Rabies Chitra S. Mani and Dennis L. Murray. DOI: /pir
|
|
|
- Gertrude Hunter
- 5 years ago
- Views:
Transcription
1 Rabies Chitra S. Mani and Dennis L. Murray Pediatrics in Review 2006;27;129 DOI: /pir The online version of this article, along with updated information and services, is located on the World Wide Web at: Pediatrics in Review is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since Pediatrics in Review is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, Copyright 2006 by the American Academy of Pediatrics. All rights reserved. Print ISSN:
2 Article emergency medicine Rabies Chitra S. Mani, MD,* Dennis L. Murray, MD* Author Disclosure Drs Mani and Murray did not disclose any financial relationships relevant to this article. Objectives After completing this article, the reader should be able to: 1. Explain the pathogenesis and epidemiology of virus. 2. Describe the clinical manifestations of. 3. Identify the most appropriate tests available to diagnose infection. 4. Outline the specific measures to be taken after exposure to. 5. Appreciate the strategies used to eradicate reservoirs of virus in terrestrial wildlife. Case Study A previously healthy 13-year-old boy is admitted to the hospital with the chief complaints of altered mental status and unsteady gait. Five days prior to this admission, he developed low-grade fever, generalized body pain, dry cough, and listlessness. Over the course of the next few days, he developed abdominal pain and nausea. Two days prior to this admission, he was noted to be confused, have an unsteady gait, and have difficulty swallowing. He has no history of trauma, ingestion, or bites. His mother mentioned that he had fed a raccoon in his backyard 2 to 3 months ago. The raccoon later was found dead. On examination, the boy s temperature is 100 F (37.8 C). He has fluctuating consciousness, hypersalivation, and hydrophobia. He has an ataxic gait and appears disoriented. The results of his cerebrospinal fluid (CSF) examination are: clear fluid with no red blood cells, 50 white blood cells/mm 3, 70% lymphocytes, 20% monocytes, glucose of 41 mg/dl (2.3 mmol/l) (serum glucose of 90 mg/dl [5 mmol/l]), protein of 155 mg/dl, and no organisms on Gram stain. CSF bacterial culture exhibits no growth at 72 hours. Introduction The word is derived from a Sanskrit word rabhas meaning to do violence. In Greek, Lyssa means mad rage ; therefore, the genus of the virus that causes is named Lyssavirus. The word hydrophobia means fear of water and is derived from two Greek words: hydor (water) and phobos (fear). Rabies, an acute, progressive encephalitis usually resulting in death, is a major public health problem in most parts of the world. However, some locations are considered -free, including Antarctica, Hawaii, many islands in the Pacific, and a few islands in the Caribbean. Rabies is a zoonotic disease because most humans acquire the disease after having been exposed to an infected animal. The incidence of has decreased significantly in developed countries, such as the United States, because of mandatory vaccination of all domestic animals. On the other hand, the incidence of remains high in developing nations of Asia and Africa because of a lack of immunization of domestic animals, resulting in significant health concerns for both the local population and tourists. History Rabies was described as early as 2300 BC. Wound cauterization to prevent was practiced in the 1st century AD. Its mode of transmission, via saliva, was recognized initially in the early 19th century. The pathogenesis and clinical signs of were described by Lord Louis Pasteur in 1880, who later developed the first vaccine. In 1903, Adelchi Negri in Milan identified the pathognomonic Negri bodies, associated with *Department of Pediatrics, Infectious Diseases, Medical College of Georgia, Augusta, Ga. Pediatrics in Review Vol.27 No.4 April
3 virus, in brain tissue. Direct fluorescent antibody testing, enabling detection of antigen in tissues, was developed in Virology Rabies is a neurotropic virus belonging to the Rhabdoviridae family in the genus Lyssavirus. It has a bulletshaped nucleocapsid with a single, negatively stranded, nonsegmented RNA core surrounded by a lipoprotein envelope. According to the World Health Organization, at least seven different serotypes of the Lyssavirus genus infect humans and animals. Most cases of human are caused by Lyssavirus serotype-1, commonly known as virus. This viral serotype is found worldwide. The other serotypes have limited geographic distribution and cause infection primarily in insectivorous bats, rarely causing human disease. Pathogenesis The virus usually is transmitted via saliva inoculated into a bite or cut on the skin or mucosa. Nonbite exposures, such as licking, scratching, or through inhalation, occasionally transmit the virus. Human-to-human transmission is rare and has been described mostly after corneal or other organ transplants. Studies in baby hamsters and adult skunks have shown that the virus replicates in the muscle tissue, at or near the site of entry, for most of the incubation period. Thereafter, it proceeds rapidly to the peripheral nerves via the neuromuscular connections. Once within the nerves, the virus may travel as rapidly as 12 to 24 mm/d. In experimental animals, mortality was reduced by amputating the inoculated limb before the virus began replicating in the peripheral nerves, indicating that maximum benefit of postexposure treatment occurs only when it is instituted as soon as possible after the exposure. After replication in the peripheral nerves, the virus reaches the central nervous system (CNS) via the dorsal root ganglia and sensory neurons. Occasionally, the virus may enter the CNS without replicating in the peripheral muscles. Upon reaching the CNS, the virus multiplies further, infecting virtually every neuron. From the CNS, the virus spreads to the rest of the body, especially the salivary glands, via the peripheral nerves. The virus can be transmitted via saliva because of active replication within the salivary glands. The pathologic changes of are minimal and disproportionate to the clinical symptoms. These changes are most evident in neuronal tissues. On gross examination, the brain in furious (see definition in Clinical Phases section) may appear to have meningeal congestion; paralytic (see definition in Clinical Phases section) primarily causes significant inflammation and necrosis of the spinal cord, resulting in acute inflammatory polyneuropathy (Guillain-Barré syndrome). Encephalitic changes may be seen microscopically, as evidenced by perivascular cuffing, neuronophagia, and limited necrosis. Occasionally, there may be evidence only of meningitis. Eosinophilic, intracytoplasmic viral inclusions, called Negri bodies, frequently are concentrated within the hippocampal pyramidal cells and less frequently in the cortical neurons and cerebellar Purkinje cells. The Negri bodies also may be seen in the tissues of the skin, cornea, adrenal glands, and other organs. The sensitivity of demonstrating Negri bodies, however, varies. Until the development of the fluorescent antibody technique, histologic detection of Negri bodies was considered the only pathognomonic test. The most remarkable systemic abnormality is myocarditis that resembles the cardiac involvement seen with tetanus or pheochromocytoma. Microscopic evidence of atrial-ganglioneuritis suggests that the virus probably reaches the heart via myocardial nerves. However, the presence of Negri bodies in the myocardium indicates direct viral invasion of the cardiac tissue. Natural infection causes significant immunosuppression, resulting in an inadequate immune response. Patients who develop a rapid cellular immune response usually progress more rapidly to fatal encephalitic than do those who do not develop this response. The virus may persist within macrophages for a long time before emerging to cause disease. This persistence could explain the long incubation period seen in some cases. Epidemiology Rabies primarily is a disease affecting many animals. The virus tends to be maintained in the wild animal population for many years despite high mortality from the infection, making eradication very difficult. Even though any mammal can be infected, certain ones appear to be reservoirs for human infections because they have a higher viral inoculum in their saliva and shed the virus for a longer period, making them more infectious. These mammals include dogs, cats, striped skunks, raccoons, bats, foxes, wolves, and jackals. Human transmission from small rodents such as squirrels and hamsters is rare, even though they are susceptible to the virus, because these animals succumb to the illness soon after acquiring the infection. However, large rodents such as woodchucks and beavers are capable of transmitting to humans. The epidemiology of human reflects that of local animal. Over the last 50 years, the incidence of human has decreased significantly worldwide, especially in developed countries. Of the 47 cases of 130 Pediatrics in Review Vol.27 No.4 April 2006
