BILLIARY DRAINAGE IN OBSTRUCTIVE JAUNDICE
|
|
|
- Lesley George
- 6 years ago
- Views:
Transcription
1 BILLIARY DRAINAGE IN OBSTRUCTIVE JAUNDICE N. Kolev, V. Ignatov, A. Tonev, A. Zlatarov, T. Kirilova, V. Bozhkov, K. Ivanov ABSTRACT First Clinic of Surgery, St. Marina University Hospital of Varna reviews In patients with obstructive jaundice, when the endoscopic approach fails to achieve biliary drainage, percutaneous cannulation and combined endoscopic/percutaneous endoprosthesis insertion can simultaneously or subsequently be performed. The present study compares these two approaches. Endoscopic retrograde biliary drainage (ERBD) and percutaneous transhepatic biliary drainage (PTBD) are the two main non-surgical treatment options for obstructive jaundice in patients with hepatocellular carcinoma (HCC). ERBD is usually the first-line treatment because of its low hemorrhage risk. Some authors have reported that the successful drainage rate ranges from 72 to 100%. Mean stent patency time and mean survival range from 1,0 to 15,9 and from 2,8 to 12,3 months, respectively. PTBD is often an important second-line treatment when ERBD is impossible. With regard to materials, metallic stents offer the benefit of longer patency than plastic stents. The dominant effect of biliary drainage suggests that successful jaundice therapy could enhance anticancer treatment by increasing the life expectancy, decreasing the mortality, or both. We present an overview of the efficacy of ERBD and PTBD for obstructive jaundice in HCC patients who are not candidates for surgical resection and summarize the current indications and outcomes of reported clinical use. Traditionally, surgical techniques have been used, however, in the last 20 years the availability of both endoscopic and interventional radiological procedures has increased. Тhe technical success of the procedure depends on the experience of the interventional radiologist performing the drainage. It can be as high as nearly 100%. Clinical efficacy is usually lower but still over 90%. When endoscopic drainage alone fails, a combined percutaneous/endoscopic procedure should only be performed if it can be carried out simultaneously. Key words: biliary drainage, obstructive jaundice, percutaneous transhepatic biliary drainage, endoscopic retrograde biliary drainage, hepatocellular carcinoma Introduction Controversy exists concerning the preferred technique of percutaneous biliary drainage (PBD), either via endoscopic retrograde biliary drainage (ERBD) or by means of antegrade percutaneous transhepatic biliary drainage (PTBD) (42). PTBD is the preferred method in Japan for relief of obstructive jaundice due to proximal obstruction. In Europe and the USA, endoscopic biliary drainage (EBD) is usually performed as primary intervention and is followed by PTBD only when EBD has failed. Address for correspondence: N. Kolev, MD, PhD, DSc First Clinic of Surgery St. Marina University Hospital of Varna 1 Hristo Smirnenski Str., 9010 Varna, Bulgaria kolevsurgery@yahoo.com Internal drainage by EBD, although a less invasive technique, carries increased risk of developing cholangitis due to bacterial contamination from the duodenum and increased risk of procedure-related complications such as duodenal perforation and post-ebd acute pancreatitis (12,22). Drainage by means of PTBD is associated with hemobilia, portal vein thrombosis, cancer seeding and potentially more patient s discomfort (2). Three published prospective randomized controlled trials comparing EBD versus PTBD include patients with unresectable bile duct tumours or carcinoma of the gallbladder and pancreas showing conflicting results. These studies address palliative treatment and although important in the context of biliary drainage, no distinction is made between distal and proximal bile duct obstruction. In patients with HCC with involvement of the segmental biliary ducts, drainage 29
2 Biliary drainage in obstructive jaundice of the intrahepatic biliary tree is challenging and mostly requires multiple drains or stents. However, in patients with a distal bile duct obstruction, usually caused by a tumour in the region of the pancreatic head, drainage is more straightforward and requires a single drain or stent. In the latter category of jaundiced patients in whom partial liver resection is usually not undertaken, PBD remains a controversial issue (11). To date, there are no studies regarding the optimal route of drainage in patients with a potentially resectable HCC. Therefore, the aim of the present study is to compare the success rate and complications of ERBD and PTBD in patients eligible for resection of a suspected HCC. Diagnostic percutaneous transhepatic cholangiography gradually develops into a technique, which allows prolonged external catheter drainage of malignant strictures in the biliary system (18). Further developments include percutaneous placement of multiple side-hole catheters into the duodenum, thereby establishing the internal bile drainage (28). Early series show a considerable number of infectious complications (approximately 40%), but further refinements produce better results (26). Percutaneous biliary drainage The technique we currently routinely use involves the use of ultrasound guidance, a thin Chiba needle and a inch guide-wire to gain access to the biliary system. A sheath is then placed over an 0.35-inch guide-wire and strictures are negotiated using standard 5-French angiographic catheters and hydrophylic guide-wires. For permanent stenting self-expandable metallic stents are used. Metal selfexpandable stents are the standard in PTBD and thus being preferred over plastic endoprostheses. Metal stents have higher patency rates than plastic ones and in case of recurrent obstruction a new stent can easily be placed in the blocked metal stent, without having to remove the old one (as opposed to plastic stents) (26). Metal stents are associated with shorter hospital stay and lower cost than plastic stents (16,22,23). A new development is the use of covered stents, which aim at reducing the incidence of recurrent jaundice by preventing tumour ingrowth into the stent. Although tumour ingrowth