Comparison of conscious sedation and general anesthesia for motor mapping and resection of tumors located near motor cortex
|
|
|
- Fay Tucker
- 5 years ago
- Views:
Transcription
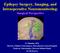
1 Neurosurg Focus 15 (1):Article 8, 2003, Click here to return to Table of Contents Comparison of conscious sedation and general anesthesia for motor mapping and resection of tumors located near motor cortex TODD W. VITAZ, M.D., WILLIAM MARX, M.D., JONATHAN D. VICTOR, M.D., PH.D., AND PHILIP H. GUTIN, M.D. Department of Neurological Surgery, University of Louisville School of Medicine, Louisville, Kentucky; Neurosurgical Service and Department of Anesthesia, Memorial Sloan Kettering Cancer Center; and the Departments of Neurology and Neuroscience and Neurological Surgery, Weill Medical College of Cornell University, New York, New York Object. The surgical treatment of tumors located near eloquent cortex carries a high risk of inducing worsening neurological deficits. Intraoperative electrocorticography techniques have been developed to help identify these areas at the time of surgery in an effort to minimize such risks. The optimal anesthetic technique for conducting these procedures, however, has never been determined. Methods. The authors conducted a retrospective study to compare patients who underwent intraoperative motor mapping between September 2000 and May Demographic and neurophysiological monitoring data were collected from the hospital records. Patients were divided into two groups based on the anesthetic technique used for surgery: in Group 1 general anesthesia was used, and in Group 2 conscious sedation. Group 1 comprised 24 patients (mean age 47 years) with 16 right- and eight left-sided lesions. Group 2 consisted of 21 patients (mean age 46 years) with 18 right- and three left-sided lesions. Pathological diagnoses were similar between the two groups. Motor stimulation was elicited in 12 patients (50%) in Group 1 and in 21 patients (100%) in Group 2 (p 0.001). In addition, the mean stimulation amplitude required was significantly higher (13 ma) in patients in whom conscious sedation was used as opposed to general anesthesia (5 ma, p ). Electrographic evidence of seizures was seen in 29% of Group 1 cmpared with 10% of Group 2 patients (p 0.05). Conclusions. The use of conscious sedation as an anesthetic technique for motor mapping not only improves the chances of achieving successful stimulation and identification of motor cortex in relationship to the lesion, but it also allows for repetitive monitoring of the patient s motor function during resection of the lesion. KEY WORDS brain tumor intraoperative mapping awake craniotomy anesthesia motor cortex The primary goal for resection of brain tumors has been maximal tumor resection while minimizing the risks of postoperative neurological deficits. In cases in which lesions abut or invade motor and speech centers, however, the ability of the surgeon to achieve these goals becomes progressively more difficult. 4,8,17 Numerous technological advances have been developed in an attempt to make safer the resection of lesions located near functionally important cortex. These include systems designed to localize functional cortex preoperatively such as fmr imaging, MEG, Wada testing, and intraoperative modalities designed to identify and differentiate tumor from surrounding brain (intraoperative ultrasonography, surgical navigation systems, and intraoperative MR imaging). 3,10,11 The gold standard for identifying functional cortex, Abbreviations used in this paper: ECS = electrocortical stimulation; fmr = functional magnetic resonance; MEG = magnetoencephalograpy; SSEP = somatosensory evoked potential. however, has remained direct ECS at the time of surgery. 2,4,8,17 This technique has been described in conjunction with both general and alert anesthesia (conscious sedation), with the latter being predominantly reserved for speech mapping. 2,4,9 The development of newer anesthetic agents, however, has made awake craniotomy simpler and more tolerable for patients. 6,7,14,16 As a result of these advances, we have tended over the past 2 years to perform more conscious sedation assisted craniotomies. To date, no comparison has been performed to evaluate the effects of these two types of anesthesia on the success of intraoperative motor mapping; therefore, we conducted a retrospective review to address this issue. CLINICAL MATERIAL AND METHODS A retrospective review of the surgical case log was performed to identify all intracranial operations in which the senior author (P.H.G.) performed intraoperative electro- Neurosurg. Focus / Volume 15 / July,
2 T. W. Vitaz, et al. corticography between September 2000 and May Cases that included any form of speech mapping were excluded because this technique mandated the use of alert anesthesia. All patients were treated by a single attending neurosurgeon, thereby limiting variability in surgical and mapping techniques. Hospital records, operative notes, and neurophysiological reports were then reviewed to collect demographic data and monitoring results. Patients were then divided into two groups: those in whom surgery and mapping were performed after induction of general anesthesia (Group 1) and those in whom conscious sedation was used (Group 2). Direct intergroup comparison was then performed, and statistical analysis was conducted using the Student t-test and chi-square test. Anesthetic Technique Goup 1. Endotracheal general anesthesia was composed of inhalation agents combined with Versed and fentanyl in the absence of paralytics. Goup 2. Patients sedation was induced via a propofol infusion. A nasal trumpet lubricated with lidocaine jelly was then inserted, and oxygen was infused throughout the procedure. A foley catheter lubricated with lidocaine jelly and an arterial line were also placed. A local field block (a 1:1 mixture of 50 ml lidocaine 1% with epinephrine [1:100,000] and 50 ml bupivicaine 0.5% with epinephrine [1:200,000] mixed with 9 ml sodium bicarbonate) was infiltrated into all of the regional nerves supplying the scalp. In addition, the pin sites anticipated for the placement of the Mayfield head holder (Ohio Medical, Cincinnati, OH) were infiltrated with the same solution. Once in place, the pin sites were reinfiltrated to ensure adequate coverage. Finally, the patient was prepared and draped, making sure that the anesthesiologist had an adequate avenue to the patient s face throughout the procedure, and the planned incision was infiltrated with 0.5% lidocaine with epinephrine (1:200,000). The patient remained sedated (via the propofol infusion) until approximately 10 minutes prior to the planned mapping at which time the infusion was discontinued. Versed, fentanyl, and labetalol were administered as needed throughout the procedure to control pain, anxiety, and hypertension. Patients remained awake throughout the