Department of Surgery, University of Alberta, 1F1.52 WMC, Street, Edmonton, AB, Canada T6G 2B7 3
|
|
|
- Domenic McLaughlin
- 6 years ago
- Views:
Transcription
1 The Scientific World Journal Volume 2012, Article ID , 7 pages doi: /2012/ The cientificworldjournal Clinical Study An Evaluation of the Responsiveness and Discriminant Validity of Shoulder Questionnaires among Patients Receiving Surgical Correction of Shoulder Instability Kyle A. R. Kemp, 1 David M. Sheps, 2 Lauren A. Beaupre, 2, 3 Fiona Styles-Tripp, 4 Charlene Luciak-Corea, 4 and Robert Balyk 2 1 Orthopaedic Research, Alberta Health Services, Capital Health Region, 1F1.52 WMC, Street, Edmonton, AB, Canada T6G 2B7 2 Department of Surgery, University of Alberta, 1F1.52 WMC, Street, Edmonton, AB, Canada T6G 2B7 3 Department of Physical Therapy, University of Alberta, 3-71 Corbett Hall, Edmonton, AB, Canada T6G 2G4 4 Department of Rehabilitation Medicine, Covenant Health-Grey Nuns Hospital, 110 Youville Drive West, Room 1107, Edmonton, AB, Canada T6L 5X8 Correspondence should be addressed to Kyle A. R. Kemp, kykemp@toh.on.ca Received 20 October 2011; Accepted 8 December 2011 Academic Editor: Kiyohisa Ogawa Copyright 2012 Kyle A. R. Kemp et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Health-related quality-of-life (HRQL) measures must detect clinically important changes over time and between different patient subgroups. Forty-three patients (32 M, 13 F; mean age = ± 8.19 years) undergoing arthroscopic Bankart repair completed three validated shoulder questionnaires (Western Ontario Shoulder Instability index (WOSI), American Shoulder and Elbow Surgeons Standardized Shoulder Assessment form (ASES), Constant score) preoperatively, and at 6, 12, and 24 months postoperatively. Responsiveness and discriminant validity was assessed between those with a satisfactory outcome and those with (1) a major recurrence of instability, (2) a single episode of subluxation, (3) any postoperative episode of instability. Eight (20%) patients reported recurrent instability. Compared to baseline, the WOSI detected improvement at the 6- (P <0.001) and 12- month (P = 0.011) evaluations. The ASES showed improvement at 6 months (P = 0.003), while the Constant score did not report significant improvement until 12 months postoperatively (P = 0.001). Only the WOSI detected differential shoulder function related to shoulder instability. Those experiencing even a single episode of subluxation reported a 10% drop in their WOSI score, attaining the previously established minimal clinically important difference (MCID). Those experiencing a frank dislocation or multiple episodes of subluxation reported a 20% decline. The WOSI allows better discrimination of the severity of postoperative instability symptoms following arthroscopic Bankart repair. 1. Introduction In orthopaedics and rehabilitation, the assessment of healthrelated quality of life (HRQL) is an important outcome to consider when assessing the effectiveness of various interventions [1, 2]. Validated patient-reported questionnaires are commonly used to obtain the patients perception of the limitations that are associated with various musculoskeletal conditions. A number of joint and disease-specific HRQL measures now exist for many of the main conditions of the shoulder, including rotator cuff tears and recurrent instability [1, 3]. Some measures were developed using rigorous and accepted methodology [4, 5], while others were developed based on clinical validity and utility [4, 6, 7]. Many of these instruments have been assessed for their reliability and validity and to a lesser degree, their responsiveness, or ability to assess change over time and have been found to be adequate [8 10]. However, it has been hypothesized that the less rigorously developed questionnaires may not be as responsive or as discriminative, when compared with newer, conditionspecific questionnaires [1, 4, 6, 11]. Questionnaire selection may play an important role in determining the extent of recovery or disability as well as
2 2 The Scientific World Journal detecting differential recovery among patients, particularly when only modest differences in outcome may be expected (e.g., comparison of different surgical interventions). Thus, it is important that appropriate HRQL assessment tools are chosen in order to detect clinically important changes (1) over repeated postoperative time periods (responsiveness) and/or (2) among different patient subgroups (discriminant validity). Patients with chronic posttraumatic shoulder instability commonly experience significant impairment during work, sports, or while performing activities of daily living (ADL). Often times, their limitations are great enough to warrant surgical intervention [12, 13]. The short-and long-term success of these techniques has been widely demonstrated within the literature, with the incidence of postoperative recurrent dislocation being less than 10% and of recurrent postoperative instability (i.e., recurrent dislocation or subjective sense of subluxation being less than 20%) [13]. Given that this population experiences significant functional gains following surgery, we felt that this condition was an appropriate one to compare how selected shoulder questionnaires perform in (1) responsiveness and (2) discrimination among preselected subsets of patients. Therefore, the goal of the present study was to perform a prospective evaluation of the performance of three different questionnaires commonly used to evaluate outcomes following surgical correction of chronic shoulder instability: (1) the disease-specific Western Ontario Shoulder Instability index (WOSI), (2) the shoulder-specific American Shoulder and Elbow Surgeons Standardized Shoulder Assessment form (ASES), and (3) the shoulder-specific Constant score. The primary aim was to compare the responsiveness of these three instruments over multiple postoperative time periods. The secondary aim was to compare the instruments abilities to discriminate among three subsets of subjects: (1) those with major recurrence of instability (e.g., frank dislocation), (2) those with a single episode of subluxation, and (3) those with any recurrence of instability (i.e., all subjects who reported any of the above described symptoms) in the first 2 years relative to those subjects who did not report a recurrence of instability. We hypothesized that the disease-specific questionnaire (WOSI) would be more responsive to change over time when compared to the two shoulder-specific instruments; the ASES and the Constant score. Further, we hypothesized that the WOSI would be better able to discriminate between those who had a successful outcome and those who experienced any recurrence of instability symptoms following surgical repair of their Bankart lesion compared with either of the two shoulder-specific questionnaires. 2. Materials and Methods Between 2001 and 2007, a total of 43 subjects (32 men, 11 women; mean age = 26.0 ± 8.2 years) with unilateral, symptomatic, recurrent posttraumatic anterior shoulder instability were included in our prospective study. To be included in the study, subjects had to have symptoms of anterior glenohumeral instability that significantly affected their ability to function in daily life and a positive apprehension test. Subjects were excluded if they had undergone previous shoulder surgery, had multidirectional instability, or were unable to speak or read the English language. Subjects underwent an arthroscopic Bankart repair using bioabsorbable Suretac anchors (Smith & Nephew Endoscopy, Andover, MA). The surgical procedures were performed by one of two subspecialty trained arthroscopic surgeons. To be eligible at surgery, subjects had to present with labral pathology indicative of a Bankart lesion (injury at the 3 6 o clock position). Those with a superior labral anterioposterior (SLAP) lesion were also included. Those with only a SLAP lesion or those with a full or partial thickness rotator cuff tear were excluded. Prior to surgery, baseline demographic information (age, sex, smoking status) and shoulder/injury characteristics (arm dominance, arm injured, level of sport competition played (when applicable), chief complaint relative to injury) were gathered. All subjects completed a standardized rehabilitation protocol. Subjects were immobilized in a simple sling for the first 4 to 6 weeks. During