Cervicothoracic radiculopathy treated using posterior cervical foraminotomy/discectomy
|
|
|
- Anastasia Bates
- 5 years ago
- Views:
Transcription
1 J Neurosurg (Spine 2) 98: , 2003 Cervicothoracic radiculopathy treated using posterior cervical foraminotomy/discectomy JAMES S. HARROP, M.D., MARCO T. SILVA, M.D., ASHWINI D. SHARAN, M.D., STEVEN J. DANTE, M.D., AND FREDERICK A. SIMEONE, M.D. Department of Neurosurgery, Thomas Jefferson University, Philadelphia, Pennsylvania Object. The authors conducted a study to identify the effectiveness and morbidity rate associated with treating cervicothoracic disc disease (radiculopathy) via a posterior approach. Methods. Nineteen patients underwent posterior cervicothoracic laminoforaminotomy during a 5.6-year period. Medical records, imaging studies, office charts, hospital records, and phone interview data were reviewed. Specific information analyzed included patient demographics, side of lesion, and conservative treatment, symptoms, and preand postoperative pain levels. Pain was rated using a visual analog scale and classified into a radicular and neck component. Data in 19 patients (seven women and 12 men) who underwent 20 procedures (one patient underwent separate bilateral foraminotomies) were analyzed. The mean patient age was 54.8 years (range years), and the follow-up period ranged from 23 to 62 months. Symptom duration ranged from 1 to 14 months (mean 3.4 months) and consisted of weakness, numbness, and painful radiculopathies in 11, 16, and 20 cases, respectively. Motor weakness was identified in 11 of 19 patients (mean grade of 4.35), and postoperatively strength normalized in eight of 11 (mean grade of 4.79). The improvement in motor scores was significant (p = 0.007). Pain was the most common presenting symptom. Preoperative radiculopathies were rated between 0 and 10 (mean 7.45), and postoperatively scores were reduced to 0 to 3 (mean 0.2) which was significant (p ). Preoperative neck pain was rated between 0 and 8 (mean 2.55), and on follow up ranged from 0 to 2 (mean 0.5), which was also significant (p = 0.001). Conclusions. Posterior cervicothoracic foraminotomy was a safe and effective procedure in the treatment of patients with laterally located disc herniations. KEY WORDS cervicothoracic spine foraminotomy posterior approach radiculopathy discectomy A NTERIOR cervical decompression with fusion has become the chosen surgical therapy for the treatment of cervical radiculopathy after failure of conservative therapy. An anterior cervical exposure is more difficult at the extremes of the cervical spine. In particular, the caudal cervical spine is confined by large vascular structures, the esophagus, pharynx, trachea, sternum, and the thoracic rib cage. This region is also the transition zone from the thoracic kyphosis to the cervical lordosis, making bone fusion difficult because of a biomechanical disadvantage. An alternative treatment option in this region is a posterior cervical foraminotomy alone or with a concurrent discectomy. To access the efficiency and safety of such approach, we retrospectively analyzed data obtained in a relatively large group of patients with cervicothoracic radiculopathy in whom surgery was performed via a posterior approach only. J. Neurosurg: Spine / Volume 98 / March, 2003 Clinical Material and Methods Patient Population Nineteen patients were treated with posterior laminoforaminotomy for either lateral disc herniation or foraminal stenosis between July 1995 and February All patients were evaluated by the senior authors (F.A.S. and S.J.D.) and were offered surgery when clinical symptoms correlated with findings on appropriate neuroimaging studies and after conservative therapy failed or when they presented with acute motor loss of hand function. During the initial evaluation, if myelopathy due to congenital cervical stenosis with a lordotic cervical spine was found, cervical laminectomy and concurrent foraminotomy were performed. No patients had sustained work-related injuries, were involved in Worker s compensation cases, or had legal representation concerning their lesions. All medical records and imaging studies were reviewed. Data were also collected through office charts, hospital records, and phone interviews. Specific information analyzed included patient demographics, side of lesion, conservative therapy regimen, symptoms (numbness and weakness), and pre- and postoperative pain levels. Pain was assessed using a visual analog scale. Pain was also divided into a radicular and isolated neck component. Muscle strength was graded using a six-point (0 5) scale. 12 Operative reports were also reviewed to determine 131
