Retroperitoneal and Transperitoneal Robot-Assisted Pyeloplasty in Adults: Techniques and Results
|
|
|
- Morgan Jefferson
- 5 years ago
- Views:
Transcription
1 EUROPEAN UROLOGY 58 (2010) available at journal homepage: Surgery in Motion Retroperitoneal and Transperitoneal Robot-Assisted Pyeloplasty in Adults: Techniques and Results Andrea Cestari *, Nicolò Maria Buffi, Giuliana Lista, Mattia Sangalli, Emanuele Scapaticci, Fabio Fabbri, Massimo Lazzeri, Patrizio Rigatti, Giorgio Guazzoni Department of Urology, Vita-Salute University, San Raffaele Hospital Turro, Milan, Italy Article info Article history: Accepted July 13, 2010 Published online ahead of print on August 4, 2010 Keywords: Robotic surgery UPJ obstruction Pyeloplasty laparoscopy Renal diseases Please visit and to view the accompanying video. Abstract Background: The surgical management of ureteropelvic junction obstruction (UPJO) has dramatically evolved over the past 20 yr due to the development of new technology. Objective: Our aim was to report the feasibility and efficacy of robot-assisted pyeloplasty (RAP) performed by either the retroperitoneal or the transperitoneal approach. Design, setting, and participants: A stage 2 investigative study was conducted including development (stage 2a) and exploration (stage 2b) of transperitoneal and retroperitoneal RAP performed in 55 patients at an urban tertiary university department of urology. Surgical procedure: Retroperitoneal RAP was performed with the patient in full flank position using a 12-mm Hasson-style optical port at the tip of the 12th rib, plus two operative 8-mm robotic trocars and an assistant 5-mm port. The stenotic ureteropelvic junction was excised, the ureter was spatulated, and a dismembered pyeloplasty was performed in all cases. Transperitoneal RAP was performed with the patients in the 608 flank position. The optical port is in the umbilical area, plus two 8-mm operative robotic ports and one 5-mm assistant port. The pyeloplasty technique is similar to the retroperitoneoscopic approach. In both groups, the stent can be positioned in an anterograde or retrograde fashion. Measurements: Success consisted of no evidence of obstruction on computed tomography urography or mercaptoacetyltriglycine-3 diuretic renal scan, no postoperative symptoms, and no further treatment. Results and limitations: Thirty-six patients underwent retroperitoneoscopic RAP and 19 transperitoneal RAP for UPJO. All the procedures were completed with robotic assistance. The overall objective success (measured by diuretic renal scan and/or imaging techniques) was 96% with two cases of recurrence (both in the retroperitoneal group). The main limitation was the short follow-up, although all patients reached at least a 6-mo follow-up. Conclusions: RAP performed either retroperitoneally or transperitoneally was revealed as a feasible and reproducible surgical option for the treatment of UPJO, offering a subjective optimal plasty reconfiguration at short follow-up. # 2010 European Association of Urology. Published by Elsevier B.V. All rights reserved. * Corresponding author. Department of Urology, San Raffaele Hospital, Vita-Salute University, San Raffaele Turro, Via Stamira D Ancona 20, Milan, Italy. Tel ; Fax: address: a_cestari@yahoo.it (A. Cestari) /$ see back matter # 2010 European Association of Urology. Published by Elsevier B.V. All rights reserved. doi: /j.eururo
2 712 EUROPEAN UROLOGY 58 (2010) Introduction 2. Methods The surgical management of ureteropelvic junction obstruction (UPJO) has dramatically evolved over the past 20 yr due to the development of new technologies. Since its introduction into clinical practice in 1993, laparoscopic pyeloplasty (LP) [1] has progressively gained popularity and acceptance in the urologic community and has become a well-established surgical option for UPJO treatment [2 5]. The long-term results are comparable with those of open surgery with success rates ranging from 90% to >95% [6 8]. LP is performed using both the transperitoneal [9,10] and retroperitoneal approaches [5,11]. Nevertheless, it remains a technically demanding procedure requiring high proficiency in laparoscopic suturing and endoscopic skills. Thus with its dependence on extensive and precise intracorporeal suturing, LP is one of the laparoscopic procedures most likely to benefit from robotic assistance. In the last 5 yr, the worldwide spread of robotic surgical machines, such as the da Vinci system (Intuitive Surgical, Inc, Sunnyvale, CA, USA), has changed the way urologists approach complex laparoscopic reconstructive procedures. Robot-assisted pyeloplasty (RAP) is usually performed by the transperitoneal approach [12 15], even though recent reports have stated the retroperitoneal robotassisted LP approach is feasible and efficient [16,17]. In this study we have investigated the feasibility and efficacy of RAP performed via either the retroperitoneoscopic route or the transperitoneal approach, with a particular focus on the surgical details of the two procedures, the indications for each approach, the subsequent advantages and disadvantages, and follow-up. We report a stage 2 investigative nonrandomized study including development (stage 2a) and exploration (stage 2b) [18] of transperitoneal and retroperitoneal robot-assisted LP performed between October 2007 and October 2009 at our urban tertiary university department of urology. The results from imaging techniques, mercaptoacetyltriglycine (MAG)-3 diuretic renal scans, and the presence of symptoms (eg, recurrent flank pain, fever, and recurrent urinary tract infection episodes) verified the need for surgical intervention for UPJO. Success rates were determined both by the subjective improvement of symptoms as well as the objective evidence showing the absence of the obstruction through a diuretic renal scan and/or imaging techniques. The follow-up program included an abdominal ultrasound, urinalysis and a urine culture after 1 mo, as well as a computed tomography urography and MAG-3 diuretic renal scan after 6 mo. Ultrasound was repeated annually, and an evaluation of symptom relief at each follow-up visit was done. Elective criteria for a transperitoneal approach included previous renal surgery (excluding endopyelotomy), a wide pelvis (ie, >6 cm in diameter), concomitant multiple or large renal stones, pelvic kidney and horseshoe kidney, and cases where imaging showed a potential vascular crossing. In the other cases of ureteropelvic junction (UPJ) repair, the decision whether to use a transperitoneal or retroperitoneoscopic approach was based on the surgeon s preference. Complications were reported according to the Clavien-Dindo classification system [19]. Patients signed an informed consent before surgery and were especially made aware of the possibility that the surgery might be converted into traditional LP or open surgery Surgical technique Retroperitoneoscopic robot-assisted pyeloplasty Patients were positioned in the full flank position, with the bed flexed to bridge the surgical area and to increase the space between the iliac crest and the costal arch (Fig. 1). The retroperitoneum was bluntly entered at the tip of the 12th rib using two S retractors through a 1.5-cm skin Fig. 1 Patient positioning for retroperitoneoscopic robot-assisted pyeloplasty. The patient is positioned in full flank position with the bed flexed (308) to widen the space between the costal arch and the iliac crest.
