COCCIDIOIDES SPP. EXPOSURE/INJURY RESPONSE PROTOCOL
|
|
|
- Erika Stafford
- 6 years ago
- Views:
Transcription
1 PLEASE POST THIS PAGE IN AREAS WHERE COCCIDIOIDES IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENTAL HEALTH AND SAFETY/BIOSAFETY COCCIDIOIDES SPP. EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent: Exposure Risk: UCSF Occupational Health Services: Exposure Hotline Pager: Office of Environmental Health & Safety: Coccidioides spp. (Coccidioides immitis and posadasii) Coccidioidomycosis 415/ (Available during work hours) 415/ (Available 24 hours) 415/ (Main number; available during work hours) or (Available 24 hours) EH&S Public Health Officer: 415/ Biosafety Officer: 415/ PROTOCOL SUMMARY In the event of an accidental exposure or injury, the protocol is as follows: 1. Modes of Transmission: a. Skin puncture or injection b. Ingestion c. Contact with mucous membranes (eyes, nose, mouth) d. Contact with non-intact skin e. Exposure to aerosols f. Respiratory exposure involving inhalation of the mold/arthroconidia form 2. First Aid: a. Skin Exposure, immediately go to the sink and thoroughly wash the skin with soap and water. Decontaminate any exposed skin surfaces with an antiseptic scrub solution. b. Skin Wound, immediately go to the sink and thoroughly wash the wound with soap and water and pat dry. c. Splash to Eye(s), Nose or Mouth, immediately flush the area with running water for at least 5-10 minutes. d. Splash Affecting Garments, remove garments that may have become soiled or contaminated and place them in a double red plastic bag. 3. Treatment: a. In the event of an acute injury resulting from a laboratory incident where the injury requires immediate medical care, the injured employee/student should report to the emergency department for medical treatment. The injured individual must take a copy of this entire protocol document to the Emergency Department, including information regarding the specific strain associated with exposure. b. In the event of exposure, with or without an injury, call the Exposure Hotline in order to get access to medical care for the exposure. The Exposure Hotline responder will provide guidance to the injured individual on necessary medical treatment and post exposure follow-up. 4. Follow up is needed in the event of any Laboratory Exposure: a. After first aid has been administered, immediately inform your supervisor of the exposure. b. In the event of a large spill, contact the emergency response team (9-911) for clean-up. c. Contact Occupational Health Services, after first aid is complete, for follow-up care by contacting the Exposure Hotline. d. Contact the Biosafety Officer at 415/ to report the injury or exposure. 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 1 of 8
2 ROLES & RESPONSIBILITIES AFTER ACCIDENTAL EXPOSURE TO COCCIDIOIDES 1. WORKER S RESPONSIBILITIES (Employee/Student Initial Self-Care) a. First Aid: Perform the recommended first aid and decontamination according to the posted instructions. b. Treatment: i) In the event of an acute injury resulting from a laboratory incident which requires immediate medical care, the injured individual should report to the Emergency Department for acute medical treatment. ii) In the event of an exposure, with or without an injury, call the Exposure Hotline in order to get access to medical care for the exposure and evaluation for possible post exposure prophylaxis. c. Access to Exposure Hotline: Call the Exposure Hotline in order to get access to medical care for the exposure. Dial 415 / d. Reporting: Inform your laboratory supervisor / principal investigator of the exposure. Complete an Employee Incident Report Form ( e. Secure the laboratory: Identify the equipment involved in the exposure and the mechanism of exposure. Make sure that the laboratory area has been secured and that notification of contamination has been posted to prevent other individuals from entering the area. f. Follow up: Students and workers should contact Occupational Health Services (OHS) at 415 / for any needed follow up care. 2. SUPERVISOR S/PI S RESPONSIBILITIES a. First Aid and Decontamination: Verify that the worker has washed and decontaminated himself/herself. Ensure that appropriate medical treatment has been received. b. Secure the laboratory: Confirm that the laboratory area has been secured and that notification of contamination has been posted to prevent other individuals from entering the area. c. Laboratory clean-up (as needed): Contact the Office of Environmental Health & Safety (OEH&S) through the UC Police Department Emergency Dispatch (from a campus telephone 9-911, from a non-campus phone 415/ ). d. Report the exposure: Call the Biosafety Officer at 415/ during regular hours to discuss the exposure. A report summarizing any suspected Coccidioides exposure needs to be submitted to the Biosafety Committee by the Principal Investigator (PI). The report must include the following: A brief description of the exposure event, a description of the area involved, and the extent of employee exposure If applicable, specification of the amount of infectious material released, time involved, and explanation of procedures used to determine the amount involved Corrective action taken to prevent the re-occurrence of the incident Coccidioides decontamination procedures e. Follow Up: Confirm that the worker has called the Exposure Hotline and has scheduled for an appointment at the UCSF Occupational Health Clinic as necessary. f. Report the Injury: Within 24 hours, report the injury to the UCSF Human Resources Disability Management Services (HR DMS) Office on the Supervisor s Report of Injury (SRI) form, available here: 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 2 of 8