2 J. S. Harrop, et al. side of operation, number of foramina decompressed, and whether a foraminotomy or discectomy was performed. Operative Technique General anesthesia was induced, and a Mayfield threepin head holder was applied. After positioning the patient prone on laminectomy rolls, the head was secured to the bed in a slightly flexed position. The knees were flexed and supported caudally, allowing the operating table to be placed at an approximately a 30 incline. A detailed description of the positioning has been previously reported. 19 A midline incision (~2.5 cm/level) was made over the affected interspace, and the paraspinal muscles were dissected in a subperiosteal manner. Attention was paid to preserving the interspinous ligaments. Intraoperative radiography confirmed the correct anatomical localization. A key-hole laminotomy was then made, which permitted palpation of the superior and inferior pedicles. The operating microscope was brought into the surgical field, and a high-speed drill was used to thin the bone over the exiting nerve root, prior to its removal by using a curved curette. Approximately one third of the medial facet joint was removed, leaving at least 50% in place. After the vascular cuff was identified, the sleeve was coagulated and divided using microsurgical technique. Once the vascular cuff was opened, the microscope provided clear visualization of both the motor and sensory divisions of cervical nerve. With microdissection, the lateral disc herniation was identified. If the herniated disc was soft, then the posterior ligament was opened and the lesion removed. The decision to open the cuff was made intraoperatively after the osseous component of the foraminotomy was performed. In cases of large disc herniations, the cuff was opened; in smaller ones, palpation of the nerve intraoperatively determined if the cuff required opening. Once the vascular cuff was opened, the nerve was gently retracted cephalad with a Rhoton No. 6 Penfield knife. Using a No. 11 blade, the disc was incised and removed using a Decker pituitary and rosen knife. When the nerve was confirmed to be decompressed, the wound was closed in layers. Statistical Analysis Statistical analysis was performed using univariate methods (chi-square, Fisher exact, and t-tests). A probability value of 0.5 was set for statistical significance. All calculations were performed using the Statview statistical computer software package (SAS, Cary, NC). Literature Review A detailed literature search was performed of the Medline database (1966 present). The following text words were used: cervicothoracic, cervical spine, foraminotomy, and discectomy. The results of these searches, along with the key references from the identified articles and known references on the subject material were reviewed. Results Twenty-one patients who were treated for degenerative cervicothoracic disease were identified (Table 1). Two patients were excluded from analysis because medical and operative records were deficient. Data in the remaining 19 patients (7 women, 12 men) who underwent 20 procedures (in one patient bilateral foraminotomies were performed at separate intervals) were analyzed. The followup period ranged from 17 to 62 months. Patients ranged in age from 38 to 73 years (mean 54.8 years). Eleven patients suffered left-sided radiculopathies and nine right-sided lesions. Onset of symptoms varied between 1 and 14 months (mean 3.4) and consisted of weakness, numbness, and painful radiculopathies in 11, 16, and 20 of 20 cases, respectively. Numbness was localized to the fourth and fifth digits; third, fourth, and fifth digits; and second, third, fourth, and fifth digits in 11, two, and one of 16 patients, respectively. The paresthesias resolved in nine of 16 patients. Seven patients suffered persistent numbness after the decompression, but their status was improved over preoperative condition. The two patients with the most severe numbness also suffered severe motor weakness. Motor weakness (mean score of 4.35) was initially identified in 11 of 19 patients, and noted to be immediately ( 1 week) and completely improved postoperatively in eight (73%) of the patients with weakness (mean score of 4.79) (p = 0.007). Of the four patients with persistent weakness, a delayed recovery occurred in two. The two patients with lingering weakness initially exhibited antigravity strength (Grade 3/5), and this improved in one to Grade 4/5 strength. No patient experienced greater weakness as a result of the decompressive surgery. In seven patients appreciable atrophy of the first dorsal interosseous muscle was observed. Pain was the most common presenting symptom. Preoperative radiculopathies were rated between 0 (no pain) and 10 (intractable