Classification of Childhood Aplastic Anemia and Myelodysplastic Syndrome
|
|
|
- Madeleine McKinney
- 6 years ago
- Views:
Transcription
1 APLASTIC ANEMIA:BONE MARROW FAILURE Classification of Childhood Aplastic Anemia and Myelodysplastic Syndrome Charlotte M. Niemeyer 1 and Irith Baumann 2 1 University Medical Center Freiburg, Freiburg, Germany; and 2 Clinical Centre South West, Boeblingen, Germany Hypoplastic BM disorders in children and adolescents comprise a broad spectrum of disorders. Acquired severe aplastic anemia (SAA), refractory cytopenia of childhood (RCC), a subtype of myelodysplastic syndrome (MDS), and inherited BM failure (IBMF) disorders are the main and most difficult hematological differential diagnoses. Whereas IBMF disorders can often be diagnosed by their clinical features and/or underlying genetic aberrations, the morphological distinction between SAA and hypocellular RCC has been controversial. The histopathological pattern of RCC consists of islands of immature erythroid precursors accompanied by sparsely distributed granulocytic cells. Megakaryocytes are significantly decreased or absent and, rarely, micromegakaryocytes are detected on immunohistochemistry. Because fatty tissue between areas of hematopoiesis can mimic SAA, 2 biopsies are recommended to facilitate the detection of representative BM spaces. Recent data indicate that the response to immunosuppressive therapy is inferior in RCC compared with SAA. Furthermore, approaches to allogeneic hematopoietic transplantation differ. Controlled prospective clinical studies in patients with hypoplastic BM failure disorders will require comprehensive guidelines for diagnosing SAA, RCC, and the different IBMF disorders. Introduction The appropriate classification of hypoplastic BM disorders in young patients continues to be a great challenge. Accurate diagnosis is the prerequisite for medical and genetic counseling, surveillance, and therapy options for these children and adolescents. Because most patients with BM failure will require allogeneic hematopoietic stem cell transplantation (HSCT), the timing of the procedure, choice of donor, preparative regimen, and estimation of complications will greatly differ among the various disease entities. Hypoplastic BM disorders in children and adolescents Pancytopenia with severe decrease of BM cellularity in children may be caused by a broad variety of underlying disorders (Table 1); of these, acquired severe aplastic anemia (SAA), refractory cytopenia of childhood (RCC), and inherited BM failure (IBMF) disorders are 3 of the most common hematopoietic diagnoses. The clinical and histopathological distinction between these 3 groups of disorders is a well-known challenge and has important therapeutic implications. Whereas SAA is considered an autoimmune-driven BM failure disorder for which most children are successfully treated with immunosuppressive therapy (IST), 1,2 RCC is classified as a subtype of myelodysplastic syndrome (MDS) generally thought to be cured by HSCT only. 3 IBMF is likely to be underdiagnosed. With the recent discoveries of underlying genetic alterations, these disorders are being diagnosed with increasing frequency in patients without phenotypic abnormalities. 4 Small populations of cells deficient in glycophosphatidylinositolanchored proteins may be noted in the absence of clinical and laboratory evidence of hemolysis in all 3 groups of BM failure disorders. They are most common in SAA, for which 40%-50% of patients carry these clones characteristic of paroxysmal nocturnal hemoglobinuria (PNH) at the time of diagnosis. 5 Response rate to IST is similar in SAA patients with or without PHN clones. In contrast to subclinical disease, overt PNH with thrombosis and hemolysis in the setting of BM failure is a rare finding in childhood. 6 Pancytopenia with a moderately or severely hypocellular BM may also herald acute leukemia. B-cell precursor acute lymphoblastic leukemia is preceded by a transient, remitting aplasia in 2% of childhood acute lymphoblastic leukemia. 7 Hematopoietic cells in the aplastic phase generally have a normal karyotype, but may carry a large number of secondary genetic changes characteristic of overt leukemia diagnosed up to 9 months later. 8 Rarely, familial and acquired hemophagocytic lymphohistiocytosis 9 or autoimmune lymphoproliferative disorder 10 may give rise to hypocellular BM. These genuine BM disorders can be mimicked by a large variety of nonhematological diseases such as viral infections, nutritional deficiencies, and metabolic disorders (Table 1). A careful medical history and presence of physical signs such as hepatosplenomegaly or lymphadenopathy may suggest an infectious origin. Interestingly, persisting or transient BM failure after varicella infection may be accompanied by multiple autoantibodies. 11 Classification of pediatric MDS The need for a pediatric approach to the diagnosis and management of MDS in children and adolescents has emerged over the past 2 decades. 12 The pediatric modification 12 of the first World Health Organization (WHO) classification 13 subdivided MDS into RCC (peripheral blood [PB] blasts 2% and BM blasts 5%), refractory anemia with excess blasts (RAEB; PB blasts 2%-19% and/or BM blasts 5%-19%) and RAEB in transformation (RAEB-T; PB and/or BM blasts 20%-29%). 12 This approach allows unambiguous classification of 95% of patients 14 and was incorporated into the second WHO classification in American Society of Hematology
2 Table 1. Disorders with hypoplastic BM Nonhematological disorders Infections (eg, CMV, EBV, herpesvirus, parvovirus, varicella virus, HIV, visceral leishmaniasis) Vitamin deficiency (eg, deficiency of vitamin B12, folate, vitamin E) Metabolic disorders (eg, mevalonate kinase deficiency) Rheumatic disease Mitochondrial deletions (Pearson syndrome) Hematological disorders Inherited BM failure disorders (eg, Fanconi anemia, dyskeratosis congenita, amegakaryocytic thrombocytopenia, thrombocytopenia with absent radii, Seckel syndrome) SAA RCC Clinical paroxysmal nocturnal hemoglobinuria in the setting of BM failure Hypoplastic prephase of B-cell precursor acute lymphoblastic leukemia Hemophagocytic lymphohistiocytosis Autoimmune lymphoproliferative disorders (eg, fas deficiency) MDS after prior chemotherapy or radiation therapy, after prior acquired aplastic anemia, or in IBMF disorders and familial diseases is generally classified as secondary MDS. All other cases are referred to as primary MDS, although it is reasonable to assume that most of these disorders are secondary to some as-yet-unknown genetic predisposition. These presumed underlying genetic changes may also give rise to subtle phenotypic abnormalities observed in many children with primary MDS. 12 Monosomy 7 is the most common cytogenetic abnormality in childhood MDS, being seen in 30% of cases Trisomy 8 and trisomy 21 are the second most common numerical abnormalities. Constitutional trisomy 21 is usually clinically obvious when present, whereas constitutional trisomy 8 mosaicism may remain unrecognized and should be tested when trisomy 8 is found in the BM. 19 The presence of a structurally complex karyotype characterized by 3 chromosomal aberrations, including at least 1 structural aberration, is the strongest independent prognostic marker predicting poor outcome. 