Comparison of short-term outcomes between laparoscopicassisted and open complete mesocolic excision (CME) for the treatment of transverse colon cancer
|
|
|
- Arline Hamilton
- 6 years ago
- Views:
Transcription
1 Original Article Page 1 of 7 Comparison of short-term outcomes between laparoscopicassisted and open complete mesocolic excision (CME) for the treatment of transverse colon cancer Yong Wang, Chuan Zhang, Yi-Fei Feng, Zan Fu, Yue-Ming Sun Department of Colorectal Surgery, The First Affiliated Hospital of Nanjing Medical University, Nanjing , China Contributions: (I) Conception and design: Y Wang; (II) Administrative support: All authors; (III) Provision of study materials or patients: Y Wang, C Zhang, YF Feng; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Yue-Ming Sun. Department of Colorectal Surgery, The First Affiliated Hospital of Nanjing Medical University, No. 300, Guangzhou Road, Nanjing , China. jssym@vip.sina.com. Background: Colorectal cancer (CRC) is the third most common cancer worldwide. Although laparoscopic-assisted complete mesocolic excision (LCME) is a superior treatment, there are few studies available on it owe to the low incidence and technical difficulty of LCME in transverse colon cancer. Methods: The clinical data of 78 patients with transverse colon cancer who were treated by LCME and open complete mesocolic excision (OCME) were retrospectively analyzed. A total of 39 cases had been treated by LCME, compared with 39 cases treated by OCME. The patient characteristics and short-term outcomes including operation time, intra-operative blood loss, length of incision, time to first flatus, first postoperative ambulation, postoperative hospitalization time, number of harvested lymph nodes, length of resected specimen and incidence of complications were evaluated. Results: There was no case converted to OCME in LCME group. LCME had significantly shorter length of incision, shorter operation time, less intra-operative blood loss, shorter postoperative hospitalization time (P<0.05). The length of resected specimen and the numbers of harvested lymph nodes were (26.5±5.4 cm) and (16.2±3.1) in LCME group, and (24.8±4.9 cm) and (15.1±3.5) in OCME group, with no differences between two groups. The incidence of wound infection was lower while the incidence of lymphatic leakage, anastomotic leakage, urinary tract infection and wound dehiscence had no significant differences between two groups. None of patients in these two groups developed urinary retention, anastomotic bleeding and postoperative intestinal obstruction. Conclusions: Our findings suggested that LCME is a safe, feasible and effective treatment method for the treatment of transverse colon cancer due to it can provide superior short-term outcomes including less intraoperative blood loss, faster recovery and lower incidence of wound infection. Keywords: Laparoscopy; complete mesocolic excision (CME); transverse colon cancer; short-term outcomes Submitted Oct 10, Accepted for publication Dec 21, doi: /cco View this article at: Introduction Colorectal cancer (CRC) is the third most common cancer worldwide (1), which is a leading cause of cancer death (2). Complete mesocolic excision (CME) is considered to be the standard CRC surgeries due to it can reduce local recurrence and improve long-term survival (3). Since the first application of laparoscopic surgery in 1991 (4), laparoscopic technique has been introduced to many surgical fields such as the treatment of CRC with the advanced laparoscopic instruments and technique (5).
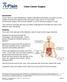
2 Page 2 of 7 Wang et al. Laparoscopic-assisted versus OCME Figure 1 The position of 5 trocars in LCME. A 10-mm trocar was introduced in the umbilical region for the placement of laparoscope. A 12-mm trocar insertion was located at the intersection of the left midclavicular line (MCL) and the horizontal line of midpoint between the xiphoid and the umbilicus which can be used as a working port. Three additional 5 mm ports were placed on the midpoints of connection line between umbilicus and both sides of anterior superior iliac spine, and 3 cm under the costal margin of right subclavian midline using as assistant working ports, respectively. 5 mm 12 mm 10 mm 5 mm 5 mm February All participants gave informed written consent. The research protocols were approved by the ethical committee of our hospital (2014-SRFA-188). Transverse colon cancer was defined as the tumor at 1/3 in the middle of transverse colon. Transverse colon cancer was confirmed by a routine biopsy, colonoscopy, computed tomography (CT) scans and magnetic resonance imaging (MRI). MRI was used to identify the suspicious liver metastatic. A total of 78 patients were included in this study. Both LCME and OCME were treatments for transverse colon cancer and the choice of surgical approach was based on patient s wishes after the surgical procedures, possible risks and discomforts of these two approaches were informed to patients. Among the 78 patients, 39 patients underwent LCME and the remaining 39 patients underwent OCME. Exclusion criteria for CME were as follows: (I) Patients with severe cardiac, pulmonary insufficiency and can not tolerate surgery after active treatment; (II) recurrent cancer patients after operation; (III) patients with tumor involving other organs; (IV) patients with tumor perforation or acute obstruction; (V) patients with secondary CRC; (VI) patients undergoing LCME converted to