GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCER
|
|
|
- Naomi Skinner
- 6 years ago
- Views:
Transcription
1 GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCER Bladder Cancer Treatment Guidelines Authors: Mr P Cornford Mr N Parr Review Date: May 2014
2 CONTENTS Page 1. Introduction What the Guideline Covers Definition of Terms Background 5 2. Presentation/Referral Criteria Other Referral Route Guidelines 7 3. Initial assessment Table 1 Investigations for Patients with Haematuria 8 4. Assessment of Identified Bladder Tumours Transurethral resection of bladder tumours (TURBT) Histological Examination of Endoscopic Tissue Resection 9 of Bladder Tumour 4.3 Urethelial tumour classification Local agreed variations from RCPath Guidance Follows 9 5. Specialist and Local Multi-disciplinary team working Referral to SMDT MDT Documentation of Action Plans and Communication 11 with GP 5.3 MDT Co-ordinators MDT Specialist Urology Nurses Investigations, Staging and Treatment guidelines New non-muscle invasive tumours Recurrent non-muscle invasive Tumours Muscle-invasive Tumours Pathologies other than Transitional Carcinoma of the Bladder Curative Treatment Options Cystectomy Radiotherapy Chemotherapy Recurrent Muscle-Invasive Tumours Follow Up After Radical Treatment Invasive Bladder cancer treated by surgery Invasive Bladder cancer treated by radiotherapy 8. Patient and Carer Information Palliative Care Data Collection 24 References 25/27 Appendices 28/ Bladder Guidelines Review Date: June 2012 Page 2 of 44
3 Appendix 1 - SMDT contacts Appendix 2 - Referral Form Appendix 3 TNM Classification of Urinary Bladder Cancer (2002) Appendix 4 - Pelvic Specialist MDT Referral Proforma Appendix 5 - TCC Algorithm: New Non-muscle Invasive Tumours Appendix 6 TCC Algorithm: Recurrent Non-muscle Appendix 7 TCC Algorithm: Muscle Invasive Tumours Appendix 8 Recurrent Muscle- Invasive Tumours Appendix 9 - Radiology Guidelines 28 29/ /45 Bladder Guidelines Review Date: June 2012 Page 3 of 44
4 1. INTRODUCTION This document sets out the guidelines for the management of patients with bladder cancer within the Merseyside and Cheshire Cancer Network (MCCN). It will act as a summary guide for the management of patients based on the available published evidence and should be regarded as a template for best practice. Its scope is to aid all health practitioners involved in the patient from primary care and referral through treatment to follow up. However, as constant modifications are being made, these guidelines should only be used to give an indication of current management. They should not be used to treat patients without checking that changes have not been made. These guidelines have been endorsed by the Merseyside and Cheshire Cancer Network Urology Site Specific Group. They will be reviewed and updated on an annual basis or more frequently as required. These guidelines should be read in conjunction with: Improving Outcomes in Urological Cancer: the Manual, National Institute for Clinical Excellence, 2002 available at What the Guideline Covers This guideline is primarily concerned with patients with a diagnosis of transitional cell carcinoma (TCC) of the bladder. It will also deal with the less common bladder tumours such as adenocarcinoma and squamous cell carcinoma. Upper tract TCC either of the ureter or renal collecting system will also be covered. Aspects of the guidelines are designed to offer the best evidence based management plan to optimise the treatment for a patient s tumour. Clearly a patient s co-morbidity, life expectancy and previous medical history will be a factor that may alter the treatment options that an individual patient can be offered. As well as the clinical aspects of patient management this guideline also defines the requirements for efficient communication between primary, secondary and tertiary care and between all these and the patient and their carers. The guideline confirms that all newly diagnosed patients should be discussed at the local MDT and also defines which patients should be referred from the local to the specialist MDT, what information must be available at the time of the specialist MDT discussion and how communications at all levels will be achieved. One of the commonest presenting symptoms of bladder cancer is haematuria, however other urological and nephrological pathologies can present with this symptom and some patients will be best investigated by the nephrology team. Bladder Guidelines Review Date: June 2012 Page 4 of 44
5 1.2 Definition of Terms Carcinoma in situ of the bladder describes a wide range of clinical situations from a small red patch on an otherwise normal looking bladder with a cautiously good prognosis to wide spread changes within the bladder often associated with significant cystitis symptoms, so called malignant cystitis, with a poor prognosis. This diagnosis is invariably made by the histopathologist and various terms are used for this pathological appearance including ptis and CIS (carcinoma in situ). This guideline will regard these terms as equivalent but the prognosis and therefore management plan will depend on numerous other factors other than just the pathologist reporting the presence of carcinoma in situ. Many patients will undergo either a diagnostic or surveillance cystoscopy using a flexible cystoscope performed under a local anaesthetic. This procedure offers many advantages by avoiding a general anaesthetic. However some patients may be best managed with a cystoscopy performed under a general anaesthetic, either to allow an EUA or to allow immediate bladder biopsy or tumour resection. Although these guidelines will on occasions specify a flexible cystoscopy the clinician will decide for individual patients whether this is appropriate or whether a GA cystoscopy is preferred. Local multidisciplinary team meetings (MDT) take place in all 7 Acute Hospital Trusts in MCCN as they are all urology cancer units. Specialist MDTs are based at the Royal Liverpool and Broadgreen University Hospital NHS Trust and Wirral University Teaching Hospital NHS Foundation Trust. SMDT members are detailed in Appendix Background Transitional cell carcinoma of the bladder is the fourth commonest cancer in males and 6th commonest in females. In England and Wales 11,000 new cases are diagnosed each year. Within the Merseyside and Cheshire Cancer Network there are approximately 440 new cases per year. The majority of tumours (70%) are non-invasive but have a risk of recurrence. Approximately 25% of these non-invasive tumours have a high risk of progression to invasive disease. Patients with superficial disease require surveillance to detect recurrence and treatment strategies to reduce recurrence rates. The overall 5 year survival for patients with muscle-invasive disease is 30% and these patients require radical treatment. Bladder Guidelines Review Date: June 2012 Page 5 of 44
6 2. PRESENTATION/REFERRAL CRITERIA Most patients will present with visible painless haematuria or microscopic haematuria and should be referred to the local urology department haematuria clinic under the rapid referral 2 week rule. The fast track referral form that has been approved by the PCTs is the preferred method of referral (see Appendix 2). Patients should be investigated in primary care to exclude an obvious cause such as Urinary Tract Infection (UTI), menses, dietary etc. Once re-tested if haematuria persists, patients should be referred as fast track cases. Patients can be risk stratified according to other factors such as symptomatic lower urinary tract symptoms, smoking history and age. Patients classified as high risk for bladder cancer include: o Visible haematuria o >45yrs with microscopic haematuria o Microscopic haematuria in the presence of risk factors; smokers, industrial chemical exposure, irritative voiding symptoms. Patients < 45yrs in the absence of risk factors are considered low risk and do not require urgent fast track referral. Hospital Fax number for urgent referral Southport and Ormskirk Aintree Royal Liverpool Whiston North Cheshire Countess of Chester Wirral Arrangements are in place for patients to be contacted and offered the earliest date available to be seen in the fast track clinics and are then sent a letter confirming the appointment date and time. The haematuria clinic investigates patients with microscopic or macroscopic haematuria to exclude urological disease. Haematuria can be broadly classified as nephrological or urological in origin. Urological causes include tumours (transitional cell carcinoma, renal carcinoma and prostate cancer), urinary tract infection, stone disease and bleeding from benign prostate conditions. Less common causes include, urethral caruncle, meatal ulcers, trauma, loin pain haematuria syndrome, familial telangiectasia, arteriovenous malformation, endometriosis, and factitious (added blood). Microscopic haematuria may be detected in the absence of any underlying pathology, e.g. after vigorous exercise. In some patients there will be no identifiable problem, in these instances patients will be reassured that a significant or sinister lesion has been excluded. If macroscopic haematuria persists or if patients with haematuria develop progressive symptoms they may require reinvestigation. Bladder Guidelines Review Date: June 2012 Page 6 of 44
7 Patients with haematuria may have an underlying nephrological disease and should be referred to the nephrology unit after appropriate urological investigation. Any glomerular disease may result in haematuria. Active glomerular nephritis and acute interstitial nephritis are associated with large numbers of usually dysmorphic RBCs and RBC casts. Nephrotic syndrome and progressive glomerular nephritis typically have fewer erythrocytes on microscopy. Other causes to consider are IgA nephritis, thin membrane disease and hereditary nephritis or Alport s disease. These cases include patients with: haematuria and proteinuria elevated creatinine elevated age related blood pressure. 2.1 Other Referral Route Guidelines Most patients will present to the GP or to other disciplines with haematuria. These patients should be referred urgently to the local urology department. If a bladder tumour is detected incidentally following other investigations or gynaecological procedures or the patient presents to another speciality such as colorectal surgery or care of the elderly, the urologist should list that patient urgently for discussion at the next local MDT, and arrange to see them urgently at the next available clinic appointment. 3. INITIAL ASSESSMENT Investigations for initial assessment are outlined in Table 1 Bladder Guidelines Review Date: June 2012 Page 7 of 44
