Chapter 121 Anemia, Polycythemia, and White Blood Cell Disorders
|
|
|
- Aubrey Miller
- 5 years ago
- Views:
Transcription
1 Chapter 121 Anemia, Polycythemia, and White Blood Cell Disorders Episode overview 1. Outline the important aspects of the history and physical for clinically severe and non-emergent anemia 2. List 6 causes of rapid intravascular red blood cell destruction 3. List the admission criteria for nonemergent anemia 4. Classify the anemias according to MCV 5. What is the differential diagnosis of normocytic anemia? 6. What are the 3 different types of thalassemia? 7. What is the underlying pathophysiology of sideroblastic anemia? List causes of sideroblastic anemia 8. List 3 causes of B12 deficiency) and 3 causes of folate deficiency 9. List 3 drugs that can cause aplastic anemia 10. List 4 intrinsic and 4 extrinsic causes of hemolytic anemia 11. List two RBC enzyme deficiencies. How do they typically present? 12. What is the pathophysiology of G6PD? What triggers G6PD symptoms? 13. List 5 drugs that cause hemolysis in G6PD 14. List 5 causes and 4 drugs of autoimmune hemolytic anemia 15. Describe what to look for on history and physical exam in consideration of hemolytic anemia. What are at least 6 lab tests diagnostic for hemolysis? 16. What are the laboratory differences between intravascular and extravascular hemolysis? Which types of hemolytic anemia tend to be intravascular? Which are extravascular? 17. What is the pathophysiology of sickle cell disease? 18. Which presentations of sickle cell disease are associated with a sudden decrease in hemoglobin? 19. List potential end-organ complications of sickle cell disease by system 20. Describe the management of a sickle cell pain crisis 21. Describe the management of a sickle cell chest crisis 22. List 5 complications of sickle cell disease and their management 23. List 5 causes of apparent and secondary polycythemia 24. How might polycythemia present in the ED? What are the types of polycythemia? How is this condition managed? 25. List 6 causes of leukocytosis and 3 causes of lymphocytosis 26. List 5 causes of neutrophilia + 5 causes of lymphocytosis 27. How to approach neutropenia in children? WiseCracks 1. How do you calculate the oxygen content of blood? 2. Which situations shift the oxygen-dissociation curve to the left? To the right? What is the significance of a leftward shift? 3. List 6 causes of anemia from production (review question) 4. List 4 causes of MAHA (review question) 5. What organ damage is seen in sickle cell disease (table 112.8)
2 6. What is leukostasis? 7. How is neutropenia with fever managed? 8. Which type of leukemia would be most likely in the following pts and why might they present to the ED? year-old with Downs syndrome 2. Previously healthy 28-year-old year-old with chest pain noted to have increased LNs [1] Outline the important aspects of the history and physical for clinically severe and non-emergent anemia Refer to boxes and for the important aspects of the history and physical for clinically severe and non-emergent anemia Clinically Severe Anemia General History Out-of-hospital status, therapy, response to therapy? Bleeding diathesis? Any previous blood transfusions? Any underlying disease? Current meds, any platelet inhibitors Trauma History Nature and time of injury Estimated blood loss Non-trauma History Skin: petechiae, bruising Respiratory: hemoptysis, epistaxis Gastrointestinal: hematemesis, hematochezia, melena, peptic ulcer Genitourinary: LMP, menorrhagia (bleeding in-between expected periods), metrorrhagia (excessive bleeding during periods), hematuria Physical Exam Serial Vital signs (including orthostatic vitals), level/content of consciousness Skin: pallor (conjunctival, palmar creases highest LHR), diaphoresis, jaundice, cyanosis, purpura/bruising, petechiae, penetrating wounds CVS: murmurs, S3, S4 Abdomen: big spleen, tender abdomen, rectal/pelvic exam, masses, stool hemoglobin testing. Nonemergent Anemia History Symptoms of anemia (chest pain, dyspnea, decreased exercise tolerance, weakness, fatigue, syncope) Bleeding diathesis Possible sites of blood loss (resp, GI, GU, Skin) Dietary history Drug use/toxin exposure, ALCOHOL?? Racial background (Mediterranean?) / Family history Underlying diseases
3 Physical Exam Similar to emergent case exam - maybe look at the fundi for hemorrhage, check some nodes, assess neurologic positional and vibratory sense? [2] List 6 causes of rapid intravascular red blood cell destruction Refer to box for causes of rapid intravascular red blood cell destruction Causes of rapid intravascular red blood cell destruction: Mechanical hemolysis associated with DIC Massive burns Toxins (poisonous venom, brown recluse spiders, cobras!) Infection (Malaria, clostridium, mycoplasma/mononucleosis leading to cold agglutinin hemolysis) G6PD deficiency with oxidative stress (ate a fava bean!) ABO incompatibility transfusion reaction Paroxysmal nocturnal hemoglobinuria exacerbated by transfusion Immune complex hemolysis (e.g., quinidine) [3] List the admission criteria for non-emergent anemia Refer to box for admission criteria for nonemergent anemia Admissions criteria for nonemergent anemia: Developing cardiac symptoms (chest pain, SOB, altered LOC) Initial unexplained Hb <80 or hematocrit <30% Difficulty obtaining outpatient care when Hb significantly low or major comorbidity [4] Classify the anemias according to MCV Refer to box for classification of anemias according to MCV Microcytic (low MCV, hypochromic) Thalassemia Anemia of chronic disease Iron deficiency Lead poisoning Sideroblastic anemia Normocytic (normal MCV) Primary bone marrow problem: aplastic anemia, myeloid metaplasia with myelofibrosis, myelophthisic anemia Secondary to underlying disease: hypothyroid, hypoadrenal, hypopituitary, uremia, chronic inflammation, liver disease Macrocytic (high MCV) Vit B12 deficiency / Folate deficiency Liver disease Hypothyroidism [5] What is the differential diagnosis of normocytic anemia? See above
