Sickle cell disease, a common genetic disorder in the
|
|
|
- Tyrone Jacobs
- 5 years ago
- Views:
Transcription
1 CLINICAL ARTICLE Treating Sickle Cell Pain: An Update from The Georgia Comprehensive Sickle Cell Center * Authors: Allan Platt, PA-C, James R. Eckman, MD, JoAnn Beasley, RN, BS, and Gaynell Miller, RN, MS, CNS, Atlanta, Ga Allan Platt is Clinical Instructor, Physician Assistant Program, Emory University School of Medicine, and Program Coordinator, The Georgia Comprehensive Sickle Cell Center at Grady Health System, Atlanta, Ga. James R. Eckman is Professor of Hematology Oncology, Winship Cancer Institute, Emory University School of Medicine, and Medical Director, The Georgia Comprehensive Sickle Cell Center at Grady Health System, Atlanta, Ga. JoAnn Beasley is Newborn Screening Coordinator-Clinical Manager, The Georgia Comprehensive Sickle Cell Center at Grady Health System, Atlanta, Ga. Gaynell Miller is Assistant VP Patient Care, Grady Health System, Atlanta, Ga. *The Georgia Comprehensive Sickle Cell Center at Grady Health System was established in 1985 as the world s first 24-hour urgent care center dedicated to the needs of patients with sickle cell disease. Staffed by nurses, physicians, physician assistants, and clinic assistants, the Center provides 24-hour emergency care for patients older than 15 years without trauma and who are not pregnant. Staff use problemspecific guidelines published on the World Wide Web at org to evaluate and manage more than 3000 visits per year, and 80% of patients treated for acute pain in the Center are able to be discharged and return home after 8 hours of treatment. Questions about the care of patients with sickle cell disease can be sent by to: aplatt@emory.edu. For reprints, write: Allan Platt, PA-C, The Georgia Comprehensive Sickle Cell Center at Grady Health Center, 80 Jesse Hill Jr Dr, PO Box 109, Atlanta, GA 30303; aplatt@emory.edu. J Emerg Nurs 2002;28: Copyright 2002 by the Emergency Nurses Association /2002 $ /1/ doi: /men Sickle cell disease, a common genetic disorder in the United States, is characterized by chronic hemolytic anemia, increased severity of infections, end-organ damage, and intermittent episodes of acute and chronic pain. In this disease, crystallized hemoglobin elongates and deforms the red cell into a rigid sickle shape, causing early red cell hemolysis and blockage of small blood vessels. 1 It is estimated that 70,000 people in the United States of different ethnic backgrounds have sickle cell disease. The disease is most common in persons whose ancestors came from areas of the world where Plasmodium falciparum malaria is endemic. Inheriting one sickle gene, or sickle cell trait, provides some protection from death in young children infected with this red cell parasite. In the United States, sickle cell syndromes are present in persons of many different ethnic backgrounds, including Greek, Italian, Saudi, South American, and those from India, but they are most common in African Americans. 1 Sickle cell disease occurs in about 1 in 400 African Americans, and 8% are carriers of the sickle gene, having the sickle trait. Clinical manifestations The clinical manifestations of sickle cell disease include hemolytic anemia, increased frequency and severity of infections, tissue and organ damage, and recurrent pain episodes. Damage to the red cell from the crystallized hemoglobin reduces the survival of the cells from a normal 120 days to 12 to 15 days. The resulting hemolytic anemia causes moderate to severe reduction in the hemoglobin level, increased production of young red cells (reticulocytes) by the bone marrow, jaundice from increases in indirect bilirubin, and elevated lactic dehydrogenase. Anemia can August :4 JOURNAL OF EMERGENCY NURSING 297
2 become life-threatening when infection or other complications reduce red cell production or there is increased trapping of red cells in the spleen or liver. Bacterial infections are causes of significant morbidity and mortality in patients with sickle cell disease. Children younger than 3 years of age are at great risk for fatal sepsis and meningitis. Early loss of splenic function contributes to a greater risk for severe infections such as meningitis, pneumonia, sepsis, osteomyelitis, and salmonella. 2 Other complications are thought to result from reduced delivery of oxygen to tissues and organs. Anemia, increased blood viscosity from changes in red blood cell deformability, adherence of blood cells to vascular walls, and activation of the coagulation system all reduce the delivery of oxygen and other nutrients by the blood. Reduced blood oxygen levels, dehydration, fever, and acidosis are treatable factors that contribute to complications from crystallization of the sickle hemoglobin, causing vascular occlusion, infarctions, ischemic necrosis, and hemorrhage. 1 Damage may occur to any organ in the body, including the brain, lungs, liver, spleen, kidneys, bones, and eyes. Recurrent pain episodes are caused by ischemia resulting from reduced blood flow and the inflammation from bone marrow and muscle necrosis. These unpredictable episodes of intense pain are the most distressing symptoms for most patients. Pain episodes Self-limited, reversible pain episodes involve the extremities, back, chest, and abdomen. Many patients have mild pain episodes of short duration that can be managed at home. More severe episodes, however, may last hours, days, or weeks. 3 Patients characterize the pain as being similar to breaking all of one s bones at the same time. The frequency of pain episodes varies with each individual and is generally related to the hemoglobin phenotype, level of fetal hemoglobin, concurrent illness, physical condition, psychological factors, and social variables. Chronic damage to bones, nerves, and other tissues with inflammation and fibrosis can lead to chronic pain syndromes as well. Management of pain episodes Pain episodes are diagnosed by patient history alone because no physical or laboratory manifestations occur during uncomplicated pain episodes. The best question to ask the patient is: Is this pain typical for your pain episodes? If the pain is typical, the patient is treated for a routine pain episode. If the pain is atypical, a search for complications or other causes is started. Pain in the chest, head, and abdomen warrants a careful evaluation for complications and non sickle-related causes. A detailed history and physical examination are important for identifying correctable precipitating factors such as infection, dehydration, increased anemia, or other precipitating complications. Laboratory evaluation does not help in the diagnosis of pain episodes, but it does help identify anemia, infection, acidosis, hypoxia, and other complications. 5 Pain assessment Pain intensity is typically assessed and recorded at the beginning of treatment and at set intervals to document the maximal response to treatment. It is helpful to use patient self-report including a Visual Analog Scale, a verbal rating from 0 to 10, or the Wong Baker Faces Scale, which are rapid tools for pain assessment. 3-4 Pain therapy The treatment of pain episodes includes control of pain, intracellular hydration with hypotonic oral or intravenous fluids, correction of hypoxia and acidosis, bed rest, and treatment of underlying infection or other complications. 3 Control of pain requires accurate pain assessment and provision of adequate analgesia by giving sufficient doses of medications on a regular schedule based on the effective half-life of the medication. Pain therapy requires choosing agents that provide rapid and sustained analgesia. Pain medication should be administered in a dose that reduces the pain to a level that is acceptable to the patient and on a fixed time schedule at an interval that provides adequate analgesia without return of pain. At the Georgia Comprehensive Sickle Cell Center, we find that most patients present with an average pain level of 8 out of 10 and are ready to go home with a supply of oral analgesics after reducing their pain intensity below 4. We use this approach to maintain a steady drug level, thereby improving control of pain, minimizing complications, and 298 JOURNAL OF EMERGENCY NURSING 28:4 August 2002
