Chronic Interstitial Pneumonia in Silicosis and Mix-Dust Pneumoconiosis*
|
|
|
- Clemence Strickland
- 6 years ago
- Views:
Transcription
1 CHEST Chronic Interstitial Pneumonia in Silicosis and Mix-Dust Pneumoconiosis* Its Prevalence and Comparison of CT Findings With Idiopathic Pulmonary Fibrosis Hiroaki Arakawa, MD; Takeshi Johkoh, MD; Koichi Honma, MD; Yoshiaki Saito, MD; Yasutsugu Fukushima, MD; Hisao Shida, MD; and Naruhumi Suganuma, MD Original Research INTERSTITIAL LUNG DISEASE Background: Increased prevalence of chronic interstitial pneumonia (CIP) is reported in dust-exposed subjects. We investigated the prevalence of CIP in silicosis and mixed-dust pneumoconiosis and sought morphologic differences of CIP between the pneumoconiosis and idiopathic pulmonary fibrosis (IPF). Methods: We reviewed CT scans of 243 silicosis and mixed-dust pneumoconiosis patients to identify any cases of parenchymal lung lesions showing a CIP pattern, and compared the CT findings with those of 62 patients with IPF. Two observers independently scored CT images and classified the CT pattern as typical or not typical for IPF. Differences were sought between the groups using a nonparametric test, Fisher exact test, and a logistic regression analysis. A radiopathologic correlation was performed in 11 pneumoconiosis patients. Results: Twenty-eight patients (11.5%) showed CIP on CT. Seven patients (25%) showed a pattern not typical of IPF, while the remaining patients showed a pattern typical of IPF, 11 of which were confirmed pathologically. The extent of fibrosis did not differ between the groups; however, patients with pneumoconiosis showed less traction bronchiectasis (odds ratio [OR], 0.19; 95% confidence interval [CI], 0.08 to 0.48; p < 0.001), more subpleural homogeneous attenuation (OR, 2.56; 95% CI, 1.55 to 4.23; p < 0.001), and fibrosis was more randomly distributed (OR, ; 95% CI, 4.68 to ; p 0.007). Pathologically, subpleural homogeneous attenuation corresponded to dense fibrosis often with abundant silicotic nodules. Conclusions: Prevalence of CIP in pneumoconiosis was approximately 12% on CT. One fourth of patients showed an atypical IPF pattern, and the others showed a typical IPF pattern. (CHEST 2007; 131: ) Key words: CT; lung diseases, interstitial; pneumoconiosis; pulmonary fibrosis; radiograph Abbreviations: CI confidence interval; CIP chronic interstitial pneumonia; IPF idiopathic pulmonary fibrosis; OR odds ratio; PMF progressive massive fibrosis; UIP usual interstitial pneumonia There is a relationship between the content of crystalline silica in exposed dust and resultant pulmonary lesions in pneumoconiosis. 1 When the *From the Departments of Radiology (Dr. Arakawa), Pathology, (Dr. Honma), and Pulmonary Medicine and Clinical Immunology (Dr. Fukushima), Dokkyo University School of Medicine, Tochigi; Department of Radiology (Dr. Johkoh), Osaka University Graduate School of Medicine, Osaka; Departments of Respiratory Medicine (Dr. Saito) and Radiology (Dr. Shida), Rosai Hospital for Silicosis, Nikko; and Department of Environmental Health (Dr. Suganuma), Fukui Medical University, Fukui, Japan. The authors have no actual or potential conflicts of interest to disclose. dust is mainly crystalline silica, the fibrotic lesions are typical silicotic nodules. However, when the dust contains crystalline silica and less fibrogenic nonfibrous silicate, both silicotic nodules and mixed-dust Manuscript received October 17, 2007; revision accepted January 18, Reproduction of this article is prohibited without written permission from the American College of Chest Physicians ( org/misc/reprints.shtml). Correspondence to: Hiroaki Arakawa, MD, Dokkyo University School of Medicine, Department of Radiology, Mibu, Tochigi , Japan; arakawa@dokkyomed. ac.jp DOI: /chest Original Research
2 nodules coexist. 2 For this condition, the term mixeddust pneumoconiosis is proposed. 3 Exposure to pure crystalline silica alone, or in conjunction with nonfibrous silicate, usually causes nodular forms of fibrosis with upper-lobe predominance. 3,4 However, chronic interstitial pneumonia (CIP) in the lower lobes has been reported from 15.9 to 19.3% in autopsy series 5,6 of silicosis and coalworkers pneumoconiosis, although the dose-response relationship has not been established. In contrast, it has been reported that subjects engaged in some specific dusty occupations showed increased risks of idiopathic pulmonary fibrosis (IPF) with odds ratios (ORs) ranging from 1.34 to From these previous reports, it may be that CIP has a pathogenic linkage with occupational exposure to some specific dusts, although prevalence seems much higher in the presence of nodular fibrosis (silicosis and mixed-dust pneumoconiosis). Radiologic reports on CIP in silicosis and mixed-dust pneumoconiosis are scanty. Indeed, there has been only one radiologic report 12 on CIP in coal workers. However, this report included patients without pneumoconiosis as well. Furthermore, there has been no report compared CT findings of CIP in pneumoconiosis with those of IPF. The aims of the present study were twofold: the first was to investigate the prevalence of CIP in patients with silicosis and mixed-dust pneumoconiosis, and the second was to identify morphologic differences, if any, between CIP in silicosis and mixed-dust pneumoconiosis and IPF, using CT. In a limited number of cases, CT findings were correlated with pathology findings. Patients Materials and Methods At the national hospital for pneumoconiosis, 243 patients with silicosis and mixed-dust pneumoconiosis were referred for chest CT between 2000 and CT scan was performed as part of an annual surveillance for patients with radiographic evidence of silicosis or mixed-dust pneumoconiosis. The diagnosis was made by our experienced physicians based on the occupational history of significant dust exposure, appropriate time interval between the exposure and the development of the disease, and radiographic abnormalities consistent with silicosis or mixed-dust pneumoconiosis (profusion of small opacities 1/0 according to International Labor Office). All patients underwent at least two scans during the period. Presence of fine inspiratory crackles on auscultation, degree of dyspnea, and pulmonary function test results were reviewed from patient charts. Degree of dyspnea was graded using a 3-point scale based on the ability of walking: mild indicates that the patient can walk like a healthy subject of similar age; moderate indicates that the patient cannot walk like a healthy subject of the similar age but can walk 50 m without rest; and severe indicates that the patient cannot walk 50 m without rest. Patients were excluded if they showed an occupational history of possible exposure to asbestos and hard metals. Spirometry was performed within 1 month of CT scans using computerized pulmonary function instruments (FUDAC 70; Fukuda Denshi; Tokyo, Japan; or CHESTAC 11; Chest; Tokyo, Japan). FVC was expressed as a percentage of the predicted value on the basis of the patient s sex, age, and height. 