Chest - Volume 139, Issue 4 (April 2011) - Copyright 2011 The American College of Chest Physicians
|
|
|
- Loren Hines
- 6 years ago
- Views:
Transcription
1 Use of this content is subject to the Terms and Conditions Cryptogenic and Secondary Organizing Pneumonia Chest - Volume 139, Issue 4 (April 2011) - Copyright 2011 The American College of Chest Physicians MDC Extra Article: This additional article is not currently cited in MEDLINE, but was found in MD Consult's full-text literature database. Original Research Diffuse Lung Disease Cryptogenic and Secondary Organizing Pneumonia Clinical Presentation, Radiographic Findings, Treatment Response, and Prognosis Fotios Drakopanagiotakis, MD a Koralia Paschalaki, MD a Muhanned Abu-Hijleh, MD, FCCP b,* Bassam Aswad, MD c Napoleon Karagianidis, MD a Emmanouil Kastanakis, MD a Sidney S. Braman, MD, FCCP b Vlasis Polychronopoulos, MD, FCCP a a From the Third Pulmonary Medicine Department, Sismanoglion General Hospital, Maroussi, Greece b Department of Medicine, Division of Pulmonary, Critical Care, and Sleep Medicine, Brown University, Providence, RI c Department of Pathology, Rhode Island Hospital The Alpert Medical School of Brown University, Providence, RI * Correspondence to: Muhanned Abu-Hijleh, MD, FCCP, Division of Pulmonary, Critical Care and Sleep Medicine, Rhode Island Hospital The Alpert Medical School of Brown University, 593 Eddy St, APC Bldg, 7th Floor, Providence, RI address: Muhanned_Abu-Hijleh@Brown.edu Manuscript received April 15, 2010, accepted July 21, 2010 Drs Drakopanagiotakis, Paschalaki, and Abu-Hijleh contributed equally to this study.reproduction of this article is prohibited without written permission from the American College of Chest Physicians ( ). PII S (11)60192-X Background Organizing pneumonia (OP) is a distinct clinical and pathologic entity. This condition can be cryptogenic (COP) or secondary to other known causes (secondary OP). In the present study, we reviewed the features associated with COP and secondary OP in patients from two teaching hospitals. Methods The medical records of 61 patients with biopsy-proven OP were retrospectively reviewed. Forty patients were diagnosed with COP and 21 patients with secondary OP. The clinical presentation, radiographic studies, pulmonary function tests (PFTs), laboratory data, BAL findings, treatment, and outcome were analyzed. Results The mean age at presentation was ± years. Malaise, cough, fever, dyspnea, bilateral alveolar infiltrates, and a
2 restrictive pattern were the most common symptoms and findings. BAL lymphocytosis was observed in 43.8% of patients with OP. The relapse rate and mortality rate after 1 year of follow-up were 37.8% and 9.4%, respectively. The in-hospital mortality was 5.7%. The clinical presentation and radiographic findings did not differ significantly between patients with COP and secondary OP. A mixed PFT pattern (obstructive and restrictive physiology) and lower blood levels of serum sodium, serum potassium, platelets, albumin, protein, and ph were observed among patients with secondary OP. Higher blood levels of creatinine, bilirubin, PaCO 2, and BAL lymphocytes were also more common among patients with secondary OP. There were no differences in the relapse rate or mortality between patients with COP and secondary OP. The 1-year mortality correlated with an elevated erythrocyte sedimentation rate, low albumin, and low hemoglobin levels. Conclusions The clinical and radiographic findings in patients with COP and secondary OP are similar and nonspecific. Although certain laboratory abnormalities are more common in secondary OP and can be associated with worse prognosis, they are likely due to the underlying disease. COP and secondary OP have similar treatment response, relapse rates, and mortality. Abbreviations ANA antinuclear antibodies COP cryptogenic organizing pneumonia DLCO diffusion capacity for carbon monoxide ESR erythrocyte sedimentation rate ɣgt ɣ-glutamyl transpeptidase Hb hemoglobin HRCT high-resolution CT OP organizing pneumonia PFT pulmonary function test RF rheumatoid factor TBB transbronchial biopsy Organizing pneumonia (OP) is a clinical entity associated with nonspecific symptoms, radiographic findings, and pulmonary
3 function test (PFT) abnormalities. The histopathologic pattern is characterized by patchy filling of the lung alveoli and respiratory bronchioles by loose plugs of granulation tissue (Masson bodies). [1] The predominant feature is that of an alveolar inflammatory and filling process rather than a small airway disease (bronchiolitis) (Fig 1). The presenting symptoms are usually nonspecific and include constitutional symptoms with flulike illness, cough, and dyspnea. The radiographic findings are also nonspecific and usually include a patchy bilateral alveolar filling process that can be recurrent and migratory in nature. Figure 1 A, Bronchoscopic transbronchial lung biopsy specimen in a patient with secondary organizing pneumonia (hemotoxylin and eosin stain, original magnification 100). B, Surgical thoracoscopic lung biopsy specimen in patient with secondary organizing pneumonia (hemotoxylin and eosin stain, original magnification 100). The biopsy specimens show evidence of proliferative bronchiolitis, with loose plugs of granulation tissue filling the alveoli (Masson bodies). The arrows point to the Masson bodies. OP can be primary (cryptogenic organizing pneumonia [COP]) or secondary (secondary OP). COP is classified as an idiopathic interstitial pneumonia, [2] whereas secondary OP is associated with a variety of diseases known to induce the OP clinical syndrome and the characteristic pathologic pattern. These entities include connective tissue diseases, infections, malignancies, drugs, radiation injury, organ transplantation, and aspiration, among others. COP is diagnosed in the appropriate clinical, radiographic, and pathologic setting after excluding diseases associated with secondary OP. [3] The significance of such distinction is important, as the management of secondary OP requires treatment of the underlying disease (eg, infection and connective tissue disease) or potential avoidance of the offending agent (eg, medication and radiation injury). Previous reports and clinical experience suggested that secondary OP could be associated with a worse prognosis and be less responsive to treatment when compared with COP. [4] The goal of this report is to review our experience with OP and highlight potential similarities and differences between COP and secondary OP. OP-specific diagnosis codes in two institutions (the Division of Pulmonary, Sleep and Critical Care Medicine, at Rhode Island Hospital, Providence, Rhode Island, and the Third Pulmonary Medicine Department of Sismanoglion General Hospital,
