Association between neuromyelitis optica and tuberculosis in a Chinese population
|
|
|
- Caren Anderson
- 5 years ago
- Views:
Transcription
1 Li et al. BMC Neurology 2014, 14:33 RESEARCH ARTICLE Open Access Association between neuromyelitis optica and tuberculosis in a Chinese population Rui Li, Xiaonan Zhong, Wei Qiu, Aimin Wu, Yongqiang Dai, Zhengqi Lu and Xueqiang Hu * Abstract Background: A number of reports have described the presence of tuberculosis (TB) in neuromyelitis optica (NMO) patients. However, a definite association between the two conditions has not been conclusively demonstrated. Methods: To investigate the association between NMO and TB in a Chinese population, we performed a retrospective review of hospital records of NMO patients, control patients and tuberculosis meningitis (TBM) patients from January 1, 1995 to December 31, Results: The frequency of preceding/simultaneous active pulmonary TB (PTB) was not significantly different between NMO patients (1.1%) and control groups (2.3% in myasthenia gravis, 1.1% in polymyositis or dermatomyositis, zero in idiopathic facial palsy and viral meningitis/meningoencephalitis). NMO cases differed from TBM cases in terms of demographics, course (recurrent or monophasic), cerebrospinal fluid analysis and magnetic resonance images. Two TBM patients shared partial clinical features with NMO (one of the TBM patients had a longitudinal extensive spinal cord lesion involving the holocord, and the other had optic neuritis before anti-tuberculosis treatment). NMO antibodies were only detected in NMO patients and not in TBM patients with myelitis or optic neuritis. Conclusions: We could not confirm previous suggestions of the association between PTB and NMO. Direct infection of the central nervous system by TB may mimic NMO in some respects, but whether NMO-like symptoms that develop during the course of TB should be considered and diagnosed as NMO is open to discussion. Keywords: Neuromyelitis optica, Tuberculosis, NMO-IgG Background Neuromyelitis optica (NMO) is a severe demyelinating disease of the central nervous system (CNS) that preferentially affects the optic nerve and spinal cord [1]. The disease is idiopathic and the discovery that patients are seropositive for aquaporin-4-specific autoantibody (AQP4- Ab or NMO-IgG) suggested the existence of an underlying immunopathogenic mechanism [1,2]. Although NMO usually occurs in isolation, reports over the past century have suggested an association between NMO and tuberculosis (TB) [3-8]. A study by Hughes and colleagues described three patients that developed acute necrotic myelopathy during the course of active pulmonary TB (PTB) [4]. A report from the Western Cape of South Africa described * Correspondence: huxueqiangzssy@qq.com Equal contributors Multiple Sclerosis Center, Department of Neurology, The Third Affiliated Hospital of Sun Yat-Sen University, No. 600 Tianhe Road, Guangzhou, Guangdong Province , China six patients with optic neuropathy and myelopathy with associated active PTB but no evidence of TB infection in the CNS [3]. Another study, also carried out in South Africa, suggested PTB-associated NMO developed in patients with active infection because 79% (11/14) of NMO patients had a preceding or simultaneous diagnosis of PTB [8]. Finally, Feng and colleagues described the benefits of anti-tuberculosis treatment in steroid-refractory Chinese NMO patients [9]. Although an association between NMO and TB has been suggested in a number of reports from different geographical regions, a definite association between the two conditions has not been conclusively demonstrated. Further investigation and clarification would be helpful in the diagnosis and treatment of patients who develop NMOlike symptoms (longitudinal extensive myelitis and optic neuritis) during the course of TB. We therefore performed a retrospective study to investigate whether 2014 Li et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
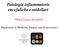
2 Li et al. BMC Neurology 2014, 14:33 Page 2 of 7 there is an association between NMO and TB in the Chinese population. Methods Ethics statement Ethical approval was given by the medical ethics committee of the third affiliated hospital of Sun Yat-sen University with the following reference number: [2007]33. Written informed consent was obtained from the patient for publication of the clinical data and any accompanying images. Patients and selection criteria To study the prevalence of PTB in NMO patients compared with controls, we performed a retrospective review of hospital records of patients with a diagnosis of NMO that were admitted to our hospital, The Third Affiliated Hospital of Sun Yat-Sen University, from January 1, 1995 to December 31, All NMO patients fulfilled the 2006 Wingerchuk criteria [10] (the 1999 Wingerchuk diagnostic criteria were used for several cases owing to a lack of NMO-IgG data [11]). Patients with evidence of sarcoidosis, vasculitis, clinically manifest systemic lupus erythematosus, Sjogren s syndrome or another explanation for optic neuritis or myelitis were excluded [12]. The control groups consisted of patients with myasthenia gravis, polymyositis or dermatomyositis, idiopathic facial palsy, and viral meningitis/meningoencephalitis (VM). To avoid any confusion with aseptic meningitis/meningoencephalitis, patients were considered to have VM when either a viral etiology was confirmed or antiviral treatment was effective. VM was only diagnosed after ruling out bacterial, fungal, and noninfectious causes of meningitis (malignancy, autoimmune disorders, neurosarcoidosis) [13]. To ensure a similar background exposure to TB, control and NMO cases were matched for sex, age at time of admission (within 10 years), and date of admission (within a range of 5 years). If more than one matching control was identified per case, the one with the closest age at admission was included. These patients were used as controls because there is no known causal association with the risk factor under investigation (TB). The following data were collected for all NMO and control cases: sex, age at onset of neurological symptoms, and the presence or absence of a diagnosis of active PTB [14]. Active PTB was defined either as a diagnosis of PTB preceding the onset of NMO by fewer than 6 months, or PTB that was not cured before admission for neurological disease. Duration from diagnosis of PTB to onset of neurological symptoms (if previously diagnosed with PTB), cerebrospinal fluid (CSF) data (if available), and NMO-IgG serum status (if available) was also collected for all