.68mm(l) and 50 μm forinsetinl. In the pathological specimens used for this study, Cux2, Rorβ, Er81 and Nurr1 mrnas were expressed in both abnormal and normal-looking neurons, which could be clearly distinguished on the basis of their differently sized bodies and nuclei (Figure 2a-d). CTGF mrna expression was scanty and observed only in a few normal cells in the deep layers and in the white matter (data not shown). In the 16 specimens showing severe laminar disorganisation and containing an adjacent perilesional area, there was a clear-cut difference in the distribution and signal intensity of gene expression moving from the core of the lesion toward the perilesional area (Figure 3a,b). Within the core of the lesion, normal-looking neurons (identified on the basis of their normal size and shape)
6 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 6 of 15 Figure 2 Layer-specific gene (LSG) expression in normal-looking neurons and DNs. a-d: Adjacent sections, obtained from a parietal lobe, showing regions expressing Cux2 (a), Rorβ (b), Er81 (c) and Nurr1 (d). In particular, areas from superficial cortex (sup.ctx), middle cortex (mid.ctx) and the boundary between the deep cortex and the white matter (wm) are shown. For each LSG, normal-looking neurons (asterisks) and DNs (stars) are easily distinguishable by their different size and shape (see high magnification images). Confocal double immunofluorescence images combining immunoreactivity for neuronal markers (SMI311 and MAP2) with ISH for Er81 and Nurr1 showed the morphology of the normal-looking neurons (e, f) and DNs (g, h,). Scale bars: 200 μm (a-d) and 60 μm for high magnification images; 55 μm (e-h). were observed within the appropriate cortical laminae: Cux2-positive cells in the upper cortex, Rorβ-positive cells in the middle of the cortex, and Er81- and Nurr1positive cells in the deeper cortex (Figure 3d,g-j,l,n-q), thus suggesting normal laminar organisation even in the core of the lesion (compare Figure 3d with 3c). Moreover, these neurons were visibly reduced in number in comparison with the adjacent perilesional area (particularly those that were positive for Rorβ), thus reflecting the reduced neuronal density inside the lesion (compare Figure 3g-j with Figure 4b-e). This data were further supported by quantitative analysis of normal-looking neurons cell density (see Additional file 2). DNs (identified on the basis of their very large size and altered morphology) showed the variable expression of all of the LSGs except for CTGF, without any laminar specificity (Figure 3g,j,l,m,r). The distribution of the DNs labelled by different LSGs was uneven regardless of the subtype of FCD (Type IIa vs IIb) and the lobar involvement of the dysplastic lesion. The details of LSG expression in each case are shown in Figure 5. In the four less severely affected specimens, the DNs were prevalently localised in layers III or V/VI (Figure 6a, f). The DNs labelled for Cux2, Er81 and Nurr1 (Figure 6d,e,i,j) retained their correct laminar position (unlike in the severely affected areas), and the normal-looking neurons intensely labelled with LSGs were properly distributed throughout the cortical thickness (Figure 6b-e, and g-j) and their density was similar to that observed in the perilesional cortex as confirmed by quantitative analysis (see Additional file 2). In the 15 specimens that included perilesional cortex beside the core of the lesion, the laminar organisation was normal (Figure 4a) with the regular distribution of the LSGs in normal-looking neurons and no evidence of labelled DNs (Figure 4b-e). However, quantitative measurement of cortical thickness showed Er81-positive cells were more widespread throughout layer V than in the control
7 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 7 of 15 Figure 3 (See legend on next page.)
8 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 8 of 15 (See figure on previous page.) Figure 3 LSG expression in Type II FCD (severe area). Typical LSG expression in a case of Type IIa FCD (occipital lobe) histopathologically characterised by a severe lesion with an adjacent perilesional area (a, SMI ir). b: Example of Er81 pattern showing intense expression in layer V of the perilesional cortex (arrowheads), and less intense and dispersed expression in the core of the lesion. c-e: Single ISH images of each gene in the severe lesion converted to pseudo-colour images (green for Cux2, fuchsia for Rorβ, yellow for Er81, andredfornurr1) for overlay representation. The cortical distributions of normal-looking neurons (NNs, d) anddns(e) are shown separately, and juxtaposed with normal cortex for purposes of comparison (c). Note the normal laminar distribution and reduced number of NNs in comparison with the dispersion of DNs. f-j: Adjacent sections from the same case as that shown in a (SMI ir) and f (thionin staining), showing the expression of Cux2 (g), Rorβ (h), Er81 (i) and Nurr1 (j) mrnas in normal-looking neurons and DNs. k-r: Details of the regions marked with asterisks in f-j showing the morphological features of the NNs and DNs. Scale bars: 5.2 mm (a, b); 240μm (c-e); 195μm (f-j); 50μm (k-r). cases (33,9 ± 8,1% for perilesional cortex versus 23,7 ± 3,8% for control cortex, p = 0,025). Layer-specific gene expression in BCs BCs were identified in 12 cases on the basis of their morphological features and vimentin immunolabelling, thus allowing a diagnosis of Type IIb FCD. They were mainly observed in the subcortical white matter (Figure 7a,b) but, in some cases, they were also distributed throughout the cortical thickness, and occasionally even invaded layer I. As in the case of the DNs, the Cux2, Rorβ, Er81 and Nurr1 riboprobes were variably expressed in BCs (Figure 7 c-j) with no specific labelling associated with their distribution in the different cortical layers or lobar involvement. These data were confirmed by the double fluorescent experiments using vimentin and the different LSGs (Figure 7k-p). Figure 5 shows the pattern of LSG expression in the BCs of each case. ps6 immunoreactivity in FCD We observed immunoreactivity for ps6 in the DNs and BCs. Labelled DNs were detected in both the severely affected (Figure 8a,c) and less severely affected areas (Figure 8b,d,e), whereas no specific expression of ps6 was detected in the normal-looking neurons in either the core of lesion or the adjacent perilesional area. Figure 4 LSG expression in perilesional cortex. Typical LSG expression in perilesional cortex (frontal lobe) histopathologically characterised by a normal laminar organization and the absence of DNs (a, SMI ir). b-e: Adjacent sections from the same case as that shown in a showing the normal expression of Cux2 (b), Rorβ (c), Er81 (d) and Nurr1 (e). Scale bars: 295 μm (a-e).
9 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 9 of 15 Figure 5 Details of layer-specific gene expression in DNs and BCs. For each case, the presence of DNs positive for the different LSG is indicated by a black or grey cell (the white cells indicate no labelling): the black cells indicate that DN distribution is severely affected, and the grey cells indicate DNs distributed in their corresponding layers. In the case of BCs, the hatched cells indicate the presence of the different LSGs, and the white cells indicate no labelling (nr = not clearly recognisable). Abbreviations: BCs: balloon cells; DNs: dysmorphic neurons; FCD: focal cortical dysplasia; ID: patient identification number. *The site is the cortical area that underwent ISH analysis (O: occipital; T: temporal; F: frontal; P: parietal). Discussion Focal cortical dysplasias are among the most frequent brain malformations encountered in epileptic patients undergoing surgical treatment. In particular, Type II FCDs, which are often recognisable at the time of clinical screening, are characterised by an early onset of epilepsy, a high seizure frequency, and particular MRI and EEG (or SEEG) pictures [29-32], and surgical treatment often leads to seizure freedom even over long follow-up periods [30]. The main neuropathological features of Type II FCDs have been established since the original description by Taylor et al. [1],andsotheirclassification has not varied in successive classification systems [2,33]. However, although many immunohistochemical studies have identified and characterised the various neuronal populations involved in Type II FCD, its aetiology and pathogenesis are unknown. The recent developmental and genetic classification of malformations of cortical development (MCD) published by Barkowich et al. [8] places Type II FCDs in the group of cortical malformations secondary to abnormal neuronal and glial proliferation, but the ontogenetic mechanisms and embryonic time window in which the derangement of cortical maturation and neuronal migration takes place remain unclear. In order to gain more insights into the pathogenesis of cortical malformations, new LSG-based approaches have been proposed. Many different LSGs have been used in studies of animal and human specimens, and their expression profiles through the cortical layers have been defined; furthermore, it has been demonstrated that the expression and laminar location of most LSGs is preserved during phylogenesis and pre- and postnatal development [16-18,34]. On the basis of the assumption that, once specified during embryonic development, neuronal identity and laminar fate are apparently impervious to change even if cell migration is abnormal, it has been suggested that LSGs can be confidently used as markers to study cortical malformations [13,35]. However, although many studies have investigated different types of MCD by means of LSGs, only a few have specifically concentrated on Type II FCD [21,24,25,36]. The neuropathological hallmarks of Type II FCDs are disrupted cortical lamination, reduced cortical neuronal density, the presence of DNs and, in subtype IIb, the presence of BCs. In relation to these, the main findings of the present study are: i) although reduced in number, normal-looking neurons retain their correct laminar position even inside the core of the lesion, thus indicating a partial laminar organisation; ii) on the contrary,