3 EUROPEAN UROLOGY 58 (2010) Fig. 2 Port placement for retroperitoneoscopic robot-assisted pyeloplasty: The patient s head is at the right side of the picture. incision. The retroperitoneal space was created by using balloon dissection using our previously described technique [20]. Port placement is shown in Fig. 2. The 12-mm Hasson-style optical port was positioned at the tip of the 12th rib. The other two operative 8-mm robotic trocars were positioned at the conjunction of the 12th rib with the erector spinae muscle and at the level of the anterior axillary line 6 8 cm cranially to the iliac crest, respectively. The assistant 5-mm port was positioned along the erector spinae muscle, some centimeters cranially to the iliac crest, and was used for suction, retraction, and needle insertion/removal. The da Vinci robotic system was then positioned as shown in Fig. 3 with the arms entering anteriorly to the head of the patient. A 308 optic was always used. Gerota s fascia was longitudinally incised to widen the surgical area and to directly expose the target structures, such as the ureter, the dilated renal pelvis, and the stenotic UPJ. Robotic bipolar forceps and monopolar scissors were used to dissect the proximal ureter and the dilated renal pelvis. The stenotic UPJ was excised; the ureter was then spatulated longitudinally and the pyeloplasty performed according to the Anderson-Hynes technique [21]. The plasty was performed with an interrupted 5-0 Vicryl suture with an RB2 curved needle in the first 12 patients. In the last series, the plasty reconfiguration was performed using running sutures to fasten the procedure. The posterior aspect of the anastomosis was performed, and then the double pigtail ureteral stent was inserted. Once the stent was correctly positioned, the anterior aspect of the anastomosis was completed. At the end of the procedure, once complete hemostasis was achieved, a suction drain was left in place. In the case of a crossing vessel, a dismembered pyeloplasty with transposition of the reanastomosed ureter ventral to the vessels was performed. Fig. 3 Da Vinci standard position for retroperitoneoscopic robot-assisted pyeloplasty. The robotic arm system enters anteriorly approximately 258 from the head of the patient Transperitoneal robot-assisted pyeloplasty Patients were positioned in a 608 flank position with the bed flexed (Fig. 4). Pneumoperitoneum was induced with the Hasson technique, typically in the umbilical area for aesthetic reasons. In obese patients the optical port was positioned on the pararectal line 2.3 cm cranially to the umbilicus. Fig. 5 shows the port placement in the case of transperitoneal
4 714 EUROPEAN UROLOGY 58 (2010) Fig. 4 Patient positioning for transperitoneal robot-assisted pyeloplasty. The patient is positioned in a 608 flank position, and the bed is slightly flexed to better expose the surgical field. RAP. The two operative robotic ports are positioned respectively at the midpoint between the anterior superior iliac spine and the umbilicus and on the pararectal line 1 cm beyond the costal arch. The 5-mm assistant port is positioned on the midline at the midpoint between the umbilicus and the xiphoid process. A 308 laparoscope (down) is routinely used. In Fig. 6 the robot arms positioning for transperitoneal pyeloplasty is shown. The right side of the parietal peritoneum, overlying Gerota s fascia, is incised, and the target structures (the ureter, the dilated renal pelvis, and eventually the aberrant crossing vessels) are exposed. On the left side, typically the white line of Toldt is incised and the left colon is mobilized medially to expose Gerota s fascia, which is incised isolating the target structures. In slender patients with a dilated pelvis, a transmesocolic approach can be used to directly reach the target structures. The pyeloplasty technique is similar to what has already been described when performing the retroperitoneoscopic approach Stent positioning The double pigtail ureteral stent can be inserted in an antegrade or retrograde fashion. In cases of anterograde insertion, the bladder is filled with 150 ml of saline with drops of indigo blue before stent insertion to have adequate bladder distension for optimal stent placement. Filling the bladder with saline also allows us to check the correct distal positioning of the stent thanks to the reflux of blue drops from the upper tip of the stent in the surgical area. In cases of retrograde insertion, the Fig. 5 Port placement for transperitoneal robotic pyeloplasty.
5 EUROPEAN UROLOGY 58 (2010) Fig. 6 Da Vinci S HD position for transperitoneal robot-assisted pyeloplasty. The robotic arm system enters from the back of the patient approximately 458 from the head. procedure is performed using a flexible cystoscope that does not require modifying the position of either the patient or the robot. Total operative time is defined as the first skin incision to the last stitch (Fig. 6) Postoperative care The indwelling catheter is removed on postoperative day 2. The drain is removed the following day after catheter removal on the condition that the output is <50 60 ml. Patients are then discharged from the hospital. The patient is seen 4 wk following the procedure and assessed via an abdominal ultrasound, urine culture, and urinalysis. The stent is usually removed at this time. 3. Results Since October 2007, 55 patients have undergone retroperitoneal (group A; n = 36) or transperitoneal (group B; n = 19) RAP for UPJO. Table 1 summarizes the demographic characteristics. All procedures were completed using robotic assistance. In both groups, port placement results proved to be adequate with no chasing swords phenomenon (the conflict of robotic arms into the operative space), and the surgical field was wide enough for optimal robotic dissection of the target structures for suturing during the plasty reconfiguration. Table 2 lists the intraoperative and perioperative results of the two groups of patients. In all patients with renal stones, it was possible to resolve the lithiases intraoperatively, in both the retroperitoneal and transperitoneal groups, as a result of the intraoperative pyeloscopy. Due to the presence of crossing vessels, the transposition of the ureter was performed in three patients in the retroperitoneal group (where the crossing vessel was not evident at the preoperative imaging) and four patients in the transperitoneal group. The mean time of indwelling catheter was similar in both groups. The drain was removed the day after catheter removal in all patients in the absence of urinary fistulas. Table 1 Demographics of patients submitted to retroperitoneoscopic (group A) and transperitoneal (group B) robot-assisted pyeloplasty Group A Group B Patients, n (male/female) 36 (20/16) 19 (9/10) Mean age, yr (median) (38) (43) Side 23 R/13 L 8 R/11 L Concomitant renal stones, n * 3 7 Previous UPJ surgery y 2 2 Body mass index (median) (21) (22.7) Symptoms Flank pain: 18 patients; UTI: 2 patients Flank pain: 12 patients; UTI: 3 patients L = left; R = right; UPJ = ureteropelvic junction; UTI = urinary tract infection. * In the retroperitoneal group, the stones were single, located in the pelvis, and <1 cm in diameter. y Two cases of failed endopyelotomy in the retroperitoneal group and one case of failed endopyelotomy and one case of failed laparoscopic pyeloplasty in the transperitoneal group.