8 3.1 Investigations for Patients Presenting with Haematuria Table 1 Patients at risk of bacterial endocarditis should be given antibiotic prophylaxis as per local guidelines. Patients with heart valve replacements to be given antibiotics by nurse practitioner following local policies and procedures Direct referral to clinic via GP with either macroscopic or microscopic haematuria. The GP should include the following tests with the referral Hb, U&Es, BP, MSU Ultrasound/CT Scan/IVU flexible cystoscopy urine cytology. MSSU. Bloods for FBC. U&Es No abnormalities seen in lower tract. Ultrasound normal. No LUTS. Appearance of prostate normal. Bleeding from prostate (benign) No abnormalities seen in bladder or on ultrasound. Prostate enlarged. Raised PSA Suspicious area suggestive of bladder tumour observed. Ultrasound/CT scan suggestive of ureteric cacull, ureteric stricture, or hydronephrosis Proteinuria 1 creatinine raised BP (beyond age related centiles Difficulty Inserting scope. Poor view. Unusual Appearance of lower urinary tract Consider 5 alpha reductase inhibiter Refer for TRUSP See prostate cancer guidelines Direct entry to theatre list patient given date Arrange CT if not done Nephrology referral Refer to proximal supervisor Refer to Nurse Practitioner for counselling and information Refer to stone team Letter to GP Bladder Guidelines Review Date: June 2012 Page 8 of 44
9 4. ASSESSMENT OF IDENTIFIED BLADDER TUMOURS 4.1 Transurethral resection of bladder tumours (TURBT) If tumour looks solid at initial flexible cystoscopy arrange MRI prior to TURBT. TURBT can be carried out under a general or regional anaesthetic although the procedure is helped if the patient is paralysed to aid full examination of the bladder and the EUA at the end of the procedure. The number and size of the bladder tumours are recorded as part of the operation note. After resection the result of the EUA is also recorded. The surgeon should resect the exophytic tumour and separate biopsies of the base of the tumour to assess for invasion into the lamina propria and muscularis propria should be taken. If the tumour is too large to be completely excised care should be taken to ensure muscle is included in the specimen to confirm muscle invasion Post-operatively, patients with superficial bladder tumours should receive intravesical mitomycin within 24 hours of the surgery. This is contraindicated if the bladder wall has been perforated. For patients with a muscle invasive bladder cancer who are thought to be best suited for radical radiotherapy, the surgeon should resect as much of the exophytic tumour as possible to de-bulk the tumour and improve the effectiveness of radiotherapy. Random biopsies of otherwise normal parts of the bladder, in particular at the bladder neck should be sent separately for histological examination to assess for carcinoma in situ in patients who are thought may be suitable for radical surgery with neobladder reconstruction. 4.2 Histological Examination of Endoscopic Tissue Resection of Bladder Tumour Pathology specimens should be handled and reported in accordance with the latest version of the Dataset for tumours of the urinary collecting system, published by the Royal College of Pathologists (current version January 2007). Standards and datasets for the reporting of bladder cancer can be found at Urothelial tumour classification The TNM classification of urinary bladder cancer (2002) can be found in Appendix Locally-agreed variations from the RCPath Guidance Follows: TURBT specimen sampling Uropathologists in Merseyside and Cheshire have agreed that TURBT specimens should be sampled according to the following protocol rather than as suggested by the RCPath dataset: Bladder tumour chippings should be weighed, and specimens weighing 12g or less should be embedded in their entirety. Larger specimens should have a further one blocked sampled for every further 5g of tissue over 12g. Page 9 of 44
10 Sampling should concentrate on larger, solid chippings. Further tissue should be examined if this initial sampling does not include muscularis propria, especially if lamina propria invasion has been demonstrated. Base of tumour specimens and random biopsies will be examined separately. Cystectomy specimens It is very helpful to the reporting pathologist if the surgeon marks the cut ends of the ureters at the time of surgery, as retraction following fixation makes them difficult to identify in the laboratory. Cases requiring SMDT pathology review Cases for pathology review should be sent directly to one of the relevant SMDT pathologists. The original slides should be submitted, with a copy of the original report. Any relevant previous slides and reports should also be sent. Receipt of the cases should be confirmed by or fax-back. (Paraffin blocks should not be sent unless specifically requested by the SMDT pathologist.) The reviewing pathologist should issue a pathology report and send copies both to the lead uropathologist at the referring hospital and to the chair of the relevant SMDT. 5. SPECIALIST AND LOCAL MULTI-DISCIPLINARY TEAM WORKING The Royal Liverpool's specialist multidisciplinary team (SMDT) provides the IOG defined service for bladder cancer cases from the local MDTs for the Northern part of the Merseyside and Cheshire Cancer Network. Local MDTs are at Aintree University Hospital NHS Foundation Trust, Southport and Ormskirk Hospital NHS Trust and St Helen s and Knowsley NHS Trust. The Wirral Hospital s SMDT provides a mirror service for the southern part of the network linked to local MDTs at Warrington and Halton Hospitals NHS Foundation Trust and Countess of Chester Hospital NHS Foundation Trust. The majority of bladder cancer patients discussed in the local MDTs are identified from the pathology reports identified by the local MDT coordinator working closely with the pathology department. It is the responsibility of the clinician to inform the MDT coordinator if a patient with TCC is identified from a non routine referral route. After each local MDT it is the responsibility of the MDT coordinator to inform the SMDT coordinator of which patients need to be discussed at the SMDT and arrange for the completed form to be transferred for the SMDT meeting. Page 10 of 44
11 5.1 Referral to the SMDT 1. It is the responsibility of the local MDT co-ordinators to establish the video link and ensure the IT suite is functional throughout the meeting. 2. Cases should be referred no later than 2.00pm on Wednesday for the following Friday SMDT. 3. Referral should be made to the SMDT co-ordinator by on a SMDTproforma (Appendix 4). 4. Referral should include: Patient details, diagnosis, stage and grade, brief clinical summary and reason for referral. 5. Patient x-ray file should be sent and loaded onto PACS by the MDT coordinator prior to the meeting 6. Path slides can be sent with referral to SMDT if a second opinion is necessary. 5.2 MDT Documentation of Action Plans and Communication with GP Patients should be referred using the SMDT proforma (Appendix 4). Patient details and clinical history will be listed with the date of meeting and the reason for discussion. The MDT coordinator is responsible for generating and distributing the MDT list to core and extended team members. Each listed case will be discussed by the SMDT. The Chair will ensure that an action plan is formulated by consensus agreement and that the action plan is recorded at the meeting. It is the responsibility of the SMDT coordinator to transcribe the action plan to the electronic format and for this to be reviewed by the Chair. The completed proforma will be distributed by the MDT coordinator within 1 working day to the following: Electronic copy to core and extended team members Faxed copy to GP Copy by way of referral to other teams to be placed in the case notes Referring clinician In some complex cases the chairman may also dictate a letter to the referring consultant with a copy to the GP and other relevant clinicians summarising the recommended treatment options. The MDT action plan will include the name of the key worker who will be a core member of the MDT. If it is intended that the SMDT provides treatment, patients will be contacted by the local CNS to inform them that their case has been discussed and that they will be seen the following week by the appropriate member of the core team. Patients with muscle invasive bladder cancer will be seen by the Surgeon, Oncologist and Clinical Nurse Specialist from the SMDT in appropriate clinics in order to discuss treatment options and receive counselling. Where possible, patients will be seen in a joint clinic. Patients who are referred back to the local MDT for further management will be contacted by the local MDT clinical key worker to inform them of the outcome and arrangements will be made for them to be seen the following week by an appropriate core member of the local MDT. The MDT action plan, relevant case files and imaging files will be prepared by the relevant local MDT team and forwarded to the clinic. This process will be co-ordinated centrally by the Specialist Nurses. See also Patient and Carer Information 7.3. Page 11 of 44
12 After the SMDT, the MDT coordinators liaise with the clinical nurse specialist (CNS) to ensure all clinical plans are carried out. Details of available trials that have been considered will also be included. Where appropriate the patient is contacted by the CNS to arrange an outpatient clinic appointment. 5.3 The MDT Co-ordinators are:- Hospital MDT Coordinator Whiston Gill Phone Number Cauldwell Aintree Claire Phillips Southport Heather Steele Royal Liverpool Claire Richards Warrington Dawn Ingham Countess of Chester Karen Beckett Wirral Graeme Totty ext The Specialist Urology Nurses are:- Hospital Clinical Nurse Specialist Phone Number (CNS) Whiston Nerys Williams Nancy Chisholm Eleri Philips Jackie Williams Aintree Claire Parker Michelle Thomas Southport Sheila Coughlan Ann Wearing Royal Liverpool Clare Teaney Salihu Samas Warrington Mo Field Jackie Thompson Countess of Chester Karen Hopkins Wirral Beverley Rogers Gill Riley INVESTIGATIONS, STAGING AND TREATMENT GUIDELINES Classification and treatment for patients with bladder cancer definitions S = standard G = guideline These guidelines must be read in conjunction with the EAU guidelines 2008 National Library of Guidelines Specialist Library This document assumes that all cases where histology is obtained are discussed initially in the local MDT, if only to agree that they proceed as per this protocol. IOG defined cases are referred to the SMDT. Page 12 of 44