3 decreasing anxiety. Most patients presenting to the hospital have failed to control the pain with oral therapy and should therefore be treated with parenteral analgesics. Intravenous therapy is the route of choice because of the rapid onset of action, predicable distribution, and minimal pain or local tissue damage from the drugs. Morphine is the opiate of choice because of flexibility in dosing forms, a predictable adverse effect profile, and proven effectiveness. 3,5 Dosing instructions for morphine are provided in Table 1. Patientcontrolled analgesia (PCA) pumps that provide constant low-dose infusion of morphine with patient-controlled demand doses provide excellent pain treatment. Similar results can be obtained by using sustained-release morphine preparations on a fixed schedule to control pain by maintaining a constant blood level and providing supplemental doses of oral or parenteral short-acting preparations on demand for breakthrough pain. Frequent adverse effects of the narcotic analgesics include itching from histamine release, nausea, vomiting, and constipation. These effects respond to concurrent administration of antihistamines, antiemetics, stool softeners, and laxatives. Unusual adverse effects, usually from excessive blood levels, include respiratory depression, hypotension, increased bladder tone, urinary retention, and decreased seizure threshold. Most experts now discourage the use of meperidine to treat sickle cell pain. When meperidine is used, a metabolite of meperidine, normeperidine, accumulates, causing irritability, reduced pain control, central nervous system stimulation, and seizures with frequent or prolonged use. Nalbuphine, a synthetic agonist-antagonist opiate, is very useful in children and adults who require infrequent pain treatment. The benefits of nalbuphine include an excellent adverse effect profile with reduced nausea, less sedation, and minimal respiratory depression. A major disadvantage is the analgesic ceiling of 20 mg every 3 hours because of the antagonist action. If pain is not controlled by this dose, nalbuphine must be stopped and a pure agonist opiate such as morphine should be titrated until the pain is controlled. Nalbuphine is contraindicated in patients with frequent or regular narcotic usage because it can cause naloxone-like, acute withdrawal symptoms when physical dependency on opiates is present. The dosage is 0.3 mg/kg up to 20 mg administered intravenously every 3 hours. TABLE 1 Pain therapy dosing for patients with sickle cell disease Morphine sulfate, 0.05 to 0.08 mg/kg (3 to 5 mg) administered intravenously every 10 minutes until pain is controlled Give the dose required to control the pain every 3 hours intravenously (NOT prn) Add ketorolac, 30 mg intravenous every 6 hours, or ibuprofen, 600 mg by mouth every 6 hours if the patient has no history of renal disease, peptic ulcer disease, or other contraindications Adjust the every-3-hour dose based on pain level and sedation Morphine patient-controlled analgesia: Morphine concentration of 5 mg/ml is used to treat adults because they generally need relatively high doses to control the pain. Loading doses of morphine up to 0.05 mg/kg every 15 minutes times 4 may be given based on need. Demand doses of to 0.04 mg/kg/dose with a 5 to 15 minute lockout are a usual range for patients with sickle cell disease. Continuous infusion doses, if necessary, may be given at night or around the clock. The usual dose ranges are between 0.01 to 0.04 mg/kg/hour. One-hour or 4-hour limits should be calculated so that the patient can get treatment for the entire period. That is, the limits should be based on the sum of the maximum demand dose plus the continuous infusion dose. Adjuvants are hydroxyzine, 25 mg administered intramuscularly every 6 hours, or promethazine, 12.5 mg every 6 hours, for nausea or anxiety. Use diphenhydramine, 25 to 50 mg every 6 hours, with morphine to prevent itching. A large number of analgesics can be used to treat the pain of sickle cell disease reliably. The important principle that can make caring for a patient with a sickle pain episode much more successful is to titrate the patient s pain level to a level that they desire. The amounts and frequency of the agonist opiate analgesics can be increased in dosage and frequency until pain control is adequate or the patient experiences excessive sedation, respiratory depression, or hypotension. Once a dose and frequency is established, the medication can be given on a regular schedule at this dose to prevent the pain from recurring at a level that is unacceptable to the patient. The dose and frequency may be different for every patient and may differ for an individual patient, depending on the severity of the pain. 3,5 August :4 JOURNAL OF EMERGENCY NURSING 299
4 TABLE 2 The ABC s for managing sickle cell pain A Assessment of the pain (use a pain assessment tool) B Believe the patient s level of pain C Complications or cause of pain (look for complications) D Drugs and distraction Pain Medication (opiates and NSAIDs, if no contraindications) Distraction with music, TV, relaxation techniques E Environment, rest in quiet area with privacy F Fluids (Hypotonic-D 5 W or D5 with 0.25 normal saline solution) Use fixed dosing; give on a time schedule; no prn dosing for pain medications A number of important medical interventions may decrease the duration of the pain episode. Oral hydration with water and juices or intravenous hypotonic fluids such as intravenous dextrose 5% with water (D 5 W) is important for 2 reasons. First, decreasing the sodium concentration outside the red cell causes water to go into the red cell. This dilutes the intracellular hemoglobin concentration, which markedly reduces the tendency of the sickle hemoglobin to crystallize. 6 The second reason is that almost all persons with sickle cell anemia and many with hemoglobin SC and hemoglobin S β-thalassemia have a renal concentrating defect that causes them to continuously lose water from the kidneys. If they stop drinking water because of the pain or other illness, free water dehydration rapidly develops. By administering replacement fluids, the duration of pain can be reduced. 