3 UNIVERSITY OF CALIFORNIA SAN FRANCISCO ENVIRONMENTAL HEALTH AND SAFETY INFECTIOUS SUBSTANCE DATA SHEET COCCIDIOIDES SPP. SECTION I Infectious Agent Organism or Agent: Coccidioides spp (immitis or posadasii) Synonym or Cross Reference: Coccidioidomycosis Characteristics: Dimorphic fungus, mold form in soil which produces infectious arthroconidia, spherule form in animals and human hosts SECTION II Recommended Precautions Containment Requirements: According to BMBL5: BSL-3 practices, containment equipment, and facilities are recommended for propagating and manipulating sporulating cultures already identified as Coccidioides spp. and for processing soil or other environmental materials known to contain infectious arthroconidia. UCSF Required Personal Protective Equipment: BSL 3 procedures for work involving the mold form, arthroconidia, and spherules. Use personal protective equipment standards as detailed in the Biosafety Use Authorization (BUA). SECTION III Handling Information Spills: Allow aerosols to settle; wearing protective clothing, gently cover spill with paper towel and apply 10% bleach (0.5% sodium hypochlorite) solution, starting at perimeter and working towards the center; allow sufficient contact time (30 min) before clean up. Disposal: Decontaminate waste contaminated with known or suspected Coccidioides in the mold form before disposal. Dispose as biohazardous waste. Storage: Store in sealed containers that are appropriately labeled. SECTION IV Health Hazards (from Canadian Pathogen Safety Data Sheet) Pathogenicity: The majority (around 60%) of individuals infected is asymptomatic or develops a very mild illness, with symptoms including cough, fever, arthralgias, myalgias, and fatigue that can last 2-6 weeks. Symptomatic individuals develop acute pneumonia or valley fever. In a small percentage of cases acute pneumonia can become chronic progressive pneumonia or pulmonary nodules and cavities can develop in the lungs, characterized by pneumonia, pleural effusion, and hilar lymphadenopathy. Dissemination occurs in 1% of infections and can affect the skin, lymph nodes, bones, and joints, causing systemic symptoms such as fever, cough, and night sweats. Meningitis is the most serious complication of coccidioidomycosis, with symptoms including headache, nausea, vomiting, and affected mental status. This may occur in 30-50% of disseminated infections, and is fatal without treatment. Coccidioidomyces infection may also lead to erythema nodosum, acute exanthema ( Toxic erythema ), erythema multiforme, Sweet s syndrome, and interstitial granulomatous dermatitis Epidemiology: Coccidioides spp. are geographically limited to the alkaline soil of semiarid climates, and in regions with hot, dry summers, and low annual rainfall. C. immitis is confined mainly to California, whereas C. posadasii occurs in the southwestern United States, northern Mexico and areas of Central and South America. The major risk factor for infection is environmental exposure to dust and soil. Disseminated infection is more common among black, Asian or Filipino individuals, pregnant women in the third trimester and immunocompromised individuals. Host Range: Humans, nearly all mammals, and some reptiles. Infectious Dose: Estimated to be 1-10 arthroconidia per Canadian MSDS. 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 3 of 8
4 Modes of Transmission: Inhalation of arthroconidia, although secondary transmission via fomites and organ transplants may occur. Incubation Period: 1 to 3 weeks, although some infections are asymptomatic. Communicability: Not contagious but has occasionally been transmitted from person-to-person via fomites or organ transplants. SECTION V Viability Drug Susceptibility: Susceptible to amphotericin B and the azole group of antifungal drugs including fluconazole, itraconazole, voriconazole, and posaconazole. Drug resistance is uncommon. Susceptibility to Disinfectants: Susceptible to 1:10 dilution of bleach, 6% hydrogen peroxide, 8% formaldehyde or 3% phenolics with a contact time of 20 minutes or more. Physical Inactivation: Fungi in soil can be inactivated by heat at 120 ºC for 30 minutes. Survival Outside Host: Coccidioidal arthroconidia are hardy and can survive for long periods of time on inanimate surfaces. They can grow in the soil in semiarid climates. FOR THE USE OF THE EXPOSURE HOTLINE SECTION VI Medical Surveillance: Monitor for symptoms. Diagnosis of coccidioidomycosis can be established using serologic, histopathologic and culture methods. Skin tests can be used to identify the disease. Any pregnant or immunocompromised worker should be evaluated by an infectious disease specialist. First Aid/Treatment: Coccidioidomycosis is generally self-limiting and will resolve without treatment. Disseminated infections, or patients who experience excessive morbidity, should be treated with antifungal medication. The type of drug and length of treatment depends on the site of infection and clinical response. Immunization: None. Prophylaxis: Exposed personnel should be given fluconazole (400 mg daily for 6 weeks). 1. Prophylaxis Recommended For: a Significant inhalational exposure to arthroconidia. b Percutaneous injury with Coccidiodies, materials contaminated by Coccidioides, or mucous membrane exposure. 2. Prophylaxis Considered For: a Potential inhalational exposures to arthroconidia in individuals with risk factors for development of systemic disease. b Potential mucous membrane exposure. 