CHRONIC PELVIC PAIN OF BLADDER ORIGIN:
|
|
|
- Warren Byrd
- 5 years ago
- Views:
Transcription
1 ACCREDITATION This activity has been planned and implemented in accordance with the Essential Areas and policies of the Accreditation Council for Continuing Medical Education through the joint sponsorship of the Dannemiller Memorial Educational Foundation and SynerMed Communications. The Dannemiller Memorial Educational Foundation is accredited by the ACCME to provide continuing medical education for physicians. Vol. 22 No. 34 November 2004 ISSN DESIGNATION OF CREDIT The Dannemiller Memorial Educational Foundation designates this educational activity for a maximum of 1 category 1 credit toward the AMA Physician s Recognition Award. Each physician should claim only those credits that he/she actually spent in the activity. Release date: November 2004 Expiration date for credit: November 30, 2005 CHRONIC PELVIC PAIN OF BLADDER ORIGIN: A Focus on Interstitial Cystitis Case Studies PRESENTED BY U.S. Department of Health and Human Services The Office on Women s Health IN COOPERATION WITH American Medical Women s Association American Urogynecologic Society National Association of Nurse Practitioners in Women s Health Jointly sponsored by Dannemiller Memorial Educational Foundation and SynerMed Communications. DANNEMILLER MEMORIAL EDUCATIONAL FOUNDATION This activity is made possible by an educational grant provided by Ortho-McNeil Pharmaceutical, Inc.
2 STATEMENT OF NEED Interstitial cystitis is commonly misdiagnosed in women as overactive bladder, recurrent urinary tract infection, or endometriosis; in men it is often mistaken for prostatitis. The impact of interstitial cystitis on a patient s quality-of-life is significant these women score lower on QOL inventories than do dialysis patients; in men, the impact is comparable to that of patients with myocardial infarction, angina, or Crohn s disease. Therefore, effective diagnostic methods, understanding of epidemiology and demographics, and proper identification of nonpharmacologic and pharmacologic options are necessary for the management of interstitial cystitis. METHOD OF PARTICIPATION This newsletter should take approximately 1 hour to complete. The participant should, in order, read the objectives and newsletter, answer the 10-question multiple-choice post-test, placing answers on the Registration/Posttest Answer Form/Evaluation on page 6. The evaluation form provides each participant with the opportunity to comment on the quality of the instructional process, the perception of enhanced professional effectiveness, the perception of commercial bias, and his or her views on future educational needs. To receive credit for this activity, follow the instructions provided on the posttest and evaluation form. This credit will be valid through November 30, No credit will be given after that date. STEERING COMMITTEE EDUCATIONAL OBJECTIVES Upon completion of this program, participants will be able to: Differentiate between chronic pain of pelvic origin versus bladder origin Discuss the epidemiology and demographics of chronic pelvic pain and interstitial cystitis Discuss the current theories regarding the underlying pathophysiology of interstitial cystitis Discuss the impact of interstitial cystitis and chronic pelvic pain on quality of life Describe the evolving role of the Pelvic Pain Urgency and Frequency Patient Symptom Scale, Potassium Sensitivity Test, and other diagnostic tools in identifying patients with interstitial cystitis Identify nonpharmacologic and pharmacologic options for the management of interstitial cystitis TARGET AUDIENCE Obstetrician/gynecologists, urologists, family physicians, nurse practitioners, and physician assistants. Jean L. Fourcroy, MD, PhD, MPH Assistant Professor/Urology Uniformed Services University of the Health Sciences Walter Reed Army Hospital Bethesda, Maryland Wanda K. Jones, DrPH Deputy Assistant Secretary for Health Office on Women's Health Department of Health and Human Services Washington, DC Daniel R. Mishell Jr, MD Lyle G. McNeile Professor and Chairman Department of Obstetrics & Gynecology Keck School of Medicine Los Angeles County & University of Southern California Women s & Children s Hospital Los Angeles, California C. Lowell Parsons, MD Professor of Surgery/Urology School of Medicine University of California, San Diego San Diego, California FACULTY DISCLOSURE STATEMENTS The Dannemiller Memorial Educational Foundation requires that the faculty participating in a continuing medical education activity disclose to participants any significant financial interest or other relationship (1) with the manufacturer(s) of any commercial product(s) and/or provider(s) of commercial services discussed in an educational presentation, or (2) with any commercial supporters of the activity. The presenting faculty reported the following: Wanda K. Jones, DrPH No financial or other relationship. Jean L. Fourcroy, MD, PhD, MPH No financial or other relationship. Daniel R. Mishell Jr, MD Speaker s Bureau: Ortho McNeil Pharmaceutical, Inc. C. Lowell Parsons, MD Consultant/Scientific Advisor: Ortho-McNeil Pharmaceutical, Inc. Discussion of Off-Label/Investigational Uses of Pharmaceutical Products: This educational activity may contain discussion of published and/or investigational uses of agents that are not indicated by FDA. The opinions expressed in the educational activity are those of the faculty. Please refer to the official prescribing information for each product for discussion of approved indications, contraindications, and warnings. Further, attendees should appraise the information presented critically and are encouraged to consult appropriate resources for any product or device mentioned in this program. The content and views presented in this educational activity are those of the authors and do not necessarily reflect those of the Dannemiller Memorial Educational Foundation, the US Department of Health and Human Services Office on Women s Health; the American Medical Women s Association; the American Urogynecologic Society; the National Association of Nurse Practitioners in Women s Health; SynerMed Communications, or the program grantor, Ortho-McNeil Pharmaceutical, Inc. This material is prepared based on a review of multiple sources of information, but is not exhaustive of the subject matter. Therefore, healthcare professionals and other individuals should review and consider other publications and materials on the subject matter before relying solely on the information contained within this educational activity.
