DISPERSAL OF THE DENGUE VECTOR AEDES AEGYPTI WITHIN AND BETWEEN RURAL COMMUNITIES
|
|
|
- Camron Gilmore
- 5 years ago
- Views:
Transcription
1 Am. J. Trop. Med. Hyg., 72(2), 2005, pp Copyright 2005 by The American Society of Tropical Medicine and Hygiene DISPERSAL OF THE DENGUE VECTOR AEDES AEGYPTI WITHIN AND BETWEEN RURAL COMMUNITIES LAURA C. HARRINGTON, THOMAS W. SCOTT, KRIANGKRAI LERDTHUSNEE, RUSSELL C. COLEMAN, ADRIANA COSTERO, GARY G. CLARK, JAMES J. JONES, SANGVORN KITTHAWEE, PATTAMAPORN KITTAYAPONG, RATANA SITHIPRASASNA, AND JOHN D. EDMAN Department of Entomology, Cornell University, Ithaca, New York; Department of Entomology, University of California, Davis, California; Department of Entomology, Armed Forces Research Institute for Medical Sciences, Bangkok, Thailand; Medical Entomology Section, Laboratory of Parasitic Diseases, National Institutes of Allergy and Infectious Diseases, National Institutes of Health, Bethesda, Maryland; Dengue Branch, Centers for Disease Control and Prevention, San Juan, Puerto Rico; Center for Vectors and Vector-Borne Diseases and Department of Biology, Faculty of Science, Mahidol University, Bangkok, Thailand Abstract. Knowledge of mosquito dispersal is critical for vector borne disease control and prevention strategies and for understanding population structure and pathogen dissemination. We determined Aedes aegypti flight range and dispersal patterns from 21 mark-release-recapture experiments conducted over 11 years ( ) in Puerto Rico and Thailand. Dispersal was compared by release location, sex, age, season, and village. For all experiments, the majority of mosquitoes were collected from their release house or adjacent house. Inter-village movement was detected rarely, with a few mosquitoes moving a maximum of 512 meters from one Thai village to the next. Average dispersal distances were similar for males and females and females released indoors versus outdoors. The movement of Ae. aegypti was not influenced by season or age, but differed by village. Results demonstrate that adult Ae. aegypti disperse relatively short distances, suggesting that people rather than mosquitoes are the primary mode of dengue virus dissemination within and among communities. INTRODUCTION Knowledge about flight range and dispersal of mosquito vectors is essential for understanding vector-borne disease transmission dynamics among human populations because flight range and dispersal influence mosquito population dynamics, patterns of genetic structure, 1,2 and pathogen transfer through vector populations. In an applied sense, dispersal is an important factor for determining appropriate control limits necessary to interrupt pathogen transmission and is a fundamental consideration for estimating gene flow in genetic control strategies. 3 With renewed interest in autocidal and genetic control strategies, there is an increased awareness of how little is known about movement of adult mosquito vectors in nature and the importance of gathering that kind of information. 4 Aedes aegypti is the primary vector of dengue, the most important arboviral human infection worldwide, and urban yellow fever. Approximately million cases occur annually and more than 2.5 billion people are at risk of infection. 5 Adult dispersal and flight range for this species have been estimated from results of a few mark-release-recapture studies Those publications cite maximum flight distances for Ae. aegypti that range from 154 to 1,207 meters. 7,14 Movement of genetically marked mosquitoes was assessed by some investigators. 19,20 It is not clear, however, if their estimates based on genetic mutants reflect dispersal of wild-type mosquitoes. Reiter and others used the detection of eggs laid by rubidium-labeled females in ovitraps to estimate a maximum flight range of 3,600 meters for Ae. aegypti in San Juan, Puerto Rico. 21 Honorio and others similarly reported detection of rubidium-marked eggs up to 800 meters from the release point in Rio de Janeiro, Brazil. 22 Published studies provide widely variable results and no clear consensus about the patterns of Ae. aegypti movement and dispersal. In an effort to contribute more definitive, replicated data, herein we present results for the first part of our analysis of Ae. aegypti flight range and dispersal from a series of 21 experiments conducted over a 10-year period in three 209 different field sites where dengue is endemic. Our second article on this topic, which will be published separately, will be an analysis of the probabilities of dispersal from one location (house) to another, which will be compared with conventional methods used in this report for estimating the distance that adult mosquitoes move by flight. MATERIALS AND METHODS A summary of the various methods for all experiments is presented in Table 1. Our methods varied among different locations and times because mark-release-recapture experiments were carried out for different reasons. In the conducting those experiments, we gathered the data on Ae. aegypti dispersal that we present and analyze herein. Although differences in methodology prohibit a simple explanation of our study design, it adds strength to our overall conclusions because our results are consistent across many different experiments conducted in a variety of regions of the world, using various release and recapture scenarios. We did not attempt to directly compare experiments using different methods. Only when the same methodology was used did we test for statistical differences among or between release-recapture experiments. This research was conducted in accordance with the following Institutional Review Board approvals: University of Maryland (A-3433), University of California at Davis ( ), Walter Reed Army Institute of Research (752), Thai Ministry of Health Ethical Review Committee for Research in Human Subjects, University of Massachusetts (M1003), and Cornell University (FWA ). Puerto Rico (January and July 1996). Field site. Our release area in Puerto Rico was described in detail by Harrington and others. 18 Briefly, releases were conducted in the village of Yanes III, Florida, a community in north central Puerto Rico ( N, W) consisting of 165 houses surrounded on three sides by limestone hills that appeared to us to be barriers to dispersal (Figure 1). Mosquitoes. Aedes aegypti eggs were collected from ovi-
2 210 HARRINGTON AND OTHERS Location TABLE 1 Summary of the methods used for mark-release recapture studies* Release site Sex No. of release houses No. of release days No. of recapture houses No. of recapture days Recapture regimen (days post-release) HSR, Thailand March June 1991 Outdoor F HSR, Thailand March June 1991 Outdoor M HSR, Thailand January 1992 Indoor F HSR, Thailand January 1995 Indoor F HSR, Thailand July 1995 Indoor F Florida, Puerto Rico January 1996 Indoor F Florida, Puerto Rico July 1996 Indoor F Lao Bao, Thailand February 2000 Indoor F (all) 10 Lao Bao, Thailand July 2000 Indoor F (all) 10 Lao Bao, Thailand January 2001 Indoor F (all) 10 Lao Bao, Thailand July 2001 Indoor F (all) 10 Mae Kasa, Thailand February 2000 Indoor F Mae Kasa, Thailand July 2000 Indoor F Mae Kasa, Thailand January 2001 Indoor F Mae Kasa, Thailand July 2001 Indoor F Pai Lom, Thailand January 2001 Indoor F (all) Pai Lom, Thailand July 2001 Indoor F (all) Lao Bao, Thailand January 2002 Indoor F (all) 4 1 Lao Bao, Thailand July 2002 Indoor F (all) 4 1 Pai Lom, Thailand January 2002 Indoor F (all) 4 1 Pai Lom, Thailand July 2002 Indoor F (all) 4 1 * HSR Hua Sam Rong. 1 4 days post-release days post-release. 1, 4, 12, and 13 days post-release in first five houses and 2, 4, 7, and 8 days post-release in second group of five houses. traps in Yanes III, hatched, and reared in the insectary of the Centers for Disease Control and Prevention in San Juan, as described previously. 17 After eclosion, adults were held in 45-cm 2 cages and allowed access to water but not food. January February Mosquitoes were divided into two cohorts. One was offered a blood meal from one of the investigators arms one day prior to release when they were 3 4 days old. The other cohort was maintained on water only. FIGURE 1. Yanes III, Florida, Puerto Rico. July A 3- and 13-day-old blood fed cohort was maintained as described previously. 18 Marking in January February and July Female mosquitoes were marked with paint and fluorescent dust following the methods of Edman and others. 17 Paint color designated release houses were marked with paint one day prior to release and marked with fluorescent dust to designate cohort. Release. Twenty-five mosquitoes from each cohort (water and blood fed in January February 1996 and 3- and 13-dayold in July 1996) were released at 5:30 PM inside six houses (total released for both cohorts 300). Recapture. Backpack aspirators (John C. Hock Co., Gainesville, FL) were used for approximately 15 minutes per house in an attempt to recapture mosquitoes for 10 days following release inside release houses as well as in 14 adjacent houses in the area. 18 Thailand, Hua Sam Rong. Releases were conducted in Village Six ( N, E), Hua Sam Rong, Amphur Pleangyao, Chachoengsao Province, located in eastcentral Thailand during March June 1991, January 1992, January 1995, and July Outdoor releases, March June The release area for the experiments is described in detail by Harrington and others 18 and was located in the west end of the village and surrounded on three sides by rice paddy (Figure 2). In these experiments, we considered the house next to the release site as the adjacent house. Mosquitoes. F 1 progeny from wild females collected in the study area were reared at Mahidol University in Bangkok under small (4,000 larvae/jar), medium (2,000 larvae/jar), and large (1,000 larvae/jar) body size diet regimens. 23 In March, April, and June 1991, cohorts of large and small body size were marked and released. In May 1991, large, medium, and small body size cohorts were similarly reared, marked, and released. Adult female wing length averages were 2.26, 2.59 and 2.93 mm for small, medium, and large body size cohorts, respectively.
3 DISPERSAL OF AE. AEGYPTI 211 FIGURE 2. Village 6, Hua Sam Rong, Thailand. Marking. Following the methods of Edman and others, 17 male and female mosquitoes were marked one day prior to or on the morning of release with fluorescent dust to designate each size cohort Release. Mosquitoes were released between 5:00 PM and 6:00 PM in a bamboo thicket on the edge of the village (Figure 2). In March 1991, 2,000 females and 2,000 males were released. In April 1991, 1,440 females and 1,615 males were released. In May 1991, 2,000 females and 1,500 males were released. In June 1991, 2,235 females and 1,835 males were released. No significant differences (P < 0.01) were found in recapture rates among diet cohorts using non-linear regression analysis (PROC IML, PROC NLIN, SAS Institute, Cary, NC) followed by bootstrapping of capture confidence intervals. 24 Consequently, the data were combined for all four months for each sex to evaluate final recapture rates and dispersal distances. Recapture. Aspirator collections (15 20 minutes/house) using modified vacuum cleaners were carried out for 12 days after release between 9:00 AM and 4:00 PM in 20 houses throughout the village at various distances from the release area. Collected mosquitoes were placed on wet ice and transported to the field laboratory where male and female Ae. aegypti were identified to species and examined for dust markings. Indoor release, January Mosquitoes. Medium and large size larvae were reared outdoors at Mahidol University in Bangkok from Hua Sam Rong colony eggs (20 30 generations in colony). Marking. Females were marked with a small dot of poster paint on their thorax to designate the house in which they were released. Release. Fifty females were released inside each of 12 houses at the far west end of Village Six. Mosquitoes were offered a blood meal on one of the investigators arms just prior to release. Recapture. Mosquitoes were recaptured with aspirators as described earlier between 9:00 AM and 4:00 PM for 10 consecutive days after release in the 12 release and 8 additional houses located in the western end of the village. Indoor release, January and July Mosquitoes. Eggs were hatched from a Mahidol University colony derived from adult females captured in Village Eight, Hua Sam Rong. Larvae were reared under a standard diet regimen to obtain medium body size. Emerged adult females were divided into four nutritional groups and offered 1) water only, 2) sugar and water, 3) blood and water, or 4) blood, sugar, and water for three days prior to release. Marking. Females were marked with different colored dust and paints to designate diet cohort and release house. Release. One hundred females (25 from each adult diet cohort) were released inside each of six houses (January 1995) and each of eight houses (July 1995) in Village Six as described earlier. Recapture. In January 1995, mosquitoes were recaptured with aspirators as described earlier between 10:00 AM and 4:00 PM in each of the six release houses and six neighboring houses for eight consecutive days after release. The same recapture method was used in July 1995 with the exception that collections began the second day after release in each of
4 212 HARRINGTON AND OTHERS the eight release houses and five neighboring houses for nine consecutive days. Thailand, Mae Sot. The release villages of Pai Lom (16 45 N, E, Figure 3) and Lao Bao (16 45 N, E, Figure 4) are located in Mae Pa district 5 km north of Mae Sot city in the westcentral region of Thailand along the Thailand- Myanmar border. The village of Mae Kasa (16 53 N, E, Figure 5) is located 20 km north of Mae Sot. All three villages are located in an area where dengue is endemic and transmission of all four dengue virus serotypes occurs. Releases were conducted during the middle of the dry season (January March) and during the middle of the rainy season (July August). In addition to climatic differences, these seasons also represented periods of low and high dengue transmission, respectively. 25 A study to determine the efficiency of aspirator collections versus sticky ovitraps 26 for capturing mosquitoes was conducted in Pai Lom during January An identical release, but only using aspirator collection was carried out in July Additional data on dispersal were gathered in Mae Sot during experiments designed to validate a cuticular hydrocarbon age-grading method and to test the hypothesis that survival is age dependent (Harrington LC, Edman JD, Scott TW, unpublished data). 27 Releases were conducted in Pai Lom in January and July 2001 and 2002, in Lao Bao in February and July 2000 and January and July , and in Mae Kasa in February and July 2000 and January and July Mosquitoes. February Aedes aegypti pupae were collected from natural development sites in the release villages of Lao Bao and Mae Kasa one month prior to the study, returned to the Armed Forces Research Institute for Medical Sciences Laboratory in Bangkok and held until adult emergence. Females were allowed to mate and were offered a blood meal from an anesthetized hamster (in compliance with National Institutes of Health guidelines for humane use of animals, Armed Forces Research Institute for Medical Sciences Protocol # 03-06). Eggs were collected, conditioned, and transported back to the field laboratory in Mae Pa, Mae Sot where they were hatched in rainwater and adults of uniform body size were reared by placing 2,000 larvae in large clay water jars (50 liters). Larvae were offered a diet of ground fish food (CP brand; Chaleorn Poolaphan Co., Bangkok, Thailand) to obtain mosquitoes of medium body size (mean wing length 2.59 mm) as described earlier. After emergence, females were placed in four-liter plastic bucket cages with mesh lids. Males were added to cages to FIGURE 3. Pai Lom village, Amphur Mae Sot, Thailand. The house symbols indicate houses or collection locations.