cases. To investigate whether patients with tuberculosis meningitis (TBM) shared partial clinical features to NMO patients fulfilling the 2006 Wingerchuk criteria, we also enrolled TBM patients admitted to our hospital during the same period using TBM criteria according to Thwaites [15]. Detailed data on clinical presentation, CSF reports, magnetic resonance imaging (MRI) reports, therapy, and outcomes were collected for NMO and TBM cases. Using MRI, spinal cord lesions extending over three or more vertebral segments on the spinal cord were defined as longitudinal extensive spinal cord lesions (LESCLs). Linear lesions were defined on T2-weighted imaging on MRI according to Misu et al. [16] as: (i) consecutive linear shape lesions on the sagittal plane and (ii) symmetric, with a preferential involvement in the central gray matter on the axial plane. Serum NMO-IgG antibodies were tested according to the manufacturer s instructions using aquaporin 4-transfected cells from a commercial sampling kit (EUROIMMUN AG, Luebeck, Germany). Statistical analysis All statistical analyses were performed using Statistical Program for Social Sciences (SPSS) statistical software (version 16.0, San Francisco, CA, USA). P <0.05 was considered statistically significant. Comparisons of the presence of PTB between NMO patients and controls were carried out using the Chi-squared test. Results We enrolled 88 patients with NMO (67 diagnosed using the 2006 Wingerchuk diagnostic criteria and 21 using the 1999 Wingerchuk diagnostic criteria) and 352 controls into our study. The data on the presence of PTB in NMO and control groups are shown in Table 1. One NMO patient among the total 88 (1.1%) had a preceding diagnosis of PTB. The frequency of active PTB in NMO patients was not significantly different from that in patients with myasthenia gravis, polymyositis or dermatomyositis, facial neuritis, and VM (P > 0.05). The single NMO patient who had a previous history of PTB showed no evidence (in either CSF or radiology reports) indicative of TB infection in the CNS. She was a 26-year-old woman who experienced visual blurring simultaneously in bilateral optic neuritis and hemiplegia of her left limbs, 2 months prior to admission. She was positive for NMO-IgG and the CSF protein concentration was 0.67 g/l, while glucose concentration and cell count were normal. Brain MRI showed non-specific white matter lesions. Spinal MRI showed a LESCL from C1 to T5 without evidence of meningeal enhancement or tuberculoma (Figure 1). The patient was diagnosed with NMO. She had consolidation in her chest X-ray 3 months prior to admission. During hospitalization she had a cough and her sputum was positive for acid-fast bacilli. Chest radiography revealed extensive bilateral
3 Li et al. BMC Neurology 2014, 14:33 Page 3 of 7 Table 1 Demography and presence of TB in NMO patients and controls Disease Number of patients, n (M/F) Age, mean ± SD, years Presence of active PTB, n (%) P value NMO 88 (17/71) 34.1 ± (1.1) Myasthenia gravis 88 (17/71) 33.5 ± (2.3) > 0.05 Polymyositis or 88 (17/71) 35.6 ± (1.1) > 0.05 dermatomyositis Idiopathic 88 (17/71) 39.7 ± (0) > 0.05 facial palsy VM 88 (17/71) 33.8 ± (0) > 0.05 TB tuberculosis; PTB pulmonary tuberculosis; NMO neuromyelitis optica; VM viral meningitis/meningoencephalitis; M male; F female; P: comparison for active PTB presence between NMO and each control groups. Figure 1 Spinal MRI of the NMO patient with active PTB. a: axial T2-weighted image showing a cervical lesion predominantly involving the central cord; b: T1-weighted contrast image revealing slight enhancement of the lesion; c: T2-weighted image showing a longitudinal extensive spinal cord lesion. confluent consolidation, predominantly involving the upper lobes. Ziehl-Neelsen microscopy showed no acid-fast bacilli in her CSF. After anti-tuberculosis treatment combined with methylprednisolone pulse therapy, her PTB recovered, but she had recurrent myelitis during the 17-month followup period. Special MRI procedures including diffusion and magnetic resonance spectroscopy were not performed because they were unavailable during that period. However, taking MRI features, discussion with neurosurgeons, and the later follow-up into consideration, intramedullary tuberculoma could be excluded. Table 2 shows the demographic and clinical features of NMO and TBM patients. Out of 92 TBM patients, 10 had myelitis (spinal meningitis, n = 2; tuberculoma, n = 1; meningitis combined with tuberculoma, n = 2; focal or extensive spinal lesions with hydrocephalus, meningitis or tuberculoma in brain MRI, n = 2; clinical manifestations indicating myelitis, n = 3). Two TBM patients had optic neuritis, of which one developed optic neuritis before anti-tuberculosis treatment. Compared with TBM related myelitis (TBM-MY), NMO patients had a higher female: male ratio (71:7 vs. 3:7), higher relapse rate of myelitis (75% vs. 0), higher seropositive rate of NMO-IgG (82.1% vs. 0%), and a higher frequency of normal cell count, protein, glucose and chloride concentration in the CSF. CSF TB-antibody positivity was found in 30% (3/10) of patients with TBM-MY, but not in NMO patients. Spinal MRI was performed in all NMO patients and 7/10 TBM-MY patients. There were no spinal MRI data for the three remaining TBM-MY patients because MRI was not available at the time. However, these patients presented with typical clinical symptoms indicating myelitis. Spinal cord lesions in NMO patients mostly extend over multiple cord levels involving central gray matter (linear lesions, shown in Figure 2) or holocord (LESCLs and spinal lesions with central/holocord involvement were found in 73.9% of patients). Compared with NMO patients, spinal image features of TBM-MY patients were different. Meningeal enhancement (57.1% of patients), or tuberculoma (42.9% of patients), which is characterized by oval lesions with low (or iso-) T1-weighted image signal, typical target sign T2-weighted image signal, and nodular or rim enhancement in spinal cord was common (Figures 3 and 4). Although one TBM-MY patient had LESCLs, similar to the characteristic spinal MRI finding in NMO, the tuberculoma in his medulla suggested direct TB infection of the CNS (Figure 5). Methylprednisolone pulse therapy was administered to all NMO patients in the acute phase. During remission, six patients received additional immunosuppressants. All 92 TBM patients received anti-tuberculosis therapy (isoniazid, rifampicin, ethambutol plus pyrazinamide or streptomycin for 86 patients and isoniazid, rifampicin, ethambutol plus second-line drugs for the remaining six patients).
