Signaling changes in the stem cell factor AKT-S6 pathway in diagnostic AML samples are associated with disease relapse
|
|
|
- Lewis Green
- 5 years ago
- Views:
Transcription
1 LETTER TO THE EDITOR Citation: (2011) 1, e3; doi: /bcj & 2011 Macmillan Publishers Limited All rights reserved /11 Signaling changes in the stem cell factor AKT-S6 pathway in diagnostic AML samples are associated with disease relapse (2011) 1, e3; doi: /bcj ; published online 11 February 2011 Although current chemotherapy regimens are effective at eliminating the bulk of acute myeloid leukemia (AML) blasts, the disease relapses in the majority of patients. 1 Whether relapse arises through the selection of a relatively rare subpopulation of cells present at diagnosis having specific characteristics that facilitate chemoresistance or through the induction of changes required to render them resistant to the chemotherapy is uncertain. Identification of the characteristics that confer chemoresistance, whether selected or induced, would allow for the implementation of additional therapies that target the lynchpin of resistance, thus improving disease outcome. This study evaluated whether single-cell network profiling (SCNP), a process that simultaneously measures post-translational protein modifications (for example, phosphorylation, acetylation and so on) in multiple signaling pathways within a single cell, could be used to functionally characterize intracellular pathways associated with in vivo AML chemotherapy resistance. 2,3 Specifically, we hypothesized that leukemic blasts at relapse have different signaling characteristics from those at diagnosis and that assessing intracellular signaling networks Table 1 Clinical characteristics of patient donors for longitudinally paired diagnosis and relapse samples Donor Age (years) Gender Sample source Secondary AML FAB Cytogenetics Cytogenetic group FLT3- ITD Induction chemotherapy Induction response Relapse CR duration (weeks) M BM No M0 46,XY,t(3;21) Unfavorable Neg IDA+HDAC CR Yes (q26;q22) F BM No M2 t(6;9) Unfavorable Pos IA+ZARNESTRA a CR Yes Abbreviations: BM, bone marrow; CR, complete response; F, female; FAB, French-American-British classification system; FLT3-ITD, FMS-like tyrosine kinase 3 receptor (FLT3) internal tandem duplications (ITD); HDAC, high-dose Ara-C; IDA, idarubicin; M, male; Neg, negative; Pos, positive. a IDA+Ara-C+Zarnestra. 1 st STEP: Longitudinal study to identify signaling profiles associated with chemoresistance. AML Diagnosis A N=2 Induction Rx CR Consolidilidation Rx Signaling Modulators Relapse B N=2 G-CSF, IL-27, SCF, FLT3L A B Signaling Readouts p-stat1, p-stat3, p-stat5, p-erk, p-s6, p-akt timepoints when samples for SCNP are collected Drug Transporters ABCG2, MRP-1 Chemokine Receptor CXCR4 2 nd STEP: Test predictive value of signaling profiles in an independent data set Intracellular signaling profiles Independent dataset 47 diagnostic AML samples with clinical annotations Prediction of Relapse Figure 1 Study schema. The two-step process involves the identification of resistance-associated signaling node subpopulations followed by testing the predictive value of these profiles for disease response in an independent data set. The top portion of the diagram shows a time continuum of AML therapy, with A and B representing the time points (diagnosis and first relapse after complete response (CR) when samples were collected on the two patients for SCNP analysis). The signaling modulators, readouts, drug transporters and chemokine receptor tested are listed. The lower portion of the schema depicts the application of the chemoresistant profiles to an independent data set of 47 patients. CR, complete response; G-CSF, granulocyte colony-stimulating factor; IL-27, interleukin-27; Rx, therapy.
2 2 using the SCNP approach in longitudinally paired (that is, from the same patient) AML bone marrow (BM) samples at diagnosis and relapse time points may enable functional characterization of the mechanisms of chemoresistance in cell subpopulations that are dominant at relapse. The above hypothesis was tested by searching for resistance-associated signaling nodes in paired diagnosis/relapse samples from two AML patients and then examining the predictive value of the identified resistanceassociated signaling nodes in an independent set of diagnostic AML samples collected from patients that had a complete disease response 4 to standard induction chemotherapy and for which clinical annotation about disease relapse was available. Clinical characteristics of the two AML patients are shown in Table 1. Both patients received high-dose cytarabinebased induction chemotherapy with complete disease response followed by relapse within 1 year. Cytogenetic analysis revealed prognostically unfavorable translocations of AML1- EVI1 and DEK-NUP214 [t(6;9)] in patients 1 and 2, respectively. In addition, patient 2 had FMS-like tyrosine kinase 3 receptor internal tandem duplications (FLT3-ITD)-positive leukemia, a known poor prognostic marker for relapse risk and overall survival and associated with the DEK-NUP214 translocation in the majority of cases. 5 Healthy control BM mononuclear cells (N ¼ 2) were derived from young healthy male volunteers (age ¼ 18 and 20 years, respectively). The cryopreserved BM samples from the above two AML patients were processed (thawed, modulated, fixed, permeabilized and incubated with antibodies to both surface and intracellular proteins) 2,3,6 to assess whether specific cell subpopulations identified using cell surface phenotypes and/or signaling profiles were present in the relapsed sample in a greater percentage than observed in the corresponding diagnostic sample (Figure 1). Next, in an independent and larger group of diagnostic patient samples, blasts with the previously identified cell profiles were examined for their association with disease relapse (Figure 1). The two longitudinally paired samples were first compared for expression of conventional surface markers used to define myeloblast maturity as shown in Figure 2a. 7 Cell subpopulations Figure 2 (a) Gating analysis to define leukemic blast population. Flow cytometry plots and sequential gating scheme. The first panel is a flow cytometry dot plot indicating how non-cellular debris was excluded using an FSC and SSC gate (R1). The second panel is a flow cytometry dot plot indicating how non-viable cells were excluded and viable cells included with an SSC and Aqua viability dye gate (R2). This gating scheme ensured that only live cells were analyzed for signaling responses. The third panel is a flow cytometry dot plot indicating CD45 þ cells (R6) that were then subdivided into groups of immature CD34 þ CD11b (R1&R2&R6&R4), mature CD33 þ CD11b þ (R1&R2&R6&R5) and intermediate (R1&R2&R6 NOT R4 &R5) myeloid leukemic blasts. (b) Cell surface markers did not identify resistance-associated myeloblast subpopulations. Shown are bar graphs that depict the percentage (of total blasts) of immature, intermediate and mature blasts (as defined above in a) found in the diagnosis and relapse samples from patient 1 (top panels) and patient 2 (bottom panels).
