The Etiological Spectrum of Acute Sensory Myelitis
|
|
|
- Carmel Hodges
- 5 years ago
- Views:
Transcription
1 Open Access pissn / eissn / J Clin Neurol 2015;11(3): / ORIGINAL ARTICLE Jae-Won Hyun a,c Jee Young Kim b Kyung Gyu Choi a Ho Jin Kim c Kee Duk Park a a Ewha Womans University Graduate School of Medicine, Seoul, Korea b Myongji Hospital, Goyang, Korea c National Cancer Center, Goyang, Korea Background and PurposezzAcute myelitis patients exhibiting only sensory deficits upon initial presentation are not commonly encountered in clinical practice, but they definitely exist. Since acute sensory myelitis has not been investigated previously, this study evaluated the etiological spectrum of the condition with the aim of describing the clinical characteristics thereof. MethodszzPatients with acute myelitis who presented at the Ewha Womans University Medical Center (during ) and the National Cancer Center (during ) with only sensory symptoms as first clinical features were enrolled in this study. Their medical records, electrophysiological and laboratory data, and MRI findings were analyzed retrospectively. ResultszzOf a total of 341 acute myelitis patients, 52 (15%) were identified as having acute sensory myelitis. The male-to-female ratio of these patients was 35:17, and their age at the onset of the condition was 41.7±10.5 years (mean±sd; range, years). developed in patients with multiple sclerosis (MS; 14%), neuromyelitis optica spectrum disorder (NMOSD; 17%), and acute myelitis associated with concurrent systemic diseases including Behçet s disease and cancer (6%). Despite detailed evaluation, the etiology of 33 patients with acute myelitis could not be determined. Longitudinally extensive transverse myelitis on spinal MRI and progression of the sensory level were observed most commonly in NMOSD patients (89% and 78%, respectively); however, these patients did not exhibit sensory dissociation. Residual negative sensory symptoms were observed more frequently in NMOSD patients (33%) than in those with acute myelitis of unknown cause (24%) or MS (14%). During the long-term follow-up (4.7±2.7 years) of patients who did not undergo maintenance immunotherapy, a monophasic clinical course was common in those with acute myelitis of unknown cause (76%), but not in NMOSD or MS patients. ConclusionszzAccurate identification of the diverse nature of acute sensory myelitis may assist in patient care. Key Wordszz myelitis, acute, sensory, etiology. INTRODUCTION Received September 25, 2014 Revised October 24, 2014 Accepted October 27, 2014 Correspondence Kee Duk Park, MD, PhD Ewha Womans University Graduate School of Medicine, 1071 Anyangcheon-ro, Yangcheon-gu, Seoul , Korea Tel Fax pkd1165@ewha.ac.kr The term myelitis covers heterogeneous inflammatory conditions of the spinal cord that are characterized by acute-to-subacute motor, sensory, and autonomic dysfunctions, and may have various causes. Myelitis symptoms are caused by destruction of ascending or descending pathways or the gray matter of the spinal cord. Patients with myelitis present with various sensory symptoms, with a disturbance in sensory level being the most characteristic feature. 1,2 A subset of patients with acute myelitis initially presents with only sensory symptoms. Acute myelitis with sensory deficits (or acute sensory myelitis ) is relatively rare in clinical practice, but it definitely exists. However, to the best of our knowledge, detailed clinical data on such patients have not yet been described. cc This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 2015 Korean Neurological Association 227
2 Detection of acute sensory myelitis requires careful neurological examination based on a clinical suspicion of the condition and a spinal cord MRI. The etiological spectrum of patients with acute myelitis who initially presented with sensory symptoms only is described herein, thus representing the first clinical issues encountered. METHODS Patients with acute myelitis who presented initially with only sensory symptoms at the Ewha Womans University Medical Center (EUMC) from January 1999 to June 2012 and the National Cancer Center (NCC) from September 2005 to April 2014 were enrolled. Patients who presented with sensory symptoms only, and particularly with sensory level, within 3 weeks of the nadir, and who exhibited high-level T2-weighted signals on spinal MRI were included according to the clinical judgment of physician. Sensory symptoms were divided into positive (neuropathic pain, hyperalgesia, allodynia, and paresthesia) and negative (hypesthesia and numbness) symptoms. All patients exhibiting other signs of motor or autonomic dysfunction upon careful neurological examination were excluded. Patients were examined neurologically and underwent spinal MRI within 1 month of disease onset. The medical records, electrophysiological and laboratory data, and MRI scans of the included patients were reviewed and analyzed retrospectively. All patients with neuromyelitis optica spectrum disorder (NMOSD) 3 were positive for the aquaporin 4 (AQP4) antibody, and all multiple sclerosis (MS) patients met the McDonald criteria. 