An approach to dyspepsia for the pharmacist
|
|
|
- Berniece Cox
- 6 years ago
- Views:
Transcription
1 An approach to dyspepsia for the pharmacist Ilse Truter, DCom, BPharm, MSc, PhD, Drug Utilization Research Unit (DURU) Department of Pharmacy, Nelson Mandela Metropolitan University Correspondence to: Ilse Truter, Abstract Dyspepsia is a symptom, or a combination of symptoms, that indicates the presence of an upper gastrointestinal tract problem. Typical symptoms include epigastric pain or burning, early satiation and postprandial fullness, belching, bloating, nausea or discomfort in the upper abdomen. Most people with dyspepsia do not seek medical care for their symptoms, although 25% of the developed world s population suffers from dyspepsia annually. Rates range between 13-40% in different countries. Antacids remain safe, simple and effective agents for the symptomatic treatment of gastric acid-related symptoms. Evidence supports a test-and-treat approach in patients with non-dominant heartburn dyspepsia symptoms. In addition to antacids, dyspepsia is treated with proton-pump inhibitors (PPIs), blockers or cytoprotective agents, for example, sucralfate. Prokinetic drugs, for example metoclopramide, domperidone and erythromycin, also have a role to play in the treatment of dyspepsia. All patients should be offered general treatment, including advice on self-treatment, lifestyle changes, patient empowerment, and the management of long-term symptoms. Pharmacists are well placed to provide counselling and support to people suffering from dyspepsia. Medpharm S Afr Pharm J 2012;79(8):9-16 Introduction Stomach pain and discomfort have been reported since ancient times. The term dyspepsia originates from the Greek words dys and pepse, meaning indigestion. 1 It was first recorded in the mid- 18 th century, and since then, the term has been widely used. In the 18 th century, dyspepsia was thought to be one of the nervous disorders, along with hypochondria and hysteria. 1 Dyspepsia is a sensation of pain or discomfort, centered in the upper abdomen. 2 It is often described as indigestion, early satiation (a sensation of having overeaten soon after beginning to eat, and out of proportion to the size of the meal, so that the food cannot be finished), postprandial fullness (prolonged persistence of food in the stomach), and gnawing or burning. 1,2 Dyspepsia is often accompanied by a combination of symptoms, including bloating, heartburn and nausea or vomiting. Enquires should be made about predominant symptoms, such as upper abdominal discomfort, pain, heartburn or reflux, in order to distinguish dyspepsia from gastro-oesophageal reflux disease (GORD). Yet, symptom assessment alone cannot be used to make a reliable diagnosis in patients with dyspepsia. 3 Symptoms Symptoms are sometimes classified as ulcer-like, dysmotility-like, or reflux-like. 2 These symptoms suggest, but do not confirm, an aetiology, and often overlap: Ulcer-like symptoms consist of pain that is localised in the epigastrium, frequently occurs before meals, and is relieved by food, antacids or blockers. Dysmotility-like symptoms consist of discomfort, rather than pain, along with early satiation, postprandial fullness, nausea, vomiting, bloating, and symptoms that are worsened by food. Reflux-like symptoms consist of heartburn or acid regurgitation. Alternating constipation and diarrhoea with dyspepsia suggests irritable bowel syndrome (IBS), or abuse of over-the-counter (OTC) laxatives or antidiarrhoeals. The association between dyspepsia and IBS is a recurring theme in recent literature. Dyspepsia symptoms that cause alarm include anorexia, nausea, emesis, weight loss, anaemia, blood in the stools, dysphagia, odynophagia, and failure to respond to standard therapy, such as blockers. Dyspepsia symptoms negatively affect the quality of life of most patients, especially with regard to sleep pattern changes, diet, and interference with work and leisure activities. The impact of dyspepsia upon quality of life is a personal experience. It can be a recurring problem, or a chronic complaint for which available treatment options may be wholly, or only partly, effective in relieving symptoms, while lifestyle changes can help to avoid trigger factors. It is appropriate to manage most patients symptoms (those without signs that cause alarm) without a formal diagnosis. Therefore, the pharmacist has an important role to play in counselling, monitoring and reassuring the patient with dyspepsia. S Afr Pharm J 9
2 Epidemiology Dyspepsia is one of the most common symptoms encountered in primary care. The exact prevalence of dyspepsia is unknown. 4 Although most people who are affected by dyspepsia do not seek medical care for their symptoms, it is estimated that approximately one quarter of the population in the developed world suffers from dyspepsia annually, and nearly everyone, at some point in his or her life, will experience an episode of dyspepsia. 4,5 Rates range from 13-40% in different countries. 5 Its prevalence is modestly higher in females than in males. 4,5 Dyspepsia remains a common and important symptom, even into the geriatric age group. 5 Follow-up of patients over five to seven years shows a benign, but recurrent, nature in 50% of cases. 5 Terminology The nomenclature for dyspepsia is confusing. Some people include all upper gastrointestinal tract symptoms under the heading of dyspepsia, while others separate patients with symptoms indicative of GORD. However, both approaches recommend identifying patients whose symptoms are suggestive of GORD, and managing them as if they have reflux disease. Dyspepsia is pain or discomfort in the upper abdomen which is usually described as a burning sensation, heaviness, or an ache. Associated symptoms include a feeling of fullness, early satiation after meals, anorexia, bloating, belching, nausea and vomiting. The symptoms of dyspepsia may be episodic, recurrent, or chronic. Symptoms are often associated with eating, but this is not always the case. Undifferentiated or uninvestigated dyspepsia is a condition for which characteristic symptoms have been clinically assessed as originating in the upper gastrointestinal tract, but which has not been investigated by upper gastrointestinal tract endoscopy recently. Symptoms include epigastric pain or burning, early satiety and postprandial fullness, belching, bloating, nausea, or discomfort in the upper abdomen. In a person at low risk of underlying pathology, symptomatic management is appropriate, without the need for further investigation. Accumulating evidence suggests that distinct subgroups of uninvestigated dyspepsia exist in the general population, signifying that separate evaluation and treatment strategies might be needed. Rome III introduced epigastric pain syndrome (EPS) and postprandial distress syndrome (PDS) subgroups to distinguish between different symptom clusters. 1 Functional or non-ulcer dyspepsia refers to a situation in which upper gastrointestinal tract endoscopy did not reveal a potential cause (underlying pathology) for the dyspepsia. In 1994, the Rome criteria were developed in an attempt to meet the clinical need to describe systematically functional gastrointestinal disorders. 1 The Rome I criteria were subsequently modified in 2000 (Rome II criteria). The most recent 2006 Rome III criteria for functional dyspepsia are provided in Table I. Functional dyspepsia includes multiple types of patients with heterogeneous complaints, and possibly different underlining pathophysiologies. Although the pathophysiology of functional dyspepsia has been widely investigated, no definite single reason was identified. Multiple mechanisms are likely to be involved (see Figure 1). Specific combinations of physiological, genetic, environmental and psychological factors in an individual patient lead to a variety of symptoms called dyspepsia. There is growing evidence that brain-gut interactions, at different levels, are also implicated. Central nervous system modulation (stress, illness behaviour) Visceral hypersensitivity (fat, H + ions, wall distension) Acid hypersensitivity Vagal neuropathy Decreased fundic accomodation Inflammation [bacteria (Helicobacter pylori), viruses] Abnormal distribution of gastric contents Delayed gastric emptying and antral hypomotility Gastric dysrhythmias Overdistended antrum Duodenal hypersensitivity Small bowel dysmotility Figure 1: Pathophysiological mechanisms in functional dyspepsia 1 S Afr Pharm J 10