13 Sixty-two IPF patients were identified from the radiology department information system at our university hospital between 2002 and Diagnosis of IPF was made based on a combination of clinical, thin-section CT, and pathologic findings. 14 Institutional review board approvals were obtained, but informed consent from patients was waived because of the retrospective analyses of this study. CT Techniques CT scanning from the lung apex to the base was performed with the patient in the supine position, and during deep inspiration without contrast material injection (Somatom-Plus 4 or Volume Zoom; Siemens Medical Systems; Forschheim, Germany). Scans were performed using the spiral technique with 10-mm collimation, and a spiral pitch of 1:1 (Somatom-Plus 4) or 2.5-mm collimation and a spiral pitch of 1:5 (Volume Zoom) to produce thick section images (10 mm and 8 mm, respectively), followed by a nonspiral technique with 1- to 2-mm collimation at 10- to 20-mm intervals. Two hundred eight patients with pneumoconiosis were scanned with the Somatom-Plus 4, and the other patients were scanned with Volume Zoom. Thin-section images were reconstructed with a high-frequency algorithm. Images were displayed and photographed with a window width of 1,200 to 1500 Hounsfield units, and at a level of 650 to 700 Hounsfield units. Image Interpretation Two chest radiologists with 14 years and 16 years of experience, respectively, in chest CT interpretation reviewed the CT images. We identified patients with CIP among silicosis and mixed-dust pneumoconiosis patients based on CT findings. CT findings suggestive of CIP included the following: (1) the presence of diffuse reticular opacities with or without ground-glass attenuation, traction bronchiectasis, honeycombing, or subpleural homogeneous attenuation 15,16 ; or (2) the presence of diffuse nonsegmental ground-glass opacities with or without reticular opacities that did not improve during follow-up of 1 year. 17 Cases with only unilateral involvement were not included. Case identification was initially performed by one of the chest radiologists who selected the candidate cases for inclusion. The final inclusion was done based on the consensus of the two chest radiologists, which was performed a few months later. After identifying CIP with silicosis and mixed-dust pneumoconiosis, CT abnormalities were evaluated by estimating the extent of each CT abnormalities at the upper, middle, and lower lung zones according to methods used by Copley et al 18 and Hering and Kraus. 19 The border of upper and middle lung zones was set at the level of tracheal carina, and that of middle and lower lung zones was set at the level of inferior pulmonary vein. All CT images were reviewed and the estimation of extent was made based on the visual assessment of each abnormality in each lung zone. CT images of patients with IPF were reviewed after those of silicosis and mixed-dust pneumoconiosis patients. Two independent chest radiologists performed the review of CT images, and the extent of each abnormality was calculated. The average of the scores was used for final analysis. Disagreements on the presence or absence of emphysema, honeycombing, and subpleural homogeneous attenuation were later resolved by consensus. Ground-glass attenuation was defined as the hazy increase of CHEST / 131 / 6/ JUNE,
3 lung attenuation that did not obscure the margins of underlying vessels. Subpleural homogeneous attenuation was defined as the area showing homogeneously increased lung attenuation that obscured the margins of vessels. 20 Traction bronchiectasis was defined as irregularly dilated bronchi in the area with groundglass attenuation of reticular opacities. 21 Honeycombing was defined as the cluster of cystic airspaces that had thick walls. 20 Extent of CIP: Extent of CIP, defined as the combined areas with reticular opacity, ground-glass attenuation, subpleural homogeneous attenuation and honeycombing, was visually estimated to the nearest 5%. The mean value represented the extent of fibrosis. Areas of Reticular Opacities, Ground-Glass Opacity, Honeycombing, Subpleural Homogeneous Attenuation, and Emphysema: Each area with reticular opacities, ground-glass opacity, honeycombing, subpleural homogeneous attenuation, and emphysema was visually estimated to the nearest 5%, and mean values were recorded. Coarseness of Fibrosis: Coarseness of fibrosis was assigned as follows: grade 0, ground-glass opacification with no reticular element or cysts; grade 1, predominantly fine intralobular fibrosis without cysts; grade 2, presence of a microcystic pattern (maximum diameter up to 4 mm); or grade 3, predominantly macrocystic pattern (maximum diameter 4 mm). Scores for the three zones were summed to provide an overall coarseness score (range, 0 to 9). Profusion of Silicotic Nodules: Profusion of silicotic nodules was graded using a 4-point scale: score 0, no nodule; score 1, definite presentation of pneumoconiotic nodules but few in number; score 2, moderately numerous pneumoconiotic nodules; and score 3, numerous nodules that obscure the normal anatomic lung structures. 