2005 PRETEXT: a revised staging system for primary malignant liver tumours of childhood developed by the SIOPEL group
|
|
|
- Lawrence Robertson
- 6 years ago
- Views:
Transcription
1 Pediatr Radiol (2007) 37: DOI /s REVIEW 2005 PRETEXT: a revised staging system for primary malignant liver tumours of childhood developed by the SIOPEL group Derek J. Roebuck & Daniel Aronson & Philippe Clapuyt & Piotr Czauderna & Jean de Ville de Goyet & Frédéric Gauthier & Gordon MacKinlay & Rudolf Maibach & Kieran McHugh & Øystein E. Olsen & Jean-Bernard Otte & Danièle Pariente & Jack Plaschkes & Margaret Childs & Giorgio Perilongo Received: 16 September 2006 / Accepted: 29 October 2006 / Published online: 21 December 2006 # Springer-Verlag 2006 Abstract Over the last 15 years, various oncology groups throughout the world have used the PRETEXT system for staging malignant primary liver tumours of childhood. This paper, written by members of the radiology and surgery committees of the International Childhood Liver Tumor Strategy Group (SIOPEL), presents various clarifications and revisions to the original PRETEXT system. Keywords Liver. Tumour. Hepatoblastoma. Staging. Children D. J. Roebuck (*) : K. McHugh : Ø. E. Olsen Department of Radiology, Great Ormond Street Hospital, London WC1N 3JH, UK roebud@gosh.nhs.uk D. Aronson Academisch Medisch Centrum/Universiteit van Amsterdam, locatie Emma Kinderziekenhuis AMC, Amsterdam, The Netherlands P. Clapuyt : J. de Ville de Goyet : J.-B. Otte Departments of Surgery and Medical Imaging, Université Catholique de Louvain, Cliniques Universitaires Saint-Luc, Brussels, Belgium P. Czauderna Department of Pediatric Surgery, Medical University of Gdansk, Gdansk, Poland F. Gauthier : D. Pariente Centre Hospital-Universitaire de Bicêtre APHP, Le Kremlin-Bicêtre cedex, France Introduction The PRETEXT system was designed by the International Childhood Liver Tumor Strategy Group (SIOPEL) for staging and risk stratification of liver tumours [1, 2]. PRETEXT is used to describe tumour extent before any therapy, thus allowing more effective comparison between studies conducted by different groups. The system has good interobserver reproducibility [3] and good prognostic value in children with hepatoblastoma [2 5], and is the basis of risk stratification in current SIOPEL hepatoblastoma studies. Most other study groups now use the PRETEXT system G. MacKinlay Department of Surgery, Royal Hospital for Sick Children, Edinburgh, UK R. Maibach SIAK Coordinating Center, Bern, Switzerland J. Plaschkes Department of Pediatric Surgery, Inselspital, Bern, Switzerland M. Childs United Kingdom Children s Cancer Study Group, Leicester, UK G. Perilongo Division of Hematology/Oncology, Department of Pediatrics, Padua University Hospital, Padua, Italy
2 124 Pediatr Radiol (2007) 37: Fig. 1 Schematic representations of the segmental anatomy of the liver. a Frontal view of the liver. The numerals label Couinaud s segments 2to8. b The hepatic veins (black) and the intrahepatic branches of the portal veins (grey) are shown. Segment 1 (equivalent to the caudate lobe) is seen to lie between the portal vein and the inferior vena cava. c Exploded frontal view of the segmental anatomy of the liver. The umbilical portion of the left portal vein (LPV) separates the left medial section from the left lateral section (LLS). Segment 1 is obscured in this view. Note that the term section has been used in preference to segment or sector (see text). d Transverse section of the liver shows the planes of the major venous structures used to determine the PRETEXT number. The hepatic (blue) and portal (purple) veins define the sections of the liver (2 8). This schematic diagram shows how the right hepatic (RHV) and middle hepatic (MHV) veins indicate the borders of the right anterior section (RAS) with the right posterior (RPS) and left medial (LMS) sections. Note that the left portal vein (LPV) actually lies caudal to the confluence of the hepatic veins and is not seen in the same transverse image. The left hepatic vein (LHV) runs between segments 2 and 3 and is not used in PRETEXT staging to describe imaging findings at diagnosis, even if this is not their main staging system. Certain limitations of the system have become obvious over the last 15 years. In addition, there have been significant advances in imaging during this period [6]. This paper is the report of a working party that met in June 2005 to update the PRETEXT system. PRETEXT staging is based on Couinaud s system of segmentation of the liver (Fig. 1) [7]. The liver segments are grouped into four sections as follows: segments 2 and 3 (left lateral section), segments 4a and 4b (left medial section), segments 5 and 8 (right anterior section) and segments 6 and 7 (right posterior section). The term section is used (where other authors use segment or sector) to avoid terminological confusion. In the original system, the caudate lobe (segment 1) was ignored. The PRETEXT number was derived by subtracting the highest number of contiguous liver sections that Table 1 Definitions of PRETEXT number (see text for PRETEXT number of tumours involving the caudate lobe) PRETEXT number I II III IV Definition One section is involved and three adjoining sections are free One or two sections are involved, but two adjoining sections are free Two or three sections are involved, and no two adjoining sections are free All four sections are involved
3 Pediatr Radiol (2007) 37: Table PRETEXT staging: additional criteria Caudate lobe involvement C C1 Tumour involving the caudate lobe All C1 patients are at C0 All other patients least PRETEXT II Extrahepatic abdominal disease E E0 No evidence of tumour spread in the abdomen (except MorN) Add suffix a if ascites is present, e.g., E0a E1 Direct extension of tumour into adjacent organs or diaphragm E2 Peritoneal nodules Tumour focality F F0 Patient with solitary tumour F1 Patient with two or more discrete tumours Tumour rupture or intraperitoneal haemorrhage H H1 Imaging and clinical findings of intraperitoneal haemorrhage H0 All other patients Distant metastases M M0 No metastases Add suffix or suffixes to M1 Any metastasis (except E and N) indicate location (see text) Lymph node metastases N N0 No nodal metastases N1 Abdominal lymph node metastases only N2 Extra-abdominal lymph node metastases (with or without abdominal lymph node metastases) Portal