The VR1 Antagonist Capsazepine Reverses Mechanical Hyperalgesia in Models of Inflammatory and Neuropathic Pain
|
|
|
- Regina Adams
- 5 years ago
- Views:
Transcription
1 /03/ $7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 304, No. 1 Copyright 2003 by The American Society for Pharmacology and Experimental Therapeutics 42010/ JPET 304:56 62, 2003 Printed in U.S.A. The VR1 Antagonist Capsazepine Reverses Mechanical Hyperalgesia in Models of Inflammatory and Neuropathic Pain KATHARINE M. WALKER, 1 LASZLO URBAN, STEPHEN J. MEDHURST, 2 SADHANA PATEL, MOHANJIT PANESAR, ALYSON J. FOX, and PETER MCINTYRE Novartis Institute for Medical Sciences, London, United Kingdom Received July 19, 2002; accepted September 9, 2002 ABSTRACT Vanilloid receptor type 1 (VR1) (TRPV1) is a ligand-gated ion channel expressed on sensory nerves that responds to noxious heat, protons, and chemical stimuli such as capsaicin. Herein, we have examined the activity of the VR1 antagonist capsazepine in models of inflammatory and neuropathic pain in the rat, mouse, and guinea pig. In naïve animals, subcutaneous administration of capsazepine ( mg/kg s.c.) did not affect withdrawal thresholds to noxious thermal or mechanical stimuli. However, pretreatment with capsazepine prevented the development of mechanical hyperalgesia induced by intraplantar injection of capsaicin, with a similar potency in all three species. Capsazepine (up to 100 mg/kg s.c.) did not affect mechanical hyperalgesia in the Freund s complete adjuvant (FCA)-inflamed hind paw of the rat or mouse. Strikingly, capsazepine (3 30 The vanilloid receptor type 1 (VR1) is a pivotal molecular integrator of noxious stimuli that is expressed on somatic and autonomic primary afferent neurons. VR1 has been confirmed as a ligand-gated ion channel after its cloning from rat (Caterina et al., 1997) and human (Hayes et al., 2000; McIntyre et al., 2001). In vitro studies using recombinant VR1 have shown that, like the native vanilloid receptor, it can be activated by a variety of plant-derived compounds, including capsaicin, a pungent component from chili peppers, and resiniferatoxin (Szallasi and Blumberg, 1999), as well as noxious heat (Caterina et al., 1997), low ph (Tominaga et al., 1998), and some lipid mediators such as anandamide (Smart et al., 2000) and the lipoxygenase product 12-(S) hydroxyeicosatetraenoic acid (Hwang et al., 2000). The experiments in this manuscript have previously been reported in abstract form at the 2001 meeting of the Society for Neuroscience (Walker K, Gentry C, Medhurst S, Patel S, Panesar M, Urban L, and McIntyre P (2001) Capsazepine shows species selective antihyperalgesic effects in models of chronic inflammatory and neuropathic pain. Soc Neurosci Abst 31:926.7). 1 Current address: Purdue Pharma, 6 Cedar Brooke Dr., Cranbury, NJ Current address: GlaxoSmithKline Pharmaceuticals Ltd., Harlow, UK. Article, publication date, and citation information can be found at DOI: /jpet mg/kg s.c.) produced up to 44% reversal of FCA-induced mechanical hyperalgesia in the guinea pig. Capsazepine also produced significant reversal of carageenan-induced thermal hyperalgesia in the guinea pig at 30 mg/kg s.c., but was ineffective in the rat. Similarly, in the partial sciatic nerve ligation model of neuropathic pain, capsazepine was surprisingly effective in the guinea pig, producing up to 80% reversal of mechanical hyperalgesia (1 30 mg/kg s.c.) but had no effect in the rat or mouse. These data show that VR1 antagonists have antihyperalgesic activity in animal models of chronic inflammatory and neuropathic pain, and illustrate species differences in the in vivo pharmacology of VR1 that correlate with differences in pharmacology previously seen in vitro. Capsazepine is a VR1 antagonist that has been shown to competitively inhibit capsaicin-mediated responses in isolated dorsal root ganglion (DRG) neurons (Bevan et al., 1992a) or tissues from rat (Bevan et al., 1992b; Maggi et al., 1993; Jerman et al., 2000), mouse (Urban and Dray, 1991), and guinea pig (Lou and Lundberg, 1992; Ellis and Undem, 1994; Fox et al., 1995). In vivo, capsazepine has also been shown to inhibit the nocifensive responses to capsaicin in mice and rats (Santos and Calixto, 1997), as well as capsaicin-induced bronchoconstriction or cough in the guinea pig (Satoh et al., 1993; Lalloo et al., 1995). However, early studies investigating the potential antihyperalgesic effects of capsazepine in rat models of acute and chronic pain led to the idea that capsaicin antagonists would be unlikely to be useful as analgesics (Perkins and Campbell, 1992). Nevertheless, other studies using capsazepine indicated possible species differences in the pharmacology of the vanilloid receptor. For example, although low ph solutions were shown to mimic the effect of capsaicin in several species, capsazepine inhibited low ph-evoked depolarization of sensory nerves in guinea pig airways (Lou and Lundberg, 1992; Satoh et al., 1993; Fox et al., 1995), but not in rat DRG neurons (Bevan et al., 1992b; Habelt et al., 2000). More recently, studies in our group ABBREVIATIONS: VR1, vanilloid receptor 1, TRPV1; DRG, dorsal root ganglion; FCA, Freund s complete adjuvant; ANOVA, analysis of variance; HSD, honestly significant difference. 56
2 VR1 Antagonist in Models of Inflammatory and Neuropathic Pain 57 using recombinant VR1 have also demonstrated clear species selectivity in the activity of capsazepine. Thus, we have found that capsazepine inhibited responses to noxious heat and protons, as well as capsaicin, at the cloned human or the cloned guinea pig VR1 expressed in Chinese hamster ovary cells, whereas at the rat VR1, it inhibited responses to capsaicin but not to low ph (McIntyre et al., 2001; Savidge et al., 2002). The accumulating evidence for the activation of VR1 by several stimuli, together with the demonstration of species differences in the pharmacology has prompted us to reevaluate the activity of capsazepine in animal models of pain. Herein, we examine the effects of capsazepine in guinea pig, rat, and mouse models of persistent inflammatory and chronic neuropathic pain. Materials and Methods Compounds and Administration Procedures. Capsazepine (Tocris Cookson, Bristol, UK), Diclofenac and carbamazepine (Sigma Chemical, Poole, Dorset, UK) were administered subcutaneously in 20% dimethyl sulfoxide/1% ethanol/1% Tween 80/78% saline in a volume of 0.5 ml, and morphine sulfate was administered subcutaneously in saline. Carbamazepine was administered orally in 0.5% methylcellulose. Capsaicin (Tocris Cookson) was dissolved in dimethyl sulfoxide to a stock solution of 10 mm with dilutions in saline and administered into the plantar region of the hind paw in a volume of 10 l. Compounds where tested under blind experimental conditions. Carageenan and Freund s complete adjuvant (FCA) were obtained from Sigma Chemical. Animals. Male Wistar rats ( g), C57/BL mice (25 30 g), and Dunkin-Hartley guinea pigs ( g) were housed in groups of six and had free access to food and water at all times. All experiments were carried out according to the Declaration of Helsinki and the UK Animals (Scientific Procedures) Act 1986 and associated guidelines, with approval from the Novartis Animal Welfare and Ethics Committee. For comparison with compound-treated groups, animals treated with the appropriate drug vehicle were included in each experiment. The volume of administration was identical for vehicle- and compound-treated rats. Vehicle-treated rats were identical to compound-treated rats with respect to all other experimental procedures. Capsaicin-Induced Hyperalgesia. Many studies have demonstrated a dose-dependent sensitization to mechanical stimulation and the development of mechanical hyperalgesia after intradermal injections of capsaicin in human (Simone et al., 1989; LaMotte et al., 1992) and rodent pain assays (Gilchrist et al., 1996). Herein, capsaicin-induced mechanical hyperalgesia was assessed in rats, mice, and guinea pigs by measuring hind paw withdrawal thresholds to an increasing pressure stimulus using an analgesymeter (7200; Ugo Basile, Comerio, Italy) with a wedge-shaped probe (area 1.75 mm 2 ). The cut-off was set at 250 g and the endpoint was taken as paw withdrawal or vocalization. In preliminary experiments, paw withdrawal thresholds were measured before and up to 30 min after an intraplantar injection of 1, 10, or 100 nmol of capsaicin into one hind paw. These experiments showed that 10 nmol of capsaicin produced a submaximal, reproducible mechanical hyperalgesia in all three species, and this dose was used for further studies. To examine the inhibition of capsaicin-induced hyperalgesia, capsazepine ( mg/kg) or vehicle was administered s.c. 30 min before capsaicin injection, and withdrawal thresholds were then measured 30 min after capsaicin injection. Percentage of inhibition of development of capsaicin-induced hyperalgesia was calculated according to the following formula: % inhibition (naive vehicle postcaps vehicle) (naive CPZ postcaps CPZ) (naive vehicle postcaps vehicle) 100% where CAPS refers to capsaicin administration and CPZ refers to capsazepine administration. Inflammatory Hyperalgesia. Mechanical hyperalgesia was examined in a model of inflammatory pain in the rat, mouse, and guinea pig using the paw pressure technique as described above. Paw withdrawal thresholds were measured in naive animals before an intraplantar injection of FCA (25 l; Sigma Chemical) into one hind paw. Withdrawal thresholds were then measured 24 h later, before (predose) and up to 6 h after drug or vehicle administration (postdose). The nonsteroidal, anti-inflammatory drug diclofenac was used as a positive control in all experiments. Reversal of mechanical hyperalgesia was calculated according to the following formula: postdose threshold predose threshold % reversal naive threshold predose threshold 100% Carageenan (Sigma Chemical)-induced thermal hyperalgesia was assessed in all three species using a Plantar Test Apparatus (Ugo Basile). During tests rats, mice or guinea pigs were placed individually and unrestrained in cm (length width height) Perspex boxes situated on a glass platform. Withdrawal latencies to an infrared source positioned underneath the mid-plantar hind paw were measured using a digital timer that stopped automatically upon paw withdrawal with an accuracy of 0.1 s. Withdrawal latencies were measured with a beam intensity of 22.9 for rats and mice and 50 for guinea pigs, with a cut-off of 32 s. Measurements were made twice on each paw, and the mean of the readings was used for data analysis. Latencies were determined in naive animals and then 24 h after carrageenan injection before (predose) and at 1 and 3 h after capsazepine or vehicle administration. Morphine was used as a positive control in all experiments. Neuropathic Hyperalgesia. Mechanical hyperalgesia was examined in a model of neuropathic pain induced by partial ligation of the sciatic nerve, in the rat, mouse, and guinea pig. Briefly, animals were anesthetized, the left sciatic nerve exposed at mid-thigh level through a small incision, and one-third to one-half of the nerve thickness was tightly ligated with a 7.0 silk ligature. The wound was closed with a single muscle suture and skin clips and the animals allowed to recover for 11 to 15 days postligation. Withdrawal thresholds were measured on both the ipsilateral and the contralateral hind paws before (predose) and up to 6 h after drug or vehicle administration. The antiepileptic drug carbamazepine (30 mg/kg p.o.) was used as a positive control. We have previously determined that partial nerve ligation does not affect contralateral withdrawal thresholds and that sham surgery does not affect ipsilateral thresholds. Reversal of hyperalgesia was therefore calculated according to the following formula that uses the contralateral paw as a reference rather than using additional groups of naïve or sham animals: % reversal ipsilateral threshold postdose ipsilateral threshold predose contralateral threshold predose ipsilateral threshold predose 100% Statistical Analyses. For all experiments, data analyses were performed on the untransformed paw withdrawal threshold or latency data by ANOVA with repeated measures, followed by Tukey s HSD post hoc analysis. Results Capsacin-Induced Mechanical Hyperalgesia. Intraplantar injection of capsaicin (1 100 nmol) produced a rapid, dose-dependent mechanical hyperalgesia indicated by a decrease in paw withdrawal thresholds in mice, rats, and guinea pigs, which was maximal 30 min after injection (Fig. 1A). From this experiment, a dose of 10 nmol of capsaicin was
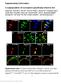
3 58 Walker et al. Fig. 1. Effect of capsazepine against capsaicin-induced hyperalgesia. A, intraplantar injection of capsaicin produced a dose-dependent mechanical hyperalgesia in rats, mice, and guinea pigs. Each point represents the mean S.E.M. paw withdrawal threshold from six animals, measured 30 min after injection of vehicle or capsaicin. B, subcutaneous administration of capsazpine 30 min before intraplantar capsaicin (10 nmol) injection inhibited the capsaicininduced hyperalgesia in rats, mice, and guinea pigs. Paw withdrawal thresholds were measured 30 min after capsaicin administration. Data are presented as percentage of inhibition of capsaicin-induced hyperalgesia from six animals per group. In A and B,, P 0.05 compared with vehicle by ANOVA followed by Tukey s HSD test carried out on threshold data. selected to investigate the effects of capsazepine. Administration of capsazepine ( mg/kg s.c.) 30 min before capsaicin injection prevented development of capsaicin-induced mechanical hyperalgesia in a dose-dependent manner, with similar potency in rats, mice, and guinea pigs (Fig. 1B). Inflammatory Hyperalgesia. FCA injection produced a pronounced mechanical hyperalgesia in all three species, with ipsilateral paw withdrawal thresholds in naive animals of approximately 100 g reduced to 55 to 65 g 24 h after treatment (data not shown). Capsazepine (3 30 mg/kg s.c.) produced a marked reversal of inflammatory mechanical hyperalgesia in the guinea pig, with a maximal 44% reversal observed 1 h after administration (Fig. 2A). The efficacy of capsazepine was comparable with that of the nonsteroidal anti-inflammatory drug diclofenac, which produced up to 48% reversal of hyperalgesia, although the effect of capsazepine was more short-lived, with a loss of antihyperalgesic activity by 3 h postadministration. In contrast, capsazepine administered at doses up to 100 mg/kg did not affect mechanical hyperalgesia in rats or mice (Fig. 2B), although diclofenac (30 mg/kg s.c.) administered as a positive control in the same experiments produced 51 and
4 VR1 Antagonist in Models of Inflammatory and Neuropathic Pain 59 Fig. 2. Activity of capsazepine against FCA-induced inflammatory mechanical hyperalgesia. A, administration of capsazepine or diclofenac 24 h after FCA treatment significantly reversed mechanical hyperalgesia in the guinea pig. Ipsilateral and contralateral paw withdrawal thresholds were measured before (predose) and up to 3 h after vehicle or drug administration. B, capsazepine did not affect FCA-induced mechanical hyperalgesia in the rat or mouse. Data are presented as percentage of reversal of hyperalgesia measured 1 h after capsazepine administration. In A and B, each point represents mean S.E.M. from six animals per group., P 0.05 compared with vehicle by ANOVA followed by Tukey s HSD test. 40% reversal in rats and mice, respectively (data not shown). There was no effect of capsazepine on contralateral paw withdrawal thresholds to mechanical stimulation in any of the species, and no other overt behavioral effects, such as motor defects or sedation, were observed. Carrageenan injection into the hind paw produced thermal hyperalgesia in rats and guinea pigs (Urban et al., 2000) that was maximal 24 h after treatment. Capsazepine did not affect established inflammatory thermal hyperalgesia in rats (data not shown) but did reverse thermal hyperalgesia in the guinea pig model producing a maximal reversal of 54% at the highest dose tested (30 mg/kg), compared with a near complete reversal by a relatively high dose of morphine (10 mg/kg) (Fig. 3). Additionally, there was no significant effect on contralateral withdrawal latencies (data not shown). Neuropathic Hyperalgesia. After partial sciatic nerve ligation in rats, guinea pigs, and mice, ipsilateral paws exhibited marked mechanical hyperalgesia, with paw withdrawal thresholds averaging approximately 60 g compared with contralateral thresholds of approximately 100 g. Capsazepine (3 30 mg/kg s.c.) produced a doserelated reversal of mechanical hyperalgesia in the guinea pig. This effect was rapid in onset, with a maximal 80% reversal seen 30 min after administration, and was absent by 3 h postdose (Fig. 4A). There were no significant changes in contralateral paw withdrawal thresholds up to 3 h after capsazepine administration. The anticonvulsant carbamazepine was less efficacious than capsazepine in this experiment, producing approximately 40% reversal of hyperalgesia 3 h after administration. As observed with the inflammatory model, capsazepine did not affect ipsilateral (Fig. 4B) or contralateral (data not shown) paw withdrawal thresholds in neuropathic rats or mice at doses up to 30 mg/kg.
