Specialist Integrated Haematological Malignancy Diagnostic Service (SIHMDS)
|
|
|
- Virgil Jeffry Nelson
- 5 years ago
- Views:
Transcription
1 Specialist Integrated Haematological Malignancy Diagnostic Service (SIHMDS) Operational Policy Version
2 Operational Policy for the Oxford NHS/BRC SIHMDS 1. Introduction Objectives Objectives of the SIHMDS process Objectives of this Operational policy General Operational Principles Detailed description of work- flows and procedures governing the SIHMDS Central Specimen Reception Contact details and shipment address Request forms Timing of requests Specimens Bone marrow samples Peripheral blood for DNA analysis Peripheral blood for RNA analysis Initial morphological assessment of samples Liquid samples Paraffin embedded material Molecular tests Clonality studies Clinical Trial Samples Algorithms to guide the requesting of additional tests At suspected diagnosis Suspected AML Suspected MDS Suspected MPN Suspected CML Suspected PRV/ET Suspected Myelofibrosis Suspected other MPNs Suspected ALL Suspected CLL/LPD Suspected Multiple Myeloma Suspected Lymphoma Follow- up samples AML follow- up MDS follow- up CML follow- up ALL follow- up CLL follow- up Lymphoma follow- up BMT samples ASCT ASCT for Multiple Myeloma Pre- BMT bone marrow
3 Post- BMT bone marrow Allogeneic transplants Pre- BMT samples Allogeneic transplant for AML/MDS/MF Allogeneic transplant for lymphoma Allogeneic transplant for CLL Allogeneic transplant for Multiple Myeloma Post BMT samples Non- CLL samples CLL samples Relapse post BMT Integrated Reporting Liquid samples Solid samples Appendix Contact details Shipment addresses Request forms Research Request Form...39 Requirements: WHO codes and scoring systems WHO Mature B cell neoplasms WHO Mature T cell and NK cell neoplasms WHO Myeloproliferative neoplasms (MPN) WHO Myelodysplastic syndrome (MDS) WHO Acute Myeloid Leukemia and related neoplasms WHO B Lymphoblastic leukemia/lymphoma WHO T Lymphoblastic leukemia/lymphoma MDS IPSS score Myelofibrosis DIPSS- plus Abbreviations
4 1. Introduction This document defines the responsibilities and operational procedures governing the Oxford NHS/BRC SIHMDS and its referring hospitals. The aim of the SIHMDS is to ensure accurate and speedy diagnosis and follow- up of patients with haematological malignancies and to produce a single interpretative report within a time frame that is of clinical usefulness. 1.1 Objectives Objectives of the SIHMDS process To ensure compliance with NICE and NCAT guidelines To ensure quality assured sample analysis within EQA schemes To guarantee the appropriate and cost- effective use of complex analysis (avoiding duplication of testing, unnecessary testing, etc) To allow formal teaching of specialist registrars in morphology, immuno- phenotyping, molecular genetics (indications for testing, analysis, interpretation, integration of results) To ensure that all patients undergoing complex analyses are issued an integrated report that is reviewed in the MDT To co- ordinate Oxford Radcliffe Biobank (ORB) and MDS Biobank tissue banking according to GLP To guarantee speedy and accurate processing of research samples Objectives of this Operational policy To clearly define the responsibilities of local laboratories and the SIHMDS in delivering the service To outline the processes involved in establishing leukaemia and lymphoma diagnostics including sample reception, processing and reporting 4
5 2. General Operational Principles The laboratory is designated by the commissioning groups and by the Thames Valley Cancer Network and is managed by the Oxford University Hospitals (OUH) and the Oxford Biomedical Research Centre. It is directed by a single head of service who reports to the Chief Executive of OUH. His/her list of responsibilities includes the design of investigational algorithms, the use of resources for diagnostics and research, and the standards of reporting. The laboratory has a single central specimen reception and issues a single integrated report including morphology, histology, immunochemistry, flow cytometry, cytogenetics, FISH and molecular studies. The different sections of the laboratory are joined up by a lab IT system that covers all investigational pathways, live sample tracking, redirection of sample at any time point depending on results at that point, pathway report generation, diagnostic coding (according to WHO classification), summary of all results on a single screen to facilitate authorisation by a single haematologist/pathologists, and on- line communication of results with users. 5
6 3. Detailed description of work- flows and procedures governing the SIHMDS OVERVIEW OF SOLID SAMPLE PATHWAYS 6
7 OVERVIEW OF LIQUID SAMPLE PATHWAYS 4. Central Specimen Reception 4. 1 Contact details and shipment address See appendix Request forms See appendix. SIHMDS request forms are also available from our website: translational- molecular- diagnostics.org.uk/home.html and from the OUH website: em/molhaem.aspx 7
8 Integrated analysis of samples is critically dependent on clinical information. It is therefore vital that all clinical and already available diagnostic information is clearly stated on the request form. In the absence of clinical information or previous results, samples will be processed on the basis of morphology and algorithms described below. 4.3 Timing of requests Whenever possible, samples should be send between Monday and Thursday morning. Urgent requests should be phoned through to the laboratory to allow urgent tracking of samples if necessary and speedy reporting of provisional results back to the requesting physician. 4.4 Specimens Specification for each type of specimen is as below Bone marrow samples 10ml of EDTA and 2 unstained or stained bedside smears Peripheral blood for DNA analysis 4ml of EDTA Peripheral blood for RNA analysis 12ml of EDTA Histopathological samples Paraffin embedded blocks or micron cut sections in eppendorf tubes. Unstained paraffin- embedded mounted and marked 4 micron sections for micro- dissection. Stained paraffin- embedded mounted sections. NB All cases paraffin embedded specimens require morphological assessment prior to any molecular testing and, if possible, all stained and unstained material should be forwarded to Oxford, including a copy of any report and full clinical details. 8