vein involvement P P0 P1 No involvement of the portal vein or its left or right branches Involvement of either the left or the right branch of the portal vein See text for definition of involvement. Add suffix a if intravascular tumour is present, e.g., P1a P2 Involvement of the main portal vein Involvement of the IVC and/ or hepatic veins V V0 V1 No involvement of the hepatic veins or inferior vena cava (IVC) Involvement of one hepatic vein but not the IVC See text for definition of involvement. Add suffix a if intravascular tumour is present, V2 Involvement of two hepatic veins but not the IVC e.g., V3a V3 Involvement of all three hepatic veins and/or the IVC were not involved by tumour from four [1]. This number is, very roughly, an estimate of the difficulty of the expected surgical procedure (Table 1). Pedunculated tumours are considered to be confined to the liver and to occupy only the section(s) from which they originate. In addition to describing the intrahepatic extent of the primary tumour(s), the PRETEXT system includes certain other criteria. These assess involvement of the inferior vena cava (IVC) or hepatic veins (designated V), involvement of the portal veins (P), extrahepatic abdominal disease (E) and distant metastases (M). The purpose of the 2005 revision was to improve the original definitions of the PRETEXT stages, to clarify the criteria for extrahepatic disease, and to add new criteria (Table 2). The term extrahepatic disease is confusing, and these categories will in future be called additional criteria. There is still much to be learned about prognostic factors in the primary malignant liver tumours of childhood. An important goal of these changes, therefore, is to improve our ability to identify prognostic imaging findings, and thereby refine risk stratification. Although the PRETEXT system is principally used for hepatoblastoma, the 2005 revision is intended to be applicable to all primary malignant liver tumours of childhood, including hepatocellular carcinoma and epithelioid haemangioendothelioma. The original SIOPEL risk stratification system for hepatoblastoma has already been modified in the protocols for current SIOPEL studies (Table 3). Firstly, tumour rupture or intraperitoneal haemorrhage at the time of diagnosis (H1, see below) is now a defining criterion of high risk. Secondly, children with alphafetoprotein levels of <100 μg/l are also considered to be high risk. The 2005 revision involves no further change in the SIOPEL risk stratification system for hepatoblastoma. Table 3 Risk stratification in hepatoblastoma for current SIOPEL studies High risk Patients with any of the following: Serum alpha-fetoprotein <100 μg/l PRETEXT IV Additional PRETEXT criteria: E1, E1a, E2, E2a H1 M1 (any site) N1, N2 P2, P2a V3, V3a Standard risk All other patients
4 126 Pediatr Radiol (2007) 37: Fig. 2 PRETEXT I. a The left lateral section (segments 2 and 3) is involved. b The right posterior section (segments 6 and 7) is involved PRETEXT grouping The traditional approach to radiological segmentation of the liver, based on the paths of the hepatic veins, is an oversimplification. This is partly due to the variability of hepatic venous anatomy [8 10]. The main problem, however, is the imperfect correlation with segments defined by the branching pattern of the portal veins [8, 11 13]. Although the plane of the right hepatic vein reliably separates the right posterior and anterior sections [9], the left hepatic vein runs to the left of the boundary between the left lateral and medial sections, which is best defined by the plane of the fissure of the ligamentum teres and the umbilical portion of the left portal vein (Fig. 1) [14]. Fig. 3 PRETEXT II. a Tumour involving only the right lobe of the liver. b A transverse T1-weighted MR image of a child with hepatoblastoma shows that the middle hepatic vein (arrow) is displaced but not involved by the tumour. This is the most common type of PRETEXT II tumour. c Tumour involving only the left lobe of the liver. d Tumour involving only the left medial section. e Tumour involving only the right anterior section. f Multifocal tumours involving only the left lateral and right posterior sections. g The tumour is confined to the caudate lobe (PRETEXT II C1, see text; RPV right portal vein)
5 Pediatr Radiol (2007) 37: PRETEXT I This group includes only a small proportion of primary malignant liver tumours of childhood. From the definition of the PRETEXT number, it can be seen that only tumours localized to either the left lateral section or the right posterior section qualify as PRETEXT I (Fig. 2). PRETEXT II Most PRETEXT II tumours are limited to either the right lobe or the left lobe of the liver. Tumours of the left medial or right anterior sections are also PRETEXT II. Multifocal tumours involving only the left lateral and right posterior sections are classified as PRETEXT II; this pattern is very rare. Tumours limited to the caudate lobe were not classifiable under the original PRETEXT system [1]. In the 2005 PRETEXT system these tumours are classified as PRETEXT II (but see also C, below). This is the only change in the PRETEXT numbering system in this revision. There is no change in numbering for tumours involving the caudate lobe and any other part of the liver, which are classified as PRETEXT II (if two or three contiguous sections are free), III (if there are no two contiguous sections free) or IV (if all four sections are involved) (Fig. 3). PRETEXT III The unifocal tumours in this category spare only the left lateral or right posterior section. These tumours are relatively common. In children with hepatoblastoma, great care must be taken to distinguish between invasion and compression of the apparently uninvolved section of the liver, because risk stratification (and/or the need for liver transplantation) may depend on this point. Anterior central liver tumours involve segment 4 and either or both of segments 5 and 8. Although recent advances in surgical Fig. 4 PRETEXT III. a Extensive tumour sparing only the left lateral section. b Extensive tumour sparing only the right posterior section. c Anterior central liver tumour involving the left medial and right anterior sections. d Contrast-enhanced CT image shows a central liver tumour lying between the left portal vein (white arrow) and the right hepatic vein (black arrow). e Multifocal PRETEXT III tumour, sparing the right anterior section. f Multifocal tumours sparing only the left lateral and right anterior sections. g Multifocal tumours sparing only the left medial and right posterior sections