3. Prophylaxis Not Recommended For: a Intact skin exposure associated with the spherule form of Coccidiodies, where there is no inhalation or percutaneous or mucous membrane exposure. Medication: Fluconazole 400 mg once daily, given with food, for 6 weeks. This drug may have significant side effects and multiple drug interactions. Fluconazole is contraindicated in pregnancy. If there is any question regarding early pregnancy, a pregnancy test should be performed before starting prophylaxis. The person who was exposed will need close follow up in UCSF Occupational Health Services. Further details on prophylactic treatment schedules and follow up as recommended by Stevens, D. A., Clemons, K. V., Levine, H. B., Pappagianis, D., Baron, E. J., Hamilton, J. R., et al. (2009) are outlined on page 5. Reporting: All laboratory exposures must be reported to the Biosafety Officer. Any known cases of coccidioides exposure must be reported to the Public Health Officer. Reporting to the San Francisco Department of Public Health is not required. 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 4 of 8
5 SECTION VII Laboratory Hazards LABORATORY-ACQUIRED INFECTIONS: 93 cases of laboratory-acquired coccidioidomycosis infections and two deaths were reported prior to An additional 15 cases were asymptomatic but identified with skin tests during that period. One symptomatic case was reported from SOURCES / SPECIMENS: Lower respiratory tract samples, cerebrospinal fluid, sputum, skin and visceral lesions, and soil samples from infected areas (southwestern United States, parts of Central and South America). PRIMARY HAZARD: Inhalation of spores, parenteral inoculation or contact with mucous membranes. SPECIAL HAZARD: None. FOR THE USE OF THE EMERGENCY DEPARTMENT SECTION VIII Emergency Medical Treatment Treatment Indications: Emergency department treatment will be required for injuries that require immediate medical care. The treatment needs to consist of the following: 1) decontaminate and debride wound, 2) repair wound, 3) consult with infectious disease specialist for high risk exposure, 4) contact the Exposure Hotline to discuss the need to start post exposure prophylaxis, if indicated (see section VI above), and 4) have patient follow up with UCSF-OHS. For significant exposures, baseline labs should be drawn. Specific information below is summarized from Stevens, D. A., Clemons, K. V., Levine, H. B., Pappagianis, D., Baron, E. J., Hamilton, J. R., et al. (2009). Expert opinion: what to do when there is Coccidioides exposure in a laboratory. Clinical Infectious Diseases : an Official Publication of the Infectious Diseases Society of America, 49(6), doi: / Baseline serum samples should be obtained promptly from exposed persons. These samples should be stored for future testing for coccidioidal immunoglobulin G and M antibodies by an experienced laboratory. Persons with prior exposures are at a lower risk of infection. All potentially exposed persons should be given a therapeutic dose of oral fluconazole (400mg daily for adults) for 6 weeks. Pregnant Women Azoles are considered teratogenic, making infection in pregnant women more complicated and the results of greater concern. If it is certain the pregnant woman was exposed, she should be treated with a prophylactic dose of intravenous amphotericin B therapy (which is safe during pregnancy) once a week until the pregnancy has concluded (then azoles could be given instead); the 6-week period concluded without any sign of coccidioidal disease; or coccidiodial infection was confirmed (then daily administration of amphotericin would be recommended). If it is uncertain if the pregnant woman was exposed, it is recommended to observe her health until coccidioidal symptoms appear at which time she should be treated with intravenous amphotericin B therapy. Post Exposure Period The potentially exposed persons should be monitored during the 6weeks of prophylaxis and for some months after. If the person was to develop a fever or cough, the persons should visit a clinician, specifying a possible exposure to Coccidioides. Retesting initial serum samples may be necessary, as the development of coccidioidal seropositivity can be delayed. 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 5 of 8
6 If the person receiving azole is diagnosed with a primary infection, then several months of treatment should be considered, in combination with an alternative antifungal agent. It is also recommended then to use an intravenous amphotericin B preparation, because no other azoles have the favorable clinical experience as itraconazole and fluconazole has in treating coccidioidal infection. In vitro susceptibility testing of an isolate could also be useful in choosing a therapeutic option. Patients with disseminated coccidioidomycosis would require longer-term therapy and follow up If there is no clinical suspicion of coccidiodomycosis after the 6week prophylaxis period, testing for coccidioidal immunoglobulin G and M antibodies along with concurrent baseline serum samples should be performed. If there is there is no seroconversion, prophylaxis can be stopped. If there is serological evidence of a subclinical infection prophylaxis can probably also be stopped, although continuing treatment may be considered for those with comorbidities or other risk factors. Natural exposures to Coccidioides may result in undiagnosed primary infections and disease arising later. It is then recommended that individuals with Coccidioides exposure, subclinical or not, be observed for one year for the possibility of developing disseminated disease. Exposure Indications: In the event of an exposure, with or without an injury, the Exposure Hotline must be called. SECTION VIII References Stevens, D. A., Clemons, K. V., Levine, H. B., Pappagianis, D., Baron, E. J., Hamilton, J. R., et al. (2009). Expert opinion: what to do when there is Coccidioides exposure in a laboratory. Clinical Infectious Diseases : an Official Publication of the Infectious Diseases Society of America, 49(6), doi: / /27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 6 of 8
