A Prospective Comparison of Procedural Sedation and Ultrasound-guided Interscalene Nerve Block for Shoulder Reduction in the Emergency Department
|
|
|
- Agnes Norman
- 5 years ago
- Views:
Transcription
1 A Prospective Comparison of Procedural Sedation and Ultrasound-guided Interscalene Nerve Block for Shoulder Reduction in the Emergency Department Michael Blaivas, MD, Srikar Adhikari, MD, RDMS, and Lina Lander, ScD Abstract Objectives: Emergency physicians (EPs) are beginning to use ultrasound (US) guidance to perform regional nerve blocks. The primary objective of this study was to compare length of stay (LOS) in patients randomized to US-guided interscalene block or procedural sedation to facilitate reduction of shoulder dislocation in the emergency department (ED). The secondary objectives were to compare one-on-one health care provider time, pain experienced by the patient during reduction, and patient satisfaction between the two groups. Methods: This was a prospective, randomized study of patients presenting to the ED with shoulder dislocation. The study was conducted at an academic Level I trauma center ED with an annual census of approximately 80,000. Patients were eligible for the study if they were at least 18 years of age and required reduction of a shoulder dislocation. A convenience sample of patients was randomized to either traditional procedural sedation or US-guided interscalene nerve block. Procedural sedation was performed with etomidate as the sole agent. Interscalene blocks were performed by hospital-credentialed EPs using sterile technique and a SonoSite MicroMaxx US machine with a high-frequency linear array transducer. Categorical variables were evaluated using Fisher s exact test, and continuous variables were analyzed using the Wilcoxon rank sum test. Results: Forty-two patients were enrolled, with 21 patients randomized to each group. The groups were not significantly different with respect to sex or age. The mean (±SD) LOS in the ED was significantly higher in the procedural sedation group (177.3 ± 37.9 min) than in the US-guided interscalene block group (100.3 ± 28.2 minutes; p < ). The mean (±SD) one-on-one health care provider time was 47.1 (±9.8) minutes for the sedation group and 5 (±0.7) minutes for the US-guided interscalene block group (p < ). There was no statistically significant difference between the two groups in patient satisfaction or pain experienced during the procedure. There were no significant differences between groups with respect to complications such as hypoxia or hypotension (p = 0.49). Conclusions: In this study, patients undergoing shoulder dislocation reduction using US-guided interscalene block spent less time in the ED and required less one-on-one health care provider time compared to those receiving procedural sedation. There was no difference in pain level or satisfaction when compared to procedural sedation patients. ACADEMIC EMERGENCY MEDICINE 2011; 18: ª 2011 by the Society for Academic Emergency Medicine Emergency physicians (EPs) are frequently called on to treat patients who have suffered a shoulder dislocation. Shoulder dislocation is the most common dislocation encountered in the emergency department (ED) population, occurring in 0.5% to 1.7% of individuals. 1,2 Procedural sedation is routinely used in the ED to facilitate shoulder dislocation reduction. Reduction techniques that do not require any sedation From the Department of Emergency Medicine, Northside Hospital-Forsyth (MB), Cuming, GA; the Department of Emergency Medicine, University of Arizona Health Sciences Center (SA), Tucson, AZ; and the Department of Epidemiology, University of Nebraska Medical Center (LL), Omaha, NE. Received November 10, 2010; revision received February 7, 2011; accepted February 16, The authors have no relevant financial information or potential conflicts of interest to disclose. Supervising Editor: Thomas G. Costantino, MD. Address for correspondence and reprints: Michael Blaivas, MD; mike@blaivas.org. ISSN ª 2011 by the Society for Academic Emergency Medicine 922 PII ISSN doi: /j x
2 ACADEMIC EMERGENCY MEDICINE September 2011, Vol. 18, No have been described in the literature and are used sporadically by EPs. More often, some form of sedation is used for muscle relaxation. 3,4 Currently propofol and etomidate are commonly used for procedural sedation, replacing the longer-acting agents such as morphine and midazolam. 5,6 While procedural sedation offers patient comfort and muscle relaxation to facilitate shoulder reduction, there are associated risks. These risks include hypotension, aspiration, and respiratory depression, among others. 7 Such risks are minimized by standard protocols in many EDs that mandate cardiac, blood pressure, oxygen saturation, and end-tidal CO 2 monitoring. 8 However, this requires one-on-one nursing care and may require use of certain critical care or higher-acuity rooms within an ED. Many EDs are not designed with full monitoring equipment and airway support capability in each room and thus patients may have to be moved. Regional nerve anesthesia is frequently used as an adjunct to general anesthesia for shoulder surgery. 9,10 Regional nerve blocks have traditionally been performed blindly and require specialized equipment such as nerve stimulators that are typically not found in the ED. 11 However, ultrasound (US) guidance is becoming an increasingly popular technique to facilitate regional nerve blocks in anesthesia practice. 12,13 Recently, multiple reports have appeared describing the use of US-guided nerve blocks by EPs This may hold significant advantages over procedural sedation in many ED settings. The primary objective of this study was to compare length of stay (LOS) in patients randomized to US-guided interscalene block or procedural sedation to facilitate reduction of shoulder dislocation in the ED. The secondary objectives were to compare one-on-one health care provider time, pain experienced by the patient during reduction, and patient satisfaction between the two groups. METHODS Study Design This was a prospective, randomized study of patients presenting to the ED with shoulder dislocation. The study was approved by the institutional review board with written informed consent obtained from each patient. Study Setting and Population The study was conducted at an academic Level I trauma center ED with an annual census of approximately 80,000. The ED has an emergency medicine residency program and an active US education program. Patients were eligible for the study if they were 18 years of age or older and required reduction of a shoulder dislocation in the ED. We excluded patients if they had known allergy to local anesthetic agents, hemodynamic instability, or respiratory distress or were unable to give consent because of altered mental status. Patients were randomized to either traditional procedural sedation or US-guided interscalene nerve block groups. Randomization was performed using a random number generator. Patients were enrolled on a convenience basis based on researcher availability. Study Protocol Ultrasound-guided interscalene nerve blocks were performed by two EPs credentialed by the hospital to perform bedside US examinations following American College of Emergency Physicians US guidelines. 