4,5 Patients with MS and acute myelitis of unknown cause were confirmed rigorously to be negative for serum AQP4 antibody via repeat assays using three different methods: the AQP4-M23 isoform commercial cell-based assay (CBA; Euroimmun, Luebeck, Germany), 6 an in-house CBA at Tohoku University, 7 and an inhouse enzyme-linked immunosorbent assay at the NCC. 8 To ensure the idiopathic nature of acute myelitis of unknown cause, patients in whom vascular and compressive lesions were identified by spinal MRI were excluded, and patients were screened for infections and metabolic problems. After this detailed evaluation, 33 patients were ultimately diagnosed with acute myelitis of unknown etiology. Of these patients, eight were not tested for AQP4 antibody because they visited our clinic prior to the NMOSD era (2004). However, all eight patients exhibited a monophasic clinical course over a 2-year follow-up period, and no involvement of the optic nerve or brain were observed, which would have supported diagnoses of NMOSD or MS, respectively. The Institutional Review Board of each participating center approved the study protocol and waived the need for informed consent since all of the data were anonymized. RESULTS Of 341 patients with acute myelitis, 52 patients (15%) satisfying the eligibility criteria for acute sensory myelitis were enrolled at the EUMC and NCC (12 of 108 EUMC patients over 13 years, and 40 of 233 NCC patients over 9 years). The age at disease onset was 41.7±10.5 years (mean±sd; range, years), and the follow-up duration was 4.7±2.7 years (range, 2 11 years); the male-to-female ratio was 35:17. The clinical characteristics and spinal MRI findings of the acute sensory myelitis patients are listed in Table 1. Etiologies The acute sensory myelitis patients had MS (n=7, 14%), NMOSD (n=9, 17%), or acute myelitis with concurrent systemic diseases, including Behçet s disease and cancer (breast and colon cancer; n=3, 6%). After detailed evaluation, the etiology of the condition remained unknown for 33 patients (Table 1). Comparison of the characteristics of acute sensory myelitis with different etiologies Table 2 provides the characteristics of acute sensory myelitis with different entities. The mean age of onset, and follow-up duration did not differ significantly among the groups of patients with different clinical entities. In patients not undergoing maintenance immunotherapy, a monophasic clinical course was observed exclusively in those with acute myelitis of unknown cause (76%), and thus not in those with MS or NMOSD. The two patients with concurrent cancer did not relapse during follow-up, even though they did not receive maintenance immunotherapy, rather only anticancer therapy. There were no significant differences in sensory symptoms or signs among patients with diseases of different etiologies. However, a trend toward the development of negative sensory symptoms was evident in MS (71%) and NMOSD (78%) patients compared with those with acute myelitis of unknown cause (67%). Furthermore, the thoracic level tended to be involved preferentially in NMOSD patients (89%); ascending and descending progression of the sensory level was also observed most commonly in these patients (78%). In contrast, dissociated sensory symptoms were not noted in NMOSD patients. Asymmetric sensory involvement and a normal deep tendon reflex were common across the etiological spectrum. In spinal MRI scans obtained during the acute phase, lesion levels did not differ significantly among patients with different disease entities. However, cervical lesions tended to be 228 J Clin Neurol 2015;11(3):
3 Hyun JW et al. Table 1. Demographics and clinical findings of acute sensory myelitis (total, n=52) Age at onset (years) 41.7±10.5 (24 72) Gender ratio (male:female) 35:17 Etiology (n, %) Multiple sclerosis 7 (14) Neuromyelitis optica spectrum disorder 9 (17) with unknown cause 33 (63) Others (with systemic diseases) 3 (6) Follow-up periods (years) 4.7±2.7 (2 11) Monophasic clinical course (n, %) 25 (48) Sensory symptoms (n, %) Sensory level Cervical 17 (33) Thoracic 26 (50) Lumbar 9 (17) Positive or negative symptoms Positive 15 (29) Negative 6 (12) Both 31 (59) Symmetric symptom development Symmetric 13 (25) Asymmetric 39 (75) Sensory level progression Ascending pattern 18 (35) Descending pattern 9 (17) None 25 (48) Neurological signs (n, %) Sensory dissociation Yes (pain and temperature only) 12/47 (26) No 35/47 (74) Deep tendon reflex Normoactive 26/40 (65) Hyperactive 13/40 (33) Hypoactive 1/40 (2) Lhermitte s sign 12/17 (71) Spinal MRI (n, %) Lesion level Cervical 20 (38) Cervicothoracic 2 (4) Thoracic 30 (58) Lesion length (vertebral segments) 2.8±1.4 (1 8) Axial location Central 17 (33) Peripheral 11 (21) Both 24 (46) Enhancement 41/44 (93) Acute treatment (n, %) Steroid 48 (92) None 4 (8) Recovery after acute phase (n, %) Table 1. Demographics and clinical findings of acute sensory myelitis (total, n=52) (continued) Complete 8 (15) Partial 29 (56) None 15 (29) Residual sensory symptoms after acute phase (n, %) Positive symptoms 26 (50) Negative symptoms 4 (8) Both symptoms 9 (17) None 13 (25) Symptomatic treatment (n, %) 29 (56) Immunotherapy for maintenance (n, %) 29 (56) Data are mean±sd (range) or n (%) values. common in MS patients (71%), whereas thoracic lesions were usually observed in NMOSD patients (89%). The mean NMOSD lesion length on spinal MRI was significantly greater than that of MS patients (p=0.036). Furthermore, longitudinally extensive transverse myelitis (LETM) extending over three vertebral segments on spinal MRI was observed more commonly among NMOSD patients (89%) than in those with MS (14%) or acute myelitis of unknown cause (52%; p=0.019). Otherwise, axial spinal MRI revealed more peripheral lesions in MS patients than in those with the other disease entities (p=0.002) (Fig. 1). Brain MRI was performed on 44 patients during followup. A greater proportion of MS patients had brain MRI lesions (100%) compared with patients with NMOSD (22%) or acute myelitis of unknown cause (19%; p<0.001). Evaluation of sensory evoked potentials revealed that conduction defects tended to occur more commonly in the MS patients (50%). Visually evoked potentials were assessed in 37 patients, and conduction defects were evident more frequently in NMOSD patients (40%) than in those with MS (14%) or acute myelitis of unknown cause (0%; p=0.036). Upon cerebrospinal fluid (CSF) evaluation during the acute stage, an immunoglobulin G (IgG) index of >0.7 was observed only in MS patients (67%). No oligoclonal band was detected, but isoelectric focusing (IEF) was not performed. During follow-up, all NMOSD patients were positive for the AQP4 antibody. Autoimmune laboratory data were abnormal in 6% of all patients (3/52), antinuclear antibodies were detected in one patient with MS and one with acute myelitis of unknown cause, and the anti-sjörgen s syndrome A antibody status was positive in one NMOSD patient. Acute treatment with high-dose steroids (methylprednisolone; 1 g/day) was usually prescribed for patients across the etiological spectrum. Partial recovery was observed commonly after such acute treatment, and residual negative sensory symptoms were more common in NMOSD patients (33%) than in those with acute myelitis of unknown cause 229
4 Table 2. Comparison of the characteristics of the different etiologies of acute sensory myelitis Multiple sclerosis (n=7) Neuromyelitis optica spectrum disorder (n=9) with unknown cause (n=33) with concurrent systemic diseases (n=3) p-value Age at onset (years) 41±16 41±11 42±9 44±18 NS Gender ratio (female:male) 4:3 8:1 4:29* 1: Follow-up (years) 3.8± ± ± ±1.2 NS Monophasic course (n, %) Overall 2 (29) 1 (11) 19 (58)* 3 (100) Without maintenance immunotherapy 0/0 (0) 0/0 (0) 16/21 (76)* 2/2 (100) <0.001 Sensory symptoms (n, %) Positive/negative symptoms Positive 2 (29) 2 (22) 11 (33) 0 (0) NS Negative 1 (14) 2 (22) 3 (9) 0 (0) NS Both 4 (57) 5 (56) 19 (58) 3 (100) NS Sensory level Cervical 3 (43) 1 (11) 13 (39) 0 (0) NS Thoracic 3 (43) 8 (89) 13 (39) 2 (67) NS Lumbar 1 (14) 0 (0) 7 (22) 1 (33) NS Symmetry Symmetric 1 (14) 3 (33) 7 (21) 2 (67) NS Asymmetric 6 (86) 6 (67) 26 (79) 1 (33) NS Level progression Ascending 3 (43) 3 (33) 11 (33) 1 (33) NS Descending 0 (0) 4 (45) 5 (15) 0 (0) NS None 4 (57) 2 (22) 17 (52) 2 (67) NS Neurological signs (n, %) Sensory dissociation Yes 2/6 (33) 0/7 (0) 10/31 (32) 0/3 (0) NS No 4/6 (67) 7/7 (100) 21/31 (68) 3/3 (100) NS Deep tendon reflex Normoactive 3/5 (60) 4/5 (80) 18/27 (67) 1/3 (33) NS Hyperactive 2/5 (40) 1 (20) 8/27 (30) 2/3 (67) NS Hypoactive 0 (0) 0 (0) 1/27 (3) 0 (0) NS Spinal MRI (n, %) Lesion level Cervical 4 (57) 1 (11) 15 (46) 0 (0) NS Cervicothoracic 1 (14) 0 (0) 1 (3) 0 (0) NS Thoracic 2 (29) 8 (89) 17 (51) 3 (100) NS Lesion length 1.9±1.0* 3.7±1.1* 2.6± ± LETM 1/7 (14) 8/9 (89)* 17/33 (52) 1/3 (33) Axial location Central 0 (0) 4 (44) 11 (33) 2 (67) Peripheral 6 (86)* 0 (0) 5 (15) 0 (0) Both 1 (14) 5 (56) 17 (52) 1 (33) Enhancement 5/6 (83) 8/8 (100) 26/27 (96) 2/3 (67) NS Brain MRI lesions (n, %) 7/7 (100)* 2/9 (22) 5/26 (19) 0/2 (0) <0.001 Abnormality on SEPs (n, %) 3/6 (50) 0/2 (0) 2/15 (13) 0/1 (0) NS Abnormality on VEPs (n, %) 1/7 (14) 2/5 (40)* 0/23 (0) 0/2 (0) CSF (n, %) 230 J Clin Neurol 2015;11(3):
5 Hyun JW et al. Table 2. Comparison of the characteristics of the different etiologies of acute sensory myelitis (continued) Multiple sclerosis (n=7) Neuromyelitis optica spectrum disorder (n=9) with unknown cause (n=33) with concurrent systemic diseases (n=3) p-value Pleocytosis 1/5 (20) 2/8 (25) 5/32 (16) 0/2 (0) NS Increased protein 1/5 (20) 1/7 (14) 6/32 (19) 0/2 (0) NS IgG index >0.7 4/6 (67)* 0/7 (0) 0/27 (0) 0/1 (0) Oligoclonal band 0/4 (0) 0/8 (0) 2/22 (9) 0/1 (0) NS Serum (n, %) Aquaporin-4 antibody 0/7 (0) 9/9 (100)* 0/25 (0) 0/2 (0) <0.001 Autoimmune antibodies 1/7 (14) 1/9 (11) 1/33 (3) 0/3 (0) NS Antinuclear antibody NS Anti-SSA antibody NS Acute treatment (n, %) Steroid 7 (100) 8 (89) 30 (91) 3 (100) NS None 0 (0) 1 (11) 3 (9) 0 (0) NS Recovery after acute treatment (n, %) Complete 3 (42) 1 (11) 8 (24) 0 (0) NS Partial 2 (29) 7 (78) 14 (43) 2 (67) NS None 2 (29) 1 (11) 11 (33) 1 (33) NS Residual sensory symptoms after acute treatment (n, %) Positive 3 (43) 5 (56) 17 (52) 2 (67) NS Negative 0 (0) 2 (22) 2 (6) 0 (0) NS Both 1 (14) 1 (11) 6 (18) 1 (33) NS None 3 (43) 1 (11) 8 (24) 0 (0) NS Symptomatic treatment (n, %) 4 (57) 5 (56) 19 (58) 1 (33) NS Immunotherapy (n, %) 7 (100)* 9 (100)* 12 (36) 1 (33) <0.001 Except where indicated otherwise, the data are mean±sd values or n (%) values. *Significantly different values among entities. CSF: cerebrospinal fluid, IgG: immunoglobulin G, LETM: longitudinally extensive transverse myelitis, NS: not significant, SEPs: sensory evoked potentials, SSA: Sjörgen s syndrome A, VEPs: visual evoked potentials. (24%) or MS (14%). Immunotherapy to prevent relapse was prescribed for MS and NMOSD patients, and for those with relapsing myelitis of unknown cause. DISCUSSION Of the acute sensory myelitis patients studied herein, some ultimately developed MS (14%), or interestingly, even