18 RAEB in children has similar morphological and immunophenotypical features to that observed in adults. Children with RAEB generally have relatively stable counts for weeks or months. A similar biological behavior is noted in some children considered RAEB-T in the French-American-British (FAB) Cooperative Group classification. Because these children may not benefit from acute myeloid leukemia type intensive chemotherapy before HSCT, the subdivision of RAEB-T was retained in the pediatric MDS classification. 12,15 RCC RCC is the most common subtype of MDS in children and adolescents, accounting for approximately half of all MDS cases. 17,20 It is diagnosed in all age groups and, in contrast to MDS with increased blast count, affects boys and girls with equal frequency. 21 Children usually present with symptoms related to pancytopenia, such as anemia, infection, and bleeding tendency. The term refractory cytopenia indicates that, in contrast to adults, thrombocytopenia and neutropenia are more frequently observed than anemia in children. In fact, 3/4 of patients present with a platelet count /L, 1/2 with an absolute neutrophil count at the time of diagnosis of /L and 1/4 of /L. Anemia with a hemoglobin concentration of 10 mg/100 ml is seen in approximately 1/2 of affected children. 21 The mean corpuscular volume of red cells and hemoglobin F are usually elevated. In contrast to adult refractory anemia, the majority of children with RCC show a marked decrease of BM cellularity. In an interim analysis of studies, the European Working Group of MDS of Childhood (EWOG-MDS) 1998 and 2006 found that 81% of patients with RCC had a hypocellular biopsy specimen (Figure 1) (EWOG-MDS, unpublished data). Because a variety of nonhematological disorders can induce secondary myelodysplasia, BM aspiration cytology constitutes only one aspect of the RCC diagnosis. In particular, the need for the differentiation from other hypocellular BM disorders requires the evaluation of a trephine biopsy. In the absence of a cytogenetic marker, the clinical course will have to be carefully evaluated and 2 BM examinations with biopsies at least 2 weeks apart are recommended before a diagnosis of RCC can be established. Figure 1. BM cellularity and karyotype in primary RCC. Interim analysis of studies EWOG-MDS 1998 and Hematology
3 Figure 2. Schematic view of the histopathological pattern in RCC with normocellular and hypocellular BM. The presence of a cytogenetic abnormality can be important in confirming the diagnosis of MDS. Because of the difficulty in establishing the diagnosis of childhood RCC, it is likely that in retrospective studies, RCC patients with chromosomal changes were preferentially reported. 17,21 In the prospective multicenter study EWOG-MDS 98, standard cytogenetics in BM cells of patients with RCC and normal or increased BM cellularity showed a normal karyotype, monosomy 7, or other aberrations in 61%, 19%, and 12% of cases, respectively (Figure 1; EWOG-MDS, unpublished data). In hypocellular RCC, the incidence of monosomy 7 and other aberrations decreased to 20% of successful analyses (Figure 1). There was no difference in morphology between cases with or without monosomy 7 or other aberrations. Loss of the long arm of chromosome 5 (5q ), the most frequent chromosomal aberration in adults with refractory anemia, is exceedingly rare in childhood. Studies are under way to evaluate whether newer techniques such as single-nucleotide polymorphism array-based karyotyping can be important in distinguishing RCC and SAA. Spontaneous disappearance of cytopenia with monosomy 7 or deletions of the long arm of chromosome 7, del (7q), has been reported in some infants, but remains a rare event. 22,23 Although chromosomal changes are not thought to be initiating events, they are probably involved in disease progression, and karyotypic evolution is generally accompanied by progression to more advanced forms of MDS in each case. Patients with monosomy 7 have a significantly higher probability of progression to advanced MDS than do patients with other chromosomal abnormalities or normal karyotype. 21 In a retrospective series of 67 patients with RCC, the estimated median time to progression for children with monosomy 7 was 1.9 years and the cumulative incidence of progression was 80% at 6 years from diagnosis. In contrast to monosomy 7, patients with trisomy 8 or normal karyotype may experience a long, stable course of their disease. Morphological distinction between hypoplastic RCC and acquired aplastic anemia Hypoplastic RCC shows a pathohistological pattern of the BM that is comparable to hyper- or normocellular RCC (Figure 2). In both, the detection of erythroids with impaired maturation is essential and is an important marker for the diagnosis of RCC. In hypoplastic RCC, one or possibly several clusters of at least 10 erythroid precursors with increased numbers of proerythroblasts and increased numbers of mitoses are distributed in a patchy pattern in an otherwise adipocytic BM. 15 Granulopoiesis is always decreased and may be left shifted as well. Megakaryocytes are markedly decreased or absent. Immunohistochemistry is indispensable for the detection of micromegakaryocytes, which can be easily be missed on hematoxylin and eosin stains of the BM trephine or aspirate. In contrast to MDS in adults, RCC shows no increase in reticulin fibers. Lymphocytes, plasma cells, and mast cells may be increased. Clusters of blast cells are not seen in RCC, and myeloperoxidase-, lysozyme-, CD34-, and/or CD117-positive myeloid blast cells are not increased. Acquired aplastic anemia reveals aplasia of all 3 hematological cell lineages. Lymphocytes, plasma cells, and mast cells may be focally increased or dispersed. Erythroid islands with an increased number of immature erythroblasts, particularly proerythroblasts and micromegakaryocytes, are absent (Table 2). After immunosuppressive therapy, the histological pattern of acquired aplastic anemia can no longer be separated from that observed in RCC. RCC and inherited BM failure disorder IBMF disorders with pancytopenia, such as Fanconi anaemia, dyskeratosis congenita, Shwachman Diamond syndrome, amegakaryocytic thrombocytopenia, and pancytopenia with radio-ulnar synostosis, show overlapping morphological features with RCC. There is macrocytosis of red cells on PB smear, elevated hemoglobin F, and undistinguishable histopathological findings on trephine biopsies. 15 Therefore, IBMF disorders have to be excluded by careful past medical and family history, meticulous physical examination for skeletal and other organ abnormalities, and the appropriate laboratory/molecular studies before a definite diagnosis of RCC can be made. For most patients, the suspicion of Fanconi anemia arises only after the development of BM failure, which generally starts in childhood 86 American Society of Hematology
