Copyright r 2015 Annals of Pediatric Surgery. Unauthorized reproduction of this article is prohibited.
|
|
|
- Aldous Hill
- 5 years ago
- Views:
Transcription
1 Original article 231 Transperitoneal laparoscopic pyeloplasty in children and adolescents: long-term results Abdelbaset A.E. Elemam a, Rafik Shalaby b, Magid Ismail b, Mohamad Shahen b, Refaat Ibrahim b and Ibrahim Gamaan b Background Open pyeloplasty has been the gold standard for the treatment of ureteropelvic junction obstruction (UPJO) in children and young adolescents. However, the use of laparoscopy for the treatment of pyeloplasty is increasing as it has the potential to provide a better and more desirable cosmetic outcome in addition to less postoperative pain and decreased recovery time. The aim of this study was to evaluate the long-term outcome of transperitoneal laparoscopic pyeloplasty (TLP) for the treatment of UPJO in children and young adolescents. Patients and methods Twenty-nine patients with UPJO with 32 renal units were subjected to TLP at Al-Azhar University Hospitals, Egypt, during the period from May 2008 to December The outcome measurements of this study included operative time, internal stent placement, hospital stay, intraoperative complications, and success rates. Success is defined as both symptomatic relief and radiographic resolution of hydronephrosis at the last follow-up. Patients were followed up with intravenous urography and diethylene triamine penta-acetic acid scan at 3, 6, and 12 months regularly for both functional and morphological outcomes. Results The study included 29 patients (12 male and 17 female) with 32 obstructed renal units. The mean age was 4.23 ± 2.1 years (range 3 16 years). All procedures were completed laparoscopically without conversion. The mean operative time was ± 23 min (range min). The mean postoperative hospital stay was 4.1 days (range 3 8 days). All patients achieved full recovery without any complications. The mean follow-up period of the patients was ± 5.18 months (range months). Success rate was 96.9%. Only one case developed recurrent UPJO and was treated with retrograde endopyelotomy and stenting. Conclusion TLP has the advantages of less postoperative pain, short hospital stay, and rapid recovery, with excellent functional and cosmetic outcomes. However, it requires advanced skill level for intracorporeal suturing and knot tying. Ann Pediatr Surg 11: c 2015 Annals of Pediatric Surgery. Annals of Pediatric Surgery 2015, 11: Keywords: children, laparoscopy, long-term results, pyeloplasty, ureteropelvic junction obstruction Departments of a Urology and b Pediatric Surgery, Al-Azhar University Hospitals, Cairo, Egypt Correspondence to Rafik Shalaby, MD, Al-Hussain University Hospital, Darrasa, Cairo 11837, Egypt Tel: , ; fax: ; rafikshalaby@hotmail.com Received 26 March 2015 accepted 15 July 2015 Introduction Ureteropelvic junction obstruction (UPJO) is the most common cause of pediatric hydronephrosis, occurring in one per newborns. The widespread use of antenatal ultrasonography and the advent of modern imaging techniques have resulted in earlier and more common diagnosis of hydronephrosis [1]. Open pyeloplasty originally described by Andersen and Hynes remains the gold standard treatment for UPJO. Over the last two decades, many new approaches for the treatment of UPJO have been evolved, from open pyeloplasty to various minimally invasive procedures such as endopyelotomy, acucise catheter incision, balloon dilatation laparoscopic and robotic pyeloplasty. These minimally invasive options were reported to be less successful compared with open pyeloplasty [2]. The first study on transperitoneal laparoscopic pyeloplasty (TLP) was conducted by Shoma et al. [3]. Laparoscopic pyeloplasty is the first minimally invasive option to match the success rate of open pyeloplasty. Laparoscopic pyeloplasty can be performed using either retroperitoneal or transperitoneal approach. The transperitoneal approach offers familiar anatomic landmarks and wide working space, but more bowel manipulation, and therefore higher likelihood of ileus. Conversely, the retroperitoneal approach offers the advantage of less potential postoperative ileus, but it has the disadvantage of limited working space. Choice of anatomic approach is dictated by surgeon experience and training [4]. The laparoscopic approach has the advantages of having less postoperative pain, shorter hospital stay, and more rapid recovery, with better cosmetic results compared with open pyeloplasty. Moreover, laparoscopy allows for excision of the structured segment, reduction pyeloplasty, transposition of the ureteropelvic junction (UPJ) over crossing vessels, and even extraction of concomitant renal calculi [5]. There is much debate about the outcomes of TLP concerning the functional recovery of renal units after repair. Although some authors reported significant functional improvement after TLP [2,5 7], others found no or slight improvement after TLP [8 10]. The aim of this study was to evaluate the long-term outcome of TLP for the treatment of UPJO in children and young adolescents. Patients and methods This study was conducted at the Department of Urology and Pediatric Surgery, Al-Azhar University Hospitals, Egypt, between May 2008 and December A total c 2015 Annals of Pediatric Surgery DOI: /01.XPS c
2 232 Annals of Pediatric Surgery 2015, Vol 11 No 4 of 29 patients with 32 renal units were subjected to TLP. All patients were evaluated by means of full history taking, thorough clinical examination, routine laboratory investigations (complete blood count, bleeding time, clotting time, random blood sugar, and liver and renal profile), and imaging workup, which included renal ultrasound, magnetic resonance urography, intravenous urography (IVU), and diuretic renography. Diethylene triamine penta-acetic acid scan was performed to evaluate drainage, glomerular filtration rate (GFR), and split renal function. Inclusion criteria included patients with pelvi-ureteric junction obstruction, whereas exclusion criteria included untreated coagulopathy, active urinary tract infection, intrarenal pelvis, previous pyeloplasty, or previous endopyelotomy. Ethical committee of our hospitals approved the study protocol, and written informed parental consent was obtained. All patients were admitted in the early morning on the day of surgery and a prophylactic intravenous antibiotic in the form of third-generation cephalosporin at a dose of 50 mg/kg body weight was given 1 h before the procedure. After induction of general anesthesia and fixation of nasogastric tube and Foley s urethral catheter, the patient was placed in the lateral kidney position, whereas patients with ectopic kidneys were placed in the supine position. The surgeon and the cameraman were on the contralateral side with the TV monitor in front of them. A 5-mm port was inserted through the umbilicus using open Hasson s technique and creation of pneumoperitoneum to a pressure of mmhg was accomplished. A 5-mm telescope with 301 was used. Two 5-mm working ports, one subcostal in the midclavicular line and the other just anterior to the anterior superior