3 ACCREDITATION This activity has been planned and implemented in accordance with the Essential Areas and policies of the Accreditation Council for Continuing Medical Education through the joint sponsorship of the Dannemiller Memorial Educational Foundation and SynerMed Communications. The Dannemiller Memorial Educational Foundation is accredited by the ACCME to provide continuing medical education for physicians. Vol. 22 No. 34 November 2004 ISSN DESIGNATION OF CREDIT The Dannemiller Memorial Educational Foundation designates this educational activity for a maximum of 1 category 1 credit toward the AMA Physician s Recognition Award. Each physician should claim only those credits that he/she actually spent in the activity. Release date: November 2004 Expiration date for credit: November 30, 2005 CHRONIC PELVIC PAIN OF BLADDER ORIGIN: A FOCUS ON INTERSTITIAL CYSTITIS CASE STUDIES INTRODUCTION Interstitial cystitis (IC) causes the symptoms of a chronic pelvic pain syndrome (CPPS) of bladder origin that is estimated to affect as many as 1 in 4.5 women. 1 IC causes the symptoms of chronic pelvic pain (CPP) and urinary urgency and frequency, but is frequently misdiagnosed as endometriosis, recurrent urinary tract infection (UTI), or overactive bladder (OAB) (Figure 1). During this past decade there has been a greater understanding of the probable underlying pathophysiology of IC, as well as significant advances in the diagnosis and management of this cause of CPPS. Consequently, clinicians now have techniques to identify and effectively treat women with IC early in the process of this disease. Refractory Patients Recurrent UTI Symptoms Failed ABS Overactive Bladder Treatment Failures Concurrent Endometriosis and/or Failed Medical Treatment FIGURE 1 HOW TO CONSIDER AN IC PATIENT Consider IC New Patients Urgency Frequency Pain - Dyspareunia This is the second of 2 issues of Clinical Courier that will focus on the assessment and management of IC in women. The objective of this activity is to provide practical information and guidelines that can be utilized to expedite the care provided to patients who experience symptoms of CPP that are eventually determined to be of bladder origin. The first issue examined 2 cases of IC that were initially diagnosed as endometriosis. In this issue, 2 case studies of women with bladder-related diagnoses will be presented and reviewed. OVERVIEW AND MAGNITUDE OF THE PROBLEM In March 2004, the American College of Obstetricians and Gynecologists (ACOG) issued a Practice Bulletin about CPP, which was defined as noncyclic pain of 6 or more months duration that localizes to the anatomic pelvis, abdominal wall at or below the umbilicus, lumbosacral back, or the buttocks and is of sufficient severity to cause functional disability or lead to medical care. 2 The origin of the pain can be genitourinary, gastrointestinal, reproductive, psychologic, or neurologic. It was noted that the severity of the pain is not necessarily associated with physical findings. A common cause of CPP is IC, described by ACOG as a chronic inflammatory condition of the bladder characterized by irritative voiding symptoms of urgency and frequency in the absence of objective evidence of another disease that could cause the symptoms. 2 IC symptoms can range from mild and intermittent pelvic pain with infrequent nighttime nocturia ( 2 times per night) to debilitating pain and frequent nighttime nocturia (>12 times per night). Although the exact incidence of IC is unknown, the ACOG Practice Bulletin estimated that 38% to 85% of women seeking gynecologic care for CPP may have IC. 2 A recent study suggested that as many as 1 in 4.5 women has IC. 1 IC is most typically diagnosed in white women of reproductive age. While the majority of women first notice symptoms of IC during their 30s, there is usually a delay of 5 to 8 years before an accurate diagnosis is established, resulting in an age range at diagnosis of 42 to 46 years. 3,4 Women consult an average of 5 to 8 healthcare professionals before receiving the correct diagnosis of IC; this problem has been attributed to a lack of understanding that the bladder is a common source of pelvic pain and the fact that there are many similarities in the clinical presentations of IC and endometriosis, UTI, and OAB. 3 Women with any of the causes of CPPS can experience dyspareunia, premenstrual flares, and diet-related exacerbations, further confounding the ability to make a correct diagnosis. PATHOPHYSIOLOGY Currently there are 3 main components of the pathogenesis of IC, and all of these components may occur in the same patient. The predominant etiologic factor is based upon the belief that patients with IC have an elevated pain response to urine solutes because of damage to the glycosaminoglycan (GAG) layer of the bladder surface. This damage results in leakage and transvesical absorption of urea and potassium into the interstitium of the bladder. In a healthy bladder, the GAG layer (mucus) prevents absorption of caustic components of urine into the bladder wall and inhibits bladder infections by preventing bacteria from adhering to urothelial surfaces. Trauma to, or a deficiency in, the GAG layer results in bladder wall exposure to potassium, resulting in tissue damage and pain, as well as urinary urgency and frequency, which are characteristic of IC. 5 However, pain can also occur in the absence of actual tissue damage. 1
4 In addition to damage or alterations to the GAG layer, it is also believed that when IC is present in the bladder wall there is neurogenic inflammation with activation of C-fibers and the release of the neuropeptic substance P (SP), as well as increased mast cell activation. Patients with IC have an increased number of C-fibers (pain-carrying nerves) that carry and release SP from sensory nerve endings. SP transmits pain information, stimulates inflammation, and can trigger mast-cell secretion, especially in the bladder submucosa. 6 Mast cells are located predominantly in the detrusor layer, in the lamina propia, and the bladder epithelium. Inside mast cells are granules that contain histamines; when the mast cells degranulate, histamines are abnormally released, causing inflammation. It has been hypothesized that this process may be responsible for the initial insult or damage to the GAG layer. In summary, the pathogenesis of IC appears to be a vicious cycle involving depletion of the GAG layer, mast cell activation with histamine release, and C-fiber activation and release of SP (Figure 2). 7 The epithelial dysfunction can affect tissue beyond the bladder wall; therefore, IC is not an end-organ disease but a visceral pain syndrome with neuropathic up-regulation as a key component. TABLE 1 DIAGNOSIS OF IC Patient History + Clinical Presentation Urinalysis and Culture Bladder Cytology Voiding Log Physical Exam PUF Patient Symptom Scale PST as appropriate Cystoscopy With Hydrodistention - only if gross/ microscopic hematuria is present More Inflammation Mast Cell Activation and Histamine Release FIGURE 2 PATHOGENESIS OF IC 7 IC is Characterized by a Vicious Cycle With Increased Symptomology With Increasing Age Bladder Insult Activation of C-fibers and Release of Substance P Epithelial Layer Dysfunction Potassium Leak Into Interstitium Adapted with permission from Evans RJ. Rev Urol. 2002;4(suppl 1):S16-S20. DIAGNOSIS The diagnosis of IC is a clinical process. There are no gross histologic changes associated with IC, nor are there, as yet, laboratory assays or biomarkers to assist in establishing the diagnosis. IC has been a diagnosis of exclusion, ruling out infection (UTI or bladder, vaginal, or sexually transmitted), endometriosis, and bladder cancer. It was originally believed that the diagnosis of IC could be made only when Hunner s ulcers, observed through cystoscopy with hydrodistention, were present. However, recent studies have reported that fewer than 10% of patients with IC have a Hunner s ulcer. 