7 Appendix I. CDC/NIH RECOMMENDATIONS FOR LABORATORY EXPOSURE TO COCCIDIOIDES Coccidioides immitis and Coccidioides posadasii Coccidioides spp. is endemic to lower sonoran deserts of the western hemisphere including northern Mexico, southern Arizona, central and southern California, and west Texas. The original species (C. immitis) has been divided into C. immitis and C. posadasii. These species are dimorphic fungal pathogens existing in nature and in laboratory cultures at room temperature as filamentous molds with asexual spores (single-cell arthroconidia three to five microns in size) that are the infectious particles that convert to spherules under the appropriate culture conditions in vitro at 37 C and in vivo in warmblooded animals. Occupational Infections Laboratory-associated coccidioidomycosis is a documented hazard of working with sporulating cultures of Coccidioides spp. Occupational exposure has also been associated in endemic regions with archeology and high dust exposure. Attack rates for laboratory and occupational exposure are higher than for ambient exposure when large numbers of spores are inhaled. Smith reported that 28 of 31 (90%) laboratory-associated infections in his institution resulted in clinical disease, whereas more than half of infections acquired in nature were asymptomatic. Risk of respiratory infection from exposure to infected tissue or aerosols of infected secretions is very low. Accidental percutaneous inoculation has typically resulted in local granuloma formation. Natural Modes of Infection Single spores can produce ambient infections by the respiratory route. Peak exposures occur during arid seasons. Coccidioides spp. grow in infected tissue as larger multicellular spherules, up to 70 microns in diameter and pose little or no risk of infection from direct exposure. The majority of ambient infections is subclinical and results in life-long protection from subsequent exposures. The incubation period is one to three weeks and manifests as a community-acquired pneumonia with immunologically mediated fatigue, skin rashes, and joint pain. One of the synonyms for coccidioidomycosis is desert rheumatism. A small proportion of infections is complicated by hematogenous dissemination from the lungs to other organs, most frequently skin, the skeleton, and the meninges. Disseminated infection is much more likely in persons with cellular immunodeficiencies (AIDS, organ transplant recipient, lymphoma). Laboratory Safety and Containment Recommendations Because of their size, the arthroconidia are conducive to ready dispersal in air and retention in the deep pulmonary spaces. The much larger size of the spherule considerably reduces the effectiveness of this form of the fungus as an airborne pathogen. Spherules of the fungus may be present in clinical specimens and animal tissues, and infectious arthroconidia in mold cultures and soil or other samples from natural sites. Inhalation of arthroconidia from environmental samples or cultures of the mold form is a serious laboratory hazard. Personnel should be aware that infected animal or human clinical specimens or tissues stored or shipped in such a manner as to promote germination of arthroconidia pose a theoretical laboratory hazard. BSL-2 practices, containment equipment, and facilities are recommended for handling and processing clinical specimens, identifying isolates, and processing animal tissues. ABSL-2 practices, containment equipment, and facilities are recommended for experimental animal studies when the route of challenge is parenteral. BSL-3 practices, containment equipment, and facilities are recommended for propagating and manipulating sporulating cultures already identified as Coccidioides spp. and for processing soil or 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 7 of 8
8 other environmental materials known to contain infectious arthroconidia. Experimental animal studies should be done at BSL-3 when challenge is via the intranasal or pulmonary route. Special Issues Transfer of Agent: Importation of this agent may require CDC and/or USDA importation permits. Domestic transport of this agent may require a permit from USDA/APHIS/VS. A DoC permit may be required for the export of this agent to another country. See Appendix C of BMBL5 for additional information. Taken directly from: 6/27/2016 UCSF Coccidioides spp. Exposure/Injury Protocol for Research Laboratories Page 8 of 8
BLASTOMYCES DERMATITIDIS EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE BLASTOMYCES DERMATITIDIS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY BLASTOMYCES DERMATITIDIS
PLEASE POST THIS PAGE IN AREAS WHERE BLASTOMYCES DERMATITIDIS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY BLASTOMYCES DERMATITIDIS
POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE POLIOVIRUSES ARE USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
PLEASE POST THIS PAGE IN AREAS WHERE POLIOVIRUSES ARE USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
HISTOPLASMA CAPSULATUM EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE HISTOPLASMA CAPSULATUM IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HISTOPLASMA CAPSULATUM EXPOSURE/INJURY
PLEASE POST THIS PAGE IN AREAS WHERE HISTOPLASMA CAPSULATUM IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HISTOPLASMA CAPSULATUM EXPOSURE/INJURY
PLEASE POST THIS PAGE IN AREAS WHERE TUBERCULOSIS IS USED