6 716 EUROPEAN UROLOGY 58 (2010) Table 2 Operative and early postoperative findings of patients who underwent retroperitoneoscopic (group A) and transperitoneal (group B) robot-assisted pyeloplasty Group A Group B Operative time, min (median) * (125) (125) Decrossing of aberrant crossing vessels 3 y 4 Catheterization time, d (median) (3) (3) Drain removal, d (median) (4) (3) Hospital stay, d (median) (4) (5) Recurrence, n 2 0 Mean follow-up, mo (median) (18) (6) * Operative time included da Vinci docking time during the procedure. y Not evident at standard preoperative imaging. No significant surgical perioperative complications were reported; one patient had transitory hyperpyrexia treated with antipyretics (Clavien-Dindo grade I). Moreover, after 4 wk, the ultrasound evaluation and urine culture were negative in all patients, and stent removal was possible in all cases. All patients reached at least a 6-mo follow-up; the mean follow-up was mo in group A and mo in group B. The overall objective success (measured by diuretic renal scan or intravenous urography) was 96%, with two patients in group A showing a recurrence of UPJO, whereas no objective failure was observed in the patients in group B. The two cases with recurrence of UPJO were successfully treated with open pyeloplasty (one patient) or endopyelotomy (one patient) 6 mo after the robotic procedure. 4. Discussion Although dismembered open Anderson-Hynes pyeloplasty shows high success rates, its morbidity is not negligible. Over the last few years, technological advances have allowed the introduction of minimally invasive (endoscopic and laparoscopic) techniques with the aim of maintaining the same functional results of classic open surgery and reducing morbidity. Endoscopic approaches were initially promising, but unfortunately the long-term success rates were lower than those reported for open pyeloplasty [22]. The success rate of endopyelotomy was 33.9% in patients with crossing vessels. A greater risk of developing fibrosis and subsequent restenosis was also prevalent [23] even though the success rates had increased in peculiar clinical conditions such as a high ureteral insertion. LP proved to duplicate the open technique, and long-term results were equivalent to those of open surgery [6 8]. Although experience and training have resulted in shorter operative times and lower complications, the major disadvantage of the LP is the fact that it is technically more challenging due to the high proficiency level needed for intracorporeal suturing [24,25]. The introduction of the da Vinci robotic system in the urologic field has expanded the breadth of UPJO repair yet at the same time has preserved the benefits of minimally invasive techniques, allowing the novice laparoscopist to perform UPJO surgery reproducibly and with short learning curves [26]. RAP is predominantly performed using the transperitoneal approach because of the bulky aspect of the da Vinci system and the friendlier vision of anatomy for the laparoscopists of the intraperitoneal anatomy [12 15]. Ten cases of retroperitoneal dismembered RAP in the adult population have only recently been reported by Kaouk et al [17], although it had already been described in the pediatric population by Olsen and Jorgensen [16]. The advantages of the retroperitoneal approach may be (1) direct access to the target structures, (2) minimized risk of injury to intraperitoneal organs, and (3) allowance for a conservative treatment in urinary fistula cases or anastomotic leakage because urine does not come into contact with the peritoneal cavity and organs. Furthermore, it may be used successfully in morbidly obese patients with body mass index >30 because the full flank position and the flexion of the surgical table allow for an anterior passage through both the subcutaneous and abdominal fat. This facilitates the surgical procedure compared with the transperitoneal approach. Nevertheless, retroperitoneoscopy has some disadvantages; the proper recognition of anatomic landmarks can be more difficult. especially at the beginning of the retroperitoneoscopic experience. The surgical field may become reduced compared with the transperitoneal approach and subsequently with the potential closeness of the operative ports. Finally, with the retroperitoneal approach it can be more difficult to properly judge the role of a crossing vessel in the obstruction and whether the vessel must be decrossed or not, especially at the beginning of the experience. The RAP technique continues to develop, and some variations of this technique deserve to be mentioned. For example, using the retroperitoneal approach, the robot positioning in our series differs from the pediatric technique [18] because it enters anteriorly and from the head of the patient rather than from the back. This allows adequate space at the level of the surgical field so the assistant can work comfortably during the entire procedure. Kaouk et al reported a similar position, although port placement is slightly different because the assistant port is positioned anteriorly [17]. In our experience, we found the assistant trocar positioned more posteriorly may reduce the risk of conflicts with the robotic arm system during the procedure. Currently, the transperitoneal approach of the robot and port placement technique is well described, and the various
7 EUROPEAN UROLOGY 58 (2010) authors report a similar technique in their series. We suggest a cranial positioning of the assistant port to ease the antegrade stent positioning. Among the elective indications for a transperitoneal approach, there is redo pyeloplasty in cases of UPJO recurrence after open pyeloplasty or LP. The transperitoneal approach allows for a wider operative field and a friendlier approach compared with the retroperitoneal one in cases of surgical repair of previously failed pyeloplasty [27]. Hemal et al supported the use of robot-assisted redo LP because it allows meticulous dissection, better delineation of the previous scarred tissue, preservation of the periureteral sheath containing blood supply to the ureter, clean and fine fashioning of ureteral and pelvic flaps, and finally, a watertight anastomosis with fine sutures [27]. In our experience, patients with failed endopyelotomy can be successfully treated with both the retroperitoneal and transperitoneal approaches without experiencing particular difficulties or disadvantages of one approach compared with the other. It has been reported that 38 71% of patients with UPJO have crossing vessels, although these vessels were noted in only 20% of patients with a normal UPJ [28]. Nevertheless, significant controversy persists regarding UPJO