pain), and the mean score was Postoperatively the scores decreased to between 0 to 3 (mean 0.2) (p ). Preoperative axial neck pain was rated between 0 and 8 (mean 2.55), and on follow-up examination ranged from 0 to 2 (mean 0.5) (p = 0.001). Statistical analysis of data regarding the patient s age, sex, level of operative treatment, side, motor status, pain symptoms, atrophy, and conservative treatment regimen compared with operative procedure (a foraminotomy alone or a combined foraminotomy/discectomy) demonstrated no positive or negative predictive factors. There was, however, a correlation between the duration of symptoms and treatment (p = 0.035); the mean presentation prior to surgical intervention for a foraminotomy was 4.9 months whereas it was only 2.1 months for those who underwent foraminotomy and concurrent discectomy. In the present series there were no superficial or deep infections. One patient underwent a second operation performed by a different surgeon 4 years after his previous surgery. This consisted of a four-level anterior C2 5, which was entirely cranial to the original posterior operation from which the patient noted complete resolution of symptoms. The second operation was not performed as a revision surgery but instead for new degenerative symptoms. One of the four patients who underwent a cervical laminectomy, instrumentation-augmented fusion, and concurrent foraminotomies developed a sudden onset of left-hand intrinsic weakness. This occurred 7 days after the original operation. Plain, flexion, and extension radiographs demonstrated no remarkable findings. Cervical 132 J. Neurosurg: Spine / Volume 98 / March, 2003
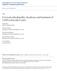
3 Posterior cervical foraminotomy/discectomy TABLE 1 Summary of data obtained in patients undergoing procedures for cervicothoracic radiculopathy* Pain Score Radicular Neck Motor Score Numbness Case Age (yrs), Duration Lamin- No. Sex Side Level(s) Surgery (mos) Preop Postop Preop Postop Preop Postop Preop Postop ectomy 1 52, F lt C7 T1 disc yes no no 2 51, F lt C7 T1 form yes no yes F rt C6 T1 disc yes no no 3 59, M rt C5 T1 form yes yes no 4 61, M lt C6 T1 form yes no no 5 40, M rt C7 T1 disc yes no no 6 73, F rt C7 T1 form yes no no 7 51, M lt C6 T1 disc no no no 8 73, F lt C7 T1 form yes yes no 9 48, M lt C7 T1 disc yes yes no 10 69, M rt C7 T1 disc yes no no 11 62, M lt C6 T1 disc no no no 12 60, M rt T1-2 disc yes no no 13 55, F rt T1-2 disc no no no 14 58, M lt C6 T1, T-12 form yes yes yes 15 38, F lt C6 T1 disc yes yes no 16 39, M lt C7 T1 form no yes no 17 42, M rt C7 T1 disc yes no no 18 70, M rt C6 T1 form yes no yes 19 44, M lt C5 T1 form yes yes yes * disc = discectomy; form = foraminotomy. myelography and postmyelography computerized tomography scanning demonstrated only thinning of the C-7 nerve root, whereas the C8 T1 nerve roots had no filling defects. The patient underwent surgical reexploration, and no nerve root compression was observed. The patient s hand function completely recovered and the cause of the weakness was proposed to be vascular in nature, related to his underlying small vessel disease secondary to diabetes. All patients underwent clinical and radiographic follow-up examination. Although the follow-up period has been brief, no cervical instability or cervical deformity has been demonstrated in any case. Discussion There have been numerous descriptions of procedures for treating cervical radiculopathy via an anterior 9,10,25,34,35 or posterior 1,7,14,18,19,33 approach. Mixter and Barr 26 first reported the posterior approach for resection of lumbar and cervical disc herniations. Their technique was modified by Scoville, et al., 33 Fager, 14 and Guanciale. 18 Recently, there have been additional variations of these procedures involving use of the endoscope 1,7 or a transpedicular route. 18 Cervicothoracic disc herniations and radiculopathies are uncommon. In several large clinical series authors have reported the incidence to be only between 4 and 7%. 1,33,37 There has been no study to address specifically the surgical treatment of this disorder via a posterior approach. In our study, therefore, we have examined this uncommon condition s symptoms and clinical outcomes and will discuss the advantages of a posterior over an anterior approach in the cervicothoracic spine. J. Neurosurg: Spine / Volume 98 / March, 2003 Symptoms of Cervicothoracic Lesion Acute or intractable pain is the major presenting symptom in patients with a monoradiculopathy. 