 PLEASE POST THIS PAGE IN AREAS WHERE TUBERCULOSIS IS USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT HEALTH AND SAFETY/BIOSAFETY TUBERCULOSIS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
PLEASE POST THIS PAGE IN AREAS WHERE TUBERCULOSIS IS USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT HEALTH AND SAFETY/BIOSAFETY TUBERCULOSIS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED
 PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED Organism or Agent: UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HUMAN IMMUNODEFICIENCY VIRUS (HIV) SIMIAN IMMUNODEFICIENCY
PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED Organism or Agent: UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HUMAN IMMUNODEFICIENCY VIRUS (HIV) SIMIAN IMMUNODEFICIENCY
UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE HERPES SIMPLEX VIRUS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY
PLEASE POST THIS PAGE IN AREAS WHERE HERPES SIMPLEX VIRUS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY
1918 Influenza; Influenza A, H1N1. Basic agent information. Section I- Infectious Agent. Section II- Dissemination
 1918 Influenza; Influenza A, H1N1 Basic agent information Section I- Infectious Agent Risk Group: - RG3 Synonym or Cross reference: - Spanish Flu - 1918 Flu - El Grippe Characteristics: - SELECT AGENT
1918 Influenza; Influenza A, H1N1 Basic agent information Section I- Infectious Agent Risk Group: - RG3 Synonym or Cross reference: - Spanish Flu - 1918 Flu - El Grippe Characteristics: - SELECT AGENT
Overview of Coccidioidomycosis (Valley Fever) Stephen Munday, MD MPH Imperial County Public Health May 21, 2013
 Overview of Coccidioidomycosis (Valley Fever) Stephen Munday, MD MPH Imperial County Public Health May 21, 2013 Objectives Assess the epidemiology of Coccidioidomycosis (aka Valley Fever) Describe the
Overview of Coccidioidomycosis (Valley Fever) Stephen Munday, MD MPH Imperial County Public Health May 21, 2013 Objectives Assess the epidemiology of Coccidioidomycosis (aka Valley Fever) Describe the
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1
 Page 1 of 8 RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1 The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure compliance with both the
Page 1 of 8 RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1 The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure compliance with both the
Chapter 7 8/23/2016. Asepsis and Infection Control. Asepsis. Asepsis (Cont.) Microorganisms. Infection control and prevention
 Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT HEALTH AND SAFETY/BIOSAFETY DIPHTHERIA TOXIN EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE DIPHTHERIA TOXIN IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT HEALTH AND SAFETY/BIOSAFETY DIPHTHERIA TOXIN EXPOSURE/INJURY RESPONSE
PLEASE POST THIS PAGE IN AREAS WHERE DIPHTHERIA TOXIN IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT HEALTH AND SAFETY/BIOSAFETY DIPHTHERIA TOXIN EXPOSURE/INJURY RESPONSE
3/16/16 COCCIDIOIDOMYCOSIS COCCIDIOIDOMYCOSIS COCCIDIOIDOMYCOSIS COCCIDIOIDOMYCOSIS COCCIDIOIDOMYCOSIS COCCIDIOIDOMYCOSIS. Selected References
 10 MARCH 2006 Updated 5 June 2008 Updated 11 February 2011 Updated 4 March 2016 Herbert Boro, M.D., F.A.C.P. Selected References 1. Fiese, Marshall J. 1958. Coccidioidomycosis. Charles C. Thomas. 253 pp.
10 MARCH 2006 Updated 5 June 2008 Updated 11 February 2011 Updated 4 March 2016 Herbert Boro, M.D., F.A.C.P. Selected References 1. Fiese, Marshall J. 1958. Coccidioidomycosis. Charles C. Thomas. 253 pp.
Bloodborne Pathogens. General
 Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
Bloodborne Pathogens
 Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Title: Public Health Reporting and National Notification for Coccidioidomycosis
 10-ID-04 Committee: Infectious Diseases Title: Public Health Reporting and National Notification for Coccidioidomycosis I. Statement of the Problem: In 1994, CSTE passed a resolution recommending key federal
10-ID-04 Committee: Infectious Diseases Title: Public Health Reporting and National Notification for Coccidioidomycosis I. Statement of the Problem: In 1994, CSTE passed a resolution recommending key federal
Center for Vaccine Biology and Immunology. Cell Sorting Facility Laboratory Safety Manual. Updated: January 25, 2012
 Center for Vaccine Biology and Immunology Cell Sorting Facility Laboratory Safety Manual Updated: January 25, 2012 I. Standard Laboratory Rules The standard BSL-2 precautions are outlined in the University
Center for Vaccine Biology and Immunology Cell Sorting Facility Laboratory Safety Manual Updated: January 25, 2012 I. Standard Laboratory Rules The standard BSL-2 precautions are outlined in the University
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Fungal Diseases of the Respiratory System
 Fungal Diseases of the Respiratory System Histoplasmosis(cave disease) Dr. Hala Al Daghistani Histoplasmosis is a disease caused by the fungus Histoplasma capsulatum. Histoplasma capsulatum, is usually
Fungal Diseases of the Respiratory System Histoplasmosis(cave disease) Dr. Hala Al Daghistani Histoplasmosis is a disease caused by the fungus Histoplasma capsulatum. Histoplasma capsulatum, is usually
California digging. Task 1 Interpret the chest radiograph. L. Hendriks
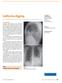 Case history An18-yr-old male presented at the emergency department with a 4-week history of fever, coughing and dyspnoea. Symptoms presented on a holiday in California (USA) searching the desert for fossils.
Case history An18-yr-old male presented at the emergency department with a 4-week history of fever, coughing and dyspnoea. Symptoms presented on a holiday in California (USA) searching the desert for fossils.