3 3 Figure 3 Examination of signaling profiles revealed differences in relapse and diagnosis samples for SCF and FLT3L. (a) Shown are flow cytometry dot plots measuring phospho-s6 (X-axis) versus phospho-akt (Y-axis) in response to no modulator/basal, modulation with SCF or modulation with FLT3L for patient 1 (left side) and patient 2 (right side) leukemia samples at diagnosis (top panels) and at first relapse after complete remission (lower panels). (b) Figure showing the percentage of cells positive for both p-akt and p-s6 in diagnostic and relapse samples. based on these characteristics of myeloblast maturity were not informative of relapse risk for either patient sample (Figure 2b). Examination of intracellular signaling profiles revealed functionally distinct cell subsets in the otherwise phenotypically similar relapse and diagnosis samples (Figure 3 and Supplementary Figure 1). Specifically, when the relapse samples from patient 1 and patient 2 were modulated using stem cell factor (SCF), both p-akt and p-s6 were induced in 3.2 and 31.7% of cells, respectively (Figure 3). A similar finding of an increased percentage of myeloblast subpopulations defined by intracellular signaling profiles in relapse versus diagnosis samples was observed when FLT3L (inducing p-s6 and p-akt, Figure 3) and interleukin-27 or granulocyte colony-stimulating factor (inducing p-signal transducer and activator of transcription (STAT)3 and p-stat5) were used as modulators (Supplementary Figure 1). To investigate whether similar cells were present at the time of diagnosis, which would support the concept of selection, or absent, supporting the idea of an induced change, we looked for the presence of cells with similar functional responses to SCF, FLT3L, interleukin-27 and granulocyte colony-stimulating factor in the corresponding diagnosis samples. While no interleukin- 27-responsive subpopulation was identified, SCF-, FLT3L- and granulocyte colony-stimulating factor-responsive cells were observed in the diagnostic AML BM samples (Figure 3 and Supplementary Figure 1), although in a lower percentage (B1%). SCF-responsive cells, defined by the SCF:p-Akt/p-S6 signaling profile, were phenotypically diverse in the relapse AML samples compared with SCF-responsive cells in healthy donor BM samples (Figure 4). In healthy BM samples, the SCF: p-akt/p-s6 profile existed specifically in a subset of progenitor cells with the CD34 þ, CD33, CD11b phenotype (Figure 4). After identifying the resistance-associated signaling nodes in the relapsed samples, we hypothesized that detection of the same nodes in the diagnostic samples might be predictive of poor outcome (early relapse). We first applied the SCF:p-Akt/ p-s6 gating scheme (as defined in Supplementary Figure 2) to an independent set of diagnostic AML samples. The clinical characteristics of these 47 patients are shown in Table 2. All patients received high-dose cytarabine-based induction chemotherapy with disease response of complete remission. Of these, 27 experienced disease relapse (complete response followed by relapse, CR Rel), while 20 remained in complete continuous remission for two or more years. Patients from whom this independent sample set was obtained were young (41/47; o60) and a high proportion (20/47) had French-American-British classification system M2 AML. In seven diagnostic AML samples, a subset of leukemic blast cells that responded to SCF modulation by phosphorylation of p-akt and p-s6 were observed (Table 2, Supplementary Table S1). Of those seven, six patients experienced disease relapse within 2 years (P ¼ 0.21, Fisher s exact test) from remission, while the seventh patient had a complete remission lasting more than 2 years; interestingly, this AML sample had favorable cytogenetics, t(8;21) (Figure 5 and Supplementary Table S1). Of note, all of the patients with this SCF-responsive profile were less than 60 years old and, with the exception mentioned above, they all had intermediate- or high-risk cytogenetics; six out of seven also had an early myeloid FAB classification of M1 or M2. Also of note, the occurrence of the SCF:pAkt/pS6 subpopulation was independent of the presence of FLT3-ITD: only one of the six samples was positive for FLT3-ITD mutation. Importantly, the predictive value of the combination of FLT3-ITD and SCF:p-Akt/ p-s6 for disease relapse was greater than that of either biomarker individually (P ¼ 0.03, Fisher s exact test, Table 3). We next examined whether expression of c-kit, the receptor for SCF, could function as a surrogate marker for the SCF:p-Akt/ p-s6 phenotype. Although only samples that expressed c-kit
4 4 Figure 4 In the relapse samples, the SCF:p-Akt/p-S6 signaling profile is present in a small subset of AML cells that are phenotypically diverse. Myeloid cells (R1&R2&R6 gatedfsee Figure 2a) are displayed on a three-parameter plot with three fluorescent cell surface markers: CD11b (X-axis), CD33 (Y-axis) and CD34 (Z-axis). Red spheres are cells that stain positive for the SCF:p-Akt/p-S6 signaling profile. Bone marrow cells from a representative healthy individual (bottom right) show that normally the SCF:p-Akt/p-S6 profile exists mostly in a subset of progenitor cells with the CD34 þ, CD33, CD11b phenotype. To the right of each plot are box and whisker plots that show the relative expression (log 10 fluorescence) of CD34 in the SCF:p-Akt/p-S6-responsive and non-responsive populations for two relapse AML samples and