is probably prevented to some extent by the covering of these stents, it is 30 unclear whether clogging is also prevented (3,14,27, 34). Potential drawbacks of such stents are the increased chance of stent migration, occlusion of side-branches, when stenting hilar lesions, and occlusion of the cystic duct, potentially leading to cholecystitis. Another concern is the potential lack of costeffectiveness of the use of such stents. Currently, there is not enough evidence to support the routine use of covered stents in malignant bile duct obstruction, although in selected cases these may be useful. At least as important as advances in PTBD technique are the improvements, which are made in pre-procedure planning by imaging with ultrasound, computed tomography (CT) and magnetic resonance cholangiopancreatography (MRCP). Particularly when performing drainage and stenting of hilar obstruction, treatment planning on the basis of imaging is crucial (10). PTBD should never be performed without a proper non-invasive evaluation of the biliary tree. Surgical versus non-surgical biliary drainage Surgical biliary bypass is often performed when exploratory laparotomy for a tumour of the pancreatic head region shows unresectability of the tumour. Adequate decompression of the biliary tree can be obtained by performing a hepatico-jejunostomy and a gastric bypass is performed simultaneously. This prevents the need for an additional laparotomy later in the course of the disease when gastric outlet obstruction may develop as a result of local tumour progression. However, mortality and morbidity rates of this double bypass procedure remain considerable, as they range from 2% to 5%, and from 17% to 37%, respectively (24,25,40). Several randomized trials compare surgical with non-surgical drainage (mostly performed endoscopically) in patients with pancreatic head carcinoma (1,15,37). Surgical treatment is associated with higher postoperative mortality and morbidity rates and a longer hospital stay than non-surgical drainage (mostly performed endoscopically), but recurrent jaundice requiring stent exchange and late duodenal obstruction are more common in the non-surgical drainage group (15,35). Similarly, a randomized study comparing percutaneous biliary drainage with surgical bypass in patients with unresectable pancreatic head cancer demonstrates successful drainage in all the patients,
3 N. Kolev, V. Ignatov, A. Tonev et al. but there are higher 30-day mortality and procedurerelated mortality as well as a longer hospital stay in the surgical group. These advantages of percutaneous drainage are partly annihilated by the higher number of readmissions for recurrent jaundice and duodenal obstruction requiring surgery (4). The endoscopic stent placement is more cost-effective than surgical biliary drainage, although frequent stent exchanges were necessary in the non-surgical group (32). It is currently accepted to consider surgical biliary drainage only in patients with pancreatic head cancer who are in an otherwise good condition and who have a life expectancy of more than 6 months (38). This means that surgical drainage is only performed in patients who undergo an exploratory laparotomy and are unresectable. The advent of duodenal stenting in addition to biliary stenting may obviate the need for surgical treatment of gastric outlet obstruction and this may further expand indications for biliary stenting in the near future. Currently, prospective studies comparing combined biliary and duodenal stenting versus surgery are lacking and the results of such studies should be awaited (39). A different situation occurs in the patients with malignant obstruction at the hilum. Patients with Bismuth type I and II lesions are surgical candidates. Resection of a type III lesion often requires major surgery and only a minority of these patients will eventually undergo resection. Type IV lesions are generally considered to be irresectable. In patients with unresectable hilar cholangiocarcinoma, performing a hepaticojejunostomy at the hilum is technically difficult and associated with higher complication and mortality rates than non-surgical stenting (20,29). In addition, gastric outlet obstruction is an uncommon sequelae of hilar cholangiocarcinoma and surgery for this complication is, therefore, only rarely required. Thus, non-surgical drainage of the biliary system is the preferred treatment option in the vast majority of patients with unresectable hilar malignancy (36). Percutaneous versus endoscopic biliary drainage When comparing percutaneous and endoscopic treatment, distal and proximal bile duct obstruction should be distinguished again. However, in a two prospective randomized trials comparing PTBD and endoscopic retrograde cholangiopancreatography (ERCP) for palliation of inoperable malignancy causing bile duct obstruction, this distinction has not been made (17,33). PTBD with self-expanding metal stents is compared with conventional endoscopic polyethylene endoprostheses (EPE) which reflects current practice in most institutions (31). The technical success rates of both procedures are similar (PTBD, 75% and EPE, 58%; p=0,29), whereas therapeutic success is higher in the PTBD group (71% versus 42%; p=0,03). Major complications are more common in the this group (61% versus 35%; p=0,09) but does not account for differences in 30- day mortality rates (PTBD, 36% and EPE, 42%; p=0,83). Overall median survival is significantly higher in the PTBD group than in the EPE one (3,7 versus 2,0 months; p=0,02). In the majority of patients (7/11) in whom endoscopic stent placement fails, subsequent percutaneous stent placement is successful. It is concluded that PTBD with placement of a self-expanding metal stent is an alternative to placement of an EPE. Numerous non-comparative studies assessing PTBD and ERCP for treatment of distal bile duct obstruction suggest that there are no significant differences in technical success rates between percutaneous and endoscopic treatment (6,7,19). Complication and mortality rates are comparable, although the type of complications differs. Pancreatitis is more often seen after ERCP, whereas bile leakage is more