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
Bloodborne Pathogens For School Employees
 Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
DRUG INFORMATION ALERT
 Paul Davis From: Sent: To: Subject: TSHP Friday, December 20, 2013 4:03 AM paul.davis@tshp.org 12-20-2013 Drug Info Alert - Unseen Danger: Dust-Born Disease DRUG INFORMATION ALERT
Paul Davis From: Sent: To: Subject: TSHP Friday, December 20, 2013 4:03 AM paul.davis@tshp.org 12-20-2013 Drug Info Alert - Unseen Danger: Dust-Born Disease DRUG INFORMATION ALERT
METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF
 Mary Pack Arthritis Program METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF Handling of premixed injectable Methotrexate (MTX) by employees who are pregnant, breast-feeding or attempting to reproduce
Mary Pack Arthritis Program METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF Handling of premixed injectable Methotrexate (MTX) by employees who are pregnant, breast-feeding or attempting to reproduce
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT
 AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Coccidioidomycosis Update for Primary Care
 Coccidioidomycosis Update for Primary Care SW Conference on Medicine April 26, 2018 John N Galgiani MD University of Arizona What Is? Caused by soil fungi Coccidioides immitis Coccidioides posadasii Other
Coccidioidomycosis Update for Primary Care SW Conference on Medicine April 26, 2018 John N Galgiani MD University of Arizona What Is? Caused by soil fungi Coccidioides immitis Coccidioides posadasii Other
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS
 INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
Bloodborne Pathogens Training For School Personnel
 Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens. Aaron Holmberg, Risk Manager. ARM, MBA, OSHA Authorized Outreach Trainer February 2018
 Bloodborne Pathogens Aaron Holmberg, Risk Manager ARM, MBA, OSHA Authorized Outreach Trainer February 2018 What s This About? Infectious microorganisms (viruses and diseases) found in blood and bodily
Bloodborne Pathogens Aaron Holmberg, Risk Manager ARM, MBA, OSHA Authorized Outreach Trainer February 2018 What s This About? Infectious microorganisms (viruses and diseases) found in blood and bodily
CDC Health Advisory 04/29/2009
 H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
Coping with Valley Fever Information for Families
 Coping with Valley Fever Information for Families Valley Children s Healthcare & University of California, Merced 9300 Valley Children s Place Madera, CA 93636 Social Worker: Margie Arreguin-Zarate, LCSW
Coping with Valley Fever Information for Families Valley Children s Healthcare & University of California, Merced 9300 Valley Children s Place Madera, CA 93636 Social Worker: Margie Arreguin-Zarate, LCSW
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
RESEARCH WITH MIDDLE EAST RESPIRATORY SYNDROME CORONAVIRUS (MERS-CoV)
 Page 1 of 5 RESEARCH WITH SYNDROME CORONAVIRUS (MERS-CoV) The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure that all Federal, State, and
Page 1 of 5 RESEARCH WITH SYNDROME CORONAVIRUS (MERS-CoV) The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure that all Federal, State, and
Bloodborne Pathogens LVHN s Annual Safety Course
 Slide 1 Bloodborne Pathogens LVHN s Annual Safety Course Nucleus Medical Media (2010). Blood Carries Nutrients. Smart Imagebase. Lehigh Valley Health Network cares about your safety especially about protecting
Slide 1 Bloodborne Pathogens LVHN s Annual Safety Course Nucleus Medical Media (2010). Blood Carries Nutrients. Smart Imagebase. Lehigh Valley Health Network cares about your safety especially about protecting
Bloodborne Infectious Diseases
 Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
Doc No: BLOOD Midland Engineering Co., Inc. Initial Issue Date 12/04/15 Safety Management System
 Revision Preparation: Safety Mgr Authority: President Issuing Dept: Safety Page: Page 1 of 15 INTRODUCTION The Occupational Safety and Health Administration (OSHA) has a variety of regulations that all
Revision Preparation: Safety Mgr Authority: President Issuing Dept: Safety Page: Page 1 of 15 INTRODUCTION The Occupational Safety and Health Administration (OSHA) has a variety of regulations that all
Life Threatening Vocational Hazards Diseases and Toxins
 Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
 Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Coccidioidomycosis, aka Valley Fever
 Coccidioidomycosis, aka Valley Fever Presented to the California Partnership for the San Joaquin Valley June 15, 2018 Karen Haught, MD, MPH Public Health Officer Tulare County Public Health Coccidioidomycosis
Coccidioidomycosis, aka Valley Fever Presented to the California Partnership for the San Joaquin Valley June 15, 2018 Karen Haught, MD, MPH Public Health Officer Tulare County Public Health Coccidioidomycosis
Prevention and Control of Healthcare-Associated Norovirus
 Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training
 Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
SAFETY DATA SHEET. Phone: Phone: Emergency Phone:
 SAFETY DATA SHEET SECTION 1. IDENTIFICATION Catalog #: 60-9549-0 Product Name: HIV Rapid Test Control Pack Synonyms: The Chembio HIV Reactive/Nonreactive Controls are quality control reagents for use with
SAFETY DATA SHEET SECTION 1. IDENTIFICATION Catalog #: 60-9549-0 Product Name: HIV Rapid Test Control Pack Synonyms: The Chembio HIV Reactive/Nonreactive Controls are quality control reagents for use with