4 Table 2. Histopathologic criteria of RCC and SAA as published in the WHO classification RCC SAA Erythropoiesis Patchy distribution Lacking or single small focus with 10 cells with maturation Left shift Increased mitoses Granulopoiesis Marked decrease Lacking or marked decrease, very few small foci with maturation Left shift Megakaryopoiesis Marked decrease Lacking or very few, no dysplastic megakaryocytes Dysplastic changes Micromegakaryocytes Lymphocytes May be increased focally or dispersed May be increased focally or dispersed CD34 cells No increase No increase (Used with permission from Baumann et al. 15 ) or adolescence. 4 Approximately 15% of consecutive German patients presenting for the first time with a histopathological pattern compatible with RCC are later diagnosed as suffering from Fanconi anemia, and in approximately 2/3 of these cases, Fanconi anemia was not the primary suspected diagnosis of the treating physician (EWOG-MDS, unpublished data). Analyses to exclude Fanconi anemia by chromosomal breakage test, G 2 cell-cycle arrest, and Western blot or mutational analyses are mandatory for all the children before the diagnosis of RCC can be confirmed. Similarly to Fanconi anemia, cytopenia can precede the appearance of the characteristic mucocutaneous triad of nail dystrophy, mucosal leucoplakia, and abnormal skin pigmentations or pulmonary symptoms in dyskeratosis congenita. 4 In a heterogenous series of patients diagnosed as having acquired aplastic anemia or low-grade MDS, heterozygous mutations in the core component of telomerase, namely the telomerase RNA component (TERC) and the telomerase reverse transcriptase component (TERT), and in the shelterin component TIN2 can be observed in 5%-10% Because telomeres of mononuclear cells in patients with dyskeratosis congenital are invariably short, telomere length is thought to be a suitable screening parameter to select patients for molecular analyses of involved genes. 28 Homozygous or compound heterozygous SBDS gene mutations were not noted in screened series of patients with acquired BM failure, indicating that in most patients with Shwachman Diamond syndrome, pancytopenia was not the only presenting clinical feature. 29,30 The significance of heterozygosity for SBDS mutations remains to be unraveled. 30 In children with congenital amegakaryocytic thrombocytopenia, BM trephine usually has normal absent or low numbers of megakaryocytes but unremarkable erythropoiesis and granulopoiesis at the time of diagnosis. 31 As disease progresses, BM hypocellularity with an RCC pattern develops. The syndrome of proximal radio-ulnar synostosis with BM failure is another rare differential diagnosis of RCC. 32 It is conceivable that several children diagnosed with hypoplastic RCC may suffer from an as-yet-undiagnosed IBMF disorder. Because family members may suffer from the same disorder, BM examination with biopsy, cytogenetic examination, and possibly measurement of telomere length is advisable for all potential family HSCT donors irrespective of PB counts. 33 Because IBMF disorders cannot be separated from RCC by morphology, progression to MDS in IBMF requires careful definition. Secondary MDS in IBMF can morphologically be diagnosed in the presence of an elevated blast percentage or increasing BM cellularity despite continuing pancytopenia. Cytogenetic abnormalities such as partial or complete deletion of chromosome 7; 21q abnormalities; losses of 11q, 20q, or 5q; and trisomy 8 may also indicate secondary MDS. However, leukemic progression in each of these IBMF disorders is associated with a complex pattern of recurrent chromosomal and genomic abnormalities, some of them specific for the disorders, others commonly found in MDS and secondary acute myeloid leukemia. In Fanconi anemia, a gain of chromosomal segment 3q26 is an adverse risk factor for leukemic progression, 34 whereas a sole gain of chromosome 1q may persist for years without development of MDS or acute myeloid leukemia. 35 Similarly, persisting or fluctuating clones have been observed in dyskeratosis congenita. 4 Patients with Shwachman Diamond syndrome and isochromosome 7q [i(7q)] or del(20q) can have a stable clinical course for years. 36 The increased incidence of i(7q) in Shwachman Diamond syndrome may suggest that it is a fairly specific clonal marker in this syndrome and that it may be related to the SDS gene, which is located on the centromeric region of chromosome7 (7p12-7q11). The clinical significance with respect to therapeutic options and clinical benefits of the various cytogenetic and molecular aberrations will need to be carefully evaluated in defined prospective studies in these individual IBMF disorders. Because abnormal clones can potentially regress in any IBMF disorder, close monitoring is advisable. Treatment options for RCC HSCT is the treatment of choice for patients with RCC and monosomy 7 or complex karyotypes early in the course of the disease. In view of a low transplantation-related mortality, HSCT can also be recommended for patients with other karyotypes if a suitable donor is available 3,20 (Figure 3). For children with hypocellular RCC, a preparative regimen with reduced-intensity conditioning represents an effective transplantation strategy in the absence of chromosomal abnormality. 3 A watch and wait strategy with careful observation may be reasonable for patients in the absence of transfusion requirements, severe cytopenia, or infections. Because early BM failure can at least in part be mediated by T-cell immunosuppression of hematopoiesis, 37 immunosuppressive therapy can be a successful therapy strategy for some children with RCC. 38,39 However, response and failure-free survival after IST is less favorable in RCC compared with SAA. 39 In a recent interim report of EWOG-MDS on 91 children given IST as frontline treatment, the response rate at 6 months was 63% and the overall and failure-free survival rates at 5 years were 90% and 40%, respectively. 40 Hematology