1,21,27,32,33,37 Most patients in our series suffered painful radiculopathies (19 of 20 cases); additionally patients also presented with concurrent hand intrinsic weakness (11 cases) or numbness (16 cases) due to compression of the C-8 or T-1 nerve roots (Figs. 1 and 2). Axial neck pain was present in the majority of cases but was a minor component (mean score of 2) and was most likely secondary to muscle spasms. The T1 2 disc herniations are extremely rare (Fig. 2). Murphey, et al., 27 noted that these lesions represented less than 1% in their series of 648 patients. These patients, contrary to those with C7 T1 lesions, present with more severe hand intrinsic weakness and less pain. In the present series, all three patients with the T1 2 compression presented with atrophy of the first dorsal interosseous muscle, and the two patients with soft-disc herniations also had a Froment sign. Although others 27 have suggested the presence of a Horner syndrome with cervicothoracic disc disease, no patient in this series sustained appreciable sympathetic dysfunction. Clinical Outcome Our clinical results correlate with those reported in other large series of posterior cervical foraminotomy in which outcome of good/excellent recovery ranged from 90 to 100%. 1,2,21,27,33,36,37 In our series there was a reduction in the radicular component of pain, the most common presenting symptom, from a mean score of 7.45 to 0.2 (p ). Improvement in motor function also occurred, as indicated by a mean increase from 4.35 to 4.79 (p 0.007). Henderson, et al., 21 reported the largest series, 133
4 J. S. Harrop, et al. FIG. 2. Imaging studies obtained in a 55-year-old woman who presented with severe radicular pain and weakness of the right hand intrinsic muscles. Upper: Preoperative sagittal T 2 -weighted MR image revealing a large lateral T1 2 disc herniation (arrow). Lower: Axial images demonstrating a lateral disc protrusion. FIG. 1. Imaging studies obtained in a 52-year-old woman who presented with severe neck and radicular pain. Upper: Preoperative sagittal T 2 -weighted magnetic resonance (MR) image illustrating a large C7 T1 disc herniation (arrow). Lower: Axial T 2 - weighted MR image demonstrating no spinal cord compression and the disc fragment occluding the left C-8 foramen (arrow). accrued during 17 years, consisting of 736 patients (846 procedures); radicular symptoms were relieved in 96% and motor defects were resolved in 98%. In their series, no surgery included removal of the herniated disc, and only foraminotomies were performed. Although the goal of surgery was to treat the radicular pain and motor weakness, there was also a statistical correlation in the reduction of axial neck pain (p = ) from a mean score of 2.55 to 0.5, which is in agreement with our series. Herkowitz, et al., 22 performed the only prospective study, which consisted of 33 patients. Seventeen patients were randomized to undergo an anterior procedure and 16 to a posterior decompression. Although a good/excellent result was associated with 85% of the anterior procedures and only 75% of the posterior foraminotomies, the difference was not statistically significant. The authors should be commended for the study. They concluded, however, that anterior discectomy and fusion is the recommended procedure for the surgical management of a cervical anterolateral disc herniation. This is not supported by the results obtained in our study. Anterior cervical discectomy and fusion also is reported to be associated with excellent relief of postoperative pain and neurological deficits. Gore and Sepic 17 have reported a 96% improvement in symptoms in 146 patients. Disc herniations situated more laterally, however, can be difficult to decompress anteriorly because of limited access and visibility. In an anatomical study, Raynor 30 found that, via a posterior decompression, between 3 and 5 mm of the cervical nerve root can be visualized, whereas only 1 to 2 mm can be appreciated via a standard anterior approach. Additionally, through a posterior approach multiple nerve roots can be decompressed simultaneously without requiring complex cervicothoracic anterior reconstruction. Biomechanical Factors Historically, posterior-approach cervical decompressive surgery has been thought to result in cervical instability and the formation of a kyphotic or swan-neck deformity. This was believed to be the result of excessive resection of the facet joints after laminectomy. Investigators of several in vitro studies have shown that the cervical spine maintains its stability if less than 50% of the facet joint is resected bilaterally after laminectomy. 8,31,38 Zdeblick, et al., 38 demonstrated that with less than 50% resection of the facet joint strain, torsional stiffness, and flexion were maintained. These studies involved bilateral laminectomy and removal of the facet joints, whereas typically in cases of a posterior foraminotomy only a unilateral procedure is performed and only a minor portion of the facet is removed. If greater than 50% destruction of the facets is required, then the motion segment may require stabilization with posterior fusion. 134 J. Neurosurg: Spine / Volume 98 / March, 2003