3 Table I: Rome III diagnostic criteria for functional dyspepsia 1 At least three months, with onset at least six months previously, of one or more of the following: Bothersome postprandial fullness Early satiation Epigastric pain Epigastric burning And There is no evidence of structural disease, including upper endoscopy, that is likely to explain the symptoms. Heartburn is described as a burning sensation rising from the epigastrium, towards the neck. Heartburn is often included within the description of dyspepsia. Heartburn, with or without associated dyspepsia is most commonly associated with GORD or reflux oesophagitis. GORD and dyspepsia are related. Patients with troublesome heartburn and acid regurgitation can be diagnosed clinically as having GORD. As already mentioned, the available literature increasingly states that IBS is often a co-morbid condition associated with dyspepsia. Therefore, there is a large overlap between GORD, IBS and dyspepsia, and they often co-exist in the same patient. For practical purposes, it is important to understand which complaints and symptoms are dominant. The severity of a patient s dyspepsia is measured by the patient s description of the impact of the symptoms on quality of life and function. If different guidelines are compared, the Canadian Dyspepsia Working Group (CanDys) and the UK National Institute for Health and Clinical Excellence (NICE) include GORD symptoms in the definition of dyspepsia. CanDys does not require a specific duration of symptoms, whereas NICE requires four weeks, while the ROME III requires 12 weeks in the previous year to qualify as dyspepsia. The American Gastroenterological Association s (AGA) technical review for the evaluation of dyspepsia excludes patients with symptoms that suggest GORD, and includes only the typical symptoms listed earlier. 5 Aetiology Common causes of dyspepsia include peptic ulcer disease, motility disorders, medicines [for example, erythromycin, aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), alendronate, angiotensin-converting enzyme (ACE) inhibitors, iron, macrolide antibiotics, metronidazole, oestrogen and theophylline], excessive alcohol, GORD, and oesophageal or gastric malignancy. 4 Therefore, it is clear that the aetiology of dyspepsia differs, depending on which condition the patient is suffering from. In addition, many patients have no physical abnormalities (functional or nonulcer dyspepsia). Others are found to have duodenitis, pyloric dysfunction, motility disturbances, Helicobactor pylori, gastritis, lactose deficiency, and cholelithiasis, which correlate poorly with the symptoms, i.e. correction of the condition does not alleviate dyspepsia. Examination and diagnosis Dyspepsia is not a diagnosis, but rather a description of intermittent symptoms that may indicate disease of the upper gastrointestinal tract. In the majority of cases, there is no clear pathological cause, and many people manage the symptoms themselves without consulting a healthcare practitioner. If medical advice is sought, a thorough medical and drug history should be undertaken by the healthcare practitioner to rule out serious pathology. When diagnosing dyspepsia, peptic ulceration (gastric or duodenal) is probably the most important diagnosis to rule out. Typically the patient will have well localised, mid-epigastric pain, described as constant, annoying or gnawing. A physical examination rarely suggests a cause of dyspepsia. Testing Routine tests include a full blood count and stool testing for occult blood to exclude gastrointestinal blood loss. If results are abnormal, additional tests, for example imaging studies or endoscopy, should be considered. Endoscopy is used to investigate signs that cause alarm, and to identify gastric and duodenal ulcers, as well as rare cases of oesophageal and gastric cancer. The important identification of the bacterium, H. pylori, in 1983, and the development of effective antibiotic treatment, has revolutionised treatment of peptic ulcer disease. Because of malignancy risks, patients who are over 50 years old, and those with the onset of new symptoms that cause alarm, should undergo upper gastrointestinal tract endoscopy. For patients who are younger than 50 years without symptoms that cause alarm, empiric therapy with antisecretory or prokinetic agents, followed by endoscopy in treatment failures, has been suggested. Screening for H. pylori infection, with a urea breath test or stool assay, has also been recommended. Oesophageal manometry and ph studies are indicated if reflux symptoms persist after upper gastrointestinal tract endoscopy, as well as a two-to-four week trial using a proton-pump inhibitor (PPI). Questionnaires Several validated questionnaires have been developed, especially for functional dyspepsia. Examples are the Nepean Dyspepsia Index, Patient Assessment of Upper Gastrointestinal Symptoms (PAGI-SYM), and the Severity of Dyspepsia Assessment (SODA) questionnaire. These questionnaires do not differentiate between different types of dyspepsia patients according to symptoms or pathophysiology, and have mostly been used to define patients for the purpose of clinical studies. Red flags associated with dyspepsia When a patient presents, complaining of indigestion, healthcare practitioners should consider all possible sources thereof, including the oesophagus, stomach, heart, liver, gallbladder, pancreas, bowel, NSAIDs, and other medication. 3 S Afr Pharm J 12
4 The following factors increase the likelihood of significant organic disease, and are trigger points for referral: 4,6 Fifty years or older at first presentation (the incidence of gastric cancer increases with age) Family history of gastric cancer, with onset age younger than 50 years Severe or persistent dyspepsia Treatment failure Previous peptic ulcer disease, particularly if complicated Ingestion of NSAIDs, including aspirin Pain described as severe or debilitating, or wakes the patient at night Referred pain Signs and symptoms of chronic gastrointestinal tract bleeding, including dark or tarry stools Iron-deficiency anaemia Dysphagia, or the sensation that food is sticking in the throat Persistent or protracted vomiting with or without blood, or persistent regurgitation of food Palpable abdominal mass Coughing spells or nocturnal aspiration Unexplained weight loss Long-standing change in bowel habit. Any of these red flags should be identified, and further investigated. They are major determinants of the need for endoscopy. The management strategy for uncomplicated dyspepsia should only be followed if there is reasonable certainly that no serious underlying pathology exists. Management strategy There are several options for initial management of the condition. Identifying a possible cause of the symptoms will guide management. Dyspepsia can be the result of medication or underlying pathology, including reflux oesophagitis, gastro-oesophageal cancer. However, the majority of patients have no distinguishable cause of their dyspepsia. These patients should be observed over time and reassured. The management goal is to provide relief of symptoms, and if present, to heal oesophageal lesions. New episode of dyspepsia sucralfate. Prokinetic drugs, for example, metoclopramide and erythromycin, given as a liquid suspension, may also be tried in patients with dysmotility-like dyspepsia. However, there is no clear evidence that matching the drug class to the specific symptoms makes a difference, for example, reflux vs. dysmotility. Misoprostol and anticholinergics are not effective in managing functional dyspepsia. Medicines that alter sensory perception, such as tricyclic antidepressants (TCAs), may be helpful. Evidence shows that use of a PPI is superior to receptor blockers in the initial treatment of H. pylori-negative dyspepsia. 7 Figure 2 illustrates an algorithm for the management of uninvestigated dyspepsia. Chronic gastrointestinal bleeding Progressive unintentional weight toss Progressive difficulty swallowing Persistent vomiting Iron deficiency anaemia Epigastric mass Suspicious barium meal or Age > 55 years and recent-onset, persistent,* unexplained dyspepsia Previous gastric ulcer or surgery Continuing need for NSAID treatment risk of gastric cancer or Anxiety about cancer Review medication for causes of dyspepsia e.g. Ca 2+ antagonists, nitrates, theophyllines, bisphosphonates, corticosteroids, and NSAIDs response/relapse PPI (e.g. omeprazole 20mg od) for 1 month response/relapse Test and treat for H. pylori response Response Relapse Acute GI bleeding? Yes Admit Yes urgent referral (<2 wk) Endoscopy Stop NSAIDs: suspend PPI/ receptor antagonists for 2 weeks prior to the procedure Yes Consider routine referral Lifestyle advice Response Return to self-care Review after 1 year or if maximum number of repeats is used Low-dose treatment (minimum to control symptoms) prn response Direct clinical evidence supports a testand-treat approach in patients with nondominant heartburn dyspepsia symptoms. 7 Symptoms are treated with PPIs, blockers or cytoprotective agents, for example, receptor antagonist, e.g. ranitidine 150 mg bd, or prokinetic, e.g. domperidone 10 mg tds, for 1 month *Do not delay > 4 6 weeks before referral Figure 2: Management of dyspepsia 8 Response S Afr Pharm J 13