4 Figure. Centers for Disease Control and Prevention data from 2001 regarding terrestrial animal reservoirs of virus. human reported in the United States between 1990 and 2004, 38 cases were acquired in the United States from contact with animals that had virus infections; the remaining cases were acquired in developing countries outside the United States. Four of the cases occurred in transplant recipients from an undetected single-organ donor; death occurred in most of these cases. In Asia, Africa, and other areas where animal control programs are not developed extensively, humans acquire primarily from infected dogs or cats (canine ). In countries that have stringent immunization and quarantine policies, human cases often occur after exposure to wild terrestrial animals and bats. The current incidence of canine in the United States from local dogs and cats is low, despite numerous reports of canine bites, especially in children. Until recently, most of the human cases in the United States had been in travelers returning from areas at risk for canine. However, with the steady increase of animal over the last 2 decades, bats, raccoons, skunks, foxes, and coyotes increasingly are becoming the major reservoir of human in North America. The Figure shows a 2001 map of animal reservoirs for virus in the United States. Two small-bodied bats, the eastern pipistrella bat (Pipistrellus subflavus) and the silverhaired bat (Lasionycteris noctivagans), are especially important reservoirs for throughout the continental United States and Alaska. In recent years, when the source of exposure has been unknown, molecular techniques frequently have determined the cause of infection to be from bats. Human is more common in males younger than 15 years of age, reflecting their greater likelihood of exposure. Clinical Manifestations Three possible outcomes follow a definite exposure: no infection, asymptomatic infection demonstrable by serologic immune response, or symptomatic. The initial signs of in animals are a change in disposition, restlessness, and fear. Wild animals may demonstrate an unusual lack of fear of humans. Over the next few days, most infected animals develop the furious syndrome that is characterized by increased restlessness, snapping, and drooling. By contrast, a few infected animals may become lethargic (dumb syndrome). Most affected canines die within 10 days of becoming symptomatic. Rarely, a few might survive for as long as 1 month before succumbing to the disease. Clinical Phases Human infection evolves through five clinical phases: incubation, prodrome, acute neurologic phase, coma, and death or recovery. Incubation The incubation period varies in length, with the patient usually being asymptomatic. The incubation period may be as short as a few days or as long as several years after exposure. The mean duration in most patients ( 75%) is 30 to 90 days. The length of the incubation period depends on the innervation of the site of bite, the number and severity of bite(s), the proximity of the bite s location to the CNS, the quantity of virus inoculated, and the age and immunity of the host. Incubation periods typically are shorter in children, in persons who have extensive bites to the face or head, and in those receiving corticosteroids. Prodrome A typical prodrome lasts 2 to 10 days and correlates with the viral invasion of the CNS, especially into the limbic system, brainstem, and spinal cord. During this phase, the patient presents with mild and nonspecific respiratory or gastrointestinal symptoms, frequently leading to the misdiagnosis of a bacterial or viral infection. These manifestations may include fever, headache, chills, malaise, Pediatrics in Review Vol.27 No.4 April
5 fatigue, sore throat, cough, nausea, vomiting, diarrhea, dysphagia, vertigo, irritability, anxiety, and apprehension. As the disease progresses, the patient develops alteration in personality, photophobia, and insomnia. A specific symptom often seen in most patients during this time is paresthesia at the site of the bite, described as burning pain, numbness, tingling, or itching. Acute Neurologic Phase This phase correlates with widespread invasion of the CNS by the virus. It begins with the patient developing obvious signs of neurologic dysfunction. Patients may present as having either furious or paralytic. Both presentations involve the development of fever, nuchal rigidity, muscle fasciculation, convulsions, hyperventilation, or hypersalivation. FURIOUS RABIES. This phase develops in 80% of cases and is characterized by anxiety, marked agitation, hallucinations, and other bizarre behavior. Signs of hydrophobia or aerophobia (fear of breeze) may occur, in which patients develop painful spasms of the pharynx, initially triggered by an attempt to drink water or by air blowing on the face. However, as the illness progresses, these signs may be triggered by a variety of tactile, audio, visual, or olfactory stimuli. Such reactions are due to violent diaphragmatic contractions from an exaggerated respiratory protective reflex. The patient s mental status initially fluctuates among periods of agitation, relative normalcy, and severe depression. Neurologic signs include hyperreflexia and excess cholinergic signs such as hypersalivation, lacrimation, mydriasis, and hyperpyrexia. Unless the patient dies abruptly, paralysis soon occurs, and the mental status rapidly deteriorates from disorientation to stupor and finally, coma. The clinical picture at this time may mimic that of meningitis, encephalitis, drug toxicity, tetanus, or polyneuropathy. PARALYTIC RABIES. This phase is seen less often (about 20% of cases). It is more frequent after exposure to bats or in persons who have received improperly inactivated vaccines that contain fixed virus strains. Hydrophobia and hyperactivity are characteristically absent. The patient may develop any one of the following four clinical patterns of paralytic : 1) the most common presentation is paresthesia and weakness (prominent at the site of the bite) that rapidly progresses to paraplegia, triplegia, or quadriplegia; 2) less often, quadriplegia at the onset of illness; 3) occasionally, presentation as transverse myelitis with combined motor and sensory involvement; or 4) rarely, clinical findings that may mimic Landry-Guillain-Barré syndrome, presenting with fever and symmetric ascending paralysis but with intact sensory function. Eventually, the patient progresses into complete respiratory paralysis. Most patients who have paralytic develop myoedema (swelling of muscles). Some patients may develop hydrophobia and signs of furious just before they become terminally ill. Coma During the transition from the acute neurologic phase to coma, a patient may develop periods of rapid, irregular, jerky (apneustic) breathing followed by generalized paralysis and coma. The patient usually dies from respiratory failure unless mechanically ventilated at this time. Ultimately, patients succumb to the complications of prolonged ventilation. Non-neurologic signs involving the following organs also may develop: Cardiac: tachycardia, arrhythmia, hypotension, or congestive cardiac failure Respiratory: hypoxia, hyperventilation, atelectasis, pneumothorax, or pneumomediastinum Diabetes insipidus, hypothermia, hyperthermia, autonomic dysfunction, or the syndrome of inappropriate antidiuretic hormone secretion involving the CNS Gastrointestinal: vomiting, diarrhea, ileus, severe gastrointestinal pain, or bleeding Differential Diagnosis Infection with virus may mimic some of the following conditions: Infectious: herpes simplex virus, arboviruses, poliomyelitis, herpes B virus, cerebral malaria, tetanus, botulism, and typhoid and rickettsial diseases Noninfectious: Guillain-Barré syndrome; intoxication with poisons, drugs, or alcohol; allergic postvaccinal encephalomyelitis; and acute porphyria Rabies hysteria: a rare psychological condition that occurs in exposed adults who believe that they have developed. Many of these adults have some knowledge about the clinical manifestations of, and they may present with symptoms and signs indistinguishable from those of. Diagnosis Human frequently is misdiagnosed, especially in countries such as the United States, where the incidence is rare. Some 20% of cases may have no documented history of exposure. No useful diagnostic tests recognize 132 Pediatrics in Review Vol.27 No.4 April 2006
6 the infection during the incubation period. During the symptomatic phase, a peripheral hematologic profile and urinalysis usually are nonspecific. In one third of patients, initial results of the CSF analysis, electroencephalography (EEG), and computed tomography (CT) scan of the head may be normal. Later in the illness, CSF may show pleocytosis (30 to 300 white blood cells/mm 3 ), a normal glucose concentration, and a moderately elevated protein level (100 to 200 mg/dl). Nonspecific abnormal changes also may be noted on an EEG or a CT scan of the head. A thorough history that includes the patient s place of residence, possible exposure, and travel to endemic areas is very important for early diagnosis. Specific tests for usually are not available in most hospitals and may have to be requested from a state health department laboratory. Direct fluorescent antibody staining (DFA) that detects -specific antigen is a reliable, rapid test. Acceptable specimens for DFA are saliva, brain tissue, and other neural tissues. Because the virus localizes to the nerve plexus surrounding the hair follicles, a good specimen that becomes positive early during the illness is a full-thickness biopsy of the skin taken from the nape of the neck at the hairline. It is important to remember that prior immunization does not induce CSF antibodies to the virus. Thus, the presence of high CSF antibody titers supports the diagnosis of clinical. Virus can be isolated in culture from saliva, CSF, urine, and respiratory secretions, usually during the second or third week of symptoms. The virus may not grow if the culture is performed too early in the course of the illness because the virus