8 Consequently, the diagnosis depends upon patient history, presenting signs and symptoms, and negative laboratory results (negative urinalysis, sterile urine culture, and normal urinary cytology) (Table 1). It is the recommendation of the editorial faculty performing cystoscopy with hydrodistention is currently recommended only for women with gross or microscopic hematuria to rule out abnormalities of the urethral or bladder surface, or for older women who smoke and have other risk factors for bladder cancer. In summary, IC should be suspected to be present in all women with CPP and urinary urgency/frequency in the absence of observed pathologic changes including women with refractory UTI who have failed antibiotics, women with refractory OAB who have failed anticholinergic treatment, and women with persistent symptoms of endometriosis who have not responded to the usual medical and surgical therapies. Women with IC frequently have suprapubic tenderness, anterior vaginal wall/bladder base tenderness, and/or rectal or levator muscle spasm during a physical examination. The physical exam can rule out vaginitis, vulvodynia, urethral diverticula, uterovaginal prolapse, and pelvic floor dysfunction. Complaints of pelvic pain are common, especially as the disease progresses. The pain can be referred to the urethra, vagina, lower abdomen, lower back, medial aspect of the thigh, inguinal region, or vulva. Some women may require additional diagnostic tests, such as an intravenous pyelogram, transvaginal ultrasound, and cystometrogram with uroflow examination. Women often report that emotional or physical stress, certain foods, and seasonal allergies exacerbate their IC symptoms. Two recent additions to the diagnostic armamentarium include the Pelvic Pain Urgency and Frequency (PUF) Patient Symptom Scale and the Potassium Sensitivity Test (PST). The PUF is an 8-question symptom scale that can be completed in the office in approximately 5 minutes; it quantifies the presence and severity of the symptoms of frequency, urgency, and pain, and includes 2 questions assessing symptoms following sexual activity (Figure 3, page 6). The maximum score on the PUF is 35 points; a high score, which is considered to be 10 points, indicates a high probability that the patient has IC. Nearly all healthy women have low PUF scores ( 2 points). The PUF has been shown to readily distinguish IC from other abdomenopelvic conditions, including UTI and gynecologic CPP. Patients with PUF scores >10 points have been shown to have a 74% likelihood of IC. 1 Further, patients with PUF scores of 5 to 10 points have been shown to have a 55% likelihood of IC. It is recommended that the PUF scale should be routinely applied to all women with CPP, and women with a PUF score of 5 points should be suspected of having IC and managed accordingly. The second advancement in the IC diagnostic process is the PST, a test that identifies patients who respond with pain and/or urgency to the introduction of a potassium solution into the bladder. Approximately 80% of patients with IC have a positive PST result. 9 It should be noted that a positive PST occurs when there is abnormal epithelial permeability, so other diseases with the symptom of an abnormal mucosa will also cause a positive PST, for example, acute bacterial cystitis and radiation cystitis. Similarly, a negative PST does not always rule out IC. Women who have recently undergone hydrodistention, heparin treatment, or bladder instillation of dimethyl sulfoxide (DMSO), or patients taking pain medication can have false negative results. Nevertheless and often with alternative initial diagnoses approximately 85% of gynecology patients with CPP have a positive PST. 1,10 The PST involves the very slow introduction into the bladder of 2 separate solutions through a thin catheter. First, 40 ml of room temperature sterile 2
5 water is slowly instilled to assess the patient s baseline of pain perception and urgency upon bladder filling. The patient is asked to rate this experience using a 0- to 5-point scale, with 5 indicating the most severe pain. The water should be retained in the bladder for about 5 minutes before it is emptied through the catheter. Then, 40 ml of a potassium chloride (KCl) solution is instilled and retained for up to 5 minutes; the patient then evaluates the severity of pain/urgency with the KCl. Any increase of 2 or more points over the baseline point with sterile water indicates a positive PST result. Less than a 2 point difference in pain or urgency with the KCI solution compared with the sterile water solution is considered a negative PST result. Women who do not initially respond to the KCl instillation but who have other signs and symptoms of IC should have the catheter removed and the bladder emptied, after which a second KCI solution is instilled. There is a strong correlation between a positive PST result and high PUF scores. 1 Ninety-one percent of patients with a PUF score >20 have a positive PST, as do 76% of patients with a PUF score of 15 to 19 and 55% of patients with a PUF score of 5 to 9. 1 Healthy women usually have 0% positive PST results and PUF scores <2. The high correlation between the PUF and PST suggests that the PUF can be used as an initial diagnostic screening test to identify women with CPP who are highly likely to have IC, reserving the PST for women whose symptoms are suggestive of IC but who have lower PUF scores (5 to 10 points). MANAGEMENT Until the approval by the US Food and Drug Administration (FDA) of oral pentosan polysulfate sodium (PPS), intravesical instillation with DMSO was the only therapy indicated for the management of IC. Intravesical instillation with DMSO provides moderate relief of the pain and urinary symptoms of IC The procedure involves passing 50 ml of a 50% aqueous solution of DMSO through a catheter into the bladder, where it is retained for up to 15 minutes before being expelled. 14,15 DMSO instillations can be performed in the office or at home by the patient on a weekly or biweekly schedule for a treatment course of 6 to 8 weeks. The procedure can be painful, and the process can leave a garlic-like taste and/or odor on the breath or skin for up to 3 days after treatment. 15 The mechanism of action is as yet unknown. Patients receiving DMSO instillations are advised to undergo blood and eye testing, including kidney and liver function tests, every 6 months. 16 Symptoms often recur after treatment with DMSO, and additional courses of therapy are needed to ensure duration of remissions. 17 DMSO therapy is being used less frequently now than previously. PPS is the only oral drug approved by the FDA for the management of the pain and urinary symptoms of IC. 18 PPS is a heparin-like compound similar in chemistry and structure to the naturally occurring GAGs that overlie the urinary epithelium (Table 2) It is believed that PPS acts by gradually and methodically repairing the defective GAG layer, thus providing a buffer to control cell permeability and preventing irritating solutes from reaching uroepithelial cells. The FDA-recommended dosage of oral PPS is 300 mg/d taken as a 100-mg capsule 3 times daily; an evolving regimen to enhance patient compliance utilizes 200 mg taken twice daily. 