9 5. Initial morphological assessment of samples Initial assessment of paraffin embedded material and blood or bone marrow smears is performed at the local hospital. If a diagnosis of a haematological malignancy is suspected, diagnostic material will be sent to the SIHMDS for confirmation of initial diagnosis and additional tests if indicated. Emergency treatment should not be delayed by the SIHMDS and should be initiated on the basis of local results if indicated. However, rapid diagnosis at the SIHMDS is possible. haematopathologists to discuss the case as soon as it arrives at SIHMDS. Please contact one of the 5.1 Liquid samples Liquid samples will be processed according to the standard operating procedures. Briefly, booking- in of samples should be performed only once. Each sample will be given a unique identifier that is the same for all tests. Two bedside slides will be sent for MGG staining. The remaining bone marrow will be pooled and mixed in a 15ml Falcon, a nucleated cell count performed and 1-2x10 7 cells will be dispatched for each test. All samples for research will be processed immediately to guarantee cell viability. Generally, 1x10 7 cells for flow cytometry, 2x10 7 cells for cytogenetics, 1x10 6 cells for DNA preparation and 1x10 7 cells for RNA preparation and ensure that the remainder of sample is banked. Tissue bankers are expected to collect research sample as soon as the sample is divided as the sample has to be processed for banking on the same day as it was received. Consent forms for tissue banking should come in the request pouches from the person taking the marrow sample at the bedside. Samples for diagnostic purposes will be stored according to downstream requirements and processed in batches on the same day or in the morning of the following day for samples arriving after 14:00. Morphological assessment of samples will be performed by the consultant haematologist on- duty for the laboratory. This assessment can be delegated to the laboratory registrar after an extended period of teaching and provided that competency has been demonstrated. On the basis of known clinical data, previous results and the current morphological assessment, additional tests will be requested to establish the precise diagnosis. The registrar reviewing the marrow and arranging further tests 9
10 should print the latest clinic letter and append it to the blue folder in order to provide maximum clinical context for the interpretation of test results. In cases where it is unclear at the time of diagnostic morphology review what additional tests will be required, DNA/RNA, cytogenetic samples and cells should be prepared for storage. Analysis of follow- up samples for response assessment should be guided by the initial diagnostic findings. The diagnostic worksheets (on- line or in paper form) must therefore contain all diagnostic information previously obtained and bone marrow reports and results of additional tests should be entered in real- time onto the worksheet and into reporting databases. 5.2 Paraffin embedded material Molecular tests Molecular tests on paraffin embedded material should be requested only by an SIHMDS haematopathologist following morphological and immunohistochemical (+/- in situ hybridisation) assessment of the case. One 4 micron section per rearrangement to be investigated should be cut on to a charged glass slide Clonality studies B and T- cell receptor clonality analysis by PCR on paraffin embedded material and cytological specimens are carried out. For paraffin embedded material, please cut 3-5 x 10 μm sections per tube into two separate microtubes, depending on specimen size. For cytological material, please cut cell blocks onto slides (multiple sections per slide are acceptable) and send as much material (smears, touch preps etc) as possible on slides. When preparing pathological material, please ensure the equipment (especially the microtome blade and water bath) is completely clean between cases to prevent cross contamination. This can be achieved by wiping the microtome blade and any other surfaces with ethanol until they are free of any debris from earlier cases. 5.3 Clinical Trial Samples Samples for commercial studies will be sent away to central laboratories by the research nurse team. Samples from investigator- led studies should also be sent off by research nurses. However, samples requiring cdna preparation should be sent via the SIHMDS in order to allow speedy sample preservation. 10
11 If a Principle Investigator (PI) uses the laboratory for tissue banking or downstream analysis, a research request form should be filled in and submitted prior to sending the samples. Processing of these samples has to be agreed with the head of the SIHMDS. All non- guideline tests being done locally above and beyond what would constitute routine clinical care should be costed for and a research request form should be filled in and submitted prior to sending the samples. For sample processing, PID numbers should be recorded on trial patients request forms. It is the responsibility of the trial nurse to clearly state on the request form which tests the patient needs if these are extra to what would constitute routine clinical care. Otherwise, the registrar reviewing the morphology will request tests as per the standard guidelines. 6. Algorithms to guide the requesting of additional tests In addition to review of morphology and histology, the SIHMDS will perform additional tests when indicated with a view of providing and integrated and interpretative report. The SIHMDS will follow national and international consensus guidelines and NICE recommendations whenever possible. Disease will be coded as per WHO classification (see appendix). It is important to note that further investigations such as flow cytometry or molecular tests/fish should only be undertaken if the abnormal cell population exceeds 5%. The following algorithms are based on the WHO classification
12 6.1 At suspected diagnosis Suspected AML Samples should be evaluated as follows: a) Evaluation of 100 cells on MGG stained slide note dysplasia and blast count. b) Flow cytometry: full panel of ELN markers to be used. c) Cytogenetics. d) In cases where APL is suspected, FISH for PML- RARA (Churchill CGN lab) and PML body staining (JR Molecular Diagnostics) should be performed urgently. RQ- PCR for PML- RARA is done in JR Molecular Diagnostics. e) All patients should be tested for FLT3 TKI and internal tandem repeat (ITD) mutations as well as NPM1 mutations and c- kit if inv16 positive (Molecular). f) If M2 morphology is seen, RQ- PCR for t(8;21) breakpoint, and inv(16) in M4. g) All diagnostic samples will be stored as DNA and RNA to allow quantitative molecular monitoring should this be indicated. h) All samples will be stored under MDS Bio i) High throughput sequencing of a panel of genes known to be mutated in AML (eg RUNX1, TET1/2, IDH1/2, DNMT3A etc) is in development. This may be requested on a research basis from now, with the clear understanding that the results cannot at this time be used for clinical decision making. 12