4 Maroussi, Greece) from January 2001 to June 2008 were reviewed. The study was approved by the institutional review boards of both institutions. If a patient was identified by lung biopsy results, the records were examined for information pertaining to OP. This included the clinical diagnosis prior to referral for biopsy, presence or absence of OP, extent of OP (OP as the predominant pattern or as a minor association with another predominant distinctive pattern), and the presence of other pathologic patterns. We reviewed patients' symptoms, duration of the disease, comorbidities, concomitant drug use, laboratory data, PFT, radiographic studies, and the response to treatment. Statistical Analysis SPSS, version 14 software (SPSS, Inc; Chicago, Illinois) was used for statistical analysis. Continuous data normal distribution is expressed as mean ± SD. We used Pearson χ 2 for nonparametric data, expressed as mean and interquartile range. Two-tailed Student t test (Mann-Whitney U test) was used for comparing continuous variables as appropriate. Clinical Presentation and Laboratory Data: All Patients We identified 61 patients with a biopsy-proven diagnosis of OP, 27 men and 34 women. The diagnosis was made by surgical lung biopsy in 20 patients (32.8%) and by bronchoscopic transbronchial biopsy (TBB) in 41 patients (67.2%). The mean age of patients was ± years. Forty patients were diagnosed with COP and 21 patients with secondary OP. Causes of secondary OP in the patients are listed in Table 1. The mean duration of symptoms before diagnosis was 96 ± 93 days. Nineteen patients were active smokers and 14 patients were previous smokers (Table 2). Table 1 -- Diseases Associated With Secondary OP Associated Diseases No. (%) Drugs and substance abuse 6 (28.5) Amiodarone β-blockers Cocaine abuse Systemic inflammatory diseases 4 (19.8) Rheumatoid arthritis Polymyositis/dermatomyositis Polymyalgia rheumatica Solid tumors 5 (23.8) Colon Breast Hematologic malignancies 3 (14.2) Non-Hodgkin's lymphoma Renal transplantation 1 (4.7) Infections 2 (9.5) OP = organizing pneumonia. Table 2 -- Clinical Characteristics of Patients With COP and Secondary OP Variable OP COP Secondary OP Age ± SD ± ± ± Male (female) 27 (34) 19 (21) 8 (13) Smoking Active smokers 19 (32.8) 14 (35.9) 5 (26.3)
5 Variable OP COP Secondary OP Previous smokers 14 (24.1) 9 (23.1) 5 (26.3) Nonsmokers 25 (43.1) 16 (41.0) 9 (47.4) Cough 40 (67.8) 25 (65.8) 15 (71.4) Sputum 24 (40.0) 15 (38.5) 9 (42.9) Hemoptysis 4 (6.7) 1 (2.6) 3 (14.3) Dyspnea 38 (63.3) 22 (56.4) 16 (76.2) Fever 39 (65.0) 28 (71.8) 11 (52.4) Chest pain 18 (30.0) 10 (25.0) 8 (40.0) Malaise 44 (74.6) 28 (71.8) 16 (80.0) Arthralgias 15 (26.3) 12 (32.4) 3 (15.0) Weight loss 17 (27.9) 9 (23.0) 8 (38.0) Cyanosis 14 (43.7) 6 (15.8) 8 (38.1) Crackles 44 (75.9) 30 (78.9) 14 (70.0) Wheezing 8 (13.8) 4 (10.5) 4 (20.0) Values are presented as No. (%). P value was not significant for any variable. COP = crytogenic organizing pneumonia. See Table 1 legend for expansion of other abbreviation. The most common symptoms were cough (67.8%), fever (65.0%), and dyspnea (63.3%). Cough was usually nonproductive (60%). Malaise was reported by the majority of patients (74.6%), whereas arthralgias (26.3%) and weight loss > 3 kg (27.9% of patients) were less common. Thirty percent of patients presented with chest pain. Physical findings included cyanosis in 43.7%, crackles in 75.9%, and wheezing in 13.8% of patients (Table 2). The chest radiograph findings included consolidation in 50 patients (82%) that was bilateral in 68.6% and unilateral in 31.4% of patients. Migratory alveolar infiltrates were observed in seven patients (11.5%). A diffuse reticulonodular pattern was present in seven patients (11.5%) and masslike lesions in five patients (8.2%). Cavitation was present in only one case. Pleural effusion was identified in seven patients (11.5%) (Table 3). High-resolution CT (HRCT) scan findings included alveolar opacities, which proved to be bilateral in 73.5% of patients, diffuse reticulonodular pattern in 9.8%, and masslike lesions in 8.2% of patients. A mixed pattern was present in 15 patients (24.6%). Reverse halo sign was not identified in the patients. Table 3 -- Radiographic Findings in Patients With COP and Secondary OP Variable OP COP Secondary OP Chest radiograph Consolidation 50 (82.0) 33 (82.5) 17 (81.0) Bilateral 35 (68.6) 24 (72.7) 11 (61.1) Diffuse reticular 7 (11.5) 4 (10.0) 3 (14.3) Masslike lesion 5 (8.2) 4 (10.0) 1 (4.8) Pleural effusion 7 (11.5) 3 (7.5) 4 (19.0) Cavitation 1 (1.6) 1 (2.5) 0 (0) Migratory lesions 7 (11.5) 7 (17.5) 0 (0) CT scan Consolidation 49 (80.3) 31 (77.5) 18 (85.7) Bilateral 36 (73.5) 25 (80.6) 11 (61.1) Diffuse reticular 6 (9.8) 4 (10) 2 (9.5)
6 Variable OP COP Secondary OP Masslike lesion 5 (8.2) 4 (10) 1 (4.8) Pleural effusion 7 (11.5) 3 (7.5) 4 (19.0) Cavitation 1 (1.6) 1 (2.5) 0 (0) Migratory lesions 7 (11.5) 7 (17.5) 0 (0) Values are presented as No. (%). P value was not significant for any variable. See [Table 1], [Table 2] legends for expansion of abbreviations. Leukocytosis was present in 25 patients (40.9%) and leukopenia in one patient (1.6%). Peripheral eosinophilia was not identified in the patients. Six patients had anemia (hemoglobin [Hb] < 11 g/dl) and 21 patients had an erythrocyte sedimentation rate (ESR) > 60 mm/h. Antinuclear antibodies (ANA) were positive in 23.8% and rheumatoid factor (RF) in 8% of the patients (Table 4). BAL analysis was available for 32 patients with a mean neutrophil, eosinophil, and lymphocyte BAL% of 26.1%, 10.2%, and 18.8%, respectively. BAL lymphocytosis (> 20%) was present in 43.8% of patients (Table 5). Table 4 -- Laboratory Data in Patients With COP and Secondary OP Variable (No. COP/Secondary OP) OP ± SD COP ± SD Secondary OP ± SD P Value WBC (37/21), 10 3 /µl ± ± ± NS Neut (36/20), % ± ± ± NS Hb (37/21), g/dl ± ± ± 1.73 NS PLT (37/21), 10 3 /µl ± ± ± ESR (32/12), mm/h ± ± ± NS Na (36/19), meq/l ± ± ± K (36/19), meq/l 4.34 ± ± ± Ca (28/14), mg/dl 8.96 ± ± ± 0.98 NS BUN (37/21), mg/dl ± ± ± NS Creat (37/21), mg/dl 0.98 ± ± ± Gluc (37/21), mg/dl ± ± ± 41.9 NS Bili (31/15), mg/dl 0.73 ± ± ± SGOT (32/15), IU/L 32.4 ± ± ± 44.9 NS SGPT (32/15), IU/L 38.4 ± ± ± 66.9 NS LDH (29/9), IU/L 355 ± ± ± NS ALP (32/15), IU/L ± ± ± 97 NS ɣgt (27/5), IU/L 48.3 ± ± ± Protein (29/13), g/dl 6.87 ± ± ± Albumin (29/13), g/dl 3.51 ± ± ± ANA positivity [a] 10/42 (23.8%) 6/33 (18.2%) 4/9 (44.4%) NS RF positivity [a] 3/36 (8%) 3/29 (10.3%) 0/7 (0%) NS Values are presented as mean ± SD. ALP = serum alkaline phosphatase; ANA = antinuclear antibody; Bili = total serum bilirubin; Ca = serum calcium; Creat = serum creatinine; ESR = eryhtrocyte sedimentation rate; ɣgt = ɣ-glutamyl transpeptidase; Gluc = glucose; Hb = hemoglobin; K = serum potassium; LDH = lactate dehydrogenase; Na = serum sodium; Neut = neutrophils; NS = not significant; PLT = platelet count; RF = rheumatoid factor; SGOT = serum glutamic oxaloacetic transaminase; SGPT = serum glutamic pyruvic transaminase. See [Table 1], [Table 2] legends for expansion of other abbreviations. a ANA and RF were not associated with clinical connective tissue disease. Values are presented as absolute number of patients with positive ANA or