6 At our Center, patients are hydrated with D 5 W at 250 ml per hour (children receive 5 ml/kg/h) for 4 hours in the absence of congestive heart failure, renal failure, or hyponatremia. The fluids should be changed to D 5 W or D 5 W with 1 4 or 1 2 normal saline solution at a slower rate, 125 ml per hour (for children, 1 to 2 ml/kg/h), for second and subsequent liters, based on electrolytes. If venous access cannot be obtained, oral hydration should be used. We do not use lower extremities for hydration except in extreme emergencies because of the increased frequency of leg ulcers. It is important to administer oxygen to patients with hypoxia or dyspnea because deoxygenation is the primary cause of sickling. Pulse oximetry can be used to diagnose and monitor oxygen saturation if the patient s anemia is not too severe. Low oxygen saturation in symptomatic patients must be investigated with arterial blood gases (ABGs), chest radiographs, and pulmonary testing. Oxygen use for routine pain episodes is not beneficial. In our Center, we keep patients for 8 hours with ongoing treatment and pain assessments. If the patient is then able to manage their pain at home, a 48-hour supply of opiate and nonsteroidal antiinflammatory drugs (NSAIDs) is given, with instructions to return if the pain escalates or if fever or other new symptoms develop. We admit the patient if his or her pain level is not adequately resolved in 8 hours, or if a complication such as fever, sequestration, infiltrate, dropping hematocrit level, or priapism is present. The ABC s of sickle cell pain management are listed in Table 2. Complications Pain episodes may continue until underlying medical problems are completely resolved. A second concern is that the pain episode may be an antecedent to a more serious sickle complication. A number of potentially life-threatening complications can present as pain episodes, or can develop as a pain episode is being treated. Table 3 details common emergency patient presentations and laboratory, radiologic, and treatment options. Fever Fever in a patient with sickle cell disease is an emergent situation. It indicates sepsis until proven otherwise. All our patients with fever receive a septic work-up, including blood cultures, complete blood cell count with differential, reticulocyte count, urinalysis, and chest radiograph. After cultures are obtained, we give the patient a long-acting parenteral antibiotic with coverage against pneumococcus. Some patients may be allowed to go home from the emergency department with next day follow-up if no high-risk features appear on history, physical examination, or laboratory evaluation, but only if outpatient follow-up can be assured JOURNAL OF EMERGENCY NURSING 28:4 August 2002
5 TABLE 3 Common problems of patients with sickle cell disease in the emergency department Signs and symptoms Diagnostic tests and differential Treatment options Symmetric hand-foot Hand foot syndrome first manifestation of Fluids and pain management swelling, infant sickle cell disease Chills and fever Sepsis, pneumonia, osteomyelitis Empirically treat with antibiotics until cultures are do a CBC, WBC differential (check for known; prevent infections with immunization and elevated bands and total WBC count), prophylactic penicillin until age 6 years blood cultures Headache Stroke, aneurysm, meningitis Treat etiology CT scan, MRI-MRA, LP Chest Pain, dyspnea, Chest syndrome, pneumonia do a chest Treat empirically with antibiotics and transfusion cough radiograph, ABG Abdominal pain and Splenic or hepatic sequestration, gallstones Transfusion for sequestration; surgery for gallstones swelling ultrasound or CT, CBC and chemistry profile New weakness, Stroke do a CT or MRI-MRA Transfuse acutely and chronic transfusion program for paresthesias, prevention difficulty talking Pain in extremities, Pain episode look for precipitating causes Hydration with oral or IV water; good pain managelow back typical such as infection, dehydration, acidosis; ment; hydrea may prevent pain episodes pain episode pain do a CBC, reticulocyte count, chemistry profile, and UA Weakness, lethargy, Aplastic episodes, do a CBC with reticulocyte Transfusion support until bone marrow responds pallor count (low hematocrit with low reticulocyte count) Acute decline after Multi-organ system failure evidenced by renal, Transfusions can be life saving routine pain hepatic, failure, ARDS, DIC episodes multiple organ failure Increasing jaundice Increased hemolysis, hepatitis, or bile duct Treat etiology; administer folate, 1 mg daily, to all obstruction; do a CBC, reticulocyte count, patients for red cell production demands chemistry profile, hepatitis screen; consider a gallbladder ultrasound Increasing ED visits Consider inadequate pain management, Provide good pain management; consider hydroxyurea for pain infection, increased anemia; assess psycho- therapy to prevent pain; case management social aspects Focal bone pain Consider bone infarction or osteomyelitis; For bone infarction and AVN, treat with long acting if hip or shoulder pain, consider AVN; NSAIDs and decreased weight bearing do a CBC and a radiograph of the area ABG, Arterial blood gas; ARDS, acute respiratory distress syndrome; AVN, avascular necrosis; CBC, complete blood cell count; CT, computed tomography; DIC, disseminated intravascular coagulation; LP, lumbar puncture; MRI-MRA, magnetic resonance imaging-magnetic resonance angiography; UA, urinalysis; WBC, white blood cell count. Abdominal pain Abdominal pain may be caused by splenic sequestration. This serious complication is second only to infections as a cause of death in infants with sickle cell disease. This event usually occurs between the ages of 4 months and 3 years, but it may happen at any age with hemoglobin SC or S β-thalassemia disease. During sequestration episodes, sickle cells are trapped in the spleen, causing rapid fall in the hemoglobin level and enlargement of the spleen. Sequestration events may be triggered by infection or can occur with no apparent antecedent. The onset of signs and symptoms is very rapid and consists of weakness, left upper quadrant August :4 JOURNAL OF EMERGENCY NURSING 301
