Opticospinal multiple sclerosis in Japanese
|
|
|
- Meredith Hodge
- 6 years ago
- Views:
Transcription
1 Neurology Asia 2008; 13 : Opticospinal multiple sclerosis in Japanese Jun-ichi Kira, Takuya Matsushita, Noriko Isobe, Takaaki Ishizu Department of Neurology, Neurological Institute, Graduate School of Medical Sciences, Kyushu University, Japan Abstract Antibodies to aquaporin-4 (AQP4) are found in a number of Japanese opticospinal multiple sclerosis (OSMS) patients. Whether anti-aqp4 antibody-positive and -negative OSMS patients are afflicted with an identical disease remains unknown. To clarify immunological differences between the two groups of patients, we studied serum antibody titres against AQP4 in 191 patients with idiopathic central nervous system demyelinating diseases and clarified any relationships with immunological parameters. The anti-aqp4 antibody positivity rate was higher in patients with OSMS (36.2%), idiopathic recurrent myelitis (23.5%), and recurrent optic neuritis (26.9%) than in conventional MS patients (8.0%), and those with other diseases (0%). Anti-AQP4 antibody titre was significantly higher in patients with SS-A/B antibodies than in those without. Anti-AQP4 antibody-negative OSMS patients showed significantly higher CD4 + IFN-γ + IL-4 - T cell percentages and intracellular IFN-γ/IL-4 ratios than anti-aqp4 antibodypositive patients, anti-aqp4 antibody-negative conventional MS patients, and healthy controls. As well, CD4 + IFN-γ + IL-4 - T cell percentages were negatively correlated with anti-aqp4 antibody titres. In CSF, OSMS patients had significantly higher levels of IFN-γ and granulocyte colony-stimulating factor levels than patients with non-inflammatory neurological diseases and other causes of myelitis. A significant increase of IL-17 compared with non-inflammatory neurological diseases patients was only found in OSMS patients, irrespective of the presence or absence of anti-aqp4 antibody. These findings suggest that high titres of anti-aqp4 antibodies are produced as a result of heightened humoral autoimmunity, and that they are likely to contribute to extensive lesion development through disturbed resolution of vasogenic oedema. Moreover, since intrathecal up-regulation of IL-17 and IFN-γ is characteristic of OSMS, Th17/Th1 cells may be critical for the initiation of inflammation and the disruption of blood-brain barrier (BBB); rendering anti-aqp4 antibody get across the BBB. INTRODUCTION Multiple sclerosis (MS) is a demyelinating disease of the central nervous system (CNS) whereas neuromyelitis optica (NMO) is an inflammatory disease of the CNS selectively affecting the optic nerves and spinal cord. The pathological hallmark in MS is sharply demarcated demyelinating plaques with axons relatively preserved. In NMO, both axons and myelin are destroyed resulting in necrotic cavitation. Although MS is rare in Asians; when it does appear, selective but severe involvement of the optic nerves and spinal cord is characteristic. 1 This form, termed opticospinal MS (OSMS), has similar features to the relapsing form of NMO in Western populations. Although the nosological position of NMO has long been a matter of debate, the recent discovery of a specific IgG against NMO, designated NMO-IgG 2, suggests that NMO is a distinct disease entity with a fundamentally different aetiology from MS. Because NMO-IgG has been reported to be present in about 50 to 60% of OSMS patients with longitudinally extensive spinal cord lesions (LESCLs) 2,3, OSMS in Asians has been suggested to be the same entity as NMO. 4 However, it remains to be elucidated whether patients with or without these antibodies are inflicted with an identical disease. NMO-IgG/ANTI-AQP4 ANTIBODY POSITIVITY RATE There are discrepancies in the detection rates for anti-aqp4 antibody among the Japanese patient series of Takahashi et al 5 (20/22, 90% in NMO patients), Tanaka et al 6 (60% in OSMS patients with LESCLs) and Matsuoka et al 7 (11/31, 35% in OSMS patients with LESCLs). The reasons might relate to differences in subjects (NMO or OSMS with LESCLs; selected or consecutive patients; northern or southern Japanese patients, who have been reported to have somewhat different clinical and laboratory features according to a Address correspondence to: Jun-ichi Kira, MD, PhD, Professor and Chairman, Department of Neurology, Neurological Institute, Graduate School of Medical Sciences, Kyushu University, Maidashi, Higashi-ku, Fukuoka , Japan. E mail: kira@neuro.med.kyushu-u.ac.jp 167
2 Neurology Asia December 2008 recent nationwide survey) 8, and in the methods (AQP4-transfected or GFP-AQP4 fusion proteintransfected; fixed transfected cell specimens or unfixed ones; 1:4 dilution or 1:400 dilution). We recently increased sensitivity (100% sensitive against NMO-IgG) by using unfixed preparations of GFP-AQP4 fusion protein-transfected cells and 1:4 diluted sera; however, the results were practically the same. Using this method, we found that the anti-aqp4 antibody positivity rate was higher in patients with OSMS (19/58, 32.7%), idiopathic recurrent myelitis (4/17, 23.5%), or recurrent optic neuritis (7/26, 26.9%) than in conventional MS (CMS) patients (6/75, 8.0%) and others (0/87). A similar positivity rate was reported in NMO patients (16/48, 33.3%) in Cuba and the French West Indies. 9 CLINICAL AND NEUROIMAGING FEATURES As compared with anti-aqp4 antibody-negative CMS patients, anti-aqp4 antibody-positive MS patients showed significantly higher frequencies of severe optic neuritis, acute transverse myelitis, and LESCLs while most conditions were also common to anti-aqp4 antibody-negative OSMS patients. 7 The LESCLs in anti-aqp4 antibodypositive patients were preferentially located at the upper-to-middle thoracic cord, while those in anti-aqp4 antibody-negative OSMS patients appeared throughout the cervical-to-thoracic cord. On axial planes, the former predominantly showed central grey matter involvement while holocord involvement was predominant in the latter. By contrast, LESCLs in anti-aqp4 antibody-negative CMS patients mainly involved the mid-cervical cord, presenting a peripheral white matter-predominant pattern as seen in short spinal cord lesions. Anti-AQP4 antibodypositive MS patients fulfilling definite NMO criteria showed female preponderance, higher relapse rate, greater frequency of brain lesions, and less frequent responses to interferon beta-1b than anti-aqp4 antibody-negative OSMS patients with LESCLs. Multiple logistic analyses revealed that the emergence of the anti-aqp4 antibody was positively associated with only a higher relapse rate, not with optic-spinal presentation or