SUBJECT: Management of Human Body Fluids/Waste (Bloodborne Pathogens)
 Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Bloodborne Pathogen Refresher Training
 Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Bloodborne Pathogens Training. Compliance with OSHA Standard 29 CFR
 Bloodborne Pathogens Training Compliance with OSHA Standard 29 CFR 1910.1030 This Training Will Cover Introduction to the OSHA Standard 29 CFR 1910.1030 Epidemiology, symptoms and modes of transmission
Bloodborne Pathogens Training Compliance with OSHA Standard 29 CFR 1910.1030 This Training Will Cover Introduction to the OSHA Standard 29 CFR 1910.1030 Epidemiology, symptoms and modes of transmission
British Columbia Institute of Technology. BCIT Safety Manual SARS VIRUS EXPOSURE CONTROL PLAN
 BCIT Safety Manual SARS VIRUS EXPOSURE CONTROL PLAN Contents 1. Introduction... 2 2. Purpose... 2 3. Definitions... 2 3.1 Severe Acute Respiratory Syndrome (SARS)... 2 3.2 Incubation Period... 2 3.3 Occupational
BCIT Safety Manual SARS VIRUS EXPOSURE CONTROL PLAN Contents 1. Introduction... 2 2. Purpose... 2 3. Definitions... 2 3.1 Severe Acute Respiratory Syndrome (SARS)... 2 3.2 Incubation Period... 2 3.3 Occupational
Environmental Health and Safety Offices BLOODBORNE PATHOGENS
 Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
Bloodborne Pathogens and Regulated Medical Waste
 Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
UCP BloodBorne Pathogens Recertification
 UCP BloodBorne Pathogens Recertification 1 OSHA Occupational Safety and Health Administration: a. In 1991 OSHA established Bloodborne Pathogen Standard 29 CFR 1910.1030. b. Set code of conduct / limit
UCP BloodBorne Pathogens Recertification 1 OSHA Occupational Safety and Health Administration: a. In 1991 OSHA established Bloodborne Pathogen Standard 29 CFR 1910.1030. b. Set code of conduct / limit
Safety Committee Prototypical Safety Program Manual
 1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
PUBLIC HEALTH SIGNIFICANCE SEASONAL INFLUENZA AVIAN INFLUENZA SWINE INFLUENZA
 INFLUENZA DEFINITION Influenza is an acute highly infectious viral disease characterized by fever, general and respiratory tract catarrhal manifestations. Influenza has 3 Types Seasonal Influenza Avian
INFLUENZA DEFINITION Influenza is an acute highly infectious viral disease characterized by fever, general and respiratory tract catarrhal manifestations. Influenza has 3 Types Seasonal Influenza Avian
SAM HOUSTON STATE UNIVERSITY ENVIRONMENTAL HEALTH, SAFETY & RISK MANAGMENT
 BLOODBORNE PATHOGENS PROGRAM I. PURPOSE The SHSU Bloodborne Pathogens program ensures SHSU compliance with Occupational Safety and Health (OSHA) Standard, 29 CFR 1910.1030, Blood Borne Pathogens. II. SCOPE
BLOODBORNE PATHOGENS PROGRAM I. PURPOSE The SHSU Bloodborne Pathogens program ensures SHSU compliance with Occupational Safety and Health (OSHA) Standard, 29 CFR 1910.1030, Blood Borne Pathogens. II. SCOPE
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
Herpes B Virus Exposure Protocol
 Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees
 BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
Biosafety in the Animal Setting. Tina Bogac Institutional Biosafety Officer
 Biosafety in the Animal Setting Tina Bogac Institutional Biosafety Officer May 27, 2009 Biohazards and Biosafety Risk groups/risk assessment Biosafety/animal biosafety levels Essential work practices Biosafety
Biosafety in the Animal Setting Tina Bogac Institutional Biosafety Officer May 27, 2009 Biohazards and Biosafety Risk groups/risk assessment Biosafety/animal biosafety levels Essential work practices Biosafety
Bloodborne Pathogens Training. July 26, 2012
 Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens]
![BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens] BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens]](/thumbs/73/68341667.jpg) BLOODBORNEPATHOGENS CAP Safety Meetings Revision: 10-2011 2011 Copyright - PEC/Premier Safety Management, Inc. All Rights Reserved Revision: [10-2011] 1 THEBLOODBORNEPATHOGENSSTANDARD The Bloodborne Pathogens
BLOODBORNEPATHOGENS CAP Safety Meetings Revision: 10-2011 2011 Copyright - PEC/Premier Safety Management, Inc. All Rights Reserved Revision: [10-2011] 1 THEBLOODBORNEPATHOGENSSTANDARD The Bloodborne Pathogens
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Miami Dade County Public Schools
 Miami Dade County Public Schools Bloodborne Pathogens Training 2017 ARTHUR J. GALLAGHER & CO. AJG.COM Objectives Introduction to bloodborne pathogens Types of bloodborne pathogens Who is at risk? Exposure
Miami Dade County Public Schools Bloodborne Pathogens Training 2017 ARTHUR J. GALLAGHER & CO. AJG.COM Objectives Introduction to bloodborne pathogens Types of bloodborne pathogens Who is at risk? Exposure
Chapter 13. Preventing Infection. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Infection Prevention Special Needs Shelters. Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC
 Infection Prevention Special Needs Shelters Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC Infection Prevention: Objectives and Your Role Know the client population and its impact on the special needs shelter
Infection Prevention Special Needs Shelters Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC Infection Prevention: Objectives and Your Role Know the client population and its impact on the special needs shelter
Safety Tips from the WorkSafe People
 Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
You will now begin the Bloodborne Pathogen Refresher Training.