this time, external rotation and abduction were not permitted; however, active and activeassisted forward flexion and internal rotation range of motion (ROM) exercises were encouraged. Following this initial period of immobilization, progressive ROM and strengthening exercises commenced. Subjects were permitted to return to full work and sports activities once they had full ROM, strength, and functional stability of the involved shoulder. As part of the prospective study, subjects underwent a musculoskeletal examination, including ROM and strength testing, by a licensed physiotherapist preoperatively, and at 6, 12, and 24 months postoperatively. During these evaluations, subjects also completed three shoulder questionnaires: the WOSI, the ASES, and the Constant score, which are the focus of the present paper Instruments. The WOSI is a condition-specific questionnaire designed for use with patients who have shoulder instability [5]. It is comprised of 21 self-reported items, divided into 4 sections; physical symptoms (10 items), sport/ recreation/work function (4 items), lifestyle function (4 items), and emotion function (3 items). Each item is scored on a 100-mm visual analog scale (VAS), with the best possible raw score being 0 points and the worst being 100 points. Therefore the best possible cumulative score is 0, indicating no disease, while the worst one is 2,100, indicating the presence of extreme disease (i.e., instability). Cumulative scores may be reported as well as subscale scores. In the present study, only cumulative scores are reported and were standardized to a scale where 100 indicated no shoulder dysfunction related to instability. This scale has been shown to be valid, reliable, and responsive [4, 14]. Further, a minimally clinically important difference (MCID) of 10%, that is, the minimal difference in the WOSI score that has to occur for a patient to rate their shoulder as having changed, has been established [5]. The patient self-evaluation section of the ASES is a shoulder-specific instrument and is comprised of 11 items,
3 The Scientific World Journal 3 which are divided into two areas; pain (1 item) and function (10 items) [7]. The pain item consists of a 10 cm visual analog scale (VAS), which asks the patient how bad is your pain today?. The 10 cm scale is divided into 1 cm increments and is anchored with verbal descriptors ( no pain at all, as bad as it can be ). The items comprising the function area of the ASES include 10 questions pertaining to activities of daily living. Patients are asked to indicate their ability to complete a given list of activities using a four-point Likert scale (0, unable to do; 1, very difficult; 2, somewhat difficult; 3, not difficult). These range from simple activities, such as putting on a coat, and combing hair, to more demanding ones, such as lifting ten pounds above shoulder level and throwing a ball in an overhand fashion. The final two items of the function section pertain to the patient s usual work and sports. For these items, patients are asked to select personal work and sports activities which are important to them, (i.e., ones in which they are likely to participate in and that they take part in frequently enough that they may provide a comment above that activity s relative difficulty throughout the year). To obtain the final score out of 100, the pain score (maximum of 10) is multiplied by five (for a total of 50), and the cumulative activity score (maximum of 30) is multiplied by 5/3 (for a total of 50), so that the pain and activity elements of the questionnaire are equally weighted. No published data exists to support this weighting scheme. Although there is limited information on development of the ASES, it has been shown to be valid, reliable and an MCID of 6.4 points has been established for this score [8, 9]. The Constant Score is the most widely used shoulder evaluation questionnaire in Europe [15], and is a shoulderspecific instrument. The score is a combination of an objective physical examination (65 points) and a subjective patient self-evaluation (35 points) [6]. The physical examination component includes a range of motion assessment (forward elevation, lateral elevation, internal rotation, and external rotation), worth a total of 40 points (maximum of 10 points for each motion). The remaining 25 points are attributed to the strength assessment, where patients are awarded one point for each pound of pull that the patient can resist in abduction. Therefore, the total possible score on the Constant Score is 100 points (best possible score = 100, worst possible score = 0). Although there is very limited data on the development of the instrument, the Constant score has been shown to be reliable, valid and responsive in assessing the impact of shoulder interventions [10]. No MCID has been established for this scale Outcomes. The primary outcome was the ability for the instruments to detect change in subjects condition over multiple time periods (responsiveness). The secondary outcome was the ability for the instruments to detect differences in outcomes among three subgroups with recurrent instability relative to those who reported no recurrent instability (discriminant validity) Definitions of Recurrence of Instability. We defined three subsets of subjects prior to starting the discriminant validity analysis. We were interested only in recurrent instability rather than any shoulder reinjury. The first subgroup was made up of those who had a major re-occurrence of instability, defined as a frank dislocation during sports or ADL (shoulder dislocation that required medical intervention to relocate) or multiple episodes of subluxation (did not require medical intervention to relocate, but each subluxation episode produced symptoms similar to preoperative symptoms of instability). The second subgroup of subjects was made up of those who experienced a single episode of subluxation (i.e., did not require medical intervention to relocate, but had one episode of subluxation that produced symptoms similar to preoperative symptoms of instability) while the final subgroup combined the initial two groups and looked at subjects who had any recurrence of instability (i.e., at least 1 episode of subluxation and/or a frank dislocation) Analysis. Statistical analysis was performed using statistical packages for the social sciences (SPSS), version 18.0 (SPSS Inc., Chicago, IL). Descriptive statistics (mean, standard deviation, range) were calculated for all variables, in order to determine statistical significance, an alpha level of α<0.05. To examine responsiveness, a repeated measures analysis of variance (ANOVA) was undertaken over four time periods with a post-hoc contrast analysis of each interval for the three questionnaires. For the discriminant analysis, baseline comparisons were made between those who experienced a satisfactory outcome and those patients who experienced (1) a major recurrence of instability as previously defined, (2) a single episode of subluxation, and (3) any postoperative episode of instability to look for any systematic baseline differences among these patients. Then, scores at 6 months and at 2 years were compared between those without any adverse stability events and each of these three subgroups of patients as all reinjuries were reported after six-months postoperatively. An independent t-test analysis was performed on the change in each of the scores between the six-month and final evaluation to determine if the outcome measures were able to detect significant differences between each subgroup relative to those who reported a successful outcome at two years. 3. Results 3.1. Demographic and Injury Characteristics. Complete demographics are provided in Table 1.Subjects were predominantly male and right hand dominant. The average age of the participants was 26.0 ± 8.2 years. Many participants (n = 26; 60.5%) competed in competitive sports at the time of their injury. The indication for surgery was instability in 40 (93%) cases and instability with pain for the other three patients. Forty (93%) patients were followed out to two years postoperatively. Three subjects reported a frank dislocation (n = 2) or multiple episodes of subluxation (n = 1). Five additional subjects reported a single episode of subluxation for a total of 8 (20%) subjects reporting recurring issues with instability.