LESCLs. These findings suggested that LESCLs are distinct according to anti-aqp4 antibody positivity and clinical phenotypes. There are cases of anti-aqp4 antibody-positive MS/NMO that are distinct from CMS and anti-aqp4 antibodynegative OSMS with LESCLs in Japanese. This indicates that the mechanisms producing LESCLs are heterogeneous even in patients with opticspinal presentation, namely AQP4 autoimmunityrelated and -unrelated. We titrated the anti-aqp4 antibody and found the following. (1) Anti-AQP4 antibody titre was significantly higher in patients with SS-A/B antibodies than in those without, but was not significantly correlated with either EDSS score or disease phase. (2) Patients with a high anti- AQP4 antibody titre ( 512) showed significantly higher frequencies of extensive brain lesions and other autoantibodies/autoimmune diseases than anti-aqp4 antibody-negative OSMS patients with LESCLs. However, the former group paradoxically showed significantly lower frequencies of acute transverse myelitis and severe motor disability than the latter, despite the optic nerve impairment being equally severe between the two. (3) Extensive brain lesions in patients with high antibody titres showed a vasogenic oedema pattern on diffusion-weighted MRI. (4) Anti-AQP4 antibody-negative OSMS patients showed significantly higher CD4 + IFN-γ + IL-4 - T cell percentages and intracellular IFN-γ/IL-4 ratios than anti-aqp4 antibody-positive OSMS patients, anti-aqp4 antibody-negative CMS patients and healthy controls, and CD4 + IFNγ + IL-4 - T cell percentages showed a significant negative correlation with anti-aqp4 antibody titres. (5) The phenotypic frequency of the HLA- DPB1*0501 allele was significantly increased in anti-aqp4 antibody-positive patients compared with controls but not in anti-aqp4 antibodynegative ones. These findings suggest that high titres of anti-aqp4 antibodies are produced as a result of heightened humoral autoimmunity and the presence of the HLA-DPB1*0501 allele in Japanese. As well, the high titres are likely to contribute to extensive lesion development through disturbed resolution of vasogenic oedema. INTRATHECAL IMMUNE RESPONSES To clarify differences in intrathecal immune responses among various inflammatory myelopathies, we used a fluorescent bead-based immunoassay to simultaneously measure 27 cytokines, chemokines and growth factors in CSF from 22 patients with atopic myelitis, 20 with OSMS, 11 with HTLV-1-associated myelopathy (HAM), 9 with Sjögren syndrome-related myelitis and 20 with other non-inflammatory neurological diseases (OND). 10 In OSMS patients, IFN-γ and 168
3 granulocyte colony-stimulating factor levels were significantly higher than patients with OND and other causes of myelitis whereas in AM patients, eotaxin and IL-9 were significantly increased as compared with OND and other myelitis patients. A significant increase in IL-17 compared with OND patients was found only in OSMS patients, irrespective of the presence or absence of anti- AQP4 antibody. In HAM patients, IP-10 and RANTES were higher than in OND and other myelitis patients. In Sjögren syndrome-related myelitis patients, MIP-1α and MIP-1β were higher than in OND patients. These findings suggested that intrathecal up-regulation of IL-17/IFN-γ is characteristic of OSMS, which is distinct from the eotaxin and Th2 cytokines-related allergic inflammatory condition of atopic myelitis. PROPOSED MECHANISM OF NMO Lucchinetti et al 11 reported perivascular immune complex deposition (IgM, IgG and C9neo) in a rim or rosette pattern in CNS lesions from autopsied NMO patients. Misu et al 12 described an extensive loss of AQP4 accompanied by decreased GFAPstaining in active perivascular lesions where MBPstaining was relatively preserved in postmortem Japanese NMO cases. Roemer et al 13 also made similar observations regarding novel NMO lesions in the spinal cord and medullary tegmentum that extended to the area postrema where the bloodbrain barrier is absent; suggesting a primary role for anti-aqp4 antibody in NMO pathology. Based on the presence of immunoglobulin and complement deposition in active perivascular lesions, astrocytic impairment associated with the loss of AQP4 caused by humoral autoimmune attack is assumed to be the primary event in NMO. Anti-AQP4 IgG1 antibodies across the BBB bind to AQP4 molecules on astrocyte foot processes and activate complements. Activated complements mobilize neutrophils and eosinophils that then facilitate tissue destruction. However, there are several concerns about this hypothesis. First, the deposited immunoglobulins in postmortem NMO lesions are mainly IgM, while the anti-aqp4 antibodies described are all IgG, not IgM. Second, in the presence of high titres of anti-aqp4 antibodies, some patients remain in remission. 14 Since AQP4 is present in the astrocyte foot processes behind the BBB, additional factors that disrupt the BBB and allow the antibody to enter through the BBB may be necessary to initiate inflammation in the parenchyma. Third, AQP4 is present in distal collecting tubules and in gastric mucosa, and NMO-IgG binds to these structures. 15 However, no impairments in either kidney or stomach have been seen in such cases, suggesting that the presence of complementfixing anti-aqp4 antibody is not enough to produce tissue damage. Fourth, AQP4 expression ubiquitously exists throughout the CNS, though its expression varies; being high in the grey matter of the spinal cord. 12 Such a ubiquitous presence cannot explain the selectiveness of lesion distribution; in the optic nerves and the spinal cord. Fifth, we have analysed serum CH50, C3, C4, and C-reactive protein (CRP) levels and their relationship to clinical phases in 118 MS patients with or without anti-aqp4 antibody. 16 Serum CH50 levels were significantly higher in patients with anti-aqp4 antibody than in OSMS and CMS patients without anti-aqp4 antibody at relapse, but not in remission. The frequency of hypercomplementemia at relapse was also higher in patients with anti-aqp4 antibody than in anti- AQP4 antibody-negative CMS patients (70.4% vs. 29.0%, P corr < 0.05). C3 and C4 levels did not differ significantly among the three groups at relapse. In patients with anti-aqp4 antibody, coexistence of both hypercomplementemia and high CRP values was more common at relapse than in the remission phase (36.0% vs. 10.5%, P < 0.05). Therefore, hypercomplementemia in anti-aqp4 antibody-positive patients seems to reflect a systemic inflammatory reaction at relapse; also, that complement consumption as seen in systemic autoimmune diseases such as systemic lupus erythematosus (SLE) and Sjögren syndrome does not occur in anti-aqp4 antibody-positive patients. OUR HYPOTEHSIS In our series, more than half the anti-aqp4 antibody-positive patients had brain lesions that fulfilled the Barkhof criteria, while anti- AQP4 antibody-negative OSMS patients with LESCLs showed substantially fewer brain lesions. 7 Moreover, some Japanese anti-aqp4 antibody-positive patients predominantly had brain lesions or even only brain lesions. Therefore, the anti-aqp4 antibody-positive condition does not completely overlap NMO or OSMS. We previously reported that IL-17 is up-regulated in the CSF of OSMS patients and that levels of both IL-17 and downstream cytokine IL-8 in CSF show a significant positive correlation with spinal cord lesion length. 17 IL-17 is produced by Th17 cells, which belong to a distinct lineage from Th1 and Th2 cells. 18 Th17 cells have come under much 169