 You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
Infectious Disease and Bloodborne Pathogens Training St. Michael-Albertville Public Schools
 Infectious Disease and Bloodborne Pathogens Training St. Michael-Albertville Public Schools Questions? Any time throughout the slide show or throughout the school year: Contact Jake Baxter at IEA Phone:
Infectious Disease and Bloodborne Pathogens Training St. Michael-Albertville Public Schools Questions? Any time throughout the slide show or throughout the school year: Contact Jake Baxter at IEA Phone:
Harvard University Exposure Control Plan
 Harvard University Exposure Control Plan Harvard University is committed to providing a safe and healthy work environment. In accordance with this goal, the Occupational Health and Safety Administration
Harvard University Exposure Control Plan Harvard University is committed to providing a safe and healthy work environment. In accordance with this goal, the Occupational Health and Safety Administration
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE
 PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING
 Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION
 TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
CHAPTER 7 Medical/Surgical Asepsis and Infection Control
 CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
Infection Control. Copyright 2011, 2007, 2003, 1999 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Infection Control Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Describe the characteristics of pathogenic microorganisms and the diseases they cause. Apply the chain-of-infection
Infection Control Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Describe the characteristics of pathogenic microorganisms and the diseases they cause. Apply the chain-of-infection
Chapter 12. Preventing Infection. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Supervisors, Department Heads and Principals will:
 The Greater Victoria School District is committed to each student s success in learning within a responsive and safe environment. REGULATION 4213 UNIVERSAL PRECAUTIONS Preamble Universal Precautions are
The Greater Victoria School District is committed to each student s success in learning within a responsive and safe environment. REGULATION 4213 UNIVERSAL PRECAUTIONS Preamble Universal Precautions are
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Goldenrod Hills Community Action. Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR
 Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
Chapter 11 PREVENTING INFECTION. Elsevier items and derived items 2010 by Mosby, Inc. an affiliate of Elsevier Inc. All rights reserved
 Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
USE OF PERSONAL PROTECTION EQUIPMENT. Standard and Isolation precautions Ana M. Bonet 6/2017
 USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
Dare County Schools. Bloodborne Pathogens Exposure Control Plan
 Dare County Schools Bloodborne Pathogens Exposure Control Plan 2017 Dare County Schools Bloodborne Pathogens Exposure Control Page 1 of 12 Dare County Schools Bloodborne Pathogen Program Purpose An infection
Dare County Schools Bloodborne Pathogens Exposure Control Plan 2017 Dare County Schools Bloodborne Pathogens Exposure Control Page 1 of 12 Dare County Schools Bloodborne Pathogen Program Purpose An infection
Infection Control Update
 Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT
 ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT During an influenza pandemic, adherence to infection control practices is extremely important to prevent transmission of influenza.
ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT During an influenza pandemic, adherence to infection control practices is extremely important to prevent transmission of influenza.
The University of Texas at El Paso BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN
 The University of Texas at El Paso BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN Table of Contents SCOPE... 3 DEFINITIONS... 3 EXPOSURE DETERMINATION... 3 METHODS OF COMPLIANCE... 4 HEPATITIS B VACCINATION
The University of Texas at El Paso BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN Table of Contents SCOPE... 3 DEFINITIONS... 3 EXPOSURE DETERMINATION... 3 METHODS OF COMPLIANCE... 4 HEPATITIS B VACCINATION
Mike Olbinski. Mike Olbinski. Michael Olbinski
 Mike Olbinski Mike Olbinski Michael Olbinski Table of Contents List of Figures and Tables... 3 Executive Summary... 4 Introduction... 5 Epidemiology in Arizona... 7 Reporting Sources and Changes in Laboratory
Mike Olbinski Mike Olbinski Michael Olbinski Table of Contents List of Figures and Tables... 3 Executive Summary... 4 Introduction... 5 Epidemiology in Arizona... 7 Reporting Sources and Changes in Laboratory
CHEROKEE COUNTY SCHOOL DISTRICT
 For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
OSHA Bloodborne Pathogens Standard. Universal Precautions
 Building a Safer Workplace OSHA Bloodborne Pathogens Standard Universal Precautions Bloodborne Pathogens Bloodborne pathogens are micro-organisms in the bloodstream that cause diseases. Bloodborne Pathogens
Building a Safer Workplace OSHA Bloodborne Pathogens Standard Universal Precautions Bloodborne Pathogens Bloodborne pathogens are micro-organisms in the bloodstream that cause diseases. Bloodborne Pathogens
Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home
 Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home The following is a summary of guidelines developed to
Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home The following is a summary of guidelines developed to
Bloodborne Pathogens Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Scope and Application This Bloodborne Pathogens Exposure Control Plan (ECP) is designed to minimize the potential for occupational exposure to bloodborne pathogens
Bloodborne Pathogens Exposure Control Plan Scope and Application This Bloodborne Pathogens Exposure Control Plan (ECP) is designed to minimize the potential for occupational exposure to bloodborne pathogens