13 For patients referred from the local MDT to the SMDT, the following information is required:- Muscle invasive TCC bladder Staging results from the pelvic MR and abdominal/chest CT scan with radiology review where required Histology report with pathology review where required Assessment regarding fitness for radical treatment including Co-morbidity, Life expectancy Bladder symptoms, bladder pathology eg diverticulum, hydronephrosis Hip replacements Renal function Bone biochemistry Radiology Guidelines Please refer to the Royal College of Radiologists guidelines attached Imaging of Cancer Patients Network approved imaging protocols are detailed in Appendix Treatment of new non-muscle invasive tumours see Figure 2/Appendix 5 At the first resection, as the histology is not available, those patients with clinically superficial bladder tumours receive intravesical MMC following resection. ptag1 or ptag2 see Figure 3 Single dose of intravesical chemotherapy at initial resection(s) [1,2] MDT (S) Cystoscopy at three months (S) At 3 month cystoscopy, assign to a recurrence risk group (S), as follows. Initial Resection 3 month Cystoscopy Recurrence risk group Solitary tumour and clear low risk of recurrence Solitary tumour and recurrence medium risk of recurrence or Multifocal tumour and clear medium risk of recurrence Multifocal tumour and recurrence high risk of recurrence Page 13 of 44
14 6.1 Page 14 of 44
15 6.1 Page 15 of 44
16 pt1g1 Rare to be discussed at SMDT pt1g2 - see Figure 4 Review of pathology by local MDT lead uropathologist with an option for review by SMDT if required(s) 2nd look TURBT may be indicated (G) [4] If substantiated, a course of 6 weekly treatments of intravesical chemotherapy (S) 1st post-chemo cystoscopy under anaesthesia, then 3 monthly flexis for two years, then six monthly for two years, then annually for life (S) ptag3 [5] or pt1g3 see Figure 5 Review of pathology by local MDT lead uropathologist with an option for review by SMDT if required(s) 2nd look TURBT (G) Consider BCG on cystectomy (S), recommend BCG [6], as below (G) An induction course of six weekly doses of BCG, with GA cystoscopy and biopsy after 1st course [7] as per local protocol If 2nd look worse than pt1g3, treat radically (S) ptis Review of pathology by local MDT lead uropathologist with an option for review by SMDT if required(s) Consider BCG and cystectomy (S), recommend BCG (G) Induction and maintenance BCG and FU as per ptag3 (S) [9] Page 16 of 44
17 6.1 Page 17 of 44
18 6.1 Page 18 of 44
19 6.2 Recurrent Non-muscle Invasive Tumours see Appendix 6 Initial ptag1 or ptag2 Disease For single recurrence resect/biopsy & diathermy single post operative dose of intravesical chemo, and flexi in three months Large or multifocal or high recurrent intravesical chemo, six week course then flexi at three months. Consider BCG if failed chemotherapy. If failed BCG consider radical therapy For Other Patients Treated with BCG (ptag3, pt1g2/3 or Cis) If recurrence, recommend radical treatment [10] 6.3 Muscle-invasive Tumours see Appendix 7 If a new tumour looks solid at initial flexible cystoscopy, arrange urgent MRI before TURBT (G) [11] if suitable for radiotherapy, some patients for cystectomy may only require deep loop biopsy before surgery. TUR biopsy of prostatic urethra (men) or bladder neck (women) (S) Document bimanual examination of clinical stage Review of pathology by local MDT lead uropathologist with an option for review by SMDT if required (S) Consider 2nd look TURBT (S): o Debulking, if RT likely (G) o Biopsy prostatic urethra (men)/bladder neck (women) if not done beforehand (G) MRI pelvis & CT scan abdomen, if not done already (S) Chest X-ray, alkaline phosphatase (bone scan if elevated alkaline phosphatase or otherwise indicated) (S) Discuss cases at SMDT Consider cystectomy or radical radiotherapy (S) [12, 13] High risk disease (vascular invasion, pn+, positive margins) MDT (S) Consider neo-adjuvant chemotherapy (S) The choice of primary treatment for muscle invasive bladder cancer should be taken after the patient has been fully counselled on short and long term risks of both surgery and radiotherapy. Performance status, co-morbidity and tumour stage may all affect treatment choice. 6.4 Pathologies other than Transitional Carcinoma of the Bladder:- Squamous cell carcinoma of the bladder This is staged and managed in the same way as TCC bladder but radiotherapy is ineffective and therefore the treatment of choice is radical cystectomy. Adenocarcinoma of the bladder This is staged and managed in the same way as TCC bladder but radiotherapy is ineffective and therefore the treatment of choice is surgical excision. If the tumour is within a urachal remnant surgical options include partial cystectomy with the en bloc removal of the urachal remnant and the umbilicus. Page 19 of 44
20 Transitional cell carcinoma of the ureter or renal collecting system. This type of tumour is often diagnosed by a combination of urine cytology, a normal cystoscopy and an abnormality identified on upper track imaging. Staging is by CT scanning. Radiotherapy is largely ineffective in the curative treatment of this type of tumour and therefore surgical excision, usually nephro-ureterectomy is the treatment of choice. Consider the POUT trial (Peri-Operative chemotherapy versus surveillance in completely resected upper Tract TCC). Sarcoma of the bladder. This is staged in the same way as TCC bladder. Where possible the only curative treatment option is surgical excision. Transitional cell carcinoma of the urethra. In the female this is staged as for TCC bladder but curative treatment is invariably by surgical excision. In male patients this is more commonly associated with TCC bladder and is staged as for TCC bladder. Surgery is invariably the only curative treatment option. 6.5 Curative Treatment Options 6.51 Cystectomy Discuss the following (S): Neo-adjuvant chemotherapy Role of lymphadenectomy [15] Nerve sparing in young males [16] Diversion/reconstruction options (all that are possible for the patient in question) [17]: o Conduit [18,19] o Bladder substitute [20, 21] o Catheterisable reservoir [22, 23] Hospital course Peri-operative mortality and complications (early & late, specific & general) [25-27] Need for life-long oncological and functional follow-up [28-30] Meeting with Nurse Specialist to discuss peri-operative course and issues around diversion/reconstruction (S) Offer meeting with patient who has had intended diversion/reconstruction (S) Check PSA, B12 & folate (S) Check GFR (G) Page 20 of 44
21 6.52 Radiotherapy Radical RT Fit patients(ps 0-1) with muscle invasive disease ideally those with no ureteric obstruction with small tumours away from trigone Younger fitter patients with limited lymphadenopathy (but no metastases) can be offered radical radiotherapy if good response to neoadjuvant chemotherapy Preference over radical surgery: Concomitant disease increasing the risks of surgery eg cardiovascular disease Inability to manage a stoma Discuss the following with the patient (S): Lack of evidence to favour RT over cystectomy. Level of current LUTS Treatment course Complications (early & late ) Need for life-long follow-up with check cystoscopy Planning CT planning 64 Gy in one phase in 32 fractions over 6.5 weeks. They are category 1 patients so require treatment twice a day (with 6hr gap) prior to long weekend breaks or service days Alternative fractionations include: o 55 Gy in 20 fractions o in relatively frail patients 30 Gy in 6 fractions over 6 weeks (1 x week ) Palliative RT Palliative radiotherapy is to control symptoms, particularly pelvic pain (not cystitis) and haematuria in the following circumstances: Frail patients Metastatic disease Fractionation used is at the discretion of the clinical oncologist: o 30 Gy in 6 fractions over 2 weeks o 8 Gy single fraction 6.53 Chemotherapy Neo adjuvant Gem / CIS (Gemcitabine and Cisplatin) or Gem/Carbo (Gemcitibine and Carboplatin) now current choice for network for patients PS 0-1 with normal renal function Concurrent Cisplatin (40mg/m 2 ) weekly if patient PS 0-1 with normal renal Function For mild renal impairment consider Carboplatin Palliative chemotherapy in young patients may be considered 6.54 Recurrent Muscle-Invasive Tumours (Appendix 8) Page 21 of 44
22 7. FOLLOW UP AFTER RADICAL TREATMENT 7.1 Invasive Bladder Cancer Treated by Surgery Cystectomy, ileal conduit or neobladder Patients will be reviewed at the cancer centre initially extending to shared care between the cancer centre and the referring local MDT. A six week post surgery visit will be arranged to exclude complications of surgery, assess recovery and inform patients of outcome and diagnosis. (S) Patients will have a physical examination including an assessment of the ileal conduit or diversion, serum haemoglobin and creatinine will be performed as well as acid base estimation in patients with bladder reconstruction.(s) For all patients either a conduitogram or an CTU should be arranged at six weeks. (S) All cystectomy patients should be seen 3 monthly in the first 2 years, then 6 monthly alternating after the first year with the local MDT as requested.(g) Patients should be seen by a specialist nurse practitioner in stoma and reconstruction. (G) 7.2 Invasive Bladder Cancer Treated by Radiotherapy 6 weeks Oncology review (S) 1st post-rt cystoscopy(ga) at 3 months (S) If clear, CT and flexible cystoscopy at 6 months (G) If clear at 6 months, flexible cystoscopy three monthly for 18 months, with CT at 1 year post RT (G) If clear, flexible cystoscopy six monthly for 4 years, then annually for life (G) If residual/recurrent tumour, restage with a low threshold for salvage cystectomy especially for high grade tumour & MDT (S) If CT shows nodes, then consider chemotherapy/palliative radiotherapy & MDT (S) 8. PATIENT AND CARER INFORMATION Patients will be contacted by the local MDT key worker to inform them that their case has been discussed at the SMDT and that they will be seen the following week by the appropriate member of the core team. This process will be co-ordinated centrally by the Specialist Nurses. The Uro-Oncology team will discuss the diagnosis, MDT action plan and care pathway with patients and carers. Patients/carers will receive relevant written information about their diagnosis and treatment plan. Patients with visual and hearing impairment will be offered aids to understand the patient information. Interpreter services are available for patients via the patient advisory liaison office. Patients will be asked if they wish to receive a copy of the permanent consultation record which outlines the information that they have been given. It includes the diagnosis and the treatment plan agreed by the patient at the meeting with the urologist. Patients should be seen by a specialist nurse practitioner in stoma and reconstruction as appropriate. Many aspects of palliative care are also applicable earlier in the course of the illness in conjunction with anti-cancer or other treatment.(please refer to the Palliative Care section) Page 22 of 44