5 Conventional NSAIDs, aspirin and cyclo-oxygenase 2 inhibitors can all cause dyspepsia. If use of these medications cannot be discontinued, co-therapy with either a PPI, misoprostol or a high-dose receptor antagonist (blocker) is recommended, although evidence is based on ulcer data, and not on dyspepsia data. 7 In patients with non-heartburn dominant dyspepsia, noninvasive testing for H. pylori should be performed, and if the result is positive, treatment must be given. Treatment Various nonpharmacological measures and lifestyle changes can be recommended, for example, healthy eating habits, weight loss, and smoking cessation. Patients should be advised to avoid precipitating factors, such as coffee, chocolate, or fatty foods. Postural measures can be recommended, for example, the head of the bed can be raised, and the main meal eaten well before going to bed. To treat dyspepsia, various complementary and alternative therapies have been investigated. Acupuncture has received considerable attention. Other treatments that have been evaluated include hypnotherapy, psychotherapy, herbal preparations derived from various plants containing complex extracts [for example, iberogast (herbal extract STW 5), Chinese and Japanese herbal medicine], and percutaneous implants of gastric electrodes. 1 From a pharmacological point of view, dyspepsia symptoms are managed by antacids, alginates, PPIs, receptor antagonists, H. pylori eradication therapy, prokinetics, TCAs and selective serotonin-reuptake inhibitors. Several other complementary and alternative treatments have been proposed. Table II provides a summary of the most common treatments for dyspepsia, and evidence of their effectiveness. Antacids For many decades, antacids have been used to treat dyspepsia, and have proven efficacy in neutralising stomach acid. Antacids act by neutralising gastric acidity; 5 ml of an average antacid liquid mixture should neutralise the normal fasting volume of gastric acid in the intact stomach. 9 Generally, the doses required to relieve dyspeptic symptoms are not associated with unacceptable side-effects. 9 Their neutralising capacity varies according to the metal salt used, as well as the onset and duration of action, for example: 9 Sodium and potassium salts are the most soluble, making them quick- but short-acting. Magnesium and aluminium salts are less soluble. Therefore, they have a slower onset, but longer duration of action. Calcium salts are both quick-acting, and have a prolonged action. Antacid active ingredients are often combined in one product to ensure quick onset and prolonged action. The addition of local Table II: Available therapies to treat functional dyspepsia 1 Pharmacological agents Benefit Evidence Helicobacter pylori eradication Proton-pump inhibitors blockers Mucosal protecting agents, and antacids Prokinetics (metoclopramide, domperidone) anaesthetics and anti-foaming agents (silicones as antiflatulants) adds no advantage to the efficacy of the antacid. 9 The addition of an antispasmodic may appear to be advantageous in some patients, but separate treatment with an antispasmodic, if it is needed, is preferred. 9 Antacids are easily available, and can be bought without the supervision of a pharmacist. When recommending antacids, the following aspects should be considered: 4 Antacids in liquid form have a greater acid-neutralising capacity and speed of onset than tablet formulations. Misuse and chronic use of antacids will result in significant systemic absorption, leading to various unwanted medical conditions. Milk-alkali syndrome has been reported in connection with chronic abuse of calcium-containing antacids, and osteomalacia, in connection with aluminium-containing products. Therefore, prior to recommending a specific product, it is important to determine patient use of antacids. Preferably, antacid therapy should not be taken for longer than two weeks. If symptoms have not resolved within that time, then other treatments, or evaluation by a general practitioner, should be recommended. Antacids should be taken after food, because gastric emptying is delayed in the presence of food. This allows antacids to exert their effect for up to three hours. Avoid antacids that might cause constipation in the elderly. Alginates (alginic acid) Positive benefit, NNT a = 17 Positive benefit, NNT = 10 Positive benefit, NNT = 7 benefit Significant benefit, NNT = 4 Tegaserod (5-HT 4 partial agonist) Probable benefit Clinical trials Itopride (D 2 antagonist, acetylcholinesterase inhibitor) benefit Clinical trials Tricyclic antidepressants Probable benefit Selective serotonin-reuptake inhibitors NNT= number needed to treat Probable benefit Clinical trials Alginates are extracted from algae. An alginate product should be the first-line treatment for patients with heartburn and reflux. When in contact with gastric acid, the alginate precipitates out, S Afr Pharm J 14
6 forming a sponge-like matrix that floats on top of the stomach contents. Products containing alginate are combination preparations containing an alginate with antacids. They are best given after each main meal and before bedtime, although they can be taken when needed. -receptor antagonists Ranitidine, famotidine and cimetidine are available in low dosages, without a prescription. Ranitidine can be given in a dose of 75 mg. If symptoms persist, another 75 mg dose may be given an hour later. The maximum dose of ranitidine is 300 mg in a 24-hour period. Famotidine can be given in a dose of 10 mg. If symptoms persist, another 10 mg can be administered an hour later. The maximum dose of famotidine is 20 mg in 24 hours. Proton-pump inhibitors The PPIs include omeprazole, esomeprazole, lansoprazole, pantoprazole and rabeprazole. These medicines are the most potent suppressors of gastric acid secretion. They act by irreversibly binding to, and inhibiting, H + /K + -ATPase enzyme of the gastric parietal cell. PPIs are indicated for the short-term management of peptic ulcer disease and GORD, the long-term prevention of GORD relapse, and as part of H. pylori eradication regimens. 9 The available PPIs have comparable clinical efficacy. 9 H. pylori eradication and other agents Evidence exists that eradicating H. pylori in non-ulcer dyspepsia is beneficial. Various other agents have been, or are, given, with varying success. Mucosal-protecting agents and antispasmodics are used, for example bismuth, sucralfate and misoprostol. Peppermint oil and caraway oil have been tried as spasmolytic agents. The prokinetic agents, metoclopramide and domperidone, are offered. Tegaserod was withdrawn from the American market because of the increased incidence of cardiac ischaemic events. Itopride, which showed promising results in Phase 2 trials, ultimately failed in Phase 3 trials. Fundic relaxants have been given, as well as agents that have an effect on visceral hypersensitivity and central pain perception. Summary of medicines Table III provides a summary of selected medicines that are commonly used to manage dyspeptic symptoms. Conclusion Once an organic cause is excluded, dyspepsia remains a complex problem in clinical practice. Management of symptoms in primary care is appropriate for most patients, rather than routinely seeking a pathophysiological diagnosis. Many recent attempts to find new treatment strategies have failed. Tegaserod, for example, has been withdrawn from the United States, and itopride, which showed promising results in Phase 2 trials, ultimately failed in Phase 3 Table III: Summary of selected medicines for dyspepsia 4,9 Medicine Use in children Likely side-effects Drug interactions Exercise care Pregnancy Antacids Sodium only >12 years ne ne Heart disease Can be used Calcium only Magnesium only Aluminium only Constipation Diarrhoea Constipation Tetracyclines, quinolones, imidazoles, phenytoin, penicillamine and biphosphonates ne Can be used Alginates > 6 years ne ne Heart disease ne antagonists > 16 years Diarrhoea, constipation, headache ne ne t recommended Proton-pump inhibitors Short-term use (< 3 months) in children > 1 year Diarrhoea, constipation, nausea, vomiting, flatulence and abdominal pain and colic, headache, vertigo, dizziness, somnolence and insomnia, predominantly in severely ill patients Agents metabolised in the liver, antacids, clopidogrel, digoxin, ketoconazole and itraconazole, tacrolimus Severely ill Gastric malignancy t recommended S Afr Pharm J 15