5 DISPERSAL OF AE. AEGYPTI 213 FIGURE 4. Lao Bao village, Amphur Mae Sot, Thailand. The house symbols indicate houses or collection locations. ensure mating. Females were offered blood from a human arm for 20 minutes daily and water throughout the holding period. July 2000 July Pupae were collected from the study villages and held in the field laboratory until emergence, and then placed in four-liter plastic bucket cages and maintained as described earlier. Marking. Mosquitoes were sedated with wet ice and marked 1 2 days prior to release with paint on the thorax to designate release house and florescent powder on the morning of release to designate release day, following the methods of Edman and others. 17 Releases in in Lao Bao and Mae Kasa. February Mosquitoes were released in a maximum of 12 houses per village each day over an 11-day period from January 31 to February 1, 2000 and from February 3 to February 11, 2000 in the villages of Mae Kasa and Lao Bao. All releases during were conducted between noon and 6:00 PM. July Mosquitoes were released from July 16 to July 25, 2000 in the villages of Mae Kasa and Lao Bao as described for February January Mosquitoes were released in two groups in 10 houses (total of 20 houses) from January 14 to January 18 for group 1, and from January 19 to January 23 for group 2. July Mosquitoes were released in two groups in 10 different houses from July 13 to July 17. Releases in 2002 in Lao Bao and Pai Lom. Ten cohorts, each composed of mosquitoes aged at two-day intervals, representing ages 1 2, 3 4, days old were simultaneously released in 12 houses in each village on January 31 and again on February 4 during the dry season in During the rainy season, 10 similar age cohorts were released into 10 houses in each village on August 2 and August 6. All releases were conducted between 10:00 AM and noon. Recaptures. Since mosquito collections using batterypowered backpack aspirators in northwestern Thailand demonstrated that the majority of Ae. aegypti are collected resting inside houses, collections were focused indoors. For all release-recapture experiments in Mae Sot, aspirator collection cartons were placed in plastic bags in a cooler of wet ice in the field and transported to the field laboratory where the mosquitoes were anesthetized with carbon dioxide and placed in tubes on wet ice. Paint and dust colors on marked Ae. aegypti were identified with the aid of a dissecting microscope and recorded Mae Kasa and Lao Bao. Release houses and approximately 20 neighboring houses were aspirated for minutes each between 8:00 AM and 6:00 PM. To obtain the greatest number possible of older mosquitoes, the timing of recaptures was modified as follows. During February 2000, collections were conducted daily on February and February 20 24; during July 2000, collections were conducted daily on July and on August 5 10; during January 2001 collections were conducted on January 19, 22, 30, and 31 and on February 1 and 2 for group 1 and on January 25, 27, 30, and 31 and on February 1 and 2 for group 2; during July August 2001, collections were conducted on July 18, 21, 29, 30, and 31 and on August 1 for group 1 and on July 23, 26, 29, 30, and 31 and August 1 for group Lao Bao and Pai Lom. Recaptures were attempted in all houses in each study village as well as in all houses between the two villages. In the dry season, recaptures were attempted on February 1, 2, 5, and 6, During the rainy season, recaptures were attempted on August 3, 4, 7, and 8, Evaluation of dispersal detection methods. To compare different methods for detecting dispersal and to determine if the aspiration method we had used in previous studies was the best approach, sticky ovitraps versus backpack aspirator collections were compared. In Pai Lom (January July 2001), mosquitoes were collected as pupae, allowed to emerge in the field laboratory, and held in plastic bucket cages as described earlier for the Mae Sot studies. Females were offered a blood meal from the arm of one of the investigators three days prior to release to ensure that gravid females were marked and released. Mosquitoes were marked with paint and dusts as described earlier for Mae Sot. In the second release, cohorts 1 and 2 were designated with a unique color placed on the thorax next to the dot on their thorax that designated their release house. January Sticky ovitraps were prepared by lining the top two-thirds of black plastic four-liter buckets ( cm; Sweda Plastic Co., Bangkok, Thailand) with adhesive (Tangle-Trap insect coating; The Tanglefoot Co., Grand Rapids, MI) coated black paper. Prior to release, three ovitraps per house (total of 105 traps) were placed in every house (two indoors and one outdoors) in the village of Pai Lom. At the time of placement of sticky ovitraps in houses, approximately one liter of water was poured into the bottom of the bucket. Release 1 was conducted between 5:45 PM and 7:00 PM on January 18, 2001 and release 2 was conducted between 4:00 PM and 5:00 PM on January 31, A total of 150 marked mosquitoes were released in 15 houses (approximately 0 per house) on one end of Pai Lom for release 1. The same methods were followed for release 2, except that fewer mosquitoes (n 60) were released. The 15 houses selected for release 2 were located on the opposite side of the village from those used in release 1.
6 214 HARRINGTON AND OTHERS FIGURE 5. Mae Kasa village, Amphur Mae Sot, Thailand. The house symbols indicate houses or collection locations. July One release was conducted from 5:00 PM to 6:00 PM on July 19, 2001 to examine the effect of releasing mosquitoes inside versus outside of the house. Mosquitoes were released inside 10 houses in the center of Pai Lom and outside (approximately 10 meters from the back of each release house). A total of 90 and 91 mosquitoes were released indoors and outdoors, respectively. Recaptures. January Aspirator collections using battery-powered backpack aspirators were carried out to recapture mosquitoes for minutes in each house in the village of Pai Lom (n 35 houses) beginning four days after release. Collections were made from 8:00 AM to 5:00 PM over four consecutive days. Captured mosquitoes were returned to the field laboratory, anesthetized with carbon dioxide, and then placed on wet ice in plastic tubes for at least 30 minutes. Female Ae. aegypti were examined carefully under a dissecting microscope for paint and/or fluorescent dust markings. The number of captured marked and wild Ae. aegypti was recorded daily for each house. During the four-day collection period, every sticky ovitrap was examined daily for marked and wild Ae. aegypti. Mosquitoes adhering to sticky ovitrap liners were returned to the field laboratory and examined under a dissecting microscope. The same methods were followed for release 2. One day after the last collection day for release 1, each house in the village, from which consent was obtained, was sprayed with deltacide (deltamethrin/resmethrin; BASF Corp., Limburgerhof, Germany). A four-day interval was allowed between spraying and release 2. Following release 2 and the collection period, all houses in Pai Lom were sprayed again with insecticide. July Aspirator collections were conducted in every house in Pai Lom for four consecutive days, beginning four days after release as described for January After the last collection day, all houses in the village were sprayed with insecticide as described earlier. Data analysis. Dispersal distances were measured and recorded for each recaptured mosquito as the distance from release to recapture house. Our dispersal estimates do not account for indirect flight patterns, but represent meaningful net movement from house to house. Distances between houses in Puerto Rico and Hua Sam Rong, Thailand were measured manually or within a geographic information system where sites have been geographically referenced. The Thai villages of Lao Bao, Pai Lom, and Mae Kasa were mapped using the geographic information system in MapInfo Professional 7.0 (MapInfo Corp., Troy, NY). Dispersal distances for each mosquito were measured, categorized by the number of houses away from the release site, and recorded. Dispersal distances for different body sized mosquitoes in
7 DISPERSAL OF AE. AEGYPTI 215 TABLE 2 Recapture rates for male and female Aedes aegypti released outdoors in Thailand from March to June 1991 (data combined) and indoors in January 1992 and January and July 1995* Overall recapture rate Adjacent or release house 1 house 2 houses Recapture rates [total number recaptured by location] (distance from site) 3 houses 4 houses 5 houses 6 houses March June 17% 65% [841] 24% [308] 7% [90] 3% [33] < 1% [7] < 1% [9] < 1% [1] 1991 (33 61 m) (60 94 m) ( m) ( m) ( m) ( m) March June 17% 72% [836] 15% [173] 5% [60] 6% [75] 2% [22] < 1% [2] 0% [0] 1991 (33 61 m) (60 94 m) ( m) ( m) ( m) ( m) January 38% 77% [173] 15% [33] 6% [14] 6% [6] 0% [0] 0 [0] 1992 (15 m) (32 m) (52 m) (67 m) (> 67 m) January 17% 83% [86] 11% [11] 5% [5] 2% [2] 0% [0] 0% [0] 1995 (15 m) (40 m) (48 m) (65 m) (> 65 m) July 16% 53% [67] 24% [30] 20% [25] 3% [4] 0% [0] 0% [0] 1995 (15 m) (36 m) (56 m) (68 m) (> 68 m) *m meters. For outdoor releases this was the house next to the release site. Released outdoors. Released indoors. Average distance from release site. outdoor releases from March to June 1991 and diet cohorts from January to July 1995 were not significantly different (P < 0.01) from each other using non-linear regression analysis (PROC IML, PROC NLIN, SAS Institute) followed by bootstrapping of capture confidence intervals. 24 Consequently, those data were combined to augment sample sizes before analysis. Data were analyzed in SAS using PROC GLM with dispersal distance as the independent variable to determine season, village, and age-related differences in dispersal. In addition to evaluation of dispersal distances, the proportions of mosquitoes captured with sticky traps versus aspirator collections in Pai Lom from January 2001 were compared. Data for release 1 and 2 in Pai Lom, January 2001, were not significantly different (P > 0.05) and were combined. RESULTS Thailand, Hua Sam Rong. Outdoor releases of males and females, March June Recapture rates for males and females across all outdoor releases were the same (17%). The majority of males (72%) and females (65%) were captured in the house adjacent to their outdoor release location. Maximum dispersal distance detected was six houses away from the release site ( meters) for females and five houses away for males ( meters) (Table 2). Indoor releases of females, January The overall recapture rate for female Ae. aegypti released indoors (38%) was greater than for the outdoor releases (1991; 17%; Table 2). The majority of recaptured mosquitoes (77%) were collected in the house from which they were released. The maximum dispersal distance detected was three houses away or 52 meters from the release site (Table 2). January and July Recapture rates for indoor released mosquitoes were lower overall in January and July 1995 (16 17%) than in The majority of females were collected in their release houses and the average maximum dispersal distance detected was similar to the indoor release in January 1992 (48 56 meters) (Table 2). Puerto Rico, Yanes III. January The overall recapture rate was 34%. Eighty-seven percent of recaptures were collected in the house where they were released and only 1% of recaptures were collected three or more houses from the release point (102 meters) (Table 3). July The overall recapture rate was 23%. Eighty percent of recaptures were collected in the house where they were released and only 1% of recaptures were collected three or more houses from the release point (102 meters) (Table 3). Thailand, Mae Sot Region. February 2000 and July 2001 releases in Mae Kasa and Lao Bao. Overall recapture rates were lower for our experiments in northwestern (Mae Sot region) than for those in eastcentral Thailand (Hua Sam Rong region), ranging from 4% to 9%. Differences were most likely due to changes in recapture protocols. Recapture attempts were attenuated and less intensive in the Mae Sot region. Recapture rates in Mae Kasa (4 8%) were consistently lower than in Lao Bao (6 9%) from July 2000 to July 2001 (Table 4). Dispersal rates were similar among seasons (dry season January and rainy season July) and within villages. Of the total mosquitoes recaptured, a large proportion in both villages (Mae Kasa 44 77%, Lao Bao 50 TABLE 3 Recapture rates and total numbers for Aedes aegypti released indoors in Puerto Rico, January 1996* Location Overall recapture rate Release house (0 m) 1 house (12 30 m) Recapture rates (total number recaptured by location) 2 houses (43 62 m) 3 houses ( m) > 3 houses (102 m) Puerto Rico January % (101) 87% (88) 5% (5) 4% (4) 3% (3) 1% (1) Puerto Rico July % (69) 80% (55) 6% (4) 9% (6) 4% (3) 1% (1) *m meters.