6 Case scenario You are the nurse on duty in the emergency department when a 19-year-old man with severe pain in his arms, legs, and back is brought in by his college roommate. You do the initial triage and find out that the student has sickle cell anemia and the pain had begun 6 hours earlier. He also has a 24-hour history of coughing, fever, and chills. His last pain episode was 8 months ago. Physical evaluation shows a well-developed man holding his arms and legs, writhing in pain. His vital signs are as follows: pulse, 110; respirations, 20; blood pressure, 130/85; temperature, 39.0 C; and pulse oximetry SaO 2, 90%. His tongue is furrowed, showing dehydration. His pain intensity is 9 out of 10 on a visual analog scale. You ask if his pain is typical for his usual episodes, and he states that it is more severe than usual and the cough is unusual. The patient has been taking ibuprofen, 600 mg every 6 hours, without much relief. You immediately assess the patient as high priority, and care for his sickle cell pain episode is started immediately. The ED physician evaluates the patient quickly. You review the history, physical examination, and orders for treatment and diagnostic evaluation. The laboratory orders include a complete blood cell count and reticulocyte count to determine the bone marrow response to the chronic hemolytic anemia. A chemistry profile, sputum for culture, blood culture, and urinalysis also are ordered. A chest radiograph and nasal oxygen at 2 L per hour are ordered because of the cough, fever, and hypoxia. A venous line is inserted and D 5 W is administered at 250 ml per hour for the first liter, then 125 ml per hour. The pain management orders are as follows: nalbuphine (Nubain), 20 mg administered intravenously every 3 hours. Nalbuphine is an agonist/antagonist that has respiratory depression ceiling. Nonsteroidal antiinflammatory drugs are held to observe for fever. You assess the patient s pain score and administer the medication slowly, intravenously. You come back in 15 minutes to reassess the pain score and ask about adverse effects, and make the patient as comfortable as possible. Your patient returns from radiology with a negative chest radiograph. His pain level has decreased during the past hour to a 5 out of possible 10 on the visual analog pain scale. His laboratory results are typical of the patient s baseline values. The physician decides to admit the patient for intravenous administration of antibiotics, pain management, and monitoring. The ED nurse has contributed significantly to the care of this patient in recognizing the patient s need for pain relief and supporting him throughout his episode. abdominal pain, fatigue, dyspnea, pending shock, tachycardia, pallor, enlarging spleen, and a falling hemoglobin and hematocrit. The diagnosis is based on the enlarging spleen and a reticulocyte count that is equal to or higher than the patient s baseline. Treatment consists of admission to an ICU with aggressive blood transfusions. Emergent splenectomy is occasionally required. Other sickle cell causes of abdominal pain include hepatic sequestration and gallstones. Chest pain Chest pain, cough, fever, or hypoxia in a patient with sickle cell disease requires evaluation with a chest radiograph and ABGs. The presence of an infiltrate is the hallmark of the acute chest syndrome (ACS), an important cause of morbidity and mortality. The etiology of ACS includes infection with viruses and bacteria, bone marrow necrosis with fat embolism, and de novo sickling in the pulmonary blood vessels. 7 Pneumonia caused by atypical bacteria is a common infectious cause of ACS. Bronchoscopy is often diagnostic and may occasionally be therapeutic. Patients should be treated with transfusions and antibiotics that cover atypical bacteria and Streptococcus pneumoniae. The occurrence of ACS in the postoperative period may be reduced by simple transfusion to a hemoglobin of 10 g/dl preoperatively and use of incentive spirometry postoperatively. Headache Acute headache or transient neurologic symptoms could indicate a hemorrhagic or thrombotic stroke or meningitis. A rapid neurologic evaluation with consideration of a computed tomography scan and/or lumbar puncture is essential. 5 Atypical pain The worst pain episode ever with other evidence of multiorgan failure is best treated with rapid blood transfusions or exchange transfusion. Transfusion of packed red cells is not indicated for the treatment of routine pain episodes. Patients may require transfusions if symptomatic anemia develops during treatment for a pain episode. Patients with sickle cell disease who have strokes, transient ischemic episodes, chest infarction, multi-organ system failure, or 302 JOURNAL OF EMERGENCY NURSING 28:4 August 2002
7 Resources for patients with sickle cell disease: Web sites, books, and CD-ROMs The Sickle Cell Information Center Web site at is a comprehensive site for providers and patients. The book Problem Oriented Management of Sickle Cell Syndromes by James Eckman, MD, and Allan Platt, PA-C, is available at this site. Ballas, SK. Sickle Cell Pain: Progress in Pain Management (vol. 11). Seattle (WA): International Association for the Study of Pain; 1998, 398 pp, hardbound, ISBN Guideline for the Management of Acute and Chronic Pain in Sickle Cell Disease, Glenview (IL): American Pain Society; Address: American Pain Society, 4700 W Lake Ave, Glenview, IL 60025; phone (847) ; fax (847) ; info@ ampainsoc.org; Web site: CD-ROM: The Wellcome Trust Presents: Topics in International Health Sickle Cell Disease. Available at: or sequestration of red cells in the spleen or liver are candidates for exchange transfusions. Preventive care and patient education Prophylactic daily penicillin is instituted from birth to 6 years for all patients with sickle cell disease to prevent pneumococcal sepsis. 8 Guidelines for discharge instructions in Table 4 can help prevent other pain episodes. To prevent pain episodes, the only approved preventive strategy is oral hydroxyurea. Be sure to mention it to your patients. Opiate addiction myths and issues Narcotic addiction is a rare occurrence, usually affecting 2% to 5% of the sickle cell patient population. It takes several days of continuous narcotics to cause physical dependence and tolerance to opiate medications. Severe pain requiring narcotics should not be confused with a true addiction, where the patient s life adversely revolves around a favorite drug. Pseudo-addiction occurs when the patient is continually undertreated and returns frequently with unresolved pain. This situation can be managed with adequate doses of long-acting agents. TABLE 4 Discharge teaching points for sickle cell patients 1. Encourage daily oral folate supplementation, which will help the bone marrow keep up red cell production. 2. Encourage follow-up care with sickle cell experts (see the Sickle Cell Information Center at for clinic locations). 3. Encourage increased water intake to prevent dehydration (this should be 8 glasses a day for adults). 4. Advise patients to avoid temperature extremes of too hot or too cold. 5. Advise patients to rest and not to overdo it. 6. Advise patients that bone pain should be treated with daily NSAIDs. 7. Advise patients on how to manage the sedation and constipation accompanying the use of opiates. 8. Advise patients to slowly taper opiates when they are taken for several days. Otherwise, they will experience withdrawal symptoms. 9. Offer patient education handouts. Several are available for printing and distribution at REFERENCES 1. Steinberg M. Management of sickle cell disease. N Engl J Med 1999;340: Ander DS, Vallee PA. Diagnostic evaluation for infectious etiology of sickle cell pain crisis. Am J Emerg Med 1997;15: Benjamin LJ, Dampier CD, Jacox A, Odesina V, Phoenix D, Shapiro, BS, et al. Guideline for the management of acute and chronic pain in sickle cell disease (American Pain Society clinical practice guidelines series, No. 1). Glenview (IL): American Pain Society; Beyer JE, Platt AF, Kinney T, Treadwell M. Practice guidelines for the assessment of children with sickle cell pain. J Soc Pediatr Nurse 1999;4: Eckman JR, Platt AF. Problem oriented management of sickle cell syndromes (1991, revised 2001). Available at: URL: SCInfo.org/prod04.htm 6. Rosa RM, Bierer BE, Thomas R, Stoff JS, Kurskall M, Robinson S, et al. A study of induced hyponatremia in the prevention and treatment of sickle cell crisis. N Engl J Med 1980;303: Vichinsky EP, Styles LA, Colangelo LH, Wright EC, Castro O, Nickerson B. Acute chest syndrome in sickle cell disease: clinical presentation and course. Cooperative study of sickle cell disease. Blood 1997;89: Overturf GD. American Academy of Pediatrics. Committee on Infectious Diseases. Technical report: prevention of pneumococcal infections, including the use of pneumococcal conjugate and polysaccharide vaccines and antibiotic prophylaxis. Pediatrics 2000;106(2 Pt 1): August :4 JOURNAL OF EMERGENCY NURSING 303