24,25 The recommended course duration is 2 to 4 months for women with mild disease, and 6 to 12 months or more for women with moderate to severe disease, as there is a long duration between initiation of therapy and relief of symptoms. 20 PPS is a well-tolerated agent with no known drug-drug interactions. 18 The efficacy of PPS for reducing the symptoms of IC has been demonstrated in numerous clinical trials. 22,26,27 PPS reduces the pelvic pain and pressure to void, and has been shown to increase bladder capacity (volume per void). PPS also significantly reduces potassium sensitivity as measured by the PST. 28 Finally, a dose ranging study demonstrated that symptomatic improvement increased with duration of therapy but not with increased dosage (Figure 4). 28 A wide range of adjunctive pharmacologic and nonpharmacologic therapies can be used to augment the primary treatment of IC. Analgesics, including acetaminophen with codeine, can provide pain relief. Anticholinergics and antispasmodics are recommended for patients with OAB symptoms, and antihistamines are recommended for patients with allergic flares. Tricyclic antidepressants, particularly amitriptyline, are often recommended at bedtime to promote pain relief. Amitriptyline also inhibits histamine secretion from mast cells. Because this agent can cause constipation and cardiac irregularities, treatment with amitriptyline should be initiated at the lowest dosage and slowly titrated up to the dose that provides the greatest symptom relief without adverse effects. 29 Although not approved by the FDA for IC, intravesical instillation of a heparin solution has been used as monotherapy and in combination with DMSO to provide prompt relief of pain and to enhance the duration of clinical remissions. 30,31 A unique intervention for women with severe IC symptoms is an anesthetic intravesical rescue solution (not FDA approved). The anesthetic solution provides immediate, although temporary, relief of urgency and pain symptoms. These therapeutic cocktails are composed of either PPS (1 or mg capsules dissolved in 10 cc of buffered normal saline or heparin (10,000 to Percentage of Patients FIGURE 4 PPS SYMPTOMATIC IMPROVEMENT INCREASES WITH DURATION OF TREATMENT 28 4 >50% Overall Improvement on PORIS* PPS 300 mg/d Weeks *PORIS = Patient s Overall Rating of Improvement of Symptoms index assessing, pain, urgency, frequency, and nocturia. Completers. TABLE 2 PENTOSAN POLYSULFATE SODIUM The only FDA-approved oral therapy for management of IC Proven effective in multicenter randomized trials with placebo 19,20 Resembles protective GAG layer that insulates bladder lining against urine 21 Reduces painful symptoms/provides long-term remissions 22 Provides relief of IC pain in many patients in 3 to 6 months 18 Some patients experience pain relief in only 4 weeks 23 Trend of PPS (300 mg/d)
6 40,000 units) as the active agent in combination with 3 cc of 8.4% sodium bicarbonate and 10 cc of 1% lidocaine or 16 cc of 2% lidocaine. 30,32,33 The solution is instilled into an empty bladder using a small catheter while the woman assumes a dorsal lithotomy position. The solution is held in the bladder for up to 30 minutes or until the patient needs to void. Clinical investigators suggest a series of 9 anesthetic solutions (3 per week for 3 weeks, or 3 during the first week and 1 per week for the next 6 weeks) to provide maximal pain relief and to facilitate reductions in urinary urgency. This regimen may be continued for additional weeks if needed. Nonpharmacologic interventions are rarely sufficient as monotherapy for IC. The most common nonpharmacologic interventions include diet modification, bladder-training techniques (often in conjunction with relaxation and distraction techniques) to increase the interval between voids, and pelvic floor relaxation exercises. Anecdotal reports indicate that avoiding foods high in acidity and those containing caffeine, potassium, or artificial sweeteners can have a beneficial effect on IC pain. Behavioral therapies such as bladdertraining techniques, are most effective for women with mild-to-moderate IC, but can also be of benefit to women with more severe symptoms. Other recommendations include taking hot sitz baths and applying a heating pad to the perineal area prior to, and ice packs after, sexual intercourse. CASE STUDY Case Study 1: The Patient With Recurrent UTI A 25-year old white female was treated 12 times in 2 years for UTI prior to referral. She presented with symptoms of urinary frequency, pelvic pain, and dyspareunia. History of Present Illness Patient 1 had a 2-year history of treatment for recurrent UTI-type symptoms, including 12 courses of antimicrobial agents (including trimethoprim sulfamethoxazole, nitrofurantoin monohydrate/macrocrystals, ciprofloxacin, and levofloxacin) and 2 urethral dilatation procedures. Most of the treatments had been initiated after phone triage her urine was examined only once during the 2 years. Her complaints of dyspareunia and chronic pelvic pain were regarded as related to the presumptive UTI diagnosis. During the initial visit, Patient 1 complained of urinary frequency and suprapubic pain and tenderness during intercourse. She reported that she was in a long-term, monogamous relationship but was afraid to commit to marriage as her problem with painful intercourse was worsening. She noted that her fiancé felt she was obsessed with her bladder after she admitted to him that she voided 18 to 20 times per day. Patient 1 also noted that she awoke 3 to 5 times each night to void. Physical Examination and Laboratory Findings Laboratory testing on Patient 1 found no urinary tract infection: results showed a negative urinalysis, sterile culture, and normal cytology. There was no evidence of vaginitis or sexually transmitted infection. Physical examination demonstrated suprapubic and perineal tenderness and bladder base tenderness. Current Diagnostic Assessment Patient 1 was given the PUF Patient Symptom Scale and scored 18. The clinician chose not to perform a PST. Cystoscopy with hydrodistention was not indicated because the patient had no risk factors for bladder cancer (she did not smoke and was young) and had no gross or microscopic hematuria. Short-Term Treatment Plan Patient 1 was given a presumptive diagnosis of IC and was placed on oral PPS (300 mg/d) and amitriptyline (25 mg at bedtime) (not indicated for IC). She was also started on an IC diet, on which she eliminated foods that contain caffeine, potassium, acidity, or artificial sweeteners, and began a pelvic muscle rehabilitation program with biofeedback. After 2 weeks of treatment, she reported good improvement in the pain and bladder symptoms; within 6 weeks of treatment initiation, she was having intercourse without pain. Follow-Up Patient 1 was seen on a monthly basis for the first year after being diagnosed with IC, and every 6 months thereafter. She was able to stop the amitriptyline after 8 months. She chose not to discontinue taking oral PPS, after a short trial without it caused a recurrence of pain and discomfort. She married her fiancé and became pregnant with her first child. Because PPS is a class B drug, the patient chose to continue taking it throughout her pregnancy. She adhered to a strict IC diet for 12 months, but eventually was able to return to a less restricted diet. She will continue to be seen every 6 months for management of IC after she has