Available online at
|
|
|
- Madlyn Harrington
- 5 years ago
- Views:
Transcription
1 Annals of Clinical & Laboratory Science, vol. 45, no. 1, 2015 Available online at Congenital Peribronchial Myofibroblastic Tumor: Case Report of an Asymptomatic Infant with a Rapidly Enlarging Pulmonary Mass and Review of the Literature Katharine E. Brock 1,2, James Wall 3, Micaela Esquivel 4, Beverley Newman 5, Neyssa Marina 1,2, Craig Albanese 3, and Florette K. Hazard 1,6 Stanford University School of Medicine, 1 Department of Pediatrics, 2 Division of Pediatric Hematology/Oncology, 3 Department of Surgery, Division of Pediatric Surgery, 4 Department of Surgery, 5 Department of Radiology, and 6 Department of Pathology, Stanford, CA, USA Abstract. Background. Congenital peribronchial myofibroblastic tumor (CPMT) is a rare, benign lung tumor of infants, with only 19 reported cases worldwide. It is often diagnosed by prenatal imaging or in the immediate postnatal period due to co-morbidities like polyhydramnios, fetal hydrops, respiratory distress, and heart failure. Observation. We report the oldest known infant (8 weeks old) diagnosed with CPMT, and present his clinical course including the relevant radiographic and histopathologic findings. Conclusions. CPMT is a rare tumor that should be considered among other primary lung tumors of infancy (developmental, benign, and malignant) even if not detected prenatally or in the immediate postnatal period. Keywords: congenital peribronchial myofibroblastic tumor, neonatal, benign lung tumor, pleuropulmonary blastoma. 83 Introduction Congenital peribronchial myofibroblastic tumor (CPMT) is a rare, benign primary lung tumor of infants with no reported cases of local recurrence or distant metastases following complete surgical resection. Only 19 cases have been reported worldwide (Table 1) [1-17]. CPMT is most often detected by prenatal imaging, although affected patients can present in the immediate postnatal period. Presenting signs/symptoms include respiratory distress, heart failure, polyhydramnios, nonimmune hydrops fetalis, and intrauterine fetal death [4,6,9,11,13]. Historically, this tumor has been known by many names: bronchopulmonary leiomyosarcoma, bronchopulmonary fibrosarcoma, congenital fibroleiomyosarcoma, hamartoma, and congenital mesenchymal/adenomatoid malformation [18]. Address correspondence to Katharine E. Brock, MD; Division of Pediatric Hematology/Oncology, Stanford University School of Medicine; 1000 Welch Road, Suite 300, Palo Alto, CA, ; phone: ; fax: ; e mail: kebrock@stanford. edu We report the case of an 8-week-old infant with an incidental, rapidly-growing CPMT. We also review the common entities considered in the differential diagnosis of lung masses in infants, describe their clinical, radiographic and pathologic features, and recommended treatment. This patient s unusual presentation illustrates the need to maintain a broad differential diagnosis when evaluating lung masses in infants; CPMT should be considered, even if not detected prenatally or in the immediate postnatal period. Case Report We report an 8-week-old Swedish/Mexican male, born at 38 weeks gestation to a 36-year-old mother. No family history of cancer was noted. Regularly scheduled prenatal ultrasounds did not reveal a mass or polyhydramnios. Chorionic villous sampling (performed for abnormal quadruple screen) confirmed a normal 46, XY karyotype. The mother had an uneventful vaginal delivery, and the infant experienced no hydrops or respiratory distress. Physical exam revealed a left pre-auricular pit and partial heterochromia of the left iris /15/ by the Association of Clinical Scientists, Inc.
2 84 Annals of Clinical & Laboratory Science, vol. 45, no. 1, 2015 Table 1. Summary of case reports of congenital peribronchial myofibroblastic tumor. Author Age at Sex Tumor Tumor Nonimmune Diagnosis Treatment Outcome presentation Location size(cm) hydrops (weeks gestation) fetalis Jones [1] 28 F RUL Hamartoma None Died, 1 hour Robb [2] 40 M LLL Fibrosarcoma Lobectomy NED,10months Guccion [3] NS M LUL 6 - Leiomyosarcoma None Died at birth Haller [4] 40 F LLL CMT None Died, 8 hours Warren [5] F LUL, LLL CMM Pneumonectomy Died, 24 hours Jimenez [6] 36 M RLL Leiomyosarcoma Lobectomy NED, 34 months Pettinato [7] NS M LUL 6 - PBPF Lobectomy NED, 6 years Pettinato [7] NS M RLL PBPF Lobectomy NED, 3 months Khong [8] 27 M RUL CMM None Died at birth McGinnis [9] 33 M RUL 5 + CPBMT Pneumonectomy Intraoperative death Alobeid [10] 35 F RML, RLL 6 - CPMT Lobectomy NED, 12 months (middle and lower) Horikoshi [11] 30 M LLL 6 + CPMT None IUFD Reiss [12] 25 M L lung CPMT None Elective termination de Noronha [13] 24 M LLL 12 + CPMT None IUFD Huppman [14] 23 M LUL, LLL 6.6^ + CPMT Lobectomy & NED, 6.5 years completion pneumonectomy Kim [15] 4 postnatal F RML, RLL CPMT Bilobectomy NED, 2 years weeks (42) Chang [16] 32.5 F LLL 5.2 # - CPMT None Died, 17 days Chang [16] Full term F RLL 6.5 # - CPMT Surgical resection Intraoperative death Calvo-Garcia [17] 30 M LUL CPMT Lobectomy by NED, 17 months intrauterine surgery Current case 8 postnatal M RLL, RML CPMT Pneumonectomy NED, 16 months weeks (46) CMT, congenital mesenchymal tumor; CMM, congenital mesenchymal malformation; CPBMT, congenital peribronchial myofibroblastic tumor; IUFD; intrauterine fetal demise; LLL, left lower lobe; LUL, left upper lobe; NED, no evidence of disease; NS, not specified; PBPF, primary bronchopulmonary fibrosarcoma; RLL, right lower lobe; RML, right middle lobe; RUL, right upper lobe; ^Fetal MRI measurement; # CT measurement
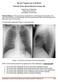