management in the presence of crossing vessels and the importance of crossing vessels in the outcome of surgical treatment. Traditionally, dismembered pyeloplasty with transposition of the UPJ anastomosis to the anterior side of the crossing vessel has been the conventional treatment. However, it is improbable that the crossing vessel alone can cause a real UPJO because the real etiology is typically a primary lesion of the UPJ that causes dilation and ballooning of the renal pelvis over the aberrant vessel, thus worsening the clinical status. We have found that it is possible to transpose the ureter even with the retroperitoneal approach. The EndoWrist and robotic technology allow for an adequate plasty reconfiguration even in challenging conditions. When the retroperitoneoscopic approach is performed, the kidney is pushed medially and anteriorly during the ancillary maneuvers for retroperitoneal cavity creation. However, the transperitoneal approach for UPJ cases makes it much easier to judge whether the crossing vessel should be decrossed or not during the procedure because the kidney is left untouched in its anatomic position. Even though some surgeons use retrograde stenting to prevent stent malpositioning, we prefer using an anterograde stenting. Mufarrij et al [26] reported that only 6 of 99 patients who were stented anterogradely required ureteroscopy to reposition the stents, which led to increased anesthesia time and a risk of manipulation or disruption of the reconstructed UPJ. In three of our patients treated with the retroperitoneal approach, the anterograde positioning of the stent was not possible due to some difficulties. In those cases a flexible cystoscope was used using retrograde positioning, avoiding patient repositioning during the procedure as well as avoiding a significant increase of operative time. Due to the limited working field offered by the retroperitoneal route, our experience shows that the anterograde stent positioning appears easier with the transperitoneal approach compared with the anterograde stent positioning in the retroperitoneal approach. Moreover, the typical cranial position of the assistant port in the transperitoneal approach (although this port positioning may create some conflicts during the dissection phase of the procedure on the right side for a right-handed surgeon) eases the anterograde stent positioning compared with the more posterior and caudal position of the assistant port in the retroperitoneal approach. We experienced two cases of UPJO recurrence. Both cases were in the retroperitoneal group and were diagnosed at a 6-mo follow-up. Failures occurred in the first 10 patients. One case was related to an unrecognized crossing vessel (the one treated with open surgery due to the patient refusing a new laparoscopic procedure); in the other, an endopyelotomy was sufficient to widely open the stenotic ring. After a review of imaging and audio recording of the procedure, we do not think that the failures were correlated to technical suturing problems or the reduced working field offered by the retroperitoneal approach. The main limitation of our study was the short follow-up due to the evolution from one technique to another. Despite the fact that failures after 6 mo are rare, according to our observations and the observations of Inagaki et al, longer follow-up is mandatory [29]. 5. Conclusions RAP performed either retroperitoneally or transperitoneally was shown to be a feasible and reproducible surgical option for the treatment of UPJO, offering a subjective optimal plasty reconfiguration at short follow-up. Author contributions: Andrea Cestari had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Cestari, Guazzoni, Lazzeri. Acquisition of data: Cestari, Lista. Analysis and interpretation of data: Cestari, Guazzoni, Buffi, Lazzeri. Drafting of the manuscript: Cestari, Buffi, Guazzoni, Lazzeri. Critical revision of the manuscript for important intellectual content: Guazzoni. Statistical analysis: Lazzeri. Obtaining funding: None. Administrative, technical, or material support: None. Supervision: Rigatti. Other (video editing): Buffi, Fabbri, Scapaticci, Sangalli. Financial disclosures: I certify that all conflicts of interest, including specific financial interests and relationships and affiliations relevant to the subject matter or materials discussed in the manuscript (eg, employment/ affiliation, grants or funding, consultancies, honoraria, stock ownership or options, expert testimony, royalties, or patents filed, received, or pending), are the following: None. Funding/Support and role of the sponsor: None. Acknowledgment statement: The authors acknowledge Amy Sussman for linguistic revision of the manuscript and Francesca Cerruti from AB Medica Italy for her great help during the film recording and editing.
8 718 EUROPEAN UROLOGY 58 (2010) Appendix A. Supplementary data The Surgery in Motion video accompanying this article can be found in the online version at doi: /j.eururo and via Subscribers to the printed journal will find the Surgery in Motion DVD enclosed. References [1] Schuessler WW, Grune MT, Tecuanhuey LV, Preminger GM. Laparoscopic dismembered pyeloplasty. J Urol 1993;150: [2] Munver R, Sosa RE, del Pizzo JJ. Laparoscopic pyeloplasty: history, evolution and future. J Endourol 2004;18: [3] Turk IA, Davis JW, Winklemann B, et al. Laparoscopic dismembered pyeloplasty the method of choice in the presence of an enlarged renal pelvis and crossing vessels. Eur Urol 2002;42: [4] Jarrett TW, Chand DY, Charambura TC, Fugita O, Kavoussi LR. Laparoscopic pyeloplasty: the first 100 cases. J Urol 2002;167: [5] Bachmann A, Ruszat R, Forster T, et al. Retroperitoneoscopic pyeloplasty for uretropelvic junction obstruction (UPJO): solving the technical difficulties. Eur Urol 2006;49: [6] Brooks JD, Kavoussi LR, Preminger GM, Schessler WW. Comparison of open and endourological approaches to the obstructed ureteropelvic junction. Urology 1995;46: [7] Bauer JJ, Bishoff JT, Moore RG, Chen RN, Iverson AJ, Kavoussi LR. Laparoscopic versus open pyeloplasty: assessment of objective and subjective outcome. J Urol 1999;162: [8] Klingler HC, Remzi M, Janetschek G, Kratzik C, Marberger MJ. Comparison of open versus laparoscopic pyeloplasty techniques in treatmentof uretero-pelvicjunctionobstruction. Eur Urol 2003;44: [9] Moore RG, Avercch TD, Schulam PG, Adams JB, Chen RN, Kavoussi LR. Laparoscopic pyeloplasty: experience with the initial 30 cases. J Urol 1997;157: [10] Pardalidis NP, Papatsoris AG, Kosmaoglou EV. Endoscopic and laparoscopic treatment of ureteropelvic junction obstruction. J Urol 2002;168: [11] Eden C, Gianduzzo T, Chang C, Thiruchelvam N, Jones