6 128 Pediatr Radiol (2007) 37: technique permit resection of these tumours without trisectionectomy [15], classification as PRETEXT III reflects the difficulty of these operations (Fig. 4). Multifocal PRETEXT III tumours may also spare the right anterior or left medial sections, or two non-contiguous sections. These patterns are rare. PRETEXT IV PRETEXT IV tumours involve all sections of the liver. These tumours are often multifocal. Alternatively, a very large solitary tumour can involve all four sections (Fig. 5). C: caudate lobe tumours The caudate lobe and caudate process (segment 1 or segments 1 and 9, depending on the system of nomenclature) can be resected with either the left or right lobe of the liver [7]. For this reason, segment 1 was not considered in the PRETEXT classification in the original system [2]. Modern surgical techniques have made resection of segment 1 safer, but these operations remain difficult. Involvement of the caudate lobe is, therefore, a potential predictor of poor outcome. If any tumour is present in segment 1 on imaging at diagnosis (Fig. 3g), the patient will be coded as C1, irrespective of the PRETEXT group (see above). All other patients should be coded as C0. E: extrahepatic abdominal disease The assessment of extrahepatic abdominal disease was one of the most confusing aspects of the original PRETEXT system, and clearly needed revision. Originally, there was a requirement for all extrahepatic abdominal spread of tumour (E+) to be proved by biopsy. Modern imaging techniques are capable, in principle, of identifying extrahepatic abdominal tumour extension in many forms. The frequency and significance of these imaging findings is different for different tumour types, and not all patterns are easily biopsied. In hepatoblastoma, for example, direct extension of tumour into other abdominal organs is unusual. Tumour extension through the diaphragm (Fig. 6) is uncommon, but can be shown quite convincingly by MRI or CT, and biopsy proof may be impractical. In the 2005 revision, patients with direct extension of tumour through the diaphragm or into other organs can be coded as E1 without biopsy proof. Pedunculated tumours are considered to be confined to the sections from which they arise, and are not extrahepatic disease. Peritoneal tumour seeding was originally not included in this category [2]. It probably indicates more advanced abdominal disease than direct extension of the primary tumour. Imaging techniques, especially ultrasonography, can often show even small peritoneal nodules clearly, and the differential diagnosis is very limited. In the 2005 revision, peritoneal nodules will be assumed to be metas- Fig. 5 PRETEXT IV. a Multifocal PRETEXT IV tumours involve all four sections. b Contrast-enhanced CT image of a patient with PRETEXT IV F1 (see text) hepatoblastoma. c Unifocal PRETEXT IV tumours often have a diffuse growth pattern. d Contrast-enhanced CT image of a patient with diffuse PRETEXT IV hepatoblastoma
7 Pediatr Radiol (2007) 37: Fig. 6 Extrahepatic abdominal tumour extension. This composite of contrast-enhanced CT images in a patient with hepatoblastoma shows growth of the primary tumour through the diaphragm into the thorax (E1). The 2005 PRETEXT system no longer requires biopsy proof for this form of tumour spread tases, and will be coded as E2. All other patients should be coded as E0. Ascites is an unusual finding at presentation in hepatoblastoma, but is more common in hepatocellular carcinoma, where it may be an independent predictor of poor prognosis. For this reason, patients with ascites will be coded as E0a, E1a or E2a as appropriate. Abdominal lymph node metastases, which were previously recorded as E+, are now coded as N (see below). F: tumour focality In SIOPEL 1, multifocal tumours were identified at the time of diagnosis in 18% of the patients with hepatoblastoma where this information was available [4]. Univariate analysis showed that the 5-year event-free survival was significantly worse for patients with multifocal tumour (40%) than for those with unifocal tumour (72%) [4]. The independent significance of this finding is unclear, as there is clearly an association between multifocality and advanced PRETEXT number. The German Society of Pediatric Oncology and Hematology reported slightly different results [16]. In its HB89 study, 21% of patients had multiple well-defined tumours, and these children had a similar disease-free survival (DFS; 87%) to those with a single tumour (86%). However, in 20% of children the tumour exhibited a diffuse growth pattern (Fig. 5), and these had a significantly worse DFS (21%) [16]. Unfortunately, a diffuse growth pattern is difficult to define, and despite the promise that this finding shows as a potential risk factor, it was decided not to incorporate it in the 2005 PRETEXT revision. Patients with one hepatic tumour should be coded as F0. All those with more than one tumour nodule (Figs. 3, 4 and 5), regardless of nodule size or PRETEXT stage, should be coded as F1. H: tumour rupture or intraperitoneal haemorrhage It is not uncommon for hepatoblastoma and hepatocellular carcinoma to present with tumour rupture [17, 18]. Originally, these patients were not automatically included as high risk in SIOPEL studies, because of the requirement that extrahepatic disease (E) be proved by biopsy. Although the data to prove this are not currently available, it seems intuitively likely that tumour rupture (usually manifesting as intraperitoneal haemorrhage) is a risk factor, and these patients should be coded as H1. Laparotomy or aspiration of peritoneal blood is not necessary for diagnostic purposes if characteristic imaging and clinical findings (such as hypotension and low haematocrit or haemoglobin level) are present. The presence of peritoneal fluid on imaging alone does not imply tumour rupture (but see E above). Since the opening of the SIOPEL 4 study in September 2004, tumour rupture has become a defining feature of high-risk hepatoblastoma in SIOPEL studies. Patients with no evidence of tumour rupture or haemorrhage, and those with only subcapsular or biopsy-related intraperitoneal bleeding, are coded as H0.