13 6.1.2 Suspected MDS Samples should be evaluated as follows: a) Evaluation of 200 cells on MGG stained slide note dysplasia and blast count. b) Where the blast count exceeds 20% AML is diagnosed and the AML flowchart to be followed. c) Cytogenetics. The person requesting the marrow will indicate whether the sample is urgent in which case it will be done in 2 weeks, or non- urgent in which case it will be done in 4 weeks. The SpR requesting the tests should then indicate this on the integrated report worksheet. d) Iron stains. These should be reported on LIMS. e) MDS Bio f) High throughput sequencing of a panel of genes known to be mutated in MDS/AML (eg RUNX1, TET1/2, IDH1/2, CBL, ASXL1 etc) is in development. This may be requested on a research basis from now, with the clear understanding that the results cannot at this time be used for clinical decision making. 13
14 6.1.3 Suspected MPN Suspected CML Samples should be evaluated as follows: a) Cytogenetics & FISH for BCR- ABL (all done at Churchill CGN) b) DNA analysis for JAK2 V617F in BCR- ABL negative cases (Molecular) c) BCR- ABL multiplex & RQ- PCR for BCR- ABL (Molecular) d) DNA and RNA samples will be stored on all cases of suspected CML e) MDS Bio 14
15 Suspected PRV/ET All samples will be tested for: a) JAK2 V617F mutations. Allelic burden will be reported as WT:mutant ratio. b) On request, JAK2 exon 12 mutation (PRV only) analysis or MPL mutation (ET only) analysis will be performed. JAK2 exon 12 should be done on marrow rather than peripheral blood if possible. c) RQ- PCR for BCR- ABL will be performed in ET JAK2 mutation negative patients. 15
16 Suspected Myelofibrosis All patients should have a) Karyotyping if MF suspected b) DNA analysis for JAK2 V617F (Molecular) c) DNA analysis for MPL if JAK2 ve (Molecular) d) MDS Bio 16
17 Suspected other MPNs These need to discussed by the clinical consultant with Dr Schuh on a case by case basis. Myeloid and lymphoid neoplasms with eosinophilia +/- aberrant mast cell involvement: Chronic Eosinophilic syndrome, AML, pre- cursor T lymphoblastic lymphoma. Possible tests available include testing for: PDGFalpha, PDGFbeta and FGFR1 (cryptic) translocations: detection by FISH and nested RT- PCR Mast cell leukaemia: c- kit mutations on D816V by nested PCR 17
18 6.1.4 Suspected ALL All samples should be analysed by: a) Flow cytometry b) Cytogenetics c) FISH for BCR- ABL (Done in Churchill CGN). d) DNA and RNA will be stored should BCR- ABL monitoring be indicated. e) ORB 18
19 6.1.5 Suspected CLL/LPD Peripheral blood a) All cases with suspected LPD, ie with persistent lymphocytosis of >5x10 9 /l for longer then 3 months should have flow cytometry performed. b) All cases of CD19+ CD5+ lymphocytosis and CLL score of 3 should be tested for the t(11;14) to exclude mantle cell lymphoma. This is done in Molecular Diagnostics. c) In selected CLL samples, prognostic markers (IGVH mutation analysis) can be performed optionally on request of the treating physician. Remaining viable cells will be stored under ORB. d) CD5 negative persistent lymphocytosis cases should be referred for further investigations including bone marrow examination and lymph node biopsy. Precise diagnosis should be established on these specimens and not on the peripheral blood. e) Cases of persistent mature T- cell lymphocytosis should be sent for clonality studies and referred for further investigations including bone marrow examination or lymph node biopsy. 19
20 Bone marrow a) Flow cytometry will only be performed if the lymphoid infiltrate is >20% b) All cases of CD19+ CD5+ lymphocytosis and CLL score of 3 should be tested for the t(11;14) to exclude mantle cell lymphoma. c) In selected CLL samples, prognostic markers (IGVH mutation analysis) can be performed optionally on request of the treating physician. Remaining viable cells will be stored under ORB. d) CD5 negative persistent lymphocytosis cases should get a precise diagnosis from histopathology specimens (marrow or LN). e) Cases of persistent mature T- cell lymphocytosis should be sent for clonality studies from the histopathological specimen. f) All cases with confirmed CLL requiring treatment should be tested for del17p by FISH and TP53 mutations. 20
21 6.1.6 Suspected Multiple Myeloma All cases should have: a) Morphology to confirm >5% plasma cells b) Flow cytometry and CD138 sort if >5% plasma cells c) Cytospin CD138 cases for FISH analysis for del17p and t(4;14) d) Storage of CD138 cells under ORB 21
22 6.1.7 Suspected Lymphoma The diagnosis of NHL and Hodgkin s lymphoma relies on histological assessment of tissue biopsies and immunostaining. Pathologists might request molecular tests in a minority of cases: T- cell and B- cell receptor rearrangement studies (by PCR) These should only be requested in cases where there is diagnostic doubt or where the MDT requests studies to identify minimal residual disease (which may involve comparison with an earlier biopsy). PCR should not be requested routinely on all B- cell lymphomas. FISH studies for rearrangements of: c- MYC t(8;14) cases with features diagnostic or suspicious of Burkitt s lymphoma; diffuse large B- cell lymphomas with a proliferation index >80% to identify double hit lymphomas. bcl- 2 t(18;14) suspected follicular lymphomas in which immunohistochemistry is inconclusive; cases where differential diagnosis lies between Burkitt lymphoma and the intermediate category between Burkitt lymphoma and diffuse large B- cell lymphoma; diffuse large B- cell lymphomas with a proliferation index >80% to identify double hit lymphomas (request at the same time as requesting FISH for a MYC rearrangement). cyclin D1 t(11;14) suspected mantle cell lymphomas in which immunohistochemistry is inconclusive. MALT1 t(11;18) all marginal zone lymphomas of MALT type without evidence of concurrent high grade transformation, provided these are treated by Oxford or regional haematologists. If the patient is being treated for a gastric marginal zone lymphoma of MALT type, the Oxford gastroenterologists do not want us to do this test. ALK- 1 t(2;5) suspected cases of ALK- 1+ anaplastic large cell lymphoma, in which immunohistochemistry is inconclusive. P53 cases of chronic lymphocytic leukaemia/ small lymphocytic lymphoma at the request of the MDT meeting only. 22