10 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 10 of 15 Figure 6 LSG expression in Type II FCD (less severe area). Typical LSG expression in a case of Type IIb FCD (frontal lobe) histopathologically characterized by a less severe lesion with DNs localised only in the deep portion of the cortex (a, SMI ir). b-e: Adjacent sections from the same case as that shown in a showing the expression of Cux2 (b), Rorβ (c), Er81 (d) and Nurr1 (e). Note that Cux2 and Rorβ are expressed only in normal-looking neurons (NNs) in the appropriate cortical laminae (b, c), whereas Er81 and Nurr1 (d, e) are expressed in both NNs and DNs in the deep layers. f-j: Details of the regions marked with asterisks in b-e showing the morphological features of the NNs and DNs (arrows). Scale bars: 280 μm (a-e); 90 μm (f-j). DNs and BCs are dispersed throughout the cortex and white matter without any laminar specificity, and show a highly variable LSG expression pattern; and iii) LSGs do not reveal any differences between Type IIa and IIb FCD. The first and previously unknown finding is that the normal-looking neurons, albeit markedly fewer in comparison with the fairly normal adjacent cortex, can be found in the appropriate cortical laminae, which suggests that a certain proportion are properly generated and migrated. This implies that the genetic programme for neuronal migration is not disrupted per se and that the laminar disorganisation is mainly (if not exclusively) due to altered DN migration. Lower neuronal density in the region of the dysplasia than in the perilesional cortex is a consistent finding in Type II FCD, and may be due to different phenomena such as a local failure of cell proliferation or enhanced neuronal vulnerability in this area [3,4,37]; however, our data highlight for the first time that the number of normal-looking neurons is particularly reduced. The second finding is that DNs are not only haphazardly displaced but (particularly within the core of the lesion) dispersed throughout the thickness of the cortex regardless of the LSG they express: for example, Nurr1- positive cells, which are normally found in the layer VI, were also present in the superficial part of the cortex, whereas Cux2-positive cells, which are normally found
11 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 11 of 15 Figure 7 Representative LSG expression in BCs. a, b. Example of Type IIb FCD (temporal lobe) characterised by a severe lesion with numerous DNs dispersed throughout the cortex (a, SMI ir), and the presence of BCs in the white matter (b, vimentin ir). Adjacent sections from the same case as that shown in a and b showing the expression of Cux2 (c), Rorβ (d), Er81 (g) and Nurr1 (h) in BCs in the white matter (boxed area in b). Note the heterogeneous expression of the LSGs in the BCs. e, f, i, j: Details of the regions marked with asterisks in c, d, g and h showing the morphological features of the BCs. Confocal double immunofluorescence images combining vimentin ir (red) with ISH for Er81 (k-m) and Nurr1 (n-p) confirmed the identification of the BCs. Scale bars:1, 41 mm (a); 1,27 (b); 357 μm (c, d, g, h); 92μm (e, f, i, j); 70μm k-p). in layers II and III, were present in the depths of the cortical ribbon and white matter. Unfortunately, technical problems prevented us from using double-labelling in order to verify whether DNs express more than one LSG. It is not possible to compare our findings with other published data concerning Type II FCD because the studies used different LSGs and different methodologies (IHC or ISH). Moreover, some published studies not specified
12 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 12 of 15 Figure 8 Representative ps6 expression in Type II FCD. Examples of ps6 expression in samples of severe (a) and less severe (b, arrows) Type II FCD; in both cases, the immunoreactivity suggests the presence of mtor pathway hyperactivation in DNs. c-e. Details of the regions marked with asterisks in a, b. Scale bars: 268 μm (a,b); 60μm (c,d,e). the cell subtypes (i.e. normal-looking neurons vs DNs and BCs) expressing different LSGs [24,25]. Furthermore, as the LSGs we used are preserved during development, we could not verify the hypothesis that some DNs may retain the expression of genes that are exclusively present prenatally as previously suggested [21,24,25]. Our finding that different LSGs are expressed in DNs improperly located in different layers of the cortex ribbon suggest that, whatever the defect, it occurred in the early period of development. Recent developmental data [38-41] indicate that radial glial cells (RGs) generate neurons by means of multiple rounds of self-renewal and asymmetric division, and that new-born neurons often use the parent cell s radial fibre to migrate to the cortical plate [42]. Furthermore, it has been observed that primate corticogenesis is characterised by the appearance of a large sub-ventricular zone (SVZ) that seems to be important for the presence of resident progenitor cells that contribute to neuronal production and control neocortical size [43]. It has also been demonstrated that two sub-classes of human RGs co-exist in the ventricular zone (VZ) and the outer part of the SVZ (OSVZ), each of which act as neural stem cells in their respective locations and provide a mechanism favouring increased neuron production, which may be important for building a larger brain [44]. Although cortical neuron production begins in the VZ during gestational week 6 (GW6), the OSVZ does not arise until GW11, but then dramatically expands over the subsequent six GW to become the predominant germinal region in the neocortex. This suggests that OSVZ expansion and proliferation may increase the number of late-born neurons destined to became the future upper cortical layers, whereas the VZ generates the earliestborn neurons destined to form the deep cortical layers. On the basis of these developmental data, we can hypothesise that, during the early stages of cortical development (when the VZ is very actively proliferating and gives rise to the post-mitotic neurons that migrate to form the deep layers and the precursor cells for the SVZ), one hit is sufficient to modify the future lineage of some but not all progenitor cells in patients with Type II FCD. Another finding of our study is that, like the DNs, the BCs expressed all of the LSGs regardless of their location and even they were found in all of the layers. These
13 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 13 of 15 cells are immature, and their immunohistochemical profiles indicate the expression of vimentin, nestin and, in some cases, markers of precursor cells [6]. They seem to arise from radial cell precursors [11,21,45], but the fact that some of them co-express neuronal markers suggests aberrant cell-fate specification [5]. It is therefore conceivable that this abnormal differentiation may have been responsible for their labelling with our panel of LSGs, which are typically expressed in excitatory neurons. In any case, the fact that the distribution of LSGs in BCs was similar to that observed in DNs further supports the hypothesis that the primary hit inducing the malformation occurs during the early stages of development. We did not identify any relationship between distinct patterns of LSG expression and FCD subtype or lobar involvement. The few published data in this regard are controversial insofar as some authors (using different LSGs) have found different distribution patterns and/or different numbers of immunopositive cells in Type IIa and IIb [24,25], whereas only Fauser et al. [36] have found differences in lobar LSG expression. The processes involved in cortical development (including neurogenesis, cell migration and differentiation) are highly synchronised and coordinated by extra- and intracellular signals that converge on cytoskeletal remodelling [46,47], and it has been demonstrated that mutations in the genes encoding cytoskeletal proteins are involved in many malformations of cortical development [48]. Interestingly, one of the main histopathological features of Type II FCD is the presence of DNs characterised by the cytoplasmic engulfment of neurofilaments pushing the nucleus to the cell periphery and disrupting the regular distribution of chromatin. Similar DNs are found in patients with TSC in whom TSC1 or TSC2 gene mutations activate the mtor cascade that affects many cell biological processes, including the regulation of actin dynamics [49]. In line with other recent findings [7,9,10], our data show that the DNs were labelled with ps6 antibody, which suggests that the mtor pathway may also be involved in Type II FCD. As no genetic impairment has been found in this disease, it can be hypothesised that an external phenomenon could hit some of the precursor cells acting on the neuronal cytoskeletal framework very early during cortical development (when the VZ is proliferating), and that this leads to cytological alterations and the subsequently aberrant migratory stream. This would explain the presence of normal-looking neurons that show no changes in migration patterns. In agreement with this hypothesis, the presence of a localized central nervous system infection during fetal brain development has been proposed as a new pathogenic mechanism for Type II FCD. In fact, recent studies have shown the presence of papillomavirus in BCs (but, surprisingly, not in DNs), and the presence of herpes and cytomegalovirus infections in both BC and DNs [50,51]. Moreover, human papillomavirus, the most common cause of cervical cancer in women, has been identified as an activator of the mtor signalling cascade and the cytopathic effect of the infection on cervical epithelium results in balloon-like cells similar to those observed in Type II FCD. Although these data need further confirmation, they are in line with the hypothesis that an external or environmental hit affecting selected precursor cells during the very early stages of cortical development may interfere and disrupt normal cortical development as a result of mtor activation. One intriguing aspect of our findings is the presence of some DNs outside the core of the lesions (namely less severe lesion) that retained their correct laminar position in the cortical ribbon. Interestingly, like those associated with severe lesions, these DNs were also labelled with ps6 antibody. We do not have any definite explanation for this feature, but hypothesise that the high frequency of epileptic discharges characterising this form of dysplasia may induce a secondary pathological plasticity leading to morphological rearrangements, as suggested in various animal models [52]. Conclusions This study shows the existence of hidden cortical lamination involving normal-looking neurons, which retain their ability to migrate correctly in the cortex, unlike DNs which, in addition to their morphological abnormalities and mtor hyperactivation, show an altered migratory pattern. BCs also expressed all of the LSGs regardless of their location. Taken together these data suggest that an external or environmental hit affecting selected precursor cells during the very early stages of cortical development may disrupt normal cortical development. Additional files Additional file 1: LSG expression in normal human temporal cortex. Description of data: Adjacent sections from the temporal cortex showing the typical expression of Cux2 (b), Rorβ (c), Er81 (d) and Nurr1 (e) mrnas. The laminar localization of each mrna is determined by the adjacent NeuN-immunostained section and is indicated by Roman numerals (a). Scale bars: 385 μm (a-e). Additional file 2: Normal-looking neurons cell density. a: Histogram showing the cell density of normal-looking neurons (NNs) positive for LSG in samples characterised by severe disruption of the cortical structure; note the significant reduction of NNs in lesional versus perilesiona areas. Conversely, in less affected samples (b), no differenced in NNs cell density is reported in lesional versus perilesional areas. Statistical significance is indicated by asterisks. Competing interest The authors declares that they have no competing interests.