replicates slowly. Likewise, the virus may not be isolated on culture, if obtained late in the infection, because of neutralization by virus-specific antibodies. The current diagnostic test of choice is reverse transcriptase-polymerase chain reaction (RT-PCR) because this type of testing is specific and is the most sensitive and earliest to yield results. The best specimens for this test are saliva or brain tissue. Unlike other diagnostic techniques, RT-PCR also can be performed successfully on decomposing brain tissue. This test has the added advantage of determining the geographic and host species origin of a particular virus, especially when the exposure is unknown. Treatment No specific anti agent is available to treat the disease once the patient becomes symptomatic; most of the management is supportive. Supplemental oxygen and mechanical ventilation are essential for most patients during the period of agitation and hyperventilation. Tranquilizers are useful in controlling hyperactivity and agitation. Focal or generalized seizures may require anticonvulsant therapy. Adequate fluid administration and vasopressors may correct hypotension. Cardiac arrhythmia may require antiarrhythmic agents. Treatment with diuretics, fluid restriction, and digoxin may be necessary to treat congestive cardiac failure. Use of -specific immunoglobulin (RIG) or vaccine after the onset of disease has not been shown to be protective or to increase the survival rate. In a recent case report, a patient who had developed after sustaining a bite from a bat was managed empirically with an intense antiexcitotoxic strategy until the patient s natural immune response matured. This regimen consisted of placing the patient in a deep, drug-induced coma by using benzodiazepines, barbiturates, ketamine, and amantadine. The latter two agents also have been reported to be effective against virus. Ribavirin was used initially in conjunction with the previously noted therapy but later was discontinued due to drug-related toxicities. The patient survived the illness with neurologic impairment. Further studies are required to determine if such a treatment protocol is truly effective in increasing survival from infection. Prognosis The prognosis in most cases of infection is grave. Death usually results from severe neurotransmitter imbalance. However, five to six survivors have been documented in the medical literature, which has provided hope for a possible cure in the future. Most survivors have been reported to suffer neurologic sequelae, usually involving the cerebellum. Hospital Isolation Rabies virus can be identified from saliva, CSF, impressions from the cornea, and urine. Because the shedding and infectivity between humans is not clearly understood, direct contact with infected secretions or tissues must be avoided. The patient suspected of having infection must be placed in contact and droplet isolation, which requires caregivers to wear gowns, gloves, masks, and goggles when in direct contact with the patient. Contacts who are exposed prior to diagnosis may be at risk of developing and should be offered postexposure prophylaxis. Prevention Because most human cases of are fatal and no specific therapy is available, the emphasis is placed on prevention. Fortunately, effective vaccines are available. Nerve tissue vaccines were developed more than 70 years Pediatrics in Review Vol.27 No.4 April
7 ago from animal brain and spinal cord tissues (Sempletype). These vaccines now are used predominantly in developing countries because they are relatively inexpensive. However, these vaccines frequently are associated with increased central and peripheral neurologic complications. Antibody titers should be monitored in all recipients of the nerve tissue vaccines because their immunogenicity may vary. Avian vaccines derived from duck embryos were the next vaccines to be introduced, but they are less immunogenic than the brain tissue vaccines. Finally, cell culture vaccines, which include human diploid cell vaccine (HDCV), rhesus monkey diploid cell vaccine ( vaccine, adsorbed), and purified chick embryo cell vaccine, among others, are available primarily in developed countries such as the United States. These vaccines are more expensive but are safe and immunogenic. In addition, antibody titers need not be monitored in recipients of cell culture vaccines unless there is reason to suspect poor antibody response. Use of steroids during vaccination may blunt the immune response. Because most human cases of infection are related primarily to infection after animal exposure, especially to canines, vaccination of domestic animals substantially decreases the incidence of human. Most developed nations have enforced strict vaccination laws for pets and livestock. Recent programs to vaccinate wild terrestrial animals with oral vaccine are becoming effective public health measures, especially in Europe and in the United States. Pre-exposure prophylaxis is administered to persons at risk for exposure to virus, including veterinarians, animal control officers, park officials, laboratory personnel working with virus, and travelers to -endemic countries. HDCV vaccine is used preferentially in the United States because of its demonstrated safety and efficacy. The vaccine is not contraindicated for use in pregnant women. It is administered in a 1-mL dose intramuscularly three times, on days 0, 7, and 21. A booster dose is recommended every 2 to 3 years, especially for individuals frequently at risk of exposure. Immunization of all travelers for the prevention of is controversial. However, selected immunization based on age and travel destination is appropriate. The Centers for Disease Control and Prevention currently recommends prophylactic vaccination for individuals planning to stay for more than 30 days in remote areas of the world without access to medical facilities. Because chloroquine may decrease antibody response, its concurrent use with vaccine is not recommended. Postexposure treatment (PET) that includes aggressive management of the bite or wound can reduce the risk of acquiring by 90%. Thorough washing with 20% soap solution and vigorous irrigation with a virucidal agent such as povidone-iodine is recommended. Mechanical scrubbing and adequate debridement are more effective than simple irrigation of the wound. Suturing or using occlusive dressings to cover the wound should be avoided when possible. Because acquiring a secondary bacterial or tetanus infection is common after an animal bite, tetanus vaccine and antibiotics should be administered when necessary. The risk of developing after exposure must be determined. Communication with local public health officials is useful in obtaining information about locally infected animal species and for the proper examination of the animals. In the United States, when an animal suspected of being infected with is available, the local or state health department should be contacted about the management of such animals that bite humans. If the biting animal is a dog, cat, or ferret and is considered otherwise healthy, the animal should be confined and observed daily for 10 days. The animal should be evaluated by a veterinarian at the first sign of illness during the period of confinement. If the bite involves a stray or unvaccinated dog, cat, or ferret, the animal should be euthanized immediately and the head submitted for examination. For animals other than dogs, cats, or ferrets, the management of the animal depends on many factors, including the biting incident and the animal s history (if available) and current heath status. The animal s brain tissue should be examined for only in a qualified laboratory as designated by the consulting local or state health department. PET is recommended after a bite by a mammal that has not been vaccinated previously or whose vaccination status is unknown (undocumented) or when the animal is not available to monitor and the integrity of the skin or mucous membrane has been breached. Because bats have infected humans without a known bite, PET is recommended for adults or children sleeping in a room in which a bat is found or in those cases where it is difficult to exclude direct contact with bats. Because the risk of acquiring is very low after a rodent bite, PET is not recommended routinely unless the rodent involved was a woodchuck or a beaver. PET should be offered to all individuals, including those who have received preexposure prophylaxis, if they become at risk for. It is important to recognize that of the 30,000 to 40,000 individuals in the United States annually receiving PET, only a few actually are at risk for infection. PET includes the administration of RIG. Two types of RIG are available: human immunoglobulin 134 Pediatrics in Review Vol.27 No.4 April 2006