5 Figure 3. Current approach to therapy of RCC in the studies bythe EWOG-MDS. Summary and future directions Improvement of clinical care for patients with BM failure disorders will depend in part on comprehensive diagnostic guidelines with internationally accepted definitions. 41 The latter will also allow the prospective enrollment of defined patient populations in registries and therapeutic trials. In the past, the term aplastic anemia has been broadly applied to hypocellular BM irrespective of the respective histopathological features. Using the same morphological criteria applied for patients with normal cellularity, the histopathological pattern of hypoplastic RCC of childhood was established. Reference review of diagnostic trephine biopsies before enrollment in the prospective study for aplastic anemia (SAA 84) or MDS (EWOG-MDS 98, 2006) greatly reduced the incidence of early clonal evolution among SAA patients. 42 In addition, hypoplastic BM with cytogenetic aberrations was solely classified as RCC (EWOG-MDS, unpublished data). Future research will have to unravel the etiology and biological nature of both SAA and RCC. Disclosures Conflict-of-interest disclosure: The authors declare no competing financial interests. Off-label drug use: None disclosed. Correspondence Charlotte M. Niemeyer, Department of Pediatric Hematology/ Oncology, University Medical Center Freiburg, Mathilden Strasse 1, D Freiburg, Germany; Phone: ; Fax: ; References 1. Yoshida N, Yagasaki H, Hama A, et al. Predicting response to immunosuppressive therapy in childhood aplastic anemia. Haematologica. 2011;96(5): Führer M, Rampf U, Baumann I, et al. Immunosuppressive therapy for aplastic anemia in children: a more severe disease predicts better survival. Blood. 2005;106: Strahm B, Locatelli F, Bader P, et al. Reduced intensity conditioning in unrelated donor transplantation for refractory cytopenia in childhood. Bone Marrow Transplant. 2007;40: Shimamura A, Alter BP. Pathophysiology and management of inherited bone marrow failure syndromes. Blood Rev. 2010;24: Scheinberg P, Marte M, Nunez O, Young NS. Paroxysmal nocturnal hemoglobinuria clones in severe aplastic anemia patients treated with horse anti-thymocyte globulin plus cyclosporine. Haematologica. 2010;95: van den Heuvel-Eibrink MM. Paroxysmal nocturnal hemoglobinuria in children. Paediatr Drugs. 2007;9: Hasle H, Heim S, Schroeder H, et al. Transient pancytopenia preceding acute lymphoblastic leukemia (pre-all). Leukemia. 1995;9: Horsley SW, Colman S, McKinley M, et al. Genetic lesions in a preleukemic aplasia phase in a child with acute lymphoblastic leukemia. Genes Chromosomes Cancer. 2008;47: Janka GE. Familial and acquired hemophagocytic lymphohistiocytosis. Eur J Pediatr. 2007;166: Bader-Meunier B, Rieux-Laucat F, Croisille L, et al. Dyserythropoiesis associated with a fas-deficient condition in childhood. Br J Haematol. 2000;108: Bader-Meunier B, Dusser A, Mersh JM, et al. Varicellaassociated pancytopenia. Eur J Pediatr. 1990;149: Hasle H, Niemeyer CM, Chessells JM, et al. A pediatric approach to the WHO classification of myelodysplastic and myeloproliferative diseases. Leukemia. 2003;17: Jaffe ES, Harris NL, Stein H, Vardiman JW. World Health Organization Classification of Tumours: Pathology and Genetics of Tumours of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC; Elghetany MT. Myelodysplastic syndromes in children: a critical review of issues in the diagnosis and classification of 887 cases from 13 published series. Arch Pathol Lab Med. 2007;131: Baumann I, Niemeyer CM, Bennett JM, Shannon K. Childhood myelodysplastic syndrome. In: Swerdlow S, Campo E, Harris NL, eds.; International Agency for Research on Cancer. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissue. Geneva, Switzerland: World Health Organization; 2008; American Society of Hematology
6 16. Luna-Fineman S, Shannon KM, Atwater SK, et al. Myelodysplastic and myeloproliferative disorders of childhood: a study of 167 patients. Blood. 1999;93: Passmore SJ, Chessells JM, Kempski H, et al. Paediatric myelodysplastic syndromes and juvenile myelomonocytic leukaemia in the UK: a population-based study of incidence and survival. Br J Haematol. 2003;121: Göhring G, Michalova K, Beverloo HB, et al. Complex karyotype newly defined: the strongest prognostic factor in advanced childhood myelodysplastic syndrome. Blood. 2010; 116: Maserati E, Aprili F, Vinante F, et al. Trisomy 8 in myelodysplasia and acute leukemia is constitutional in 15-20% of cases. Genes Chromosomes Cancer. 2002;33: Niemeyer CM, Baumann I. Myelodysplastic syndrome in children and adolescents. Semin Hematol. 2008;45: Kardos G, Baumann I, Passmore SJ, et al. Refractory anemia in childhood: a retrospective analysis of 67 patients with particular reference to monosomy 7. Blood. 2003;102: Parker TM, Klaassen RJ, Johnston DL. Spontaneous remission of myelodysplastic syndrome with monosomy 7 in a young boy. Cancer Genet Cytogenet. 2008;182: Mantadakis E, Shannon KM, Singer DA, et al. Transient monosomy 7: a case series in children and review of the literature. Cancer. 1999;85: Yamaguchi H, Baerlocher GM, Lansdorp PM, et al. Mutations of the human telomerase RNA gene (TERC) in aplastic anemia and myelodysplastic syndrome. Blood. 2003;102: Yamaguchi H, Calado RT, Ly H, et al. Mutations in TERT, the gene for telomerase reverse transcriptase, in aplastic anemia. N Engl J Med. 2005;352: Ortmann CA, Niemeyer CM, Wawer A, et al. TERC mutations in children with refractory cytopenia. Haematologica. 2006;91: Walne AJ, Vulliamy T, Beswick R, Kirwan M, Dokal I. TINF2 mutations result in very short telomeres: analysis of a large cohort of patients with dyskeratosis congenita and related bone marrow failure syndromes. Blood. 2008;112: Du HY, Pumbo E, Ivanovich J, et al. TERC and TERT gene mutations in patients with bone marrow failure and the significance of telomere length measurements. Blood. 2009;113: Karow A, Flotho C, Schneider M, Fliegauf M, Niemeyer CM. Mutations of the Shwachman-Bodian-Diamond syndrome gene in patients presenting with refractory cytopenia do we have to screen? Haematologica. 2010;95: Calado RT, Graf SA, Wilkerson KL, et al. Mutations in the SBDS gene in acquired aplastic anemia. Blood. 2007;110: Leguit RJ, van den Tweel JG. The pathology of bone marrow failure. Histopathology. 2010;57: Castillo-Caro P, Dhanraj S, Haut P, et al. Proximal radio-ulnar synostosis with bone marrow failure syndrome in an infant without a HOXA11 mutation. J Pediatr Hematol Oncol. 2010;32: Fogarty PF, Yamaguchi H, Wiestner A, et al. Late presentation of dyskeratosis congenita as apparently acquired aplastic anaemia due to mutations in telomerase RNA. Lancet. 2003;362: Tönnies H, Huber S, Kuhl JS, et al. Clonal chromosomal aberrations in bone marrow cells of Fanconi anemia patients: gains of the chromosomal segment 3q26q29 as an adverse risk factor. Blood. 2003;101: Quentin S, Cuccuini W, Ceccaldi R, et al. Myelodysplasia and leukemia of Fanconi anemia are associated with a specific pattern of genomic abnormalities that includes cryptic RUNX1/ AML1 lesions. Blood. 