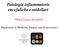
4 Neurology Asia December 2008 attention because increasing evidence suggests that they, but not Th1 cells, are responsible for organ-specific autoimmune diseases such as experimental autoimmune encephalomyelitis (EAE). 18,19 IL-8 is a chemokine for neutrophils. In OSMS patients, CSF neutrophilia and infiltration of neutrophils to severely destructed lesions have been observed. 17 Elevated IL-8 is assumed to be partly responsible for such neutrophil activation and mobilization in OSMS. Indeed, myeloperoxidase, an activated neutrophil product, is up-regulated in sera from OSMS patients, especially in those with LESCLs at relapse. 20 Th17 cells carrying granzyme B have recently been shown to efficiently disrupt BBB tight junctions and loosen the BBB. 21 Therefore, autoimmune Th17 cells may initiate BBB disruption and inflammation in OSMS, causing vasogenic oedema in the CNS (Fig. 1). Regarding other factors that possibly have effects on vascular permeability; we have reported that levels of vascular endothelial growth factor (VEGF) in sera are significantly increased in OSMS patients, showing a significant positive correlation with spinal cord lesion length. 22 IL-17 has also been shown to induce VEGF production in target tissues. 23 Moreover, a mutation in the platelet activating factor acetylhydrolase (PAF- AH) gene, which inactivates its enzymatic activity of metabolizing PAF into an inactive form, is significantly more frequent in OSMS patients than healthy controls. 24 Indeed, PAF-AH activity in peripheral blood is decreased in OSMS patients 24, which likely prolongs PAF activity and increasing vascular permeability as well as vascular growth. These vascular-acting factors also enhance tissue oedema in OSMS (Fig. 1). Figure 1. Th17 cell-mediated mechanism producing extensive spinal cord lesions in opticospinal multiple sclerosis (OSMS). Autoimmune Th17 cells produce IL-17, which then induces IL-8 production in various cells in tissues. IL-8 activates and mobilizes neutrophils. In OSMS patients, serum myeloperoxidase levels are elevated, especially at relapse. Thus the IL-17/IL-8 axis may contribute to severe tissue destruction in OSMS. Platelet activating factor (PAF) acetylhydrolase (PAF-AH) metabolizes PAF to an inactive form. Mutation in the PAF-AH gene, which inactivates its enzymatic activity, is significantly more frequent in OSMS patients than healthy controls. Moreover, vascular endothelial growth factor (VEGF) is increased in sera from OSMS patients. It is possible that elevated VEGF and prolonged PAF activity increase vascular permeability and cause tissue oedema. MPO=myeloperoxidase. 170
5 As AQP4 knock-out mice showed prolongation of vasogenic oedema 25, but a decrease of cytotoxic oedema 26, anti-aqp4 antibody produced by heightened humoral autoimmune background or secondarily by tissue breakdown may prolong resolution of tissue oedema, thereby contributing to further tissue destruction in NMO/OSMS patients. NMO-IgG/anti-AQP4 antibody-positive patients show a significantly higher frequency of severe optic nerve damage as compared with anti- AQP4 antibody-negative CMS ones. 3,7 We recently investigated multimodality evoked potentials (visual evoked potentials, motor evoked potentials and somatosensory evoked potentials) in 111 relapsing-remitting or relapsing-progressive MS patients, 18 of whom were seropositive for anti- AQP4 antibody. We found that more patients with anti-aqp4 antibody showed a lack of the P100 VEP component than those without the antibody (11/17, 64.7% vs. 20/84, 23.8%, p=0.003), whereas the frequency of delayed P100 latency was significantly higher in the latter group than in the former (1/17, 5.9% vs. 28/84, 33.3%, p=0.021). Optic nerves are especially vulnerable to the detrimental effects of tissue oedema in the optic canal where space is tight and increased tissue pressure easily causes circulatory insufficiency. In the spinal cord, the thoracic cord is prone to develop LESCLs in anti-aqp4 antibody-positive patients as it acts as the watershed for vascular supply in the spinal cord. However, AQP4 is widely present from the cervical to sacral cord. Therefore, even in the spinal cord, vulnerability to ischaemia may be one factor contributing to the development of LESCLs. Prolongation of vasogenic oedema at sites where the surrounding space is tight or vascular supply is poor may cause poor recovery from tissue damage in patients with anti-aqp4 antibody. Anti-AQP4 antibody may directly cause NMO or a disease distinct from either MS or NMO (anti-aqp4 autoimmune syndrome of the CNS). Alternatively, anti-aqp4 antibody is a secondary product that is produced following tissue destruction. Once produced it may modify the disease course as a functional autoantibody like anti-neurofascin antibody in chronic progressive MS (Fig. 2) 27, or could simply be an epiphenomenon without any function in vivo. Figure 2. Two hypothetical mechanisms in MS and NMO. (A) Anti-AQP4 antibody directly causes NMO, which is distinct from MS. (B) Myelin-specific Th17/ Th1 cells initiate CNS inflammation. Anti-myelin antibody produces myelin loss, anti-neurofascin antibody causes axonal loss and anti-aqp4 antibody induces astrocyte foot process destruction. 171