8 (HRIG) and equine immunoglobulin (ERIG). Only HRIG is available in the United States. Purified ERIG, available outside the United States, is as safe and as well tolerated as HRIG. RIG must be administered to the exposed individual as soon as possible and within 7 days of exposure. RIG always should be used in combination with vaccine (active immunization) after primary exposure, but should not be used in individuals who have received prior vaccination. The total dose of 20 IU/ kg is infiltrated primarily around the bite site. Any remaining volume should be administered intramuscularly at a site distant from the wound. RIG is safe and usually free of adverse reactions. HDCV vaccine (1 ml/dose) is administered intramuscularly on days 0, 3, 7, 14, and 28 in unvaccinated individuals. Previously immunized individuals require a booster dose of 1 ml/dose on days 0 and 3. The vaccine must be injected in the deltoid muscle because if the muscle is missed in gluteal injections, there may be vaccine failure. Booster doses may be given either intramuscularly or intradermally. In the United States, booster doses are given by intramuscular injection only. Intradermal vaccines currently are available outside the United States. The vaccine must never be administered at the same site as RIG because the antibodies in RIG might interfere with the immune uptake of the vaccine. The development of local reactions such as swelling, pain, or induration is common. Rarely, other symptoms such as fever, headache, malaise, nausea, abdominal pain, and adenopathy may develop. The previous information is available in tabular form in the American Academy of Pediatrics Red Book (see Suggested Reading). Future Prospects Improved wildlife surveillance has begun to provide a better understanding of disease in animals. More widespread wildlife vaccinations using oral vaccine might provide a safe and effective method to control the disease in the wild, thereby eradicating the animal reservoir for. Molecular technology has allowed better identification of viral strains, allowing determination of their geographic location and frequency of occurrence. Development of virus-specific monoclonal antibodies may provide effective passive immunotherapy. The availability of new antiviral therapy and specific immunomodulators might improve treatment and be curative. Finally, designing a subunit vaccine might provide a safer and more effective preventive tool. Summary Rabies is a zoonotic infection that results in progressive encephalitis and death. It is caused by a virus of the Lyssavirus genus. Rabies is a major public health problem all over the world. In the United States, most cases occur after exposure to wild terrestrial animals or bats. The virus usually replicates at the point of entry for a period of time before invading the CNS via peripheral nerves. Symptomatic may present as the more common furious form or the less common paralytic type. Reliable and rapid diagnostic tests include DFA and RT-PCR. Currently, no therapeutic agents for treating disease caused by virus are effective. However, there are effective and safe preventive measures, such as human diploid cell vaccine and HRIG, which should be administered as soon as possible after exposure. Suggested Reading American Academy of Pediatrics. Rabies. In: Pickering LK, ed. Red Book 2003: Report of the Committee on Infectious Diseases. 26th ed. Elk Grove Village, Ill: American Academy of Pediatrics; 2003: Baer GM, Bellini WJ, Fishbein DB. Rhabdoviruses. In: Fields BN, Knipe DM, Chanock RM, et al, eds. Fundamental Virology. 2nd ed. New York, NY: Raven Press; 1990: Bleck TP, Rupprecht CE. Rhabdoviruses. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and Practice of Infectious Diseases. 6th ed. St Louis, Mo: Elsevier Churchill and Livingstone; 2005: Centers for Disease Control and Prevention. Compendium of animal prevention and control. MMWR Recomm Rep. 2003;52(RR-5):1 6 Centers for Disease Control and Prevention. Human Florida, MMWR Morbid Mortal Wkly Rep. 2005;54: Centers for Disease Control and Prevention. Human Rabies Prevention United States, Recommendations of the Advisory Committee on Immunization Practices (ACIP) MMWR Recomm Rep. 1999;48(RR-1):1 21 Centers for Disease Control and Prevention. National Centers for Infectious Diseases. Traveler s Health. Available at: gov/travel/diseases/.htm Plotkin SA. Rabies virus. In: Long SS, Pickering LK, Prober CG, eds. Principles and Practice of Pediatric Infectious Diseases. 2nd ed. Philadelphia, Pa: Churchill and Livingstone; 2003: Plotkin SA, Rupprecht CE, Koprowski CR. Rabies vaccine. In: Plotkin SA, Orenstein WA, eds. Vaccines. 4th ed. Philadelphia, Pa: Saunders; 2004: Rupprecht CE, Gibbons RV. Prophylaxis against. N Engl J Med. 2004;351: Storch GA. Central nervous system infections. In: Essentials of Diagnostic Virology. Philadelphia, Pa: Churchill Livingstone; 2000: Willoughby RE Jr, Tieves KS, Hoffman GM, et al. Survival after treatment of with induction of coma. N Engl J Med. 2005;352: Pediatrics in Review Vol.27 No.4 April
9 PIR Quiz Quiz also available online at 5. The virus affects both wild and domestic animals, with the added risk that certain mammals are more contagious with the virus than others. The animal that is less likely to transmit to humans is the: A. Bat. B. Dog. C. Fox. D. Racoon. E. Squirrel. 6. In African countries such as Ethiopia, in contrast to the United States, the most likely animal to transmit to humans is the: A. Bat. B. Dog. C. Fox. D. Hyena. E. Skunk. 7. The incubation period after exposure to a -infected animal varies, but shorter incubation periods are more often seen in a(n): A. Adult. B. Bat aerosol exposure. C. Face bite. D. Finger bite. E. Leg bite. 8. The best test to confirm a diagnosis of earliest in a suspected human case is a(n): A. Cerebrospinal fluid antibody test. B. Computed tomography scan of the brain. C. Direct fluorescent antibody test of the saliva for -specific antigen. D. Electroencephalogram. E. Reverse transcriptase-polymerase chain reaction test of the saliva for antigen. 9. A 5-year-old boy is playing in his backyard when he encounters a raccoon, which bites him on his hand. The animal escapes, and the child is brought to the emergency department for treatment. The wound is cleaned with 20% soap and povidone-iodine solution. The best next course of action is to: A. Administer one dose of human diploid vaccine (HDVC) as soon as possible. B. Administer one dose of immune globulin (RIG) and HDVC in the buttocks while awaiting the pathology report on the raccoon s brain. C. Administer RIG immediately in the deltoid and start the HDCV, giving it on days 0, 3, 7, 14, and 28. D. Contact animal control to capture the raccoon for examination and administer RIG and HDVC to the boy as soon as it is determined that the raccoon has. E. Infiltrate the wound with RIG and immediately start HDCV vaccine, giving it on days 0, 3, 7, 14, and Pediatrics in Review Vol.27 No.4 April 2006
10 Rabies Chitra S. Mani and Dennis L. Murray Pediatrics in Review 2006;27;129 DOI: /pir Updated Information & Services References Subspecialty Collections Permissions & Licensing Reprints including high resolution figures, can be found at: This article cites 5 articles, 0 of which you can access for free at: This article, along with others on similar topics, appears in the following collection(s): Emergency Medicine y_medicine_sub Infectious Diseases _diseases_sub Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: /site/misc/permissions.xhtml Information about ordering reprints can be found online: /site/misc/reprints.xhtml
RABIES Pr P ese e n se t n er e : J. J. K a K m a bo b n o a n a (M.B. B Ch C. h B; B M.Med e ) d
 RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
RABIES. Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department
 RABIES Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department Please focus on the pathogenesis and prophylaxis plus wound care!! What is
RABIES Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department Please focus on the pathogenesis and prophylaxis plus wound care!! What is
CNS MODULE. Dr Hamed Al-Zoubi Ass. Prof. of Microbiology
 CNS MODULE Dr Hamed Al-Zoubi Ass. Prof. of Microbiology Enteroviruses Picornaviridae family 1. Enteroviruses a) Polioviruses types 1, 2 and 3 b) Coxsackieviruses A1-A24 (no A23), B1-B6 c) Echoviruses 1
CNS MODULE Dr Hamed Al-Zoubi Ass. Prof. of Microbiology Enteroviruses Picornaviridae family 1. Enteroviruses a) Polioviruses types 1, 2 and 3 b) Coxsackieviruses A1-A24 (no A23), B1-B6 c) Echoviruses 1
Rabies Epidemiology K require rabies post-exposure prophylaxis annually. Medical urgency, not medical emergency $300 million annually
 Rabies Rabies Epidemiology 16-39K require rabies post-exposure prophylaxis annually Medical urgency, not medical emergency $300 million annually About 1 or 2 cases of rabies annually in US Sources of Exposure
Rabies Rabies Epidemiology 16-39K require rabies post-exposure prophylaxis annually Medical urgency, not medical emergency $300 million annually About 1 or 2 cases of rabies annually in US Sources of Exposure
Rabies. By Rosa Reynoso. Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4)
 Rabies By Rosa Reynoso Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4) Transmision: It is a zoonotic disease transmitted from infected animals to humans (4). Infected animals
Rabies By Rosa Reynoso Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4) Transmision: It is a zoonotic disease transmitted from infected animals to humans (4). Infected animals
Policy Statement Rabies-Prevention Policy Update: New Reduced-Dose Schedule
 FROM THE AMERICAN ACADEMY OF PEDIATRICS Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children Policy Statement Rabies-Prevention Policy Update:
FROM THE AMERICAN ACADEMY OF PEDIATRICS Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children Policy Statement Rabies-Prevention Policy Update:
Rabies. By Alexa Smith. Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission:
 Rabies By Alexa Smith Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission: The virus can enter a host via a parenteral route. The saliva of the infected host
Rabies By Alexa Smith Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission: The virus can enter a host via a parenteral route. The saliva of the infected host
This is risky. Rabies. Are you at risk?