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Putting some hematology into Pediatric Hematology/Oncology: a review of Hemophilia and Sickle Cell Disease in the Pediatric Patient
 Putting some hematology into Pediatric Hematology/Oncology: a review of Hemophilia and Sickle Cell Disease in the Pediatric Patient Kristina Haley, DO March 10, 2012 Jovita Reyes Memorial Pediatric Hematology/Oncology
Putting some hematology into Pediatric Hematology/Oncology: a review of Hemophilia and Sickle Cell Disease in the Pediatric Patient Kristina Haley, DO March 10, 2012 Jovita Reyes Memorial Pediatric Hematology/Oncology
PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE
 PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE 1. PAIN Principles To educate patients, family and other caregivers about prevention, rapid identification and management of vaso-occlusive
PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE 1. PAIN Principles To educate patients, family and other caregivers about prevention, rapid identification and management of vaso-occlusive
Sickle Cell Disease. Edward Malters, MD
 Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM. Is This Strictly a Pain Episode? Decision 7: Referrals
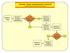 ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
Acute Complications of Sickle Cell Disease
 Management of Acute Complications of Sickle Cell Disease A Pocket Guide for the Clinician Timothy McCavit, MD, MSCS 1 Payal Desai, MD 1 University of Texas Southwestern Medical Center The Ohio State University,
Management of Acute Complications of Sickle Cell Disease A Pocket Guide for the Clinician Timothy McCavit, MD, MSCS 1 Payal Desai, MD 1 University of Texas Southwestern Medical Center The Ohio State University,
Managing Emergencies
 Managing Emergencies Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian Hemoglobinopathy Association
Managing Emergencies Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian Hemoglobinopathy Association
Acute vaso-occlusive Pain in children
 Acute vaso-occlusive Pain in children Dr François Angoulvant 1 Dr Sebastien Redant 2 Dr Malika Benkerrou 1 Pr Alina Ferster 2 Hôpital Robert Debré - Paris Hôpital des Enfants Reine Fabiola Bruxelles Réseau
Acute vaso-occlusive Pain in children Dr François Angoulvant 1 Dr Sebastien Redant 2 Dr Malika Benkerrou 1 Pr Alina Ferster 2 Hôpital Robert Debré - Paris Hôpital des Enfants Reine Fabiola Bruxelles Réseau
Sickle cell disease. Fareed Omar 10 March 2018
 Sickle cell disease Fareed Omar 10 March 2018 Physiology Haemoglobin structure HbA2: 2α and 2δ chains (2-3%) HbF: 2α and 2γ chains (
Sickle cell disease Fareed Omar 10 March 2018 Physiology Haemoglobin structure HbA2: 2α and 2δ chains (2-3%) HbF: 2α and 2γ chains (
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm
 Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Full Case: Questions: What is sickle cell crisis?
 Full Case: 30 y/o with avascular necrosis of her right hip was admitted for a total hip arthroplasty. Her hematocrit was 22%, blood pressure was 130/90 mm Hg, and pulse was 107 beats per minute. She had
Full Case: 30 y/o with avascular necrosis of her right hip was admitted for a total hip arthroplasty. Her hematocrit was 22%, blood pressure was 130/90 mm Hg, and pulse was 107 beats per minute. She had
Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143
 Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Lessons in Management of Sickle Cell Disease. CME Conference, Lloyd Erskine Sandiford Centre, November 15, 2015
 Lessons in Management of Sickle Cell Disease CME Conference, Lloyd Erskine Sandiford Centre, November 15, 2015 Age at Death in African SS Disease The greatest chance of death is in the first is in the
Lessons in Management of Sickle Cell Disease CME Conference, Lloyd Erskine Sandiford Centre, November 15, 2015 Age at Death in African SS Disease The greatest chance of death is in the first is in the
SICKLE CELL DISEASE. Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH. Assistant Professor FACULTY OF MEDICINE -JAZAN
 SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
Congenital Haemoglobinopathies
 Congenital Haemoglobinopathies L. DEDEKEN, MD H O P I T A L U N I V E R S I T A I R E D E S E N F A N T S R E I N E F A B I O L A U N I V E R S I T E L I B R E DE B R U X E L L E S Red Blood Cell Disorders
Congenital Haemoglobinopathies L. DEDEKEN, MD H O P I T A L U N I V E R S I T A I R E D E S E N F A N T S R E I N E F A B I O L A U N I V E R S I T E L I B R E DE B R U X E L L E S Red Blood Cell Disorders
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE
 ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
Sickle Cell Disease and impact on the society
 Sickle Cell Disease and impact on the society Professor Z.A.Jeremiah Ph.D, FRCPath (London) Professor of Haematology and Blood Transfusion Science Niger Delta University, Wilberforce Island Outline What
Sickle Cell Disease and impact on the society Professor Z.A.Jeremiah Ph.D, FRCPath (London) Professor of Haematology and Blood Transfusion Science Niger Delta University, Wilberforce Island Outline What
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease
 Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Guidelines for Shared Care Centres and Community Staff
 Reference: CG1411 Written by: Dr Jenny Welch Peer reviewer Dr Jeanette Payne Approved: September 2015 Approved by D&TC: 10 th July 2015 Review Due: September 2018 Intended Audience This document contains
Reference: CG1411 Written by: Dr Jenny Welch Peer reviewer Dr Jeanette Payne Approved: September 2015 Approved by D&TC: 10 th July 2015 Review Due: September 2018 Intended Audience This document contains
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Hemolytic anemias (2 of 2)
 Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Hematology/Oncology/BMT
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Hematology/Oncology/BMT 1. GOAL: Understand the role of the pediatrician in preventing hematologic or oncologic conditions,
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Hematology/Oncology/BMT 1. GOAL: Understand the role of the pediatrician in preventing hematologic or oncologic conditions,
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques
 Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
Aneurin Bevan University Health Board Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines
 Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Acute Chest Syndrome: Can a Chest Radiograph Predict the Course Severity of the Disease?