7 trials. Future treatments will depend to a significant extent, on the careful evaluation of patients, and an analysis of their symptoms, as well as on new insights into the pathophysiology of symptoms in the upper gastrointestinal tract. Pharmacists can provide both the first point of contact and ongoing support for patients suffering from dyspepsia. It has been demonstrated that advice on self-medication and counselling by pharmacists has a measurable impact on health-related quality of life, and that patients value the information that pharmacists provide. 3 In managing dyspepsia, the role of the pharmacist is to offer initial and ongoing help for people suffering from symptoms, including advice about lifestyle changes, like, healthy eating, weight reduction and smoking cessation; over-the-counter and prescribed medicine; and when to consult a general practitioner. 10 All patients should be given advice on self-treatment, lifestyle changes, and the management of long-term symptoms. Longterm care should emphasise patient empowerment in managing their condition. References 1. Brun R, Kuo B. Functional dyspepsia. Ther Adv Gastroenterol. 2010;3(3): The Merck Manual. 18 th ed. Beers MH, Porter RS, Jones TV, et al, editors. Whitehouse Station: Merck Research Laboratories, Dyspepsia, section 2: dyspepsia in the community. Edinburgh: Scottish Intercollegiate Guidelines Network (SIGN), 2011 [homepage on the Internet]. c2011. Available from: 4. Rutter P. Community p0harmacy: symptoms, diagnosis and treatment. Edinburgh: Churchill Livingstone, Assessment of dyspepsia. Best practice. BMJ Publishing Group, 2011 [homepage on the Internet]. c2011. Available from: 6. Managing dyspepsia and heartburn in general practice: an update. BPJ. 2011;(34): Veldhuyzen van Zanten SO, Bradette M, Chiba N, et al. Evidence-based recommendations for short- and long-term management of uninvestigated dyspepsia in primary care: an update of the Canadian Dyspepsia Working Group (CanDys) clinical management tool. Can J Gastroenterol. 2005;19(5): Simon C, Everitt H, Van Dorp F. Oxford handbook of general practice. 3 rd ed. Oxford: Oxford University Press, South African Medicines Formulary (SAMF). 9 th ed. Rossiter D, editor. Cape Town: Health and Medical Publishing Group of the South African Medical Association, Dyspepsia: managing dyspepsia in adults in primary care. Newcastle upon Tyne: rth of England Dyspepsia Guideline Development Group, Evidence-based clinical practice guideline, Centre for Health Services Research Report 112. S Afr Pharm J 16
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Reflux of gastric contents, particularly acid, into the esophagus
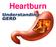 Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
Gastro-oesophageal reflux disease and peptic ulcer disease. By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D
 Gastro-oesophageal reflux disease and peptic ulcer disease By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D Gastro-oesophageal reflux disease and peptic ulcer disease Learning objectives:
Gastro-oesophageal reflux disease and peptic ulcer disease By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D Gastro-oesophageal reflux disease and peptic ulcer disease Learning objectives:
Management of Dyspepsia
 MPharm Programme Management of Dyspepsia Slide 1 of 28 Learning Objectives Understand the principles and wider implications underpinning evidence based therapeutics in the key clinical specialities Objectively
MPharm Programme Management of Dyspepsia Slide 1 of 28 Learning Objectives Understand the principles and wider implications underpinning evidence based therapeutics in the key clinical specialities Objectively
Management of dyspepsia in adults in primary care
 Dyspepsia Management of dyspepsia in adults in primary care June 2005. The recommendations on referral for endoscopy in this NICE guideline have been amended in line with the recommendation in the NICE
Dyspepsia Management of dyspepsia in adults in primary care June 2005. The recommendations on referral for endoscopy in this NICE guideline have been amended in line with the recommendation in the NICE
Management of dyspepsia and of Helicobacter pylori infection
 Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Guidelines for the Management of Dyspepsia and GORD. Gastroenterology/ Acute Adult Governance. Drugs and Therapeutics Committee
 Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
Functional Dyspepsia
 Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
June By: Reza Gholami
 ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
Non-Ulcer Dyspepsia: what is it? What can we do with these patients? Overview. Dyspepsia Definition. Functional Dyspepsia. Dyspepsia the Basics
 Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
6/25/ % 20% 50% 19% Functional Dyspepsia Peptic Ulcer GERD Cancer Other
 Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
GASTROINTESTINAL AND ANTIEMETIC DRUGS. Submitted by: Shaema M. Ali
 GASTROINTESTINAL AND ANTIEMETIC DRUGS Submitted by: Shaema M. Ali GASTROINTESTINAL AND ANTIEMETIC DRUGS by: Shaema M. Ali There are four common medical conditions involving the GI system 1) peptic ulcers
GASTROINTESTINAL AND ANTIEMETIC DRUGS Submitted by: Shaema M. Ali GASTROINTESTINAL AND ANTIEMETIC DRUGS by: Shaema M. Ali There are four common medical conditions involving the GI system 1) peptic ulcers
Dyspepsia. Dyspepsia covers upper abdominal pain, fullness, early satiety, bloating, and nausea.
 Antacids Hawler medical university Collage of pharmacy/ fourth year /pharmacy practice Sham A. Talat Shareef (B.Sc. Msc. clinical pharmacy) 2017-2018 Sham_talat@yahoo.com Head of Department Of Clinical
Antacids Hawler medical university Collage of pharmacy/ fourth year /pharmacy practice Sham A. Talat Shareef (B.Sc. Msc. clinical pharmacy) 2017-2018 Sham_talat@yahoo.com Head of Department Of Clinical
Peptic ulcer disease Disorders of the esophagus
 Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Outline. Definition (s) Epidemiology Pathophysiology Management With an emphasis on recent developments
 Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Functional Heartburn and Dyspepsia
 Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Indigestion (dyspepsia)
 Commissioning pathways Indigestion (dyspepsia) Supplementary information to be read in conjunction with the pathway Reference Supplementary Information 1.1 Symptom Description Annual incidence 40%. Prevalence
Commissioning pathways Indigestion (dyspepsia) Supplementary information to be read in conjunction with the pathway Reference Supplementary Information 1.1 Symptom Description Annual incidence 40%. Prevalence
SASKATCHEWAN REGISTERED NURSES ASSOCIATION
 DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
Proton Pump Inhibitor De-prescribing Guidance
 Amendment History Proton Pump Inhibitor De-prescribing Guidance VERSION DATE AMENDMENT HISTORY 1.0 2013 Previous version 2.0 September 2015 Comments Amendment to Flow chart and addition of Rationale page
Amendment History Proton Pump Inhibitor De-prescribing Guidance VERSION DATE AMENDMENT HISTORY 1.0 2013 Previous version 2.0 September 2015 Comments Amendment to Flow chart and addition of Rationale page
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW
 PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
Number of studies. Endoscopic finding. Number of subjects. Pooled prevalence 95% CI
 Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Nexium 24HR Pharmacy Training
 Nexium 24HR Pharmacy Training Your pharmacist's advice is required. Always read the label. Use only as directed. If symptoms persist, consult your doctor/ healthcare professional. Pfizer Consumer Healthcare
Nexium 24HR Pharmacy Training Your pharmacist's advice is required. Always read the label. Use only as directed. If symptoms persist, consult your doctor/ healthcare professional. Pfizer Consumer Healthcare
Heartburn, also referred to acid reflux, happens when stomach acid flows back (refluxes) into your esophagus.