OCME; (VII) patients with tumor involving adjacent tissues and organs and can not be cured by resection; (VIII) patients with non-adenocarcinoma. Previous studies have reported that LCME is a superior approach for CRC benefit from less pain and blood loss, shorter recovery and hospital stays, better cosmetics and short-term outcomes, and reduced morbidity (6,7). However, there was no significant difference in disease-free survival of patients between LCME and OCME in a larger trials (8). Presumably because of the low incidence and technical difficulty of laparoscopic CME in transverse colon cancer (9) including safely take down and fully mobilization of the splenic flexure and hepatic flexure, large separating surface and high-precision technique (10), there are few studies available on it (11). In this study, we aim to compare the short-term outcomes of the CME for transverse colon cancer between laparoscopic and open approaches and to identify the safety and feasibility about LCME. Methods Patient selection We retrospectively collected the clinical data of patients with transverse colon cancer between October 2014 and Surgical techniques Preoperative evaluations Before surgery, routine examination including blood, coagulation, blood type, biochemical tests, electrocardiography (ECG), five hepatitis B, HIV, HCV, RPR, urine, stool, colonoscopy, chest and abdomen enhanced CT, and MRI were performed to make definite diagnosis and exclude surgical contraindications. Before surgery, all patients were fasted for 12 h, forbidden to drink for 4 h. On the evening before surgery, all patients took polyethylene glycol electrolyte powder solution for bowel preparation. All the surgeries in both groups were performed with the same surgeon. Endotracheal intubation was performed under general anesthesia and routine catheterization. All patients were placed in supine position with legs separated and fixed. The surgeon stood to the left side of the patient, the first assistant stood to the right side of the patient, while the second assistant holding a mirror stood between the two legs of patients. LCME Five-trocar method (Figure 1) was applied in CME. After
3 Chinese Clinical Oncology, Vol 6, No 1 February 2017 routine abdominal exploration, procedures were performed with a median-to-lateral approach. Below the horizontal part of duodenum, we dissected the serous membrane, and dissected the sheath of superior mesenteric vein (SMV) (Figure 2A). Dissection was proceeded along the SMV. After entering the sub-fascial space of the pancreatoduodenal fascia, we dissect the superior mesenteric artery (SMA), removed connective tissues and lymph nodes in front of SMA, then enter the right Toldt s gap, followed by a dissection extending upward to the hepatic flexure ligament of the colon and outward until the lateral fusion fascia of ascending colon. After dissecting the middle colic artery along with SMV, we removed the lymph nodes following by the division of the middle colic artery from the root after the (Figure 2B). Thereafter, we dissected the Henle s trunk, and divided the right colic vein (Figure 2C) with the preservation of right gastric-omentum vein. After dividing the middle colic vein, we divided the lower edge of pancreas and anterior pancreatic space (Figure 2D), and separated the space between pancreatic and gastric. The surgeon exchanged the position with the first assistant. Then we pulled out the inferior mesenteric vein and dissected the serous membrane and extended upward to the lower edge of pancreas, and downward to the root region of the inferior mesenteric artery. Entered the left side of Toldt s gap with a dissection extended upward the lower edge of the pancreas tail and outward until the lateral fusion fascia of descending colon. Then the upper region of colon was steered. After opening the gastrocolic ligament, we resected the greater omentum. Then we divided the pancreas attachment of the root region of right side of the transverse mesocolon, cut off the hepatic flexure ligament of colon (Figure 2E), divided the outside fusion fascia of ascending colon and converged into the inferior separation of gap. Thereafter we divided the pancreas attachment of the root region of the left side of the transverse mesocolon root, resected the ligament of splenic flexure (Figure 2F), divided the outside fusion fascia of descending colon and converged into the inferior separation of gap. Through above procedures, we completely separated the transverse colon, hepatic flexure, ascending colon, descending colon and splenic flexure. Finally, the resected specimen was obtained (Figure 2G). OCME A 5-cm incision protected with the protective sleeve made on the upper abdominal midline. After pulling out the transverse colon in vitro, the classic transverse CME techniques were conducted. Postoperative treatment Page 3 of 7 Conventional ECG monitoring was conducted in all patients for 12 hours. Three days after surgery, all patients were routinely given treatment including supplement of body fluid, anti-infection, acid suppression, maintain the balance of acid-base and water electrolyte. On the first postoperative day, the motion of patients was encouraged. Approximately 3 days after surgery, a liquid diet was begun after first flatus which was allowed to transition to a normal diet. On the third postoperative day, blood and biochemical tests were performed to all patients, patients who were anemia or hypoproteinemia were given a