 Original Article Elmer Press Acute Chest Syndrome: Can a Chest Radiograph Predict the Course Severity of the Disease? Arie Franco a, c, Kathleen Tarrant McKie b, Patrick Ryan Henderson a, Kristopher Neal
Original Article Elmer Press Acute Chest Syndrome: Can a Chest Radiograph Predict the Course Severity of the Disease? Arie Franco a, c, Kathleen Tarrant McKie b, Patrick Ryan Henderson a, Kristopher Neal
Division of General Internal Medicine and Geriatrics Hospital Medicine 2014
 Division of General Internal Medicine and Geriatrics Hospital Medicine 2014 Objectives Understand workup of acute pain crisis Identify key aspects of management of acute pain crisis in sickle cell patients
Division of General Internal Medicine and Geriatrics Hospital Medicine 2014 Objectives Understand workup of acute pain crisis Identify key aspects of management of acute pain crisis in sickle cell patients
Education Visit #1 *** All Sickle Cell Patients*** from A Parent s Handbook for Sickle Cell Disease Booklet.
 Education Visit #1 *** All Sickle Cell Patients*** Step 1: Administer Pretest A. Step 2: Education Watch DVD: Education Visit #1 For All Patients Handout So You Have Sickle Cell Disorder Handout Infection
Education Visit #1 *** All Sickle Cell Patients*** Step 1: Administer Pretest A. Step 2: Education Watch DVD: Education Visit #1 For All Patients Handout So You Have Sickle Cell Disorder Handout Infection
Tenth Visit posttest
 Test Code 10C Patient s name: Tenth Visit posttest Patient s birth date: Your name and relationship to patient: Today s date: 1. Which one of the medications listed below should every child with a sickle
Test Code 10C Patient s name: Tenth Visit posttest Patient s birth date: Your name and relationship to patient: Today s date: 1. Which one of the medications listed below should every child with a sickle
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
Medical and Surgical Complications of Sickle Cell Anemia
 Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Department of Surgery Dar A lalafia Medical Company Qatif
Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Medical and Surgical Complications of Sickle Cell Anemia Ahmed Al-Salem Department of Surgery Dar A lalafia Medical Company Qatif
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1
 Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Gaining perspective on the spectrum of sickle cell anemia: Question: What do all these real life presentations have in common?
 Sickle-Cell Management Objectives: After reading this lecture the participant should be able to: 1. Explain the basic disease process of Sickle Cell Anemia 2. Have an understanding of the precipitants
Sickle-Cell Management Objectives: After reading this lecture the participant should be able to: 1. Explain the basic disease process of Sickle Cell Anemia 2. Have an understanding of the precipitants
*Monitor for significant side effects, especially symptoms of neurological or cardiovascular events.
 Assessment Prior to administration: Obtain complete health history including allergies, drug history, and possible drug reactions Assess reason for drug administration such as presence/history of anemia
Assessment Prior to administration: Obtain complete health history including allergies, drug history, and possible drug reactions Assess reason for drug administration such as presence/history of anemia
Rationale for RBC Transfusion in SCD
 Rationale for RBC Transfusion in SCD Dilution of HgbS-containing RBCs via the addition of HgbA-containing cells from the blood of normal donors Suppression of erythropoietin release caused by the rise
Rationale for RBC Transfusion in SCD Dilution of HgbS-containing RBCs via the addition of HgbA-containing cells from the blood of normal donors Suppression of erythropoietin release caused by the rise
Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone
 Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Nursing Process Focus: Patients Receiving Dextran 40 (Gentran 40)
 Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
Psychology of Pain DR. ARNEL BANAGA SALGADO,
 Psychology of Pain DR. ARNEL BANAGA SALGADO, Doctor of Psychology (USA) FPM (Ph.D.) Psychology (India) Doctor of Education (Phl) Master of Arts in Nursing (Phl) Master of Arts in Teaching Psychology (PNU)
Psychology of Pain DR. ARNEL BANAGA SALGADO, Doctor of Psychology (USA) FPM (Ph.D.) Psychology (India) Doctor of Education (Phl) Master of Arts in Nursing (Phl) Master of Arts in Teaching Psychology (PNU)
Anemia s. Troy Lund MSMS PhD MD
 Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS.
 Page 1 The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS. Appendix TABLE E-1 Care-Module Trigger Events That May Indicate an Adverse
Page 1 The following content was supplied by the author as supporting material and has not been copy-edited or verified by JBJS. Appendix TABLE E-1 Care-Module Trigger Events That May Indicate an Adverse
HASPI Medical Biology Lab 03
 Patient 1001 is a 42-year-old female that is experiencing severe heartburn, abdominal pain, bloating, nausea, and vomiting. Ulcers Bleeding sores in the stomach or intestine Gallbladder Disease Gallstones
Patient 1001 is a 42-year-old female that is experiencing severe heartburn, abdominal pain, bloating, nausea, and vomiting. Ulcers Bleeding sores in the stomach or intestine Gallbladder Disease Gallstones
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT
 PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
PRESCRIBER SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR THE HEALTHCARE PROVIDER
 PRESCRIBER SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR THE HEALTHCARE PROVIDER BEFORE STARTING YOUR PATIENTS ON SOLIRIS Important safety information for the healthcare provider Prior to initiating
PRESCRIBER SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR THE HEALTHCARE PROVIDER BEFORE STARTING YOUR PATIENTS ON SOLIRIS Important safety information for the healthcare provider Prior to initiating
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Health Maintenance and Education for Children and Adults
 Health Maintenance and Education for Children and Adults Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian
Health Maintenance and Education for Children and Adults Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian
Sickle Cell Disease 101. Objectives. What is SCD? 4/20/2016. Discuss the pathophysiology & genetics of Sickle Cell Disease (SCD).