4 [6] What are the 3 different types of thalassemia? Homozygous beta-chain thalassemia (Thalassemia major) Mediterranean, severe anemia, most common single gene disoder Heterozygous beta-chain thalassemia (Thalassemia minor) Mild anemia, mostly asymptomatic Alpha-thalassemia Wide spectrum of manifestation, viable forms in Asian/Afro-Americans [7] What is the underlying pathophysiology of sideroblastic anemia? List causes of sideroblastic anemia Pathophysiology: Defect in porphyrin synthesis causes impaired Hb production leading to excess iron deposited in mitochondria of RBC precursors poor erythropoiesis (anemia) Causes of Sideroblastic Anemia: Primary: Rare sex-linked form and idiopathic in elderly with refractory anemia Secondary: Toxins, Hemolytic/megaloblastic anemia, infections, carcinoma, leukemia, rheumatoid arthritis, lead poisoning, and alcohol abuse [8] List 3 causes of B12 deficiency and 3 causes of folate deficiency Refer to box for causes of Vitamin B12 deficiency - Inadequate dietary intake (total vegan, chronic alcoholism), - Inadequate absorption (pernicious gastrectomy/anemia, abnormal ileum), - Inadequate use (enzyme deficiency, abnormal vitamin B12 binding protein) Refer to box for causes of Folate deficiency: - Inadequate dietary intake, - Inadequate absorption (Celiac sprue, blind loop syndrome, phenytoin or barbiturates), - Inadequate use (metabolic block caused by methotrexate, etc.), - Increased requirement (pregnancy, poor erythropoiesis, hemolytic anemia, chronic blood loss, lymphoproliferative diseases) [9] List 3 drugs that can cause aplastic anemia Refer to table for drugs or chemicals that can cause aplastic anemia Chloramphenicol (61% relative incidence) Phenylbutazone (19%) Anticonvulsants (4%) [10] List 4 intrinsic and 4 extrinsic causes of hemolytic anemia (Box 112.8) Refer to box for intrinsic and extrinsic causes of hemolytic anemia Intrinsic Causes of Hemolytic Anemia Enzyme defect (pyruvate kinase deficiency, G6PD deficiency) Membrane defect (spherocytosis, elliptostomatocytosis, paroxysmal nocturnal hemoglobinuria) Hemoglobin defect (Thalassemias, hemoglobin M, unstable hemoglobin, sickle cell)
5 Extrinsic Causes of Hemolytic Anemia Immunologic (allo or autoantibodies) Mechanical (Microangiopathic hemolytic anemias (MAHA), prosthetic HVs) Environmental (Drugs, toxins, infections, thermal) Abnormal sequestration hypersplenism [11] List two RBC enzyme deficiencies. How do they typically present? 1) Pyruvate kinase deficiency presents as hemolytic jaundice around infancy 2) G6PD deficiency presents as acute hemolytic episode hours after ingestion of oxidant drug/material [12] What is the pathophysiology of G6PD? What triggers G6PD symptoms? Deficiency of an enzyme in the early steps of glycolysis (glucose-6-phosphate dehydrogenase) means there isn t sufficient NADPH produced from glycolysis to maintain reduced glutathione, an essential molecule in protecting Hb from oxidative stress. Hb are then extra vulnerable to any ingested oxidant!! [13] List 5 drugs that cause hemolysis in G6PD Refer to box for drugs that cause hemolysis in G6PD Analgesics (aspirin, acetanilide) Antimalarials (Primaquine, quinacrine, quinine) Nitrofurans Sulfa drugs Miscellaneous (FAVA beans, methylene blue, phenylhydralazine) [14] List 5 causes and 4 drugs of autoimmune hemolytic anemia Refer to boxes and for disease causing AHA and drugs causing AHA Diseases causing AHA: Neoplasms (CLL, CML, lymphoma, myeloma, thymoma, ovarian teratoma) Collagen vascular disease (SLE, RA, periarteritis nodosa) Infections (Mycoplasma, syphilis, malaria, Bartonella, viruses CMV, mono, coxsackie) Miscellaneous (thyroid d/o, ulcerative colitis, drug immune reactions) Drugs causing AHA: Quinidine Sulfa drugs Penicillin dosages >20 million units/day D-methyldopa + L-dopa Cephalosporins at dosages >4g/day
6 [15] Describe what to look for on hx and physical exam in consideration for hemolytic anemia; What are at least 6 lab tests diagnostic for hemolysis? (box ) Refer to box for pertinent history and physical exam findings with hemolytic anemia History: alteration of urine colour, association with new drugs, cold, sleep, ethnic background, family history of anemia or jaundice, drug or toxin exposure, diseases associated with hemolysis (SLE, renal disease lymphoma, mono, prosthetic HVs) Physical: jaundice (scleral icterus), hepatosplenomegaly, ulcerations, enlarged lymph nodes Refer to box for diagnostic lab tests for hemolysis Peripheral blood smear Corrected retic index Haptoglobin (low=hemolysis) Plasma free Hb LDH level (high=hemolysis) Fractionated bilirubin Direct/indirect Coombs test [16] What are the laboratory differences between intravascular and extravascular hemolysis? Extravascular peripheral smear