19 Scores of the three zones were summed to provide an overall score (range, 0 to 9). Severity of Traction Bronchiectasis: Severity of traction bronchiectasis was graded comparing the diameter of the airway with that of the adjacent pulmonary artery using a 4-point scale, and scores in three lung zones were summed to yield an overall score (range, 0 to 9): score 0, no traction bronchiectasis; score 1, traction bronchiectasis present but mild in degree (comparable diameter with the artery); score 2, moderately severe traction bronchiectasis (up to twice the diameter of the artery); and score 3, severe traction bronchiectasis (more than twice the diameter of the artery). Predominant Distributions of Fibrosis: Predominant distributions of fibrosis were determined to be subpleural, peribronchial, or random. Summation of Diameters: Summation of diameters of all the progressive massive fibrosis (PMF) observed in each patient was calculated in centimeters. PMF was defined as the pneumoconiotic nodule 1 cm in largest diameter. Following assessment of images, the overall findings were classified into either pattern typical or atypical of IPF. 15,16,22,23 Pathology Data The lungs were inflated with formalin, and a pathologist with 24 years of experience in pneumoconiosis prepared tissue specimens. Hematoxylin-eosin and elastic-goldner stains were usually employed. Tissue specimens from the corresponding areas with CIP on CT were examined with a microscope. Profusion of silicotic nodules was evaluated, and patterns of fibrosis were assessed as usual interstitial pneumonia (UIP), nonspecific interstitial pneumonia, or desquamative interstitial pneumonia patterns. 14 Statistical Analysis Results were expressed as medians with ranges. Group comparisons of continuous variables were performed using the Kruskal Wallis test with the analysis software (SPSS version 11.01J; SPSS Japan; Tokyo, Japan). The Fisher exact test was used to examine differences in proportions for each CT finding between groups. Observer variation was evaluated using the weighted coefficient for semicategorical variables 24 or the single-determined SD for quantitative data. 18,25 Independent differences in CT features between IPF and pneumoconiosis were identified using a stepwise logistic regression. Age, sex, extent of ground glass opacification, irregular opacities, honeycombing, emphysema, severity of bronchiectasis, coarseness of fibrosis, and distribution of fibrosis were included as covariates. Variables were retained in logistic regression models if they contributed to the explanatory power of the regression equation (p 0.10). Results Demographic Data of Patients With Pneumoconiosis Among the 243 cases of pneumoconiosis, 28 patients (11.5%) were identified to have CIP on CT. Their ages ranged from 63 to 82 years (median, 72 years), and all were men. Eleven patients were tunnel workers, 8 patients were metal ore miners, 3 patients were coal miners, 2 patients were stonemasons, and 1 patient was a foundry worker. The other three patients were exposed to various occupational dusts. Mean exposure period was 24 years (range, 11 to 40 years). Four patients were current smokers, 21 patients were ex-smokers, and 2 patients never smoked. Smoking history was not available for one patient. Clinical findings and results of pulmonary function tests are shown in Table 1. Clinically, 13 patients showed fine inspiratory crackles on auscultation, 17 patients had a dry cough, and 10 patients showed restrictive pulmonary functional deficits as measured by a vital capacity 70%. Ten patients (35.7%) complained of no or only mild dyspnea, all of whom showed both scores for fibrosis and emphysema 15% and 18%, respectively. Primary lung cancer developed in five patients (17.9%) during the follow-up period. Table 1 Demographic Data in Patients With Pneumoconiosis and IPF* Variables IPF (n 62) Pneumoconiosis (n 28) p Value Age, yr 72 (56 91) 71 (63 82) NS Male/female gender 47/15 28/ Smoking, pack-yr 32 (0 200) 30 (0 74) NS No smoking data 2 (3.2) 1 (3.6) NS *Data are presented as median (range) or No. unless otherwise indicated. NS not significant. Data are presented as No. of patients (%) Original Research
4 Pneumoconiosis vs IPF Diagnosis of IPF was made from surgical lung biopsies in 14 patients, and by clinical and CT findings without surgical lung biopsy in 48 patients. 14 Age and smoking habit did not differ between the two groups (p 0.05; Table 1). CT features of the 62 patients with IPF and 28 patients with silicosis and mixed-dust pneumoconiosis are summarized in Table 2. For the combined group of 90 patients, interobserver variation expressed as the single-determination SD was 7.4% for the extent of fibrosis, 5.9% for the extent of groundglass opacity, 4.8% for the extent of reticular opacity, 2.6% for the extent of honeycombing, 1.3% for the extent of subpleural homogeneous attenuation, and 2.8% for the extent of emphysema. The weighted coefficients for coarsenesses of fibrosis, traction bronchiectasis, and silicotic nodules were 0.70, 0.68, and 0.70, respectively. Besides pneumoconiotic nodules and PMF, extents of the following CT abnormalities differed significantly between the IPF and pneumoconiosis groups, respectively (Table 2): ground-glass opacity (12.1% vs 7.9%, p 0.028), reticular opacity (11.7% vs 8.3%, p 0.023), subpleural homogeneous attenuation (0 vs 1.3%, p 0.001), emphysema (1.3% vs 3.8%, p 0.017), and traction bronchiectasis (2.0 vs 1.0, p 0.046). However, extent of fibrosis, honeycombing, and coarseness of fibrosis did not differ between the two groups. Incidence of subpleural homogeneous attenuation differed significantly (p 0.01); however, incidences of honeycombing and emphysema did not differ between the two groups. Distribution of fibrosis was predominantly peripheral in 21 cases (75%) of silicosis and mixeddust pneumoconiosis and 57 cases (91.9%) of IPF (Table 2). A predominant random distribution was noted in seven patients (25%) with silicosis and mixed-dust pneumoconiosis, and two patients (3.2%) with IPF, and the difference in distributions was significant (p 0.004). A logistic regression model was used to identify CT features that differed independently between IPF and pneumoconiosis. After adjustment for age and sex, patients with silicosis and mixed-dust pneumoconiosis were shown to have less traction bronchiectasis (OR, 0.19; 95% confidence interval [CI], 0.08 to 0.48; p 0.001), more subpleural homogeneous attenuation (OR, 2.56; 95% CI, 1.55 to 4.23; p 0.001), and fibrosis was more randomly distributed (OR, ; 95% CI, 4.68 to ; p 0.007). These findings were independent of the proportion of ground-glass opacity, reticular opacities, emphysema, honeycombing, and coarseness of fibrosis, none of which differed independently between IPF and pneumoconiosis. CT images of CIP in silicosis and mixed-dust pneumoconiosis showed predominant ground-glass opacities in 11 patients (39.3%). The pattern typical of IPF was observed in 21 patients, and a pattern not typical of IPF was seen in 7 patients (25%). The seven patients with a pattern not typical of IPF showed predominantly ground-glass opacity with no focal area of honeycombing (n 5) [Fig 1] or with a focal area of