23 All patients will be offered clear and comprehensive information in a format which is suitable to their needs and stage of treatment in the cancer journey, this should include: Nature of the disease Diagnostic procedures being undertaken Treatment options available Likely outcomes of treatment in terms of benefits, risks and side effects Management of side effects of treatment, and who would be most appropriate to contact for advice Details of future appointments/contacts Contact details of clinical nurse specialist/key worker for urological cancers Contact details of clinical nurse specialist for other individual issues (stoma care/continence advice/sexual issues/body image issues) as appropriate Cancer information services such as Cancer BACKUP Where appropriate patients should receive a copy of any medical/clinical communications e.g. from surgeon/gp Details of MDT The role and responsibilities of their CNS Hard copies of the information, available within the Merseyside and Cheshire Cancer Network for patients with urological cancer and their carers, can be obtained from the clinical nurse. This information will meet agreed MCCN / National Patient Information Guidelines, as per mapping Access will be made available for all patients/carers to a named nurse whose specialist knowledge is in urological cancers As the concept of the information prescription is introduced, urology patients will be included in the process. Patient satisfaction surveys will be carried out annually and results acted upon. 9. PALLIATIVE CARE Palliative Care is defined by the World Health Organisation (WHO 2002) as:...the active holistic care of patients with advanced progressive illness. Management of pain and other symptoms and provision of psychological, social and spiritual support is paramount. The goal of palliative care is achievement of the best quality of life for patients and their families. Many aspects of palliative care are also applicable earlier in the course of the illness in conjunction with other treatments Many patients with advanced incurable bladder cancer will not require referral to specialist palliative care, but will find that their supportive care can be managed by their GP and district nursing team. Patients felt to be in the last 6 12 months of life should be included on the GP practice s Supportive Care Register (also known as a GSF register). This will ensure that the needs of both the patient and their carers are regularly assessed and will promote discussions about Advance Care Planning. An Holistic Needs Assessment should be undertaken to identify the patient s needs and ensure the care plan meets those needs. Page 23 of 44
24 Patients with the following problems may benefit from referral to specialist palliative care services: Pain or other symptoms which are difficult to control Complex psychological or spiritual issues Complex family dynamics including the presence of young children in need of support Advice required for complex placement issues Accessing Specialist Palliative Care Advice Specialist Palliative Care Advice is available in each locality from the community and hospital specialist teams, and also from the local Specialist Inpatient Unit. Many inpatient units are able to give 24 hour telephone advice to healthcare professionals. Useful resources For patients - Macmillan support line: For health care professionals Holistic Needs Assessment for people with cancer: DATA COLLECTION All newly presenting patients with a urological cancer are registered on BAUS. The minimum data set should be collected via the Somerset Cancer Register. A complex operation data set should be completed for patients who have had: Cystectomy Nephroureterectomy Page 24 of 44
25 References 1. Tolley DA, Parmar MK, Grigor KM, Lallemand G, Benyon LL, Fellows J, Freedman LS, Grigor KM, Hall RR, Hargreave TB, Munson K, Newling DW, Richards B, Robinson MR, Rose MB, Smith PH, Williams JL, Whelan P. The effect of intravesical mitomycin C on recurrence of newly diagnosed superficial bladder cancer: a further report with 7 years of follow up. J Urol Apr;155(4): Pawinski A, Sylvester R, Kurth KH, Bouffioux C, van der Meijden A, Parmar MK, Bijnens L. A combined analysis of European Organization for Research and Treatment of Cancer, and Medical Research Council randomized clinical trials for the prophylactic treatment of stage TaT1 bladder cancer. European Organization for Research and Treatment of Cancer Genitourinary Tract Cancer Co-operative Group and the Medical Research Council Working Party on Superficial Bladder Cancer. J Urol Dec; 156(6): Hall RR, Parmar MK, Richards AB, Smith PH. Proposal for changes in cystoscopic follow up of patients with bladder cancer and adjuvant intravesical chemotherapy. BMJ Jan 22;308(6923): Herr HW. The value of a second transurethral resection in evaluating patients with bladder tumors. J Urol Jul;162(1): Herr HW Tumor progression and survival of patients with high grade, noninvasive papillary (TaG3) bladder tumors: 15-year outcome. J Urol Jan;163(1): Sylvester RJ, van der Meijden AP, Lamm DL. Intravesical bacillus Calmette-Guerin reduces the risk of progression in patients with superficial bladder cancer: a meta-analysis of the published results of randomized clinical trials. J Urol Nov;168(5): Dalbagni G, Rechtschaffen T, Herr HW. Is transurethral biopsy of the bladder necessary after 3 months to evaluate response to bacillus Calmette-Guerin therapy? J Urol Sep;162(3 Pt 1): Lamm DL, Blumenstein BA, Crissman JD, Montie JE, Gottesman JE, Lowe BA, Sarosdy MF, Bohl RD, Grossman HB, Beck TM, Leimert JT, Crawford ED. Maintenance bacillus Calmette-Guerin immunotherapy for recurrent TA, T1 and carcinoma in situ transitional cell carcinoma of the bladder: a randomized Southwest Oncology Group Study. J Urol Apr;163(4): Griffiths TR, Charlton M, Neal DE, Powell PH. Treatment of carcinoma in situ with intravesical bacillus Calmette-Guerin without maintenance. J Urol Jun;167(6): Herr HW, Sogani PC. Does early cystectomy improve the survival of patients with high risk superficial bladder tumors? J Urol Oct;166(4): Kim B, Semelka RC, Ascher SM, et al. Bladder tumor staging: comparison of contrastenhanced CT, T1- and T2-weighted MR imaging, dynamic gadolinium-enhanced imaging, and late gadolinium-enhanced imaging. Radiology 1994;193: Stein J, Lieskovsky G, Cote R. Radical cystectomy in the treatment of invasive bladder cancer; long term results in 1,054 patients. J Clin Oncol 2001;19: Page 25 of 44
26 13. Bell C, Lydon A, Kernick V, et al. Contemporary results of radical radiotherapy for bladder transitional cell carcinoma in a district general hospital with cancer centre status. BJU Int 1999;83: Advanced Bladder Cancer Meta-analysis Collaboration. Neoadjuvant chemotherapy in invasive bladder cancer: a systematic review and metaanalysis. Lancet Jun 7;361(9373): Mills RD, Turner WH, Fleischmann A, Markwalder R, Thalmann GN, Studer UE. Pelvic lymph node metastases from bladder cancer: outcome in 83 patients after radical cystectomy and pelvic lymphadenectomy. J Urol Jul;166(1): Turner WH, Danuser H, Moehrle K, Studer UE. The effect of nerve sparing cystectomy technique on postoperative continence after orthotopic bladder substitution. J Urol Dec;158(6): Turner WH, Studer UE. Cystectomy and urinary diversion. Semin Surg Oncol Sep-Oct;13(5): Hautmann RE. Urinary diversion: ileal conduit to neobladder. J Urol Mar; 169(3): Madersbacher S, Schmidt J, Eberle JM, Thoeny HC, Burkhard F, Hochreiter W, Studer UE. Long-term outcome of ileal conduit diversion. J Urol Mar;169(3): Studer UE, Danuser H, Hochreiter W, Springer JP, Turner WH, Zingg EJ. Summary of 10 years' experience with an ileal low-pressure bladder substitute combined with an afferent tubular isoperistaltic segment. World J Urol. 1996;14(1): Mills RD, Studer UE. Female orthotopic bladder substitution: a good operation in the right circumstances. J Urol May;163(5): Mansson A, Davidsson T, Hunt S, Mansson W. The quality of life in men after radical cystectomy with a continent cutaneous diversion or orthotopic bladder substitution: is there a difference? BJU Int Sep;90(4): Mansson W. Continent urinary reconstruction--method-to-patient matching. J Urol Sep;156(3): el Mekresh MM, Hafez AT, Abol-Enein H, Ghoneim MA. Double folded rectosigmoid bladder with a new ureterocolic antireflux technique. J Urol Jun;157(6): Ghoneim MA, el-mekresh MM, el-baz MA, el-attar IA, Ashamallah A. Radical cystectomy for carcinoma of the bladder: critical evaluation of the results in 1,026 cases. J Urol Aug;158(2): Hautmann RE, de Petriconi R, Gottfried HW, Kleinschmidt K, Mattes R, Paiss T. The ileal neobladder: complications and functional results in 363 patients after 11 years of follow up. J Urol Feb;161(2): Soulie M, Straub M, Game X, Seguin P, De Petriconi R, Plante P, Hautmann RE. A multicenter study of the morbidity of radical cystectomy in select elderly patients with bladder cancer. J Urol Mar;167(3): Page 26 of 44