5 60 Walker et al. Fig. 3. Capsazpeine and morphine dose-response curves against inflammatory thermal hyperalgesia in the guinea pig. Withdrawal latencies to a noxious thermal stimulus applied to the plantar surface of the ipsilateral paw were measured in guinea pigs before (naive) and 24 h after carageenan treatment (predose), and then 1 h after vehicle or capsazepine administration. Each point represents mean S.E.M. from six animals., P 0.05 compared with vehicle. Discussion We have studied the potential role of VR1 in chronic pain conditions by examining the antihyperalgesic activity of the VR1 antagonist capsazepine in models of persistent neuropathic and inflammatory pain. Experiments were carried out in rats, mice, and guinea pigs test the species selectivity of capsazepine indicated by in vitro studies (Savidge et al., 2002). As expected, capsazepine acts as an antagonist of capsaicin-induced mechanical hyperalgesia over the same dose range in the three species tested (Fig. 1). However, the most striking finding of this study is that capsazepine produces effective reversal of mechanical hyperalgesia associated with partial sciatic nerve ligation (Fig. 4) and both mechanical and thermal hyperalgesia associated with hind paw inflammation in the guinea pig (Figs. 2 and 3). The antihyperalgesic effects of capsazepine in the guinea pig models of persistent inflammatory and neuropathic pain were produced over the same dose range that inhibited the development of capsaicin-induced hyperalgesia and is, therefore, consistent with its VR1 receptor antagonist activity. Paw withdrawal thresholds from the noninjured contralateral paw were not altered after capsazepine administration, indicating that the antihyperalgesic effects of capsazepine in the guinea pig were restricted to hyperalgesia associated with inflammation or nerve injury, rather than reflecting an acute analgesic activity. The antihyperalgesic activity of capsazepine observed in guinea pigs is in marked contrast to its lack of effect in mice and rats, where no antihyperalgesic activity was observed in either the neuropathic (Fig. 4B) or inflammatory models (Fig. 2B). This is in agreement with the findings of Perkins and Campbell (1992) who found that capsazepine administered alone did not have antinociceptive activity in several models of acute and chronic pain in rats (tail-flick, hot-plate, and carrageenan-induced inflammatory mechanical hyperalgesia). In contrast to these findings, other groups have reported Fig. 4. Activity of capsazepine against neuropathic mechanical hyperalgesia. A, administration of capsazepine (3, 10, and 30 mg/kg s.c.) significantly reversed mechanical hyperalgesia induced by partial sciatic nerve ligation in the guinea pig at 15, 30, and 60 min after administration. Carbamazepine also significantly reversed neuropathic mechanical hyperalgesia (30 mg/kg p.o.) 3 h after administration. Ipsilateral and contralateral paw withdrawal thresholds were measured before (predose) and 15 min to 3 h after vehicle or drug administration. B, capsazepine did not affect neuropathic hyperalgesia in the rat or mouse, whereas the control compound, carbamazepine, was effective in all species. Data are presented as percentage of reversal of hyperalgesia measured 30 min after capsazepine administration. In A and B, each point represents mean S.E.M. from six animals per group., P 0.05 compared with vehicle by ANOVA followed by Tukey s HSD test. that capsazepine prevents the early phase of formalin-induced mechanical hyperalgesia when administered intradermally in rats (Kwak et al., 1998) or mice (Santos and Calixto, 1997) and inhibits carageenan-induced inflammatory hyperalgesia in the rat (Kwak et al., 1998). However, in both these studies, extremely high concentrations of capsazepine ( 10 M) were injected directly into the paw, which may have resulted in nonspecific actions of capsazepine on other ion channels (Docherty et al., 1997; Liu and Simon, 1997). Interestingly, normal mice and mice lacking VR1 show comparable behavioral responses to formalin injection (Caterina et al., 2000), showing that VR1 activation is not essential for the formalin response. The observation of species differences in the in vivo antihyperalgesic activity of capsazepine between guinea pig and rodents is consistent with previous in vitro and in vivo findings. As discussed in the Introduction, capsazepine is a potent antagonist of capsaicin effects in a variety of in vitro and in vivo assays in rats, mice, and guinea pigs. However, there are clear differences in the activity of capsazepine against other VR1 stimuli. Thus, it blocks responses of native VR1 to
6 VR1 Antagonist in Models of Inflammatory and Neuropathic Pain 61 low ph in the guinea pig airways (Satoh et al., 1993; Fox et al., 1995; Lalloo et al., 1995), as well responses of both guinea pig and human VR1 to low ph and noxious heat (McIntyre et al., 2001; Savidge et al., 2002). In contrast, capsazepine does not affect responses of rat DRG neurons to low ph (Bevan et al., 1992b) or of the recombinant rat VR1 to low ph or heat (McIntyre et al., 2001; Savidge et al., 2002). The present findings therefore support the apparent species differences in the responses of VR1 uncovered by capsazepine, and further suggest that compounds that can block capsaicin, low ph and heat stimulation of human VR1, will be antihyperalgesic in humans. Capsazepine was found to be weakly active against thermal hyperalgesia in guinea pigs (Fig. 3). This activity is in agreement with the role of VR1 in thermal hyperalgesia observed in studies of VR1 knockout mice. Thus, VR1 null mice show marked deficits to noxious thermal stimuli (Caterina et al., 2000) and a complete absence of carrageenaninduced thermal hyperalgesia (Davis et al., 2000). However, the hyperalgesic effects of heat cannot be explained by the action of VR1 alone, because mice lacking VR1 retain normal sensation of noxious heat (Caterina et al., 2000; Davis et al., 2000), suggesting the involvement of additional thermal receptors. In keeping with this hypothesis two VR1 homologues, VRL-1 (TRPV2) and TRPV3, have been reported to be insensitive to capsaicin or protons but respond to either highor low-threshold heat stimulation and neither is blocked by capsazepine (Caterina et al., 1999; Peier et al., 2002). The finding that capsazepine inhibits both thermal and mechanical hyperalgesia in guinea pig models of inflammatory and chronic pain was unexpected. Although no direct link between mechanical stimulation and VR1 activation has previously been demonstrated, stimuli that activate VR1 have been shown to induce mechanical hypersensitivity. It is known that activation of the VR1 by capsaicin causes both thermal and mechanical hyperalgesia in rat, primate, and human subjects (Simone et al., 1988; LaMotte et al., 1991; Torebjork et al., 1992). In fact, the mechanical hyperalgesia observed after capsaicin injection is more robust than the thermal hyperalgesia both in terms of duration of action and the size of the area of secondary hyperalgesia (Gilchrist et al., 1996). It has been shown that an intradermal capsaicin injection facilitates the responses of dorsal horn neurons due to input of low-threshold mechanoreceptors and nociceptors (LaMotte et al., 1991; Simone et al., 1991;). Thus, in inflamed tissue, local ph decreases may ultimately activate VR1, sensitizing nociceptors and low-threshold mechanoreceptors, decreasing the threshold at which mechanical stimuli result in the detection of noxious stimuli. A role for VR1 in neuropathic and inflammatory pain is supported by several recent studies indicating that VR1 is up-regulated in both inflammatory and neuropathic conditions. Peripheral inflammation has been shown to increase the sensitivity of isolated DRG to capsaicin (Nicholas et al., 1999). Moreover, VR1 can be sensitized or activated by molecules such as prostaglandin E 2 and bradykinin (Vyklicky et al., 1998), which are present in inflamed tissues and activation of PKC can either directly activate (Premkumar and Ahern, 2000) or sensitize (Vellani et al., 2001) VR1. After peripheral nerve injury VR1 protein is up-regulated in undamaged neurons and down-regulated in damaged neurons (Hudson et al., 2001). Taken together, these studies show that the expression and function of VR1 are regulated under conditions of altered noxious sensory input, which may explain why VR1 blockers can affect the sensation of noxious stimuli under pathophysiological, but not under normal conditions. It is not clear why capsazepine was more effective in blocking the mechanical hyperalgesia associated with nerve injury (Fig. 4) than inflammation (Fig. 2) in the guinea pig. Perhaps it has to do with different levels of VR1 up-regulation or sensitization in these two conditions. The ability of capsazepine to reduce mechanical hyperalgesia after partial ligation of the guinea pig sciatic nerve may be attributed in part to altered expression of VR1. Partial ligation of rat sciatic nerve results in decreased VR1 immunoreactivity in damaged (ligated) neurons, but increased VR1 immunoreactivity in undamaged neurons (Hudson et al., 2001). It is interesting that the increased VR1 immunoreactivity was present not only in C fibers in the L5 DRG but also in myelinated A fibers (Hudson et al., 2001), which provides evidence for the involvement of VR1 in mechanical sensitivity after nerve injury and supplies a rationale for why a VR1 antagonist is effective in reversing the pain behavior associated with mechanical hyperalgesia. The increased levels of VR1 may then also prime