6 Neurology Asia December 2008 Figure 3. Distinct Th subsets produce distinct inflammatory (demyelinating) CNS disorders, when regulatory T cells (Treg) can not effectively suppress Th effector activities. FUTURE PERSPECTIVES It remains to be elucidated whether anti-aqp4 antibody-negative NMO/OSMS patients have the same disease as anti-aqp4 antibody-positive NMO/OSMS patients. If these patients do have the same disease, which is distinct from MS, then what is the actual cause or specific autoantigen? If AQP4 is one of the autoantigens, are there also other autoantigens responsible for seronegative NMO/OSMS? How is the anti-aqp4 antibody produced and how does the antibody get across the BBB to reach the astrocyte foot process? If the big picture of immunology produces a spectrum of idiopathic inflammatory (demyelinating) diseases of the CNS, Th17 cells may produce OSMS/ NMO with or without anti-aqp4 antibody, Th1 cells may cause classical MS and Th2 cells may induce atopic myelitis (Fig. 4). There are many questions remaining to be answered. REFERENCES 1. Kira, J. Multiple sclerosis in the Japanese population. Lancet Neurol 2003; 2(2): Lennon VA, Wingerchuk DM, Kryzer TJ, et al. A serum autoantibody marker of neuromyelitis optica: distinction from multiple sclerosis. Lancet 2004; 364(9451): Nakashima I, Fujihara K, Miyazawa I, et al. Clinical and MRI features of Japanese patients with multiple sclerosis positive for NMO-IgG. J Neurol Neurosurg Psychiatry 2006; 77(9): Weinshenker BG, Wingerchuk DM, Nakashima I, et al. OSMS is NMO, but not MS: proven clinically and pathologically. Lancet Neurol 2006; 5(2): Takahashi T, Fujihara K, Nakashima I, et al. Antiaquaporin-4 antibody is involved in the pathogenesis of NMO: a study on antibody titre. Brain 2007(Pt 5); 130: Tanaka K, Tani T, Tanaka M, et al. Anti-aquaporin 4 antibody in selected Japanese multiple sclerosis patients with long spinal cord lesions. Mult Scler 2007; 13(7): Matsuoka T, Matsushita T, Kawano Y, et al. Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese. Brain 2007; 130(Pt 5): Osoegawa M*, Kira J*, Fukazawa K, et al. Temporal changes and geographical differences in multiple sclerosis phenotypes in Japanese: nationwide survey results over 30 years. Mult Scler (In press). *Equal contribution 9. Cabrera-Gomez JA, Philippe C, Saiz A, et al. Neuromyelitis optica (NMO) positive antibodies confer a worse course in relapsing-nmo in Cuba and French West Indies. Mult Scler 2008; 14(Supple 1): S Tanaka M, Matsushita T, Tateishi T, et al. Distinct CSF cytokine/chemokine profiles in atopic myelitis and other causes of myelitis. Neurology 2008; 71(13): Lucchinetti CF, Mandler RN, McGavern D, et al. A role for humoral mechanisms in the pathogenesis of Devic s neuromyelitis optica. Brain 2002; 125(Pt 7): Misu T, Fujihara K, Kakita A, et al. Loss of aquaporin 4 in lesions of neuromyelitis optica: distinction from multiple sclerosis. Brain 2007; 130(Pt 5):
7 13. Roemer SF, Parisi JE, Lennon VA, et al. Patternspecific loss of aqaporin-4 immunoreactivity distinguishes neuromyelitis optica from multiple sclerosis. Brain 2007; 130(Pt 5): Jarius, S. et al. Neuromyelitis optica and longitudinally extensive transverse myelitis following thymectomy for myasthenia gravis. 23 rd Congress of the ECTRIMS. Mult Scler 2007; 13:S Wingerchuk DM, Lennon VA, Lucchinetti CF, et al. The spectrum of neuromyelitis optica. Lancet Neurol 2007; 6(9): Doi H, Matsushita T, Isobe N, et al. Hypercomplementemia at relapse in patients with anti-aquaporin-4. Mult Scler (In press). 17. Ishizu T, Osoegawa M, Mei FJ, et al. Intrathecal activation of the IL-17/IL-8 axis in opticospinal multiple sclerosis. Brain 2005; 128(Pt 5): Weaver CT, Hatton RD, Mangan PR, et al. IL-17 family cytokines and the expanding diversity of effector T cell lineages. Annu Rev Immunol 2007; 25: Cua DJ, Sherlock J, Chen Y, et al. Interleukin-23 rather than interleukin-12 is the critical cytokine for autoimmune inflammation of the brain. Nature 2003; 421: Minohara M, Matsuoka T, Li W, et al. Upregulation of myeloperoxidase in patients with opticospinal multiple sclerosis: positive correlation with disease severity. J Neuroimmunol 2006; 178(1-2): Kebir H, Kreymborg K, Ifergan I, et al. Human TH17 lymphocytes promote blood-brain barrier disruption and central nervous system inflammation. Nat Med 2007; 13(10): Su JJ, Osoegawa M, Matsuoka T, et al. Upregulation of vascular endothelial growth factor in multiple sclerosis: correlation with MR findings. J Neurol Sci 2006; 243(1-2): Ryu S, Lee JH, Kim SI. IL-17 increased the production of vascular endothelial growth factor in rheumatoid arthritis synoviocytes. Clin Rheumatol 2006; 25(1): Osoegawa M, Niino M, Ochi H, et al. Plateletactivating factor acetylhydrolase gene polymorphism and its activity in Japanese patients with multiple sclerosis. J Neuroimmunol 2004; 150(1-2): Papadopoulos MC, Manley GT, Krishna S, et al. Aquaporin-4 facilitates reabsorption of excess fluid in vasogenic brain edema. FASEB J 2004; 18(11): Manley GT, Fujimura M, Ma T, et al. Aquaporin-4 deletion in mice reduces brain edema after acute water intoxication and ischemic stroke. Nat Med 2006; 6(2): Mathey EK, Derfuss T, Storch MK, et al. Neurofascin as a novel target for autoantibody-mediated axonal injury. J Exp Med 2007; 204(10):
Multiple sclerosis in Japan: Nationwide surveys over 30 years
 Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
Neurology Asia 28; 13 : 131 143 Multiple sclerosis in Japan: Nationwide surveys over 3 years Jun-ichi Kira, Takaaki Ishizu, Manabu Osoegawa, and The Research Committee of Neuroimmunological Diseases Department
Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese Multiple Sclerosis
 International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
International Scholarly Research Network ISRN Neurology Volume 211, Article ID 9476, 4 pages doi:1.542/211/9476 Research Article Optic Nerve and Spinal Cord Are the Major Lesions in Each Relapse of Japanese
MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients
 Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
Neurology Asia 2013; 18(1) : 73 81 MRI features and anti-aqp4 antibody status in Idiopathic inflammatory demyelinating CNS disease (IIDCD) in Thai patients 1 Naraporn Prayoonwiwat MD, 2 Orasa Chawalparit
The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies
 Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Neurology Asia 2007; 12 : 135 139 VIEWS AND REVIEW The role of anti-aquaporin-4 antibody in Asian patients with multiple sclerosis: Confusions and controversies HT Chong, *AG Kermode, CT Tan Department
Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore
 Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Case Reports 26 Autologous Hematopoietic Stem Cell Transplantation for the Treatment of Neuromyelitis Optica in Singapore Koh Yeow Hoay, Pavanni Ratnagopal Abstract Introduction: Neuromyelitis optica (NMO)
Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome)
 J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
ORIGINAL CONTRIBUTION Markedly Elevated Soluble Intercellular Adhesion Molecule 1, Soluble Vascular Cell Adhesion Molecule 1 Levels, and Blood-Brain Barrier Breakdown in Neuromyelitis Optica Akiyuki Uzawa,
Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese
 doi:10.1093/brain/awm027 Brain (2007), 130,1206^1223 Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese Takeshi Matsuoka, 1 Takuya Matsushita, 1 Yuji Kawano,
doi:10.1093/brain/awm027 Brain (2007), 130,1206^1223 Heterogeneity of aquaporin-4 autoimmunity and spinal cord lesions in multiple sclerosis in Japanese Takeshi Matsuoka, 1 Takuya Matsushita, 1 Yuji Kawano,
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
 The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
The Journal of International Medical Research 2012; 40: 1483 1491 Blood Brain Barrier Disruption is More Severe in Neuromyelitis Optica than in Multiple Sclerosis and Correlates with Clinical Disability
 Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Title Neuromyelitis Optica in Japanese Author(s) TANAKA, Yuji Citation [Internal Medicine] vol.[50] no.[ Issue Date 2011 Rights The Japanese Society of Internal 内科学会 ) Version 出版社版 (publisher version)
Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system
 Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
Neurology Asia 2014; 19(3) : 295 300 Neuromyelitis optica and neuromyelitis optica-igg seropositivity in Saudis with demyelinating diseases of the central nervous system 1,2 Ali M Al-Khathaami FRCPC, 2
Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report
 Tohoku J. Exp. Med., 2006, Loss 209, of Aquaporin-4 269-275 in the Lesions of Neuromyelitis Optica 269 Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report Case Report
Tohoku J. Exp. Med., 2006, Loss 209, of Aquaporin-4 269-275 in the Lesions of Neuromyelitis Optica 269 Loss of Aquaporin-4 in Active Perivascular Lesions in Neuromyelitis Optica: A Case Report Case Report
RSR RSR RSR RSR RSR. ElisaRSR AQP4 Ab RSR. Aquaporin-4 Autoantibody Assay Kit
 To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
MULTIPLE SCLEROSIS MSJ
 431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
431727MSJ18610.1177/1352458511431727Estiasari et al.multiple Sclerosis Journal 2012 Research Paper MULTIPLE SCLEROSIS JOURNAL MSJ Comparison of clinical, immunological and neuroimaging features between
Salintip Kunadison MD, Chaiwiwat Tungkasereerak MD, Surin Saetang MD, Pawut Mekawichai MD
 Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
Neurology Asia 2018; 23(1) : 55 59 Comparison of clinical features between aquaporin-4 antibody seropositive and seronegative patients in neuromyelitis optica and neuromyelitis optica spectrum disorder
Wingerchuk et al, Neurol, 2006
 Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
Current Understanding of Neuromyelitis Optica Jacqueline A. Leavitt, M.D. Mayo Clinic Rochester, MN I have no financial disclosures 46 y/o F Pain in R temple worse with head movements, resolved in days
Neuromyelitis Optica: A Case Report
 Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Pediatr Neonatol 2010;51(6):347 352 CASE REPORT Neuromyelitis Optica: A Case Report Wei-Chia Chia 1, Jian-Nan Wang 1, Ming-Chi Lai 2 * 1 Department of Family Medicine, Chi-Mei Medical Center, Yong Kang
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview
 Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Neuromyelitis optica (NMO), or Devic s disease, is a rare
 Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
NMO-IgG: A specific biomarker for neuromyelitis optica
 Disease Markers 22 (2006) 197 206 197 IOS Press NMO-IgG: A specific biomarker for neuromyelitis optica Brian G. Weinshenker a,, Dean M. Wingerchuk d, Sean J. Pittock a,b, Claudia F. Lucchinetti a and Vanda
Disease Markers 22 (2006) 197 206 197 IOS Press NMO-IgG: A specific biomarker for neuromyelitis optica Brian G. Weinshenker a,, Dean M. Wingerchuk d, Sean J. Pittock a,b, Claudia F. Lucchinetti a and Vanda
MYELITIS. A Mochan Neurology
 MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
MYELITIS A Mochan Neurology ATM MS LETM NMOSD ATM LETM MS NMOSD Acute Transverse Myelitis Longitudinally Extensive Transverse Myelitis Multiple Sclerosis Neuromyelitis Optica Spectrum Disorders ATM ADEM
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância. Silvia Tenembaum
 Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
 Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Mod Rheumatol (13) 3:87 831 DOI 1.17/s1165-1-715-9 CASE REPORT Clinical improvement in a patient with neuromyelitis optica following therapy with the anti-il-6 receptor monoclonal antibody tocilizumab
Professor Yasser Metwally. Neuromyelitis optica. EPIDEMIOLOGY
 180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
180 Professor Yasser Metwally Neuromyelitis optica www.yassermetwally.com N EPIDEMIOLOGY Afro-Caribbean, and South American descent implying underlying genetic mechanisms in the expression of demyelinating
Disease of Myelin. Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019
 Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
ORIGINAL CONTRIBUTION. Painful Tonic Spasm in Neuromyelitis Optica. Incidence, Diagnostic Utility, and Clinical Characteristics
 ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
ORIGINAL CONTRIBUTION Painful Tonic Spasm in Neuromyelitis Optica Incidence, Diagnostic Utility, and Clinical Characteristics Sung-Min Kim, MD; Min Jin Go, MS; Jung-Joon Sung, MD, PhD; Kyung Seok Park,
Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated
 UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
UK Nationally Commissioned NMO team Setting the Scene: Neuromyelitis Optica epidemiology, population variability, subgroups: relapsing/monophasic, Ab +ve/-ve, NMO/SD, treated/untreated Jackie Palace Disclosures
The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica
 Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
Neurology Asia 2014; 19(4) : 375 385 The use of AQP4-antibody testing in diagnosis Thai patients with neuromyelitis optica 1,2 Sasitorn Siritho MD, 3 Metha Apiwattanakul MD, 1 Naraporn Prayoonwiwat MD
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS ILOS 1. to understand differences and similarities between diseases of myelin in CNS and PNS. 2. to understand
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS ILOS 1. to understand differences and similarities between diseases of myelin in CNS and PNS. 2. to understand
Patologie infiammatorie encefaliche e midollari
 Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Function of aquaporin in the brain and brain edema
 Nagoya Med. J., 199 Function of aquaporin in the brain and brain edema KAZUYA SOBUE Department of Anesthesiology and Medical crisis Management, Nagoya City University Graduate School of Medical Sciences