will have specific RBC morphologies suggesting etiology (bite cells, sickle cells, spherocytes, spur cells, Howell-Jolly bodies, etc.) Intravascular peripheral smear will predominantly show schistocytes (RBC fragments) [17] Which types of hemolytic anemia tend to be intravascular? Which are extravascular? Extravascular enzyme/membrane/hemoglobin defects, autoimmune hemolysis, toxins, hypersplenism Intravascular MAHA (DIC, TTP, HUS), transfusion reactions, sepsis, heat injury, paroxysmal nocturnal hemoglobinuria [18] What is the pathophysiology of sickle cell disease? Abnormal allele at gene loci for Hb beta chain relates to a single amino acid change within the beta chain and a resultant Hb chain with abnormal tertiary structure (sickled). Sickle RBCs are less deformable, increase blood viscosity, and tend to be sequestered more readily within the spleen. This pathologic process leads to vaso-occlusive crises, chronic hemolysis, and end-organ injury.
7 [19] Which presentations of sickle cell disease are associated with a sudden decrease in hemoglobin? The hemolysis phenotype genetically indeterminable from vaso-occlusive phenotype. Unknown why some present with hemolysis while others present with acute pain. [20] List potential end-organ complications of sickle cell disease by system Skin stasis ulcer CNS CVA Eye retinal hemorrhage, retinopathy Cardiac CHF Pulmonary PE, infarct, infection Vascular occlusive phenomenon ANYWHERE Liver infarct, transfusion-related hepatitis, hepatic sequestration, cholestasis Gallbladder increased bilirubin gallstone production Spleen acute sequestration Urinary hematuria, hyposthenuria Genital decreased fertility, impotence, priapism Skeletal bone infarcts, osteomyelitis, aseptic necrosis Placenta insufficiency with fetal wastage Leukocytes relative immunodeficiency Erythrocytes chronic hemolysis [21] Describe the management of a sickle cell pain crisis Acute: analgesia (patient dependent/directed) with opioids +/- NSAIDS Chronic: Hydroxyurea reduces pain crisis frequency in adults with >3 pain crises / year Cure: bone marrow transplantation (up to 90% disease-free survival rates) [22] Describe the management of a sickle cell chest crisis. Supportive management with judicial rehydration, analgesia, incentive spirometry, maintain good oxygenation/ventilation, and empiric antibiotics (similar coverage for CAP) [23] List 3 complications of sickle cell disease and their management 1) Acute stroke: exchange transfusion, tpa use in this setting is the same as for acute non-hemorrhagic stroke without sickle cell disease 2) Acute splenic sequestration: exchange transfusion, IV antibiotics against Staphylococcus and encapsulated organisms (Pneumococcus, H. influenza, Salmonella) 3) Acute chest syndrome: exchange transfusion + supportive management
8 [24] List some causes of secondary polycythemia Refer to box for causes of secondary polycythemia Appropriate response to tissue hypoxia states: congenital heart disease with R-to-L shunt, pulmonary disease, carboxyhemoglobin, high-altitude acclimatization, hemoglobinopathies with high oxygen affinity Inappropriate erythropoiesis production states: renal carcinomas, uterine fibroids, hepatoma of adrenal origin, cerebellar hemangioma, congenital overproduction, pure erythrocytosis, AIDS [25] How might polycythemia present in the ED? What are the types of polycythemia? How is this condition managed? Presentation: may vary from mild headaches to full-blown hypervolemia (vertigo, blurred vision, severe headache), hyperviscosity (venous thrombosis), and platelet dysfunction (epistaxis, spontaneous bruising, GI bleeding) Types of PV Apparent (dehydration, cigarette smoking), Primary (myeloproliferative disoder), and Secondary (carcinomas increasing erythropoietin, other conditions, see Q24) Management: phlebotomy (500ml removed and replaced with equal amount saline). Final goal for hematocrit is <55%. ASA 81mg daily has been shown to prevent thrombotic complications (acute and chronic treatment) [26] List 6 causes of leukocytosis and 3 causes of lymphocytosis Refer to box for causes of leukocytosis and lymphocytosis Causes of leukocytosis (increased WBC count) Primary: myeloproliferative disorders (CML, PV), hereditary neutrophilia Secondary: Infection, tissue necrosis (cancer, burns, infarctions), metabolic disorders (DKA, thyrotoxicosis, uremia), stress (exercise, pain, surgery, hypoxia, seizures, trauma), drugs (epinephrine, corticosteroids, lithium, cocaine), lab error Causes of lymphocytosis (increased lymphocytes) Viral (mono, rubeola, rubella, varicella, toxoplasmosis), CLL, autoimmune diseases, graft rejection, immunizations [27] How to approach neutropenia in children? Determine absolute neutrophil count (ANC) Consider etiology: decreased production, increased destruction, or sequestration. Patient more susceptible to infections. Therefore, anyone with FEVER and low ANC warrants full radiographic and direct examination for potential infectious sources and cultures obtained for sputum, urine, and blood Early involvement of appropriate specialties Empiric antibiotics