8 216 HARRINGTON AND OTHERS TABLE 4 Recapture rates for Aedes aegypti released indoors in Thailand conducted from 2000 to 2001 in the villages of Lao Bao and Mae Kasa Location Overall recapture rate Release house Adjacent house % Recaptured of total recaptures by location (total number recaptured by location) 2 houses 3 houses > 3 houses Lao Bao February % (62) 66% (41) 11% (7) 10% (6) 2% (1) 11% (7) Lao Bao July % (83) 70% (58) 12% (10) 13% (11) 2% (2) 2% (2) Lao Bao January % (68) 50% (34) 20% (13) 13% (9) 6% (4) 12% (8) Lao Bao July % (69) 65% (44) 15% (11) 10% (7) 3% (2) 7% (5) Mae Kasa February % (48) 77% (37) 17% (8) 0% (0) 0% (0) 6% (3) Mae Kasa July % (39) 44% (17) 5% (2) 15% (6) 3% (1) 33% (13) Mae Kasa January % (35) 57% (20) 29% (10) 6% (2) 6% (2) 3% (1) Mae Kasa July % (52) 75% (39) 12% (6) 2% (1) 0% (0) 12% (6) 70%) was captured in their release houses. However, a large proportion of recaptures in July 2000 in Mae Kasa (33%) were made greater than three houses from their release sites (Table 4). The mean ± SE dispersal distance in Mae Kasa (75 ± 33 meters for February and 199 ± 29 meters for July 2000) was greater than for mosquitoes recaptured in Lao Bao (71 ± 16 meters for February and 40 ±5meters for July 2000) (Table 5). Of those mosquitoes released, the majority was recaptured within 100 meters of their release site (Figure 6). Age of mosquitoes recaptured (Figure 6), season, and year were not significant effects on dispersal. Village was the only significant factor affecting dispersal distance (F 5.75, degrees of freedom [df] 21, P < 0.001; age F 1.32, df 18, P 0.171; season F 0.90, df 1, P 0.344; village F 96.62, df 1, P < 0.001; year F 1.29, df 1, P 0.257, by SAS PROC GLM). No interactions were statistically significant. The maximum dispersal distance detected was 566 meters in Mae Kasa (July 2001) and 512 meters in Lao Bao (January 2001). January July 2002 releases in Lao Bao and Pai Lom. During 2002 in the Mae Sot region, overall recapture rates were greater during the rainy season (July) than in the dry season (January) in each village (Table 6). Mosquitoes moved farther in the rainy season (mean ± SE 117 ± 27 meters) than in the dry season (45 ±6meters) and in Pai Lom (156 ± 36 meters) than in Lao Bao (68 ± 30 meters) (Table 5). Of those mosquitoes that did move from release houses, the majority was recaptured within 50 meters of their release site (Figure 7). One mosquito released in Pai Lom in July 2002 was collected in a house in Lao Bao 346 meters from its release house. Village (Pai Lom > Lao Bao) was the only significant variable impacting dispersal distances (F 1.51, df 22, P 0.07; age F 1.34, df 20, P 0.16; season F 0.84, df 1, P 0.36; village F 5.86, df 1, P 0.016, by SAS PROC GM). No interactions were significant. Agedependent dispersal effects were not detected (Figure 7), consistent with results from our release-recapture experiments. Comparison of dispersal detection methods (Pai Lom). January Recaptures: release 1 and 2 combined. Twenty-two percent of the marked mosquitoes were recaptured (Table 7). Nearly all of recaptured mosquitoes (n 44, 21%) were collected with the backpack aspirator method rather than with sticky ovitraps (1%). Only two marked Ae. aegypti females and one wild male were found in indoor sticky ovitraps. None were TABLE 5 Dispersal of Aedes aegypti released indoors in Thailand and Puerto Rico from 1992 to 2002* Location Total released No. of mosquitoes moving Distance traveled (m) Minimum Maximum Mean ± SE Puerto Rico 300 January Puerto Rico 300 July Thailand-Lao Bao 703 February ± 16 Thailand-Mae Kasa 610 February ± 33 Thailand-Lao Bao 937 July ± 5 Thailand-Mae Kasa 988 July ± 29 Thailand-Pai Lom 210 January ± 35 Thailand-Lao Bao 983 January ± 25 Thailand-Mae Kasa 904 January ± 24 Thailand-Pai Lom 181 July out 40 ± 22 out (2 out/6 in) in 36 ± 7 in Thailand-Lao Bao 995 July ± 7 Thailand-Mae Kasa 1,005 July ± 53 Thailand-Lao Bao 1,047 January ± 3 Thailand-Pai Lom 1,067 January ± 12 Thailand-Lao Bao 531 July ± 30 Thailand-Pai Lom 594 July ± 36 *m meters. Distances were recorded in ranges from the release point instead of actual values.
9 DISPERSAL OF AE. AEGYPTI 217 FIGURE 6. Dispersal of Aedes aegypti by age since emergence over all seasons and villages in Thailand, February 2000 July FIGURE 7. Dispersal of Aedes aegypti by age since emergence over all seasons and villages in Thailand, January July captured in outdoor sticky traps. The majority (77%) of mosquitoes were collected in their release house or the house adjacent to it (Table 7). Dispersal: release 1 and 2. The greatest distance that we could detect dispersal within Pai Lom was 290 meters. The mean ± SE dispersal distance of those mosquitoes that moved was 124 ± 35 meters. Three females released in Pai Lom were collected in the neighboring village of Lao Bao (maximum distance 512 meters, Table 5). July Recaptures. More Ae. aegypti from indoor releases were captured (n 8, 8.8%) than from outdoor releases (n 5, 5.5%). Dispersal. The mean ± SE dispersal distances for mosquitoes released outdoors versus indoors were similar (40 ± 22 meters indoors and 36 ± 7 meters outdoors, Table 5). No marked mosquitoes released in Pai Lom were collected in Lao Bao during July DISCUSSION Results from our studies repeatedly indicate limited movement of the dengue vector Ae. aegypti regardless of sex (males versus females), release village, release location (indoors versus outdoors), season (high or low dengue transmission season), date, geographic region, or experimental protocol. The majority of released mosquitoes were recaptured in the same house or an adjacent house to where they were released. This pattern in recapture results was consistent among our three different field sites, two in Thailand and one in Puerto Rico. We did not directly assess the effects of marking on mosquito survival and behavior, but other investigators reported no adverse effects from marking with paints 28,29 or Dayglo dusts. 30 Our comparison of aspirator collections versus sticky ovitraps for assessing dispersal clearly indicated that our aspirator collections were far more efficient. Other investigators have reported higher rates of capture with sticky ovitraps and sticky panels ranging from 3.6% to 13%, 16,26 and sticky ovitraps were an efficient means of capturing wild Ae. aegypti in Australia. 31 None of these studies, however, compared ovitraps with the aspirator collection method. Perhaps natural ovipostion sites were less abundant at the study sites of other investigators than in Pai Lom. We designed our study to be conducted with gravid females during the dry season when oviposition trap efficiency should have been optimal. We assessed mosquito movement in Lao Bao and Mae Kasa from 2000 to 2001 over a protracted recapture period (24 days), which should have allowed marked mosquitoes maximum opportunity to move. The only factor that impacted dispersal distances in that series of experiments was the village in which mosquitoes were released. That effect may have been due to differences in the layout of houses and distances between houses in the respective villages. Lao Bao (where mean dispersal was meters) is a smaller village than Mae Kasa, in which houses are spatially clustered with footpaths between houses. In Mae Kasa, where we detected a maximum dispersal distance of 566 meters and the mean ranged from 75 to 199 meters, houses were located farther apart along one main paved road with fewer foot paths between them. Other studies have similarly cited the effect of TABLE 6 Recapture rates for Aedes aegypti released indoors in Thailand from January to July 2002 in the villages of Lao Bao and Pai Lom Location Overall recapture rate Release house Adjacent house % Recaptured of total recaptures by location (total number recaptured by location) 1 house 2 houses > 2 houses Lao Bao January % (80) 59% (47) 25% (20) 16% (13) 0% (0) 0% (0) Lao Bao July % (55) 82% (45) 4% (2) 5% (3) 5% (3) 4% (2) Pai Lom January % (92) 70% (64) 15% (14) 7% (6) 5% (5) 3% (3) Pai Lom July % (40) 75% (30) 3% (1) 0% (0) 5% (2) 17% (7)
10 218 HARRINGTON AND OTHERS TABLE 7 Recapture rates for Aedes aegypti released indoors in Pai Lom, Thailand to assess dispersal, January July 2001 Location Overall recapture rate Release house % Recaptured of total recaptures by location (total number recaptured by location) Adjacent house 1 house 2 houses > 2 houses Pai Lom January % (46) 47% (22) 30% (14) 9% (4) 7% (3) 7% (3) Pai Lom July % (13) 38% (5) 31% (4) 23% (3) 0% (0) 8% (1) house distribution and pattern on Ae. aegypti dispersal. In a study conducted in China, Tsuda and others reported less dispersal of released Ae. aegypti in areas where the houses were clustered closer together than when they were farther apart. 32 Releases in Lao Bao and Pai Lom ( ) provided an ideal situation for assessing inter-village movement between rural communities. Pai Lom is more similar to Lao Bao than Mae Kasa in layout and the two villages are approximately 300 meters apart. During the course of our experiments in the Mae Sot area, we detected inter-village movement only four times in 834 mosquitoes recaptured (0.5%) and 7,511 marked mosquitoes released, indicating that this range of movement is unusual for flying adult female Ae. aegypti. During 2002, recaptures in Lao Bao and Pai Lom were conducted over a short period of time (two days after release) and provide an indication of movement in the initial days after release or emergence. Overall, mosquitoes recaptured during this shorter interval were recovered within 50 meters of the release house, whereas those recaptured over the more protracted period ( ) were collected within 100 meters of their release site. During our 2000 experiments in Lao Bao and Mae Kasa, mosquitoes dispersed greater distances during the rainy compared with the dry season. This indicated that greater dispersal occurs initially during the rainy season, but may even out over several days, as was detected during the experiments. Despite the differences in the recapture interval, no age-dependent dispersal was detected in either series of experiments. Some investigators have reported greater dispersal among teneral or very young female Ae. aegypti. 