4 Li et al. BMC Neurology 2014, 14:33 Page 4 of 7 Table 2 Demographic and clinical features of NMO and TBM patients NMO n = 88 TBM Total n = 92 TBM-MY n = 10 TBM-ON n = 2 Sex ratio, F/M 71/7 40/52 3/7 1/1 Age, mean ± SD, years 35.3 ± ± ± , 41 Relapse of myelitis, n(%) 66/88 (75.0%) -- 0/6 (0) -- CSF Pleocytosis, n(%) 16/88 (18.2%) 92/92 (100.0%) 10/10 (100%) 2/2 (100%) Increased protein level, n(%) 14/88 (15.9%) 92/92 (100.0%) 10/10 (100%) 2/2 (100%) Decreased glucose level, n(%) 1/88 (1.1%) 92/92 (100.0%) 10/10 (100%) 2/2 (100%) TB-antibody positivity, n(%) 0/45 (0) 27/92 (29.3%) 3/10 (30%) 0/2 (0) Mycobacterium tuberculosis, n(%) 0/45 (0) 0/92 (0) 0/10 (0) 0/2 (0) Seropositive NMO-IgG, n(%) 55/67 (82.1%) 0/5 (0) 0/3 (0) 0/1 (0) Spinal MRI Linear lesions, n(%) 41/88 (46.6%) -- 0/7 (0) -- LESCLs, n(%) 65/88 (73.9%) -- 1/7 (14.3%) -- Central or holocord involvement, n(%) 65/88 (73.9%) -- 1/7 (14.3%) -- Tuberculoma, n(%) 0/88 (0) -- 3/7 (42.9%) -- Meningeal enhancement, n(%) 7/88 (8.0%) -- 4/7 (57.1%) -- Follow-up duration, median (range), months 28.5 (12 106) 14.5 (5 96) 18.0 (6 84) 24, 17 NMO neuromyelitis optica; TBM tuberculosis meningitis; TBM-MY:TBM related-melitis; TBM-ON:TBM related-optic neuritis; F female; M: male; CSF cerebrospinal fluid; MRI magnetic resonance imaging; LESCLs longitudinal extensive spinal cord lesions. Discussion Several reports have suggested PTB-related NMO is caused by an immune response to TB infection. Acute necrotic myelopathy or NMO occurred in a few patients with active PTB. A postmortem study found demyelination in the spinal cord without any evidence of TB involvement [3,4]. The study by Hughes and colleagues suggested tubercle bacillus, the bacterium that causes TB, shares antigens with myelin basic protein so that lymphocytes sensitized against mycobacterium recognize Figure 2 Spinal cord lesion in an NMO patient. The lesions are shown by arrows. a: T2-weighted image showing a linear-shape lesion; b: axial T2-weighted image showing a cervical lesion predominantly involving the central gray matter in the spinal cord. Figure 3 Spinal MRI of a CNS-TB patient with spinal cord involvement. a b: meningeal and whole lesion enhancement on a T1-weighted contrast image; c: T2-weighted image showing an isolated lesion at the T5 level of the spinal cord.
5 Li et al. BMC Neurology 2014, 14:33 Page 5 of 7 Figure 4 Spinal MRI findings in a CNS-TB patient with spinal cord involvement. a: tuberculoma with iso-intensity on sagittal T1-weighted image; b: T1-weighted contrast image showing enhancement of the whole lesion and meninges; c: tuberculoma with iso-intensity on a sagittal T2-weighted image. and attack myelin [4]. Recently, a report from South Africa described a higher proportion of active PTB in NMO patients compared with controls (79% vs. 14%, P = < 0.05) [8]. CNS-TB was excluded in all cases. In contrast to this previous report, we could not confirm an association of NMO with PTB. Only one (1.1%) of the 88 patients in the NMO group was previously diagnosed with PTB and this was similar to the percentage observed in the control group (P > 0.05). Western Cape Province in South Africa had an annual TB incidence of 517 per in 2007 [8], while the estimated national incidence for China was considerably lower than that in South Africa (approximately 154 per in 2006 according to World Health Organization reports [17], and even as low as 70 per in some areas of China [18]). It is therefore likely that the prevalence of NMO in regions with a high incidence of TB is different from the idiopathic autoimmune form seen in areas of relatively low TB incidence. Another possible explanation for TB-related NMO relates to a nonspecific adjuvant effect of TB that amplifies the immune response. It is relatively easy to induce an autoimmune disease in genetically susceptible animals via immunization with complete Freund s adjuvant (containing inactivated M. tuberculosis) and an autoantigen [19-21]. Although we do not know to what extent the adjuvant effect of M. tuberculosis contributes to the pathogenesis of the experimental autoimmune encephalitis (EAE) model, a myelin-specific antigen in incomplete Freund s adjuvant lacking M. tuberculosis can also induce EAE in marmosets [22], suggesting that, at least in Figure 5 Spinal MRI of a CNS-TB patient with spinal cord involvement. a: axial T2-weighted image showing central gray matter involvement of the spinal cord. b: T1-weighted contrast image revealing tuberculoma enhancement in the medulla but no enhancement of the spinal cord lesion; c: T2-weighted image showing a longitudinal extensive spinal cord lesion without a well-demarcated boundary. some species, this agent is not necessary for induction of EAE. It has also been proposed that some NMO cases are caused by a direct CNS infection with tuberculosis. In a small controlled study carried out by Feng and colleagues from China, positivity for M. tuberculosis DNA in the CSF of 2 out of 12 steroid-refractory NMO patients (confirmed using nested polymerase chain reaction and the long-term clinical efficacy of anti-tuberculosis treatment in these patients) suggested pathogenesis involves direct CNS infection [9]. However, it is possible that Feng et al. s study may have been subjected to selection bias because the authors used the original criteria for NMO diagnosis (Wingerchuck 1999), which did not require NMO-IgG