 This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
RABIES PROTECTION PROGRAM
 Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
Presented by. Professor Dr. Md. Zakir Hossain. Professor & Head Department of Medicine Rangpur Medical College & Hospital
 Rabies Presented by Professor Dr. Md. Zakir Hossain MBBS, FCPS, MD(Internal Medicine), FACP Professor & Head Department of Medicine Rangpur Medical College & Hospital Rangpur Medical College Rangpur Medical
Rabies Presented by Professor Dr. Md. Zakir Hossain MBBS, FCPS, MD(Internal Medicine), FACP Professor & Head Department of Medicine Rangpur Medical College & Hospital Rangpur Medical College Rangpur Medical
Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2
 Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2 Post-exposure Rabies Vaccine Schedule Update The March 19, 2010 issue of the Centers for Disease Control
Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2 Post-exposure Rabies Vaccine Schedule Update The March 19, 2010 issue of the Centers for Disease Control
Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel
 U.S. Army Public Health Command Public Health Notice Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel December 2012 U.S. Army Public Health Command
U.S. Army Public Health Command Public Health Notice Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel December 2012 U.S. Army Public Health Command
NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) (518) (after hours)
 NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) 474-3186 (518) 465-9720 (after hours) SUBJECT: Guidance Regarding Human Rabies Exposure and Treatment Decisions
NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) 474-3186 (518) 465-9720 (after hours) SUBJECT: Guidance Regarding Human Rabies Exposure and Treatment Decisions
NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES
 NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES NEW JERSEY GUIDE TO POST-EXPOSURE RABIES PROPHYLAXIS FOR THE HEALTH CARE PROFESSIONAL July 2011 BACKGROUND Raccoon rabies entered New Jersey in the fall
NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES NEW JERSEY GUIDE TO POST-EXPOSURE RABIES PROPHYLAXIS FOR THE HEALTH CARE PROFESSIONAL July 2011 BACKGROUND Raccoon rabies entered New Jersey in the fall
Considerations for Tetanus While Treating an Exposure to Rabies
 Considerations for Tetanus While Treating an Exposure to Rabies Since rabies and tetanus are not as common in the United States (US) as they used to be, 1,2 people may not be fully aware of these diseases
Considerations for Tetanus While Treating an Exposure to Rabies Since rabies and tetanus are not as common in the United States (US) as they used to be, 1,2 people may not be fully aware of these diseases
Acute neurological syndromes
 Acute neurological syndromes Assoc.Prof. Murat Sayan Kocaeli Üniversitesi, Rutin PCR Lab. Sorumlu Öğt.Üyesi Yakın Doğu Üniversitesi, DESAM Kurucu Öğrt. Üyesi sayanmurat@hotmail.com 0533 6479020 Medical
Acute neurological syndromes Assoc.Prof. Murat Sayan Kocaeli Üniversitesi, Rutin PCR Lab. Sorumlu Öğt.Üyesi Yakın Doğu Üniversitesi, DESAM Kurucu Öğrt. Üyesi sayanmurat@hotmail.com 0533 6479020 Medical
Poliovirus replication
 Poliovirus Poliovirus It belongs to the Enteroviruses genus of the picornavirus family which replicate mainly in the gut. Single stranded naked RNA virus with icosahedral symmetry Capsid has 60 copies
Poliovirus Poliovirus It belongs to the Enteroviruses genus of the picornavirus family which replicate mainly in the gut. Single stranded naked RNA virus with icosahedral symmetry Capsid has 60 copies
GENUS LYSSAVIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS.
 GENUS LYSSAVIRUS RABIES VIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS. IT HAS BEEN KNOWN SINCE THE 23 CENTURY B.C. RABIES IS PRESENT IS THE SALIVA OF RABID ANIMALS AND IS TRANSMITTED
GENUS LYSSAVIRUS RABIES VIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS. IT HAS BEEN KNOWN SINCE THE 23 CENTURY B.C. RABIES IS PRESENT IS THE SALIVA OF RABID ANIMALS AND IS TRANSMITTED
2018 Infection Prevention and Control Update. Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC
 2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
GUIDELINES FOR MANAGEMENT OF SUSPECTED RABIES EXPOSURES January, 2010
 Ministry of Health and Long-Term Care Ministère de la Santé et des Soins de longue durée GUIDELINES FOR MANAGEMENT OF SUSPECTED RABIES EXPOSURES January, 2010 All suspected incidents must be reported to
Ministry of Health and Long-Term Care Ministère de la Santé et des Soins de longue durée GUIDELINES FOR MANAGEMENT OF SUSPECTED RABIES EXPOSURES January, 2010 All suspected incidents must be reported to
Twelve Common Questions About Human Rabies and Its Prevention
 Published in Infectious Diseases in Clinical Practice (2000) 9:202-207 Twelve Common Questions About Human Rabies and Its Prevention Robert V. Gibbons, MD, MPH Charles Rupprecht, DVM Viral and Rickettsial
Published in Infectious Diseases in Clinical Practice (2000) 9:202-207 Twelve Common Questions About Human Rabies and Its Prevention Robert V. Gibbons, MD, MPH Charles Rupprecht, DVM Viral and Rickettsial
Animal Bites and Rabies. Patty W. Wright, M.D. 2018
 Animal Bites and Rabies Patty W. Wright, M.D. 2018 Objectives To inform participants about the treatment of common animal bites To discuss the indications for and administration of pre- and post-exposure
Animal Bites and Rabies Patty W. Wright, M.D. 2018 Objectives To inform participants about the treatment of common animal bites To discuss the indications for and administration of pre- and post-exposure
Rabies. By Sarah C. Rivera
 Rabies By Sarah C. Rivera Etiologic Agent: As a current veterinary technician, rabies is a word spoken all too often and without thinking twice. The clinic where I work is an approved rabies quarantine
Rabies By Sarah C. Rivera Etiologic Agent: As a current veterinary technician, rabies is a word spoken all too often and without thinking twice. The clinic where I work is an approved rabies quarantine
Below you will find information about diseases, the risk of contagion, and preventive vaccinations.
 Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
PUBLIC HEALTH SIGNIFICANCE SEASONAL INFLUENZA AVIAN INFLUENZA SWINE INFLUENZA
 INFLUENZA DEFINITION Influenza is an acute highly infectious viral disease characterized by fever, general and respiratory tract catarrhal manifestations. Influenza has 3 Types Seasonal Influenza Avian
INFLUENZA DEFINITION Influenza is an acute highly infectious viral disease characterized by fever, general and respiratory tract catarrhal manifestations. Influenza has 3 Types Seasonal Influenza Avian
Canadian Immunization Guide
 Home > Immunization & Vaccines > Canadian Immunization Guide > Rabies Vaccine Canadian Immunization Guide T [Previous page] [Table of Contents] [Next page] Part 4 Active Vaccines Rabies Vaccine Epidemiology
Home > Immunization & Vaccines > Canadian Immunization Guide > Rabies Vaccine Canadian Immunization Guide T [Previous page] [Table of Contents] [Next page] Part 4 Active Vaccines Rabies Vaccine Epidemiology
 Page 1 of 11 Medical Summary RABIES GENERAL INFORMATION Introduction Rabies is an acute, progressive infection of the central nervous system caused by neurotropic viruses in the family Rhabdoviridae, genus
Page 1 of 11 Medical Summary RABIES GENERAL INFORMATION Introduction Rabies is an acute, progressive infection of the central nervous system caused by neurotropic viruses in the family Rhabdoviridae, genus
4/24/2013. Haemophilus influenzae Meningitis. Neisseria Meningitis. Streptococcus pneumoniae Meningitis
 1 2 3 4 5 6 7 Chapter 22 Microbial Diseases of the Nervous System The Human Nervous System Meninges protect brain and spinal cord Dura mater: Outermost layer Arachnoid mater: Middle layer Subarachnoid
1 2 3 4 5 6 7 Chapter 22 Microbial Diseases of the Nervous System The Human Nervous System Meninges protect brain and spinal cord Dura mater: Outermost layer Arachnoid mater: Middle layer Subarachnoid
Rabies. By: Christopher Solomon. Disease: Rabies etiologic agent: Lyssavirus (1)
 Rabies By: Christopher Solomon Disease: Rabies etiologic agent: Lyssavirus (1) Transmission: Transmission of this disease is most often transmitted by the bite of an infected or rabid animal (2). Reservoirs:
Rabies By: Christopher Solomon Disease: Rabies etiologic agent: Lyssavirus (1) Transmission: Transmission of this disease is most often transmitted by the bite of an infected or rabid animal (2). Reservoirs:
BBS2711 Virology. Central Nervous System (CNS) Viruses. Dr Paul Young, Department of Microbiology & Parasitology.
 BBS2711 Virology Central Nervous System (CNS) Viruses Dr Paul Young, Department of Microbiology & Parasitology. p.young@mailbox.uq.edu.au Viruses of the CNS Many human pathogenic viruses are capable of
BBS2711 Virology Central Nervous System (CNS) Viruses Dr Paul Young, Department of Microbiology & Parasitology. p.young@mailbox.uq.edu.au Viruses of the CNS Many human pathogenic viruses are capable of
Case Classification West Nile Virus Neurological Syndrome (WNNS)
 WEST NILE VIRUS Case definition Case Classification West Nile Virus Neurological Syndrome (WNNS) CONFIRMED CASE West Nile Virus Neurological Syndrome (WNNS) Clinical criteria AND at least one of the confirmed
WEST NILE VIRUS Case definition Case Classification West Nile Virus Neurological Syndrome (WNNS) CONFIRMED CASE West Nile Virus Neurological Syndrome (WNNS) Clinical criteria AND at least one of the confirmed
Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally
 Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally Susan Moore, Rabies Laboratory/KSVDL/College of Veterinary Medicine/Kansas State University, Manhattan, KS 66502,
Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally Susan Moore, Rabies Laboratory/KSVDL/College of Veterinary Medicine/Kansas State University, Manhattan, KS 66502,
OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY
 OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY Review 06-2010 No changes to the PRE-EXPOSURE protocol of 2008. See
OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY Review 06-2010 No changes to the PRE-EXPOSURE protocol of 2008. See
DISCLOSURES. I have no actual or potential conflicts of interest in this presentation.