the sensory neurons to respond to other physiological consequences of nerve damage that occur postinjury, such as the release of inflammatory mediators from macrophages during Wallerian degeneration (Syriatowicz et al., 1999). The discovery of a role for VR1 in models of persistent and chronic pain may have been delayed by the fact that previous studies investigating capsazepine s effects were only carried out in rat or mouse models of chronic pain. In this study, we provide evidence that capsazepine is an effective antihyperalgesic in guinea pig models of chronic pain and that this correlates with the effectiveness of this compound in blocking VR1 activation by low ph and capsaicin (Savidge et al., 2002). In contrast, capsazepine does not reverse chronic pain in rats and mice, where it blocks only capsaicin-induced VR1 activation. These data therefore suggest that the antinociceptive effects of VR1 antagonists are predicted by their ability to block noxious heat- and proton- as well as capsaicin-induced activation of VR1 and provide evidence for a potential therapeutic benefit of VR1 antagonists in the treatment of chronic neuropathic and inflammatory pain conditions. Acknowledgments We thank Stuart Bevan for critically reading the manuscript. References Bevan S, Hothi S, Hughes G, James IF, Rang HP, Shah K, Walpole CS, and Yeats JC (1992a) Capsazepine: a competitive antagonist of the sensory neurone excitant capsaicin. Br J Pharmacol 107: Bevan S, Rang HP, and Shah K (1992b) Capsazepine does not block the protoninduced activation of rat sensory neurones. Br J Pharmacol 107:235P. Caterina MJ, Leffler A, Malmberg AB, Martin WJ, Trafton J, Petersen-Zeitz KR, Koltzenburg M, Basbaum AI, and Julius D (2000) Impaired nociception and pain in mice lacking the capsaicin receptor. Nature (Lond) 288: Caterina MJ, Rosen TA, Tominaga M, Brake AJ, and Julius D (1999) A capsaicin receptor homologue with a high threshold for noxious heat. Nature (Lond) 398: Caterina MJ, Schumacher MA, Tominaga M, Rosen TA, Levine JD, and Julius D (1997) The capsaicin receptor: a heat-activated ion channel in the pain pathway. Nature (Lond) 389: Davis JB, Gray J, Gunthorpe MJ, Hatcher JP, Davey PT, Overend P, Harries MH, Latcham J, Clapham C, Atkinson K, Hughes SA, et al. (2000) Vanilloid receptor-1 is essential for inflammatory thermal hyperalgesia. Nature (Lond) 405: Docherty RJ, Yeats JC, and Piper AS (1997) Capsazepine block of voltage-activated
7 62 Walker et al. calcium channels in adult rat dorsal root ganglion neurons in culture. Br J Pharmacol 121: Ellis JL and Undem BJ (1994) Inhibition by capsazepine of resiniferatoxin- and capsaicin-induced contractions of guinea-pig trachea. J Pharmacol Exp Ther 268: Fox AJ, Urban L, Barnes PJ, and Dray A (1995) Effects of capsazepine against capsaicin- and proton-evoked excitation of single airway C-fibres and vagus nerve from the guinea-pig. Neuroscience 67: Gilchrist HD, Allard BL, and Simone DA (1996) Enhanced withdrawal responses to heat and mechanical stimuli following intraplantar injection of capsaicin in rats. Pain 67: Habelt C, Kessler F, Distler C, Kress M, and Reeh PW (2000) Interactions of inflammatory mediators and low ph not influenced by capsazepine in rat cutaneous nociceptors. Neuroreport 11: Hayes P, Meadows HJ, Gunthorpe MJ, Harries MH, Duckworth DM, Cairns W, Harrison DC, Clarke CE, Ellington K, Prinjha RK, et al. (2000) Cloning and functional expression of a human orthologue of rat vanilloid receptor-1. Pain 88: Hudson LJ, Bevan S, Wotherspoon G, Gentry C, Fox A, and Winter J (2001) VR1 protein expression increases in undamaged DRG neurons after partial nerve injury. Eur J Neurosci 13: Hwang SW, Kwak JY, Lee S-L, Kang C-J, Jung J, Cho S, Min KH, Suh YG, Kim D and Oh U (2000) Direct activation of capsaicin receptors by products of lipoxygenases: endogenous capsaicin-like substances. Proc Natl Acad Sci USA 97: Jerman JC, Brough SJ, Prinjha R, Harries MH, Davis JB, and Smart D (2000) Characterization using FLIPR of rat vanilloid receptor (rvr1) pharmacology. Br J Pharmacol 130: Kwak JY, Jung JY, Hwang SW, Lee WT, and Oh U (1998) A capsaicin-receptor antagonist, capsazepine, reduces inflammation-induced hyperalgesic responses in the rat: evidence for an endogenous capsaicin-like substance. Neurosci 86: Lalloo UG, Fox AJ, Belvisi MG, Chung KF, and Barnes PJ (1995) Capsazepine inhibits cough induced by capsaicin and citric acid but not by hypertonic saline in guinea-pigs. J Appl Physiol 79: LaMotte RH, Lundberg LE, and Torebjork HE (1992) Pain, hyperalgesia and activity in nociceptive C units in humans after intradermal injection of capsaicin. J Physiol (Lond) 448: LaMotte RH, Shain CN, Simone DA, and Tsai EFP (1991) Neurogenic hyperalgesia: psychophysical studies of underlying mechanisms. J Neurophysiol 66: Liu L and Simon SA (1997) Capsazepine, a vanilloid receptor antagonist, inhibits nicotinic acetylcholine receptors in rat trigeminal ganglia. Neurosci Lett 228: Lou YP and Lundberg JM (1992) Inhibition of low ph evoked activation of airway sensory nerves by capsazepine, a novel capsaicin-receptor antagonist. Biochem Biophys Res Commun 189: Maggi CA, Bevan S, Walpole CS, Rang HP, and Giuliani S (1993) A comparison of capsazepine and ruthenium red as capsaicin antagonists in the rat isolated urinary bladder and vas deferens. Br J Pharmacol 108: McIntyre P McLatchie L, Chambers A, Phillips E, Clarke M, Savidge J, Toms C, Peacock M, Shah K, Winter J, et al. (2001) Pharmacological differences between the human and rat vanilloid receptor 1 (VR1). Br J Pharmacol 132: Nicholas RS, Winter J, Wren P, Bergmann R, and Woolf CJ (1999) Peripheral inflammation increases the capsaicin sensitivity of dorsal root ganglion neurons in a nerve growth factor-dependent manner. Neuroscience 91: Peier AM, Reeve AJ, Andersson DA, Moqrich A, Earley TJ, Hergarden AC, Story GC, Colley S, Hogenesch JB, McIntyre P, et al. (2002) A Heat-sensitive TRP channel expressed in keratinocytes. Science (Wash DC) 296: Perkins MN and Campbell EA (1992) Capsazepine reversal of the antinociceptive action of capsaicin in vivo. Br J Pharmacol 107: Premkumar LS and Ahern GP (2000) Induction of vanilloid receptor channel activity by protein kinase C. Nature (Lond) 408: Santos AR and Calixto JB (1997) Ruthenium red and capsazepine antinociceptive effect in formalin and capsaicin models of pain in mice. Neurosci Lett 235: Satoh H, Lou YP, and Lundberg JM (1993) Inhibitory effects of capsazepine and SR on citric acid-induced bronchoconstriction in guinea-pigs. Eur J Pharmacol 236: Savidge J, Davis C, Shah K, Colley S, Phillips E, Ranasinghe S, Winter J, Kotsonis P, Rang H, and McIntyre P (2002) Cloning and functional characterization of the guinea-pig vanilloid receptor 1. Neuropharmacology 43: Simone DA, Baumann TK, and LaMotte RH (1989) Dose-dependent pain and mechanical hyperalgesia in humans after intradermal injection of capsaicin. Pain 38: Simone DA, Sorkin LS, Oh U, Chung JM, Owens C, LaMotte RH, and Willis WD (1991) Neurogenic hyperalgesia: central neural correlates in response of spinothalamic tract neurons. J Neurophysiol 66: Smart D, Gunthorpe MJ, Jerman JC, Nasir S, Gray J, Muir AI, Chambers JK, Randall AD, and Davis JB (2000) The endogenous lipid anandamide is a full agonist at the human vanilloid receptor (hvr1). Br J Pharmacol 129: Syriatowicz JP, Hu D, Walker JS, and Tracey DJ (1999) Hyperalgesia due to nerve injury: role of prostaglandins. Neuroscience 94: Szallasi A and Blumberg PM (1999) Vanilloid (capsaicin) receptors and mechanisms. Pharmacol Rev 51: Tominaga M, Caterina MJ, Malmberg AB, Rosen TA, Gilbert H, Skinner K, Raumann BE, Basbaum AI, and Julius D (1998) The cloned capsaicin receptor integrates multiple pain-producing stimuli. Neuron 21: Torebjork HE, Lundberg JM, and LaMotte RH (1992) Central changes in processing of mechanoreceptive input in capsaicin-induced secondary hyperalgesia in humans. J Physiol (Lond) 448: Urban L, Campbell EA, Gentry C, Patel S, Chaudry N, and James I (2000) Pharmacological profile of SDZ , a novel capsaicin agonist. Pain 89: Urban L and Dray A (1991) Capsazepine, a novel capsaicin antagonist, selectively antagonises the effects of capsaicin in the mouse spinal cord in vitro. Neurosci Lett 134:9 11. Vellani V, Mapplebeck S, Moriondo A, Davis JB, and McNaughton PA (2001) Protein kinase C activation potentiates gating of the vanilloid receptor VR1 by capsaicin, protons, heat and anandamide. J Physiol (Lond) 534: Vyklicky L, Knotkova-Urbancova H, Vitaskova Z, Vlachova V, Kress M, and Reeh PW (1998) Inflammatory mediators at acidic ph activate capsaicin receptors in cultured sensory neurons from newborn rats. J Neurophysiol 79: Address correspondence to: Dr. Peter McIntyre, Molecular Biology Laboratory, Novartis Institute for Medical Sciences, 5 Gower Place, London WC1E 6BN, UK. peter.mcintyre@pharma.novartis.com
JAMES D. POMONIS, JAMES E. HARRISON, LILLY MARK, DAVID R. BRISTOL, KENNETH J. VALENZANO, and KATHARINE WALKER
 0022-3565/03/3061-387 393$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 306, No. 1 Copyright 2003 by The American Society for Pharmacology and Experimental Therapeutics 46268/1076303
0022-3565/03/3061-387 393$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 306, No. 1 Copyright 2003 by The American Society for Pharmacology and Experimental Therapeutics 46268/1076303
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (12), Page
 The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (12), Page 2172-2177 Blockage of HCN Channels with ZD7288 Attenuates Mechanical Hypersensitivity in Rats Model of Diabetic Neuropathy Hussain