17 These physicians received specialized training in USguided regional anesthesia from a commercial US course. The education consisted of a 2-hour didactic course focusing on regional anesthesia applications, including the interscalene block, followed by hands-on training. All had at least 2 years of US experience in the ED before the study, and each had performed at least 10 interscalene blocks before the study. Procedural sedation was performed using etomidate as the sole agent, by physicians with hospital credentialing for procedural sedation. All procedural sedation patients received sedation in critical care rooms in the ED. Hemodynamic monitoring included blood pressure, cardiac, and pulse oximetry monitoring. End-tidal CO 2 monitoring was not used in our facility at this time. Following hospital procedures, at least one physician and one nurse were required to be present with the patient during the procedural sedation. A nurse was also required to stay with the patient one on one during the recovery period. Recovery requires the patient being able to converse, drink fluids, and ambulate. One-on-one nursing time was recorded on a hospital procedural sedation form that tracked vital signs and recovery measures in a standard manner. Interscalene blocks were performed using sterile technique and a SonoSite MicroMaxx (SonoSite, Inc., Bothell, WA) with a high-frequency (10 5 MHz) linear array transducer. Neurovascular checks were performed prior to attempting the block to confirm absence of neurologic deficits. A sterile cover was used over the transducer along with sterile US gel. The patient s ipsilateral neck was prepped with Betadine or chlorhexidine prior to the procedure. EPs acquired standard images of the brachial plexus in the interscalene position using a short-axis view of the nerves (Figure 1). Confirmation imaging was performed using anatomical landmarks and power Doppler to verify that targets were not vascular structures. Twenty-one-gauge 1.5-inch noncutting needles were used to deliver regional anesthetic to the brachial plexus (Figure 2). Twenty to 30 ml of anesthetic was injected, enough to envelope the nerve roots on US. The spread of local anesthetic was visualized in real time using US to monitor the hypoechoic signal dispersal around the nerve roots. Lidocaine with epinephrine was chosen over bupivacaine for its shorter duration of action. Block effectiveness was tested 15 minutes after completion of the US-guided nerve block and then in 10-minute intervals after. The physicians performed light touch and pin prick testing in a descending pattern from the shoulder into the arm. When skin anesthesia was present, complete anesthesia was tested with gentle shoulder palpation and then movement. After patients reported complete absence of pain, they were judged ready for the procedure. The physicians did not wait for complete distal anesthesia and paralysis, as in our experience this is not required for shoulder reduction.
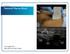
3 924 Blaivas et al. ULTRASOUND-GUIDED INTERSCALENE BLOCK FOR SHOULDER REDUCTION Figure 1. The interscalene location for the brachial plexus is shown on this US image. Arrows identify the heads of the plexus; in this case four separate nerves are seen. US = ultrasound. performed shoulder dislocation reduction. Patients randomized to US-guided interscalene nerve block group were monitored for complications such as hypotension, hypoxia, Horner s syndrome, hoarseness, and diaphragmatic symptoms during their ED stay by the treating EP. Patients randomized to the procedural sedation group were monitored for hypotension and hypoxia by the nurse involved in the patient care. Following the procedure, patients were asked to rate their associated pain using a visual analog scale (VAS; on a scale of 0 to 10, with 0 representing no pain and 10 representing the worst pain). In addition, patients were asked to rate their satisfaction with service provided regarding the orthopedic procedure prior to discharge on a standard 10-point VAS, with 1 representing extremely dissatisfied and 10 extremely satisfied. The pain and satisfaction scores were obtained by researchers prior to patient discharge, when the patients were fully recovered. Data were collected using a standardized data extraction form that included information such as patient demographics, the need for additional analgesia, any adverse reactions, LOS in the ED, nursing time, and time taken to perform US-guided interscalene block. Outcomes Our primary outcome in this study was LOS in the ED. Secondary outcome variables included one-on-one health care provider time, pain experienced by the patient during reduction, and patient satisfaction. LOS was defined as the time between entry into a room in the ED to the time of discharge from ED. One-on-one health care provider time was defined as total time spent by either the nurse or EP monitoring the patient. Data Analysis Categorical variables were evaluated using Fisher s exact test, and continuous variables were analyzed using the Wilcoxon rank sum test. All analyses were performed in SAS Version 9.1 (SAS Institute Inc., Cary, NC). A p value of <0.05 was considered as statistically significant. Sample size was calculated based on prior studies comparing procedural sedation to alternate techniques. Approximately 20 patients in each group was determined to have 90% power at a = 0.05 (twotailed) to detect a 30-minute difference in LOS in the ED. RESULTS Figure 2. A needle (small arrowheads) is shown approaching the brachial plexus (large arrowheads) at the interscalene location. Local anesthetic agent (LA) has started to be injected and envelops some of the nerves. Nursing help was not required while performing the block. ED technicians assisted with shoulder reduction in both groups. The interscalene blocks or procedural sedation were performed by the same EP who Forty-two patients were enrolled, with 21 patients randomized to the procedural sedation group and 21 to the US-guided interscalene block group. US-guided interscalene block was successfully performed in all patients randomized to that group. The reductions in the procedural sedation group were performed by nine different physicians and in the US-guided interscalene nerve block group by seven physicians. The success rate for reduction was 100% in both groups. The patient groups were not significantly different with respect to sex or age. There were six (29%) women in the procedural sedation group and five (24%) in the US-guided interscalene block group (p = 0.99). On average, patients in