 OVERVIEW ON MEASLES Oneka B. Marriott, DO, MPH, FAAP, FACOP Assistant Professor of Pediatrics and Public Health Nova Southeastern University College of Osteopathic Medicine Presentation to FSACOFP Annual
OVERVIEW ON MEASLES Oneka B. Marriott, DO, MPH, FAAP, FACOP Assistant Professor of Pediatrics and Public Health Nova Southeastern University College of Osteopathic Medicine Presentation to FSACOFP Annual
Ebola Virus Patient Advisory
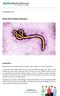 22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
Epidemiology of Rabies Post-exposure Prophylaxis in Ontario:
 Epidemiology of Rabies Post-exposure Prophylaxis in Ontario: 2007-2011 The CIPHI 2013 Ontario Branch Conference September 16-18, 2013 Karen Johnson, Senior Epidemiologist Communicable Diseases Prevention
Epidemiology of Rabies Post-exposure Prophylaxis in Ontario: 2007-2011 The CIPHI 2013 Ontario Branch Conference September 16-18, 2013 Karen Johnson, Senior Epidemiologist Communicable Diseases Prevention
Explain the laboratory diagnosis of Rabies?
 Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
INTERNATIONAL SOCIETY FOR HEART AND LUNG TRANSPLANTATION a Society that includes Basic Science, the Failing Heart, and Advanced Lung Disease
 International Society of Heart and Lung Transplantation Advisory Statement on the Implications of Pandemic Influenza for Thoracic Organ Transplantation This advisory statement has been produced by the
International Society of Heart and Lung Transplantation Advisory Statement on the Implications of Pandemic Influenza for Thoracic Organ Transplantation This advisory statement has been produced by the
Clinical Information on West Nile Virus (WNV) Infection
 Clinical Information on West Nile Virus (WNV) Infection Introduction In 1999, West Nile Virus (WNV), an Old World flavivirus, producing a spectrum of disease including severe meningoencephalitis, appeared
Clinical Information on West Nile Virus (WNV) Infection Introduction In 1999, West Nile Virus (WNV), an Old World flavivirus, producing a spectrum of disease including severe meningoencephalitis, appeared
Streptococcus Pneumoniae
 Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Rhabdoviruses. Rabies is a viral disease that produces an almost uniformly fatal. Virology. Epidemiology
 163 Rhabdoviruses SARICE L. BASSIN CHARLES E. RUPPRECHT THOMAS P. BLECK Rabies is a viral disease that produces an almost uniformly fatal encephalitis in humans and most other mammals. It has been present
163 Rhabdoviruses SARICE L. BASSIN CHARLES E. RUPPRECHT THOMAS P. BLECK Rabies is a viral disease that produces an almost uniformly fatal encephalitis in humans and most other mammals. It has been present
Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005)
 Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Philippe Lagacé Wiens M.D., DTM&H, FRCPC
 Philippe Lagacé Wiens M.D., DTM&H, FRCPC ay yah FYAH lah yer kuhl 1. Describe the pathogenesis (steps in causing disease) of the rabies virus starting from the bite of an infected animal death of the
Philippe Lagacé Wiens M.D., DTM&H, FRCPC ay yah FYAH lah yer kuhl 1. Describe the pathogenesis (steps in causing disease) of the rabies virus starting from the bite of an infected animal death of the
West Nile Virus. Syndrome. (Family: Flaviviridae) Severe Manifestations (Typically >50 years of age) NEUROLOGICAL (Meningoencephalitis >Meningitis)
 Severe Manifestations (Typically >50 years of age) Syndrome NEUROLOGICAL (Meningoencephalitis >Meningitis) CSF WBC Protein Glucose-WNL Confusion Change in Sensorium Stupor Seizures Ataxia Cranial Nerve
Severe Manifestations (Typically >50 years of age) Syndrome NEUROLOGICAL (Meningoencephalitis >Meningitis) CSF WBC Protein Glucose-WNL Confusion Change in Sensorium Stupor Seizures Ataxia Cranial Nerve
Produced by Agriculture and Extension Communications, Virginia Tech
 revised 2005 publication 420-036 Rabies: Its Ecology, Control, and Treatment Kari Signor, former student, Department of Fisheries and Wildlife Sciences, Virginia Tech James Parkhurst, associate professor,
revised 2005 publication 420-036 Rabies: Its Ecology, Control, and Treatment Kari Signor, former student, Department of Fisheries and Wildlife Sciences, Virginia Tech James Parkhurst, associate professor,
RABIES IMMUNOGLOBULIN. Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji Institute of Pharmacy, Nathdwara. (Raj.)
 Available online on www.ijarpb.com Review Article Received on 17/12/2013; Revised on 20/12/2014; Accepted 28/12/2013; Abstract RABIES IMMUNOGLOBULIN Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji
Available online on www.ijarpb.com Review Article Received on 17/12/2013; Revised on 20/12/2014; Accepted 28/12/2013; Abstract RABIES IMMUNOGLOBULIN Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji
Trichinosis Table of Contents
 Subsection: Trichinosis Page 1 of 9 Trichinosis Table of Contents Trichinosis Trichinosis (Trichinellosis) Fact Sheet Investigation of Trichinosis Surveillance Case Report (CDC 54.7) Subsection: Trichinosis
Subsection: Trichinosis Page 1 of 9 Trichinosis Table of Contents Trichinosis Trichinosis (Trichinellosis) Fact Sheet Investigation of Trichinosis Surveillance Case Report (CDC 54.7) Subsection: Trichinosis
Animal caused Injuries פגיעות בעלי חיים כל הזכויות שמורות למד"א מרחב ירושלים
 Animal caused Injuries פגיעות בעלי חיים Snake bite נחש In Israel there are 9 kinds of poisonous snakes. 3 mechanisms of venom action: Vascular Neurological Cardiac Small amount of venom goes through the
Animal caused Injuries פגיעות בעלי חיים Snake bite נחש In Israel there are 9 kinds of poisonous snakes. 3 mechanisms of venom action: Vascular Neurological Cardiac Small amount of venom goes through the
Dilemmas in the Management of Meningitis & Encephalitis HEADACHE AND FEVER. What is the best initial approach for fever, headache, meningisums?
 Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Appendix B: Provincial Case Definitions for Reportable Diseases
 Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: West Nile Virus Illness Revised March 2017 West Nile Virus Illness
Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: West Nile Virus Illness Revised March 2017 West Nile Virus Illness
2015 JUNIOR DISEASES
 2015 JUNIOR DISEASES EASY 2641 (easy) HS47/TH332 Q: What is an acute infection? A: Symptoms appear quickly 2642 (easy) HIH630-1/TH600 Q: What is another name for Equine Infectious Anemia? A: EIA OR swamp
2015 JUNIOR DISEASES EASY 2641 (easy) HS47/TH332 Q: What is an acute infection? A: Symptoms appear quickly 2642 (easy) HIH630-1/TH600 Q: What is another name for Equine Infectious Anemia? A: EIA OR swamp
Rabies. Issues for Travel. Kevin C. Kain MD Professor of Medicine, University of Toronto Director, Center for Travel and Tropical Medicine
 Rabies Issues for Travel Kevin C. Kain MD Professor of Medicine, University of Toronto Director, Center for Travel and Tropical Medicine Copyright 2017 by Sea Courses Inc. All rights reserved. No part
Rabies Issues for Travel Kevin C. Kain MD Professor of Medicine, University of Toronto Director, Center for Travel and Tropical Medicine Copyright 2017 by Sea Courses Inc. All rights reserved. No part
Introduction to Measles a Priority Vaccine Preventable Disease (VPD) in Africa
 Introduction to Measles a Priority Vaccine Preventable Disease (VPD) in Africa Nigeria Center for Disease Control Federal Ministry of Health Abuja July 2015 Outline 1. Measles disease 2. Progress towards
Introduction to Measles a Priority Vaccine Preventable Disease (VPD) in Africa Nigeria Center for Disease Control Federal Ministry of Health Abuja July 2015 Outline 1. Measles disease 2. Progress towards
Measles Update. March 16, 2015 Lisa Miller, MD, MSPH Communicable Disease Branch Chief Lynn Trefren MSN, RN Immunization Branch Chief
 Measles Update March 16, 2015 Lisa Miller, MD, MSPH Communicable Disease Branch Chief Lynn Trefren MSN, RN Immunization Branch Chief Colorado Department of Public Health and Environment Presenters have
Measles Update March 16, 2015 Lisa Miller, MD, MSPH Communicable Disease Branch Chief Lynn Trefren MSN, RN Immunization Branch Chief Colorado Department of Public Health and Environment Presenters have
Herpes B Virus Exposure Protocol
 Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Herpesviruses. -Recurrence: clinically obvious disease due to reactivation. **Reactivation and recurrence are used interchangeably.