2011;117:e161-e Dror Y, Durie P, Ginzberg H, et al. Clonal evolution in marrows of patients with Shwachman-Diamond syndrome: a prospective 5-year follow-up study. Exp Hematol. 2002;30: de Vries AC, Langerak AW, Verhaaf B, et al. T-cell receptor Vbeta CDR3 oligoclonality frequently occurs in childhood refractory cytopenia (MDS-RC) and severe aplastic anemia. Leukemia. 2008;22: Sloand EM, Wu CO, Greenberg P, Young N, Barrett J. Factors affecting response and survival in patients with myelodysplasia treated with immunosuppressive therapy. J Clin Oncol. 2008;26: Yoshimi A, Baumann I, Fuhrer M, et al. Immunosuppressive therapy with anti-thymocyte globulin and cyclosporine A in selected children with hypoplastic refractory cytopenia. Haematologica. 2007;92: Yoshimi-Nöllke A, van den Heuvel-Eibrink MM, Baumann I, et al. Immunosuppressive therapy with anti-thymocyte globin and cyclosporine A in patients with refractory cytopenia in childhood [Abstract]. Bone Marrow Transplant. 2011;46:S Pulsipher MA, Young NS, Tolar J, et al. Optimization of therapy for severe aplastic anemia based on clinical, biologic, and treatment response parameters: conclusions of an international working group on severe aplastic anemia convened by the Blood and Marrow Transplant Clinical Trials Network, March Biol Blood Marrow Transplant. 2011;17: Führer M, Burdach S, Ebell W, et al. Relapse and clonal disease in children with aplastic anemia (AA) after immunosuppressive therapy (IST): the SAA 94 experience. German/Austrian Pediatric Aplastic Anemia Working Group. Klin Padiatr. 1998;210: Hematology
The current perspective of low grade myelodysplastic syndrome in children
 Int J Hematol (2016) 103:360 364 DOI 10.1007/s12185-016-1965-7 PROGRESS IN HEMATOLOGY Pediatric MDS/MPN The current perspective of low grade myelodysplastic syndrome in children Daisuke Hasegawa 1 Received:
Int J Hematol (2016) 103:360 364 DOI 10.1007/s12185-016-1965-7 PROGRESS IN HEMATOLOGY Pediatric MDS/MPN The current perspective of low grade myelodysplastic syndrome in children Daisuke Hasegawa 1 Received:
The histopathology of bone marrow failure in children
 Journal of clinical and experimental hematopathology Vol. 58 No.2, 68-86, 2018 JC lin EH xp ematopathol Review Article The histopathology of bone marrow failure in children Hideto Iwafuchi Bone marrow
Journal of clinical and experimental hematopathology Vol. 58 No.2, 68-86, 2018 JC lin EH xp ematopathol Review Article The histopathology of bone marrow failure in children Hideto Iwafuchi Bone marrow
Outline. What is aplastic anemia? 9/19/2012. Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options
 Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed
 MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
Aplastic Anemia: Understanding your Disease and Treatment Options
 Aplastic Anemia: Understanding your Disease and Treatment Options No financial relationships or commercial interest related to the content of this presentation Josh Sasine, MD, PhD Hematopoietic Cell Transplant
Aplastic Anemia: Understanding your Disease and Treatment Options No financial relationships or commercial interest related to the content of this presentation Josh Sasine, MD, PhD Hematopoietic Cell Transplant
The function of the bone marrow. Living with Aplastic Anemia. A Case Study - I. Hypocellular bone marrow failure 5/14/2018
 The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
Overview of Aplastic Anemia. Overview of Aplastic Anemia. Epidemiology of aplastic anemia. Normal hematopoiesis 10/6/2017
 Overview of Aplastic Anemia Overview of Aplastic Anemia Peter Westervelt, MD, PhD Professor of Medicine Chief, BMT/Leukemia Section Washington University School of Medicine Epidemiology Normal hematopoiesis
Overview of Aplastic Anemia Overview of Aplastic Anemia Peter Westervelt, MD, PhD Professor of Medicine Chief, BMT/Leukemia Section Washington University School of Medicine Epidemiology Normal hematopoiesis
Review Article. MYELODYSPLASIA IN CHILDHOOD Shantaraman. K
 MYELODYSPLASIA IN CHILDHOOD Shantaraman. K Review Article Abstract: Myelodysplasia is a heterogenous group of disorders that was earlier described as preleukemia, refractory anemia with excess of blasts,
MYELODYSPLASIA IN CHILDHOOD Shantaraman. K Review Article Abstract: Myelodysplasia is a heterogenous group of disorders that was earlier described as preleukemia, refractory anemia with excess of blasts,
Aplastic Anemia Pathophysiology and Approach to Therapy
 Aplastic Anemia Pathophysiology and Approach to Therapy BSMCON 2018 Dr. Syed Ghulam Mogni Mowla MBBS, FCPS, FACP Introduction Aplastic anaemia (AA) is the paradigm of the human bone marrow failure syndromes
Aplastic Anemia Pathophysiology and Approach to Therapy BSMCON 2018 Dr. Syed Ghulam Mogni Mowla MBBS, FCPS, FACP Introduction Aplastic anaemia (AA) is the paradigm of the human bone marrow failure syndromes
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood
 Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood V. TOULIATOU 1, A. KOLIALEXI 1, G.TH. TSANGARIS 2, M. MOSCHOVI 3, S.
Conventional Cytogenetics and Fluorescence In Situ Hybridization in Persistent Cytopenias and Myelodysplastic Syndromes in Childhood V. TOULIATOU 1, A. KOLIALEXI 1, G.TH. TSANGARIS 2, M. MOSCHOVI 3, S.
3/31/2014. New Directions in Aplastic Anemia Treatment: What s on the Horizon? Objectives
 New Directions in Aplastic Anemia Treatment: What s on the Horizon? AA & MDS International Foundation Living with, MDS, or PNH Patient and Family Conferences in 2014 April 5, 2014 Objectives To provide
New Directions in Aplastic Anemia Treatment: What s on the Horizon? AA & MDS International Foundation Living with, MDS, or PNH Patient and Family Conferences in 2014 April 5, 2014 Objectives To provide
9/9/2015 HISTORY & EPIDEMIOLOGY. Objectives. Textbook Definition of Aplastic anemia (AA) Epidemiology. History
 Objectives Aplastic Anemia: Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Amy E. DeZern, MD, MHS Assistant Professor of Oncology and Medicine The Johns Hopkins University School
Objectives Aplastic Anemia: Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Amy E. DeZern, MD, MHS Assistant Professor of Oncology and Medicine The Johns Hopkins University School
SESSION 1 Reactive cytopenia and dysplasia
 SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
Bone marrow failure. By Zahraa Nasooh Al_Saaty
 Bone marrow failure By Zahraa Nasooh Al_Saaty Pancytopenia : Pancytopenia describes a reduction in the blood count of all the major cell lines-red cells,white cell and platelets. It has several causes
Bone marrow failure By Zahraa Nasooh Al_Saaty Pancytopenia : Pancytopenia describes a reduction in the blood count of all the major cell lines-red cells,white cell and platelets. It has several causes
MDS: Who gets it and how is it diagnosed?
 MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
Year 2002 Paper two: Questions supplied by Jo 1
 Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
Myelodysplastic Syndrome: Let s build a definition
 1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
Border between aplastic anemia and myelodysplastic syndrome
 Int J Hematol (2013) 97:558 563 DOI 10.1007/s12185-013-1324-x PROGRESS IN HEMATOLOGY Advances in the management of acquired aplastic anemia (AA) Border between aplastic anemia and myelodysplastic syndrome
Int J Hematol (2013) 97:558 563 DOI 10.1007/s12185-013-1324-x PROGRESS IN HEMATOLOGY Advances in the management of acquired aplastic anemia (AA) Border between aplastic anemia and myelodysplastic syndrome
Disclosers Updates: Management of Aplastic Anemia and Congenital Marrow Failure 5/9/2017
 2017 Updates: Management of Aplastic Anemia and Congenital Marrow Failure Sachit Patel, MD Department of Pediatrics Division of Hematology-Oncology Blood and Marrow Transplantation Disclosers None 1 Objectives:
2017 Updates: Management of Aplastic Anemia and Congenital Marrow Failure Sachit Patel, MD Department of Pediatrics Division of Hematology-Oncology Blood and Marrow Transplantation Disclosers None 1 Objectives:
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Aplastic Anemia. is a bone marrow failure disease 9/19/2017. What you need to know about. The 4 major components of blood
 What you need to know about Aplastic Anemia Stuart Goldberg MD Aplastic Anemia is a bone marrow failure disease The bone marrow is the factory that makes blood The 4 major components of blood Red Blood
What you need to know about Aplastic Anemia Stuart Goldberg MD Aplastic Anemia is a bone marrow failure disease The bone marrow is the factory that makes blood The 4 major components of blood Red Blood
June 11, Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI
 June 11, 2018 Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI 53713 policycomments@wpsic.com RE: Draft Local Coverage Determination: MolDX: MDS FISH (DL37772) Dear Dr. Noel Thank you for the opportunity
June 11, 2018 Ella Noel, D.O., FACOI 1717 West Broadway Madison, WI 53713 policycomments@wpsic.com RE: Draft Local Coverage Determination: MolDX: MDS FISH (DL37772) Dear Dr. Noel Thank you for the opportunity
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Myelodysplastic and myeloproliferative disorders of childhood
 PEDIATRIC HEMATOLOGIC MALIGNANCIES Myelodysplastic and myeloproliferative disorders of childhood Henrik Hasle Department of Pediatrics, Aarhus University Hospital, Aarhus, Denmark Myelodysplastic syndrome
PEDIATRIC HEMATOLOGIC MALIGNANCIES Myelodysplastic and myeloproliferative disorders of childhood Henrik Hasle Department of Pediatrics, Aarhus University Hospital, Aarhus, Denmark Myelodysplastic syndrome
myelodysplastic syndrome MDS MDS MDS
 myelodysplastic syndrome MDS MDS 15 10 3 2004 15 MDS 400 2 65 61 70 MDS MDS 1 1 2 3 3 4 1 4 2 3 4 MDS 1982 Bennett French- American-BritishFAB 1 2 WHO 1999 3 2001 4 2002 Vardiman MDS 5 2WHO FAB refractory
myelodysplastic syndrome MDS MDS 15 10 3 2004 15 MDS 400 2 65 61 70 MDS MDS 1 1 2 3 3 4 1 4 2 3 4 MDS 1982 Bennett French- American-BritishFAB 1 2 WHO 1999 3 2001 4 2002 Vardiman MDS 5 2WHO FAB refractory
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
APPROACHING TO PANCYTOPENIA
 APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Changes to the 2016 WHO Classification for the Diagnosis of MDS
 Changes to the 2016 WHO Classification for the Diagnosis of MDS Welcome to Managing MDS. I am Dr. Ulrich Germing, and today, I will provide highlights from the 14th International Symposium on MDS in Valencia,
Changes to the 2016 WHO Classification for the Diagnosis of MDS Welcome to Managing MDS. I am Dr. Ulrich Germing, and today, I will provide highlights from the 14th International Symposium on MDS in Valencia,
Table 1: biological tests in SMD
 Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
7/13/2017. PreventionGenetics. How are genes associated with bone marrow failure?
 Personalized Medicine: tic Testing and the Implications for Future Therapies Preventiontics Michael Chicka, PhD, Molecular ticist, Preventiontics Founded in 2004 in Marshfield Wisconsin by Dr. Jim Weber
Personalized Medicine: tic Testing and the Implications for Future Therapies Preventiontics Michael Chicka, PhD, Molecular ticist, Preventiontics Founded in 2004 in Marshfield Wisconsin by Dr. Jim Weber
INHERITED PANCYTOPENIA SYNDROMES Fanconi anemia Shwachman-Diamond syndrome Dyskeratosis congenita Congenital amegakaryocytic thrombocytopenia
 The Pancytopenias The Inherited Pancytopenias Pancytopenia refers to a reduction below normal values of all 3 peripheral blood component: leukocytes, platelets, and erythrocytes. Pancytopenia requires
The Pancytopenias The Inherited Pancytopenias Pancytopenia refers to a reduction below normal values of all 3 peripheral blood component: leukocytes, platelets, and erythrocytes. Pancytopenia requires
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
 Preface In recent years, the pathogenesis of hematological disorders in children has been clarified, which has led to remarkable progress in the treatment outcome for these disorders. In particular, molecular
Preface In recent years, the pathogenesis of hematological disorders in children has been clarified, which has led to remarkable progress in the treatment outcome for these disorders. In particular, molecular
Severe Aplastic Anemia in Children and Adolescents. Brigitte Strahm 21. April 2018
 Severe Aplastic Anemia in Children and Adolescents Brigitte Strahm 21. April 2018 Acquired Aplastic Anemia in children What is aquired aplastic anemia? Camitta, Blood 1976 How A.L.G. acts is unknown, but
Severe Aplastic Anemia in Children and Adolescents Brigitte Strahm 21. April 2018 Acquired Aplastic Anemia in children What is aquired aplastic anemia? Camitta, Blood 1976 How A.L.G. acts is unknown, but
How I treat acquired aplastic anemia
 How I treat acquired aplastic anemia Phillip Scheinberg and Neal S. Young Blood Volume 120(6):1185-1196 August 9, 2012 2012 by American Society of Hematology Symptoms, Signs, and Lab Findings Bruising,
How I treat acquired aplastic anemia Phillip Scheinberg and Neal S. Young Blood Volume 120(6):1185-1196 August 9, 2012 2012 by American Society of Hematology Symptoms, Signs, and Lab Findings Bruising,
Pediatrics. Aplastic Anemia in Children Prognosis and Survival Rate. Definition of Aplastic Anemia. See online here
 Pediatrics Aplastic Anemia in Children Prognosis and Survival Rate See online here Aplastic anemia is a rare disease affecting 1 2 people per one million of the population. The hallmark of the disease
Pediatrics Aplastic Anemia in Children Prognosis and Survival Rate See online here Aplastic anemia is a rare disease affecting 1 2 people per one million of the population. The hallmark of the disease
Etiology. Definition MYELODYSPLASTIC SYNDROMES. De novo. Secondary MDS (10 years earlier than primary) transformation
 MYELODYSPLASTIC SYNDROMES Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics The University of Texas M.D. Anderson Cancer Center Houston, Texas No relevant COIs to
MYELODYSPLASTIC SYNDROMES Rashmi Kanagal-Shamanna, MD Assistant Professor Hematopathology & Molecular Diagnostics The University of Texas M.D. Anderson Cancer Center Houston, Texas No relevant COIs to
RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165
 RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165 Sebastian J. Sasu, M.D. UCLA Medical Center, Hematopathology Los Angeles, CA and Saint John s s Health Center Santa Monica, CA Clinical History
RAEB-2 2 Transforming to Acute Erythroleukemia Case # 165 Sebastian J. Sasu, M.D. UCLA Medical Center, Hematopathology Los Angeles, CA and Saint John s s Health Center Santa Monica, CA Clinical History
Aplastic Anemia: Current Thinking
 Aplastic Anemia: Current Thinking ANDREW C. DIETZ, MD, MSCR PEDIATRIC BLOOD AND MARROW TRANSPLANTATION CHILDREN S HOSPITAL LOS ANGELES, UNIVERSITY OF SOUTHERN CALIFORNIA Outline Ø What is Aplastic Anemia?
Aplastic Anemia: Current Thinking ANDREW C. DIETZ, MD, MSCR PEDIATRIC BLOOD AND MARROW TRANSPLANTATION CHILDREN S HOSPITAL LOS ANGELES, UNIVERSITY OF SOUTHERN CALIFORNIA Outline Ø What is Aplastic Anemia?