 WHILE almost everyone experiences mild heartburn from time to time and many individuals have some antacids or another medication on hand for its relief, talk to your doctor, if you have heartburn more
WHILE almost everyone experiences mild heartburn from time to time and many individuals have some antacids or another medication on hand for its relief, talk to your doctor, if you have heartburn more
James Paget University Hospitals. NHS Foundation Trust. Hiatus hernia. Patient Information
 James Paget University Hospitals NHS Foundation Trust Hiatus hernia Patient Information What is a hiatus hernia? A hiatus hernia can cause highly irritating stomach contents, such as acid, to move up into
James Paget University Hospitals NHS Foundation Trust Hiatus hernia Patient Information What is a hiatus hernia? A hiatus hernia can cause highly irritating stomach contents, such as acid, to move up into
QUICK QUERIES. Topical Questions, Sound Answers
 QUICK QUERIES Topical Questions, Sound Answers Dyspepsia: An Evidence-Based Approach Alan B. R. Thomson, MD, PhD, FRCPC, FACP, FACG Presented at the University of Alberta s Medical Grand Rounds, University
QUICK QUERIES Topical Questions, Sound Answers Dyspepsia: An Evidence-Based Approach Alan B. R. Thomson, MD, PhD, FRCPC, FACP, FACG Presented at the University of Alberta s Medical Grand Rounds, University
Dyspepsia: alarm symptoms, investigation and management
 Drug review Dyspepsia Dyspepsia: alarm symptoms, investigation and management SPL Steven Fong MRCP and Jason Dunn PhD, MRCP Dyspepsia is a common symptom and the priority is to identify alarm signals that
Drug review Dyspepsia Dyspepsia: alarm symptoms, investigation and management SPL Steven Fong MRCP and Jason Dunn PhD, MRCP Dyspepsia is a common symptom and the priority is to identify alarm signals that
Copy right protected Page 1
 DRUGS USED IN ULCERS AND GIT DISORDERS A peptic ulcer, also known as PUD or peptic ulcer disease is an ulcer of an area of the gastrointestinal tract that is usually acidic and thus extremely painful.
DRUGS USED IN ULCERS AND GIT DISORDERS A peptic ulcer, also known as PUD or peptic ulcer disease is an ulcer of an area of the gastrointestinal tract that is usually acidic and thus extremely painful.
GI Pharmacology. Dr. Alia Shatanawi 5/4/2018
 GI Pharmacology Dr. Alia Shatanawi 5/4/2018 Drugs Used in Gastrointestinal Diseases Drugs used in Peptic Ulcer Diseases. Drugs Stimulating Gastrointestinal Motility &Laxatives. Antidiarrheal Agents. Drugs
GI Pharmacology Dr. Alia Shatanawi 5/4/2018 Drugs Used in Gastrointestinal Diseases Drugs used in Peptic Ulcer Diseases. Drugs Stimulating Gastrointestinal Motility &Laxatives. Antidiarrheal Agents. Drugs
The usual dose is 40 mg daily with amoxycillin 1.5 g (750 mg b.d.) for 2 weeks. Up to 2 g/day of amoxycillin has been used in clinical trials.
 Name Gasec - 2 Gastrocaps Composition Gasec-20 Gastrocaps Each Gastrocaps contains: Omeprazole 20 mg (in the form of enteric-coated pellets) Properties, effects Proton Pump Inhibitor Omeprazole belongs
Name Gasec - 2 Gastrocaps Composition Gasec-20 Gastrocaps Each Gastrocaps contains: Omeprazole 20 mg (in the form of enteric-coated pellets) Properties, effects Proton Pump Inhibitor Omeprazole belongs
Helicobacter 2008;13:1-6. Am J Gastroent 2007;102: Am J of Med 2004;117:31-35.
 An Update on Helicobacter pylori and Its Treatment Trenika Mitchell, PharmD, BCPS Clinical Assistant Professor University of Kentucky College of Pharmacy October 18, 2008 Objectives Review the epidemiology
An Update on Helicobacter pylori and Its Treatment Trenika Mitchell, PharmD, BCPS Clinical Assistant Professor University of Kentucky College of Pharmacy October 18, 2008 Objectives Review the epidemiology
Definition, Pathogenesis, and Management of That Cursed Dyspepsia
 Clinical Gastroenterology and Hepatology 2018;16:467 479 Definition, Pathogenesis, and Management of That Cursed Dyspepsia Pramoda Koduru, Malcolm Irani, and Eamonn M. M. Quigley IM F1 김영기 Dyspepsia Umbrella
Clinical Gastroenterology and Hepatology 2018;16:467 479 Definition, Pathogenesis, and Management of That Cursed Dyspepsia Pramoda Koduru, Malcolm Irani, and Eamonn M. M. Quigley IM F1 김영기 Dyspepsia Umbrella
Functional Dyspepsia. Norbert Welkovics Heine van der Walt
 Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Self-care information on indigestion
 Self-care information on indigestion 2 What is indigestion? Indigestion (also known as dyspepsia) is a term which describes pain or discomfort in your chest or stomach. What causes indigestion? It is caused
Self-care information on indigestion 2 What is indigestion? Indigestion (also known as dyspepsia) is a term which describes pain or discomfort in your chest or stomach. What causes indigestion? It is caused
Management of Functional Dyspepsia (FD)
 Management of Functional Dyspepsia (FD) Amy S. Oxentenko, MD, FACG Program Director and Associate Chair, IM Associate Professor of Medicine Mayo Clinic, Rochester Outline Define functional dyspepsia (FD)
Management of Functional Dyspepsia (FD) Amy S. Oxentenko, MD, FACG Program Director and Associate Chair, IM Associate Professor of Medicine Mayo Clinic, Rochester Outline Define functional dyspepsia (FD)
The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia. Disclosures
 The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia Lana Bistritz MD FRCPC Royal Alexandra Hospital GI Update 2016 Disclosures I have no relevant financial disclosures I will be discussing off
The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia Lana Bistritz MD FRCPC Royal Alexandra Hospital GI Update 2016 Disclosures I have no relevant financial disclosures I will be discussing off
EMILOK Global. (omeprazole) Composition: Each capsule contains 20 mg omeprazole as enteric-coated
 EMILOK Global (omeprazole) Composition: Each capsule contains 20 mg omeprazole as enteric-coated granules. Properties: Emilok (omeprazole) belongs to the group of proton pump inhibitors, inhibits both
EMILOK Global (omeprazole) Composition: Each capsule contains 20 mg omeprazole as enteric-coated granules. Properties: Emilok (omeprazole) belongs to the group of proton pump inhibitors, inhibits both
COMPUS OPTIMAL THERAPY REPORT. Supporting Informed Decisions. À l appui des décisions éclairées
 OPTIMAL THERAPY REPORT COMPUS Volume 1, Issue 5 March 2007 Current Practice Analysis Report for the Prescribing and Use of Proton Pump Inhibitors (PPIs) Supporting Informed Decisions À l appui des décisions
OPTIMAL THERAPY REPORT COMPUS Volume 1, Issue 5 March 2007 Current Practice Analysis Report for the Prescribing and Use of Proton Pump Inhibitors (PPIs) Supporting Informed Decisions À l appui des décisions
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
SUPPLEMENTARY INFORMATION Associated with
 Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
In studies where all patients in the general population presenting with dyspepsia were referred for endoscopy, the prevalence of pathology was:
 There is so much we don t know in medicine that could make a difference, and often we focus on the big things, and the little things get fgotten. To highlight some smaller but imptant issues, we ve put
There is so much we don t know in medicine that could make a difference, and often we focus on the big things, and the little things get fgotten. To highlight some smaller but imptant issues, we ve put
ALL YOU NEED TO KNOW ABOUT INDIGESTION FUNDING RESEARCH INTO DISEASES OF THE GUT, LIVER & PANCREAS