3 Congenital peribronchial myofibroblastic tumor: a case and review 85 Figure 1. Imaging. A. Chest X-ray demonstrating a right parahilar and lower lobe rounded opacity with air bronchograms. The remaining lung appears normally aerated. B and C. MRI (B. axial STIR series, C. Coronal T1 post-gad) showing right parahilar, T2 bright, moderately enhancing lesion that includes fluidfilled cysts, with extension into the posterior mediastinum, encasement of central bronchi, air bronchograms extending peripherally (C) and mediastinal shift. D and E. Contrast enhanced CT (D. Mediastinal window, E. Lung window) confirming the cystic and solid nature of the lesion surrounding central vessels and bronchi and extending to the posterior mediastinum. A few air-filled cysts can be seen anteriorly in panel E (arrow). At 8 weeks of age, he presented to a local emergency department with fever, congestion, and cough for one day. His oxygen saturations remained above 95%, and he had no respiratory distress. Chest x-ray revealed a well-demarcated, rounded consolidation in the right lower lobe with air bronchograms and hilar lymphadenopathy (Figure 1A). Complete blood count, chemistry panel, lactate dehydrogenase, and uric acid were normal. Magnetic resonance imaging (MRI) of the chest (and subsequent computed tomography (CT)) showed a large enhancing, mixed solid and cystic lesion in the parahilar right lung extending to the mediastinum, causing mediastinal shift (Figure 1B,C). The radiographic differential included an infected congenital pulmonary airway malformation (CPAM), neoplasm such as pleuropulmonary blastoma (PPB), and round pneumonia. An infected CPAM or PPB were thought to be the most likely diagnoses, and the patient was taken for an open thoracotomy which revealed a large, predominately solid mass occupying the right upper, middle, and lower lobes without edema, purulence, effusion, or pleural nodularity. The mass firmly adhered to the esophagus, pericardium, and pulmonary hilar vessels. Frozen section evaluation was consistent with malignancy. A right pneumonectomy was performed, followed by segmental resection of a portion of the remaining right mainstem bronchus, to achieve complete resection. The infant recovered without complications and was discharged on postoperative day five. Based on concern for PPB, a metastatic work-up was completed (bone scan, brain MRI, CT of the chest/abdomen/pelvis, and ultrasound of the kidneys and urinary bladder). No imaging studies showed metastases. Within two months of the resection, the patient s breathing pattern normalized. Given the presence of tumor at the hilar resection margin, follow-up has included alternating chest CT and chest x-ray. He is currently 16 months post-resection with no evidence of disease recurrence. Pathologic examination. The right lung measured 10.0x8.5x4.5 cm and, upon sectioning, was noted to contain a 3.5 cm firm white mass involving the right upper, middle, and lower lobes without visceral pleural involvement. Histologic sections confirmed the presence of a highly cellular spindle-cell proliferation arranged in fascicles, with extension to the hilar surgical margin (Figure 2). The spindled tumor cells showed moderate nuclear pleomorphism, some nuclear membrane irregularities, moderate to high nucleus to cytoplasm ratios, vesicular chromatin, occasional prominent nucleoli, eosinophilic cytoplasm, and frequent mitotic figures. There were no atypical mitotic figures present. Abundant cartilage formation was noted throughout, with several irregular cartilaginous islands. Scattered atrophic-appearing bronchioles and variably sized cystic spaces were also noted. With appropriate controls, immunohistochemical stains for cytokeratin (AE1 and CAM5.2), actin, desmin, CD34, and myogenin were negative within the
4 86 Annals of Clinical & Laboratory Science, vol. 45, no. 1, 2015 Figure 2. Pathology, Congenital Peribronchiolar Myofibroblastic Tumor. A. Lung hilum showing tumor infiltration adjacent to the cartilage of the bronchus (H&E stain; 10X magnification). B. Cellular spindled proliferation with admixed irregular cartilage islands (H&E stain; 40X magnification). C. Neoplastic spindled cells with moderate nuclear pleomorphism and frequent mitotic figures (H&E stain; 400X magnification). tumor cells. Fluorescent in situ hybridization testing for ALK gene mutations was negative. Cytogenetic analysis and genomic sequencing were not performed. An initial diagnosis of PPB Type II (solid and cystic) was rendered. However, based on the patient s young age, a cystic Type I PPB would have been expected. Thus, no further adjuvant therapy was given while expert consultative review was obtained, and the diagnosis was revised to congenital peribronchial myofibroblastic tumor (CPMT). Discussion Clinically, CPMT is a benign primary lung tumor of infants that is generally detected by prenatal imaging studies or in the immediate postnatal period. There is no predilection for gender, lobe, or laterality. It is associated with respiratory distress, heart failure, polyhydramnios, nonimmune fetal hydrops, and intrauterine fetal demise [1-7,9-14,18]. Treatment is complete surgical resection; there have been no recurrences described, even in cases with positive resection margins [14,15]. Chemotherapy and/or radiotherapy are not indicated for this benign tumor. However, due to the tumor s intimate association with the bronchial tree, lobectomy or pneumonectomy is often required. Despite the excellent prognosis after surgical resection, clinicians should be aware of pneumonectomy-related morbidity, notably mediastinal shift and post-pneumonectomy syndrome. The mediastinum and residual lung shift over time to fill the contralateral potential space. Post-pneumonectomy syndrome occurs when chronic extreme mediastinal shift leads to dynamic