Supplementary Appendix
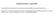 Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
Hematopoietic Cell Transplantation in Bone Marrow Failure Syndromes
 Hematopoietic Cell Transplantation in Bone Marrow Failure Syndromes The The 44 th th WBMT WBMT SYMPOSIUM 2017 2017 Riyadh, Saudi Saudi Arabia Arabia Mouhab Mouhab Ayas, Ayas, MD MD Department of Pediatric
Hematopoietic Cell Transplantation in Bone Marrow Failure Syndromes The The 44 th th WBMT WBMT SYMPOSIUM 2017 2017 Riyadh, Saudi Saudi Arabia Arabia Mouhab Mouhab Ayas, Ayas, MD MD Department of Pediatric
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Myelodysplastic Syndrome Case 158
 Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification
 What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes.
 Protocol Synopsis Study Title A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes. Short Title European MDS
Protocol Synopsis Study Title A prospective, multicenter European Registry for newly diagnosed patients with Myelodysplastic Syndromes of IPSS low and intermediate-1 subtypes. Short Title European MDS
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Bor-Sheng Ko. Hematology Division, Department of Internal Medicine, National Taiwan University Hospital
 Bor-Sheng Ko Hematology Division, Department of Internal Medicine, National Taiwan University Hospital On behalf of Members of Aplastic Anemia Consensus Meeting Diagnosis and classification: Treatment
Bor-Sheng Ko Hematology Division, Department of Internal Medicine, National Taiwan University Hospital On behalf of Members of Aplastic Anemia Consensus Meeting Diagnosis and classification: Treatment
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Constitutional Aplastic Anemias. Uma Kundu, M.D. July 17, 2006
 Constitutional Aplastic Anemias Uma Kundu, M.D. July 17, 2006 Overview Erythroid lineage only (pure red cell aplasia) Two cell lines (bicytopenia) All hematopoietic cells (aplastic anemia) Aplastic anemias
Constitutional Aplastic Anemias Uma Kundu, M.D. July 17, 2006 Overview Erythroid lineage only (pure red cell aplasia) Two cell lines (bicytopenia) All hematopoietic cells (aplastic anemia) Aplastic anemias
Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled. in EWOG-MDS Studies
 Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled in EWOG-MDS Studies EWOG-MDS Consensus Conference Freiburg, October 25/26, 2016 These guidelines
Guidelines for Hematopoietic Stem Cell Transplantation (HSCT) in Childhood MDS and JMML for Patients enrolled in EWOG-MDS Studies EWOG-MDS Consensus Conference Freiburg, October 25/26, 2016 These guidelines
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
INTRODUCTION TO CYTOGENETICS AND MOLECULAR TESTING IN MDS
 INTRODUCTION TO CYTOGENETICS AND MOLECULAR TESTING IN MDS Saturday, September 29, 2018 Cyrus C. Hsia, HBSc, MD, FRCPC Associate Professor of Medicine, Schulich School of Medicine and Dentistry, Western
INTRODUCTION TO CYTOGENETICS AND MOLECULAR TESTING IN MDS Saturday, September 29, 2018 Cyrus C. Hsia, HBSc, MD, FRCPC Associate Professor of Medicine, Schulich School of Medicine and Dentistry, Western
UKGTN Testing Criteria
 UKGTN Testing Criteria Test name: Inherited Bone Marrow Failure Syndromes 44 Gene Panel Approved name disorder/(s): See Appendix 1 Approved name (s): See Appendix 1 (s): (s): Patient name: Patient postcode:
UKGTN Testing Criteria Test name: Inherited Bone Marrow Failure Syndromes 44 Gene Panel Approved name disorder/(s): See Appendix 1 Approved name (s): See Appendix 1 (s): (s): Patient name: Patient postcode:
Cynthia Fata, MD, MSPH 6/23/15
 Cynthia Fata, MD, MSPH 6/23/15 Clinical case presentation Introduction to thrombopoietin Development of thrombopoietic agents Clinical Indications Eltrombopag use in aplastic anemia Future uses 33 yo F
Cynthia Fata, MD, MSPH 6/23/15 Clinical case presentation Introduction to thrombopoietin Development of thrombopoietic agents Clinical Indications Eltrombopag use in aplastic anemia Future uses 33 yo F
Study of diagnostic features of bone marrow in aplastic anaemia
 Original article: Study of diagnostic features of bone marrow in aplastic anaemia 1Dr. Poonam Nanwani, 2 Dr. Sativan Khatri* 1MD Pathologist, Assistant Professor, Department of Pathology, M.G.M. Medical
Original article: Study of diagnostic features of bone marrow in aplastic anaemia 1Dr. Poonam Nanwani, 2 Dr. Sativan Khatri* 1MD Pathologist, Assistant Professor, Department of Pathology, M.G.M. Medical
CASE SERIES Juvenile myelomonocytic leukaemia: a case series
 Malaysian J Pathol 2009; 31(2) : 121 128 CASE SERIES Juvenile myelomonocytic leukaemia: a case series RZ Azma MBBS, MPath., AL Zarina* MBBS, MMed., A Hamidah* MD, MMed., R Jamal* MRCPI, PhD, NA Sharifah
Malaysian J Pathol 2009; 31(2) : 121 128 CASE SERIES Juvenile myelomonocytic leukaemia: a case series RZ Azma MBBS, MPath., AL Zarina* MBBS, MMed., A Hamidah* MD, MMed., R Jamal* MRCPI, PhD, NA Sharifah
Treatment of low risk MDS
 Treatment of low risk MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu International Prognostic Scoring
Treatment of low risk MDS Matteo G Della Porta Cancer Center IRCCS Humanitas Research Hospital & Humanitas University Rozzano Milano, Italy matteo.della_porta@hunimed.eu International Prognostic Scoring
CHALLENGING CASES PRESENTATION
 CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
YEREVAN STATE MEDICAL UNIVERSITY DEPARTMENT OF HEMATOLOGY COURSE DESCRIPTION HEMATOLOGY
 1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
Therapeutic Advances in Treatment of Aplastic Anemia. Seiji Kojima MD. PhD.
 Therapeutic Advances in Treatment of Aplastic Anemia Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific
Therapeutic Advances in Treatment of Aplastic Anemia Seiji Kojima MD. PhD. Department of Pediatrics Nagoya University Graduate School of Medicine Chairman of the Severe Aplastic Anemia Working Party Asia-Pacific
BONE MARROW EXAMINATION FINDINGS OF A SINGLE CENTRE- AN ORIGINAL ARTICLE.