4 4 The Scientific World Journal Variable Table 1: Demographic & preinjury characteristics of sample with shoulder instability. All n = 43 No recurrence n = 32 Recurrence of instability n = 8 Demographics Mean age in years (SD) 26.0 (8.2) 25.5 (7.8) 28.4 (10.0) Male sex (%) 32 (74) 24 (75) 6 (75) Smokers (%) 8 (19) 5 (17) 2 (25) Shoulder characteristics Right side injury (%) 25 (58) 22 (62) 3 (38) Right hand dominance (%) 39 (91) 28 (88) 8 (100) Competitive sport level International(%) 1(2) 1(3) 0(0) National (%) 1 (2) 1 (3) 0 (0) Provincial (%) 7 (16) 5 (17) 1 (12) Local (%) 17 (40) 11 (34) 4 (50) Not applicable (%) 17 (40) 14 (43) 3 (38) Table 2: Responsiveness (change over time) of three common shoulder questionnaires. WOSI Preoperative 6-month postoperative 12-month postoperative 24-month postoperative Score (mean (standard deviation)) 48.1 (19.8) 78.1 (16.6) 84.1 (14.6) 85.1 (14.6) P value < ASES Preoperative 6-Month Postoperative 12-Month Postoperative 24-month postoperative Score (mean (standard deviation)) 84.7 (7.8) 91.5 (10.3) 94.4 (4.9) 94.2 (7.7) P value Constant Preoperative 6-Month Postoperative 12-Month Postoperative 24-month postoperative Score 9(mean (standard deviation)) 81.6 (15.9) 82.5 (14.2) 92.2 (7.7) 93.6 (6.6) P value Using Post Hoc contrasts (repeated) to measure changes between intervals Responsiveness. Table 2 reports the scores for each of the outcome measures over time. The WOSI had a substantially lower preoperative score than either the Constant or ASES scores. The WOSI was also able to detect significant improvements in the subjects shoulder symptoms at both the six-and 12-month evaluation, with no substantial changes noted in shoulder function between 12 and 24 months postoperatively (Table 2 and Figure 1). In contrast, the ASES showed a significant improvement between preoperative and six-month scores, but no significant improvements were detected after that time (Table 2 and Figure 1). The Constant did not report a significant improvement until 12 months postoperatively with no further improvements noted after the 12-month evaluation (Table 2 and Figure 1) Change at 6 months WOSI ASES Constant Change at 12 months Change at 24 months 3.3. Discriminant Validity. Thepreoperativescoresforsubjects who had any recurrence of instability and those who were not significantly different for all three of the outcome measures (Table 3). However, the WOSI was able to detect significant differences in outcomes between subjects who had any reported episodes of instability with a score of reduction of at least 10 points reported between the pre- and post- reinjury assessment, including those subjects who reported only a single episode of subluxation. Those who reported a frank Figure 1: Mean change from preoperative evaluation over time of three common shoulder questionnaires. dislocation or multiple episodes of subluxation reported a mean reduction of over 20 points in the WOSI (Table 3). In contrast, the ASES was not able to detect changes in shoulder function in subjects who reported any kind of reinjury (Table 3). The Constant score appeared better able to detect group differences, but changes in the Constant score
5 The Scientific World Journal 5 Table 3: Discriminant validity of three common shoulder questionnaires. WOSI Preoperative P value 6-month postoperative 24-month postoperative Difference P value Recurrence Yes 47.3 (17.2) 71.4 (27.1) 50.8 (6.0) 20.6 (21.0) 0.96 No 46.8 (17.2) 75.3 (17.7) 84.4 (17.0) 9.2 (16.6) 0.02 Single subluxation Yes 79.8 (9.3) 76.3 (25.4) 65.7 (27.1) 10.5 (9.1) 0.73 No 80.1 (13.6) 74.8 (16.8) 85.4 (15.2) 10.6 (17.4) 0.02 Any Reinjury Yes 44.6 (20.8) 74.9 (23.6) 61.5 (23.4) 13.4 (12.4) 0.86 No 45.9 (17.6) 75.1 (16.6) 88.0 (12.1) 13.0 (15.0) < ASES Preoperative P value 6-month postoperative 24-month postoperative Difference P value Recurrence Yes 84.5 (11.5) 88.0 (5.2) 88.2 (5.2) 0.2 (00) 0.75 No 82.7 (9.0) 88.2 (15.7) 92.5 (14.5) 4.3 (11.7) 0.63 Single subluxation Yes 79.8 (9.3) 82.1 (30.7) 79.5 (32.0) 2.6 (1.8) 0.96 No 80.1 (13.6) 89.2 (11.6) 94.4 (7.7) 5.2 (12.3) 0.17 Any reinjury Yes 81.6 (9.6) 83.8 (25.3) 82.0 (25.6) 1.8 (2.0) 0.73 No 79.8 (13.8) 89.2 (12.0) 94.8 (7.7) 5.6 (12.7) 0.14 Constant Preoperative P value 6-month postoperative 24-month postoperative Difference P value Recurrence Yes 80.1 (18.7) 91.2 (0.28) 83.8 (18.0) 7.5 (17.7) 0.98 No 79.9 (12.8) 82.7 (17.2) 92.1 (13.4) 9.4 (12.4) 0.08 Single subluxation Yes 71.9 (17.8) 74.8 (35.3) 75.7 (31.8) 1.9 (3.6) 0.41 No 78.3 (16.0) 84.8 (12.6) 94.0 (6.6) 9.2 (13.8) 0.31 Any reinjury Yes 75.0 (17.3) 79.6 (28.8) 78.4 (26.3) 1.2 (9.7) 0.63 No 78.1 (16.0) 84.2 (13.0) 94.8 (4.8) 10.6 (12.9) 0.05 were less than nine points between pre- and post- reinjury (Table 3). 4. Discussion In a cohort of 43 patients who underwent arthroscopic surgery for recurrent glenohumeral instability, three commonly used shoulder evaluation questionnaires were able to detect improvements in patients postoperative shoulder function. However, as hypothesized, the WOSI was the most responsive of the three instruments and was able to detect incremental improvement over time. When compared to preoperative values, significant improvements in the WOSI were noted six months postoperatively with further substantial improvements between six and 12 months postoperatively. In contrast, the ASES scale noted significant functional improvements beginning at the six-month mark, but did not detect further improvements at either the 12- or 24-month assessment. The Constant score did not detect significant postoperative functional change until 12 months following surgery. Further, in predefined subsets of patients who might be expected to report differential postoperative recovery, only the WOSI was able to discriminate differential shoulder function related to shoulder instability. Although only three (7.5%) patients were identified as a postoperative failure and five additional subjects reported recurrent symptoms of instability at the 24-month postoperative period, the WOSI score changed in alignment with the severity of the postoperative complication even with these limited numbers. A recurrent dislocation rate of approximately 10% has been reported in previous literature with rates of any instability recurrence being reported between 10 and 20%. These differences reported in the literature may reflect both the different definitions of recurrent instability that were used among studies as well as the difference in surgical techniques or rehabilitation programs. We had over recurrent instability rates that were at the higher end of the reported range, which may reflect the poorer performance of the SureTac, a device that has mostly been abandoned in current practice, or may reflect the stringent measurement of recurrent instability symptoms. Subjects who we considered to have a major recurrence (frank dislocation or multiple episodes of subluxation) reported a 20% decline in their WOSI score, well beyond the established