airway compromise. The empty thoracic cavity may need to be filled with prosthetic material to counteract mediastinal shift prior to irreversible airway distortion [19]. This 8-week-old infant with CPMT is unique in that there was no mass on prenatal imaging studies, and he was asymptomatic. The diagnosis of CMPT was challenging on multiple levels: radiographically, air bronchograms initially created diagnostic confusion as these are atypical of most intrapulmonary neoplasms; pathologically, this lesion resembled a Type II PPB. While the diagnosis of CMPT is complicated by its extreme rarity and need for multiple pathologic reviews, ultimately, our patient s lack of significant cytologic atypia, the tumor s close association with the bronchial tree, and the young age of the patient all support the diagnosis of CPMT. When considering primary lung masses in infants, the differential diagnosis should remain broad and include developmental malformations such as intralobar sequestration and congenital pulmonary airway malformation (CPAM); benign tumors such as fetal lung interstitial tumor (FLIT), infantile myofibromatosis, and CPMT; and malignant tumors such as pleuropulmonary blastoma (PPB) and infantile fibrosarcoma (Table 2). CPMT is thought to arise from pleuripotent peribronchial interstitial mesenchymal cells found at 12 weeks of gestation, and may therefore
5 Congenital peribronchial myofibroblastic tumor: a case and review 87 share similar pathogenesis with other mesenchymal lesions such as FLIT and PPB [20]. CPMT tends to be a firm, yellow, rubbery mass with interlacing fascicles of spindle cells surrounding normal lobules of alveolated parenchyma, and extending along bronchovascular bundles, interlobular septa, and (less commonly) the pleura. Importantly, there is no destruction or invasion of the airways. Mitotic figures can be frequent, but there is no significant cytologic atypia or atypical mitoses. Generally, immunohistochemistry is diffusely positive for vimentin with focal positivity for muscle specific actin, smooth muscle actin, and desmin. The tumor is negative for alpha-fetoprotein (AFP), GFAP, MyoD1, CD99, ALK1, S100, and cytokeratin [18]. Cytogenetics have been scarcely reported in the literature, but one case did show a complex rearrangement of chromosomes 4, 8, and 10[10]. Pulmonary sequestrations may be intralobar (an aerated focus of lung parenchyma that developed separately from the surrounding lung, with its own arterial blood supply) or extralobar (a solid and non-aerated mass). Their histopathologic features are similar to normal lung parenchyma [21]. Congenital pulmonary airway malformation (CPAM) is characterized by a haphazard distribution of bronchioles with an incomplete branching pattern, variably sized cysts and occasional metaplastic changes. These malformations may regress through the first year of life. Large, symptomatic CPAMs are associated with increased fetal morbidity/mortality and may require resection. Postnatal surgical resection is recommended for lesions that do not regress, become infected, cause respiratory distress, or develop solid components, indicating possible malignancy [21]. Fetal lung interstitial tumor (FLIT) is a benign, well-demarcated tumor that recapitulates fetal canalicular stage development, occurring at weeks gestation. It is hypothesized that FLIT reflects focal regions of arrested lung development (Table 2) [20]. Pleuropulmonary blastoma (PPB) is a malignant tumor of interstitial cells that is associated with DICER1 gene mutations and may be familial or sporadic [20]. Infants usually present with the cystic form (Type I), and as they age, can progress to the cystic solid form (Type II) and solid form (Type III) (Table 2). Chemotherapy recommendations for Types II and III continue to evolve, but vincristine, actinomycin D, ifosfamide, and doxorubicin are thought to be active agents in the treatment of PPB. While complete surgical resection may be curative, close monitoring for local recurrence, distant metastases, and associated tumors (i.e. cystic nephroma, thyroid goiters, and ovarian sex cord stromal tumors) is required [18]. Distinguishing Type II PPB from CPMT by radiography and histopathology can be challenging. The distinction is largely based on age, as PPB in a child less than one-year-old should be purely cystic (Type I) with a mild expansion of septa and a uniform population of primitive mesenchymal cells. Type II PPB develops at a median of three years of age. Our patient, despite having a mixed cystic/ solid lesion consistent with Type II PPB, presented at 8 weeks of age. This is an important clinical distinction, as Type II/III PPB have metastatic potential and are generally treated with chemotherapy, whereas CPMT does not recur or metastasize after surgical resection. Infantile (congenital) fibrosarcoma is a malignant tumor of interstitial/mesenchymal cells that rarely occurs in the lung. It is characterized by t(12;15) (p13;q25) leading to a ETV6-NTRK3 fusion. Treatment with observation alone (in patients with a complete resection), or with vincristine/doxorubicin/cyclophosphamide, or vincristine/dactinomycin/cyclophosphamide (in patients with incomplete resection) yields five-year event-free survival rates near 70% [22]. In summary, we report a diagnosis, at the most advanced age known, of a CPMT that was not present on prenatal imaging studies or within the immediate postnatal period. CPMT is a benign primary lung tumor of infancy with complications that range from respiratory distress, heart failure, polyhydramnios, and nonimmune hydrops fetalis to intrauterine fetal death. Pathologic diagnosis is characterized by bland spindled cells and atypical cartilage islands with an infiltrative growth pattern arising from the peribronchial interstitial