 *Herpesviruses: A large group of viruses (100 strains), but we are concerned with only 8 strains as they are the only ones to infect human beings *herpesviruses groups: HSV-1 HSV-2 VZV CMV EBV HHV-6 HHV-7
*Herpesviruses: A large group of viruses (100 strains), but we are concerned with only 8 strains as they are the only ones to infect human beings *herpesviruses groups: HSV-1 HSV-2 VZV CMV EBV HHV-6 HHV-7
NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet)
 NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet) ASSESSMENT Prior to administration: Obtain complete health history including allergies, drug history, and possible drug interactions.
NURSING PROCESS FOCUS: Patients Receiving Amphotericin B (Fungizone, Abelcet) ASSESSMENT Prior to administration: Obtain complete health history including allergies, drug history, and possible drug interactions.
Novel H1N1 Influenza A Update. William Muth MD 2 Oct 2009
 Novel H1N1 Influenza A Update William Muth MD 2 Oct 2009 Novel H1N1 Influenza A Update Epidemiology Treatment Chemoprophylaxis Vaccine Infection Prevention Novel H1N1 Influenza A International Epidemiology
Novel H1N1 Influenza A Update William Muth MD 2 Oct 2009 Novel H1N1 Influenza A Update Epidemiology Treatment Chemoprophylaxis Vaccine Infection Prevention Novel H1N1 Influenza A International Epidemiology
LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION
 LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION Supawat Chatchen, Shakil Ibrahim, Pataporn Wisetsing and Kriengsak Limkittikul Department of Tropical Pediatrics,
LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION Supawat Chatchen, Shakil Ibrahim, Pataporn Wisetsing and Kriengsak Limkittikul Department of Tropical Pediatrics,
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
Guidance Document for the Management of Suspected Rabies Exposures
 Guidance Document for the Management of Suspected Rabies Exposures This document is in support of the Rabies Prevention and Control Protocol, 2008 (or as current) under the Ontario Public Health Standards.
Guidance Document for the Management of Suspected Rabies Exposures This document is in support of the Rabies Prevention and Control Protocol, 2008 (or as current) under the Ontario Public Health Standards.
Virus - Cannot reproduce. Uses the hosts cells to reproduce. 400 types of viruses are known.
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Infectious and Communicable Disease Revised: 11/2013 Infectious disease is illness caused by germ.
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Infectious and Communicable Disease Revised: 11/2013 Infectious disease is illness caused by germ.
Nervous System Defenses
 Chapter 19 Infectious Diseases: Nervous System Topics - Nervous System Defenses - Nervous System Diseases Nervous System Defenses Nervous system Normal flora 1 2 Nervous system Central nervous system (CNS)
Chapter 19 Infectious Diseases: Nervous System Topics - Nervous System Defenses - Nervous System Diseases Nervous System Defenses Nervous system Normal flora 1 2 Nervous system Central nervous system (CNS)
Mosquitoborne Viral Diseases
 Mosquitoborne Viral Diseases Originally prepared by Tom J. Sidwa, D.V.M, M.P.H State Public Health Veterinarian Zoonosis Control Branch Manager Texas Department of State Health Services 1 AGENT Viruses
Mosquitoborne Viral Diseases Originally prepared by Tom J. Sidwa, D.V.M, M.P.H State Public Health Veterinarian Zoonosis Control Branch Manager Texas Department of State Health Services 1 AGENT Viruses
12 June The average EVD case fatality rate has been around 50 per cent.
 12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
The pathogenesis of nervous distemper
 Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
UTSW/BioTel EMS TRAINING BULLETIN October EMS TB Ebola Virus Disease (EVD)
 UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
Orthomyxoviridae and Paramyxoviridae. Lecture in Microbiology for medical and dental medical students
 Orthomyxoviridae and Paramyxoviridae Lecture in Microbiology for medical and dental medical students Orthomyxoviridae and Paramyxoviridae are ss RNA containng viruses Insert Table 25.1 RNA viruses 2 SIZE
Orthomyxoviridae and Paramyxoviridae Lecture in Microbiology for medical and dental medical students Orthomyxoviridae and Paramyxoviridae are ss RNA containng viruses Insert Table 25.1 RNA viruses 2 SIZE
Aseptic meningitis: inflammation of meninges with sterile CSF (without any causative organisms which can be grown on culture media).
 You have to refer to the slides, since I have included the extra information only. Slide #1: Both illnesses aseptic meningitis and encephalitis can be caused by the same viruses; that viruses which cause
You have to refer to the slides, since I have included the extra information only. Slide #1: Both illnesses aseptic meningitis and encephalitis can be caused by the same viruses; that viruses which cause
Viral Vaccines I 5/17/04 LECTURE OUTLINE I. CASE HISTORY
 Viral Vaccines I I. CASE HISTORY LECTURE OUTLINE 5/17/04 A 22-year-old Amish woman became ill with a headache, fever, and generalized muscle pain. Two days later, she developed right and then left lower
Viral Vaccines I I. CASE HISTORY LECTURE OUTLINE 5/17/04 A 22-year-old Amish woman became ill with a headache, fever, and generalized muscle pain. Two days later, she developed right and then left lower
Disease Prevention in Horses
 Disease Prevention in Horses Dr. Laura Parisio BvetMed, MRCVS Sponsors Disease Prevention the big picture Vaccination Environmental Management Vaccination Which vaccines, which horses, when? Age Use Breed
Disease Prevention in Horses Dr. Laura Parisio BvetMed, MRCVS Sponsors Disease Prevention the big picture Vaccination Environmental Management Vaccination Which vaccines, which horses, when? Age Use Breed
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases
 Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases are caused by bacteria. Pneumococcal bacteria (Streptococcus pneumoniae) are the
Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases are caused by bacteria. Pneumococcal bacteria (Streptococcus pneumoniae) are the
The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003
 Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2011 The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003 Marilyn Goss Haskell
Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2011 The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003 Marilyn Goss Haskell
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
THIS ACTIVITY HAS EXPIRED. CME CREDIT IS NO LONGER AVAILABLE
 THIS ACTIVITY HAS EXPIRED. CME CREDIT IS NO LONGER AVAILABLE The following content is provided for informational purposes only. PREVENTION AND CONTROL OF INFLUENZA Lisa McHugh, MPH Influenza can be a serious
THIS ACTIVITY HAS EXPIRED. CME CREDIT IS NO LONGER AVAILABLE The following content is provided for informational purposes only. PREVENTION AND CONTROL OF INFLUENZA Lisa McHugh, MPH Influenza can be a serious
Thomas McGee, L.C. 920 Main Street, Suite 1700 Kansas City, MO (816) * Toll Free (800) WEST NILE VIRUS
 Thomas McGee, L.C. 920 Main Street, Suite 1700 Kansas City, MO 64105 (816) 842-4800 * Toll Free (800) 423-9044 www.thomasmcgee.com WEST NILE VIRUS What Is West Nile Virus (WNV)? Potentially serious illness
Thomas McGee, L.C. 920 Main Street, Suite 1700 Kansas City, MO 64105 (816) 842-4800 * Toll Free (800) 423-9044 www.thomasmcgee.com WEST NILE VIRUS What Is West Nile Virus (WNV)? Potentially serious illness
Structure of viruses
 Antiviral Drugs o Viruses are obligate intracellular parasites. o lack both a cell wall and a cell membrane. o They do not carry out metabolic processes. o Viruses use much of the host s metabolic machinery.
Antiviral Drugs o Viruses are obligate intracellular parasites. o lack both a cell wall and a cell membrane. o They do not carry out metabolic processes. o Viruses use much of the host s metabolic machinery.
Overview, Prevention, and Treatment of Rabies
 Overview, Prevention, and Treatment of Rabies Andrea Julia Nigg, Pharm.D., and Pamela L. Walker, Pharm.D. Each year, approximately 55,000 individuals worldwide die from an infection due to the rabies virus.