one healthy sample. In the box and whisker plots, boxes contain 50% of the sample data with the median values indicated by a horizontal bar. Whiskers contain 1.5 the interquartile range and outliers past this range are shown as individual points. were able to respond to SCF, no association between c-kit expression levels and likelihood of leukemia relapse (Figure 6a) was observed, suggesting that c-kit expression is a necessary but not sufficient condition for SCF-induced intracellular signaling. In line with this observation, the removal of non-c-kitexpressing samples improved relapse prediction (Figure 6b). Furthermore, when blast cells from an AML sample were simultaneously examined for c-kit and the downstream signaling marker p-akt, intra-patient heterogeneity in c-kit expression and response to SCF within c-kit-expressing cells were observed (Figure 6c). We also examined whether FLT3L:p-Akt/p-S6, granulocyte colony-stimulating factor:p-stat3/5 or interleukin-27:p-stat3/ 5 signaling nodes predicted poor outcome in the same independent set of diagnostic AML samples. Unlike SCF:p-Akt/ p-s6 gate, no association was found with disease relapse (Supplementary Table S2). Relapse due to chemoresistant residual disease is a major cause of death in both adult and pediatric patients with AML, and aberrant signal transduction within pathways that control cell proliferation and survival is thought to have an important role in secondary chemoresistance. In this study, we used SCNP as a strategy to identify specific signaling pathway profiles associated with in vivo chemoresistance using paired diagnosis and relapse samples. Although it was performed on a limited number of paired AML samples, our study provides unique insights into the nature of AML secondary chemoresistance in rare cell populations, identifying a functionally characterized cell subset associated with likelihood of early relapse when the assay was applied in a separate patient cohort. A subset of leukemia cells with enhanced activity within the phosphoinositide 3-kinase/Akt cascade (SCF:p-Akt/p-S6) was found to be commonly expanded in the two leukemia samples collected at relapse. Importantly, the presence of cell subpopulations expressing this same signaling profile at diagnosis was associated with disease relapse after complete response to induction chemotherapy in an independent sample set of AML diagnostic samples. Although the SCF:p-Akt/p-S6 profile was not present in all patients with relapsed disease, all but one patient with a diagnostic sample containing a subpopulation of X3%
5 Table 2 Clinical characteristics of independent test set of 47 patient samples 5 Characteristic Total 40 non-scf responsive 7 SCF responsive Total samples ¼ 47 CCR CR Rel CCR CR Rel CCR 20 (74%) 19 1 CR Rel 27 (26%) 21 6 Age o60 years 41 (87%) years 6 (13%) Cytogenetics Favorable 6 (12.7%) Intermediate 24 (51%) Unfavorable 17 (29.7%) FAB M M M M M4EOS M5 (A,B,C) M Unknown FLT3 mutation ITD 10 (21.3%) WT 35 (74.5%) Unknown 2 (4.2%) Abbreviations: CCR, complete continuous remission; CR, complete response; CR Rel, complete response followed by relapse; SCF, stem cell factor; WT, wild type. Table 3 status The SCF: pakt/ps6 profile is independent of FLT3-ITD SCF non-responsive and FLT3-WT SCF responsive or FLT3-ITD CCR 17 3 CR Rel Fisher s test P ¼ 0.03 Abbreviations: CCR, complete continuous remission; CR, complete response; SCF, stem cell factor; WT, wild type. Figure 5 Application of SCF:p-Akt/p-S6 gate identifies a subset of patients with relapsed disease. Shown are box and whisker plots of patients with leukemia that relapsed within 2 years (complete response (CR) Rel, right side) versus those in complete continuous remission for 2 or more years (CCR, left side) and the percentage of SCF-responsive (inducing p-s6 and p-akt) blasts. To the right of the plots each symbol represents an individual sample. A circle is drawn around the six patient samples whose diagnostic samples showed X3% of SCF:p-Akt/ p-s6 cells and who experienced disease relapse. The cytogenetics of the CCR sample with the SCF-responsive subpopulation is depicted. Note: In box and whisker plots, boxes contain 50% of the sample data, with the median values indicated by a horizontal bar. Whiskers contain 1.5 the interquartile range and outliers past this range are shown as individual points. SCF:p-Akt/p-S6 cells relapsed within 2 years of remission. These data support the marked biological heterogeneity at the basis of AML secondary chemoresistance and lend merit to the approach of studying signaling profiles in functionally distinct subpopulations in longitudinally collected AML samples before and after therapy to identify poor-prognostic cell populations. Currently there are no measures to indicate why patients with similar clinically appearing disease have different responses to therapy, with some remaining disease free while others undergo disease relapse and ultimately succumb. SCNP permits an accurate characterization of each individual s leukemia signaling pathway phenotype and biological heterogeneity, allowing for a more efficient delineation of the normality or pathology of leukemic subpopulations. This study shows that leukemic cell populations differ quantitatively and qualitatively before and after in-vivo therapeutic pressure in AML, and that SCNP offers a novel approach to identify chemotherapy-resistant subpopulations that may predispose patients to disease relapse.