5 Posterior cervical foraminotomy/discectomy Anterior procedures, in contrast, are typically performed in conjunction with fusion. The distraction provided by the bone graft allows the neural foramen to be opened wider and causes the posterior longitudinal ligament to become stretched, reducing any buckling. The elimination of posterior ligamentous buckling theoretically increases the size of the spinal canal. Anterior fusion has been shown to reduce motion by 50 to 100%, 8 which may improve axial neck pain. This, however, may result in increased stresses on the adjacent vertebral segments. 23,24 Hilibrand, et al., 23 have shown that 10 years after cervical interbody fusion 19% of their patients suffered accelerated adjacent-level degeneration. Procedure-Related Complications Posterior cervical foraminotomy is a safe procedure associated with a very low rate of complications (0 4%). 1,2, 21,37 The greatest complications are wound infections or serous drainage. 21,22 Other complications include cerebrospinal fluid leakage secondary to a dural puncture, wound hematomas, and, rarely, transient or permanent nerve root symptoms. An anterior cervical operation requires dissection around soft tissue and vascular structures. Inadvertent traction or dissection can lead to esophageal perforations, 29 vertebral artery injury, 16 pneumothorax, 11 Horner syndrome (due to injured sympathetic nerves), 3,13 and tracheal/laryngeal injury or dysfunction. 4,9,15,20 These laryngeal/tracheal injuries can lead to dysphonia, hoarseness, dysphagia, and aspiration. 28 The reported rates of vocal cord paralysis after anterior cervical spine surgery have been reported between 0.98 and 3% for permanent paralysis, 6,11,20 and 1.7 and 11% for temporary vocal cord injury. 4,20,28 Finally, via either approach the nerve root and spinal cord may also be transiently or permanently injured. Typically, after completion of the anterior discectomy a bone graft is placed, with or without instrumentation, to enhance a fusion. This can be accomplished using autograft or allograft. Allograft is associated with the theoretical risk of transmitting an infection from the donor. Autograft harvest as well can be associated with significant pain and infection. Boockvar, et al., 5 reported a 36% rate of graft/ plate failure after anterior reconstruction at the cervicothoracic junction. This is most likely due to a biomechanical disadvantage created by the transition from the cervical lordosis to a thoracic kyphosis along with a lesser exposure resulting from anatomical constraints. To date in our series, no patient has developed cervicothoracic kyphosis, but further long-term follow-up data are necessary. Conclusions Although posterior foraminotomy is an established treatment, this technique has not been specifically reported on for application in the cervicothoracic region. The procedure can be performed with minimal risks and achieves excellent outcomes, while not exposing the patient to the infrequent but numerous complications of an anterior procedure at the cervicothoracic junction. Acknowledgment The authors thank Edward Benzel, M.D., for his thorough review and revisions of earlier versions of this manuscript. J. Neurosurg: Spine / Volume 98 / March, 2003 References 1. Adamson TE: Microendoscopic posterior cervical laminoforaminotomy for unilateral radiculopathy: results of a new technique in 100 cases. J Neurosurg (Spine 1) 95:51 57, Aldrich F: Posterolateral microdiscectomy for cervical monoradiculopathy caused by posterolateral soft disc sequestration. J Neurosurg 72: , An HA, Vaccaro A, Cotler JM, et al: Spinal disorders at the cervicothoracic junction. Spine 19: , Apfelbaum RI, Kriskovich MD, Haller JD: On the incidence, cause, and prevention of recurrent laryngeal nerve palsies during anterior cervical spine surgery. Spine 25: , Boockvar JA, Philips MF, Telfeian AE, et al: Results and risk factors for anterior cervicothoracic junction surgery. J Neurosurg (Spine 1) 94:12 17, Bulger RF, Rejowski JE, Beatty RA: Vocal cord paralysis associated with anterior cervical fusion: considerations for prevention and treatment. J Neurosurg 62: , Burke TG, Caputy A: Microendoscopic posterior cervical foraminotomy: a cadaveric model and clinical application for cervical radiculopathy. J Neurosurg (Spine 1) 93: , Chen BH, Natarajan RN, An HS, et al: Comparison of biomechanical response to surgical procedures used for cervical radiculopathy: posterior keyhole foraminotomy versus anterior foraminotomy and discectomy versus anterior discectomy and fusion. J Spinal Disord 14:17 20, Cloward R: New methods of diagnosis and treatment of cervical disc disease. Clin Neurosurg 8:93 123, Cloward RB: The anterior approach for removal of ruptured cervical disks. J Neurosurg 15: , Cloward RB: Complications of anterior cervical disc operation and their treatment. Surgery 69: , Ditunno JF, Young W, Donovan WH, et al: The international standards booklet for neurological and functional classification of spinal cord injury. American Spinal Injury Association. Paraplegia 32:70 80, Ebraheim NA, Lu J, Yang H, et al: Vulnerability of the sympathetic trunk during the anterior approach to the lower cervical spine. Spine 25: , Fager CA: Management of cervical disc lesions and spondylosis by posterior approaches. Clin Neurosurg 24: , Flynn TB: Neurologic complications of anterior cervical interbody fusion. Spine 7: , Golfinos JG, Dickman CA, Zabramski JM, et al: Repair of vertebral artery injury during anterior cervical decompression. Spine 19: , Gore DR, Sepic SB: Anterior cervical fusion for degenerated or protruded discs. A review of one hundred forty-six patients. Spine 9: , Grundy PL, Germon TJ, Gill SS: Transpedicular approaches to cervical uncovertebral osteophytes causing radiculopathy. J Neurosurg (Spine 1) 93:21 27, Guanciale AF: Positioning for posterior cervical spine surgery, in Dillin WH, Simeone FA (eds): Posterior Cervical Spine Surgery. Philadelphia: Lippincott-Raven, 1998, pp Heeneman M: Vocal cord paralysis following approaches to the anterior cervical spine. Laryngoscope 83:17 21, Henderson CM, Hennessy RG, Shuey HM Jr, et al: Posteriorlateral foraminotomy as an exclusive operative technique for cervical radiculopathy: a review of 846 consecutively operated cases. Neurosurgery 13: , Herkowitz HN, Kurz LT, Overholt DP: Surgical management of cervical soft disc herniation. A comparison between the anterior and posterior approach. Spine 15: , Hilibrand AS, Yoo JU, Carlson GD, et al: The success of anterior cervical arthrodesis adjacent to a previous fusion. Spine 22: ,
6 J. S. Harrop, et al. 24. Hunter LY, Braunstein EM, Bailey RR: Radiographic changes following anterior cervical fusion. Spine 5: , Jho HD: Microsurgical anterior cervical foraminotomy for radiculopathy: a new approach to cervical disc herniation. J Neurosurg 84: , Mixter WJ, Barr JS: Rupture of the intervertebral disc with involvement of the spinal canal. N Engl J Med 211: , Murphey F, Simmons JC, Brunson B: Surgical treatment of laterally ruptured cervical disc. Review of 648 cases, J Neurosurg 38: , Netterville JL, Koriwchak MJ, Winkle M, et al: Vocal fold paralysis following the anterior approach to the cervical spine. Ann Otol Rhinol Laryngol 105:85 91, Newhouse KE, Lindsey RW, Clark CR: Esophageal perforation following anterior cervical spine surgery. Spine 14: , Raynor RB: Anterior or posterior approach to the cervical spine: an anatomic and radiographic evaluation and comparison. Neurosurgery 12:7 13, Raynor RB, Pugh J, Shapiro I: Cervical facetectomy and its effect on spine strength. J Neurosurg 63: , Rodrigues MA, Hanel RA, Prevedello DMS, et al: Posterior approach for soft cervical disc herniation: a neglected technique? Surg Neurol 55:17 22, Scoville WB, Dohrmann GJ, Corkill G: Late results of cervical disc surgery. J Neurosurg 45: , Smith GW, Robinson RA: The treatment of cervical spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg (Am) 40: , Tascioglu AO, Attar A, Tascioglu B: Microsurgical anterior cervical foraminotomy (uncinatectomy) for cervical disc herniation. Report of three cases. J Neurosurg (Spine 1) 94: , Williams RW: Microcervical foraminotomy. A surgical alternative for intractible radicular pain. Spine 8: , Woertgen C, Holzschuh M, Rothoerl RD, et al: Prognostic factors of posterior cervical disc surgery: a prospective, consecutive study of 54 patients. Neurosurgery 40: , Zdeblick TA, Zou D, Warden KE, et al: Cervical stability after foraminotomy. A biomechanical in vitro analysis. J Bone Joint Surg Am 74:22 27, 1992 Manuscript received May 6, Accepted in final form December 11, Address reprint requests to: James Harrop, M.D., 909 Walnut Street, Third Floor, Philadelphia, Pennsylvania EJHarrop@aol.com. 136 J. Neurosurg: Spine / Volume 98 / March, 2003
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Comparison of Surgical Results between Soft Ruptured Disc and Foraminal Stenosis Patients in Posterior Cervical Laminoforaminotomy
 CLINICAL ARTICLE Korean J Neurotrauma 2017;13(2):124-129 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2017.13.2.124 Comparison of Surgical Results between Soft Ruptured Disc and Foraminal