delivered her child. Discussion Women are frequently treated empirically for UTI without ever obtaining confirmation of a bacterial etiology. It is therefore common for women to receive numerous courses of antimicrobial therapy, often with different antimicrobial agents, without experiencing significant improvement in their CPP and bladder symptomatology. Case Study 2: The Patient Misdiagnosed With OAB A 32-year old lawyer has been treated by her family physician for OAB for the past 4 years. She complains of urinary frequency and urgency, reduced urinary output, and pelvic pain. History of Present Illness Patient 2 has been treated for OAB for the past 4 years with antimuscarinic agents, such as oxybutynin and tolterodine. These agents do not appear to be of benefit in fact, she reports increasing pain and urinary retention. She has no history of UTI or treatment for UTI, and no history of involuntary leakage of urine. The increased number of voiding episodes and pelvic pain was interfering with her ability to work, and she noted that her social life was suffering because of these symptoms. Physical Examination and Laboratory Findings Patient 2 was asked to keep a voiding/bladder diary for 1 week, and to record the volume of urine for each voiding episode. The voiding log demonstrated that she was voiding 1 to 2 times per hour, with an average voided volume of 20 to 40 ml per void. She reported considerable pain when the void volume was 90 ml. On examination, her urine was clear with minimal postvoid residual urine. Pelvic examination found suprapubic tenderness to be present. Current Diagnostic Assessment The PUF was administered and Patient 2 scored 20. Her high PUF score, in addition to her history, negative laboratory findings, and clinical presentation suggested a presumptive diagnosis of IC. It was decided that the PST and cystoscopy with hydrodistention procedures were unnecessary at this time. Short-Term Treatment Plan Patient 2 was directed to stop taking the antimuscarinics. Oral PPS (300 mg/d) was initially prescribed. She was given a series of 9 intravesical anesthetic solutions over a 7-week period. She received instructions for bladder training techniques, where she learned to schedule her voids with the short-term goal (3 months) of voiding once every 3 hours. She was given written instructions regarding the IC diet. Follow-Up Patient 2 returned for follow-up at 3 months, 6 months, and 1 year after initiation of treatment. At 3 months, she reported a reduction in her pelvic pain, and her interval between voids had increased to nearly 2 hours. Her average voided volume had also increased, and she no longer reported significant discomfort 4
7 with larger voided volumes. She continued taking oral PPS for a total of 9 months, and was symptom-free by 1 year after initiation of treatment. Discussion Patient 2 was initially diagnosed with OAB and treated with antimuscarinic agents that did not address her underlying IC. While antimuscarinic agents may be of benefit to a small subset of women with IC, these drugs treat only the symptoms and not the disease process. Antimuscarinic agents should be used carefully as they can increase the pelvic pain and lead to urinary retention in some women. CONCLUSIONS IC is frequently misdiagnosed as either OAB or UTI, especially when no laboratory analyses are performed. All 3 conditions have similar presentations of pelvic pain with urinary urgency and frequency, but only UTIs have a bacterial etiology. It is therefore important for all women with this clinical presentation and absence of definitive pathology to be screened for IC using the PUF; women who score 5 points should be considered to have IC that should be addressed and treated accordingly. REFERENCES 1. Parsons CL, Dell J, Stanford EJ, et al. Increased prevalence of interstitial cystitis: previously unrecognized urologic and gynecologic cases identified using a new symptom questionnaire and intravesical potassium sensitivity. Urology 2002;60: ACOG Committee on Practice Bulletins - Gynecology. ACOG Practice Bulletin No. 51. Chronic pelvic pain. Obstet Gynecol 2004;103: Curhan GC, Speizer FE, Hunter DJ, Curhan SG, Stampfer MJ. Epidemiology of interstitial cystitis: a population based study. J Urol 1999;161: Propert KJ, Schaeffer AJ, Brensinger CM, et al. A prospective study of interstitial cystitis: results of longitudinal followup of the interstitial cystitis data base cohort. The Interstitial Cystitis Data Base Study Group. J Urol 2000;163: Parsons CL, Greenberger M, Gabal L, Bidair M, Barme G. The role of urinary potassium in the pathogenesis and diagnosis of interstitial cystitis. J Urol 1998;159: Pang X, Marchand J, Sant GR, Kream RM, Theoharides TC. Increased number of substance P positive nerve fibres in interstitial cystitis. Br J Urol 1995;75: Evans R. Treatment approaches for interstitial cystitis: multimodal therapy. Rev Urol 2002;4:S16-S Nigro DA, Wein AJ, Foy M, et al. Associations among cystoscopic and urodynamic findings for women enrolled in the Interstitial Cystitis Data Base (ICDB) Study. Urology 1997;49: Parsons CL. Prostatitis, interstitial cystitis, chronic pelvic pain, and urethral syndrome share a common pathophysiology: lower urinary dysfunctional epithelium and potassium recycling. Urology 2003; 62: Parsons CL, Bullen M, Kahn BS, Stanford EJ, Willems JJ. Gynecologic presentation of interstitial cystitis as detected by intravesical potassium sensitivity. Obstet Gynecol 2001;98: Stewart BH, Shirley SW. Further experience with intravesical dimethyl sulfoxide in the treatment of interstitial cystitis. J Urol 1976;116: Stout L, Gerspach JM, Levy SM, et al. Dimethyl sulfoxide does not trigger urine histamine release in interstitial cystitis. Urology 1995;46: Perez-Marrero R, Emerson LE, Feltis JT. A controlled study of dimethyl sulfoxide in interstitial cystitis. J Urol 1988;140: Barker SB, Matthews PN, Philip PF, Williams G. Prospective study of intravesical dimethyl sulphoxide in the treatment of chronic inflammatory bladder disease. Br J Urol 1987;59: Sant GR. Intravesical 50% dimethyl sulfoxide (Rimso-50) in treatment of interstitial cystitis. Urology 1987;29: RIMSO-50. Physicians Desk Reference. Montvale, NJ: Thomson PDR; p Ghoniem GM, McBride D, Sood OP, Lewis V. Clinical experience with multiagent intravesical therapy in interstitial cystitis patients unresponsive to single-agent therapy. World J Urol 1993;11: Elmiron. Physicians Desk Reference. 58th ed. Montvale, NJ: Thomson PDR; p Parsons CL. The therapeutic role of sulfated polysaccharides in the urinary bladder. Urol Clin North Am 1994;21: Parsons CL, Benson G, Childs SJ, et al. A quantitatively controlled method to study prospectively interstitial cystitis and demonstrate the efficacy of pentosan polysulfate. J Urol 1993;150: Hurst R, Roy J, Min K, et al. A deficit of chondroitin sulfate proteoglycans on the bladder uroepithelium in interstitial cystitis. Urology 1996; 48: Hanno PM. Analysis of long-term Elmiron therapy for interstitial cystitis. Urology 1997;49: Nickel JC, Forrest J, Barkin J, Payne C, Mosbaugh P. Safety and efficacy of up to 900 mg/day polysulfate sodium (Elmiron) in patients with interstitial cystitis. Urology 2001;57: Dell J, Parsons C. Intravesical instillation therapy using PPS in patients with interstitial cystitis. Poster presented at: Research Insights into Interstitial Cystitis. Alexandria, Virginia; October 30-November 1, Rosenberg M, Page S, Roth L, al. e. Pentosan polysulfate sodium for the treatment of interstitial cystitis: Rapid (1-month) and sustained symptom relief. Paper presented at: Research Insights into Interstitial Cystitis (A Basic and Clinical Science Symposium), October 30 November 1, 2003; Alexandria, Virginia. 