mapping and during critical portions of the resection as determined by the surgeon. Once tumor resection was completed, the propofol infusion was restarted to sedate the patient during the closure procedure. Fig. 1. Intraoperative photograph showing orientation of monitoring electrode for intraoperative SSEP. 1, Location of phase reversal. Mapping Technique The mapping technique was the same in both groups. After induction of general anesthesia or conscious sedation, monitoring needles for upper- and sometimes lowerextremity SSEPs and reference leads were inserted. Following adequate exposure, an eight-panel subdural electrode was placed on the cortical surface spanning the area of the presumed central sulcus with a slightly oblique alignment from posteromedial to anterolateral. Somatosensory evoked potentials were then recorded with the area of phase reversal, which is usually consistent with the central sulcus and was marked with a sterile paper ticket (Fig. 1). After localization of the central sulcus, an Ojemann stimulator (Radionics, Burlington, MA) (60 Hz, biphasic square wave, 1 msec) was used for direct ECS. During this procedure the subdural electrode was positioned at the edge of the operative field and used to monitor electroencephalography for the presence of afterdischarges or electrical seizure activity. Stimulation was typically initiated at an intensity of 4 ma (peak-to-peak) and increased as needed until a positive response or repetitive afterdischarges or clinical seizure activities were encountered. Once the motor cortex (both groups) or sensory cortex (awake group) was identified, the area over the region of the tumor was stimulated at a slightly higher intensity. All positive results were marked with numbered tickets (Fig. 2) and the mapping-related results as well as the surgical navigation system and intraoperative ultrasonography data were used to determine the best avenue for resection of the lesion. In circumstances in which the lesion abutted or was within the motor cortex, Group 2 patients were left alert and underwent intermittent motor function monitoring (hand grasp, dorsi-plantar flexion) until the resection was completed (Fig. 3). RESULTS The senior author performed resections in 45 patients with intracranial tumors located near motor cortex. Twenty-four patients underwent surgery after induction of general anesthesia (Group 1) and 21 after induction of conscious sedation (Group 2). Histological diagnosis, and tumor locations for the two groups are shown in Table 1. The use of SSEP confirmed localization an area of phase reversal in 83 and 86% of Groups 1 and 2 patients, respectively. Direct cortical stimulation elicited positive results in 12 of 24 (50%) Group 1 patients and 21 of 21 (100%) Group 2 patients (p 0.001). The mean intensities required to obtain these results were 13 ma (range 4 18 ma, median 16 ma) in Group 1 and 5 ma (range 4 10 ma, median 4 ma) in Group 2 (p ). Finally, there was a trend toward higher seizure incidence in Group 1 patients, although this did not reach statistical significance (29% [Group 1] and 10% [Group 2], p = 0.14). These results are shown in Table 2. 2 Neurosurg. Focus / Volume 15 / July, 2003
3 Mapping techniques for motor cortex tumors Fig. 2. Imaging studies obtained in a patient with metastatic adenocarcinoma. The patient refused stereotactic radiosurgery and instead opted for resection with awake mapping. Left and Center: Preoperative axial contrast-enhanced (left) and noncontrast (center) MR images. The red lines indicate the central sulcus based on radiographic landmarks. Right: Intraoperative photograph showing the location of tumor within sensorimotor cortex. Paper tickets identify areas of positive stimulation. 1, motor for thumb; 2, sensory for hand; 3, motor for face. DISCUSSION Enormous effort has recently gone into developing noninvasive techniques for preoperative localization of eloquent portions of the brain. The various modalities range from topographic measurements and radiographic landmarks to fmr imaging and MEG. 3,10,11 Their ability to localize motor cortex adequately increases from 50 to 67% when topographic landmarks are used, from 80 to 97% when fmr imaging is performed, and from 85 to 100% when MEG is conducted. 3,8,10,11 Although these modalities in their current state may help to differentiate between cases requiring mapping-assisted tumor resection and those not, the gold standard remains intraoperative direct ECS. Historically, motor mapping has been performed after induction of general anesthesia; however, we have shown that these procedures can also be performed safely after administration of conscious sedation without any significant anesthesia-related perioperative complications. The biggest concern related to this technique includes loss of an adequate airway and subsequent failure to control hypercapnia-induced brain swelling; however, this is typically not a significant problem with an incidence of less than 1% in most studies. 6,9,12,16 Likewise, we have not found this to be a significant problem, and brain swelling can typically be controlled using a combination of perioperative mannitol and dexamethasone (with furosemide being reserved for resistant cases). The success of motor mapping depends highly on the depth of anesthesia and may be difficult when general anesthesia is administered (50% in our study). We do not believe that the absence of stimulation in the operative field correlates with the absence of functional cortex in the TABLE 1 Summary of data in 45 patients undergoing tumor resection Group 1 Group 2 Characteristic (general anesthesia) (conscious sedation) Fig. 3. Preoperative axial postcontrast MR image obtained in a patient with metastatic sarcoma who had previously undergone a right lower-extremity amputation; the lesion was located in the right motor cortex. Neurosurg. Focus / Volume 15 / July, 2003 no. of patients mean age in yrs (range) 46 ( ) 47.2 ( ) sex female 8 5 male pathological entity (%) glioblastoma multiforme 6 (25) 1 (5) anaplastic astrocytoma 8 (33) 3 (14) low-grade glioma 5 (21) 10 (48) metastasis 5 (21) 5 (24) radiation necrosis 0 1 (5) abcess 0 1 (5) location left 8 (33) 3 (14) right 16 (67) 18 (86) frontal 19 (79) 17 (81) parietal 5 (21) 4 (19) 3