6 6 The Scientific World Journal MCID [5]. The five additional subjects who reported only a single episode of subluxation in the initial 24 months postoperatively reported a more modest, but still detectible reduction in their function as measured by the WOSI that attained the previously established MCID [5]. In contrast, neither the ASES nor the Constant were able to discriminate in outcomes among these subgroups. These findings were not unexpected, as the items on the WOSI focus on restrictions that are commonly reported by subjects experiencing shoulder instability. Our findings expand upon previous research, which showed that the WOSI was more responsive at the 2-week and 3-month postoperative periods, when compared with several other measures of shoulder function, including the ASES and Constant Score [5, 14], as well as measures of general health such as the 12-Item Short-Form Health Survey [14]. To our knowledge, however, this is the first time that the ability of questionnaires to discriminate among predefined subsets of patients has been examined. It was surprising to see the level of discrimination attained by the WOSI, where those who had only a single episode of recurrent instability had a detectible change in function. This level of discrimination would be very useful in studies that do direct comparisons of different surgical techniques for shoulder instability when only modest outcome differences are expected. Previous literature has hypothesized that the ASES may have poor responsiveness, especially among patients with better function [16 19]. As each item is scored based on difficulty associated with certain tasks, it may be relatively easy to improve one s ASES score by one point, creating a potential ceiling effect within certain patients [16, 18]. Conversely, the Constant score has been reported to have substantial floor effects because subjects may have difficulty completing the strength testing due to the prescribed testing position [19]. However, in a previous study, Conboy et al. reported that all subjects in a study of 25 patients with recurrent instability scored well on the Constant score even prior to intervention [17]. Our results replicate this finding in that preoperatively, the average Constant score did not indicate a great deal of shoulder dysfunction, leaving very little room for postoperative improvement. The study has a number of strengths including the high rate of followup out to 24 months and a prospective study design with preoperative assessment that diminishes the amount of bias that may occur in nonrandomized studies. Unlike most previously published series, the prospective data collection, with outcomes established a priori, has allowed assessment of subjective shoulder function at regular postoperative intervals. This methodology has allowed us to examine recovery over time to determine when the majority of recovery occurs and when shoulder function appears to stabilize over time. Further, it also allowed us to detect when subjects experience a loss of function due to recurrent symptoms or failure of the intervention. However, there are some notable limitations to this paper. We did not have a comparison group, and only a small number of subjects experienced an adverse postoperative outcome. Because we had such a small study group, our results should be applied with some caution and these measurements should be repeated in larger studies examining the management of recurrent instability. Despite these limitations, our study demonstrates the importance of considering expected outcomes and choosing instruments that will allow the best discrimination amongst various patient subsets and that can monitor small change in shoulder function over time. 5. Conclusion Our findings suggest that similar to other studies examining psychometric properties of common shoulder evaluations, all three of the instruments could be called responsive instruments. However, when compared with other items, the WOSI is the most appropriate subjective questionnaire for detecting postoperative functional change in recurrent shoulder instability population both over time and between groups and should be selected over other measures in this clinical population. References [1] A. Kirkley and S. Griffin, Development of disease-specific quality of life measurement tools, Arthroscopy, vol. 19, no. 10, pp , [2] L. A. Michener and A. R. Snyder, Evaluation of health-related quality of life in patients with shoulder pain: are we doing the best we can? Clinics in Sports Medicine, vol. 27, no. 3, pp , [3]A.A.Romeo,B.R.Bach,andK.L.O Halloran, Scoring systems for shoulder conditions, American Journal of Sports Medicine, vol. 24, no. 4, pp , [4] A. Kirkley, S. Griffin, and K. Dainty, Scoring systems for the functional assessment of the shoulder, Arthroscopy, vol. 19, no. 10, pp , [5]A.Kirkley,S.Griffin, H. McLintock, and L. Ng, The development and evaluation of a disease-specific quality of life measurement tool for shoulder instability: the Western Ontario Shoulder Instability Index (WOSI), American Journal of Sports Medicine, vol. 26, no. 6, pp , [6] C. R. Constant and A. H. G. Murley, A clinical method of functional assessment of the shoulder, Clinical Orthopaedics and Related Research, vol. 214, pp , [7] R. R. Richards, K. N. An, L. U. Bigliani et al., A standardized method for the assessment of shoulder function, Journal of Shoulder and Elbow Surgery, vol. 3, pp , [8] M. S. Kocher, M. P. Horan, K. K. Briggs, T. R. Richardson, J. O Holleran, and R. J. Hawkins, Reliability, validity, and responsiveness of the American Shoulder and Elbow Surgeons subjective shoulder scale in patients with shoulder instability, rotator cuff disease, and glenohumeral arthritis, The Journal of Bone and Joint Surgery Series A, vol. 87, no. 9, pp , [9] J. S. Roy, J. C. Macdermid, and L. J. Woodhouse, Measuring shoulder function: a systematic review of four questionnaires, Arthritis Care and Research, vol. 61, no. 5, pp , [10] J. S. Roy, J. C. MacDermid, and L. J. Woodhouse, A systematic review of the psychometric properties of the Constant-Murley score, Journal of Shoulder and Elbow Surgery, vol. 19, no. 1, pp , 2010.