A. Extraperitoneal laparoscopic pyeloplasty for primary and secondary ureteropelvic junction obstruction. J Urol 2004;172: [12] Patel V. Robotic-assisted laparoscopic dismembered pyeloplasty. Urology 2005;66:45 9. [13] Gettman MT, Neururer R, Bartsch G, Peschel R. Anderson-Hynes dismembered pyeloplasty performed using the da Vinci robotic system. Urology 2002;60: [14] Hubert J. Robotic pyeloplasty. Curr Urol Rep 2003;4: [15] Badwan K, Bhayani S. Robotic pyeloplasty: a critical appraisal. Int J Med Robotics Comput Assist Surg 2007;3:20 2. [16] Olsen LH, Jorgensen TM. Computer assisted pyeloplasty in children: the retroperitoneal approach. J Urol 2004;171: [17] Kaouk JH, Afron J, Parekattil S, et al. Is retroperitoneal approach feasible for robotic dismembered pyeloplasty: initial experience and long term results. J Endourol 2008;22: [18] Barkun JS, Aronson JK, Feldman LS, et al. Evaluation and stages of surgical innovations. Lancet 2009;374: [19] Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240: [20] Cestari A, Guazzoni G, Naspro R, et al. Original dissecting balloon for retroperitoneal laparoscopy: cost-effective alternative to commercially available device. J Endourol 2007;21: [21] Anderson JC, Hynes W. Plastic operation for hydronephrosis. Proc R Soc Med 1951;44:4 5. [22] Uberoi J, Disick GI, Munver R. Minimally invasive surgical management of pelvic-ureteric junction obstruction: update on the current status of robotic-assisted pyeloplasty. BJU Int 2009;104: [23] Van Cangh PJ, Nesa S, Galeon M, et al. Vessels around the ureteropelvic junction: significance and imaging by conventional radiology. J Endourol 1996;10: [24] Frede T, Stock C, Renner C, Budair Z, Abdel-Salam Y, Rassweiler J. Geometry of laparoscopic suturing and knotting techniques. J Endourol 1999;13: [25] Frede T, Stock C, Rassweiler JJ, Alken P. Retroperitoneoscopic and laparoscopic suturing: tips and strategies for improving efficiency. J Endourol 2000;14: [26] Mufarrij PW, Woods M, Shah OD, et al. Robotic dismembered pyeloplasty: a 6-year, multi-institutional experience. J Urol 2008;180: [27] Hemal AK, Mishra S, Mukharjee S, Suryavanshi M. Robot assisted laparoscopic pyeloplasty in patients of ureteropelvic junction obstruction with previously failed open surgical repair. Int J Urol 2008; 15: [28] Zeltser IS, Liu JB, Bagley DH. The incidence of crossing vessels in patients with normal ureteropelvic junction examined with endoluminal ultrasound. J Urol 2004;172: [29] Inagaki T, Rha KH, Ong AM, Kavoussi LR, Jarrett TW. Laparoscopic pyeloplasty: current status. BJU Int 2005;95:102 5.
Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic Single-Site (R-LESS) Pyeloplasty Using a New Single-Port Platform
 EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
Hydronephrosis after retroperitoneal laparoscopic. dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction.
 101 original paper TRAUMA AND RECONSTRUCTIVE UROLOGY Hydronephrosis after retroperitoneal laparoscopic dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction:
101 original paper TRAUMA AND RECONSTRUCTIVE UROLOGY Hydronephrosis after retroperitoneal laparoscopic dismembered Anderson Hynes pyeloplasty in adult patients with ureteropelvic junction obstruction:
Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience
 LAPAROSCOPIC UROLOGY Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience Zhen-yu Ou, Jin-bo Chen, Zhi Chen, Min-feng Chen,
LAPAROSCOPIC UROLOGY Retroperitoneoscopic Dismembered Pyeloplasty for Ureteropelvic Junction Obstruction: Modification of the Procedure and Our Experience Zhen-yu Ou, Jin-bo Chen, Zhi Chen, Min-feng Chen,
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
ORIGINAL ARTICLES Endourology
 Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique
 Original paper Videosurgery Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique Tomasz Szydelko 1, Wojciech Apoznanski 2, Piotr Koleda
Original paper Videosurgery Laparoscopic pyeloplasty with cephalad translocation of the crossing vessel a new approach to the Hellström technique Tomasz Szydelko 1, Wojciech Apoznanski 2, Piotr Koleda
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe Kidneys
 Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in Adults: 6 Years Experience in One Center
 Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
Surgery Illustrated Surgical Atlas
 Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
Surgery Illustrated SURGERY ILLUSTRATEDMURPHY ET AL MURPHY ET AL. BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Robotically assisted laparoscopic pyeloplasty Declan Murphy, Ben Challacombe,
Although open surgery has stood the test of time for
 JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 463 467 DOI: 10.1089=end.2008.0208 Laparoscopic Pyeloplasty: Our New Gold Standard Stephanie J. Symons, M.D., Parag S.
JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 463 467 DOI: 10.1089=end.2008.0208 Laparoscopic Pyeloplasty: Our New Gold Standard Stephanie J. Symons, M.D., Parag S.
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Study of laparoscopic retroperitoneal pyeloplasty
 International Surgery Journal Gajbhiye R et al. Int Surg J. 2015 Feb;2(1):53-59 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: 10.5455/2349-2902.isj20150210 Study of laparoscopic
International Surgery Journal Gajbhiye R et al. Int Surg J. 2015 Feb;2(1):53-59 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: 10.5455/2349-2902.isj20150210 Study of laparoscopic
ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD
 ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD Chairman, The Departments of Urology & Pediatric Urology, Shaare Zedek Medical Center
ROBOTIC ASSISTED LAPAROSCOPIC PYELOPLASTY (RALP) Does The Patients Weight Effect The Surgical Results? Boris Chertin MD Chairman, The Departments of Urology & Pediatric Urology, Shaare Zedek Medical Center
Original Article. Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice
 Original Article www.jpgmonline.com Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice Bryant RJ, Craig E, Oakley N Department of Urological Surgery,
Original Article www.jpgmonline.com Laparoscopic pyeloplasty: The retroperitoneal approach is suitable for establishing a de novo practice Bryant RJ, Craig E, Oakley N Department of Urological Surgery,
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic pyeloplasty Introduction This overview has been prepared to assist members
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic pyeloplasty Introduction This overview has been prepared to assist members
Copyright r 2015 Annals of Pediatric Surgery. Unauthorized reproduction of this article is prohibited.