4 ACADEMIC EMERGENCY MEDICINE September 2011, Vol. 18, No Table 1 Comparison of Outcome Measures of Two Randomized Groups Procedural Sedation Group (n = 21) US-guided Interscalene Block Group (n = 21) p-value LOS, mean (±SD) (±37.9) (±28.2) < Health care provider 47.1 (±9.8) 5 (±0.7) < one-on-one time, mean (±SD) Patient satisfaction, mean (±SD) 8.2 (±1.3) 8.3 (±1.1) Pain, median (range) 0 (0 4) 0 (0 3) O 2 saturation < 95%, n (%) 2 (10) Hypotension, n (%) 2 (10) Time is reported in minutes. LOS = length of stay; US = ultrasound. the procedural sedation group were 35.9 (±15.1) years old, and patients in the US-guided interscalene block group were 39 (±19.7) years old (p = 0.88; Table 1 ). The mean (±SD) LOS in the ED was significantly higher in the procedural sedation group (177.3 ± 37.9 minutes), compared to in the US-guided interscalene block group (100.3 ± 28.2 minutes; p < ). The one-onone health care provider time was 47.1 (±9.8) minutes on average for the sedation group and 5 (±0.7) minutes for the US-guided interscalene block group (p < ). The patient satisfaction and pain scores were similar for patients in the two groups. Patient satisfaction ranged from 5 to 10 (median, 9) for the procedural sedation and 6 to 10 (median, 8) for the US-guided interscalene block group. The mean (±SD) patient satisfaction scores were 8.2 (±1.3) for the sedation group and 8.3 (±1.1) for the US-guided interscalene block group (p = 0.93). The self-reported pain scores ranged from 0 to 4 (median, 0) for the procedural sedation and 0 to 3 (median, 0) for the US-guided interscalene block group (p = 0.80). There were no significant differences between groups with respect to complications such as hypoxia or hypotension (p = 0.49). No rescue interventions were required during procedural sedation. None of the subjects in the US-guided interscalene block required additional analgesia or sedation while performing shoulder reduction. Transient motor paralysis occurred in all patients who received US-guided interscalene block. The exact duration of the motor paralysis was not recorded. The patients were not followed up after discharge. However, no return ED visits were identified on chart review for persistent residual motor paralysis. None of the patients who received interscalene block developed complications such as Horner s syndrome, hoarseness, or symptoms related to diaphragmatic paralysis. DISCUSSION The requirements for documentation, monitoring, and nurse involvement for procedural sedation have grown significantly over the past two decades in response to increased calls for patient safety and medical treatment monitoring. 18 Preprocedural fasting, continuous hemodynamic monitoring, and observation during postprocedural recovery frequently result in prolonged ED stay. 19 Concurrently, an increasing number of EDs around the country face overcrowding and increasing waiting room times, as well as prolonged ED LOS. 20,21 Procedural sedation requires considerable documentation and close monitoring on the part of any nurse involved. Recent evidence suggests that increasing nursing staff workload contributes to increased LOS in the ED. 22,23 With limited staffing in many busy EDs in the country, removal of one nurse from the number designated to an ED can significantly slow the overall flow. While patient safety cannot be overlooked, it might be helpful to explore safe alternatives such as regional anesthesia to decrease LOS in the ED. There may be additional advantages of regional nerve blockade over procedural sedation. Complications such as respiratory depression and aspiration can potentially be avoided with US-guided regional anesthesia. Due to the lack of nerve stimulation equipment, most EPs historically have not performed regional nerve blocks such as interscalene, axillary, and femoral nerve blocks. With the development of US guidance for regional nerve anesthesia, EPs have been increasingly using US for this purpose The effectiveness of regional nerve anesthesia under US guidance has been well described in the emergency medicine and anesthesia literature The success rates for regional nerve blocks under US guidance have actually been shown to be higher compared to traditional approaches. 32,33 Prior studies using US-guided regional nerve anesthesia have suggested decreased LOS. Although limited by small numbers, Stone et al. 34 showed a marked decrease in LOS for US-guided nerve block patients. Our study also demonstrated decreased LOS in the USguided interscalene block group. Additionally, there was a significant difference in one-on-one health care provider time between two groups. Our data analyses failed to find any significant difference in patient satisfaction, pain scores, or complication rates between the two groups. Our study results indicate the potential benefits of using US-guided regional anesthesia for shoulder dislocation in the ED. Interscalene blocks have been well studied and frequently used in shoulder surgery. Hence, in our study we decided to use interscalene blocks instead of other techniques such as suprascapular block. While not
5 926 Blaivas et al. ULTRASOUND-GUIDED INTERSCALENE BLOCK FOR SHOULDER REDUCTION encountered in our study, the complications from interscalene block include hematoma, nerve penetration, and possible intravascular injection of anesthesia. These complications can be minimized with proper US guidance technique. However, one that is still periodically encountered is involvement of nearby nerves such as the recurrent laryngeal and phrenic nerves. Select patients who may be compromised by transient ipsilateral vocal cord or diaphragm paralysis may need to be counseled or even avoid the procedure altogether. LIMITATIONS Neither participants nor investigators were blinded to interventions. Since the investigators were not blinded to the interventions, it is possible that they assisted with certain components that would have decreased the LOS in the interscalene block group. The total ED LOS might have been influenced by other factors unrelated to the intervention, such as time to being seen by physician, time to obtain an x-ray, and time to finding a special room for procedural sedation. Unfortunately we did not keep track of the reduction technique used, actual time of reduction, and exact time from the beginning of nerve block or procedural sedation until discharge. ED settings vary, and our setting may not be representative of other emergency medicine practice environments. Another limitation of the study is the convenience-sample design, which introduces a selection bias. Patients were enrolled in the study when credentialed EP sonologists were on duty. The information regarding the total number of ED patients with shoulder dislocation during the study period was not available to the study investigators. We did not compare interscalene block to other methods of analgesia such as intraarticular lidocaine. Since patients were not followed-up after the discharge, no information was available regarding long-term complications from the interscalene block. Our study physicians may have more scanning experience compared to an average EP sonologist, which may limit the generalizability of these results. Finally, the relatively small sample size limits the conclusions that can be reached from the study. A future prospective study with a large sample would allow broader generalizations. CONCLUSIONS In this study, patients undergoing shoulder dislocation reduction using ultrasound-guided interscalene block spent less time in the ED and required less one-on-one health