4 T. W. Vitaz, et al. Variable TABLE 2 Results of cortical mapping Group 1 Group 2 (general anesthesia) (conscious sedation) SSEP localization (%) 20 (83) 18 (86) positive stimulation no. of cases (%) 12 (50) 21 (100) mean amplitude (range) 13 ma (4 18 ma) 5 ma (4 10 ma) electrical seizure activity (%) 7 (29) 2 (10) area being stimulated and have encountered such cases in which the patient awoke with a neurological deficit. Only when the motor cortex can be adequately identified can the surgeon be confident of its relationship to the tumor. 4,8,17 The higher stimulation amplitudes often required to induce positive stimulation after induction of general anesthesia (13 ma compared with 5 ma in conscious sedation treated patients, p ) might also increase the risk of inducing seizure activity (29% in Group 1 and 10% in Group 2, p 0.05), which may further hinder the chances for successful stimulation if it becomes generalized. Although general anesthesia is known to have superb antiepileptic properties, its depth must be sufficiently decreased to allow for positive stimulation. This low-level anesthesia combined with the higher amplitudes required to induce positive stimulation results may increase the possibility of eliciting seizure activity. Finally, the propofol that is used in the conscious sedation treated patients is known to have antiepileptic properties, which may be further protective in this group. 1,5,13,15 The development of seizure activity is important for two reasons: it can lead to airway problems and, if this activity becomes diffuse or generalized, it may impair further attempts at stimulation or patient interaction because of the postictal refractory state of the brain. Finally, the ability to obtain direct intraoperative physiological feedback from the patient significantly lessens the risks of producing new neurological deficits. When intraoperative deficits are encountered, the surgeon can either modify the approach or cease resection to minimize the chance of further injury. 2,12 Danks, et al., 6 reported that of 33 patients who underwent awake mapping and developed a deficit intraoperatively only two suffered permanent deficits. Although we have shown that conscious sedation may be superior to general anesthesia as an adjuvant during resection of lesions located near motor cortex, the former is not the anesthetic of choice in all patients. Patients are not considered candidates for awake anesthesia if profound preoperative neurological deficits are present, which may preclude eliciting a positive response to stimulation, nor in the presence of significant comorbidities, such as severe cardiac or pulmonary disease, or psychological disorders that may interfere with their ability to undergo such a procedure. In addition, this modality is not typically performed in children younger than 15 years of age because of emotional immaturity. Danks, et al., 7 prospectively evaluated their patients perceptions and pain levels during such procedures and found that 81% suffered amnesia with regard to most or all of the procedure. In addition, only 5% complained of severe pain and 10% stated they felt anxious or uncomfortable during part of the procedure; 18 of the 21 patients said they would undergo the procedure again if necessary. Although we did not conduct this study to demonstrate the different effects of anesthetic methods on successful intraoperative mapping, the retrospective design prevents intergroup comparison of neurological and radiographical outcomes. Memorial Sloan Kettering Cancer Center is a quaternary referral center and, as such, many of the patients were not available for long-term follow-up assessment of neurological status; additionally preoperative radiographs were unavailable for review in most cases because they were typically returned to the home institution postoperatively. A frequent concern among surgeons when evaluating new techniques is their impact on the overall length of a procedure. Although an awake craniotomy requires an additional 5 or 10 minutes, this time is usually recovered later during the procedure. Conscious sedation assisted mapping often proceeds at a much faster pace because successful stimulation is often achieved using very low stimulation parameters and because sensory stimulation can be reported, which helps direct the surgeon to the location of motor cortex. CONCLUSIONS Overall we believe that conscious sedation assisted resection of lesions near motor cortex requiring electrocortical mapping is superior to general anesthesia in selected patients. Successful stimulation was obtained in 100% of the conscious sedation treated patients with significantly lower thresholds (5 ma) compared with 50% positive stimulation in the general anesthesia treated patients (13 ma). Finally, the ability to obtain direct physiological feedback from the patient during the most critical portion of the resection empowers the surgeon by providing more information that allows maximization of tumor resection and minimization of neurological deficits. References 1. Begemann M, Rowan AJ, Tuhrim S: Treatment of refractory complex-partial status epilepticus with propofol: case report. Epilepsia 41: , Berger M: Functional mapping-guided resection of low-grade gliomas. Clin Neurosurg 42: , Berger MS, Cohen WA, Ojemann GA: Correlation of motor cortex brain mapping data with magnetic resonance imaging. J Neurosurg 72: , Black PM, Ronner SF: Cortical mapping for defining the limits of tumor resection. Neurosurgery 20: , Brown L, Levin G: Role of propofol in refractory status epilepticus. Ann Pharmacother 32: , Danks RA, Aglio LS, Gugino LD, et al: Craniotomy under local anesthesia and monitored conscious sedation for the resection of tumors involving eloquent cortex. J Neurooncol 49: , Danks RA, Rogers M, Aglio LS, et al: Patient tolerance of craniotomy performed with the patient under local anesthesia and monitored conscious sedation. Neurosurgery 42:28 36, Duffau H, Capelle L, Sichez J, et al: Intra-operative direct electrical stimulations of the central nervous system: the Salpetriere experience with 60 patients. Acta Neurochir 141: , Neurosurg. Focus / Volume 15 / July, 2003
5 Mapping techniques for motor cortex tumors 9. Haglund MM, Berger MS, Shamseldin M, et al: Cortical localization of temporal lobe language sites in patients with gliomas. Neurosurgery 34: , Hirsch J, Ruge MI, Kim KH, et al: An intergrated functional magnetic resonance imaging procedure for preoperative mapping of cortical areas associated with tactile, motor, language, and visual functions. Neurosurgery 47: , Lehericy S, Duffau H, Cornu P, et al: Correspondence between functional magnetic resonance imaging somatotopy and individual brain anatomy of the central region: comparison with intraoperative stimulation in patients with brain tumors. J Neurosurg 92: , Meyer FB, Bates LM, Goerss SJ, et al: Awake craniotomy for aggressive resection of primary gliomas located in eloquent brain. Mayo Clin Proc 76: , Prasad A, Worrall BB, Bertram EH, et al: Propofol and midazolam in the treatment of refractory status epilepticus. Epilepsia 42: , Silbergeld DL, Mueller WM, Colley PS, et al: Use of propofol (Diprivan) for awake craniotomies: technical note. Surg Neurol 38: , Stecker MM, Kramer TH, Raps EC, et al: Treatment of refractory status epilepticus with propofol: clinical and pharmacokinetic findings. Epilepsia 90:18 26, Taylor MD, Bernstein M: Awake craniotomy with brain mapping as the routine surgical approach to treating patients with supratentorial intraaxial tumors: a prospective trial of 200 cases. J Neurosurg 90:35 41, Yingling CD, Ojemann S, Dodson B, et al: Identification of motor pathways during tumor surgery facilitated by multichannel electromyogrhaphic recording. J Neurosurg 91: , 1999 Manuscript received May 28, Accepted in final form June 13, Address reprint requests to: Todd W. Vitaz, M.D., 210 E. Gray Street, Suite 1102, Louisville, Kentucky Tvitaz@ NIKY.com. Neurosurg. Focus / Volume 15 / July,