8 130 Pediatr Radiol (2007) 37: M: distant metastases Patients with distant metastases at diagnosis are coded as M1. In hepatoblastoma, these metastases are predominantly found in the lungs. Although the best imaging modality for the identification of lung metastases is currently CT, the defining characteristics of lung metastases in this context have not been specifically studied. It is believed, however, that factors favouring a diagnosis of metastasis include multiple lesions, a rounded, well-defined contour and a subpleural location. In most parts of the world, a single rounded lung lesion with a diameter of >5 mm in a child with a primary liver tumour is very likely to be a metastasis. Patients with these findings on chest CT scans should be classified as M1. Biopsy is not required for staging purposes, because it is uncommon for other lesions to mimic metastases in this clinical context. The protocols of the SIOPEL studies recommend central radiological review if there is any doubt about the presence of lung metastases. Other metastases are infrequently found at diagnosis in hepatoblastoma, but are more common in hepatocellular carcinoma. The imaging findings of brain metastases are usually characteristic, and biopsy is not required. Bone scintigraphy is recommended for staging in children with hepatocellular carcinoma, but not hepatoblastoma. Abnormal calcium metabolism is common in children with hepatoblastoma, and may cause abnormal uptake on bone scintigraphy, especially in the ribs [19], whereas bone metastases are rare [20]. Biopsy proof is therefore mandatory for suspected bone metastases in hepatoblastoma, unless the findings of cross-sectional imaging are characteristic and the patient is already in the high-risk category for some other reason, such as the presence of lung metastases. Bone marrow biopsy is not recommended in children with hepatoblastoma, because bone marrow spread is rare [20]. It is not known whether metastases at different sites have different prognostic implications. For statistical purposes, it is therefore recommended that one or more suffixes be added to M1 to indicate the major sites of metastasis: pulmonary (p), skeletal (s), central nervous system (c), bone marrow (m), and other sites (x). A child with lung, brain, and adrenal metastases would therefore be coded as M1cpx. Patients with no evidence of haematogenous metastatic spread of tumour should be coded as M0. N: lymph node metastases Because porta hepatis (and other abdominal) lymph node metastases are quite unusual in hepatoblastoma, SIOPEL trials have always required this form of tumour spread to be proved by biopsy. In fact, benign enlargement of lymph nodes is probably not uncommon, and the accuracy of positron emission tomography is not known in this context. Because biopsy of equivocal lymph nodes inevitably carries some risk, the SIOPEL committee actively discourages this. Biopsy may, however, be required if there is significant nodal enlargement (for example short axis >15 mm) in a child with no other criteria for high-risk hepatoblastoma. Lymph node metastases are quite common in hepatocellular carcinoma and fibrolamellar carcinoma, and biopsy proof is not required if the imaging abnormality is unequivocal. An arbitrary threshold short axis diameter of 15 mm is suggested for this purpose. Children with no lymph node metastases by these criteria are coded as N0, those with nodal metastases limited to the abdomen (i.e. caudal to the diaphragm and cranial to the inguinal ligament) as N1, and those with extra-abdominal nodal metastases as N2. P: portal vein involvement Involvement of the main portal vein and/or both major branches has been considered a risk factor in hepatoblastoma, because this has obvious implications for the resectability of the tumour. It is also possible that portal vein invasion detected by imaging is an independent risk factor for tumour recurrence [21]. The original PRETEXT criteria, however, did not specifically define the word involvement. It is well recognized that a tumour that abuts or displaces a major portal venous branch at imaging performed at diagnosis (Fig. 7) may shrink away from the vein following preoperative chemotherapy. Imaging evidence of complete obstruction or circumferential encasement (Fig. 7) is therefore required to qualify as portal vein involvement. Failure to identify the portal vein or one of its major branches in either its normal position or its expected displaced location, on good quality images, is strong evidence of obstruction. The other form of involvement, portal vein invasion, is not uncommon, and is often best detected by ultrasound (Fig. 7). Various US signs may be present [22, 23], and analogous findings can be seen on CT and MR imaging. Patients with no imaging evidence of involvement of the main portal vein, its bifurcation, or either of its main branches will be coded as P0. Those who fulfil the original PRETEXT definition of P+ (involvement of the main portal vein, its bifurcation, or both of its main branches), as well as those with cavernous transformation of the portal vein will be coded as P2. P2, however, represents very advanced disease. For this reason, the category P1 has been created for patients with evidence of involvement of one major
9 Pediatr Radiol (2007) 37: Fig. 7 Involvement of the portal and hepatic venous systems. a When the tumour (grey) approaches or abuts the vein (black), there is no venous involvement, even if the vein is partly encased. b Complete obstruction or encasement of the vein is one form of involvement. Obstruction of the inferior vena cava by extrinsic compression, however, does not count as involvement (see text). c Intravascular tumour growth in the portal and/or hepatic venous systems is not uncommon in children with hepatoblastoma or hepatocellular carcinoma. d Transverse ultrasound image of the right lobe of the liver in a patient with hepatoblastoma. The tumour (white circles) has grown into the right branch of the portal vein (P1a), disrupting the normal white line of the vein wall (arrows) branch of the portal vein. In addition, the detection of portal vein invasion should be marked by the suffix a (e.g., P2a). V: involvement of the IVC and/or hepatic veins The same definitions of involvement (venous obstruction, encasement and/or invasion) used