frequently seen after PTBD. An advantage of ERCP over PTBD is the absence of a percutaneous drainage tube, which may be uncomfortable for the patient and requires removal after several days in most cases. Futhermore, PTBD may be painful in some patients, but patient s preference for either technique has not been studied. Success and complication rates for both ERCP and PTBD depend on the operator s skills and experience and this may influence the choice for one of these techniques in different institutions. In most centres, ERCP is used as the primary procedure for palliative stenting of malignant distal bile duct obstruction. Until recently, ERCP is considered an important diagnostic tool for assessment of patients with malignant distal bile duct obstruction, too. Its diagnostic role is now replaced by ultrasound, CT, and MRCP almost completely and the only diagnostic value of ERCP lies in its ability to obtain brush cytology of suspected lesions. In spite of the 31
4 Biliary drainage in obstructive jaundice evidence of superior patency of metallic stents, plastic endoprostheses are usually inserted during ERCP only to be replaced by metallic stents when they occlude after short intervals (6,41). As a result, frequent stent exchanges are necessary using this approach and this may counterbalance the short term cost benefit of applying the plastic stents (13,43). In current practice, PTBD in distal bile duct obstruction is mostly reserved for cases where ERCP fails or is impossible. The most common reasons for this are duodenal stenosis, failure to pass the biliary stricture or to cannulate the papilla (e.g. because of its position in a duodenal diverticulum), altered anatomy after surgery (B2 stomach), or prior creation of a bilioenteric anastomosis. In most of such cases, PTBD is technically successful and PTBD use as a secondary tool after failure of or inability to perform ERCP is widely accepted. In hilar obstruction, the situation is less clear and both PTBD and ERCP are used as a primary drainage modality in different institutions. PTBD has a distinct advantage over ERCP in that with ultrasound guidance one or more appropriate segments for drainage can be chosen and injection of contrast matter in segments too small to be drained can be prevented. As stated before, ultrasound guidance during PTBD is extremely useful in such patients. Furthermore, negotiating the hilar strictures and draining the appropriate segments can be very difficult with ERCP and success rates are lower than for distal strictures (5,8). Whether PTBD or ERCP is used as the primary tool in patients with hilar obstruction depends on specific patient s circumstances and the referring physician s preference as well as on local availability and expertise. As hilar cholangiocarcinoma is a relatively rare tumour and both percutaneous and endoscopic palliations require considerable expertise, it is probably useful to concentrate. In conclusion, the technical success of the procedure depends on the experience of the interventional radiologist performing the drainage. It can be as high as nearly 100%. Clinical efficacy is usually lower but still over 90%. When endoscopic drainage alone fails, a combined percutaneous/ endoscopic procedure should only be performed if it can be carried out simultaneously. 32 References 1. Andersen, J. R., S. M. Sorensen, A. Kruse, M. Rokkjaer, P. Matzen. Randomised trial of endoscopic endoprosthesis versus operative bypass in malignant obstructive jaundice.- Gut, 30, 1989, No 8, Arner, O., S. Hagsberg, S. I. Seldinger. Percutaneous transhepatic cholangiography: puncture of dilated and non-dilated bile ducts under roentgen televison control.- Surgery, 52, 1962, Bezzi, M., A. Zolovkins, V. Cantisani, F. M. Salvatori, M. Rossi, F. Fanelli, et al. New eptfe/ FEP-covered stent in the palliative treatment of malignant biliary obstruction.- J. Vasc. Interv. Radiol., 13, 2002, No 6, Bornman, P. C., E. P. Harries-Jones, R. Tobias, G. Van Stiegmann, J. Terblanche. Prospective controlled trial of transhepatic biliary endoprosthesis versus bypass surgery for incurable carcinoma of head of pancreas.- Lancet, 1, 1986, No 8472, Cheng, J. L., M. J. Bruno, J. J. Bergman, E. A. Rauws, G. H. Tytgat, K. Huibregtse. Endoscopic palliation of patients with biliary obstruction caused by nonresectable hilar cholangiocarcinoma: efficacy of self-expandable metallic Wallstents.- Gastrointest. Endosc., 56, 2002, No 1, Davids, P. H., A. G. Groen, E. A. Rauws, G. N. Tytgat, K. Huibregste. Randomized trial of selfexpanding metal stents versus polyethylene stents for distal malignant biliary obstruction.- Lancet, 340, 1992, No , Dowsett, J. F., S. J. Williams, A. R. Hatfield, D. Vaira, C. Ainley, A. A. Polydorou, et al. Endoscopic management of low biliary obstruction due to inresectable primary pancreato-biliary malignancy. A review of 463 consecutive cases.- Gastroenterology, 96, 1989, A Ducreux, M., C. Liguory, J. F. Lefebvre, O. Ink, A. Choury. Management of malignant hilar biliary obstruction by endoscopy. Results and prognostic factors.- Dig. Dis. Sci., 37, 1992, No 5, Ferruci, J. T., Jr, P. R. Mueller, W. P. Harbin. Percutaneous transhepatic biliary drainage.- Radiology, 135, 1980, No Freeman, M. L., C. Overby. Selective MRCP and CT-targeted drainage of malignant hilar biliary obstruction with self-expanding metallic stents.- Gastrointest. Endosc., 58, 2003, No 1,