care provider time compared to procedural sedation. There was no difference in pain level or satisfaction when compared to procedural sedation patients. The authors thank Dr. Matt Lyon, Medical College of Georgia, for help in conducting this study. References 1. Perron AD, Ingerski MS, Brady WJ, Erling BF, Ullman EA. Acute complications associated with shoulder dislocation at an academic emergency department. J Emerg Med. 2003; 24: Milgrom C, Mann G, Finestone A. A prevalence study of recurrent shoulder dislocations in young adults. J Shoulder Elbow Surg. 1998; 7: Orlinsky M, Shon S, Chiang C, Chan L, Carter P. Comparative study of intra-articular lidocaine and intravenous meperidine diazepam for shoulder dislocations. J Emerg Med. 2002; 22: Matthews DE, Roberts T. Intraarticular lidocaine versus intravenous analgesic for reduction of acute anterior shoulder dislocations. A prospective randomized study. Am J Sports Med. 1995; 23: Burton JH, Bock AJ, Strout TD, Marcolini EG. Etomidate and midazolam for reduction of anterior shoulder dislocation: a randomized, controlled trial. Ann Emerg Med. 2002; 40: Taylor D, O Brien D, Ritchie P, Pasco J, Cameron P. Propofol versus midazolam fentanyl for reduction of anterior shoulder dislocation. Acad Emerg Med. 2004; 12: Roback MG, Wathen JE, Bajaj L, Bothner JP. Adverse events associated with procedural sedation and analgesia in a pediatric emergency department: a comparison of common parenteral drugs. Acad Emerg Med. 2005; 12: Godwin SA, Caro DA, Wolf SJ, et al. American College of Emergency Physicians Clinical policy: procedural sedation and analgesia in the emergency department. Ann Emerg Med. 2005; 45: Borgeat A, Ekatodramis G. Anaesthesia for shoulder surgery. Best Pract Res Clin Anaesthesiol. 2002; 16: Singelyn FJ, Lhotel L, Fabre B. Pain relief after arthroscopic shoulder surgery: a comparison of intraarticular analgesia, suprascapular nerve block, and interscalene brachial plexus block. Anesth Analg. 2004; 99: Urmey WF. Using the nerve stimulator for peripheral or plexus nerve blocks. Minerva Anestesiol. 2006; 72: Davis JJ, Swenson JD, Greis PE, Burks RT, Tashjian RZ. Interscalene block for postoperative analgesia using only ultrasound guidance: the outcome in 200 patients. J Clin Anesth. 2009; 21: Liu SS, Zayas VM, Gordon MA, et al. A prospective, randomized, controlled trial comparing ultrasound versus nerve stimulator guidance for interscalene block for ambulatory shoulder surgery for postoperative neurological symptoms. Anesth Analg. 2009; 109: Blaivas M, Lyon M. Ultrasound-guided interscalene block for shoulder dislocation reduction in the ED. Am J Emerg Med. 2006; 24: Beaudoin FL, Nagdev A, Merchant RC, Becker BM. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med. 2010; 28: Reid N, Stella J, Ryan M, Ragg M. Use of ultrasound to facilitate accurate femoral nerve block in the emergency department. Emerg Med Australas. 2009; 21:
6 ACADEMIC EMERGENCY MEDICINE September 2011, Vol. 18, No American College of Emergency Physicians. Emergency ultrasound guidelines. Ann Emerg Med. 2009; 53: Swoboda TK, Munyak J. Use of a sedation-analgesia datasheet in closed shoulder reductions. J Emerg Med. 2005; 29: Green SM, Krauss B. Pulmonary aspiration risk during emergency department procedural sedation an examination of the role of fasting and sedation depth. Acad Emerg Med. 2002; 9: Horwitz LI, Green J, Bradley EH. US emergency department performance on wait time and length of visit. Ann Emerg Med. 2010; 55: Herring A, Wilper A, Himmelstein DU, et al. Increasing length of stay among adult visits to US emergency departments, Acad Emerg Med. 2009; 16: Robinson KS, Jagim MM, Ray CE. Nursing workforce issues and trends affecting emergency departments. Nurs Manage. 2005; 36: Robinson K. Nursing s perfect storm staff shortages and patient ratios. J Emerg Nurs. 2003; 29: Liebmann O, Price D, Mills C, et al. Feasibility of forearm ultrasonography-guided nerve blocks of the radial, ulnar, and median nerves for hand procedures in the emergency department. Ann Emerg Med. 2006; 48: Wathen JE, Gao D, Merritt G, Georgopoulos G, Battan FK. A randomized controlled trial comparing a fascia iliaca compartment nerve block to a traditional systemic analgesic for femur fractures in a pediatric emergency department. Ann Emerg Med. 2007; 50: Herring A, Price DD, Nagdev A, Simon B. Superior cluneal nerve block for treatment of buttock abscesses in the emergency department. J Emerg Med. 2010; 39: Christiansen TG, Nielsen R. Reduction of shoulder dislocations under interscalene brachial blockade. Arch Orthop Trauma Surg. 1988; 107: Stone MB, Price DD, Wang R. Ultrasound-guided supraclavicular block for the treatment of upper extremity fractures, dislocations, and abscesses in the ED. Am J Emerg Med. 2007; 25: Chan VW. Applying ultrasound imaging to interscalene brachial plexus block. Reg Anesth Pain Med. 2003; 28: Chan VW, Perlas A, Rawson R, Odukoya O. Ultrasound-guided supraclavicular brachial plexus block. Anesth Analg. 2003; 97: De Andres J, Sala-Blanch X. Ultrasound in the practice of brachial plexus anesthesia. Reg Anesth Pain Med. 2002; 27: Williams SR, Chouinard P, Arcand G, et al. Ultrasound guidance speeds execution and improves the quality of supraclavicular block. Anesth Analg. 2003; 97: Kapral S, Greher M, Huber G, et al. Ultrasonographic guidance improves the success rate of interscalene brachial plexus blockade. Reg Anesth Pain Med. 2008; 33: Stone MB, Wang R, Price DD. Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies. Am J Emerg Med. 2008; 26:
Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies
 American Journal of Emergency Medicine (2008) 26, 706 710 www.elsevier.com/locate/ajem Brief Report Ultrasound-guided supraclavicular brachial plexus nerve vs procedural for the treatment of upper extremity
American Journal of Emergency Medicine (2008) 26, 706 710 www.elsevier.com/locate/ajem Brief Report Ultrasound-guided supraclavicular brachial plexus nerve vs procedural for the treatment of upper extremity
Ultrasound-guided nerve blocks in the emergency department
 Full Text Online @ www.onlinejets.org Case Series DOI: 10.4103/0974-2700.58655 Ultrasound-guided nerve blocks in the emergency department Sanjeev Bhoi, Amit Chandra 1, Sagar Galwankar 2 Department of Emergency
Full Text Online @ www.onlinejets.org Case Series DOI: 10.4103/0974-2700.58655 Ultrasound-guided nerve blocks in the emergency department Sanjeev Bhoi, Amit Chandra 1, Sagar Galwankar 2 Department of Emergency
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
Interscalene brachial plexus blockade - indications, anatomy, practical performance
 08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
Ultrasound in Emergency Medicine
 doi:10.1016/j.jemermed.2012.01.050 The Journal of Emergency Medicine, Vol. 43, No. 4, pp. 692 697, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$ - see front matter
doi:10.1016/j.jemermed.2012.01.050 The Journal of Emergency Medicine, Vol. 43, No. 4, pp. 692 697, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$ - see front matter
S Kannan, Prem Kumar. Assistant Professor, Saveetha Medical College and Hospital, Chennai.
 Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
Investigation performed at the University of Rochester, Department of Orthopaedics and Rehabilitation, Rochester, NY USA
 Intra-articular cocktail offers clinical advantages over femoral nerve block for postoperative analgesia in patients undergoing arthroscopic hip surgery Sean Childs, MD; Sonia Pyne, MD; Kiritpaul Nandra,
Intra-articular cocktail offers clinical advantages over femoral nerve block for postoperative analgesia in patients undergoing arthroscopic hip surgery Sean Childs, MD; Sonia Pyne, MD; Kiritpaul Nandra,
CHAPTER 5 Femoral Nerve Block. Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS
 CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
Comparison of Procedural Sedation for the Reduction of Dislocated Total Hip Arthroplasty
 ORIGINAL RESEARCH for the Reduction of Dislocated Total Hip Arthroplasty Jonathan E. dela Cruz, MD* Donald N. Sullivan, MD Eric Varboncouer, MD Joseph C. Milbrandt, PhD* Myto Duong, MD * Scott Burdette,
ORIGINAL RESEARCH for the Reduction of Dislocated Total Hip Arthroplasty Jonathan E. dela Cruz, MD* Donald N. Sullivan, MD Eric Varboncouer, MD Joseph C. Milbrandt, PhD* Myto Duong, MD * Scott Burdette,
A Staged Approach to Analgesia After Hip Arthroscopy Using Multimodal Analgesia & Elective Ultrasound Guided Fascia Iliaca Block
 A Staged Approach to Analgesia After Hip Arthroscopy Using Multimodal Analgesia & Elective Ultrasound Guided Fascia Iliaca Block James T. Beckmann MD Stephen K. Aoki MD Stephen Guyette MD Jeffrey Swenson
A Staged Approach to Analgesia After Hip Arthroscopy Using Multimodal Analgesia & Elective Ultrasound Guided Fascia Iliaca Block James T. Beckmann MD Stephen K. Aoki MD Stephen Guyette MD Jeffrey Swenson
Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach
 American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Andrew B. Wolff, MD a Geoffrey Hogan, BA a James Capon, BS, MS a Hayden Smith, BA a Alexandra Napoli, BS a Patrick Gaspar, MD b
 Pre-operative Lumbar Plexus Block Provides Superior Post-operative Analgesia when compared with Fascia Iliaca Block or General Anesthesia alone in Hip Arthroscopy Andrew B. Wolff, MD a Geoffrey Hogan,
Pre-operative Lumbar Plexus Block Provides Superior Post-operative Analgesia when compared with Fascia Iliaca Block or General Anesthesia alone in Hip Arthroscopy Andrew B. Wolff, MD a Geoffrey Hogan,
British Journal of Anaesthesia 101 (4): (2008) doi: /bja/aen229 Advance Access publication August 4, 2008
 British Journal of Anaesthesia 11 (4): 49 6 (28) doi:1.193/bja/aen229 Advance Access publication August 4, 28 REGIONAL ANAESTHESIA Effect of local anaesthetic volume (2 vs ml) on the efficacy and respiratory
British Journal of Anaesthesia 11 (4): 49 6 (28) doi:1.193/bja/aen229 Advance Access publication August 4, 28 REGIONAL ANAESTHESIA Effect of local anaesthetic volume (2 vs ml) on the efficacy and respiratory
ULTRASOUND GUIDED NERVE BLOCKS
 2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
Sign up to receive ATOTW weekly
 PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length
 ABSTRACT NUMBER: 020-0094 ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length of Stay AUTHORS: Mark J. Lenart, MD Vanderbilt University 1301 Medical Center Drive Nashville,
ABSTRACT NUMBER: 020-0094 ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length of Stay AUTHORS: Mark J. Lenart, MD Vanderbilt University 1301 Medical Center Drive Nashville,
An evaluation of brachial plexus block using a nerve stimulator versus ultrasound guidance: A randomized controlled trial
 Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator Guided and Ultrasound Guided.
 DOI: 10.21276/aimdr.2016.2.3.16 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator
DOI: 10.21276/aimdr.2016.2.3.16 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 A Comparative Evaluation of Techniques in Interscalene Brachial Plexus Block: Conventional blind, Nerve Stimulator
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder
 Upper limb Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder A DOUBLE-BLIND, RANDOMISED CONTROLLED TRIAL J. Kean, C. A. Wigderowitz,
Upper limb Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder A DOUBLE-BLIND, RANDOMISED CONTROLLED TRIAL J. Kean, C. A. Wigderowitz,
Comparison Of 0.5%Bupivacaine And 0.5% Bupivacaine Plus Buprenorphine in Brachial Plexus Block
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
ULTRASOUND-GUIDED peripheral
 392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
Ultrasound-guided reduction of distal radius fractures
 American Journal of Emergency Medicine (2010) 28, 1002 1008 www.elsevier.com/locate/ajem Original Contribution Ultrasound-guided reduction of distal radius fractures Shiang-Hu Ang, Shu-Woan Lee, Kai-Yet
American Journal of Emergency Medicine (2010) 28, 1002 1008 www.elsevier.com/locate/ajem Original Contribution Ultrasound-guided reduction of distal radius fractures Shiang-Hu Ang, Shu-Woan Lee, Kai-Yet
Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique
 Cronicon OPEN ACCESS ANAESTHESIA Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique Amna 1 *, Saira Mehboob 2, Waqas Alam 3, Amna Gulraze 4
Cronicon OPEN ACCESS ANAESTHESIA Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique Amna 1 *, Saira Mehboob 2, Waqas Alam 3, Amna Gulraze 4
Oral versus Intravenous Opioid Dosing for the Initial Treatment of Acute Musculoskeletal Pain in the Emergency Department
 CLINICAL INVESTIGATION Oral versus Intravenous Opioid Dosing for the Initial Treatment of Acute Musculoskeletal Pain in the Emergency Department James R. Miner, MD, Johanna Moore, MD, Richard O. Gray,
CLINICAL INVESTIGATION Oral versus Intravenous Opioid Dosing for the Initial Treatment of Acute Musculoskeletal Pain in the Emergency Department James R. Miner, MD, Johanna Moore, MD, Richard O. Gray,
DORIS DUKE MEDICAL STUDENTS JOURNAL Volume V,
 Continuous Femoral Perineural Infusion (CFPI) Using Ropivacaine after Total Knee Arthroplasty and its Effect on Postoperative Pain and Early Functional Outcomes Eric Lloyd Scientific abstract Total Knee
Continuous Femoral Perineural Infusion (CFPI) Using Ropivacaine after Total Knee Arthroplasty and its Effect on Postoperative Pain and Early Functional Outcomes Eric Lloyd Scientific abstract Total Knee
Is There an Ideal Regimen for CPNB?