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (12), Page 2172-2177 Blockage of HCN Channels with ZD7288 Attenuates Mechanical Hypersensitivity in Rats Model of Diabetic Neuropathy Hussain
NMDA-Receptor Antagonists and Opioid Receptor Interactions as Related to Analgesia and Tolerance
 Vol. 19 No. 1(Suppl.) January 2000 Journal of Pain and Symptom Management S7 Proceedings Supplement NDMA-Receptor Antagonists: Evolving Role in Analgesia NMDA-Receptor Antagonists and Opioid Receptor Interactions
Vol. 19 No. 1(Suppl.) January 2000 Journal of Pain and Symptom Management S7 Proceedings Supplement NDMA-Receptor Antagonists: Evolving Role in Analgesia NMDA-Receptor Antagonists and Opioid Receptor Interactions
Enhanced formalin nociceptive responses following L5 nerve ligation in the rat reveals neuropathy-induced inflammatory hyperalgesia
 University of Kentucky From the SelectedWorks of Renee R. Donahue 2001 Enhanced formalin nociceptive responses following L5 nerve ligation in the rat reveals neuropathy-induced inflammatory hyperalgesia
University of Kentucky From the SelectedWorks of Renee R. Donahue 2001 Enhanced formalin nociceptive responses following L5 nerve ligation in the rat reveals neuropathy-induced inflammatory hyperalgesia
Potential for delta opioid receptor agonists as analgesics in chronic pain therapy
 Potential for delta opioid receptor agonists as analgesics in chronic pain therapy David Kendall & Bengt von Mentzer; PharmNovo AB/UK Alex Conibear & Eamonn Kelly, University of Bristol Junaid Asghar,
Potential for delta opioid receptor agonists as analgesics in chronic pain therapy David Kendall & Bengt von Mentzer; PharmNovo AB/UK Alex Conibear & Eamonn Kelly, University of Bristol Junaid Asghar,
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients
 Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Abbott s TRPV1 Antagonist Program
 Abbott s TRPV1 Antagonist Program Connie R. Faltynek, Ph.D. Sr. Director, Neuroscience and Pain Discovery American Pain Society Annual Meeting Basic Science Dinner Symposium May 9, 2008 Early History of
Abbott s TRPV1 Antagonist Program Connie R. Faltynek, Ph.D. Sr. Director, Neuroscience and Pain Discovery American Pain Society Annual Meeting Basic Science Dinner Symposium May 9, 2008 Early History of
A subpopulation of nociceptors specifically linked to itch
 Supplementary Information A subpopulation of nociceptors specifically linked to itch Liang Han 1, Chao Ma 3,4, Qin Liu 1,2, Hao-Jui Weng 1,2, Yiyuan Cui 5, Zongxiang Tang 1,2, Yushin Kim 1, Hong Nie 4,
Supplementary Information A subpopulation of nociceptors specifically linked to itch Liang Han 1, Chao Ma 3,4, Qin Liu 1,2, Hao-Jui Weng 1,2, Yiyuan Cui 5, Zongxiang Tang 1,2, Yushin Kim 1, Hong Nie 4,
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007)
 Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
SPECIAL REPORT Anandamide activates peripheral nociceptors in normal and arthritic rat knee joints
 British Journal of Pharmacology (2001) 132, 617 ± 621 ã 2001 Nature Publishing Group All rights reserved 0007 ± 1188/01 $15.00 SPECIAL REPORT Anandamide activates peripheral nociceptors in normal and arthritic
British Journal of Pharmacology (2001) 132, 617 ± 621 ã 2001 Nature Publishing Group All rights reserved 0007 ± 1188/01 $15.00 SPECIAL REPORT Anandamide activates peripheral nociceptors in normal and arthritic
Local administration of 9 -tetrahydrocannabinol attenuates capsaicin-induced thermal nociception in rhesus monkeys: a peripheral cannabinoid action
 Psychopharmacology (1999) 143:322 326 Springer-Verlag 1999 RAPID COMMUNICATION Mei-Chuan Ko James H. Woods Local administration of 9 -tetrahydrocannabinol attenuates capsaicin-induced thermal nociception
Psychopharmacology (1999) 143:322 326 Springer-Verlag 1999 RAPID COMMUNICATION Mei-Chuan Ko James H. Woods Local administration of 9 -tetrahydrocannabinol attenuates capsaicin-induced thermal nociception
Repeated intra-articular injections of acidic saline produce long-lasting joint pain and. widespread hyperalgesia
 Repeated intra-articular injections of acidic saline produce long-lasting joint pain and widespread hyperalgesia N. Sugimura 1, M. Ikeuchi 1 *, M. Izumi 1, T. Kawano 2, K. Aso 1, T. Kato 1, T. Ushida 3,
Repeated intra-articular injections of acidic saline produce long-lasting joint pain and widespread hyperalgesia N. Sugimura 1, M. Ikeuchi 1 *, M. Izumi 1, T. Kawano 2, K. Aso 1, T. Kato 1, T. Ushida 3,
Capsaicin Responses in Heat-Sensitive and Heat-Insensitive A-Fiber Nociceptors
 The Journal of Neuroscience, June 15, 2001, 21(12):4460 4468 Capsaicin Responses in Heat-Sensitive and Heat-Insensitive A-Fiber Nociceptors Matthias Ringkamp, 1 Yuan B. Peng, 1 Gang Wu, 1 Timothy V. Hartke,
The Journal of Neuroscience, June 15, 2001, 21(12):4460 4468 Capsaicin Responses in Heat-Sensitive and Heat-Insensitive A-Fiber Nociceptors Matthias Ringkamp, 1 Yuan B. Peng, 1 Gang Wu, 1 Timothy V. Hartke,
Evaluation of Gabapentin and S-( )-3-Isobutylgaba in a Rat Model of Postoperative Pain
 0022-3565/97/2823-1242$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 282, No. 3 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/97/2823-1242$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 282, No. 3 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
A role for uninjured afferents in neuropathic pain
 Acta Physiologica Sinica, October 25, 2008, 60 (5): 605-609 http://www.actaps.com.cn 605 Review A role for uninjured afferents in neuropathic pain Richard A. Meyer 1,2,3,*, Matthias Ringkamp 1 Departments
Acta Physiologica Sinica, October 25, 2008, 60 (5): 605-609 http://www.actaps.com.cn 605 Review A role for uninjured afferents in neuropathic pain Richard A. Meyer 1,2,3,*, Matthias Ringkamp 1 Departments
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle.
 What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
Competitive Inhibition of the Capsaicin Receptor-Mediated Current by Dehydroepiandrosterone in Rat Dorsal Root Ganglion Neurons
 0022-3565/04/3112-529 536$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 311, No. 2 Copyright 2004 by The American Society for Pharmacology and Experimental Therapeutics 69096/1172254
0022-3565/04/3112-529 536$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 311, No. 2 Copyright 2004 by The American Society for Pharmacology and Experimental Therapeutics 69096/1172254
Lessons from peppers and peppermint: the molecular logic of thermosensation Sven-Eric Jordt, David D McKemy and David Julius
 487 Lessons from peppers and peppermint: the molecular logic of thermosensation Sven-Eric Jordt, David D McKemy and David Julius report a wide range of temperatures, from noxious heat to noxious cold.
487 Lessons from peppers and peppermint: the molecular logic of thermosensation Sven-Eric Jordt, David D McKemy and David Julius report a wide range of temperatures, from noxious heat to noxious cold.
Peripheral Antinociception by Carbamazepine in an Inflammatory Mechanical Hyperalgesia Model in the Rat: a New Target for Carbamazepine?
 J Pharmacol Sci 100, 310 314 (2006) Journal of Pharmacological Sciences 2006 The Japanese Pharmacological Society Short Communication Peripheral Antinociception by Carbamazepine in an Inflammatory Mechanical
J Pharmacol Sci 100, 310 314 (2006) Journal of Pharmacological Sciences 2006 The Japanese Pharmacological Society Short Communication Peripheral Antinociception by Carbamazepine in an Inflammatory Mechanical
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor
 Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Biomechanics of Pain: Dynamics of the Neuromatrix
 Biomechanics of Pain: Dynamics of the Neuromatrix Partap S. Khalsa, D.C., Ph.D. Department of Biomedical Engineering The Neuromatrix From: Melzack R (1999) Pain Suppl 6:S121-6. NIOSH STAR Symposium May
Biomechanics of Pain: Dynamics of the Neuromatrix Partap S. Khalsa, D.C., Ph.D. Department of Biomedical Engineering The Neuromatrix From: Melzack R (1999) Pain Suppl 6:S121-6. NIOSH STAR Symposium May
Sudan JMS Vol. 8, No.4. Dec
 bü z ÇtÄ TÜà väx Awad E M 1 *, Ahmed E M 2 and El-hadiyah T MH 3 ABSTRACT Background: Vanilloid receptors 1 (VR 1), a group of transient receptor potential channels family was cloned in 1997. They were
bü z ÇtÄ TÜà väx Awad E M 1 *, Ahmed E M 2 and El-hadiyah T MH 3 ABSTRACT Background: Vanilloid receptors 1 (VR 1), a group of transient receptor potential channels family was cloned in 1997. They were
Sensory coding and somatosensory system
 Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
HERBERT M. HIMMEL, 1 THOMAS KISS, SEBESTYÉN J. BORVENDEG, CLEMENS GILLEN, and PETER ILLES
 0022-3565/02/3013-981 986$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 301, No. 3 Copyright 2002 by The American Society for Pharmacology and Experimental Therapeutics 0/987474 JPET
0022-3565/02/3013-981 986$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 301, No. 3 Copyright 2002 by The American Society for Pharmacology and Experimental Therapeutics 0/987474 JPET
Enhancement of Potency and Efficacy of NADA by PKC-Mediated Phosphorylation of Vanilloid Receptor
 J Neurophysiol 91: 1442 1449, 2004; 10.1152/jn.00745.2003. Enhancement of Potency and Efficacy of NADA by PKC-Mediated Phosphorylation of Vanilloid Receptor Louis S. Premkumar, Zhan-Heng Qi, Jeremy Van
J Neurophysiol 91: 1442 1449, 2004; 10.1152/jn.00745.2003. Enhancement of Potency and Efficacy of NADA by PKC-Mediated Phosphorylation of Vanilloid Receptor Louis S. Premkumar, Zhan-Heng Qi, Jeremy Van
Overactive Bladder; OAB. Aδ silent C. Adenosine triphosphate; ATP SD g n Key words