 Sickle Cell Disease 101 Jennifer Young, RN, MS, CPNP-AC Sickle Cell & Thalassemia Nurse Practitioner Nationwide Children s Hospital Objectives Discuss the pathophysiology & genetics of Sickle Cell Disease
Sickle Cell Disease 101 Jennifer Young, RN, MS, CPNP-AC Sickle Cell & Thalassemia Nurse Practitioner Nationwide Children s Hospital Objectives Discuss the pathophysiology & genetics of Sickle Cell Disease
PATIENT INFORMATION FROM YOUR SURGEON & SAGES. Laparoscopic Spleen Removal (Splenectomy)
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Spleen Removal (Splenectomy)
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Spleen Removal (Splenectomy)
Drug and Therapeutics committee, Clinical Haematology Directorate. Department of Haematology, Nottingham City Hospital
 Version: 5 Date: 03/08/2005 Date Ratified: 03/08/2005 Date Reviewed 3/08/2017 Date due for Review: August 2018 Approval: Author: Drug and Therapeutics committee, Clinical Haematology Directorate Dr Jennifer
Version: 5 Date: 03/08/2005 Date Ratified: 03/08/2005 Date Reviewed 3/08/2017 Date due for Review: August 2018 Approval: Author: Drug and Therapeutics committee, Clinical Haematology Directorate Dr Jennifer
1. Adequate diet and iron intake to prevent iron deficiency 2. Signs and symptoms of malignant disease
 Hematology/Oncology Description: The pediatric hematology-oncology division sees a wide spectrum of pediatric disease including but not limited to leukemia, hemophilia, solid tumors, ITP, and other blood
Hematology/Oncology Description: The pediatric hematology-oncology division sees a wide spectrum of pediatric disease including but not limited to leukemia, hemophilia, solid tumors, ITP, and other blood
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013 What type of tissue is blood? Blood is considered liquid connective
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: HEMATOLOGY Revised: 11/2013 What type of tissue is blood? Blood is considered liquid connective
Introduction reduction in output alter the amino acid sequence combination
 Sickle cell anemia. Introduction Mutations in the globin genes can cause a quantitative reduction in output from that gene or alter the amino acid sequence of the protein produced or a combination of the
Sickle cell anemia. Introduction Mutations in the globin genes can cause a quantitative reduction in output from that gene or alter the amino acid sequence of the protein produced or a combination of the
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
PATIENT SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR PATIENTS. Before starting on Soliris Important safety information for patients
 PATIENT SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR PATIENTS Before starting on Soliris Important safety information for patients Before you begin Soliris (eculizumab) treatment, your physician will
PATIENT SAFETY BROCHURE; IMPORTANT SAFETY INFORMATION FOR PATIENTS Before starting on Soliris Important safety information for patients Before you begin Soliris (eculizumab) treatment, your physician will
Iron Overload in Sickle Cell Disease Review of Cause and Treatment
 Iron Overload in Sickle Cell Disease Review of Cause and Treatment Susan M. Carson RN, MSN, CPNP Nurse Practitioner III Hematology Program Children s Hospital Los Angeles Objectives Describe the effect
Iron Overload in Sickle Cell Disease Review of Cause and Treatment Susan M. Carson RN, MSN, CPNP Nurse Practitioner III Hematology Program Children s Hospital Los Angeles Objectives Describe the effect
Treating acute painful sickle cell episodes in hospital
 Understanding NICE guidance Information for people who use NHS services Treating acute painful sickle cell episodes in hospital NICE clinical guidelines advise the NHS on caring for people with specific
Understanding NICE guidance Information for people who use NHS services Treating acute painful sickle cell episodes in hospital NICE clinical guidelines advise the NHS on caring for people with specific
Sickle Cell Disease Patient Handbook
 Sickle Cell Disease Patient Handbook , Important Contact Information Office/Unit Phone Number: Outpatient Clinic: 708.684.3898 Make an appointment: 708.684.3113 Please leave a message and a receptionist
Sickle Cell Disease Patient Handbook , Important Contact Information Office/Unit Phone Number: Outpatient Clinic: 708.684.3898 Make an appointment: 708.684.3113 Please leave a message and a receptionist
Instructor s Manual Chapter 26 Hematological Alterations. 1. A man and woman both test positive for the sickle cell trait. The couple asks the
 1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
RBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
Sickle Cell Disease: How Should YOU Reassess Management & Treatment?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/changing-conversation-sickle-cell-disease/sickle-cell-disease-howshould-you-reassess-management-treatment/10184/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/changing-conversation-sickle-cell-disease/sickle-cell-disease-howshould-you-reassess-management-treatment/10184/
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Peri-Operative Management: Guidelines for Inpatient Management of Children with Sickle Cell Disease
 Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
DIC. Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated.
 Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
Miss. kamlah 1 DIC Disseminated intravascular coagulation, is a life threatening pathological process in which clotting factors are abnormally activated. Resulting in wide spread of clot formation in the
MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT
 MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT MAC PS 2013-002 Appropriate treatment of acute pain in the prehospital arena offers an opportunity to positively impact many patients.
MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT MAC PS 2013-002 Appropriate treatment of acute pain in the prehospital arena offers an opportunity to positively impact many patients.
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet)
 NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet) ASSESSMENT Prior to administration: Obtain complete health history including allergies, drug history, and possible drug interactions.
NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet) ASSESSMENT Prior to administration: Obtain complete health history including allergies, drug history, and possible drug interactions.
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Cycle 1 PERTuzumab (day 1) and trastuzumab (day 2) loading doses: Drug Dose BC Cancer Administration Guideline
 BC Cancer Protocol Summary for Palliative Therapy for Metastatic Breast Cancer Using PERTuzumab, Trastuzumab (HERCEPTIN), and PACLItaxel as First-Line Treatment for Advanced Breast Cancer Protocol Code:
BC Cancer Protocol Summary for Palliative Therapy for Metastatic Breast Cancer Using PERTuzumab, Trastuzumab (HERCEPTIN), and PACLItaxel as First-Line Treatment for Advanced Breast Cancer Protocol Code:
Before starting on Soliris.
 Before starting on Soliris. Important safety information for patients Before you begin Soliris (eculizumab) treatment, your physician will give you a: Medication Guide Soliris Patient Safety Information
Before starting on Soliris. Important safety information for patients Before you begin Soliris (eculizumab) treatment, your physician will give you a: Medication Guide Soliris Patient Safety Information
DOSING GUIDE. Indications. Important Safety Information. Enable the immune system. RECOGNIZE. RESPOND.