23 6.2 Follow- up samples AML follow- up Follow- up samples should be reviewed together with all previous results. The main follow up test pathways are outlined below: a) PML- RARA, RUNX1- ETV6 (AML1- ETO1), CBFB- MYH (inv16) positive AML: follow- up samples should be tested by RQ- PCR (JR Molecular). The person requesting tests should check previous results to see whether this is indicated. b) AML is currently not routinely monitored by molecular means and will be assessed through the SIHMDS by morphology only. NPM1 molecular monitoring will be available shortly, and assay validation is in progress. c) AML with complex cytogenetics will be monitored by morphology and metaphase analysis/fish (Churchill CGN). Other cytogenetic markers abnormal at diagnosis can also be followed up in the same way. d) Patients who had been in previous CR and now have relapsed should have all the tests as indicated in diagnostic samples e) MDS Bio 23
24 6.2.2 MDS follow- up Some MDS patients will have yearly bone marrows to monitor disease. They should have: a) Evaluation of 100 cells on MGG stained slide note dysplasia and blast count. b) Where the blast count exceeds 20% and AML is suspected, flow cytometry with the full panel of ELN markers to be used. c) Cytogenetics d) Iron stains for patients who had ring sideroblasts e) MDS Bio 24
25 6.2.3 CML follow- up Monitoring of CML should follow the European Leukaemia Net (ELN) guidelines. a) 3 monthly bone marrow cytogenetics/fish until absence of Philadelphia chromosome. Alternatively, peripheral blood FISH monitoring is acceptable. b) Once the patient has become negative for the cytogenetic abnormality t(9;22), 3 monthly monitoring by RQ- PCR from peripheral blood (JR Molecular) should be initiated until a major molecular response (~3 log reduction from base- line) has been achieved. Once the patient is in MMR, 6 monthly monitoring is acceptable. RQ- PCR for BCR- ABL is never performed on bone marrow, even as part of the clinical trials. c) Yearly bone marrow examination for conventional metaphase analysis should at least be considered as per ELN guidelines d) Suboptimal responders and treatment failures: 3 monthly monitoring by the appropriate test. Kinase mutations should be excluded. T315I will be routinely done. If negative, sequencing of the kinase domain will be carried out. e) MDS Bio 25
26 6.2.4 ALL follow- up BCR- ABL positive cases should be monitored for BCR- ABL transcript levels by RQ- PCR (paired PB and BM- JR Molecular). Patients with abnormal cytogenetics should be monitored by cytogenetics/fish until they become negative. 26
27 6.2.5 CLL follow- up Follow- up samples prior to treatment should be tested for del17p and TP53 mutation analysis (JR Molecular). MRD monitoring by flow cytometry is not performed routinely (except post transplant, see relevant section). However, on request of the treating physician s samples can be forwarded to Leeds HMDS. 27
28 6.2.6 Lymphoma follow- up NHL that tested positive at diagnosis for a particular marker might be followed- up by PCR or FISH: T- cell and B- cell receptor rearrangement studies (by PCR). If possible, aspirates should be sent for this analysis, as bone marrow trephines often do not yield sufficient DNA quality. In JR Molecular Diagnostic lab, FISH studies for rearrangements of: c- MYC(8;14) bcl- 2(18;14) cyclin D1(11;14) MALT1(11;18) ALK- 1(2;5). The necessity for this will be considered on an individual basis, often following MDT discussion. 28
29 6.3 BMT samples ASCT ASCT for Multiple Myeloma Pre- BMT bone marrow The aim of the marrow sample is to assess disease burden. This is done by morphological assessment only (% plasma cells on aspirate). The sample should not be sent for cytogenetics, FISH or flow cytometry Post- BMT bone marrow The aim of the marrow sample is to assess disease burden. This is done by morphological assessment only (% plasma cells on aspirate). If the patient was poor risk (p53 del, t(4,14)) at diagnosis, there is no need to repeat the FISH. If, however, the patient was good risk, do need to do the FISH. 29
30 ASCT for Lymphoma The aspirate will only be done if the marrow was involved at diagnosis or relapse. If an aspirate is taken pre- transplant and the patient s marrow was not involved at diagnosis or relapse, the slides will be stored unexamined and no further tests will be requested on the aspirate. If the marrow was previously involved, the slides will be examined and flow cytometry will be carried out if the lymphoid infiltrate exceeds 20%. 30
31 6.3.2 Allogeneic transplants Pre- BMT samples Allogeneic transplant for AML/MDS/MF a) Morphology: count >100 cells and record blasts and morphology b) If abnormal karyotype/fish at diagnosis or relapse, check again pre- transplant. Otherwise send and store for cytogenetics. c) Molecular markers are not monitored pre- transplant, irrespective of whether they were positive or negative at diagnosis/relapse. However, all patients should have DNA stored for later analysis if required. d) MDS Bio 31
32 Allogeneic transplant for lymphoma The aspirate should only be done if the marrow was involved at diagnosis or relapse. However, many of these patients are heavily pre- treated and an aspirate may be taken to assess for secondary myelodysplasia. a) Morphology: count >100 cells and record % infiltrate and morphology b) Send all aspirates for cytogenetics to detect 2 MDS. c) For a lymphoid infiltrate >20%, flow cytometry may be considered (eg poor or no trephine taken). d) ORB 32
33 Allogeneic transplant for CLL These patients are all generally heavily pre- treated and an assessment for 2 MDS is often undertaken. However, there is no need to do FISH or molecular markers in these patients as MRD monitoring is more sensitively done by flow cytometry and these samples are all sent to Leeds HMDS for this assessment. a) Morphology: count >100 cells and record % infiltrate and morphology and dysplasia b) Send all aspirates for cytogenetics to detect 2 MDS. c) No molecular markers d) All samples to Leeds HMDS. e) ORB 33
34 Allogeneic transplant for Multiple Myeloma As for autografts, Molecular tests (FISH for p53 and t(4;14))are only carried out in previously good risk myelomas. 34
35 Post BMT samples Non- CLL samples Chimerism studies are different depending on the patient group. Falling levels of % donor levels especially in T- deplete MUDs are an indication for DLI to reduce relapse. A. AML/MDS/MF patients have chimerism studies done both on peripheral blood CD3 cells and marrow CD34 sorted cells (just write chimerism studies in the molecular tests section). B. For patients with a translocation that can be followed- up by RQ- PCR across the breakpoint (PML- RARA, BCR- ABL, inv16, 8:21), then please do NOT request chimerism studies, but request RQ- PCR for that breakpoint, as this is a far more sensitive test than chimerism. THIS INCLUDES PH+ ALL. C. For non- myeloid indications, chimerism studies are only done on CD3 cells from peripheral blood (just write chimerism studies in the molecular tests section). ****Please note: Chimerism studies are NEVER carried out by cytogenetics, even where there is a sex mismatch between donor and recipient (not very sensitive technique). **** 35