7 The Scientific World Journal 7 [11] B. Kirshner and G. Guyatt, A methodological framework for assessing health indices, Journal of Chronic Diseases, vol. 38, no. 1, pp , [12] H. H. Handoll, M. A. Almaiyah, and A. Rangan, Surgical versus non-surgical treatment for acute anterior shoulder dislocation, Cochrane Database of Systematic Reviews, no. 1, Article ID CD004325, [13] R. S. Pulavarti, T. H. Symes, and A. Rangan, Surgical interventions for anterior shoulder instability in adults, Cochrane Database of Systematic Reviews, vol. 4, Article ID CD005077, [14] A. Kirkley, R. Werstine, A. Ratjek, and S. Griffin, Prospective randomized clinical trial comparing the effectiveness of immediate arthroscopic stabilization versus immobilization and rehabilitation in first traumatic anterior dislocations of the shoulder: long-term evaluation, Arthroscopy, vol. 21, no. 1, pp , [15] C. R. Constant, An evaluation of the Constant-Murley shoulder assessment, The Journal of Bone and Joint Surgery Series B, vol. 79, no. 4, pp , [16] F. Angst, M. John, J. Goldhahn et al., Comprehensive assessment of clinical outcome and quality of life after resection interposition arthroplasty of the thumb saddle joint, Arthritis Care and Research, vol. 53, no. 2, pp , [17] V.B.Conboy,R.W.Morris,J.Kiss,andA.J.Carr, Anevaluation of the Constant-Murley shoulder assessment, The Journal of Bone and Joint Surgery Series B, vol.78,no.2,pp , [18] J. Goldhahn, F. Angst, S. Drerup, G. Pap, B. R. Simmen, and A. F. Mannion, Lessons learned during the cross-cultural adaptation of the American Shoulder and Elbow Surgeons shoulder form into German, Journal of Shoulder and Elbow Surgery, vol. 17, no. 2, pp , [19] A. Othman and G. Taylor, Is the Constant score reliable in assessing patients with frozen shoulder? 60 Shoulders scored 3 years after manipulation under anaesthesia, Acta Orthopaedica Scandinavica, vol. 75, no. 1, pp , 2004.
Evaluation of Rotator Cuff Repair Using Korean Shoulder Scoring System
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.206 CiSE Clinics in Shoulder and Elbow Evaluation of Rotator Cuff Repair Using Korean
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.206 CiSE Clinics in Shoulder and Elbow Evaluation of Rotator Cuff Repair Using Korean
SHOULDER AND ELBOW. M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps
 M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps From University of Alberta, Edmonton, Alberta, Canada M. Bouliane, MD, FRCS(C), Orthopaedic Surgeon D. Saliken, MD, Orthopaedic
M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps From University of Alberta, Edmonton, Alberta, Canada M. Bouliane, MD, FRCS(C), Orthopaedic Surgeon D. Saliken, MD, Orthopaedic
Surgical versus conservative treatment for acute first-time anterior shoulder dislocation: the evidence
 J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
First-Time Anterior Shoulder Dislocation: Is it time to take a stand?
 Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
The Patient-Rated Elbow Evaluation (PREE) User Manual. June 2010
 The Patient-Rated Elbow Evaluation (PREE) User Manual June 2010 Joy C. MacDermid, BScPT, MSc, PhD School of Rehabilitation Science, McMaster University, Hamilton, Ontario, Canada Clinical Research Lab,
The Patient-Rated Elbow Evaluation (PREE) User Manual June 2010 Joy C. MacDermid, BScPT, MSc, PhD School of Rehabilitation Science, McMaster University, Hamilton, Ontario, Canada Clinical Research Lab,
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
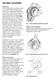 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Anatomy GH Joint. Glenohumeral Instability. Components of Stability. Components of Stability 7/7/2017. AllinaHealthSystem
 Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Body Planes. (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal
 Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Management of Anterior Shoulder Instability
 Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
My shoulder popped out what now?
 My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
Rotator cuff strength following open subscapularis tendon repair
 Acta Orthop. Belg., 2008, 74, 173179 ORIGAL STUDY Rotator cuff strength following open subscapularis tendon repair Roger P. VAN RIET, Sean T. O LEARY, Alexander HOOP, Simon N. BELL From the Melbourne Shoulder
Acta Orthop. Belg., 2008, 74, 173179 ORIGAL STUDY Rotator cuff strength following open subscapularis tendon repair Roger P. VAN RIET, Sean T. O LEARY, Alexander HOOP, Simon N. BELL From the Melbourne Shoulder
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
SLAP Repair. Pre-operatively. Acute phase (0-4 weeks 1 ) Sling. Restrictions? What can I do from day 1? Commence strengthening?