5 N. Kolev, V. Ignatov, A. Tonev et al. 11. Glenn, F., J. A. Evans, Z. Mujahed, B. Thorbjarnson. Percutaneous transhepatic cholangiography.- Ann. Surg., 156, 1962, Günther, R. W., H. Schild, M. Thelen. Percutaneous transhepatic biliary drainage: experience with 311 procedures.- Cardiovasc. Intervent. Radiol., 11, 1988, No 2, Harewood, G. C., T. H. Baron, A. J. LeRoy, B. T. Petersen. Cost-effectiveness analysis of alternative strategies for palliation of distal biliary obstruction after a failed cannulation attempt.- Am. J. Gastroenterol., 97, 2002, No 7, Hausegger, K. A., S. Thurnher, G. Bodendorfer, C. L. Zollikofer, M. Uggowitzer, C. Kugler, et al. Treatment of malignant biliary obstruction with polyurethane-covered Wallstents.- Am. J. Roentgenol., 170, 1998, No 2, Hyöty, M. K., I. H. Nordback. Biliary stent or surgical bypass in unresectable pancreatic cancer with obstructive jaundice.- Acta Chir. Scand., 156, 1990, No 5, Indar AA, Lobo DN, Gilliam AD, Gregson R, Davidson I, Whittaker S, et al. Percutaneous biliary metal wall stenting in malignant obstructive jaundice.- Eur. J. Gastroenterol. Hepatol., 15, 2003, No 8, Jarnagin, W. R., M. Shoup. Surgical management of cholangiocarcinoma.- Semin. Liver Dis., 24, 2004, No 2, Kaude, J. V., C. H. Weidenmier, O. F. Agee. Decompression of bile ducts with the percutaneous transhepatic technique.- Radiology, 93, 1969, No 1, Kaufman, S. L. Percutaneous palliation of unresectable pancreatic cancer.- Surg. Clin. North Am., 75, 1995, No 5, Kaw, M., S. Singh, H. Gagneja, P. Azad. Role of self-expandable metal stents in the palliation of malignant duodenal obstruction.- Surg. Endosc., 17, 2003, No 4, Laméris, J. S., H. Obertop, J. Jeekel. Biliary drainage by ultrasound-guided puncture of the left hepatic duct.- Clin. Radiol., 36, 1985, No 3, Lammer, J., K. A. Hausegger, F. Fluckiger, F. W. Winkelbauer, R. Wildling, G. E. Klein, et al. Common bile duct obstruction due to malignancy: treatment with plastic versus metal stents.- Radiology, 201, 1996, No 1, Lee, B. H., D. H. Choe, J. H. Lee, K. H. Kim, S. Y. Chin. Metallic stents in malignant biliary obstruction: prospective long-term results.- Am. J. Roentgenol., 168, 1997, No 3, Lesurtel, M., N. Dehni, E. Tiret, R. Parc, F. Paye. Palliative surgery for unresectable pancreatic and periampullary cancer: a reappraisal.- J. Gastrointest. Surg., 10, 2006, No 2, Lillemoe, K. D., P. K. Sauter, H. A. Pitt, C. J. Yeo, J. L. Cameron. Current status of surgical palliation of periampullary carcinoma.- Surg. Gynecol. Obstet., 176, 1993, No 1, McPherson, G. A., J. S. Benjamin, N. A. Habib, N. B. Bowley, L. H. Blumgart. Percutaneous transhepatic drainage in obstructive jaundice: advantages and problems.- Br. J. Surg., 69, 1982, No 5, Miyayama, S., O. Matsui, Y. Akakura, T. Yamamoto, H. Nishida, K. Yoneda, et al. Efficacy of covered metallic stents in the treatment of unresectable malignant biliary obstruction.- Cardiovasc. Intervent. Radiol., 27, 2004, No 4, Molnar, W., A. E. Stockum. Relief of obstructive jaundice through percutaneous transhepatic catheter. A new therapeutic method.- Am. J. Roentgenol., 122, 1974, No 2, Moss, A. C., E. Morris, P. Mac Mathuna. Palliative biliary stents for obstructing pancreatic carcinoma.- Cochrane Database Syst. Rev., 1, 2006 Jan. 25, CD Naggar, E., E. Krag, P. Matzen. Endoscopically inserted biliary endoprosthesis in malignant obstructive jaundice. A survey of the literature.- Liver, 10, 1990, No 6, Pinol, V., A. Castelis, J. M. Bordas, M. I. Real, J. Llach, X. Montana, et al. Percutaneous selfexpanding metal stents versus endoscopic polyethylene endoprostheses for treating malignant biliary obstruction: randomized clinical trial.- Radiology, 225, 2002, No 1, Raikar, G. V., M. M. Melin, A. Ress, S. Z. Lettieri, J. J. Poterucha, D. M. Nagorney, et al. Cost-effective analysis of surgical palliation versus endoscopic stenting in the management of unresectable pancreatic cancer.- Ann. Surg. Oncol., 3, 1996, No 5, Rumalla, A., T. H. Baron. Evaluation and endoscopic palliation of cholangiocarcinoma. 33
6 Biliary drainage in obstructive jaundice Management of cholangiocarcinoma.- Dig. Dis., 17, 1999, No 4, Schoder, M., P. Rossi, R. Uflacker, M. Bezzi, A. Stadler, M. A. Funovics, et al. Malignant biliary obstruction: treatment with eptfefep-covered endoprostheses - initial technical and clinical experiences in a multicenter trial.- Radiology, 225, 2002, No 1, Shepherd, H. A., H. A. Royle, A. P. Ross, A. Diba, M. Arthur, D. Colin-Jones. Endoscopic biliary endoprosthesis in the palliation of malignant obstruction of the distal common bile duct: a randomized trial.- Br. J. Surg., 75, 1988, No 12, Singhal, D., T. M. Van Gulik, D. J. Gouma. Palliative management of hilar cholangiocarcinoma.- Surg. Oncol., 14, 2005, No 2, Smith, A. C., J. F. Dowsett, R. C. Russell, A. R. Hatfield, R. B. Cotton. Randomised trial of endoscopic stenting versus surgical bypass in malignant low bile duct obstruction.- Lancet, 344, 1994, No 8938, Taylor, M. C., R. S. McLeod, B. Langer. Biliary stenting versus bypass surgery for the palliation of malignant distal bile duct obstruction: a metaanalysis.- Liver Transpl., 6, 2000, No 3, Van den Bosch, R. P., G. P. van der Schelling, J. H. Klinkenbijl, P. G. Mulder, M. van Blankenstein, J. Jeekel. Guidelines for the application of surgery and endoprostheses in the palliation of obstructive jaundice in advanced cancer of the pancreas.- Ann. Surg., 219, 1994, No 1, Van Wagensveld, B. A., P. P. Coene, T. M. van Gulik, E. A. Rauws, H. Obertop, D. J. Gouma. Outcome of palliative biliary and gastric bypass surgery for pancreatic head carcinoma in 126 patients.- Br. J. Surg., 84, 1997, No 10, Wagner, H. J., K. Knyrim, N. Vakil, K. J. Klose. Plastic endoprostheses versus metal stents in the palliative treatment of malignant hilar biliary obstruction.- Endoscopy, 25, 1993, No 3, Yee, A. C., C. S. Ho. Percutaneous biliary drainage: a review.- Crit. Rev. Diagn. Imaging., 30, 1990, No 3, Yeoh, K. G., M. J. Zimmerman, J. T. Cunningham, P. B. Cotton. Comparative costs of metal versus plastic biliary stent strategies for malignant obstructive jaundice by decision analysis.- Gastrointest. Endosc., 49, 1999, No 4, Pt 1,
Peripancreatic carcinoma in most patients may
 Original Article / Pancreas Quality of survival in patients treated for malignant biliary obstruction caused by unresectable pancreatic head cancer: surgical versus non-surgical palliation Hyung Ook Kim,
Original Article / Pancreas Quality of survival in patients treated for malignant biliary obstruction caused by unresectable pancreatic head cancer: surgical versus non-surgical palliation Hyung Ook Kim,
Early Infectious Complications of Percutaneous Metallic Stent Insertion for Malignant Biliary Obstruction
 Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Covered biliary stents with proximal bare stent extension for the palliation of malignant biliary disease: can we reduce tumour overgrowth rate?