iliac spine under vision. The colon was reflected medially, and the dilated renal pelvis and upper ureter were identified and dissected free from the surrounding tissues. The crossing vessel was identified and, if present, adequate care was taken to separate it safely from the renal pelvis for transposition. Laparoscopic dismembered pyeloplasty was performed for all cases. The ureter was cut at UPJ; the narrow segment was excised with spatulation of the upper ureter. (Figs 1 and 2) To minimize operative time, redundant renal pelvis was transcutaneously fixed to the anterior abdominal wall with prolene 2/0 for retraction and sparing a trocar. Extraction of multiple concomitant calyceal stones from ectopic kidney was carried out by introduction of the ureteroscope from the operating trocar sheath. The anastomosis was performed with continuous intracorporeal suture using 4-0 vicryl suture. The first suture was placed at the apex of the spatulated ureter from outside in, and then taken through the most distal part of the pelvis. The posterior anastomosis was completed running up the length of the spatulated ureter and pelvis. A double-j stent (4.8 Fr, 18 cm) was mounted on the guidewire and passed through the proximal ureter into the bladder. The upper coil of the double-j stent was left within the renal pelvis. In cases of aberrant vessels the anastomosis was brought anterior to the vessels. Drain was inserted adjacent to the site of repair (Figs 3 and 4). Foley s catheter was removed after 24 h and the tube drain was removed when it ceased output. Internal stent was removed by means of cystoscopy after 6 weeks. Patients were followed up with IVU, magnetic resonance urography, and diethylene triamine penta-acetic acid scan, for both functional and morphological outcome at 3, 6, and 12 months. Success was defined as both symptomatic relief and radiographic resolution of obstruction at last follow-up. Statistics analysis Data were collected and processed using SPSS, version 18 (SPSS Inc., Chicago, Illinois, USA). P-values less than 0.05 were considered statistically significant. Results This study included 29 patients with a mean age of 4.23 ± 2.1 years (range 3 16 years). There were 12 male and 17 female patients with 32 obstructed renal units at UPJ (three bilateral). Thirteen patients had right-sided UPJO, 13 had left-sided UPJO, and three had bilateral UPJO. The most common presentation was loin pain (25 cases), whereas two patients presented with hematuria and two patients were accidently discovered. Twenty-six patients had unilateral UPJO (four out of them had a congenital ectopic kidneys). All cases were completed laparoscopically without any conversion. Aberrant vessels were detected in six patients. Concomitant multiple renal stones were found in one case. The mean operative time was ± 22.6 (range ) (Table 1). All patients were given diclofenac sodium to control postoperative pain. The mean postoperative hospital stay was 4.1 ± 1.5 days (range 3 8 days). Tube drains were removed on the third postoperative day when drainage had stopped, with a mean of 3.4 ± 1.2 days (range 2 8 days). One patient developed postoperative fever and was managed conservatively with proper antibiotics. The mean duration of stenting was 5.8 ± 2.11 weeks (range 6 10 weeks). The mean follow-up of the patients was ± 5.18 months (range months). There was one case of recurrence UPJO giving a success rate of 96.9%. Two (6.9%) patients had persistent urine leakage after TLP and were managed conservatively and the leakage stopped after 2 weeks (Table 2). One of them improved without further intervention, whereas the other patient developed recurrent UPJO, which was managed with double-j fixation first and then with retrograde endopyelotomy after 1 year. Postoperative evaluation was carried out with abdominal ultrasound; IVU and renal scan were performed 3 8 months later. In all patients there was significant improvement in UPJO with improved renal functions and reduction in the size of renal pelvis (Figs 3 and 4). Comparative analysis of preoperative and postoperative
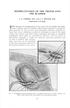
3 Transperitoneal laparoscopic pyeloplasty Elemam et al. 233 Fig. 1 Identification of the dilated renal pelvis and the upper ureter (a). Excision of the dilated renal pelvis with the atretic ureteral segment (b d). IVU revealed statistically significant differences between preoperative and postoperative results as regards the degree of hydronephrosis (P = 0.016) (Table 3). Discussion Laparoscopic pyeloplasty is a first-line option for the management of UPJO. It has a greater success rate than that of endopyelotomy and is associated with a shorter and less intense convalescence compared with open pyeloplasty. The technique is well established and reproducible, although it is more difficult in certain situations, such as after a previous pyeloplasty and intrarenal pelvis [11]. The transperitoneal approach is more familiar to most surgeons and offers the following advantages: much wider workspace that would allow easier addition of techniques, such as transposition of polar vessels or remodeling of the pelvis and resolution of secondary lithiasis, and the anatomical landmarks allow better guidance and more easily reproduce the steps of open surgery [12]. In our study, as well as in other studies [3,5,13], the incidence of intraoperative blood loss was minimal and the requirement for blood transfusion was rare. The estimated blood loss in our study was less than 50 ml in 86.2% of patients and between 50 and 100 ml in 13.8%. None required blood transfusion. Inagaki et al. [14] found that the mean blood loss was 158 ml. Such results are comparable to blood loss reported in open pyeloplasty. The mean operative time in the present study was min (range min), which is nearly similar to that reported by other researchers [5,15,16]. In the work of Mandahani et al. [15], the mean operative time was 246 min (range min). Recently, Juliano and
4 234 Annals of Pediatric Surgery 2015, Vol 11 No 4 Fig. 2 Spatulaion of the upper ureter. Fig. 3 Insertion of double-j into the upper ureter and starting ureteropelvic anastomosis. colleagues reported a mean operative time of 127 min (range min). The significant difference in the operative time found in several studies may be attributed to the presence of different surgeons with different experiences. The technique of suturing, the methods used for knot tying, the inclusion of recurrent UPJO, and the occurrence of intraoperative complications are important factors related to operative time [7]. The type of TLP is another factor in determining the mean operative time. Szydełko and colleagues found that patients who underwent nondismembered Y-V plasty had significantly shorter operative time while maintaining similar postoperative outcomes. The shorter operative time in the Y-V plasty group was explained by the fact that fewer anastomotic sutures were needed in this procedure, which made it technically easier and more feasible [17]. Many urologists prefer to perform retrograde urography before proceeding with TLP, to more precisely define the length and location of the strictured segment and to rule out distal obstruction and then insert double-j stent retrogradely before completion of the anastomosis. However, such technique adds to the increased operative