6 6 Figure 6 (a) c-kit (SCF receptor) expression is not predictive of SCF responsiveness. Shown are box and whisker plots of patients with leukemia that relapsed within 2 years (complete response (CR) Rel, right side) versus those in complete continuous remission for 2 or more years (CCR, left side) and the percentage of cells with c-kit surface expression. To the right of the plots each symbol represents an individual sample. Note: In box and whisker plots, boxes contain 50% of the sample data, with the median values indicated by a horizontal bar. Whiskers contain 1.5 the interquartile range and outliers past this range are shown as individual points. (b) Only samples that expressed c-kit were able to respond to SCF. Scatter plot of SCF-responsive SCF-p-Akt/p-S6 (X-axis) and percent-positive cells for c-kit (Y-axis) for relapsed samples (circles) and CCR samples (pluses). (c) Simultaneous staining of c-kit and p-akt shows multiple c-kit þ cell subsets that vary in p-akt signaling in response to SCF. Phospho- Akt versus c-kit 2-D contour plots with and without SCF for 15-min incubation. Quadrant gate was applied based on the isotype controls. Conflict of interest Dr Cohen, Dr Woronicz and Dr Fantl were employees of Nodality during the time the research was conducted. Todd Covey, Dr Putta, Dr Gayko and Dr Cesano were employees of Nodality during the time the research was conducted and are presently employed by Nodality. Dr Kornblau declares no conflict of interest. SM Kornblau 1, T Covey 2, S Putta 2, A Cohen 2, J Woronicz 2, WJ Fantl 2,3, U Gayko 2 and A Cesano 2 1 Department of Leukemia, The University of Texas MD Anderson Cancer Center, Houston, TX, USA and 2 Nodality Inc., South San Francisco, CA, USA; 3 Current address: Department of Microbiology and Immunology, Stanford University, Palo Alto, CA, USA alessandra.cesano@nodality.com References 1 Estey E, Dohner H. Acute myeloid leukaemia. Lancet 2006; 368: Kornblau SM, Minden MD, Rosen DB, Putta S, Cohen A, Covey T et al. Dynamic single-cell network profiles in acute myelogenous leukemia are associated with patient response to standard induction therapy. Clin Cancer Res 2010; 16: Rosen DB, Minden MD, Kornblau SM, Cohen A, Gayko U, Putta S et al. Functional characterization of FLT3 receptor signaling deregulation in acute myeloid leukemia by single cell network profiling (SCNP). PLoS One 2010; 5: e Cheson BD, Bennett JM, Kopecky KJ, Buchner T, Willman CL, Estey EH et al. Revised recommendations of the International Working Group for Diagnosis, Standardization of Response Criteria, Treatment Outcomes, and Reporting Standards for Therapeutic Trials in Acute Myeloid Leukemia. J Clin Oncol 2003; 21: Chi Y, Lindgren V, Quigley S, Gaitonde S. Acute myelogenous leukemia with t(6;9)(p23;q34) and marrow basophilia: an overview. Arch Pathol Lab Med 2008; 132: Irish JM, Hovland R, Krutzik PO, Perez OD, Bruserud O, Gjertsen BT et al. Single cell profiling of potentiated phospho-protein networks in cancer cells. Cell 2004; 118: Stelzer GT, Goodpasture L. Use of multiparameter flow cytometry and immunophenotyping for the diagnosis and classification of acute myeloid leukemia. In: Stewart CC, Nicholson JKA (eds). Immunophenotyping. Wiley-Liss: Wilmington, DE, 2000, pp This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit creativecommons.org/licenses/by-nc-nd/3.0/ Supplementary Information accompanies the paper on website (
SUPPLEMENTARY FIG. S3. Kaplan Meier survival analysis followed with log-rank test of de novo acute myeloid leukemia patients selected by age <60, IA
 Supplementary Data Supplementary Appendix A: Treatment Protocols Treatment protocols of 123 cases patients were treated with the protocols as follows: 110 patients received standard DA (daunorubicin 45
Supplementary Data Supplementary Appendix A: Treatment Protocols Treatment protocols of 123 cases patients were treated with the protocols as follows: 110 patients received standard DA (daunorubicin 45
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Can we classify cancer using cell signaling?
 Can we classify cancer using cell signaling? Central hypotheses (big ideas) Alterations to signaling genes would cause leukemic cells to react in an inappropriate or sensitized manner to environmental
Can we classify cancer using cell signaling? Central hypotheses (big ideas) Alterations to signaling genes would cause leukemic cells to react in an inappropriate or sensitized manner to environmental
Corporate Medical Policy. Policy Effective February 23, 2018
 Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Mixed Phenotype Acute Leukemias
 Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials
 Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials Fda.gov Adriano Venditti Hematology, University Tor Vergata, Rome, Italy Minimal Residual Disease 10 12 Relapse
Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials Fda.gov Adriano Venditti Hematology, University Tor Vergata, Rome, Italy Minimal Residual Disease 10 12 Relapse
N Engl J Med Volume 373(12): September 17, 2015
 Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Acute myeloid leukemia: prognosis and treatment. Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg
 Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Pearson r = P (one-tailed) = n = 9
 8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
VUmc Basispresentatie
 Clinical diagnostic cytometry Gerrit J Schuurhuis Dept of Hematology VU University Medical Center Amsterdam, Netherlands Use of immunophenotyping at diagnosis to trace residual disease after therapy 1.
Clinical diagnostic cytometry Gerrit J Schuurhuis Dept of Hematology VU University Medical Center Amsterdam, Netherlands Use of immunophenotyping at diagnosis to trace residual disease after therapy 1.
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Supplementary Materials Extracting a Cellular Hierarchy from High-dimensional Cytometry Data with SPADE
 Supplementary Materials Extracting a Cellular Hierarchy from High-dimensional Cytometry Data with SPADE Peng Qiu1,4, Erin F. Simonds2, Sean C. Bendall2, Kenneth D. Gibbs Jr.2, Robert V. Bruggner2, Michael