6 Table 2. Clinical, radiographic and pathologic features of congenital lung lesions and their usual treatment. 88 Diagnosis Congenital Fetal Lung Pleuropulmonary Congenital Congenital Sequestration Peribronchial Interstitial Tumor Blastoma Infantile Pulmonary (Intralobar/ Myofibroblastic (FLIT) (PPB) Fibrosarcoma Airway Extrolobar) Tumor (CPMT) (CIFS) Malformation (CPAM) Annals of Clinical & Laboratory Science, vol. 45, no. 1, 2015 Clinical Features Respiratory +/-100% +/- (8/10 cases) [20] ++ +/- 2/3 of cases +/- insufficiency(%) Many detected 100% Type I - 54% (median 10 months) 80% 90% Likely majority for both Diagnosed in prenatally Often within first 10 Type II - 3% (median 34 months) Very rarely intralobar and extralobar first year of life days of life, up to Type III - 1% [18] type 3 (with increased utilization 3 months[20] (median 44 months) of prenatal ultrasound) Nonimmune fetal hydrops +/- (9/20 cases) +/- (rare) +/- (rare) +/- 5-10% of cases - Pleural effusion +/- (5/20 cases) - +/- (rare) +/- +/- +/- Polyhydramnios +/- (6/20 cases) - +/- (rare) - +/- - Radiographic Features Pneumothorax - +/- + +/- +/- +/- Other features Solid, enhancing Solid, enhancing Type 1- air filled, single cyst Generally a solid Lobar, single. Most often medial, left, mass. mass. or multicystic mass. Peripheral, mass. Types 1 and 2 lower lobe. Often mixed Can have cystic Generally single, lobar. multifocal lesions more common. Only rarely are aerated soon solid and cystic. Intralobar or necrotic May contain small cysts. Type 2- both cystic and solid reported in after birth. often aerated and hyperinflated. components. components or cysts with nodules the lung. Type 1-multiple, Extralobar usually solid. Often central Type 3- usually large and solid larger air filled Systemic artery(s) arise from in location. with pleural/mediastinal cysts >3.5cm aorta. Possible air extension Type 2-small cysts bronchograms Type 3-solid appearing with some enhancement Pathologic Features Spindled interstitial/ Yes No Yes Yes No No mesenchymal proliferation Systemic feeding artery No No No No No Yes Gene mutations None None DICER1 [20] ETV6-NTRK3 [22] None None TP53 mutations Cytogenetic abnormalities Rearrangements None Trisomy 8 t (12;15)(p13;q25) None None of ch. 4, 8 and 10 Trisomy 2 [23] in one patient [10] Treatment Most reported treatment Lobectomy or Wedge excision Lobectomy with complete Complete surgical Close observation, Close observation versus in the literature pneumonectomy or lobectomy resection of locally invasive disease resection, or if requires surgical resection when feasible, +/- chemotherapy resection, +/- chemotherapy +/- radiation therapy segmentectomy vs +/- radiation therapy lobectomy
7 Congenital peribronchial myofibroblastic tumor: a case and review 89 mesenchyme. This case illustrates the need to maintain a broad differential diagnosis and consider CPMT when evaluating lung masses in infants, even those outside the immediate postnatal period. In addition, we would recommend that in future cases, detailed immunohistochemical and cytogenetic analysis be performed, and that tissue be banked for genomic sequencing. Great care should be taken to avoid common pitfalls of misdiagnosing CPMT as a developmental malformation, malignant neoplasm, or pneumonia. References 1. Jones CJ. Unusual hamartoma of the lung in a newborn infant. Arch. Pathol. 1949;48(2): Robb D. A case of neonatal fibrosarcoma of lung. Br. J. Surg. 1958;46(196): Guccion JG, Rosen SH. Bronchopulmonary leiomyosarcoma and fibrosarcoma. A study of 32 cases and review of the literature. Cancer. 1972;30(3): Haller JO, Kauffman SL, Kassner EG. Congenital mesenchymal tumour of the lung. Br. J. Radiol. 1977;50(591): Warren JS, Seo IS, Mirkin LD. Massive congenital mesenchymal malformation of the lung: a case report with ultrastructural study. Pediatr. Pathol. Affil. Int. Paediatr. Pathol. Assoc. 1985;3(2-4): Jimenez JF, Uthman EO, Townsend JW, Gloster ES, Seibert JJ. Primary bronchopulmonary leiomyosarcoma in childhood. Arch. Pathol. Lab. Med. 1986;110(4): Pettinato G, Manivel JC, Saldana MJ. Primary bronchopulmonary fibrosarcoma of childhood and adolescence: reassessment of a low-grade malignancy. Clinicopathologic study of five cases and review of the literature. Hum. Pathol. 1989;20(5): Khong TY, Keeling JW. Massive congenital mesenchymal malformation of the lung: another cause of non-immune hydrops. Histopathology. 1990;16(6): McGinnis M, Jacobs G, el-naggar A, Redline RW. Congenital peribronchial myofibroblastic tumor (so-called congenital leiomyosarcoma ). A distinct neonatal lung lesion associated with nonimmune hydrops fetalis. Mod. Pathol. Off. J. United States Can. Acad. Pathol. Inc. 1993;6(4): Alobeid B, Beneck D, Sreekantaiah C, Abbi RK, Slim MS. Congenital pulmonary myofibroblastic tumor: a case report with cytogenetic analysis and review of the literature. Am. J. Surg. Pathol. 1997;21(5): Horikoshi T, Kikuchi A, Matsumoto Y, Tatematsu M, Takae K, Ogiso Y, Nakayama M, Unno N. Fetal hydrops associated with congenital pulmonary myofibroblastic tumor. J. Obstet. Gynaecol. Res. 2005;31(6): Reiss A, Goldberg Y, Monichor M, Drugan A. Congenital pulmonary myofibroblastic tumor--pathology and prenatal sonographic appearance. Prenat. Diagn. 2005;25(11): De Noronha L, Cecílio WAC, da Silva TFA, MaggioEM, Serapiao, MJ. Congenital peribronchial myofibroblastic tumor: a case report. Pediatr. Dev. Pathol. Off. J. Soc. Pediatr. Pathol. Paediatr. Pathol. Soc. 2010;13(3): Huppmann AR, Coffin CM, Hoot AC, Kahwash S, Pawel BR. Congenital peribronchial myofibroblastic tumor: comparison of fetal and postnatal morphology. Pediatr. Dev. Pathol. Off. J. Soc. Pediatr. Pathol. Paediatr. Pathol. Soc. 2011;14(2): Kim Y, Park HY, Cho J, Han J, Cho EY. Congenital peribronchial myofibroblastic tumor: a case study and literature review. Korean J. Pathol. 