 SLAP Repair Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* No combined AB/ER and end range ER until 6 weeks. Dependent
SLAP Repair Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* No combined AB/ER and end range ER until 6 weeks. Dependent
Labral Tears. Fig 1: Intact labrum and biceps tendon
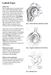 Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Address Correspondence to: Mininder S. Kocher, MD, MPH Department of Orthopaedic Surgery, Children s Hospital
 Patient-Derived Outcomes Assessment: Psychometric Validation of Outcomes Instruments, Patient Satisfaction with Outcome, and Expected Value Decision Analysis Mininder S. Kocher, MD, MPH Department of Orthopaedic
Patient-Derived Outcomes Assessment: Psychometric Validation of Outcomes Instruments, Patient Satisfaction with Outcome, and Expected Value Decision Analysis Mininder S. Kocher, MD, MPH Department of Orthopaedic
Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery
 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength in Patients with Shoulder Disorders: A Preliminary Report
 The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
J oints. Validity and reliability of the SPORTS score for shoulder instability. Abstract. Introduction
 Validity and reliability of the SPORTS score for shoulder instability DaVIDe BlONNa 1, enrico BellatO 2, FraNCeSCO CaraNZaNO 1, DaVIDe e. BONaSIa 2, antongiulio MarMOttI 1, roberto rossi 1, FIlIPPO CaStOlDI
Validity and reliability of the SPORTS score for shoulder instability DaVIDe BlONNa 1, enrico BellatO 2, FraNCeSCO CaraNZaNO 1, DaVIDe e. BONaSIa 2, antongiulio MarMOttI 1, roberto rossi 1, FIlIPPO CaStOlDI
Revision Instability Repair
 Revision Instability Repair Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Revision Instability Repair Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Chronic Shoulder Instability
 Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
ATRAUMATIC SHOULDER CONDITIONS. Matthew J. Landfried, MD Orthopaedic Surgeon Genesee Orthopaedics and Sports Medicine
 ATRAUMATIC SHOULDER CONDITIONS Matthew J. Landfried, MD Orthopaedic Surgeon Genesee Orthopaedics and Sports Medicine MATTHEW LANDFRIED MD Board Certified in Orthopedic Surgery and Sports Medicine Received
ATRAUMATIC SHOULDER CONDITIONS Matthew J. Landfried, MD Orthopaedic Surgeon Genesee Orthopaedics and Sports Medicine MATTHEW LANDFRIED MD Board Certified in Orthopedic Surgery and Sports Medicine Received
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Rotator Cuff Repair Outcomes. Patrick Birmingham, MD
 Rotator Cuff Repair Outcomes Patrick Birmingham, MD Outline Arthroscopic Vs. Mini-open Subjective Outcomes Objective Outcomes Timing Arthroscopic Vs. Mini-open Sauerbrey Arthroscopy 2005 Twenty-six patients
Rotator Cuff Repair Outcomes Patrick Birmingham, MD Outline Arthroscopic Vs. Mini-open Subjective Outcomes Objective Outcomes Timing Arthroscopic Vs. Mini-open Sauerbrey Arthroscopy 2005 Twenty-six patients
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Do Outcomes Differ after Rotator Cuff Repair for Patients Receiving Workers Compensation?
 Clin Orthop Relat Res (2008) 466:3025 3033 DOI 10.1007/s11999-008-0475-1 ORIGINAL ARTICLE Do Outcomes Differ after Rotator Cuff Repair for Patients Receiving Workers Compensation? R. Balyk MD, FRCS (C),
Clin Orthop Relat Res (2008) 466:3025 3033 DOI 10.1007/s11999-008-0475-1 ORIGINAL ARTICLE Do Outcomes Differ after Rotator Cuff Repair for Patients Receiving Workers Compensation? R. Balyk MD, FRCS (C),
SLAP Lesions Assessment & Treatment
 SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
P.O. Box Sierra Park Road Mammoth Lakes, CA Orthopedic Surgery & Sports Medicine
 P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
Measures of Adult Shoulder Function
 Arthritis Care & Research Vol. 63, No. S11, November 2011, pp S174 S188 DOI 10.1002/acr.20630 2011, American College of Rheumatology MEASURES OF PATHOLOGY AND SYMPTOMS Measures of Adult Shoulder Function
Arthritis Care & Research Vol. 63, No. S11, November 2011, pp S174 S188 DOI 10.1002/acr.20630 2011, American College of Rheumatology MEASURES OF PATHOLOGY AND SYMPTOMS Measures of Adult Shoulder Function
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Shoulder Instability and Stabilisation
 Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
Instability of the shoulder Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life
 Author's response to reviews Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life Authors: Jean-Sébastien Roy (jean-sebastien.roy.1@ulaval.ca)
Author's response to reviews Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life Authors: Jean-Sébastien Roy (jean-sebastien.roy.1@ulaval.ca)
Traumatic Instability Understanding your shoulder injury and its repair
 Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Chronic Shoulder Disorders
 Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Excision arthroplasty following shoulder replacement
 Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
The Shoulder. By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson
 The Shoulder By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson Learning Objectives/Agenda Review the anatomy of the shoulder Describe the main diseases of the shoulder Describe the
The Shoulder By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson Learning Objectives/Agenda Review the anatomy of the shoulder Describe the main diseases of the shoulder Describe the
Department of Orthopaedic Surgery University of California, Davis
 Department of Orthopaedic Surgery University of California, Davis Lloyd W. Taylor Resident Award: Diagnostic Accuracy of MRI in SLAP Tears: A Retrospective Review of 444 Patients Utilizing Musculoskeletal
Department of Orthopaedic Surgery University of California, Davis Lloyd W. Taylor Resident Award: Diagnostic Accuracy of MRI in SLAP Tears: A Retrospective Review of 444 Patients Utilizing Musculoskeletal
SLAP Repair Therapy Protocol
 PHASE I: PRE-OPERATIVE PHASE (OPTIONAL) SLAP Repair Therapy Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Restore full AROM and PROM Restore full strength
PHASE I: PRE-OPERATIVE PHASE (OPTIONAL) SLAP Repair Therapy Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Restore full AROM and PROM Restore full strength
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
Rotator Cuff Pathology. Shoulder Instability. Adhesive Capsulitis. AC Joint Dysfunction
 Shoulder Pain Red Flags Unexplained deformity or swelling Significant weakness not due to pain Suspected malignancy Fever/chills/malaise Significant/unexplained sensory/motor deficit Pulmonary or vascular