 DOSING GUIDE For patients with unresectable Stage III NSCLC following concurrent CRT For patients with locally advanced or metastatic UC previously treated with platinum-based therapy Enable the immune
DOSING GUIDE For patients with unresectable Stage III NSCLC following concurrent CRT For patients with locally advanced or metastatic UC previously treated with platinum-based therapy Enable the immune
Unrestricted. Dr ppooransari fellowship of perenatalogy
 Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
ARTICLE. Intravenous Ketorolac in the Emergency Department Management of Sickle Cell Pain and Predictors of Its Effectiveness
 ARTICLE Intravenous Ketorolac in the Emergency Department Management of Sickle Cell Pain and Predictors of Its Effectiveness James L. Beiter, Jr, MD; Harold K. Simon, MD; C. Robert Chambliss, MD; Thomas
ARTICLE Intravenous Ketorolac in the Emergency Department Management of Sickle Cell Pain and Predictors of Its Effectiveness James L. Beiter, Jr, MD; Harold K. Simon, MD; C. Robert Chambliss, MD; Thomas
DONE BY : RaSHA RAKAN & Bushra Saleem
 DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Hydroxyurea Treatment for Sickle Cell Disease
 Hydroxyurea Treatment for Sickle Cell Disease Before Hydroxyurea After Hydroxyurea Hydroxyurea Treatment for Sickle Cell Disease This document is not intended to take the place of the care and attention
Hydroxyurea Treatment for Sickle Cell Disease Before Hydroxyurea After Hydroxyurea Hydroxyurea Treatment for Sickle Cell Disease This document is not intended to take the place of the care and attention
Sound View Acupuncture and Chinese Herbs 5410 California Ave SW, #202, Seattle, WA
 Sound View Acupuncture and Chinese Herbs 5410 California Ave SW, #202, Seattle, WA 98136 206.200.3595 Today s date Name Legal name (if different) Phone (primary) (secondary) Address City State Zip Email
Sound View Acupuncture and Chinese Herbs 5410 California Ave SW, #202, Seattle, WA 98136 206.200.3595 Today s date Name Legal name (if different) Phone (primary) (secondary) Address City State Zip Email
Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests. CBC, Electrolytes, Urea, Creatinine, Glucose, INR, PTT, Urinalysis
 of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Use of abatacept in rheumatoid arthritis - patient information
 Practical management of patients receiving abatacept 1 Use of abatacept in rheumatoid arthritis - patient information Evidence-based Medicine Official Recommendations Expert opinion Key points 1. Abatacept
Practical management of patients receiving abatacept 1 Use of abatacept in rheumatoid arthritis - patient information Evidence-based Medicine Official Recommendations Expert opinion Key points 1. Abatacept
To provide guidelines for the identification, management and reporting of a suspected transfusion reaction to Transfusion Medicine Laboratory (TML).
 PURPOSE To provide guidelines for the identification, management and reporting of a suspected transfusion reaction to Transfusion Medicine Laboratory (TML). SITE APPLICABILITY BC Children s Hospital and
PURPOSE To provide guidelines for the identification, management and reporting of a suspected transfusion reaction to Transfusion Medicine Laboratory (TML). SITE APPLICABILITY BC Children s Hospital and
BJF Acute Pain Team Formulary Group
 Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
Routine Clinic Lab Studies
 Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals
 Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals Suzanne A Nesbit, PharmD, CPE Clinical Pharmacy Specialist, Pain Management The Johns Hopkins Hospital Objectives and Disclosures
Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals Suzanne A Nesbit, PharmD, CPE Clinical Pharmacy Specialist, Pain Management The Johns Hopkins Hospital Objectives and Disclosures
Sickle Cell Anemia. Sickle cell anemia is an inherited disorder of the blood which occurs when just one base pair substitution
 Rose Farrington and Rachel Nash BIOL 362 Lab M. Bulgarella Genetic Diseases 10/14/2008 Sickle Cell Anemia Introduction Sickle cell anemia is an inherited disorder of the blood which occurs when just one
Rose Farrington and Rachel Nash BIOL 362 Lab M. Bulgarella Genetic Diseases 10/14/2008 Sickle Cell Anemia Introduction Sickle cell anemia is an inherited disorder of the blood which occurs when just one
Anna s Death - Organizer. by: Lindsay Markworth
 Anna s Death - Organizer by: Lindsay Markworth Anna s Cause of Death Ketoacidosis leads to diabetic coma death cells don t get enough glucose due to lack of insulin body goes to stored fats for energy
Anna s Death - Organizer by: Lindsay Markworth Anna s Cause of Death Ketoacidosis leads to diabetic coma death cells don t get enough glucose due to lack of insulin body goes to stored fats for energy
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase: Pediatric Spine Surgery General Orders
 - Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
- Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Care of School Age Children with Sickle Cell Disease. Lesley Ann Owen, RN, MSN Vanderbilt Children s Hospital Pediatric Sickle Cell Clinic
 Care of School Age Children with Sickle Cell Disease Lesley Ann Owen, RN, MSN Vanderbilt Children s Hospital Pediatric Sickle Cell Clinic Sickle cell disease around the world African Americans Latin Americans
Care of School Age Children with Sickle Cell Disease Lesley Ann Owen, RN, MSN Vanderbilt Children s Hospital Pediatric Sickle Cell Clinic Sickle cell disease around the world African Americans Latin Americans
Blood Transfusion Guidelines in Clinical Practice
 Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
UNDERSTANDING CYSTIC FIBROSIS
 UNDERSTANDING CYSTIC FIBROSIS INTRODUCTION Cystic fibrosis is a chronic disease that affects the respiratory and gastrointestinal systems. People with cystic fibrosis have a genetic defect of the lungs
UNDERSTANDING CYSTIC FIBROSIS INTRODUCTION Cystic fibrosis is a chronic disease that affects the respiratory and gastrointestinal systems. People with cystic fibrosis have a genetic defect of the lungs
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC
 RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
Pediatrics. Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment. Definition. Epidemiology of Pyruvate Kinase Deficiency.
 Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
POLICY and PROCEDURE
 Misericordia Community Hospital Administration of Intravenous FentaNYL During Labour POLICY and PROCEDURE Labour and Delivery Manual Original Date Revised Date Approved by: Director, Women s Health, Covenant
Misericordia Community Hospital Administration of Intravenous FentaNYL During Labour POLICY and PROCEDURE Labour and Delivery Manual Original Date Revised Date Approved by: Director, Women s Health, Covenant