 ALL YOU NEED TO KNOW ABOUT INDIGESTION FUNDING RESEARCH INTO DISEASES OF THE GUT, LIVER & PANCREAS THIS FACTSHEET IS ABOUT INDIGESTION Indigestion (also known as dyspepsia) is a term used to describe unpleasant
ALL YOU NEED TO KNOW ABOUT INDIGESTION FUNDING RESEARCH INTO DISEASES OF THE GUT, LIVER & PANCREAS THIS FACTSHEET IS ABOUT INDIGESTION Indigestion (also known as dyspepsia) is a term used to describe unpleasant
Grigoris Leontiadis, MD PhD. McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group
 Grigoris Leontiadis, MD PhD McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group No relevant financial relationships with any commercial interests CDDW/CASL Meeting Session:
Grigoris Leontiadis, MD PhD McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group No relevant financial relationships with any commercial interests CDDW/CASL Meeting Session:
RABEPRAZOL 10mg and 20mg Gastro-resistant Tablets
 PACKAGE LEAFLET: INFORMATION FOR THE USER RABEPRAZOL 10mg and 20mg Gastro-resistant Tablets RABEPRAZOLE This leaflet is a copy of the Summary of Product Characteristics and Patient Information Leaflet
PACKAGE LEAFLET: INFORMATION FOR THE USER RABEPRAZOL 10mg and 20mg Gastro-resistant Tablets RABEPRAZOLE This leaflet is a copy of the Summary of Product Characteristics and Patient Information Leaflet
TBURN TBURN BURN ARTBURN EARTBURN EART HEARTBURN: HOW TO GET IT OFF YOUR CHEST
 TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
Unmet Needs in the Management of Gastroesophageal Reflux Disease
 Unmet Needs in the Management of Gastroesophageal Reflux Disease Ronnie Fass MD Professor of Medicine Case Western Reserve University Chairman, Division of Gastroenterology and Hepatology Director, Esophageal
Unmet Needs in the Management of Gastroesophageal Reflux Disease Ronnie Fass MD Professor of Medicine Case Western Reserve University Chairman, Division of Gastroenterology and Hepatology Director, Esophageal
Second term/
 Second term/ 2015-2016 L. 1 Dr Mohammed AL-Zobaidy Learning objectives GIT pharmacology After completing this chapter the student will be able to: Recognise pathophysiological factors implicated in acid-peptic
Second term/ 2015-2016 L. 1 Dr Mohammed AL-Zobaidy Learning objectives GIT pharmacology After completing this chapter the student will be able to: Recognise pathophysiological factors implicated in acid-peptic
* Adults. NSAID associated peptic ulceration: - Acute treatment: 150 mg twice daily for 8 to 12 weeks, or 300mg nocte.
 Trade Name Aciloc 75 mg & 300 mg Film-coated tablets Generic Name Ranitidine Composition Each Aciloc 300 mg film-coated tablet contains: - Active ingredient: Ranitidine hydrochloride 336 mg equivalent
Trade Name Aciloc 75 mg & 300 mg Film-coated tablets Generic Name Ranitidine Composition Each Aciloc 300 mg film-coated tablet contains: - Active ingredient: Ranitidine hydrochloride 336 mg equivalent
Indigestion (1 of 5) What is indigestion? What causes indigestion?
 i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
EU RISK MANAGEMENT PLAN (EU RMP)
 EU RISK MANAGEMENT PLAN (EU RMP) Active substance(s) (INN or common name): Esomeprazole Pharmaco-therapeutic group (ATC Code): A02B C05 Name of Marketing Authorisation Holder or Applicant: Strength and
EU RISK MANAGEMENT PLAN (EU RMP) Active substance(s) (INN or common name): Esomeprazole Pharmaco-therapeutic group (ATC Code): A02B C05 Name of Marketing Authorisation Holder or Applicant: Strength and
 Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2017 UpToDate Patient education: Acid reflux (gastroesophageal reflux disease) in adults (The Basics) Written by the doctors and editors at UpToDate
Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2017 UpToDate Patient education: Acid reflux (gastroesophageal reflux disease) in adults (The Basics) Written by the doctors and editors at UpToDate
Concise guide to management of reflux disease in primary care
 Drug review GORD Concise guide to management of reflux disease in primary care Kumar Kanti Basu BSc, FRCP Reflux is a common disorder often aggravated by lifestyle and other medications. Our Drug review
Drug review GORD Concise guide to management of reflux disease in primary care Kumar Kanti Basu BSc, FRCP Reflux is a common disorder often aggravated by lifestyle and other medications. Our Drug review
Helicobacter Pylori Testing HELICOBACTER PYLORI TESTING HS-131. Policy Number: HS-131. Original Effective Date: 9/17/2009
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Approaches to uninvestigated dyspepsia
 iv42 DYSPEPSIA MANAGEMENT Approaches to uninvestigated dyspepsia R H Jones... Uninvestigated dyspepsia refers to patients with new or recurrent dyspeptic symptoms in whom no investigations have previously
iv42 DYSPEPSIA MANAGEMENT Approaches to uninvestigated dyspepsia R H Jones... Uninvestigated dyspepsia refers to patients with new or recurrent dyspeptic symptoms in whom no investigations have previously
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
High use of maintenance therapy after triple therapy regimes in Ireland
 High use of maintenance therapy after triple therapy regimes in Ireland K Bennett, H O Connor, M Barry, C O Morain, J Feely Department of Pharmacology & Therapeutics Department of Gastroenterology Trinity
High use of maintenance therapy after triple therapy regimes in Ireland K Bennett, H O Connor, M Barry, C O Morain, J Feely Department of Pharmacology & Therapeutics Department of Gastroenterology Trinity
Proton Pump Inhibitors Drug Class Prior Authorization Protocol
 Proton Pump Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review
Proton Pump Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review
SUCRALFATE TABLETS, USP
 1234567890 10 210002-01 SUCRALFATE TABLETS, USP DESCRIPTION Sucralfate is an -D-glucopyranoside, -D-fructofuranosyl-, octakis-(hydrogen sulfate), aluminum complex. It has the following structural formula:
1234567890 10 210002-01 SUCRALFATE TABLETS, USP DESCRIPTION Sucralfate is an -D-glucopyranoside, -D-fructofuranosyl-, octakis-(hydrogen sulfate), aluminum complex. It has the following structural formula:
HOW TO NATURALLY TREAT INDIGESTION YOGI CAMERON
 HOW TO NATURALLY TREAT INDIGESTION YOGI CAMERON Indigestion is a condition that is often a symptom of another, underlying condition and is associated with various forms of discomfort in the stomach including
HOW TO NATURALLY TREAT INDIGESTION YOGI CAMERON Indigestion is a condition that is often a symptom of another, underlying condition and is associated with various forms of discomfort in the stomach including
Clinical Trial of Efcid (Himcocid) in Patients of Acid Peptic Disease
 [The Antiseptic (2001): (98), 2, 50] Clinical Trial of Efcid (Himcocid) in Patients of Acid Peptic Disease Rangamani, K., Professor of Medicine, Bowring and Lady Curzon Hospitals, Shivajinagar, Bangalore,
[The Antiseptic (2001): (98), 2, 50] Clinical Trial of Efcid (Himcocid) in Patients of Acid Peptic Disease Rangamani, K., Professor of Medicine, Bowring and Lady Curzon Hospitals, Shivajinagar, Bangalore,
Urea Breath Test for Diagnosis of Helicobactor pylori. Original Policy Date 12:2013
 MP 2.04.04 Urea Breath Test for Diagnosis of Helicobactor pylori Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index
MP 2.04.04 Urea Breath Test for Diagnosis of Helicobactor pylori Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index
PATIENT INFORMATION LEAFLET PEPLOC RANGE
 Scheduling Status: S4 Proprietary name, Strength and Pharmaceutical Form: Peploc 20 mg tablets Peploc 40 mg tablets Read all of this leaflet carefully before using PEPLOC 20 mg or 40 mg Keep this leaflet.