27 28. Madersbacher S, Hochreiter W, Burkhard F, Thalmann GN, Danuser H, Markwalder R, Studer UE. Radical cystectomy for bladder cancer today--a homogeneous series without neoadjuvant therapy. J Clin Oncol Feb 15;21(4): Mills RD, Studer UE. Metabolic consequences of continent urinary diversion. J Urol Apr;161(4): Gerharz EW, Turner WH, Kalble T, Woodhouse CR. Metabolic and functional consequences of urinary reconstruction with bowel. BJU Int Jan;91(2): Page 27 of 44
28 Appendix 1 - SMDT contacts RLUH Mr Philip A Cornford Dr Vijay Aachi Chair of SMDT Lead Histopathologist Phone: Phone: Fax: Fax: Philip.Cornford@rlbuht.nhs.uk Vijay.aachi@rlbuht.nhs.uk Dr Jane Belfield Mr Claire Richards Lead Imaging/Radiologist MDT Co-ordinator Phone: Phone: Jane.Belfield@rlbuht.nhs.uk Claire.Richards@rlbuht.nhs.uk Arrowe Park Mr Nigel Parr Dr Ranjula Seneviratne Chair of SMDT Lead Histopathologist Phone: ext 2233 (sec) Phone: ext 2563 (sec) Fax: 0151 Fax: Nigel.Parr@whnt.nhs.uk Hani.zakhour@whnt.nhs.uk Dr David Hughes Mr Graeme Totty Lead Imaging/Radiologist MDT Co-ordinator Phone: ext 8137 Phone: ext david.hughes@whnt.nhs.uk graeme.totty@whnt.nhs.uk Page 28 of 44
29 Urology Appendix 2 Referral Form SUSPECTED UROLOGICAL CANCER REFERRAL FORM Referring GP Registered GP GP Address & postcode GP Tel. No. GP Fax. No. Date seen by GP: To make an URGENT REFERRAL, Fax / to: Telephone Contact No.: REFERRER S DETAILS GP Code: Decision to refer date: PATIENT DETAILS Title & Surname Forename(s) D.O.B. AGE: Gender: Male Female Address Postcode *Tel. No. (day) Mobile Tel. *Tel. No. (evening) NHS No. Hospital No. * N.B. It is essential that you provide a current contact telephone number for the patient so that the Trust can contact the patient within 24-hours to arrange a convenient appointment. CULTURAL, MOBILITY, IMPAIRMENT ISSUES What is the patient s preferred first language?.. Does the patient require Translation or Interpretation Services? YES NO Please list any hearing or visual impairments requiring specialist help (Sign language, Braille, Loop Induction systems) Is Disabled Access Required? YES NO Is transport required? YES NO Ethnic Origin:.. Religion: Is the patient from overseas? YES NO Is the patient a temporary visitor? YES NO REFERRAL INFORMATION (referral guidelines are provided below / attached to proforma) PROSTATE Hard irregular prostate on DRE YES NO PSA Value..ng/ml symptoms (including symptoms of metastases) and raised PSA Raised age-related PSA Age related cut-off measurements: >3.0ng/ml; >4.0ng/ml; >5.0ng/ml. Elderly patients or those with significant co-morbidity do not require urgent referral for mildly elevated PSA in the absence of symptoms. Exclude urinary infection before PSA testing. YES NO YES NO Page 29 of 44
30 BLADDER & RENAL Painless visible haematuria (any age) YES NO Unexplained microscopic haematuria ( 50+ years) YES NO Haematuria associated with recurrent/persistent UTI (40+ years) YES NO Palpable renal mass or solid renal mass on U/S scan YES NO Attach copies of all completed investigations i.e. MSU, U&E s, U/S TESTICULAR Swelling or mass in the body of the testis. YES NO Attach Ultrasound Report, if completed. PENILE Ulceration/mass in the glans or prepuce. YES NO Any additional information Is the patient aware of the reason & urgency for referral & aware that they will be seen within 2 weeks? YES NO Referral Criteria: NICE Clinical Guideline 27 (issued June, 2005) Urgent referral = the patient is seen within the national target for urgent referrals = currently 2 weeks PROSTATE: Refer urgently patients: With a hard, irregular prostate typical of a prostate carcinoma. Prostate-specific antigen (PSA) should be measured and the result should accompany the referral. (An urgent referral is not needed if the prostate is simply enlarged and the PSA is in the age-specific reference range 1 - see below) With a normal prostate, but rising/raised age-specific PSA, with or without lower urinary tract symptoms. (In patients compromised by other co-morbidities, a discussion with the patient or carers and/or a specialist may be more appropriate.) With symptoms and high PSA levels. BLADDER & RENAL: Refer urgently patients: Of any age with painless macroscopic haematuria Aged 40 years and older who present with recurrent or persistent urinary tract infection associated with haematuria Aged 50 years and older who are found to have unexplained microscopic haematuria With an abdominal mass identified clinically or on imaging that is thought to arise from the urinary tract TESTICULAR: Refer urgently patients with a swelling or mass in the body of the testis. PENILE: Refer urgently patients with symptoms or signs of penile cancer. These include progressive ulceration or a mass in the glans or prepuce particularly, but can involve the skin of the penile shaft. (Lumps within the corpora cavernosa can indicate Peyronie s disease, which does not require urgent referral.) 1 The age specific cut-off PSA measurements recommended by the Prostate Cancer Risk Management Programme are as follows: Aged ng/ml Aged ng/ml Aged 70 and over 5.0 ng/ml. Note that there are no age-specific reference ranges for men over 80 years. Nearly all men of this age have at least a focus of cancer in the prostate. Prostate cancer only needs to be diagnosed in this age group if it is likely to need palliative treatment. Page 30 of 44
31 Non-urgent referral Refer non-urgently patients under 50 years of age with microscopic haematuria. Patients with proteinuria or raised serum creatinine should be referred to a renal physician. If there is no proteinuria and serum creatinine is normal, a non-urgent referral to an urologist should be made. Investigations In an asymptomatic male with a borderline level of PSA, repeat the PSA test after 1 to 3 months. If the PSA level is rising, refer the patient urgently. A digital rectal examination and a PSA test (after counselling) are recommended for patients with any of the following unexplained symptoms: o Inflammation or obstructive lower urinary tract symptoms o Erectile dysfunction o Haematuria o Lower back pain o Bone pain o Weight loss, especially in the elderly Exclude urinary infection before PSA testing. Postpone the PSA test for at least 1 month after treatment of a proven urinary tract infection. In male or female patients with symptoms suggestive of a urinary infection and macroscopic haematuria, diagnose and treat the infection before considering referral. If infection is not confirmed, refer them urgently. Consider an urgent ultrasound in men with a scrotal mass that does not transluminate and/or when the body of the testis cannot be distinguished. An algorithm 2 summarising the principal recommendations on how to proceed when a patient presents with the following symptoms. Page 31 of 44
32 2. National Institute for Health and Clinical Excellence: Referral guidelines for suspected cancer - Clinical Guideline 27 (issued June, 2005) Definitions Urgent : the patient is seen within the national target for urgent referrals (currently 2 weeks) Persistent as used in the recommendations in this guideline refers to the continuation of specified symptoms and/or signs beyond a period that would normally be associated with self-limiting problems. The precise period will vary depending on the severity of symptoms and associated features, as assessed by the healthcare professional. In many cases, the upper limit the professional will permit symptoms and/or signs to persist before initiating referral will be 4 6 weeks. Page 32 of 44
33 Unexplained as used in the recommendations in this guideline refers to a symptom(s) and/or sign(s) that has not led to a diagnosis being made by the primary care professional after initial assessment of the history, examination and primary care investigations (if any). An algorithm 2 summarising the principal recommendations on how to proceed when a patient presents with the following symptoms. 2. National Institute for Health and Clinical Excellence: Referral guidelines for suspected cancer - Clinical Guideline 27 (issued June, 2005) Page 33 of 44
34 Definitions Urgent : the patient is seen within the national target for urgent referrals (currently 2 weeks) Persistent as used in the recommendations in this guideline refers to the continuation of specified symptoms and/or signs beyond a period that would normally be associated with self-limiting problems. The precise period will vary depending on the severity of symptoms and associated features, as assessed by the healthcare professional. In many cases, the upper limit the professional will permit symptoms and/or signs to persist before initiating referral will be 4 6 weeks. Unexplained as used in the recommendations in this guideline refers to a symptom(s) and/or sign(s) that has not led to a diagnosis being made by the primary care professional after initial assessment of the history, examination and primary care investigations (if any). Page 34 of 44
35 Appendix 3 TNM Classification of Urinary Bladder Cancer (2002) Page 35 of 44
36 Appendix 4 PELVIC SPECIALIST MDT REFERRAL PROFORMA PELVIC SPECIALIST MDT REFERRAL PROFORMA FAXBACK NUMBER: PATIENT DETAILS PATIENT ID DOB Postcode Name REFERRER DETAILS NAME: TELEPHONE NO: FAX NO: DATE OF REFERRAL: GP DETAILS Name Postcode Address RADIOLOGIST / PATHOLOGIST REVIEW REQUEST N.B Images must be received at the latest by Wednesday before the meeting. Radiology to be reviewed? If so, specific Pathology to be reviewed? question to be asked: Films referred to (SMDT Radiologist) Date: Slides referred to (SMDT Pathologist) Date: Histological grade and stage Clinical stage BLADDER CANCER - CHECKLIST PRIOR TO REFERRAL U & Es LFTs MRI CT scan Co-morbidity / medication Upper Tract Status No Hydronephrosis Unilateral Hydronephrosis Bilateral Hydronephrosis Question Decision Page 36 of 44