 Original Article Covered biliary stents with proximal bare stent extension for the palliation of malignant biliary disease: can we reduce tumour overgrowth rate? Miltiadis Krokidis 1, Adam Hatzidakis 2
Original Article Covered biliary stents with proximal bare stent extension for the palliation of malignant biliary disease: can we reduce tumour overgrowth rate? Miltiadis Krokidis 1, Adam Hatzidakis 2
Metal versus plastic stents for malignant biliary obstruction: An update meta-analysis
 Clinics and Research in Hepatology and Gastroenterology (2013) xxx, xxx xxx Available online at www.sciencedirect.com ORIGINAL ARTICLE Metal versus plastic stents for malignant biliary obstruction: An
Clinics and Research in Hepatology and Gastroenterology (2013) xxx, xxx xxx Available online at www.sciencedirect.com ORIGINAL ARTICLE Metal versus plastic stents for malignant biliary obstruction: An
Double-Stent System with Long Duodenal Extension for Palliative Treatment of Malignant Extrahepatic Biliary Obstructions: A Prospective Study
 Original Article Intervention https://doi.org/10.3348/kjr.2018.19.2.230 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2018;19(2):230-236 Double-Stent System with Long Duodenal Extension for Palliative
Original Article Intervention https://doi.org/10.3348/kjr.2018.19.2.230 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2018;19(2):230-236 Double-Stent System with Long Duodenal Extension for Palliative
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Primary patency of percutaneously inserted self-expanding metallic stents in patients with malignant biliary obstructionhpb_
 DOI:10.1111/j.1477-2574.2009.00069.x HPB ORIGINAL ARTICLE Primary patency of percutaneously inserted self-expanding metallic stents in patients with malignant biliary obstructionhpb_069 358..363 Ursula
DOI:10.1111/j.1477-2574.2009.00069.x HPB ORIGINAL ARTICLE Primary patency of percutaneously inserted self-expanding metallic stents in patients with malignant biliary obstructionhpb_069 358..363 Ursula
Self Expandable Metallic Stents in Malignant Biliary Obstruction: Safety and Efficacy
 METALLIC THE IRAQI POSTGRADUATE STENTS IN MALIGNANT MEDICAL JOURNAL BILIARY OBSTRUCTION Self Expandable Metallic Stents in Malignant Biliary Obstruction: Safety and Efficacy Rabah Hiab Asreah*,Qasim Lefta
METALLIC THE IRAQI POSTGRADUATE STENTS IN MALIGNANT MEDICAL JOURNAL BILIARY OBSTRUCTION Self Expandable Metallic Stents in Malignant Biliary Obstruction: Safety and Efficacy Rabah Hiab Asreah*,Qasim Lefta
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases
 Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Percutaneous biliary drainage: complications and efficiency at short and mean terms: about 50 cases Poster No.: C-1497 Congress: ECR 2016 Type: Scientific Exhibit Authors: M. Matri, L. Ben Farhat, I. Marzouk
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
 Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1
 Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1 Kyu-Hong Park, M.D., Soon Gu Cho, M.D., Sung-Gwon Kang, M.D. 1,2, Don Haeng Lee, M.D. 3, Woo Cheol Kim, M.D. 4,
Intraluminal Brachytherapy after Metallic Stent Placement in Primary Bile Duct Carcinoma 1 Kyu-Hong Park, M.D., Soon Gu Cho, M.D., Sung-Gwon Kang, M.D. 1,2, Don Haeng Lee, M.D. 3, Woo Cheol Kim, M.D. 4,
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Stent Placement vs
 ORIGINAL ARTICLE Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Placement vs. Hepaticojejunostomy Marius Distler 1, Stephan
ORIGINAL ARTICLE Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Placement vs. Hepaticojejunostomy Marius Distler 1, Stephan
Clinical Study Multicenter Randomized Trial of 10-French versus 11.5-French Plastic Stents for Malignant Biliary Obstruction
 Diagnostic and Therapeutic Endoscopy Volume 2013, Article ID 891915, 6 pages http://dx.doi.org/10.1155/2013/891915 Clinical Study Multicenter Randomized Trial of 10-French versus 11.5-French Plastic Stents
Diagnostic and Therapeutic Endoscopy Volume 2013, Article ID 891915, 6 pages http://dx.doi.org/10.1155/2013/891915 Clinical Study Multicenter Randomized Trial of 10-French versus 11.5-French Plastic Stents
Paola Figueroa-Barojas, Mihir R. Bakhru, Nagy A. Habib, Kristi Ellen, Jennifer Millman, Armeen Jamal-Kabani, Monica Gaidhane, and Michel Kahaleh
 Oncology Volume 2013, Article ID 910897, 5 pages http://dx.doi.org/10.1155/2013/910897 Clinical Study Safety and Efficacy of Radiofrequency Ablation in the Management of Unresectable Bile Duct and Pancreatic
Oncology Volume 2013, Article ID 910897, 5 pages http://dx.doi.org/10.1155/2013/910897 Clinical Study Safety and Efficacy of Radiofrequency Ablation in the Management of Unresectable Bile Duct and Pancreatic
Partially Covered Metal Stents May Not Prolong Stent Patency Compared to Uncovered Stents in Unresectable Malignant Distal Biliary Obstruction
 Gut and Liver, Vol. 11, No. 3, May 217, pp. 44-446 ORiginal Article Partially Covered Metal Stents May Not Prolong Stent Patency Compared to Uncovered Stents in Unresectable Malignant Distal Biliary Obstruction
Gut and Liver, Vol. 11, No. 3, May 217, pp. 44-446 ORiginal Article Partially Covered Metal Stents May Not Prolong Stent Patency Compared to Uncovered Stents in Unresectable Malignant Distal Biliary Obstruction