CLINICAL ARTICLE Korean J Neurotrauma 2017;13(2):124-129 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2017.13.2.124 Comparison of Surgical Results between Soft Ruptured Disc and Foraminal
Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University, Wakayama, JAPAN
 SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients
 Original Article 7 Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients Author Y. Ş. Ça ǧ lar1, M. Bozkurt 1, G. Kahilogullari 1, H. Tu na 1, A. Bakir 2, F. To r u n 1, H. C. U
Original Article 7 Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients Author Y. Ş. Ça ǧ lar1, M. Bozkurt 1, G. Kahilogullari 1, H. Tu na 1, A. Bakir 2, F. To r u n 1, H. C. U
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
1. Introduction: 3. Surgical Procedures. 2. Indications. 3.a. Surgical Instruments. 3.b. Patient Positioning. 3.c. Surgical Technique
 1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Anthem Blue Cross and Blue Shield Central Region Clinical Claim Edit
 Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
Use of the operating microscope anterior cervical discectomy without fusion. KEY WORDS 9 cervical discectomy 9 fusion 9 intervertebral disc
 Use of the operating microscope anterior cervical discectomy without fusion in HAL L. HANKINSON, M.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California School of
Use of the operating microscope anterior cervical discectomy without fusion in HAL L. HANKINSON, M.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California School of
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy
 Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Codes for Back and Spinal Procedures
 20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Case Report Two-year follow-up results of artificial disc replacement C7-T1
 Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Cervical Motion Preservation
 Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury
 J Neurosurg Spine 4:273 277, 2006 Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury CRAIG KILBURG, HUMBERT G. SULLIVAN, M.D., AND
J Neurosurg Spine 4:273 277, 2006 Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury CRAIG KILBURG, HUMBERT G. SULLIVAN, M.D., AND
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Cervical Spine in Baseball
 Cervical Spine in Baseball Robert G Watkins, IV, MD Co-Director, Marina Spine Center Marina del Rey, CA Vice Chief of Staff Cedars-Marina del Rey Hospital Disclosures n Pioneer / RTI Consulting, Royalties
Cervical Spine in Baseball Robert G Watkins, IV, MD Co-Director, Marina Spine Center Marina del Rey, CA Vice Chief of Staff Cedars-Marina del Rey Hospital Disclosures n Pioneer / RTI Consulting, Royalties
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set
 Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set Benzel, E ISBN-13: 9781437705874 Table of Contents SECTION 1 - HISTORY 1 - History 2 - History of Spine Instrumentation -
Spine Surgery: Techniques, Complication Avoidance, and Management. 2 Volume Set Benzel, E ISBN-13: 9781437705874 Table of Contents SECTION 1 - HISTORY 1 - History 2 - History of Spine Instrumentation -
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
History. Symptoms and Signs. Spine
 Spine A Review of Laminoforaminotomy For The Management of Lateral and Foraminal Cervical Disc Herniations or Spurs Nancy E. Epstein, M.D. Clinical Professor of Neurological Surgery, The Albert Einstein
Spine A Review of Laminoforaminotomy For The Management of Lateral and Foraminal Cervical Disc Herniations or Spurs Nancy E. Epstein, M.D. Clinical Professor of Neurological Surgery, The Albert Einstein
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases Han Jo Kim Weill Cornell Medical
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases Han Jo Kim Weill Cornell Medical
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Spine Tango annual report 2012
 DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
Endoscopic transpedicular thoracic discectomy
 Neurosurg Focus 6 (5):Article 1, 1999 Endoscopic transpedicular thoracic discectomy Hae-Dong Jho, M.D., Ph.D. Department of Neurological Surgery, University of Pittsburgh School of Medicine, Pittsburgh,
Neurosurg Focus 6 (5):Article 1, 1999 Endoscopic transpedicular thoracic discectomy Hae-Dong Jho, M.D., Ph.D. Department of Neurological Surgery, University of Pittsburgh School of Medicine, Pittsburgh,
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Fixation of multiple level anterior cervical disc using cages versus cages and plating
 Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose
 Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries.