 Is There an Ideal Regimen for CPNB? Dr Eric Albrecht, MD, DESA Department of Anesthesiology, CHUV 2nd SARA Annual Symposium June 2013 Manuel pratique d ALR échoguidé, Elsevier Masson, Paris, 2013 Albrecht
Is There an Ideal Regimen for CPNB? Dr Eric Albrecht, MD, DESA Department of Anesthesiology, CHUV 2nd SARA Annual Symposium June 2013 Manuel pratique d ALR échoguidé, Elsevier Masson, Paris, 2013 Albrecht
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven
 Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
British Journal of Anaesthesia 103 (3): (2009) doi: /bja/aep173 Advance Access publication July 8, 2009
 REGIONAL ANAESTHESIA Comparison of economical aspects of interscalene brachial plexus blockade and general anaesthesia for arthroscopic shoulder surgery C. Gonano, S. C. Kettner, M. Ernstbrunner, K. Schebesta,
REGIONAL ANAESTHESIA Comparison of economical aspects of interscalene brachial plexus blockade and general anaesthesia for arthroscopic shoulder surgery C. Gonano, S. C. Kettner, M. Ernstbrunner, K. Schebesta,
Objectives. Conflict of Interest Disclosure. Neuraxial and Regional Anesthesia in the Pediatric Population
 Neuraxial and Regional Anesthesia in the Pediatric Population Lauren Renner, MS, RN-BC, PNP Sharon Wrona, DNP, RN-BC, PNP, PMHS, AP- PMN.... Conflict of Interest Disclosure Conflicts of Interest for ALL
Neuraxial and Regional Anesthesia in the Pediatric Population Lauren Renner, MS, RN-BC, PNP Sharon Wrona, DNP, RN-BC, PNP, PMHS, AP- PMN.... Conflict of Interest Disclosure Conflicts of Interest for ALL
Acute Pain and Peripheral nerve block in Emergency Department.
 III. Pan-Arab Pain Congress/ VIII.National Congress of SAETD. Algiers. 3-5.October.2012. Acute Pain and Peripheral nerve block in Emergency Department. Dr A.Tirichine. Z.Djili. A.Benbouzid. Unit of Anesthesiology
III. Pan-Arab Pain Congress/ VIII.National Congress of SAETD. Algiers. 3-5.October.2012. Acute Pain and Peripheral nerve block in Emergency Department. Dr A.Tirichine. Z.Djili. A.Benbouzid. Unit of Anesthesiology
Comparison of Intra-Articular Lidocaine and Intravenous Sedation for Reduction of Shoulder Dislocations A RANDOMIZED, PROSPECTIVE STUDY
 2135 COPYRIGHT 2002 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Comparison of Intra-Articular Lidocaine and Intravenous Sedation for Reduction of Shoulder Dislocations A RANDOMIZED, PROSPECTIVE
2135 COPYRIGHT 2002 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Comparison of Intra-Articular Lidocaine and Intravenous Sedation for Reduction of Shoulder Dislocations A RANDOMIZED, PROSPECTIVE
The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care settings,
 American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
Regional Anaesthesia: Minimizing risk and complications. Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh
 Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Peripheral Nerve Blocks
 Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Original Article INTRODUCTION. Abstract
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/147 Comparing Two Different Doses of Clonidine as an Adjuvant to Bupivacaine in Blind Fascia Iliaca Compartment Block
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/147 Comparing Two Different Doses of Clonidine as an Adjuvant to Bupivacaine in Blind Fascia Iliaca Compartment Block
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Original contribution. Department of Anesthesiology, Sapporo Medical University, School of Medicine, Sapporo, Hokkaido, Japan
 Journal of Clinical Anesthesia (2007) 19, 25 29 Original contribution A comparison of spinal anesthesia with small-dose lidocaine and general anesthesia with fentanyl and propofol for ambulatory prostate
Journal of Clinical Anesthesia (2007) 19, 25 29 Original contribution A comparison of spinal anesthesia with small-dose lidocaine and general anesthesia with fentanyl and propofol for ambulatory prostate
Australian and New Zealand Registry of Regional Anaesthesia (AURORA)
 Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
Ultrasound-guided regional anesthesia for the pain management of elderly patients with hip fractures in the emergency department
 Clin Exp Emerg Med 214;1(1):49-55 http://dx.doi.org/1.15441/ceem.14.8 Ultrasound-guided regional anesthesia for the pain management of elderly patients with hip fractures in the emergency department Hee
Clin Exp Emerg Med 214;1(1):49-55 http://dx.doi.org/1.15441/ceem.14.8 Ultrasound-guided regional anesthesia for the pain management of elderly patients with hip fractures in the emergency department Hee
Ultrasound in Peripheral Nerve Interventions
 Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal fossa
 British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation
 Original Article Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation 125 Elnaz Vahidi, Rezvan Hemati, Mehdi Momeni, Amirhossein Jahanshir, Morteza Saeedi
Original Article Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation 125 Elnaz Vahidi, Rezvan Hemati, Mehdi Momeni, Amirhossein Jahanshir, Morteza Saeedi
Pre-operative Care For Surgery of Forearm Fracture. WONG Mei Chee OT (CMC)
 Pre-operative Care For Surgery of Forearm Fracture WONG Mei Chee OT (CMC) Pre-operative Nursing Considerations for Surgery of Forearm Fracture 1. Patient s problems - Diagnosis: Clinical features, x-ray
Pre-operative Care For Surgery of Forearm Fracture WONG Mei Chee OT (CMC) Pre-operative Nursing Considerations for Surgery of Forearm Fracture 1. Patient s problems - Diagnosis: Clinical features, x-ray
Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report
 Rev Bras Anestesiol 2012; 62: 5: 741-747 CLINICAL INFORMATION CLINICAL INFORMATION Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report Beatriz L. S. Mandim 1, Rodrigo R. Alves 2,
Rev Bras Anestesiol 2012; 62: 5: 741-747 CLINICAL INFORMATION CLINICAL INFORMATION Pneumothorax Post Brachial Plexus Block Guided by Ultrasound: a Case Report Beatriz L. S. Mandim 1, Rodrigo R. Alves 2,
British Journal of Anaesthesia 98 (6): (2007) doi: /bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultr
 British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
Table-2: Fastrack Criteria-According to White and Song
 Interscalene Brachial Plexus Block for Hydrodilatation with Normal Saline in Patients of Frozen Shoulder Divya Srivastav, Anup Chandani, 3 JC Vasava & Assistant Professor, 3 Professor, GMERS, Medical College