9 WiseCracks [1] How do you calculate the oxygen content of blood? Content in blood depends on the saturation level of hemoglobin plus the amount of O2 dissolved in the blood based on partial pressures of O2: CaO2 = (Hb * 1.34 * SaO2) + (PaO2 * ) Where 1g of normal Hb carries 1.36 ml of O2 [2] Which situations shift the oxygen-dissociation curve to the left? To the right? What is the significance of a leftward shift? Right Shift = Hb has decreased affinity for O2 (gives it up more readily to the tissues) Increased CO2, increased acidity (decreased ph), increased 2,3-BPG, increased temperature Basically the environment of overworked, oxygen starved tissues yields a right shift toward Hb giving up more O2 Left Shift = Hb has increased affinity for O2 (Hb gives up less O2 to tissues) Opposite factors to above list [3] List 6 causes of anemia from decreased production (review question) 1. Iron deficiency, 2. Vitamin B12/folate deficiency, 3. Aplastic anemia, 4. Myeloid metaplasia with myelofibrosis, 5. Hypoendocrine state, 6. Renal disease [4] List 5 causes of MAHA (review question) 1. DIC, 2. TTP, 3. HUS, 4. Malignant hypertension, 5. Preeclampsia [5] What organ damage is seen in sickle cell disease? Skin stasis ulcer CNS CVA Eye retinal hemorrhage, retinopathy Cardiac CHF Pulmonary PE, infarct, infection
10 Vascular occlusive phenomenon ANYWHERE Liver infarct, transfusion-related hepatitis, hepatic sequestration, cholestasis Gallbladder increased bilirubin gallstone production Spleen acute sequestration Urinary hematuria, hyposthenuria Genital decreased fertility, impotence, priapism Skeletal bone infarcts, osteomyelitis, aseptic necrosis Placenta insufficiency with fetal wastage Leukocytes relative immunodeficiency Erythrocytes chronic hemolysis [6] What is leukostasis? An extreme form of leukocytosis (WBC >100,000/microL). Characterized by abnormal intravascular WBC aggregation and clumping, seen predominantly in leukemia patients. [7] How is neutropenia with fever managed? Source identification and control (with radiography and direct investigation) Empiric antibiotics and judicial fluids Early involvement of appropriate specialists (hemo-oncologist, ID, med oncology, etc.) Many patients on chemo have been given treatment protocols by their oncologist [8] Which type of leukemia would be most likely in the following patients and why might they present to the ED? 1) 20-year-old with Downs syndrome Increased risk (500x) for subtype of AML and 20x increased risk for ALL Usually presenting early in life with hepatosplenomegaly, jaundice, leukocytosis, lots of blast cells of peripheral blood smear, anemia, and vesicopapular rash/purpura. 2) Previously healthy 28-year-old Iron deficiency anemia is the most common cause of anemia among healthy young people (especially females and those on special minimalist diets or are vegan) Fatigue, light-headedness, weakness, severe menstrual flow, hypochromic/low MCV anemia with poikilocytes on smear. 3) 70-year-old with chest pain noted to have increased LNs.
General Characterisctics
 Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009
 HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
Introduction and Approach to Anemia
 2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
Diagnostic Approach to Patients with Anemia
 J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
Peripheral Blood Smear Examination. Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital
 1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
Sickle Cell Disease. Edward Malters, MD
 Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
Approach to a pale child
 Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss
 Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
I. Definitions. V. Evaluation A. History B. Physical Exam C. Laboratory evaluation D. Bone marrow examination E. Specialty referrals
 I. Definitions II. III. Red blood cell life cycle Iron metabolism IV. Causes of anemia A. Kinetic approach 1. decreased production 2. increased destruction 3. blood loss B. Morphologic approach 1. normocytic
I. Definitions II. III. Red blood cell life cycle Iron metabolism IV. Causes of anemia A. Kinetic approach 1. decreased production 2. increased destruction 3. blood loss B. Morphologic approach 1. normocytic
Evaluation of Anemia. Md. Shafiqul Bari Associate professor (Medicine) SOMC
 Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89
 Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Factors affecting oxygen dissociation curve
 P a g e 1 Factors affecting oxygen dissociation curve As you know, hemoglobin contains 4 heme molecules that bind 4 oxygen molecules (8 atoms). These 4 heme molecules, however, do not bind oxygen all at
P a g e 1 Factors affecting oxygen dissociation curve As you know, hemoglobin contains 4 heme molecules that bind 4 oxygen molecules (8 atoms). These 4 heme molecules, however, do not bind oxygen all at
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
C. treatment with Desferal (deferoxamine mesylate USP, iron-chelating agent)
 HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
HAEMOLYTIC ANAEMIA. Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician
 HAEMOLYTIC ANAEMIA Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician Haemolysis Definition shortening of the normal red blood lifespan of 120 days Increase in unconjugated bilirubin, increased
HAEMOLYTIC ANAEMIA Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician Haemolysis Definition shortening of the normal red blood lifespan of 120 days Increase in unconjugated bilirubin, increased
Extra Notes 3. Warm. In the core (center) of the body, where the temperature is 37 C.
 Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
The Irony of Anemia How to interpret the CBC
 Jaideep Shenoi MD Hematology Oncology Northwest Medical Specialities Tacoma, WA The Irony of Anemia How to interpret the CBC March 10 th, 2018 Disclosures: Advisory Board for Pharmacyclics, Janssen, Takeda,
Jaideep Shenoi MD Hematology Oncology Northwest Medical Specialities Tacoma, WA The Irony of Anemia How to interpret the CBC March 10 th, 2018 Disclosures: Advisory Board for Pharmacyclics, Janssen, Takeda,
PCCN Review Hematology
 PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
11. An acute leukemia causing. 12. An adult patient presents with acute. 13. Anemia due to renal failure may be
 Hematology Study online at 1. A 23 year old white female has weakness, fatigue and has developed a habit of chewing ice. What are the expected findings in regard to TIBC and Ferritin? 2. A 25 year old
Hematology Study online at 1. A 23 year old white female has weakness, fatigue and has developed a habit of chewing ice. What are the expected findings in regard to TIBC and Ferritin? 2. A 25 year old
3 Ruba hussein Dr. ahmad Dr. ahmad
 3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
Diseases Of The Blood
 Diseases Of The Blood DR. Associate Professor Of Pathology Faculty Of Medicine Ain Shams University Red Blood Cells and Anemia RBC=4-6 million/mm 2 Hb=12-18 g/dl Oxygen Carrying Molecule Hemoglobin Tetramer:
Diseases Of The Blood DR. Associate Professor Of Pathology Faculty Of Medicine Ain Shams University Red Blood Cells and Anemia RBC=4-6 million/mm 2 Hb=12-18 g/dl Oxygen Carrying Molecule Hemoglobin Tetramer:
Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University
 Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University Anemias Over 30 types Myeloproliferative Neoplasm Polycythemia Leukemia AML:M6
Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University Anemias Over 30 types Myeloproliferative Neoplasm Polycythemia Leukemia AML:M6
رناد زكريا Dr. ahmad Dr. ahmad. P a g e 1
 5 رناد زكريا Dr. ahmad Dr. ahmad P a g e 1 Before we start. -This sheet was written according to section 2 s record and reviewed according to section 1 s record by Ruba Hussien with all thanks and I referred
5 رناد زكريا Dr. ahmad Dr. ahmad P a g e 1 Before we start. -This sheet was written according to section 2 s record and reviewed according to section 1 s record by Ruba Hussien with all thanks and I referred
Anemia s. Troy Lund MSMS PhD MD
 Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
RBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
SICKLE CELL DISEASE. Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH. Assistant Professor FACULTY OF MEDICINE -JAZAN
 SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
RBCs Disorders 2. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
HAEMATOLOGICAL EVALUATION OF ANEMIA. Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore
 HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
(anemia) ก hemoglobin concentration, hematocrit deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2
 ก ก. ก ก.. ก (anemia) ก hemoglobin concentration, hematocrit ก ก ก 2 Standard deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2 Hemoglobin hematocrit MCV (g/dl) (%) (fl) ( ) 0.5-1.9
ก ก. ก ก.. ก (anemia) ก hemoglobin concentration, hematocrit ก ก ก 2 Standard deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2 Hemoglobin hematocrit MCV (g/dl) (%) (fl) ( ) 0.5-1.9
Microcytic Hypochromic Anemia An Approach to Diagnosis
 Microcytic Hypochromic Anemia An Approach to Diagnosis Decreased hemoglobin synthesis gives rise to microcytic hypochromic anemias. Hypochromic anemias are characterized by normal cellular proliferation
Microcytic Hypochromic Anemia An Approach to Diagnosis Decreased hemoglobin synthesis gives rise to microcytic hypochromic anemias. Hypochromic anemias are characterized by normal cellular proliferation
Types of Anaemias and their Management. S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014
 Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Sickle Cell Disease and impact on the society
 Sickle Cell Disease and impact on the society Professor Z.A.Jeremiah Ph.D, FRCPath (London) Professor of Haematology and Blood Transfusion Science Niger Delta University, Wilberforce Island Outline What
Sickle Cell Disease and impact on the society Professor Z.A.Jeremiah Ph.D, FRCPath (London) Professor of Haematology and Blood Transfusion Science Niger Delta University, Wilberforce Island Outline What
Anemia. A case-based approach. David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017
 Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
The Evaluation and Classification of Anemia
 Case studies and research for better care To refer a patient, call. The Evaluation and Classification of Anemia A diagnostic approach BY AMANDA BRANDOW, DO, MS Anemia is defined as hemoglobin concentration
Case studies and research for better care To refer a patient, call. The Evaluation and Classification of Anemia A diagnostic approach BY AMANDA BRANDOW, DO, MS Anemia is defined as hemoglobin concentration
Faculty of Medicine Dr. Tariq Aladily
 Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Red cell disorder. Dr. Ahmed Hasan
 Red cell disorder Dr. Ahmed Hasan Things to be learned in this lecture Definition and clinical feature of anemia. Classification of anemia. Know some details of microcytic anemia Question of the lecture:
Red cell disorder Dr. Ahmed Hasan Things to be learned in this lecture Definition and clinical feature of anemia. Classification of anemia. Know some details of microcytic anemia Question of the lecture:
Examination Tests from Pathological Physiology. Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc.
 Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
It should be noted that in the initial stage, nearly all anemias are normocytic. The major primary causes of normocytic anemia are given in Table 1.
 Normocytic Anemia JOHN R. BRILL, M.D., and DENNIS J. BAUMGARDNER, M.D., University of Wisconsin Medical School, Milwaukee Clinical Campus, Milwaukee, Wisconsin Am Fam Physician. 2000 Nov 15;62(10):2255
Normocytic Anemia JOHN R. BRILL, M.D., and DENNIS J. BAUMGARDNER, M.D., University of Wisconsin Medical School, Milwaukee Clinical Campus, Milwaukee, Wisconsin Am Fam Physician. 2000 Nov 15;62(10):2255
Drop of Blood Unravels Mysteries. Prof. Salma Afrose Department of Hematology Dhaka Medical College
 Drop of Blood Unravels Mysteries Prof. Salma Afrose Department of Hematology Dhaka Medical College Peripheral Blood Film (PBF) PBF is a laboratory workup that involves cytology of Peripheral blood cell
Drop of Blood Unravels Mysteries Prof. Salma Afrose Department of Hematology Dhaka Medical College Peripheral Blood Film (PBF) PBF is a laboratory workup that involves cytology of Peripheral blood cell
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal tumors, in children, 530 531 Alkalinization, in tumor lysis syndrome, 516 Allopurinol, in tumor lysis syndrome, 515 Anaphylaxis, drug
Note: Page numbers of article titles are in boldface type. A Abdominal tumors, in children, 530 531 Alkalinization, in tumor lysis syndrome, 516 Allopurinol, in tumor lysis syndrome, 515 Anaphylaxis, drug
Hematologic changes in systemic diseases. Chittima Sirijerachai
 Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
DIC. Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated.
 Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
Interpreting the CBC. Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired
 Interpreting the CBC Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired The CBC 3 Cell Lines RBCs WBCs Platelets Assess general health Make
Interpreting the CBC Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired The CBC 3 Cell Lines RBCs WBCs Platelets Assess general health Make
Year 2004 Paper two: Questions supplied by Megan 1
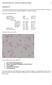 Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 93 A 16yo adolescent male presents with lethargy and lower respiratory tract infection. Physical examination shows him to be febrile, icteric
Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 93 A 16yo adolescent male presents with lethargy and lower respiratory tract infection. Physical examination shows him to be febrile, icteric
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Pediatrics. Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment. Definition. Epidemiology of Pyruvate Kinase Deficiency.
 Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Anemia In the Insurance Applicant What do the numbers mean?
 Anemia In the Insurance Applicant What do the numbers mean? Lisa Duckett, M.D. Vice President and Medical Director September 12, 2017 Goals of the presentation Develop a consistent way to analyze Complete
Anemia In the Insurance Applicant What do the numbers mean? Lisa Duckett, M.D. Vice President and Medical Director September 12, 2017 Goals of the presentation Develop a consistent way to analyze Complete
Hemolytic anemias (2 of 2)
 Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
The Complete Blood Count
 The Complete Blood Count (Cartesian Thinking at Its Best) A SEM Image of Normal Human Blood Laurie Larsson February 22, 2010 Anatomy and Philology II Dr. Danil Hammoudi Introduction A complete blood count
The Complete Blood Count (Cartesian Thinking at Its Best) A SEM Image of Normal Human Blood Laurie Larsson February 22, 2010 Anatomy and Philology II Dr. Danil Hammoudi Introduction A complete blood count
INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED
 INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED Rationale for Combining Iron & Vit-D Vit D deficiency and Iron deficiency Anaemia the two most menacing disorders - are inter-related
INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED Rationale for Combining Iron & Vit-D Vit D deficiency and Iron deficiency Anaemia the two most menacing disorders - are inter-related
RBCs Disorders 2. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC
 HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
Normal Development. Normal Development 10/16/2012. Hematopoietic and Lymph Node Pathology. Red Blood Cell Maturation & Anemias
 Hematopoietic and Lymph Node Pathology Normal Development Red Blood Cell Maturation & Anemias Normal Development Differentiation of Hematopoietic Cells 1 Bone Marrow Bone Marrow Bone Marrow, RBC Precursors
Hematopoietic and Lymph Node Pathology Normal Development Red Blood Cell Maturation & Anemias Normal Development Differentiation of Hematopoietic Cells 1 Bone Marrow Bone Marrow Bone Marrow, RBC Precursors
Approach to the child with anemia. Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital
 Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013 What type of tissue is blood? Blood is considered liquid connective