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Clinical Performance of GORE VIABIL Biliary Endoprosthesis in the Treatment of Malignant Strictures
 Clinical Performance of GORE VIABIL Biliary Endoprosthesis in the Treatment of Malignant Strictures Scientific Literature Summary (n = 663 patients) * GORE VIABIL Biliary Endoprosthesis Advancing Biliary
Clinical Performance of GORE VIABIL Biliary Endoprosthesis in the Treatment of Malignant Strictures Scientific Literature Summary (n = 663 patients) * GORE VIABIL Biliary Endoprosthesis Advancing Biliary
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Placement of self-expanding metal stents is a safe and effective palliative
 Diagn Interv Radiol 2012; 18:360 364 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Placement of duodenal stents across the duodenal papilla may predispose to acute pancreatitis:
Diagn Interv Radiol 2012; 18:360 364 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Placement of duodenal stents across the duodenal papilla may predispose to acute pancreatitis:
Malignant Obstructive Jaundice has dismal
 Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Interventional Endoscopy in PB Malignancy
 Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Percutaneous transhepatic and endoscopic biliary drainage for malignant biliary tract obstruction: a meta-analysis
 Leng et al. World Journal of Surgical Oncology 2014, 12:272 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Percutaneous transhepatic and endoscopic biliary drainage for malignant biliary tract
Leng et al. World Journal of Surgical Oncology 2014, 12:272 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Percutaneous transhepatic and endoscopic biliary drainage for malignant biliary tract
Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic Cancer, Which Palliative Treatment Is Better in Developing
 Open Journal of Gastroenterology, 2017, 7, 154-164 http://www.scirp.org/journal/ojgas ISSN Online: 2163-9469 ISSN Print: 2163-9450 Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic
Open Journal of Gastroenterology, 2017, 7, 154-164 http://www.scirp.org/journal/ojgas ISSN Online: 2163-9469 ISSN Print: 2163-9450 Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer
 SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
Percutaneous Palliation of Pancreatic Head Cancer: Randomized Comparison of eptfe/fep Covered Versus Uncovered Nitinol Biliary Stents
 Cardiovasc Intervent Radiol (2011) 34:352 361 DOI 10.1007/s00270-010-9880-4 CLINICAL INVESTIGATION Percutaneous Palliation of Pancreatic Head Cancer: Randomized Comparison of eptfe/fep Covered Versus Uncovered
Cardiovasc Intervent Radiol (2011) 34:352 361 DOI 10.1007/s00270-010-9880-4 CLINICAL INVESTIGATION Percutaneous Palliation of Pancreatic Head Cancer: Randomized Comparison of eptfe/fep Covered Versus Uncovered
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series
 ORIGINAL ARTICLE Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series Yoshihiro Miyasaka, Yasuhisa Mori, Kohei Nakata, Takao Ohtsuka, Masafumi
ORIGINAL ARTICLE Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series Yoshihiro Miyasaka, Yasuhisa Mori, Kohei Nakata, Takao Ohtsuka, Masafumi
P atients with malignant biliary obstruction generally have
 729 BILIARY DISEASE A prospective randomised study of covered versus uncovered diamond stents for the management of distal malignant biliary obstruction H Isayama, Y Komatsu, T Tsujino, N Sasahira, K Hirano,
729 BILIARY DISEASE A prospective randomised study of covered versus uncovered diamond stents for the management of distal malignant biliary obstruction H Isayama, Y Komatsu, T Tsujino, N Sasahira, K Hirano,
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Review of Percutaneous Biliary Drainage in Malignant Biliary Obstruction and Accompanying Bilomas
 Article ID: WMC003123 ISSN 2046-1690 Review of Percutaneous Biliary Drainage in Malignant Biliary Obstruction and Accompanying Bilomas Corresponding Author: Dr. Bilgin Kadri Aribas, Radiologist, Department
Article ID: WMC003123 ISSN 2046-1690 Review of Percutaneous Biliary Drainage in Malignant Biliary Obstruction and Accompanying Bilomas Corresponding Author: Dr. Bilgin Kadri Aribas, Radiologist, Department
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma
 DOI:10.1111/j.1477-2574.2008.00015.x HPB ORIGINAL ARTICLE Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma Edwina N. Scott, Giuseppe Garcea, Helena Doucas, Will P. Steward,
DOI:10.1111/j.1477-2574.2008.00015.x HPB ORIGINAL ARTICLE Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma Edwina N. Scott, Giuseppe Garcea, Helena Doucas, Will P. Steward,
Endoscopic Stent Placement in the Palliation of Malignant Biliary Obstruction
 REVIEW Clin Endosc 2011;44:76-86 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2011.44.2.76 Open Access Endoscopic Stent Placement in the Palliation of Malignant Biliary Obstruction
REVIEW Clin Endosc 2011;44:76-86 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2011.44.2.76 Open Access Endoscopic Stent Placement in the Palliation of Malignant Biliary Obstruction
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Abstract Background Stent blockage is a multifactorial process in which stent design and materials, bacteria, proteins, and bile viscosity