Scheduling Status: S4 Proprietary name, Strength and Pharmaceutical Form: Peploc 20 mg tablets Peploc 40 mg tablets Read all of this leaflet carefully before using PEPLOC 20 mg or 40 mg Keep this leaflet.
INFORMATION FOR THE CONSUMER
 INFORMATION FOR THE CONSUMER IMPORTANT INFORMATION YOU SHOULD KNOW ABOUT NAT-Omeprazole DR (omeprazole magnesium delayed release tablets) Read this leaflet carefully. It contains general points about NAT-Omeprazole
INFORMATION FOR THE CONSUMER IMPORTANT INFORMATION YOU SHOULD KNOW ABOUT NAT-Omeprazole DR (omeprazole magnesium delayed release tablets) Read this leaflet carefully. It contains general points about NAT-Omeprazole
Gastroesophageal Reflux Disease (GERD)
 Gastroesophageal Reflux Disease (GERD) Information for patients UHN Read this handout to learn about: What gastroesohageal reflux (GERD) is Signs and symptoms How your doctor will know if you have it Tests
Gastroesophageal Reflux Disease (GERD) Information for patients UHN Read this handout to learn about: What gastroesohageal reflux (GERD) is Signs and symptoms How your doctor will know if you have it Tests
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY
 GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
Setting The setting was primary care. The economic study was conducted in Canada.
 Treating Helicobacter pylori infection in primary care patients with uninvestigated dyspepsia: the Canadian adult dyspepsia empiric treatment - Helicobacter pylori positive (CADET-Hp) randomised controlled
Treating Helicobacter pylori infection in primary care patients with uninvestigated dyspepsia: the Canadian adult dyspepsia empiric treatment - Helicobacter pylori positive (CADET-Hp) randomised controlled
Fecal incontinence causes 196 epidemiology 8 treatment 196
 Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
KK College of Nursing Peptic Ulcer Badil D ass Dass, Lecturer 25th July, 2011
 KK College of Nursing Peptic Ulcer Badil Dass, Lecturer 25 th July, 2011 Objectives: By the end of this lecture, the students t will be able to: Define peptic pp ulcer Describe the etiology and pathology
KK College of Nursing Peptic Ulcer Badil Dass, Lecturer 25 th July, 2011 Objectives: By the end of this lecture, the students t will be able to: Define peptic pp ulcer Describe the etiology and pathology
Dyspepsia is a problem commonly seen by primary
 Concise Review for Clinicians Nonulcer Dyspepsia: What It Is and What It Is Not G. RICHARD LOCKE III, MD Nonulcer dyspepsiais a description of persistent or recurrent upper abdominal pain or discomfort
Concise Review for Clinicians Nonulcer Dyspepsia: What It Is and What It Is Not G. RICHARD LOCKE III, MD Nonulcer dyspepsiais a description of persistent or recurrent upper abdominal pain or discomfort
DYSPEPSIA Dyspepsia indigestion during or after eating Full Heat, burning or pain Note: one of every four people
 What Is Dyspepsia? Dyspepsia, also known as indigestion, can have multiple symptoms. Feelings of indigestion happen during or after eating. If you have indigestion you might feel: Full during a meal. Painful
What Is Dyspepsia? Dyspepsia, also known as indigestion, can have multiple symptoms. Feelings of indigestion happen during or after eating. If you have indigestion you might feel: Full during a meal. Painful
Dr. Patsy Smyth, FNP-BC
 Dr. Patsy Smyth, FNP-BC Gastroparesis literally translated means stomach paralysis. Gastroparesis is a syndrome characterized by delayed gastric emptying in absence of mechanical obstruction of the stomach.
Dr. Patsy Smyth, FNP-BC Gastroparesis literally translated means stomach paralysis. Gastroparesis is a syndrome characterized by delayed gastric emptying in absence of mechanical obstruction of the stomach.
A Trip Through the GI Tract: Common GI Diseases and Complaints. Jennifer Curtis, MD
 A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
SUCRALFATE TABLETS, USP
 1234567890 10 210002 SUCRALFATE TABLETS, USP DESCRIPTION Sucralfate is an -D-glucopyranoside, -D-fructofuranosyl-, octakis-(hydrogen sulfate), aluminum complex. It has the following structural formula:
1234567890 10 210002 SUCRALFATE TABLETS, USP DESCRIPTION Sucralfate is an -D-glucopyranoside, -D-fructofuranosyl-, octakis-(hydrogen sulfate), aluminum complex. It has the following structural formula:
Patient information. Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4
 Patient information Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4 You have been diagnosed with laryngopharyngeal reflux (LPR), otherwise known as extra-oesophageal reflux
Patient information Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4 You have been diagnosed with laryngopharyngeal reflux (LPR), otherwise known as extra-oesophageal reflux
Omeprazole generichealth Enteric-coated Tablets
 Enteric-coated Tablets contain the active ingredient omeprazole CONSUMER MEDICINE INFORMATION What is in this leaflet This leaflet answers some common questions about. It does not contain all of the available
Enteric-coated Tablets contain the active ingredient omeprazole CONSUMER MEDICINE INFORMATION What is in this leaflet This leaflet answers some common questions about. It does not contain all of the available
Ranitidine hydrochloride syrup containing 150mg Ranitidine per 10mL
 Peptisoothe Ranitidine hydrochloride syrup containing 150mg Ranitidine per 10mL Presentation PEPTISOOTHE is a clear to pale yellow syrup with a spearmint flavour. Each 10mL of the syrup contains ranitidine
Peptisoothe Ranitidine hydrochloride syrup containing 150mg Ranitidine per 10mL Presentation PEPTISOOTHE is a clear to pale yellow syrup with a spearmint flavour. Each 10mL of the syrup contains ranitidine
IBS Irritable Bowel syndrome Therapeutics II PHCL 430
 Salman Bin AbdulAziz University College Of Pharmacy IBS Irritable Bowel syndrome Therapeutics II PHCL 430 Email:- ahmedadel.pharmd@gmail.com Ahmed A AlAmer PharmD R.S is 32-year-old woman experiences intermittent
Salman Bin AbdulAziz University College Of Pharmacy IBS Irritable Bowel syndrome Therapeutics II PHCL 430 Email:- ahmedadel.pharmd@gmail.com Ahmed A AlAmer PharmD R.S is 32-year-old woman experiences intermittent
NEXIUM INTRAVENOUS esomeprazole sodium
 NEXIUM INTRAVENOUS esomeprazole sodium Consumer Medicine Information What is in this leaflet This leaflet answers some of the common questions people ask about NEXIUM Intravenous (IV). It does not contain
NEXIUM INTRAVENOUS esomeprazole sodium Consumer Medicine Information What is in this leaflet This leaflet answers some of the common questions people ask about NEXIUM Intravenous (IV). It does not contain
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. (omeprazole delayed release capsules USP)
 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr Sandoz Omeprazole (omeprazole delayed release capsules USP) Read this carefully before you start taking Sandoz Omeprazole
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr Sandoz Omeprazole (omeprazole delayed release capsules USP) Read this carefully before you start taking Sandoz Omeprazole
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST
 COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
Dyspepsia and Chronic Gastritis
 Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Dyspepsia and Chronic Gastritis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky,
Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Dyspepsia and Chronic Gastritis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky,
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
1. The proposed strength, quantity, dosage form, dose and route of administration of the medicine including indication
 Investigation 10mg 1. The proposed strength, quantity, dosage form, dose and route of administration of the medicine including indication Blister packs of 14 Solid dose form for oral administration. It
Investigation 10mg 1. The proposed strength, quantity, dosage form, dose and route of administration of the medicine including indication Blister packs of 14 Solid dose form for oral administration. It
-Mohammad Ashraf. -Anas Raed. -Alia Shatnawi. 1 P a g e
 -1 -Mohammad Ashraf -Anas Raed -Alia Shatnawi 1 P a g e Dr. Alia started the lecture by talking about subjects we are going to cover through this course; you can refer to the record if you are interested.