5 Transperitoneal laparoscopic pyeloplasty Elemam et al. 235 Fig. 4 Completion of the posterior layer and coil of the double-j stent left within the renal pelvis (a). Table 1 Perioperative parameters in 32 transperitoneal laparoscopic pyeloplasty procedures Parameters Minimum Maximum Mean ± SD Mean age (years) ± 21 Operative time (min) ± 22.6 Mean postoperative hospital stay (days) ± 1.5 Mean duration of stenting (weeks) ± 2.11 Mean follow-up (months) ± 5.18 time [1,18,19]. Others performed double-j placement in an antegrade manner just preoperatively. In this study, double-j stent was inserted in all cases antegradely during theoperation.twostepsmayhavearoleindiminishingthe mean operative time in this study: the first step was the fixation of redundant renal pelvis to anterior abdominal wall using vicryl 2/0 as a sling, which acts as retraction, and sparing one trocar; and the second step was the insertion of double-j stent over the guidewire passed through puncture needle after spatulation of the ureter [20 22]. A double-j stenting is a standard of care to drain pyeloplasty in many centers (25). It may have an advantage of lessened nursing care and reduced morbidity after pyeloplasty. Egan and colleagues have shown that double-j stenting may result in more rapid resolution of hydronephrosis after pyeloplasty. The double-j ureteral stent is often placed after ureteral spatulation and before beginning the anterior wall of the anastomosis to minimize the risk for undue traction or compromise to the reanastomosis [23]. However, stent malpositioning has been reported with blind antegrade stenting. Malpositioning of the lower end of the double-j stent is usually associated with difficulties in negotiating the ureterovesical junction [20]. Most surgeons perform the anastomosis in a running manner. Lapra-Ty clips may be used to minimize knot tying, and
6 236 Annals of Pediatric Surgery 2015, Vol 11 No 4 Table 2 Early postoperative complications in 32 units of 29 cases after transperitoneal laparoscopic pyeloplastyupjo, ureteropelvic junction obstruction Complications Number of cases Clavien classification % Blood loss (ml) < Grade Grade Urine 1 Grade leakage > 100 ml 1 Grade 3 as the case treated by double J Recurrent UPJO 1 Grade Total Table 4 Results of preoperative and postoperative glomerular filtration rate after 6 monthsgfr, glomerular filtration rate GFR values Preoperative [n (%)] Postoperative [n (%)] Rt kidney < 20 0 (0) 0 (0) (18.75) 0 (0) > (31.25) 16 (50) Lt kidney < 20 2 (6.25) 0 (0) (25) 1 (3.1) > 40 6 (18.75) 15 (46.9) Total 32 (100) 32 (100) Table 3 Results of preoperative and postoperative intravenous urography IVU Preoperative [n (%)] Postoperative [n (%)] Normal 0 (0.0) 12 (37.5) Unilateral mild hydronephrosis 8 (25) 15 (46.9) Unilateral moderate hydronephrosis 15 (46.9) 4 (12.5) Unilateral marked hydronephrosis 6 (18.7) 1 (3.1) Bilateral moderate hydronephrosis 3 (9.4) 0 (0.0) Total 32 (100) 32 (100) w 2 -Test w P-value Postoperative GFR also showed significant improvement compared with preoperative GFR (Tables 4 and 5). GFR, glomerular filtration rate; IVU, intravenous urography. specialized instruments such as the endostitch device may facilitate suturing. Important principles include the creation of a tension-free watertight anastomosis with preservation of the periureteral blood supply [24]. In this study, we performed the anastomosis in a continuous running vicryl suture. The authors started TLP after gaining a good experience in different laparoscopic procedures and mastering intracorporeal suturing and knot tying. The presence of stones is recognized as a complication of the UPJO, and the diagnosis creates dilemmas as regards treatment. Inagaki et al. [14] reported the presence of kidney stones in 16% of patients. Rivas et al. [12] reported on concomitant kidney stones in 12 of 62 patients (19%) who had undergone transperitoneal TLP. They removed stones in eight cases using a flexible cystoscope and a nitinol N-circle basket, whereas in the remaining four cases the stones were extracted using laparoscopic grasping instruments. In cases of UPJO associated with renal stones, a flexible cystoscope or ureteroscope can be inserted through a laparoscopic port into the pyelotomy before closing the defect for removing the stone from the renal pelvis or calyces using forceps or Dormia basket. The light source and camera can be transferred to the cystoscope or the ureteroscope [11]. In this study, extraction of multiple concomitant calyceal stones from ectopic kidney was carried out by introduction of the ureteroscope from the operating trocar sheath. In this study, one case developed urine leakage, which stopped spontaneously within 2 weeks. Another case developed recurrent UPJO, which was managed with double-j stent first and with retrograde endopyelotomy after 1 year. Shoma et al. [3] reported two cases of postoperative Table 5 Results of preoperative and postoperative glomerular filtration rate and split renal functionsgfr, glomerular filtration rate Paired t-test Results Range (ml/min) Mean ± SD t P-value GFR Rt Preoperative ± Postoperative ± * Lt Preoperative ± Postoperative ± < 0.001* Split functions Rt Preoperative ± Postoperative ± Lt Preoperative ± Postoperative ± *P-value < means significant. complications: one had mild hematuria, which was managed conservatively, and the second developed urine leakage, which stopped on the ninth postoperative day. Lasmar et al. [5] reported a postoperative complication rate of 10.9% in 10 patients in the form of urine leakage (six cases), urinary fistula (one case), and port site infection (three case), and all were managed conservatively. Juliano et al. [7] reported 9.6% postoperative complication rate, and urine leakage occurred in eight cases (6.1%); all cases were managed conservatively. One of the most distressing complications of TLP is conversion to open surgery. This conversion has been reported to be in the range of 0 1.8% [5,7]. In this study, there was no single case of conversion to open surgery and all operations were completed laparoscopically without any complication. This is in agreement with that mentioned by Shoma et al. [3], whostudied40casesoftlpwithoutconversiontoopen surgery. The success rate of TLP in the current study was 96.9% (31/32), which is compatible with that reported in the literature. The success rate of TLP has been reported to be consistently high, at 87 98% [3,5 7]. In contrast, Metzelder et al. [20] reported poor success for laparoscopic nondismembered Y-V pyeloplasty. Moreover, Casale and colleagues reported a success rate of 94% for dismembered pyeloplasty and 43% for nondismembered pyeloplasty in children with UPJO. The difference in outcomes between the two laparoscopic techniques was attributed to the dysplastic tissue found in pelviureteric junction obstructions, which is only rearranged in nondismembered procedures but resected in Anderson-Hynes dismembered pyeloplasty [21].