7 RF/total number of available patients with OP, COP, and secondary OP (%). Table 5 -- BAL Findings in COP and Secondary OP Variable (No. COP/Secondary OP) OP ± SD COP ± SD Secondary OP ± SD P Value Macrophages (27/5) ± ± ± NS Lymphocytes (27/5) ± ± ± Neutrophils (27/5) ± ± ± NS Eosinophils (27/5) ± ± ± 5.50 NS Mast cells (27/5) 2.28 ± ± ± 1.73 NS Lymphocytes > 20% 14 (43.8) 10 (37) 4 (80) NS Values are presented as mean ± SD or No. (%). See Table 1, 2, and 4 legends for expansion of abbreviations. PFT data were available for 36 patients. A reduced FVC was observed in 43% of patients, and a reduced diffusion capacity for carbon monoxide (DLCO) was observed in 42% of patients. Airflow obstructive pattern, restrictive pattern, and mixed patterns were observed in 25%, 41.7%, and 5.6% of patients, respectively. A total of 27.8% of the patients had normal PFT (Tables 6, 7). Table 6 -- PFTs and Arterial Blood Gases of Patients With COP and Secondary OP Variable (No. COP/Secondary OP) OP ± SD COP ± SD Secondary OP ± SD P Value PaO 2 (28/11) ± ± ± NS PaCO 2 (28/11) ± ± ± ph (28/11) 7.44 ± ± ± HCO 3 (23/13) ± ± ± 3.53 NS FEV 1 % (28/8) ± ± ± NS FVC % (28/7) ± ± ± NS DLCO % (16/3) ± ± ± NS SpO 2 (38/19) ± ± ± 6.77 NS Values are presented as mean ± SD. DLCO = diffusion capacity for carbon monoxide; HCO 3 = serum bicarbonate ion; PFT = pulmonary function test; SpO 2 = oxygen saturation. See Table 1, 2, and 4 legends for expansion of other abbreviations. Table 7 -- Specific Patterns of PFTs in Patients With COP and Secondary OP Variable OP COP Secondary OP P Value PFT pattern Restrictive 15 (41.7) 12 (42.9) 3 (37.5) NS Obstructive 9 (25) 9 (32.1) 0 (0) NS Normal 10 (27.8) 7 (25) 3 (37.5) NS Mixed 2 (5.6) 0 (0) 2 (25).044 DLCO < 60% 8 (42.1) 7 (43.8) 1 (33.1) NS PaO 2 < 80 mm Hg 28 (71.8) 21 (75) 7 (63.6) NS Values are presented as No. (%). See Table 1, 2, 4, and 6 legends for expansion of abbreviations.
8 Clinical Presentation and Laboratory Data: COP vs Secondary OP The age, sex, and smoking distribution among patients with COP or secondary OP were not significantly different. The duration of symptoms was slightly longer in secondary OP, although not statistically significant (P =.724). Diagnosis by bronchoscopic TBB (67.2%) was equally distributed among patients. The symptoms and physical findings in patients with OP were nonspecific, and did not differentiate COP from secondary OP. Cyanosis was more common among patients with secondary OP (38.1% vs 15.8%) but did not reach statistical significance (Table 2). Laboratory data demonstrated lower serum sodium levels (P =.022), potassium levels (P =.016), and platelet counts (P =.001), with higher blood creatinine (P =.014) and bilirubin (P =.001) levels in patients with secondary OP. The total protein (P =.027) and albumin levels (P =.042) were also lower in patients with secondary OP. Severe anemia (Hb < 7 g/dl), leukocytosis (WBC > /µl), ESR elevation (> 60 mm/h), and ANA or RF positivity (not associated with clinical connective tissue disease) were equally present among patients with COP and secondary OP (Table 4). BAL mean lymphocyte count was significantly higher in patients with secondary OP (P =.002). The majority of cases with COP (54%) did not have lymphocytosis (> 20%) in the BAL (Table 5). There was no difference in lung volumes, DLCO, or PaO2 among the two groups, but a mixed PFT pattern was more common in patients with secondary OP (P =.044). Patients with COP had a significantly higher ph (P =.007) and lower PaCO2 (P =.023) (Tables 6, 7). Treatment and Prognosis Specific treatment and prognosis data were available for 53 patients with OP. The majority of the patients were treated with systemic steroids, three patients were treated with macrolide antibiotics, nine patients were not treated because of the lack of specific symptoms or physical limitations, and three patients underwent surgery for removal of a solitary pulmonary nodule that was proven to be unexpected OP on the biopsy specimens. Patients with COP were treated similar to those with secondary OP (Table 8). Table 8 -- Treatment and Prognosis in Patients With COP and Secondary OP Treatment OP COP Secondary OP Corticosteroids 41 (77.4) 30 (81.1) 11 (68.8) Macrolides 3 (5.7) 2 (5.4) 1 (6.3) No treatment 9 (17) 5 (13.5) 4 (25.0) Relapse 17 (37.8) 13 (38.2) 4 (36.4) 1-y mortality 5 (9.4) 2 (5.3) 3 (20) In-hospital mortality 3 (5.7) 1 (2.6) 2 (13.3) Values are presented as No. (%). P value was not significant for any variable. See [Table 1], [Table 2] legends for expansion of abbreviations. Mortality data were available for 53 of the hospitalized patients at the time of discharge, and 45 patients were followed 1 year after the initial diagnosis. In-hospital mortality and 1-year mortality in patients with OP were 5.7% and 9.4%, respectively. There was no difference between COP and secondary OP regarding in-hospital mortality (P =.190) or mortality at 1 year after discharge (P =.131) (Table 8). Death 1 year after hospitalization correlated with low Hb (Hb < 11 g/dl, P =.002), an ESR > 60 mm/h (P =.048), and serum albumin < 3.5 g/dl (P =.017) at the time of diagnosis. Mortality did not correlate with BAL lymphocytosis, a reticulonodular pattern on HRCT scan, or hypoxemia (PaO2 < 80 mm Hg) (Table 9). The relapse rate within 1 year was 37.8%. We found no difference in the number of patients with COP or secondary OP who relapsed within 1 year after diagnosis (P =.602) or in the number of patients who relapsed while on active treatment (P =.682). Furthermore, the relapse rate did not correlate with low PaO2, low albumin level, BAL lymphocytosis (> 20%), or the presence of a reticulonodular pattern on HRCT imaging (Table 10). Table 9 -- One-Year All-Cause Mortality Variable Deceased Alive P Value Hb < 11 g/dl 4 (80) 1 (20).02 WBC > /µl 3 (60) 2 (40) NS
9 Variable Deceased Alive P Value ESR > 60 mm/h 4 (100) 0 (0).048 Albumin < 3.5 g/dl 4 (100) 0 (0).017 PaO 2 < 80 mm Hg 3 (75) 1 (25) NS BAL lymphocytes > 20% 1 (100) 0 (0) NS HRCT scan reticular 0 (0) 5 (100) NS Values are presented as No. (%). HRCT = high-resolution CT. See Table 4 for expansion of other abbreviations. Table Relapse Rate in Patients With OP Variable Relapse No Relapse Hb < 11 g/dl 2 (33.3) 4 (66.7) WBC > /µl 7 (46.7) 8 (53.3) ESR > 60 9 (50) 9 (50) Albumin < 3.5 g/dl 5 (45.5) 6 (54.5) PaO 2 < 80 mm Hg 10 (41.7) 14 (58.3) BAL lymphocytes > 20% 6 (42.9) 8 (57.1) HRCT scan reticular 0 (0) 4 (100) Values are presented as No. (%). P value was not significant for any variable. See Tables 1, 4, and 9 legends for expansion of abbreviations. The term organizing pneumonia has replaced the previously used term bronchiolitis obliterans with organizing pneumonia. The nonspecific clinical, radiographic and pathologic pattern of OP may be associated with a variety of other conditions, such as malignancy, interstitial lung disease, and Wegener granulomatosis. [1] This suggests that OP may represent a nonspecific repair process in response to local or distant injury. OP can also present as a distinct clinical and pathologic entity, unrelated to any other condition. When a patient presents with the clinical syndrome of OP and a condition known to be associated with the pathologic pattern of OP, the term secondary OP is applied. [2] COP is the term used in the absence of such known associated conditions. The classification of OP into COP and secondary OP is clinically important, as the management of patients with secondary OP includes not only the treatment of OP but also the management of underlying disease and avoidance of any known offending agents. To date, it remains unclear if COP and secondary OP represent two