NMOSD (17%), which require long-term immunotherapy. Spinal MRI revealed variations in lesion length (ranging from one to eight vertebral segments), and LETM was also observed. LETM and progression of the sensory level, which may reflect the presence of severe inflammation, were most commonly observed in NMOSD patients (89% and 78%, respectively). In contrast, NMOSD patients did not exhibit sensory dissociation. Patients commonly received steroid therapy during the acute phase (92%), and residual negative sensory symptoms, which represent disabilities, were observed more frequently in NMOSD (33%) patients than in those with acute myelitis of unknown cause (24%) or MS (14%). During the long-term follow-up (4.7±2.7 years) of patients not undergoing maintenance immunotherapy, a monophasic clinical course was common in those with acute myelitis of unknown cause (76%), but not in patients with NMOSD or MS. Brain MRI (in 100% of MS patients), and sensory evoked potentials (in 50% of MS patients) revealing defects in the posterior column pathway were commonly observed abnormalities in MS patients. Assessment of visually evoked potentials usually revealed conduction defects in NMOSD patients (40%). IgG index abnormalities (scores of >0.7) were observed only in MS patients (67%), but no oligoclonal band was detected, probably because of a technical limitation (IEF was not performed). 9 The etiological or concurrent diseases suffered by our pa
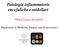
6 A B C Fig. 1. High signal lesions (arrowheads) on T2-weighted spinal MRI (transverse, longitudinal section) of patients with multiple sclerosis (A), neuromyelitis optica spectrum disorder (B), and acute myelitis of unknown cause (C). tients included MS, NMOSD, Behçet s disease, and cancer. After careful evaluation, the diseases of 33 patients who tended to present with monophasic clinical courses were ultimately categorized as unknown etiology. The specific involvement of the sensory system suggests that involvement of specific tracts and immunological processes contribute to the pathogenic mechanisms of the disease. For example, some patients with paraneoplastic syndromes, such as amphiphysin autoimmunity, exhibited tract-restricted signal abnormalities on spinal MRI. Although the patient who was positive for amphiphysin antibody exhibited predominantly motor system involvement, this constitutes evidence that the immune response is anatomically confined. Thus, paraneoplastic myelopathy may be another cause of acute sensory myelitis. 10 The retrospective nature of the present study rendered it impossible to check for paraneoplastic antibodies, but two patients had concurrent breast or colon cancer. Moreover, atopic myelitis, which triggers prominent sensory symptoms with or without mild motor weakness, 11,12 exhibits similar features, and may cause acute sensory myelitis. Further prospective studies with larger cohorts and longer follow-up periods may answer the question of the unknown etiology of acute sensory myelitis. The retrospective nature of this study was associated with methodological shortcomings and limitations due to the participation of only two referral centers. Thus, the observed etiological spectrum may be biased by the inclusion of a relatively small proportion of MS patients, possibly due to referral bias or patient s ethnicity. In addition, some patients were not subjected to paraclinical evaluation of CSF properties and/or were not evaluated electrophysiologically. Finally, sensory recovery was estimated by the treating physicians not always using a defined scale. The etiological spectrum of patients presenting initially with acute sensory myelitis alone was described in this study. An understanding of the diverse nature of acute sensory myelitis is important when seeking to improve the quality of life of these patients. Conflicts of Interest Dr. Hyun, Kim JY, Choi, Park report no disclosures. Dr. Kim HJ has given talks, consulted and received honoraria and/or research support from Bayer Schering Pharma, Biogen Idec, Genzyme, Kael-Gem Vax, Merck Sereno, Novartis, Teva-Handok, and UCB. He serves on a steering committee for MedImmune. 232 J Clin Neurol 2015;11(3):
7 Hyun JW et al. REFERENCES 1. Transverse Myelitis Consortium Working Group. Proposed diagnostic criteria and nosology of acute transverse myelitis. Neurology 2002; 59: Frohman EM, Wingerchuk DM. Clinical practice. Transverse myelitis. N Engl J Med 2010;363: Wingerchuk DM, Lennon VA, Lucchinetti CF, Pittock SJ, Weinshenker BG. The spectrum of neuromyelitis optica. Lancet Neurol 2007; 6: Polman CH, Reingold SC, Edan G, Filippi M, Hartung HP, Kappos L, et al. Diagnostic criteria for multiple sclerosis: 2005 revisions to the McDonald Criteria. Ann Neurol 2005;58: Polman CH, Reingold SC, Banwell B, Clanet M, Cohen JA, Filippi M, et al. Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 2011;69: Jarius S, Probst C, Borowski K, Franciotta D, Wildemann B, Stoecker W, et al. Standardized method for the detection of antibodies to aquaporin-4 based on a highly sensitive immunofluorescence assay employing recombinant target antigen. J Neurol Sci 2010;291: Sato DK, Nakashima I, Takahashi T, Misu T, Waters P, Kuroda H, et al. Aquaporin-4 antibody-positive cases beyond current diagnostic criteria for NMO spectrum disorders. Neurology 2013;80: Kim W, Lee JE, Li XF, Kim SH, Han BG, Lee BI, et al. Quantitative measurement of anti-aquaporin-4 antibodies by enzyme-linked immunosorbent assay using purified recombinant human aquaporin-4. Mult Scler 2012;18: Freedman MS, Thompson EJ, Deisenhammer F, Giovannoni G, Grimsley G, Keir G, et al. Recommended standard of cerebrospinal fluid analysis in the diagnosis of multiple sclerosis: a consensus statement. Arch Neurol 2005;62: Pittock SJ, Lucchinetti CF, Parisi JE, Benarroch EE, Mokri B, Stephan CL, et al. Amphiphysin autoimmunity: paraneoplastic accompaniments. Ann Neurol 2005;58: Kira J, Yamasaki K, Kawano Y, Kobayashi T. Acute myelitis associated with hyperigeemia and atopic dermatitis. J Neurol Sci 1997;148: Yoon JH, Joo IS, Li WY, Sohn SY. Clinical and laboratory characteristics of atopic myelitis: Korean experience. J Neurol Sci 2009;285:
Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome)
 J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients
 Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese Multiple Sclerosis
 International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
Neuromyelitis optica (NMO), or Devic s disease, is a rare
 Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore
 Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated
 UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
Myelitis. Case 2. History. Examination. Mahtab Ghadiri
 Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância. Silvia Tenembaum
 Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
ORIGINAL CONTRIBUTION. Painful Tonic Spasm in Neuromyelitis Optica. Incidence, Diagnostic Utility, and Clinical Characteristics
 ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
MYELITIS. A Mochan Neurology
 MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
Neuromyelitis Optica: A Case Report
 Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system
 Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica
 Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
Salintip Kunadison MD, Chaiwiwat Tungkasereerak MD, Surin Saetang MD, Pawut Mekawichai MD
 Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
Patologie infiammatorie encefaliche e midollari
 Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Objective: To assess the evidence for diagnostic tests and therapies for transverse myelitis (TM) and make evidence-based recommendations.
 Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
 The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Multiple sclerosis in Japan: Nationwide surveys over 30 years
 Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview
 Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
RSR RSR RSR RSR RSR. ElisaRSR AQP4 Ab RSR. Aquaporin-4 Autoantibody Assay Kit
 To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
Wingerchuk et al, Neurol, 2006
 Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS
 NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies
 Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
 Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis
 NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
An overview of NMO Spectrum Disorder and the diagnostic utility of anti-nmo antibodies
 The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
Immunoadsorption in patients with neuromyelitis optica spectrum disorder
 646332TAN0010.1177/1756285616646332Therapeutic Advances in Neurological DisordersS Faissner, J Nikolayczik research-article2016 Therapeutic Advances in Neurological Disorders Original Research Immunoadsorption
646332TAN0010.1177/1756285616646332Therapeutic Advances in Neurological DisordersS Faissner, J Nikolayczik research-article2016 Therapeutic Advances in Neurological Disorders Original Research Immunoadsorption
Neuroimaging and Other Biomarkers. MRI for Diagnosis, Prognosis and Treatment Decisions in MS
 Neuroimaging and Other Biomarkers MRI for Diagnosis, Prognosis and Treatment Decisions in MS Eric Klawiter, MD MSc Massachusetts General Hospital May 30, 2014 Disclosures and Funding Disclosures: Consulting
Neuroimaging and Other Biomarkers MRI for Diagnosis, Prognosis and Treatment Decisions in MS Eric Klawiter, MD MSc Massachusetts General Hospital May 30, 2014 Disclosures and Funding Disclosures: Consulting
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis
 The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
 Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology
 Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study
 Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Paraparesis. Differential Diagnosis. Ran brauner, Tel Aviv university
 Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica
 Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
Neuromyelitis optica mimics the morphology of spinal cord tumors
 The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
 Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Neuromyelitis optica (NMO) is characterized as a
 Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
ORIGINAL CONTRIBUTION. Multiple Sclerosis That Is Progressive From the Time of Onset
 ORIGINAL CONTRIBUTION Multiple Sclerosis That Is Progressive From the Time of Onset Clinical Characteristics and Progression of Disability P. B. Andersson, MBChB, DPhil; E. Waubant, MD; L. Gee, MPH; D.
ORIGINAL CONTRIBUTION Multiple Sclerosis That Is Progressive From the Time of Onset Clinical Characteristics and Progression of Disability P. B. Andersson, MBChB, DPhil; E. Waubant, MD; L. Gee, MPH; D.