 25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
Deficits in Visceral Pain and Referred Hyperalgesia in Nav1.8 (SNS/ PN3)-Null Mice
 The Journal of Neuroscience, October 1, 2002, 22(19):8352 8356 Brief Communication Deficits in Visceral Pain and Referred Hyperalgesia in Nav1.8 (SNS/ PN3)-Null Mice Jennifer M. A. Laird, 1 Veronika Souslova,
The Journal of Neuroscience, October 1, 2002, 22(19):8352 8356 Brief Communication Deficits in Visceral Pain and Referred Hyperalgesia in Nav1.8 (SNS/ PN3)-Null Mice Jennifer M. A. Laird, 1 Veronika Souslova,
Potentiation of antinociceptive effect of NSAIDs by a specific lipooxygenase inhibitor, acetyl 11-keto-beta boswellic acid
 Indian Journal of Experimental Biology Vol. 44, February 2006, pp. 128-132 Potentiation of antinociceptive effect of NSAIDs by a specific lipooxygenase inhibitor, acetyl 11-keto-beta boswellic acid Mahendra
Indian Journal of Experimental Biology Vol. 44, February 2006, pp. 128-132 Potentiation of antinociceptive effect of NSAIDs by a specific lipooxygenase inhibitor, acetyl 11-keto-beta boswellic acid Mahendra
17 -Estradiol Mediates the Sex Difference in Capsaicin- Induced Nociception in Rats
 0022-3565/09/3313-1104 1110$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 331, No. 3 Copyright 2009 by The American Society for Pharmacology and Experimental Therapeutics 158402/3537286
0022-3565/09/3313-1104 1110$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 331, No. 3 Copyright 2009 by The American Society for Pharmacology and Experimental Therapeutics 158402/3537286
axion Application Note Modeling Pain with Rat Dorsal Root Ganglion Neurons on MEAs BioSystems
 axion BioSystems Application Note Modeling Pain with Rat Dorsal Root Ganglion Neurons on MEAs Trademarks Axion BioSystems, Inc. and the logo are trademarks of Axion BioSystems, and may not be used without
axion BioSystems Application Note Modeling Pain with Rat Dorsal Root Ganglion Neurons on MEAs Trademarks Axion BioSystems, Inc. and the logo are trademarks of Axion BioSystems, and may not be used without
The Pain Pathway. dorsal root ganglion. primary afferent nociceptor. TRP: Transient Receptor Potential
 Presented by Issel Anne L. Lim 1 st Year PhD Candidate Biomedical Engineering Johns Hopkins University 580.427/580.633 Ca Signals in Biological Systems Outline The Pain Pathway TRP: Transient Receptor
Presented by Issel Anne L. Lim 1 st Year PhD Candidate Biomedical Engineering Johns Hopkins University 580.427/580.633 Ca Signals in Biological Systems Outline The Pain Pathway TRP: Transient Receptor
The antihyperalgesic effects of gabapentinoids, carbamazepine and its keto analogue, oxcarbazepine, in capsaicin-induced thermal hyperalgesia
 World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article The antihyperalgesic effects of gabapentinoids,
World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article The antihyperalgesic effects of gabapentinoids,
The Role of Peripheral Mu Opioid Receptors in the Modulation of Capsaicin-Induced Thermal Nociception in Rhesus Monkeys 1,2
 0022-3565/98/2861-0150$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 286, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/98/2861-0150$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 286, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
Thimerosal decreases TRPV1 activity by oxidation of extracellular sulfhydryl residues
 Neuroscience Letters 369 (2004) 250 255 Thimerosal decreases TRPV1 activity by oxidation of extracellular sulfhydryl residues Yunju Jin a, Dong Kwan Kim a, Lee-Yong Khil b, Uhtaek Oh c, Jun Kim a, Jiyeon
Neuroscience Letters 369 (2004) 250 255 Thimerosal decreases TRPV1 activity by oxidation of extracellular sulfhydryl residues Yunju Jin a, Dong Kwan Kim a, Lee-Yong Khil b, Uhtaek Oh c, Jun Kim a, Jiyeon
Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I. Mr.D.Raju,M.pharm, Lecturer
 Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I Mr.D.Raju,M.pharm, Lecturer Mechanisms of Pain and Nociception Nociception is the mechanism whereby noxious peripheral stimuli are transmitted to
Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I Mr.D.Raju,M.pharm, Lecturer Mechanisms of Pain and Nociception Nociception is the mechanism whereby noxious peripheral stimuli are transmitted to
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
International Conference on Biological Sciences and Technology (BST 2016)
 International Conference on Biological Sciences and Technology (BST 2016) Analgesic Contrast of Diverse Administrations of Botulinum Neurotoxin A (BoTN/A) Using Rat Neuropathic Pain Model Qiong-Fang YANG1,3,
International Conference on Biological Sciences and Technology (BST 2016) Analgesic Contrast of Diverse Administrations of Botulinum Neurotoxin A (BoTN/A) Using Rat Neuropathic Pain Model Qiong-Fang YANG1,3,
Extracellular Protons Both Increase the Activity and Reduce the Conductance of Capsaicin-Gated Channels
 The Journal of Neuroscience, 2000, Vol. 20 RC80 1of5 Extracellular Protons Both Increase the Activity and Reduce the Conductance of Capsaicin-Gated Channels Thomas K. Baumann 1,2 and Melissa E. Martenson
The Journal of Neuroscience, 2000, Vol. 20 RC80 1of5 Extracellular Protons Both Increase the Activity and Reduce the Conductance of Capsaicin-Gated Channels Thomas K. Baumann 1,2 and Melissa E. Martenson
TMC9 as a novel mechanosensitive ion channel
 TMC9 as a novel mechanosensitive ion channel Mechanical forces play numerous roles in physiology. When an object contacts our skin, it exerts a force that is encoded as touch or pain depending on its intensity.
TMC9 as a novel mechanosensitive ion channel Mechanical forces play numerous roles in physiology. When an object contacts our skin, it exerts a force that is encoded as touch or pain depending on its intensity.
P2X3 receptors are present on sensory afferent neurons. Nociceptive Responses in the Uninjured State
 The Journal of Pain, Vol 8, No 7 (July), 2007: pp 556-562 Available online at www.sciencedirect.com 1 -Adrenergic Receptors Augment P2X 3 Receptor Mediated Nociceptive Responses in the Uninjured State
The Journal of Pain, Vol 8, No 7 (July), 2007: pp 556-562 Available online at www.sciencedirect.com 1 -Adrenergic Receptors Augment P2X 3 Receptor Mediated Nociceptive Responses in the Uninjured State
themes G. F. GEBHART Department of Pharmacology, The University of Iowa, College of Medicine, Iowa City, Iowa 52242
 Am J Physiol Gastrointest Liver Physiol 278: G834 G838, 2000. themes Pathobiology of Visceral Pain: Molecular Mechanisms and Therapeutic Implications IV. Visceral afferent contributions to the pathobiology
Am J Physiol Gastrointest Liver Physiol 278: G834 G838, 2000. themes Pathobiology of Visceral Pain: Molecular Mechanisms and Therapeutic Implications IV. Visceral afferent contributions to the pathobiology
Centrally Mediated Anti-Hyperalgesic and Anti-Allodynic Effect of Tolperisone in Spared Nerve Injury Model of Neuropathic Pain
 Centrally Mediated Anti-Hyperalgesic and Anti-Allodynic Effect of Tolperisone in Spared Nerve Injury Model of Neuropathic Pain Keyur S Patel *, Punam D Sachdeva Department of Pharmacology, A.R.College
Centrally Mediated Anti-Hyperalgesic and Anti-Allodynic Effect of Tolperisone in Spared Nerve Injury Model of Neuropathic Pain Keyur S Patel *, Punam D Sachdeva Department of Pharmacology, A.R.College
Analgesia Mediated by the TRPM8 Cold Receptor in Chronic Neuropathic Pain
 Current Biology 16, 1591 1605, August 22, 2006 ª2006 Elsevier Ltd All rights reserved DOI 10.1016/j.cub.2006.07.061 Analgesia Mediated by the TRPM8 Cold Receptor in Chronic Neuropathic Pain Article Clare
Current Biology 16, 1591 1605, August 22, 2006 ª2006 Elsevier Ltd All rights reserved DOI 10.1016/j.cub.2006.07.061 Analgesia Mediated by the TRPM8 Cold Receptor in Chronic Neuropathic Pain Article Clare
Special Issue on Pain and Itch
 Special Issue on Pain and Itch Title: Recent Progress in Understanding the Mechanisms of Pain and Itch Guest Editor of the Special Issue: Ru-Rong Ji, PhD Chronic pain is a major health problem world-wide.
Special Issue on Pain and Itch Title: Recent Progress in Understanding the Mechanisms of Pain and Itch Guest Editor of the Special Issue: Ru-Rong Ji, PhD Chronic pain is a major health problem world-wide.
Mechanisms of capsaicin- and lactic acid-induced bronchoconstriction in the newborn dog
 Keywords: 8530 Journal of Physiology (1999), 515.2, pp. 567 578 567 Mechanisms of capsaicin- and lactic acid-induced bronchoconstriction in the newborn dog M. A. Nault, S. G. Vincent and J. T. Fisher Departments
Keywords: 8530 Journal of Physiology (1999), 515.2, pp. 567 578 567 Mechanisms of capsaicin- and lactic acid-induced bronchoconstriction in the newborn dog M. A. Nault, S. G. Vincent and J. T. Fisher Departments
211MDS Pain theories
 211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
SUPPLEMENTARY INFORMATION. The Calcium-activated Chloride Channel Anoctamin 1 acts as a Heat. Sensor in Nociceptive Neurons
 SUPPLEMENTARY INFORMATION The Calcium-activated Chloride Channel Anoctamin 1 acts as a Heat Sensor in Nociceptive Neurons Hawon Cho, Young Duk Yang, Jesun Lee, Byeongjoon Lee, Tahnbee Kim Yongwoo Jang,
SUPPLEMENTARY INFORMATION The Calcium-activated Chloride Channel Anoctamin 1 acts as a Heat Sensor in Nociceptive Neurons Hawon Cho, Young Duk Yang, Jesun Lee, Byeongjoon Lee, Tahnbee Kim Yongwoo Jang,
Chapter 16. Sense of Pain
 Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
NIH Public Access Author Manuscript CNS Neurol Disord Drug Targets. Author manuscript; available in PMC 2010 June 1.