26. Parsons CL, Mulholland SG. Successful therapy of interstitial cystitis with pentosan polysulfate. J Urol 1987;138: Mulholland SG, Hanno P, Parsons CL, Sant GR, Staskin DR. Pentosan polysulfate sodium for therapy of interstitial cystitis. A double-blind placebo-controlled clinical study. Urology 1990;35: Parsons CL, Forrest J, Nickel JC, et al. Effect of pentosan polysulfate therapy on intravesical potassium sensitivity. Urology 2002;59: Hanno PM. Amitriptyline in the treatment of interstitial cystitis. Urol Clin North Am 1994;21: Parsons CL, Housley T, Schmidt JD, Lebow D. Treatment of interstitial cystitis with intravesical heparin. Br J Urol 1994;73: Kuo HC. Urodynamic results of intravesical heparin therapy for women with frequency urgency syndrome and interstitial cystitis. J Formos Med Assoc 2001;100: Bade JJ, Laseur M, Nieuwenburg A, van der Weele LT, Mensink HJ. A placebo-controlled study of intravesical pentosan polysulfate for the treatment of interstitial cystitis. Br J Urol 1997;79: Parsons CL, Davis EL. Pentosan polysulfate sodium intravesical instillation: end-organ therapy. Practice Building Today. September 2003:
8 FIGURE 3 PELVIC PAIN AND URGENCY/FREQUENCY (PUF) PATIENT SYMPTOM SCALE Patient s Name: Today s date: Please circle the answer that best describes how you feel for each question SYMPTOM SCORE BOTHER SCORE 1 How many times do you go to the bathroom during the day? 2 a. How many times do you go to the bathroom at night? b. If you get up at night to go to the bathroom, does it bother you? 3 Are you currently sexually active? YES NO Never bothers Occasionally Usually Always 4 a. IF YOU ARE SEXUALLY ACTIVE, do you now or have you ever had pain or symptoms during or after sexual activity? b. If you have pain, does it make you avoid sexual activity? 5 Do you have pain associated with your bladder or in your pelvis (vagina, labia, lower abdomen, urethra, perineum, penis, testes, or scrotum)? 6 a. If you have pain, is it usually b. Does your pain bother you? 7 Do you still have urgency after you go to the bathroom? Mild Moderate Severe 8 a. If you have urgency, is it usually b. Does your urgency bother you? Mild Moderate Severe SYMPTOM SCORE (1, 2a, 4a, 5, 6a, 7, 8a) BOTHER SCORE (2b, 4b, 6b, 8b) TOTAL SCORE (Symptom Score + Bother Score) = Total score ranges are from 1 to 35. A total score of = 74% likelihood of positive PST; = 76%; 20+ = 91% Potassium Positive Printed with permission C. Lowell Parsons, M.D.
9 Editor: Clinical Courier SynerMed Communications Department Route 513 PO Box 458 Califon, NJ Presorted Standard US Postage PAID A&E Mailers Vol. 22 No. 34 IMPORTANT CME MATERIALS ENCLOSED 2004 SynerMed Communications (BBOP248E) All rights reserved Printed in USA
10 CHRONIC PELVIC PAIN OF BLADDER ORIGIN: A FOCUS ON INTERSTITIAL CYSTITIS CASE STUDIES Release date: November 2004 CME POSTTEST/REGISTRATION/EVALUATION (04-726D) Expiration Date for credit: November 30, 2005 Instructions: Please mark your answers on the Posttest Answer Form below. This activity should take approximately 1 hour to complete. The participant should, in order, read the educational objectives contained in this newsletter, answer the 10-question multiplechoice posttest, below, and complete the registration/evaluation form. If you wish to receive CME credit and a certificate, please mail/fax a copy of your completed answers to: If CME credit and a certificate are desired, please mail/fax this completed form or a copy of it to: Dannemiller Memorial Educational Foundation Attention: D 5711 Northwest Parkway, Suite 100, San Antonio, TX Fax (210) Phone: (800) Expiration date for credit: November 30, 2005 POSTTEST/SELF ASSESSMENT (Circle the single most appropriate answer below.) 1. IC is frequently misdiagnosed in women as: a. CPP due to abdominopelvic adhesions b. Vulvar dermatitis c. Recurrent UTI or OAB d. Pelvic inflammatory disease 2. The average age of IC diagnosis is: a years b years c years d years 3. The pain and urinary symptoms that characterize IC are most probably caused by: a. The presence of unusual organisms in bladder cells b. Damage to the GAG layer allowing bladder wall exposure to potassium c. Autoimmune processes d. All of the above 4. A PST should be performed on: a. All women with a history and clinical presentation suggestive of IC b. Women with suspected IC and a PUF score >10 c. Women with suspected IC and a PUF score between 5-10 d. All women who present with CPP 5. The PUF test measures: a. Epithelial permeability b. Bladder capacity c. The presence and severity of IC symptoms d. All of the above 6. The recommended course duration for treatment of moderate to severe IC with oral PPS is: a. 1 to 2 months c. 4 to 6 months b. 3 to 4 months d. 6 to 12 months 7. PPS is believed to act by: a. Preventing irritating solutes from reaching epithelial cells b. Providing a buffer to control cell permeability c. Replenishing the defective GAG layer d. All of the above 8. Which of the following is recommended for short-duration use to supplement oral PPS in women with severe IC? a. Intravesical instillations with DMSO b. Intravesical instillations with heparin c. Intravesical instillations with anesthetic rescue solutions d. Bladder training techniques 9. Women with IC will demonstrate which of the following during a pelvic examination? a. Perineal tenderness d. All of the above b. Suprapubic tenderness e. None of the above c. Bladder base tenderness 10. IC should be suspected in women with: a. Recurrent UTIs b. Recalcitrant OAB c. History or suspicion of endometriosis d. All of the above PROGRAM EVALUATION Full Name MD/DO/Other Street City State ZIP Code PHYSICIANS: Are you licensed in the US? (circle) YES or NO I certify that I completed this CME activity: The actual amount of time I spent in this activity was: hours minutes Signature Date Completed The Dannemiller Memorial Educational Foundation would appreciate your comments regarding the quality of the information presented. Later, via , we would also like to send you a website link to a follow-up survey regarding the material presented. May we contact you? (Please check one.) Yes, via . No, please do not contact me. 1. The program objectives were fully met. Strongly Agree Agree Disagree Strongly Disagree 2. The quality of the educational process (method of presentation and information provided) was satisfactory and appropriate. Strongly Agree Agree Disagree Strongly Disagree 3. The educational activity has enhanced my professional effectiveness to treat patients. Strongly Agree Agree Disagree Strongly Disagree NA 4. The educational activity will result in a change in my practice behavior. Strongly Agree Agree Disagree Strongly Disagree NA 5. The information presented was without promotional or commercial bias. Strongly Agree Agree Disagree Strongly Disagree (When answering this question, please refer to the following guidelines set forth by the ACCME regarding commercial bias and fair balance: Discussion of commercial products must be free of bias for or against any one product and must present objective information about each product discussed: only generic names of therapeutic options should be used, however if trades names are used, those of several companies must be discussed in the activity.) 6. Comments/suggestions regarding this material. 7. Recommendations for topics of future presentations.