7 Transperitoneal laparoscopic pyeloplasty Elemam et al. 237 Fig. 5 Preoperative intravenous urography (IVU) showing bilateral hydronephrosis (a). Post-transperitoneal laparoscopic pyeloplasty (TLP) IVU (b) showing no obstruction, with good configuration of both kidneys. Despite observed success in relieving obstruction, functional improvement after UPJO repair is less certain. One study showed no improvement after pyeloplasty in patients, with preoperative renal function of less than 20% 18 [8]. In another study, only two of 10 patients with preoperative renal function less than 30% improved after the repair [9]. In the work of Khan et al. [10], the majority of patients had persistent hydronephrosis after surgery and the improvement in renal function and T½ was noted in less than 50% of cases. In the present study, there was a statistically significant difference between preoperative and postoperative IVU results as regards the degree of hydronephrosis (P = 0.016). Moreover, there was a statistically significant improvement in the postoperative GFR than in the preoperative values after 6 months of follow-up (P = 0.006). This can be explained by the fact that 93.8% of renal units we studied had preoperative GFR greater than 20 ml/min/1.73 m 2 and 50% of renal units had GFR greater than 40 ml/min/1.73 m 2. Our study may be limited by the lack of randomization, the small number of cases, and the heterogeneity of patients studied as regards ages and type of TLP (Tables 4 and 5, Fig. 5). Conclusion Laparoscopic pyeloplasty has a minimal level of morbidity, short hospital stay, better cosmesis, and excellent radiological and functional outcomes. Acknowledgements My gratitude and sincere thanks to Prof. Eraky, Professor of Urology, Mansura Urology and Nephrology Institute for his continuous support and learning brilliant ideas. My deep thanks to Prof. Hussein Galal, Staff members and colleges in the Department of Urology and Pediatric Surgery, Al-Azher Univesity for their support and advice. Conflicts of interest There are no conflicts of interest. References 1 Lee H, Han SW. Ureteropelvic junction obstruction: what we know and what we don t know. KJU 2009; 50: Schuessler WW, Grune MT, Tecuanhuey LV, Preminger GM. Laparoscopic dismembered pyeloplasty. J Urol 1993; 150: Shoma AM, El Nahas AR, Bazeed MA. Laparoscopic pyeloplasty: a prospective randomized comparison between the transperitoneal approach and retroperitoneoscopy. J Urol 2007; 178: Calvert RC, Morsy MM, Zelhof B, Rhodes M, Burgess NA. Comparison of laparoscopic and open pyeloplasty in 100 patients with pelvi-ureteric junction obstruction. Surg Endosc 2008; 22: Lasmar MT, Castro HA Jr, Vengjer A, Guerra FA, Souza EA, Rocha LM. Transperitoneal laparoscopic pyeloplasty: Brazilian initial experience with 55 cases. Int Braz J Urol 2010; 36: Adeyoju AB, Hrouda D, Gill IS. Laparoscopic pyeloplasty: the first decade. BJU Int 2004; 94: Juliano RV, Mendonca RR, Meyer F, Rubinstein M, Lasmar MT, Korkes F, et al. Long-term outcome of laparoscopic pyeloplasty: multicentric comparative study of techniques and accesses. J Laparoendosc Adv Surg Tech A 2011; 21: Gupta M, Tuncay OL, Smith AD. Open surgical exploration after failed endopyelotomy: a 12-year perspective. J Urol 1997; 157:
8 238 Annals of Pediatric Surgery 2015, Vol 11 No 4 9 Dimarco DS, Gettman MT, McGee SM. Longterm success of antegrade endopyelotomy compared with pyeloplasty at a single institution. J Endourol 2006; 20: Tripathi M, Kumar R, Chandrashekar N, Sharma S, Bal C, Bandopadhyaya G, Malhotra A. Diuretic radionuclide renography in assessing Anderson-Hynes pyeloplasty in unilateral pelviureteric junction obstruction. Hell J Nucl Med 2005; 8: Wolf JS. Laparoscopic transperitoneal pyeloplasty. J Endourology 2011; 25: Rivas JG, Alonso Y Gregorio S, Sanchez LC, Guerin Cde C, Gomez AT, Togores LH, Barthel JJ. Approach to kidney stones associated with ureteropelvic junction obstruction during laparoscopic pyeloplasty. Cent European J Urol 2014; 66: Zhang X, Li HZ, Ma X, Zheng T, Lang B, Zhang J, et al. Retrospective comparison of retroperitoneal laparoscopic versus open dismembered pyeloplasty for ureteropelvic junction obstruction. JUrol2006; 176: Inagaki T, Rha KH, Ong AM, Kavoussi LR, Jarrett TW. Laparoscopic pyeloplasty: current status. BJU Int 2005; 95 (Suppl 2): Mandhani A, Kumar D, Kumar A, Kapoor R, Dubey D, Srivastava A, Bhandari M. Safety profile and complications of transperitoneal laparoscopic pyeloplasty: a critical analysis. J Endourol 2005; 19: Bachmann A, Ruszat R, Forster T, Eberli D, Zimmermann M, Muller A, et al. Retroperitoneoscopic pyeloplasty for ureteropelvic junction obstruction (UPJO): solving the technical difficulties. Eur Urol 2006; 49: Szydełko T, Kasprzak J, Apoznański W, et al. Comparison of dismembered and nondismembered Y-V laparoscopic pyeloplasty in patients with primary hydronephrosis. J Laparoendosc Adv Surg Tech A 2010; 20: Moon DA, El-Shazly MA, Cm Chang, et al. Laparoscopic pyeloplasty evaluation of a new gold standard. Urology 2006; 67: Bansal P, Gupta A, Mongha R. Laparoscopic versus open pyeloplasty: comparison of two surgical approaches a single center experience of three years. J Min Access Surg 2008; 4: Metzelder ML, Schier F, Petersen C, Truss M, Ure BM. Laparoscopic transabdominal pyeloplasty in children is feasible irrespective of age. J Urol 2006; 175: Casale P, Grady RW, Joyner BD, Zeltser IS, Figueroa TE, Mitchell ME. Comparison of dismembered and nondismembered laparoscopic pyeloplasty in the pediatric patient. J Endourol 2004; 18: Pahwa M, Pahwa AR, Girotra M, Abrahm RR, Kathuria S, Sharma A. Defining the pros and cons of open, conventional laparoscopy, and robot-assisted pyeloplasty in a developing nation. Adv Urol 2014; 2014: Egan SC, Stock JA, Hanna MK. Renal ultrasound changes after internal double-j stented pyeloplasty for ureteropelvic junction obstruction. Tech Urol 2001; 7: Klingler HC, Remzi M, Janetschek G, et al. Comparison of open versus laparoscopic pyeloplasty techniques in treatment of ureteropelvic junction obstruction. Eur Urol 2003; 44:
Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique
 Original paper Videosurgery Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique Tomasz Szydelko 1, Wojciech Apoznanski 2, Piotr Koleda
Original paper Videosurgery Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique Tomasz Szydelko 1, Wojciech Apoznanski 2, Piotr Koleda
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in Adults: 6 Years Experience in One Center
 Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
ORIGINAL ARTICLES Endourology
 Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Hydronephrosis after retroperitoneal laparoscopic. dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction.