 Gut 2000;46:395 400 395 Radiology, South Manchester University Hospitals NHS Trust, Withington, Nell Lane, Manchester M20 2LR, UK R E England D F Martin Medical Statistics, South Manchester University
Gut 2000;46:395 400 395 Radiology, South Manchester University Hospitals NHS Trust, Withington, Nell Lane, Manchester M20 2LR, UK R E England D F Martin Medical Statistics, South Manchester University
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN VAN DER LEIJ, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+
 THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+ DISCLOSURES None 78 Y/O FEMALE Painful RUQ Fever Lab: Raised Leukocytes/CRP CHOLECYSTITIS 3-9% patients ER
THE INTERVENTIONAL RADIOLOGIST CHRISTIAAN, MD. EBIR. INTERVENTIONAL RADIOLOGY MAASTRICHT UMC+ DISCLOSURES None 78 Y/O FEMALE Painful RUQ Fever Lab: Raised Leukocytes/CRP CHOLECYSTITIS 3-9% patients ER
Interventional Radiology Rounds:
 1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
Percutaneous treatment in malignant biliary obstruction: a prospective study
 Percutaneous treatment in malignant biliary obstruction: a prospective study Poster No.: C-2620 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Rroji, E. Enesi, F. Bilaj, F. Tuka, S. Butorac; Tirana/AL
Percutaneous treatment in malignant biliary obstruction: a prospective study Poster No.: C-2620 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Rroji, E. Enesi, F. Bilaj, F. Tuka, S. Butorac; Tirana/AL
Key Words: bile duct obstruction, biliary drainage, obstructive jaundice, endoscopic drainage
 HPB, 2007; 9: 408413 PRESIDENTIAL ADDRESS Stent versus surgery DIRK J. GOUMA Abstract Following the introduction of percutaneous and endoscopic biliary drainage there has been an ongoing debate about the
HPB, 2007; 9: 408413 PRESIDENTIAL ADDRESS Stent versus surgery DIRK J. GOUMA Abstract Following the introduction of percutaneous and endoscopic biliary drainage there has been an ongoing debate about the
Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden
 Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients
 Progress report Gut, 1983, 24, 845-852 Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients A retrospective study of 373 patients undergoing surgery
Progress report Gut, 1983, 24, 845-852 Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients A retrospective study of 373 patients undergoing surgery
CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S
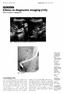 Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
RESEARCH ARTICLE. Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction
 DOI:http://dx.doi.org/10.7314/APJCP.2014.15.16.6823 RESEARCH ARTICLE Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction Fei Gao 1 *, Shuren Ma
DOI:http://dx.doi.org/10.7314/APJCP.2014.15.16.6823 RESEARCH ARTICLE Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction Fei Gao 1 *, Shuren Ma
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure
 To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
FAST TRACK MANAGEMENT OF PANCREATIC CANCER
 FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
The case against preoperative biliary drainage with pancreatic resection
 HPB, 2006; 8: 426431 REVIEW ARTICLE The case against preoperative biliary drainage with pancreatic resection RURIK C. JOHNSON & STEVEN A. AHRENDT Department of Surgery, University of Pittsburgh Medical
HPB, 2006; 8: 426431 REVIEW ARTICLE The case against preoperative biliary drainage with pancreatic resection RURIK C. JOHNSON & STEVEN A. AHRENDT Department of Surgery, University of Pittsburgh Medical
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline
 Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Percutaneous Metallic Stent Placement for Palliative Management of Malignant Biliary Hilar Obstruction
 Original Article Intervention https://doi.org/10.3348/kjr.2018.19.4.597 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2018;19(4):597-605 Percutaneous Metallic Stent Placement for Palliative Management
Original Article Intervention https://doi.org/10.3348/kjr.2018.19.4.597 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2018;19(4):597-605 Percutaneous Metallic Stent Placement for Palliative Management
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Manuel José Antunes Liberato * and Jorge Manuel Tavares Canena
 Liberato and Canena BMC Gastroenterology 2012, 12:103 RESEARCH ARTICLE Open Access Endoscopic stenting for hilar cholangiocarcinoma: efficacy of unilateral and bilateral placement of plastic and metal
Liberato and Canena BMC Gastroenterology 2012, 12:103 RESEARCH ARTICLE Open Access Endoscopic stenting for hilar cholangiocarcinoma: efficacy of unilateral and bilateral placement of plastic and metal
Long-term Results of a Primary End-to-end Anastomosis in Peroperative Detected Bile Duct Injury
 J Gastrointest Surg (2007) 11:296 302 DOI 10.1007/s11605-007-0087-1 Long-term Results of a Primary End-to-end Anastomosis in Peroperative Detected Bile Duct Injury P. R. de Reuver & O. R. C. Busch & E.
J Gastrointest Surg (2007) 11:296 302 DOI 10.1007/s11605-007-0087-1 Long-term Results of a Primary End-to-end Anastomosis in Peroperative Detected Bile Duct Injury P. R. de Reuver & O. R. C. Busch & E.
THE LONGMIRE PROCEDURE: IS IT WORTHWHILE?