Primary low-grade brain tumors in
 O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Intraoperative Monitoring: Role in Epilepsy Based Tumor Surgery December 2, 2012
 Intraoperative Monitoring: Role in Epilepsy Based Tumor Surgery December 2, 2012 Aatif M. Husain, M.D. Duke University and Veterans Affairs Medical Centers, Durham, NC American Epilepsy Society Annual
Intraoperative Monitoring: Role in Epilepsy Based Tumor Surgery December 2, 2012 Aatif M. Husain, M.D. Duke University and Veterans Affairs Medical Centers, Durham, NC American Epilepsy Society Annual
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT. Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018
 EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EMG, EEG, and Neurophysiology in Clinical Practice
 Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
SUPPLEMENTARY INFORMATION. Table 1 Patient characteristics Preoperative. language testing
 Categorical Speech Representation in the Human Superior Temporal Gyrus Edward F. Chang, Jochem W. Rieger, Keith D. Johnson, Mitchel S. Berger, Nicholas M. Barbaro, Robert T. Knight SUPPLEMENTARY INFORMATION
Categorical Speech Representation in the Human Superior Temporal Gyrus Edward F. Chang, Jochem W. Rieger, Keith D. Johnson, Mitchel S. Berger, Nicholas M. Barbaro, Robert T. Knight SUPPLEMENTARY INFORMATION
Awake Craniotomy for Removal of Intracranial Tumor: Considerations for Early Discharge
 Awake Craniotomy for Removal of Intracranial Tumor: Considerations for Early Discharge Hannah J. Blanshard, FRCA*, Frances Chung, FRCPC*, Pirjo H. Manninen, FRCPC*, Michael D. Taylor, MD, and Mark Bernstein,
Awake Craniotomy for Removal of Intracranial Tumor: Considerations for Early Discharge Hannah J. Blanshard, FRCA*, Frances Chung, FRCPC*, Pirjo H. Manninen, FRCPC*, Michael D. Taylor, MD, and Mark Bernstein,
Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry. Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA
 Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA Overview Definition of epileptic circuitry Methods of mapping
Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA Overview Definition of epileptic circuitry Methods of mapping
Subject: Magnetoencephalography/Magnetic Source Imaging
 01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
Small and Big Operations: New Tools of the Trade for Brain Tumors. Disclosure. Incidence of Childhood Cancer
 Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective
 Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Technique of Localizing the Central Sulcus under Awake Anesthesia for Treatment of Gliomas in or near Motor Areas
 DOI: 10.5137/1019-5149.JTN.21802-17.3 Received: 08.10.2017 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Technique of Localizing the Central Sulcus under
DOI: 10.5137/1019-5149.JTN.21802-17.3 Received: 08.10.2017 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Technique of Localizing the Central Sulcus under
Navigated Transcranial Magnetic Stimulation. Description
 Subject: Navigated Transcranial Magnetic Stimulation Page: 1 of 11 Last Review Status/Date: December 2016 Navigated Transcranial Magnetic Stimulation Description Navigated transcranial magnetic stimulation
Subject: Navigated Transcranial Magnetic Stimulation Page: 1 of 11 Last Review Status/Date: December 2016 Navigated Transcranial Magnetic Stimulation Description Navigated transcranial magnetic stimulation
Audit and Compliance Department 1
 Introduction to Intraoperative Neuromonitoring An intro to those squiggly lines Kunal Patel MS, CNIM None Disclosures Learning Objectives History of Intraoperative Monitoring What is Intraoperative Monitoring
Introduction to Intraoperative Neuromonitoring An intro to those squiggly lines Kunal Patel MS, CNIM None Disclosures Learning Objectives History of Intraoperative Monitoring What is Intraoperative Monitoring
Clinical Policy: Functional MRI Reference Number: CP.MP.43
 Clinical Policy: Reference Number: CP.MP.43 Effective Date: 09/09 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.43 Effective Date: 09/09 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Insulo-opercular Gliomas: Four Different Natural Progression Patterns and Implications for Surgical Indications
 Neurol Med Chir (Tokyo) 50, 286 290, 2010 Insulo-opercular Gliomas: Four Different Natural Progression Patterns and Implications for Surgical Indications Ryuta SAITO, Toshihiro KUMABE, Masayuki KANAMORI,
Neurol Med Chir (Tokyo) 50, 286 290, 2010 Insulo-opercular Gliomas: Four Different Natural Progression Patterns and Implications for Surgical Indications Ryuta SAITO, Toshihiro KUMABE, Masayuki KANAMORI,
Presurgical Language Mapping Kathleen B. McDermott, 1 Jason M. Watson, 1 and Jeffrey G. Ojemann 2
 CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE Presurgical Language Mapping Kathleen B. McDermott, 1 Jason M. Watson, 1 and Jeffrey G. Ojemann 2 1 Washington University in St. Louis and 2 University of Washington
CURRENT DIRECTIONS IN PSYCHOLOGICAL SCIENCE Presurgical Language Mapping Kathleen B. McDermott, 1 Jason M. Watson, 1 and Jeffrey G. Ojemann 2 1 Washington University in St. Louis and 2 University of Washington
The Changing Surgical Landscape in Kids
 The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
ChosingPhase 2 Electrodes
 ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
RIGHT HEMISPHERE LANGUAGE MAPPING USING ELECTROCORTICAL STIMULATION IN PATIENTS WITH BILATERAL LANGUAGE
 RIGHT HEMISPHERE LANGUAGE MAPPING USING ELECTROCORTICAL STIMULATION IN PATIENTS WITH BILATERAL LANGUAGE Rosette A. Jabbour, MD Gail L. Risse, PhD Patricia E. Penovich, MD Frank J. Ritter, MD John R. Gates,
RIGHT HEMISPHERE LANGUAGE MAPPING USING ELECTROCORTICAL STIMULATION IN PATIENTS WITH BILATERAL LANGUAGE Rosette A. Jabbour, MD Gail L. Risse, PhD Patricia E. Penovich, MD Frank J. Ritter, MD John R. Gates,
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES. Mr. Johnson. Seizures at 29 Years of Age. Dileep Nair, MD Juan Bulacio, MD
 Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Epilepsy & Functional Neurosurgery
 Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2018;42(5):767-772 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.5.767 Annals of Rehabilitation Medicine Limitation of Intraoperative Transcranial Electrical
Case Report Ann Rehabil Med 2018;42(5):767-772 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.5.767 Annals of Rehabilitation Medicine Limitation of Intraoperative Transcranial Electrical