36 CLL samples MRD monitoring is sensitively monitored by flow cytometry and these samples are all sent to Leeds HMDS for this assessment. Chimerism studies are done on peripheral blood CD3 cells. Cytogenetics will be stored for later analysis if myelodysplasia becomes a question Relapse post BMT At relapse, a sample should be treated as a newly diagnosed sample would be, following those workflows for ordering further tests. 36
37 7. Integrated Reporting 7.1 Liquid samples It is the responsibility of the SIHMDS haematologist to review all results on a weekly basis and to prepare an integrated report containing a clinical summary. This will be done within 2 weeks of the samples arriving in the lab. Where some test results are unavailable in this timeframe, an interim report will be issued. The reports will be uploaded into ARIA. The WHO classification will be followed, and an assessment of prognosis (where the scoring system is dependent on test results only) will be provided. 7.2 Solid samples It is the responsibility of the SIHMDS haemato- pathologist to prepare an integrated report containing histology, immunostaining results and molecular tests. The integrated report will be the basis of the MDT discussion. Only raw data of complex cases, especially those with conflicting results will be presented in the MDT. 37
38 8. Appendix 8.1 Contact details (for FFPE samples) (for liquid samples) 8.2 Shipment addresses Paraffin embedded blocks: Professor Gatter/ Professor Pezzella/ Dr Soilleux Department of Cellular Pathology Level 1, Academic Block John Radcliffe Hospital Headley Way Headington Oxford OX3 9DU Liquid samples: Laboratory Haematology Level 4 John Radcliffe Hospital Headley Way Headington Oxford OX3 9DU 8.3 Request forms Diagnostic Request Form W129 : ORH BM Request Form (Version 1) W128 : TVHMDS Request Form (Version 2) 38
39 Research Request Form W131 : ORB/MDS Biobank Forms (Research Samples) Standard Operating Procedure HC 2309 : Integrated reporting of bone marrow aspirate samples Diagnostic Worksheet Log W116 (Version 3) : Bone Marrow Aspirate Sample Integrated Report Log Sheet Integrated Bone Marrow Report W130 : Molecular Integrated Report Database (Oxford BRC Hemato- Oncology Service Bone Marrow Integrated Report) Research Request Form Requirements: Designation of the SIHMDS head Daily sample transport to regional hospitals Specimen reception open on Saturday Internal lab IT support to allow access of early reports in each section Web based or ARIA based reporting system. 39
40 8.4 WHO codes and scoring systems WHO 2008 Diseases shown in italics are newly included in the 2008 WHO classification. *These represent provisional entities or provisional subtypes of other neoplasms WHO Mature B cell neoplasms Chronic lymphocytic leukemia/small lymphocytic lymphoma B- cell prolymphocytic leukemia Splenic marginal zone lymphoma Hairy cell leukemia Splenic lymphoma/leukemia, unclassifiable Splenic diffuse red pulp small B- cell lymphoma* Hairy cell leukemia- variant* Lymphoplasmacytic lymphoma Waldenström macroglobulinemia Heavy chain diseases Alpha heavy chain disease Gamma heavy chain disease Mu heavy chain disease Plasma cell myeloma Solitary plasmacytoma of bone Extraosseous plasmacytoma Extranodal marginal zone B- cell lymphoma of mucosa- associated lymphoid tissue (MALT lymphoma) Nodal marginal zone B- cell lymphoma (MZL) Pediatric type nodal MZL Follicular lymphoma Pediatric type follicular lymphoma Primary cutaneous follicle center lymphoma Mantle cell lymphoma 40
41 Diffuse large B- cell lymphoma (DLBCL), not otherwise specified T cell/histiocyte rich large B- cell lymphoma DLBCL associated with chronic inflammation Epstein- Barr virus (EBV) + DLBCL of the elderly Lymphomatoid granulomatosis Primary mediastinal (thymic) large B- cell lymphoma Intravascular large B- cell lymphoma Primary cutaneous DLBCL, leg type ALK + large B- cell lymphoma Plasmablastic lymphoma Primary effusion lymphoma Large B- cell lymphoma arising in HHV8- associated multicentric Castleman disease Burkitt lymphoma B- cell lymphoma, unclassifiable, with features intermediate between diffuse large B- cell lymphoma and Burkitt lymphoma B- cell lymphoma, unclassifiable, with features intermediate between diffuse large B- cell lymphoma and classical Hodgkin lymphoma Hodgkin Lymphoma Nodular lymphocyte- predominant Hodgkin lymphoma Classical Hodgkin lymphoma Nodular sclerosis classical Hodgkin lymphoma Lymphocyte- rich classical Hodgkin lymphoma Mixed cellularity classical Hodgkin lymphoma WHO Mature T cell and NK cell neoplasms T- cell prolymphocytic leukemia T- cell large granular lymphocytic leukemia Chronic lymphoproliferative disorder of NK- cells* Aggressive NK cell leukemia 41
42 Systemic EBV + T- cell lymphoproliferative disease of childhood (associated with chronic active EBV infection) Hydroa vacciniforme- like lymphoma Adult T- cell leukemia/lymphoma Extranodal NK/T cell lymphoma, nasal type Enteropathy- associated T- cell lymphoma Hepatosplenic T- cell lymphoma Subcutaneous panniculitis- like T- cell lymphoma Mycosis fungoides Sézary syndrome Primary cutaneous CD30 + T- cell lymphoproliferative disorder Lymphomatoid papulosis Primary cutaneous anaplastic large- cell lymphoma Primary cutaneous aggressive epidermotropic CD8 + cytotoxic T- cell lymphoma* Primary cutaneous gamma- delta T- cell lymphoma Primary cutaneous small/medium CD4 + T- cell lymphoma* Peripheral T- cell lymphoma, not otherwise specified Angioimmunoblastic T- cell lymphoma Anaplastic large cell lymphoma (ALCL), ALK + Anaplastic large cell lymphoma (ALCL), ALK * *These represent provisional entities or provisional subtypes of other neoplasms. Diseases shown in italics are newly included in the 2008 WHO classification WHO Myeloproliferative neoplasms (MPN) Chronic myelogenous leukemia, BCR- ABL1 positive Chronic neutrophilic leukemia Polycythemia vera Primary myelofibrosis Essential thrombocythemia Chronic eosinophilic leukemia, not otherwise specified Mastocytosis Myeloproliferative neoplasms, unclassifiable Myeloid and lymphoid neoplasms associated with eosinophilia and abnormalities of PDGFRA, 42