honeycombing (n 2). Interobserver agreement was almost perfect ( 0.91). Pathology Analysis Pathology data were obtained from autopsies (n 9) or surgically resected lower lobes (n 2) at a mean of 6 months (range, 1 to 14 months) after CT study. Diagnoses in all patients (median age, 74 years) were made pathologically with UIP patterns with honeycombing, while consensus reading of CT images in these 11 patients revealed the pattern typical of IPF in 10 patients and pattern not typical of IPF in 1 patient. The extents of ground-glass opacity, reticular opacity, honeycombing, and subpleural homogeneous attenuation were 8.3% (range, 3 to 43%), 15% (range, 5.8 to 21.7%), 6.7% (range, 1.7 to 20.8%), and 4.2% (range, 0 to 12.5%), respectively. The area with subpleural homogeneous atten- Table 2 Thin-Section CT Scores in Patients With Pneumoconiosis and IPF* Variables IPF (n 62) Pneumoconiosis (n 28) p Value Ground-glass opacity 12.1 (1 41) 7.9 ( ) Reticular opacity 11.7 ( ) 8.3 ( ) Honeycombing 3.3 (0 51.7) 2.5 (0 23.3) NS Fibrosis extent 21.3 ( ) 17.9 ( ) NS Subpleural homogeneous density 0 (0 8.3) 1.3 (0 14.2) Emphysema 1.3 (0 38.3) 3.8 (0 47.5) Traction bronchiectasis 2 (0 7) 1 (0 5.5) Coarseness 5 (2.3 9) 3.5 (0 6.5) NS Silicotic nodules (0 6.5) PMF 0 3 (0 20) *Data are presented as median (range). See Table 1 for expansion of abbreviation. CHEST / 131 / 6/ JUNE,
5 Figure 1. Top, A: CIP in an 82-year-old man with silicosis. This was the only case in which CT and pathologic diagnoses were contradictory. Thin-section CT scans at the right middle and lower lobes showed patchy and extensive ground-glass opacity with reticulation. Traction bronchiectasis is seen in the ground-glass opacity (arrows), but honeycombing is lacking. Peripheral predominance of fibrosis is not obvious. The CT diagnosis by two reviewers was, coincidentally, a nonspecific interstitial pneumonia pattern. Bottom, B: Photomicrograph (Elastic-Goldner stain, original 5) from the right lower lobe showing CIP with honeycombing, and mildly scattered silicotic nodules (arrows) in the interstitium. Pathology diagnosis was an UIP pattern with honeycombing. uation on CT was found to correspond pathologically to an area with dense collagen deposition often with silicotic nodules (Fig 2). In all cases, silicotic nodules were identified in the area with CIP: mild in two patients, moderate in six patients, and severe in three patients. In moderate and severe cases, silicotic Figure 2. Top, A: CIP in a 74-year-old man with silicosis. Thin-section CT scan at the lung base shows subpleural honeycomb cysts and homogeneous attenuation; note that there is small right pleural effusion (arrows). Both reviewers interpreted this case as an IPF/UIP pattern. Bottom, B: Photomicrograph (Elastic-Goldner stain, original 5) from the right lower lobe showing coalescence of numerous silicotic nodules with interstitial fibrosis in the area with subpleural cysts (honeycombing). This corresponds to subpleural homogeneous attenuation on CT. Pathology diagnosis was a UIP pattern with honeycombing Original Research
6 nodules diffusely scattered in the area with CIP (Fig 1), or were extremely abundant in and around areas of honeycomb cysts (Fig 2). In the latter cases, silicotic nodules coalesced to form dense areas of fibrosis, which corresponded to subpleural homogeneous attenuation on CT. Discussion Our study revealed that 11.5% of patients with silicosis and mixed-dust pneumoconiosis showed CIP on CT. Among them, 35.7% had no or only mild clinical findings typical for IPF. This was not surprising considering that the study population included patients who were under surveillance for pneumoconiosis. Patients who did not have significant symptoms showed both CT scores for emphysema and fibrosis 18% and 15%, respectively, and this might indicate that CT measures of abnormalities were useful in estimating clinical derangements of lung diseases. Considering the estimate of prevalence of CIP in the general population of approximately 20 per 100,000 adult males, 26 the figure of 11.5% seen in our 243 consecutive silicosis and mixed-dust pneumoconiosis patients was extremely high in spite that patients were not exposed to asbestos or other minerals known to cause CIP. Pathology confirmation of CIP in silicosis and mixed-dust pneumoconiosis has been made from several autopsy series. 5,6 McConnochie et al 6 reported a prevalence of 15.9 to 17.1% among a randomly selected series with coal dust exposure, and Honma and Chiyotani 5 reported a 19.3% among 233 consecutive silicosis and mixeddust pneumoconiosis. Katabami et al, 27 based on CT observation, reported the prevalence of 10% among 563 patients exposed mainly to coal dust. It might be interesting to note that prevalence of CIP does not differ among patients exposed to different fibrogenic potential because the crystalline silica is much more fibrogenic than the coal dust. 28 Even with the epidemiologic evidence that some kinds of inhaled dusts enhance development of pulmonary fibrosis with ORs ranging from 1.34 to 12.55, 8 11 and that a few reports 7,9 confirmed the dose-response relationship that indicated a significant increase of OR with increasing exposure time to metal, the prevalence in silicosis and mixed-dust pneumoconiosis seems extremely high. The increased prevalence of IPF in dust-exposed patients is partly explained by repeated injuries of alveolar epithelial cells, which is modified by the host condition including the clearance of inhaled dust and genetic predisposition. 