epilepsy center About Epilepsy Surgery
 epilepsy center About Epilepsy Surgery Epilepsy Surgery Advances in Epilepsy Surgery Are You a Candidate for Surgery? If anticonvulsant medications have failed to control your epilepsy, or you are experiencing
epilepsy center About Epilepsy Surgery Epilepsy Surgery Advances in Epilepsy Surgery Are You a Candidate for Surgery? If anticonvulsant medications have failed to control your epilepsy, or you are experiencing
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
3D diffuse tensor imaging important acquisition in diagnostic and preoperative planning of intracranial lesions
 110 Rizea et al 3D diffuse tensor imaging for preoperative planning 3D diffuse tensor imaging important acquisition in diagnostic and preoperative planning of intracranial lesions R.E. Rizea, A.V. Ciurea,
110 Rizea et al 3D diffuse tensor imaging for preoperative planning 3D diffuse tensor imaging important acquisition in diagnostic and preoperative planning of intracranial lesions R.E. Rizea, A.V. Ciurea,
SEP Monitoring. Outline. Outline 1/22/2015. Development of SEPs Stimulation and recording techniques Predictive value of SEP Uses of SEP monitoring
 SEP Monitoring Andres A Gonzalez, MD Director, Surgical Neurophysiology Keck Medical Center of USC University of Southern California Outline Development of SEPs Stimulation and recording techniques Predictive
SEP Monitoring Andres A Gonzalez, MD Director, Surgical Neurophysiology Keck Medical Center of USC University of Southern California Outline Development of SEPs Stimulation and recording techniques Predictive
Jason Rusnak M.S. CNIM Biotronic NeuroNetwork Tuesday, May 31, Motor Cortical Mapping
 Jason Rusnak M.S. CNIM Biotronic NeuroNetwork Tuesday, May 31, 2016 Motor Cortical Mapping Motor Cortical Mapping Cortical Mapping Success Cortical Mapping Success Depends on: Knowing General Anatomy Where
Jason Rusnak M.S. CNIM Biotronic NeuroNetwork Tuesday, May 31, 2016 Motor Cortical Mapping Motor Cortical Mapping Cortical Mapping Success Cortical Mapping Success Depends on: Knowing General Anatomy Where
Post-Operative Supplementary Motor Area Syndrome
 Med. J. Cairo Univ., Vol. 80, No. 1, June: 385-389, 2012 www.medicaljournalofcairouniversity.com Post-Operative Supplementary Motor Area Syndrome KHALED ANBAR, M.D. The Department of Neurosurgery, Faculty
Med. J. Cairo Univ., Vol. 80, No. 1, June: 385-389, 2012 www.medicaljournalofcairouniversity.com Post-Operative Supplementary Motor Area Syndrome KHALED ANBAR, M.D. The Department of Neurosurgery, Faculty
1/22/2015. Royalties from Demos Medical Publishing. Learn how to. Mirela Simon, M.D., M.Sc. Massachusetts General Hospital Boston, MA
 Mirela Simon, M.D., M.Sc. Massachusetts General Hospital Boston, MA Royalties from Demos Medical Publishing Learn how to - plan a functional mapping procedure - perform and interpret central sulcus localization
Mirela Simon, M.D., M.Sc. Massachusetts General Hospital Boston, MA Royalties from Demos Medical Publishing Learn how to - plan a functional mapping procedure - perform and interpret central sulcus localization
Integration of preoperative and intraoperative functional brain mapping in a frameless stereotactic environment for lesions near eloquent cortex
 J Neurosurg 90:591Ð598, 1999 Integration of preoperative and intraoperative functional brain mapping in a frameless stereotactic environment for lesions near eloquent cortex Technical note JEFFREY D. MCDONALD,
J Neurosurg 90:591Ð598, 1999 Integration of preoperative and intraoperative functional brain mapping in a frameless stereotactic environment for lesions near eloquent cortex Technical note JEFFREY D. MCDONALD,
SEP Monitoring. Andres A Gonzalez, MD Director, Surgical Neurophysiology Keck Medical Center of USC University of Southern California
 SEP Monitoring Andres A Gonzalez, MD Director, Surgical Neurophysiology Keck Medical Center of USC University of Southern California Outline Development of SEPs Stimulation and recording techniques Predictive
SEP Monitoring Andres A Gonzalez, MD Director, Surgical Neurophysiology Keck Medical Center of USC University of Southern California Outline Development of SEPs Stimulation and recording techniques Predictive
Functional Magnetic Resonance Imaging of the Brain
 Page: 1 of 9 Last Review Status/Date: December 2016 Description Functional magnetic resonance imaging (fmri) is a noninvasive method for localizing areas of brain function and has been used for the presurgical
Page: 1 of 9 Last Review Status/Date: December 2016 Description Functional magnetic resonance imaging (fmri) is a noninvasive method for localizing areas of brain function and has been used for the presurgical
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
L ack of neurological deficit with either congenital or slow
 PAPER Long term reshaping of language, sensory, and motor maps after glioma resection: a new parameter to integrate in the surgical strategy H Duffau, D Denvil, L Capelle... See end of article for authors
PAPER Long term reshaping of language, sensory, and motor maps after glioma resection: a new parameter to integrate in the surgical strategy H Duffau, D Denvil, L Capelle... See end of article for authors
fmri and Pre-operative Planning for CNS tumors
 fmri and Pre-operative Planning for CNS tumors Miami Brain Symposium Andrei I. Holodny, M.D. Chief of Neuroradiology Director of the fmri Lab Memorial Sloan-Kettering Cancer Center Disclosures: 1. NIH-NIBIB
fmri and Pre-operative Planning for CNS tumors Miami Brain Symposium Andrei I. Holodny, M.D. Chief of Neuroradiology Director of the fmri Lab Memorial Sloan-Kettering Cancer Center Disclosures: 1. NIH-NIBIB
Objectives. Presenter Disclosure Information 11/29/2016
 Current State of Neurosurgical Treatment of Cerebral Glioma and Clinical Trials Testing Future Advances John D. Heiss, M.D. Chair, Surgical Neurology Branch, NINDS, National Institutes of Health Presenter
Current State of Neurosurgical Treatment of Cerebral Glioma and Clinical Trials Testing Future Advances John D. Heiss, M.D. Chair, Surgical Neurology Branch, NINDS, National Institutes of Health Presenter
Vestibular Schwannoma Surgery with the use of Intraoperative Monitoring
 Vestibular Schwannoma Surgery with the use of Intraoperative Monitoring Division of Neurosurgery, University of Cape Town August 2018 SNSA Sonia Nunes, Alan Taylor, David Le Feveure Vestibular Schwannoma
Vestibular Schwannoma Surgery with the use of Intraoperative Monitoring Division of Neurosurgery, University of Cape Town August 2018 SNSA Sonia Nunes, Alan Taylor, David Le Feveure Vestibular Schwannoma
5/22/2009. Pediatric Neurosurgery Pediatric Neurology Neuroradiology Neurophysiology Neuropathology Neuropsychology
 Current Surgical Treatment Strategies for the Management of Pediatric Epilepsy University of California, San Francisco Department of Neurological Surgery San Francisco, California Kurtis Ian Auguste, M.D.