for the portal veins apply to the hepatic veins (Fig. 7). A hepatic vein can be assumed to be involved if it cannot be identified at all, and its expected course runs through a large tumour mass. It is important to look carefully for the hepatic veins, preferably with ultrasonography as well as CT and/or MRI, as they may be displaced from their expected position by the tumour. Complete obstruction of the IVC can occur with mass effect alone, without any tumour extension to the vein itself. Inability to visualize the IVC, and the presence of an enlarged azygos vein, are not, therefore, sufficient criteria for involvement. Patients with no imaging evidence of involvement of the hepatic veins or IVC will be coded as V0. As for the portal vein, the original classification of involvement (V+) indicated a very advanced level of disease. Intermediate categories have therefore been created. V1 and V2 indicate involvement of one or two main hepatic veins respectively. V3 indicates involvement of either the IVC or all three of the hepatic veins. In addition, the detection of hepatic vein or IVC invasion should be marked by the suffix a (e.g., V2a). The presence of tumour in the right atrium automatically makes a patient V3a. SIOPEL risk stratification for patients with hepatoblastoma The SIOPEL risk stratification for children with hepatoblastoma is essentially unchanged by this revision. Patients
10 132 Pediatr Radiol (2007) 37: with any one or more of certain criteria (Table 3) are high risk. All other SIOPEL patients are standard risk. Presurgical re-evaluation Although the timing of surgery will depend on the treatment protocol and the patient s response to therapy, preoperative reimaging is almost always necessary. All of the PRETEXT categories should be reassessed after preoperative chemotherapy, as near as possible to the time of surgery, and recorded as POSTEXT (post-treatment extent of disease). Comparison of surgical findings with POSTEXT will allow prospective assessment of the accuracy of imaging techniques. Acknowledgements We would like to thank the many radiologists from all over the world who have referred images (some of which have been used in this paper) for a second opinion. PRETEXT staging is heavily dependent on accurate interpretation of high-quality imaging studies. In case of doubt, rapid radiology review is available for patients who may be eligible for SIOPEL studies (see References 1. MacKinlay GA, Pritchard J (1992) A common language for childhood liver tumours. Pediatr Surg Int 7: Pritchard J, Brown J, Shafford E et al (2000) Cisplatin, doxorubicin, and delayed surgery for childhood hepatoblastoma: a successful approach results of the first prospective study of the International Society of Pediatric Oncology. J Clin Oncol 18: Aronson DC, Schnater JM, Staalman CR et al (2005) Predictive value of the pretreatment extent of disease system in hepatoblastoma: results from the International Society of Pediatric Oncology Liver Tumor Study Group SIOPEL-1 study. J Clin Oncol 23: Brown J, Perilongo G, Shafford E et al (2000) Pretreatment prognostic factors for children with hepatoblastoma results from the International Society of Paediatric Oncology (SIOP) study SIOPEL 1. Eur J Cancer 36: Perilongo G, Shafford E, Maibach R et al (2004) Risk-adapted treatment for childhood hepatoblastoma. final report of the second study of the International Society of Paediatric Oncology-SIOPEL 2. Eur J Cancer 40: Roebuck DJ, Olsen Ø, Pariente D (2006) Radiological staging in children with hepatoblastoma. Pediatr Radiol 36: Couinaud C (1994) The paracaval segments of the liver. J Hepatobiliary Pancreat Surg 2: Ishibashi Y, Sato TJ, Hirai I et al (2001) Ramification pattern and topographical relationship between the portal and hepatic veins in the left anatomical lobe of the human liver. Okajimas Folia Anat Jpn 78: Murakami G, Hata F (2002) Human liver caudate lobe and liver segment. Anat Sci Int 77: Onishi H, Kawarada Y, Das BC et al (2000) Surgical anatomy of the medial segment (S4) of the liver with special reference to bile ducts and vessels. Hepatogastroenterology 47: Fasel JH, Selle D, Evertsz CJ et al (1998) Segmental anatomy of the liver: poor correlation with CT. Radiology 206: Fischer L, Cardenas C, Thorn M et al (2002) Limits of Couinaud s liver segment classification: a quantitative computer-based three-dimensional analysis. J Comput Assist Tomogr 26: Sales JP, Hannoun L, Sichez JP et al (1984) Surgical anatomy of liver segment IV. Anat Clin 6: Goldsmith NA, Woodburne RT (1957) The surgical anatomy pertaining to liver resection. Surg Gynecol Obstet 105: Ohno Y, Furui J, Kanematsu T (2004) Is a modified central bisegmentectomy a volume-saving operation for pediatric hepatoblastoma? J Pediatr Surg 39:E13 E Von Schweinitz D, Hecker H, Schmidt-von-Arndt G et al (1997) Prognostic factors and staging systems in childhood hepatoblastoma. Int J Cancer 74: Ishak KG, Glunz PR (1967) Hepatoblastoma and hepatocarcinoma in infancy and childhood. Report of 47 cases. Cancer 20: Iida T, Suenaga M, Takeuchi Y et al (2004) Successful resection of a ruptured hepatoblastoma prior to chemotherapy: report of a case. Surg Today 34: Archer D, Babyn P, Gilday D et al (1993) Potentially misleading bone scan findings in patients with hepatoblastoma. Clin Nucl Med 18: Exelby PR, Filler RM, Grosfeld JL (1975) Liver tumors in children in the particular reference to hepatoblastoma and hepatocellular carcinoma: American Academy of Pediatrics Surgical Section Survey J Pediatr Surg 10: von Schweinitz D, Wischmeyer P, Leuschner I et al (1994) Clinico-pathological criteria with prognostic relevance in hepatoblastoma. Eur J Cancer 30A: Sato M, Ishida H, Konno K et al (2000) Liver tumors in children and young patients: sonographic and color Doppler findings. Abdom Imaging 25: Ohtsuka Y, Takahashi H, Ohnuma N et al (1997) Detection of tumor thrombus in children using color Doppler ultrasonography. J Pediatr Surg 32:
Assessment of extrahepatic abdominal extension in primary malignant liver tumours of childhood
 Pediatr Radiol (2007) 37:1096 1100 DOI 10.1007/s00247-007-0513-2 REVIEW Assessment of extrahepatic abdominal extension in primary malignant liver tumours of childhood Derek J. Roebuck & Neil J. Sebire