Supplementary Materials Extracting a Cellular Hierarchy from High-dimensional Cytometry Data with SPADE Peng Qiu1,4, Erin F. Simonds2, Sean C. Bendall2, Kenneth D. Gibbs Jr.2, Robert V. Bruggner2, Michael
ETP - Acute Lymphoblastic Leukaemia
 ETP - Acute Lymphoblastic Leukaemia Dr Sally Campbell - Royal Children s Hospital Melbourne 24 February 2017 T-ALL 12-15% of all newly diagnosed ALL cases in pediatrics are T-ALL T-ALL behaves differently
ETP - Acute Lymphoblastic Leukaemia Dr Sally Campbell - Royal Children s Hospital Melbourne 24 February 2017 T-ALL 12-15% of all newly diagnosed ALL cases in pediatrics are T-ALL T-ALL behaves differently
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
Tools for MRD in AML: flow cytometry
 ACUTE MYELOID LEUKEMIA MEETING Ravenna - October 27, 2017 Tools for MRD in AML: flow cytometry Francesco Buccisano Can MRD improve outcome determina3on? No. of leukemic cells 10 12 10 10 10 8 10 6 10 4
ACUTE MYELOID LEUKEMIA MEETING Ravenna - October 27, 2017 Tools for MRD in AML: flow cytometry Francesco Buccisano Can MRD improve outcome determina3on? No. of leukemic cells 10 12 10 10 10 8 10 6 10 4
Stem cell transplantation for patients with AML in Republic of Macedonia: - 15 years of experience -
 Stem cell transplantation for patients with AML in Republic of Macedonia: - 15 years of experience - R E S E A R C H A S S O C I A T E P R O F. D - R Z L A T E S T O J A N O S K I Definition Acute myeloid
Stem cell transplantation for patients with AML in Republic of Macedonia: - 15 years of experience - R E S E A R C H A S S O C I A T E P R O F. D - R Z L A T E S T O J A N O S K I Definition Acute myeloid
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia
 Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
MRD detection in AML. Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome
 MRD detection in AML Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome Determinants of Treatment Response Leukemia Tumor burden Growth potential Drug resistance Karyotype Genetics Host
MRD detection in AML Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome Determinants of Treatment Response Leukemia Tumor burden Growth potential Drug resistance Karyotype Genetics Host
HD1 (FLU) HD2 (EBV) HD2 (FLU)
 ramer staining + anti-pe beads ramer staining a HD1 (FLU) HD2 (EBV) HD2 (FLU).73.11.56.46.24 1.12 b CD127 + c CD127 + d CD127 - e CD127 - PD1 - PD1 + PD1 + PD1-1 1 1 1 %CD127 + PD1-8 6 4 2 + anti-pe %CD127
ramer staining + anti-pe beads ramer staining a HD1 (FLU) HD2 (EBV) HD2 (FLU).73.11.56.46.24 1.12 b CD127 + c CD127 + d CD127 - e CD127 - PD1 - PD1 + PD1 + PD1-1 1 1 1 %CD127 + PD1-8 6 4 2 + anti-pe %CD127
GENETIC TESTING FOR FLT3, NPM1 AND CEBPA VARIANTS IN CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA
 CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
Myeloperoxidase Expression in Acute Myeloid Leukemia Helps Identifying Patients to Benefit from Transplant
 Original Article http://dx.doi.org/1349/ymj.212.53.3.53 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 53(3):53-536, 212 Myeloperoxidase Expression in Acute Myeloid Leukemia Helps Identifying Patients
Original Article http://dx.doi.org/1349/ymj.212.53.3.53 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 53(3):53-536, 212 Myeloperoxidase Expression in Acute Myeloid Leukemia Helps Identifying Patients
Impact of Day 14 Bone Marrow Biopsy on Re-Induction Decisions and Prediction of a Complete Response in Acute Myeloid Leukemia Cases
 DOI:10.22034/APJCP.2018.19.2.421 RESEARCH ARTICLE Editorial Process: Submission:08/01/2017 Acceptance:12/09/2017 Impact of Day 14 Bone Marrow Biopsy on Re-Induction Decisions and Prediction of a Complete
DOI:10.22034/APJCP.2018.19.2.421 RESEARCH ARTICLE Editorial Process: Submission:08/01/2017 Acceptance:12/09/2017 Impact of Day 14 Bone Marrow Biopsy on Re-Induction Decisions and Prediction of a Complete
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
Acute Leukemia. Sebastian Giebel. Geneva 03/04/
 Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Supplementary Figure 1. BMS enhances human T cell activation in vitro in a
 Supplementary Figure 1. BMS98662 enhances human T cell activation in vitro in a concentration-dependent manner. Jurkat T cells were activated with anti-cd3 and anti-cd28 antibody in the presence of titrated
Supplementary Figure 1. BMS98662 enhances human T cell activation in vitro in a concentration-dependent manner. Jurkat T cells were activated with anti-cd3 and anti-cd28 antibody in the presence of titrated
Characteristics and Outcome of Therapy-Related Acute Promyelocytic Leukemia After Different Front-line Therapies
 Characteristics and Outcome of Therapy-Related Acute Promyelocytic Leukemia After Different Front-line Therapies Sabine Kayser, * Julia Krzykalla, Michelle A. Elliott, Kelly Norsworthy, Patrick Gonzales,
Characteristics and Outcome of Therapy-Related Acute Promyelocytic Leukemia After Different Front-line Therapies Sabine Kayser, * Julia Krzykalla, Michelle A. Elliott, Kelly Norsworthy, Patrick Gonzales,
Aberrant Expression of CD7 in Myeloblasts Is Highly Associated With De Novo Acute Myeloid Leukemias With FLT3/ITD Mutation
 Hematopathology / CD7 Expression and FLT3/ITD Mutation in AML Aberrant Expression of CD7 in Myeloblasts Is Highly Associated With De Novo Acute Myeloid Leukemias With FLT3/ITD Mutation Veronica Rausei-Mills,
Hematopathology / CD7 Expression and FLT3/ITD Mutation in AML Aberrant Expression of CD7 in Myeloblasts Is Highly Associated With De Novo Acute Myeloid Leukemias With FLT3/ITD Mutation Veronica Rausei-Mills,
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy. Not so fast!
 All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Personalized Therapy for Acute Myeloid Leukemia. Patrick Stiff MD Loyola University Medical Center
 Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12
 1 Supplementary Data Figure legends Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12 serum levels measured by multiplex ELISA (Luminex) in FL patients before
1 Supplementary Data Figure legends Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12 serum levels measured by multiplex ELISA (Luminex) in FL patients before
Nature Genetics: doi: /ng Supplementary Figure 1. HOX fusions enhance self-renewal capacity.