 101 original paper TRAUMA AND RECONSTRUCTIVE UROLOGY Hydronephrosis after retroperitoneal laparoscopic dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction:
101 original paper TRAUMA AND RECONSTRUCTIVE UROLOGY Hydronephrosis after retroperitoneal laparoscopic dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction:
Although open surgery has stood the test of time for
 JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 463 467 DOI: 10.1089=end.2008.0208 Laparoscopic Pyeloplasty: Our New Gold Standard Stephanie J. Symons, M.D., Parag S.
JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 463 467 DOI: 10.1089=end.2008.0208 Laparoscopic Pyeloplasty: Our New Gold Standard Stephanie J. Symons, M.D., Parag S.
Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience
 LAPAROSCOPIC UROLOGY Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience Zhen-yu Ou, Jin-bo Chen, Zhi Chen, Min-feng Chen,
LAPAROSCOPIC UROLOGY Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience Zhen-yu Ou, Jin-bo Chen, Zhi Chen, Min-feng Chen,
The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe Kidneys
 Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
Downloaded from Medico Research Chronicles Pelvi-ureteric junction obstruction - A ten year single center review in north central Nigeria.
 PELVI-URETERIC JUNCTION OBSTRUCTION - A TEN YEAR SINGLE CENTER REVIEW IN NORTH CENTRAL NIGERIA. 1,2 1,2 1 1 Atim T, Aisuodionoe-Shadrach O, Ajibola O. H, Magnus F. E Division of Urology, Departments of
PELVI-URETERIC JUNCTION OBSTRUCTION - A TEN YEAR SINGLE CENTER REVIEW IN NORTH CENTRAL NIGERIA. 1,2 1,2 1 1 Atim T, Aisuodionoe-Shadrach O, Ajibola O. H, Magnus F. E Division of Urology, Departments of
TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
 Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Facing Surgery. for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option
 Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty?
 Turk J Urol 2017; 43(4): 497-501 DOI: 10.5152/tud.2017.77775 LAPAROSCOPY Original Article 497 Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty? Mustafa Suat Bolat,
Turk J Urol 2017; 43(4): 497-501 DOI: 10.5152/tud.2017.77775 LAPAROSCOPY Original Article 497 Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty? Mustafa Suat Bolat,
Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study
 466 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study Omar Fahmy 1, Abdel-Rahman El-Fayoumi
466 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study Omar Fahmy 1, Abdel-Rahman El-Fayoumi
Original Article. Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice
 Original Article www.jpgmonline.com Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice Bryant RJ, Craig E, Oakley N Department of Urological Surgery,
Original Article www.jpgmonline.com Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice Bryant RJ, Craig E, Oakley N Department of Urological Surgery,
ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD
 ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD Chairman, The Departments of Urology & Pediatric Urology, Shaare Zedek Medical Center
ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD Chairman, The Departments of Urology & Pediatric Urology, Shaare Zedek Medical Center
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical team experience with 38 cases
 ORIGINAL ARTICLE Vol. 43 (3): 512-517, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0198 Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical
ORIGINAL ARTICLE Vol. 43 (3): 512-517, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0198 Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical
Study of laparoscopic retroperitoneal pyeloplasty
 International Surgery Journal Gajbhiye R et al. Int Surg J. 2015 Feb;2(1):53-59 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: 10.5455/2349-2902.isj20150210 Study of laparoscopic
International Surgery Journal Gajbhiye R et al. Int Surg J. 2015 Feb;2(1):53-59 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: 10.5455/2349-2902.isj20150210 Study of laparoscopic
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients
 Review Article Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients Francesco Turrà 1, Maria Escolino 1, Alessandra Farina 1, Alessandro Settimi 1, Ciro Esposito 1, François
Review Article Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients Francesco Turrà 1, Maria Escolino 1, Alessandra Farina 1, Alessandro Settimi 1, Ciro Esposito 1, François
Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
 Int J Clin Exp Med 2016;9(5):8587-8592 www.ijcem.com /ISSN:1940-5901/IJCEM0017894 Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
Int J Clin Exp Med 2016;9(5):8587-8592 www.ijcem.com /ISSN:1940-5901/IJCEM0017894 Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
 ORIGINAL Article Vol. 39 (2): 195-202, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.07 Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
ORIGINAL Article Vol. 39 (2): 195-202, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.07 Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic Single-Site (R-LESS) Pyeloplasty Using a New Single-Port Platform
 EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
ENDOPYELOTOMY WITH THE ACUCISE CATHETER
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 302-310, July - August, 2002 ENDOPYELOTOMY WITH THE ACUCISE CATHETER ARTUR H. BRITO, ANUAR I.