ORIGINAL CONTRIBUTION. Long-term Follow-up of Acute Partial Transverse Myelitis
 ORIGINAL CONTRIBUTION Long-term Follow-up of Acute Partial Transverse Myelitis Bertrand Bourre, MD; Hélène Zéphir, MD; Jean-Claude Ongagna, CRA; Charlotte Cordonnier, MD, PhD; Nicolas Collongues, MD; Stephanie
ORIGINAL CONTRIBUTION Long-term Follow-up of Acute Partial Transverse Myelitis Bertrand Bourre, MD; Hélène Zéphir, MD; Jean-Claude Ongagna, CRA; Charlotte Cordonnier, MD, PhD; Nicolas Collongues, MD; Stephanie
MULTIPLE SCLEROSIS PROFILE
 MULTIPLE SCLEROSIS PROFILE What is Multiple Sclerosis? Multiple sclerosis (MS) is a chronic, inflammatory disease of unknown etiology that involves an immune-mediated attack on the central nervous system
MULTIPLE SCLEROSIS PROFILE What is Multiple Sclerosis? Multiple sclerosis (MS) is a chronic, inflammatory disease of unknown etiology that involves an immune-mediated attack on the central nervous system
Neurological update: MOG antibody disease
 https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
Clinical Application of 2017 McDonald Diagnostic Criteria for Multiple Sclerosis
 JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2018;14(3):387-392 / https://doi.org/10.3988/jcn.2018.14.3.387 ORIGINAL ARTICLE Clinical Application of 2017 McDonald Diagnostic Criteria
JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2018;14(3):387-392 / https://doi.org/10.3988/jcn.2018.14.3.387 ORIGINAL ARTICLE Clinical Application of 2017 McDonald Diagnostic Criteria
Clinical insights for early detection of acute transverse myelitis in the emergency department
 Clin Exp Emerg Med 2015;2(1):44-50 http://dx.doi.org/10.15441/ceem.14.034 Clinical insights for early detection of acute transverse myelitis in the emergency department Yo Huh, Eun-Jung Park, Ju-Won Jung,
Clin Exp Emerg Med 2015;2(1):44-50 http://dx.doi.org/10.15441/ceem.14.034 Clinical insights for early detection of acute transverse myelitis in the emergency department Yo Huh, Eun-Jung Park, Ju-Won Jung,
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW
 Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Relation between the Peripherofacial Psoriasis and Scalp Psoriasis
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
MULTIPLE SCLEROSIS MSJ
 431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
Myelopathies: Autoimmune and other mimickers of MS. Eoin P. Flanagan, MB, BCh Assistant Professor of Neurology Mayo Clinic, Rochester, MN DISCLOSURE
 Myelopathies: Autoimmune and other mimickers of MS Eoin P. Flanagan, MB, BCh Assistant Professor of Neurology Mayo Clinic, Rochester, MN 2011 MFMER slide-1 DISCLOSURE Relevant Financial Relationship(s)
Myelopathies: Autoimmune and other mimickers of MS Eoin P. Flanagan, MB, BCh Assistant Professor of Neurology Mayo Clinic, Rochester, MN 2011 MFMER slide-1 DISCLOSURE Relevant Financial Relationship(s)
Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases.
 Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
Negative prognostic impact of MRI spinal lesions in the early stages of relapsing remitting multiple sclerosis
 Original Article Negative prognostic impact of MRI spinal lesions in the early stages of relapsing remitting multiple sclerosis E D Amico, F Patti, C Leone, S Lo Fermo and M Zappia Multiple Sclerosis Journal
Original Article Negative prognostic impact of MRI spinal lesions in the early stages of relapsing remitting multiple sclerosis E D Amico, F Patti, C Leone, S Lo Fermo and M Zappia Multiple Sclerosis Journal
Real-World Effectiveness of Disease-Modifying Therapies in Korean Patients with Relapsing Multiple Sclerosis
 Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2018 ORIGINAL ARTICLE Real-World Effectiveness of Disease-Modifying Therapies in Korean Patients with Relapsing Multiple Sclerosis Su-Hyun
Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2018 ORIGINAL ARTICLE Real-World Effectiveness of Disease-Modifying Therapies in Korean Patients with Relapsing Multiple Sclerosis Su-Hyun
Anti-MOG antibodies are present in a subgroup of patients with a neuromyelitis optica phenotype
 Pröbstel et al. Journal of Neuroinflammation (2015) 12:46 DOI 10.1186/s12974-015-0256-1 JOURNAL OF NEUROINFLAMMATION SHORT REPORT Open Access Anti-MOG antibodies are present in a subgroup of patients with
Pröbstel et al. Journal of Neuroinflammation (2015) 12:46 DOI 10.1186/s12974-015-0256-1 JOURNAL OF NEUROINFLAMMATION SHORT REPORT Open Access Anti-MOG antibodies are present in a subgroup of patients with
MRI and differential diagnosis in patients suspected of having MS
 Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Pattern II and pattern III MS are entities distinct from pattern I MS: evidence from cerebrospinal fluid analysis
 Jarius et al. Journal of Neuroinflammation (2017) 14:171 DOI 10.1186/s12974-017-0929-z RESEARCH Pattern II and pattern III MS are entities distinct from pattern I MS: evidence from cerebrospinal fluid
Jarius et al. Journal of Neuroinflammation (2017) 14:171 DOI 10.1186/s12974-017-0929-z RESEARCH Pattern II and pattern III MS are entities distinct from pattern I MS: evidence from cerebrospinal fluid
MRI diagnostic criteria for multiple sclerosis: an update
 MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
PMH: No medications; Immunizations UTD No hospitalizations or surgeries Speech Delay. Birth Hx: 24 WGA, NICU x6 months
 HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
AND RELAPSING REMITTING COURSES
 original research THE VALUE OF INTRATHECAL MRZ REACTION AND OLIGOCLONAL IgG BANDS FOR DISCRIMINATION BETWEEN THE PRIMARY PROGRESSIVE AND RELAPSING REMITTING COURSES OF MULTIPLE SCLEROSIS Štourač P. 1,
original research THE VALUE OF INTRATHECAL MRZ REACTION AND OLIGOCLONAL IgG BANDS FOR DISCRIMINATION BETWEEN THE PRIMARY PROGRESSIVE AND RELAPSING REMITTING COURSES OF MULTIPLE SCLEROSIS Štourač P. 1,