6 Li et al. BMC Neurology 2014, 14:33 Page 6 of 7 data, and their patients showed a high rate of CSF abnormalities (CSF protein levels were increased in 53.9% of patients and 50% had elevated CSF leukocyte counts) [9]. The present study used the newer, revised criteria that are more specific for NMO diagnosis than the original criteria [10]. Contrary to the findings in Feng et al. s study,elevated protein level (15.9% of patients) and pleocytosis (18.2% of patients) in CSF were not common in our NMO patients (Table 2). Although these relatively low frequencies contrast with some reports from Western countries (which found abnormal CSF cell counts in the majority of patients in the acute phase [11,23]), our data are consistent with some previous studies carried out in Asia (27.3% of NMO patients had CSF pleocytosis in southern China [24], 25% in Japan [25], and 0 in Iran [26]). Although our data show that TBM patients may develop myelitis or optic neuritis, many of these TBM patients can be differentiated from NMO patients on the basis of demographics, course (recurrent or monophasic), CSF, and neuroimaging features. However, it is worthwhile to note that two TBM patients shared partial clinical features with NMO; one of the TBM patients had LESCLs involving holocord, similar to the characteristic spinal MRI finding in NMO, and the other had optic neuritis before anti-tuberculosis treatment. This finding supports the notion that direct TB infection of the CNS may incidentally mimic NMO in some aspects. The presence of NMO-IgG has rarely been tested in TB-related NMO cases in older studies because NMO- IgG was not discovered until 2004 [2]. Only one report has described two patients who developed NMO-like symptoms during the course of TB, but both patients showed seronegativity for NMO-IgG [7]. Consistent with this previous report, the two patients who shared partial clinical features with NMO in our study were also negative for NMO-IgG. We presume that these NMO-like symptoms with NMO-IgG negativity may differ from NMO with NMO-IgG positivity. In fact, reports have shown that NMO-IgG negative NMO differs clinically and epidemiologically from NMO-IgG positive disease and may even have a distinct pathogenesis [27]. Despite the high specificity of NMO-IgG for diagnosis of NMO [1,2,10], NMO-IgG negativity cannot rule out its diagnosis absolutely. This is because NMO-IgG levels and even serostatus can vary during follow-up [28]. Thus, diseases that mimic NMO, including CNS infections with a focus on the spinal cord and optic nerves, still have the potential to be diagnosed as NMO with NMO-IgG negativity. Recently, Miller and co-workers suggested that patients showing evidence of another explanation for NMO-like symptoms should be excluded from NMO diagnosis [12]. Therefore, it is still debatable whether NMO-like symptoms that develop during the course of TB should be considered and diagnosed as NMO. Conclusions The nature of NMO and its association with TB in the Chinese population may differ from populations from other regions. We could not confirm previous suggestions of an association between PTB and NMO. Direct TB infection of CNS may incidentally mimic NMO in some respects, but whether NMO-like symptoms that develop during the course of TB are diagnosed and treated as NMO is open to discussion. Although our findings argue against a causal association of NMO and TB, this study is limited by its retrospective design. We only focused on the relationship between NMO and active PTB and TBM because of limited datasets. A broader association of TB (for instance, distant or treated TB) and NMO should also be explored. Moreover, TB (the risk factor) does not occur at a sufficiently high frequency in either NMO patients or controls in our study to draw a definitive conclusion; therefore, a possible association between NMO and TB may be missed because of the small sample size. A larger prospective investigation with a long-term follow-up will be helpful in answering this question. Abbreviations CNS: Central nervous system; CSF: Cerebrospinal fluid; LESCL: Longitudinal extensive spinal cord lesions; MRI: Magnetic resonance imaging; NMO: Neuromyelitis optica; PTB: Active pulmonary tuberculosis; TB: Tuberculosis; TBM: Tuberculosis meningitis; TBM-MY: Tuberculosis meningitis-related myelitis; VM: Viral meningitis/meningoencephalitis. Competing interests The authors declare no conflicts of interest. Authors contribution All authors have made substantial contributions to the intellectual content of the paper. RL and XZ contributed to the conception, design, and drafting of the manuscript. AW and YD contributed to the acquisition, analysis, and interpretation of data. WQ, ZL, and XH revised the manuscript critically for intellectual content. All authors read and approved the final manuscript. Acknowledgments This study was supported by grants from the National Science Foundation of China (No ) and the graduate innovation fund of Sun Yat-Sen University (No. [2013]202). Received: 23 October 2013 Accepted: 18 February 2014 Published: 20 February 2014 References 1. Wingerchuk DM, Lennon VA, Lucchinetti CF, Pittock SJ, Weinwhenker BG: The spectrum of neuromyelitis optica. Lancet Neurol 2007, 6: Lennon VA, Wingerchuk DM, Kryzer TJ, Pittock SJ, Lucchinetti CF, Fujihara K, Nakashima I, Weinshenker BG: A serum autoantibody marker of neuromyelitis optica: distinction from multiple sclerosis. Lancet 2004, 364: Silber MH, Willcox PA, Bowen RM, Unger A: Neuromyelitis optica (Devic s syndrome) and pulmonary tuberculosis. Neurology 1990, 40: Hughes RA, Mair WG: Acute necrotic myelopathy with pulmonary tuberculosis. Brain 1977, 100: Barbizet J, Degos JD, Meyrignac C: Acute neuromyelitis optica and acute pulmonary tuberculosis (author s transl). Rev Neurol 1980, 136: French.