11 In our experiments from 2002, 1 2-day-old mosquitoes released in January and July dispersed an average of 56 meters, a distance that was not significantly different among a variety of age groups that we released and recaptured. In a series of 21 mark-release-recapture studies conducted over a 10-year period, we did not detect dispersal of Ae. aegypti far from its release site. Our data were derived from replicated releases in several villages, seasons, and geographic locations using different collection procedures. Although maximum flight range has been emphasized by researchers in the past, we chose to focus on the mean dispersal distance, which we consider a more epidemiologically meaningful population parameter than the maximum distance moved by relatively few mosquitoes. The mean dispersal distances detected in our study ranged from 28 to 199 meters depending on the site, village, and country. Although, most mosquitoes did not move from their release houses, the majority of those that did move were recaptured within 100 meters of their release site. Even though in several of our experiments we could have caught mosquitoes that moved thousands of meters, we did not detect the kind of long distance dispersal reported by investigators who assayed for rubidium in Ae. aegypti eggs. 21,22 Our data indicate that in rural habitats with abundant human hosts and oviposition sites, Ae. aegypti do not disperse far from their development site in and around homes and tend to be spatially clustered at the household level. Interestingly, the same conclusion was made using a different approach, spatial statistics, to analyze data on different measures of Ae. aegypti density in Iquitos, Peru. 33 Our results lead to at least three predictions for different dengue prevention strategies. First, female Ae. aegypti may spend their lifetime in or around the houses where they emerged as adults, which is consistent with the feasibility of killing infected mosquitoes by applying localized, intensive vector control around areas of clinically apparent human dengue infection. Second, our data also support the idea that people rather than mosquitoes rapidly move dengue virus within and among communities. 34,35 By itself, therefore, localized insecticide application around a dengue patient s home or community is not likely to prevent the spread of dengue infections. By the time a clinical human infection is detected the resident infected mosquito may have bitten another person who transported the virus beyond the house or community where the mosquito resides. Third, our results highlight the challenges that genetic and autocidal control programs 36 will face. Inoculative releases 37 of modified mosquitoes over relatively short distances (< 100 meters) will be essential to ensure comprehensive introductions, mating with wild type conspecifics, and sweeps of transgenes through populations. Received March 9, Accepted for publication May 30, Acknowledgments: We are indebted to the people of Yanes III, Puerto Rico; Village 6 Hua Sam Rong; and the villages of Pai Lom, Lao Bao, and Mae Kasa, Mae Sot, Thailand, for allowing us to work in their homes and their support, cooperation, and assistance with this study. We thank Dr. W. Swaddigwongporni and Dr. J. Pradit and all of the members of the Community Health Program at Mae Sot Hospital, Pirom Sangsuab at Hua Sam Rong Health Center, and Boonruang Yakeaw at Mae Pa Health Center for their support. From AFRIMS in Bangkok, Somporn Changimongkol, Alongkot Ponlawat, Warisa Tangjinjai, Siriporn Mungviriya, and Patcharee Khongtak assisted with the Thai field studies. Health volunteers Porapol Meungcheun and Lan Chummoi assisted with releases. Benjamas Pongnapakul assisted as a driver. Somboon Intawong, Pornchai Harujai, Aun Manowong, Chaiwut Lerchai, Somboon Kantang, Manit Chaiya, Chatree Chumpen, and Boonkuea Malisor assisted with collections in the Mae Sot region. Somboon Srimarat, Kitti Theinthong, and Samnieng Theinthong assisted with research and collections in the Hua Sam Rong region. We also thank Daniel Strickman for the Hua Sam Rong Village 6 map and Elizabeth Kurrle for creating the Mae Sot region maps. Financial support: This research was supported by the National Institutes of Health grant AI
11 DISPERSAL OF AE. AEGYPTI 219 Authors addresses: Laura C. Harrington, Department of Entomology, Cornell University, Ithaca, NY 14850, Telephone: , Fax: , Thomas W. Scott and John D. Edman, Department of Entomology, University of California, 1 Shields Avenue, Davis, CA , s: twscott@ucdqavis.edu and jdedman@ucdavis.edu. Kriangkrai Lerdthusnee, Russell C. Coleman, James J. Jones, and Ratana Sithiprasasna, Department of Entomology, Armed Forces Research Institute for Medical Sciences, Bangkok, Thailand, s: Colemanre@amedd.army.mil, james.jones@afrims.org, and ratanas@afrims.org. Adriana Costero, Medical Entomology Section. Laboratory of Parasitic Diuseases, National Institutes of Allergy and Infectious Diseases, National Institutes of Health, Bethesda, MD , acostero@niaid.hih.gov. Gary G. Clark, Dengue Branch, Centers for Disease Control and Prevention, San Juan, PR , ggc1@cdc.gov. Sangvorn Kitthawee, Department of Biology, Faculty of Science, Mahidol University, Bangkok, Thailand, grskt@mucc.mahidol.ac.th. Pattamaporn Kittayapong, Center for Vectors and Vector-Borne Diseases and Department of Biology, Faculty of Science, Mahidol University, Bangkok, Thailand, grpkt@mucc.mahidol.ac.th. Reprint requests: Laura C. Harrington, Department of Entomology, Cornell University, Ithaca, NY REFERENCES 1. Kuno G, Factors influencing the transmission of dengue viruses. Gubler DJ, Kuno G, eds. Dengue and Dengue Hemorrhagic Fever. New York: CAB International, Service MW, Mosquito (Diptera: Culicidae) dispersal: the long and short of it. J Med Entomol 34: Service M, Mark-recapture techniques and adult dispersal. Mosquito Ecology: Field Sampling Methods. New York: Chapman and Hall, Scott TW, Takken W, Knols BJG, Boëte C, The ecology of genetically modified mosquitoes. Science 298: Gubler DJ, Dengue and dengue hemorrhagic fever: its history and resurgence as a global public health problem. Gubler DJ, Kuno G eds. Dengue and Dengue Hemorrhagic Fever. Wallingford, United Kingdom: CAB International, Gubler DJ, Kuno G, eds. Dengue and Dengue Hemorrhagic Fever. Wallingford, United Kingdom: CAB International. 7. Burgher JC, Taylor M, Radiophosphorus and radiostrontium in mosquitoes. Preliminary report. Science 110: Morland HB, Hayes RO, Urban dispersal and activity of Aedes aegypti. Mosq News 18: Trpis M, Seasonal Variation in the Adult Populations of Aedes aegypti in the Dar es Salaam Area Tanzania. Geneva: World Health Organization. WHO/VBC Hervy JP, Experience de marquage-lacher-recapture portant sur Aedes aegypti Linne, en zone de savane soudanienne ouest Africaine. II. Relastions entre habitat, morphologie et comportement. Cah ORSTOM Entomol Med Parasitol 15: Sheppard PM, Macdonald WW, Tonn RJ, Grab B, The dynamics of an adult population of Aedes aegypti in relation to dengue haemorrhagic fever in Bangkok. J Anim Ecol 38: Trpis M, Hausermann W, Demonstration of differential domesticity of Aedes aegypti (L.) (Diptera, Culicidae) in Africa by mark-release-recapture. Bull Entomol Res 65: Trpis M, Hausermann W, Genetics of house-entering behaviour in east African populations of Aedes aegypti (L.) (Diptera: Culicidae) and its relevance to speciation. Bull Entomol Res 68: Trpis M, Hausermann W, Dispersal and other population parameters of Aedes aegypti in an African village and their possible significance in epidemiology of vector-borne diseases. AmJTropMedHyg35: Trpis M, Hausermann W, Craig GB, Estimates of population size, dispersal, and longevity of domestic Aedes aegypti (Diptera: Culicidae) by mark-release-recapture in the village of Shauri Moyo in eastern Kenya. J Med Entomol 32: Muir L, Kay BH, Aedes aegypti survival and dispersal estimated by mark-release-recapture in northern Australia. Am J Trop Med Hyg 58: Edman JD, Scott TW, Costero A, Morrison AC, Harrington LC, Clark GG, Aedes aegypti (Diptera: Culicidae) movement influenced by availability of oviposition sites. J Med Entomol 35: Harrington LC, Bounaccorsi JP, Edman JD, Costero A, Kittayapong P, Clark GG, Scott TW, Analysis of survival of young and old Ae. aegypti (Diptera: Culicidae) from Puerto Rico and Thailand. J Med Entomol 38: Bond HA, Craig GB, Fay RW, Field mating and movement of Aedes aegypti. Mosq News 30: Hausermann W, Fay RW, Hacker CS, Dispersal of genetically marked female Aedes aegypti in Mississippi. Mosq News 31: Reiter P, Amador MA, Anderson RA, Clark GG, Short report: Dispersal of Aedes aegypti in an urban area after blood feeding as demonstrated by rubidium-marked eggs. AmJTrop Med Hyg 52: Honorio NA, da Costa SW, Leite PJ, Goncalves JM, Lounibos LP, de Lourenco RO, Dispersal of Ae. aegypti and Ae. albopictus (Diptera: Culicidae) in an urban endemic dengue area in the State of Rio de Janeiro, Brazil. Mem Inst Oswaldo Cruz 98: Day JF, Edman JD, Scott TW, Reproductive fitness and survivorship of Aedes aegypti (Diptera: Culicidae) maintained on blood, with field observations from Thailand. J Med Entomol 31: Buonaccorsi J, Harrington LC, Edman JD, Estimation and comparison of mosquito survival rates with release-captureremoval data. J Med Entomol 40: Nimmannitya S, Halstead SB, Cohen SN, Dengue and Chikungunya virus infection in man in Thailand, I. Observations on hospitalized patients with haemorrhagic fever. Am J Trop Med Hyg 18: Ordonez-Gonzalez JG, Mercado-Hernandez HR, Flores-Suarez AE, Fernandez-Salas I, The use of sticky ovitraps to estimate dispersal of Aedes aegypti in northeastern Mexico. J Am Mosq Control Assoc 17: Gerade BB, Lee SH, Scott TW, Edman JD, Harrington LC, Kitthawee S, Jones JW, Clark JM, Field validation of Aedes aegypti (Diptera: Culicidae) age estimation by analysis of cuticular hydrocarbons. J Med Entomol 41: Macdonald WW, Sebastian A, Maung Tun M, A markrelease-recapture experiment with Culex pipiens fatigans in the village of Okpo, Burma. Ann Trop Med Parasitol 62: Sheppard PM, MacDonald WW, Tonn RJ, Grab B, The dynamics of an adult population of Aedes aegpyti in relation to dengue haemorrhagic fever in Bangkok. J Anim Ecol 38: Sinsko MJ, Craig GB, Dynamics of an isolated population of Aedes triseriatus (Diptera: Culicidae). J Med Entomol 15: Ritchie SA, Long S, Smith G, Pyke A, Knox TB, Entomological investigations in a focus of dengue transmission in Cairns, Queensland, Australia, by using the sticky ovitraps. J Med Entomol 41: Tsuda Y, Takagi M, Wang S, Wang Z, Tang L, Movement of Aedes aegypti (Diptera: Culicidae) released in a small isolated village on Hainan Island, China. J Med Entomol 38: Getis A, Morrison AC, Gray K, Scott TW, Characteristics of the spatial pattern of the dengue vector, Aedes aegypti, in Iquitos, Peru. Am J Trop Med Hyg 69: Morrison AC, Getis A, Santiago M, Rigau-Perez JG, Reiter P,
Further Evaluation of Indoor Resting Boxes for Aedes aegypti Surveillance
 Further Evaluation of Indoor Resting Boxes for Aedes aegypti Surveillance By Pattamaporn Kittayapong Department of Biology, Faculty of Science, Mahidol University, Bangkok, Thailand Kenneth J. Linthicum
Further Evaluation of Indoor Resting Boxes for Aedes aegypti Surveillance By Pattamaporn Kittayapong Department of Biology, Faculty of Science, Mahidol University, Bangkok, Thailand Kenneth J. Linthicum
Title Mosquito, Aedes aegypti (Diptera: C. Issue Date Right.