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013 What type of tissue is blood? Blood is considered liquid connective
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS. Dr. Tariq Aladily
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS Third year medical students First semester Faculty 2018/2019 of Medicine Hereditary Spherocytosis Intrinsic defects
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS Third year medical students First semester Faculty 2018/2019 of Medicine Hereditary Spherocytosis Intrinsic defects
Clinical & Laboratory Assessment
 Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE
 Log Out Help current login :lcytryn@montefiore.org HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE Lawrence Cytryn, M.D. - Course Director 1998 Edward Burns, M.D. Images used by permission within AECOM
Log Out Help current login :lcytryn@montefiore.org HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE Lawrence Cytryn, M.D. - Course Director 1998 Edward Burns, M.D. Images used by permission within AECOM
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011)
 The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
YEREVAN STATE MEDICAL UNIVERSITY DEPARTMENT OF HEMATOLOGY COURSE DESCRIPTION HEMATOLOGY
 1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
Preferred Clinical Services for Leading Age Florida August 26-27, 2015
 DIAGNOSIS CODING ESSENTIALS FOR LONG-TERM CARE: CHAPTER 3, D CODES DISEASES OF THE BLOOD AND BLOOD-FORMING ORGANS AND CERTAIN DISORDERS INVOLVING THE IMMUNE MECHANISM Preferred Clinical Services for Leading
DIAGNOSIS CODING ESSENTIALS FOR LONG-TERM CARE: CHAPTER 3, D CODES DISEASES OF THE BLOOD AND BLOOD-FORMING ORGANS AND CERTAIN DISORDERS INVOLVING THE IMMUNE MECHANISM Preferred Clinical Services for Leading
Dr Anzo William Adiga
 Anemia Dr Anzo William Adiga +256777363201 anzoism2008@gmail.com Definition of Anemia Deficiency in the oxygen-carrying capacity of the blood due to a diminished erythrocyte mass. May be due to: Erythrocyte
Anemia Dr Anzo William Adiga +256777363201 anzoism2008@gmail.com Definition of Anemia Deficiency in the oxygen-carrying capacity of the blood due to a diminished erythrocyte mass. May be due to: Erythrocyte
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital
 Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour
 4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
Does Morphology Matter in 2017
 Does Morphology Matter in 2017 ISLH May 2017 Kathryn Foucar Distinguished Professor Emerita kfoucar@salud.unm.edu Objectives Recognize unique RBC and WBC abnormalities in non-neoplastic disorders Learn
Does Morphology Matter in 2017 ISLH May 2017 Kathryn Foucar Distinguished Professor Emerita kfoucar@salud.unm.edu Objectives Recognize unique RBC and WBC abnormalities in non-neoplastic disorders Learn
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Management. (By the World Health Organization according to the magnitude of the enzyme deficiency and the severity of hemolysis)
 Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Congenital Haemoglobinopathies
 Congenital Haemoglobinopathies L. DEDEKEN, MD H O P I T A L U N I V E R S I T A I R E D E S E N F A N T S R E I N E F A B I O L A U N I V E R S I T E L I B R E DE B R U X E L L E S Red Blood Cell Disorders
Congenital Haemoglobinopathies L. DEDEKEN, MD H O P I T A L U N I V E R S I T A I R E D E S E N F A N T S R E I N E F A B I O L A U N I V E R S I T E L I B R E DE B R U X E L L E S Red Blood Cell Disorders
Classifications of Anemia (table 2.2)
 Classifications of Anemia (table 2.2) Anemia is a general name given to a group of circulating RBC deficiencies, both qualitativeand quantitative. Anemia can be caused by decreased RBC production, excess
Classifications of Anemia (table 2.2) Anemia is a general name given to a group of circulating RBC deficiencies, both qualitativeand quantitative. Anemia can be caused by decreased RBC production, excess
Care of the Patient with a Blood or Lymphatic Disorder. ph Volume pints. Red blood cells (RBC) White blood cells (WBC)
 Slide 1 Chapter 7 Care of the Patient with a Blood or Lymphatic Disorder 1 Slide 1 Overview of Anatomy and Physiology Characteristics of blood Consistency (viscous) 45% blood cells RBC WBC Platelets 55%
Slide 1 Chapter 7 Care of the Patient with a Blood or Lymphatic Disorder 1 Slide 1 Overview of Anatomy and Physiology Characteristics of blood Consistency (viscous) 45% blood cells RBC WBC Platelets 55%
Hematology Unit Lab 1 Review Material
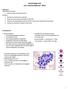 Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
ACQUIRED COAGULATION ABNORMALITIES
 ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
How to Write a Life Care Plan for a Child with Hemoglobinopathy
 How to Write a Life Care Plan for a Child with Hemoglobinopathy Tamar Fleischer, BSN, MSN, CNLCP & Mona Yudkoff, RN, MPH, CRRN, CNLCP BalaCare Solutions March 2018 St. Peterburg, Florida What is Hemoglobinopathy?
How to Write a Life Care Plan for a Child with Hemoglobinopathy Tamar Fleischer, BSN, MSN, CNLCP & Mona Yudkoff, RN, MPH, CRRN, CNLCP BalaCare Solutions March 2018 St. Peterburg, Florida What is Hemoglobinopathy?