distinctive clinical entities or if they are a common entity of nonspecific lung injury and repair. Previous studies have reported conflicting results. To address this question, we reviewed our experience with OP. We did not identify significant differences between the clinical characteristics of patients with COP and secondary OP. Patients with COP and secondary OP present during the fifth or sixth decade of life, [5], [6] without sex differences. The association of OP with current or previous smoking has been a controversial issue. [7], [8] In our study, 56% of the patients with OP had a smoking history and there was no difference between the COP and secondary OP groups. OP typically presents as a flulike illness followed by a nonresolving pneumonia despite adequate treatment. [9] The mean duration of symptoms prior to diagnosis in our series was approximately 3 months, compared with the 2 months reported by King and Mortenson. [7] The delay in the diagnosis of OP is likely because of its rarity and because it is underrecognized by physicians. [10] The nonspecific symptoms of malaise, cough, fever, and dyspnea occurred in more than two-thirds of the patients. Hemoptysis as previously described [7], [11] was uncommon, and chest pain, reported to be rare, [12], [13] was present in 30% of the patients. This is similar to a report by Lohr et al. [14] We and others have found that peripheral bilateral consolidation is the most common radiographic finding. [15], [16] Migratory pulmonary infiltrates, considered by some a classic radiographic presentation, were only present in 11.5% of the patients. This is significantly lower than previous reports. [5], [17] Our study confirmed that pleural effusions (11.5%) are not common in OP, [7], [18] and contrary to the findings by Vasu et al, [5] the prevalence was similar among patients with COP and
10 secondary OP. Other roentgenographic findings in our study included: a diffuse reticular pattern (11.5%), a mixed pattern of alveolar opacities and interstitial infiltrates (24.6%), and masslike lesions (8.2%). We did not identify any patient with the reversed halo sign (central ground glass opacities surrounded by crescentic or ring-shaped consolidation). [19] Analysis of the laboratory data showed subtle but statistically significant findings. Mild leukocytosis (10.44 ± 4.31) and elevated ESR (61.61 ± 39.56) were common findings in the patients. ANA and RF positivity, previously reported in OP, [20], [21] were found in some of the patients, similar to the report by Basarakodu et al. [10] The significance of the lower levels of serum sodium, serum potassium, platelet count, total serum protein, and serum albumin, and higher levels of creatinine, bilirubin, and ɣ-glutamyl transferase (ɣgt) in the patients with secondary OP is not completely clear. This may be a reflection of the severity of secondary OP and/or the associated underlying disease. A low serum albumin level has been reported in patients with secondary OP [22] and may be a risk factor for relapse. A low serum albumin level was one of the predictors of 1-year mortality (but not relapse) in our series. A higher ɣgt level, another risk factor for relapse, [8] was also observed in the patients with secondary OP. Patients with OP usually present with a restrictive pattern on PFT. [7], [15] Our results confirm this finding (40% of the patients). An obstructive pattern and normal PFT were also common findings in the patients (Tables 6, 7). There was no difference in the smoking history of the patients with COP and secondary OP, whereas the finding of a mixed obstructiverestrictive PFT pattern was more common in patients with secondary OP. The significance of the lower PaCO2 and higher ph levels in patients with COP is unclear but could reflect a somewhat higher degree of ventilatory drive. BAL is an important tool in the evaluation of patients with OP. [23] It typically shows expansion of all cell lines (lymphocytes, neutrophils, eosinophils, and mast cells). Foamy macrophages, plasma cells, and a CD4/CD8 ratio of < 0.9 are other potential supportive findings. [23], [24] Paucity of lymphocytes has been suggested as a risk factor for relapse. A significant portion of the patients with secondary OP had BAL lymphocytosis. We did not find a significant correlation between BAL lymphocyte levels and relapse rates. Two-thirds of the patients had a pathologic diagnosis of OP by bronchoscopic TBB. Surgical lung biopsy (by thoracoscopic approach or open thoracotomy) remains the gold standard for optimal pathologic diagnosis of OP, as it is more able to rule out other predominant pathologic features or specific diseases with adjacent OP features. However, in the proper clinical and radiographic setting, TBB and BAL can confirm the clinical diagnosis of OP. [4], [23], [24] Our current practice and experience is to reserve surgical biopsies for patients with high clinical suspicion for a finding other than OP, unusual clinical or radiographic features (eg, nodules), or rapidly progressive disease, and when there is a lack of response to treatment. The majority of the patients were treated with systemic corticosteroids. Only three patients received macrolide antibiotics for their antiinflammatory properties. The relapse rate in our series (37.8% after 1 year of follow-up) was similar to other reports. Contrary to previous studies, we did not find correlation of the relapse rate with low albumin, low or high percentage of BAL lymphocytes, specific pattern on CT scan (reticulonodular pattern), or low PaO2. [12], [22] In-hospital mortality (5.7%) was similar to other studies. [5], [10], [11] The 1-year all-cause mortality (9.4%) was similar among patients with COP and secondary OP, and showed a correlation with anemia (Hb < 11 g/dl), ESR (> 60 mm/h), and a lower albumin level (< 3.5 g/dl) at the time of diagnosis. This correlation was not previously reported and is probably a reflection of the severity of the OP and underlying disease. In conclusion, this report highlights many similarities and minor differences between COP and secondary OP. The clinical features of OP are nonspecific and do not differ between COP and secondary OP. Laboratory abnormalities, such as severe anemia, high ESR, and low serum albumin, are more common in patients with secondary OP and can be associated with worse prognosis. The relapse rates and 1-year all-cause mortality are similar for both groups. Our findings suggest that the pathologic and clinical features of both COP and secondary OP are caused by common lung injury and repair mechanisms. The cryptogenic nature of COP could be related to our limited knowledge about all the entities that can lead to secondary OP. This report adds to our knowledge about OP, recognizing the limitations of this retrospective review of patients with OP in two different institutions. Acknowledgments Author contributions: Dr Abu-Hijleh had access to and takes responsibility for the integrity of the data and the accuracy of the data analysis. Dr Drakopanagiotakis: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Paschalaki: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Abu-Hijleh: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript.