 NAOSITE: Nagasaki University's Ac Title Author(s) Effect of Body Size and Sugar Meals Mosquito, Aedes aegypti (Diptera: C Tsunoda, Takashi; Fukuchi, Atsuko; Citation Journal of Vector Ecology, 35(1), p
NAOSITE: Nagasaki University's Ac Title Author(s) Effect of Body Size and Sugar Meals Mosquito, Aedes aegypti (Diptera: C Tsunoda, Takashi; Fukuchi, Atsuko; Citation Journal of Vector Ecology, 35(1), p
The importance of schools and other non-household sites for dengue entomological risk
 The importance of schools and other non-household sites for dengue entomological risk Audrey Lenhart, MPH, PhD US Centers for Disease Control and Prevention (CDC) Liverpool School of Tropical Medicine
The importance of schools and other non-household sites for dengue entomological risk Audrey Lenhart, MPH, PhD US Centers for Disease Control and Prevention (CDC) Liverpool School of Tropical Medicine
Heterogeneous Feeding Patterns of the Dengue Vector, Aedes aegypti, on Individual Human Hosts in Rural Thailand
 Heterogeneous Feeding Patterns of the Dengue Vector, Aedes aegypti, on Individual Human Hosts in Rural Thailand Laura C. Harrington 1 *, Andrew Fleisher 2, Diego Ruiz-Moreno 1 a, Francoise Vermeylen 3,
Heterogeneous Feeding Patterns of the Dengue Vector, Aedes aegypti, on Individual Human Hosts in Rural Thailand Laura C. Harrington 1 *, Andrew Fleisher 2, Diego Ruiz-Moreno 1 a, Francoise Vermeylen 3,
INTRODUCTION. efforts and to assess the efficacy of community-based vector control. MATERIALS AND METHODS
 Am. J. Trop. Med. Hyg., 68(2), 2003, pp. 209 217 Copyright 2003 by The American Society of Tropical Medicine and Hygiene DENGUE AND ITS VECTORS IN THAILAND: CALCULATED TRANSMISSION RISK FROM TOTAL PUPAL
Am. J. Trop. Med. Hyg., 68(2), 2003, pp. 209 217 Copyright 2003 by The American Society of Tropical Medicine and Hygiene DENGUE AND ITS VECTORS IN THAILAND: CALCULATED TRANSMISSION RISK FROM TOTAL PUPAL
Aedes aegypti Larval Habitats and Dengue Vector Indices in a Village of Ubonratchathani Province in the North-East of Thailand
 254 KKU Res. J. 2015; 20(2) KKU Res.j. 2015; 20(2) : 254-259 http://resjournal.kku.ac.th Aedes aegypti Larval Habitats and Dengue Vector Indices in a Village of Ubonratchathani Province in the North-East
254 KKU Res. J. 2015; 20(2) KKU Res.j. 2015; 20(2) : 254-259 http://resjournal.kku.ac.th Aedes aegypti Larval Habitats and Dengue Vector Indices in a Village of Ubonratchathani Province in the North-East
Habitat and Density of Oviposition Opportunity Influences Aedes aegypti (Diptera: Culicidae) Flight Distance
 Vector-Borne Diseases, Surveillance, Prevention Journal of Medical Entomology, 54(5), 2017, 1385 1389 doi: 10.1093/jme/tjx083 Advance Access Publication Date: 15 April 2017 Research article Habitat and
Vector-Borne Diseases, Surveillance, Prevention Journal of Medical Entomology, 54(5), 2017, 1385 1389 doi: 10.1093/jme/tjx083 Advance Access Publication Date: 15 April 2017 Research article Habitat and
ELISA as an alternative tool for epidemiological surveillance for dengue in mosquitoes: a report from Thailand
 J Vector Borne Dis 44, December 2007, pp. 272 276 ELISA as an alternative tool for epidemiological surveillance for dengue in mosquitoes: a report from Thailand Mayuna Srisuphanunt a, Ratana Sithiprasasna
J Vector Borne Dis 44, December 2007, pp. 272 276 ELISA as an alternative tool for epidemiological surveillance for dengue in mosquitoes: a report from Thailand Mayuna Srisuphanunt a, Ratana Sithiprasasna
Landing periodicity of Aedes aegypti with implications for dengue transmission in Trinidad, West Indies
 158 Journal of Vector Ecology December, 2000 Landing periodicity of Aedes aegypti with implications for dengue transmission in Trinidad, West Indies Dave D. Chadee and Raymond Martinez Insect Vector Control
158 Journal of Vector Ecology December, 2000 Landing periodicity of Aedes aegypti with implications for dengue transmission in Trinidad, West Indies Dave D. Chadee and Raymond Martinez Insect Vector Control
Eliminate Dengue: Our Challenge
 March 2013 Eliminate Dengue: Our Challenge Wolbachia pipientis Discovered in 1924 in Culex pipiens ovaries W W m W W Only lives inside host cells Not infectious Only transmitted through the eggs TEM by
March 2013 Eliminate Dengue: Our Challenge Wolbachia pipientis Discovered in 1924 in Culex pipiens ovaries W W m W W Only lives inside host cells Not infectious Only transmitted through the eggs TEM by
Body size-associated survival and dispersal rates of Aedes aegypti in Rio de Janeiro
 Medical and Veterinary Entomology (2007) 21, 284 292 Body size-associated survival and dispersal rates of Aedes aegypti in Rio de Janeiro R. MACIEL-DE-FREITAS 1, C. T. CODEÇO 2 and R. LOURENÇO-DE-OLIVEIRA
Medical and Veterinary Entomology (2007) 21, 284 292 Body size-associated survival and dispersal rates of Aedes aegypti in Rio de Janeiro R. MACIEL-DE-FREITAS 1, C. T. CODEÇO 2 and R. LOURENÇO-DE-OLIVEIRA
LARVAL HABITATS AND DISTRIBUTION PATTERNS OF AEDES AEGYPTI (LINNAEUS) AND AEDES ALBOPICTUS (SKUSE), IN THAILAND
 LARVAL HABITATS AND DISTRIBUTION PATTERNS OF AEDES AEGYPTI (LINNAEUS) AND AEDES ALBOPICTUS (SKUSE), IN THAILAND Theeraphap Chareonviriyaphap, Pongthep Akratanakul,2, Sommawan Nettanomsak and Sataporn Huntamai
LARVAL HABITATS AND DISTRIBUTION PATTERNS OF AEDES AEGYPTI (LINNAEUS) AND AEDES ALBOPICTUS (SKUSE), IN THAILAND Theeraphap Chareonviriyaphap, Pongthep Akratanakul,2, Sommawan Nettanomsak and Sataporn Huntamai
Invasive Aedes Mosquito Response Plan
 23187 Connecticut Street Hayward, CA 94545 T: (510) 783-7744 F: (510) 783-3903 acmad@mosquitoes.org Board of Trustees President Richard Guarienti Dublin Vice-President Kathy Narum Pleasanton Secretary
23187 Connecticut Street Hayward, CA 94545 T: (510) 783-7744 F: (510) 783-3903 acmad@mosquitoes.org Board of Trustees President Richard Guarienti Dublin Vice-President Kathy Narum Pleasanton Secretary
Duane J. Gubler, ScD Professor and Founding Director, Signature Research Program in Emerging Infectious Diseases, Duke-NUS Medical School, Singapore
 Duane J. Gubler, ScD Professor and Founding Director, Signature Research Program in Emerging Infectious Diseases, Duke-NUS Medical School, Singapore AGENDA Other arboviruses with the potential for urban
Duane J. Gubler, ScD Professor and Founding Director, Signature Research Program in Emerging Infectious Diseases, Duke-NUS Medical School, Singapore AGENDA Other arboviruses with the potential for urban
Studies on Insecticides Susceptibility of Aedes Aegypti and Aedes Albopictus Vectors of Dengue and Zika in Central West Highland, Viet Nam
 International Journal of Animal Biology Vol. 4, No. 3, 2018, pp. 39-44 http://www.aiscience.org/journal/ijab ISSN: 2381-7658 (Print); ISSN: 2381-7666 (Online) Studies on s Susceptibility of Aedes Aegypti
International Journal of Animal Biology Vol. 4, No. 3, 2018, pp. 39-44 http://www.aiscience.org/journal/ijab ISSN: 2381-7658 (Print); ISSN: 2381-7666 (Online) Studies on s Susceptibility of Aedes Aegypti
Vector Hazard Report: CHIKV in the Americas and Caribbean
 Vector Hazard Report: CHIKV in the Americas and Caribbean Notes, photos and habitat suitability models gathered from The Armed Forces Pest Management Board, VectorMap and The Walter Reed Biosystematics
Vector Hazard Report: CHIKV in the Americas and Caribbean Notes, photos and habitat suitability models gathered from The Armed Forces Pest Management Board, VectorMap and The Walter Reed Biosystematics
UNDERSTANDING ZIKA AND MOSQUITO BORNE ILLNESSES
 UNDERSTANDING ZIKA AND MOSQUITO BORNE ILLNESSES Dr. Roxanne Connelly, Professor Medical Entomology State Specialist University of Florida, IFAS, Florida Medical Entomology Laboratory http://fmel.ifas.ufl.edu/
UNDERSTANDING ZIKA AND MOSQUITO BORNE ILLNESSES Dr. Roxanne Connelly, Professor Medical Entomology State Specialist University of Florida, IFAS, Florida Medical Entomology Laboratory http://fmel.ifas.ufl.edu/
Prevention of arboviral diseases. Willem Takken & Sander Koenraadt Laboratory of Entomology Wageningen University and Research
 Prevention of arboviral diseases Willem Takken & Sander Koenraadt Laboratory of Entomology Wageningen University and Research Brussel, 25 januari 2018 Arbivoral diseases affecting humans Mosquito borne:
Prevention of arboviral diseases Willem Takken & Sander Koenraadt Laboratory of Entomology Wageningen University and Research Brussel, 25 januari 2018 Arbivoral diseases affecting humans Mosquito borne:
The Allee effect in site choice behaviour of egg-laying dengue vector mosquitoes
 Tropical Biomedicine 25(2): 140 144 (2008) The Allee effect in site choice behaviour of egg-laying dengue vector mosquitoes Craig R. Williams, Katherine J. Leach, Natasha J. Wilson and Veronica R. Swart
Tropical Biomedicine 25(2): 140 144 (2008) The Allee effect in site choice behaviour of egg-laying dengue vector mosquitoes Craig R. Williams, Katherine J. Leach, Natasha J. Wilson and Veronica R. Swart
Correlation of Aedes aegypti infestation indices in the urban area of Merida, Mexico
 Correlation of Aedes aegypti infestation indices in the urban area of Merida, Mexico Pablo Manrique Saide P. Coleman & C. Davies UADY-FMVZ-Departamento de Zoología London School of Hygiene & Tropical Medicine
Correlation of Aedes aegypti infestation indices in the urban area of Merida, Mexico Pablo Manrique Saide P. Coleman & C. Davies UADY-FMVZ-Departamento de Zoología London School of Hygiene & Tropical Medicine
Ecology of La Crosse Encephalitis in endemic western North Carolina
 In Collaboration with: Ecology of La Crosse Encephalitis in endemic western North Carolina MARCELO SCHWARZ UNC GREEENSBORO - BIOLOGY DEPARTMENT MARCH 2014 La Crosse Encephalitis (LACE) No treatment. No
In Collaboration with: Ecology of La Crosse Encephalitis in endemic western North Carolina MARCELO SCHWARZ UNC GREEENSBORO - BIOLOGY DEPARTMENT MARCH 2014 La Crosse Encephalitis (LACE) No treatment. No
Supplementary Materials for
 advances.sciencemag.org/cgi/content/full/3/2/e1602024/dc1 Supplementary Materials for Combining contact tracing with targeted indoor residual spraying significantly reduces dengue transmission Gonzalo
advances.sciencemag.org/cgi/content/full/3/2/e1602024/dc1 Supplementary Materials for Combining contact tracing with targeted indoor residual spraying significantly reduces dengue transmission Gonzalo
EFFECTS OF SUGAR AND ANIMAL BLOOD AVAILABILITY ON ATTRACTION OF AEDES (STEGOMYIA) SPP. TO HUMANS
 Proceedings of the Sixth International Conference on Urban Pests William H Robinson and Dániel Bajomi (editors), 2008 Printed by OOK-Press Kft., H-8200 Veszprém, Pápai út 37/a, Hungary 197 EFFECTS OF SUGAR
Proceedings of the Sixth International Conference on Urban Pests William H Robinson and Dániel Bajomi (editors), 2008 Printed by OOK-Press Kft., H-8200 Veszprém, Pápai út 37/a, Hungary 197 EFFECTS OF SUGAR
RESISTANCE OF AEDES AEGYPTI (L.) LARVAE TO TEMEPHOS IN SURABAYA, INDONESIA
 RESISTANCE OF AEDES AEGYPTI (L.) LARVAE TO TEMEPHOS IN SURABAYA, INDONESIA Kris Cahyo Mulyatno 1,2, Atsushi Yamanaka 1,3, Ngadino 4 and Eiji Konishi 3,5,6* 1 Indonesia-Japan Collaborative Research Center
RESISTANCE OF AEDES AEGYPTI (L.) LARVAE TO TEMEPHOS IN SURABAYA, INDONESIA Kris Cahyo Mulyatno 1,2, Atsushi Yamanaka 1,3, Ngadino 4 and Eiji Konishi 3,5,6* 1 Indonesia-Japan Collaborative Research Center
RESEARCH NOTE IDENTIFICATION OF DENGUE VIRUS IN AEDES MOSQUITOES AND PATIENTS SERA FROM SI SA KET PROVINCE, THAILAND
 RESEARCH NOTE IDENTIFICATION OF DENGUE VIRUS IN AEDES MOSQUITOES AND PATIENTS SERA FROM SI SA KET PROVINCE, THAILAND Chai Teerasut 1, Udom Petphuwadee 1, Suwich Thammapalo 2, Wipawee Jampangern 3 and Kriengsak
RESEARCH NOTE IDENTIFICATION OF DENGUE VIRUS IN AEDES MOSQUITOES AND PATIENTS SERA FROM SI SA KET PROVINCE, THAILAND Chai Teerasut 1, Udom Petphuwadee 1, Suwich Thammapalo 2, Wipawee Jampangern 3 and Kriengsak
Mosquito Surveillance/Control in Texas
 Mosquito Surveillance/Control in Texas Infectious Disease Taskforce Austin, Texas, May 6, 2016 Tom J. Sidwa, DVM, MPH State Public Health Veterinarian Zoonosis Control Branch Manager Objectives Mosquito
Mosquito Surveillance/Control in Texas Infectious Disease Taskforce Austin, Texas, May 6, 2016 Tom J. Sidwa, DVM, MPH State Public Health Veterinarian Zoonosis Control Branch Manager Objectives Mosquito
Updating in container selection and temperature relation of Aedes Mosquito Species in Bangkok Thailand.