Interscalene Brachial Plexus Block for Hydrodilatation with Normal Saline in Patients of Frozen Shoulder Divya Srivastav, Anup Chandani, 3 JC Vasava & Assistant Professor, 3 Professor, GMERS, Medical College
CREDENTIALING AND PRIVILEGING FOR ULTRASOUND GUIDED REGIONAL ANAESTHESIA
 CREDENTIALING AND PRIVILEGING FOR ULTRASOUND GUIDED REGIONAL ANAESTHESIA With regards to Credentialing and Privileging, The American Society of Regional Anaesthesia (ASRA) and the European Society of Regional
CREDENTIALING AND PRIVILEGING FOR ULTRASOUND GUIDED REGIONAL ANAESTHESIA With regards to Credentialing and Privileging, The American Society of Regional Anaesthesia (ASRA) and the European Society of Regional
Objectives 9/7/2012. Optimizing Analgesia to Enhance the Recovery After Surgery CME FACULTY DISCLOSURE
 Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
USRA OF THE LOWER EXTREMITY
 USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Effect of Ondansetron on the Incidence of Vomiting Associated With Ketamine Sedation in Children: A Double-Blind, Randomized, Placebo-Controlled Trial
 PEDIATRICS/ORIGINAL RESEARCH Effect of Ondansetron on the Incidence of Vomiting Associated With Ketamine Sedation in Children: A Double-Blind, Randomized, Placebo-Controlled Trial William T. Langston,
PEDIATRICS/ORIGINAL RESEARCH Effect of Ondansetron on the Incidence of Vomiting Associated With Ketamine Sedation in Children: A Double-Blind, Randomized, Placebo-Controlled Trial William T. Langston,
Ultrasound-guided oblique approach for peripheral venous access in a phantom model
 Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 Performance Accuracy of Hand-on-needle versus Hand-on-syringe Technique for Ultrasound-guided Regional Anesthesia Simulation for Emergency Medicine Residents The Harvard community has made this article
Performance Accuracy of Hand-on-needle versus Hand-on-syringe Technique for Ultrasound-guided Regional Anesthesia Simulation for Emergency Medicine Residents The Harvard community has made this article
Interscalene Anesthesia for Shoulder Arthroscopy in a Community-Sized Military Hospital
 Interscalene Anesthesia for Shoulder Arthroscopy in a Community-Sized Military Hospital LTC Robert A. Arciero, M.D., MAJ Dean C. Taylor, M.D., 2LT Steven A. Harrison, B.A., LTC Robert J. Snyder, M.D.,
Interscalene Anesthesia for Shoulder Arthroscopy in a Community-Sized Military Hospital LTC Robert A. Arciero, M.D., MAJ Dean C. Taylor, M.D., 2LT Steven A. Harrison, B.A., LTC Robert J. Snyder, M.D.,
Case Report Unique Phrenic Nerve-Sparing Regional Anesthetic Technique for Pain Management after Shoulder Surgery
 Hindawi Case Reports in Anesthesiology Volume 2017, Article ID 1294913, 4 pages https://doi.org/10.1155/2017/1294913 Case Report Unique Phrenic Nerve-Sparing Regional Anesthetic Technique for Pain Management
Hindawi Case Reports in Anesthesiology Volume 2017, Article ID 1294913, 4 pages https://doi.org/10.1155/2017/1294913 Case Report Unique Phrenic Nerve-Sparing Regional Anesthetic Technique for Pain Management
Regional Anesthesia. procedure if required. However, many patients prefer to receive sedation either during the
 1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
Bird M : Acute Pain Management: A New Area of Liability for Anesthesiologist. ASA Newsletter 71(8), 2007.
 Citation Bird M : Acute Pain Management: A New Area of Liability for Anesthesiologist. ASA Newsletter 71(8), 2007. Full Text A 71-year-old obese female smoker with hypertension and diabetes underwent a
Citation Bird M : Acute Pain Management: A New Area of Liability for Anesthesiologist. ASA Newsletter 71(8), 2007. Full Text A 71-year-old obese female smoker with hypertension and diabetes underwent a
BJA Advance Access published January 26, British Journal of Anaesthesia Page 1 of 10 doi: /bja/aen384
 BJA Advance Access published January 26, 2009 British Journal of Anaesthesia Page 1 of 10 doi:10.1093/bja/aen384 Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block:
BJA Advance Access published January 26, 2009 British Journal of Anaesthesia Page 1 of 10 doi:10.1093/bja/aen384 Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block:
PERIPHERAL REGIONAL BLOCKS. by Mike DeBroeck, DNP, CRNA
 PERIPHERAL REGIONAL BLOCKS by Mike DeBroeck, DNP, CRNA Why am I bothering with this topic at all? Do CRNAs REALLY even do peripheral regional anesthetics? YES!!!!!!! TOPICS GENERAL INFO SUCCESS RATES
PERIPHERAL REGIONAL BLOCKS by Mike DeBroeck, DNP, CRNA Why am I bothering with this topic at all? Do CRNAs REALLY even do peripheral regional anesthetics? YES!!!!!!! TOPICS GENERAL INFO SUCCESS RATES
The use of Pudendal Nerve Block in Hemorrhoidectomy Operations: A Prospective Double Blind Placebo Control Study
 Kasr El Aini Journal of Surgery VOL., 10, NO 3 September 2009 97 The use of Pudendal Nerve Block in Hemorrhoidectomy Operations: A Prospective Double Blind Placebo Control Study Sherif Adly and Mohamed
Kasr El Aini Journal of Surgery VOL., 10, NO 3 September 2009 97 The use of Pudendal Nerve Block in Hemorrhoidectomy Operations: A Prospective Double Blind Placebo Control Study Sherif Adly and Mohamed
Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block
 Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement
 AIRWAY/BRIEF RESEARCH REPORT Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement Sandra L. Werner, MD, RDMS Charles E. Smith, MD Jessica R. Goldstein, MD Robert
AIRWAY/BRIEF RESEARCH REPORT Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement Sandra L. Werner, MD, RDMS Charles E. Smith, MD Jessica R. Goldstein, MD Robert
The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia
 The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia This study has been published: The intensity of preoperative pain is directly correlated
The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia This study has been published: The intensity of preoperative pain is directly correlated
Procedural Sedation. Conscious Sedation AAP Sedation Guidelines: Disclosures. What does it mean for my practice? We have no disclosures
 2016 AAP Sedation Guidelines: What does it mean for my practice? Amber P. Rogers MD FAAP Assistant Professor of Section of Hospital Medicine and Anesthesiology Corrie E. Chumpitazi MD FAAP FACEP Assistant