Overview, Prevention, and Treatment of Rabies Andrea Julia Nigg, Pharm.D., and Pamela L. Walker, Pharm.D. Each year, approximately 55,000 individuals worldwide die from an infection due to the rabies virus.
Neurosciences- Lecture 2 Virus associated meningitis Polio Virus
 Al- Balqa Applied University Faculty of Medicine Neurosciences- Lecture 2 Virus associated meningitis Polio Virus Dr. Hala Al Daghistani The most important Enteroviruses are the three poliovirus serotypes
Al- Balqa Applied University Faculty of Medicine Neurosciences- Lecture 2 Virus associated meningitis Polio Virus Dr. Hala Al Daghistani The most important Enteroviruses are the three poliovirus serotypes
Council of State and Territorial Epidemiologists Position Statement
 04-ID-01 Committee: Title: Infectious Disease Revision of the National Surveillance Case Definition of Diseases Caused by Neurotropic Domestic Arboviruses, Including the Addition to the NNDSS of Non-Neuroinvasive
04-ID-01 Committee: Title: Infectious Disease Revision of the National Surveillance Case Definition of Diseases Caused by Neurotropic Domestic Arboviruses, Including the Addition to the NNDSS of Non-Neuroinvasive
Viral Hepatitis. Background
 Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
West Nile Fever. F. Karup Pedersen 2012
 F. Karup Pedersen 2012 West Nile virus first isolated 1937 in West Nile district, Uganda Japanese encephalitis reconvalescens serum could neutralize West Nile virus Virus antigenically related to Japanese
F. Karup Pedersen 2012 West Nile virus first isolated 1937 in West Nile district, Uganda Japanese encephalitis reconvalescens serum could neutralize West Nile virus Virus antigenically related to Japanese
Advisory on Plague WHAT IS PLAGUE? 19 October 2017
 19 October 2017 Advisory on Plague WHAT IS PLAGUE? Plague is an infectious disease caused by the zoonotic bacteria, Yersinia pestis. This bacteria often infects small rodents (like rats, mice, and squirrels)
19 October 2017 Advisory on Plague WHAT IS PLAGUE? Plague is an infectious disease caused by the zoonotic bacteria, Yersinia pestis. This bacteria often infects small rodents (like rats, mice, and squirrels)
Aurora Health Care South Region EMS st Quarter CE Packet
 Name: Dept: Date: Aurora Health Care South Region EMS 2010 1 st Quarter CE Packet Meningitis Meningitis is an inflammatory disease of the leptomeninges. Leptomeninges refer to the pia matter and the arachnoid
Name: Dept: Date: Aurora Health Care South Region EMS 2010 1 st Quarter CE Packet Meningitis Meningitis is an inflammatory disease of the leptomeninges. Leptomeninges refer to the pia matter and the arachnoid
Chapters 21-26: Selected Viral Pathogens
 Chapters 21-26: Selected Viral Pathogens 1. DNA Viral Pathogens 2. RNA Viral Pathogens 1. DNA Viral Pathogens Smallpox (pp. 623-4) Caused by variola virus (dsdna, enveloped): portal of entry is the respiratory
Chapters 21-26: Selected Viral Pathogens 1. DNA Viral Pathogens 2. RNA Viral Pathogens 1. DNA Viral Pathogens Smallpox (pp. 623-4) Caused by variola virus (dsdna, enveloped): portal of entry is the respiratory
Canine Influenza FAQ. Questions, Answers, and Interim Guidelines
 Page 1 of 5 https://www.avma.org/kb/resources/faqs/pages/control-of-canine-influenza-in-dogs.aspx?pf=1 Canine Influenza FAQ Questions, Answers, and Interim Guidelines Updated April 22, 2015 Q: What is
Page 1 of 5 https://www.avma.org/kb/resources/faqs/pages/control-of-canine-influenza-in-dogs.aspx?pf=1 Canine Influenza FAQ Questions, Answers, and Interim Guidelines Updated April 22, 2015 Q: What is
SHASTA COUNTY Health and Human Services Agency
 FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
CE Unit. Viruses and Vaccines
 CE Unit Viruses and Vaccines DO NOT WRITE What is a virus? Have you ever had a virus? What is a vaccine? How is a virus different from bacteria? What are the deadliest viruses? 10. Dengue fever 50 million
CE Unit Viruses and Vaccines DO NOT WRITE What is a virus? Have you ever had a virus? What is a vaccine? How is a virus different from bacteria? What are the deadliest viruses? 10. Dengue fever 50 million
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
Control of Canine Influenza in Dogs Questions, Answers, and Interim Guidelines October 17, 2005
 Control of Canine Influenza in Dogs Questions, Answers, and Interim Guidelines October 17, 2005 The following document has been developed via consultation among the American Veterinary Medical Association,
Control of Canine Influenza in Dogs Questions, Answers, and Interim Guidelines October 17, 2005 The following document has been developed via consultation among the American Veterinary Medical Association,
INFLUENZA VIRUS. INFLUENZA VIRUS CDC WEBSITE
 INFLUENZA VIRUS INFLUENZA VIRUS CDC WEBSITE http://www.cdc.gov/ncidod/diseases/flu/fluinfo.htm 1 THE IMPACT OF INFLUENZA Deaths: PANDEMICS 1918-19 S p a n is h flu 5 0 0,0 0 0 U S 2 0,0 0 0,0 0 0 w o rld
INFLUENZA VIRUS INFLUENZA VIRUS CDC WEBSITE http://www.cdc.gov/ncidod/diseases/flu/fluinfo.htm 1 THE IMPACT OF INFLUENZA Deaths: PANDEMICS 1918-19 S p a n is h flu 5 0 0,0 0 0 U S 2 0,0 0 0,0 0 0 w o rld
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN. Active ingredient: Human proteins mg
 IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
TREATING THE REHAB PATIENT WITH WEST NILE VIRUS. Amy J. Wilson MD Medical Director, Baylor Institution of Rehabilitation January 2014
 TREATING THE REHAB PATIENT WITH WEST NILE VIRUS Amy J. Wilson MD Medical Director, Baylor Institution of Rehabilitation January 2014 FIGHT THE BITE! OBJECTIVES 1. Review local incidence of West Nile virus
TREATING THE REHAB PATIENT WITH WEST NILE VIRUS Amy J. Wilson MD Medical Director, Baylor Institution of Rehabilitation January 2014 FIGHT THE BITE! OBJECTIVES 1. Review local incidence of West Nile virus
Clinical Guidance for 2009 H1N1 Influenza and Seasonal Influenza. Barbara Wallace, MD New York State Department of Health (Updated 10/8/09)
 Clinical Guidance for 2009 H1N1 Influenza and Seasonal Influenza Barbara Wallace, MD New York State Department of Health (Updated 10/8/09) 1 Outline Clinical assessment Diagnostic testing Antiviral medications
Clinical Guidance for 2009 H1N1 Influenza and Seasonal Influenza Barbara Wallace, MD New York State Department of Health (Updated 10/8/09) 1 Outline Clinical assessment Diagnostic testing Antiviral medications
Khaled Ali Abu Ali. BSN. MPH. Ph.D. cand. -Nursing. Director of Epidemiology Department UCAS Lecturer
 Khaled Ali Abu Ali BSN. MPH. Ph.D. cand. Director of Epidemiology Department UCAS Lecturer -Nursing Khaled_abuali@yahoo.com Communicable Disease Surveillance during Gaza War, 214. Introduction Public Health
Khaled Ali Abu Ali BSN. MPH. Ph.D. cand. Director of Epidemiology Department UCAS Lecturer -Nursing Khaled_abuali@yahoo.com Communicable Disease Surveillance during Gaza War, 214. Introduction Public Health
Confirmed (Laboratory Tests) Serum positive for IgM anti-hbc or, hepatitis B surface antigen (HbsAg).
 Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA
 24 th December 2018 A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA BACKGROUND Zika virus infection, which erupted on a large scale in 2015-2016, has infected more than 1.5 million people.
24 th December 2018 A RELOOK AT ZIKA VIRAL INFECTION AND ITS LATEST OUTBREAK IN INDIA BACKGROUND Zika virus infection, which erupted on a large scale in 2015-2016, has infected more than 1.5 million people.
General HIV/AIDS Information
 General HIV/AIDS Information The History of HIV In the summer of 1981, physicians in San Francisco observed that young, previously healthy homosexual men were developing an unusual type of pneumonia which
General HIV/AIDS Information The History of HIV In the summer of 1981, physicians in San Francisco observed that young, previously healthy homosexual men were developing an unusual type of pneumonia which