 NIH Public Access Author Manuscript Published in final edited form as: CNS Neurol Disord Drug Targets. 2009 December ; 8(6): 403 421. The Endocannabinoid System and Pain Josée Guindon and Andrea G. Hohmann
NIH Public Access Author Manuscript Published in final edited form as: CNS Neurol Disord Drug Targets. 2009 December ; 8(6): 403 421. The Endocannabinoid System and Pain Josée Guindon and Andrea G. Hohmann
Amiloride-blockable acid-sensing ion channels are leading acid sensors expressed in human nociceptors
 Amiloride-blockable acid-sensing ion channels are leading acid sensors expressed in human nociceptors Shinya Ugawa, Takashi Ueda, Yusuke Ishida, Makoto Nishigaki, Yasuhiro Shibata, and Shoichi Shimada
Amiloride-blockable acid-sensing ion channels are leading acid sensors expressed in human nociceptors Shinya Ugawa, Takashi Ueda, Yusuke Ishida, Makoto Nishigaki, Yasuhiro Shibata, and Shoichi Shimada
Somatosensation. Recording somatosensory responses. Receptive field response to pressure
 Somatosensation Mechanoreceptors that respond to touch/pressure on the surface of the body. Sensory nerve responds propotional to pressure 4 types of mechanoreceptors: Meissner corpuscles & Merkel discs
Somatosensation Mechanoreceptors that respond to touch/pressure on the surface of the body. Sensory nerve responds propotional to pressure 4 types of mechanoreceptors: Meissner corpuscles & Merkel discs
A pro-nociceptive phenotype unmasked in mice lacking fatty-acid amide hydrolase
 Research Article A pro-nociceptive phenotype unmasked in mice lacking fatty-acid amide hydrolase Molecular Pain Volume 12: 1 23! The Author(s) 2016 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Research Article A pro-nociceptive phenotype unmasked in mice lacking fatty-acid amide hydrolase Molecular Pain Volume 12: 1 23! The Author(s) 2016 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Modulation of TRP channels by resolvins in mouse and human
 July 9, 2015, Ion Channel Retreat, Vancouver Ion Channel and Pain Targets Modulation of TRP channels by resolvins in mouse and human Ru-Rong Ji, PhD Pain Research Division Department of Anesthesiology
July 9, 2015, Ion Channel Retreat, Vancouver Ion Channel and Pain Targets Modulation of TRP channels by resolvins in mouse and human Ru-Rong Ji, PhD Pain Research Division Department of Anesthesiology
What it Takes to be a Pain
 What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
TRAMADOL, A CENTRALLY ACTING OPIOID : ANTICONVULSANT EFFECT AGAINST MAXIMAL ELECTROSHOCK SEIZURE IN MICE
 Indian J Physiol Pharmacol 1998; 42 (3) : 407-411 TRAMADOL, A CENTRALLY ACTING OPIOID : ANTICONVULSANT EFFECT AGAINST MAXIMAL ELECTROSHOCK SEIZURE IN MICE ANSHU MANOCHA, KRISHNA K. SHARMA* AND PRAMOD K.
Indian J Physiol Pharmacol 1998; 42 (3) : 407-411 TRAMADOL, A CENTRALLY ACTING OPIOID : ANTICONVULSANT EFFECT AGAINST MAXIMAL ELECTROSHOCK SEIZURE IN MICE ANSHU MANOCHA, KRISHNA K. SHARMA* AND PRAMOD K.
Parvalbumin and TRPV1 Receptor Expression in Dorsal Root Ganglion Neurons after Acute Peripheral Inflammation
 Physiol. Res. 58: 305-309, 2009 RAPID COMMUNICATION Parvalbumin and TRPV1 Receptor Expression in Dorsal Root Ganglion Neurons after Acute Peripheral Inflammation G. ZACHAŘOVÁ, J. PALEČEK Department of
Physiol. Res. 58: 305-309, 2009 RAPID COMMUNICATION Parvalbumin and TRPV1 Receptor Expression in Dorsal Root Ganglion Neurons after Acute Peripheral Inflammation G. ZACHAŘOVÁ, J. PALEČEK Department of
Animal Model of Trigeminal Neuralgia Induced by Chronic Constriction Injury Applied to the Ophthalmic Nerve in the Rat
 Showa Univ. J. Med. Sci. 9(2), 8995, December 1997 Original Animal Model of Trigeminal Neuralgia Induced by Chronic Constriction Injury Applied to the Ophthalmic Nerve in the Rat Kazuo HANAKAWA, Takao
Showa Univ. J. Med. Sci. 9(2), 8995, December 1997 Original Animal Model of Trigeminal Neuralgia Induced by Chronic Constriction Injury Applied to the Ophthalmic Nerve in the Rat Kazuo HANAKAWA, Takao
GABA B Receptor Agonist Baclofen Has Non-Specific Antinociceptive Effect in the Model of Peripheral Neuropathy in the Rat
 Physiol. Res. 3: 31-3, GABA B Receptor Agonist Baclofen Has Non-Specific Antinociceptive Effect in the Model of Peripheral Neuropathy in the Rat M. FRANĚK, Š. VACULÍN, R. ROKYTA Department of Normal, Pathological
Physiol. Res. 3: 31-3, GABA B Receptor Agonist Baclofen Has Non-Specific Antinociceptive Effect in the Model of Peripheral Neuropathy in the Rat M. FRANĚK, Š. VACULÍN, R. ROKYTA Department of Normal, Pathological
Suramin Affects Capsaicin Responses and Capsaicin-Noxious Heat Interactions in Rat Dorsal Root Ganglia Neurones
 Physiol. Res. 51: 193-198, 2002 Suramin Affects Capsaicin Responses and Capsaicin-Noxious Heat Interactions in Rat Dorsal Root Ganglia Neurones V. VLACHOVÁ, A. LYFENKO, L. VYKLICKÝ, R.K. ORKAND 1 Institute
Physiol. Res. 51: 193-198, 2002 Suramin Affects Capsaicin Responses and Capsaicin-Noxious Heat Interactions in Rat Dorsal Root Ganglia Neurones V. VLACHOVÁ, A. LYFENKO, L. VYKLICKÝ, R.K. ORKAND 1 Institute
Effects of Palonosetron, a 5-HT3 Receptor Antagonist, on Mechanical Allodynia in a Rat Model of Postoperative Pain
 Original Article Korean J Pain 2013 April; Vol. 26, No. 2: 125-129 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.125 Effects of Palonosetron, a 5-HT3 Receptor Antagonist, on Mechanical
Original Article Korean J Pain 2013 April; Vol. 26, No. 2: 125-129 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.125 Effects of Palonosetron, a 5-HT3 Receptor Antagonist, on Mechanical
Departments of Biological Chemistry and Neuroscience, Center for Sensory Biology, Johns Hopkins School of Medicine, Baltimore, Maryland
 Am J Physiol Regul Integr Comp Physiol 292: R64 R76, 2007. First published September 14, 2006; doi:10.1152/ajpregu.00446.2006. CALL FOR PAPERS Physiology and Pharmacology of Temperature Regulation Transient
Am J Physiol Regul Integr Comp Physiol 292: R64 R76, 2007. First published September 14, 2006; doi:10.1152/ajpregu.00446.2006. CALL FOR PAPERS Physiology and Pharmacology of Temperature Regulation Transient
PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus. MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive
 PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
SUPPLEMENTARY INFORMATION
 METHODS Mice and rats. Behavioural experiments were performed in male and female 7 12 week old mice or in male 7 10 week old Wistar rats. Permissions for the animal experiments have been obtained from
METHODS Mice and rats. Behavioural experiments were performed in male and female 7 12 week old mice or in male 7 10 week old Wistar rats. Permissions for the animal experiments have been obtained from
Neural Injury, Repair, and Adaptation in the GI Tract II. The elusive action of capsaicin on the vagus nerve *
 themes Neural Injury, Repair, and Adaptation in the GI Tract II. The elusive action of capsaicin on the vagus nerve * PETER HOLZER Department of Experimental and Clinical Pharmacology, University of Graz,
themes Neural Injury, Repair, and Adaptation in the GI Tract II. The elusive action of capsaicin on the vagus nerve * PETER HOLZER Department of Experimental and Clinical Pharmacology, University of Graz,
Mechanical sensitization of cutaneous sensory fibers in the spared nerve injury mouse model
 Smith et al. Molecular Pain 2013, 9:61 MOLECULAR PAIN SHORT REPORT Open Access Mechanical sensitization of cutaneous sensory fibers in the spared nerve injury mouse model Amanda K Smith, Crystal L O Hara
Smith et al. Molecular Pain 2013, 9:61 MOLECULAR PAIN SHORT REPORT Open Access Mechanical sensitization of cutaneous sensory fibers in the spared nerve injury mouse model Amanda K Smith, Crystal L O Hara
Risk Factors That Predispose Patients to Orofacial Pain
 Risk Factors That Predispose Patients to Orofacial Pain Paul Durham, PhD Distinguished Professor of Cell Biology Director Center for Biomedical & Life Sciences Missouri State University Cluster Headache
Risk Factors That Predispose Patients to Orofacial Pain Paul Durham, PhD Distinguished Professor of Cell Biology Director Center for Biomedical & Life Sciences Missouri State University Cluster Headache
CRITICALLY APPRAISED PAPER (CAP) Evidence / Title of article
 CRITICALLY APPRAISED PAPER (CAP) Evidence / Title of article Sensory findings after stimulation of the thoracolumbar fascia with hypertonic saline suggest its contribution to low back pain Schilder A et
CRITICALLY APPRAISED PAPER (CAP) Evidence / Title of article Sensory findings after stimulation of the thoracolumbar fascia with hypertonic saline suggest its contribution to low back pain Schilder A et
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD
 Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
D. Nishizawa 1, N. Gajya 2 and K. Ikeda 1, * Global Research & Development, Nagoya Laboratories, Pfizer Japan Inc, Nagoya, Japan
 Current Neuropharmacology, 2011, 9, 113-117 113 Identification of Selective Agonists and Antagonists to G Protein-Activated Inwardly Rectifying Potassium Channels: Candidate Medicines for Drug Dependence