11 Dr Aswad: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Karagianidis: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Kastanakis: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Braman: contributed to data collection, organization, analysis, preparation, review, and submission of this manuscript. Dr Polychronopoulos: contributed to envisioning the initial concept and design of this project, data collection, organization, analysis, preparation, review, and submission of this manuscript. Financial/nonfinancial disclosures: The authors have reported to CHEST that no potential conflicts of interest exist with any companies/organizations whose products or services may be discussed in this article. Other contributions: This was a collaborative project between the Division of Pulmonary, Sleep, and Critical Care Medicine, at Rhode Island Hospital, Providence The Alpert Medical School of Brown University, Providence, RI and the Third Pulmonary Medicine Department of Sismanoglion General Hospital, Maroussi, Greece. REFERENCES: 1 Epler GR: Bronchiolitis obliterans organizing pneumonia. Arch Intern Med 161. (2): ; Abstract 2 American Thoracic Society, European Respiratory Society : American Thoracic Society/European Respiratory Society International Multidisciplinary Consensus Classification of the Idiopathic Interstitial Pneumonias. This joint statement of the American Thoracic Society (ATS), and the European Respiratory Society (ERS) was adopted by the ATS board of directors, June 2001 and by the ERS Executive Committee, June Am J Respir Crit Care Med 165. (2): ; Citation 3 Drakopanagiotakis F, Polychronopoulos V, Judson MA: Organizing pneumonia. Am J Med Sci 335. (1): ; Abstract 4 Cordier JF: Cryptogenic organising pneumonia. Eur Respir J 28. (2): ; Abstract 5 Vasu TS, Cavallazzi R, Hirani A, Sharma D, Weibel SB, Kane GC: Clinical and radiologic distinctions between secondary bronchiolitis obliterans organizing pneumonia and cryptogenic organizing pneumonia. Respir Care 54. (8): ; Abstract 6 Epler GR: Bronchiolitis obliterans organizing pneumonia: definition and clinical features. Chest 102. (1 suppl): 2S-6S.1992; Abstract 7 King, Jr, JrTE, Mortenson RL: Cryptogenic organizing pneumonitis. The North American experience. Chest 102. (1 suppl): 8S-13S.1992; Abstract 8 Lazor R, Vandevenne A, Pelletier A, Leclerc P, Court-Fortune I, Cordier JF: Cryptogenic organizing pneumonia. Characteristics of relapses in a series of 48 patients. The Groupe d'etudes et de Recherche sur les Maladles Orphelines Pulmonaires (GERM O P). Am J Respir Crit Care Med 162. (2 pt 1): ; Abstract 9 Epler GR: Bronchiolitis obliterans organizing pneumonia. Semin Respir Infect 10. (2): ; Abstract 10 Basarakodu KR, Aronow WS, Nair CK, et al: Differences in treatment and in outcomes between idiopathic and secondary forms of organizing pneumonia. Am J Ther 14. (5): ; Abstract 11 Sveinsson OA, Isaksson HJ, Sigvaldason A, Yngvason F, Aspelund T, Gudmundsson G: Clinical features in secondary and cryptogenic organising pneumonia. Int J Tuberc Lung Dis 11. (6): ; Abstract 12 Cordier JF, Loire R, Brune J: Idiopathic bronchiolitis obliterans organizing pneumonia. Definition of characteristic clinical profiles in a series of 16 patients. Chest 96. (5): ; Abstract 13 Cazzato S, Zompatori M, Baruzzi G, et al: Bronchiolitis obliterans-organizing pneumonia: an Italian experience. Respir Med 94. (7): ; Full Text 14 Lohr RH, Boland BJ, Douglas WW, et al: Organizing pneumonia. Features and prognosis of cryptogenic, secondary, and focal variants. Arch Intern Med 157. (12): ; Abstract 15 Epler GR, Colby TV, McLoud TC, Carrington CB, Gaensler EA: Bronchiolitis obliterans organizing pneumonia. N Engl J Med 312. (3): ; Abstract 16 Alasaly K, Muller N, Ostrow DN, Champion P, FitzGerald JM: Cryptogenic organizing pneumonia. A report of 25 cases and a review of the literature. Medicine (Baltimore) 74. (4): ; Abstract 17 Oymak FS, Demirbaş HM, Mavili E, et al: Bronchiolitis obliterans organizing pneumonia. Clinical and roentgenological features in 26 cases. Respiration 72. (3): ; Abstract 18 Oikonomou A, Hansell DM: Organizing pneumonia: the many morphological faces. Eur Radiol 12. (6): ; Abstract 19 Kim SJ, Lee KS, Ryu YH, et al: Reversed halo sign on high-resolution CT of cryptogenic organizing pneumonia: diagnostic implications. AJR Am J Roentgenol 180. (5): ; Abstract
12 20 Chang J, Han J, Kim DW, et al: Bronchiolitis obliterans organizing pneumonia: clinicopathologic review of a series of 45 Korean patients including rapidly progressive form. J Korean Med Sci 17. (2): ; Abstract 21 Yamamoto M, Ina Y, Kitaichi M, Harasawa M, Tamura M: Clinical features of BOOP in Japan. Chest 102. (1 Suppl): 21S-25S.1992; Citation 22 Watanabe K, Senju S, Wen FQ, Shirakusa T, Maeda F, Yoshida M: Factors related to the relapse of bronchiolitis obliterans organizing pneumonia. Chest 114. (6): ; Full Text 23 Poletti V, Cazzato S, Minicuci N, Zompatori M, Burzi M, Schiattone ML: The diagnostic value of bronchoalveolar lavage and transbronchial lung biopsy in cryptogenic organizing pneumonia. Eur Respir J 9. (12): ; Abstract 24 Costabel U, Teschler H, Guzman J: Bronchiolitis obliterans organizing pneumonia (BOOP): the cytological and immunocytological profile of bronchoalveolar lavage. Eur Respir J 5. (7): ; Abstract
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Focal Organizing Pneumonia on Surgical Lung Biopsy* Causes, Clinicoradiologic Features, and Outcomes
 CHEST Focal Organizing Pneumonia on Surgical Lung Biopsy* Causes, Clinicoradiologic Features, and Outcomes Fabien Maldonado, MD; Craig E. Daniels, MD; Elizabeth A. Hoffman, MD; Eunhee S. Yi, MD; and Jay
CHEST Focal Organizing Pneumonia on Surgical Lung Biopsy* Causes, Clinicoradiologic Features, and Outcomes Fabien Maldonado, MD; Craig E. Daniels, MD; Elizabeth A. Hoffman, MD; Eunhee S. Yi, MD; and Jay
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Diffuse interstitial lung diseases (DILDs) are a heterogeneous group of non-neoplastic, noninfectious