Shoulder Pain Red Flags Unexplained deformity or swelling Significant weakness not due to pain Suspected malignancy Fever/chills/malaise Significant/unexplained sensory/motor deficit Pulmonary or vascular
Outcomes of Isolated Type II SLAP Lesions Treated With Arthroscopic Fixation Using a Bioabsorbable Tack
 Outcomes of Isolated Type II SLAP Lesions Treated With Arthroscopic Fixation Using a Bioabsorbable Tack David B. Cohen, M.D., Struan Coleman, M.D., Ph.D. Mark C. Drakos, M.D., Answorth A. Allen, M.D.,
Outcomes of Isolated Type II SLAP Lesions Treated With Arthroscopic Fixation Using a Bioabsorbable Tack David B. Cohen, M.D., Struan Coleman, M.D., Ph.D. Mark C. Drakos, M.D., Answorth A. Allen, M.D.,
Assessment of functional outcome of mini-open rotator cuff repair: a hospital based prospective study
 International Journal of Research in Orthopaedics http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180681 Assessment of functional outcome of
International Journal of Research in Orthopaedics http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180681 Assessment of functional outcome of
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder
 Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
COPYRIGHT Ó BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED ACEVEDO ET AL. ASURVEY OF EXPERT OPINION REGARDING ROTATOR CUFF REPAIR
 Page 1 of 23 Appendix 1 Page 2 of 23 Page 3 of 23 Page 4 of 23 Page 5 of 23 Page 6 of 23 Page 7 of 23 Page 8 of 23 Page 9 of 23 Page 10 of 23 Page 11 of 23 Page 12 of 23 Page 13 of 23 Page 14 of 23 Page
Page 1 of 23 Appendix 1 Page 2 of 23 Page 3 of 23 Page 4 of 23 Page 5 of 23 Page 6 of 23 Page 7 of 23 Page 8 of 23 Page 9 of 23 Page 10 of 23 Page 11 of 23 Page 12 of 23 Page 13 of 23 Page 14 of 23 Page
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
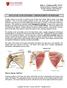 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
WESTERN ONTARIO ROTATOR CUFF INDEX (WORC)
 WESTERN ONTARIO ROTATOR CUFF INDEX (WORC) A disease-specific quality of life measurement tool for patients with rotator cuff disease Copyright 1998 (#474673) A. Kirkley MD, S. Griffin, CSS, C. Alvarez,
WESTERN ONTARIO ROTATOR CUFF INDEX (WORC) A disease-specific quality of life measurement tool for patients with rotator cuff disease Copyright 1998 (#474673) A. Kirkley MD, S. Griffin, CSS, C. Alvarez,
An Analysis of Shoulder Outcomes Scores in 275 Consecutive Patients: Disease-Specific Correlation Across Multiple Shoulder Conditions
 MILITARY MEDICINE, 177, 8:975, 2012 An Analysis of Shoulder Outcomes Scores in 275 Consecutive Patients: Disease-Specific Correlation Across Multiple Shoulder Conditions CDR Matthew T. Provencher, MC USN*;
MILITARY MEDICINE, 177, 8:975, 2012 An Analysis of Shoulder Outcomes Scores in 275 Consecutive Patients: Disease-Specific Correlation Across Multiple Shoulder Conditions CDR Matthew T. Provencher, MC USN*;
The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior Shoulder Instability
 Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
The impact of the Belgian workers compensation system on return to work after rotator cuff surgery
 Acta Orthop. Belg., 2010, 76, 592-597 ORIGINAL STUDY The impact of the Belgian workers compensation system on return to work after rotator cuff surgery Karolien DiDDEN, Geert LEiRs, Peter AERts From Mariaziekenhuis,
Acta Orthop. Belg., 2010, 76, 592-597 ORIGINAL STUDY The impact of the Belgian workers compensation system on return to work after rotator cuff surgery Karolien DiDDEN, Geert LEiRs, Peter AERts From Mariaziekenhuis,
Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair
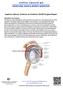 Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair Indications for Surgery The labrum is a fibrocartilaginous soft tissue that encircles the rim of the glenoid (socket of the shoulder). The
Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair Indications for Surgery The labrum is a fibrocartilaginous soft tissue that encircles the rim of the glenoid (socket of the shoulder). The
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai
 POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
Isolated electrothermal capsulorrhaphy in overhand athletes
 Isolated electrothermal capsulorrhaphy in overhand athletes Jerome G. Enad, MD, Neal S. ElAttrache, MD, James E. Tibone, MD, and Lewis A. Yocum, MD, Los Angeles, CA The purpose of this study was to determine
Isolated electrothermal capsulorrhaphy in overhand athletes Jerome G. Enad, MD, Neal S. ElAttrache, MD, James E. Tibone, MD, and Lewis A. Yocum, MD, Los Angeles, CA The purpose of this study was to determine
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
RESULTS. Three patients in the LB group and 4 patients in the EB group were lost to follow up, and these patients
 RESULTS Three patients in the LB group and 4 patients in the EB group were lost to follow up, and these patients were excluded from the analysis. Finally, 71 patients were included in the analysis (36
RESULTS Three patients in the LB group and 4 patients in the EB group were lost to follow up, and these patients were excluded from the analysis. Finally, 71 patients were included in the analysis (36
Posterior Shoulder Instability
 Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Intern Arthroscopy Course 2015 Shoulder Arthroscopy Cases
 Intern Arthroscopy Course 2015 Shoulder Arthroscopy Cases Mary Lloyd Ireland, M.D. University of Kentucky Dept. of Orthopaedic Surgery & Sports Medicine Lexington, KY Broken screw s/p Bristow procedure
Intern Arthroscopy Course 2015 Shoulder Arthroscopy Cases Mary Lloyd Ireland, M.D. University of Kentucky Dept. of Orthopaedic Surgery & Sports Medicine Lexington, KY Broken screw s/p Bristow procedure
Citation for published version (APA): Bruinsma, W. E. (2014). Classification and management of shoulder and elbow trauma
 UvA-DARE (Digital Academic Repository) Classification and management of shoulder and elbow trauma Bruinsma, W.E. Link to publication Citation for published version (APA): Bruinsma, W. E. (2014). Classification
UvA-DARE (Digital Academic Repository) Classification and management of shoulder and elbow trauma Bruinsma, W.E. Link to publication Citation for published version (APA): Bruinsma, W. E. (2014). Classification
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
S ORIGINAL ARTICLE Stiffness after arthroscopic shoulder surgery: incidence, management and classification
 Shoulder & Elbow. ISSN 1758-5732 S ORIGINAL ARTICLE Stiffness after arthroscopic shoulder surgery: incidence, management and classification Puneet Monga, Holly N. Raghallaigh & Lennard Funk Upper Limb