2013;47(2): Chang C, Hung L-Y, Thanh TT, Lai CH, Chang KC. Congenital peribronchial myofibroblastic tumour with features of maturation in the older infant: report of two cases with a literature review. Histopathology. 2014;64(5): Calvo-Garcia MA, Lim F-Y, Stanek J, Bitters C, Kline-Fath BM. Congenital peribronchial myofibroblastic tumor: prenatal imaging clues to differentiate from other fetal chest lesions. Pediatr. Radiol. 2014;44(4): Dishop MK, Kuruvilla S. Primary and metastatic lung tumors in the pediatric population: a review and 25-year experience at a large children s hospital. Arch. Pathol. Lab. Med. 2008;132(7): Soll C, Hahnloser D, Frauenfelder T, Russi EW, Weder W, Kestenholz PB. The postpneumonectomy syndrome: clinical presentation and treatment. Eur. J. Cardio-Thorac. Surg. Off. J. Eur. Assoc. Cardio-Thorac. Surg. 2009;35(2): Dishop MK, McKay EM, Kreiger PA, Priest JR, Williams GM, Langston C, Jarzembowski J, Suchi M, Dehner LP, Hill DA. Fetal lung interstitial tumor (FLIT): A proposed newly recognized lung tumor of infancy to be differentiated from cystic pleuropulmonary blastoma and other developmental pulmonary lesions. Am. J. Surg. Pathol. 2010;34(12): Langston C. New concepts in the pathology of congenital lung malformations. Semin. Pediatr. Surg. 2003;12(1): Loh ML, Ahn P, Perez-Atayde AR, Gebhardt MC, Shamberger RC, Grier HE. Treatment of infantile fibrosarcoma with chemotherapy and surgery: results from the Dana-Farber Cancer Institute and Children s Hospital, Boston. J. Pediatr. Hematol. Oncol. 2002;24(9): Quilichini B, Andre N, Bouvier C, Chrestian MA, Rome A, Intagliata D, Coze C, Lena G, Zattara H. Hidden chromosomal abnormalities in pleuropulmonary blastomas identified by multiplex FISH. BMC Cancer. 2006;6:4.
Congenital Peribronchial Myofibroblastic Tumor: A Case Study and Literature Review
 The Korean Journal of Pathology 2013; 47: 172-176 CSE STUDY Congenital Peribronchial Myofibroblastic Tumor: Case Study and Literature Review Yuil Kim Ha Young Park Junhun Cho Joungho Han Eun Yoon Cho Department
The Korean Journal of Pathology 2013; 47: 172-176 CSE STUDY Congenital Peribronchial Myofibroblastic Tumor: Case Study and Literature Review Yuil Kim Ha Young Park Junhun Cho Joungho Han Eun Yoon Cho Department
Case Based Fetal Lung Masses
 Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation
 e10 Case Report: Thoracic THIEME It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation Fayza Haider 1 Khulood Al Saad 2 Fatima Al-Hashimi 3 Hakima Al-Hashimi
e10 Case Report: Thoracic THIEME It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation Fayza Haider 1 Khulood Al Saad 2 Fatima Al-Hashimi 3 Hakima Al-Hashimi
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration
 Canadian Respiratory Journal Volume 2016, Article ID 1460480, 4 pages http://dx.doi.org/10.1155/2016/1460480 Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration Nao
Canadian Respiratory Journal Volume 2016, Article ID 1460480, 4 pages http://dx.doi.org/10.1155/2016/1460480 Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration Nao
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Imaging of the Lung in Children
 Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS
 HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
A case of giant benign localized fibrous tumor of the pleura
 Turkish Journal of Cancer Vol.30 / No. 4/2000 A case of giant benign localized fibrous tumor of the pleura ALİ KEMAL UZUNLAR 1, MEHMET YALDIZ 1, İBRAHİM H. ÖZERCAN 2, FAHRİ YILMAZ 1, AKIN E. BALCI 3 1
Turkish Journal of Cancer Vol.30 / No. 4/2000 A case of giant benign localized fibrous tumor of the pleura ALİ KEMAL UZUNLAR 1, MEHMET YALDIZ 1, İBRAHİM H. ÖZERCAN 2, FAHRİ YILMAZ 1, AKIN E. BALCI 3 1
57th Annual HSCP Spring Symposium 4/16/2016
 An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The Spectrum of Management of Pulmonary Ground Glass Nodules
 The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
Division of Pathology
 Case 38 Adult woman with a 35mm right breast lump at the 10 o clock position. Excision performed. (Case contributed by Dr Mihir Gudi, KKH) Division of Pathology Merlion, One Fullerton Singapore Diagnosis
Case 38 Adult woman with a 35mm right breast lump at the 10 o clock position. Excision performed. (Case contributed by Dr Mihir Gudi, KKH) Division of Pathology Merlion, One Fullerton Singapore Diagnosis
أملس عضلي غرن = Leiomyosarcoma. Leiomyosarcoma 1 / 5
 Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation
 246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
Case 1. Clinical history
 Case 1 Case 1 Clinical history 17-month-old boy with a kidney tumor found during routine childhood care program. CT scan showed a solid mass. Chemotherapy was given for 4 weeks using actinomycin D and
Case 1 Case 1 Clinical history 17-month-old boy with a kidney tumor found during routine childhood care program. CT scan showed a solid mass. Chemotherapy was given for 4 weeks using actinomycin D and
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
PLEUROPULMONARY BLASTOMA - A RARE PEDIATRIC
 IJCRR Vol 04 issue 22 Section: Healthcare Category: Case Report Received on: 09/09/12 Revised on: 20/09/12 Accepted on: 02/10/12 PLEUROPULMONARY BLASTOMA - A RARE PEDIATRIC MALIGNANCY Rucha Ashar, Nandita
IJCRR Vol 04 issue 22 Section: Healthcare Category: Case Report Received on: 09/09/12 Revised on: 20/09/12 Accepted on: 02/10/12 PLEUROPULMONARY BLASTOMA - A RARE PEDIATRIC MALIGNANCY Rucha Ashar, Nandita