 Supplementary Figure 1 HOX fusions enhance self-renewal capacity. Mouse bone marrow was transduced with a retrovirus carrying one of three HOX fusion genes or the empty mcherry reporter construct as described
Supplementary Figure 1 HOX fusions enhance self-renewal capacity. Mouse bone marrow was transduced with a retrovirus carrying one of three HOX fusion genes or the empty mcherry reporter construct as described
Molecular Hematopathology Leukemias I. January 14, 2005
 Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Acute Myeloid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplant_for_acute_myeloid_leukemia
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Acute Myeloid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplant_for_acute_myeloid_leukemia
Acute Lymphoblastic and Myeloid Leukemia
 Acute Lymphoblastic and Myeloid Leukemia Pre- and Post-Disease Form Acute Lympoblastic Leukemia Mary Eapen MD, MS Acute Lymphoblastic Leukemia SEER Age-adjusted incidence rate 1.6 per 100,000 men and women
Acute Lymphoblastic and Myeloid Leukemia Pre- and Post-Disease Form Acute Lympoblastic Leukemia Mary Eapen MD, MS Acute Lymphoblastic Leukemia SEER Age-adjusted incidence rate 1.6 per 100,000 men and women
Indication for unrelated allo-sct in 1st CR AML
 Indication for unrelated allo-sct in 1st CR AML It is time to say! Decision of allo-sct: factors to be considered Cytogenetic risk status Molecular genetics FLT3; NPM1, CEBPA. Response to induction Refractoriness
Indication for unrelated allo-sct in 1st CR AML It is time to say! Decision of allo-sct: factors to be considered Cytogenetic risk status Molecular genetics FLT3; NPM1, CEBPA. Response to induction Refractoriness
MPL W515L K mutation
 MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Measure Specifications Measure Description
 CMS ID/CMS QCDR ID: CAP 17 Title: FMS-like Tyrosine 3-Internal Tandem Duplication (FLT3-ITD) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Acute Myeloid Leukemia
CMS ID/CMS QCDR ID: CAP 17 Title: FMS-like Tyrosine 3-Internal Tandem Duplication (FLT3-ITD) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Acute Myeloid Leukemia
Evolving Targeted Management of Acute Myeloid Leukemia
 Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
Long-Term Outcome of Autologous Hematopoietic Stem Cell Transplantation (AHSCT) for Acute Myeloid Leukemia (AML)- Single Center Retrospective Analysis
 Pathol. Oncol. Res. (2018) 24:469 475 DOI 10.1007/s12253-017-0266-7 ORIGINAL ARTICLE Long-Term Outcome of Autologous Hematopoietic Stem Cell Transplantation (AHSCT) for Acute Myeloid Leukemia (AML)- Single
Pathol. Oncol. Res. (2018) 24:469 475 DOI 10.1007/s12253-017-0266-7 ORIGINAL ARTICLE Long-Term Outcome of Autologous Hematopoietic Stem Cell Transplantation (AHSCT) for Acute Myeloid Leukemia (AML)- Single
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Minimal residual disease (MRD) in AML; coming of age. Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital
 Minimal residual disease (MRD) in AML; coming of age Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital 1. The logistics of MRD assessment in AML 2. The clinical
Minimal residual disease (MRD) in AML; coming of age Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital 1. The logistics of MRD assessment in AML 2. The clinical
JAK2 V617F analysis. Indication: monitoring of therapy
 JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia
 Acute Myeloid Leukemia Articles Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia Bruno C. Medeiros, 1 Megan Othus, 2,3 Min Fang, 3,4 Frederick R. Appelbaum,
Acute Myeloid Leukemia Articles Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia Bruno C. Medeiros, 1 Megan Othus, 2,3 Min Fang, 3,4 Frederick R. Appelbaum,
Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia
 Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia Martha Arellano, MD 1 ; Suchita Pakkala, MD 1 ; Amelia Langston, MD 1 ; Mourad Tighiouart,
Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia Martha Arellano, MD 1 ; Suchita Pakkala, MD 1 ; Amelia Langston, MD 1 ; Mourad Tighiouart,
The Past, Present, and Future of Acute Myeloid Leukemia
 The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
Nature Immunology: doi: /ni.3412
 Supplementary Figure 1 Gata1 expression in heamatopoietic stem and progenitor populations. (a) Unsupervised clustering according to 100 top variable genes across single pre-gm cells. The two main cell
Supplementary Figure 1 Gata1 expression in heamatopoietic stem and progenitor populations. (a) Unsupervised clustering according to 100 top variable genes across single pre-gm cells. The two main cell
Human chronic myeloid leukemia stem cells are insensitive to imatinib despite inhibition of BCR-ABL activity
 Research article Related Commentary, page 22 Human chronic myeloid leukemia stem cells are insensitive to imatinib despite inhibition of BCR-ABL activity Amie S. Corbin, 1,2 Anupriya Agarwal, 1 Marc Loriaux,
Research article Related Commentary, page 22 Human chronic myeloid leukemia stem cells are insensitive to imatinib despite inhibition of BCR-ABL activity Amie S. Corbin, 1,2 Anupriya Agarwal, 1 Marc Loriaux,
New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke
 University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
Welcome and Introductions
 Information for Patients With Acute Myeloid Leukemia (AML) Welcome and Introductions Information for Patients With Acute Myeloid Leukemia (AML) Mark B. Juckett, MD Vice Chair for Clinical Affairs and Quality
Information for Patients With Acute Myeloid Leukemia (AML) Welcome and Introductions Information for Patients With Acute Myeloid Leukemia (AML) Mark B. Juckett, MD Vice Chair for Clinical Affairs and Quality
Test Name Results Units Bio. Ref. Interval. Positive
 Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Standard immunophenotyping of leukemia cells in acute myeloid leukemia (AML)
 Clinical immunology Standard immunophenotyping of leukemia cells in acute myeloid leukemia (AML) ` JOLANTA WOZNIAK, JOANNA KOPEÆ-SZLÊZAK Department of Haematological Cytobiology, Institut of Haematology