14 Rossini et al. Acta Neuropathologica Communications 2014, 2:45 Page 14 of 15 Acknowledgements The study was supported by grants from the Italian Ministry of Health, the Fondazione Banca del Monte di Lombardia (FBML), the Associazione Paolo Zorzi per le Neuroscienze, and EU grant FP7 (Desire) No We would like to thank Dr. A. Watakabe and Dr. T. Yamamori for providing the riboprobes, and Dr C. Frassoni for critically reading the manuscript. Author details 1 Clinical Epileptology and Experimental Neurophysiology Unit, Istituto Neurologico C. Besta, Via Amadeo 42, Milano, Italy. 2 C. Munari Epilepsy Surgery Centre, Niguarda Hospital, Milan, Italy. 3 Department of Neurosurgery, Fondazione IRCCS, Istituto Neurologico C. Besta, Milan, Italy. 4 Department of Pathology, Niguarda Hospital, Milan, Italy. Received: 6 February 2014 Accepted: 4 April 2014 Published: 15 April 2014 References 1. Taylor DC, Falconer MA, Bruton CJ, Corsellis JA (1971) Focal dysplasia of the cerebral cortex in epilepsy. J Neurol Neurosurg Psychiatry 34: Blumcke I, Thom M, Aronica E, Armstrong DD, Vinters HV, Palmini A, Jacques TS, Avanzini G, Barkovich AJ, Battaglia G, Becker A, Cepeda C, Cendes F, Colombo N, Crino P, Cross JH, Delalande O, Dubeau F, Duncan J, Guerrini R, Kahane P, Mathern G, Najm I, Ozkara C, Raybaud C, Represa A, Roper SN, Salamon N, Schulze-Bonhage A, Tassi L et al (2011) The clinicopathologic spectrum of focal cortical dysplasias: a consensus classification proposed by an ad hoc Task Force of the ILAE Diagnostic Methods Commission. Epilepsia 52: Thom M, Martinian L, Sen A, Cross JH, Harding BN, Sisodiya SM (2005) Cortical neuronal densities and lamination in focal cortical dysplasia. Acta Neuropathol 110: Alonso-Nanclares L, Garbelli R, Sola RG, Pastor J, Tassi L, Spreafico R, DeFelipe J (2005) Microanatomy of the dysplastic neocortex from epileptic patients. Brain 128: Englund C, Folkerth RD, Born D, Lacy JM, Hevner RF (2005) Aberrant neuronal-glial differentiation in Taylor-type focal cortical dysplasia (type IIA/B). Acta Neuropathol 109: Sisodiya SM, Fauser S, Cross JH, Thom M (2009) Focal cortical dysplasia type II: biological features and clinical perspectives. Lancet Neurol 8: Yasin SA, Latak K, Becherini F, Ganapathi A, Miller K, Campos O, Picker SR, Bier N, Smith M, Thom M, Anderson G, Helen Cross J, Harkness W, Harding B, Jacques TS (2010) Balloon cells in human cortical dysplasia and tuberous sclerosis: isolation of a pathological progenitor-like cell. Acta Neuropathol 120: Barkovich AJ, Guerrini R, Kuzniecky RI, Jackson GD, Dobyns WB (2012) A developmental and genetic classification for malformations of cortical development: update Brain 135: Miyata H, Chiang AC, Vinters HV (2004) Insulin signaling pathways in cortical dysplasia and TSC-tubers: tissue microarray analysis. Ann Neurol 56: Ljungberg MC, Bhattacharjee MB, Lu Y, Armstrong DL, Yoshor D, Swann JW, Sheldon M, D Arcangelo G (2006) Activation of mammalian target of rapamycin in cytomegalic neurons of human cortical dysplasia. Ann Neurol 60: Lamparello P, Baybis M, Pollard J, Hol EM, Eisenstat DD, Aronica E, Crino PB (2007) Developmental lineage of cell types in cortical dysplasia with balloon cells. Brain 130: Hua Y, Crino PB (2003) Single cell lineage analysis in human focal cortical dysplasia. Cereb Cortex 13: Hevner RF (2007) Layer-specific markers as probes for neuron type identity in human neocortex and malformations of cortical development. J Neuropathol Exp Neurol 66: Molyneaux BJ, Arlotta P, Menezes JR, Macklis JD (2007) Neuronal subtype specification in the cerebral cortex. Nat Rev Neurosci 8: Ferrere A, Vitalis T, Gingras H, Gaspar P, Cases O (2006) Expression of Cux-1 and Cux-2 in the developing somatosensory cortex of normal and barreldefective mice. Anat Rec A: Discov Mol Cell Evol Biol 288: Watakabe A, Ichinohe N, Ohsawa S, Hashikawa T, Komatsu Y, Rockland KS, Yamamori T (2007) Comparative analysis of layer-specific genes in Mammalian neocortex. Cereb Cortex 17: Moroni RF, Inverardi F, Regondi MC, Watakabe A, Yamamori T, Spreafico R, Frassoni C (2009) Expression of layer-specific markers in the adult neocortex of BCNU-Treated rat, a model of cortical dysplasia. Neuroscience 159: Moroni RF, Cipelletti B, Inverardi F, Regondi MC, Spreafico R, Frassoni C (2011) Development of cortical malformations in BCNU-treated rat, model of cortical dysplasia. Neuroscience 175: Ferland RJ, Batiz LF, Neal J, Lian G, Bundock E, Lu J, Hsiao YC, Diamond R, Mei D, Banham AH, Brown PJ, Vanderburg CR, Joseph J, Hecht JL, Folkerth R, Guerrini R, Walsh CA, Rodriguez EM, Sheen VL (2009) Disruption of neural progenitors along the ventricular and subventricular zones in periventricular heterotopia. Hum Mol Genet 18: Garbelli R, Rossini L, Moroni RF, Watakabe A, Yamamori T, Tassi L, Bramerio M, Russo GL, Frassoni C, Spreafico R (2009) Layer-specific genes reveal a rudimentary laminar pattern in human nodular heterotopia. Neurology 73: Hadjivassiliou G, Martinian L, Squier W, Blumcke I, Aronica E, Sisodiya SM, Thom M (2010) The application of cortical layer markers in the evaluation of cortical dysplasias in epilepsy. Acta Neuropathol 120: Rossini L, Moroni RF, Tassi L, Watakabe A, Yamamori T, Spreafico R, Garbelli R (2011) Altered layer-specific gene expression in cortical samples from patients with temporal lobe epilepsy. Epilepsia 52: Saito T, Hanai S, Takashima S, Nakagawa E, Okazaki S, Inoue T, Miyata R, Hoshino K, Akashi T, Sasaki M, Goto Y, Hayashi M, Itoh M (2011) Neocortical layer formation of human developing brains and lissencephalies: consideration of layer-specific marker expression. Cereb Cortex 21: Arai A, Saito T, Hanai S, Sukigara S, Nabatame S, Otsuki T, Nakagawa E, Takahashi A, Kaneko Y, Kaido T, Saito Y, Sugai K, Sasaki M, Goto Y, Itoh M (2012) Abnormal maturation and differentiation of neocortical neurons in epileptogenic cortical malformation: unique distribution of layer-specific marker cells of focal cortical dysplasia and hemimegalencephaly. Brain Res 1470: Sakakibara T, Sukigara S, Saito T, Otsuki T, Takahashi A, Kaneko Y, Kaido T, Saito Y, Sato N, Kimura Y, Nakagawa E, Sugai K, Sasaki M, Goto Y, Itoh M (2012) Delayed maturation and differentiation of neurons in focal cortical dysplasia with the transmantle sign: analysis of layer-specific marker expression. J Neuropathol Exp Neurol 71: Tassi L, Garbelli R, Colombo N, Bramerio M, Lo Russo G, Deleo F, Milesi G, Spreafico R (2010) Type I focal cortical dysplasia: surgical outcome is related to histopathology. Epileptic Disord 12: , doi: /epd Garbelli R, Munari C, De Biasi S, Vitellaro-Zuccarello L, Galli C, Bramerio M, Mai R, Battaglia G, Spreafico R (1999) Taylor s cortical dysplasia: a confocal and ultrastructural immunohistochemical study. Brain Pathol 9: Hirokawa J, Watakabe A, Ohsawa S, Yamamori T (2008) Analysis of area-specific expression patterns of RORbeta, ER81 and Nurr1 mrnas in rat neocortex by double in situ hybridization and cortical box method. PLoS One 3:e Colombo N, Tassi L, Deleo F, Citterio A, Bramerio M, Mai R, Sartori I, Cardinale F, Lo Russo G, Spreafico R (2012) Focal cortical dysplasia type IIa and IIb: MRI aspects in 118 cases proven by histopathology. Neuroradiology 54: Tassi L, Garbelli R, Colombo N, Bramerio M, Russo GL, Mai R, Deleo F, Francione S, Nobili L, Spreafico R (2012) Electroclinical, MRI and surgical outcomes in 100 epileptic patients with type II FCD. Epileptic Disord 14: Tassi L, Colombo N, Garbelli R, Francione S, Lo Russo G, Mai R, Cardinale F, Cossu M, Ferrario A, Galli C, Bramerio M, Citterio A, Spreafico R (2002) Focal cortical dysplasia: neuropathological subtypes, EEG, neuroimaging and surgical outcome. Brain 125: Chassoux F, Devaux B, Landre E, Turak B, Nataf F, Varlet P, Chodkiewicz JP, Daumas-Duport C (2000) Stereoelectroencephalography in focal cortical dysplasia: a 3D approach to delineating the dysplastic cortex. Brain 123(Pt 8): Palmini A, Najm I, Avanzini G, Babb T, Guerrini R, Foldvary-Schaefer N, Jackson G, Luders HO, Prayson R, Spreafico R, Vinters HV (2004) Terminology and classification of the cortical dysplasias. Neurology 62:S2 S8 34. Wang WZ, Hoerder-Suabedissen A, Oeschger FM, Bayatti N, Ip BK, Lindsay S, Supramaniam V, Srinivasan L, Rutherford M, Mollgard K, Clowry GJ, Molnar Z (2010) Subplate in the developing cortex of mouse and human. J Anat 217: Hevner RF, Daza RA, Rubenstein JL, Stunnenberg H, Olavarria JF, Englund C (2003) Beyond laminar fate: toward a molecular classification of cortical projection/pyramidal neurons. Dev Neurosci 25:
New Classification of Focal Cortical Dysplasia: Application to Practical Diagnosis
 New Classification of Focal Cortical Dysplasia: Application to Practical Diagnosis Original Article Journal of Epilepsy Research pissn 2233-6249 / eissn 2233-6257 Yoon-Sung Bae, MD 1, Hoon-Chul Kang, MD,
New Classification of Focal Cortical Dysplasia: Application to Practical Diagnosis Original Article Journal of Epilepsy Research pissn 2233-6249 / eissn 2233-6257 Yoon-Sung Bae, MD 1, Hoon-Chul Kang, MD,
Advanced multimodal imaging in malformations of cortical development
 Advanced multimodal imaging in malformations of cortical development Seok Jun Hong (sjhong@bic.mni.mcgill.ca) NOEL Neuroimaging of Epilepsy Lab MICA Multimodal Imaging and Connectome Analysis Lab w4 w5
Advanced multimodal imaging in malformations of cortical development Seok Jun Hong (sjhong@bic.mni.mcgill.ca) NOEL Neuroimaging of Epilepsy Lab MICA Multimodal Imaging and Connectome Analysis Lab w4 w5
Is Focal Cortical Dysplasia an Infectious Disease?
 Current Literature In Basic Science Is Focal Cortical Dysplasia an Infectious Disease? Detection of Human Papillomavirus in Human Focal Cortical Dysplasia Type IIB. Chen J, Tsai V, Parker WE, Aronica E,
Current Literature In Basic Science Is Focal Cortical Dysplasia an Infectious Disease? Detection of Human Papillomavirus in Human Focal Cortical Dysplasia Type IIB. Chen J, Tsai V, Parker WE, Aronica E,
Malformations of cortical development in children: clinical manifestation, neuroimaging and neuropathology in selected cases
 Original article Malformations of cortical development in children: clinical manifestation, neuroimaging and neuropathology in selected cases Ewa Emich-Widera 1, Dawid Larysz 2, Ewa Kluczewska 3, Patrycja
Original article Malformations of cortical development in children: clinical manifestation, neuroimaging and neuropathology in selected cases Ewa Emich-Widera 1, Dawid Larysz 2, Ewa Kluczewska 3, Patrycja
Electroclinical, MRI and surgical outcomes in 100 epileptic patients with type II FCD
 Original article Epileptic Disord 2012; 14 (3): 257-66 Electroclinical, MRI and surgical outcomes in 100 epileptic patients with type II FCD Laura Tassi 1, Rita Garbelli 2, Nadia Colombo 3, Manuela Bramerio
Original article Epileptic Disord 2012; 14 (3): 257-66 Electroclinical, MRI and surgical outcomes in 100 epileptic patients with type II FCD Laura Tassi 1, Rita Garbelli 2, Nadia Colombo 3, Manuela Bramerio
Type I focal cortical dysplasia: surgical outcome is related to histopathology
 Original article Epileptic Disord 2010; 12 (3): 181-91 Type I focal cortical dysplasia: surgical outcome is related to histopathology Laura Tassi 1, Rita Garbelli 2, Nadia Colombo 3, Manuela Bramerio 4,
Original article Epileptic Disord 2010; 12 (3): 181-91 Type I focal cortical dysplasia: surgical outcome is related to histopathology Laura Tassi 1, Rita Garbelli 2, Nadia Colombo 3, Manuela Bramerio 4,
Epilepsy & Behavior Case Reports
 Epilepsy & Behavior Case Reports 1 (2013) 45 49 Contents lists available at ScienceDirect Epilepsy & Behavior Case Reports journal homepage: www.elsevier.com/locate/ebcr Case Report Partial disconnection
Epilepsy & Behavior Case Reports 1 (2013) 45 49 Contents lists available at ScienceDirect Epilepsy & Behavior Case Reports journal homepage: www.elsevier.com/locate/ebcr Case Report Partial disconnection
High Resolution MRI in the evaluation of cerebral focal cortical dysplasias
 High Resolution MRI in the evaluation of cerebral focal cortical dysplasias Poster No.: C-0966 Congress: ECR 2012 Type: Scientific Exhibit Authors: M. Stefanetti, E. Antichi, T. Tartaglione, F. Lanza,
High Resolution MRI in the evaluation of cerebral focal cortical dysplasias Poster No.: C-0966 Congress: ECR 2012 Type: Scientific Exhibit Authors: M. Stefanetti, E. Antichi, T. Tartaglione, F. Lanza,
Good interobserver and intraobserver agreement in the evaluation of the new ILAE classification of focal cortical dysplasias
 FULL-LENGTH ORIGINAL RESEARCH Good interobserver and intraobserver agreement in the evaluation of the new ILAE classification of focal cortical dysplasias *Roland Coras, yonno J. de Boer, zdawna Armstrong,
FULL-LENGTH ORIGINAL RESEARCH Good interobserver and intraobserver agreement in the evaluation of the new ILAE classification of focal cortical dysplasias *Roland Coras, yonno J. de Boer, zdawna Armstrong,
Blurring the Lines Between Lesional and Nonlesional MRI
 Current Literature In Clinical Science Blurring the Lines Between Lesional and Nonlesional MRI Blurring in Patients With Temporal Lobe Epilepsy: Clinical, High-field Imaging and Ultrastructural Study.
Current Literature In Clinical Science Blurring the Lines Between Lesional and Nonlesional MRI Blurring in Patients With Temporal Lobe Epilepsy: Clinical, High-field Imaging and Ultrastructural Study.
Optimizing MR Imaging Detection of Type 2 Focal Cortical Dysplasia: Best Criteria for Clinical Practice
 Published May 3, 2012 as 10.3174/ajnr.A3081 ORIGINAL RESEARCH C. Mellerio M.-A. Labeyrie F. Chassoux C. Daumas-Duport E. Landre B. Turak F.-X. Roux J.-F. Meder B. Devaux C. Oppenheim Optimizing MR Imaging
Published May 3, 2012 as 10.3174/ajnr.A3081 ORIGINAL RESEARCH C. Mellerio M.-A. Labeyrie F. Chassoux C. Daumas-Duport E. Landre B. Turak F.-X. Roux J.-F. Meder B. Devaux C. Oppenheim Optimizing MR Imaging
Differential localisation of hamartin and tuberin and increased S6 phosphorylation in a tuber
 Differential localisation of hamartin and tuberin in a tuber 10 Differential localisation of hamartin and tuberin and increased S6 phosphorylation in a tuber Floor Jansen*, Robbert Notenboom*, Mark Nellist*,
Differential localisation of hamartin and tuberin in a tuber 10 Differential localisation of hamartin and tuberin and increased S6 phosphorylation in a tuber Floor Jansen*, Robbert Notenboom*, Mark Nellist*,
Identification and immunophenotype of abnormal cells present in focal cortical dysplasia type IIb
 Sousa et al. Surgical and Experimental Pathology (2018) 1:9 https://doi.org/10.1186/s42047-018-0024-5 Surgical and Experimental Pathology RESEARCH Open Access Identification and immunophenotype of abnormal
Sousa et al. Surgical and Experimental Pathology (2018) 1:9 https://doi.org/10.1186/s42047-018-0024-5 Surgical and Experimental Pathology RESEARCH Open Access Identification and immunophenotype of abnormal
Hemimegalencephaly without seizures: report of a case and review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Hemimegalencephaly without seizures: report of a case and review of literature Agrawal Atul, Dutta Gautam, Singh Daljit, Sachdeva
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Hemimegalencephaly without seizures: report of a case and review of literature Agrawal Atul, Dutta Gautam, Singh Daljit, Sachdeva
Supplementary Figure 1
 Supplementary Figure 1 Kif1a RNAi effect on basal progenitor differentiation Related to Figure 2. Representative confocal images of the VZ and SVZ of rat cortices transfected at E16 with scrambled or Kif1a
Supplementary Figure 1 Kif1a RNAi effect on basal progenitor differentiation Related to Figure 2. Representative confocal images of the VZ and SVZ of rat cortices transfected at E16 with scrambled or Kif1a
Molecular alterations in epilepsy-associated malformations of cortical development Boer, K.