HEMOLY L TIC AN A EMIA
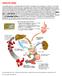 HEMOLYTIC ANEMIA In a healthy person, a red blood cell survives 90 to 120 days in the circulation, so about 1% of human red blood cells break down each day. The spleen (part of the reticulo-endothelial
HEMOLYTIC ANEMIA In a healthy person, a red blood cell survives 90 to 120 days in the circulation, so about 1% of human red blood cells break down each day. The spleen (part of the reticulo-endothelial
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease
 Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology
 Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology - Anemia: It is a reduction in number of RBCs or Hb concentration > 2 SD below the mean for a corresponding
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology - Anemia: It is a reduction in number of RBCs or Hb concentration > 2 SD below the mean for a corresponding
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Wang, M. (2016). Iron Deficiency and Other Types of Anemia in Infants and Children. American Family Physician. 93 (4): 270-278. Objectives Recognize common signs
The McMaster at night Pediatric Curriculum Wang, M. (2016). Iron Deficiency and Other Types of Anemia in Infants and Children. American Family Physician. 93 (4): 270-278. Objectives Recognize common signs
Clinical implications for decreased lymphocytes (lymphopenia) o Corticosteroid therapy, adrenocortical hyperfunction, stress, shock
 Learning Objectives At the completion of this program, the participants will be able to: 1. Identify the components of the CBC and Differential and their clinical implications. 2. Identify normal pediatric
Learning Objectives At the completion of this program, the participants will be able to: 1. Identify the components of the CBC and Differential and their clinical implications. 2. Identify normal pediatric
Definitions: Hematocrit <41% in men or <36 in women Hemoglobin <13.5 gm\dl in men or <12 gm\dl in women
 1 Nadanotes.com Definitions: Hematocrit
1 Nadanotes.com Definitions: Hematocrit
PNH Glossary of Terms
 AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
2013 Pathology Student
 About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
Done by :Aseel Twaijer & Laith Sorour Hemolytic Anemias
 Hemolytic Anemias Hemolytic anemias share the following features: - A shortened red cell life < 120 days - Elevated erythropoietin levels (compensatory increase in erythropoiesis) - Accumulation of hemoglobin
Hemolytic Anemias Hemolytic anemias share the following features: - A shortened red cell life < 120 days - Elevated erythropoietin levels (compensatory increase in erythropoiesis) - Accumulation of hemoglobin
Medical and Surgical Complications of Sickle Cell Anemia
 Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Department of Surgery Dar A lalafia Medical Company Qatif
Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Department of Surgery Dar A lalafia Medical Company Qatif
Chronic Myeloproliferative Disorders
 1 Chronic Myeloproliferative Disorders 15th 9 April2015 Polycythemia vera Essential thrombocythemia Idiopathic primary myelofibrosis 2 Learning objectives To appreciate types of polycythaemia (erythrocytosis)
1 Chronic Myeloproliferative Disorders 15th 9 April2015 Polycythemia vera Essential thrombocythemia Idiopathic primary myelofibrosis 2 Learning objectives To appreciate types of polycythaemia (erythrocytosis)
Things to never miss in the office. Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC
 Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Approach to Hemolysis
 Objectives: Approach to Hemolysis To know the function of platelets and the relationship between the platelet count in peripheral blood and the extent of abnormal bleeding. To know about the diseases associated
Objectives: Approach to Hemolysis To know the function of platelets and the relationship between the platelet count in peripheral blood and the extent of abnormal bleeding. To know about the diseases associated
Symptoms and Signs in Hematology (2)/ 2013
 Symptoms and Signs in Hematology (2)/ 2013 Abdallah Abbadi.MD.FRCP Professor of Medicine,Hematology & Oncology University of Jordan & JUH Email: abdalla.awidi@gmail.com Case one: A 24 yr old female complains
Symptoms and Signs in Hematology (2)/ 2013 Abdallah Abbadi.MD.FRCP Professor of Medicine,Hematology & Oncology University of Jordan & JUH Email: abdalla.awidi@gmail.com Case one: A 24 yr old female complains
Dana Alsulaibi. - Ahmad Almuhtaseb. - Tariq Al - Adaily
 - 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
- 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE?
 COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE? M. DE SLOOVERE (1), L. HARLET (2), S. VAN STEENWEGHEN (3), E. MOREAU (1), D. DE SMET (1) (1) DEPARTMENT OF LABORATORY MEDICINE,
COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE? M. DE SLOOVERE (1), L. HARLET (2), S. VAN STEENWEGHEN (3), E. MOREAU (1), D. DE SMET (1) (1) DEPARTMENT OF LABORATORY MEDICINE,
Chapter 28. Media Directory. Hematopoiesis. Regulation of Hematopoiesis. Erythropoietin. Drugs for Hematopoietic Disorders
 Chapter 28 Drugs for Hematopoietic Disorders Slide 35 Media Directory Epoetin Alfa Animation Upper Saddle River, New Jersey 07458 All rights reserved. Hematopoiesis Figure 28.1 Hematopoiesis Process of
Chapter 28 Drugs for Hematopoietic Disorders Slide 35 Media Directory Epoetin Alfa Animation Upper Saddle River, New Jersey 07458 All rights reserved. Hematopoiesis Figure 28.1 Hematopoiesis Process of
MYELOPROLIFARATIVE NEOPLASMS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin).
 MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