Professor Yasser Metwally. Neuromyelitis optica. EPIDEMIOLOGY
 180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
Treatment Outcomes With Rituximab in 100 Patients With Neuromyelitis Optica. on the Therapeutic Response to Rituximab
 Research Original Investigation Treatment Outcomes With Rituximab in 100 Patients With Neuromyelitis Optica Influence of FCGR3A Polymorphisms on the Therapeutic Response to Rituximab Su-Hyun Kim, MD; In
Research Original Investigation Treatment Outcomes With Rituximab in 100 Patients With Neuromyelitis Optica Influence of FCGR3A Polymorphisms on the Therapeutic Response to Rituximab Su-Hyun Kim, MD; In
Opticospinal multiple sclerosis in Japanese
 Neurology Asia 2008; 13 : 167 173 Opticospinal multiple sclerosis in Japanese Jun-ichi Kira, Takuya Matsushita, Noriko Isobe, Takaaki Ishizu Department of Neurology, Neurological Institute, Graduate School
Neurology Asia 2008; 13 : 167 173 Opticospinal multiple sclerosis in Japanese Jun-ichi Kira, Takuya Matsushita, Noriko Isobe, Takaaki Ishizu Department of Neurology, Neurological Institute, Graduate School
A new classification system of nasal contractures
 Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
MRI Imaging of Neuromyelitis Optica
 July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
Supplementary Online Content
 Supplementary Online Content Schlaeger R, Papinutto N, Zhu AH, et al. Association between thoracic spinal cord gray matter atrophy and disability in multiple sclerosis. JAMA Neurol. Published online June
Supplementary Online Content Schlaeger R, Papinutto N, Zhu AH, et al. Association between thoracic spinal cord gray matter atrophy and disability in multiple sclerosis. JAMA Neurol. Published online June
Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D
 Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D Maureen A. Mealy, PhD(c), RN; Audra Boscoe, PhD; Jaime Caro, MDCM; Michael Levy, MD, PhD From the Department of Neurology,
Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D Maureen A. Mealy, PhD(c), RN; Audra Boscoe, PhD; Jaime Caro, MDCM; Michael Levy, MD, PhD From the Department of Neurology,
Syndrome of inappropriate antidiuretic hormone secretion associated with seronegative neuromyelitis optica spectrum disorder
 Case Report Kidney Res Clin Pract 36:100-104, 2017(1) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2017.36.1.100 Kidney Research and Clinical Practice Syndrome of inappropriate antidiuretic
Case Report Kidney Res Clin Pract 36:100-104, 2017(1) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2017.36.1.100 Kidney Research and Clinical Practice Syndrome of inappropriate antidiuretic
Multiple sclerosis mimics: Diagnostic error and management decisions
 Multiple sclerosis mimics: Diagnostic error and management decisions John R Rinker, II, MD Mitchell Wallin, MD Paralyzed Veterans Summit, Washington Harbor, MD August 30, 2017 Disclosures Dr. Rinker and
Multiple sclerosis mimics: Diagnostic error and management decisions John R Rinker, II, MD Mitchell Wallin, MD Paralyzed Veterans Summit, Washington Harbor, MD August 30, 2017 Disclosures Dr. Rinker and
TECFIDERA (dimethyl fumarate) oral capsule
 TECFIDERA (dimethyl fumarate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
TECFIDERA (dimethyl fumarate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
GILENYA (fingolimod) oral capsule
 GILENYA (fingolimod) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
GILENYA (fingolimod) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
Association between neuromyelitis optica and tuberculosis in a Chinese population
 Li et al. BMC Neurology 2014, 14:33 RESEARCH ARTICLE Open Access Association between neuromyelitis optica and tuberculosis in a Chinese population Rui Li, Xiaonan Zhong, Wei Qiu, Aimin Wu, Yongqiang Dai,
Li et al. BMC Neurology 2014, 14:33 RESEARCH ARTICLE Open Access Association between neuromyelitis optica and tuberculosis in a Chinese population Rui Li, Xiaonan Zhong, Wei Qiu, Aimin Wu, Yongqiang Dai,
MEDIA BACKGROUNDER. Multiple Sclerosis: A serious and unpredictable neurological disease
 MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review.
 Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
Neuroimmunology testing services
 Neuroimmunology testing services Neuroimmunology Quest Diagnostics is your source for neuroimmunological testing with expanded offerings for several autoimmune neurological disorders Neuroimmunology is
Neuroimmunology testing services Neuroimmunology Quest Diagnostics is your source for neuroimmunological testing with expanded offerings for several autoimmune neurological disorders Neuroimmunology is
Epidemiologic characteristics of cervical cancer in Korean women
 Review Article J Gynecol Oncol Vol. 25, No. 1:70-74 pissn 2005-0380 eissn 2005-0399 Epidemiologic characteristics of cervical cancer in Korean women Hyun-Joo Seol, Kyung-Do Ki, Jong-Min Lee Department
Review Article J Gynecol Oncol Vol. 25, No. 1:70-74 pissn 2005-0380 eissn 2005-0399 Epidemiologic characteristics of cervical cancer in Korean women Hyun-Joo Seol, Kyung-Do Ki, Jong-Min Lee Department
Interferon-β-related tumefactive brain lesion in a Caucasian patient with neuromyelitis optica and clinical stabilization with tocilizumab
 Harmel et al. BMC Neurology (2014) 14:247 DOI 10.1186/s12883-014-0247-3 CASE REPORT Open Access Interferon-β-related tumefactive brain lesion in a Caucasian patient with neuromyelitis optica and clinical
Harmel et al. BMC Neurology (2014) 14:247 DOI 10.1186/s12883-014-0247-3 CASE REPORT Open Access Interferon-β-related tumefactive brain lesion in a Caucasian patient with neuromyelitis optica and clinical
Myelitis. Myelitis. Multiple Sclerosis (MS) Acute demyelinating syndrome (ADS) Indictions for spinal cord MRI in MS.
 Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
NIH Public Access Author Manuscript Arch Neurol. Author manuscript; available in PMC 2012 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
Magnetic Resonance Imaging in the Acquired Demyelinating Disorders: A Pediatric Cohort Study
 Journal of Pharmacy and Pharmacology 6 (2018) 20-31 doi: 10.17265/2328-2150/2018.01.003 D DAVID PUBLISHING Magnetic Resonance Imaging in the Acquired Demyelinating Disorders: A Pediatric Cohort Study Santa
Journal of Pharmacy and Pharmacology 6 (2018) 20-31 doi: 10.17265/2328-2150/2018.01.003 D DAVID PUBLISHING Magnetic Resonance Imaging in the Acquired Demyelinating Disorders: A Pediatric Cohort Study Santa
AUBAGIO (teriflunomide) oral tablet
 AUBAGIO (teriflunomide) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
AUBAGIO (teriflunomide) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs. MRI Diagnostic Red Flags
 Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs MRI Diagnostic Red Flags UBC MS and NMO Research Programs LEARNING OBJECTIVES By the end of this presentation,
Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs MRI Diagnostic Red Flags UBC MS and NMO Research Programs LEARNING OBJECTIVES By the end of this presentation,
Thashi Chang 1,2* and Milinda Withana 2
 Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY
 THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
Youming Long 1,2, Yangbo Zheng 1,2, Mengyu Chen 1,2, Bin Zhang 1,2, Cong Gao 1,2 *, Fulan Shan 1,2, Ning Yang 3, Yongxiang Fan 1,2.
 Serum Thyroid-Stimulating Hormone and Anti- Thyroglobulin Antibody Are Independently Associated with Lesions in Spinal Cord in Central Nervous System Demyelinating Diseases Youming Long 1,2, Yangbo Zheng
Serum Thyroid-Stimulating Hormone and Anti- Thyroglobulin Antibody Are Independently Associated with Lesions in Spinal Cord in Central Nervous System Demyelinating Diseases Youming Long 1,2, Yangbo Zheng
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Anaesthesia recommendations for patients suffering from Neuromyelitis optica spectrum disorder
 orphananesthesia Anaesthesia recommendations for patients suffering from Neuromyelitis optica spectrum disorder Disease name: Neuromyelitis optica spectrum disorder ICD 10: G36.0 Synonyms: Devic's Disease,
orphananesthesia Anaesthesia recommendations for patients suffering from Neuromyelitis optica spectrum disorder Disease name: Neuromyelitis optica spectrum disorder ICD 10: G36.0 Synonyms: Devic's Disease,
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
MOG encephalomyelitis: international recommendations on diagnosis and antibody testing
 Jarius et al. Journal of Neuroinflammation (2018) 15:134 https://doi.org/10.1186/s12974-018-1144-2 REVIEW MOG encephalomyelitis: international recommendations on diagnosis and antibody testing Open Access
Jarius et al. Journal of Neuroinflammation (2018) 15:134 https://doi.org/10.1186/s12974-018-1144-2 REVIEW MOG encephalomyelitis: international recommendations on diagnosis and antibody testing Open Access
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Neuroimmunology testing services
 Neuroimmunology testing services Neuroimmunology Quest Diagnostics is your source for neuroimmunological testing with expanded offerings for several autoimmune neurological disorders Neuroimmunology is
Neuroimmunology testing services Neuroimmunology Quest Diagnostics is your source for neuroimmunological testing with expanded offerings for several autoimmune neurological disorders Neuroimmunology is
Title. CitationInternal Medicine, 46(8): Issue Date Doc URL. Type. File Information
 Title Scapular Winging as a Symptom of Cervical Flexion My Author(s)Yaguchi, Hiroaki; Takahashi, Ikuko; Tashiro, Jun; Ts CitationInternal Medicine, 46(8): 511-514 Issue Date 2007-04-17 Doc URL http://hdl.handle.net/2115/20467
Title Scapular Winging as a Symptom of Cervical Flexion My Author(s)Yaguchi, Hiroaki; Takahashi, Ikuko; Tashiro, Jun; Ts CitationInternal Medicine, 46(8): 511-514 Issue Date 2007-04-17 Doc URL http://hdl.handle.net/2115/20467
CHAIR SUMMIT 7TH ANNUAL #CHAIR2014. Master Class for Neuroscience Professional Development. September 11 13, Westin Tampa Harbour Island
 #CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Use of MRI in Clinical Decision- Making
#CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Use of MRI in Clinical Decision- Making
PATIENTS WITH MULTIPLE SCLEROSIS
 3 PATIENTS WITH MULTIPLE SCLEROSIS PREFER EARLY DIAGNOSIS Abstract The new diagnostic criteria for multiple sclerosis (MS) allow for a definite diagnosis in earlier stages of disease. Yet, clinicians may
3 PATIENTS WITH MULTIPLE SCLEROSIS PREFER EARLY DIAGNOSIS Abstract The new diagnostic criteria for multiple sclerosis (MS) allow for a definite diagnosis in earlier stages of disease. Yet, clinicians may
Journal of Neurology and Therapeutics
 Journal of Neurology and Therapeutics An Open Access Publisher Baranello RJ et al., J Neurol Ther 2015, 1(1):9-14 Review article Open Access Neuromyelitis optica spectrum disorders with and without aquaporin
Journal of Neurology and Therapeutics An Open Access Publisher Baranello RJ et al., J Neurol Ther 2015, 1(1):9-14 Review article Open Access Neuromyelitis optica spectrum disorders with and without aquaporin
Focal Anterior Displacement of the Thoracic Spinal Cord without Evidence of Spinal Cord Herniation or an Intradural Mass
 Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum disorders: a case series study
 Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
Clinicopathological Conference
 Clinicopathological Conference Amar Dhand, MD DPhil Richard Cuneo, MD Andrew Bollen, DVM, MD Malaise History Bilateral leg numbness and weakness Urinary retention Examination Temp = 38.8 1.7 liters of
Clinicopathological Conference Amar Dhand, MD DPhil Richard Cuneo, MD Andrew Bollen, DVM, MD Malaise History Bilateral leg numbness and weakness Urinary retention Examination Temp = 38.8 1.7 liters of