 Original article 231 Transperitoneal laparoscopic pyeloplasty in children and adolescents: long-term results Abdelbaset A.E. Elemam a, Rafik Shalaby b, Magid Ismail b, Mohamad Shahen b, Refaat Ibrahim
Original article 231 Transperitoneal laparoscopic pyeloplasty in children and adolescents: long-term results Abdelbaset A.E. Elemam a, Rafik Shalaby b, Magid Ismail b, Mohamad Shahen b, Refaat Ibrahim
Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical team experience with 38 cases
 ORIGINAL ARTICLE Vol. 43 (3): 512-517, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0198 Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical
ORIGINAL ARTICLE Vol. 43 (3): 512-517, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0198 Laparoscopic management of recurrent ureteropelvic junction obstruction following pyeloplasty: a single surgical
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty?
 Turk J Urol 2017; 43(4): 497-501 DOI: 10.5152/tud.2017.77775 LAPAROSCOPY Original Article 497 Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty? Mustafa Suat Bolat,
Turk J Urol 2017; 43(4): 497-501 DOI: 10.5152/tud.2017.77775 LAPAROSCOPY Original Article 497 Does antegrade JJ stenting affect the total operative time during laparoscopic pyeloplasty? Mustafa Suat Bolat,
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal Approach During the Learning Curve
 JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study
 466 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study Omar Fahmy 1, Abdel-Rahman El-Fayoumi
466 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY Role of laparoscopy in ureteropelvic junction obstruction with concomitant pathology: a case series study Omar Fahmy 1, Abdel-Rahman El-Fayoumi
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Facing Surgery. for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option
 Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
The Management of Ureteropelvic Junction Obstruction Presenting with Prenatal Hydronephrosis
 Review Special Issue: Pre- and Postnatal Management of Hydronephrosis TheScientificWorldJOURNAL (2009) 9, 400 403 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.51 The Management of Ureteropelvic Junction
Review Special Issue: Pre- and Postnatal Management of Hydronephrosis TheScientificWorldJOURNAL (2009) 9, 400 403 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.51 The Management of Ureteropelvic Junction
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
 ORIGINAL Article Vol. 39 (2): 195-202, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.07 Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
ORIGINAL Article Vol. 39 (2): 195-202, March - April, 2013 doi: 10.1590/S1677-5538.IBJU.2013.02.07 Minimally Invasive Pyeloplasty in Horseshoe Kidneys with Ureteropelvic Junction obstruction: A case series
International Journal of Sciences & Applied Research. Management of PUJ obstruction IJSAR, 2(2), 2015; 22-31
 International Journal of Sciences & Applied Research www.ijsar.in Management of PUJ obstruction Chugh A.*, Agarwal P.N., Singh R., Mishra A., Jain V., Meena M. Dept of General Surgery, MAMC. Correspondence
International Journal of Sciences & Applied Research www.ijsar.in Management of PUJ obstruction Chugh A.*, Agarwal P.N., Singh R., Mishra A., Jain V., Meena M. Dept of General Surgery, MAMC. Correspondence
TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
 Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
 Int J Clin Exp Med 2016;9(5):8587-8592 www.ijcem.com /ISSN:1940-5901/IJCEM0017894 Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
Int J Clin Exp Med 2016;9(5):8587-8592 www.ijcem.com /ISSN:1940-5901/IJCEM0017894 Original Article Application of dual-knot continuous suture technique in retroperitoneal laparoscopic dismembered pyeloplasty
Mini incision open pyeloplasty - Improvement in patient outcome
 ORIGINAL ARTICLE Vol. 41 (5): 927-934, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0024 Mini incision open pyeloplasty - Improvement in patient outcome Vishwajeet Singh 1, Manish Garg 1,
ORIGINAL ARTICLE Vol. 41 (5): 927-934, September - October, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0024 Mini incision open pyeloplasty - Improvement in patient outcome Vishwajeet Singh 1, Manish Garg 1,
Robotics, Laparoscopy & Endosurgery
 Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients
 Review Article Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients Francesco Turrà 1, Maria Escolino 1, Alessandra Farina 1, Alessandro Settimi 1, Ciro Esposito 1, François
Review Article Pyeloplasty techniques using minimally invasive surgery (MIS) in pediatric patients Francesco Turrà 1, Maria Escolino 1, Alessandra Farina 1, Alessandro Settimi 1, Ciro Esposito 1, François
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Laparoscopic Radical Nephrectomy- the current gold standard
 Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
A Comparison of Laparoscopic Pyeloplasty Performed with the davinci Robotic System versus Standard Laparoscopic Techniques: Initial Clinical Results
 European Urology European Urology 42 (2002) 453±458 A Comparison of Laparoscopic Pyeloplasty Performed with the davinci Robotic System versus Standard Laparoscopic Techniques: Initial Clinical Results
European Urology European Urology 42 (2002) 453±458 A Comparison of Laparoscopic Pyeloplasty Performed with the davinci Robotic System versus Standard Laparoscopic Techniques: Initial Clinical Results
URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Pelvioureteric junction obstruction of the lower collecting system associated with incomplete ureteral duplication: A case report
 Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports
 Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours
 Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
Surgical Atlas The posterior lumbotomy
 Original Article SURGERY ILLUSTRATED PANSADORO Surgical Atlas The posterior lumbotomy VITO PANSADORO Urology, Vincenzo Pansadoro Foundation, Rome, Italy ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
Original Article SURGERY ILLUSTRATED PANSADORO Surgical Atlas The posterior lumbotomy VITO PANSADORO Urology, Vincenzo Pansadoro Foundation, Rome, Italy ILLUSTRATIONS by STEPHAN SPITZER, www.spitzer-illustration.com
Laparoscopic Nephroureterectomy for Upper Tract Transitional Cell Carcinoma: Comparison of Laparoscopic and Open Surgery