Current Surgical Treatment Strategies for the Management of Pediatric Epilepsy University of California, San Francisco Department of Neurological Surgery San Francisco, California Kurtis Ian Auguste, M.D.
Faculty/Presenter Disclosure. Intracranial EEG Recording. Objectives. General Themes. Why invasive recordings? 6/27/2018
 CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
Seizure control following tumor surgery for childhood cortical low-grade gliomas
 J Neurosurg 80:998-1003, 1994 Seizure control following tumor surgery for childhood cortical low-grade gliomas ROGER J. PACKER, M.D., LESLIE N. SuttON, M.D., KANTILAL M. PATEL, PH.D., ANN-CImtSTINE DUnAIME,
J Neurosurg 80:998-1003, 1994 Seizure control following tumor surgery for childhood cortical low-grade gliomas ROGER J. PACKER, M.D., LESLIE N. SuttON, M.D., KANTILAL M. PATEL, PH.D., ANN-CImtSTINE DUnAIME,
Combined Use of DES, EMG and MEP Monitoring, ECoG and EEG for Surgical Resection of Gliomas
 Combined Use of DES, and MEP Monitoring, ECoG and for Surgical Resection of Gliomas a report by Lorenzo Bello, Enrica Fava, Giorgio Carrabba and Giulio Bertani Department of Neurological Sciences, Università
Combined Use of DES, and MEP Monitoring, ECoG and for Surgical Resection of Gliomas a report by Lorenzo Bello, Enrica Fava, Giorgio Carrabba and Giulio Bertani Department of Neurological Sciences, Università
Br a i n surgery in an unanesthetized patient was
 J Neurosurg 114:633 639, 2011 A retrospective cohort-matched comparison of conscious sedation versus general anesthesia for supratentorial glioma resection Clinical article Pi e r pa o l o Pe r u z z i,
J Neurosurg 114:633 639, 2011 A retrospective cohort-matched comparison of conscious sedation versus general anesthesia for supratentorial glioma resection Clinical article Pi e r pa o l o Pe r u z z i,
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES
 MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
The Surgical Treatment of Epilepsy
 The Surgical Treatment of Epilepsy Jeffrey S. Schweitzer, MD, PhD Kaiser Los Angeles Medical Center Division of Restorative Neurosurgery Ancient craniotomy When Cao started complaining about splitting
The Surgical Treatment of Epilepsy Jeffrey S. Schweitzer, MD, PhD Kaiser Los Angeles Medical Center Division of Restorative Neurosurgery Ancient craniotomy When Cao started complaining about splitting
A Patient s Guide to Intraoperative Monitoring
 A Patient s Guide to Intraoperative Monitoring 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Intraoperative Monitoring 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
What is NBS? Nextstim NBS System
 Nextstim NBS System What is NBS? NBS means navigated brain stimulation, and is used to precisely map the areas controlling muscle movements/activity in the brain. This procedure provides advanced patient
Nextstim NBS System What is NBS? NBS means navigated brain stimulation, and is used to precisely map the areas controlling muscle movements/activity in the brain. This procedure provides advanced patient
Subject: Functional Brain MRI
 Subject: Functional Brain MRI Guidance Number: MCG-136 Revision Date(s): Original Effective Date: 6/26/13 Medical Coverage Guidance Approval Date: 6/26/13 PREFACE This Medical Guidance is intended to facilitate
Subject: Functional Brain MRI Guidance Number: MCG-136 Revision Date(s): Original Effective Date: 6/26/13 Medical Coverage Guidance Approval Date: 6/26/13 PREFACE This Medical Guidance is intended to facilitate
PAPER. H Duffau, D Denvil, M Lopes, F Gasparini, L Cohen, L Capelle, R van Effenterre...
 733 PAPER Intraoperative mapping of the cortical areas involved in multiplication and subtraction: an electrostimulation study in a patient with a left parietal glioma H Duffau, D Denvil, M Lopes, F Gasparini,
733 PAPER Intraoperative mapping of the cortical areas involved in multiplication and subtraction: an electrostimulation study in a patient with a left parietal glioma H Duffau, D Denvil, M Lopes, F Gasparini,
IOM at University of. Training for physicians. art of IOM. neurologic. injury during surgery. surgery on by IOM. that rate is.
 Topics covered: Overview of science and art of IOM IOM at University of Michigan Hospital and Health Systems What is the purpose of Intraoperative monitoring? Training for physicians Overview of science
Topics covered: Overview of science and art of IOM IOM at University of Michigan Hospital and Health Systems What is the purpose of Intraoperative monitoring? Training for physicians Overview of science
Name of Policy: Navigated Transcranial Magnetic Stimulation (ntms)
 Name of Policy: Navigated Transcranial Magnetic Stimulation (ntms) Policy #: 556 Latest Review Date: June 2017 Category: Medicine Policy Grade: C Background/Definitions: As a general rule, benefits are
Name of Policy: Navigated Transcranial Magnetic Stimulation (ntms) Policy #: 556 Latest Review Date: June 2017 Category: Medicine Policy Grade: C Background/Definitions: As a general rule, benefits are
Cortical Stimulation for Epilepsy (NeuroPace )
 (NeuroPace ) Last Review Date: October 13, 2017 Number: MG.MM.SU.69 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit
(NeuroPace ) Last Review Date: October 13, 2017 Number: MG.MM.SU.69 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Morbidity of Stereotactic Biopsy for Intracranial Lesions
 Kobe J. Med. Sci., Vol. 56, No. 4, pp. E148-E153, 2010 Morbidity of Stereotactic Biopsy for Intracranial Lesions MASAMITSU NISHIHARA 1 *, TAKASHI SASAYAMA 2, HIROSHI KUDO 3, and EIJI KOHMURA 2 1 Department
Kobe J. Med. Sci., Vol. 56, No. 4, pp. E148-E153, 2010 Morbidity of Stereotactic Biopsy for Intracranial Lesions MASAMITSU NISHIHARA 1 *, TAKASHI SASAYAMA 2, HIROSHI KUDO 3, and EIJI KOHMURA 2 1 Department
ION Intraoperative Neurophysiology
 ION Intraoperative Neurophysiology EMG Course in Bucharest, September 18-19, 2012 Roland Flink Prof MD PhD Department of Clinical Neurophysiology What to monitor? Cortical function Tumour surgery Epilepsy
ION Intraoperative Neurophysiology EMG Course in Bucharest, September 18-19, 2012 Roland Flink Prof MD PhD Department of Clinical Neurophysiology What to monitor? Cortical function Tumour surgery Epilepsy
Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan
 Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
Surgery Within and Around Critical White Matter Tracts
 Surgery Within and Around Critical White Matter Tracts Kaisorn L. Chaichana, M.D. Assistant Professor of Neurosurgery, Oncology, and Otolaryngology-Head & Neck Surgery Mayo Clinic Florida, Jacksonville,
Surgery Within and Around Critical White Matter Tracts Kaisorn L. Chaichana, M.D. Assistant Professor of Neurosurgery, Oncology, and Otolaryngology-Head & Neck Surgery Mayo Clinic Florida, Jacksonville,
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology. Tim Lucas, MD, PhD Neurosurgery
 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Functional Outcome after Language Mapping for Glioma Resection
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Functional Outcome after Language Mapping for Glioma Resection Nader Sanai, M.D., Zaman Mirzadeh, Ph.D., and Mitchel S. Berger, M.D.