Clinical immunology Standard immunophenotyping of leukemia cells in acute myeloid leukemia (AML) ` JOLANTA WOZNIAK, JOANNA KOPEÆ-SZLÊZAK Department of Haematological Cytobiology, Institut of Haematology
Supplementary Materials for
 www.sciencetranslationalmedicine.org/cgi/content/full/8/339/339ra69/dc1 Supplementary Materials for The caspase-8 inhibitor emricasan combines with the SMAC mimetic birinapant to induce necroptosis and
www.sciencetranslationalmedicine.org/cgi/content/full/8/339/339ra69/dc1 Supplementary Materials for The caspase-8 inhibitor emricasan combines with the SMAC mimetic birinapant to induce necroptosis and
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Acute Myeloid Leukemia: A Patient s Perspective
 Acute Myeloid Leukemia: A Patient s Perspective Patrick A Hagen, MD, MPH Cardinal Bernardin Cancer Center Loyola University Medical Center Maywood, IL Overview 1. What is AML? 2. Who gets AML? Epidemiology
Acute Myeloid Leukemia: A Patient s Perspective Patrick A Hagen, MD, MPH Cardinal Bernardin Cancer Center Loyola University Medical Center Maywood, IL Overview 1. What is AML? 2. Who gets AML? Epidemiology
Supplementary Information
 Supplementary Information Distinct bone marrow-derived and tissue resident macrophage lineages proliferate at key stages during inflammation. 1 Luke C. Davies, 1 Marcela Rosas, 2 Stephen J. Jenkins, 1
Supplementary Information Distinct bone marrow-derived and tissue resident macrophage lineages proliferate at key stages during inflammation. 1 Luke C. Davies, 1 Marcela Rosas, 2 Stephen J. Jenkins, 1
Jeanne Palmer February 26, 2017 Mayo Clinic, Phoenix, AZ
 Jeanne Palmer February 26, 2017 Mayo Clinic, Phoenix, AZ What is acute leukemia? Cancer of the white blood cells Acute leukemia- Acute myelogenous leukemia Acute myeloid leukemia Myelofibrosis- Blast phase
Jeanne Palmer February 26, 2017 Mayo Clinic, Phoenix, AZ What is acute leukemia? Cancer of the white blood cells Acute leukemia- Acute myelogenous leukemia Acute myeloid leukemia Myelofibrosis- Blast phase
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Update on the WHO Classification of Acute Myeloid Leukemia. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Case 089: Therapy Related t(8;21)(q22;q22) AML and
 Case 089: Therapy Related t(8;21)(q22;q22) AML and SM-AHNMD ST Pullarkat 1, V Pullarkat 2, SH Kroft 3, CS Wilson 4, M Thein 5, WW Grody 1, and RK Brynes 5 1 UCLA, 2 City of Hope National Med Ctr, 3 Med
Case 089: Therapy Related t(8;21)(q22;q22) AML and SM-AHNMD ST Pullarkat 1, V Pullarkat 2, SH Kroft 3, CS Wilson 4, M Thein 5, WW Grody 1, and RK Brynes 5 1 UCLA, 2 City of Hope National Med Ctr, 3 Med
Supplementary Figure 1. Example of gating strategy
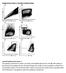 Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD
 Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
Treating Higher-Risk MDS. Case presentation. Defining higher risk MDS. IPSS WHO IPSS: WPSS MD Anderson PSS
 Treating Higher-Risk MDS Eyal Attar, M.D. Massachusetts General Hospital Cancer Center eattar@partners.org 617-724-1124 Case presentation 72 year old man, prior acoustic neuroma WBC (X10 3 /ul) 11/08 12/08
Treating Higher-Risk MDS Eyal Attar, M.D. Massachusetts General Hospital Cancer Center eattar@partners.org 617-724-1124 Case presentation 72 year old man, prior acoustic neuroma WBC (X10 3 /ul) 11/08 12/08
Remission induction in acute myeloid leukemia
 Int J Hematol (2012) 96:164 170 DOI 10.1007/s12185-012-1121-y PROGRESS IN HEMATOLOGY How to improve the outcome of adult acute myeloid leukemia? Remission induction in acute myeloid leukemia Eytan M. Stein
Int J Hematol (2012) 96:164 170 DOI 10.1007/s12185-012-1121-y PROGRESS IN HEMATOLOGY How to improve the outcome of adult acute myeloid leukemia? Remission induction in acute myeloid leukemia Eytan M. Stein
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Hematology Measure #1: Myelodysplastic Syndrome (MDS) and Acute Leukemias: Baseline Cytogenetic Testing Performed on Bone Marrow
 Hematology Measure #1: Myelodysplastic Syndrome (MDS) and Acute Leukemias: Baseline Cytogenetic Testing Performed on Bone Marrow This measure may be used as an Accountability measure Clinical Performance
Hematology Measure #1: Myelodysplastic Syndrome (MDS) and Acute Leukemias: Baseline Cytogenetic Testing Performed on Bone Marrow This measure may be used as an Accountability measure Clinical Performance
NUMERATOR: Patients who had baseline cytogenetic testing performed on bone marrow
 Quality ID #67 (NQF 0377): Hematology: Myelodysplastic Syndrome (MDS) and Acute Leukemias: Baseline Cytogenetic Testing Performed on Bone Marrow National Quality Strategy Domain: Effective Clinical Care
Quality ID #67 (NQF 0377): Hematology: Myelodysplastic Syndrome (MDS) and Acute Leukemias: Baseline Cytogenetic Testing Performed on Bone Marrow National Quality Strategy Domain: Effective Clinical Care
AML IN OLDER PATIENTS Whenever possible, intensive induction therapy should be considered
 AML IN OLDER PATIENTS Whenever possible, intensive induction therapy should be considered Charles A. Schiffer, M.D. Karmanos Cancer Institute Wayne State University School of Medicine Detroit, MI WHY ARE
AML IN OLDER PATIENTS Whenever possible, intensive induction therapy should be considered Charles A. Schiffer, M.D. Karmanos Cancer Institute Wayne State University School of Medicine Detroit, MI WHY ARE
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
Prospective Randomization Trial of G-CSF-Primed Induction Regimen versus Standard Regimen in Patients with AML
 Original Article-Cancer and stem cells www.cmj.ac.kr Prospective Randomization Trial of G-CSF-Primed Induction Regimen versus Standard Regimen in Patients with AML Yoo Jin Lee, Joon Ho Moon, Jong Gwang
Original Article-Cancer and stem cells www.cmj.ac.kr Prospective Randomization Trial of G-CSF-Primed Induction Regimen versus Standard Regimen in Patients with AML Yoo Jin Lee, Joon Ho Moon, Jong Gwang
OUTCOME OF ACUTE MYELOID LEUKEMIA IN PATIENTS UP TO 65 YEARS OF AGE AT HEMATOLOGY AND BONE MARROW TRANSPLANTATION UNIT IN ALGIERS DURING 14 YEARS
 OUTCOME OF ACUTE MYELOID LEUKEMIA IN PATIENTS UP TO 65 YEARS OF AGE AT HEMATOLOGY AND BONE MARROW TRANSPLANTATION UNIT IN ALGIERS DURING 14 YEARS S.Akhrouf, F.Belhadri, A.Talbi, H.Moussaoui, M.Benakli,