7 Li et al. BMC Neurology 2014, 14:33 Page 7 of 7 6. El Otmani H, Rafai MA, Moutaouakil F, EI Moutawakkil B, Gam I, EI Meziane A, Slassi I: Devic s optic neuromyelitis and pulmonary tuberculosis. Rev Mal Respir 2005, 22: French. 7. Rafai MA, Boulaajaj FZ, Gynerane M, El Moutawakkil B, Slassi I: Devic-like syndrome in the course of pulmonary tuberculosis. Acta Neurol Belg 2010, 110: Zatjirua V, Butler J, Carr J, Henning F: Neuromyelitis optica and pulmonary tuberculosis: a case control study. Int J Tuberc Lung Dis 2011, 15: Feng YQ, Guo N, Huang F, Chen X, Sun QS, Liu JX: Anti-tuberculosis treatment for Devic s neuromyelitis optica. J Clin Neurosci 2010, 17: Wingerchuk DM, Lennon VA, Pittock SJ, Lucchinetti CF, Weinshenker BG: Revised diagnostic criteria for neuromyelitis optica. Neurology 2006, 66: Wingerchuk DM, Hogancamp WF, O Brien PC, Weinshenker BG: The clinical course of neuromyelitis optica (Devic s syndrome). Neurology 1999, 53: Miller DH, Weinshenker BG, Filippi M, Banwell BL, Cohen JA, Freedman MS, Galetta SL, Hutchinson M, Johnson RT, Kappos L, Kira J, Lublin FD, McFarland HF, Montalban X, Panitch H, Richert JR, Reingold SC, Polman CH: Differential diagnosis of suspected multiple sclerosis: a consensus approach. Mult Scler 2008, 14: Hristea A, Olaru ID, Baicus C, Moroti R, Arama V, Ion M: Clinical prediction rule for differentiating tuberculous from viral meningitis. Int J Tuberc Lung Dis 2012, 16: Tuberculosis branch of Chinese medical association: Diagnosis and treatment of pulmonary tuberculosis. Chin J Tuberc Respir Dis 2001, 24: Chinese. 15. Thwaites GE, Nguyen DB, Nguyen HD, Hoang TQ, Do TT, Nguyen TC, Nguyen QH, Nguyen TT, Nguyen NH, Nguyen TN, Nguyen NL, Nguyen HD, Vu NT, Cao HH, Tran TH, Pham PM, Nguyen TD, Stepniewska K, White NJ, Tran TH, Farrar JJ: Dexamethasone for the treatment of tuberculous meningitis in adolescents and adults. N Engl J Med 2004, 351: Misu T, Fujihara K, Nakashima I, Sato S, Itoyama Y: Intractable hiccup and nausea with periaqueductal lesions in neuromyelitis optica. Neurology 2005, 65: Global tuberculosis control: WHO Report. Geneva: WHO/HTM/TB/2010.7; Yang YR, McManus DP, Gray DJ, Wang XL, Yang SK, Ross AG, Williams GM, Ellis MK: Evaluation of the tuberculosis programme in Ningxia Hui autonomous region, the People s Republic of China: a retrospective case study. BMC Public Health 2012, 12: Kabat EA, Wolf A, Bezer AE: The rapid production of acute disseminated encephalomyelitis in rhesus monkeys by injection of heterologous and homologous brain tissue with adjuvants. J Exp Med 1947, 85: Billiau A, Matthys P: Modes of action of Freund s adjuvants in experimental models of autoimmune diseases. J Leukoc Biol 2001, 70: Batista-Duharte A, Lindblad EB, Oviedo-Orta E: Progress in understanding adjuvant immunotoxicity mechanisms. Toxicol Lett 2011, 203: Jagessar SA, Kap YS, Heijmans N, van Driel N, van Straalen L, Bajramovic JJ: Induction of progressive demyelinating autoimmune encephalomyelitis in common marmoset monkeys using MOG34-56 peptide in incomplete freund adjuvant. J Neuropathol Exp Neurol 2010, 69: Zaffaroni M, Italian Devic s Study Group: Cerebrospinal fluid findings in Devic s neuromyelitis optica. Neurol Sci 2004, 25(Suppl 4):S368 S Li R, Qiu W, Lu Z, Dai Y, Wu A, Long Y, Wang Y, Bao J, Hu X: Acute transverse myelitis in demyelinating diseases among the Chinese. J Neurol 2011, 258: Yamasaki K, Horiuchi I, Minohara M, Kawano Y, Ohyagi Y, Yamada T, Mihara F, Ito H, Nishimura Y, Kira J: HLA-DPB1*0501-associated opticospinal multiple sclerosis: clinical, neuroimaging and immunogenetic studies. Brain 1999, 122(Pt 9): Kalanie H, Kholghie Y, Shamsai GR, Ghorbani M: Opticospinal multiple sclerosis in Iran. J Neurol Sci 2009, 276: Papadopoulos MC, Verkman AS: Aquaporin 4 and neuromyelitis optica. Lancet Neurol 2012, 11: Kim W, Kim SH, Kim HJ: New insights into neuromyelitis optica. J Clin Neurol 2011, 7: doi: / Cite this article as: Li et al.: Association between neuromyelitis optica and tuberculosis in a Chinese population. BMC Neurology :33. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese Multiple Sclerosis
 International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome)
 J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância. Silvia Tenembaum
 Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients
 Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
Neuromyelitis Optica: A Case Report
 Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore
 Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Patologie infiammatorie encefaliche e midollari
 Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Neuromyelitis optica (NMO), or Devic s disease, is a rare
 Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
 Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies
 Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Multiple sclerosis in Japan: Nationwide surveys over 30 years
 Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
The Etiological Spectrum of Acute Sensory Myelitis
 Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(3):227-233 / http://dx.doi.org/10.3988/jcn.2015.11.3.227 ORIGINAL ARTICLE Jae-Won Hyun a,c Jee Young Kim b Kyung Gyu Choi a Ho Jin
Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(3):227-233 / http://dx.doi.org/10.3988/jcn.2015.11.3.227 ORIGINAL ARTICLE Jae-Won Hyun a,c Jee Young Kim b Kyung Gyu Choi a Ho Jin
 Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Salintip Kunadison MD, Chaiwiwat Tungkasereerak MD, Surin Saetang MD, Pawut Mekawichai MD
 Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
RSR RSR RSR RSR RSR. ElisaRSR AQP4 Ab RSR. Aquaporin-4 Autoantibody Assay Kit
 To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Wingerchuk et al, Neurol, 2006
 Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview
 Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Professor Yasser Metwally. Neuromyelitis optica. EPIDEMIOLOGY
 180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
MYELITIS. A Mochan Neurology
 MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica
 Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
Opticospinal multiple sclerosis in Japanese
 Neurology Asia 2008; 13 : 167 173 Opticospinal multiple sclerosis in Japanese Jun-ichi Kira, Takuya Matsushita, Noriko Isobe, Takaaki Ishizu Department of Neurology, Neurological Institute, Graduate School
Neurology Asia 2008; 13 : 167 173 Opticospinal multiple sclerosis in Japanese Jun-ichi Kira, Takuya Matsushita, Noriko Isobe, Takaaki Ishizu Department of Neurology, Neurological Institute, Graduate School
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study
 Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Myelitis. Myelitis. Multiple Sclerosis (MS) Acute demyelinating syndrome (ADS) Indictions for spinal cord MRI in MS.
 Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
 The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system
 Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
ORIGINAL CONTRIBUTION. Painful Tonic Spasm in Neuromyelitis Optica. Incidence, Diagnostic Utility, and Clinical Characteristics
 ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
The updated incidences and mortalities of major cancers in China, 2011
 DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica
 Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated
 UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
Mædica - a Journal of Clinical Medicine. Neurology Department, University Emergency Hospital, Bucharest, Romania b
 MAEDICA a Journal of Clinical Medicine 2016; 11(3):245-249 Mædica - a Journal of Clinical Medicine CASE REPORTS An Uncommon Cause of Longitudinally Extensive Transverse Myelitis Catalina COCLITU a, Athena
MAEDICA a Journal of Clinical Medicine 2016; 11(3):245-249 Mædica - a Journal of Clinical Medicine CASE REPORTS An Uncommon Cause of Longitudinally Extensive Transverse Myelitis Catalina COCLITU a, Athena
Neuromyelitis optica mimics the morphology of spinal cord tumors
 The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
Contents 1 Immunology for the Non-immunologist 2 Neurology for the Non-neurologist 3 Neuroimmunology for the Non-neuroimmunologist
 1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
MRI and differential diagnosis in patients suspected of having MS
 Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Neuromyelitis optica (NMO) is characterized as a
 Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
Myelitis. Case 2. History. Examination. Mahtab Ghadiri
 Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Clinical prospective study of visual function in patients with acute optic neuritis
 Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
ORIGINAL CONTRIBUTION. The Natural History of Recurrent Optic Neuritis
 ORIGINAL CONTRIBUTION The Natural History of Recurrent Optic Neuritis Istvan Pirko, MD; Lori K. Blauwet, MD; Timothy G. Lesnick, MSc; Brian G. Weinshenker, MD, FRCP(C) Background: Optic neuritis (ON) may
ORIGINAL CONTRIBUTION The Natural History of Recurrent Optic Neuritis Istvan Pirko, MD; Lori K. Blauwet, MD; Timothy G. Lesnick, MSc; Brian G. Weinshenker, MD, FRCP(C) Background: Optic neuritis (ON) may
Thashi Chang 1,2* and Milinda Withana 2
 Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum disorders: a case series study
 Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
NMO-IgG: A specific biomarker for neuromyelitis optica
 Disease Markers 22 (2006) 197 206 197 IOS Press NMO-IgG: A specific biomarker for neuromyelitis optica Brian G. Weinshenker a,, Dean M. Wingerchuk d, Sean J. Pittock a,b, Claudia F. Lucchinetti a and Vanda
Disease Markers 22 (2006) 197 206 197 IOS Press NMO-IgG: A specific biomarker for neuromyelitis optica Brian G. Weinshenker a,, Dean M. Wingerchuk d, Sean J. Pittock a,b, Claudia F. Lucchinetti a and Vanda
MRI Imaging of Neuromyelitis Optica
 July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
MEDIA BACKGROUNDER. Multiple Sclerosis: A serious and unpredictable neurological disease
 MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
ORIGINAL CONTRIBUTION. Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression Sean J. Pittock, MD; Brian G. Weinshenker, MD; Claudia F. Lucchinetti, MD; Dean M. Wingerchuk,
ORIGINAL CONTRIBUTION Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression Sean J. Pittock, MD; Brian G. Weinshenker, MD; Claudia F. Lucchinetti, MD; Dean M. Wingerchuk,
Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases.
 Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis
 NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
MRI diagnostic criteria for multiple sclerosis: an update
 MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
PMH: No medications; Immunizations UTD No hospitalizations or surgeries Speech Delay. Birth Hx: 24 WGA, NICU x6 months
 HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
Clinical differences between young and older patients with optic neuritis
 Original Article Page 1 of 5 Clinical differences between young and older patients with optic neuritis Wenjing Luo 1 *, Qiu-Shui Huang 2 *, Jian-Feng He 2, Min Han 1, Bo Liu 1, Yi Du 2 1 The Cadre Ward
Original Article Page 1 of 5 Clinical differences between young and older patients with optic neuritis Wenjing Luo 1 *, Qiu-Shui Huang 2 *, Jian-Feng He 2, Min Han 1, Bo Liu 1, Yi Du 2 1 The Cadre Ward
Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese
 doi:10.1093/brain/awm027 Brain (2007), 130,1206^1223 Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese Takeshi Matsuoka, 1 Takuya Matsushita, 1 Yuji Kawano,
doi:10.1093/brain/awm027 Brain (2007), 130,1206^1223 Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese Takeshi Matsuoka, 1 Takuya Matsushita, 1 Yuji Kawano,
Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report
 Tohoku J. Exp. Med., 2006, Loss 209, of Aquaporin-4 269-275 in the Lesions of Neuromyelitis Optica 269 Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report Case Report
Tohoku J. Exp. Med., 2006, Loss 209, of Aquaporin-4 269-275 in the Lesions of Neuromyelitis Optica 269 Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report Case Report
NIH Public Access Author Manuscript Arch Neurol. Author manuscript; available in PMC 2012 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
Original Article Risk factors for pneumonia complication in Neuromyelitis optica spectrum disorders
 Int J Clin Exp Med 2018;11(6):6113-6118 www.ijcem.com /ISSN:1940-5901/IJCEM0063991 Original Article Risk factors for pneumonia complication in Neuromyelitis optica spectrum disorders Bingjun Zhang 1*,
Int J Clin Exp Med 2018;11(6):6113-6118 www.ijcem.com /ISSN:1940-5901/IJCEM0063991 Original Article Risk factors for pneumonia complication in Neuromyelitis optica spectrum disorders Bingjun Zhang 1*,
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Continuum (Minneap Minn) 2013;19(4):
 Review Article Address correspondence to Dr Brian G. Weinshenker, Department of Neurology, Mayo Clinic, 200 First St SW, Rochester, MN 55905, weinb@mayo.edu. Relationship Disclosure: Dr Wingerchuk receives
Review Article Address correspondence to Dr Brian G. Weinshenker, Department of Neurology, Mayo Clinic, 200 First St SW, Rochester, MN 55905, weinb@mayo.edu. Relationship Disclosure: Dr Wingerchuk receives
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology
 Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW
 Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
MULTIPLE SCLEROSIS MSJ
 431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis
 The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review.
 Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
A rare association of tuberculous longitudinally extensive transverse myelitis (LETM) with brain tuberculoma
 DOI 10.1186/s40064-015-1232-z CASE STUDY A rare association of tuberculous longitudinally extensive transverse myelitis (LETM) with brain tuberculoma Rajendra Singh Jain 1, Sunil Kumar 1* and Shankar Tejwani
DOI 10.1186/s40064-015-1232-z CASE STUDY A rare association of tuberculous longitudinally extensive transverse myelitis (LETM) with brain tuberculoma Rajendra Singh Jain 1, Sunil Kumar 1* and Shankar Tejwani
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
TECFIDERA (dimethyl fumarate) oral capsule
 TECFIDERA (dimethyl fumarate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
TECFIDERA (dimethyl fumarate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Subdural hemorrhages in acute lymphoblastic leukemia: case report and literature review
 Yin et al. Chinese Neurosurgical Journal (2016) 2:25 DOI 10.1186/s41016-016-0045-4 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Subdural hemorrhages in acute lymphoblastic leukemia:
Yin et al. Chinese Neurosurgical Journal (2016) 2:25 DOI 10.1186/s41016-016-0045-4 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Subdural hemorrhages in acute lymphoblastic leukemia:
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS
 NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
Objective: To assess the evidence for diagnostic tests and therapies for transverse myelitis (TM) and make evidence-based recommendations.
 Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
THE FIRST DESCRIPTION OF BIlateral
 CLINICAL SCIENCES Clinical Course of Optic Neuritis in Patients With Relapsing Neuromyelitis Optica Regina Maria Papais-Alvarenga, MD, MSc, PhD; Sandro Carvalho Carellos, MD, MSc; Marcos Papais Alvarenga,
CLINICAL SCIENCES Clinical Course of Optic Neuritis in Patients With Relapsing Neuromyelitis Optica Regina Maria Papais-Alvarenga, MD, MSc, PhD; Sandro Carvalho Carellos, MD, MSc; Marcos Papais Alvarenga,
An overview of NMO Spectrum Disorder and the diagnostic utility of anti-nmo antibodies
 The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
 Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Neurological update: MOG antibody disease
 https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children
 Original article A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children Sumit Sachan, Ravi Singh Chauhan, Ajay Kumar Dept of Pediatrics, Rohilkhand Medical College
Original article A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children Sumit Sachan, Ravi Singh Chauhan, Ajay Kumar Dept of Pediatrics, Rohilkhand Medical College
Atypical presentations of neuromyelitis optica
 View and review Arq Neuropsiquiatr 2011;69(5):824-828 Atypical presentations of neuromyelitis optica Douglas Sato 1,2, Kazuo Fujihara 3 ABSTRACT Neuromyelitis optica (NMO) is an inflammatory disease of
View and review Arq Neuropsiquiatr 2011;69(5):824-828 Atypical presentations of neuromyelitis optica Douglas Sato 1,2, Kazuo Fujihara 3 ABSTRACT Neuromyelitis optica (NMO) is an inflammatory disease of
Severe visual loss due to optic neuritis (ON) is the most