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 302-310, July - August, 2002 ENDOPYELOTOMY WITH THE ACUCISE CATHETER ARTUR H. BRITO, ANUAR I.
Retroperitoneal and Transperitoneal Robot-Assisted Pyeloplasty in Adults: Techniques and Results
 EUROPEAN UROLOGY 58 (2010) 711 718 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Retroperitoneal and Transperitoneal Robot-Assisted Pyeloplasty in Adults:
EUROPEAN UROLOGY 58 (2010) 711 718 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Retroperitoneal and Transperitoneal Robot-Assisted Pyeloplasty in Adults:
International Journal of Sciences & Applied Research. Management of PUJ obstruction IJSAR, 2(2), 2015; 22-31
 International Journal of Sciences & Applied Research www.ijsar.in Management of PUJ obstruction Chugh A.*, Agarwal P.N., Singh R., Mishra A., Jain V., Meena M. Dept of General Surgery, MAMC. Correspondence
International Journal of Sciences & Applied Research www.ijsar.in Management of PUJ obstruction Chugh A.*, Agarwal P.N., Singh R., Mishra A., Jain V., Meena M. Dept of General Surgery, MAMC. Correspondence
Hydronephrosis. Nephrosis. Refers to the kidney
 What is hydronephrosis? Hydro Nephrosis Refers to water or fluid Refers to the kidney A build-up of fluid (urine) in the kidney is the medical term for a build-up of urine in the kidney. As the urine builds
What is hydronephrosis? Hydro Nephrosis Refers to water or fluid Refers to the kidney A build-up of fluid (urine) in the kidney is the medical term for a build-up of urine in the kidney. As the urine builds
G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve.
 G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. ANTENATAL HYRONEPHROSIS UROLOGICAL ASPECTS Dr Gianantonio Manzoni, FEAPU FRCS U.O.
G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. ANTENATAL HYRONEPHROSIS UROLOGICAL ASPECTS Dr Gianantonio Manzoni, FEAPU FRCS U.O.
Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach
 CASE REPORT Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach Nand Kishore Arvind, Onkar Singh, Shilpi Singh Gupta ABSTRACT Background and Objectives: Testicular vein syndrome (TVS)
CASE REPORT Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach Nand Kishore Arvind, Onkar Singh, Shilpi Singh Gupta ABSTRACT Background and Objectives: Testicular vein syndrome (TVS)
ISSN East Cent. Afr. J. surg. (Online)
 87 Ureteroscopy in a Resource Limited Setting: The Tikur Anbessa General Specialized Hospital Experience in Addis Ababa, Ethiopia. D. Andualem, L. Be-ede, T. Mulat, L. Samodi Addis Ababa University-School
87 Ureteroscopy in a Resource Limited Setting: The Tikur Anbessa General Specialized Hospital Experience in Addis Ababa, Ethiopia. D. Andualem, L. Be-ede, T. Mulat, L. Samodi Addis Ababa University-School
Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants
 Hydronephrosis Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants Eduardo Ruiz, Ricardo Soria, Edurne Ormaechea, Mauricio Marcelo Urquizo
Hydronephrosis Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants Eduardo Ruiz, Ricardo Soria, Edurne Ormaechea, Mauricio Marcelo Urquizo
Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy, and Robot-Assisted Pyeloplasty in a Developing Nation
 Hindawi Publishing Corporation Advances in Urology Volume 2014, Article ID 850156, 6 pages http://dx.doi.org/10.1155/2014/850156 Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy,
Hindawi Publishing Corporation Advances in Urology Volume 2014, Article ID 850156, 6 pages http://dx.doi.org/10.1155/2014/850156 Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy,
Surgery Illustrated Surgical Atlas
 Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
Mini incision open pyeloplasty - Improvement in patient outcome
 ORIGINAL ARTICLE Vol. 41 (5): 927-934, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0024 Mini incision open pyeloplasty - Improvement in patient outcome Vishwajeet Singh 1, Manish Garg 1,
ORIGINAL ARTICLE Vol. 41 (5): 927-934, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0024 Mini incision open pyeloplasty - Improvement in patient outcome Vishwajeet Singh 1, Manish Garg 1,
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
The Management of Ureteropelvic Junction Obstruction Presenting with Prenatal Hydronephrosis
 Review Special Issue: Pre- and Postnatal Management of Hydronephrosis TheScientificWorldJOURNAL (2009) 9, 400 403 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.51 The Management of Ureteropelvic Junction
Review Special Issue: Pre- and Postnatal Management of Hydronephrosis TheScientificWorldJOURNAL (2009) 9, 400 403 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.51 The Management of Ureteropelvic Junction
Pelvioureteric junction obstruction of the lower collecting system associated with incomplete ureteral duplication: A case report
 Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Impact of ureteral stenting prior to ureterorenoscopy on stone-free rates and complications
 World J Urol (2013) 31:855 859 DOI 10.1007/s00345-011-0789-6 ORIGINAL ARTICLE Impact of ureteral stenting prior to ureterorenoscopy on stone-free rates and complications P. P. Lumma P. Schneider A. Strauss
World J Urol (2013) 31:855 859 DOI 10.1007/s00345-011-0789-6 ORIGINAL ARTICLE Impact of ureteral stenting prior to ureterorenoscopy on stone-free rates and complications P. P. Lumma P. Schneider A. Strauss
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study
 Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic pyeloplasty Introduction This overview has been prepared to assist members
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic pyeloplasty Introduction This overview has been prepared to assist members
Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones: our experience
 Liang et al. BMC Urology (2017) 17:15 DOI 10.1186/s12894-017-0205-7 RESEARCH ARTICLE Open Access Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones:
Liang et al. BMC Urology (2017) 17:15 DOI 10.1186/s12894-017-0205-7 RESEARCH ARTICLE Open Access Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones:
THE operation of reimplantation of the ureter into the bladder has undergone
 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET
 LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child