37 Appendix 5 - TCC Algorithm: New Non-muscle Invasive Tumour First TURBT Non Muscle invasive Muscle Invasive See Muscle invasive algorithm G1pTa / G2pTa G2pT1 G3pTa, G3pT1 or CIS Local MDT Single dose of intravesical chemo at resection Flexi cysto at 3/12 (GA or Flexi) Assign risk group at first cystectomy Solitary tumour initially Local MDT 6x weekly intravesical chemotherapy 1 st check cysto under GA at 4/12 then 3/12 flexis for 2 years, then 6/12 for 2 years, then annual for life Multifocal tumour initially SMDT Pathology review by experienced uropathologist Consider 2 nd look TURBT BCG Consider cystectomy Clear Recurrence Clear Recurrence Low Risk Flexi at 1 year then annually for 5 years as per EAU Guidance. Then annual urine cytology analysis by GP Medium Risk 3/12 flexis for 1 year then 6/12 flexis for 3 years then annual flexis for life High Risk 6 doses of intravesical chemo then 3/13 flexi for 1 year then 6/12 flexi for 2 years then annual flexi for life BCG protocol Induction course 6 weeks with GA cysto and biopsy 8/52 after maintenance schedule as agreed local protocol. Monitoring 3/12 flexi for 2 years then 6/12 for 3 years then annually for life Page 37 of 44
38 Appendix 6 - TCC Algorithm: Recurrent Non-muscle Invasive Tumours G1pTa, G2pTa or G2pT1 Patients previously treated with BCG i.e. G3pTa, G3pT1 and CIS Single recurrence <5mm Single recurrence >5mm or multifocal recurrence Recurrence >5mm or multifocal recurrence after single dose of intravesical chemo Recurrence >5mm or multifocal recurrence after course of chemotherapy Recurrence after previous BCG Resect / biopsy / diathermy Single post op dose of intravesical chemotherapy & flexi in 3 months 6 week course of intravesical chemo then flexi at 3 months BCG and GA cysto and biopsy at 3 months If recurrence radical treatment recommended Page 38 of 44
39 Appendix 7 TCC Algorithm: Muscle Invasive Tumours First TURT Muscle invasive If tumour looks solid at initial flexi - arrange MRI prior to TURT - Bx prostatic urethra (men or bladder neck (women) Review in SMDT Consider 2 nd look TURT Debulk if radiotherapy likely Biopsy prostatic urethra / bladder neck if not already done CXR, LFTs, alk phos (bone scan if elevated) MRI/CT scan abdo and pelvis Consider suitability for trial Chemotherapy MVAC Neo adjuvant to surgery or radiotherapy improves survival by 5% at 5 years toxic regimen requiring careful patient selection Gemcitabine & Cisplatin has similar outcome with less side-effects Cystectomy Radiotherapy Discuss the following Lack of evidence to favour cystectomy over RT LUTS. Role of lymphadenectomy Neo Chemo adjuvant for locally advanced disease Nerve sparing Diversion vs reconstruction Peri-operative mortality/morbidity Need for life long oncological & functional follow up Meeting with Sp nurse to discuss periop course and issues around diversion/reconstruction Offer meeting with patient who has intended diversion/reconstruction If pathologically high risk (pn+, pm+ or positive margins) discuss in spmdt with a view to adjuvant chemotherapy Radical Radiotherapy Fit patients with muscle invasive but not extravesical disesase Younger fitter patients with limited N+ disease (but not M+ ) can be offered radical RT after good response to neoadjuvant chemo Preference over cystectomy if comorbidity precludes surgery or inability to manage Palliative Radiotherapy To control symptoms esp pelvic pain and haematuria Typically 30Gy in 6 fractions over 2 weeks or 8Gy single fraction Follow up schedule 6/52 oncology review. 1st post cysto (GA) at 3 months if clear CT and flexi 3/12ly for 18 months with CT 1 year post RT then 6/12ly for 4 years then annually for life. Residual /recurrent tumour consider salvage cystectomy if CT shows nodes consider FNA then chemo + chemo + TURT vs salvage cystectomy Page 39 of 44
40 Appendix 8 Recurrent Muscle-invasive Tumours Page 40 of 44
3.1 Investigations for Patients Presenting with Haematuria Table 1
 3.1 Investigations for Patients Presenting with Haematuria Table 1 Patients at risk of bacterial endocarditis should be given antibiotic prophylaxis as per local guidelines. Patients with heart valve replacements
3.1 Investigations for Patients Presenting with Haematuria Table 1 Patients at risk of bacterial endocarditis should be given antibiotic prophylaxis as per local guidelines. Patients with heart valve replacements
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Appendix 4 Urology Care Pathways
 Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
GUIDELINES FOR THE MANAGEMENT OF BLADDER CANCER
 GUIDELINES FOR THE MANAGEMENT OF BLADDER CANCER For approvals and version control see Document Management Record on page 9 Ref: AngCN-SSG-U4 Page 1 of 11 Approved and Published: Aug 2012 TABLE OF CONTENTS
GUIDELINES FOR THE MANAGEMENT OF BLADDER CANCER For approvals and version control see Document Management Record on page 9 Ref: AngCN-SSG-U4 Page 1 of 11 Approved and Published: Aug 2012 TABLE OF CONTENTS
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Guidelines for the Management of Bladder Cancer
 Guidelines for the Management of Bladder Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Version 3 and 4 Sections 5.2 and 8 updated Page 1 of 9 1. Scope of
Guidelines for the Management of Bladder Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Version 3 and 4 Sections 5.2 and 8 updated Page 1 of 9 1. Scope of
Bladder cancer - suspected
 Background information Information resources for patients and carers Updates to this care map Bladder cancer - clinical presentation History Examination Consider differential diagnoses Clinical indications
Background information Information resources for patients and carers Updates to this care map Bladder cancer - clinical presentation History Examination Consider differential diagnoses Clinical indications
6 UROLOGICAL CANCERS. 6.1 Key Points
 6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER
 GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
Bladder Cancer in Primary Care. Dr Penny Kehagioglou Consultant Clinical Oncologist
 Bladder Cancer in Primary Care Dr Penny Kehagioglou Consultant Clinical Oncologist Objectives Patient presentation in primary care Investigating bladder cancer Management of bladder cancer Differential
Bladder Cancer in Primary Care Dr Penny Kehagioglou Consultant Clinical Oncologist Objectives Patient presentation in primary care Investigating bladder cancer Management of bladder cancer Differential
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Update on Haematuria and Bladder Cancer
 Update on Haematuria and Bladder Cancer Hugh Mostafid FRCS(urol) FEBU Consultant Urologist, Royal Surrey County Hospital and Honorary Senior Lecturer, University of Surrey Guildford None Declarations Recent
Update on Haematuria and Bladder Cancer Hugh Mostafid FRCS(urol) FEBU Consultant Urologist, Royal Surrey County Hospital and Honorary Senior Lecturer, University of Surrey Guildford None Declarations Recent
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
Haematuria and Bladder Cancer
 Haematuria and Bladder Cancer Dr Pardeep Kumar Consultant Urological Surgeon Haematuria 3 Haematuria Macroscopic vs Microscopic Painful vs Painless Concurrent abdo pain/urinary symptoms Previous testing?
Haematuria and Bladder Cancer Dr Pardeep Kumar Consultant Urological Surgeon Haematuria 3 Haematuria Macroscopic vs Microscopic Painful vs Painless Concurrent abdo pain/urinary symptoms Previous testing?
Acute Oncology Induction Training Specification
 Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
Cancer of Unknown Primary Service
 Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
NMIBC. Piotr Jarzemski. Department of Urology Jan Biziel University Hospital Bydgoszcz, Poland
 NMIBC Piotr Jarzemski Department of Urology Jan Biziel University Hospital Bydgoszcz, Poland 71 year old male patient was admitted to the Department of Urology First TURBT - 2 months prior to the hospitalisation.
NMIBC Piotr Jarzemski Department of Urology Jan Biziel University Hospital Bydgoszcz, Poland 71 year old male patient was admitted to the Department of Urology First TURBT - 2 months prior to the hospitalisation.
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Guidelines for Management of Penile Cancer
 Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
Non Muscle Invasive Bladder Cancer. Primary and Recurrent TCC 4/10/2010. Two major consequences: Strategies: High-Risk NMI TCC
 Intravesical Therapy 2010-When, with What, When to Stop Friday, April 9, 2010 Ralph de VereWhite, MD Director, UC Davis Cancer Center Associate Dean for Cancer Programs Professor, Department of Urolgoy
Intravesical Therapy 2010-When, with What, When to Stop Friday, April 9, 2010 Ralph de VereWhite, MD Director, UC Davis Cancer Center Associate Dean for Cancer Programs Professor, Department of Urolgoy
Costing report: Bladder cancer
 Putting NICE guidance into practice Costing report: Bladder cancer Implementing the NICE guideline on bladder cancer (NG2) Published: February 2015 Updated September 2015 to update the unit cost of transurethral
Putting NICE guidance into practice Costing report: Bladder cancer Implementing the NICE guideline on bladder cancer (NG2) Published: February 2015 Updated September 2015 to update the unit cost of transurethral
Staging and Grading Last Updated Friday, 14 November 2008
 Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
MDT IMPROVEMENT PROJECT. Professor Muntzer Mughal, UCLH
 MDT IMPROVEMENT PROJECT Professor Muntzer Mughal, UCLH 1995..assessment and management of rare cancers in multidisciplinary teams.. 2000 the care of all patients with cancer should be formally reviewed
MDT IMPROVEMENT PROJECT Professor Muntzer Mughal, UCLH 1995..assessment and management of rare cancers in multidisciplinary teams.. 2000 the care of all patients with cancer should be formally reviewed
When to Integrate Surgery for Metatstatic Urothelial Cancers
 When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
Trimodality Therapy for Muscle Invasive Bladder Cancer
 Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
A patient with recurrent bladder cancer presents with the following history:
 MP/H Quiz A patient with recurrent bladder cancer presents with the following history: 9/23/06 TURB 1/12/07 TURB 4/1/07 TURB 7/12/07 TURB 11/14/07 Non-invasive papillary transitional cell carcinoma from
MP/H Quiz A patient with recurrent bladder cancer presents with the following history: 9/23/06 TURB 1/12/07 TURB 4/1/07 TURB 7/12/07 TURB 11/14/07 Non-invasive papillary transitional cell carcinoma from
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Carcinoma of the Urinary Bladder Histopathology
 Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
5/26/16: CT scan of the abdomen showed a multinodular liver disease highly suspicious for metastasis and hydronephrosis of the right kidney.