blood transfusion, albumin transfusion therapy respectively. On the first or second postoperative day, the catheter was removed. A measurement of drainage fluid and observation characters was performed and the drainage tube was removed on the fifth or sixth postoperative day. Clinical characteristics, including operation time, intra-operative blood loss, length of incision, number of harvested lymph nodes and length of resected specimen were compared between the LCME and OCME groups. Short-term surgical outcomes including first flatus, first postoperative motion/movement, postoperative hospitalization time and complications were compared between the LCME and OCME groups. Statistical analysis Data were analyzed by using SPSS for Windows (version 18.0). We used chi-square test to compare categorical values between LCME and OCME group. An independent t-test was applied to compare measurement data between each two groups. Quantitative data are expressed as means ± standard deviations (SD), and measurement data are expressed as n or percentage. P values of less than 0.05 were considered statistically significant. Results Baseline characteristics There were 39 cases in LCME group and 39 cases in OCME group, respectively. In LCME group, 21 were men and 18 were women, with a mean age of 58.3±5.8 years (range, years). The distribution of tumors according to TNM stage was as follows: Stage I in 4 patients, Stage II in 16, Stage III in 19. In OCME group, 20 were men and 19 were women, with a mean age of 57.5±6.9 years (range, 28
4 Wang et al. Laparoscopic-assisted versus OCME Page 4 of 7 A D B C E F G Figure 2 Laparoscopic-assisted complete mesocolic excision (LCME) for transverse colon cancer. (A) Free the root of transverse mesocolon; (B) lymph nodes resection at the root of transverse mesocolon; (C) amputated the right colic vein; (D) free the space in front of the head of the pancreas; (E) free the hepatic flexure of colon; (F) free the splenic flexure of colon; (G) resected specimen after LCME. 85 years). TNM stage was as follows: Stage I in 3 patients, Stage II in 15, Stage III in 21 (Table 1). There was no statistical significant difference regarding age, gender and TNM stage between the two groups. Perioperative outcomes LCME group were significantly better than OCME group (P<0.05) in intra-operative blood loss (61.6±18.7 vs ±35.4), length of incision (7.3±1.8 vs. 18.7±4.7), time to first flatus (1.5±0.6 vs. 3.2±0.9), and first postoperative Chinese Clinical Oncology. All rights reserved. ambulation (1.3±0.4 vs. 2.9±0.8). There were no significant differences in operation time (119.7±27.5 vs ±30.1), postoperative hospitalization time (8.1±2.9 vs. 10.1±2.2), number of harvested lymph nodes (16.2±3.1 vs. 15.1±3.5), and length of resected specimen (26.5±5.4 vs. 24.8±4.9) between LCME group and OCME group (Table 2). There was no significant difference in the total incidence of short-term postoperative complications between LCME and OCME groups (12.81% vs , P>0.05). However, the incidence of wound infection was significantly lower with laparoscopy (2.56%) than by the open approach cco.amegroups.com
5 Chinese Clinical Oncology, Vol 6, No 1 February 2017 Page 5 of 7 Table 1 Patient demographics Variable LCME (n=39) OCME (n=39) P value Age 58.3± ± Male/female Male Female TNM classification I 4 3 II III LCME, laparoscopic-assisted complete mesocolic excision; OCME, open complete mesocolic excision. Table 3 Complications in LCME and OCME groups Complications, n (%) LCME (n=39) (%) OCME (n=39) (%) P value Wound infection* 1 (2.56) 6 (7.69) Lymphatic leakage 2 (5.13) 1 (2.56) Anastomotic leakage Urinary tract infection 1 (2.56) 1 (2.56) 1 1 (2.56) 0 1 Wound dehiscence 0 1 (2.56) 1 Total incidence 5 (12.81) 6 (15.38) *Statistically significant between-group difference (P values<0.05). LCME, laparoscopic-assisted complete mesocolic excision; OCME, open complete mesocolic excision. Table2 Postoperative short-term outcomes in the LCME and OCME groups Variable LCME (n=39) OCME (n=39) P value Operation time, min 119.7± ± Intra-operative blood loss*, ml Length of incision *, cm 61.6± ±35.4 < ± ±4.7 < Time to first flatus *, d 1.5± ±0.9 < First postoperative ambulation*, d Postoperative hospitalization time, d number of harvested lymph nodes, n Length of resected specimen, cm 1.3± ±0.8 < ± ± ± ± ± ± *, statistically significant between-group difference (P values <0.05). LCME, laparoscopic-assisted complete mesocolic excision; OCME, open complete mesocolic excision. (7.69%). Lymphatic leakage, anastomotic leakage, urinary tract infection and wound dehiscence were occurred in 1 group or both 2 groups, there was no significant difference in the incidence (Table 3). None of patients in both groups developed urinary retention, anastomotic bleeding and intestinal obstruction. Discussion Although previous studies have demonstrated that LCME is a safe and feasible treatment for CRC (6,7,10), the majority of trials excluded cases of transverse colon cancer due to the technical difficulty (10,12,13). Our study compared the feasibility, safety and short-term outcomes between LCME and OCME groups. In terms of intra-operative outcomes, the length of incision was significantly shorter and the blood loss was less in LCME group than OCME group which suggested that LCME is more precise. Although there was no significant difference in operation time between these two groups, the operation time in LCME is shorter. It suggested that we can overcome the