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Functional Outcome after Language Mapping for Glioma Resection Nader Sanai, M.D., Zaman Mirzadeh, Ph.D., and Mitchel S. Berger, M.D.
Functional PET scanning in the assessment of cerebral arteriovenous malformations RICHARD LEBLANC, M.D., F.R.C.S.(C), AND ERNST MEYER, PH.D.
 J Neurosurg 73:615-619, 1990 Functional PET scanning in the assessment of cerebral arteriovenous malformations Case report RICHARD LEBLANC, M.D., F.R.C.S.(C), AND ERNST MEYER, PH.D. Department of Neurology
J Neurosurg 73:615-619, 1990 Functional PET scanning in the assessment of cerebral arteriovenous malformations Case report RICHARD LEBLANC, M.D., F.R.C.S.(C), AND ERNST MEYER, PH.D. Department of Neurology
PARIETAL LOBE. Vasilios A. Zerris MD, MPH, MSc, FAANS
 PARIETAL LOBE Vasilios A. Zerris MD, MPH, MSc, FAANS Diplomate of the American Board of Neurological Surgery Fellow of the American Association of Neurological Surgeons Professor of Neurosurgery, European
PARIETAL LOBE Vasilios A. Zerris MD, MPH, MSc, FAANS Diplomate of the American Board of Neurological Surgery Fellow of the American Association of Neurological Surgeons Professor of Neurosurgery, European
Intra-operative neurologic injuries: Avoidance and prompt response
 Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM
 INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
Corporate Medical Policy
 Corporate Medical Policy Brachytherapy, Intracavitary Balloon Catheter for Brain Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_intracavitary_balloon_catheter_for_brain_cancer
Corporate Medical Policy Brachytherapy, Intracavitary Balloon Catheter for Brain Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_intracavitary_balloon_catheter_for_brain_cancer
Decreased Amplitude and Increased Latency in OR Communication During Anterior/Posterior Spinal Fusion
 Title: Moderators: Decreased Amplitude and Increased Latency in OR Communication During Anterior/Posterior Spinal Fusion Wendy Binstock, M.D. Associate Professor, Department of Anesthesia and Critical
Title: Moderators: Decreased Amplitude and Increased Latency in OR Communication During Anterior/Posterior Spinal Fusion Wendy Binstock, M.D. Associate Professor, Department of Anesthesia and Critical
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
The neurolinguistic toolbox Jonathan R. Brennan. Introduction to Neurolinguistics, LSA2017 1
 The neurolinguistic toolbox Jonathan R. Brennan Introduction to Neurolinguistics, LSA2017 1 Psycholinguistics / Neurolinguistics Happy Hour!!! Tuesdays 7/11, 7/18, 7/25 5:30-6:30 PM @ the Boone Center
The neurolinguistic toolbox Jonathan R. Brennan Introduction to Neurolinguistics, LSA2017 1 Psycholinguistics / Neurolinguistics Happy Hour!!! Tuesdays 7/11, 7/18, 7/25 5:30-6:30 PM @ the Boone Center
SEIZURE OUTCOME AFTER EPILEPSY SURGERY
 SEIZURE OUTCOME AFTER EPILEPSY SURGERY Prakash Kotagal, M.D. Head, Pediatric Epilepsy Cleveland Clinic Epilepsy Center LEFT TEMPORAL LOBE ASTROCYTOMA SEIZURE OUTCOME 1 YEAR AFTER EPILEPSY SURGERY IN ADULTS
SEIZURE OUTCOME AFTER EPILEPSY SURGERY Prakash Kotagal, M.D. Head, Pediatric Epilepsy Cleveland Clinic Epilepsy Center LEFT TEMPORAL LOBE ASTROCYTOMA SEIZURE OUTCOME 1 YEAR AFTER EPILEPSY SURGERY IN ADULTS
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
The supplementary motor area (SMA) is an eloquent. FOCUS Neurosurg Focus 44 (6):E3, 2018
 NEUROSURGICAL FOCUS Neurosurg Focus 44 (6):E3, 2018 Prediction of recovery from supplementary area syndrome after brain tumor surgery: preoperative diffusion tensor tractography analysis and postoperative
NEUROSURGICAL FOCUS Neurosurg Focus 44 (6):E3, 2018 Prediction of recovery from supplementary area syndrome after brain tumor surgery: preoperative diffusion tensor tractography analysis and postoperative
Why can t we get good baseline motor evoked potentials in this. patient? Laura Hemmer, M.D. Antoun Koht, M.D.