 Bladder Case Scenario 1 History 5/23/16: A 52-year-old male, smoker was admitted to our hospital with a 3-month history of right pelvic pain, multiple episodes of gross hematuria, dysuria, and extreme
Bladder Case Scenario 1 History 5/23/16: A 52-year-old male, smoker was admitted to our hospital with a 3-month history of right pelvic pain, multiple episodes of gross hematuria, dysuria, and extreme
BLADDER CANCER PATHWAY (E&W) Version 1
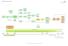 BLADDER CANCER PATHWAY (E&W) Version 1 Flexi cysto FU (via cystoscopy) ptag1/2 and OP instillations MMC ptag3/cis BCG BCG cancer One-stop Haematuria Clinic TURBT Histology presented Decision to refer to
BLADDER CANCER PATHWAY (E&W) Version 1 Flexi cysto FU (via cystoscopy) ptag1/2 and OP instillations MMC ptag3/cis BCG BCG cancer One-stop Haematuria Clinic TURBT Histology presented Decision to refer to
Urological Tumours 1 Kidney tumours 2 Bladder tumours
 Urological Tumours 1 Kidney tumours 2 Bladder tumours Tim Bracey SpR Histopathology Derriford Hospital Kidney tumours What are we going to talk about?! Anatomy of urinary tract! Types of kidney tumours!
Urological Tumours 1 Kidney tumours 2 Bladder tumours Tim Bracey SpR Histopathology Derriford Hospital Kidney tumours What are we going to talk about?! Anatomy of urinary tract! Types of kidney tumours!
One Stop Prostate Biopsy Protocol Author Consultation Date Approved
 One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
Chemotherapy Treatment Algorithms for Urology Cancer
 Chemotherapy Treatment Algorithms for Urology Cancer Chemoradiation for bladder cancer; Chemotherapy algorithm for non TCC bladder cancer Squamous cell carcinoma; Chemotherapy Algorithm for Non Transitional
Chemotherapy Treatment Algorithms for Urology Cancer Chemoradiation for bladder cancer; Chemotherapy algorithm for non TCC bladder cancer Squamous cell carcinoma; Chemotherapy Algorithm for Non Transitional
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
CHEMO-RADIOTHERAPY FOR BLADDER CANCER. Dr Darren Mitchell Consultant Clinical Oncologist Northern Ireland Cancer Centre
 CHEMO-RADIOTHERAPY FOR BLADDER CANCER Dr Darren Mitchell Consultant Clinical Oncologist Northern Ireland Cancer Centre AIMS Muscle invasive disease Current Gold-Standard Rationale behind Chemo-Radiotherapy
CHEMO-RADIOTHERAPY FOR BLADDER CANCER Dr Darren Mitchell Consultant Clinical Oncologist Northern Ireland Cancer Centre AIMS Muscle invasive disease Current Gold-Standard Rationale behind Chemo-Radiotherapy
Management of High Grade, T1 Bladder Cancer Douglas S. Scherr, M.D.
 Management of High Grade, T1 Bladder Cancer Douglas S. Scherr, M.D. Assistant Professor of Urology Clinical Director, Urologic Oncology Weill Medical College-Cornell University Estimated new cancer cases.
Management of High Grade, T1 Bladder Cancer Douglas S. Scherr, M.D. Assistant Professor of Urology Clinical Director, Urologic Oncology Weill Medical College-Cornell University Estimated new cancer cases.
An Undergraduate Syllabus for Urology. Produced on behalf of the British Association of Urological Surgeons. March 2012
 An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
Case 1. Receives induction BCG weekly x 6 without significant toxicity Next step should be:
 Case 1 89 year old male with initial occurrence of gross hematuria Office flexible cystoscopy shows two papillary tumors with some surface necrosis Complete TURBT into muscle Florescence cysto shows two
Case 1 89 year old male with initial occurrence of gross hematuria Office flexible cystoscopy shows two papillary tumors with some surface necrosis Complete TURBT into muscle Florescence cysto shows two
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Bladder tumour resection (TURBT): procedure-specific information
 PATIENT INFORMATION Bladder tumour resection (TURBT): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association
PATIENT INFORMATION Bladder tumour resection (TURBT): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British Association
Diagnosis and classification
 Patient Information English 2 Diagnosis and classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour is present.
Patient Information English 2 Diagnosis and classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour is present.
Haematuria and Modern Bladder Cancer Treatment
 Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
Haematuria and Modern Bladder Cancer Treatment Mr Nikhil Vasdev MBBS MRCS MCh(Urol) FRCS(Urol) RCSEng/BAUS Robotic Fellowship Accredited and Trained Consultant Urological and Robotic Surgeon Hertfordshire
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY
 COLORECTAL CLINICAL SUBGROUP RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY Finalised by: Dr Simon Gollins Mr Andrew Renehan Dr Mark Saunders Mr Nigel Scott Dr Shabbir
COLORECTAL CLINICAL SUBGROUP RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY Finalised by: Dr Simon Gollins Mr Andrew Renehan Dr Mark Saunders Mr Nigel Scott Dr Shabbir
Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016
 BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Transperineal ultrasound-guided biopsy of the prostate gland
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient biopsy of the prostate gland affix patient label What is a transperineal (TP) ultrasound-guided prostate
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient biopsy of the prostate gland affix patient label What is a transperineal (TP) ultrasound-guided prostate
MEDitorial March Bladder Cancer
 MEDitorial March 2010 Bladder Cancer Last month, my article addressed the issue of blood in the urine ( hematuria ). A concerning cause of hematuria is bladder cancer, a variably malignant tumor starting
MEDitorial March 2010 Bladder Cancer Last month, my article addressed the issue of blood in the urine ( hematuria ). A concerning cause of hematuria is bladder cancer, a variably malignant tumor starting
Radical removal of the kidney (radical nephrectomy): procedure-specific information
 PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES. U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease
 PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease Refer back to original requester with this paperwork and review previous
PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease Refer back to original requester with this paperwork and review previous
Citation International journal of urology (2. Right which has been published in final f
 Title Novel constant-pressure irrigation of renal pelvic tumors after ipsila Nakamura, Kenji; Terada, Naoki; Sug Author(s) Toshinori; Matsui, Yoshiyuki; Imamu Kazutoshi; Kamba, Tomomi; Yoshimura Citation
Title Novel constant-pressure irrigation of renal pelvic tumors after ipsila Nakamura, Kenji; Terada, Naoki; Sug Author(s) Toshinori; Matsui, Yoshiyuki; Imamu Kazutoshi; Kamba, Tomomi; Yoshimura Citation
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr Prasad Bollina, NHS Lothian
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr Prasad Bollina, NHS Lothian
Inspection/examination of the ureter & biopsy : procedure-specific information
 PATIENT INFORMATION Inspection/examination of the ureter & biopsy : procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the
PATIENT INFORMATION Inspection/examination of the ureter & biopsy : procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
NICE BULLETIN Diagnosis & treatment of prostate cancer
 Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer
 Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer Reference: NHS England B14X08 Information Reader Box (IRB) to be inserted on inside front cover for documents of 6
Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer Reference: NHS England B14X08 Information Reader Box (IRB) to be inserted on inside front cover for documents of 6
Care of bladder cancer patients diagnosed in Northern Ireland 2010 & 2011 (Summary)
 Care of bladder cancer patients diagnosed in 2010 & 2011 (Summary) Bannon, F., Ranaghan, L., & Gavin, A. (2014). Care of bladder cancer patients diagnosed in 2010 & 2011 (Summary). N. Cancer Registry,
Care of bladder cancer patients diagnosed in 2010 & 2011 (Summary) Bannon, F., Ranaghan, L., & Gavin, A. (2014). Care of bladder cancer patients diagnosed in 2010 & 2011 (Summary). N. Cancer Registry,
H(a)ematuria. FX Keeley Consultant Urologist Bristol Urological Institute
 H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
H(a)ematuria FX Keeley Consultant Urologist Bristol Urological Institute From Philadelphia to Bristol, England Southmead Hospital, 1916 Southmead Hospital, 2013 Southmead Hospital, 2014 H(a)ematuria Blood
UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT
 Urological Cancer Audit 2009 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr
Urological Cancer Audit 2009 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr
AUA Guidelines for Invasive Bladder Cancer: What s New?