 ORIGINAL ARTICLE Mahmud Aurangzeb Department of Surgery, Khyber Teaching Hospital, Peshawar ABSTRACT Objective: To evaluate the peripheral intrahepatic cholangiojejunostomy (Longmire procedure) for the
ORIGINAL ARTICLE Mahmud Aurangzeb Department of Surgery, Khyber Teaching Hospital, Peshawar ABSTRACT Objective: To evaluate the peripheral intrahepatic cholangiojejunostomy (Longmire procedure) for the
Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction
 Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction YOSHIMI IWASAKI, MITSURU ISHIZUKA, MASATO KATO, JUNJI KITA, MITSUGI SHIMODA
Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction YOSHIMI IWASAKI, MITSURU ISHIZUKA, MASATO KATO, JUNJI KITA, MITSUGI SHIMODA
Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser
 16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Postoperative bile leakage: endoscopic management
 1118 Gut 1992; 33:1118-1122 Department of Gastroenterology, Academic Medical Centre, University of Amsterdam, The Netherlands PH P Davids E A J Rauws G NJ Tytgat K Huibregtse Correspondence to: Dr P H
1118 Gut 1992; 33:1118-1122 Department of Gastroenterology, Academic Medical Centre, University of Amsterdam, The Netherlands PH P Davids E A J Rauws G NJ Tytgat K Huibregtse Correspondence to: Dr P H
Percutaneous Biliary Forceps Biopsy for Suspect Malignant Biliary Obstruction
 Chin J Radiol 2004; 29: 123-127 123 Percutaneous Biliary Forceps Biopsy for Suspect Malignant Biliary Obstruction ANDY SHAU-BIN CHOU 1,3 PAU-YANG CHANG 1 YUNG-HSIANG HSU 2 CHAU-CHIN LEE 1 SEA-KIAT LEE
Chin J Radiol 2004; 29: 123-127 123 Percutaneous Biliary Forceps Biopsy for Suspect Malignant Biliary Obstruction ANDY SHAU-BIN CHOU 1,3 PAU-YANG CHANG 1 YUNG-HSIANG HSU 2 CHAU-CHIN LEE 1 SEA-KIAT LEE
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Surgical Workload, Outcome and Research Database: V1.1
 Technical Guidance for Surgical Workload, Outcome and Research Database: V1.1 Contents 1. Standard Indicators... 5 1.1. Activity Volume... 5 1.2. Average Length of Stay (Days)... 5 1.3. 2/7/30 day Re-admission
Technical Guidance for Surgical Workload, Outcome and Research Database: V1.1 Contents 1. Standard Indicators... 5 1.1. Activity Volume... 5 1.2. Average Length of Stay (Days)... 5 1.3. 2/7/30 day Re-admission
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
cholecystectomy Treatment of bile duct lesions after laparoscopic cholecystectomy does, however, carry an injuries.7 11 Comparatively few papers,9 12
 Gut 1996; 38: 141-147 Treatment of bile duct lesions after laparoscopic cholecystectomy 141 Departments of Gastroenterology J J G H M Bergman G R van den Brink E A J Rauws K Huibregtse G N J Tytgat and
Gut 1996; 38: 141-147 Treatment of bile duct lesions after laparoscopic cholecystectomy 141 Departments of Gastroenterology J J G H M Bergman G R van den Brink E A J Rauws K Huibregtse G N J Tytgat and
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer
 Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the Elderly and Unwell
 Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
Afferent Loop Syndrome: Treatment by Means of the Placement of Dual Stents
 Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Surgical. Gastroenterology. Evaluating the efficacy of tumor markers CA 19-9 and CEA to predict operability and survival in pancreatic malignancies
 Tropical Gastroenterology 2010;31(3):190 194 Surgical Gastroenterology Evaluating the efficacy of tumor markers and CEA to predict operability and survival in pancreatic malignancies Jay Mehta, Ramkrishna
Tropical Gastroenterology 2010;31(3):190 194 Surgical Gastroenterology Evaluating the efficacy of tumor markers and CEA to predict operability and survival in pancreatic malignancies Jay Mehta, Ramkrishna
Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report
 ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
Management of Patients with Suspected Cholangiocarcinoma CLINICAL GUIDELINES
 London Cancer Hepatic Pancreatic and Biliary (HPB) Faculty Management of Patients with Suspected Cholangiocarcinoma CLINICAL GUIDELINES JULY 2014 This operational policy is agreed and accepted by: Designated
London Cancer Hepatic Pancreatic and Biliary (HPB) Faculty Management of Patients with Suspected Cholangiocarcinoma CLINICAL GUIDELINES JULY 2014 This operational policy is agreed and accepted by: Designated
Temporary Placement of Stent Grafts in Postsurgical Benign Biliary Strictures: a Single Center Experience
 Original Article http://dx.doi.org/10.3348/kjr.2011.12.6.708 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(6):708-713 Temporary Placement of Stent Grafts in Postsurgical Benign Biliary Strictures:
Original Article http://dx.doi.org/10.3348/kjr.2011.12.6.708 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(6):708-713 Temporary Placement of Stent Grafts in Postsurgical Benign Biliary Strictures:
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5153-5160 Role of Interventional Radiology in the Management of Postoperative Biliary Complications 1 Hana Hamdy Nasif, 1 Mennatallah
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5153-5160 Role of Interventional Radiology in the Management of Postoperative Biliary Complications 1 Hana Hamdy Nasif, 1 Mennatallah
The Endoscopic Management of PSC
 The Endoscopic Management of PSC Raj J. Shah, M.D. Associate Professor of Medicine Director, Pancreaticobiliary Endoscopy Services University of Colorado at Denver and the Health Sciences Center Why did
The Endoscopic Management of PSC Raj J. Shah, M.D. Associate Professor of Medicine Director, Pancreaticobiliary Endoscopy Services University of Colorado at Denver and the Health Sciences Center Why did
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Clinical Study Efficacy of the New Double-Layer Stent for Unresectable Distal Malignant Biliary Obstruction: A Single-Center Retrospective Study
 Diagnostic and Therapeutic Endoscopy Volume 212, Article ID 68963, 8 pages doi:1.1155/212/68963 Clinical Study Efficacy of the New Double-Layer Stent for Unresectable Distal Malignant Biliary Obstruction:
Diagnostic and Therapeutic Endoscopy Volume 212, Article ID 68963, 8 pages doi:1.1155/212/68963 Clinical Study Efficacy of the New Double-Layer Stent for Unresectable Distal Malignant Biliary Obstruction:
Slide 1. Slide 2. Slide 3 Pancreatic Cancer- Case #1. Endoscopic management of GI malignancy. Endoscopic approaches in GI malignancy- Agenda
 Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Air cholangiography in endoscopic bilateral stent-in-stent placement of metallic stents for malignant hilar biliary obstruction
 618132TAG0010.1177/1756283X15618132Therapeutic Advances in GastroenterologyJM Lee, SH Lee research-article2015 Therapeutic Advances in Gastroenterology Original Research Air cholangiography in endoscopic
618132TAG0010.1177/1756283X15618132Therapeutic Advances in GastroenterologyJM Lee, SH Lee research-article2015 Therapeutic Advances in Gastroenterology Original Research Air cholangiography in endoscopic
Endoscopic biliary self-expandable metallic stent in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis
 Review Endoscopic biliary self-expandable metallic in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis Authors Benedetto Mangiavillano 1, 2, Amedeo Montale
Review Endoscopic biliary self-expandable metallic in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis Authors Benedetto Mangiavillano 1, 2, Amedeo Montale
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