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis
 19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
Disclosure. Relevant Financial Relationship(s) None. Off Label Usage None MFMER slide-1
 Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Case 8 Soft tissue swelling
 Case 8 Soft tissue swelling 26-year-old female presented with a swelling on the back of the left knee joint since the last 6 months and chronic pain in the calf and foot since the last 2 months. Pain in
Case 8 Soft tissue swelling 26-year-old female presented with a swelling on the back of the left knee joint since the last 6 months and chronic pain in the calf and foot since the last 2 months. Pain in
Imaging in pediatric lung diseases The roles of CT and pathology in diagnosing inherited and developmental lung diseases
 Imaging in pediatric lung diseases The roles of CT and pathology in diagnosing inherited and developmental lung diseases Dr Alistair D Calder Consultant Radiologist We re not so different, you and I. Invasiveness
Imaging in pediatric lung diseases The roles of CT and pathology in diagnosing inherited and developmental lung diseases Dr Alistair D Calder Consultant Radiologist We re not so different, you and I. Invasiveness
Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma
 49 Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma Loredana Miglietta a Maria Angela Parodi b Luciano Canobbio b Luca Anselmi c a Medical
49 Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma Loredana Miglietta a Maria Angela Parodi b Luciano Canobbio b Luca Anselmi c a Medical
Part 1. Slides 1-38, Rita Alaggio Soft tissue tumors Trondheim 14. mars 2013
 Part 1 Slides 1-38, Rita Alaggio Soft tissue tumors Trondheim 14. mars 2013 Pediatric Pathology Soft Tissue Tumors AN UPDATE Rita Alaggio Azienda Ospedaliera Università di Padova Soft Tissue Tumors More
Part 1 Slides 1-38, Rita Alaggio Soft tissue tumors Trondheim 14. mars 2013 Pediatric Pathology Soft Tissue Tumors AN UPDATE Rita Alaggio Azienda Ospedaliera Università di Padova Soft Tissue Tumors More
Interstitial Lung Disease in Infants and Children
 Interstitial Lung Disease in Infants and Children David A. Mong, MD SUNDAY Andrew Mong MD Beyond the interstitium (path includes airways/airspace) Radiographic diffuse disease Adult Interstitial Lung Disease
Interstitial Lung Disease in Infants and Children David A. Mong, MD SUNDAY Andrew Mong MD Beyond the interstitium (path includes airways/airspace) Radiographic diffuse disease Adult Interstitial Lung Disease
ACCME/Disclosures ALK FUSION-POSITIVE MESENCHYMAL TUMORS. Tumor types with ALK rearrangements. Anaplastic Lymphoma Kinase. Jason L.
 Companion Meeting of the International Society of Bone and Soft Tissue Pathology The Evolving Concept of Mesenchymal Tumors ALK FUSION-POSITIVE MESENCHYMAL TUMORS Jason L. Hornick, MD, PhD March 13, 2016
Companion Meeting of the International Society of Bone and Soft Tissue Pathology The Evolving Concept of Mesenchymal Tumors ALK FUSION-POSITIVE MESENCHYMAL TUMORS Jason L. Hornick, MD, PhD March 13, 2016
CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. CYSTIC NEPHROMA
 Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
Lung Tumor Cases: Common Problems and Helpful Hints
 Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT
 Case Reports in Pulmonology Volume 2012, Article ID 276012, 4 pages doi:10.1155/2012/276012 Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT Serdar Şen, 1 Nilgün
Case Reports in Pulmonology Volume 2012, Article ID 276012, 4 pages doi:10.1155/2012/276012 Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT Serdar Şen, 1 Nilgün
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
1 NORMAL HISTOLOGY AND METAPLASIAS
 1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
Pulmonary Salivary Gland Type Tumors With Features of Malignant Mixed Tumor (Carcinoma Ex Pleomorphic Adenoma) A Clinicopathologic Study of Five Cases
 Anatomic Pathology / Pulmonary Salivary Gland Type Tumors Pulmonary Salivary Gland Type Tumors With Features of Malignant Mixed Tumor (Carcinoma Ex Pleomorphic Adenoma) A Clinicopathologic Study of Five
Anatomic Pathology / Pulmonary Salivary Gland Type Tumors Pulmonary Salivary Gland Type Tumors With Features of Malignant Mixed Tumor (Carcinoma Ex Pleomorphic Adenoma) A Clinicopathologic Study of Five
No financial or other disclosures
 Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Pulmonary Sequestration
 July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
Signs in Chest Radiology
 Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
years old female with paratracheal lymph nodes infiltration and mediastinal extension, who presented
 Case Report Inflammatory Myofibroblastic Tumour of the Trachea with Paratracheal Lymph Nodes and Mediastinal Invasion Salina Husain From Department of Otolaryngology, Univerti Kebengsaan, Malaysia. Received:
Case Report Inflammatory Myofibroblastic Tumour of the Trachea with Paratracheal Lymph Nodes and Mediastinal Invasion Salina Husain From Department of Otolaryngology, Univerti Kebengsaan, Malaysia. Received:
Thoracoscopic treatment of congenital malformation of the lung
 Jemis, 1 2013 Thoracoscopic treatment of congenital malformation of the lung Preliminary experience with preoperative 3D virtual rendering F. Destro M. Maffi T. Gargano G. Ruggeri L. Soler M. Lima Table
Jemis, 1 2013 Thoracoscopic treatment of congenital malformation of the lung Preliminary experience with preoperative 3D virtual rendering F. Destro M. Maffi T. Gargano G. Ruggeri L. Soler M. Lima Table
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Classification (1) Classification (3) Classification (2) Spindle cell lesions. Spindle cell lesions of bladder (Mills et al.