 UvA-DARE (Digital Academic Repository) Boer, K. Link to publication Citation for published version (APA): Boer, K. (2009).. General rights It is not permitted to download or to forward/distribute the text
UvA-DARE (Digital Academic Repository) Boer, K. Link to publication Citation for published version (APA): Boer, K. (2009).. General rights It is not permitted to download or to forward/distribute the text
Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
 Seizure 2002; 11: 330 334 doi:10.1053/seiz.2001.0610, available online at http://www.idealibrary.com on CASE REPORT Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
Seizure 2002; 11: 330 334 doi:10.1053/seiz.2001.0610, available online at http://www.idealibrary.com on CASE REPORT Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
Epilepsy surgery is an increasingly recognized therapeutic
 J Neurosurg Pediatrics 14:68 80, 2014 AANS, 2014 Magnetic resonance imaging abnormalities in the resection region correlate with histopathological type, gliosis extent, and postoperative outcome in pediatric
J Neurosurg Pediatrics 14:68 80, 2014 AANS, 2014 Magnetic resonance imaging abnormalities in the resection region correlate with histopathological type, gliosis extent, and postoperative outcome in pediatric
Gene co-expression networks in the mouse, monkey, and human brain July 16, Jeremy Miller Scientist I
 Gene co-expression networks in the mouse, monkey, and human brain July 16, 2013 Jeremy Miller Scientist I jeremym@alleninstitute.org Outline 1. Brief introduction to previous WGCNA studies in brain 2.
Gene co-expression networks in the mouse, monkey, and human brain July 16, 2013 Jeremy Miller Scientist I jeremym@alleninstitute.org Outline 1. Brief introduction to previous WGCNA studies in brain 2.
Temporal lobe epilepsy: neuropathological and clinical correlations in 243 surgically treated patients
 Original article Epileptic Disord 2009; 11 (4): 281-92 Temporal lobe epilepsy: neuropathological and clinical correlations in 243 surgically treated patients Laura Tassi 1, Alessandra Meroni 2, Francesco
Original article Epileptic Disord 2009; 11 (4): 281-92 Temporal lobe epilepsy: neuropathological and clinical correlations in 243 surgically treated patients Laura Tassi 1, Alessandra Meroni 2, Francesco
Supplementary Figure 1
 Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Human Cortical Dysplasia and Epilepsy: An Ontogenetic Hypothesis Based on Volumetric MRI and NeuN Neuronal Density and Size Measurements
 Cerebral Cortex February 2005;15:194-210 doi:10.1093/cercor/bhh122 Advance Access publication August 5, 2004 Human Cortical Dysplasia and Epilepsy: An Ontogenetic Hypothesis Based on Volumetric MRI and
Cerebral Cortex February 2005;15:194-210 doi:10.1093/cercor/bhh122 Advance Access publication August 5, 2004 Human Cortical Dysplasia and Epilepsy: An Ontogenetic Hypothesis Based on Volumetric MRI and
Bottom-of-Sulcus Dysplasia: Imaging Features
 Neuroradiology/Head and Neck Imaging Original Research Hofman et al. ottom-of-sulcus Dysplasia Neuroradiology/Head and Neck Imaging Original Research Paul. M. Hofman 1,2,3 Gregory J. Fitt 4. Simon Harvey
Neuroradiology/Head and Neck Imaging Original Research Hofman et al. ottom-of-sulcus Dysplasia Neuroradiology/Head and Neck Imaging Original Research Paul. M. Hofman 1,2,3 Gregory J. Fitt 4. Simon Harvey
Neurodevelopment II Structure Formation. Reading: BCP Chapter 23
 Neurodevelopment II Structure Formation Reading: BCP Chapter 23 Phases of Development Ovum + Sperm = Zygote Cell division (multiplication) Neurogenesis Induction of the neural plate Neural proliferation
Neurodevelopment II Structure Formation Reading: BCP Chapter 23 Phases of Development Ovum + Sperm = Zygote Cell division (multiplication) Neurogenesis Induction of the neural plate Neural proliferation
OBSERVATION. Identifying Subtle Cortical Gyral Abnormalities as a Predictor of Focal Cortical Dysplasia and a Cure for Epilepsy
 OSERVATION Identifying Subtle Cortical Gyral Abnormalities as a Predictor of Focal Cortical Dysplasia and a Cure for Epilepsy Joel M. Oster, MD; Eme Igbokwe, MD; G. Rees Cosgrove, MD, FRCS(C); Andrew J.
OSERVATION Identifying Subtle Cortical Gyral Abnormalities as a Predictor of Focal Cortical Dysplasia and a Cure for Epilepsy Joel M. Oster, MD; Eme Igbokwe, MD; G. Rees Cosgrove, MD, FRCS(C); Andrew J.
Challenges and opportunities for understanding epilepsy and cognitive and behavioral comorbidities. Eleonora Aronica
 Biobanks and Databases -Basis for Translational Research Challenges and opportunities for understanding epilepsy and cognitive and behavioral comorbidities Eleonora Aronica Department of (Neuro)Pathology,
Biobanks and Databases -Basis for Translational Research Challenges and opportunities for understanding epilepsy and cognitive and behavioral comorbidities Eleonora Aronica Department of (Neuro)Pathology,
Int J Clin Exp Pathol 2013;6(10): /ISSN: /IJCEP Hidehiro Takei 1, Meenakshi B Bhattacharjee 2
 Int J Clin Exp Pathol 2013;6(10):2267-2271 www.ijcep.com /ISSN:1936-2625/IJCEP1307056 Case Report Encephalomalacic dysplastic mass lesion associated with vascular abnormalities in an elderly man. Is this
Int J Clin Exp Pathol 2013;6(10):2267-2271 www.ijcep.com /ISSN:1936-2625/IJCEP1307056 Case Report Encephalomalacic dysplastic mass lesion associated with vascular abnormalities in an elderly man. Is this
MALFORMATIONS OF CORTICAL DEVELOPMENT: A PICTORIAL REVIEW
 MALFORMATIONS OF CORTICAL DEVELOPMENT: A PICTORIAL REVIEW Padmaja K. Naidu, M.D. Usha D. Nagaraj, M.D. William T. O Brien, Sr., D.O. AOCR Annual Conference 2018 Scottsdale, Arizona @CincyKidsRad facebook.com/cincykidsrad
MALFORMATIONS OF CORTICAL DEVELOPMENT: A PICTORIAL REVIEW Padmaja K. Naidu, M.D. Usha D. Nagaraj, M.D. William T. O Brien, Sr., D.O. AOCR Annual Conference 2018 Scottsdale, Arizona @CincyKidsRad facebook.com/cincykidsrad
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
In 2005, Wang and coworkers 1 described a report of 8
 Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy
 Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
Neural stem cells and the neurobiology of ageing. Chen Siyun 1, Dawe G.S. 2
 ABSTRACT Neural stem cells and the neurobiology of ageing Chen Siyun 1, Dawe G.S. 2 Department of Physics, Faculty of Science, National University of Singapore 10 Kent Ridge Road, Singapore 117546 The
ABSTRACT Neural stem cells and the neurobiology of ageing Chen Siyun 1, Dawe G.S. 2 Department of Physics, Faculty of Science, National University of Singapore 10 Kent Ridge Road, Singapore 117546 The
OSVZ progenitors of human and ferret neocortex are epithelial-like and
 OSVZ progenitors of human and ferret neocortex are epithelial-like and expand by integrin signaling Simone A Fietz, Iva Kelava, Johannes Vogt, Michaela Wilsch-Bräuninger, Denise Stenzel, Jennifer L Fish,
OSVZ progenitors of human and ferret neocortex are epithelial-like and expand by integrin signaling Simone A Fietz, Iva Kelava, Johannes Vogt, Michaela Wilsch-Bräuninger, Denise Stenzel, Jennifer L Fish,
Fetal CNS MRI. Daniela Prayer. Division of Neuroradiology And Musculoskeletal Radiology. Medical University of Vienna, AUSTRIA
 Fetal CNS MRI Daniela Prayer Division of Neuroradiology And Musculoskeletal Radiology Medical University of Vienna, AUSTRIA Methods Normal development Malformations Acquired pathology MR- methods for assessment
Fetal CNS MRI Daniela Prayer Division of Neuroradiology And Musculoskeletal Radiology Medical University of Vienna, AUSTRIA Methods Normal development Malformations Acquired pathology MR- methods for assessment
doi: /brain/awr204 Brain 2011: 134; Morphometric MRI analysis improves detection of focal cortical dysplasia type II
 doi:10.1093/brain/awr204 Brain 2011: 134; 2844 2854 2844 BRAIN A JOURNAL OF NEUROLOGY Morphometric MRI analysis improves detection of focal cortical dysplasia type II Jan Wagner, 1,2 Bernd Weber, 1,2,3
doi:10.1093/brain/awr204 Brain 2011: 134; 2844 2854 2844 BRAIN A JOURNAL OF NEUROLOGY Morphometric MRI analysis improves detection of focal cortical dysplasia type II Jan Wagner, 1,2 Bernd Weber, 1,2,3
PRESURGICAL EVALUATION. ISLAND OF COS Hippocrates: On the Sacred Disease. Disclosure Research-Educational Grants. Patients with seizure disorders
 PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
Supplementary Information
 Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
Imaging of Pediatric Epilepsy MRI. Epilepsy: Nonacute Situation
 Imaging of Pediatric Epilepsy Epilepsy: Nonacute Situation MR is the study of choice Tailor MR study to suspected epileptogenic zone Temporal lobe Extratemporal A. James Barkovich, MD University of California
Imaging of Pediatric Epilepsy Epilepsy: Nonacute Situation MR is the study of choice Tailor MR study to suspected epileptogenic zone Temporal lobe Extratemporal A. James Barkovich, MD University of California
Neuroimaging in identifying focal cortical dysplasia and prognostic factors in pediatric and adolescent epilepsy surgery
 FULL-LENGTH ORIGINAL RESEARCH Neuroimaging in identifying focal cortical dysplasia and prognostic factors in pediatric and adolescent epilepsy surgery *Yoon Hee Kim, *Hoon-Chul Kang, ydong-seok Kim, zse
FULL-LENGTH ORIGINAL RESEARCH Neuroimaging in identifying focal cortical dysplasia and prognostic factors in pediatric and adolescent epilepsy surgery *Yoon Hee Kim, *Hoon-Chul Kang, ydong-seok Kim, zse
Molecular alterations in epilepsy-associated malformations of cortical development Boer, K.