In evaluating a patient with lower urinary tract symptoms (LUTS), urologists
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
DELAYED DIAGNOSIS. Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >60%
 DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
Bladder pain syndrome / Interstitial cystitis
 Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website:
 Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
INTERSTITIAL CYSTITIS (IC)
 INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
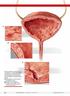 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective?
 Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Chronic Pelvic Pain of Bladder Origin: Interstitial Cystitis
 OBSTETRICS AND GYNECOLOGY BOARD REVIEW MANUAL STATEMENT OF EDITORIAL PURPOSE The Hospital Physician Obstetrics and Gynecology Board Review Manual is a peer-reviewed study guide for residents and practicing
OBSTETRICS AND GYNECOLOGY BOARD REVIEW MANUAL STATEMENT OF EDITORIAL PURPOSE The Hospital Physician Obstetrics and Gynecology Board Review Manual is a peer-reviewed study guide for residents and practicing
Edward L. Davis, Samar R. El Khoudary, Evelyn O. Talbott,* Josephine Davis and Lisa J. Regan
 Safety and Efficacy of the Use of Intravesical and Oral Pentosan Polysulfate Sodium for Interstitial Cystitis: A Randomized Double-Blind Clinical Trial Edward L. Davis, Samar R. El Khoudary, Evelyn O.
Safety and Efficacy of the Use of Intravesical and Oral Pentosan Polysulfate Sodium for Interstitial Cystitis: A Randomized Double-Blind Clinical Trial Edward L. Davis, Samar R. El Khoudary, Evelyn O.
CME/CE POSTTEST CME/CE QUESTIONS
 CME/CE POSTTEST CME/CE QUESTIONS Controlling Asthma Severity: Identifying Unmet Needs and Optimizing Therapeutic Options There are no fees for participating in and receiving continuing medical education
CME/CE POSTTEST CME/CE QUESTIONS Controlling Asthma Severity: Identifying Unmet Needs and Optimizing Therapeutic Options There are no fees for participating in and receiving continuing medical education
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC Department of Surgery, Division of Urology,
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS The Role of Pentosan Polysulfate in Treatment Approaches for Interstitial Cystitis Joel M.H. Teichman, MD, FRCSC Department of Surgery, Division of Urology,
Painful Bladder Syndrome
 Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
A Review on Interstitial Cystitis Syndrome (ICS)
 31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Interstitial Cystitis/ Bladder Pain Syndrome
 page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Citation for published version (APA): Bade, J. J. (1996). Interstitial cystitis: new clinical aspects Groningen: s.n.
 University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Interstitial cystitis Bade, Jurjen Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Interstitial Cystitis
 Clinical Communiqué Winter 2002 Interstitial Cystitis A Clinical Spectrum Jack Barkin, MD Chief of Urology, Humber River Regional Hospital, Toronto, Ontario Editorial Choosing the right treatment by J.
Clinical Communiqué Winter 2002 Interstitial Cystitis A Clinical Spectrum Jack Barkin, MD Chief of Urology, Humber River Regional Hospital, Toronto, Ontario Editorial Choosing the right treatment by J.
UroToday International Journal. Volume 2 - October 2009
 UroToday International Journal Robert J. Evans, 1 Jeffrey Proctor, 2 Robert M. Moldwin 3 1 Alliance Urology Specialists, Greensboro, NC; 2 Georgia Urology, Cartersville, GA; 3 The Arthur Smith Institute
UroToday International Journal Robert J. Evans, 1 Jeffrey Proctor, 2 Robert M. Moldwin 3 1 Alliance Urology Specialists, Greensboro, NC; 2 Georgia Urology, Cartersville, GA; 3 The Arthur Smith Institute
Interstitial cystitis (IC), also
 Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Interstitial Cystitis. Dr. Gerard Testa
 Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
Interstitial Cystitis
 J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 24-31 Review Article Interstitial Cystitis Satpathy Hemant K, Taylor Richert Department of Obstetrics and Gynecology, CUMC, Omaha, NE, USA,
J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 24-31 Review Article Interstitial Cystitis Satpathy Hemant K, Taylor Richert Department of Obstetrics and Gynecology, CUMC, Omaha, NE, USA,
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS)
 Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS) Ene G. George M.D., FACOG, FPMRS Kaiser Permanente Baldwin Park Division of Urogynecology Department of Obstetrics and Gynecology PBS/IC I have
Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS) Ene G. George M.D., FACOG, FPMRS Kaiser Permanente Baldwin Park Division of Urogynecology Department of Obstetrics and Gynecology PBS/IC I have
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Interstitial and chronic cystitis. Have you heard about the 2-component protection for the bladder wall?
 Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Interstitial cystitis
 Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
RIMSO-50 PRODUCT MONOGRAPH. (Dimethyl Sulfoxide 500 mg/g) Intravesical Instillation for the Treatment of Interstitial Cystitis
 PRODUCT MONOGRAPH Pr RIMSO-50 (Dimethyl Sulfoxide 500 mg/g) Intravesical Instillation for the Treatment of Interstitial Cystitis Mylan Pharmaceuticals ULC 85 Advance Road Etobicoke, ON M8Z 2S6 Date of
PRODUCT MONOGRAPH Pr RIMSO-50 (Dimethyl Sulfoxide 500 mg/g) Intravesical Instillation for the Treatment of Interstitial Cystitis Mylan Pharmaceuticals ULC 85 Advance Road Etobicoke, ON M8Z 2S6 Date of
Patients With Chronic Pelvic Pain: Endometriosis or Interstitial Cystitis/Painful Bladder Syndrome?
 SCIENTIFIC PAPER Patients With Chronic Pelvic Pain: Endometriosis or Interstitial Cystitis/Painful Bladder Syndrome? Charles W. Butrick, MD ABSTRACT Background: Endometriosis and interstitial cystitis/painful
SCIENTIFIC PAPER Patients With Chronic Pelvic Pain: Endometriosis or Interstitial Cystitis/Painful Bladder Syndrome? Charles W. Butrick, MD ABSTRACT Background: Endometriosis and interstitial cystitis/painful
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Review of treatments for interstitial cystitis
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
Alkalinized Lidocaine and Heparin Provide Immediate Relief of Pain and Urgency in Patients with Interstitial Cystitisjsm_
 207 Alkalinized Lidocaine and Heparin Provide Immediate Relief of Pain and Urgency in Patients with Interstitial Cystitisjsm_2542 207..212 C. Lowell Parsons, MD,* Paul Zupkas, PhD,* Jeffrey Proctor, MD,
207 Alkalinized Lidocaine and Heparin Provide Immediate Relief of Pain and Urgency in Patients with Interstitial Cystitisjsm_2542 207..212 C. Lowell Parsons, MD,* Paul Zupkas, PhD,* Jeffrey Proctor, MD,
WHAT IS INTERSTITIAL CYSTITIS?
 Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information
 Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Bladder Cancer Knowing the Risks and Warning Signs. Part II: Warning Signs
 Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Mini-Reviews. Interstitial Cystitis in Adolescents and Children: A Review
 J Pediatr Adolesc Gynecol (2004) 17:7 11 Mini-Reviews Interstitial Cystitis in Adolescents and Children: A Review T.F. Mattox, MD, FACOG Department of Obstetrics and Gynecology, Division of Urogynecology,
J Pediatr Adolesc Gynecol (2004) 17:7 11 Mini-Reviews Interstitial Cystitis in Adolescents and Children: A Review T.F. Mattox, MD, FACOG Department of Obstetrics and Gynecology, Division of Urogynecology,
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Chronic Pelvic Pain Case Study
 Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
C. Lowell Parsons UC San Diego Medical Center, Department of Surgery/Urology, La Jolla, CA, USA
 ; 2010 Mini Reviews BLADDER SYMPTOMS CAUSED BY LEAKY EPITHELIUM AND POTASSIUM PARSONS ET AL. BJUI The role of a leaky epithelium and potassium in the generation of bladder symptoms in interstitial cystitis/overactive
; 2010 Mini Reviews BLADDER SYMPTOMS CAUSED BY LEAKY EPITHELIUM AND POTASSIUM PARSONS ET AL. BJUI The role of a leaky epithelium and potassium in the generation of bladder symptoms in interstitial cystitis/overactive
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy
 Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Evidence on Therapeutic Uses of Pentosan Polysulfate Sodium
 Evidence on Therapeutic Uses of Pentosan Polysulfate Sodium Excerpts from: Drugdex Monograph on Pentosan Edition: online URL: www.thomsonhc.com/home/dispatch Date Added: 29/04/2010 17:42:55 Source Notes:Evidence
Evidence on Therapeutic Uses of Pentosan Polysulfate Sodium Excerpts from: Drugdex Monograph on Pentosan Edition: online URL: www.thomsonhc.com/home/dispatch Date Added: 29/04/2010 17:42:55 Source Notes:Evidence
CHRONIC PELVIC PAIN SYNDROME. Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary
 CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS
 Guest Lecture Series Transcript IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS Featuring: Dr. Bruce Kahn, MD, FACOG Department
Guest Lecture Series Transcript IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS Featuring: Dr. Bruce Kahn, MD, FACOG Department
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Primary Care management of Overactive Bladder (OAB)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676
 This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676 CME Information CME Released: 02/15/2012; Valid for credit through 02/15/2013 Target Audience www.medscape.org
This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676 CME Information CME Released: 02/15/2012; Valid for credit through 02/15/2013 Target Audience www.medscape.org
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Case L.M. Question 1 4/17/2013. Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin
 Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors
 DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
s r e t n I sititsyc laititsret ystitis Interstitial Cystitis Interstitial Cystitis In itial Ctsretn IC I sititsyc laititsretni PRODUCT MONOGRAPH
 Interstitial Cystitis Interstitial Cystitis Interstitial Cystitis Intersti t i a l Cystitis Interstitial Cystitis Inters IC CONTENTS Interstitial Cystitis: An Overview Introduction... Epidemiology of
Interstitial Cystitis Interstitial Cystitis Interstitial Cystitis Intersti t i a l Cystitis Interstitial Cystitis Inters IC CONTENTS Interstitial Cystitis: An Overview Introduction... Epidemiology of
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
SELECTED POSTER PRESENTATIONS
 SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Interstitial Cystitis:
 Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Urinary tract disorders
 Urinary tract disorders Medicines Formulary Contents: 1. Urinary retention 1 2. Urinary incontinence 2 3. Urethral pain prevention during catheterisation 3 4. Indwelling catheters maintenance of patency
Urinary tract disorders Medicines Formulary Contents: 1. Urinary retention 1 2. Urinary incontinence 2 3. Urethral pain prevention during catheterisation 3 4. Indwelling catheters maintenance of patency
Stress incontinence -- occurs during certain activities like coughing, sneezing, laughing, or exercise.
 Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Chronic pelvic pain-when surgery fails
 Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA
 PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA E.O. Stakhovsky, PhD, MD, Professor, Head of the Scientific and Research Department of Plastic and Reconstructive Oncourology,
PRACTICAL APPLICATION INSTYLAN MODERN PROTECTOR OF URINARY BLADDER MUCOSA E.O. Stakhovsky, PhD, MD, Professor, Head of the Scientific and Research Department of Plastic and Reconstructive Oncourology,
ESSIC 2008 Annual Meeting Rome
 Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Interstitial cystitis: bladder pain and beyond
 Interstitial cystitis: bladder pain and beyond Review 1. Introduction 2. Methods 3. Presentation 4. Other invasive approaches 5. Conclusion 6. Expert opinion Theoharis C Theoharides, Kristine Whitmore,
Interstitial cystitis: bladder pain and beyond Review 1. Introduction 2. Methods 3. Presentation 4. Other invasive approaches 5. Conclusion 6. Expert opinion Theoharis C Theoharides, Kristine Whitmore,
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
flow resulting from damage to blood vessels can also contribute to sexual dysfunction.
 U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH Troublesome bladder symptoms and changes in sexual function are common health problems as people age. Having diabetes can mean
U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH Troublesome bladder symptoms and changes in sexual function are common health problems as people age. Having diabetes can mean
Diagnosis and Management of UTI s in Care Home Settings. To Dip or Not to Dip?
 Diagnosis and Management of UTI s in Care Home Settings To Dip or Not to Dip? 1 Key Summary Points: Treat the patient NOT the urine In people 65 years, asymptomatic bacteriuria is common. Treating does
Diagnosis and Management of UTI s in Care Home Settings To Dip or Not to Dip? 1 Key Summary Points: Treat the patient NOT the urine In people 65 years, asymptomatic bacteriuria is common. Treating does
THE OVER-ACTIVE BLADDER (OAB)
 THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
National Kidney and Urologic Diseases Information Clearinghouse
 Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
The Mystery and Misery of Chronic Pelvic Pain
 The Mystery and Misery of Chronic Pelvic Pain By Page Leggett Contributing Expert: Andrew Cook, MD Chronic pelvic pain (CPP) affects more than 15 million women, yet its cause is often difficult to identify.
The Mystery and Misery of Chronic Pelvic Pain By Page Leggett Contributing Expert: Andrew Cook, MD Chronic pelvic pain (CPP) affects more than 15 million women, yet its cause is often difficult to identify.
Urogynecology Associates of Philadelphia URODYNAMIC TESTING
 URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
BPS/IC: evolution of definition and prevalence
 BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