Shoulder & Elbow. ISSN 1758-5732 S ORIGINAL ARTICLE Stiffness after arthroscopic shoulder surgery: incidence, management and classification Puneet Monga, Holly N. Raghallaigh & Lennard Funk Upper Limb
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./0123
 ST Choi PYT Tse ORIGINAL ARTICLE Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./03 Objective. To review the outcomes of arthroscopic stabilisation
ST Choi PYT Tse ORIGINAL ARTICLE Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./03 Objective. To review the outcomes of arthroscopic stabilisation
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Case 1: Primary Dislocation. How I Manage Failed Instability Surgery. Case Presentations: Shoulder Instability
 Case Presentations: Shoulder Instability Chicago Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Case Presentations: Shoulder Instability Chicago Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Outcomes After Arthroscopic Bankart Repair in Adolescent Athletes Participating in Collision and Contact Sports
 Original Research Outcomes After Arthroscopic Bankart Repair in Adolescent Athletes Participating in Collision and Contact Sports Michael G. Saper,* DO, ATC, Charles Milchteim, MD, Robert L. Zondervan,
Original Research Outcomes After Arthroscopic Bankart Repair in Adolescent Athletes Participating in Collision and Contact Sports Michael G. Saper,* DO, ATC, Charles Milchteim, MD, Robert L. Zondervan,
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
EVALUATION OF ACUTE SHOULDER INJURIES. Douglas J. Moran, MD Orthopaedic Sports Medicine
 EVALUATION OF ACUTE SHOULDER INJURIES Douglas J. Moran, MD Orthopaedic Sports Medicine DISCLOSURES None of the planners or presenters of this session have disclosed any conflict or commercial interest
EVALUATION OF ACUTE SHOULDER INJURIES Douglas J. Moran, MD Orthopaedic Sports Medicine DISCLOSURES None of the planners or presenters of this session have disclosed any conflict or commercial interest
Glenohumeral Joint Instability: An Athlete s Perspective
 Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Shoulder Instability and Tendon Injuries
 Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012
 Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair
 Review Article Page 1 of 7 First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair Tanner Gurney-Dunlop, Ahmed Shawky Eid, Jason Old, James
Review Article Page 1 of 7 First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair Tanner Gurney-Dunlop, Ahmed Shawky Eid, Jason Old, James
Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Sports Medicine and Minimally Invasive (MGH & Shriners) Junior Residents
 Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Sports Medicine and Minimally Invasive (MGH & Shriners) Junior Residents The following document is intended to guide you in
Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Sports Medicine and Minimally Invasive (MGH & Shriners) Junior Residents The following document is intended to guide you in
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Sidus Stem-Free Shoulder. Secure fixation through a bone-sparing design
 Sidus Stem-Free Shoulder Secure fixation through a bone-sparing design An efficient, bone-sparing solution, should revision become necessary Humeral shaft is untouched, minimal bone is removed from the
Sidus Stem-Free Shoulder Secure fixation through a bone-sparing design An efficient, bone-sparing solution, should revision become necessary Humeral shaft is untouched, minimal bone is removed from the
Shoulder Stabilization in Athletes
 Shoulder Stabilization in Athletes When Can I Play Kevin E. Wilk, DPT, PT,FAPTA Kevin E Wilk, PT, DPT,FAPTA 2016 U of Colorado Sports Medicine Symposium Faculty Disclosure: Theralase Laser Medical Advisory
Shoulder Stabilization in Athletes When Can I Play Kevin E. Wilk, DPT, PT,FAPTA Kevin E Wilk, PT, DPT,FAPTA 2016 U of Colorado Sports Medicine Symposium Faculty Disclosure: Theralase Laser Medical Advisory
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
No Disclosures. The University of Michigan Rotator Cuff Registry: Lessons we have learned WHY I CHOSE TO STUDY ROTATOR CUFF DISEASE
 The University of Michigan Rotator Cuff Registry: Lessons we have learned Bruce S. Miller, MD, MS Department of Orthopaedic Surgery, University of Michigan No Disclosures WHY I CHOSE TO STUDY ROTATOR CUFF
The University of Michigan Rotator Cuff Registry: Lessons we have learned Bruce S. Miller, MD, MS Department of Orthopaedic Surgery, University of Michigan No Disclosures WHY I CHOSE TO STUDY ROTATOR CUFF
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Factors Associated With Work Ability in Patients Undergoing Surgery for Cervical Radiculopathy
 Factors Associated With Work Ability in Patients Undergoing Surgery for Cervical Radiculopathy Eunice Ng, Venerina Johnston, Johanna Wibault, Hakan Lofgren, Asa Dedering, Birgitta Öberg, Peter Zsigmond
Factors Associated With Work Ability in Patients Undergoing Surgery for Cervical Radiculopathy Eunice Ng, Venerina Johnston, Johanna Wibault, Hakan Lofgren, Asa Dedering, Birgitta Öberg, Peter Zsigmond
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F WAL-MART ASSOCIATES, INC. CLAIMS MANAGEMENT, INC. CARRIER
 BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F712377 WAYNE OWENS WAL-MART ASSOCIATES, INC. CLAIMS MANAGEMENT, INC. CARRIER CLAIMANT RESPONDENT RESPONDENT OPINION FILED DECEMBER 22, 2009
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F712377 WAYNE OWENS WAL-MART ASSOCIATES, INC. CLAIMS MANAGEMENT, INC. CARRIER CLAIMANT RESPONDENT RESPONDENT OPINION FILED DECEMBER 22, 2009
Rehabilitation Program for Rotator Cuff & Scapular Muscles
 Kansas City Sports Medicine Sports Medicine & Arthroscopy Olathe, KS Lansing, KS Kansas City, KS/MO Ph: 913-351-3005 Fax: 913-351-3009 Prem Parmar, M.D., F.R.C.S.(C) Sports Medicine and Arthroscopy Fellow
Kansas City Sports Medicine Sports Medicine & Arthroscopy Olathe, KS Lansing, KS Kansas City, KS/MO Ph: 913-351-3005 Fax: 913-351-3009 Prem Parmar, M.D., F.R.C.S.(C) Sports Medicine and Arthroscopy Fellow
No Financial Disclosures
 Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
An examination of bias in shoulder scoring instruments among healthy collegiate and recreational athletes
 An examination of bias in shoulder scoring instruments among healthy collegiate and recreational athletes Mark R. Brinker, MD, a,b,c Jeffrey S. Cuomo, MD, a George J. Popham, MD, a Daniel P. O Connor,
An examination of bias in shoulder scoring instruments among healthy collegiate and recreational athletes Mark R. Brinker, MD, a,b,c Jeffrey S. Cuomo, MD, a George J. Popham, MD, a Daniel P. O Connor,