 UvA-DARE (Digital Academic Repository) Molecular alterations in epilepsy-associated malformations of cortical development Boer, K. Link to publication Citation for published version (APA): Boer, K. (009).
UvA-DARE (Digital Academic Repository) Molecular alterations in epilepsy-associated malformations of cortical development Boer, K. Link to publication Citation for published version (APA): Boer, K. (009).
Prss56, a novel marker of adult neurogenesis in the mouse brain. - Supplemental Figures 1 to 5- Brain Structure and Function
 Prss56, a novel marker of adult neurogenesis in the mouse brain - Supplemental Figures 1 to 5- Brain Structure and Function Alexandre Jourdon 1,2, Aurélie Gresset 1, Nathalie Spassky 1, Patrick Charnay
Prss56, a novel marker of adult neurogenesis in the mouse brain - Supplemental Figures 1 to 5- Brain Structure and Function Alexandre Jourdon 1,2, Aurélie Gresset 1, Nathalie Spassky 1, Patrick Charnay
Plasticity of Cerebral Cortex in Development
 Plasticity of Cerebral Cortex in Development Jessica R. Newton and Mriganka Sur Department of Brain & Cognitive Sciences Picower Center for Learning & Memory Massachusetts Institute of Technology Cambridge,
Plasticity of Cerebral Cortex in Development Jessica R. Newton and Mriganka Sur Department of Brain & Cognitive Sciences Picower Center for Learning & Memory Massachusetts Institute of Technology Cambridge,
Electrocorticographic Discharge Patterns in Glioneuronal Tumours and Focal Cortical Dysplasia
 Electrocorticographic Discharge Patterns in Glioneuronal Tumours and Focal Cortical Dysplasia C.H. Ferrier E. Aronica F.S.S. Leijten W.G.M. Spliet A.C. van Huffelen P.C. van Rijen C.D. Binnie Epilepsia
Electrocorticographic Discharge Patterns in Glioneuronal Tumours and Focal Cortical Dysplasia C.H. Ferrier E. Aronica F.S.S. Leijten W.G.M. Spliet A.C. van Huffelen P.C. van Rijen C.D. Binnie Epilepsia
A new subtype of progenitor cell in the mouse embryonic neocortex. Xiaoqun Wang, Jin-Wu Tsai, Bridget LaMonica & Arnold R.
 A new subtype of progenitor cell in the mouse embryonic neocortex Xiaoqun Wang, Jin-Wu Tsai, Bridget LaMonica & Arnold R. Kriegstein Supplementary Figures 1-6: Supplementary Movies 1-9: Supplementary
A new subtype of progenitor cell in the mouse embryonic neocortex Xiaoqun Wang, Jin-Wu Tsai, Bridget LaMonica & Arnold R. Kriegstein Supplementary Figures 1-6: Supplementary Movies 1-9: Supplementary
Hamartomas and epilepsy: clinical and imaging characteristics
 Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012
 Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
Relevance of Residual Histologic and Electrocorticographic Abnormalities for Surgical Outcome in Frontal Lobe Epilepsy
 Relevance of Residual Histologic and Electrocorticographic Abnormalities for Surgical Outcome in Frontal Lobe Epilepsy C.H. Ferrier G. Alarcón J. Engelsman C.D. Binnie M. Koutroumanidis C.E. Polkey I.
Relevance of Residual Histologic and Electrocorticographic Abnormalities for Surgical Outcome in Frontal Lobe Epilepsy C.H. Ferrier G. Alarcón J. Engelsman C.D. Binnie M. Koutroumanidis C.E. Polkey I.
Early-onset symptomatic focal epilepsy: a dilemma in the timing of surgery
 Anatomo-electro-clinical correlations Epileptic Disord 2008; 10 (4): 356-61 Anatomo-electro-clinical correlations: the Great Ormond Street Hospital, UK Case Report - Case 05-2008 Early-onset symptomatic
Anatomo-electro-clinical correlations Epileptic Disord 2008; 10 (4): 356-61 Anatomo-electro-clinical correlations: the Great Ormond Street Hospital, UK Case Report - Case 05-2008 Early-onset symptomatic
A quantitative study of white matter hypomyelination and oligodendroglial maturation in focal cortical dysplasia type II
 FULL-LENGTH ORIGINAL RESEARCH A quantitative study of white matter hypomyelination and oligodendroglial maturation in focal cortical dysplasia type II *Caterina Shepherd, *Joan Liu, *Joanna Goc, *Lillian
FULL-LENGTH ORIGINAL RESEARCH A quantitative study of white matter hypomyelination and oligodendroglial maturation in focal cortical dysplasia type II *Caterina Shepherd, *Joan Liu, *Joanna Goc, *Lillian
Pathological assessment of epilepsy surgery brain tissue
 pathologica 2016;108:80-86 Original article Pathological assessment of epilepsy surgery brain tissue G. Marucci 1, M. Giulioni 2 1 Section of Pathology, Bellaria Hospital, Azienda USL IRCCS-ISNB Institute
pathologica 2016;108:80-86 Original article Pathological assessment of epilepsy surgery brain tissue G. Marucci 1, M. Giulioni 2 1 Section of Pathology, Bellaria Hospital, Azienda USL IRCCS-ISNB Institute
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective
 Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Supplementary Figure S1: Tanycytes are restricted to the central/posterior hypothalamus
 Supplementary Figure S1: Tanycytes are restricted to the central/posterior hypothalamus a: Expression of Vimentin, GFAP, Sox2 and Nestin in anterior, central and posterior hypothalamus. In the anterior
Supplementary Figure S1: Tanycytes are restricted to the central/posterior hypothalamus a: Expression of Vimentin, GFAP, Sox2 and Nestin in anterior, central and posterior hypothalamus. In the anterior
doi: /brain/aws149 Brain 2012: 135;
 doi:10.1093/brain/aws149 Brain 2012: 135; 2337 2349 2337 BRAIN A JOURNAL OF NEUROLOGY Blurring in patients with temporal lobe epilepsy: clinical, high-field imaging and ultrastructural study Rita Garbelli,
doi:10.1093/brain/aws149 Brain 2012: 135; 2337 2349 2337 BRAIN A JOURNAL OF NEUROLOGY Blurring in patients with temporal lobe epilepsy: clinical, high-field imaging and ultrastructural study Rita Garbelli,
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 AWARD NUMBER: W81XWH-15-1-0112 TITLE: Molecular Mechanisms Underlying the Epileptogenesis and Seizure Progression in Tuberous Sclerosis Complex 1 Deficient Mouse Models PRINCIPAL INVESTIGATOR: James E.
AWARD NUMBER: W81XWH-15-1-0112 TITLE: Molecular Mechanisms Underlying the Epileptogenesis and Seizure Progression in Tuberous Sclerosis Complex 1 Deficient Mouse Models PRINCIPAL INVESTIGATOR: James E.