Nagoya Med. J., 199 Function of aquaporin in the brain and brain edema KAZUYA SOBUE Department of Anesthesiology and Medical crisis Management, Nagoya City University Graduate School of Medical Sciences
Clinical Study Interferon Alpha Association with Neuromyelitis Optica
 Clinical and Developmental Immunology Volume 2013, Article ID 713519, 6 pages http://dx.doi.org/10.1155/2013/713519 Clinical Study Interferon Alpha Association with Neuromyelitis Optica Nasrin Asgari,
Clinical and Developmental Immunology Volume 2013, Article ID 713519, 6 pages http://dx.doi.org/10.1155/2013/713519 Clinical Study Interferon Alpha Association with Neuromyelitis Optica Nasrin Asgari,
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism
 MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis
 NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
NMO IgG (Aquaporin-4) autoantibodies in immune-mediated optic neuritis A Petzold, Sean J Pittock, Vanda Lennon, Cosimo Maggiore, B G Weinshenker, Gordon T Plant To cite this version: A Petzold, Sean J
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow
 Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System
 Neurology Research International Volume 2012, Article ID 460825, 13 pages doi:10.1155/2012/460825 Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System Jiwon
Neurology Research International Volume 2012, Article ID 460825, 13 pages doi:10.1155/2012/460825 Review Article Neuromyelitis Optica: An Antibody-Mediated Disorder of the Central Nervous System Jiwon
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
The Etiological Spectrum of Acute Sensory Myelitis
 Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(3):227-233 / http://dx.doi.org/10.3988/jcn.2015.11.3.227 ORIGINAL ARTICLE Jae-Won Hyun a,c Jee Young Kim b Kyung Gyu Choi a Ho Jin
Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(3):227-233 / http://dx.doi.org/10.3988/jcn.2015.11.3.227 ORIGINAL ARTICLE Jae-Won Hyun a,c Jee Young Kim b Kyung Gyu Choi a Ho Jin
Potential Rebalancing of the Immune System by Anti-CD52 Therapy
 Potential Rebalancing of the Immune System by Anti-CD52 Therapy Johanne Kaplan, PhD VP Neuroimmunology Research Genzyme March 26, 2013 RESTRICTED USE SEE TRAINING MEMO 2011 DO Genzyme NOT 1COPY Corporation
Potential Rebalancing of the Immune System by Anti-CD52 Therapy Johanne Kaplan, PhD VP Neuroimmunology Research Genzyme March 26, 2013 RESTRICTED USE SEE TRAINING MEMO 2011 DO Genzyme NOT 1COPY Corporation
What is Autoimmunity?
 Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
What is Autoimmunity?
 Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
Objective: To assess the evidence for diagnostic tests and therapies for transverse myelitis (TM) and make evidence-based recommendations.
 Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
Published Ahead of Print on December 7, 2011 as 10.1212/WNL.0b013e31823dc535 SPECIAL ARTICLE Evidence-based guideline: Clinical evaluation and treatment of transverse myelitis Report of the Therapeutics
Neuromyelitis optica (NMO) is characterized as a
 Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
Neuromyelitis optica (NMO) is characterized as a severe, relapsing inflammatory disease resulting in vision loss and impaired mobility. As with multiple sclerosis, clinical symptoms result from demyelination
Copyright Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited.
 Comparative immunopathogenesis of acute disseminated encephalomyelitis, neuromyelitis optica, and multiple sclerosis Dean M. Wingerchuk a and Claudia F. Lucchinetti b Purpose of review Advanced immunopathological
Comparative immunopathogenesis of acute disseminated encephalomyelitis, neuromyelitis optica, and multiple sclerosis Dean M. Wingerchuk a and Claudia F. Lucchinetti b Purpose of review Advanced immunopathological
Bachelor of Chinese Medicine ( ) AUTOIMMUNE DISEASES
 Bachelor of Chinese Medicine (2002 2003) BCM II Dr. EYT Chan February 6, 2003 9:30 am 1:00 pm Rm 134 UPB AUTOIMMUNE DISEASES 1. Introduction Diseases may be the consequence of an aberrant immune response,
Bachelor of Chinese Medicine (2002 2003) BCM II Dr. EYT Chan February 6, 2003 9:30 am 1:00 pm Rm 134 UPB AUTOIMMUNE DISEASES 1. Introduction Diseases may be the consequence of an aberrant immune response,
Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
 Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
Mao et al. BMC Neurology (2015) 15:160 DOI 10.1186/s12883-015-0417-y RESEARCH ARTICLE Open Access Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositive patients in a Chinese population
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study
 Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Soliris in NMOSD Phase 3 PREVENT Study Topline Results September 24, 2018
 Soliris in NMOSD Phase 3 PREVENT Study Topline Results September 24, 2018 Forward-Looking Statements This presentation contains forward-looking statements within the meaning of the Private Securities Litigation
Soliris in NMOSD Phase 3 PREVENT Study Topline Results September 24, 2018 Forward-Looking Statements This presentation contains forward-looking statements within the meaning of the Private Securities Litigation
Contents 1 Immunology for the Non-immunologist 2 Neurology for the Non-neurologist 3 Neuroimmunology for the Non-neuroimmunologist
 1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
Neurological update: MOG antibody disease
 https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
https://doi.org/10.1007/s00415-018-9122-2 NEUROLOGICAL UPDATE Neurological update: MOG antibody disease Ray Wynford Thomas 1,2 Anu Jacob 3 Valentina Tomassini 1,2,4 Received: 17 August 2018 / Revised:
ORIGINAL CONTRIBUTION. Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression Sean J. Pittock, MD; Brian G. Weinshenker, MD; Claudia F. Lucchinetti, MD; Dean M. Wingerchuk,
ORIGINAL CONTRIBUTION Neuromyelitis Optica Brain Lesions Localized at Sites of High Aquaporin 4 Expression Sean J. Pittock, MD; Brian G. Weinshenker, MD; Claudia F. Lucchinetti, MD; Dean M. Wingerchuk,
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
Association between neuromyelitis optica and tuberculosis in a Chinese population
 Li et al. BMC Neurology 2014, 14:33 RESEARCH ARTICLE Open Access Association between neuromyelitis optica and tuberculosis in a Chinese population Rui Li, Xiaonan Zhong, Wei Qiu, Aimin Wu, Yongqiang Dai,
Li et al. BMC Neurology 2014, 14:33 RESEARCH ARTICLE Open Access Association between neuromyelitis optica and tuberculosis in a Chinese population Rui Li, Xiaonan Zhong, Wei Qiu, Aimin Wu, Yongqiang Dai,
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review.
 Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
Neuromyelitis Optica Spectrum Disorder (NMOSD): Brain MRI findings in patients at our institution and literature review. Poster No.: C-0817 Congress: ECR 2014 Type: Educational Exhibit Authors: G. I. MICHELIN,
Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica
 Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
Elmer ress Case Report J Neurol Res. 2014;4(5-6):145-149 Ocular Oscillations and Transient Oscillopsia in Neuromyelitis Optica Nitin Nema a, c, Abha Verma a, Urvija Choudhary a, Pramod Sakhi b Abstract
CASE OF THE WEEK PROFESSOR YASSER METWALLY
 CLINICAL PICTURE CLINICAL PICTURE: A 25 years old male patient presented clinically with transverse myelitis of acute onset. The patient gave a history of flu- like symptoms 10 days before the onset of
CLINICAL PICTURE CLINICAL PICTURE: A 25 years old male patient presented clinically with transverse myelitis of acute onset. The patient gave a history of flu- like symptoms 10 days before the onset of
MEDIA BACKGROUNDER. Multiple Sclerosis: A serious and unpredictable neurological disease
 MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
Neuroimmunology. Innervation of lymphoid organs. Neurotransmitters. Neuroendocrine hormones. Cytokines. Autoimmunity
 Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
An overview of NMO Spectrum Disorder and the diagnostic utility of anti-nmo antibodies
 The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
The Hong Kong College of Pathologists, Incorporated in Hong Kong with Limited Liability Volume 13, Issue 1 January 2018 Editorial note: NMOSD is an immune mediated demyelinating disease. Though its clinical
MRI Imaging of Neuromyelitis Optica
 July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
Thashi Chang 1,2* and Milinda Withana 2
 Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
Chang and Withana BMC Research Notes (2015) 8:36 DOI 10.1186/s13104-015-0991-5 CASE REPORT Open Access Gaze palsy, hypogeusia and a probable association with miscarriage of pregnancy - the expanding clinical
NIH Public Access Author Manuscript Arch Neurol. Author manuscript; available in PMC 2012 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2011 July ; 68(7): 870 878. doi:10.1001/archneurol.2011.34. Beneficial Plasma Exchange Response in CNS Inflammatory Demyelination
This is an Open Access document downloaded from ORCA, Cardiff University's institutional repository:
 This is an Open Access document downloaded from ORCA, Cardiff University's institutional repository: http://orca.cf.ac.uk/100325/ This is the author s version of a work that was submitted to / accepted
This is an Open Access document downloaded from ORCA, Cardiff University's institutional repository: http://orca.cf.ac.uk/100325/ This is the author s version of a work that was submitted to / accepted
PMH: No medications; Immunizations UTD No hospitalizations or surgeries Speech Delay. Birth Hx: 24 WGA, NICU x6 months
 HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
. Autoimmune disease. Dr. Baha,Hamdi.AL-Amiedi Ph.D.Microbiology
 . Autoimmune disease Dr. Baha,Hamdi.AL-Amiedi Ph.D.Microbiology, Paul Ehrich The term coined by the German immunologist paul Ehrich ( 1854-1915) To describe the bodys innate aversion to immunological
. Autoimmune disease Dr. Baha,Hamdi.AL-Amiedi Ph.D.Microbiology, Paul Ehrich The term coined by the German immunologist paul Ehrich ( 1854-1915) To describe the bodys innate aversion to immunological
Neuromyelitis optica mimics the morphology of spinal cord tumors
 The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
The Turkish Journal of Pediatrics 2016; 58: 309-314 Case Report Neuromyelitis optica mimics the morphology of spinal cord tumors İlknur Erol 1, Murat Özkale 2, Tülin Savaş 1, Özlem Alkan 3, Melih Çekinmez
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt.
 MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES
 NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES Dean M. Wingerchuk, MD, MSc, FRCP(C) Mayo Clinic Scottsdale, AZ Neuromyelitis optica (NMO; Devic s syndrome) consists of optic neuritis and transverse
NMOSD: CURRENT AND EMERGING THERAPIES AND STRATEGIES Dean M. Wingerchuk, MD, MSc, FRCP(C) Mayo Clinic Scottsdale, AZ Neuromyelitis optica (NMO; Devic s syndrome) consists of optic neuritis and transverse
The Pathogenesis of Chlamydia pneumoniae in Multiple Sclerosis: Current Thoughts and Future Directions
 The Pathogenesis of Chlamydia pneumoniae in Multiple Sclerosis: Current Thoughts and Future Directions Seminars in Pathology March 9, 2010 Charles W. Stratton, M.D. Features of C. pneumoniae Infection
The Pathogenesis of Chlamydia pneumoniae in Multiple Sclerosis: Current Thoughts and Future Directions Seminars in Pathology March 9, 2010 Charles W. Stratton, M.D. Features of C. pneumoniae Infection
Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum disorders: a case series study
 Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
Jiao et al. BMC Neurology (2018) 18:47 https://doi.org/10.1186/s12883-018-1056-x RESEARCH ARTICLE Open Access Dose effects of mycophenolate mofetil in Chinese patients with neuromyelitis optica spectrum
THE FIRST DESCRIPTION OF BIlateral
 CLINICAL SCIENCES Clinical Course of Optic Neuritis in Patients With Relapsing Neuromyelitis Optica Regina Maria Papais-Alvarenga, MD, MSc, PhD; Sandro Carvalho Carellos, MD, MSc; Marcos Papais Alvarenga,
CLINICAL SCIENCES Clinical Course of Optic Neuritis in Patients With Relapsing Neuromyelitis Optica Regina Maria Papais-Alvarenga, MD, MSc, PhD; Sandro Carvalho Carellos, MD, MSc; Marcos Papais Alvarenga,
Yoko Warabi, Mikihiro Yamazaki, Toshio Shimizu, and Masahiro Nagao. 1. Introduction. 2. Patients and Methods
 BioMed Research International Volume 2013, Article ID 847670, 6 pages http://dx.doi.org/10.1155/2013/847670 Research Article Abnormal Nerve Conduction Study Findings Indicating the Existence of Peripheral
BioMed Research International Volume 2013, Article ID 847670, 6 pages http://dx.doi.org/10.1155/2013/847670 Research Article Abnormal Nerve Conduction Study Findings Indicating the Existence of Peripheral
New Insights into Neuromyelitis Optica
 REVIEW J Clin Neurol 2011;7:115-127 Print ISSN 1738-6586 / On-line ISSN 2005-5013 http://dx.doi.org/10.3988/jcn.2011.7.3.115 Open Access New Insights into Neuromyelitis Optica Woojun Kim, Su-Hyun Kim,
REVIEW J Clin Neurol 2011;7:115-127 Print ISSN 1738-6586 / On-line ISSN 2005-5013 http://dx.doi.org/10.3988/jcn.2011.7.3.115 Open Access New Insights into Neuromyelitis Optica Woojun Kim, Su-Hyun Kim,
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Myelitis. Myelitis. Multiple Sclerosis (MS) Acute demyelinating syndrome (ADS) Indictions for spinal cord MRI in MS.
 Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
Myelitis Myelitis Majda M Thurnher Professor of Radiology Medical University of Vienna University Hospital Vienna Department of Biomedical Imaging and Image-Guided Therapy Vienna Austria Acute demyelinating
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Implication of aquaporins in ischemic stroke. New target?
 Implication of aquaporins in ischemic stroke. New target? Balseanu Tudor-Adrian, MD, PhD EXPERIMENTAL RESEARCH CENTER OF NORMAL AND PATHOLOGICAL AGING University of Medicine and Pharmacy of Craiova, Romania
Implication of aquaporins in ischemic stroke. New target? Balseanu Tudor-Adrian, MD, PhD EXPERIMENTAL RESEARCH CENTER OF NORMAL AND PATHOLOGICAL AGING University of Medicine and Pharmacy of Craiova, Romania
The Incidence and Prevalence of Neuromyelitis Optica
 The Incidence and Prevalence of Neuromyelitis Optica A Systematic Review Ruth Ann Marrie, MD, PhD; Caroline Gryba, BSc Interest in neuromyelitis optica (NMO) has increased substantially over the last few
The Incidence and Prevalence of Neuromyelitis Optica A Systematic Review Ruth Ann Marrie, MD, PhD; Caroline Gryba, BSc Interest in neuromyelitis optica (NMO) has increased substantially over the last few
Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a
 Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a hematoma that compresses the brain surface. - Clinically,
Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a hematoma that compresses the brain surface. - Clinically,
Multiple Sclerosis and Neuroinflammation: Considering Gender differences to design therapeutic agents HALINA OFFNER
 Multiple Sclerosis and Neuroinflammation: Considering Gender differences to design therapeutic agents HALINA OFFNER Sex differences in autoimmune disease Ratio Target Sex distribution of major autoimmune
Multiple Sclerosis and Neuroinflammation: Considering Gender differences to design therapeutic agents HALINA OFFNER Sex differences in autoimmune disease Ratio Target Sex distribution of major autoimmune
DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI Page 1 Page 2 multiple sclerosis the history of a disease multiple sclerosis the history pdf multiple sclerosis the history
DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI Page 1 Page 2 multiple sclerosis the history of a disease multiple sclerosis the history pdf multiple sclerosis the history
Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation
 Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation Marcelo C. Pasquini, MD, MSc HVD05_1.ppt Outline Review of autoimmune diseases (AID). Role of transplantation for AID Data collection:
Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation Marcelo C. Pasquini, MD, MSc HVD05_1.ppt Outline Review of autoimmune diseases (AID). Role of transplantation for AID Data collection:
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Immunology. Lecture- 8
 Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
An autoimmune perspective on neuromuscular diseases
 An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis
 The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
The Use of Serum Glial Fibrillary Acidic Protein Measurements in the Diagnosis of Neuromyelitis Optica Spectrum Optic Neuritis Mithu Storoni 1,2 *, Axel Petzold 1,3, Gordon T. Plant 1,2 1 The National
Mucosal Immune System
 Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Clinical Study The Diagnostic and Prognostic Value of Neurofilament Heavy Chain Levels in Immune-Mediated Optic Neuropathies
 Multiple Sclerosis International Volume 0, Article ID 780, 5 pages doi:0.55/0/780 Clinical Study The Diagnostic and Prognostic Value of Neurofilament Heavy Chain Levels in Immune-Mediated Optic Neuropathies
Multiple Sclerosis International Volume 0, Article ID 780, 5 pages doi:0.55/0/780 Clinical Study The Diagnostic and Prognostic Value of Neurofilament Heavy Chain Levels in Immune-Mediated Optic Neuropathies
CNS third year med students Summary of midterm material H Awad
 CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
Atypical presentations of neuromyelitis optica
 View and review Arq Neuropsiquiatr 2011;69(5):824-828 Atypical presentations of neuromyelitis optica Douglas Sato 1,2, Kazuo Fujihara 3 ABSTRACT Neuromyelitis optica (NMO) is an inflammatory disease of
View and review Arq Neuropsiquiatr 2011;69(5):824-828 Atypical presentations of neuromyelitis optica Douglas Sato 1,2, Kazuo Fujihara 3 ABSTRACT Neuromyelitis optica (NMO) is an inflammatory disease of
Interactive Cases: Demyelinating Diseases and Mimics. Disclosures. Case 1 25 yo F with nystagmus; look for tumor 4/14/2017
 Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D
 Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D Maureen A. Mealy, PhD(c), RN; Audra Boscoe, PhD; Jaime Caro, MDCM; Michael Levy, MD, PhD From the Department of Neurology,
Assessment of Patients with Neuromyelitis Optica Spectrum Disorder Using EQ-5D Maureen A. Mealy, PhD(c), RN; Audra Boscoe, PhD; Jaime Caro, MDCM; Michael Levy, MD, PhD From the Department of Neurology,
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology
 Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Transverse Myelitis and Myelopathy in the VA system: Etiology and Epidemiology Stacey L. Clardy MD PhD Staff Neurologist, Salt Lake City VA Assistant Professor of Neurology, University of Utah Director,
Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases.
 Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
Author's response to reviews Title: Recurrent myelitis after allogeneic stem cell transplantation. Report of two cases. Authors: Martin Voss (Martin.Voss@kgu.de) Felix Bischof (Felix.Bischof@uni-tuebingen.de)