43 PDGFRB, or FGFR1 Myeloid and lymphoid neoplasms associated with PDGFRA rearrangement Myeloid neoplasms associated with PDGFRB rearrangement Myeloid and lymphoid neoplasms associated with FGFR1 abnormalities Myelodysplastic/myeloproliferative neoplasms (MDS/MPN) Chronic myelomonocytic leukemia Atypical chronic myeloid leukemia, BCR- ABL1 negative Juvenile myelomonocytic leukemia Myelodysplastic/myeloproliferative neoplasm, unclassifiable Provisional entity: refractory anemia with ring sideroblasts and thrombocytosis WHO Myelodysplastic syndrome (MDS) Refractory cytopenia with unilineage dysplasia Refractory anemia Refractory neutropenia Refractory thrombocytopenia Refractory anemia with ring sideroblasts Refractory cytopenia with multilineage dysplasia Refractory anemia with excess blasts Myelodysplastic syndrome with isolated del(5q) Myelodysplastic syndrome, unclassifiable Childhood myelodysplastic syndrome Provisional entity: refractory cytopenia of childhood WHO Acute Myeloid Leukemia and related neoplasms Acute myeloid leukemia with recurrent genetic abnormalities 43
44 AML with t(8;21)(q22;q22); RUNX1- RUNX1T1 AML with inv(16)(p13.1q22) or t(16;16)(p13.1;q22); CBFB- MYH11 APL with t(15;17)(q22;q12); PML- RARA AML with t(9;11)(p22;q23); MLLT3- MLL AML with t(6;9)(p23;q34); DEK- NUP214 AML with inv(3)(q21q26.2) or t(3;3)(q21;q26.2); RPN1- EVI1 AML (megakaryoblastic) with t(1;22)(p13;q13); RBM15- MKL1 Provisional entity: AML with mutated NPM1 Provisional entity: AML with mutated CEBPA Acute myeloid leukemia with myelodysplasia- related changes Therapy- related myeloid neoplasms Acute myeloid leukemia, not otherwise specified AML with minimal differentiation AML without maturation AML with maturation Acute myelomonocytic leukemia Acute monoblastic/monocytic leukemia Acute erythroid leukemia Pure erythroid leukemia Erythroleukemia, erythroid/myeloid Acute megakaryoblastic leukemia Acute basophilic leukemia Acute panmyelosis with myelofibrosis Myeloid sarcoma Myeloid proliferations related to Down syndrome Transient abnormal myelopoiesis 44
45 Myeloid leukemia associated with Down syndrome Blastic plasmacytoid dendritic cell neoplasm Acute leukemias of ambiguous lineage Acute undifferentiated leukemia Mixed phenotype acute leukemia with t(9;22)(q34;q11.2); BCR- ABL1 Mixed phenotype acute leukemia with t(v;11q23); MLL rearranged Mixed phenotype acute leukemia, B- myeloid, NOS Mixed phenotype acute leukemia, T- myeloid, NOS Provisional entity: natural killer (NK) cell lymphoblastic leukemia/lymphoma WHO B Lymphoblastic leukemia/lymphoma B lymphoblastic leukemia/lymphoma, NOS B lymphoblastic leukemia/lymphoma with recurrent genetic abnormalities B lymphoblastic leukemia/lymphoma with t(9;22)(q34;q11.2);bcr- ABL 1 B lymphoblastic leukemia/lymphoma with t(v;11q23);mll rearranged B lymphoblastic leukemia/lymphoma with t(12;21)(p13;q22) TEL- AML1 (ETV6- RUNX1) B lymphoblastic leukemia/lymphoma with hyperdiploidy B lymphoblastic leukemia/lymphoma with hypodiploidy B lymphoblastic leukemia/lymphoma with t(5;14)(q31;q32) IL3- IGH B lymphoblastic leukemia/lymphoma with t(1;19)(q23;p13.3);tcf3- PBX1 45
46 8.4.6 WHO T Lymphoblastic leukemia/lymphoma 46
47 8.4.7 MDS IPSS score (Greenberg 1997) Prognostic variable BM blasts (%) < Karyotype* Good Intermed. Poor Cytopenias 0/1 2/3 *Good: normal,-y,del(5q),del(20q). Poor: complex (>3 abnormalities) or chromosome 7 anomalies. Intermediate: other abnormalities. Risk group Score Median survival (yrs) Time to AML transformation (for 25% in yrs) Low risk INT INT High risk > Myelofibrosis DIPSS- plus The Dynamic International Prognostic Scoring System (DIPSS) plus prognostic model for primary myelofibrosis (PMF). The DIPSS and prognostic model for PMF uses 8 risk factors for inferior survival: age > 65 years, hemoglobin level < 10 g/dl, leukocyte count > /L, circulating blasts 1%, presence of constitutional symptoms, presence of unfavorable karyotype, platelet count < /L, and the presence of red cell transfusion need.40 *Please note that a transfusion- dependent patient automatically has 2 risk factors because of transfusion need (1 risk point) and hemoglobin level < 10 g/dl (1 risk point). **Constitutional symptoms constitute weight loss > 10% of baseline value in the year preceding diagnosis, unexplained fever, or excessive sweats persisting for > 1 month.38 ***Unfavorable karyotype constitutes complex karyotype or sole or 2 abnormalities that include +8, 7/7q, i(17q), inv(3), 5/5q 12p, or 11q23 rearrangement. (ref: Teferri, Blood 2011) 47
48 8.4.9 CML response criteria (ELN website) Aplastic Anaemia severity score (BCSH guidelines, 2009) 48
49 9. Abbreviations ALL: acute lymphoblastic leukaemia AML: acute myeloid leukaemia ASCT: autologous stem cell transplant BRC: Biomedical Research Centre BM: bone marrow BMT: bone marrow transplant CGN: cytogenetics CLL: chronic lymphocytic leukaemia CML: chronic myeloid leukaemia CMML: chronic myelomonocytic leukaemia EDTA: Ethylenediaminetetraacetic acid ELN: European Leukaemia Network ET: essential thrombocythemia EQA schemes: externalquality assessment FISH: fluorescence in situ hybridisation GLP: good laboratory practice IT: information technology LIMS: laboratory information management system LN: lymph node LPD: lymphoproliferative disease MDS: myelodysplastic syndrome MDT: multidisciplinary team meeting 49
50 MF: myelofibrosis MGG: May- Grunwald- Giemsa MPN: myeloproliferative neoplasms MRD: minimal residual disease MUD: matched unrelated donor NCAT: national cancer action team NHL: Non- Hodgkin s lymphoma NICE: national institute for clinical excellence ORB: Oxford Radcliffe Biobank OUH: Oxford University Hospitals PB: peripheral blood PCR: polymerase chain reaction PRV: polycythaemia rubra vera RQ- PCR: real- time quantitative PCR SIHMDS: specialist integrated haematological malignancy diagnostic service 10. References 1. Greenberg P, Cox C, LeBeau MM, Fenaux P, Morel P, Sanz G, Sanz M, Vallespi T, Hamblin T, Oscier D, Ohyashiki K, Toyama K, Aul C, Mufti G, Bennett J. (1997). International scoring system for evaluating prognosis in myelodysplastic syndromes. Blood 89(6): Marsh JCW, Ball SE, Cavenagh J, Darbyshire P, Dokal I, Gordon- Smith ECKeidan J, Laurie A, Martin A, Mercieca J, Killick SB, Stewart R, Yin JAL (2009). Guidelines for the diagnosis and management of aplastic anaemia. Brit J Haematol 147: Tefferi A. (2011) How I treat myelofibrosis. Blood 117(13): goals- ph- cml/eln- recommendations.jsp 50
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Combinations of morphology codes of haematological malignancies (HM) referring to the same tumour or to a potential transformation
 Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Introduction: The Revised (4 th Edition) World Health Organization (WHO) Classification of Tumors of Hematopoietic and Lymphoid Tissues
 Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual
 Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow*
 Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow* Version: Protocol Posting Date: January 2018 This protocol is NOT required for accreditation
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow* Version: Protocol Posting Date: January 2018 This protocol is NOT required for accreditation
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Hepatic Lymphoma Diagnosis An Algorithmic Approach
 Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Update on the WHO Classification of Acute Myeloid Leukemia. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation
 a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
WHO Classification 7/2/2009
 Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Oxford BRC Haemato-Molecular Diagnostic Service
 Short User Guide Oxford BRC Haemato-Molecular Diagnostic Service The Oxford University Hospitals NHS trust s department of Haematology provides a comprehensive molecular diagnostic service for a range
Short User Guide Oxford BRC Haemato-Molecular Diagnostic Service The Oxford University Hospitals NHS trust s department of Haematology provides a comprehensive molecular diagnostic service for a range
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
Myeloid malignancies Chronic myeloid disorders
 Myeloid malignancies Chronic myeloid disorders Myeloproliferative neoplasms (MPN) Mastocytosis / Mast cell diseases Myeloid/lymphoid neoplasms with eosinophilia and gene rearrangement Myelodysplastic/myeloproliferative
Myeloid malignancies Chronic myeloid disorders Myeloproliferative neoplasms (MPN) Mastocytosis / Mast cell diseases Myeloid/lymphoid neoplasms with eosinophilia and gene rearrangement Myelodysplastic/myeloproliferative
Non-Hodgkin Lymphoma. Protocol applies to non-hodgkin lymphoma involving any organ system except the gastrointestinal tract.
 Non-Hodgkin Lymphoma Protocol applies to non-hodgkin lymphoma involving any organ system except the gastrointestinal tract. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
Non-Hodgkin Lymphoma Protocol applies to non-hodgkin lymphoma involving any organ system except the gastrointestinal tract. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
Clinical Policy: Bendamustine (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307
 Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Policy Specific Section:
 Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Hematology Page 1 of 8
 Hematology Page 1 of 8 Hematology Major Category Code Headings Revised 12/17 1 Basic methodology and test armamentarium 20000 2 Normal hematopoiesis & hemostasis 20100 3 RBC disorders, non-neoplastic 20340
Hematology Page 1 of 8 Hematology Major Category Code Headings Revised 12/17 1 Basic methodology and test armamentarium 20000 2 Normal hematopoiesis & hemostasis 20100 3 RBC disorders, non-neoplastic 20340
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
WHO Classification. B-cell chronic lymphocytic leukemia/small T-cell granular lymphocytic leukemia
 Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Practical Diagnosis of Hematologic Disorders. Vol 2 Malignant Disorders
 5 th ed Practical Diagnosis of Hematologic Disorders Vol 2 Malignant Disorders Vol2_FrontMatter_v03_0804 final.indd i 8/6/2009 10:00:11 PM Authors Carl R Kjeldsberg, MD Professor of Pathology, University
5 th ed Practical Diagnosis of Hematologic Disorders Vol 2 Malignant Disorders Vol2_FrontMatter_v03_0804 final.indd i 8/6/2009 10:00:11 PM Authors Carl R Kjeldsberg, MD Professor of Pathology, University
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Protocol for the Examination of Hematologic Malignancies in Bone Marrow
 Protocol for the Examination of Hematologic Malignancies in Bone Marrow Version: Bone Marrow 4.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of this protocol is recommended
Protocol for the Examination of Hematologic Malignancies in Bone Marrow Version: Bone Marrow 4.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of this protocol is recommended
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
Integrated Hematopathology. Morphology and FCI with IHC
 Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
GENETICS OF HEMATOLOGICAL MALIGNANCIES
 de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
MPL W515L K mutation
 MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow
 Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow Based on AJCC/UICC TNM, 7 th Edition Protocol web posting date: February 1, 2011 Procedures
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow Based on AJCC/UICC TNM, 7 th Edition Protocol web posting date: February 1, 2011 Procedures
TEST MENU TEST CPT CODES TAT. Chromosome Analysis Bone Marrow x 2, 88264, x 3, Days
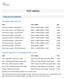 TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party. The European Group for Blood and Marrow Transplantation
 36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
JAK2 V617F analysis. Indication: monitoring of therapy
 JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Initial Diagnostic Workup of Acute Leukemia
 Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Welcome to Master Class for Oncologists. Session 3: 9:15 AM - 10:00 AM
 Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Molecular Diagnostics Centre
 Directorate of Central Manchester Haematology Service Molecular Diagnostics Centre Haemato-Oncology User Guide 2014 Page 1 of 13 Directorate of CONTENTS About Us 3 Contact Details 3 Location 3 Postal Address
Directorate of Central Manchester Haematology Service Molecular Diagnostics Centre Haemato-Oncology User Guide 2014 Page 1 of 13 Directorate of CONTENTS About Us 3 Contact Details 3 Location 3 Postal Address
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Diagnostic Molecular Pathology of Myeloid Neoplasms
 Diagnostic Molecular Pathology of Myeloid Neoplasms Beirut, Lebanon Tuesday November 29, 2011: Pre-congress workshop Adam Bagg University of Pennsylvania Philadelphia, USA Myeloid neoplasms Myeloproliferative
Diagnostic Molecular Pathology of Myeloid Neoplasms Beirut, Lebanon Tuesday November 29, 2011: Pre-congress workshop Adam Bagg University of Pennsylvania Philadelphia, USA Myeloid neoplasms Myeloproliferative
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Diagnostic Approach for Eosinophilia and Mastocytosis. Curtis A. Hanson, M.D.
 Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Contractor Name: Novitas Solutions, Inc. Contractor Number: Contractor Type: MAC A. LCD ID Number: L35032 Status: A-Approved
 LCD for Flow Cytometry (L35032) Contractor Name: Novitas Solutions, Inc. Contractor Number: 12501 Contractor Type: MAC A LCD ID Number: L35032 Status: A-Approved Contractor Information LCD Information
LCD for Flow Cytometry (L35032) Contractor Name: Novitas Solutions, Inc. Contractor Number: 12501 Contractor Type: MAC A LCD ID Number: L35032 Status: A-Approved Contractor Information LCD Information
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Reviewing the ICD-10 classification of haematological neoplasms on its way to ICD-11
 WHO-FIC NETWORK MEETING Tokyo, Japan haematological neoplasms on its way to ICD-11 Ulrich Vogel, Robert Jakob, Michael Schopen, Harald Stein, Stefan Krause Abstract: haematological neoplasms on its way
WHO-FIC NETWORK MEETING Tokyo, Japan haematological neoplasms on its way to ICD-11 Ulrich Vogel, Robert Jakob, Michael Schopen, Harald Stein, Stefan Krause Abstract: haematological neoplasms on its way
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual
 Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
COPYRIGHTED MATERIAL. Introduction CHAPTER 1. Examination of p atients. Classification of c utaneous l ymphomas. Staging i nvestigations
 CHAPTER 1 Introduction Primary cutaneous lymphomas represent distinct clinical and histopathologic subtypes of extranodal lymphomas. They can be defined as neoplasms of the immune system, characterized
CHAPTER 1 Introduction Primary cutaneous lymphomas represent distinct clinical and histopathologic subtypes of extranodal lymphomas. They can be defined as neoplasms of the immune system, characterized
Small B-cell (Histologically Low Grade) Lymphoma
 Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Molecular Hematopathology
 Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
The College of American Pathologists offers these protocols
 Strategies for Laboratory and Patient Management Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms of the Bone Marrow A Basis for Checklists LoAnn C. Peterson, MD; Steven
Strategies for Laboratory and Patient Management Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms of the Bone Marrow A Basis for Checklists LoAnn C. Peterson, MD; Steven
Case 1. Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX
 Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
Case #16: Diagnosis. T-Lymphoblastic lymphoma. But wait, there s more... A few weeks later the cytogenetics came back...
 Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
The primary medical content categories of the blueprint are shown below, with the percentage assigned to each for a typical exam:
 Hematology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified hematologist
Hematology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified hematologist
During past decades, because of the lack of knowledge
 Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Krishna Reddy CH and Ashwin Dalal. Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad
 Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand
 Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand This list provides indications for the majority of adult BMTs that are performed in New Zealand. A small number of BMTs
Appendix 6: Indications for adult allogeneic bone marrow transplant in New Zealand This list provides indications for the majority of adult BMTs that are performed in New Zealand. A small number of BMTs
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms
 Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
Change Summary - Form 2018 (R3) 1 of 12
 Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Aggressive B-cell Lymphoma 2013
 Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
The spectrum of flow cytometry of the bone marrow
 The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
Molecular. Oncology & Pathology. Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine. Liquid Biopsy.
 Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Non-Hodgkin s Lymphomas Version
 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Hodgkin s Lymphomas Version 2.2015 NCCN.org Continue Use of Immunophenotyping/ Genetic Testing in Differential Diagnosis of Mature B-Cell
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Hodgkin s Lymphomas Version 2.2015 NCCN.org Continue Use of Immunophenotyping/ Genetic Testing in Differential Diagnosis of Mature B-Cell
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor
 HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation
 Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
HEMATOPATHOLOGY SERVICES
 HEMATOPATHOLOGY SERVICES Know what your patient s future holds, NOW. Driven by patient care, GoPath Laboratories has set a new standard for hematologic cancer testing. thick, 2 slides per probe minimum
HEMATOPATHOLOGY SERVICES Know what your patient s future holds, NOW. Driven by patient care, GoPath Laboratories has set a new standard for hematologic cancer testing. thick, 2 slides per probe minimum
Role of FISH in Hematological Cancers
 Role of FISH in Hematological Cancers Thomas S.K. Wan PhD,FRCPath,FFSc(RCPA) Honorary Professor, Department of Pathology & Clinical Biochemistry, Queen Mary Hospital, University of Hong Kong. e-mail: wantsk@hku.hk
Role of FISH in Hematological Cancers Thomas S.K. Wan PhD,FRCPath,FFSc(RCPA) Honorary Professor, Department of Pathology & Clinical Biochemistry, Queen Mary Hospital, University of Hong Kong. e-mail: wantsk@hku.hk
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms
 Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Kylie Lepic BSc, MD, FRCPC CAGPO Conference
 Acute Leukemia Kylie Lepic BSc, MD, FRCPC CAGPO Conference Oct 19, 2013 1 Disclosures No conflicts of interest 2 Objectives Case presentation Classification of leukemia Clinical manifestations Diagnosis
Acute Leukemia Kylie Lepic BSc, MD, FRCPC CAGPO Conference Oct 19, 2013 1 Disclosures No conflicts of interest 2 Objectives Case presentation Classification of leukemia Clinical manifestations Diagnosis
Approach to Core Biopsy Specimens
 BDIAP 108th Symposium on Haematopathology Joint Meeting of the BDIAP and BLPG at-bristol, Anchor Road, Harbourside, Bristol BS1 5DB 15th - 17th May 2014 Approach to Core Biopsy Specimens Dr Stefan Dojcinov
BDIAP 108th Symposium on Haematopathology Joint Meeting of the BDIAP and BLPG at-bristol, Anchor Road, Harbourside, Bristol BS1 5DB 15th - 17th May 2014 Approach to Core Biopsy Specimens Dr Stefan Dojcinov
The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare
 The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare Jessica Wang-Rodriguez, MD Chief, VISN22 Consolidated Pathology and Laboratory Medicine Services
The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare Jessica Wang-Rodriguez, MD Chief, VISN22 Consolidated Pathology and Laboratory Medicine Services
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Hypereosinophili c syndrome
 Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