Intracranial Studies Of Human Epilepsy In A Surgical Setting
 Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Postmortem MR imaging has been used to evaluate the fetal
 ORIGINAL RESEARCH E. Widjaja S. Geibprasert S. Zarei Mahmoodabadi N.E. Brown P. Shannon Corroboration of Normal and Abnormal Fetal Cerebral Lamination on Postmortem MR Imaging with Postmortem Examination
ORIGINAL RESEARCH E. Widjaja S. Geibprasert S. Zarei Mahmoodabadi N.E. Brown P. Shannon Corroboration of Normal and Abnormal Fetal Cerebral Lamination on Postmortem MR Imaging with Postmortem Examination
Supplemental Figure 1. Intracranial transduction of a modified ptomo lentiviral vector in the mouse
 Supplemental figure legends Supplemental Figure 1. Intracranial transduction of a modified ptomo lentiviral vector in the mouse hippocampus targets GFAP-positive but not NeuN-positive cells. (A) Stereotaxic
Supplemental figure legends Supplemental Figure 1. Intracranial transduction of a modified ptomo lentiviral vector in the mouse hippocampus targets GFAP-positive but not NeuN-positive cells. (A) Stereotaxic
No relevant disclosures
 No relevant disclosures - Epileptic Encephalopathy (EE): Epileptic activity itself contributes to cognitive and behavioural impairments - Developmental and Epileptic Encephalopathy (DEE): Impairments occur
No relevant disclosures - Epileptic Encephalopathy (EE): Epileptic activity itself contributes to cognitive and behavioural impairments - Developmental and Epileptic Encephalopathy (DEE): Impairments occur
Clinical features of a series of non-surgical patients with focal cortical dysplasia and epilepsy
 American Journal of Psychiatry and Neuroscience 2014; 2(1): 8-12 Published online January 30, 2014 (http://www.sciencepublishinggroup.com/j/ajpn) doi: 10.11648/j.ajpn.20140201.12 Clinical features of a
American Journal of Psychiatry and Neuroscience 2014; 2(1): 8-12 Published online January 30, 2014 (http://www.sciencepublishinggroup.com/j/ajpn) doi: 10.11648/j.ajpn.20140201.12 Clinical features of a
Imaging of malformations of cortical development
 Review article Epileptic Disord 2009; 11 (3): 194-205 Imaging of malformations of cortical development Nadia Colombo 1, Noriko Salamon 2, Charles Raybaud 3, Çigdem Özkara 4, A. James Barkovich 5 1 Department
Review article Epileptic Disord 2009; 11 (3): 194-205 Imaging of malformations of cortical development Nadia Colombo 1, Noriko Salamon 2, Charles Raybaud 3, Çigdem Özkara 4, A. James Barkovich 5 1 Department
Malformations of cortical development. Clinical and imaging findings.
 Malformations of cortical development. Clinical and imaging findings. Poster No.: C-2086 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Alba de Caceres, B. García-Castaño, L. Ibañez, E. Roa,
Malformations of cortical development. Clinical and imaging findings. Poster No.: C-2086 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Alba de Caceres, B. García-Castaño, L. Ibañez, E. Roa,
Refractory focal epilepsy: findings by MRI.
 Refractory focal epilepsy: findings by MRI. Doctors Nicolás Sgarbi, Osmar Telis Clinical Radiology Department Hospital de Clínicas Montevideo- Uruguay ABSTRACT Epilepsy is one of the most frequent neurological
Refractory focal epilepsy: findings by MRI. Doctors Nicolás Sgarbi, Osmar Telis Clinical Radiology Department Hospital de Clínicas Montevideo- Uruguay ABSTRACT Epilepsy is one of the most frequent neurological
Malformations of cortical development. Clinical and imaging findings.
 Malformations of cortical development. Clinical and imaging findings. Poster No.: C-2086 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Alba de Caceres, B. García-Castaño, L. Ibañez, E. Roa 1
Malformations of cortical development. Clinical and imaging findings. Poster No.: C-2086 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Alba de Caceres, B. García-Castaño, L. Ibañez, E. Roa 1
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity
 Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
Advanced MR Imaging of Cortical Dysplasia with or without Neoplasm: A Report of Two Cases
 AJNR Am J Neuroradiol 23:1686 1691, November/December 2002 Case Report Advanced MR Imaging of Cortical Dysplasia with or without Neoplasm: A Report of Two Cases Jay J. Pillai, Richard B. Hessler, Jerry
AJNR Am J Neuroradiol 23:1686 1691, November/December 2002 Case Report Advanced MR Imaging of Cortical Dysplasia with or without Neoplasm: A Report of Two Cases Jay J. Pillai, Richard B. Hessler, Jerry
Advanced magnetic resonance imaging for monitoring brain development and injury
 Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Expression of tuberin and hamartin in tuberous sclerosis complex-associated and sporadic cortical dysplasia of Taylor's balloon cell type
 Original article Expression of tuberin and hamartin in tuberous sclerosis complex-associated and sporadic cortical dysplasia of Taylor's balloon cell type Wiesława Grajkowska 1, Katarzyna Kotulska 2, 3,
Original article Expression of tuberin and hamartin in tuberous sclerosis complex-associated and sporadic cortical dysplasia of Taylor's balloon cell type Wiesława Grajkowska 1, Katarzyna Kotulska 2, 3,
Supplemental Information. Induction of Expansion and Folding. in Human Cerebral Organoids
 Cell Stem Cell, Volume 20 Supplemental Information Induction of Expansion and Folding in Human Cerebral Organoids Yun Li, Julien Muffat, Attya Omer, Irene Bosch, Madeline A. Lancaster, Mriganka Sur, Lee
Cell Stem Cell, Volume 20 Supplemental Information Induction of Expansion and Folding in Human Cerebral Organoids Yun Li, Julien Muffat, Attya Omer, Irene Bosch, Madeline A. Lancaster, Mriganka Sur, Lee
The Changing Surgical Landscape in Kids
 The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
Brain Structure and Epilepsy: The Impact of Modern Imaging
 Commentary Brain Structure and Epilepsy: The Impact of Modern Imaging Frederick Andermann, Professor of Neurology and Paediatrics, Department of Neurology and Neurosurgery, McGill University, Montreal,
Commentary Brain Structure and Epilepsy: The Impact of Modern Imaging Frederick Andermann, Professor of Neurology and Paediatrics, Department of Neurology and Neurosurgery, McGill University, Montreal,
Supplementary Figure 1. Nature Neuroscience: doi: /nn.4547
 Supplementary Figure 1 Characterization of the Microfetti mouse model. (a) Gating strategy for 8-color flow analysis of peripheral Ly-6C + monocytes from Microfetti mice 5-7 days after TAM treatment. Living
Supplementary Figure 1 Characterization of the Microfetti mouse model. (a) Gating strategy for 8-color flow analysis of peripheral Ly-6C + monocytes from Microfetti mice 5-7 days after TAM treatment. Living
Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1.
 Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1. Youngsoo Lee, Sachin Katyal, Yang Li, Sherif F. El-Khamisy, Helen R. Russell, Keith W. Caldecott and Peter J. McKinnon.
Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1. Youngsoo Lee, Sachin Katyal, Yang Li, Sherif F. El-Khamisy, Helen R. Russell, Keith W. Caldecott and Peter J. McKinnon.
CASE OF THE WEEK PROFESSOR YASSER METWALLY
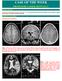 CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
Terminology. Terminology. Terminology. Terminology. Terminology. Bromodeoxyuridine
 Kateřina Náměstková, Zuzana Šimonová, Eva Syková Behavioural Brain Research Bromodeoxyuridine : Doublecortin : DCX Glial Fibrillary Acidic Protein : GFAP Trace eye blink conditioning 1 Volume 163 : pp.
Kateřina Náměstková, Zuzana Šimonová, Eva Syková Behavioural Brain Research Bromodeoxyuridine : Doublecortin : DCX Glial Fibrillary Acidic Protein : GFAP Trace eye blink conditioning 1 Volume 163 : pp.
Functional Development of Neuronal Networks in Culture -An in vitro Assay System of Developing Brain for Endocrine Disruptors
 Functional Development of Neuronal Networks in Culture -An in vitro Assay System of Developing Brain for Endocrine Disruptors Masahiro Kawahara and Yoichiro Kuroda Tokyo Metropolitan Institute for Neuroscience
Functional Development of Neuronal Networks in Culture -An in vitro Assay System of Developing Brain for Endocrine Disruptors Masahiro Kawahara and Yoichiro Kuroda Tokyo Metropolitan Institute for Neuroscience
Taylor-type focal cortical dysplasia: is the epilepsy always resistant to medical treatment?