 Focused Issue of This Month Diagnostic Approaches to Diffuse Interstitial Lung Diseases Dong Soon Kim, MD Department of Pulmonary and Critical Care Medicine, University of Ulsan College of Medicine E -
Focused Issue of This Month Diagnostic Approaches to Diffuse Interstitial Lung Diseases Dong Soon Kim, MD Department of Pulmonary and Critical Care Medicine, University of Ulsan College of Medicine E -
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation
 Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
CASE REPORT PHOTOGRAPHIC NEGATIVE OF PULMONARY EDEMA. DIFFERENTIATING CHRONIC EOSINOPHILIC PNEUMONIA FROM CHRONIC HYPERSENSITIVITY PNEUMONITIS.
 CASE REPORT PHOTOGRAPHIC NEGATIVE OF PULMONARY EDEMA. DIFFERENTIATING CHRONIC EOSINOPHILIC PNEUMONIA FROM CHRONIC HYPERSENSITIVITY PNEUMONITIS. Talha Mahmud, Muhammad Omer Naeem, Muhammad Siddique ABSTRACT:
CASE REPORT PHOTOGRAPHIC NEGATIVE OF PULMONARY EDEMA. DIFFERENTIATING CHRONIC EOSINOPHILIC PNEUMONIA FROM CHRONIC HYPERSENSITIVITY PNEUMONITIS. Talha Mahmud, Muhammad Omer Naeem, Muhammad Siddique ABSTRACT:
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION!
 UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Imaging Small Airways Diseases: Not Just Air trapping. Eric J. Stern MD University of Washington
 Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
Clinical features of organizing pneumonia associated with rheumatoid arthritis
 Original Article Clinical features of organizing pneumonia associated with rheumatoid arthritis Harutsugu Okada 1, Kazuhiro Kurasawa 1,2, Ryutaro Yamazaki 1, Ayae Tanaka 1, Satoko Arai 1, Takayoshi Owada
Original Article Clinical features of organizing pneumonia associated with rheumatoid arthritis Harutsugu Okada 1, Kazuhiro Kurasawa 1,2, Ryutaro Yamazaki 1, Ayae Tanaka 1, Satoko Arai 1, Takayoshi Owada
Clinical and Radiologic Distinctions Between Secondary Bronchiolitis Obliterans Organizing Pneumonia and Cryptogenic Organizing Pneumonia
 Original Research Clinical and Radiologic Distinctions Between Bronchiolitis Obliterans Organizing neumonia and Cryptogenic Organizing neumonia Tajender S Vasu MD, Rodrigo Cavallazzi MD, Amyn Hirani MD,
Original Research Clinical and Radiologic Distinctions Between Bronchiolitis Obliterans Organizing neumonia and Cryptogenic Organizing neumonia Tajender S Vasu MD, Rodrigo Cavallazzi MD, Amyn Hirani MD,
Title. CitationJapanese Journal of Ophthalmology, 50(6): Issue Date Doc URL. Rights. Type. File Information
 Title Chronic panuveitis and scleritis in a patient with c Author(s)Saito, Wataru; Saito, Akari; Namba, Kenichi; Kase, S CitationJapanese Journal of Ophthalmology, 50(6): 558-561 Issue Date 2006 Doc URL
Title Chronic panuveitis and scleritis in a patient with c Author(s)Saito, Wataru; Saito, Akari; Namba, Kenichi; Kase, S CitationJapanese Journal of Ophthalmology, 50(6): 558-561 Issue Date 2006 Doc URL
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Acute organizing interstitial pneumonia and interstitial nephritis due to salazosulfapyridine in a patient with rheumatoid arthritis
 Allergology International (2003) 52: 37 41 Case Report Acute organizing interstitial pneumonia and interstitial nephritis due to salazosulfapyridine in a patient with rheumatoid arthritis Haruhiko Ogawa,
Allergology International (2003) 52: 37 41 Case Report Acute organizing interstitial pneumonia and interstitial nephritis due to salazosulfapyridine in a patient with rheumatoid arthritis Haruhiko Ogawa,
Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients
 Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
A Cryptogenic Case of Fulminant Fibrosing Organizing Pneumonia
 CASE REPORT A Cryptogenic Case of Fulminant Fibrosing Organizing Pneumonia Takehiko Kobayashi 1, Masanori Kitaichi 2-4, Kazunobu Tachibana 1,2, Yutaro Kishimoto 1,5, Yasushi Inoue 1, Tomoko Kagawa 1,2,
CASE REPORT A Cryptogenic Case of Fulminant Fibrosing Organizing Pneumonia Takehiko Kobayashi 1, Masanori Kitaichi 2-4, Kazunobu Tachibana 1,2, Yutaro Kishimoto 1,5, Yasushi Inoue 1, Tomoko Kagawa 1,2,
A 24-Year-Old Woman With Bilateral Pulmonary Infiltrates, Pericardial Effusion, and Bilateral Pleural Effusions*
 A 24-Year-Old Woman With Bilateral Pulmonary Infiltrates, Pericardial Effusion, and Bilateral Pleural Effusions* Chandra K. Katikireddy, MD; Ganesh Krishna, MD; Gerald Berry, MD; John Faul, MD; and Ware
A 24-Year-Old Woman With Bilateral Pulmonary Infiltrates, Pericardial Effusion, and Bilateral Pleural Effusions* Chandra K. Katikireddy, MD; Ganesh Krishna, MD; Gerald Berry, MD; John Faul, MD; and Ware
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas
 Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Received February 23, Received revised March 15, Accepted for publication March 16, University of California, Davis, CA, USA
 643990HICXXX10.1177/2324709616643990Journal of Investigative Medicine High Impact Case ReportsNguyen et al case-report2016 Case Report Acute Fibrinous and Organizing Pneumonia Associated With Allogenic
643990HICXXX10.1177/2324709616643990Journal of Investigative Medicine High Impact Case ReportsNguyen et al case-report2016 Case Report Acute Fibrinous and Organizing Pneumonia Associated With Allogenic
Radiation Pneumonitis Joseph Junewick, MD FACR
 Radiation Pneumonitis Joseph Junewick, MD FACR 03/19/2010 History 16 year old with history of relapsed stage IV-A Hodgkin disease. Prior pulmonary involvement was irradiated. Diagnosis Radiation Pneumonitis
Radiation Pneumonitis Joseph Junewick, MD FACR 03/19/2010 History 16 year old with history of relapsed stage IV-A Hodgkin disease. Prior pulmonary involvement was irradiated. Diagnosis Radiation Pneumonitis
Eosinophils and effusion: a clinical conundrum
 Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Professor Rob Miller
 BHIVA AUTUMN CONFERENCE 2013 Including CHIVA Parallel Sessions Professor Rob Miller University College London Medical School COMPETING INTEREST OF FINANCIAL VALUE > 1,000: Speaker Name Prof Rob Miller
BHIVA AUTUMN CONFERENCE 2013 Including CHIVA Parallel Sessions Professor Rob Miller University College London Medical School COMPETING INTEREST OF FINANCIAL VALUE > 1,000: Speaker Name Prof Rob Miller
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