 european urology 49 (2006) 332 336 available at www.sciencedirect.com journal homepage: www.europeanurology.com Laparoscopy Laparoscopic Nephroureterectomy for Upper Tract Transitional Cell Carcinoma:
european urology 49 (2006) 332 336 available at www.sciencedirect.com journal homepage: www.europeanurology.com Laparoscopy Laparoscopic Nephroureterectomy for Upper Tract Transitional Cell Carcinoma:
BJUI. Robotic nephrectomy for the treatment of benign and malignant disease
 . JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
. JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
Chapter 2. Simple Nephrectomy. Please Give Three Tips for Laparoscopic Simple Nephrectomy. Dr. de la Rosette
 Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Department of Urology, Columbia University School of Medicine, New York, NY
 Laparoscopic Partial Nephrectomy Jaime Landman, MD Associate Professor of Urology Director of Minimally Invasive Urology Columbia University Department of Urology Department of Urology, Columbia University
Laparoscopic Partial Nephrectomy Jaime Landman, MD Associate Professor of Urology Director of Minimally Invasive Urology Columbia University Department of Urology Department of Urology, Columbia University
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors
 Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Circumcaval Ureter: Embryology
 european urology supplements 5 (2006) 444 448 available at www.sciencedirect.com journal homepage: www.europeanurology.com Circumcaval Ureter: Embryology Arianna Lesma *, Aldo Bocciardi, Patrizio Rigatti
european urology supplements 5 (2006) 444 448 available at www.sciencedirect.com journal homepage: www.europeanurology.com Circumcaval Ureter: Embryology Arianna Lesma *, Aldo Bocciardi, Patrizio Rigatti
Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants
 Hydronephrosis Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants Eduardo Ruiz, Ricardo Soria, Edurne Ormaechea, Mauricio Marcelo Urquizo
Hydronephrosis Simplified Open Approach to Surgical Treatment of Ureteropelvic Junction Obstruction in Young Children and Infants Eduardo Ruiz, Ricardo Soria, Edurne Ormaechea, Mauricio Marcelo Urquizo
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Original Article A novel approach to locate renal artery during retroperitoneal laparoendoscopic single-site radical nephrectomy
 Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Ostruzione pieloureterale polari anomali «hitching technique»
 Ostruzione pieloureterale da vasi polari anomali «hitching technique» S.F. Chiarenza dept. pediatric AND UROLOGIC surgery s.bortolo hospital vicenza italy ITALY 1949 Hellstrom : trasposition polar vessels
Ostruzione pieloureterale da vasi polari anomali «hitching technique» S.F. Chiarenza dept. pediatric AND UROLOGIC surgery s.bortolo hospital vicenza italy ITALY 1949 Hellstrom : trasposition polar vessels
Minimally invasive surgery in urology oncology. Dr. Tongchai Nakamont 23 Jan 2014
 Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Identifying unrecognized collecting system entry and the integrity of repair during open partial nephrectomy: comparison of two techniques
 ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
ENDOPYELOTOMY WITH THE ACUCISE CATHETER
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 302-310, July - August, 2002 ENDOPYELOTOMY WITH THE ACUCISE CATHETER ARTUR H. BRITO, ANUAR I.
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 302-310, July - August, 2002 ENDOPYELOTOMY WITH THE ACUCISE CATHETER ARTUR H. BRITO, ANUAR I.
Downloaded from Medico Research Chronicles Pelvi-ureteric junction obstruction - A ten year single center review in north central Nigeria.
 PELVI-URETERIC JUNCTION OBSTRUCTION - A TEN YEAR SINGLE CENTER REVIEW IN NORTH CENTRAL NIGERIA. 1,2 1,2 1 1 Atim T, Aisuodionoe-Shadrach O, Ajibola O. H, Magnus F. E Division of Urology, Departments of
PELVI-URETERIC JUNCTION OBSTRUCTION - A TEN YEAR SINGLE CENTER REVIEW IN NORTH CENTRAL NIGERIA. 1,2 1,2 1 1 Atim T, Aisuodionoe-Shadrach O, Ajibola O. H, Magnus F. E Division of Urology, Departments of
Pattern of Renal Function Deterioration as a Predictive Factor of Unilateral Ureteropelvic Junction Obstruction Treatment
 european urology 51 (2007) 551 555 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pediatric Urology Pattern of Renal Function Deterioration as a Predictive Factor of Unilateral
european urology 51 (2007) 551 555 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pediatric Urology Pattern of Renal Function Deterioration as a Predictive Factor of Unilateral
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment
 Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy, and Robot-Assisted Pyeloplasty in a Developing Nation
 Hindawi Publishing Corporation Advances in Urology Volume 2014, Article ID 850156, 6 pages http://dx.doi.org/10.1155/2014/850156 Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy,
Hindawi Publishing Corporation Advances in Urology Volume 2014, Article ID 850156, 6 pages http://dx.doi.org/10.1155/2014/850156 Clinical Study Defining the Pros and Cons of Open, Conventional Laparoscopy,
RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES
 1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach
 CASE REPORT Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach Nand Kishore Arvind, Onkar Singh, Shilpi Singh Gupta ABSTRACT Background and Objectives: Testicular vein syndrome (TVS)
CASE REPORT Testicular Vein Syndrome and Its Treatment with a Laparoscopic Approach Nand Kishore Arvind, Onkar Singh, Shilpi Singh Gupta ABSTRACT Background and Objectives: Testicular vein syndrome (TVS)
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
Outcomes of Re-Intervention for Laparoscopic Transperitoneal Pyeloplasty in Children. Leung, L; Chan, HYI; Chung, HY; Lan, CLL; Wong, KKY; Tam, PKH
 Title Outcomes of Re-Intervention for Laparoscopic Transperitoneal Pyeloplasty in Children Author(s) Leung, L; Chan, HYI; Chung, HY; Lan, CLL; Wong, KKY; Tam, PKH Citation Journal of Laparoendoscopic &
Title Outcomes of Re-Intervention for Laparoscopic Transperitoneal Pyeloplasty in Children Author(s) Leung, L; Chan, HYI; Chung, HY; Lan, CLL; Wong, KKY; Tam, PKH Citation Journal of Laparoendoscopic &
G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve.