 Available online at www.buuconference.buu.ac.th 5 th Burapha University International Conference 2016 Harmonization of Knowledge towards the Betterment of Society Updating in container selection and temperature
Available online at www.buuconference.buu.ac.th 5 th Burapha University International Conference 2016 Harmonization of Knowledge towards the Betterment of Society Updating in container selection and temperature
Recent Trends in Arboviruses Found in the United States
 Recent Trends in Arboviruses Found in the United States Janet C. McAllister, Ph.D. Arboviral Diseases Branch Division of Vector-Borne Infectious Diseases Centers for Disease Control and Prevention The
Recent Trends in Arboviruses Found in the United States Janet C. McAllister, Ph.D. Arboviral Diseases Branch Division of Vector-Borne Infectious Diseases Centers for Disease Control and Prevention The
COMPARISON OF BI-DIRECTIONAL FAY, OMNI-DIRECTIONAL, CDC, AND DUPLEX CONE TRAPS FOR SAMPLING ADULT AEDES ALBOPICTU,S AND AEDES AEGYPTI IN NORTH FLORIDA
 Journal of the American Mosquito Control Association, l0(l):74-78, 1994 COMPARISON OF BI-DIRECTIONAL FAY, OMNI-DIRECTIONAL,, AND DUPLEX CONE TRAPS FOR SAMPLING ADULT AEDES ALBOPICTU,S AND AEDES AEGYPTI
Journal of the American Mosquito Control Association, l0(l):74-78, 1994 COMPARISON OF BI-DIRECTIONAL FAY, OMNI-DIRECTIONAL,, AND DUPLEX CONE TRAPS FOR SAMPLING ADULT AEDES ALBOPICTU,S AND AEDES AEGYPTI
The correlation between temperature and humidity with the population density of Aedes aegypti as dengue fever s vector
 IOP Conference Series: Earth and Environmental Science PAPER OPEN ACCESS The correlation between temperature and humidity with the population density of Aedes aegypti as dengue fever s vector To cite this
IOP Conference Series: Earth and Environmental Science PAPER OPEN ACCESS The correlation between temperature and humidity with the population density of Aedes aegypti as dengue fever s vector To cite this
Malaria Risk Areas in Thailand Border
 Malaria Risk Areas in Thailand Border Natthawut Kaewpitoon PhD*, **, Ryan A Loyd MD***, Soraya J Kaewpitoon MD**, ***, Ratana Rujirakul MEd** * Faculty of Public Health, Vongchavalitkul University, Nakhon
Malaria Risk Areas in Thailand Border Natthawut Kaewpitoon PhD*, **, Ryan A Loyd MD***, Soraya J Kaewpitoon MD**, ***, Ratana Rujirakul MEd** * Faculty of Public Health, Vongchavalitkul University, Nakhon
Dispersal of Aedes aegypti and Aedes albopictus (Diptera: Culicidae) in an Urban Endemic Dengue Area in the State of Rio de Janeiro, Brazil
 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 98(2): 191-198, March 2003 191 Dispersal of Aedes aegypti and Aedes albopictus (Diptera: Culicidae) in an Urban Endemic Dengue Area in the State of Rio de Janeiro,
Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 98(2): 191-198, March 2003 191 Dispersal of Aedes aegypti and Aedes albopictus (Diptera: Culicidae) in an Urban Endemic Dengue Area in the State of Rio de Janeiro,
Mosquito Threats in LA County West Nile virus & Zika
 Mosquito Threats in LA County West Nile virus & Zika The District at a Glance An independent special district formed under authority of the CA State Health and Safety Code Formed in 1952 and governed by
Mosquito Threats in LA County West Nile virus & Zika The District at a Glance An independent special district formed under authority of the CA State Health and Safety Code Formed in 1952 and governed by
ZIKA Virus and Mosquito Management. ACCG Rosmarie Kelly, PhD MPH 30 April 16
 ZIKA Virus and Mosquito Management ACCG Rosmarie Kelly, PhD MPH 30 April 16 What is Zika Virus? Zika virus (ZIKV) is a flavivirus related to yellow fever, dengue, West Nile, and Japanese encephalitis viruses.
ZIKA Virus and Mosquito Management ACCG Rosmarie Kelly, PhD MPH 30 April 16 What is Zika Virus? Zika virus (ZIKV) is a flavivirus related to yellow fever, dengue, West Nile, and Japanese encephalitis viruses.
Bannie Hulsey MIT Holding, Inc.
 Bannie Hulsey MIT Holding, Inc. Thomas M. Kollars, Jr. PhD, ACE CSO ProVector, LLC; CSA MIT Holding, Inc. Epidemiology Consultant, Afro-European Medical and Research Network Contact Information Address:
Bannie Hulsey MIT Holding, Inc. Thomas M. Kollars, Jr. PhD, ACE CSO ProVector, LLC; CSA MIT Holding, Inc. Epidemiology Consultant, Afro-European Medical and Research Network Contact Information Address:
Epidemiology of Vector-Borne Diseases Laura C. Harrington, PhD
 Epidemiology of Vector- Borne Diseases Associate Professor Department of Entomology Cornell University 1 Before we begin Review lectures on transmission, arboviruses and malaria Focus on biologically transmitted
Epidemiology of Vector- Borne Diseases Associate Professor Department of Entomology Cornell University 1 Before we begin Review lectures on transmission, arboviruses and malaria Focus on biologically transmitted
Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012
 Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012 Dengue Lecture Outline Dengue Virus Dengue Epidemiology Military Significance Clinical
Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012 Dengue Lecture Outline Dengue Virus Dengue Epidemiology Military Significance Clinical
Oxitec Mosquito Vector Control Technology. A New Paradigm to combat Dengue, chikungunya and the emerging threat of Zika
 Oxitec Mosquito Vector Control Technology A New Paradigm to combat Dengue, chikungunya and the emerging threat of Zika 2 Mosquitoes The World s Deadliest Animal The Impact of Zika on the Health System
Oxitec Mosquito Vector Control Technology A New Paradigm to combat Dengue, chikungunya and the emerging threat of Zika 2 Mosquitoes The World s Deadliest Animal The Impact of Zika on the Health System
UNDERSTANDING THE ENVIRONMENTAL DRIVERS INFLUENCING THE EPIDEMIOLOGICAL RISK OF VECTOR BORNE DISEASES
 UNDERSTANDING THE ENVIRONMENTAL DRIVERS INFLUENCING THE EPIDEMIOLOGICAL RISK OF VECTOR BORNE DISEASES Paola Angelini, Alba Carola Finarelli, Andrea Mattivi, Roberto Cagarelli Public Health Department D.G.
UNDERSTANDING THE ENVIRONMENTAL DRIVERS INFLUENCING THE EPIDEMIOLOGICAL RISK OF VECTOR BORNE DISEASES Paola Angelini, Alba Carola Finarelli, Andrea Mattivi, Roberto Cagarelli Public Health Department D.G.
Aedes (Diptera: Culicidae) vectors of arboviruses in Mayotte: distribution area and breeding sites by Leïla BAGNY PhD student
 Aedes (Diptera: Culicidae) vectors of arboviruses in Mayotte: distribution area and breeding sites by Leïla BAGNY PhD student Directed by S. QUILICI (CIRAD) and D. FONTENILLE (IRD) Introduction Mayotte
Aedes (Diptera: Culicidae) vectors of arboviruses in Mayotte: distribution area and breeding sites by Leïla BAGNY PhD student Directed by S. QUILICI (CIRAD) and D. FONTENILLE (IRD) Introduction Mayotte
A SURVEY OF KNOWLEDGE, ATTITUDE AND PRACTICE OF THE PREVENTION OF DENGUE HEMORRHAGIC FEVER IN AN URBAN COMMUNITY OF THAILAND
 A SURVEY OF KNOWLEDGE, ATTITUDE AND PRACTICE OF THE PREVENTION OF DENGUE HEMORRHAGIC FEVER IN AN URBAN COMMUNITY OF THAILAND Witaya Swaddiwudhipong, Ploenjai Lerdlukanavonge, Presert Khumklam, Supawan
A SURVEY OF KNOWLEDGE, ATTITUDE AND PRACTICE OF THE PREVENTION OF DENGUE HEMORRHAGIC FEVER IN AN URBAN COMMUNITY OF THAILAND Witaya Swaddiwudhipong, Ploenjai Lerdlukanavonge, Presert Khumklam, Supawan
Biology, distribution, and insecticide susceptibility status of Florida vectors of Zika virus.
 Biology, distribution, and insecticide susceptibility status of Florida vectors of Zika virus. Roxanne Connelly, PhD Professor University of Florida, IFAS Florida Medical Entomology Laboratory Vero Beach,
Biology, distribution, and insecticide susceptibility status of Florida vectors of Zika virus. Roxanne Connelly, PhD Professor University of Florida, IFAS Florida Medical Entomology Laboratory Vero Beach,
MODULE 3: Transmission
 MODULE 3: Transmission Dengue Clinical Management Acknowledgements This curriculum was developed with technical assistance from the University of Malaya Medical Centre. Materials were contributed by the
MODULE 3: Transmission Dengue Clinical Management Acknowledgements This curriculum was developed with technical assistance from the University of Malaya Medical Centre. Materials were contributed by the
Fact sheet. Yellow fever
 Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
Fact sheet Key facts is an acute viral haemorrhagic disease transmitted by infected mosquitoes. The yellow in the name refers to the jaundice that affects some patients. Up to 50% of severely affected
 Walailak Procedia 2018; 2018(2): st43 Container types and water qualities affecting on number of Aedes larvae in Trang province, Thailand Anantanit Chumsri 1,*, Patchara Pongmanawut 2, Fahmida Wazed Tina
Walailak Procedia 2018; 2018(2): st43 Container types and water qualities affecting on number of Aedes larvae in Trang province, Thailand Anantanit Chumsri 1,*, Patchara Pongmanawut 2, Fahmida Wazed Tina
SHORT COMMUNICATION. Rafael Maciel-de-Freitas, Jaylei Monteiro Gonçalves*, Ricardo Lourenço-de-Oliveira/ +
 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 99(8): 823-827, December 2004 823 SHORT COMMUNICATION Efficiency of Rubidium Marking in Aedes albopictus (Diptera: Culicidae): Preliminary Evaluation on Persistence
Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 99(8): 823-827, December 2004 823 SHORT COMMUNICATION Efficiency of Rubidium Marking in Aedes albopictus (Diptera: Culicidae): Preliminary Evaluation on Persistence
Arbovirus Surveillance in Massachusetts 2016 Massachusetts Department of Public Health (MDPH) Arbovirus Surveillance Program
 INTRODUCTION Arbovirus Surveillance in Massachusetts 2016 Massachusetts Department of Public Health (MDPH) Arbovirus Surveillance Program There are two mosquito-borne diseases of concern for transmission
INTRODUCTION Arbovirus Surveillance in Massachusetts 2016 Massachusetts Department of Public Health (MDPH) Arbovirus Surveillance Program There are two mosquito-borne diseases of concern for transmission
Comparative Studies on the Biology and Filarial Susceptibility of Selected Blood-feeding and Autogenous Aedes togoi Sub-colonies
 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 98(4): 481-485, June 2003 481 Comparative Studies on the Biology and Filarial Susceptibility of Selected Blood-feeding and Autogenous Aedes togoi Sub-colonies
Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 98(4): 481-485, June 2003 481 Comparative Studies on the Biology and Filarial Susceptibility of Selected Blood-feeding and Autogenous Aedes togoi Sub-colonies
Geographical structure of dengue transmission and its determinants in Thailand
 Epidemiol. Infect., Page 1 of 9. f 2007 Cambridge University Press doi:10.1017/s0950268807008990 Printed in the United Kingdom Geographical structure of dengue transmission and its determinants in Thailand
Epidemiol. Infect., Page 1 of 9. f 2007 Cambridge University Press doi:10.1017/s0950268807008990 Printed in the United Kingdom Geographical structure of dengue transmission and its determinants in Thailand
Field evaluation of lethal ovitraps impregnated with deltamethrin against dengue vectors in Lahore, Pakistan
 BIOLOGIA (PAKISTAN) 2011, 57 (1&2), 7-13 PK ISSN 0006-3096 Field evaluation of lethal ovitraps impregnated with deltamethrin against dengue vectors in Lahore, Pakistan * NUSRAT JAHAN 1, MUHAMMAD SAJJAD
BIOLOGIA (PAKISTAN) 2011, 57 (1&2), 7-13 PK ISSN 0006-3096 Field evaluation of lethal ovitraps impregnated with deltamethrin against dengue vectors in Lahore, Pakistan * NUSRAT JAHAN 1, MUHAMMAD SAJJAD
Aedes Aegypti - A Medical Dictionary, Bibliography, And Annotated Research Guide To Internet References By Icon Health Publications
 Aedes Aegypti - A Medical Dictionary, Bibliography, And Annotated Research Guide To Internet References By Icon Health Publications If searching for a book by Icon Health Publications Aedes Aegypti - A
Aedes Aegypti - A Medical Dictionary, Bibliography, And Annotated Research Guide To Internet References By Icon Health Publications If searching for a book by Icon Health Publications Aedes Aegypti - A
Dengue Virus-Danger from Deadly Little Dragon