29 Our pneumoconiosis patients, all of whom showed evidence of nodular fibrosis in upper lobes, must have been exposed to a large amount of dust containing silica and nonfibrous silicate, and both the bronchial and lymphatic clearance systems were impaired. We suppose that these host conditions as well as smoking, longstanding exposure to a large amount of dust, effect of repeated infections, and hypersensitivity reactions to inhaled dust could contribute to the high prevalence of CIP in our subjects. Although 21 patients in our series showed IPF patterns on CT (11 cases were pathologically confirmed), 7 patients (25%) showed a pattern not typical of IPF. In addition, the typical peripheral distribution of fibrosis was lacking in seven pneumoconiosis patients, and this was one of the independent factors strongly suggestive of CIP associated with pneumoconiosis. When each CT abnormality was analyzed separately, however, only subpleural homogeneous attenuation, lack of traction bronchiectasis, and random distribution of fibrosis were independent factors suggestive of CIP associated with silicosis and mixed-dust pneumoconiosis. The presence of silicotic nodules was presumed to contribute to differences in CT appearances. Pathologically, areas of homogeneous attenuation were composed of dense accumulations of collagen and silicotic nodules. Because areas with interstitial fibrosis shrink, profusion of silicotic nodules in these areas is expected to be extremely high, forming the basis for dense collagen deposits giving the appearance of homogeneous attenuation in subpleural zones. Mildness of traction bronchiectasis in silicosis and mixeddust pneumoconiosis is considered to result from stiff lungs with fibrotic nodules diffusely scattered, and it may not be easy for airways to become dilated. We suppose that CIP of our pneumoconiosis patients might well correspond to pathologic UIP, with CT features being modified by coexistence of pneumoconiotic nodules, retraction of lung parenchyma, and extensive fibrotic process involving both the peripheral and central portions of lungs on axial section. One of the possible limitations of our study was that we scored each CT finding, and compared extents between pneumoconiosis and IPF groups. However, we did not compare combined CT appearances between the two groups, which might be a limitation in our methodologies. Although subpleural homogeneous attenuation and traction bronchiectasis differed significantly, overall appearance may not be similar to each other. This was suggested by the fact that seven cases were regarded as atypical of IPF on CT. We suppose that the use of two different methods in comparing the two groups will complement our understanding of differences. Second, not all patients had pathology diagnosis of CIP. To exclude transient interstitial abnormalities, we included only those cases that showed persistent abnormalities over years. Third, the pathology data were obtained 6 months after CT study on average. CHEST / 131 / 6/ JUNE,
7 The pathology changes observed on the autopsy or surgical specimen might not completely correspond to those observed by CT. However, because the progression of CIP is slow, and what we observed and correlated between CT and pathology were chronic changes such as the profusion of silicotic nodules, we suppose the discrepancies were small. Fourth, in the CT review session, we scored the pneumoconiosis cases followed by IPF cases. This can be interpreted as the source for bias. However, in reality, the reviewer could easily notice whether the case under review was IPF or pneumoconiosis because all the pneumoconiosis cases showed pneumoconiotic nodules or PMF in the upper lobes. In conclusion, CIP was seen in 11.5% of 243 consecutive patients who underwent chest CT, and was considered a frequent manifestation in silicosis and mixed-dust pneumoconiosis. Pattern atypical of IPF was not uncommon (25% of cases), and the predominant distribution of subpleural fibrosis, which is characteristic in IPF, was often lacking. The other distinguishing CT findings were the higher incidence and extent of subpleural homogeneous attenuation and less prominent traction bronchiectasis in the pneumoconiosis group than in the IPF group. ACKNOWLEDGMENT: The Rosai Hospital for Silicosis was closed at the end of March 2006 by the decision of Japanese Government. The authors thank for Reiko Hirayama and Hiromi Nakayama for their assistance. References 1 Nagelschmidt G. The relation between lung dust and lung pathology in pneumoconiosis. Br J Ind Med 1960; 17: Green FH, Churg A. Diseases due to nonasbestos silicates. In: Churg A, Green FH, eds. Pathology of occupational lung disease. Baltimore, MD: Williams and Wilkins, 1998; Honma K, Abraham JL, Chiyotani K, et al. Proposed criteria for mixed-dust pneumoconiosis: definition, descriptions, and guidelines for pathologic diagnosis and clinical correlation. Hum Pathol 2004; 35: Diseases associated with exposure to silica and nonfibrous silicate minerals. Silicosis and Silicate Disease Committee. Arch Pathol Lab Med 1988; 112: Honma K, Chiyotani K. Diffuse interstitial fibrosis in nonasbestos pneumoconiosis: a pathological study. Respiration 1993; 60: McConnochie K, Green FHY, Vallyathan V, et al. Interstitial fibrosis in coal workers: experience in Wales and West Virginia. In: Dodgson J, McCallum RI, Bailey MR, et al, eds. British Occupational Hygiene Society 6th International Symposium. Cambridge, UK: Pergamon Press, 1988; Baumgartner KB, Samet JM, Coultas DB, et al. Occupational and environmental risk factors for idiopathic pulmonary fibrosis: a multicenter case-control study: collaborating Centers. Am J Epidemiol 2000; 152: Iwai K, Mori T, Yamada N, et al. Idiopathic pulmonary fibrosis: epidemiologic approaches to occupational exposure. Am J Respir Crit Care Med 1994; 150: Hubbard R, Lewis S, Richards K, et al. Occupational exposure to metal or wood dust and aetiology of cryptogenic fibrosing alveolitis. Lancet 1996; 347: Scott J, Johnston I, Britton J. What causes cryptogenic fibrosing alveolitis? A case-control study of environmental exposure to dust. BMJ 1990; 301: Miyake Y, Sasaki S, Yokoyama T, et al. Occupational and environmental factors and idiopathic pulmonary fibrosis in Japan. Ann Occup Hyg 2005; 49: Brichet A, Tonnel AB, Brambilla E, et al. Chronic interstitial pneumonia with honeycombing in coal workers. Sarcoidosis Vasc Diffuse Lung Dis 2002; 19: American Thoracic Society. Standardization of spirometry, 1994 update. Am J Respir Crit Care Med 1995; 152: American Thoracic Society/European Respiratory Society International Multidisciplinary Consensus Classification of the idiopathic interstitial pneumonias. Am J Respir Crit Care Med 2002; 165: MacDonald SL, Rubens MB, Hansell DM, et al. Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparative appearances at and diagnostic accuracy of thinsection CT. Radiology 2001; 221: Nishimura K, Kitaichi M, Izumi T, et al. Usual interstitial pneumonia: histologic correlation with high-resolution CT. Radiology 1992; 182: Hartman TE, Swensen SJ, Hansell DM, et al. Nonspecific interstitial pneumonia: variable appearance at high-resolution chest CT. Radiology 2000; 217: Copley SJ, Wells AU, Sivakumaran P, et al. Asbestosis and idiopathic pulmonary fibrosis: comparison of thin-section CT features. Radiology 2003; 229: Hering K, Kraus T. Coding CT-classification in occupational and environmental respiratory disease. In: Kusaka Y, Hering K, Parker J, eds. International classification of HRCT for occupational and environmental respiratory diseases. Tokyo, Japan: Springer, 2005; Austin JH, Muller NL, Friedman PJ, et al. Glossary of terms for CT of the lungs: recommendations of the Nomenclature Committee of the Fleischner Society. Radiology 1996; 200: Webb WR, Muller NL, Naidich DP. An illustrated glossary of HRCT terms. In: Webb WR, Muller NL, Naidich DP, eds. High-resolution CT of the lung. Philadelphia, PA: Lippincott- Raven, 2001; Sumikawa H, Johkoh T, Ichikado K, et al. Usual interstitial pneumonia and chronic idiopathic interstitial pneumonia: analysis of CT appearance in 92 patients. Radiology 2006; 241: Tsubamoto M, Muller NL, Johkoh T, et al. Pathologic subgroups of nonspecific interstitial pneumonia: differential diagnosis from other idiopathic interstitial pneumonias on high-resolution computed tomography. J Comput Assist Tomogr 2005; 29: Cohen J. Weighted : nominal scale agreement with provision for scaled disagreement or partial credit. Psychol Bull 1968; 70: Brennan P, Silman A. Statistical methods for assessing observer variability in clinical measures. BMJ 1992; 304: Coultas DB, Zumwalt RE, Black WC, et al. The epidemiology of interstitial lung diseases. Am J Respir Crit Care Med 1994; 150: Katabami M, Dosaka-Akita H, Honma K, et al. Pneumoconiosis-related lung cancers: preferential occurrence from diffuse interstitial fibrosis-type pneumoconiosis. Am J Respir Crit Care Med 2000; 162: Heppleston AG, Kulonen E, Potila M. In vitro assessment of the fibrogenicity of mineral dusts. Am J Ind Med 1984; 6: Taskar VS, Coultas DB. Is idiopathic pulmonary fibrosis an environmental disease? Proc Am Thorac Soc 2006; 3: Original Research
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
Asbestosis and other pulmonary fibrosis in asbestos-exposed workers: high-resolution CT features with pathological correlations
 Eur Radiol (2016) 26:1485 1492 DOI 10.1007/s00330-015-3973-z CHEST Asbestosis and other pulmonary fibrosis in asbestos-exposed workers: high-resolution CT features with pathological correlations Hiroaki
Eur Radiol (2016) 26:1485 1492 DOI 10.1007/s00330-015-3973-z CHEST Asbestosis and other pulmonary fibrosis in asbestos-exposed workers: high-resolution CT features with pathological correlations Hiroaki
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Restrictive lung diseases
 Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Idiopathic interstitial pneumonias (IIPs) are a group of
 SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
DISEASES OF THE RESPIRATORY SYSTEM LECTURE 5 DR HEYAM AWAD FRCPATH
 DISEASES OF THE RESPIRATORY SYSTEM LECTURE 5 DR HEYAM AWAD FRCPATH RESTRICTIVE, INTERSTITIAL LUNG DISESAES. FIROSING DISESES. GRANULOMATOUS DISEASES. EOSINOPHILIC. SMOKING RELATED. FIBROSING DISEASES
DISEASES OF THE RESPIRATORY SYSTEM LECTURE 5 DR HEYAM AWAD FRCPATH RESTRICTIVE, INTERSTITIAL LUNG DISESAES. FIROSING DISESES. GRANULOMATOUS DISEASES. EOSINOPHILIC. SMOKING RELATED. FIBROSING DISEASES
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
Daria Manos RSNA 2016 RC 401. https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html
 Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Tomodensitometric detection in pneumoconiosis due to amorphous silica: correlation between conditions of exposure and radiological patterns.
 Tomodensitometric detection in pneumoconiosis due to amorphous silica: correlation between conditions of exposure and radiological patterns. Poster No.: C-1590 Congress: ECR 2011 Type: Scientific Exhibit
Tomodensitometric detection in pneumoconiosis due to amorphous silica: correlation between conditions of exposure and radiological patterns. Poster No.: C-1590 Congress: ECR 2011 Type: Scientific Exhibit
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Is it really honeycombing? Limitations and pitfalls in radiological diagnosis of honeycombing.
 Is it really honeycombing? Limitations and pitfalls in radiological diagnosis of honeycombing. J. Arenas-Jiménez, E. García-Garrigós, M. Sirera-Matilla; M.C. Planells-Alduvin, F.I. Aranda* Hospital General
Is it really honeycombing? Limitations and pitfalls in radiological diagnosis of honeycombing. J. Arenas-Jiménez, E. García-Garrigós, M. Sirera-Matilla; M.C. Planells-Alduvin, F.I. Aranda* Hospital General
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP)
 Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview
 The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
Jingcai Xing 1,2,, Xiji Huang 1,, Lijuan Yang 3, Yuewei Liu 1, Hai Zhang 1 and Weihong Chen 1. Journal of Occupational Health
 Jingcai XING, et al.: Comparison of HRCT and FSR in Coal Workers Pneumoconiosis J Occup Health 2014; 56: 301 308 301 Journal of Occupational Health Comparison of High-resolution Computerized Tomography
Jingcai XING, et al.: Comparison of HRCT and FSR in Coal Workers Pneumoconiosis J Occup Health 2014; 56: 301 308 301 Journal of Occupational Health Comparison of High-resolution Computerized Tomography
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel
 Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Epidemiology and classification of smoking related interstitial lung diseases
 Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX
 INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
THE ROLE OF COAL MINE DUST EXPOSURE IN THE DEVELOPMENT OF PULMONARY EMPHYSEMA
 Ann. occup. Hyg., Vol. 41, Supplement 1, pp. 352-357. 1997 British Occupational Hygiene Society Published by Elsevier Science Ltd Printed in Great Britain 0003-4878/97 $17.00 + 0.00 Inhaled Particles VIII
Ann. occup. Hyg., Vol. 41, Supplement 1, pp. 352-357. 1997 British Occupational Hygiene Society Published by Elsevier Science Ltd Printed in Great Britain 0003-4878/97 $17.00 + 0.00 Inhaled Particles VIII
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
Dr. Heyam Awad Pathology sheet #5 cont. Restrictive lung diseases
 We were talking about the restrictive lung diseases (interstitial lung diseases) and they're:- Fibrosing diseases. Granulomatous diseases. Eosinophilic. smoking related. * Notes:- 1) Cough occur in restrictive
We were talking about the restrictive lung diseases (interstitial lung diseases) and they're:- Fibrosing diseases. Granulomatous diseases. Eosinophilic. smoking related. * Notes:- 1) Cough occur in restrictive
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review.
 Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Non-neoplastic Lung Disease II
 Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
The radiological differential diagnosis of the UIP pattern
 5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after smoking cessation
 Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Diagnostic challenges in IPF
 Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Low Grade Coal Worker's Pneumoconiosis
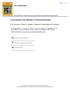 Acta Radiologica ISSN: 0284-181 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Low Grade Coal Worker's Pneumoconiosis P. A. Gevenois, E. Pichot, F. Dargent, S. Dedeire,
Acta Radiologica ISSN: 0284-181 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Low Grade Coal Worker's Pneumoconiosis P. A. Gevenois, E. Pichot, F. Dargent, S. Dedeire,
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Patient with IPF and no honeycombing on HRCT. Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens
 Patient with IPF and no honeycombing on HRCT Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 76-year-old male patient presented with progressive exertional dyspnoea refractory
Patient with IPF and no honeycombing on HRCT Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 76-year-old male patient presented with progressive exertional dyspnoea refractory
Case 1 : Question. 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random
 Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Xiaohuan Pan 1,2 *, Xinguan Yang 1,2 *, Jingxu Li 1,2, Xiao Dong 1,2, Jianxing He 2,3, Yubao Guan 1,2. Original Article
 Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping
 Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis
 Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Lung Cancer in Chronic Interstitial Pneumonia: Early Manifestation From Serial CT Observations
 Cardiopulmonary Imaging Original Research Yoshida et al. CT of Lung Cancer Cardiopulmonary Imaging Original Research Rika Yoshida 1 Hiroaki rakawa Yasushi Kaji Yoshida R, rakawa H, Kaji Y Keywords: CT,
Cardiopulmonary Imaging Original Research Yoshida et al. CT of Lung Cancer Cardiopulmonary Imaging Original Research Rika Yoshida 1 Hiroaki rakawa Yasushi Kaji Yoshida R, rakawa H, Kaji Y Keywords: CT,
Interstitial Lung Abnormalities in a CT Lung Cancer Screening Population: Prevalence and Progression Rate 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Gong Yong Jin, MD,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Gong Yong Jin, MD,
Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer
 Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer Hiroaki Sugiura, MD, Atsuya Takeda, MD, PhD, Toshiko Hoshi, MD, PhD, Yoshinori Kawabata, MD, Koichi Sayama, MD, PhD, Masahiro
Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer Hiroaki Sugiura, MD, Atsuya Takeda, MD, PhD, Toshiko Hoshi, MD, PhD, Yoshinori Kawabata, MD, Koichi Sayama, MD, PhD, Masahiro
Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function
 Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function Yeon Joo Jeong, MD 1, 2 Kyung Soo Lee, MD 1 Nestor L. Muller, MD
Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function Yeon Joo Jeong, MD 1, 2 Kyung Soo Lee, MD 1 Nestor L. Muller, MD
Thin-Section CT Findings of Arc-Welders Pneumoconiosis
 Thin-Section CT Findings of Arc-Welders Pneumoconiosis Daehee Han, MD 1 Jin Mo Goo, MD 1 Jung-Gi Im, MD 1 Kyung Soo Lee, MD 2 Do Myung Paek, MD 3 Seong Ho Park, MD 1 Index words: Lungs, diseases Lungs,
Thin-Section CT Findings of Arc-Welders Pneumoconiosis Daehee Han, MD 1 Jin Mo Goo, MD 1 Jung-Gi Im, MD 1 Kyung Soo Lee, MD 2 Do Myung Paek, MD 3 Seong Ho Park, MD 1 Index words: Lungs, diseases Lungs,
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS
 USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
Interstitial lung diseases in a lung cancer screening trial
 Eur Respir J 2011; 38: 392 400 DOI: 10.1183/09031936.00201809 CopyrightßERS 2011 Interstitial lung diseases in a lung cancer screening trial N. Sverzellati*, L. Guerci*, G. Randi #, E. Calabrò ", C. La
Eur Respir J 2011; 38: 392 400 DOI: 10.1183/09031936.00201809 CopyrightßERS 2011 Interstitial lung diseases in a lung cancer screening trial N. Sverzellati*, L. Guerci*, G. Randi #, E. Calabrò ", C. La
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines
 Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Pediatric High-Resolution Chest CT
 Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
CT in Idiopathic Pulmonary Fibrosis: Diagnosis and Beyond
 Cardiopulmonary Imaging Review Gruden CT of Idiopathic Pulmonary Fibrosis Cardiopulmonary Imaging Review James F. Gruden 1 Gruden JF FOCUS ON: Keywords: CT, diagnosis, high-resolution CT, idiopathic pulmonary
Cardiopulmonary Imaging Review Gruden CT of Idiopathic Pulmonary Fibrosis Cardiopulmonary Imaging Review James F. Gruden 1 Gruden JF FOCUS ON: Keywords: CT, diagnosis, high-resolution CT, idiopathic pulmonary
Radiologists toolbox to differentiate alveolar versus interstitial lung diseases
 Radiologists toolbox to differentiate alveolar versus interstitial lung diseases Dr Sumer Shikhare, Dr Trishna Shimpi, Dr Ashish Chawla Khoo Teck Puat Hospital Singapore. Relevant financial disclosures
Radiologists toolbox to differentiate alveolar versus interstitial lung diseases Dr Sumer Shikhare, Dr Trishna Shimpi, Dr Ashish Chawla Khoo Teck Puat Hospital Singapore. Relevant financial disclosures
Computed Tomography-Based Centrilobular Emphysema Subtypes Relate with Pulmonary Function
 Send Orders of Reprints at reprints@benthamscience.net 54 The Open Respiratory Medicine Journal, 213, 7, 54-59 Computed Tomography-Based Centrilobular Emphysema s Relate with Pulmonary Function Mamoru
Send Orders of Reprints at reprints@benthamscience.net 54 The Open Respiratory Medicine Journal, 213, 7, 54-59 Computed Tomography-Based Centrilobular Emphysema s Relate with Pulmonary Function Mamoru
Survival in Patients With Cryptogenic Fibrosing Alveolitis*
 Survival in Patients With Cryptogenic Fibrosing Alveolitis* A Population-Based Cohort Study Richard Hubbard, DM; Ian johnston, MD; and john Britton, MD Study objectives: To determine the median survival
Survival in Patients With Cryptogenic Fibrosing Alveolitis* A Population-Based Cohort Study Richard Hubbard, DM; Ian johnston, MD; and john Britton, MD Study objectives: To determine the median survival
Hypersensitivity Pneumonitis: Spectrum of High-Resolution CT and Pathologic Findings
 CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
CT Findings in the Elderly Lung
 CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
Silicoproteinosis: High-Resolution CT Findings in 13 Patients
 CT of Silicoproteinosis Chest Imaging Clinical Observations Edson Marchiori 1 Carolina lthoff Souza 2 Tatiana Gontijo arbassa 1 Dante L. Escuissato 3 Emerson L. Gasparetto 1 rthur Soares Souza, Jr. 4 Marchiori
CT of Silicoproteinosis Chest Imaging Clinical Observations Edson Marchiori 1 Carolina lthoff Souza 2 Tatiana Gontijo arbassa 1 Dante L. Escuissato 3 Emerson L. Gasparetto 1 rthur Soares Souza, Jr. 4 Marchiori
Thin-Section CT Findings in 32 Immunocompromised Patients with Cytomegalovirus Pneumonia Who Do Not Have AIDS
 Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Dr.kassim.m.sultan F.R.C.P
 Dr.kassim.m.sultan F.R.C.P inflammatory disorder of the lung, involving alveolar walls and terminal airways, that is induced, in a susceptible host, by repeated inhalation of a variety of organic agents.