 Why can t we get good baseline motor evoked potentials in this SNACC Neuromonitoring Subcommittee Linda Aglio, M.D., M.S. Laura Hemmer, M.D. Antoun Koht, M.D. David L. Schreibman, M.D. patient? Laura Hemmer,
Why can t we get good baseline motor evoked potentials in this SNACC Neuromonitoring Subcommittee Linda Aglio, M.D., M.S. Laura Hemmer, M.D. Antoun Koht, M.D. David L. Schreibman, M.D. patient? Laura Hemmer,
Frontal Contributions to Memory Encoding Before and After Unilateral Medial Temporal Lobectomy
 Frontal Contributions to Memory Encoding Before and After Unilateral Medial Temporal Lobectomy Jeff Ojemann, MD Department of Neurological Surgery University of Washington Children s Hospital & Regional
Frontal Contributions to Memory Encoding Before and After Unilateral Medial Temporal Lobectomy Jeff Ojemann, MD Department of Neurological Surgery University of Washington Children s Hospital & Regional
Non-therapeutic and investigational uses of non-invasive brain stimulation
 Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
COMMUNICATIONS BIOPHYSICS
 XVIII. * COMMUNICATIONS BIOPHYSICS Prof. W. A. Rosenblith Dr. N. Y-S. Kiang A. H. Crist Prof. M. H. Goldstein, Jr. Dr. J. W. Kuiper**' G. E. Forsen Dr. J. S. Barlowt Dr. T. T. Sandel Margaret Z. Freeman
XVIII. * COMMUNICATIONS BIOPHYSICS Prof. W. A. Rosenblith Dr. N. Y-S. Kiang A. H. Crist Prof. M. H. Goldstein, Jr. Dr. J. W. Kuiper**' G. E. Forsen Dr. J. S. Barlowt Dr. T. T. Sandel Margaret Z. Freeman
AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY
 AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY Part I Content Outline I. Physiology and Instrumentation 30% A. Physiology 1. Anatomy of neural generation 2. Mechanisms of EEG and evoked potential generation
AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY Part I Content Outline I. Physiology and Instrumentation 30% A. Physiology 1. Anatomy of neural generation 2. Mechanisms of EEG and evoked potential generation
Protocol. Intraoperative Neurophysiologic Monitoring (sensoryevoked potentials, motor-evoked potentials, EEG monitoring)
 Intraoperative Neurophysiologic Monitoring (sensoryevoked potentials, motor-evoked potentials, EEG monitoring) (70158) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
Intraoperative Neurophysiologic Monitoring (sensoryevoked potentials, motor-evoked potentials, EEG monitoring) (70158) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
Navigated Transcranial Magnetic Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Accepted Manuscript. Editorial. Responsive neurostimulation for epilepsy: more than stimulation. Jayant N. Acharya
 Accepted Manuscript Editorial Responsive neurostimulation for epilepsy: more than stimulation Jayant N. Acharya PII: S2467-981X(18)30022-2 DOI: https://doi.org/10.1016/j.cnp.2018.06.002 Reference: CNP
Accepted Manuscript Editorial Responsive neurostimulation for epilepsy: more than stimulation Jayant N. Acharya PII: S2467-981X(18)30022-2 DOI: https://doi.org/10.1016/j.cnp.2018.06.002 Reference: CNP
9/30/2016. Advances in Epilepsy Surgery. Epidemiology. Epidemiology
 Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Re s e c t i o n of tumors in the proximity of eloquent
 J Neurosurg 114:719 726, 2011 Intraoperative magnetic resonance imaging guided tractography with integrated monopolar subcortical functional mapping for resection of brain tumors Clinical article Su j
J Neurosurg 114:719 726, 2011 Intraoperative magnetic resonance imaging guided tractography with integrated monopolar subcortical functional mapping for resection of brain tumors Clinical article Su j
Neuromodulation in Epilepsy. Gregory C. Mathews, M.D., Ph.D.
 Neuromodulation in Epilepsy Gregory C. Mathews, M.D., Ph.D. Disclosure There are no disclosures to share with regards to this presentation. Epilepsy Basics What is epilepsy? Partial versus generalized
Neuromodulation in Epilepsy Gregory C. Mathews, M.D., Ph.D. Disclosure There are no disclosures to share with regards to this presentation. Epilepsy Basics What is epilepsy? Partial versus generalized
Corporate Medical Policy
 Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Epilepsy. Seizures and Epilepsy. Buccal Midazolam vs. Rectal Diazepam for Serial Seizures. Epilepsy and Seizures 6/18/2008
 Seizures and Epilepsy Paul Garcia, M.D. UCSF Epilepsy Epileptic seizure: the physical manifestation of aberrant firing of brain cells Epilepsy: the tendency to recurrent, unprovoked epileptic seizures
Seizures and Epilepsy Paul Garcia, M.D. UCSF Epilepsy Epileptic seizure: the physical manifestation of aberrant firing of brain cells Epilepsy: the tendency to recurrent, unprovoked epileptic seizures
Biomedical Research 2013; 24 (3): ISSN X
 Biomedical Research 2013; 24 (3): 359-364 ISSN 0970-938X http://www.biomedres.info Investigating relative strengths and positions of electrical activity in the left and right hemispheres of the human brain
Biomedical Research 2013; 24 (3): 359-364 ISSN 0970-938X http://www.biomedres.info Investigating relative strengths and positions of electrical activity in the left and right hemispheres of the human brain
Reorganization of Language Areas in Patient with a Frontal Lobe Low Grade Glioma fmri Case Study
 Signature: Pol J Radiol, 2015; 80: 290-295 DOI: 10.12659/PJR.893897 CASE REPORT Received: 2015.02.18 Accepted: 2015.03.05 Published: 2015.06.04 Authors Contribution: A Study Design B Data Collection C
Signature: Pol J Radiol, 2015; 80: 290-295 DOI: 10.12659/PJR.893897 CASE REPORT Received: 2015.02.18 Accepted: 2015.03.05 Published: 2015.06.04 Authors Contribution: A Study Design B Data Collection C
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Intraoperative mapping during repeat awake craniotomy reveals the functional plasticity of adult cortex
 clinical article J Neurosurg 124:146 1469, 216 Intraoperative mapping during repeat awake craniotomy reveals the functional plasticity of adult cortex *Derek G. Southwell, MD, PhD, Shawn L. Hervey-Jumper,
clinical article J Neurosurg 124:146 1469, 216 Intraoperative mapping during repeat awake craniotomy reveals the functional plasticity of adult cortex *Derek G. Southwell, MD, PhD, Shawn L. Hervey-Jumper,
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
R esection of infiltrative tumours such as low grade gliomas
 PAPER Functional recovery after surgical resection of low grade gliomas in eloquent brain: hypothesis of brain compensation H Duffau, L Capelle, D Denvil, N Sichez, P Gatignol, M Lopes, M-C Mitchell, J-P
PAPER Functional recovery after surgical resection of low grade gliomas in eloquent brain: hypothesis of brain compensation H Duffau, L Capelle, D Denvil, N Sichez, P Gatignol, M Lopes, M-C Mitchell, J-P
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
ADVANCES IN Anesthesia
 ADVANCES IN Anesthesia CONTENTS VOLUME 24 2006 Associate Editors vii Contributors ix Anesthetic Considerations for Nonobstetric Surgery During Pregnancy By Howard H. Bernstein and Jerome You Case 1 1 Teratogenic
ADVANCES IN Anesthesia CONTENTS VOLUME 24 2006 Associate Editors vii Contributors ix Anesthetic Considerations for Nonobstetric Surgery During Pregnancy By Howard H. Bernstein and Jerome You Case 1 1 Teratogenic