 Coding/Billing By Kim Pollock, MS, RN, MBA, CPC Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries. It seems like coding spine cases is as complicated
Coding/Billing By Kim Pollock, MS, RN, MBA, CPC Procedure Coding Made Simple Five principles will help you capture appropriate charges for spine surgeries. It seems like coding spine cases is as complicated
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
PART III IN HOSPITAL ON CALL ANESTHESIA COVERAGE
 Anesthesia g) A consultation may not be claimed where the patient is referred to the anesthetist for the sole purpose of providing post-operative Patient Controlled Analgesia. h) Tariff 8406 may not be
Anesthesia g) A consultation may not be claimed where the patient is referred to the anesthetist for the sole purpose of providing post-operative Patient Controlled Analgesia. h) Tariff 8406 may not be
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
The Spinal Column Biomechanics and Surgical Outcomes Laboratory, and 2 Department of Neurosurgery, Johns Hopkins Hospital, Baltimore, Maryland
 DOI: 10.3171/2014.7.SPINE131110 AANS, 2014 Long-term patient outcomes after posterior cervical foraminotomy: an analysis of 151 cases Clinical article *Mohamad Bydon, M.D., 1,2 Dimitrios Mathios, M.D.,
DOI: 10.3171/2014.7.SPINE131110 AANS, 2014 Long-term patient outcomes after posterior cervical foraminotomy: an analysis of 151 cases Clinical article *Mohamad Bydon, M.D., 1,2 Dimitrios Mathios, M.D.,
Long term prognosis of young adults after ACDF
 Long term prognosis of young adults after ACDF Tuomas Hirvonen MD 1,2 Johan Marjamaa MD, PhD 1,2 Jari Siironen MD, PhD 1 Anniina Koski-Palkén MD, PhD 1 1 Department of Neurosrugery, Helsinki University
Long term prognosis of young adults after ACDF Tuomas Hirvonen MD 1,2 Johan Marjamaa MD, PhD 1,2 Jari Siironen MD, PhD 1 Anniina Koski-Palkén MD, PhD 1 1 Department of Neurosrugery, Helsinki University
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc
 Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc The patient services department (PSD) supports LSI patients post surgery. Herniated Disc searching for the most effective solution
Post Operative Care Following Spinal Surgery For A Cervical Herniated Disc The patient services department (PSD) supports LSI patients post surgery. Herniated Disc searching for the most effective solution
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy and fusion
 Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Intra-operative neurologic injuries: Avoidance and prompt response
 Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
Thoracic disc herniation: Postero-lateral approach
 Thoracic disc herniation: Postero-lateral approach Antonino Raco MD Professor and Chairman of Neurosurgery Department of Neurosciences, Mental Health and Sense Organs (NESMOS), Sapienza Università di Roma
Thoracic disc herniation: Postero-lateral approach Antonino Raco MD Professor and Chairman of Neurosurgery Department of Neurosciences, Mental Health and Sense Organs (NESMOS), Sapienza Università di Roma
Orthopedic Coding Changes for 2012
 Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
New York Science Journal 2017;10(8)
 Outcome of surgical intervention with different modalities in treatment of lumbar canal stenosis. Ahmed Mohamed Shaker Eidarous Elakhras 1, Ahmed M. El Sherif 2 and Mostafa Elsyed Mohamed 3 1 Neurosurgical
Outcome of surgical intervention with different modalities in treatment of lumbar canal stenosis. Ahmed Mohamed Shaker Eidarous Elakhras 1, Ahmed M. El Sherif 2 and Mostafa Elsyed Mohamed 3 1 Neurosurgical
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Upper limb involvement in cervical spondylosis
 Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 386-390 DOUGLAS G. PHILLIPS From the Department of Neurological Surgery, Frenchay Hospital, Bristol SYNOPSIS Analysis of 200 cases reveals
Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 386-390 DOUGLAS G. PHILLIPS From the Department of Neurological Surgery, Frenchay Hospital, Bristol SYNOPSIS Analysis of 200 cases reveals
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES
 REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
Assessment of Anterior Cervical Discectomy
 Original Article Assessment of Anterior Cervical Discectomy Ali Reza Zali, Afsaneh Zarghi, MD, MPH, PhD, Amir Saied Seddighi,MD, Ahmadreza Rajabi, MD, Reza Khoshnoud Jalili, MD Functional Neurosurgery
Original Article Assessment of Anterior Cervical Discectomy Ali Reza Zali, Afsaneh Zarghi, MD, MPH, PhD, Amir Saied Seddighi,MD, Ahmadreza Rajabi, MD, Reza Khoshnoud Jalili, MD Functional Neurosurgery
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
This procedure lacks scientific evidence of effectiveness, and is not covered.
 ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
UPPER CERVICAL RADICULOPATHY: THE HIDDEN PATHOLOGY OF THE SPINE
 REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH UPPER CERVICAL RADICULOPATHY: THE HIDDEN PATHOLOGY OF THE SPINE Grant D. Shifflett 1), Sravisht Iyer 2), Peter B. Derman 2), Philip K. Louie 2) and Howard
REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH UPPER CERVICAL RADICULOPATHY: THE HIDDEN PATHOLOGY OF THE SPINE Grant D. Shifflett 1), Sravisht Iyer 2), Peter B. Derman 2), Philip K. Louie 2) and Howard
The Artificial Cervical Disc: 2016 update
 The Artificial Cervical Disc: 2016 update Anthony K. Frempong-Boadu, MD Associate Professor Co-Director NYU Langone Spine Center Director - Division of Spinal Surgery Department of Neurosurgery New York
The Artificial Cervical Disc: 2016 update Anthony K. Frempong-Boadu, MD Associate Professor Co-Director NYU Langone Spine Center Director - Division of Spinal Surgery Department of Neurosurgery New York