OUTCOME OF ACUTE MYELOID LEUKEMIA IN PATIENTS UP TO 65 YEARS OF AGE AT HEMATOLOGY AND BONE MARROW TRANSPLANTATION UNIT IN ALGIERS DURING 14 YEARS S.Akhrouf, F.Belhadri, A.Talbi, H.Moussaoui, M.Benakli,
Normal & Leukaemic haematopoiesis. Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore
 Normal & Leukaemic haematopoiesis 2010 Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore Use of Immunophenotyping today Lineage assignment Differentiation of
Normal & Leukaemic haematopoiesis 2010 Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore Use of Immunophenotyping today Lineage assignment Differentiation of
Th17 and Th17/Treg ratio at early HIV infection associate with protective HIV-specific CD8 + T-cell responses and disease progression
 Th17 and Th17/Treg ratio at early HIV infection associate with protective HIV-specific CD8 T-cell responses and disease progression Juliana Falivene 1, Yanina Ghiglione 1, Natalia Laufer 1,3, María Eugenia
Th17 and Th17/Treg ratio at early HIV infection associate with protective HIV-specific CD8 T-cell responses and disease progression Juliana Falivene 1, Yanina Ghiglione 1, Natalia Laufer 1,3, María Eugenia
Keywords: Acute Myeloid Leukemia, FLT3-ITD Mutation, FAB Subgroups, Cytogenetic Risk Groups
 Original Articleeee fms Like Tyrosine kinase3- Internal Tandem Duplication (FLT3-ITD) in Acute Myeloid Leukemia, Mutation Frequency and its Relation with Complete Remission, 2007-2008 Emami AH, 1 Shekarriz
Original Articleeee fms Like Tyrosine kinase3- Internal Tandem Duplication (FLT3-ITD) in Acute Myeloid Leukemia, Mutation Frequency and its Relation with Complete Remission, 2007-2008 Emami AH, 1 Shekarriz
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Acute myeloid leukemia: a comprehensive review and 2016 update
 OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
SUPPLEMENTARY INFORMATION
 DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Page: 1 of 12. Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Leukemia
 Page: 1 of 12 Last Review Status/Date: September 2015 Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Description Treatment of acute myeloid leukemia (AML) is based upon risk stratification,
Page: 1 of 12 Last Review Status/Date: September 2015 Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Description Treatment of acute myeloid leukemia (AML) is based upon risk stratification,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD
 Photo by Tynan Studio Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD 96 Atlas of Childhood Cancer in Ontario (1985-2004) Chapter 6: Leukemia 6 Leukemia Atlas of Childhood
Photo by Tynan Studio Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD 96 Atlas of Childhood Cancer in Ontario (1985-2004) Chapter 6: Leukemia 6 Leukemia Atlas of Childhood
Case #16: Diagnosis. T-Lymphoblastic lymphoma. But wait, there s more... A few weeks later the cytogenetics came back...
 Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
BL-8040: BEST-IN-CLASS CXCR4 ANTAGONIST FOR TREATMENT OF ONCOLOGICAL MALIGNANCIES. Overview and Mechanism of Action Dr.
 BL-8040: BEST-IN-CLASS CXCR4 ANTAGONIST FOR TREATMENT OF ONCOLOGICAL MALIGNANCIES Overview and Mechanism of Action Dr. Leah Klapper, CSO 88 BL-8040: Novel CXCR4 Antagonist For Hematological Cancers Indications:
BL-8040: BEST-IN-CLASS CXCR4 ANTAGONIST FOR TREATMENT OF ONCOLOGICAL MALIGNANCIES Overview and Mechanism of Action Dr. Leah Klapper, CSO 88 BL-8040: Novel CXCR4 Antagonist For Hematological Cancers Indications:
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4
 Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
CHALLENGING CASES PRESENTATION
 CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
Single Technology Appraisal (STA) Midostaurin for untreated acute myeloid leukaemia
 Single Technology Appraisal (STA) Midostaurin for untreated acute myeloid leukaemia Response to consultee and commentator comments on the draft remit and draft scope (pre-referral) Please note: Comments
Single Technology Appraisal (STA) Midostaurin for untreated acute myeloid leukaemia Response to consultee and commentator comments on the draft remit and draft scope (pre-referral) Please note: Comments
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Supplementary Table; Supplementary Figures and legends S1-S21; Supplementary Materials and Methods
 Silva et al. PTEN posttranslational inactivation and hyperactivation of the PI3K/Akt pathway sustain primary T cell leukemia viability Supplementary Table; Supplementary Figures and legends S1-S21; Supplementary
Silva et al. PTEN posttranslational inactivation and hyperactivation of the PI3K/Akt pathway sustain primary T cell leukemia viability Supplementary Table; Supplementary Figures and legends S1-S21; Supplementary
Gilteritinib for relapsed or refractory acute myeloid
 NIHR Innovation Observatory Evidence Briefing: May 2018 Gilteritinib for relapsed or refractory acute myeloid leukaemia (AML) with an FLT3 mutation second line NIHRIO (HSRIC) ID: 11486 NICE ID: 8749 LAY
NIHR Innovation Observatory Evidence Briefing: May 2018 Gilteritinib for relapsed or refractory acute myeloid leukaemia (AML) with an FLT3 mutation second line NIHRIO (HSRIC) ID: 11486 NICE ID: 8749 LAY
MUD SCT for Paediatric AML?
 7 th South African Symposium on Haematopoietic Stem Cell Transplantation MUD SCT for Paediatric AML? Alan Davidson Haematology / Oncology Service Red Cross Children s Hospital THE SCENARIO A 10 year old
7 th South African Symposium on Haematopoietic Stem Cell Transplantation MUD SCT for Paediatric AML? Alan Davidson Haematology / Oncology Service Red Cross Children s Hospital THE SCENARIO A 10 year old
CME/SAM. Acute Myeloid Leukemia With Monosomal Karyotype. Morphologic, Immunophenotypic, and Molecular Findings
 AJCP / Original Article Acute Myeloid Leukemia With Monosomal Karyotype Morphologic, Immunophenotypic, and Molecular Findings Olga K. Weinberg, MD, 1 Robert S. Ohgami, MD, PhD, 2 Lisa Ma, 2 Katie Seo,
AJCP / Original Article Acute Myeloid Leukemia With Monosomal Karyotype Morphologic, Immunophenotypic, and Molecular Findings Olga K. Weinberg, MD, 1 Robert S. Ohgami, MD, PhD, 2 Lisa Ma, 2 Katie Seo,