 G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. ANTENATAL HYRONEPHROSIS UROLOGICAL ASPECTS Dr Gianantonio Manzoni, FEAPU FRCS U.O.
G.Manzoni has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. ANTENATAL HYRONEPHROSIS UROLOGICAL ASPECTS Dr Gianantonio Manzoni, FEAPU FRCS U.O.
NIH Public Access Author Manuscript Eur Urol. Author manuscript; available in PMC 2009 March 1.
 NIH Public Access Author Manuscript Published in final edited form as: Eur Urol. 2008 March ; 53(3): 514 521. doi:10.1016/j.eururo.2007.09.047. ROBOTIC PARTIAL NEPHRECTOMY FOR COMPLEX RENAL TUMORS: SURGICAL
NIH Public Access Author Manuscript Published in final edited form as: Eur Urol. 2008 March ; 53(3): 514 521. doi:10.1016/j.eururo.2007.09.047. ROBOTIC PARTIAL NEPHRECTOMY FOR COMPLEX RENAL TUMORS: SURGICAL
Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon
 Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Weill Medical College of Cornell
Robotic Surgery for Prostate Cancer: A Realistic Approach to Getting Started The Evolution of a Robotic Surgeon Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Weill Medical College of Cornell
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Training Course for Advanced Oncologic Laparoscopy. Robotic Urology. Ch.-H. Rochat Geneva
 Training Course for Advanced Oncologic Laparoscopy Robotic Urology Ch.-H. Rochat Geneva St Petersbourg 16 February 2006 Urology and mini-invasive surgery radical prostatectomy nephrectomy (partial or total)
Training Course for Advanced Oncologic Laparoscopy Robotic Urology Ch.-H. Rochat Geneva St Petersbourg 16 February 2006 Urology and mini-invasive surgery radical prostatectomy nephrectomy (partial or total)
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
Forgotten JJ stent: A rare case report
 Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET
 LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Hydronephrosis. Nephrosis. Refers to the kidney
 What is hydronephrosis? Hydro Nephrosis Refers to water or fluid Refers to the kidney A build-up of fluid (urine) in the kidney is the medical term for a build-up of urine in the kidney. As the urine builds
What is hydronephrosis? Hydro Nephrosis Refers to water or fluid Refers to the kidney A build-up of fluid (urine) in the kidney is the medical term for a build-up of urine in the kidney. As the urine builds
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy
 A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy BY JUNYA TSURUKIRI, HIDEFUMI SANO, YOSUKE TANAKA, TAKAO SATO, HIROKAZU TAGUCHI Abstract An 18-year-old
A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy BY JUNYA TSURUKIRI, HIDEFUMI SANO, YOSUKE TANAKA, TAKAO SATO, HIROKAZU TAGUCHI Abstract An 18-year-old
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments
 Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Complication of long indwelling urinary catheter and stent COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT
 151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair
 Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair Pankaj P. Dangle, James Kearns, Blake Anderson and Mohan S. Gundeti* From the Department of Surgery, Division
Outcomes of Infants Undergoing Robot-Assisted Laparoscopic Pyeloplasty Compared to Open Repair Pankaj P. Dangle, James Kearns, Blake Anderson and Mohan S. Gundeti* From the Department of Surgery, Division
Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis
 Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis Abstract M. Naeem,K. Anwar ( Department of Urology, Pakistan Institute of Medical Sciences, Islamabad. ) Objective:
Latrogenic Injuries of Renal Pelvis and Ureter Following Open Surgery for Urolithiasis Abstract M. Naeem,K. Anwar ( Department of Urology, Pakistan Institute of Medical Sciences, Islamabad. ) Objective:
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Lecture 56 Kidney and Urinary System
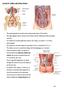 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
HOW I DO IT. Introduction and patient selection. Surgical technique, see Table 1 for key points
 HOW I DO IT Ureteric re-implant for the strictured renal allograft: How I do it Thomas McGregor, MD, 1 Tadeuz Kroczak, MD, 1 Chun Huang, MD, 1 Joshua Koulack, MD 2 1 Division of Urology, Department of
HOW I DO IT Ureteric re-implant for the strictured renal allograft: How I do it Thomas McGregor, MD, 1 Tadeuz Kroczak, MD, 1 Chun Huang, MD, 1 Joshua Koulack, MD 2 1 Division of Urology, Department of
Objectives. Pelvic Anatomy: Staying Out of Trouble. Disclosures. Anatomy 101. Anterior Abdominal Wall. Arcuate Line. Abheha Satkunaratnam MD, FRCS(C)
 Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Objectives Pelvic Anatomy: Staying Out of Trouble Abheha Satkunaratnam MD, FRCS(C) To focus on key anatomy for the gynaecologic surgeon advancing their minimally invasive gynaecologic skills To provide
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
A Comparative Study between Open and Laparoscopic Pyeloplasty
 A Comparative Study between Open and Laparoscopic Pyeloplasty Ali Hamdan Fahad College of Medicine, University of Al-Qadisiyah, Iraq Abstract: Background: Historically open pyeloplasty has been regarded
A Comparative Study between Open and Laparoscopic Pyeloplasty Ali Hamdan Fahad College of Medicine, University of Al-Qadisiyah, Iraq Abstract: Background: Historically open pyeloplasty has been regarded
Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor Thrombectomy
 EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
Percutaneous nephrolithotomy (PCNL), as primary. Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy. Case Report
 JOURNAL OF ENDOUROLOGY CASE REPORTS Volume 3.1, 2017 Mary Ann Liebert, Inc. Pp. 52 56 DOI: 10.1089/cren.2017.0011 Case Report Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy Eugenio Di Grazia,
JOURNAL OF ENDOUROLOGY CASE REPORTS Volume 3.1, 2017 Mary Ann Liebert, Inc. Pp. 52 56 DOI: 10.1089/cren.2017.0011 Case Report Subcapsular Kidney Urinoma After Percutaneous Nephrolithotomy Eugenio Di Grazia,
Role of imaging in evaluation of genitourinary i trauma Spectrum of GU injuries Relevance of imaging findings in determining management Focus on MDCT
 Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