2016 AAP Sedation Guidelines: What does it mean for my practice? Amber P. Rogers MD FAAP Assistant Professor of Section of Hospital Medicine and Anesthesiology Corrie E. Chumpitazi MD FAAP FACEP Assistant
Prevention and Treatment Patrick Levelle, MD
 Prevention and Treatment Patrick Levelle, MD LOCAL ANESTHETIC TOXICITY 1. PERIPHERAL NERVE BLOCKS 2. ROLE OF THE PERIANESTHESIA RN 3. LOCAL ANESTHETIC TOXICITY Use of Lipid Emulsion Regional and Peripheral
Prevention and Treatment Patrick Levelle, MD LOCAL ANESTHETIC TOXICITY 1. PERIPHERAL NERVE BLOCKS 2. ROLE OF THE PERIANESTHESIA RN 3. LOCAL ANESTHETIC TOXICITY Use of Lipid Emulsion Regional and Peripheral
Comparison of analgesic properties of perineural and systemic dexamethasone in patients undergoing upper limb surgeries under supraclavicular block
 Original Research Article Comparison of analgesic properties of perineural and systemic dexamethasone in patients undergoing upper limb surgeries under supraclavicular block Sathyan Natarajan 1*, Karthikeyan
Original Research Article Comparison of analgesic properties of perineural and systemic dexamethasone in patients undergoing upper limb surgeries under supraclavicular block Sathyan Natarajan 1*, Karthikeyan
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR
 GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES
 ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
Peripheral regional anaesthesia and outcome: lessons learned from the last 10 years
 British Journal of Anaesthesia 114 (5): 728 45 (2015) Advance Access publication 17 February 2015. doi:10.1093/bja/aeu559 REVIEW ARTICLES Peripheral regional anaesthesia and outcome: lessons learned from
British Journal of Anaesthesia 114 (5): 728 45 (2015) Advance Access publication 17 February 2015. doi:10.1093/bja/aeu559 REVIEW ARTICLES Peripheral regional anaesthesia and outcome: lessons learned from
An unusual shoulder injury
 An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (1), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (1), Page 5736-5742 Supraclavicular Brachial Plexus Nerve Block versus Patient Controlled Analgesia for Post-Operative Pain Management in
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (1), Page 5736-5742 Supraclavicular Brachial Plexus Nerve Block versus Patient Controlled Analgesia for Post-Operative Pain Management in
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Regional Anaesthesia for Children
 Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun
 Comparison of Postoperative Pain Control Methods After Bony Surgery In the Foot And Ankle Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun Department of Orthopedic Surgery, College of Medicine,
Comparison of Postoperative Pain Control Methods After Bony Surgery In the Foot And Ankle Gi-Soo Lee, Chan Kang*, You Gun Won, Byung-Hak Oh, June-Bum Jun Department of Orthopedic Surgery, College of Medicine,
Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries
 Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Emergency Department Guideline. Procedural Sedation and Analgesia Policy for the Registered Nurse
 Emergency Department Guideline Purpose: To ensure safe, consistent patient monitoring and documentation standards when procedure related sedation and analgesia is indicated. Definitions: Minimal Sedation
Emergency Department Guideline Purpose: To ensure safe, consistent patient monitoring and documentation standards when procedure related sedation and analgesia is indicated. Definitions: Minimal Sedation
REGIONAL/LOCAL ANESTHESIA and OBESITY
 REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
Preprocedural Fasting and Adverse Events in Procedural Sedation and Analgesia in a Pediatric Emergency Department: Are They Related?
 PEDIATRICS/ORIGINAL RESEARCH Preprocedural Fasting and Adverse Events in Procedural Sedation and Analgesia in a Pediatric Emergency Department: Are They Related? Mark G. Roback, MD Lalit Bajaj, MD, MPH
PEDIATRICS/ORIGINAL RESEARCH Preprocedural Fasting and Adverse Events in Procedural Sedation and Analgesia in a Pediatric Emergency Department: Are They Related? Mark G. Roback, MD Lalit Bajaj, MD, MPH
Peripheral intravenous (IV) access is often a vital
 What You See (Sonographically) Is What You Get: Vein and Patient Characteristics Associated With Successful Ultrasound-guided Peripheral Intravenous Placement in Patients With Difficult Access Nova L.
What You See (Sonographically) Is What You Get: Vein and Patient Characteristics Associated With Successful Ultrasound-guided Peripheral Intravenous Placement in Patients With Difficult Access Nova L.
Better Post-Op Pain Control Starts Here
 Better Post-Op Pain Control Starts Here POST-OP PAIN CONTROL PUMP It s Easy to Get Started About the ACCUFUSER Pump Thank you for considering the This brochure makes it easy for For complete information
Better Post-Op Pain Control Starts Here POST-OP PAIN CONTROL PUMP It s Easy to Get Started About the ACCUFUSER Pump Thank you for considering the This brochure makes it easy for For complete information
Fascia Iliaca Compartment Block. Angela Stewart ANP 10/11/17
 Fascia Iliaca Compartment Block Angela Stewart ANP 10/11/17 1 Driving force Dr J. Mitchell from acute pain service Ayr hospital produced a comprehensive guideline to authorise Non-medical prescribers (NMP)
Fascia Iliaca Compartment Block Angela Stewart ANP 10/11/17 1 Driving force Dr J. Mitchell from acute pain service Ayr hospital produced a comprehensive guideline to authorise Non-medical prescribers (NMP)
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative
 Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)
![(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune) (Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)](/thumbs/82/85649280.jpg) IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
Fascia Iliaca Compartment Block. Angela Stewart ANP 22/08/17
 Fascia Iliaca Compartment Block Angela Stewart ANP 22/08/17 Motivation Anaesthetist Dr Joellene Mitchell from acute pain service Ayr hospital produced a guideline to allow Non-medical prescribers (NMP)
Fascia Iliaca Compartment Block Angela Stewart ANP 22/08/17 Motivation Anaesthetist Dr Joellene Mitchell from acute pain service Ayr hospital produced a guideline to allow Non-medical prescribers (NMP)
Ultrasound Guided Peripheral Intravenous Access
 Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