Dr.kassim.m.sultan F.R.C.P inflammatory disorder of the lung, involving alveolar walls and terminal airways, that is induced, in a susceptible host, by repeated inhalation of a variety of organic agents.
Silicosis in Turkish denim sandblasters
 Occupational Medicine 2006;56:554 558 Published online 4 October 2006 doi:10.1093/occmed/kql094 Silicosis in Turkish denim sandblasters Metin Akgun 1, Arzu Mirici 1, Elif Yilmazel Ucar 1, Mecit Kantarci
Occupational Medicine 2006;56:554 558 Published online 4 October 2006 doi:10.1093/occmed/kql094 Silicosis in Turkish denim sandblasters Metin Akgun 1, Arzu Mirici 1, Elif Yilmazel Ucar 1, Mecit Kantarci
punctiform type of coalworkers' In 1958 a stratified random sample of 300 miners and a private census in the Rhondda Fach in Glamorgan
 British Journal of Industrial Medicine, 1974, 31, 196-200 Mortality in pneumoconiosis punctiform type of coalworkers' W. E. WATERS1, A. L. COCHRANE, and F. MOORE Medical Research Council's Epidemiology
British Journal of Industrial Medicine, 1974, 31, 196-200 Mortality in pneumoconiosis punctiform type of coalworkers' W. E. WATERS1, A. L. COCHRANE, and F. MOORE Medical Research Council's Epidemiology
Cystic Lung Disease: a Comparison of Cystic Size, as Seen on Expiratory and Inspiratory HRCT Scans
 Cystic Lung Disease: a Comparison of Cystic Size, as Seen on Expiratory and Inspiratory HRCT Scans Ki-Nam Lee, MD 1 Seong-Kuk Yoon, MD 1 Seok Jin Choi, MD 2 Jin Mo Goo, MD 3 Kyung-Jin Nam, MD 1 Index words:
Cystic Lung Disease: a Comparison of Cystic Size, as Seen on Expiratory and Inspiratory HRCT Scans Ki-Nam Lee, MD 1 Seong-Kuk Yoon, MD 1 Seok Jin Choi, MD 2 Jin Mo Goo, MD 3 Kyung-Jin Nam, MD 1 Index words:
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 5: restrictive lung diseases, part 1: fibrosing lung diseases
 DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 5: restrictive lung diseases, part 1: fibrosing lung diseases Reference: Robbins, 9 th : 472-478, 10 th : 506-512 INTRODUCTION: RESTRICTIVE
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 5: restrictive lung diseases, part 1: fibrosing lung diseases Reference: Robbins, 9 th : 472-478, 10 th : 506-512 INTRODUCTION: RESTRICTIVE
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2
 Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Bronkhorst colloquium Interstitiële longziekten. Katrien Grünberg, klinisch patholoog
 Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
A case of a patient with IPF treated with nintedanib. Prof. Kreuter and Prof. Heussel
 A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances in Knowledge since 20021
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances
This copy is for personal use only. To order printed copies, contact reprints@rsna.org American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Comparison of CT Findings
 Newly Detected Pulmonary Nontuberculous Mycobacterial Infection and Peripheral Lung Cancers in Patients During Follow-Up of Idiopathic Interstitial Pneumonia Comparison of CT Findings Sang Young Oh, MD,
Newly Detected Pulmonary Nontuberculous Mycobacterial Infection and Peripheral Lung Cancers in Patients During Follow-Up of Idiopathic Interstitial Pneumonia Comparison of CT Findings Sang Young Oh, MD,
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
IPF - Inquadramento clinico
 IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
Chronic Interstitial (Restrictive) Lung Disease
 Chronic Interstitial (Restrictive) Lung Disease Fibrosing Usual interstitial pneumonia (idiopathic pulmonary fibrosis) IPF/UIP Nonspecific interstitial pneumonia(nsip) Cryptogenic organizing pneumonia(cop)
Chronic Interstitial (Restrictive) Lung Disease Fibrosing Usual interstitial pneumonia (idiopathic pulmonary fibrosis) IPF/UIP Nonspecific interstitial pneumonia(nsip) Cryptogenic organizing pneumonia(cop)
Case 1: Question. 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule
 HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
Idiopathic Pulmonary of Care
 Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
C aring for patients with interstitial lung disease is an
 980 INTERSTITIAL LUNG DISEASE Incidence and mortality of idiopathic pulmonary fibrosis and sarcoidosis in the UK J Gribbin, R B Hubbard, I Le Jeune, C J P Smith, J West, L J Tata... See end of article
980 INTERSTITIAL LUNG DISEASE Incidence and mortality of idiopathic pulmonary fibrosis and sarcoidosis in the UK J Gribbin, R B Hubbard, I Le Jeune, C J P Smith, J West, L J Tata... See end of article
Significance of irregular opacities in the radiology of coalworkers' pneumoconiosis
 British Journal of Industrial Medicine, 1974, 31, 36-44 Significance of irregular opacities in the radiology of coalworkers' pneumoconiosis J. P. LYONS, R. C. RYDER, H. CAMPBELL, W. G. CLARKE, and J. GOUGH
British Journal of Industrial Medicine, 1974, 31, 36-44 Significance of irregular opacities in the radiology of coalworkers' pneumoconiosis J. P. LYONS, R. C. RYDER, H. CAMPBELL, W. G. CLARKE, and J. GOUGH
Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
 ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