 CASE REPORT Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child Manickam Ramalingam, MCh, Kallappan Senthil, MCh, Anandan Murugesan, MCh, Mizar Ganapathy Pai, MCh ABSTRACT Low compliance
CASE REPORT Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child Manickam Ramalingam, MCh, Kallappan Senthil, MCh, Anandan Murugesan, MCh, Mizar Ganapathy Pai, MCh ABSTRACT Low compliance
Manual on Preparation of Tissue for Neonatal Skills Course. Version 1.0_2018. Prepared by: Haitham Dagash. MBBS, FRCSEd (Paed)
 Manual on Preparation of Tissue for Neonatal Skills Course Version 1.0_2018 Prepared by: Haitham Dagash MBBS, FRCSEd (Paed) University of Leicester and Leicester Infirmary Hospital Prof.Kokila Lakhoo PhD,FRCS(ENG+EDIN),FCS(SA),FCS(SA:PAED),MRCPCH,MBCHB
Manual on Preparation of Tissue for Neonatal Skills Course Version 1.0_2018 Prepared by: Haitham Dagash MBBS, FRCSEd (Paed) University of Leicester and Leicester Infirmary Hospital Prof.Kokila Lakhoo PhD,FRCS(ENG+EDIN),FCS(SA),FCS(SA:PAED),MRCPCH,MBCHB
Percutaneous nephrolithotomy (PCNL), as primary. Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy. Case Report
 JOURNAL OF ENDOUROLOGY CASE REPORTS Volume 3.1, 2017 Mary Ann Liebert, Inc. Pp. 52 56 DOI: 10.1089/cren.2017.0011 Case Report Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy Eugenio Di Grazia,
JOURNAL OF ENDOUROLOGY CASE REPORTS Volume 3.1, 2017 Mary Ann Liebert, Inc. Pp. 52 56 DOI: 10.1089/cren.2017.0011 Case Report Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy Eugenio Di Grazia,
The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study
 Bahrain Medical Bulletin, Vol.26, No. 1, Mach 2004 The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study Waleed Ali, FRCS* Mohammed Al-Durazi, FRCS** Reem Al-Bareeq,
Bahrain Medical Bulletin, Vol.26, No. 1, Mach 2004 The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study Waleed Ali, FRCS* Mohammed Al-Durazi, FRCS** Reem Al-Bareeq,
Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis
 Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis Abstract M. Naeem,K. Anwar ( Department of Urology, Pakistan Institute of Medical Sciences, Islamabad. ) Objective:
Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis Abstract M. Naeem,K. Anwar ( Department of Urology, Pakistan Institute of Medical Sciences, Islamabad. ) Objective:
Prenatal Hydronephrosis
 Prenatal Hydronephrosis What is hydronephrosis? Hydronephrosis is dilation of the kidney, specifically the renal pelvis (place where urine is stored after its production). This can be the result of an
Prenatal Hydronephrosis What is hydronephrosis? Hydronephrosis is dilation of the kidney, specifically the renal pelvis (place where urine is stored after its production). This can be the result of an
Objectives: To analyze various factors predicting success of retrograde ureteric stenting in managing patients with ureteric obstruction.
 ISPUB.COM The Internet Journal of Urology Volume 14 Number 1 Factors Predicting Success Rate Of Retrograde Ureteric Stenting In Managing Patients With Ureteric Obstruction- Our Experiences In A South Indian
ISPUB.COM The Internet Journal of Urology Volume 14 Number 1 Factors Predicting Success Rate Of Retrograde Ureteric Stenting In Managing Patients With Ureteric Obstruction- Our Experiences In A South Indian
Long-term results of percutaneous nephrolithotomy for treatment of staghorn stones
 ; 2010 Laparoscopic and Robotic Urology LONG-TERM RESULTS OF PNL FOR STAGHORN STONES EL-NAHAS et al. BJUI Long-term results of percutaneous nephrolithotomy for treatment of staghorn stones Ahmed R. EL-Nahas,
; 2010 Laparoscopic and Robotic Urology LONG-TERM RESULTS OF PNL FOR STAGHORN STONES EL-NAHAS et al. BJUI Long-term results of percutaneous nephrolithotomy for treatment of staghorn stones Ahmed R. EL-Nahas,
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Ostruzione pieloureterale polari anomali «hitching technique»
 Ostruzione pieloureterale da vasi polari anomali «hitching technique» S.F. Chiarenza dept. pediatric AND UROLOGIC surgery s.bortolo hospital vicenza italy ITALY 1949 Hellstrom : trasposition polar vessels
Ostruzione pieloureterale da vasi polari anomali «hitching technique» S.F. Chiarenza dept. pediatric AND UROLOGIC surgery s.bortolo hospital vicenza italy ITALY 1949 Hellstrom : trasposition polar vessels
Researcher 2017;9(4) Outcome of Percutaneous Nephrolithotomy for Staghorn Stones: Al-Azhar 5-Years Experience
 Outcome of Percutaneous Nephrolithotomy for Staghorn Stones: Al-Azhar 5-Years Experience Ibrahim Ahmed El Sotohi Department of Urology, Faculty of Medicine, Al-Azhar University, Cairo, Egypt ibrahimelsotohi@gmail.com
Outcome of Percutaneous Nephrolithotomy for Staghorn Stones: Al-Azhar 5-Years Experience Ibrahim Ahmed El Sotohi Department of Urology, Faculty of Medicine, Al-Azhar University, Cairo, Egypt ibrahimelsotohi@gmail.com
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Complication of long indwelling urinary catheter and stent COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT
 151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal Approach During the Learning Curve
 JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES
 1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
Endoscopic Removal of a Long Fibroepithelial Polyp of the Ureter in an Adolescent *
 Open Journal of Clinical & Medical Abstract Case Reports Volume 2 (2016) Issue 12 ISSN 2379-1039 Endoscopic Removal of a Long Fibroepithelial Polyp of the Ureter in an Adolescent * Case M. Wood, MD; Andrew
Open Journal of Clinical & Medical Abstract Case Reports Volume 2 (2016) Issue 12 ISSN 2379-1039 Endoscopic Removal of a Long Fibroepithelial Polyp of the Ureter in an Adolescent * Case M. Wood, MD; Andrew
JMSCR Vol 05 Issue 08 Page August 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i8.06 A Comparative study between Retroperitoneoscopic
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i8.06 A Comparative study between Retroperitoneoscopic
A Comparative Study between Open and Laparoscopic Pyeloplasty
 A Comparative Study between Open and Laparoscopic Pyeloplasty Ali Hamdan Fahad College of Medicine, University of Al-Qadisiyah, Iraq Abstract: Background: Historically open pyeloplasty has been regarded
A Comparative Study between Open and Laparoscopic Pyeloplasty Ali Hamdan Fahad College of Medicine, University of Al-Qadisiyah, Iraq Abstract: Background: Historically open pyeloplasty has been regarded