pulmonary and critical care pearls
 pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
BRONCHOALVEOLAR LAVAGE (BAL) Venerino Poletti Osp GB Morgagni, Forlì (I)
 BRONCHOALVEOLAR LAVAGE (BAL) Venerino Poletti Osp GB Morgagni, Forlì (I) BAL-OTELLI Typical microliths (calcospherites) Acute Respiratory Failure. Clinical history. Treated for GI cancer Bollèe G, et
BRONCHOALVEOLAR LAVAGE (BAL) Venerino Poletti Osp GB Morgagni, Forlì (I) BAL-OTELLI Typical microliths (calcospherites) Acute Respiratory Failure. Clinical history. Treated for GI cancer Bollèe G, et
A Case of Statin-Induced Interstitial Pneumonitis due to Rosuvastatin
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.281 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:281-285 A Case of Statin-Induced Interstitial Pneumonitis due to Rosuvastatin
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.281 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:281-285 A Case of Statin-Induced Interstitial Pneumonitis due to Rosuvastatin
Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after smoking cessation
 Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
Interstitial lung disease (ILD) is a group of diseases with
 Diagnostic Surgical Lung Biopsies for Suspected Interstitial Lung Diseases: A Retrospective Study Martin I. Sigurdsson, MD, Helgi J. Isaksson, MD, Gunnar Gudmundsson, MD, PhD, and Tomas Gudbjartsson, MD,
Diagnostic Surgical Lung Biopsies for Suspected Interstitial Lung Diseases: A Retrospective Study Martin I. Sigurdsson, MD, Helgi J. Isaksson, MD, Gunnar Gudmundsson, MD, PhD, and Tomas Gudbjartsson, MD,
Tables of Normal Values (As of February 2005)
 Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
Complicated echinococcal cyst to Biopsy or not to biopsy. V. Rusanov MR Kramer Pulmonary Institute, Rabin medical center
 Complicated echinococcal cyst to Biopsy or not to biopsy V. Rusanov MR Kramer Pulmonary Institute, Rabin medical center Case 1 84 y.o. Male, Iraq descend, past smoker 40 PY Medical History- HTN, Rheumatoid
Complicated echinococcal cyst to Biopsy or not to biopsy V. Rusanov MR Kramer Pulmonary Institute, Rabin medical center Case 1 84 y.o. Male, Iraq descend, past smoker 40 PY Medical History- HTN, Rheumatoid
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Clinical spectrum of cryptogenic organising pneumonitis
 554 Thorax 1991;46:554-558 Departments of Respiratory Medicine and Tissue Pathology, Monash Medical Centre, Melbourne 3004, Victoria, Australia R Bellomo M Finlay P McLaughlin E Tai Reprint requests to:
554 Thorax 1991;46:554-558 Departments of Respiratory Medicine and Tissue Pathology, Monash Medical Centre, Melbourne 3004, Victoria, Australia R Bellomo M Finlay P McLaughlin E Tai Reprint requests to:
Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment
 Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Scholars Journal of Medical Case Reports
 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2015; 3(9B):928-932 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Medical Case Reports Sch J Med Case Rep 2015; 3(9B):928-932 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Α 78-year-old female who presents with a non-resolving pneumonia: what is your diagnosis?
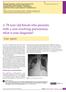 Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
A Rapidly Progressive Case of Interstitial Pneumonia
 CASE REPORT A Rapidly Progressive Case of Interstitial Pneumonia Toshiyuki Katoh, Takashi Ohishi, Nobuya Ikuta, Yoshinori Kawabata*, Kenzo Takagi and Tetsuo Hayakawa Wetreated a 51-year-old womanwho had
CASE REPORT A Rapidly Progressive Case of Interstitial Pneumonia Toshiyuki Katoh, Takashi Ohishi, Nobuya Ikuta, Yoshinori Kawabata*, Kenzo Takagi and Tetsuo Hayakawa Wetreated a 51-year-old womanwho had
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Bronchiolitis obliterans with organising pneumonia: outcome
 Thorax 1995;50(Suppl 1):S59-S64 Bronchiolitis obliterans with organising pneumonia: outcome Ulrich Costabel, Josune Guzman, Helmut Teschler Abteilung Pneumologie/Allergologie, Ruhrlandklinik, Essen, Germany
Thorax 1995;50(Suppl 1):S59-S64 Bronchiolitis obliterans with organising pneumonia: outcome Ulrich Costabel, Josune Guzman, Helmut Teschler Abteilung Pneumologie/Allergologie, Ruhrlandklinik, Essen, Germany
A Vietnamese woman with a 2-week history of cough
 Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern
 ORIGINAL ARTICLE Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern Tetsuro Sawata, Masashi Bando, Masayuki Nakayama, Naoko Mato, Hideaki Yamasawa
ORIGINAL ARTICLE Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern Tetsuro Sawata, Masashi Bando, Masayuki Nakayama, Naoko Mato, Hideaki Yamasawa
Efficacy of short-term prednisolone treatment in patients with chronic eosinophilic pneumonia
 ORIGINAL ARTICLE INTERSTITIAL AND ORPHAN LUNG DISEASE Efficacy of short-term prednisolone treatment in patients with chronic eosinophilic pneumonia Yoshiyuki Oyama 1, Tomoyuki Fujisawa 1, Dai Hashimoto
ORIGINAL ARTICLE INTERSTITIAL AND ORPHAN LUNG DISEASE Efficacy of short-term prednisolone treatment in patients with chronic eosinophilic pneumonia Yoshiyuki Oyama 1, Tomoyuki Fujisawa 1, Dai Hashimoto
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Nitrofurantoin Pulmonary Toxicity: A Brief Review
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 6 Number 2 B Vahid, B Wildemore Citation B Vahid, B Wildemore.. The Internet Journal of Pulmonary Medicine. 2005 Volume 6 Number 2. Abstract
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 6 Number 2 B Vahid, B Wildemore Citation B Vahid, B Wildemore.. The Internet Journal of Pulmonary Medicine. 2005 Volume 6 Number 2. Abstract
Lung Injury after HCT
 Lung Injury after HCT J. Douglas Rizzo, MD, MS Financial Disclosure None SCS06_1.ppt Background HCT an important therapeutic modality for malignant and non-malignant diseases Pulmonary Toxicity common
Lung Injury after HCT J. Douglas Rizzo, MD, MS Financial Disclosure None SCS06_1.ppt Background HCT an important therapeutic modality for malignant and non-malignant diseases Pulmonary Toxicity common