 Non-epithelial tumours and nonepithelial tumour-like lesions of the bladder Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Classification (1) Myofibroblastic proliferations and
Non-epithelial tumours and nonepithelial tumour-like lesions of the bladder Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Classification (1) Myofibroblastic proliferations and
ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH. Leonard E. Swischuk, M.D. University of Texas Medical Branch
 ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH Leonard E. Swischuk, M.D. University of Texas Medical Branch AUTHOR HAS NOTHING TO DECLARE LEARNING OBJETIVES Understand the pathophysiology
ACUTE PULMNARY INFECTIONS: UNDERSTANDING THE CHEST RADIOGRAPH Leonard E. Swischuk, M.D. University of Texas Medical Branch AUTHOR HAS NOTHING TO DECLARE LEARNING OBJETIVES Understand the pathophysiology
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Case Report Primary myoepithelial carcinoma of the lung: a case report and review of literature
 Int J Clin Exp Pathol 2015;8(2):2111-2116 www.ijcep.com /ISSN:1936-2625/IJCEP0004274 Case Report Primary myoepithelial carcinoma of the lung: a case report and review of literature Jianguo Wei 1, Xiaolu
Int J Clin Exp Pathol 2015;8(2):2111-2116 www.ijcep.com /ISSN:1936-2625/IJCEP0004274 Case Report Primary myoepithelial carcinoma of the lung: a case report and review of literature Jianguo Wei 1, Xiaolu
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program
 Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation
 Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation 1 Dr.Varsha Rathi, 2 Dr. Saurabh Deshpande*, 3 Dr.Almas Nazim, 4 Dr.Shilpa Domkundwar 1 Professor, Department
Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation 1 Dr.Varsha Rathi, 2 Dr. Saurabh Deshpande*, 3 Dr.Almas Nazim, 4 Dr.Shilpa Domkundwar 1 Professor, Department
Newer soft tissue entities
 Newer soft tissue entities Examples among fibroblastic tumors Turku, May 6, 2010 Markku Miettinen, M.D. AFIP, Washington, DC Fibroblastic neoplasms Solitary fibrous tumor /Hemangiopericytoma Low-grade
Newer soft tissue entities Examples among fibroblastic tumors Turku, May 6, 2010 Markku Miettinen, M.D. AFIP, Washington, DC Fibroblastic neoplasms Solitary fibrous tumor /Hemangiopericytoma Low-grade
Primary Rhabdomyosarcoma
 CASE REPORTS Primary Rhabdomyosarcoma of the Bronchus Graham Fallon, M.D., Medad Schiller, M.D., and James W. Kilman, M.D. ABSTRACT A 6-year-old child with an unresectable rhabdomyosarcoma of the right
CASE REPORTS Primary Rhabdomyosarcoma of the Bronchus Graham Fallon, M.D., Medad Schiller, M.D., and James W. Kilman, M.D. ABSTRACT A 6-year-old child with an unresectable rhabdomyosarcoma of the right
Bronchial syndrome. Atelectasis Draining bronchus Bronchiectasis
 Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
CONSULTATION DURING SURGERY / NOT A FINAL DIAGNOSIS. FROZEN SECTION DIAGNOSIS: - A. High grade sarcoma. Wait for paraffin sections results.
 Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
Pathology Report Date: 3/5/02 A, B. Biopsy right distal femur- high grade spindle cell sarcoma Immunohistochemistry studies are pending to further classify the nature of the tumor. CONSULTATION DURING
Brief History. Identification : Past History : HTN without regular treatment.
 Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS
 International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
Inflammatory Pseudotumor Suspected of Lung Cancer Treated by Thoracoscopic Resection
 Ann Thorac Cardiovasc Surg 2011; 17: 48 52 Case Report Inflammatory Pseudotumor Suspected of Lung Cancer Treated by Thoracoscopic Resection Shinji Hirai, MD, 1 Tatsuya Katayama, MD, 1 Naru Chatani, MD,
Ann Thorac Cardiovasc Surg 2011; 17: 48 52 Case Report Inflammatory Pseudotumor Suspected of Lung Cancer Treated by Thoracoscopic Resection Shinji Hirai, MD, 1 Tatsuya Katayama, MD, 1 Naru Chatani, MD,
Congenital lung anomalies: can we postpone resection?