technical difficulty, shorten the operative time and be proficient in LCME. In our study, the numbers of lymph nodes retrieved in these two groups were similar. We can conclude that not only LCME but also OCME have the same oncologic clearance effects. Previous studies have demonstrated that the postoperative hospitalization time in LCME for CRC is always shorter (7,14). Since the technical difficulty there was no significant difference in postoperative hospitalization time between these two groups, it was still shorter in LCME. In addition, LCME was found to be better in time to the first flatus and first postoperative ambulation after surgery. It suggested that recovery of patients in LCME was faster. Similar or reduced complications were always reported in LCME for right colon cancer (7,15-18). There was no significant difference in the total incidence of short-term
6 Page 6 of 7 Wang et al. Laparoscopic-assisted versus OCME postoperative complications between these two groups in our study. A systematic review and meta-analysis have reported that complications were similar in LCME and OCME for transverse colon cancer, which supported our results (15). However, the incidence of wound infection was significantly less with laparoscopy due to the shorter incision. So LCME is as safe and feasible as OCME. Due to the high-definition vision, amplification effect of laparoscope, and with the application of ultrasonic knife, laparoscopic surgery can be applied to separation of surgical surfaces, based on the similar operative effects, the length of incision in LCME is shorter and it s helpful to reduce the blood loss and recover faster. Moreover, no tumor metastasis and recurrence is crucial for prognosis of CRC. To prevent the metastasis and local recurrence of CRC, intraperitoneal chemotherapy was proposed. Cytoreductive surgery and intraperitoneal chemotherapy may significantly increase the exposure of cancer drugs to cancer present within the peritoneal cavity or liver which may be helpful to repress the metastasis and local recurrence of CRC and are closely associated with prolonged overall survival and even cure of CRC (19-21). In our study, to prevent the formation of the incision planter and further implement the principle of non-contact, we removed the tumor with the incision was protected by protective sleeve. To prevent the formation of planter induced by direct contact between the polluted laparoscopic instruments and the puncture hole, the trocar was fixed to the abdominal wall. To prevent the formation of incision planter induced by intraperitoneal gas which carried tumor cells, we removed the trocar after the discharge with the puncture sheath in the end of surgery. In addition, Kim et al. has reported that central ligation of the main feeding vessels, complete removal of the mesocolon with sharp dissection, and adequate proximal and distal margins were benefit for improved oncologic outcomes. In our study, we resected both ends of the 10cm bowel of tumor, dissected the lymph nodes of mesenteric roots and removed the whole transverse mesocolon to manage for infrapyrolic node or splenic node metastases. To ensure the security and effectiveness of CME and repress tumor metastase, several key points were concluded from our operative experiences in CME. These principles were as follows: (I) Explore the liver, spleen, stomach, pelvic, mesenteric root, tumor and adjacent organs from far to near; (II) resect adequate bowel (both ends of the 10 cm bowel of tumor) and dissect the lymph nodes of mesenteric roots; (III) separate the Toldt s gap accurately, maintain the integrity of Toldt s fascia and resect the lesions bowel and mesentery from roots completely; (IV) apply medianto-lateral approach, ligate the mesenteric vessels on the root firstly and then performed resection and dissociation; (V) precise and gentle operating practice. Last but not least, LCME was reported to reduce the postoperative mortality and to have more clinical significance especially in elderly patients (22). The main drawback in the present study is the deficiency of long-term oncological follow-up and need further research. In conclusion, despite the technique difficult in surgery, LCME is more safe and feasible for the treatment of transverse colon cancer because it could provide better short-term outcomes including less blood loss and faster recovery compared to that of OCME. Further studies with longer term of follow up are required to confirm the efficacy of LCME/ confirm our findings Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Ethical Statement: All participants gave informed written consent. The research protocols were approved by the ethical committee of our hospital (2014-SRFA-188). References 1. Zhang GJ, Zhou T, Tian HP, et al. High expression of ZEB1 correlates with liver metastasis and poor prognosis in colorectal cancer. Oncol Lett 2013;5: Torre LA, Bray F, Siegel RL, et al. Global cancer statistics, CA-CANCER J CLIN 2015;65: Hohenberger W, Weber K, Matzel K, et al. Standardized surgery for colonic cancer: complete mesocolic excision and central ligation--technical notes and outcome. Colorectal Dis 2009;11:354-64; discussion Jacobs M, Verdeja JC, Goldstein HS. Minimally invasive colon resection (laparoscopic colectomy). Surg Laparosc Endosc 1991;1: Kim WR, Baek SJ, Kim CW, et al. Comparative study of oncologic outcomes for laparoscopic vs. open surgery in transverse colon cancer. Ann Surg Treat Res 2014;86:28-34.