Lec-8 جراحة بولية د.نعمان
 4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA
 ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours
 Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
Robotic-Assisted Laparoscopic Pyeloplasty
 Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
LAPAROSCOPIC PYELOPLASTY
 LAPAROSCOPIC PYELOPLASTY Urology Clinic GW Medical Faculty Associates The George Washington University 2150 Pennsylvania Avenue, NW Washington, DC 20037 PURPOSE. Laparoscopic Pyeloplasty is a minimally
LAPAROSCOPIC PYELOPLASTY Urology Clinic GW Medical Faculty Associates The George Washington University 2150 Pennsylvania Avenue, NW Washington, DC 20037 PURPOSE. Laparoscopic Pyeloplasty is a minimally
Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair
 Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair Pankaj P. Dangle, James Kearns, Blake Anderson and Mohan S. Gundeti* From the Department of Surgery, Division
Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair Pankaj P. Dangle, James Kearns, Blake Anderson and Mohan S. Gundeti* From the Department of Surgery, Division
Evaluation of Efficiency and Safety of Transperitoneal Laparoscopic Ureterolithotomy for Treatment of Lumbar Ureteric Stones
 Med. J. Cairo Univ., Vol. 85, No. 3, June: 1075-1080, 2017 www.medicaljournalofcairouniversity.net Evaluation of Efficiency and Safety of Transperitoneal Laparoscopic Ureterolithotomy for Treatment of
Med. J. Cairo Univ., Vol. 85, No. 3, June: 1075-1080, 2017 www.medicaljournalofcairouniversity.net Evaluation of Efficiency and Safety of Transperitoneal Laparoscopic Ureterolithotomy for Treatment of
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY. THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel
 PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
Congenital midureteric stricture: A rare entity in pediatric patient
 PEDIATRIC UROLOGY CASE REPORTS DOI: 10.14534/PUCR.2016622492 DOI: Open Access Congenital midureteric stricture: A rare entity in pediatric patient Prashant Sadashiv Patil, Gupta Abhaya, Kothari Paras L,
PEDIATRIC UROLOGY CASE REPORTS DOI: 10.14534/PUCR.2016622492 DOI: Open Access Congenital midureteric stricture: A rare entity in pediatric patient Prashant Sadashiv Patil, Gupta Abhaya, Kothari Paras L,
In Situ Extracorporeal Shock Wave Lithotripsy (ESWL) and ESWL after Push Back For Upper Ureteric Calculi: A Comparative Study
 ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment
 Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Retroperitoneoscopic Ablative Renal Surgery in Children: The Feasibility of Using Three Trocars
 Tayfun Oktar, Oner Sanli, Ömer Acar, Tzevat Tefik, Serkan Karakus, Orhan Ziylan LAPAROSCOPIC UROLOGY Retroperitoneoscopic Ablative Renal Surgery in Children: The Feasibility of Using Three Trocars Department
Tayfun Oktar, Oner Sanli, Ömer Acar, Tzevat Tefik, Serkan Karakus, Orhan Ziylan LAPAROSCOPIC UROLOGY Retroperitoneoscopic Ablative Renal Surgery in Children: The Feasibility of Using Three Trocars Department
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Identifying unrecognized collecting system entry and the integrity of repair during open partial nephrectomy: comparison of two techniques
 ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
Forgotten JJ stent: A rare case report
 Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience
 Original research Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience Aziz Khambati, MD; Elias Wehbi, MD; Walid A.
Original research Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience Aziz Khambati, MD; Elias Wehbi, MD; Walid A.
Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized, Controlled Trial
 Minimally Invasive Surgery, Article ID 892890, 4 pages http://dx.doi.org/10.1155/2014/892890 Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized,
Minimally Invasive Surgery, Article ID 892890, 4 pages http://dx.doi.org/10.1155/2014/892890 Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized,
Department of Urology, Theodor Bilharz research Institute, Cairo, Egypt
 Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Parapelvic cyst- an unusual cause of pelviureteric obstruction with laparoscopic management of the same
 ISPUB.COM The Internet Journal of Urology Volume 7 Number 2 Parapelvic cyst- an unusual cause of pelviureteric obstruction with laparoscopic management of the G Abraham, K Das, G Datson, T Thachill, O
ISPUB.COM The Internet Journal of Urology Volume 7 Number 2 Parapelvic cyst- an unusual cause of pelviureteric obstruction with laparoscopic management of the G Abraham, K Das, G Datson, T Thachill, O
JMSCR Volume 03 Issue 05 Page May 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Laparoendoscopic Pfannenstiel Nephrectomy using Conventional Laparoscopic Instruments - Preliminary Experience
 Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
Modified Differential Renal Function Measurement Revised by Renal Cross Sectional Area in Children with Ureteropelvic Junction Obstruction
 www.kjurology.org DOI:10.4111/kju.2010.51.4.271 Pediatric Urology Modified Differential Renal Function Measurement Revised by Renal Cross Sectional Area in Children with Ureteropelvic Junction Obstruction
www.kjurology.org DOI:10.4111/kju.2010.51.4.271 Pediatric Urology Modified Differential Renal Function Measurement Revised by Renal Cross Sectional Area in Children with Ureteropelvic Junction Obstruction
Case Presentation - Pediatric Endourology
 Case Presentation - Pediatric Endourology PA N E L : E U G ENE M I N EV I C H, U S A J O NAT H A N G L A S S, UK R OY M O R AG, I S R A E L YO R A M M O R, I S R A E L P I N C H AS L I V N E, I S R A E
Case Presentation - Pediatric Endourology PA N E L : E U G ENE M I N EV I C H, U S A J O NAT H A N G L A S S, UK R OY M O R AG, I S R A E L YO R A M M O R, I S R A E L P I N C H AS L I V N E, I S R A E
Excretory urography (EU) or IVP US CT & radionuclide imaging
 Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Robotics, Laparoscopy & Endosurgery
 Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Role of imaging in evaluation of genitourinary i trauma Spectrum of GU injuries Relevance of imaging findings in determining management Focus on MDCT
 Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