 Molecular Medicine Dengue Virus-Danger from Deadly Little Dragon Dr.G.MATHAN Assistant Professor Department of Biomedical Science Bharathidasan University Tiruchirappalli, Tamil Nadu Vector (A carrier)
Molecular Medicine Dengue Virus-Danger from Deadly Little Dragon Dr.G.MATHAN Assistant Professor Department of Biomedical Science Bharathidasan University Tiruchirappalli, Tamil Nadu Vector (A carrier)
Global Climate Change and Mosquito-Borne Diseases
 Global Climate Change and Mosquito-Borne Diseases Theodore G. Andreadis Center for Vector Biology & Zoonotic Diseases The Connecticut Agricultural Experiment Station New Haven, CT Evidence for Global Climate
Global Climate Change and Mosquito-Borne Diseases Theodore G. Andreadis Center for Vector Biology & Zoonotic Diseases The Connecticut Agricultural Experiment Station New Haven, CT Evidence for Global Climate
p<piens Complex Mosquitoes from Memphis, Tennessee
 386 Mosquito Systematics Vol. lz(4) 1980 Additional Studies of Male Progeny of Overwintering CuZex p
386 Mosquito Systematics Vol. lz(4) 1980 Additional Studies of Male Progeny of Overwintering CuZex p
The Complex Relationship between Weather and Dengue Virus Transmission in Thailand
 Am. J. Trop. Med. Hyg., 89(6), 2013, pp. 1066 1080 doi:10.4269/ajtmh.13-0321 Copyright 2013 by The American Society of Tropical Medicine and Hygiene The Complex Relationship between Weather and Dengue
Am. J. Trop. Med. Hyg., 89(6), 2013, pp. 1066 1080 doi:10.4269/ajtmh.13-0321 Copyright 2013 by The American Society of Tropical Medicine and Hygiene The Complex Relationship between Weather and Dengue
Climate change and vector-borne diseases of livestock in the tropics. Peter Van den Bossche
 Climate change and vector-borne diseases of livestock in the tropics Peter Van den Bossche Climate change & animal health Climate change in Africa: Temperature Rainfall Variability Climate change & animal
Climate change and vector-borne diseases of livestock in the tropics Peter Van den Bossche Climate change & animal health Climate change in Africa: Temperature Rainfall Variability Climate change & animal
Outbreaks of Zika Virus: What Do We Know? Presented by Dr Jonathan Darbro Mosquito Control Lab, QIMR Berhgofer 15 September 2016
 Outbreaks of Zika Virus: What Do We Know? Presented by Dr Jonathan Darbro Mosquito Control Lab, QIMR Berhgofer 15 September 2016 Overview History Distribution Modes of Transmission Symptoms Some Causal
Outbreaks of Zika Virus: What Do We Know? Presented by Dr Jonathan Darbro Mosquito Control Lab, QIMR Berhgofer 15 September 2016 Overview History Distribution Modes of Transmission Symptoms Some Causal
SUPPLEMENTARY INFORMATION
 !""#$%&'()*(+$,-./$!"#$%&"#'($)'(*'+$,-$.'#/.0$!12$,134-0$ 5+(6)+7#8#')$9:$;+
!""#$%&'()*(+$,-./$!"#$%&"#'($)'(*'+$,-$.'#/.0$!12$,134-0$ 5+(6)+7#8#')$9:$;+
Maria Eugenia Toledo Institute of Tropical Medicine Pedro Kouri, Cuba
 Maria Eugenia Toledo Institute of Tropical Medicine Pedro Kouri, Cuba The most important arthropod borne viral disease No vaccine DENGUE No curative treatment Vector-control strategies failed to counter
Maria Eugenia Toledo Institute of Tropical Medicine Pedro Kouri, Cuba The most important arthropod borne viral disease No vaccine DENGUE No curative treatment Vector-control strategies failed to counter
Dengue Control in North Queensland, Australia: Case Recognition and Selective Indoor Residual Spraying
 Dengue Control in North Queensland, Australia: Case Recognition and Selective Indoor Residual Spraying by Scott A Ritchie* #, Jeffrey N Hanna*, Susan L Hills**, John P Piispanen**, W John H McBride***,
Dengue Control in North Queensland, Australia: Case Recognition and Selective Indoor Residual Spraying by Scott A Ritchie* #, Jeffrey N Hanna*, Susan L Hills**, John P Piispanen**, W John H McBride***,
Annual report MRCU - June 2017 Friendly Aedes aegypti project in West Bay
 Annual report MRCU - June 2017 Friendly Aedes aegypti project in West Bay Introduction A collaborative project has been established between the Mosquito Research and Control Unit (MRCU) and Oxitec to deliver
Annual report MRCU - June 2017 Friendly Aedes aegypti project in West Bay Introduction A collaborative project has been established between the Mosquito Research and Control Unit (MRCU) and Oxitec to deliver
2000s. 1900s. 1800s. Dengue Dog heartworm EEE La Crosse Malaria SLE WEE. Dengue Malaria Yellow Fever
 Dengue Malaria Yellow Fever Dengue Dog heartworm EEE La Crosse Malaria SLE WEE 1900s Chikungunya Dengue Dog heartworm EEE La Crosse Malaria SLE West Nile WEE Zika 2000s 1800s Amanda Young https://www.mosquitoillnessalliance.org/personal-stories
Dengue Malaria Yellow Fever Dengue Dog heartworm EEE La Crosse Malaria SLE WEE 1900s Chikungunya Dengue Dog heartworm EEE La Crosse Malaria SLE West Nile WEE Zika 2000s 1800s Amanda Young https://www.mosquitoillnessalliance.org/personal-stories
, Japan. Culicidae) Thahsin Farjana and Nobuko Tuno
 Section: Ecology Corresponding author address: Dr. Nobuko Tuno Graduate School of Natural Science and Technology, Kanazawa University, Kanazawa 920-1192, Japan. Email: tuno@staff.kanazawa-u.ac.jp Fax:+81-76-264-6214
Section: Ecology Corresponding author address: Dr. Nobuko Tuno Graduate School of Natural Science and Technology, Kanazawa University, Kanazawa 920-1192, Japan. Email: tuno@staff.kanazawa-u.ac.jp Fax:+81-76-264-6214
Mosquito Feeding Periodicy in an Isolated, Domesticated Environment. Chris Tarrand
 Mosquito Feeding Periodicy in an Isolated, Domesticated Environment Chris Tarrand Study Abroad Program, Dominica 2014 Dr. Jim Woolley, Dr. Thomas Lacher Department of Entomology Texas A&M University, College
Mosquito Feeding Periodicy in an Isolated, Domesticated Environment Chris Tarrand Study Abroad Program, Dominica 2014 Dr. Jim Woolley, Dr. Thomas Lacher Department of Entomology Texas A&M University, College
Mating affects egg maturation in Anopheles gambiae Giles (Diptera: Culicidae)
 June, 24 Journal of Vector Ecology 135 Mating affects egg maturation in Anopheles gambiae Giles (Diptera: Culicidae) Marc J. Klowden and Richard C. Russell Division of Entomology, University of Idaho,
June, 24 Journal of Vector Ecology 135 Mating affects egg maturation in Anopheles gambiae Giles (Diptera: Culicidae) Marc J. Klowden and Richard C. Russell Division of Entomology, University of Idaho,
UNITED STATES ENVIRONMENTAL PROTECTION AGENCY WASHINGTON, D.C August 30, 2016
 UNITED STATES ENVIRONMENTAL PROTECTION AGENCY WASHINGTON, D.C. 20460 OFFICE OF CHEMICAL SAFETY AND POLLUTION PREVENTION August 30, 2016 Stephen L. Dobson, Ph.D. University of Kentucky, Department of Entomology
UNITED STATES ENVIRONMENTAL PROTECTION AGENCY WASHINGTON, D.C. 20460 OFFICE OF CHEMICAL SAFETY AND POLLUTION PREVENTION August 30, 2016 Stephen L. Dobson, Ph.D. University of Kentucky, Department of Entomology
SOEDARTO SOEKIMAN*, EIJI KONISHI AND TAKEO MATSUMURA Received October /Accepted January
 Japan. J. Trop. Med. Hyg., Vol. 15, No. 1, 1987, pp. 37-41 Short Communication A COMPARATIVE STUDY ON GROWTH OF DENGUE TYPE 3 AND CHIKUNGUNYA VIRUSES IN INDONESIAN COLONIES OF AEDES AEGYPTI AND AEDES ALBOPICTUS
Japan. J. Trop. Med. Hyg., Vol. 15, No. 1, 1987, pp. 37-41 Short Communication A COMPARATIVE STUDY ON GROWTH OF DENGUE TYPE 3 AND CHIKUNGUNYA VIRUSES IN INDONESIAN COLONIES OF AEDES AEGYPTI AND AEDES ALBOPICTUS
Mosquito Control Update. Board of County Commissioners Work Session February 16, 2016
 Mosquito Control Update Board of County Commissioners Work Session February 16, 2016 1 Presentation Overview Mosquito Control Division Mosquito-borne Diseases Control Techniques Outlook 2 Mosquito Control
Mosquito Control Update Board of County Commissioners Work Session February 16, 2016 1 Presentation Overview Mosquito Control Division Mosquito-borne Diseases Control Techniques Outlook 2 Mosquito Control
Effects of Blackberry Leaf Infusion on Survival Rate and Outcomes of Intraspecific Competition of Culex restuans and Aedes aegypti
 Inquiry in ACES: An Undergraduate Research Journal Special Edition: Research Apprentice Program 2014 College of Agricultural, Consumer and Environmental Sciences University of Illinois at Urbana-Champaign
Inquiry in ACES: An Undergraduate Research Journal Special Edition: Research Apprentice Program 2014 College of Agricultural, Consumer and Environmental Sciences University of Illinois at Urbana-Champaign
Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year
 Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year 2005-2010 TIEN ZUBAIDAH * ABSTRACT Environment is one of instrumental factor in the
Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year 2005-2010 TIEN ZUBAIDAH * ABSTRACT Environment is one of instrumental factor in the
Interim report MRCU - February 2017 Friendly Aedes aegypti project in West Bay
 Interim report MRCU - February 2017 Friendly Aedes aegypti project in West Bay Introduction A nine month collaborative project has been established between the Mosquito Research and Control Unit (MRCU)
Interim report MRCU - February 2017 Friendly Aedes aegypti project in West Bay Introduction A nine month collaborative project has been established between the Mosquito Research and Control Unit (MRCU)
ZIKA VIRUS. Causes, Symptoms, Treatment and Prevention
 ZIKA VIRUS Causes, Symptoms, Treatment and Prevention Introduction Zika virus is spread to people through mosquito bites. The most common symptoms of Zika virus disease are fever, rash, joint pain, and
ZIKA VIRUS Causes, Symptoms, Treatment and Prevention Introduction Zika virus is spread to people through mosquito bites. The most common symptoms of Zika virus disease are fever, rash, joint pain, and
Waiting in the Wings: Emergence, Impact and Control of Mosquito-Borne Viruses
 International Center for Enterprise Preparedness (InterCEP) Waiting in the Wings: Emergence, Impact and Control of Mosquito-Borne Viruses Web Forum On April 14, 2016, Kathryn A. Hanley, Professor in the
International Center for Enterprise Preparedness (InterCEP) Waiting in the Wings: Emergence, Impact and Control of Mosquito-Borne Viruses Web Forum On April 14, 2016, Kathryn A. Hanley, Professor in the
An alternative strategy to eliminate dengue fever
 Project update: October 2010 An alternative strategy to eliminate dengue fever In July 2011, FHI became FHI 360. FHI 360 is a nonprofit human development organization dedicated to improving lives in lasting
Project update: October 2010 An alternative strategy to eliminate dengue fever In July 2011, FHI became FHI 360. FHI 360 is a nonprofit human development organization dedicated to improving lives in lasting
Updated Reported Distribution of Aedes (Stegomyia) aegypti and Aedes (Stegomyia) albopictus (Diptera: Culicidae) in the United States,
 Short Communication Journal of Medical Entomology, 54(5), 2017, 1420 1424 doi: 10.1093/jme/tjx088 Advance Access Publication Date: 19 June 2017 Short Communication Updated Reported Distribution of Aedes
Short Communication Journal of Medical Entomology, 54(5), 2017, 1420 1424 doi: 10.1093/jme/tjx088 Advance Access Publication Date: 19 June 2017 Short Communication Updated Reported Distribution of Aedes
Factsheet about Chikungunya
 Factsheet about Chikungunya Chikungunya fever is a viral disease transmitted to humans by infected mosquitoes that is characterized by fever, headache, rash, and severe joint and muscle pain. The name
Factsheet about Chikungunya Chikungunya fever is a viral disease transmitted to humans by infected mosquitoes that is characterized by fever, headache, rash, and severe joint and muscle pain. The name
Véronique Chevalier. UR AGIRs «Animal et Gestion Intégrée des Risques» CIRAD ES
 The use and application of epidemiological clusters in surveillance and control of Rift Valley fever Véronique Chevalier UR AGIRs «Animal et Gestion Intégrée des Risques» CIRAD ES Epidemiological system
The use and application of epidemiological clusters in surveillance and control of Rift Valley fever Véronique Chevalier UR AGIRs «Animal et Gestion Intégrée des Risques» CIRAD ES Epidemiological system
Why did Gorgas succeed?