7 Chinese Clinical Oncology, Vol 6, No 1 February 2017 Page 7 of 7 6. Gao F, Cao YF, Chen LS. Meta-analysis of short-term outcomes after laparoscopic resection for rectal cancer. Int J Colorectal Dis 2006;21: Pecorelli N, Amodeo S, Frasson M, et al. Ten-year outcomes following laparoscopic colorectal resection: results of a randomized controlled trial. Int J Colorectal Dis 2016;31: Colon Cancer Laparoscopic or Open Resection Study Group, Buunen M, Veldkamp R, et al. Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 2009;10: Clinical Outcomes of Surgical Therapy Study Group. A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 2004;350: Okuda J, Yamamoto M, Tanaka K, et al. Laparoscopic resection of transverse colon cancer at splenic flexure: technical aspects and results. Updates Surg 2016;68: Hahn KY, Baek SJ, Joh YG, et al. Laparoscopic resection of transverse colon cancer: long-term oncologic outcomes in 58 patients. J Laparoendosc Adv Surg Tech A 2012;22: Agarwal S, Gincherman M, Birnbaum E, et al. Comparison of long-term follow up of laparoscopic versus open colectomy for transverse colon cancer. Proc (Bayl Univ Med Cent) 2015;28: Nakanishi M, Kokuba Y, Murayama Y, et al. A new approach to laparoscopic lymph node excision in cases of transverse colon cancer. Digestion 2012;85: Athanasiou CD, Markides GA, Kotb A, et al. Open compared with laparoscopic complete mesocolic excision with central lymphadenectomy for colon cancer: a systematic review and meta-analysis. Colorectal Dis 2016;18:O Chand M, Siddiqui MRS, Rasheed S, et al. A systematic review and meta-analysis evaluating the role of laparoscopic surgical resection of transverse colon tumours. Surg Endosc 2014;28: Storli KE, Søndenaa K, Furnes B, et al. Outcome after introduction of complete mesocolic excision for colon cancer is similar for open and laparoscopic surgical treatments. Dig Surg 2013;30: Bae SU, Saklani AP, Lim DR, et al. Laparoscopic-assisted versus open complete mesocolic excision and central vascular ligation for right-sided colon cancer. Ann Surg Oncol 2014;21: Huang JL, Wei HB, Fang JF, et al. Comparison of laparoscopic versus open complete mesocolic excision for right colon cancer. Int J Surg 2015;23: Markman M. Intraperitoneal chemotherapy in the management of colon cancer. Semin Oncol 1999;26: Zhuchenko AP, Kalganov ID, Filon AF. Cytoreductive surgery with intraperitoneal chemotherapy in patients with colon cancer and peritoneal carcinomatosis. Antibiot Khimioter 2003;48: Nadler A, McCart JA, Govindarajan A. Peritoneal Carcinomatosis from Colon Cancer: A Systematic Review of the Data for Cytoreduction and Intraperitoneal Chemotherapy. Clin Colon Rectal Surg 2015;28: Law WL, Chu KW, Tung PH. Laparoscopic colorectal resection: a safe option for elderly patients. J Am Coll Surg 2002;195: Cite this article as: Wang Y, Zhang C, Feng YF, Fu Z, Sun YM. Comparison of short-term outcomes between laparoscopic-assisted and open complete mesocolic excision (CME) for the treatment of transverse colon cancer. Chin Clin Oncol 2017;6(1):6. doi: /cco
Laparoscopic extended right hemicolectomy with D3
 Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Clinical outcome of laparoscopic complete mesocolic excision in the treatment of right colon cancer
 Wang et al. World Journal of Surgical Oncology (2017) 15:174 DOI 10.1186/s12957-017-1236-y RESEARCH Open Access Clinical outcome of laparoscopic complete mesocolic excision in the treatment of right colon
Wang et al. World Journal of Surgical Oncology (2017) 15:174 DOI 10.1186/s12957-017-1236-y RESEARCH Open Access Clinical outcome of laparoscopic complete mesocolic excision in the treatment of right colon
Laparoscopic extended right hemicolectomy with D3 lymphadenectomy
 Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Li Yang, Diancai Zhang, Fengyuan Li, Xiang Ma. Introduction
 Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Komplette Mesokolische Exzision (CME) Ergebnisse und Ausblicke
 Komplette Mesokolische Exzision (CME) Ergebnisse und Ausblicke Werner Hohenberger Chirurgische Universitätsklinik Erlangen Friedrich-Alexander-Universität Erlangen-Nürnberg Colon Cancer Cancer related
Komplette Mesokolische Exzision (CME) Ergebnisse und Ausblicke Werner Hohenberger Chirurgische Universitätsklinik Erlangen Friedrich-Alexander-Universität Erlangen-Nürnberg Colon Cancer Cancer related
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer
 Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominoperineal excision, of rectal cancer, 93 111 current controversies in, 106 109 extent of perineal dissection and removal of pelvic floor,
Note: Page numbers of article titles are in boldface type. A Abdominoperineal excision, of rectal cancer, 93 111 current controversies in, 106 109 extent of perineal dissection and removal of pelvic floor,
Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in 106 patients with advanced gastric cancer
 JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Colon Cancer Surgery
 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
A study evaluating the safety of laparoscopic radical operation for colorectal cancer
 Original Article A study evaluating the safety of laparoscopic radical operation for colorectal cancer Min-Hua Zheng, Ai-Guo Lu, Bo Feng, Yan-Yan Hu, Jian-Wen Li, Ming-Liang Wang, Feng Dong, Jing-Li Cai,
Original Article A study evaluating the safety of laparoscopic radical operation for colorectal cancer Min-Hua Zheng, Ai-Guo Lu, Bo Feng, Yan-Yan Hu, Jian-Wen Li, Ming-Liang Wang, Feng Dong, Jing-Li Cai,
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
Complete mesocolic excision for colon cancer is technically challenging but the most oncological appealing
 Editorial Complete mesocolic excision for colon cancer is technically challenging but the most oncological appealing Ionut Negoi 1,2, Mircea Beuran 1,2, Sorin Hostiuc 1,3, Massimo Sartelli 4, Federico
Editorial Complete mesocolic excision for colon cancer is technically challenging but the most oncological appealing Ionut Negoi 1,2, Mircea Beuran 1,2, Sorin Hostiuc 1,3, Massimo Sartelli 4, Federico
COLON AND RECTAL CANCER
 COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
Current innovations in colorectal surgery
 Current innovations in colorectal surgery KS Chapple Consultant Colorectal Surgeon Sheffield Teaching Hospitals NHS Trust Do we need more innovations? What innovations are there and are they worthwhile?
Current innovations in colorectal surgery KS Chapple Consultant Colorectal Surgeon Sheffield Teaching Hospitals NHS Trust Do we need more innovations? What innovations are there and are they worthwhile?
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
New ports placement in laparoscopic central lymph nodes dissection with left colic artery preservation for sigmoid colon and rectal cancer
 223 ORIGINAL New ports placement in laparoscopic central lymph nodes dissection with left colic artery preservation for sigmoid colon and rectal cancer Jun Higashijima, Mitsuo Shimada, Takashi Iwata, Kozo
223 ORIGINAL New ports placement in laparoscopic central lymph nodes dissection with left colic artery preservation for sigmoid colon and rectal cancer Jun Higashijima, Mitsuo Shimada, Takashi Iwata, Kozo
Clinical Study Laparoscopic versus Open Surgery for Colorectal Cancer: A Retrospective Analysis of 163 Patients in a Single Institution
 Minimally Invasive Surgery, Article ID 530314, 6 pages http://dx.doi.org/10.1155/2014/530314 Clinical Study Laparoscopic versus Open Surgery for Colorectal Cancer: A Retrospective Analysis of 163 Patients
Minimally Invasive Surgery, Article ID 530314, 6 pages http://dx.doi.org/10.1155/2014/530314 Clinical Study Laparoscopic versus Open Surgery for Colorectal Cancer: A Retrospective Analysis of 163 Patients
COLON AND RECTAL CANCER
 No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
Kurumboor Prakash, N P Kamalesh, K Pramil, I S Vipin, A Sylesh, Manoj Jacob
 Original Article Does case selection and outcome following laparoscopic colorectal resection change after initial learning curve? Analysis of 235 consecutive elective laparoscopic colorectal resections
Original Article Does case selection and outcome following laparoscopic colorectal resection change after initial learning curve? Analysis of 235 consecutive elective laparoscopic colorectal resections
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for Unroofing of Hepatic Cysts
 SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
Laparoscopic Resection Of Colon & Rectal Cancers. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
LONG TERM OUTCOME OF ELECTIVE SURGERY
 LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
11/21/13 CEA: 1.7 WNL
 Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips
 Review Article Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips Ru-Hong Tu, Ping Li, Jian-Wei Xie, Jia-Bin Wang, Jian-Xian Lin, Jun Lu, Qi-Yue Chen, Long-Long
Review Article Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips Ru-Hong Tu, Ping Li, Jian-Wei Xie, Jia-Bin Wang, Jian-Xian Lin, Jun Lu, Qi-Yue Chen, Long-Long
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Laparoscopic Right Colectomy
 Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Anatomy of the Large Intestine
 Large intestine Anatomy of the Large Intestine 2 Large Intestine Extends from ileocecal valve to anus Length = 1.5-2.5m = 5 feet Regions Cecum = 2.5-3 inch Appendix= 3-5 inch Colon Ascending= 5 inch Transverse=
Large intestine Anatomy of the Large Intestine 2 Large Intestine Extends from ileocecal valve to anus Length = 1.5-2.5m = 5 feet Regions Cecum = 2.5-3 inch Appendix= 3-5 inch Colon Ascending= 5 inch Transverse=
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
How much colon should be resected?