 Ocular Oscillations in the Neuromyelitis Optica Spectrum Rabih Hage, Jr, MD, Harold Merle, MD, Séverine Jeannin, MD, Philippe Cabre, MD Abstract: Four French West Indian women complained of oscillopsia
Ocular Oscillations in the Neuromyelitis Optica Spectrum Rabih Hage, Jr, MD, Harold Merle, MD, Séverine Jeannin, MD, Philippe Cabre, MD Abstract: Four French West Indian women complained of oscillopsia
Tuberculous meningitis diagnosis and treatment in adults: A series of 189 suspected cases
 2770 Tuberculous meningitis diagnosis and treatment in adults: A series of 189 suspected cases MENGCHUAN LUO 1, WEIFEI WANG 2, QIUMING ZENG 1, YUEBEI LUO 1, HUAN YANG 1 and XIAOSU YANG 1 1 Department of
2770 Tuberculous meningitis diagnosis and treatment in adults: A series of 189 suspected cases MENGCHUAN LUO 1, WEIFEI WANG 2, QIUMING ZENG 1, YUEBEI LUO 1, HUAN YANG 1 and XIAOSU YANG 1 1 Department of
The Transverse Myelitis Association Page 39
 The Transverse Myelitis Association Page 39 Neurosarcoidosis: Clinical, Pathological and Therapeutic Issues Carlos Pardo, M.D. Directory, Transverse Myelitis Center Department of Neurology Johns Hopkins
The Transverse Myelitis Association Page 39 Neurosarcoidosis: Clinical, Pathological and Therapeutic Issues Carlos Pardo, M.D. Directory, Transverse Myelitis Center Department of Neurology Johns Hopkins
GILENYA (fingolimod) oral capsule
 GILENYA (fingolimod) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
GILENYA (fingolimod) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow
 Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem
 Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating Optic Neuritis
 Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating
Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating
Disease of Myelin. Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019
 Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES
 NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES Dean M. Wingerchuk, MD, MSc, FRCP(C) Mayo Clinic Scottsdale, AZ Neuromyelitis optica (NMO; Devic s syndrome) consists of optic neuritis and transverse
NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES Dean M. Wingerchuk, MD, MSc, FRCP(C) Mayo Clinic Scottsdale, AZ Neuromyelitis optica (NMO; Devic s syndrome) consists of optic neuritis and transverse
CONTINUING EDUCATION MRI OF MYELITIS* JBR BTR, 2012, 95: J. Hodel 1,2, O. Outteryck 3, P. Jissendi 1, M. Zins 2, X. Leclerc 1, J.-P.
 JR TR, 2012, 95: 270-276. ONTINUING EDUTION MRI OF MYELITIS* J. Hodel 1,2, O. Outteryck 3, P. Jissendi 1, M. Zins 2, X. Leclerc 1, J.-P. Pruvo 1 MRI of myelitis The diagnosis of myelitis relies on MRI.
JR TR, 2012, 95: 270-276. ONTINUING EDUTION MRI OF MYELITIS* J. Hodel 1,2, O. Outteryck 3, P. Jissendi 1, M. Zins 2, X. Leclerc 1, J.-P. Pruvo 1 MRI of myelitis The diagnosis of myelitis relies on MRI.
Youming Long 1,2, Yangbo Zheng 1,2, Mengyu Chen 1,2, Bin Zhang 1,2, Cong Gao 1,2 *, Fulan Shan 1,2, Ning Yang 3, Yongxiang Fan 1,2.
 Serum Thyroid-Stimulating Hormone and Anti- Thyroglobulin Antibody Are Independently Associated with Lesions in Spinal Cord in Central Nervous System Demyelinating Diseases Youming Long 1,2, Yangbo Zheng
Serum Thyroid-Stimulating Hormone and Anti- Thyroglobulin Antibody Are Independently Associated with Lesions in Spinal Cord in Central Nervous System Demyelinating Diseases Youming Long 1,2, Yangbo Zheng
Analysis of prognostic significance of clinical and paraclinical indices in case of different types of acute disseminated encephalomyelitis course.
 1 2 Analysis of prognostic significance of clinical and paraclinical indices in case of different types of acute disseminated encephalomyelitis course. 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21
1 2 Analysis of prognostic significance of clinical and paraclinical indices in case of different types of acute disseminated encephalomyelitis course. 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21
Interactive Cases: Demyelinating Diseases and Mimics. Disclosures. Case 1 25 yo F with nystagmus; look for tumor 4/14/2017
 Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
AUBAGIO (teriflunomide) oral tablet
 AUBAGIO (teriflunomide) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
AUBAGIO (teriflunomide) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Paraparesis. Differential Diagnosis. Ran brauner, Tel Aviv university
 Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY
 THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
Journal of Neurology and Therapeutics
 Journal of Neurology and Therapeutics An Open Access Publisher Baranello RJ et al., J Neurol Ther 2015, 1(1):9-14 Review article Open Access Neuromyelitis optica spectrum disorders with and without aquaporin
Journal of Neurology and Therapeutics An Open Access Publisher Baranello RJ et al., J Neurol Ther 2015, 1(1):9-14 Review article Open Access Neuromyelitis optica spectrum disorders with and without aquaporin
Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians
 Neurology Asia 2006; 11 : 129 133 Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians 1 Heng-Thay CHONG MRCP, 1 Norlisah RAMLI FRCR, 2 Kwang-Ho LEE MD, 2 Byung-Joon
Neurology Asia 2006; 11 : 129 133 Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians 1 Heng-Thay CHONG MRCP, 1 Norlisah RAMLI FRCR, 2 Kwang-Ho LEE MD, 2 Byung-Joon
Difficult Diagnosis: Case History. 7 months prior, she happened to have undergone a C-spine MRI after a car accident
 Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System
 Neurology Research International Volume 2012, Article ID 460825, 13 pages doi:10.1155/2012/460825 Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System Jiwon
Neurology Research International Volume 2012, Article ID 460825, 13 pages doi:10.1155/2012/460825 Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System Jiwon
Demyelinating and Immunologic Disorders
 Demyelinating and Immunologic Disorders Nicholas Johnson, MD University of Utah Salt Lake City, Utah The nervous system may be affected by a number of autoimmune conditions. The most common of these conditions
Demyelinating and Immunologic Disorders Nicholas Johnson, MD University of Utah Salt Lake City, Utah The nervous system may be affected by a number of autoimmune conditions. The most common of these conditions