 Why did Gorgas succeed? (And why have we failed?) Paul Reiter Institut Pasteur My heroes! The European CUC The European cuckoo Cuckoo expert Fellow of the Royal Society (FRS) The Broad Street Pump The
Why did Gorgas succeed? (And why have we failed?) Paul Reiter Institut Pasteur My heroes! The European CUC The European cuckoo Cuckoo expert Fellow of the Royal Society (FRS) The Broad Street Pump The
Highlights of Medical Entomology
 Highlights of Medical Entomology 16 November 2015 3:15 pm Donald A. Yee University of Southern Mississippi Hattiesburg, MS Copy of this talk? email: donald.yee@usm.edu Twitter: @_dayee_ Criteria for selection
Highlights of Medical Entomology 16 November 2015 3:15 pm Donald A. Yee University of Southern Mississippi Hattiesburg, MS Copy of this talk? email: donald.yee@usm.edu Twitter: @_dayee_ Criteria for selection
DEVELOPMENT AND EVALUATION OF A PYRIPROXYFEN- TREATED DEVICE TO CONTROL THE DENGUE VECTOR, AEDES AEGYPTI (L.) (DIPTERA:CULICIDAE)
 A Pyriproxyfen Treated Device for Ae. aegypti Control DEVELOPMENT AND EVALUATION OF A PYRIPROXYFEN- TREATED DEVICE TO CONTROL THE DENGUE VECTOR, AEDES AEGYPTI (L.) (DIPTERA:CULICIDAE) Alongkot Ponlawat
A Pyriproxyfen Treated Device for Ae. aegypti Control DEVELOPMENT AND EVALUATION OF A PYRIPROXYFEN- TREATED DEVICE TO CONTROL THE DENGUE VECTOR, AEDES AEGYPTI (L.) (DIPTERA:CULICIDAE) Alongkot Ponlawat
Larval growth and foraging behavior of Aedes albopictus and Aedes japonicus. Deborah O Donnell Ph.D. Candidate Georgetown University VMCA 2/7/07
 Larval growth and foraging behavior of Aedes albopictus and Aedes japonicus Deborah O Donnell Ph.D. Candidate Georgetown University VMCA 2/7/07 Invasive Disease Vectors Introduction of new vector often
Larval growth and foraging behavior of Aedes albopictus and Aedes japonicus Deborah O Donnell Ph.D. Candidate Georgetown University VMCA 2/7/07 Invasive Disease Vectors Introduction of new vector often
Challenges for dengue control in Brazil: overview of socioeconomic and environmental factors associated with virus circulation
 1 Challenges for dengue control in Brazil: overview of socioeconomic and environmental factors associated with virus circulation Paulo de Tarso R. Vilarinhos # Abstract Successive epidemics of dengue have
1 Challenges for dengue control in Brazil: overview of socioeconomic and environmental factors associated with virus circulation Paulo de Tarso R. Vilarinhos # Abstract Successive epidemics of dengue have
Universiti Kebangsaan Malaysia, Faculty of Allied Health Sciences, Jalan Raja Muda Abdul Aziz 50300, Kuala Lumpur, Malaysia 2
 Tropical Biomedicine 28(1): 48 54 (2011) Ovitrap surveillance of the dengue vectors, Aedes (Stegomyia) aegypti (L.) and Aedes (Stegomyia) albopictus Skuse in selected areas in Bentong, Pahang, Malaysia
Tropical Biomedicine 28(1): 48 54 (2011) Ovitrap surveillance of the dengue vectors, Aedes (Stegomyia) aegypti (L.) and Aedes (Stegomyia) albopictus Skuse in selected areas in Bentong, Pahang, Malaysia
West Nile Virus Los Angeles County
 West Nile Virus Los Angeles County Rachel Civen, M.D., M.P.H., F.A.A.P. Medical Epidemiologist County of Los Angeles Department of Public Health D16:\WNV_Tarzana_July 2012.ppt No. 2 WNV ECOLOGY Virus maintained
West Nile Virus Los Angeles County Rachel Civen, M.D., M.P.H., F.A.A.P. Medical Epidemiologist County of Los Angeles Department of Public Health D16:\WNV_Tarzana_July 2012.ppt No. 2 WNV ECOLOGY Virus maintained
Studies on the Life Cycle Parameters of Stegomyia aegypti
 Academic Journal of Entomology 10 (2): 25-31, 2017 ISSN 1995-8994 IDOSI Publications, 2017 DOI: 10.5829/idosi.aje.2017.25.31 Studies on the Life Cycle Parameters of Stegomyia aegypti 1 2 Mohd. Ayoub Bhat
Academic Journal of Entomology 10 (2): 25-31, 2017 ISSN 1995-8994 IDOSI Publications, 2017 DOI: 10.5829/idosi.aje.2017.25.31 Studies on the Life Cycle Parameters of Stegomyia aegypti 1 2 Mohd. Ayoub Bhat
Is Climate Change Affecting Vector-borne Disease Transmission?
 Is Climate Change Affecting Vector-borne Disease Transmission? Donald E. Champagne Department of Entomology and Center for Tropical and Emerging Global Diseases University of Georgia Why focus on vector-borne
Is Climate Change Affecting Vector-borne Disease Transmission? Donald E. Champagne Department of Entomology and Center for Tropical and Emerging Global Diseases University of Georgia Why focus on vector-borne
Dengue Haemorrhagic Fever in Thailand
 By Wiwat Rojanapithayakorn Office of Dengue Control, Department of Communicable Diseases Control, Ministry of Public Health, Thailand Abstract Dengue haemorrhagic fever was first reported in Thailand in
By Wiwat Rojanapithayakorn Office of Dengue Control, Department of Communicable Diseases Control, Ministry of Public Health, Thailand Abstract Dengue haemorrhagic fever was first reported in Thailand in
A comparative study on sampling techniques for Aedes aegypti(diptera: Culicidae) surveillance in Madurai,
 ~ Tropical Biomedicine 16: 25-29 (1999) A comparative study on sampling techniques for Aedes aegypti(diptera: Culicidae) surveillance in Madurai, South India (f) N. Arunachalam, P Philip Samuel, J. Hiriyan
~ Tropical Biomedicine 16: 25-29 (1999) A comparative study on sampling techniques for Aedes aegypti(diptera: Culicidae) surveillance in Madurai, South India (f) N. Arunachalam, P Philip Samuel, J. Hiriyan
Epidemiological Characteristics of Clinically- Confirmed Cases of Chikungunya in Teculutan, Guatemala
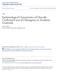 University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2016 Epidemiological Characteristics of Clinically- Confirmed Cases of Chikungunya
University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2016 Epidemiological Characteristics of Clinically- Confirmed Cases of Chikungunya
Inform'ACTION n 27 SEPTEMBER 2007
 Eradication: the only way to control dengue in Australia Dengue outbreaks have become a regular occurrence in north Queensland, Australia. Since 1995, dengue transmission has occurred every year, with
Eradication: the only way to control dengue in Australia Dengue outbreaks have become a regular occurrence in north Queensland, Australia. Since 1995, dengue transmission has occurred every year, with
Mosquito Control Matters
 Mosquito Control Matters Gary Goodman General Manager Sacramento-Yolo Mosquito & Vector Control District Sacramento Yolo Mosquito & Vector Control District To provide safe, effective and economical mosquito
Mosquito Control Matters Gary Goodman General Manager Sacramento-Yolo Mosquito & Vector Control District Sacramento Yolo Mosquito & Vector Control District To provide safe, effective and economical mosquito
Female mating patterns and mate quality in the dengue vector mosquito, Aedes aegypti. By Lori Ying
 Female mating patterns and mate quality in the dengue vector mosquito, Aedes aegypti Summary By Lori Ying Dengue fever affects 50-100 million people annually (Rigau, 1998). Scientists have recently developed
Female mating patterns and mate quality in the dengue vector mosquito, Aedes aegypti Summary By Lori Ying Dengue fever affects 50-100 million people annually (Rigau, 1998). Scientists have recently developed
Mosquito-borne virus prevention and control: a global perspective
 Mosquito-borne virus prevention and control: a global perspective Chikungunya 2017, Sapienza Universita di Roma 10 November 2017 Erika Garcia Mathematical Epidemiologist World Health Organization Geneva,
Mosquito-borne virus prevention and control: a global perspective Chikungunya 2017, Sapienza Universita di Roma 10 November 2017 Erika Garcia Mathematical Epidemiologist World Health Organization Geneva,
RELATIONSHIP BETWEEN BODY SIZE AND SEVERITY OF DENGUE HEMORRHAGIC FEVER AMONG CHILDREN AGED 0-14 YEARS
 BODY SIZE AND SEVERITY OF DHF AMONG CHILDREN RELATIONSHIP BETWEEN BODY SIZE AND SEVERITY OF DENGUE HEMORRHAGIC FEVER AMONG CHILDREN AGED 0-14 YEARS Natchaporn Pichainarong 1, Noparat Mongkalangoon 2, Siripen
BODY SIZE AND SEVERITY OF DHF AMONG CHILDREN RELATIONSHIP BETWEEN BODY SIZE AND SEVERITY OF DENGUE HEMORRHAGIC FEVER AMONG CHILDREN AGED 0-14 YEARS Natchaporn Pichainarong 1, Noparat Mongkalangoon 2, Siripen
INJURY OR DEATH FROM WEST NILE, ZIKA OR OTHER VIRUSES VECTORED BY MOSQUITOES
 INJURY OR DEATH FROM WEST NILE, ZIKA OR OTHER VIRUSES VECTORED BY MOSQUITOES Dawn H. Gouge B.Sc. Ph. D. Arthropod borne viruses are vectored to people primarily through the bites of infected mosquitoes.
INJURY OR DEATH FROM WEST NILE, ZIKA OR OTHER VIRUSES VECTORED BY MOSQUITOES Dawn H. Gouge B.Sc. Ph. D. Arthropod borne viruses are vectored to people primarily through the bites of infected mosquitoes.
On the road to a mosquito SIT programme: Mass rearing tools and quality control
 On the road to a mosquito SIT programme: Mass rearing tools and quality control R&D for Mosquito SIT in Northern State, Sudan Fabrizio Balestrino, Mark Benedict, Clélia Oliva, Hanano Yamada, Sharon Soliban,
On the road to a mosquito SIT programme: Mass rearing tools and quality control R&D for Mosquito SIT in Northern State, Sudan Fabrizio Balestrino, Mark Benedict, Clélia Oliva, Hanano Yamada, Sharon Soliban,
Malaria and Global Warming. Jocelyn Maher & Mickey Rowe
 Malaria and Global Warming Jocelyn Maher & Mickey Rowe What is Malaria? Malaria is an infectious disease caused by parasites. It is spread by the Anopheles mosquito. Malaria is an immediate concern because
Malaria and Global Warming Jocelyn Maher & Mickey Rowe What is Malaria? Malaria is an infectious disease caused by parasites. It is spread by the Anopheles mosquito. Malaria is an immediate concern because
Social Mobilization Using Strategies of Education and Communication to Prevent Dengue Fever in Bucaramanga, Colombia
 Case Study 3 Social Mobilization Using Strategies of Education and Communication to Prevent Dengue Fever in Bucaramanga, Colombia Jorge E Luna* #, Ivan Chain*, Jackeline Hernandez*, Gary G Clark**, Adriana
Case Study 3 Social Mobilization Using Strategies of Education and Communication to Prevent Dengue Fever in Bucaramanga, Colombia Jorge E Luna* #, Ivan Chain*, Jackeline Hernandez*, Gary G Clark**, Adriana
Zika as a reportable condition Testing approval and result notification Zika pregnancy registry Is there a risk of local transmission?
 Zika as a reportable condition Testing approval and result notification Zika pregnancy registry Is there a risk of local transmission? Immediate NC surveillance activities Building entomologic capacity
Zika as a reportable condition Testing approval and result notification Zika pregnancy registry Is there a risk of local transmission? Immediate NC surveillance activities Building entomologic capacity
THE GEOGRAPHIC INFORMATION SYSTEM AS AN EPIDEMIOLOGICAL TOOL IN THE SURVEILLANCE OF DENGUE VIRUS-INFECTED AEDES MOSQUITOS
 THE GEOGRAPHIC INFORMATION SYSTEM AS AN EPIDEMIOLOGICAL TOOL IN THE SURVEILLANCE OF DENGUE VIRUS-INFECTED AEDES MOSQUITOS Ratana Sithiprasasna, Somboon Patpoparn, Watcharee Attatippaholkun 4, Saravudh
THE GEOGRAPHIC INFORMATION SYSTEM AS AN EPIDEMIOLOGICAL TOOL IN THE SURVEILLANCE OF DENGUE VIRUS-INFECTED AEDES MOSQUITOS Ratana Sithiprasasna, Somboon Patpoparn, Watcharee Attatippaholkun 4, Saravudh