 BONE MARROW EXAMINATION FINDINGS OF A SINGLE CENTRE- AN ORIGINAL ARTICLE. ISHRAT JAHAN SHIMU¹, M. MEHFUZ-E- KHODA², M. A. SATTAR SARKER 3, FATEMA AHMED 4, PALASH MITRA 5, FAKHRUDDIN BHUIYAN 6, ALAMGIR
BONE MARROW EXAMINATION FINDINGS OF A SINGLE CENTRE- AN ORIGINAL ARTICLE. ISHRAT JAHAN SHIMU¹, M. MEHFUZ-E- KHODA², M. A. SATTAR SARKER 3, FATEMA AHMED 4, PALASH MITRA 5, FAKHRUDDIN BHUIYAN 6, ALAMGIR
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
MUD HSCT as first line Treatment in Idiopathic SAA. Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK
 MUD HSCT as first line Treatment in Idiopathic SAA Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK No Financial Disclosures Guidelines for management of aplastic anaemia British
MUD HSCT as first line Treatment in Idiopathic SAA Dr Sujith Samarasinghe Great Ormond Street Hospital for Children, London, UK No Financial Disclosures Guidelines for management of aplastic anaemia British
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression
 Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic syndromes
 Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
When Cancer Looks Like Something Else: How Does Mutational Profiling Inform the Diagnosis of Myelodysplasia?
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Evaluation of bone marrow aspirate in paediatric patients with pancytopenia: a 2 years study
 International Journal of Research in Medical Sciences Baig MA. Int J Res Med Sci. 2015 Oct;3(10):2775-2779 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150830
International Journal of Research in Medical Sciences Baig MA. Int J Res Med Sci. 2015 Oct;3(10):2775-2779 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150830
Advances in genetic studies of inherited bone marrow failure syndromes and their associated malignancies
 Review Article Advances in genetic studies of inherited bone marrow failure syndromes and their associated malignancies Qi-Hong Yu 1, Shu-Ye Wang 2, Zhanhe Wu 3 1 Department of Gastroenterology, Chang
Review Article Advances in genetic studies of inherited bone marrow failure syndromes and their associated malignancies Qi-Hong Yu 1, Shu-Ye Wang 2, Zhanhe Wu 3 1 Department of Gastroenterology, Chang
Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment
 7/23/212 Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment Danielle Townsley, MD, MSc Hematology Branch National, Heart, Lung and Blood Institute National Institutes
7/23/212 Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment Danielle Townsley, MD, MSc Hematology Branch National, Heart, Lung and Blood Institute National Institutes
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment
 4/18/212 Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment Bogdan Dumitriu, MD Hematology Branch National, Heart, Lung and Blood Institute National Institutes of Health
4/18/212 Aplastic Anemia: Current Thinking on Disease, Diagnosis and Non- Transplant Treatment Bogdan Dumitriu, MD Hematology Branch National, Heart, Lung and Blood Institute National Institutes of Health
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Policy Specific Section:
 Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand
 Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand This list provides indications for the majority of adult BMTs that are performed in New Zealand. A small number of BMTs
Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand This list provides indications for the majority of adult BMTs that are performed in New Zealand. A small number of BMTs
NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION
 ORIGINAL ARTICLES NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION Ilina Micheva 1, Rosen Rachev 1, Hinco Varbanov 1, Vladimir
ORIGINAL ARTICLES NOVEL APPROACHES IN THE CLASSIFICATION AND RISK ASSESSMENT OF PATIENTS WITH MYELODYSPLASTIC SYNDROMES-CLINICAL IMPLICATION Ilina Micheva 1, Rosen Rachev 1, Hinco Varbanov 1, Vladimir
Extramedullary precursor T-lymphoblastic transformation of CML at presentation
 Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
CME/SAM. Mixed Phenotype Acute Leukemia
 AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
Improved prognosis for acquired aplastic anaemia
 158 Department of Haematology and Oncology, Great Ormond Street Hospital for Children NHS Trust, London WC1N 3JH, UK L A Pitcher I M Hann JPMEvans P Veys J M Chessells DKHWebb Correspondence to: Dr Webb.
158 Department of Haematology and Oncology, Great Ormond Street Hospital for Children NHS Trust, London WC1N 3JH, UK L A Pitcher I M Hann JPMEvans P Veys J M Chessells DKHWebb Correspondence to: Dr Webb.
THE PATHOLOGY OF BONE MARROW FAILURE
 THE PATHOLOGY OF BONE MARROW FAILURE Roos Leguit, Jan G Van den Tweel To cite this version: Roos Leguit, Jan G Van den Tweel. THE PATHOLOGY OF BONE MARROW FAILURE. Histopathology, Wiley, 2010, 57 (5),
THE PATHOLOGY OF BONE MARROW FAILURE Roos Leguit, Jan G Van den Tweel To cite this version: Roos Leguit, Jan G Van den Tweel. THE PATHOLOGY OF BONE MARROW FAILURE. Histopathology, Wiley, 2010, 57 (5),
Myelodysplastic scoring system with flow cytometry. G Detry B Husson
 Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Guidelines for diagnosis and management of Adult Myelodysplastic Syndromes (MDS)
 Guidelines for diagnosis and management of Adult Myelodysplastic Syndromes (MDS) Author: Dr A Pillai, Consultant Haematologist On behalf of the Haematology CNG Re- Written: February 2011, Version 2 Revised:
Guidelines for diagnosis and management of Adult Myelodysplastic Syndromes (MDS) Author: Dr A Pillai, Consultant Haematologist On behalf of the Haematology CNG Re- Written: February 2011, Version 2 Revised:
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Late Complications Following Treatment for Severe Aplastic Anemia (SAA) with High-Dose Cyclophosphamide (Cy): Follow up of a Randomized Trial
 Blood First Edition Paper, prepublished online June 28, 2002; DOI 10.1182/blood-2002-02-0494 Late Complications Following Treatment for Severe Aplastic Anemia (SAA) with High-Dose Cyclophosphamide (Cy):
Blood First Edition Paper, prepublished online June 28, 2002; DOI 10.1182/blood-2002-02-0494 Late Complications Following Treatment for Severe Aplastic Anemia (SAA) with High-Dose Cyclophosphamide (Cy):
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
Leukaemia Section Review
 Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Leukaemia Section Review Classification of myelodysplasic syndromes Georges Flandrin Laboratoire d'hématologie,
Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Leukaemia Section Review Classification of myelodysplasic syndromes Georges Flandrin Laboratoire d'hématologie,
ACCME/Disclosures. History. Hematopathology Specialty Conference Case #4 4/13/2016
 Hematopathology Specialty Conference Case #4 Sherrie L. Perkins MD, PhD University of Utah ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose
Hematopathology Specialty Conference Case #4 Sherrie L. Perkins MD, PhD University of Utah ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose
Correspondence should be addressed to Anas Khanfar;
 Case Reports in Oncological Medicine, Article ID 949515, 4 pages http://dx.doi.org/10.1155/2014/949515 Case Report Durable Hematological and Major Cytogenetic Response in a Patient with Isolated 20q Deletion
Case Reports in Oncological Medicine, Article ID 949515, 4 pages http://dx.doi.org/10.1155/2014/949515 Case Report Durable Hematological and Major Cytogenetic Response in a Patient with Isolated 20q Deletion