Pediatr Radiol (2007) 37:1096 1100 DOI 10.1007/s00247-007-0513-2 REVIEW Assessment of extrahepatic abdominal extension in primary malignant liver tumours of childhood Derek J. Roebuck & Neil J. Sebire
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Childhood Liver Tumours The SIOPEL experience. Giorgio Perilongo, Clinica Pediatrica, Dipartimento A.I. Di Pediatria di Padova
 Childhood Liver Tumours The SIOPEL experience Giorgio Perilongo, Clinica Pediatrica, Dipartimento A.I. Di Pediatria di Padova On behalf of the International Childhood Liver Tumour Strategy Group - SIOPEL
Childhood Liver Tumours The SIOPEL experience Giorgio Perilongo, Clinica Pediatrica, Dipartimento A.I. Di Pediatria di Padova On behalf of the International Childhood Liver Tumour Strategy Group - SIOPEL
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
PLUTO First report. Pediatric Transplantation DOI: /j x
 Pediatr Transplantation 2010 Ó 2010 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/j.1399-3046.2010.01395.x PLUTO First report Otte J-B, Meyers R. PLUTO First report. Pediatr Transplantation
Pediatr Transplantation 2010 Ó 2010 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/j.1399-3046.2010.01395.x PLUTO First report Otte J-B, Meyers R. PLUTO First report. Pediatr Transplantation
Normal Sonographic Anatomy
 hapter 2:The Liver DUNSTAN ABRAHAM Normal Sonographic Anatomy Homogeneous, echogenic texture (Figure 2-1) Measures approximately 15 cm in length and 10 12.5 cm anterior to posterior; measurement taken
hapter 2:The Liver DUNSTAN ABRAHAM Normal Sonographic Anatomy Homogeneous, echogenic texture (Figure 2-1) Measures approximately 15 cm in length and 10 12.5 cm anterior to posterior; measurement taken
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Leukaemia 35% Lymphoma 14%
 Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Cisplatin versus Cisplatin plus Doxorubicin for Standard-Risk Hepatoblastoma
 The new england journal of medicine original article versus plus Doxorubicin for Standard-Risk Hepatoblastoma Giorgio Perilongo, M.D., Rudolf Maibach, Ph.D., Elisabeth Shafford, M.D., Laurence Brugieres,
The new england journal of medicine original article versus plus Doxorubicin for Standard-Risk Hepatoblastoma Giorgio Perilongo, M.D., Rudolf Maibach, Ph.D., Elisabeth Shafford, M.D., Laurence Brugieres,
Wilms Tumor and Neuroblastoma
 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Liver Ultrasound - Beyond the Basics. Pamela Parker Lead Sonographer
 Liver Ultrasound - Beyond the Basics Pamela Parker Lead Sonographer Aims Review what we know about the liver Reasons for imaging Focal lesions Diffuse disease Can we do more? The Liver The Liver The Liver
Liver Ultrasound - Beyond the Basics Pamela Parker Lead Sonographer Aims Review what we know about the liver Reasons for imaging Focal lesions Diffuse disease Can we do more? The Liver The Liver The Liver
Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C.
 Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Anatomy Jessica Ferguson Ashley Dobos May 31, 2006 LIVER
 Anatomy Jessica Ferguson Ashley Dobos May 31, 2006 LIVER 1) Other Names: Reidel s Lobe normal anatomic variant; projection of the right lobe that can extend as far as the iliac crest (Tempkin, p.54, Anatomy).
Anatomy Jessica Ferguson Ashley Dobos May 31, 2006 LIVER 1) Other Names: Reidel s Lobe normal anatomic variant; projection of the right lobe that can extend as far as the iliac crest (Tempkin, p.54, Anatomy).
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Pre-operative assessment of patients for cytoreduction and HIPEC
 Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
Newcastle HPB MDM updated radiology imaging protocol recommendations. Author Dr John Scott. Consultant Radiologist Freeman Hospital
 Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Hilar cholangiocarcinoma. Frank Wessels, Maarten van Leeuwen, UMCU utrecht
 Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Interesting Cases from Liver Tumor Board. Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine
 Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview
 Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Intrahepatic ramifications of the portal vein in the horse
 Intrahepatic ramifications of the portal vein in the horse Tadjalli, M. 1* and Moslemy, H. R. 2 1 Department of Anatomical Sciences, School of Veterinary Medicine, University of Shiraz, Shiraz, Iran; 2
Intrahepatic ramifications of the portal vein in the horse Tadjalli, M. 1* and Moslemy, H. R. 2 1 Department of Anatomical Sciences, School of Veterinary Medicine, University of Shiraz, Shiraz, Iran; 2
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Liver imaging takes a step forward with Ingenia
 Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Management of Colorectal Liver Metastases
 Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Sectional Anatomy Quiz - III
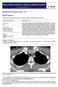 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
SURVIVAL AND TREATMENT OUTCOMES IN PEDIATRIC HEPATOBLASTOMA: THE FIRST REPORT FROM THAILAND
 SURVIVAL AND TREATMENT OUTCOMES IN PEDIATRIC HEPATOBLASTOMA: THE FIRST REPORT FROM THAILAND Kamon Phuakpet 1, Kleebsabai Sanpakit 1, Pongwut Tanaanunmongkol 1, Gavivann Veerakul 1, Nassawee Vathana 1,
SURVIVAL AND TREATMENT OUTCOMES IN PEDIATRIC HEPATOBLASTOMA: THE FIRST REPORT FROM THAILAND Kamon Phuakpet 1, Kleebsabai Sanpakit 1, Pongwut Tanaanunmongkol 1, Gavivann Veerakul 1, Nassawee Vathana 1,
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Surface Anatomy. Location Shape Weight Role of Five Surfaces Borders Fissures Lobes Peritoneal Lig
 The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
Intrahepatic Cholangiocarcinoma (ICC) Detected by Sonography
 661245JDMXXX10.1177/8756479316661245Journal of Diagnostic Medical SonographyHamer research-article2016 Case Study Intrahepatic Cholangiocarcinoma (ICC) Detected by Sonography Journal of Diagnostic Medical
661245JDMXXX10.1177/8756479316661245Journal of Diagnostic Medical SonographyHamer research-article2016 Case Study Intrahepatic Cholangiocarcinoma (ICC) Detected by Sonography Journal of Diagnostic Medical
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning
 Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Nephroblastoma: Does The Decrease In Tumour Volume Under Preoperative Chemotherapy Predict The Lymph Nodes Status At Surgery?