 Case report Epileptic Disord 2006; 8 (4): 289-93 Taylor-type focal cortical dysplasia: is the epilepsy always resistant to medical treatment? Ennio Del Giudice 1, Maria Cristina Bianchi 2, Michela Tosetti
Case report Epileptic Disord 2006; 8 (4): 289-93 Taylor-type focal cortical dysplasia: is the epilepsy always resistant to medical treatment? Ennio Del Giudice 1, Maria Cristina Bianchi 2, Michela Tosetti
mr brain volume analysis using brain assist
 mr brain volume analysis using brain assist This Paper describes the tool named BrainAssist, which can be used for the study and analysis of brain abnormalities like Focal Cortical Dysplasia (FCD), Heterotopia
mr brain volume analysis using brain assist This Paper describes the tool named BrainAssist, which can be used for the study and analysis of brain abnormalities like Focal Cortical Dysplasia (FCD), Heterotopia
Downregulation of CD47 and CD200 in patients with focal cortical dysplasia type IIb and tuberous sclerosis complex
 Sun et al. Journal of Neuroinflammation (2016) 13:85 DOI 10.1186/s12974-016-0546-2 RESEARCH Open Access Downregulation of CD47 and CD200 in patients with focal cortical dysplasia type IIb and tuberous
Sun et al. Journal of Neuroinflammation (2016) 13:85 DOI 10.1186/s12974-016-0546-2 RESEARCH Open Access Downregulation of CD47 and CD200 in patients with focal cortical dysplasia type IIb and tuberous
The Role of Brain Inflammation in Epileptogenesis in TSC. CONTRACTING ORGANIZATION: Washington University School of Medicine St Louis, M
 AD Award Number: W81XWH-12-1-0190 TITLE: The Role of Brain Inflammation in Epileptogenesis in TSC PRINCIPAL INVESTIGATOR: Michael Wong CONTRACTING ORGANIZATION: Washington University School of Medicine
AD Award Number: W81XWH-12-1-0190 TITLE: The Role of Brain Inflammation in Epileptogenesis in TSC PRINCIPAL INVESTIGATOR: Michael Wong CONTRACTING ORGANIZATION: Washington University School of Medicine
Journal of Child Neurology
 Journal of Child Neurology http://jcn.sagepub.com/ Perfusion Imaging of Focal Cortical Dysplasia Using Arterial Spin Labeling: Correlation With Histopathological Vascular Density Pia Wintermark, Mirna
Journal of Child Neurology http://jcn.sagepub.com/ Perfusion Imaging of Focal Cortical Dysplasia Using Arterial Spin Labeling: Correlation With Histopathological Vascular Density Pia Wintermark, Mirna
Amyotrophic lateral sclerosis (ALS) is a progressive neurodegenerative
 ORIGINAL RESEARCH E. Matsusue S. Sugihara S. Fujii T. Kinoshita T. Nakano E. Ohama T. Ogawa Cerebral Cortical and White Matter Lesions in Amyotrophic Lateral Sclerosis with Dementia: Correlation with MR
ORIGINAL RESEARCH E. Matsusue S. Sugihara S. Fujii T. Kinoshita T. Nakano E. Ohama T. Ogawa Cerebral Cortical and White Matter Lesions in Amyotrophic Lateral Sclerosis with Dementia: Correlation with MR
Ahtiainen et al., http :// /cgi /content /full /jcb /DC1
 Supplemental material JCB Ahtiainen et al., http ://www.jcb.org /cgi /content /full /jcb.201512074 /DC1 THE JOURNAL OF CELL BIOLOGY Figure S1. Distinct distribution of different cell cycle phases in the
Supplemental material JCB Ahtiainen et al., http ://www.jcb.org /cgi /content /full /jcb.201512074 /DC1 THE JOURNAL OF CELL BIOLOGY Figure S1. Distinct distribution of different cell cycle phases in the
Accepted Manuscript. Editorial. Responsive neurostimulation for epilepsy: more than stimulation. Jayant N. Acharya
 Accepted Manuscript Editorial Responsive neurostimulation for epilepsy: more than stimulation Jayant N. Acharya PII: S2467-981X(18)30022-2 DOI: https://doi.org/10.1016/j.cnp.2018.06.002 Reference: CNP
Accepted Manuscript Editorial Responsive neurostimulation for epilepsy: more than stimulation Jayant N. Acharya PII: S2467-981X(18)30022-2 DOI: https://doi.org/10.1016/j.cnp.2018.06.002 Reference: CNP
Big brains may hold clues to origins of autism
 VIEWPOINT Big brains may hold clues to origins of autism BY KONSTANTINOS ZARBALIS 23 FEBRUARY 2016 A persistent challenge to improving our understanding of autism is the fact that no single neurological
VIEWPOINT Big brains may hold clues to origins of autism BY KONSTANTINOS ZARBALIS 23 FEBRUARY 2016 A persistent challenge to improving our understanding of autism is the fact that no single neurological
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Cerebral Cortex 1. Sarah Heilbronner
 Cerebral Cortex 1 Sarah Heilbronner heilb028@umn.edu Want to meet? Coffee hour 10-11am Tuesday 11/27 Surdyk s Overview and organization of the cerebral cortex What is the cerebral cortex? Where is each
Cerebral Cortex 1 Sarah Heilbronner heilb028@umn.edu Want to meet? Coffee hour 10-11am Tuesday 11/27 Surdyk s Overview and organization of the cerebral cortex What is the cerebral cortex? Where is each
Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication
 Original article Epileptic Disord 2008; 10 (4): 260-5 Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication Naotaka Usui, Tadahiro Mihara, Koichi
Original article Epileptic Disord 2008; 10 (4): 260-5 Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication Naotaka Usui, Tadahiro Mihara, Koichi
Epilepsy affects more than 50 million people worldwide. FOCUS Neurosurg Focus 45 (3):E5, 2018
 NEUROSURGICAL FOCUS Neurosurg Focus 45 (3):E5, 2018 Ultrasonographic features of focal cortical dysplasia and their relevance for epilepsy surgery Kevin Akeret, MD, 1 David Bellut, MD, 1 Hans-Jürgen Huppertz,
NEUROSURGICAL FOCUS Neurosurg Focus 45 (3):E5, 2018 Ultrasonographic features of focal cortical dysplasia and their relevance for epilepsy surgery Kevin Akeret, MD, 1 David Bellut, MD, 1 Hans-Jürgen Huppertz,
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES. Mr. Johnson. Seizures at 29 Years of Age. Dileep Nair, MD Juan Bulacio, MD
 Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
8 th International Summer School for Neuropathology and Epilepsy Surgery INES July 26-29, 2018 University Hospital, Erlangen Krankenhausstr.
 8 th International Summer School for Neuropathology and Epilepsy Surgery INES 2018 July 26-29, 2018 University Hospital, Erlangen Krankenhausstr. 12 Course Directors: For more information, please contact:
8 th International Summer School for Neuropathology and Epilepsy Surgery INES 2018 July 26-29, 2018 University Hospital, Erlangen Krankenhausstr. 12 Course Directors: For more information, please contact:
USCAP Neuropathology. Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC
 USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Broad Integration of Expression Maps and Co-Expression Networks Compassing Novel Gene Functions in the Brain
 Supplementary Information Broad Integration of Expression Maps and Co-Expression Networks Compassing Novel Gene Functions in the Brain Yuko Okamura-Oho a, b, *, Kazuro Shimokawa c, Masaomi Nishimura b,
Supplementary Information Broad Integration of Expression Maps and Co-Expression Networks Compassing Novel Gene Functions in the Brain Yuko Okamura-Oho a, b, *, Kazuro Shimokawa c, Masaomi Nishimura b,
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT. Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018
 EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
FIU Digital Commons. Florida International University. Brenda Luna Florida International University,
 Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 7-13-2011 Prenatal Environmental Exposure and Neurodevelopmentally Important Gene
Florida International University FIU Digital Commons FIU Electronic Theses and Dissertations University Graduate School 7-13-2011 Prenatal Environmental Exposure and Neurodevelopmentally Important Gene
Discrete domains of gene expression in germinal layers distinguish the development of gyrencephaly
 Manuscript EMBO-2015-91176 Discrete domains of gene expression in germinal layers distinguish the development of gyrencephaly Camino De Juan Romero, Carl Bruder, Ugo Tomasello, Jose Miguel Sanz-Anquela
Manuscript EMBO-2015-91176 Discrete domains of gene expression in germinal layers distinguish the development of gyrencephaly Camino De Juan Romero, Carl Bruder, Ugo Tomasello, Jose Miguel Sanz-Anquela
The relevance of somatosensory auras in refractory temporal lobe epilepsies
 BRIEF COMMUNICATION The relevance of somatosensory auras in refractory temporal lobe epilepsies Ghazala Perven, Ruta Yardi, Juan Bulacio, Imad Najm, William Bingaman, Jorge Gonzalez-Martinez, and Lara
BRIEF COMMUNICATION The relevance of somatosensory auras in refractory temporal lobe epilepsies Ghazala Perven, Ruta Yardi, Juan Bulacio, Imad Najm, William Bingaman, Jorge Gonzalez-Martinez, and Lara
Genetics and Hydrocephalus
 Genetics and Hydrocephalus James P. (Pat) McAllister II, PhD 1,2,4 1 Pediatric Neurosurgery, Primary Children s Medical Center & University of Utah, Salt Lake City, UT 2 Bioengineering and 3 Physiology,
Genetics and Hydrocephalus James P. (Pat) McAllister II, PhD 1,2,4 1 Pediatric Neurosurgery, Primary Children s Medical Center & University of Utah, Salt Lake City, UT 2 Bioengineering and 3 Physiology,
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