 Colon Cancer Surgical Standard of Care and Operative Techniques Madhulika G. Varma MD Professor and Chief Section of Colorectal Surgery University of California, San Francisco How much colon should be
Colon Cancer Surgical Standard of Care and Operative Techniques Madhulika G. Varma MD Professor and Chief Section of Colorectal Surgery University of California, San Francisco How much colon should be
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018)
 2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018) Clinical Study on the Treatment of Metastatic Malignant Bowel Obstruction with Transgastric Intestinal Obstruction
2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018) Clinical Study on the Treatment of Metastatic Malignant Bowel Obstruction with Transgastric Intestinal Obstruction
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Impact of conversion during laparoscopic gastrectomy on outcomes of patients with gastric cancer
 JBUON 2017; 22(4): 926-931 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Impact of conversion during laparoscopic gastrectomy on outcomes of
JBUON 2017; 22(4): 926-931 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Impact of conversion during laparoscopic gastrectomy on outcomes of
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer
 Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Original Article A preliminary comparison of clinical efficacy between laparoscopic and open surgery for the treatment of colorectal cancer
 Int J Clin Exp Med 2016;9(1):341-345 www.ijcem.com /ISSN:1940-5901/IJCEM0015805 Original Article A preliminary comparison of clinical efficacy between laparoscopic and open surgery for the treatment of
Int J Clin Exp Med 2016;9(1):341-345 www.ijcem.com /ISSN:1940-5901/IJCEM0015805 Original Article A preliminary comparison of clinical efficacy between laparoscopic and open surgery for the treatment of
Locally Advanced Colon Cancer. Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery
 Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer: a prospective randomized study
 Int J Clin Exp Med 2017;10(3):5001-5010 www.ijcem.com /ISSN:1940-5901/IJCEM0042542 Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer:
Int J Clin Exp Med 2017;10(3):5001-5010 www.ijcem.com /ISSN:1940-5901/IJCEM0042542 Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer:
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
DIVERTICULAR DISEASE. Dr. Irina Murray Casanova PGY IV
 DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic Surgery for Colorectal Disease
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM
 OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
Single incision vs conventional laparoscopic anterior resection for sigmoid colon cancer: a case-matched study
 The American Journal of Surgery (2013) 206, 320-325 Clinical Science Single incision vs conventional laparoscopic anterior resection for sigmoid colon cancer: a case-matched study Seung-Jin Kwag, M.D.,
The American Journal of Surgery (2013) 206, 320-325 Clinical Science Single incision vs conventional laparoscopic anterior resection for sigmoid colon cancer: a case-matched study Seung-Jin Kwag, M.D.,
Survival after Complete Mesocolic Excision (CME) for Right Sided Coloncancer Compared to Standard Surgery
 Send Orders for Reprints to reprints@benthamscience.net 6 The Open Surgery Journal, 213, 7, 6-1 Open Access Survival after Complete Mesocolic Excision () for Right Sided Coloncancer Compared to Standard
Send Orders for Reprints to reprints@benthamscience.net 6 The Open Surgery Journal, 213, 7, 6-1 Open Access Survival after Complete Mesocolic Excision () for Right Sided Coloncancer Compared to Standard
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Laparoscopy assisted versus open surgery for multiple colorectal cancers with two anastomoses: a cohort study
 DOI 10.1186/s40064-016-1948-4 RESEARCH Open Access Laparoscopy assisted versus open surgery for multiple colorectal cancers with two anastomoses: a cohort study Hiroaki Nozawa *, Soichiro Ishihara, Koji
DOI 10.1186/s40064-016-1948-4 RESEARCH Open Access Laparoscopy assisted versus open surgery for multiple colorectal cancers with two anastomoses: a cohort study Hiroaki Nozawa *, Soichiro Ishihara, Koji
Management of Perforated Colon Cancers
 Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
The Learning Curve for Minimally Invasive Esophagectomy
 The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
Patient Presentation. 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201
 Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Single port laparoscopic colectomy for colonic cancer
 Single port laparoscopic colectomy for colonic cancer Trung Vy Pham, Nhu Hiep Pham *, Huu Thien Ho, Anh Vu Pham, Hai Thanh Phan, Thanh Xuan Nguyen, Nghiem Trung Tran, Xuan Dong Pham, Tien Nhan Van, Trung
Single port laparoscopic colectomy for colonic cancer Trung Vy Pham, Nhu Hiep Pham *, Huu Thien Ho, Anh Vu Pham, Hai Thanh Phan, Thanh Xuan Nguyen, Nghiem Trung Tran, Xuan Dong Pham, Tien Nhan Van, Trung
Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera.
 Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera. Layers of the peritoneum: 1. Outer Layer ( Parietal Peritoneum) : lines
Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera. Layers of the peritoneum: 1. Outer Layer ( Parietal Peritoneum) : lines
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Laparoscopic-assisted total gastrectomy for early gastric cancer with situs inversus totalis: report of a first case
 Morimoto et al. BMC Surgery (2015) 15:75 DOI 10.1186/s12893-015-0059-4 CASE REPORT Open Access Laparoscopic-assisted total gastrectomy for early gastric cancer with situs inversus totalis: report of a
Morimoto et al. BMC Surgery (2015) 15:75 DOI 10.1186/s12893-015-0059-4 CASE REPORT Open Access Laparoscopic-assisted total gastrectomy for early gastric cancer with situs inversus totalis: report of a
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Karen Lok Man Tung, Michael Ka Wah Li. Introduction
 Original Article Page 1 of 5 Hybrid natural orifice transluminal endoscopic surgery colectomy versus conventional laparoscopic colectomy for left-sided colonic tumors: intermediate follow up of a randomized
Original Article Page 1 of 5 Hybrid natural orifice transluminal endoscopic surgery colectomy versus conventional laparoscopic colectomy for left-sided colonic tumors: intermediate follow up of a randomized
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Guidelines for Extended Lymphadenectomy in Gastric Cancer: A Prospective Comparative Study
 Ann Surg Oncol DOI 10.1245/s10434-012-2544-7 ORIGINAL ARTICLE GASTROINTESTINAL ONCOLOGY Guidelines for Extended Lymphadenectomy in Gastric Cancer: A Prospective Comparative Study Oktar Asoglu, MD 1, Tugba
Ann Surg Oncol DOI 10.1245/s10434-012-2544-7 ORIGINAL ARTICLE GASTROINTESTINAL ONCOLOGY Guidelines for Extended Lymphadenectomy in Gastric Cancer: A Prospective Comparative Study Oktar Asoglu, MD 1, Tugba
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
Robotic-assisted left inferior lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
[A RESEARCH COORDINATOR S GUIDE]
![[A RESEARCH COORDINATOR S GUIDE] [A RESEARCH COORDINATOR S GUIDE]](/thumbs/88/117127924.jpg) 2013 COLORECTAL SURGERY GROUP Dr. Carl J. Brown Dr. Ahmer A. Karimuddin Dr. P. Terry Phang Dr. Manoj J. Raval Authored by Jennifer Lee A cartoon about colonoscopies. 1 [A RESEARCH COORDINATOR S GUIDE]
2013 COLORECTAL SURGERY GROUP Dr. Carl J. Brown Dr. Ahmer A. Karimuddin Dr. P. Terry Phang Dr. Manoj J. Raval Authored by Jennifer Lee A cartoon about colonoscopies. 1 [A RESEARCH COORDINATOR S GUIDE]
The Feasibility of Laparoscopic Surgery Compared to Open Surgery in Patients with T4 Colorectal Cancer Staged by Preoperative Computed Tomography
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 216;19(1):32-38 Journal of Minimally Invasive Surgery The Feasibility of Laparoscopic Surgery Compared to Open Surgery in Patients
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 216;19(1):32-38 Journal of Minimally Invasive Surgery The Feasibility of Laparoscopic Surgery Compared to Open Surgery in Patients
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Comparison of lymph node number and prognosis in gastric cancer patients with perigastric lymph nodes retrieved by surgeons and pathologists
 Original Article Comparison of lymph node number and prognosis in gastric cancer patients with perigastric lymph nodes retrieved by surgeons and pathologists Lixin Jiang, Zengwu Yao, Yifei Zhang, Jinchen
Original Article Comparison of lymph node number and prognosis in gastric cancer patients with perigastric lymph nodes retrieved by surgeons and pathologists Lixin Jiang, Zengwu Yao, Yifei Zhang, Jinchen
Laparoscopic right-sided colon resection for colon cancer has the control group so far been chosen correctly?
 Pelz et al. World Journal of Surgical Oncology (2018) 16:117 https://doi.org/10.1186/s12957-018-1417-3 RESEARCH Open Access Laparoscopic right-sided colon resection for colon cancer has the control group
Pelz et al. World Journal of Surgical Oncology (2018) 16:117 https://doi.org/10.1186/s12957-018-1417-3 RESEARCH Open Access Laparoscopic right-sided colon resection for colon cancer has the control group
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
The jejunum and the Ileum. Prof. Oluwadiya KS
 The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
Mousa Salah. Dr. Mohammad Al. Mohtasib. 1 P a g e
 8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Laparoscopic Colorectal Surgery
 Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
Comparative study of oncologic outcomes for laparo scopic vs. open surgery in transverse colon cancer
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.86.1.28 Annals of Surgical Treatment and Research Comparative study of oncologic outcomes for laparo scopic vs. open
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.86.1.28 Annals of Surgical Treatment and Research Comparative study of oncologic outcomes for laparo scopic vs. open
Stage III Colon Cancer Susquehanna Cancer Center Warren L Robinson, MD, FACP May 9, 2007
 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Warren L Robinson, MD, FACP May 9, 27 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Colorectal cancer is the third most common cancer
Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Warren L Robinson, MD, FACP May 9, 27 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Colorectal cancer is the third most common cancer