-1 -Mohammad Ashraf -Anas Raed -Alia Shatnawi 1 P a g e Dr. Alia started the lecture by talking about subjects we are going to cover through this course; you can refer to the record if you are interested.
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. OMEPRAZOLE Omeprazole Delayed-Release Capsules
 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr OMEPRAZOLE Omeprazole Delayed-Release Capsules Read this carefully before you start taking OMEPRAZOLE and each time
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr OMEPRAZOLE Omeprazole Delayed-Release Capsules Read this carefully before you start taking OMEPRAZOLE and each time
OVERALL SUMMARY OF THE SCIENTIFIC EVALUATION OF LOSEC AND ASSOCIATED NAMES (SEE ANNEX I)
 ANNEX II SCIENTIFIC CONCLUSIONS AND GROUNDS FOR AMENDMENT OF THE SUMMARY OF PRODUCT CHARACTERISTICS, LABELLING AND PACKAGE LEAFLET PRESENTED BY THE EMEA 21 SCIENTIFIC CONCLUSIONS OVERALL SUMMARY OF THE
ANNEX II SCIENTIFIC CONCLUSIONS AND GROUNDS FOR AMENDMENT OF THE SUMMARY OF PRODUCT CHARACTERISTICS, LABELLING AND PACKAGE LEAFLET PRESENTED BY THE EMEA 21 SCIENTIFIC CONCLUSIONS OVERALL SUMMARY OF THE
Heartburn. Understanding and Treating. Heal n Cure For appointments call
 A C P S P E C I A L R E P O R T Understanding and Treating Heartburn What is Heartburn? It begins as a burning pain in the middle of your chest, behind the breastbone, often after a big meal. The burning
A C P S P E C I A L R E P O R T Understanding and Treating Heartburn What is Heartburn? It begins as a burning pain in the middle of your chest, behind the breastbone, often after a big meal. The burning
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 14 September 2011
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 14 September 2011 GAVISCON PEPPERMINT, chewable tablet B/20 (CIP code: 367 909-6) GAVISCON, oral suspension 250 ml
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 14 September 2011 GAVISCON PEPPERMINT, chewable tablet B/20 (CIP code: 367 909-6) GAVISCON, oral suspension 250 ml
PPIs: Good or Bad? 1. Basics of PPIs. Gastric Acid Basics. Outline. Gastric Acid Basics. Proton Pump Inhibitors (PPI)
 Outline Quick basics on Proton Pump Inhibitors (PPIs) PPIs: Good or Bad? What are potential risks of PPI therapy? How to approach your patients American Gastroenterology Association (AGA) recommendations
Outline Quick basics on Proton Pump Inhibitors (PPIs) PPIs: Good or Bad? What are potential risks of PPI therapy? How to approach your patients American Gastroenterology Association (AGA) recommendations
Rpts. GENERAL General Schedule (Code GE) Program Prescriber type: Dental Medical Practitioners Nurse practitioners Optometrists Midwives
 Esomeprazole 20mg Name, Restriction, Manner of esomeprazole 20 mg enteric tablet, 30 (8886Q) (029W) Gastric ulcer Peptic ulcer Treatment Phase: Initial treatment The therapy must be for initial treatment
Esomeprazole 20mg Name, Restriction, Manner of esomeprazole 20 mg enteric tablet, 30 (8886Q) (029W) Gastric ulcer Peptic ulcer Treatment Phase: Initial treatment The therapy must be for initial treatment
Investigating dyspepsia Rocco Maurizio Zagari, Lorenzo Fuccio, Franco Bazzoli
 DATE: 11/5/2008-10:27:27 ID:(BMJ)zagr584193 /(Jouve)bmj-001985 DOI: 10.1136/bmj.a1400 Topic(s): Type: InSection:review-article For the full versions of these articles see bmj.com CLINICAL REVIEW Investigating
DATE: 11/5/2008-10:27:27 ID:(BMJ)zagr584193 /(Jouve)bmj-001985 DOI: 10.1136/bmj.a1400 Topic(s): Type: InSection:review-article For the full versions of these articles see bmj.com CLINICAL REVIEW Investigating
How Rabeprazole Sandoz works
 Rabeprazole (as sodium) enteric coated tablets Consumer Medicine Information WHAT IS IN THIS LEAFLET This leaflet answers some common questions about Rabeprazole Sandoz. It does not contain all the available
Rabeprazole (as sodium) enteric coated tablets Consumer Medicine Information WHAT IS IN THIS LEAFLET This leaflet answers some common questions about Rabeprazole Sandoz. It does not contain all the available
Appropriate Use of Proton Pump Inhibitors (PPIs) Anderson Mabour, Pharm.D., BCPS Clinical Pharmacy Specialist
 Appropriate Use of Proton Pump Inhibitors (PPIs) Anderson Mabour, Pharm.D., BCPS Clinical Pharmacy Specialist Disclosures I have no actual or potential conflicts of interest to report in relation to this
Appropriate Use of Proton Pump Inhibitors (PPIs) Anderson Mabour, Pharm.D., BCPS Clinical Pharmacy Specialist Disclosures I have no actual or potential conflicts of interest to report in relation to this
Nexium 24HR. Tools and information for you and your pharmacy team NOW OTC FOR FREQUENT HEARTBURN. Consumer Healthcare Pfizer Inc.
 NOW OTC FOR FREQUENT HEARTBURN w e N Nexium 24HR P H A R M A S S I S T K I T Tools and information for you and your pharmacy team 2014 Pfizer Inc. NXM041468 05/14 Q: What is the indication for Nexium 24HR
NOW OTC FOR FREQUENT HEARTBURN w e N Nexium 24HR P H A R M A S S I S T K I T Tools and information for you and your pharmacy team 2014 Pfizer Inc. NXM041468 05/14 Q: What is the indication for Nexium 24HR
Functional Dyspepsia
 Linköping University Medical Dissertations No. 792 Functional Dyspepsia Symptoms and Response to Omeprazole in the Short Term by Elisabeth Bolling-Sternevald Department of Biomedicine and Surgery, Faculty
Linköping University Medical Dissertations No. 792 Functional Dyspepsia Symptoms and Response to Omeprazole in the Short Term by Elisabeth Bolling-Sternevald Department of Biomedicine and Surgery, Faculty
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. OMEPRAZOLE Omeprazole Delayed-Release Capsules
 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION OMEPRAZOLE Omeprazole Delayed-Release Capsules Read this carefully before you start taking OMEPRAZOLE and each time
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION OMEPRAZOLE Omeprazole Delayed-Release Capsules Read this carefully before you start taking OMEPRAZOLE and each time