Hiroyuki Kamiya 1), Soichiro Ikushima 1), Tetsu Sakamoto 1), Kozo Morimoto 1), Tsunehiro Ando 1), Masaru Oritsu 1), Atsuo Goto 2), Tamiko Takemura 3)
 29 2001 ACE39.7IU/l X TBLB 2002 11 Langhans [ ] A Case of Granulomatous Interstitial Nephritis with Progressive Renal Impairment Due to Sarcoidosis in the Course of Spontaneous Improvement of Pulmonary
29 2001 ACE39.7IU/l X TBLB 2002 11 Langhans [ ] A Case of Granulomatous Interstitial Nephritis with Progressive Renal Impairment Due to Sarcoidosis in the Course of Spontaneous Improvement of Pulmonary
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease
 Monaldi Arch Chest Dis 2006; 65: 2, 96-101 ORIGINAL ARTICLE Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease C. Robalo Cordeiro 1, S. Freitas 1, B. Rodrigues 1, A. Catarino 1,
Monaldi Arch Chest Dis 2006; 65: 2, 96-101 ORIGINAL ARTICLE Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease C. Robalo Cordeiro 1, S. Freitas 1, B. Rodrigues 1, A. Catarino 1,
Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia
 Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
A 72-year-old male with worsening interstitial infiltrates and respiratory failure
 A 72-year-old male with worsening interstitial infiltrates and respiratory failure Case report On November 24, 2004, a 72-year-old male was admitted to the medical intensive care unit (ICU) with a history
A 72-year-old male with worsening interstitial infiltrates and respiratory failure Case report On November 24, 2004, a 72-year-old male was admitted to the medical intensive care unit (ICU) with a history
Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient
 doi: 10.2169/internalmedicine.9338-17 Intern Med 57: 1281-1285, 2018 http://internmed.jp CASE REPORT Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient Yuki Hosono, Nobuhiko Sawa,
doi: 10.2169/internalmedicine.9338-17 Intern Med 57: 1281-1285, 2018 http://internmed.jp CASE REPORT Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient Yuki Hosono, Nobuhiko Sawa,
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Atopic Pulmonary Disease: Findings on Thoracic Imaging
 July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy
 Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
Pulmonary Pearls. Medical Pearls. Case 1: Case 1 (cont.): Case 1: What is the Most Likely Diagnosis? Case 1 (cont.):
 Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Review Article Correlation between Clinical Characteristics and Chest Computed Tomography Findings of Pulmonary Cryptococcosis
 Pulmonary Medicine Volume 2015, Article ID 703407, 7 pages http://dx.doi.org/10.1155/2015/703407 Review Article Correlation between Clinical Characteristics and Chest Computed Tomography Findings of Pulmonary
Pulmonary Medicine Volume 2015, Article ID 703407, 7 pages http://dx.doi.org/10.1155/2015/703407 Review Article Correlation between Clinical Characteristics and Chest Computed Tomography Findings of Pulmonary
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
The Pathologic Manifestations of Small Airway Disease. Samuel A. Yousem, MD. Small Airway Disease (SAD) SAD
 The Pathologic Manifestations of Small Airway Disease Samuel A. Yousem, MD Small Airway Disease (SAD) A clinicopathologic syndrome reflecting a CHRONIC inflammatory and cicatricial process primarily affecting
The Pathologic Manifestations of Small Airway Disease Samuel A. Yousem, MD Small Airway Disease (SAD) A clinicopathologic syndrome reflecting a CHRONIC inflammatory and cicatricial process primarily affecting
Pneumocystis Pneumonia. Dr. Pradeep kumar II yr Pulmonary Medicine
 Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Cryptogenic Organising Pneumonia As The Initial Presenting Manifestation of SLE
 BMH Medical Journal 2015;2(3):79-83 Case Report Cryptogenic Organising Pneumonia As The Initial Presenting Manifestation of SLE Neena Mampilly MD, G Manoj MD, Binoy J Paul MD, PhD, DNB, FRCP Baby Memorial
BMH Medical Journal 2015;2(3):79-83 Case Report Cryptogenic Organising Pneumonia As The Initial Presenting Manifestation of SLE Neena Mampilly MD, G Manoj MD, Binoy J Paul MD, PhD, DNB, FRCP Baby Memorial
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Radiological Imaging of Drug-Induced Pulmonary Lesions
 Review Article imedpub Journals www.imedpub.com Journal of Clinical Radiology and Case Reports Radiological Imaging of Drug-Induced Pulmonary Lesions D souza M *, Rajiah P, Khan A and Irion K Department
Review Article imedpub Journals www.imedpub.com Journal of Clinical Radiology and Case Reports Radiological Imaging of Drug-Induced Pulmonary Lesions D souza M *, Rajiah P, Khan A and Irion K Department
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis
 Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Methods ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE
 ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
Careful histopathological evaluation has shown the traditionally clinical diagnosis of
 Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
9/15/11. Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September Scleroderma. Hard skin
 Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
EOSINOPHLIC LUNG DISEASES
 EOSINOPHLIC LUNG DISEASES A wide spectrum of infiltrative lung diseases characterized by infiltration of lung parenchyma with eosinophils and/or peripheral blood eosinophilia. How is the diagnosis made?
EOSINOPHLIC LUNG DISEASES A wide spectrum of infiltrative lung diseases characterized by infiltration of lung parenchyma with eosinophils and/or peripheral blood eosinophilia. How is the diagnosis made?
Pulmonary migratory infiltrates due to mycoplasma infection: case report and review of the literature
 Case Report Pulmonary migratory infiltrates due to mycoplasma infection: case report and review of the literature Wenjie You 1 *, Bi Chen 1 *, Jing Li 2, Juan Shou 3, Shan Xue 1, Xueqing Liu 1, Handong
Case Report Pulmonary migratory infiltrates due to mycoplasma infection: case report and review of the literature Wenjie You 1 *, Bi Chen 1 *, Jing Li 2, Juan Shou 3, Shan Xue 1, Xueqing Liu 1, Handong