 Nephroblastoma: Does The Decrease In Tumour Volume Under Preoperative Chemotherapy Predict The Lymph Nodes Status At Surgery? Jan Godzinski,, Harm van Tinteren,, Jan de Kraker,, Norbert Graf, Christophe
Nephroblastoma: Does The Decrease In Tumour Volume Under Preoperative Chemotherapy Predict The Lymph Nodes Status At Surgery? Jan Godzinski,, Harm van Tinteren,, Jan de Kraker,, Norbert Graf, Christophe
Hematologic Malignancies of the Liver : Spectrum of Disease. Zhou Jian
 Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer
 Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, :00 12:10 p.m.
 SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
University of Colorado Health Sciences Center, Denver Colorado ******************** ******************
 University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
MR Tumor Staging for Treatment Decision in Case of Wilms Tumor
 MR Tumor Staging for Treatment Decision in Case of Wilms Tumor G. Schneider, M.D., Ph.D.; P. Fries, M.D. Dept. of Diagnostic and Interventional Radiology, Saarland University Hospital, Homburg/Saar, Germany
MR Tumor Staging for Treatment Decision in Case of Wilms Tumor G. Schneider, M.D., Ph.D.; P. Fries, M.D. Dept. of Diagnostic and Interventional Radiology, Saarland University Hospital, Homburg/Saar, Germany
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer
 Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN
 Research Article International Journal of Bioassays ISSN: 2278-778X www.ijbio.com STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN Anju Balaji More Department of Anatomy, Sree
Research Article International Journal of Bioassays ISSN: 2278-778X www.ijbio.com STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN Anju Balaji More Department of Anatomy, Sree
Alison Douglass Gillian Lieberman, MD. November. Colon Cancer. Alison Douglass, Harvard Medical School Year III Gillian Lieberman, MD
 November Colon Cancer Alison Douglass, Harvard Medical School Year III Our Patient Mr. K. is a 67 year old man with no prior medical problems other than hemorrhoids which have caused occasional rectal
November Colon Cancer Alison Douglass, Harvard Medical School Year III Our Patient Mr. K. is a 67 year old man with no prior medical problems other than hemorrhoids which have caused occasional rectal
Afternoon Session Cases
 Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
Use of Ultrasound in NAFLD
 Institute for Liver and Digestive Health Use of Ultrasound in NAFLD Dr. Davide Roccarina Specialist in General Medicine Specialist Doctor in Clinical Ultrasound and non-invasive liver assessment Hepatology
Institute for Liver and Digestive Health Use of Ultrasound in NAFLD Dr. Davide Roccarina Specialist in General Medicine Specialist Doctor in Clinical Ultrasound and non-invasive liver assessment Hepatology
Liver metastases: treatment planning. PJ Valette
 Liver metastases: treatment planning PJ Valette Liver metastases removal December 2010 April 2011 : after chemotherapy June 2011 : after resection of left lobe mets & portal embol. Sept 2011 : 1 year after
Liver metastases: treatment planning PJ Valette Liver metastases removal December 2010 April 2011 : after chemotherapy June 2011 : after resection of left lobe mets & portal embol. Sept 2011 : 1 year after
EFSUMB Course Book, 2 nd Edition
 Ultrasound of the liver. 11.04.2018 10:01 1 EFSUMB Course Book, 2 nd Edition Editor: Christoph F. Dietrich Ultrasound of the liver Christoph F. Dietrich, Carla Serra 2, Maciej Jedrzejczyk 3 1 Caritas-Krankenhaus
Ultrasound of the liver. 11.04.2018 10:01 1 EFSUMB Course Book, 2 nd Edition Editor: Christoph F. Dietrich Ultrasound of the liver Christoph F. Dietrich, Carla Serra 2, Maciej Jedrzejczyk 3 1 Caritas-Krankenhaus
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Pediatric Liver Tumors and Transplantation. Northwest Regional Pediatric Live Disease Symposium, Seattle WA, April 12, 2008
 Pediatric Liver Tumors and Transplantation Northwest Regional Pediatric Live Disease Symposium, Seattle WA, April 12, 2008 Liver transplantation for primary liver tumours in children WHEN? - patient selection
Pediatric Liver Tumors and Transplantation Northwest Regional Pediatric Live Disease Symposium, Seattle WA, April 12, 2008 Liver transplantation for primary liver tumours in children WHEN? - patient selection
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls
 MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls Poster No.: C-0987 Congress: ECR 2015 Type: Educational Exhibit Authors: D. V. Bhargavi, R. Avantsa, P. Kala; Bangalore/IN
MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls Poster No.: C-0987 Congress: ECR 2015 Type: Educational Exhibit Authors: D. V. Bhargavi, R. Avantsa, P. Kala; Bangalore/IN
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
US LI-RADS v2017 CORE
 US LI-RADS v2017 CORE Screening or surveillance US in patient at high risk for HCC US category US-1 US-2 US-3 Negative Subthreshold Positive Category Concept Definition US-1 Negative US-2 Subthreshold
US LI-RADS v2017 CORE Screening or surveillance US in patient at high risk for HCC US category US-1 US-2 US-3 Negative Subthreshold Positive Category Concept Definition US-1 Negative US-2 Subthreshold
Lesions of the pancreaticoduodenal groove, a pictorial review
 Lesions of the pancreaticoduodenal groove, a pictorial review Poster No.: C-2131 Congress: ECR 2013 Type: Educational Exhibit Authors: E. Ni Mhurchu, L. Lavelle, I. Murphy, S. Skehan ; IE, Dublin/ IE Keywords:
Lesions of the pancreaticoduodenal groove, a pictorial review Poster No.: C-2131 Congress: ECR 2013 Type: Educational Exhibit Authors: E. Ni Mhurchu, L. Lavelle, I. Murphy, S. Skehan ; IE, Dublin/ IE Keywords:
Biliary cancers: imaging diagnosis. Study of 30 cases
 Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
NAACCR Webinar Series 1
 Collecting Cancer Data: Liver 2013 2014 NAACCR Webinar Series June 5, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Liver 2013 2014 NAACCR Webinar Series June 5, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT
 The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
CASE 1 11/1/2016 HEPATOBILIARY IMAGING CASE PRESENTATIONS DECLARATION. Dr. Chirag Patel ORGAN IMAGING yr old lady
 HEPATOBILIARY IMAGING CASE PRESENTATIONS DECLARATION No financial disclosures or affiliations with commercial organisations No discussion of investigational or off-label use of medical devices, products
HEPATOBILIARY IMAGING CASE PRESENTATIONS DECLARATION No financial disclosures or affiliations with commercial organisations No discussion of investigational or off-label use of medical devices, products
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES
 MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
State of the Art Imaging for Hepatic Malignancy: My Assignment
 State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Ovarian Tumors. Andrea Hayes-Jordan MD FACS, FAAP Section Chief, Pediatric Surgery/Surgical Onc. UT MD Anderson Cancer Center
 Ovarian Tumors Andrea Hayes-Jordan MD FACS, FAAP Section Chief, Pediatric Surgery/Surgical Onc. UT MD Anderson Cancer Center Case 13yo female with abdominal pain Ultrasound shows huge ovarian mass Surgeon
Ovarian Tumors Andrea Hayes-Jordan MD FACS, FAAP Section Chief, Pediatric Surgery/Surgical Onc. UT MD Anderson Cancer Center Case 13yo female with abdominal pain Ultrasound shows huge ovarian mass Surgeon
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1
 Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Question 1 History. Likely Diagnosis Differential. Further Investigation or Management. Requires Paediatric Surgical referral for laparotomy
 Question 1 Male newborn spilling green tinged vomit day 1 of life Imaging Abdominal X-Rays performed on 03/05/2012 Upper and lower gastrointestinal contrast studies performed on 03/05/2012 Abdominal X-Rays
Question 1 Male newborn spilling green tinged vomit day 1 of life Imaging Abdominal X-Rays performed on 03/05/2012 Upper and lower gastrointestinal contrast studies performed on 03/05/2012 Abdominal X-Rays
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
MALIGNANT HEPATIC NEOPLASMS: USING ULTRASONOGRAPHY AS A MEANS OF DEFINING HEPATIC LESIONS. 1.5 Contact Hours. Presented by: CEU Professor 7
 MALIGNANT HEPATIC NEOPLASMS: USING ULTRASONOGRAPHY AS A MEANS OF DEFINING HEPATIC LESIONS 1.5 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group,
MALIGNANT HEPATIC NEOPLASMS: USING ULTRASONOGRAPHY AS A MEANS OF DEFINING HEPATIC LESIONS 1.5 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group,
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Renal and adrenal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Renal cell carcinoma 3 Clinical
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Renal and adrenal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Renal cell carcinoma 3 Clinical
GUIDELINES ON RENAL CELL CARCINOMA
 GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary)
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Local staging of colon cancer: the current role of CT
 Local staging of colon cancer: the current role of CT Poster No.: C-2699 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit A. P. Pissarra, R. R. Domingues Madaleno, C. Sanches, L. Curvo-
Local staging of colon cancer: the current role of CT Poster No.: C-2699 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit A. P. Pissarra, R. R. Domingues Madaleno, C. Sanches, L. Curvo-
Malignant Focal Liver Lesions
 Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Liver resection for HCC
 8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
Liver Cancer And Tumours
 Liver Cancer And Tumours What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood from all parts of the body, cancer cells from elsewhere can
Liver Cancer And Tumours What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood from all parts of the body, cancer cells from elsewhere can
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest
 ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest J Gossner Citation J Gossner. Appearance And Visibility
ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest J Gossner Citation J Gossner. Appearance And Visibility
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS
 Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Basic Abdominal Sonography
 24S Basic Abdominal Sonography Procedural Overview JOHN FATCHETT II, RDMS is provided. Patient preparation (i.e., fasting) scanning techniques, spleen, transducer. evaluation of abdominal anatomy in the
24S Basic Abdominal Sonography Procedural Overview JOHN FATCHETT II, RDMS is provided. Patient preparation (i.e., fasting) scanning techniques, spleen, transducer. evaluation of abdominal anatomy in the
Radiologic assessment of response of tumors to treatment. Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1
 Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Liver Tumors. Prof. Dr. Ahmed El - Samongy
 Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Abdomen and Retroperitoneum Ultrasound Protocols
 Abdomen and Retroperitoneum Ultrasound Protocols Reviewed By: Anna Ellermeier, MD Last Reviewed: March 2018 Contact: (866) 761-4200, Option 1 **NOTE for all examinations: 1. If documenting possible flow
Abdomen and Retroperitoneum Ultrasound Protocols Reviewed By: Anna Ellermeier, MD Last Reviewed: March 2018 Contact: (866) 761-4200, Option 1 **NOTE for all examinations: 1. If documenting possible flow