 Journal of Pediatric Surgery (2012) 47, 87 92 www.elsevier.com/locate/jpedsurg Congenital lung anomalies: can we postpone resection? Nadja Colon a, Cameron Schlegel a, John Pietsch a, Dai H. Chung a,b,
Journal of Pediatric Surgery (2012) 47, 87 92 www.elsevier.com/locate/jpedsurg Congenital lung anomalies: can we postpone resection? Nadja Colon a, Cameron Schlegel a, John Pietsch a, Dai H. Chung a,b,
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
Synchronous squamous cell carcinoma of the breast. and invasive lobular carcinoma
 Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
A 25 year old female with a palpable mass in the right lower quadrant of her abdomen
 May 2016 A 25 year old female with a palpable mass in the right lower quadrant of her abdomen Contributed by: Paul Ndekwe, MD, Resident Physician, Indiana University School of Department of Pathology and
May 2016 A 25 year old female with a palpable mass in the right lower quadrant of her abdomen Contributed by: Paul Ndekwe, MD, Resident Physician, Indiana University School of Department of Pathology and
Congenital pulmonary fibrosarcoma in a newborn with hypoglycemia and respiratory distress: case report
 The Turkish Journal of Pediatrics 2010; 52: 325-329 Case Congenital pulmonary fibrosarcoma in a newborn with hypoglycemia and respiratory distress: case report Davut Şahin 1, Nermin Koç 1, Şeref Etker
The Turkish Journal of Pediatrics 2010; 52: 325-329 Case Congenital pulmonary fibrosarcoma in a newborn with hypoglycemia and respiratory distress: case report Davut Şahin 1, Nermin Koç 1, Şeref Etker
The International Association for the Study of Lung Cancer (IASLC) Lung Cancer Staging Project, Data Elements
 Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Imaging of cardio-pulmonary treatment related damage. Radiotheraphy and Lung
 Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
Diagnostic challenge: Sclerosing Hemangioma of the Lung. Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and
 Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
Bronchial carcinosarcoma
 Bronchial carcinosarcoma Carolina Carcano 1*, Edward Savage 2, Maria Julia Diacovo 3, Jacobo Kirsch 1 1. Division of Radiology, Cleveland Clinic Florida, Weston, Fl, USA 2. Department of Thoracic and Cardiovascular
Bronchial carcinosarcoma Carolina Carcano 1*, Edward Savage 2, Maria Julia Diacovo 3, Jacobo Kirsch 1 1. Division of Radiology, Cleveland Clinic Florida, Weston, Fl, USA 2. Department of Thoracic and Cardiovascular
Uniportal video-assisted thoracoscopic surgery segmentectomy
 Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Respiratory Tract Cytology
 Respiratory Tract Cytology 40 th European Congress of Cytology Liverpool, UK Momin T. Siddiqui M.D. Professor of Pathology and Laboratory Medicine Director of Cytopathology Emory University Hospital, Atlanta,
Respiratory Tract Cytology 40 th European Congress of Cytology Liverpool, UK Momin T. Siddiqui M.D. Professor of Pathology and Laboratory Medicine Director of Cytopathology Emory University Hospital, Atlanta,
Excavated pulmonary nodule: steps to diagnosis?
 Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Special slide seminar
 Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Synonyms. Nephrogenic metaplasia Mesonephric adenoma
 Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Disclosures. Giant Cell Rich Tumors of Bone. Outline. The osteoclast. Giant cell rich tumors 5/21/11
 Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010
 LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
Primitive Neuroectodermal Tumor of Mediastinum in an Adult: A Case Report 1
 Primitive Neuroectodermal Tumor of Mediastinum in an Adult: A Case Report 1 Young Jae Sung, M.D., Jeung Sook Kim, M.D. A peripheral primitive neuroectodermal tumor (PNET) is a rare and aggressive malignant
Primitive Neuroectodermal Tumor of Mediastinum in an Adult: A Case Report 1 Young Jae Sung, M.D., Jeung Sook Kim, M.D. A peripheral primitive neuroectodermal tumor (PNET) is a rare and aggressive malignant
May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Dermatology Volume 6 Number 1 Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature J Frey, C Huerter, J Shehan Citation J Frey, C Huerter,
ISPUB.COM The Internet Journal of Dermatology Volume 6 Number 1 Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature J Frey, C Huerter, J Shehan Citation J Frey, C Huerter,
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
-The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
- In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration
 Chin J Radiol 2002; 27: 191-195 191 Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration SIU-CHEUNG CHAN 1 MUN-CHING WONG 1 SHIU-FENG HUANG 2 WAN-CHAK
Chin J Radiol 2002; 27: 191-195 191 Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration SIU-CHEUNG CHAN 1 MUN-CHING WONG 1 SHIU-FENG HUANG 2 WAN-CHAK
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
UERMMMC Department of Radiology. Basic Chest Radiology
 UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, :30am - 11:30am FACULTY COPY
 SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Case 27 Male 42. Painless, static, well-circumscribed, subcutaneous nodule right lower leg,?lipoma. The best diagnosis is:
 Case 27 Male 42. Painless, static, well-circumscribed, subcutaneous nodule right lower leg,?lipoma. The best diagnosis is: A. Angiosarcoma B. Haemangiopericytoma C.Myopericytoma D.Myofibroma E. Angioleiomyoma
Case 27 Male 42. Painless, static, well-circumscribed, subcutaneous nodule right lower leg,?lipoma. The best diagnosis is: A. Angiosarcoma B. Haemangiopericytoma C.Myopericytoma D.Myofibroma E. Angioleiomyoma