Current Neuropharmacology, 2011, 9, 113-117 113 Identification of Selective Agonists and Antagonists to G Protein-Activated Inwardly Rectifying Potassium Channels: Candidate Medicines for Drug Dependence
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Jejunal afferent nerve sensitivity in wild-type and TRPV1 knockout mice
 J Physiol 560.3 (2004) pp 867 881 867 Jejunal afferent nerve sensitivity in wild-type and TRPV1 knockout mice Weifang Rong 1,Kirk Hillsley 1,John B. Davis 2, Gareth Hicks 2,Wendy J. Winchester 2 and David
J Physiol 560.3 (2004) pp 867 881 867 Jejunal afferent nerve sensitivity in wild-type and TRPV1 knockout mice Weifang Rong 1,Kirk Hillsley 1,John B. Davis 2, Gareth Hicks 2,Wendy J. Winchester 2 and David
Capsaicin receptors mediate free radical-induced activation of cardiac afferent endings
 Ž. Cardiovascular Research 38 1998 348 355 Capsaicin receptors mediate free radical-induced activation of cardiac afferent endings Harold D. Schultz, Elena E. Ustinova Department of Physiology and Biophysics,
Ž. Cardiovascular Research 38 1998 348 355 Capsaicin receptors mediate free radical-induced activation of cardiac afferent endings Harold D. Schultz, Elena E. Ustinova Department of Physiology and Biophysics,
EVALUATION OF ANTI-NOCICEPTIVE EFFECT OF TOLPERISONE BY COMPARING ITS EFFECT WITH TRAMADOL IN NEUROPATHIC PAIN
 Journal of Pharmaceutical Biology www.jpbjournal.com e-issn - 2249-7560 Print ISSN - 2249-7579 EVALUATION OF ANTI-NOCICEPTIVE EFFECT OF TOLPERISONE BY COMPARING ITS EFFECT WITH TRAMADOL IN NEUROPATHIC
Journal of Pharmaceutical Biology www.jpbjournal.com e-issn - 2249-7560 Print ISSN - 2249-7579 EVALUATION OF ANTI-NOCICEPTIVE EFFECT OF TOLPERISONE BY COMPARING ITS EFFECT WITH TRAMADOL IN NEUROPATHIC
Opioid Receptor Trafficking in Pain States
 Encyclopedia of Pain Springer-Verlag Berlin Heidelberg 2007 10.1007/978-3-540-29805-2_2962 Robert F. Schmidt and William D. Willis Opioid Receptor Trafficking in Pain States Catherine M. Cahill 3, Anne
Encyclopedia of Pain Springer-Verlag Berlin Heidelberg 2007 10.1007/978-3-540-29805-2_2962 Robert F. Schmidt and William D. Willis Opioid Receptor Trafficking in Pain States Catherine M. Cahill 3, Anne
PAIN MANAGEMENT in the CANINE PATIENT
 PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
TRP channels: Targets for the relief of pain
 Biochimica et Biophysica Acta 1772 (2007) 989 1003 www.elsevier.com/locate/bbadis Review TRP channels: Targets for the relief of pain Jon D. Levine, Nicole Alessandri-Haber Departments of Oral and Maxillofacial
Biochimica et Biophysica Acta 1772 (2007) 989 1003 www.elsevier.com/locate/bbadis Review TRP channels: Targets for the relief of pain Jon D. Levine, Nicole Alessandri-Haber Departments of Oral and Maxillofacial
Novel Expression of Vanilloid Receptor 1 on Capsaicin- Insensitive Fibers Accounts for the Analgesic Effect of Capsaicin Cream in Neuropathic Pain
 0022-3565/03/3043-940 948$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 304, No. 3 Copyright 2003 by The American Society for Pharmacology and Experimental Therapeutics 46250/1044501
0022-3565/03/3043-940 948$7.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 304, No. 3 Copyright 2003 by The American Society for Pharmacology and Experimental Therapeutics 46250/1044501
Central Terminal Sensitization of TRPV1 by Descending Serotonergic Facilitation Modulates Chronic Pain
 Article Central Terminal Sensitization of TRPV1 by Descending Serotonergic Facilitation Modulates Chronic Pain Yu Shin Kim, 1,7 Yuxia Chu, 2,7 Liang Han, 1 Man Li, 2,3 Zhe Li, 1 Pamela Colleen LaVinka,
Article Central Terminal Sensitization of TRPV1 by Descending Serotonergic Facilitation Modulates Chronic Pain Yu Shin Kim, 1,7 Yuxia Chu, 2,7 Liang Han, 1 Man Li, 2,3 Zhe Li, 1 Pamela Colleen LaVinka,
EFFECTS OF CAPSAICIN ON RAT SCIATIC NERVE IN VINCRISTINE-INDUCED NEUROPATHIC PAIN MODEL
 IJPSR (2013), Vol. 4, Issue 2 (Research Article) Received on 17 October, 2012; received in revised form, 29 November, 2012; accepted, 30 January, 2013 EFFECTS OF CAPSAICIN ON RAT SCIATIC NERVE IN VINCRISTINE-INDUCED
IJPSR (2013), Vol. 4, Issue 2 (Research Article) Received on 17 October, 2012; received in revised form, 29 November, 2012; accepted, 30 January, 2013 EFFECTS OF CAPSAICIN ON RAT SCIATIC NERVE IN VINCRISTINE-INDUCED
Update on the Neurophysiology of Pain Transmission and Modulation: Focus on the NMDA-Receptor
 S2 Journal of Pain and Symptom Management Vol. 19 No. 1(Suppl.) January 2000 Proceedings Supplement NMDA-Receptor Antagonists: Evolving Role in Analgesia Update on the Neurophysiology of Pain Transmission
S2 Journal of Pain and Symptom Management Vol. 19 No. 1(Suppl.) January 2000 Proceedings Supplement NMDA-Receptor Antagonists: Evolving Role in Analgesia Update on the Neurophysiology of Pain Transmission
Sigma-1 Receptor Antagonist BD1047 Reduces Allodynia and Spinal ERK Phosphorylation Following Chronic Compression of Dorsal Root Ganglion in Rats
 Korean J Physiol Pharmacol Vol 14: 359-364, December, 2010 DOI: 10.4196/kjpp.2010.14.6.359 Sigma-1 Receptor Antagonist BD1047 Reduces Allodynia and Spinal ERK Phosphorylation Following Chronic Compression
Korean J Physiol Pharmacol Vol 14: 359-364, December, 2010 DOI: 10.4196/kjpp.2010.14.6.359 Sigma-1 Receptor Antagonist BD1047 Reduces Allodynia and Spinal ERK Phosphorylation Following Chronic Compression
THE VANILLOID RECEPTOR:A Molecular Gateway to the Pain Pathway
 Annu. Rev. Neurosci. 2001. 24:487 517 Copyright c 2001 by Annual Reviews. All rights reserved THE VANILLOID RECEPTOR:A Molecular Gateway to the Pain Pathway Michael J Caterina 1 and David Julius 2 1 Department
Annu. Rev. Neurosci. 2001. 24:487 517 Copyright c 2001 by Annual Reviews. All rights reserved THE VANILLOID RECEPTOR:A Molecular Gateway to the Pain Pathway Michael J Caterina 1 and David Julius 2 1 Department
Intracellular signalling cascades associated with TRP channels
 Gerald Thiel Intracellular signalling cascades associated with TRP channels Current state of investigations and potential applications Saarland University, Germany Campus Saarbrücken Department of Medical
Gerald Thiel Intracellular signalling cascades associated with TRP channels Current state of investigations and potential applications Saarland University, Germany Campus Saarbrücken Department of Medical
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D.
 Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Pathophysiology of Pain
 Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Receptors and Neurotransmitters: It Sounds Greek to Me. Agenda. What We Know About Pain 9/7/2012
 Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. Pain is always subjective
 Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Neuroscience Research, Global Pharmaceutical Research and Development, Abbott Laboratories, Abbott Park, Illinois
 0022-3565/05/3141-410 421$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 314, No. 1 Copyright 2005 by The American Society for Pharmacology and Experimental Therapeutics 83915/3039299
0022-3565/05/3141-410 421$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 314, No. 1 Copyright 2005 by The American Society for Pharmacology and Experimental Therapeutics 83915/3039299
CHAPTER 10 THE SOMATOSENSORY SYSTEM
 CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
SENSORY AND SIGNALING MECHANISMS OF BRADYKININ, EICOSANOIDS, PLATELET-ACTIVATING FACTOR, AND NITRIC OXIDE IN PERIPHERAL NOCICEPTORS
 SENSORY AND SIGNALING MECHANISMS OF BRADYKININ, EICOSANOIDS, PLATELET-ACTIVATING FACTOR, AND NITRIC OXIDE IN PERIPHERAL NOCICEPTORS Gábor Pethő and Peter W. Reeh Physiol Rev 92: 1699 1775, 2012 doi:10.1152/physrev.00048.2010
SENSORY AND SIGNALING MECHANISMS OF BRADYKININ, EICOSANOIDS, PLATELET-ACTIVATING FACTOR, AND NITRIC OXIDE IN PERIPHERAL NOCICEPTORS Gábor Pethő and Peter W. Reeh Physiol Rev 92: 1699 1775, 2012 doi:10.1152/physrev.00048.2010
Supporting Information
 Supporting Information Synthesis and Evaluation of Antiallodynic and Anticonvulsant Activity of Novel Amide and Urea Derivatives of Valproic Acid Analogues Dan Kaufmann, Meir Bialer, $, Jakob Avi Shimshoni,
Supporting Information Synthesis and Evaluation of Antiallodynic and Anticonvulsant Activity of Novel Amide and Urea Derivatives of Valproic Acid Analogues Dan Kaufmann, Meir Bialer, $, Jakob Avi Shimshoni,
Pain Mechanisms. Prof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong. The Somatosensory System
 ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
What Does the Mechanism of Spinal Cord Stimulation Tell Us about Complex Regional Pain Syndrome?pme_
 Pain Medicine 2010; 11: 1278 1283 Wiley Periodicals, Inc. What Does the Mechanism of Spinal Cord Stimulation Tell Us about Complex Regional Pain Syndrome?pme_915 1278..1283 Joshua P. Prager, MD, MS Center
Pain Medicine 2010; 11: 1278 1283 Wiley Periodicals, Inc. What Does the Mechanism of Spinal Cord Stimulation Tell Us about Complex Regional Pain Syndrome?pme_915 1278..1283 Joshua P. Prager, MD, MS Center