 AUA Guidelines for Invasive Bladder Cancer: What s New? Michael S. Cookson, MD, MMHC Professor and Chairman Department of Urology, University of Oklahoma History 1999: AUA guidelines Panel Non-muscle invasive
AUA Guidelines for Invasive Bladder Cancer: What s New? Michael S. Cookson, MD, MMHC Professor and Chairman Department of Urology, University of Oklahoma History 1999: AUA guidelines Panel Non-muscle invasive
North of Scotland Cancer Network Clinical Management Guideline for Carcinoma of the Uterine Cervix
 THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
9/13/2017. Highgate Private Hospital & Whittington Health NHS Trust. London Cancer Urology Guidelines for Target Referrals. Urological Cancer Groups
 London Cancer Urology Guidelines for Target Referrals Mr Paul Erotocritou MBBS BSc MSc, MRCS, FRCS (Urol)Eng Highgate Private Hospital & Whittington Health NHS Trust Urological Cancer Groups 5 groups:
London Cancer Urology Guidelines for Target Referrals Mr Paul Erotocritou MBBS BSc MSc, MRCS, FRCS (Urol)Eng Highgate Private Hospital & Whittington Health NHS Trust Urological Cancer Groups 5 groups:
Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases
 Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases Date: April 2015 Date for review: April 2018 1. Principles The recognised specialist HPB MDT for Greater
Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases Date: April 2015 Date for review: April 2018 1. Principles The recognised specialist HPB MDT for Greater
UROTHELIAL CELL CANCER
 UROTHELIAL CELL CANCER Indications and regimens for neoadjuvant systemic treatment Astrid A. M. van der Veldt, MD, PhD, medical oncologist Department of Medical Oncology Erasmus Medical Center Cancer Institute
UROTHELIAL CELL CANCER Indications and regimens for neoadjuvant systemic treatment Astrid A. M. van der Veldt, MD, PhD, medical oncologist Department of Medical Oncology Erasmus Medical Center Cancer Institute
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs. Gynaecological sarcomas Version 1
 Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
BLADDER CANCER CONTENT CREATED BY. Learn more at
 BLADDER CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK TO YOUR DOCTOR Table of Contents WHAT IS BLADDER CANCER? 4 TYPES OF BLADDER CANCER 5 GRADING AND STAGING 8 TREATMENT OVERVIEW
BLADDER CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK TO YOUR DOCTOR Table of Contents WHAT IS BLADDER CANCER? 4 TYPES OF BLADDER CANCER 5 GRADING AND STAGING 8 TREATMENT OVERVIEW
The Clinical Impact of the Classification of Carcinoma In Situ on Tumor Recurrence and their Clinical Course in Patients with Bladder Tumor
 Original Article Japanese Journal of Clinical Oncology Advance Access published December 17, 2010 Jpn J Clin Oncol 2010 doi:10.1093/jjco/hyq228 The Clinical Impact of the Classification of Carcinoma In
Original Article Japanese Journal of Clinical Oncology Advance Access published December 17, 2010 Jpn J Clin Oncol 2010 doi:10.1093/jjco/hyq228 The Clinical Impact of the Classification of Carcinoma In
The group seemed largely happy with the proposed GDG membership. Additional comments and clarifications as below:
 Bladder Cancer Guideline Draft Scope Stakeholder Workshop: Group Notes Group 1 John Graham Andrew Champion Julia Verne Elise Hasler Nathan Bromham Suzanne Langley Sue Norman Lyndon Gommersall Dr Kate Williamson
Bladder Cancer Guideline Draft Scope Stakeholder Workshop: Group Notes Group 1 John Graham Andrew Champion Julia Verne Elise Hasler Nathan Bromham Suzanne Langley Sue Norman Lyndon Gommersall Dr Kate Williamson
Bladder Cancer Canada November 21st, Bladder Cancer 2018: A brighter light at the end of the cystoscope
 Bladder Cancer Canada November 21st, 2018 Bladder Cancer 2018: A brighter light at the end of the cystoscope Chris Morash MD FRCSC Associate Professor, University of Ottawa Head, Urological Oncology Bladder
Bladder Cancer Canada November 21st, 2018 Bladder Cancer 2018: A brighter light at the end of the cystoscope Chris Morash MD FRCSC Associate Professor, University of Ottawa Head, Urological Oncology Bladder
NICE guideline Published: 25 February 2015 nice.org.uk/guidance/ng2
 Bladder cancer: diagnosis and management NICE guideline Published: 25 February 2015 nice.org.uk/guidance/ng2 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Bladder cancer: diagnosis and management NICE guideline Published: 25 February 2015 nice.org.uk/guidance/ng2 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
September 10, Dear Dr. Clark,
 September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
EAU GUIDELINES ON NON-MUSCLE INVASIVE (TaT1, CIS) BLADDER CANCER
 EU GUIDELINES ON NON-MUSLE INVSIVE (TaT1, IS) LDDER NER (Limited text update March 2017) M. abjuk (hair), M. urger (Vice-hair), E. ompérat, P. Gontero,.H. Mostafid, J. Palou,.W.G. van Rhijn, M. Rouprêt,
EU GUIDELINES ON NON-MUSLE INVSIVE (TaT1, IS) LDDER NER (Limited text update March 2017) M. abjuk (hair), M. urger (Vice-hair), E. ompérat, P. Gontero,.H. Mostafid, J. Palou,.W.G. van Rhijn, M. Rouprêt,
Improving services for upper GI (OG) cancer Application template (Version 2)
 Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO)
 North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
NICE Quality Standards and COF
 NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Information for patients This information is for people with cancer of unknown primary (CUP) and covers symptoms, investigations/tests and treatment options. If there is
Cancer of Unknown Primary (CUP) Information for patients This information is for people with cancer of unknown primary (CUP) and covers symptoms, investigations/tests and treatment options. If there is
IAUN Conference Dublin, January Helen Forristal Cancer Nurse Co- Ordinator Jonathan Borwell Bladder Cancer Clinical Nurse Specialist
 IAUN Conference Dublin, January 2014 Helen Forristal Cancer Nurse Co- Ordinator Jonathan Borwell Bladder Cancer Clinical Nurse Specialist Theoretical component Observation Supervised practice Assessment
IAUN Conference Dublin, January 2014 Helen Forristal Cancer Nurse Co- Ordinator Jonathan Borwell Bladder Cancer Clinical Nurse Specialist Theoretical component Observation Supervised practice Assessment
South East London Cancer Network GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCERS. June 2012
 South East London Cancer Network GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCERS June 2012 Review date: August 2013 1 SOUTH EAST LONDON CANCER NETWORK UROLOGY DIAGNOSTIC AND TREATMENT GUIDELINES Index
South East London Cancer Network GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCERS June 2012 Review date: August 2013 1 SOUTH EAST LONDON CANCER NETWORK UROLOGY DIAGNOSTIC AND TREATMENT GUIDELINES Index
Guidelines for the Management of Adult Patients with Urological Cancers 2013
 Guidelines for the Management of Adult Patients with Urological Cancers 2013 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date Approved:
Guidelines for the Management of Adult Patients with Urological Cancers 2013 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date Approved:
Symptoms, Diagnosis and Classification
 Patient Information English 2 Symptoms, Diagnosis and Classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour
Patient Information English 2 Symptoms, Diagnosis and Classification The underlined terms are listed in the glossary. Signs and symptoms Blood in the urine is the most common symptom when a bladder tumour
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
Issues in the Management of High Risk Superficial Bladder Cancer
 Issues in the Management of High Risk Superficial Bladder Cancer MICHAEL A.S. JEWETT DIVISION OF UROLOGY, DEPARTMENT OF SURGICAL ONCOLOGY, PRINCESS MARGARET HOSPITAL & THE UNIVERSITY OF TORONTO 1 Carcinoma
Issues in the Management of High Risk Superficial Bladder Cancer MICHAEL A.S. JEWETT DIVISION OF UROLOGY, DEPARTMENT OF SURGICAL ONCOLOGY, PRINCESS MARGARET HOSPITAL & THE UNIVERSITY OF TORONTO 1 Carcinoma
A06/S(HSS)b Ex-vivo partial nephrectomy service (Adult)
 A06/S(HSS)b 2013/14 NHS STANDARD CONTRACT FOR EX-VIVO PARTIAL NEPHRECTOMY SERVICE (ADULT) PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATION Service Specification No. Service Commissioner
A06/S(HSS)b 2013/14 NHS STANDARD CONTRACT FOR EX-VIVO PARTIAL NEPHRECTOMY SERVICE (ADULT) PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATION Service Specification No. Service Commissioner
Guideline for the Management of Patients Suitable for Immediate Breast Reconstruction
 Version History Guideline for the Management of Patients Suitable for Immediate Breast Reconstruction Version Summary of change Date Issued 2.0 Endorsed by the Governance Committee 20.02.08 2.1 Circulated
Version History Guideline for the Management of Patients Suitable for Immediate Breast Reconstruction Version Summary of change Date Issued 2.0 Endorsed by the Governance Committee 20.02.08 2.1 Circulated
Guideline for the Diagnosis of Breast Cancer
 Guideline for the Diagnosis of Breast Cancer Version History Version Date Brief Summary of Change Issued 2.0 May 2007 Approved by the Governance Committee 2.0 25.11.08 Discussed at the NSSG 2.1 5.12.08
Guideline for the Diagnosis of Breast Cancer Version History Version Date Brief Summary of Change Issued 2.0 May 2007 Approved by the Governance Committee 2.0 25.11.08 Discussed at the NSSG 2.1 5.12.08
